Peritonitis: Diagnosis of PD Peritonitis
Diunggah oleh
Fathur Rahman Mutiara Hikmah0 penilaian0% menganggap dokumen ini bermanfaat (0 suara)
35 tayangan7 halamanhih
Judul Asli
p4
Hak Cipta
© © All Rights Reserved
Format Tersedia
DOC, PDF, TXT atau baca online dari Scribd
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen Inihih
Hak Cipta:
© All Rights Reserved
Format Tersedia
Unduh sebagai DOC, PDF, TXT atau baca online dari Scribd
0 penilaian0% menganggap dokumen ini bermanfaat (0 suara)
35 tayangan7 halamanPeritonitis: Diagnosis of PD Peritonitis
Diunggah oleh
Fathur Rahman Mutiara Hikmahhih
Hak Cipta:
© All Rights Reserved
Format Tersedia
Unduh sebagai DOC, PDF, TXT atau baca online dari Scribd
Anda di halaman 1dari 7
PERITONITIS
Peritonitis is a serious complication of peritoneal dialysis. Repeated episodes of peritonitis
may be implicated in early failure of the peritoneal membrane and subsequent failure of
peritoneal dialysis.
Guidelines provide a framework around which an individual patient's management can be
based, but must be interpreted in light of the clinical condition of each patient. It is suggested
that guidelines be reviewed every year to ensure they remain up to date. he !edical
"irector and attending physicians should make all medication decisions and approve any
guidelines.
Diagnosis of PD Peritonitis
#. $ymptoms and signs of peritonitis
%bdominal pain
&ausea and vomiting
'onstipation or diarrhea
(ever
Rebound tenderness
)lood leucocytosis
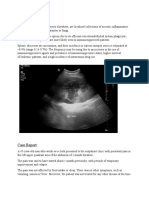
*. 'loudy P" fluid with P" +hite cell count ,#--.mm/ 0,1-2 polymorphonuclear
neutrophils is supportive of the diagnosis of microbial3induced peritonitis4.
0P" fluid is clear and colourless before draining in. P" effluent should be clear but
may be 5yellow6 in colour. 5'loudy6 fluid looks like
5Pineapple 7uice6 and it is difficult to read te8t through the bag.4
'auses of cloudy dialysate
Infective peritonitis 3 bacterial, fungal, ), other
'ulture &egative peritonitis
$econdary to other intra3abdominal pathology 3 diverticulitis, appendicitis,
perforated bowel, abscess, transcolonic migration of catheter
9osinophilic peritonitis 3 %symptomatic cloudy dialysate fluid with ,#12
eosinophils on differential cell count
BLOODSTAINED PD FLUID
$ometimes seen in females during menstruation is common and harmless. It can also
happen if the small blood vessels in the peritoneum break 0e.g. lifting something heavy,
playing sports4. It usually clears quickly in a few e8changes but patients should be seen if
the fluid is very bloody or not clearing or they are unwell in any way. Initial investigations
should include e8clusion of peritonitis, abdominal film and consideration of surgical review.
MANAGEMENT
Peritonitis is a potentially life3threatening condition. In the presence of cloudy
fluid and.or abdominal pain and.or fever prompt initiation of antibiotic therapy
is needed.
#. !easure and record )P 0lying and standing4, pulse and temperature.
*. % sample of the appropriate 0i.e., , : hours' dwell time4 dialysate effluent should be
obtained for laboratory evaluation including a cell count with differential, Gram stain,
and culture.
/. 98amine e8it site; swab if there appears to be e8it site infection and send for e8it site
wound culture. 98amine tunnel for evidence of tunnel infection.
:. 'heck for patient allergies.
1. Review recent episodes of peritonitis and e8it site infections.
<. (lush peritoneum per protocol or physician order.
=. 'hange catheter e8tension set.
>. 'ommence empirical antibiotics per protocol or physician order.
?. 'hoice of final therapy should always be guided by antibiotic sensitivities.
PROPHYLACTIC ANTIBIOTICS FOLLOWING ACCIDENTAL TOUCH
CONTAMINATION
(ollowing a break in sterile technique call physician for antibiotic orders and change the
patient@s catheter e8tension set before any further e8changes are performed.
FREUENCY OF CULTURES
It is important to obtain the first cloudy effluent for culture. he probability of positive
diagnostic culture is greatest from this specimen. Patients should be instructed, therefore, to
bring the first cloudy fluid to the laboratory immediately. %fter the initial culture, repeat
effluent cultures are not recommended if the cell count is decreasing appropriately and the
patient is responding symptomatically. If cell counts are either rising or not decreasing
appropriately by / days, repeat cultures should be taken and management guidelines should
be consulted.
INITIAL EMPIRIC ANTIBIOTIC SELECTION
If the effluent sediment Gram stain suggests gram3positive bacteria, a gram3negative
organism, or is unavailable, delayed, or negative for any specific organisms, empiric therapy
is indicated 0I$P" Guidelines.Recommendations %dult Peritoneal "ialysis3 Related Peritonitis reatment
RecommendationsA *--- Bpdate able *4. o prevent routine use of Cancomycin and thus prevent
emergence of resistant organisms, it is recommended that a first3generation 'ephalosporin,
for e8ample, 'efaDolin or 'ephalothin 0# g daily in the long dwell4, in combination with
'eftaDidime # g be initiated. hese antibiotics can be mi8ed in the same dialysate bag as
either loading or maintenance doses, without significant loss of bioactivity. 0I$P"
Guidelines.Recommendations %dult Peritoneal "ialysis3 Related Peritonitis reatment RecommendationsA *--- Bpdate able
/4.
0(or more on medication selection please see I$P" Guidelines.Recommendations %dult Peritoneal "ialysis3 Related Peritonitis
reatment RecommendationsA *--- Bpdate httpA..www.ispd.org4
SAMPLE! PERITONITIS MEDICATION GUIDELINES
IP Cancomycin single dose, dwell <hours #.1g if E<- kg body weight
*.-g if ,<- kg body weight
'iproflo8acin 1--mg PF )I" 8 : days
IP Geparin #--- units per e8change
: days 0continue until bags clear and no fibrin clots present4
&oteA 'iproflo8acin should be taken * hours before calcium and iron preparations 0e.g.
ums, Phoslo4 as they interfere with absorption.
SAMPLE! Peritonitis Protocol
'linical diagnosis of P" peritonitis, no e8it site, no tunnel infection
9mpirical treatment
Fral 'iproflo8acin 1-- mg bid
FR IP Gentamicin -.<mg.kg.day if vomiting4
IP Cancomycin *g0,<- kg4 #.1g 0E<- kg4 single dose
0then review4
IP Geparin #---u in each e8change
%fter 'ultures receivedA
Gram positives inc. 9nterococcus,
$taph
Pseudomonas, yeast, mi8ed gram
negative and culture negative
0$pecial cases, see detailed
protocols.call for specific orders4
Gram negatives 0e8cept
Pseudomonas4
$top 'iproflo8acin.Gentamicin
Give day = Cancomycin, same dose
#: days oral 'iproflo8acin.
&o further Cancomycin
If $taph aureusA
H 'onsider Rifampicin and.or
(luclo8acillin
H give day = and #: Cancomycin.
If recurrent $taph epidermidisA
H give day = and #: vancomycin.
Laboratory Follow up
#. "ay four of therapyA
Repeat cell counts and differential
Repeat routine culture and sensitivity
'onfirm sensitivies
Ideal specimen is overnight dwell
!ore laboratory tests may be ordered PR& patient's status
*. (our days after completion of therapy
(inal cell count and differential
(inal routine cultures
E"IT SITE INFECTION
%n e8it site infection is defined by the presence of purulent drainage with or without
erythema of the skin at the catheter3epidermal interface. 98it3site and tunnel infections are
important because they may lead to refractory or relapsing peritonitis and subsequent
catheter loss.
A#$te E%it&Site Infe#tion is defined as purulent and.or bloody drainage from the e8it site,
which may be associated with erythema, tenderness, e8uberant granulation tissue, and
edema 0wardowski and Prowant, #??<b4. he erythema is more than twice the catheter
diameter and there is regression of the epithelium in the sinus. %n acute catheter infection
may be accompanied by pain and the presence of a scab, but crusting alone is not indicative
of infection
C'roni# E%it&Site Infe#tions may be the result of an untreated or inadequately treated
acute infection. It may also be a sequela of a resolved acute infection, which recurs after
withdrawal of antibiotic therapy. $ymptoms of chronic infection are similar to those of acute
infections; however, e8uberant granulation tissue is more common both e8ternally and in the
sinus. Granulation tissue at the e8ternal e8it is sometimes covered by a large stubborn crust
or scab. Pain, erythema, and swelling are frequently absent in chronic infection.
An E($i)o#a* E%it Site is defined as purulent and.or bloody drainage only in the sinus that
cannot be e8pressed outside, accompanied by regression of the epithelium and the
occurrence of slightly e8uberant granulation tissue in the sinus. 9rythema may be present
but with a diameter less than twice the width of the catheter. Pain, swelling, and e8ternal
drainage is absent 0wardowski and Prowant, #??<b4. he equivocal infected e8it site
represents low3grade infection. %lthough some equivocal e8its improve spontaneously, most
progress to overt infection if untreated.
T$nne* Infe#tion is defined as erythema, edema, and.or tenderness over the subcutaneous
pathway, and may be characteriDed by intermittent or chronic, purulent, bloody, or gooey
drainage which discharges spontaneously or after pressure on the cuff. unnel infections are
often occult 0Plum et al., #??:4 and can sometimes be detected by ultrasonography of the
subcutaneous pathway 0Plum et al., #??:; Golley et al., #?>?4. !ost, but not all, tunnel
infections occur in association with e8it3site infections. Gere the risk for subsequent
peritonitis is increased.
Tra$+ati,e- E%it Site appearances depend on the intensity of the trauma and the time
interval until e8amination. 'ommon features are pain, bleeding, scab, and deterioration of
e8it appearance.
Pat'ogens! $taph. %ureus is responsible for the ma7ority of e8it3site and tunnel infections.
Pseudo. %eruginosa is much less common, but like $taph. %ureus is difficult to eradicate and
frequently leads to peritonitis if catheter removal is delayed. $taph. 9pidermidis is a relatively
infrequent cause of tunnel infection in contrast to peritonitis. Fther gram3positive organisms,
other gram3negative bacilli, and, rarely, fungi account for the remaining infections.
E%it&Site C$*t$res! within * I : weeks after catheter implantation, bacteria coloniDe almost
all e8it sites. Positive cultures from normal3appearing e8it sites indicate coloniDation, not
infection. +henever possible, the cultures should be taken from the e8udate 0wardowski
and Prowant #??<a, #??<c4. 'ultures should only be taken from abnormal3looking e8it sites
$elected Readings
International $ociety Ff Peritoneal "ialysis http://www.ispd.org
I$P" Guidelines.Recommendations %dult Peritoneal "ialysis3 Related Peritonitis reatment RecommendationsA *--- Bpdate
wardowski JK, Prowant )(. 98it3site study methods and results. Perit "ial Int #??<a; #<0$uppl /4A$<I/#.
wardowski JK, Prowant )(. 'lassification of normal and diseased e8it sites. Perit "ial Int #??<b; #<0$uppl /4A$/*I1-.
Plum K, $udkamp $, Grabensee ). Results of ultrasound3assisted diagnosis of tunnel infections in '%P". %m K Lidney "is
#??:; */A??I#-:.
Golley KG, (oulkes 'K, !ers %G, +illard ". Bltrasound as a tool in the diagnosis and management of e8it3site infections in
patients undergoing '%P". %m K Lidney "is #?>?; #:A*##I#<.
Reviewed: 06-2011
Hngklslgfs
Lngls
Nlsmg
Hkgs
Lsnkg
Lknlkg
Lnf
kjnsf
S
Mg
Knvxdgvd
Jjfd
Bnxdlgvd
Lklks
Kjkj
Ch
Fhtfvj
Vnvj
Fdxfd
Gfxgfxg
Bchbb
Hcbcv
Anda mungkin juga menyukai
- Peritonitis: Diagnosis of PD PeritonitisDokumen7 halamanPeritonitis: Diagnosis of PD PeritonitisFathur Rahman Mutiara HikmahBelum ada peringkat
- Peritonitis: Diagnosis of PD PeritonitisDokumen7 halamanPeritonitis: Diagnosis of PD PeritonitisFathur Rahman Mutiara HikmahBelum ada peringkat
- Peritonitis: Diagnosis of PD PeritonitisDokumen7 halamanPeritonitis: Diagnosis of PD PeritonitisFathur Rahman Mutiara HikmahBelum ada peringkat
- Peritonitis: Diagnosis of PD PeritonitisDokumen7 halamanPeritonitis: Diagnosis of PD PeritonitisFathur Rahman Mutiara HikmahBelum ada peringkat
- Case 013: Fever in A Cirrhotic PatientDokumen5 halamanCase 013: Fever in A Cirrhotic PatientFitri 1997Belum ada peringkat
- Pathogens: Hepatic AbscessDokumen8 halamanPathogens: Hepatic Abscessalberto cabelloBelum ada peringkat
- Peritonitis: Presentan: FAUZAN AKBAR YUSYAHADI - 12100118191Dokumen21 halamanPeritonitis: Presentan: FAUZAN AKBAR YUSYAHADI - 12100118191Fauzan Fourro100% (1)
- Management of Adult Febrile Neutropenia: 15011500-10123 99 Street Edmonton, Alberta T5J 3H1Dokumen4 halamanManagement of Adult Febrile Neutropenia: 15011500-10123 99 Street Edmonton, Alberta T5J 3H1Tio Prima SBelum ada peringkat
- PeritonitisDokumen28 halamanPeritonitisdea_p27Belum ada peringkat
- Liver AbsesDokumen8 halamanLiver AbsesS FznsBelum ada peringkat
- Urinary Tract InfectionsDokumen46 halamanUrinary Tract InfectionsNino PeterBelum ada peringkat
- EMPYEMADokumen27 halamanEMPYEMAMark Bin S. DilangalenBelum ada peringkat
- Hepatology 04Dokumen7 halamanHepatology 04Fedhi As'adi THearthiefBelum ada peringkat
- Epidemiology of Infectious Disease Amebiasis: University of Fallujah College of Medicine Community MedicineDokumen7 halamanEpidemiology of Infectious Disease Amebiasis: University of Fallujah College of Medicine Community MedicineMohamed HamoodBelum ada peringkat
- Amebic Liver Abscess Diagnosis and Treatment ReviewDokumen3 halamanAmebic Liver Abscess Diagnosis and Treatment ReviewKerin VictoriaBelum ada peringkat
- Coliforms: Causative Agents DiseaseDokumen3 halamanColiforms: Causative Agents DiseaseShanelle Fia LomboyBelum ada peringkat
- Oncologic Emergencies: SepsisDokumen4 halamanOncologic Emergencies: SepsisPilar KrammBelum ada peringkat
- General care of the peritonitis patientDokumen7 halamanGeneral care of the peritonitis patientRadenJeremySoeriawidjajaBelum ada peringkat
- Amebiasis LECDokumen67 halamanAmebiasis LECfraolBelum ada peringkat
- Diagnosis and Treatment of Urinary Tract Infections in ChildrenDokumen7 halamanDiagnosis and Treatment of Urinary Tract Infections in ChildrenmahendraBelum ada peringkat
- 1.7B AppendixDokumen4 halaman1.7B AppendixDulce Kriselda E. FaigmaniBelum ada peringkat
- Urinalysis (Ua) and The Diagnosis of UtisDokumen5 halamanUrinalysis (Ua) and The Diagnosis of UtisErawati ArmayaniBelum ada peringkat
- Pleural Effusion TypesDokumen3 halamanPleural Effusion Typesshaifullah9219Belum ada peringkat
- Acute or Chronic Penetrate: PyloriDokumen5 halamanAcute or Chronic Penetrate: PyloriSidBelum ada peringkat
- Allergy Immunology (3) (MedicalBooksVN - Com)Dokumen9 halamanAllergy Immunology (3) (MedicalBooksVN - Com)malbertal1Belum ada peringkat
- 17 Urological InfectionsDokumen18 halaman17 Urological InfectionsntadudulBelum ada peringkat
- Abdomen Agudo Qco1Dokumen10 halamanAbdomen Agudo Qco1María Paula Boada EscandónBelum ada peringkat
- Enterocutaneous FistulaDokumen4 halamanEnterocutaneous Fistulaeglatine100% (1)
- SBP Investigation and TreatmentDokumen3 halamanSBP Investigation and TreatmentBaihaqi SaharunBelum ada peringkat
- URINARY TRACT INFECTION - FinalDokumen86 halamanURINARY TRACT INFECTION - FinalShreyance Parakh100% (2)
- InTech-Perforated AppendicitisDokumen18 halamanInTech-Perforated Appendicitismelinda tannousBelum ada peringkat
- Abdominal ParacentesisDokumen5 halamanAbdominal Paracentesisw wBelum ada peringkat
- Infectious Endophthalmitis After: CataractDokumen6 halamanInfectious Endophthalmitis After: CataractSurendar KesavanBelum ada peringkat
- Acute AppendicitisDokumen25 halamanAcute Appendicitisnura100% (1)
- Hepatic Abscess Diagnosis and TreatmentDokumen8 halamanHepatic Abscess Diagnosis and TreatmentAngieBelum ada peringkat
- Causes, Signs and Symptoms of Dengue Fever and Typhoid FeverDokumen24 halamanCauses, Signs and Symptoms of Dengue Fever and Typhoid FeverrefkyjuliandriBelum ada peringkat
- Nursing Interventions for Prostate Cancer Client with Back PainDokumen3 halamanNursing Interventions for Prostate Cancer Client with Back PainKathleen Joy PingenBelum ada peringkat
- Syphilis: Etiology, Pathogenesis, Transmission, Stages, Manifestations and TreatmentDokumen39 halamanSyphilis: Etiology, Pathogenesis, Transmission, Stages, Manifestations and TreatmentEINSTEIN2D100% (1)
- I. Urinary Tract Infections Overview: A. Acute Uncomplicated UTI in WomenDokumen13 halamanI. Urinary Tract Infections Overview: A. Acute Uncomplicated UTI in WomenDominique VioletaBelum ada peringkat
- Infections in DialysisDokumen20 halamanInfections in DialysisZiad LalmiBelum ada peringkat
- 260-Article Text-875-1-10-20220728Dokumen4 halaman260-Article Text-875-1-10-20220728hasan andrianBelum ada peringkat
- Typhoid Fever: Causes, Symptoms, Diagnosis and TreatmentDokumen5 halamanTyphoid Fever: Causes, Symptoms, Diagnosis and TreatmentElvisBelum ada peringkat
- Elizabeth King I ADokumen3 halamanElizabeth King I AAlba UrbinaBelum ada peringkat
- Liver Abscess DissertationDokumen4 halamanLiver Abscess DissertationPayForAPaperAtlanta100% (1)
- A Case of Acute IdiopathicDokumen19 halamanA Case of Acute IdiopathicSAIMA BATOOLBelum ada peringkat
- 338 Typhoid Enteric FeverDokumen6 halaman338 Typhoid Enteric FeverSurbhi ThakurBelum ada peringkat
- Signs, Symptoms and Treatment of AppendicitisDokumen14 halamanSigns, Symptoms and Treatment of AppendicitisMary Joy BunuanBelum ada peringkat
- QuinsyDokumen10 halamanQuinsyAmr ElmarasyBelum ada peringkat
- UTIDokumen17 halamanUTIBongkotchakorn Mind PhonchaiBelum ada peringkat
- Tuberculosis Pleural Effusion - Management: Introduction: ETBDokumen29 halamanTuberculosis Pleural Effusion - Management: Introduction: ETBLeonardo AraujoBelum ada peringkat
- Urinary Tract Infection, Complicated (UTI) - Johns Hopkins ABX GuideDokumen5 halamanUrinary Tract Infection, Complicated (UTI) - Johns Hopkins ABX GuideLaoMed plusBelum ada peringkat
- EntericDokumen17 halamanEntericToqeer HussainBelum ada peringkat
- Infeksi Saluran KemihDokumen6 halamanInfeksi Saluran KemihGabreilla HanochBelum ada peringkat
- Typhoid Ileal Perforation: DR - ArifusmanDokumen28 halamanTyphoid Ileal Perforation: DR - ArifusmanMudassar SaeedBelum ada peringkat
- Updated Guideline On Diagnosis and TreatmentDokumen5 halamanUpdated Guideline On Diagnosis and TreatmentRidho WahyutomoBelum ada peringkat
- Radiology Case Report - Splenic AbscessDokumen6 halamanRadiology Case Report - Splenic AbscessAbeebBelum ada peringkat
- Leptospirosis: Cavite State University Indang, CaviteDokumen9 halamanLeptospirosis: Cavite State University Indang, CavitePatricia Marie MojicaBelum ada peringkat
- Onc EmergenciesDokumen4 halamanOnc EmergencieslanamdBelum ada peringkat
- Agranulocytosis, A Simple Guide to The Condition, Diagnosis, Treatment And Related ConditionsDari EverandAgranulocytosis, A Simple Guide to The Condition, Diagnosis, Treatment And Related ConditionsBelum ada peringkat
- Female Urinary Tract Infections in Clinical PracticeDari EverandFemale Urinary Tract Infections in Clinical PracticeBob YangBelum ada peringkat
- When We Were Young ChordDokumen3 halamanWhen We Were Young ChordFathur Rahman Mutiara HikmahBelum ada peringkat
- P 24 OppDokumen9 halamanP 24 OppFathur Rahman Mutiara HikmahBelum ada peringkat
- P 24Dokumen8 halamanP 24Fathur Rahman Mutiara HikmahBelum ada peringkat
- P 24Dokumen8 halamanP 24Fathur Rahman Mutiara HikmahBelum ada peringkat
- Peritonitis: Diagnosis of PD PeritonitisDokumen7 halamanPeritonitis: Diagnosis of PD PeritonitisFathur Rahman Mutiara HikmahBelum ada peringkat
- Pathogenesis SJSDokumen10 halamanPathogenesis SJSCritikal AcclaimBelum ada peringkat
- Nephrology PDFDokumen74 halamanNephrology PDFthejbond100% (1)
- Dailymed - Nlm.nih - Gov METRONIDAZOLEDokumen16 halamanDailymed - Nlm.nih - Gov METRONIDAZOLELip StickBelum ada peringkat
- IRMDokumen11 halamanIRMPfunzo Jeffrey MunyaiBelum ada peringkat
- CRF TextbookDokumen5 halamanCRF TextbookThirdie LacorteBelum ada peringkat
- SOAP Note - Peter The DeanDokumen5 halamanSOAP Note - Peter The DeanWu TracyBelum ada peringkat
- New Insights in Dialysis Membrane BiocompatibilityDokumen7 halamanNew Insights in Dialysis Membrane BiocompatibilityDani ursBelum ada peringkat
- 4008 GBDokumen8 halaman4008 GBrulodiBelum ada peringkat
- Telephone No. 333-2273/ 260-0543/ 260-5782 Email AddressDokumen10 halamanTelephone No. 333-2273/ 260-0543/ 260-5782 Email AddressCHARIEMAE CA�AZARESBelum ada peringkat
- Topical Issues in Anesthesia 2016Dokumen207 halamanTopical Issues in Anesthesia 2016Ketzalzin DmgBelum ada peringkat
- Hypertension in Hemodialysis PatientDokumen54 halamanHypertension in Hemodialysis PatientIchtiar MahesaBelum ada peringkat
- Belco Formula User ManualDokumen386 halamanBelco Formula User ManualMahmoud Diaa100% (21)
- NP4 ExamDokumen14 halamanNP4 ExamArnie Jude CaridoBelum ada peringkat
- Dry Weight in HemodialysisDokumen12 halamanDry Weight in HemodialysisAnik PriyaniBelum ada peringkat
- 5130 w08 QP 1Dokumen16 halaman5130 w08 QP 1mstudy123456Belum ada peringkat
- Hesi Practice QuestionsDokumen31 halamanHesi Practice QuestionsEbookslatinosEbookslatinos75% (12)
- Restless Legs SyndromDokumen9 halamanRestless Legs Syndromakhmad afifBelum ada peringkat
- Chapter 3 Separation Processes (Unit Operations)Dokumen10 halamanChapter 3 Separation Processes (Unit Operations)almutaz9879Belum ada peringkat
- Day 7-12 Rules For LifeDokumen26 halamanDay 7-12 Rules For LifeLuna DonjuánBelum ada peringkat
- Kajian Ilmiah CKD KDIGO 2012Dokumen27 halamanKajian Ilmiah CKD KDIGO 2012giggs_libraBelum ada peringkat
- Capstone Project Desktop Version 270519Dokumen22 halamanCapstone Project Desktop Version 270519api-385688041Belum ada peringkat
- Kavikuyil G: Clinical Research - Clinical Data Management - Pharmacovigilance - Medical Chart ReviewDokumen3 halamanKavikuyil G: Clinical Research - Clinical Data Management - Pharmacovigilance - Medical Chart Reviewmubarak patelBelum ada peringkat
- A Clinical Review of Peritoneal DialysisDokumen14 halamanA Clinical Review of Peritoneal DialysisClinicaVeterinariaCorhuilaBelum ada peringkat
- 4008S (NG) Op 04 12 10 SW 11 10 enDokumen318 halaman4008S (NG) Op 04 12 10 SW 11 10 enPAPPU RANJITH KUMAR100% (10)
- Pediatric NephrologyDokumen147 halamanPediatric Nephrologyj100% (1)
- RenalDokumen54 halamanRenalUSC Upstate Nursing Coaches100% (1)
- Activity Packet V 4Dokumen15 halamanActivity Packet V 4api-300831071Belum ada peringkat
- ROL - Dialysis ResearchDokumen4 halamanROL - Dialysis ResearchTukki TukkiBelum ada peringkat
- Dialysis: Prepared byDokumen31 halamanDialysis: Prepared byVimal PatelBelum ada peringkat
- Causes and Treatment of Renal FailureDokumen50 halamanCauses and Treatment of Renal FailureASHRAFQOTMOSH100% (2)
- Acute Renal Failure Lecture 1 Critical Care NursingDokumen52 halamanAcute Renal Failure Lecture 1 Critical Care NursingDina Rasmita100% (2)