s12916 014 0178 2
Diunggah oleh
Muhammad Sukri JafarJudul Asli
Hak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
s12916 014 0178 2
Diunggah oleh
Muhammad Sukri JafarHak Cipta:
Format Tersedia
Goldschneider et al.
BMC Medicine 2014, 12:178
http://www.biomedcentral.com/1741-7015/12/178
GUIDELINE
Open Access
Pain care for patients with epidermolysis bullosa:
best care practice guidelines
Kenneth R Goldschneider1*, Julie Good2, Emily Harrop3, Christina Liossi4,5, Anne Lynch-Jordan6, Anna E Martinez7,
Lynne G Maxwell8 and Danette Stanko-Lopp9
Abstract
Background: Inherited epidermolysis bullosa (EB) comprises a group of rare disorders that have multi-system effects
and patients present with a number of both acute and chronic pain care needs. Effects on quality of life are substantial.
Pain and itching are burdensome daily problems. Experience with, and knowledge of, the best pain and itch care for
these patients is minimal. Evidence-based best care practice guidelines are needed to establish a base of knowledge and
practice for practitioners of many disciplines to improve the quality of life for both adult and pediatric patients with EB.
Methods: The process was begun at the request of Dystrophic Epidermolysis Bullosa Research Association International
(DEBRA International), an organization dedicated to improvement of care, research and dissemination of knowledge for
EB patients worldwide. An international panel of experts in pain and palliative care who have extensive experience
caring for patients with EB was assembled. Literature was reviewed and systematically evaluated. For areas of care
without direct evidence, clinically relevant literature was assessed, and rounds of consensus building were conducted.
The process involved a face-to-face consensus meeting that involved a family representative and methodologist, as well
as the panel of clinical experts. During development, EB family input was obtained and the document was reviewed by
a wide variety of experts representing several disciplines related to the care of patients with EB.
Results: The first evidence-based care guidelines for the care of pain in EB were produced. The guidelines are clinically
relevant for care of patients of all subtypes and ages, and apply to practitioners of all disciplines involved in the care of
patients with EB. When the evidence suggests that the diagnosis or treatment of painful conditions differs between
adults and children, it will be so noted.
Conclusions: Evidence-based care guidelines are a means of standardizing optimal care for EB patients, whose disease is
often times horrific in its effects on quality of life, and whose care is resource-intensive and difficult. The guideline
development process also highlighted areas for research in order to improve further the evidence base for future care.
Keywords: Epidermolysis bullosa, Pain, Practice guidelines, RDEB, DEBRA, Acute pain, Chronic pain, Recessive dystrophic
epidermolysis bullosa, Dystrophic Epidermolysis Bullosa Research Association International
Background
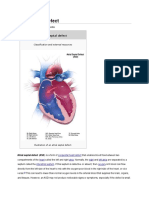
Inherited epidermolysis bullosa (EB) comprises a group of
rare disorders, generally thought of as skin diseases. However, EB has multi-system effects and patients present with
a number of both acute and chronic pain care needs [1].
Effects on quality of life are substantial [2,3]. Due to its
low prevalence, expertise in pain care for patients with this
disease is often restricted to a few specialized care centers.
* Correspondence: Kenneth.goldschneider@cchmc.org
1
Pain Management Center, Department of Anesthesiology, Cincinnati Childrens
Hospital Medical Center, Cincinnati, Ohio, USA
Full list of author information is available at the end of the article
Even then, evidence-based pain care is limited by a near
absence of scientific literature specific to EB. This set of
guidelines was requested by Dystrophic Epidermolysis
Bullosa Research Association International (DEBRA International) to help standardize the approach to pain care for
both adult and pediatric patients with EB in all parts of
the world. Consequently, a group of clinical pain care experts from a few countries have come together to lend
their experience to the limited scientific literature to create these guidelines.
The present guidelines on pain care for patients with
EB are based on a review and synthesis of the available
2014 Goldschneider et al.; licensee BioMed Central Ltd. This is an Open Access article distributed under the terms of the
Creative Commons Attribution License (http://creativecommons.org/licenses/by/2.0), which permits unrestricted use,
distribution, and reproduction in any medium, provided the original work is properly credited. The Creative Commons Public
Domain Dedication waiver (http://creativecommons.org/publicdomain/zero/1.0/) applies to the data made available in this
article, unless otherwise stated.
Goldschneider et al. BMC Medicine 2014, 12:178
http://www.biomedcentral.com/1741-7015/12/178
literature, guided by expert consensus and thoughtful
application of theory. The guidelines are divided into
four topics: psychological treatment of pain and pruritus,
acute pain, chronic and recurrent pain, and special
topics. The Psychological and Integrative Treatments
section leads off because the information it contains
applies to all the topics that follow. The Acute Pain
section focuses on postoperative pain. The Chronic
and Recurrent Pain section includes dressing changes,
baths, skin pain and joint and other body pains. The
Special Topics section includes pain care in infants
with EB and pain care at the end of life. While not pain
per se, itching is a major source of discomfort [4] and
is also discussed.
The aim of the guidelines is to provide the user with
information on pain care for children and adults with
EB. These guidelines can be applied to all patients diagnosed with hereditary forms of EB. Patients with acquired forms are not included in the guidelines. The
guidelines contain two types of guidance. Recommendations are graded and highlighted in text boxes at the end
of the manuscript. Good Practice Points are located at
the end of each topical section and summarize concepts
and best practices, based on the clinical experience of
the guidelines development group.
The daily routine of many patients with severe forms
of EB will have a number of painful events, each of
which may suggest the need for intervention. However,
addressing each one pharmacologically may lead to a
level of sedation that prevents a meaningful level of
productivity. It is important to discuss the needs of the
patient and the options for caring for those needs with
the patient and family. Together, the patient, family and
practitioner can transform the guidelines into an individualized care plan. It is to be expected that each patients
needs will be dynamic; periodic review of the needs and
goals will optimize care at each step of the patients life.
Of note, the term EB will be used throughout the
text. However, four major types of EB are known and
are categorized as Simplex (EBS), Junctional (JEB), dystrophic types (DEB) and Kindler Syndrome. A recent
consensus statement was released that reclassified the
subtypes further based on anatomic location within the
skin and pattern of involvement, and discouraged the use
of eponyms (with the exception of Kindler Syndrome).
EBS is sub-typed as EBS suprabasal and EBS basal, JEB
as JEB generalized and JEB localized, DEB as Recessive
DEB and Dominant DEB (RDEB and DDEB, respectively) [5]. Additionally, there are at least 18 genes associated with the different types of EB [5]. The proposed
new classification does not address the relation to painful conditions, and, thus, the four major types will be
referenced throughout the guidelines. There is a wide
range of severity within the types. EBS is usually due to
Page 2 of 23
autosomal dominant mutations in keratin 5 or 14 or in
plectin and is often of milder severity. JEB can result
from mutations in any of six different basement membrane components, is inherited as an autosomal recessive disorder, and can range from mild to fatal early in
life. DEB can be in a mild dominant form (DDEB) or a
more severe recessive one (RDEB), both due to mutations in collagen 7. The recommendations that follow
are intended to be generally applicable to all patients
with EB who experience pain. The pain conditions vary
in prevalence among the types of EB, and readers will
find relevant guidelines to apply in the care of the particular pain problems they and their patients face. Resources (for example, particular medications and formulations,
trained medical, nursing and therapy personnel) will
vary by location, and practitioners and families will,
therefore, need to adapt the recommendations based
on what is available in their locale. DEBRA International
[6] is an optimal facilitating organization that can aid
implementation of the guidelines by way of providing
information, support and means of contacting expert
care providers.
Methods
In 2011, a multidisciplinary working group formed to
develop best care practice guidelines for pain associated
with EB. The group comprised representatives from
nursing, medicine and psychology who were expert in
the clinical care of patients with EB. Guidelines topics
and subtopics were chosen by the multidisciplinary
group with input from outside clinicians, based on issues
presented in the literature, seen clinically and raised for
discussion at DEBRA International Congress meetings.
Individuals or small groups were assigned to the various
subtopics. After relevant literature was reviewed, preliminary recommendations for each subsection were made.
Recommendations were circulated by email among the
entire panel of experts for review and input/feedback
was incorporated. Initial citations were added or removed as required for accuracy and appropriateness,
and criticism made of areas of weakness. Thus, the
group formed the first iteration of expert consensus. The
revised recommendations were recirculated to the group
for review, to establish consensus more firmly. A panel
of outside reviewers, comprising both clinicians and patients/families, then reviewed the document for comprehensibility, omissions and applicability.
Following external review (see Acknowledgements for
reviewers), funding became available and a subsequent
systematic evidence review was conducted by a trained
methodologist (author DSL). Clinical questions and the
systematic search strategy were developed, based on the
guideline topics and subtopics from the working group.
The population of interest comprises patients with pain
Goldschneider et al. BMC Medicine 2014, 12:178
http://www.biomedcentral.com/1741-7015/12/178
who have any variant of EB. The interventions included,
but were not limited to, pharmacological, holistic, psychological, psychical therapy and/or environmental interventions. Outcomes of interest were improvement in
symptom control (for example, pain, itch) and level of
function.
Systematic literature searches were conducted using
MedLine, CINAHL, PsycInfo and The Cochrane Library.
Search terms for epidermolysis bullosa and pain, regional anesthesia, or nerve block were used as medical
subject headings and/or keywords in all databases. The
search was only limited to articles published in English.
No other restrictions, limits or filters were used. Publication dates were not restricted for any topic or subtopic,
as the diagnosis is rare and there were few studies of
higher level, directly-related evidence (that is, systematic
reviews, meta-analyses, randomized controlled trials).
Reference lists were searched to identify studies. Studies
submitted by the working group and used in the initial
consensus processes were also reviewed. The most recent systematic search for pediatric acute, chronic, or recurrent pain management in EB patients was conducted
in December 2011.
Citations from the evidence searches were reviewed by
title and abstract for potential inclusion, regardless of
study design (n = 1,061). Evidence related to the clinical
questions from systematic reviews, meta-analyses and
RCTs as well as observational studies, case reports and
expert opinion articles were reviewed (see Figure 1). A
total of 57 references were found and evaluated that
were specific to the cross match of EB and the painrelated keywords (see above), of which only 8 were included into specific recommendations. The rationale for
including and excluding these references is found in
Table 1 and in Additional file 1.
Page 3 of 23
All included articles were critically appraised using evidence appraisal forms from the LEGEND (Let Evidence
Guide Every New Decision) evidence evaluation system
[7,8]. The methodologist assessed risk of bias in the included studies by evaluating quality for all individual
studies by domain and study design. The quality levels
for included studies were recorded (see Table 2). The
reader will find the evidence level for each article used
to directly support each recommendation noted after its
citation in the Reference section of the Summary of recommendations (Table 3). Age specificity of each recommendation is also noted. Data were collected on
descriptive characteristics of patients, characteristics of
the pain management interventions, and associated outcomes of reported pain management interventions.
Using the Grade for the Body of Evidence tool in the LEGEND system [7] provided objective criteria for evaluating evidence related to each recommendation (see
Table 4).
Given the paucity of data for statistical analysis, it was
deemed appropriate to conduct a face-to-face consensus
meeting on 4, 5 May 2012 in Cincinnati, OH. The LEGEND tool for Judging the Strength of a Recommendation (see Table 4) was used as a guide for finalizing
recommendation statements by discussing the body of
evidence and discussing safety/harm and other dimensions [7]. The overall GRADE (A, B, C, D) for each recommendation statement was then determined, based on
this process and the established criteria for GRADE
[9,10].
Updating procedure
The guidelines will be updated every three years after
the first version. If new relevant evidence is detected before the update, the information will be published on the
1,046 records identified through
database searches
1,160 records identified
114 records identified from the
working group
120 duplicates removed
1,040 records screened by title
and abstract review
787 records excluded
253 records reviewed
in full text for eligibility
196 records included in
guideline body of evidence
57 records excluded
(not related to the clinical question,
once reviewed in full text)
Figure 1 Flow of information through the evidence evaluation process.
Goldschneider et al. BMC Medicine 2014, 12:178
http://www.biomedcentral.com/1741-7015/12/178
Page 4 of 23
Table 1 EB-specific articles used in producing recommendations
Study citation
Study type
Population (setting, patients)
Intervention/Comparison groups
Outcomes
Chiu 1999 [68]
Case report
Country: Canada Setting: Childrens
Hospital Age: 11 years Gender:
Male Patient with Severe JEB
Amitryptiline (25 mg at night) was
prescribed and patient started on a
program of cognitive behavioral
training (hypnotic imagery, distraction).
Oral midazolam (7.5 mg) was initiated
20 minutes prior to bath or dressing
change
Pain management
Goldschneider
2010 [41,42]
Review articles
Country: United States Setting:
Childrens Hospital Patients
with EB
Pain management and prevention
Pain management
Herod 2002 [44]
Review article
Country: England (London) Setting:
Childrens Hospital Patients with EB
General pain management
Pain management
Mellerio 2007 [152]
Review article
Country: United States, England,
Chile Setting: Hospital Patients
with EB
Medical management
General pain management
Saroyan 2009 [156]
Case report
Country: United States Setting:
Hospital Female infant with EBS,
severe, Dowling-Meara subtype
Use of IV ketamine given orally Oral
administration of IV ketamine (10 mgmL,
Monarch Pharmaceuticals) at a starting
dose of 0.5 mg (0.125 mgkg dose) Over
four days, the dose was titrated to 3 mg
(0.75 mgkgdose) in response to observed
effect
Achieve analgesia during
painful dressing changes
van Scheppingen
2008 [4]
Qualitative study
(Interviews)
Country: Netherlands Setting:
Center for Blistering Diseases
Age: 6 to 18 years Children
with different (sub)types of EB)
Interviews conducted at homes or in hospital
Questions explored were: (i) What problems
do children with EB actually experience as
being the most difficult? (ii) What is the
impact of these problems on their daily life?
(iii) Are there differences in experiences
between mildly and severely affected
children?
Themes of pain for severe
disease (generalized blistering
with motion impairment) and
for mild disease (localized
blistering or generalized
blistering without motion
impairment).
Watterson 2004 [74]
Case report
Country: United States Setting:
Hospital Children with EB using
peripheral opioids
Topical morphine gel applied to the most
painful areas of skin at that time for each
child
Pain scores
EB, epidermolysis bullosa, EBS, epidermolysis bullosa simples; JEB, junctional epidermolysis bullosa.
web page for DEBRA International that is dedicated to
clinical the Pain guidelines [11].
Results and discussion
Psychological and integrative approaches
Introduction
A biopsychosocial approach emphasizing medical, psychological and physical therapies for pain management
has been suggested to be the most useful for adults and
Table 2 Evidence levels [8]
Quality level
Definition
1aa or 1ba
Systematic review, meta-analysis,
or meta-synthesis of multiple studies
2a or 2b
Best study design for domain
3a or 3b
Fair study design for domain
4a or 4b
Weak study design for domain
5a or 5b
General review, expert opinion,
case report, consensus report,
or guideline
Local Consensus
a = good quality study; b = lesser quality study.
children with acute and chronic pain [12]. This approach
has also been advocated for EB patients [3] and should
be initiated from early in youth and modified with maturation. It is recommended that psychological interventions be used in conjunction with physical and
pharmacologic therapies.
Types of therapies
Psychological therapies for pain management have been
shown to modify pain intensity, reduce related distress,
decrease pain-related functional disability and improve
pain coping. Painful experiences amenable to treatment
include acute pain related to procedures (for example,
whirlpool treatments) or medical routines (for example,
bandage changes, bathing), and chronic pain conditions
such as headache, abdominal pain or other disease-related
conditions. Psychological therapies include cognitive behavioral therapy (CBT), hypnosis, biofeedback and relaxation training, among others. CBT focuses on changing
the catastrophic thinking and negative emotions surrounding pain as well as modifying lifestyle to promote
wellness behavior despite chronic pain [13]. Hypnosis is a
Goldschneider et al. BMC Medicine 2014, 12:178
http://www.biomedcentral.com/1741-7015/12/178
Page 5 of 23
Table 3 Summary of recommendations
Application
Level of
Target age Key references (evidence grade)
recommendation group
A. Psychological therapies offer effective approaches to management of chronic and acute pain as well as itching.
For chronic pain management use cognitive behavioral
therapy (CBT).
All
Gerik 2005 [13] (5a), Palermo 2005 [17] (5a)
For acute pain management, offer the patient distraction,
hypnosis, visualization, relaxation or other forms of CBT
All
Green 2005 [14] (5a), Uman 2006 [21]
Consider habit reversal training, and other psychological
techniques for management of pruritus
All
Chida 2007 [29] (1a), Ehlers 1995 [32] (2b), Azrin 1973 [30]
(4b), Hagermark 1995 [28] (5a), Rosenbaum 1981 [31] (5a)
B. Postoperative pain can be handled as for other patients in the same setting, with modifications.
Basic perioperative assessment and pain treatments
should be used as for non-EB patients, with modification
All
Goldschneider 2010 [41] (5a), Goldschneider 2010b [42] (5a)
Transmucosal (including intranasal fentanyl and
transbuccal opioids) should be considered for short
procedures and pain of brief duration when intravenous
and enteral routes are unavailable
All
Manjushree et al., 2002 [45] (2b); Borland et al., 2007 [46]
(2b); Desjardins et al., 2000 [47] (2a)
Perioperative opioid use must account for preoperative
exposure, with appropriate dose increases to account for
tolerance
All
Hartrick 2008 [56] (1a), Mhuircheartaigh 2009 [55] (1a),
Viscusi 2005 [54] (2a)
Regional anesthesia is appropriate for pain resulting from
a number of major surgeries. Dressing of catheters must
be non-adhesive and monitored carefully
All
Diwan 2001 [51] (5a), Doi 2006 [53] (5b), Englbrecht
2010 [52] (5a), Kelly 1988 [48] (5b), Sopchak 1993 [49] (5a),
Yee 1989 [50] (5a)
C. Skin wounds and related pain are the hallmark of EB of most subtypes. Prevention and rapid healing of wounds through activity
pacing, optimal nutrition and infection control are important. A number of pharmacologic treatments are available
Maintain optimal nutrition and mobility and treat
infections as indicated
All
Denyer 2010 [57] (5a)
Consider topical therapies for pain
All
Cepeda 2010 [77] (1a), Lander 2006 [76] (1a), LeBon 2009
[73] (1a), Twillman 1999 [72] (5a), Watterson 2004 [74](5a)
Systemic pharmacologic therapy should be adapted to
treat both acute and chronic forms of skin pain
All
Noble 2010 [59] (1a), Moore, 2011 [ 67] (1a), Nicholson
2009 [65] (1a)
Monitor potential long-term complications of chronically
administered medications
Pediatric
Huh 2010 [62] (4a), Camilleri 2011 [66] (5a), Chiu 1999 [68]
(5a), Cruciani 2008 [63] (5a), Gray 2008 [69] (5a)
D. Baths and dressing changes require attention to both pain and anxiety
Anxiolytics and analgesics should be used for procedural
pain and fear. Care must be taken when combining such
medications due to cumulative sedative effects
All
Bell 2009 [85] (1a), Blonk 2010 [84] (1b), Ezike 2011 [82]
(2a), Desjardins 2000 [47] (2a), Borland 2007 [46] (2b),
Manjushree 2002 [45] (2b), Humphries 1997 [83] (2b),
Wolfe 2010 [81] (5a), Ugur 2009 [86] (5a)
Cognitive behavioral techniques should be implemented
as the child becomes old enough to use them
effectively. Specifically, distraction should be used for
younger children
All
Green 2005 [14] (5a); Gerik 2005 [13] (5a), Palermo 2005
[17] (5a)
Environmental measures such as adding salt to the water
to make it isotonic and keeping the room warm are
recommended
All
Arbuckle 2010 [78] (5a), Cerio 2010 [79] (5a), Peterson
(Poster) 2011 [80] (5b)
E. EB affects the gastrointestinal tract in its entirety. Pain from ulcerative lesions responds to topical therapy. GERD and esophageal
strictures have nutritional as well as comfort implications and should be addressed promptly when found. Maintaining good bowel habits
and reducing iatrogenic causes of constipation are crucial.
Topical treatments are recommended for oral and
perianal pain
All
Ergun 1992 [98] (4a), Travis 1992 [97] (4b), Marini 2001
[99] (5a), Buchsel 2008 [100] (5a), Buchsel 2003 [101] (5b),
Cingi 2010 [102] (2a)
Therapy should be directed to manage gastroesophageal
reflux and esophageal strictures using standard
treatments
All
Freeman 2008 [95] (4a)
Constipation should be addressed nutritionally, with
hydration and addition of fiber in the diet to keep stool
soft, by minimizing medication-induced dysmotility and
with stool softeners
All
Belsey 2010 [112] (1a), Freeman 2008 [98] (4a), Hanson
2006 [113] (4a)
Goldschneider et al. BMC Medicine 2014, 12:178
http://www.biomedcentral.com/1741-7015/12/178
Page 6 of 23
Table 3 Summary of recommendations (Continued)
F. Bone pain treatment must account for factors that include nutrition, mobility, potential occult fractures and is treated by combinations of
nutritional, physical, pharmacologic and psychological interventions.
Joint pain should be treated with mechanical interventions, C
physical therapy, CBT and surgical correction
All
Bruckner 2011 [126] (4b), Gandrud 2003 [131] (4b), Martinez
2010 [125] (5a), Lacativa 2010 [127] (5a), Tilg 2008 [128] (5a),
Noguera 2003 [130] (5a), Falcini 1996 [132] (5a)
Osteoporosis should be treated to reduce pain in EB
All
Levis 2012 [129] (1a), Martinez 2010 [125] (5a)
Back pain should be addressed with standard
multi-disciplinary care
All
Chou, et al., 2007 [133] (5a)
G. Corneal abrasions are common in EB, prevention and supportive care are appropriate
Care should include general supportive and analgesic care,
protecting the eye from further damage, and topical
therapies
All
Watson, 2012 [136] (1a), Calder 2005 [138] (1a)
H. Pain in infants is as widespread as in any other age, but unique pharmacologic, developmental and physiologic issues must be accounted for
in infants with all types of EB
Assess patients as needed and prior to and after
interventions; health care workers should use validated
measures. (Grade: A)
Infants
Gibbins 2014 [139] (2a) Stevens 2014 [140] (2a), Hummel
2008 [141] (2a), Krechel 1995 [142] (2b), Lawrence 1993
[143] (2b), Manworren 2002 [144] (2a)
Sucrose solutions should be administered for mild to
moderate pain alone or as an adjunct
Young
infants
Harrison 2010 [150] (1a), Yamada 2008 [149] (1a) Cignacco
2012 [151] (2a)
Standard analgesics should be used in infants as in older
patients with careful attention to dosing and monitoring
Infants
Tremlett 2010 [153] (5a), MacDonald 2010 [154] (5b)
I. End of Life pain care is an expected part of care for EB, which in many cases is life-limiting in nature. All basic principles of palliative care apply
as they do for other terminal disease states.
Assess and manage physical, emotional and spiritual
suffering of the patient, while providing support for the
whole family
All
Craig 2007 [165] (5a), AAP 2000 [166] (5b), WHO [167] (5b)
Opioids are the cornerstone of good analgesia in this
setting. Opioid rotation may need to be considered to
improve analgesia and reduce side effects, and adjuncts
may need to be added
All
Eisenberg 2009 [174] (1a), Quigley 2010 [172] (1a), Davies
2008 [61] (4a), Bruera 1996 [171] (4b), Watterson 2005 (5b)
Consider targeted medication for neuropathic pain when
pain proves refractory to conventional therapies
All
Allegaert 2010 (5a), Saroyan 2009 (5a). Clements 1982 (5a),
Watterson 2005 [87] (5b)
Continuous subcutaneous infusion of combinations of
medication is an option when parenteral therapy is
needed in the terminal phase
All
Reymond 2003 [178] (2b), ONeil 2001 [176] (5a), Watterson
2005 [87] (5b)
Where needed, breakthrough medication can be given
B
transmucosally (oral or nasal) for rapid onset and avoidance
of the enteral route
All
Zeppetella 2009 [182] (1a)
J. A combination of environmental, cognitive-behavioral and pharmacologic therapies are available for use for EB-related pruritus, which can be a
severe symptom of the disease.
Use environmental and behavioral interventions for itch
control
All
Nischler 2008 [183] (5b), EB Nurse Website [187] (5b)
Antihistamines are recommended and can be chosen
depending upon desirability of sedating effects
All
Ahuja 2011 [188] (2b), Goutos 2010 [186] (3a)
Gabapentin, pregabalin, TCA, SNRIs and other
non-traditional antipruritics agents should be strongly
considered for itch treatment
All
Goutos 2010 [186] (3a), Ahuja 2013 [189] (2a), Murphy 2003
[197] (2a)
EB, epidermolysis bullosa; GERD, gastroesophageal reflux disease; SNRI, serotonin norepinephrine reuptake inhibitors; TCA, tricyclic antidepressant.
psychological state of heightened awareness and focused
attention, in which critical faculties are reduced and susceptibility and receptiveness to ideas are greatly enhanced
[14]. Relaxation training usually includes techniques,
such as diaphragmatic breathing, muscle relaxation and
visualization/imagery, that assist in adaptive coping via
distraction, reduced emotional arousal and activation of
the parasympathetic nervous system. While these interventions are frequently patient-focused, CBT can also include
parent/family training related to behavioral management,
reducing caregiver distress and enhancing environmental
factors necessary for positive coping [15].
Goldschneider et al. BMC Medicine 2014, 12:178
http://www.biomedcentral.com/1741-7015/12/178
Table 4 Table for judging the strength of a
recommendation [8]
Dimension
Definition
Grade of the body of evidence
High, Moderate, Low, Not Assignable
Safety/harm (side effects and
risks)
Minimal, Moderate, Serious
Health benefit to patient
Significant, Moderate, Minimal
Burden on patient to adhere to
recommendation
Low, Unable to determine, High
Cost-effectiveness to healthcare
system
Cost-effective, Inconclusive, Not
cost-effective
Directness of the evidence for
this target population
Directly relates, Some concern of
directness, Indirectly relates
Impact on morbidity/mortality
or quality of life
High, Medium, Low
Page 7 of 23
Psychological interventions are useful for the management of acute pediatric pain (see Box 1) although evidence
for their efficacy varies depending on the type of pain.
For procedure related pain, particularly needle procedures, distraction, hypnosis and CBT are effective, evidence based interventions [20-24].
In a review of non-pharmacological treatments to reduce the distress due to acute wound care in burn patients, some evidence has been shown that healthcare
provider interventions (massage and maximizing patient
control and predictability), child interventions (for example, virtual reality gaming [25] and therapist coaching
of stress management techniques [26]) are beneficial.
For postoperative pain, there is insufficient evidence for
the efficacy of most psychological interventions, but preparation, guided imagery and CBT are promising [27].
Psychological interventions for itch
As an adjunct to relaxation training, biofeedback monitors physiological functions (for example, heart rate,
muscle tension, temperature) in order to improve control of bodily processes that might ease chronic pain.
Frequently, sensors are attached to the skin by adhesive,
which is relatively contraindicated in EB. Clip on pulse
oximeter probes can be safely used in patients with EB
to track heart rate, and provide an alternative method of
biofeedback.
Efficacy of psychological interventions in chronic and acute
pain management
Psychological therapies have been shown to be effective in decreasing pain intensity and frequency in other
pediatric chronic pain conditions [16,17] with emerging evidence showing improvement in pain-related
functional disability as well [17,18]. The addition of
biofeedback to relaxation training does not necessarily
result in superior pain outcomes [17]. Modest data
support the use of CBT in adults with chronic pain
and disability [19] (see Box 1).
Box 1. Recommendations for use of cognitive
behavioral therapies in EB
Patients with EB may experience severe itch, which not
only intensifies their suffering but can also be a source
of social embarrassment secondary to the appearance of
the excoriated skin and the preoccupation with scratching in social situations. Beyond this, damage of the integrity of the skin can create a portal of entry for
systemic infections. Regardless of the underlying cause,
itch evokes the behavior of scratching that increases inflammation and stimulates nerve fibers, leading to more
itching and scratching [28]. Perpetuation of the itchscratch cycle alters the integrity of skin leading to barrier
damage. Scratching also causes undesirable changes in
skin, such as lichenification and prurigo nodule formation. Successful treatment of itch requires interruption
of this cycle. Non-pharmacological treatments, such as
CBT, hypnosis, meditation, prayer, biofeedback and eye
movement desensitization and reprocessing (EMDR),
have been used with some success in both adults and
children with conditions such as atopic dermatitis
[29]. Habit reversal is a specific behavioral intervention whereby habitual behaviors are brought into conscious awareness and specific behavioral techniques
are developed as a competing response to the urge to
itch [30,31] (see Box 1). In practice, this technique is
frequently combined with CBT and relaxation as part
of a treatment package applicable to patients of all
ages [29,32].
1. For chronic pain management use cognitive behavioral
therapy (CBT). (Grade: B)
2. For acute pain management, offer the patient distraction,
hypnosis, visualization, relaxation or other forms of CBT.
(Grade: B)
3. Consider habit reversal training, and other psychological
techniques for management of pruritus. (Grade: C)
Integrative medicine therapies
Complementary and alternative medicine (CAM) practices constitute therapies that are often requested by
patients and families for a variety of chronic pain conditions. This class of treatments includes, but is not
limited to: acupuncture, meditation, massage, herbal
preparations, yoga and chiropractic work. The evidence for therapies such as acupuncture [33], music
Goldschneider et al. BMC Medicine 2014, 12:178
http://www.biomedcentral.com/1741-7015/12/178
therapy [34], chiropractic care, or yoga [35] is modest
in the pediatric and adult pain populations, with no
specific studies in EB. Prima facie evidence would suggest that massage and chiropractic interventions might
be harmful given the skin fragility and the osteopenia
that is often seen in EB. With regard to herbal supplementation, one of the chief side effects for a number
of these preparations is bleeding, although the evidence is not clear [36]. Thus, this treatment may be
contraindicated in patients having surgery, open
wounds or a history of gastrointestinal tract bleeding.
The active ingredients in the herbal preparations may
also have interactions with any other prescribed
medication; attention to potential drug-drug interactions should be considered.
Good practice points Assessment of the suitability of
psychological therapies for EB patients experiencing
chronic and acute pain should always take into account
developmental issues including age, cognitive level and
psychopathology [37]. Include parents in behavioral
pain management interventions [38] for children and
adolescents.
Acute pain care: postoperative pain management
Introduction
As a multisystem disorder, EB causes a variety of disruptions to body systems that are amenable to surgical
intervention. While there are no controlled trials of
postoperative pain therapies in EB, general principles
of pain care apply.
Assessment
As for all patients, pain should be regularly assessed,
and then reassessed after intervention to evaluate analgesic efficacy and detect side effects. Numeric rating
scales have been shown to be effective for children of a
developmental level above eight years who can verbalize
their pain scores as well as for adults. Pain assessment
in younger or nonverbal patients can be completed
using the Face Legs Arms Cry Consolability (FLACC)
and Childrens Hospital of Eastern Ontario Pain Scale
(CHEOPS) [39,40] augmented by reports of parents or
other close family care-givers.
Systemic therapies
Analgesic treatment starts before and during surgery
and includes the use of opioids, non-steroidal antiinflammatory drugs, acetaminophen and, when appropriate for the type of surgery, regional anesthesia [41,42].
Patient controlled analgesia (PCA) technology is a safe
and useful way to deliver opioids to patents of all ages
with EB, as it is for non-EB patients (see Box 2).
Page 8 of 23
Box 2. Recommendations for acute pain care in EB
1. Basic perioperative pain assessment and treatments should be
used as for non-EB patients, with modification. (Grade: A)
2. Transmucosal (including intranasal fentanyl and trans buccal
opioids) should be considered for short procedures and pain
of brief duration when intravenous and enteral routes are
unavailable. (Grade: B)
3. Perioperative opioid use must take preoperative exposure
into consideration, with appropriate dose increases to
account for tolerance. (Grade: B)
4. Regional anesthesia is appropriate for pain resulting from a
number of major surgeries. Dressing of catheters must be
non-adhesive and monitored carefully. (Grade: C)
In the postoperative period, EB patients may be slow to
resume oral intake, especially after oropharyngeal procedures, such as esophageal dilatation or dental rehabilitation. For patients lacking gastrostomy tubes, intravenous
analgesia may be required. Intravenous analgesia should be
multimodal and may include opioids (for example, morphine or hydromorphone), nonsteroidal anti-inflammatory
drugs (NSAIDS; when postoperative bleeding is not a
risk and renal function is normal (for example, ketorolac))
and acetaminophen (enteral or intravenous). Given the
high rate of superficial bleeding from skin wounds,
cyclooxygenase-2 inhibitors may have a role to play, given
they have prothrombotic features in some studies [43].
Due to the risk of blister formation with rectal manipulation, there is controversy regarding whether the rectal
route of administration may be used in EB patients [44].
Intranasal opioids can be effective for short-term treatment, if other routes are not available [45-47], and may be
particularly helpful for procedures of short duration
when rapid-acting analgesia is desired in the absence
of intravenous access. Oral disintegrating and transbuccal formulations may be helpful as well, although
they presume intact mucosa, which may not be applicable (see Box 2).
Patients with prolonged postoperative pain because of
extensive surgery may benefit from the use of opioidbased PCA with dose adjustments that take into consideration prior opioid use. While no EB-specific literature
exists, this modality is standard treatment in many centers for patients old enough to understand the concept
(typically seven years of age or older). Activation of the
dosing button may be limited by pseudosyndactyly, so
use should be determined on a case-by-case basis. PCAby-proxy (dose administered by a nurse or designated
family member) is practiced in some pediatric centers
Goldschneider et al. BMC Medicine 2014, 12:178
http://www.biomedcentral.com/1741-7015/12/178
and may be an alternative approach to PCA dosing for
children.
Preoperative tolerance
The preoperative pain status of the patient should be
taken into consideration when choosing opioid dose,
both intra- and post-operatively. Many EB patients have
recurring acute and/or chronic pain and may be taking
opioids daily, either prior to bathing/dressing changes or
for ongoing pain. These patients require increased doses of
opioids for adequate analgesic effect, due to the development of tolerance. Their usual daily opioid intake should
be considered the baseline opioid dose to which the postoperative analgesia should be added (see Box 2). Drug
pharmacokinetics may be altered in patients chronically
exposed to sedatives and opioids. Flexibility in dosing, review of prior anesthetic records and discussion with the
patient or family can aid appropriate dosing.
Page 9 of 23
Non-pharmacologic therapies
Non-pharmacologic techniques should also be employed
in combination with the pharmacologic techniques listed
above. These include, but are not limited to, distraction
(music, reading, video games and movies), visualization,
imagery/virtual reality and breathing techniques (see Efficacy of Psychological Interventions in Chronic and
Acute Pain Management, above and Box 1). Effective
approaches used in the past should be discussed with the
patient or parents and their use supported whenever
possible.
Good practice points Postoperative pain can be managed as for other patients in the same setting, with modifications to account for the ability to self-administer
medications, prior drug exposure, and the condition of
the skin at potential regional anesthesia injection/catheter
sites.
Regional anesthesia
Chronic and recurrent pain care
Some common procedures (and the corresponding regional
anesthesia technique used) in EB patients include: fundoplication (epidural) [48-50], hand and foot surgery (peripheral
nerve block, either single shot or continuous peripheral
nerve catheter infusion following bolus injection) and hand
surgery (both axillary and infraclavicular approaches have
been used for brachial plexus block) [51,52].
Regional anesthesia techniques should be modified in
patients with EB to minimize damage to the skin. Skin
preparation may be performed by pouring prep solution
(povidone-iodine or chlorhexidine) on the site without
rubbing, then blotting and allowing the solution to dry.
Ultrasound guidance can be used for peripheral nerve
blocks with generous use of gel to minimize skin abrasion when moving the probe. When a catheter is placed
(epidural or peripheral nerve), it may be tunnelled subcutaneously if desired [53] then secured to the skin
using silicone-based tapes and dressings (MepitacW,
MepitelW, MepilexW) or other soft non-adhesive dressings. Adhesive dressings and adhesive adjuncts should
be avoided. If there is any doubt about the safety of
using a dressing, it should be tested on a small area of
skin with patient or parental consent. With local infection
being a relative contraindication to regional anesthesia,
examination of the skin overlying the point of entry is
mandatory prior to attempting a catheter placement. If leaving a catheter in the epidural space is undesirable, then a
single injection of a long-acting form of opioid (DepoDurW)
may be a good option when available [54,55], although
monitoring is important due to risk of hypoventilation
[56]. Lidocaine infiltration may be used by dentists/
oral surgeons when extractions are necessary, but care
must be taken when injecting to avoid mucosal blister
formation (see Box 2).
EB has a large number of painful complications, some
chronic and others acute but repetitive. Care of EB involves painful interventions on a daily basis. Almost
every organ system can be affected, but the following are
the major sources of pain: skin, gastrointestinal tract,
musculoskeletal system, eyes.
Skin and wound pain
Introduction The classic presentation of EB is the development of skin wounds that are painful in their own
right, but which often become infected, heal poorly and
frequently lead to scarring. This combination makes skin
and wound pain a prominent complaint of patients with
EB.
Environmental and behavioral approaches Dressings
that are non-adhesive upon removal, such as siliconebased products, are helpful in reducing skin-trauma
pain. Different subtypes of EB and different individuals
seem to have varying dressing requirements [57]. Nutrition is important in promoting wound healing, and
anecdotally, patients with poor nutritional status have
more wounds and slower healing, which lead to increased pain. Experience suggests that attention to
good nutrition, surveillance for superficial infection
and aggressive treatment of infection reduce pain. As
discussed in the section on psychological interventions, CBT is helpful for a number of painful conditions and should be applied in EB.
Systemic approaches The pharmacological treatment of
skin and wound pain is non-specific, with no evidence in
the EB population to promote one treatment over another. NSAIDs, acetaminophen, tramadol and opioids
Goldschneider et al. BMC Medicine 2014, 12:178
http://www.biomedcentral.com/1741-7015/12/178
are used with success. Cannabinoids have some anecdotal support. Itch is a major problem (see below) that
can lead to increased scratching and subsequent development of painful wounds. Hence, managing pruritus is
important to prevent wound-related pain.
Many patients with severe types of EB use longacting opioid preparations to provide a basal comfort
level. Of note, there are no clear guidelines that longacting opioids are preferable to use of intermittent
opioids for non-cancer pain [58], although there is
modest evidence for opioid use, in general, for noncancer pain in adults [58,59]. Individualization of therapy is recommended.
Regular and frequent dosing of opioids is common
and merits special attention. Regardless of the opioid
chosen, chronic use of opioids may have endocrinologic effects, such as hypogonadism [60]. Monitoring
should be considered, especially given the propensity
for osteopenia and delayed puberty in adolescents
and young adults with EB. In the absence of data, the
use of opioids is recommended as clinically indicated
(see Box 3).
Box 3. Recommendations for wound pain treatment
1. Maintain optimal nutrition and mobility and treat infections
as indicated (Grade: D)
2. Consider topical therapies for pain (Grade: C)
3. Systemic pharmacologic therapy should be adapted to treat
both acute and chronic forms of skin pain. (Grade: B)
4. Monitor potential long-term complications of chronically
administered medications. (Grade: C)
Methadone merits particular consideration. Dose titration can be unpredictable due to long and variable halflife as well as to saturable plasma protein binding [61].
The long and variable half-life, as well as the risk of
methadone-induced prolonged QT syndrome [62,63],
mandates care in its use alone and with other drugs that
may also prolong the QT interval. Guidelines on electrocardiographic screening are limited [64] (especially for
adult patients of smaller stature and children). Given the
risk of prolonged QT and methadones complex and variable pharmacokinetics, it is recommended that methadone only be prescribed by practitioners with experience
evaluating and monitoring its use [65]. Methadone use is,
therefore, best done with input from a pain management
and/or palliative care specialist.
Among the common side effects of opioids, constipation [66] and pruritus are particularly significant. Both
Page 10 of 23
are significant baseline problems in EB and the reader is
referred to the sections on gastrointestinal pain and
pruritus.
The pain of extensive wounds has a quality suggestive
of neuropathic pain; both are often described as burning in quality. There is evidence supporting the use of
gabapentin for neuropathic pain in other conditions
[67]. Medications such as tricyclic antidepressants and
gabapentin have shown anecdotal success in EB skin
pain in a child [68], as well as for adult patients with
acute skin pain due to burns [69]. The potential for tricyclic antidepressants to prolong the QT interval means
that caution should be taken using this class of medications in RDEB patients, who are at risk for developing
cardiomyopathy [70], as a lethal outcome in this setting
has been reported [71].
Topical approaches For localized wounds, topical lidocaine jelly (2% concentration) has been used anecdotally.
Morphine mixed in hydrogel formulations has been used
in different types of localized painful wounds [72,73] but
has only limited anecdotal experience in EB wounds [74]
(see Box 3). Use of these medication vehicles raises
questions of absorption and systemic effects that require
further investigation before full recommendations can be
made. Limited anecdotal evidence supports the use of
keratinocyte hydrogel dressings for poorly healing wounds
and RDEB [75].
Blood draws and intravenous access as well as the
need for skin biopsies are minor technical procedures
that can be very distressing, especially for children. Topical anesthetics are commonly used in non-EB populations with good effect. Amethocaine appears to be more
effective than a eutectic mixture of local anesthetics
(EMLAW) [76]. These may have a role when applied to
intact skin, but cannot be recommended for use on
wounds due to unknown rate and extent of absorption
of lidocaine. Blistering as a localized allergic reaction
to EMLAW (or its contents) has been rarely observed,
indicating caution in its use even on intact skin. Lidocaine injected with a small gauge needle is a standard
approach to superficial analgesia in all age groups.
Additionally, it is recommended that bicarbonate be
added to buffer the pH of the lidocaine to reduce the
pain of injection [77]. As noted above, CBT (for example, distraction and relaxation) is effective in the
acute pain setting [21] and should be employed whenever possible in conjunction with medication management (see Box 1).
Good practice points Prevention and rapid healing of
wounds through non-adherent dressings, optimal nutrition and infection control are priorities.
Goldschneider et al. BMC Medicine 2014, 12:178
http://www.biomedcentral.com/1741-7015/12/178
Bathing and dressing changes
Introduction Bathing and bandage changes are a source of
significant recurrent pain and anxiety for patients with EB.
Environmental treatment Oatmeal and salt have been
added to bath water to reduce the pain of immersion
[78]. The former may have anti-pruritic, cleansing and
protective properties for dermatologic conditions in general [79] that may be similarly effective in EB. Salt is
added to make the water isotonic, which has anecdotal
support from many families of patients with EB including preliminary survey data from EB families [80]. Isotonic saline (0.9% NaCl) is 9 grams of salt/1 liter of
water; total amount of salt varying according to the desired
water volume. Bleach and vinegar are anecdotally helpful
in drying the skin and reducing bacterial colonization,
which some patients find comforting while others report
increased pain at the wound sites. The salt water does not
require plain water rinse, whereas vinegar and bleach baths
require rinsing to reduce the risk of itch. Many patients
elect to reduce the frequency of bathing as a simple measure to minimize bath-related pain. Anecdotally, starting
the bath by immersing the patient still in his/her bandages
can ease the transition into the water and help reduce the
pain of removing the dressings. Other patients find drafts
from heating and cooling systems to be painful on open
wounds, so attention to general environmental factors is
recommended (see Box 4).
Box 4. Recommendations for bathing and dressing
change pain treatment
1. Anxiolytics and analgesics should be used for procedural pain
and fear. Care must be taken when combining such
medications due to cumulative sedative effects (Grade: B).
2. Cognitive behavioral techniques should be implemented as
the child becomes old enough to use them effectively.
Specifically, distraction should be used for younger children
(Grade: B).
3. Environmental comfort measures are recommended; these
include adding salt to the water to make it isotonic and
keeping the room warm (Grade: B).
Analgesics Analgesics used by patients with EB have included enteral opioids, NSAIDs and acetaminophen.
The nasal route may permit administration of medications when intravenous access is absent [81]. Fentanyl
works well by this route for non-EB patients in the
Page 11 of 23
perioperative setting [45], for breakthrough cancer pain
(see section on Breakthrough pain medication at the end
of life) and has been used for acute pain management in
the emergency department with success [46]. Butorphanol
is a mixed agonistantagonist that can be used via the intranasal route and is effective both for pain (for example,
dental postoperative pain [47]) as well as for opioidinduced pruritus. Fixed dose spray is available for outpatient use in the United States, which limits the ability to
adjust for patient size. Timing of medication administration should be adjusted to match expected peak analgesia
with anticipated peak pain (see Box 4).
Ketamine can be administered enterally for wound care
pain, for which there are data from adult and pediatric
burn populations [82,83] but not for EB patients. The IV
form of ketamine given orally has been used with variable
success for other chronic pain conditions [84] as well as in
cancer patients [85] and in pediatric palliative care [86].
Inhaled nitrous oxide has been suggested for pediatric
wound care in EB in some texts and review articles
[44,87], but its use in EB patients has not been studied
or reported. Nitrous oxide has been used for painful procedures in other settings [88] and is available in both
fixed 50:50 and variable combinations with oxygen. Depending on the delivery system (mouth piece, face mask,
or nasal mask) concerns arise about environmental pollution and exposure of health care personnel [89]. In the
absence of evidence of efficacy, concern must be raised
about repeated use for wound care or dressing changes
because of longstanding evidence of megaloblastic bone
marrow changes and neurologic abnormalities due to inhibition of methionine synthase and cobalamin activity
with repeated exposure to nitrous oxide [90,91].
Anxiolysis The pain caused by baths and dressing changes
is commonly cited by families as generating anxiety in the
patient, which in turn is stressful for the caregiver. Medications used for acute anxiolysis in this population include
midazolam, diazepam and lorazepam and are considered
good treatment for acute anxiety in other populations (for
example, children for dental procedures, [92,93]; prior to
adult burn procedures [94]). In addition to anxiolysis, the
pre-procedural use of benzodiazepines offers the possibility
of anterograde amnesia which may prevent the development of increased anxiety with repeated procedures. When
using benzodiazepines in combination with opioids, care
must be taken to avoid over sedation (see Box 4). As response to each medication will have individual variation,
dose adjustments should be made carefully and preferably one drug at a time, when more than one is being
administered.
Other behavioral comfort measures In addition to
medication management, recommendations from caregivers
Goldschneider et al. BMC Medicine 2014, 12:178
http://www.biomedcentral.com/1741-7015/12/178
include preparing all materials ahead of bandage removal to reduce the amount of time wounds are exposed to air. Involving children in the process at as
early an age as possible helps them to develop a sense
of control. Maintaining room temperature at a moderately warm level has also been recommended. CBT can
be applied to treating the anxiety and pain associated
with bathing and bandage changes (see section on psychological approaches, above).
Good practice points Bathing and dressing changes are
recurrent sources of both pain and anxiety. Therapy
should focus on both symptoms, using environmental,
psychological and pharmacologic approaches.
Pain related to the gastrointestinal tract
Introduction Gastrointestinal complications are common in children and adults with EB with specific complications linked to different subtypes [95-97].
Upper gastrointestinal tract
Topical treatments Oral ulceration, blistering and mucositis are the most frequent gastrointestinal complications in patients with EB [98]. While oral ulceration
can occur in all types of EB, it is most common and
problematic in patients with the severe types of this
disease. Oral ulceration can be extremely painful and
lead to difficulties in feeding and maintaining dental
hygiene. Apart from oral analgesics, topical preparations
are available. Sucralfate suspension has been used to
prevent and manage oral blisters in five children, 6- to
11-years-old, with RDEB when applied four times a day
for six months [99]. The number of blisters reduced
within three weeks and pain reduced within one week
(see Box 5).
Box 5. Recommendations for gastrointestinal pain
treatment
1. Topical treatments are recommended for oral and perianal
pain. (Grade: C)
2. Therapy should be directed to manage gastroesophageal
reflux and esophageal strictures using standard treatments.
(Grade: C)
Page 12 of 23
Polyvinylpyrrolidone-sodium hyaluronate gel (GelclairW)
either used as a mouth rinse or applied directly to a
mouth lesion in children, has been used anecdotally in EB.
Secondary evidence comes from two recent reviews which
showed that GelclairW may be useful as an adjunctive therapy in decreasing the painful lesions of oral mucositis in
cancer patients [100,101]. Chlorhexidine gluconate and
benzydamine hydrochloride mouth spray is used regularly
in EB patients at the London centers with reported benefit
but has not been evaluated systematically. Secondary
evidence for the potential efficacy of this intervention
exists for treating the pain of acute viral pharyngitis in
adults [102].
Gastroesophageal reflux Patients with EB are at high
risk for gastroesophageal reflux disease (GERD) - especially
infants with generalized EBS, JEB and patients with severe
generalized RDEB who can develop esophagitis [95]. While
children with GERD may not complain of dyspeptic symptoms until they are older, crying and sleep disturbance are
commonly associated with this symptom. Management is
guided by standard treatment in non-EB patients, and
may involve treating the reflux with antacids, histamine H2-blockers and proton pump inhibitors and,
rarely, surgery [103,104] (see Box 5).
Esophageal strictures Esophageal stricture formation
and dysphagia are most common in patients with severe
generalized RDEB with a cumulative risk of developing
strictures or stenosis rising steadily from 6.73% at age
1 year to 94.72% at age 45 years [105]. However, strictures
can also be seen in other subtypes of EB including Kindler
syndrome [106]. Dysphagia and delayed progression of
food through the stricture can present with retrosternal
chest pain. Esophageal strictures, if symptomatic, require
treatment with a fluoroscopically guided balloon dilatation
with peri- and post-operative steroids administered to reduce the recurrent stenosis rate [107-109] (see Box 5).
Acute symptoms can respond temporarily to oral dexamethasone or nebulized budesonide, based on anecdotal
evidence. A recent case report examined the use of daily
oral viscous budesonide therapy (0.5 mg/2 mL budesonide
nebulizer solution mixed with 5 g of sucralose and maltodextrin) in two children with RDEB who had recurrent
proximal esophageal strictures [110]. Both children had a
reduction in the rate of stricture formation and symptoms
of dysphagia.
3. Constipation should be addressed nutritionally, with
hydration and addition of fiber in the diet to keep stool soft,
with stool softeners and by minimizing medication-induced
dysmotility. (Grade: C)
Lower gastrointestinal tract
Constipation Constipation has been shown to be present
in 35% of children with all types of EB [95] and can cause
abdominal pain and pain on defecation as well as lead to
perianal trauma. A case of colonic perforation and early
Goldschneider et al. BMC Medicine 2014, 12:178
http://www.biomedcentral.com/1741-7015/12/178
death resulting from severe constipation in DEB has been
described [111]. Chronic perianal pain during defecation
can produce stool withholding behavior which exacerbates
constipation. Chronic opioid use may contribute to poor
bowel motility. First line management is prevention
with dietary manipulation; however, patients with severe
types of EB often require the regular use of a laxative
(see Box 5). Polyethylene glycol is effective clinically in
treating constipation in children and adults with EB,
with empiric evidence of efficacy in adult [112] and
pediatric [113] non-EB cohorts.
Colitis A subgroup of children with RDEB may develop
colitis, presenting with abdominal pain and other symptoms [95,114]. Dietary restriction and anti-inflammatory
drugs, such as sulfasalazine, have been used but with
variable effects on controlling the colitis [95].
Perianal pain Perianal blistering and ulceration is common and debilitating in children and adults with severe
types of EB. Topically, sucralfate has been shown to be superior to petroleum jelly in facilitating anal fistulotomy
healing and lessening wound pain [115]. Sucralfate suspension has also been used to lessen the pain of oral and
genital ulceration in patients with Behcets disease [116].
Anecdotally, topical sucralfate combined with Cavilon
(an alcohol-free liquid barrier film that dries quickly to
form a breathable, transparent coating on the skin, containing hexamethyldisiloxane, isooctane, acrylate terpolymer, polyphenylmethylsiloxane) appears to improve pain
in perianal lesions of some patients with EB. Non-surgical
treatment is of small benefit for both pain and healing of
chronic anal fissures [117], with recommendations of topical diltiazem and glyceryl trinitrate followed by surgery if
needed in adults [118]. No data on anal fissure treatment
in EB patients exist (see Box 5).
Good practice points EB affects the gastrointestinal
tract in its entirety. Pain that originates from ulcerative
lesions may respond to topical therapy. GERD and
esophageal strictures have nutritional as well as comfort
implications and should be addressed promptly when
found. Maintaining good bowel habits and reducing iatrogenic causes of constipation are crucial.
Musculoskeletal pain
Introduction Musculoskeletal complications are common and frequently painful for patients with EB. These
conditions include pseudosyndactyly, osteopenia, back
pain, fractures and occasional co-morbid rheumatologic
disorders.
Joint pain Pseudosyndactyly affects hands, feet, ankles
and wrists. Painful hyperkeratotic lesions develop on the
Page 13 of 23
soles of patients with EBS. Occupational therapy approaches can improve function and decrease pain via use
of adaptive equipment and specially designed orthotics and
clothing. Physical and occupational therapy play crucial
roles in encouraging patient mobility. For weight-bearing
patients, careful attention to footwear, nails, orthotics and
hyperkeratosis management are important aspects of pain
care [119]. Referring patients to programs to maintain or
regain strength, to prevent or minimize joint contractures,
and to optimize mobility is recommended based on anecdotal evidence (see Box 6). Coping skills training and activity pacing can enhance effectiveness of therapy [120].
Surgical intervention has had some success in increasing
mobility and reducing pain [121]. EB patients can also have
inflammatory arthritis [122,123]; appropriate imaging can
be helpful in determining inflammatory causes of pain.
Given that inflammatory markers are usually elevated in
EB patients, these markers alone are not likely to be useful
to diagnose joint pathology.
Box 6. Recommendations for musculoskeletal pain
treatment
1. Joint pain should be treated with mechanical interventions,
physical therapy, cognitive behavioral therapy and surgical
correction (Grade: C).
2. Osteoporosis should be treated to reduce pain in EB (Grade: D).
3. Back pain should be addressed with standard multi-disciplinary
care (Grade: C).
Bone pain Osteopenia, osteoporosis and fractures are
now well recognized and commonly seen in patients with
the severest types of EB [124-126], as a cause of bone and
joint pain. The causes are multifactorial and include reduced mobility, delayed puberty, limited exposure of the
skin to sunlight, inadequate nutritional intake for metabolic requirements and chronic inflammation. Chronic inflammation causes increased osteoclast activity [127,128].
As a consequence of the osteoporosis, a significant
proportion of patients develop fractures. The incidence
of vertebral fractures in patients with RDEB is unknown,
but may be underestimated due to the fact that fractures
of the lumbar and thoracic spine may be clinically silent,
or present without overt or localized back pain on palpation [125]. Anecdotally, however, some patients can
present with back pain, in which case a high index of
suspicion should be maintained. Treatment of osteoporosis and derivative pain is based upon standard treatment of osteoporosis in non-EB patients, which relies on
vitamin D and calcium supplementation, exercise and
bisphosphonate treatment [129] (see Box 6).
Goldschneider et al. BMC Medicine 2014, 12:178
http://www.biomedcentral.com/1741-7015/12/178
Anecdotally, bisphosphonates have been found useful
in treating patients with evidence of osteoporosis without fracture. Bisphosphonates appear to improve fractures
on annual X-rays and lead to a noticeable improvement in
pain. Indirect support for the use of bisphosphonates
comes from its use in rheumatologic and other pediatric
conditions, associated with osteopenia [130,131] and resolution of back pain [131,132], but efficacy specifically in
patients with EB has not been formally studied.
Back pain Older patients with EB can have back pain.
Beyond osteopenia-related issues, biomechanical causes
can be involved. Foot blisters and painful hyperkeratosis
can cause abnormal gait and compensatory postures.
Further, impaired mobility can add a myofascial component to pain. Management of back pain includes optimal
foot care, assessment of primary and secondary mechanical factors, evaluation and treatment of osteopenia and
fractures, physical therapy, standard analgesics and CBT
interventions. Back pain treatment in the EB population
is extrapolated from basic principles recommended for
the general population [133], for lack of EB-specific
evidence (see Box 6).
NSAIDs are routinely used for bone and joint pain of
a variety of types and are appropriate for these types of
pain in EB. Care should be taken to monitor for side effects, and the cyclooxygenase-2 inhibitors may be useful
in those patients who experience improved pain control
but note increasing blood loss from wounds, or who
have gastrointestinal upset with standard NSAIDs. Acetaminophen does not affect bleeding and can be useful.
Tramadol and opioids are also useful for more severe
pain. Some prefer use of long-acting opioid preparations,
with methadone being the only one available in liquid
form. Limitations in methadone use are discussed in
sub-section on systemic approaches under Skin and
Wound Pain.
Good practice points Bone health should be optimized
with calcium and vitamin D supplements as needed,
maintenance of maximum mobility, minimization of joint
deformity and monitoring for/treatment of pubertal delay.
Routine screening for bone mineral density may be useful
to ascertain cases of osteopenia before they progress to
osteoporosis and fractures. Care must be taken not to
overlook inflammatory joint disease, as pain secondary
to this will respond to disease modifying therapy. Multidisciplinary treatment modalities are helpful in addressing back pain and apply to such pain in the EB
population as well.
Eye pain
Ophthalmologic involvement is pervasive in EB [134,135].
Eye pain is often caused by corneal abrasions. Comfort
Page 14 of 23
measures such as avoiding bright light (a natural reaction
to the photophobia that results from the trauma), lubricating eye drops, NSAIDs and antibiotic drops have been
used. Evidence for these treatments for recurrent corneal
abrasions of other etiologies is modest [136]. The use of
eye patches in non-EB patients does not aid pain relief
and, therefore, is not recommended for use in EB patients
either [137]. There is some evidence that topical NSAIDs
provide analgesia for acute, traumatic corneal abrasions
[138] (see Box 7).
Box 7. Recommendations for eye pain treatment
1. Care should include general supportive and analgesic care,
protecting the eye from further damage and topical therapies
(Grade: C).
Good practice points Corneal abrasions are painful and
common in EB; prevention and supportive care are
appropriate.
Special Topics
Pain care in infants with EB
Introduction In the severe forms of EB, pain starts immediately, and great care needs to be taken in most
of the activities of daily living. Infants with EB require
careful attention to environmental factors at a higher
level than for older children but otherwise can receive pain care using guidelines for specific types of
discomfort.
Pain assessment Pain assessment should be completed
on all neonates with EB at regular intervals and as
needed (see Box 8). A valid neonatal pain scale should
be used, considering both physiologic and behavioral
measures. Some examples include: the Premature Infant
Pain Profile (PIPP) [139,140], the Neonatal Pain Agitation and Sedation Scale (N-PASS) [141], the Crying, Requires oxygen, Increased vital signs, Expression and Sleepless
pain scale (CRIES) [142], and the Neonatal Infant Pain Scale
(NIPS) [143]. The Face Legs Arms Cry Consolability
(FLACC) scale is recommended for infants between 1 to
12 months [144]. These pain scales have been validated
for use by nurses, although training could be generalized
to non-nurse care givers and family members. Pain should
be reassessed frequently during and after interventions
and until comfort is achieved based on a combination of
one of the above scales and clinical judgment. Analgesic
interventions should match degree or level of pain. Of
note, infants, especially neonates, seem to be a higher risk
Goldschneider et al. BMC Medicine 2014, 12:178
http://www.biomedcentral.com/1741-7015/12/178
for respiratory compromise [145,146] due to reduced
clearance of opioids in infants younger than two months
[147,148]. Therefore, careful clinical and cardiopulmonary
monitoring is crucial when providing opioids to this population (see Box 8).
Box 8. Recommendations for infant pain care
1. Assess patients as needed and prior to and after
interventions; health care workers should use validated
measures. (Grade: A)
2. Sucrose solutions should be administered for mild to
moderate pain alone or as an adjunct. (Grade: B)
3. Standard analgesics should be used in infants as in older
patients with careful attention to dosing and monitoring.
(Grade: B)
Procedural pain As for older patients, procedures are
one of the major sources of pain for infants with EB.
Wound care specifically requires a multidisciplinary team
approach to ensure consistent and optimized pain control.
There is evidence that a variety of pharmacologic and
non-pharmacologic interventions are helpful in both
term and pre-term infants [149]. Therefore, pain management interventions should precede all scheduled
painful procedures, such as dressing changes, bathing
and venipuncture. The range of analgesics and the routes
by which they can be administered are the same as for
older patients. Oral sucrose is an analgesic unique to
young infants and can be used alone for mild pain (for example, immunization pain [150]) or in conjunction with
other analgesics as well as physical and environmental interventions for more severe acute pain [40,151].
Bathing and dressing changes To maintain appropriate
moisture levels and facilitate the healing of wounds,
dressings should be non-adherent as for older patients
and appropriate in size. Infected wounds will require
more frequent dressing changes [57,152]. Changing
dressings one limb at a time is advocated in infants, to
reduce the likelihood of having the skin rubbed off the
opposite limb by feet kicking together, causing new,
painful lesions (see Box 8). This approach also decreases
the chance of bacterial spread from a colonized wound to
an uncontaminated area [57,78]. For baths, adding salt to
the water is recommended as for older patients (see subsection on environmental treatment under Bathing and
Dressing Changes).
In addition to environmental adjustments, many infants
will require analgesics with bath and dressing changes.
Page 15 of 23
NSAIDs, acetaminophen and opioids are all used, as for
older patients (see Section Bathing and Dressing Changes)
(see Box 8). Codeine is not recommended, when alternatives are available, as neonates lack the capacity to
metabolize the drug into active metabolites, and clinical
responses are highly variable at all ages, due to polymorphisms in codeines metabolic pathway [153,154].
Severely affected hospitalized infants Severely affected
newborns with deep tissue damage may require extensive pharmacologic support to achieve a level of comfort
(see Box 8). These infants may require around the clock
or continuous infusion of opioids and an adjuvant. A
transition to methadone for better steady state levels
should be considered (refer to sub-section on systemic
approaches under Skin and Wound Pain) for caveats
about methadone use). A case study has shown effective
pain control in an infant with severe chronic pain (and
possibly pruritus) when treated with gabapentin [155].
Patients receiving frequent opioid treatment may require
extra care in avoiding opioid-induced constipation and
in maintaining adequate caloric intake.
Oral ketamine has been used to supplement opioids
when pain associated with dressing changes is severe
[156]. Use of ketamine raises concerns due to findings of
adverse neurodevelopmental effects in young animals
who received prolonged intravenous infusions of ketamine [157]. However, these effects are not known to
occur in human infants and are unlikely to occur with
small doses administered at intervals.
Good practice points Infants benefit from the same
range of analgesics as older patients. They can uniquely
benefit from oral sucrose for brief painful episodes.
Careful monitoring is crucial in infants receiving sedating medications. Babies with EB and their parents benefit from close physical contact like any other families.
Holding and cuddling can be done safely, with scrupulous attention to lifting and handling in order to prevent
new lesions and pain.
End of life pain care
Introduction The epidemiology of death in EB varies by
type [158], but is not limited to dermatologic causes. Patients with JEB, generalized severe type are at greatest
risk of fatality early in life from a range of causes
[159,160]. Persons with RDEB may succumb in early to
mid-adulthood from multiple causes [161-163] whereas
patients with generalized types of EB simplex are at risk
of laryngotracheal complications [164].
The palliative approach to pain experienced by individuals who are facing life-threatening illness addresses the
physical, emotional and spiritual suffering of the patient
Goldschneider et al. BMC Medicine 2014, 12:178
http://www.biomedcentral.com/1741-7015/12/178
and includes support for the whole family [165-167]
(see Box 9). Squamous cell carcinoma is frequently diagnosed in patients with severe subtypes [168] and can
present challenges typical of cancer-related pain when
it metastasizes. The World Health Organization ladder
approach to pain care for those patients with cancer
and other persistent illnesses recommends a two-step
ladder as a framework for pain care [169].
Box 9. Recommendations for end of life pain
treatment
1. Assess and manage physical, emotional and spiritual suffering
of the patient, while providing support for the whole family.
(Grade: A)
2. Opioids are the cornerstone of good analgesia in this setting.
Opioid rotation may need to be considered to improve
analgesia and reduce side effects, and adjuncts may need to
be added. (Grade: B)
3. Consider targeted medication for neuropathic pain or when
pain proves refractory to convention therapies. (Grade: D)
4. Continuous subcutaneous infusion of medication is an option
when parenteral therapy is needed in the terminal phase.
(Grade: C)
5. Where needed, breakthrough medication can be given
transmucosally (oral or nasal) for rapid onset and avoidance
of the enteral route. (Grade: B)
Opioids Opioids have a role in EB pain management, as
previously indicated in these guidelines (see Box 9). Patients in the palliative phase of their illness may be given
an oral opioid sustained release medication [170]. Opioids should be titrated against pain and side effects, with
differences in approach needed depending on issues
such as opioid tolerance and rate of development of new
pain problems [170]. However, if appropriate opioid increases are not effective, it is important to consider
pharmacologic tolerance, poor absorption and neuropathic pain. Tolerance can be addressed by rotating the
opioid to capitalize upon incomplete cross-tolerance
[171,172]. In the face of poor absorption, parenteral
therapy may be needed (see below). If neuropathic pain
is suspected, methadone may be an option to consider.
It has N-methyl-D-aspartate (NMDA) antagonist action
in addition to mu-agonist properties common to standard opioids, and can be beneficial for neuropathic pain
[173] and does not rely on renal excretion [61], which
may be reduced in the palliative phase of EB [87].
Page 16 of 23
Although a recent meta-analysis could not establish differences in efficacy among types of opioids for neuropathic pain, it was determined that intermediate term
(weeks to months) use of opioids for neuropathic pain
may be helpful [174]. Cautions in the use of methadone
are discussed in the sub-section on systemic approaches
under Skin and Wound Pain.
Adjunctive measures for neuropathic pain Many EB
patients will have been treated with adjunctive agents
such as amitriptyline or gabapentin earlier in their illness, often with good effect [87,155]. These both may
take a period of time to achieve full analgesic effect and
usually need to be given by the enteral route. Ketamine is
more rapidly effective and can be given orally [84-86,175]
or used subcutaneously (see below). It should be noted
that when ketamine by-passes hepatic first pass metabolism, the relative proportion of norketamine is reduced and
the patient may experience more sedation and hallucinations and less analgesia for a given dose [175]. Other
options for addressing neuropathic pain (see Box 9) in
terminal care include opioid rotation to methadone
(see above), which can also be included in a subcutaneous infusion (see below).
Infusions and issues of drug delivery Parenteral administration of analgesia may be needed in the palliative
phase, when ability to take enteral medications is no longer an option or if rapid escalation of therapy is needed.
There has been an historic reluctance to use continuous
subcutaneous infusions, due to the fear of precipitating
further blistering. However, subcutaneous infusions have
been reported to be tolerated in the final days of life in
an adult EB patient [176] (see Box 9).
In non-EB patients with cancer pain, the subcutaneous
route of morphine is effective to a similar degree as the
intravenous [177]. Other alternatives, such as adherent
transdermal delivery systems, need regular removal and
replacement. Repeated subcutaneous/intramuscular injections are very frightening for children, as are attempts
to obtain IV access. Alternatively, sites of subcutaneous
needle insertion last reasonably well [87,177]. If subcutaneous sites do become inflamed, some benefit has been
shown from adding low dose dexamethasone to the infusion [178], although this has not been used to our knowledge in children with EB.
Breakthrough pain medication at the end of life Even
when good baseline pain relief has been achieved, most
patients will require occasional breakthrough doses of
analgesia. Uniformly effective breakthrough dosing protocols have not been determined for children with EB at
end of life, although there are general recommendations
Goldschneider et al. BMC Medicine 2014, 12:178
http://www.biomedcentral.com/1741-7015/12/178
from several international sources [169,179] and data to
support the use of up to 20% of total daily opioid consumption [180,181] in adults with cancer. In general, a
short-acting, immediate release form of opioid should be
given at approximately 10% to 15% of the total background opioid dose of the previous 24 hours. If rescue
dosing is used frequently and consistently, then the
baseline opioid dosing needs to be increased. Individual
patient factors should be taken into consideration (including prior opioid exposure, renal and hepatic function, other medication use) and consultation with an
expert in pain management and/or palliative care is recommended. The same principle is recommended for
opioids given via all routes of administration. When very
rapid onset is needed, transmucosal administration of
opioids may be preferable (see Box 9). Commercially
available transmucosal preparations of fentanyl are available in doses likely to be suitable for older children and
adults. Evidence supports the use of transbuccal fentanyl
for breakthrough pain in cancer patients [182]. An additional benefit of fentanyl is that it is not dependent on
renal excretion. In some centers, the injectable formulations of morphine or diamorphine have been used buccally at around a third of the standard enteral dose
(equivalent to the intravenous dose), allowing more
flexibility of dosing. It is also important to remember
that extreme anxiety may confound pain perception or
expression and that there may be benefit in offering additional doses of buccal midazolam where this is felt to be
a significant factor. Therapy should be targeted at specific symptoms whenever possible, although combination therapy is not unusual. Breakthrough analgesia
should be offered in the face of unexplained agitation in
case of undiagnosed pain, after which medication for
primary agitation/anxiety may be considered. While it is
likely that both of these would cause a degree of sedation at higher doses, this should not be the primary aim
of treatment.
Good practice points Palliative pain care is an expected
part of care for EB, which in many cases is life-limiting
in nature. All basic principles of palliative care apply as
they do for other terminal disease states.
Pruritus
Introduction Itch is a prominent, debilitating and damaging symptom for children with EB, but the mechanisms which lead to the manifestation of pruritus are
poorly understood [183]. Promising new insights into
the causes and potential treatments of chronic itch in
animal models [184], in human chronic itch generally
[185] and in recovering burn patients [186] may hold
potential for application in the EB population.
Page 17 of 23
Non-pharmacological approaches Multiple environmental and behavioral approaches to address itch have been
suggested [183,187] and include: prevention of dry skin
(systemic hydration and emollients), gentle debridement
of dry/dead/crusted skin, prevention and treatment of skin
wound infection; maintaining/supporting the healing
process by attention to anemia and nutritional status,
limiting damage to the skin by avoiding shear forces
imposed by scratching (short nails, occlusive barriers,
patting rather than pulling or tearing at a site), avoiding overheating and using measures to keep the body
cool (see Box 10). CBT is useful to reduce habitual
scratching behaviors (see section on psychological approaches). It is important to avoid and treat secondary
causes when present (such as drugs, environmental itch
triggers, underlying co-morbidities). Opioid-induced itch
in EB can be a problem and a difficult side effect to balance against the desired analgesia; opioid rotation may be
helpful.
Box 10. Recommendations for itch treatment
1. Use environmental and behavioral interventions for itch
control. (Grade: C)
2. Antihistamines are recommended and can be chosen
depending upon desirability of sedating effects. (Grade: D)
3. Gabapentin, pregabalin, TCA, serotonin norepinephrine
reuptake inhibitors (SNRIs) and other non-traditional
antipruritic agents should be strongly considered for itch
treatment. (Grade: C)
Pharmacological therapies Pharmacological therapies
include traditional oral antihistaminic medications (see
Box 10). Some patients prefer sedating formulations at
bedtime (for example, diphenhydramine, hydroxyzine,
chlorpheniramine) and others non-sedating preparations
during the day (for example, cetirizine, loratadine and
fexofenadine). Efficacy is variable and recommendations
are based on anecdotal experience for lack of good evidence in EB and other dermatologic conditions. Centrally
acting medications, such as gabapentin and pregabalin,
have evidence for efficacy from the burn literature
[186,188,189] and may have application in EB. Many of
these medications have also been used successfully for
neuropathic pain (see sub-section on adjunctive measures for neuropathic pain under End of Life Pain).
Antidepressants with nortriptyline re-uptake inhibitory
actions have been used for various pruritic conditions
with some evidence for efficacy, with mirtazapine showing
Goldschneider et al. BMC Medicine 2014, 12:178
http://www.biomedcentral.com/1741-7015/12/178
promise [190-193]. Low-dose cyclosporine has been used
in a single case of dominant dystrophic EB to reduce generalized itching [185,194]. Anecdotal success has been reported with ondansetron in EB; however, the same had
been reported for pruritus from cholestatic jaundice, although controlled trials did not confirm efficacy [195].
Similar suggestions were made related to the pruritus
of uremia [196,197], leading to recommendations that
ondansetron should be considered, although clinical
trials are needed in EB.
Other medications that have shown sporadic clinical
success in treating itch in EB include: cyproheptadine;
selective serotonin re-uptake inhibitors (SSRIs; fluoxetine, paroxetine, sertraline, fluvoxamine) [193]; tricyclic
antidepressants (doxepin, amitriptyline, nortriptyline) [192];
opioid antagonists (naloxone, naltrexone); kappa receptor
agonists (butorphanol, dextromethorphan, nalbuphine);
other 5-HT3 receptor antagonists (granisetron, dolasetron); antipsychotic agents (olanzapine, pimozide) and
cannabinoids. These agents and the NK-1 receptor antagonist aprepitant may prove to be useful in certain subsets
of patients, although evidence to guide therapy is lacking
[198] and practitioners are encouraged to pursue the aforementioned therapies based on patient response to prior
medications, potential interactions within the patients
medication list and medication availability (see Box 10).
It is common practice for medications from different
drug classes to be used concurrently and for agents in
the same class to be rotated due to the observation that
a particular medication may have improved efficacy after
intermittent drug holiday.
Good practice points A combination of environmental,
cognitive-behavioral and pharmacologic therapies is available for use for EB-related pruritus, which can be a severe
symptom of the disease.
Conclusions
These guidelines represent the initial effort to organize pain
management for patients with EB based on existing evidence. While the guidelines were developed using current
evidence and a rigorous evaluation process, there are limitations in the clinical use of the recommendations. The two
Table 5 Implementation barriers
1. Availability of resources (for example, medications and equipment)
Page 18 of 23
Table 6 Areas of research
Psychological and integrative approaches:
1. Test the efficacy of well-established cognitive behavioral
interventions for acute and chronic pain management in EB.
2. Develop EB-specific pain assessment measures for both acute and
chronic pain.
3. Evaluate the efficacy of cognitive behavioral therapy for EB-related
pruritus
4. Evaluate the role for Integrative Medicine techniques for the EB
population.
Acute pain:
1. Improve the balance between analgesia and side effects specific to
EB (for example, itching).
2. Establish optimal treatment of needle-related pain.
3. Define the role for ketamine and other non-opioid agents.
Chronic and recurrent pain:
1. Evaluate topical therapies including opioids, local anesthetics and
NSAIDs.
2. Determine optimal environmental interventions for bath and
dressing changes including bath additives (salt, bleach, oatmeal).
3. Define optimal perianal pain therapies.
4. Clarify the role of bone density screening in preventing bone pain
and fractures.
5. Determine the role of topical NSAIDs in treatment of corneal
abrasion pain.
6. Explore the role for various physical and occupational therapy
interventions for joint, bone and back pain.
Infants:
1. Validate observational pain scales in the setting of bandaged infants.
2. Determine the safety and dosing of adjunct medications, such as
gabapentin and topical agents.
Pruritus:
1. Establish the mechanisms of pruritus in EB and effective treatment
thereof.
2. Refine the management of opioid-exacerbated itch.
End of life:
1. Define how best to integrate palliative care into the overall care of
patients with EB prior to end of life.
2. Define optimal treatments for pain at the end of life.
A focused list to represent the broad categories that would benefit from
studies in patients with EB.
broad areas of concern involve practical limitations of implementation and the level of available evidence. Tables 5
and 6 identify issues for implementation of the guidelines
as well as general recommendations areas for research to
enhance the level of evidence.
2. Legal and social restrictions on the use of various medications and
therapies.
3. Limited and uneven distribution of knowledge and expertise
4. International dissemination of guidelines and EB-related information
to local care providers and families (includes translation and access
to electronic and print media)
Additional file
Additional file 1: EB-specific articles that were excluded from use in
making recommendations, with rationales.
Goldschneider et al. BMC Medicine 2014, 12:178
http://www.biomedcentral.com/1741-7015/12/178
Abbreviations
CBT: cognitive behavioral therapy/techniques; CHEOPS: Childrens Hospital of
Eastern Ontario Pain Scale; CRIES: Crying, requires oxygen, Increased vital
signs, Expression and Sleepless Pain Scale; DDEB: dominant dystrophic
epidermolysis bullosa; DEB: dystrophic epidermolysis bullosa (dominant and
recessive types); EB: epidermolysis bullosa; EBS: epidermolysis bullosa simplex
(basal and suprabasal types); FLACC: Face Legs Arms Cry Consolability Pain
Scale; GERD: gastroesophageal reflux disease; JEB: junctional epidermolysis
bullosa (generalized and localized); NIPS: Neonatal Infant Pain Scale;
NMDA: N-methyl-d-aspartate; NSAIDs: non-steroidal anti-inflammatory drugs;
N-PASS: Neonatal Pain Agitation and Sedation Scale; PCA: patient controlled
analgesia; PIPP: Premature Infant Pain Profile; RDEB: recessive dystrophic
epidermolysis bullosa.
Page 19 of 23
3.
4.
5.
6.
7.
Competing interests
The authors declare that they have no competing interests.
8.
Authors contributions
This work was initiated and led by KRG with active input from all authors. JG,
EH, CL, ALJ, AEM, LGM and DSL participated in the review process and
recommendation/guideline draft, see text for details. DSL led the systematic
evidence analysis and provided methodological support and guidance.
Multi-disciplinary clinician input was obtained as was input from patients
and families early in the process (see Acknowledgments, below). The
consensus meeting (see text) was attended in person or via Skype by
KRG, ALJ, EH, JG, CL, LGM and BK (see Acknowledgements). All authors
read and approved the final manuscript.
9.
10.
11.
Acknowledgments
Guideline development was supported by a small grant from DEBRA USA to
defray the costs of travel, accommodation and preparation related to the
consensus meeting, held on 4, 5 May 2012 in Cincinnati, Ohio, USA. The
following members of the original guidelines development committee
helped with initial content development and recommendations: Beverly Inge
Walti, Kara Malcolm, Teresa Mingrone, and Stacy Shipley.
The following Clinician Reviewers are gratefully acknowledged: Anna L.
Bruckner, MD, Elizabeth Ely, RN, PhD, Kim Hazelbaker, RN, Barbara Hoggart,
MD, Richard F. Howard, BSc, FRCA, Anne Lucky, MD, Geraldine Mancuso-Kelly,
RN, Elena Pope, MD, Susan Rowe, RN, Alexandra Szabova, MD, Jean Whalen, RN.
Warm thanks to the following Family and Patient Reviewers: Patsy
DiGiovanna, Michelle Starkey, Natasha Starkey and *Brett Kopelan
(*participated in consensus meeting).
Special thanks to Andrea Ayers (administrative assistant to KRG), Brett
Kopelin (DEBRA USA), Francis Palisson (DEBRA Chile) and Avril Keenan
(DEBRA Ireland) for their support.
Author details
1
Pain Management Center, Department of Anesthesiology, Cincinnati Childrens
Hospital Medical Center, Cincinnati, Ohio, USA. 2Lucille Packard Childrens
Hospital, Department of Anesthesia (by courtesy, Pediatrics), Stanford University,
Stanford, California, USA. 3Helen and Douglas Hospices, Oxford and John
Radcliffe Hospital, Oxford, USA. 4University of Southampton, Southampton, UK.
5
Great Ormond Street Hospital for Children NHS Trust, London, UK. 6Pain
Management Center and Division of Behavioral Medicine and Clinical
Psychology, Cincinnati Childrens Hospital Medical Center, Cincinnati, Ohio, USA.
7
National Paediatric Epidermolysis Bullosa Centre, Great Ormond Street Hospital
NHS Foundation Trust, London, UK. 8Department of Anesthesiology and Critical
Care, Childrens Hospital of Philadelphia, Philadelphia, Pennsylvania, USA. 9James
M. Anderson Center for Health Systems Excellence, Cincinnati Childrens
Hospital Medical Center, Cincinnati, Ohio, USA.
12.
13.
14.
15.
16.
17.
18.
19.
20.
21.
22.
Received: 19 December 2013 Accepted: 9 September 2014
23.
References
1. Fine JD, Johnson LB, Weiner M, Suchindran C: Assessment of mobility,
activities, and pain in different subtypes of epidermolysis bullosa. Clin
Exp Dermatol 2004, 29:122127.
2. Tabolli S, Sampogna F, Di Pietro C, Paradisi A, Uras C, Zotti P, Castiglia D,
Zambruno G, Abeni D: Quality of life in patients with epidermolysis
bullosa. Br J Dermatol 2009, 161:869877.
24.
25.
Margari F, Lecce PA, Santamato W, Ventura P, Sportelli N, Annicchiarico G,
Bonifazi E: Psychiatric symptoms and quality of life in patients affected
by epidermolysis bullosa. J Clin Psychol Med Settings 2010, 17:333339.
Van Scheppingen C, Lettinga AT, Duipmans JC, Maathius CG, Jonkman MF:
Main problems experienced by children with Epidermolysis Bullosa: a
qualitative study with semi-structured interviews. Acta Derm Venerol 2008,
88:143150.
Fine J, Bruckner-Tuderman L, Eady RA, Bauer EA, Bauer JW, Has C, Heagerty A,
Hintner H, Hovnanian A, Jonkman MF, Leigh I, Marinkovich P, Martinez AE,
McGrath JA, Mellerio JE, Moss C, Murrell DF, Shimizu H, Uitto J, Woodley D,
Zambruno G: Inherited epidermolysis bullosa: updated recommendations
on diagnosis and classification. J Am Acad Dermatol 2014, 70:11031126.
Debra International [http://www.debra-international.org/homepage.html]
Clark E, Burkett K, Stanko-Lopp D: Let Evidence Guide Every New Decision
(LEGEND): an evidence evaluation system for point-of-care clinicians and
guideline development teams. J Eval Clin Pract 2009, 15:10541060.
Cincinnati Childrens Hospital Medical Center: LEGEND documents. 2013.
http://www.cincinnatichildrens.org/service/j/anderson-center/evidencebased-care/legend/.
Brozek JL, Akl EA, Alonso-Coello P, Lang D, Jaeschke R, Williams JW: Grading
quality of evidence and strength of recommendations in clinical practice
guidelines. Part 1 of 3. An overview of the GRADE approach and grading
quality of evidence about interventions. Allergy 2009, 64:669677.
Guyatt GH, Oxman AD, Vist GE, Kunz R, Falck-Ytter Y, Alonso-Coello P,
Schnemann HJ, GRADE Working Group: GRADE: an emerging consensus
on rating quality of evidence and strength of recommendations. BMJ 2008,
336:924926.
Debra International pain management guidelines page [http://www.
debra-international.org/med-professionals/best-clinical-practice-guidelinesbcpg/pain-management.html]
Gatchel RJ, Peng YB, Peters ML, Fuchs PN, Turk DC: The biopsychosocial
approach to chronic pain: scientific advances and future directions.
Psychol Bull 2007, 133:581624.
Gerik SM: Pain management in children: developmental considerations
and mind-body therapies. South Med J 2005, 98:295302.
Green JP, Barabasz AF, Barrett D, Montgomery GH: Forging ahead: the
2003 APA Division 30 definition of hypnosis. Int J Clin Exp Hypn 2005,
53:259264.
Palermo TM, Chambers CT: Parent and family factors in pediatric chronic
pain and disability: an integrative approach. Pain 2005, 119:14.
Eccleston C, Palermo TM, Williams AC, Lewandowski A, Morely S: Psychological
therapies for the management of chronic and recurrent pain in children and
adolescents. Cochrane Database Syst Rev 2009, 2, CD003968.
Palermo TM, Eccleston C, Lewandowski AS, Williams AC, Morley S:
Randomized controlled trials of psychological therapies for management
of chronic pain in children and adolescents: an updated meta-analytic
review. Pain 2010, 148:387397.
Kashikar-Zuck S, Swain NF, Jones BA, Graham TB: Efficacy of cognitivebehavioral intervention for juvenile primary fibromyalgia syndrome.
J Rheumatol 2005, 32:15941602.
Eccleston C, Williams AC, Morley S: Psychological therapies for the
management of chronic pain (excluding headache) in adults. Cochrane
Database Syst Rev 2009, 2, CD007407.
Richardson J, Smith JE, McCall G, Pilkington K: Hypnosis for procedure-related
pain and distress in pediatric cancer patients: a systematic review of
effectiveness and methodology related to hypnosis interventions. J Pain
Symptom Manage 2006, 31:7084.
Uman LS, Chambers CT, McGrath PJ, Kisely S: Psychological interventions
for needle-related procedural pain and distress in children and adolescents.
Cochrane Database Syst Rev 2006, 4, CD005179.
Chambers CT, Taddio A, Uman LS, McMurtry CM, HELPinKIDS Team: Psychological
interventions for reducing pain and distress during routine childhood
immunizations: a systematic review. Clin Ther 2009, 31:S77S103.
Kleiber C, Harper DC: Effects of distraction on children's pain and
distress during medical procedures: a meta-analysis. Nurs Res 1999,
48:4449.
Liossi C, White P, Hatira P: A randomized clinical trial of a brief hypnosis
intervention to control venepuncture-related pain of paediatric cancer
patients. Pain 2009, 142:255263.
Malloy KM, Milling LS: The effectiveness of virtual reality distraction for
pain reduction: a systematic review. Clin Psychol Rev 2010, 30:10111018.
Goldschneider et al. BMC Medicine 2014, 12:178
http://www.biomedcentral.com/1741-7015/12/178
26. Hanson MD, Gauld M, Wathen CN, Macmillan HL: Nonpharmacological
interventions for acute wound care distress in pediatric patients with
burn injury: a systematic review. J Burn Care Res 2008, 29:730741.
27. Liossi C, Franck L: Psychological interventions for acute pediatric pain. In
Clinical Pain Management Acute Pain. Edited by Macintyre P, Rowbotham D,
Walker S. London: Hodder Arnold; 2008:308323.
28. Hagermark O, Wahlgren C: Treatment of itch. Semin Dermatol 1995,
14:320325.
29. Chida Y, Steptoe A, Hirakawa N, Sudo N, Kubo C: The effects of
psychological intervention on atopic dermatitis. A systematic review and
meta-analysis. Int Arch Allergy Immunol 2007, 144:19.
30. Azrin NH, Nunn RG: Habit-reversal: a method of eliminating nervous
habits and tics. Behav Res Ther 1973, 11:619628.
31. Rosenbaum MS, Ayllon T: The behavioral treatment of neurodermatitis
through habit-reversal. Behav Res Ther 1981, 19:313318.
32. Ehlers A, Stangier U, Gieler U: Treatment of atopic dermatitis: a
comparison of psychological and dermatological approaches to relapse
prevention. J Consult Clin Psychol 1995, 63:624635.
33. Hopton A, MacPherson H: Acupuncture for chronic pain: is acupuncture
more than an effective placebo? A systematic review of pooled data
from meta-analyses. Pain Pract 2010, 10:94102.
34. Cepeda MS, Carr DB, Lau J, Alvarez H: Music for pain relief. Cochrane
Database Syst Rev 2006, 2, CD004843.
35. Bussing A, Ostermann T, Ludtke R, Michalsen A: Effects of yoga
interventions on pain and pain-associated disability: a meta-analysis.
J Pain 2012, 13:19.
36. Cordier W, Steenkamp V: Herbal remedies affecting coagulation: a review.
Pharm Biol 2012, 50:443452.
37. Kashikar-Zuck S, Lynch AM: Psychological interventions for chronic pain.
In Pain in Children: A Practical Guide for Primary Care. Edited by Walco GA,
Goldschneider KR. Totowa, NJ: Humana Press; 2008:145152.
38. Power N, Liossi C, Franck L: Helping parents to help their child with
procedural and everyday pain: practical, evidence-based advice. J Spec
Pediatr Nurs 2007, 12:203209.
39. von Baeyer CL, Spagrud LJ: Systematic review of observational
(behavioral) measures of pain for children and adolescents aged 3 to
18 years. Pain 2007, 127:140150.
40. Stinson JN, Kavanagh T, Yamada J, Gill N, Stevens B: Systematic review of
the psychometric properties, interpretability and feasibility of self-report
pain intensity measures for use in clinical trials in children and adolescents.
Pain 2006, 125:143157.
41. Goldschneider K, Lucky AW, Mellerio JE, Palisson F, del Carmen Viuela Miranda M,
Azizkhan RG: Perioperative care of patients with epidermolysis bullosa:
proceedings of the 5th international symposium on epidermolysis bullosa,
Santiago Chile, December 46, 2008. Pediatr Anaesth 2010, 20:797804.
42. Goldschneider KR, Lucky AW: Pain management in epidermolysis bullosa.
Dermatol Clin 2010, 28:273282.
43. Steffel J, Luscher TF, Ruschitzka F, Tanner FC: Cyclooxygenase-2 inhibition
and coagulation. J Cardiovasc Pharmacol 2006, 47:S15S20.
44. Herod J, Denyer J, Goldman A, Howard R: Epidermolysis bullosa in
children: pathophysiology, anaesthesia and pain management. Paediatr
Anaesth 2002, 12:388397.
45. Manjushree R, Lahiri A, Ghosh BR, Laha A, Handa K: Intranasal fentanyl provides
adequate postoperative analgesia in pediatric patients. Can J Anaesth 2002,
49:190193.
46. Borland M, Jacobs I, King B, O'Brien D: A randomized controlled trial
comparing intranasal fentanyl to intravenous morphine for managing
acute pain in children in the emergency department. Ann Emerg Med
2007, 49:335340.
47. Desjardins PJ, Norris LH, Cooper SA, Reynolds DC: Analgesic efficacy of
intranasal butorphanol (Stadol NS) in the treatment of pain after dental
impaction surgery. J Oral Maxillofac Surg 2000, 58:1926.
48. Kelly RE: Regional anesthesia in children with epidermolysis bullosa
dystrophica. Anesthesiology 1988, 68:469.
49. Sopchak AM, Thomas PS, Clark WR: Regional anesthesia in a patient with
epidermolysis bullosa. Reg Anesth 1993, 18:132134.
50. Yee LL, Gunter JB, Manley CB: Caudal epidural anesthesia in an infant
with epidermolysis bullosa. Anesthesiology 1989, 70:149151.
51. Diwan R, Vas L, Shah T, Raghavendran S, Ponde V: Continuous axillary
block for upper limb surgery in a patient with epidermolysis bullosa
simplex. Paediatr Anaesth 2001, 11:603606.
Page 20 of 23
52. Englbrecht JS, Langer M, Hahnenkamp K, Ellger B: Ultrasound-guided
axillary plexus block in a child with dystrophic epidermolysis bullosa.
Anaesth Intensive Care 2010, 38:11011105.
53. Doi S, Horimoto Y: Subcutaneous tunnelling of an epidural catheter in a
child with epidermolysis bullosa. Acta Anaesth Scand 2006, 50:394395.
54. Viscusi ER, Martin G, Hartrick CT, Singla N, Manvelian G, EREM Study Group:
Forty-eight hours of postoperative pain relief after total hip arthroplasty
with a novel, extended-release epidural morphine formulation.
Anesthesiology 2005, 102:10141022.
55. Mhuircheartaigh RJ, Moore RA, McQuay HJ: Analysis of individual patient data
from clinical trials: epidural morphine for postoperative pain. Br J Anaesth
2009, 103:874881.
56. Hartrick CT, Hartrick KA: Extended-release epidural morphine (DepoDur):
review and safety analysis. Expert Rev Neurother 2008, 8:16411648.
57. Denyer JE: Wound management for children with epidermolysis bullosa.
Dermatol Clin 2010, 28:257264.
58. Chou R, Fanciullo GJ, Fine PG, Adler JA, Ballantyne JC, Davies P, Donovan MI,
Fishbain DA, Foley KM, Fudin J, Gilson AM, Kelter A, Mauskop A, O'Connor PG,
Passik SD, Pasternak GW, Portenoy RK, Rich BA, Roberts RG, Todd KH,
Miaskowski C, American Pain Society-American Academy of Pain Medicine
Opioids Guidelines Panel: Clinical guidelines for the use of chronic
opioid therapy in chronic noncancer pain. J Pain 2009, 10:113130.
59. Noble M, Treadwell JR, Tregear SJ, Coates VH, Wiffen PJ, Akafomo C,
Schoelles KM: Long-term opioid management for chronic noncancer
pain. Cochrane Database Syst Rev 2010, 1, CD006605.
60. Katz N, Mazer NA: The impact of opioids on the endocrine system. Clin J
Pain 2009, 25:170175.
61. Davies D, Vlaming D, Haines C: Methadone analgesia for children with
advanced cancer. Pediatr Blood Cancer 2008, 51:393397.
62. Huh B, Park CH: Retrospective analysis of low-dose methadone and QTc
prolongation in chronic pain patients. Korean J Anesthesiol 2010, 58:338343.
63. Cruciani RA: Methadone: to ECG or not to ECGThat is still the question.
J Pain Symptom Manage 2008, 36:545552.
64. Martin JA, Campbell A, Killip T, Kotz M, Krantz MJ, Kreek MJ, McCarroll BA,
Mehta D, Payte JT, Stimmel B, Taylor T, Haigney MC, Wilford BB, Substance
Abuse and Mental Health Services Administration: QT interval screening in
methadone maintenance treatment: report of a SAMHSA expert panel.
J Addict Dis 2011, 30:283306.
65. Nicholson AB: Methadone for cancer pain. Cochrane Database Syst Rev
2009, 4, CD003971.
66. Camilleri M: Opioid-induced constipation: challenges and therapeutic
opportunities. Am J Gastroenterol 2011, 106:835842.
67. Moore RA, Wiffen PJ, Derry S, McQuay HJ: Gabapentin for chronic
neuropathic pain and fibromyalgia in adults. Cochrane Database Syst Rev
2011, 3, CD007938.
68. Chiu YK, Prendiville JS, Bennett SM, Montgomery CJ, Oberlander TF: Pain
management of junctional epidermolysis bullosa in an 11-year-old boy.
Pediatr Dermatol 1999, 16:465468.
69. Gray P, Williams B, Cramond T: Successful use of gabapentin in acute
pain management following burn injury: a case series. Pain Med 2008,
9:371376.
70. Lara-Corrales I, Mellerio JE, Martinez AE, Green A, Lucky AW, Azizkhan RG,
Murrell DF, Agero AL, Kantor PF, Pope E: Dilated cardiomyopathy in
epidermolysis bullosa: a retrospective, multicenter study. Pediatr Dermatol
2010, 27:238243.
71. Taibjee SM, Ramani P, Brown R, Moss C: Lethal cardiomyopathy in
epidermolysis bullosa associated with amitriptyline. Arch Dis Child 2005,
90:871872.
72. Twillman RK, Long TD, Cathers TA, Mueller DW: Treatment of painful skin
ulcers with topical opioids. J Pain Symptom Manage 1999, 17:288292.
73. LeBon B, Zeppetella G, Higginson IJ: Effectiveness of topical
administration of opioids in palliative care: a systematic review. J Pain
Symptom Manage 2009, 37:913917.
74. Watterson G, Howard R, Goldman A: Peripheral opioids in inflammatory
pain. Arch Dis Child 2004, 89:679681.
75. Than MP, Smith RA, Cassidy S, Kelly R, Marsh C, Maderal A, Kirsner RS: Use
of a keratin-based hydrogel in the management of recessive dystrophic
epidermolysis bullosa. J Dermatol Treat 2013, 24:290291.
76. Lander JA, Weltman BJ, So SS: EMLA and amethocaine for reduction of
childrens pain associated with needle insertion. Cochrane Database Syst
Rev 2006, 3, CD004236.
Goldschneider et al. BMC Medicine 2014, 12:178
http://www.biomedcentral.com/1741-7015/12/178
77. Cepeda MS, Tzortzopoulou A, Thackrey M, Hudcova J, Arora Gandhi P,
Schumann R: Adjusting the pH of lidocaine for reducing pain on
injection. Cochrane Database Syst Rev 2010, 12, CD006581.
78. Arbuckle HA: Bathing for individuals with Epidermolysis bullosa.
Dermatol Clin 2010, 28:265266.
79. Cerio R, Dohil M, Jeanine D, Magina S, Mah E, Stratigos AJ: Mechanism of
action and clinical benefits of colloidal oatmeal for dermatologic
practice. J Drugs Dermatol 2010, 9:11161120.
80. Peterson B, Berman S, Arbuckle A: The effectiveness of saltwater baths in
the treatment of patients with epidermolysis bullosa. Poster presented at
the 37th Annual Meeting of the Society of Pediatric Dermatology, Baltimore
July 710, 2011.
81. Wolfe TR, Braude DA: Intranasal medication delivery for children: a brief
review and update. Pediatrics 2010, 126:532537.
82. Ezike HA, Odiakosa MC: Oral ketamine for wound care procedures in
adult patients with burns. South Afr J Anaesth Analg 2011, 17:242248.
83. Humphries Y, Melson M, Gore D: Superiority of oral ketamine as an
analgesic and sedative for wound care procedures in the pediatric
patient with burns. J Burn Care Rehabil 1997, 18:3436.
84. Blonk MI, Koder BG, van den Bemt PM, Huygen FJ: Use of oral ketamine in
chronic pain management: a review. Eur J Pain 2010, 14:466472.
85. Bell RF, Eccleston C, Kalso EA: Ketamine as an adjuvant to opioids for
cancer pain. Cochrane Database Syst Rev 2012, 11, CD003351.
86. Ugur F, Gulcu N, Boyaci A: Oral ketamine for pain relief in a child with
abdominal malignancy. Pain Med 2009, 10:120121.
87. Watterson G, Denyer J, Hain R: Skin Symptoms. In Oxford Textbook of
Palliative Care for Children. Edited by Goldman A, Hain R, Liben S. Oxford, UK:
Oxford University Press; 2005:448459.
88. Burton JH, Auble TE, Fuchs SM: Effectiveness of 50% nitrous oxide/50%
oxygen during laceration repair in children. Acad Emerg Med 1998, 5:112117.
89. Rowland AS, Baird DD, Shore DL, Weinberg CR, Savitz DA, Wilcox AJ:
Nitrous oxide and spontaneous abortion in female dental assistants.
Am J Epidemiol 1995, 141:531538.
90. Nunn JF, Chanarin I, Tanner AG, Owen ER: Megaloblastic bone marrow
changes after repeated nitrous oxide anaesthesia. Reversal with folinic
acid. Br J Anaesth 1986, 58:14691470.
91. Sanders RD, Weimann J, Maze M: Biologic effects of nitrous oxide: a
mechanistic and toxicologic review. Anesthesiology 2008, 109:707722.
92. Loureno-Matharu L, Ashley PF, Furness S: Sedation of children undergoing
dental treatment. Cochrane Database Syst Rev 2012, 3, CD003877.
93. Tyagi P, Dixit U, Tyagi S, Jain A: Sedative effects of oral midazolam,
intravenous midazolam and oral diazepam. J Clin Pediatr Dent 2012,
36:383388.
94. Patterson DR, Ptacek JT, Carrougher GJ, Sharar SR: Lorazepam as an
adjunct to opioid analgesics in the treatment of burn pain. Pain 1997,
72:367374.
95. Freeman EB, Kglmeier J, Martinez AE, Mellerio JE, Haynes L, Sebire NJ,
Lindley KJ, Shah N: Gastrointestinal complications of epidermolysis
bullosa in children. Br J Dermatol 2008, 158:13081314.
96. Fine JD, Mellerio JE: Extracutaneous manifestations and complications
of inherited epidermolysis bullosa: part I. Epithelial associated tissues.
J Am Acad Dermatol 2009, 61:367384.
97. Travis SP, McGrath JA, Turnbull AJ, Schofield OM, Chan O, O'Connor AF,
Mayou B, Eady RA, Thompson RP: Oral and gastrointestinal manifestations
of epidermolysis bullosa. Lancet 1992, 340:15051506.
98. Ergun GA, Lin AN, Dannenberg AJ, Carter DM: Gastrointestinal
manifestations of epidermolysis bullosa. A study of 101 patients.
Medicine 1992, 71:121127.
99. Marini I, Vecchiet F: Sucralfate: a help during oral management in
patients with epidermolysis bullosa. J Periodontol 2001, 72:691695.
100. Buchsel PC: Gelclair oral gel. Clin J Oncol Nurs 2003, 7:109110.
101. Buchsel PC: Polyvinylpyrrolidone-sodium hyaluronate gel (Gelclair): a
bioadherent oral gel for the treatment of oral mucositis and other
painful oral lesions. Expert Opin Drug Metab Toxicol 2008, 4:14491454.
102. Cingi C, Songu M, Ural A, Yildirim M, Erdogmus N, Bal C: Effects of
chlorhexidine/benzydamine mouth spray on pain and quality of life in
acute viral pharyngitis: a prospective, randomized, double-blind,
placebo-controlled, multicenter study. Ear Nose Throat J 2010, 89:546549.
103. Vandenplas Y, Rudolph CD, Di Lorenzo C, Hassall E, Liptak G, Mazur L,
Sondheimer J, Staiano A, Thomson M, Veereman-Wauters G, Wenzl TG,
North American Society for Pediatric Gastroenterology Hepatology and
Page 21 of 23
104.
105.
106.
107.
108.
109.
110.
111.
112.
113.
114.
115.
116.
117.
118.
119.
120.
121.
122.
123.
124.
125.
126.
Nutrition, European Society for Pediatric Gastroenterology Hepatology and
Nutrition: Pediatric gastroesophageal reflux clinical practice guidelines:
joint recommendations of the North American Society for Pediatric
Gastroenterology, Hepatology, and Nutrition (NASPGHAN) and the
European Society for Pediatric Gastroenterology, Hepatology, and
Nutrition (ESPGHAN). J Pediatr Gastroenterol Nutr 2009, 49:498547.
Nwokediuko SC: Current trends in the management of gastroesophageal
reflux disease: a review. ISRN Gastroenterol 2012, 2012:391631.
Fine JD, Johnson LB, Weiner M, Suchindran C: Gastrointestinal
complications of inherited epidermolysis bullosa: cumulative experience
of the National Epidermolysis Bullosa Registry. J Pediatr Gastroenterol Nutr
2008, 46:147158.
Lai-Cheong JE, McGrath JA: What is Kindler syndrome? Skinmed 2011,
9:145146.
Azizkhan RG, Stehr W, Cohen AP, Wittkugel E, Farrell MK, Lucky AW,
Hammelman BD, Johnson ND, Racadio JM: Esophageal strictures in
children with recessive dystrophic epidermolysis bullosa: an 11-year
experience with fluoroscopically guided balloon dilatation. J Pediatr
Surg 2006, 41:5560.
Anderson SH, Meenan J, Williams KN, Eady RA, Prinja H, Chappiti U, Doig L,
Thompson RP: Efficacy and safety of endoscopic dilation of esophageal
strictures in epidermolysis bullosa. Gastrointest Endosc 2004, 59:2832.
Mortell AE, Azizkhan RG: Epidermolysis bullosa: management of
esophageal strictures and enteric access by gastrostomy. Dermatol Clin
2010, 28:311318.
Dohil R, Aceves SS, Dohil MA: Oral viscous budesonide therapy in children
with epidermolysis bullosa and proximal esophageal strictures. J Pediatr
Gastroenterol Nutr 2011, 52:776777.
Hsieh CH, Huang CJ, Lin GT: Death from colonic disease in epidermolysis
bullosa dystrophica. BMC Dermatol 2006, 6:2.
Belsey JD, Geraint M, Dixon TA: Systematic review and meta analysis:
polyethylene glycol in adults with non-organic constipation. Int J Clin
Pract 2010, 64:944955.
Hanson S, Bansal N: The clinical effectiveness of Movicol in children with
severe constipation: an outcome audit. Paediatr Nurs 2006, 18:2428.
Shah N, Freeman E, Martinez A, Mellerio J, Smith VV, Lindley KJ, Sebire NJ:
Histopathological features of gastrointestinal mucosal biopsy specimens
in children with epidermolysis bullosa. J Clin Pathol 2007, 60:843844.
Gupta PJ, Heda PS, Shrirao SA, Kalaskar SS: Topical sucralfate treatment of
anal fistulotomy wounds: a randomized placebo-controlled trial. Dis
Colon Rectum 2011, 54:699704.
Alpsoy E, Er H, Durusoy C, Yilmaz E: The use of sucralfate suspension in
the treatment of oral and genital ulceration of Behet disease: a
randomized, placebo-controlled, double-blind study. Arch Dermatol 1999,
135:529532.
Nelson RL, Thomas K, Morgan J, Jones A: Non surgical therapy for anal
fissure. Cochrane Database Syst Rev 2012, 2, CD003431.
Poh A, Tan KY, Seow-Choen F: Innovations in chronic anal fissure treatment:
a systematic review. World J Gastrointest Surg 2010, 27:231241.
Khan MT: Podiatric management in epidermolysis bullosa. Dermatol Clin
2010, 28:325333.
Thastum M, Herlin T, Zachariae R: Relationship of pain-coping strategies
and pain-specific beliefs to pain experience in children with juvenile
idiopathic arthritis. Arthritis Rheum 2005, 53:178184.
Terrill PJ, Mayou BJ, McKee PH, Eady RA: The surgical management of
dystrophic epidermolysis bullosa (excluding the hand). Br J Plast Surg
1992, 45:426434.
Maritsi D, Martinez AE, Mellerio JE, Eleftheriou D, Pilkington CA: An unusual
case of epidermolysis bullosa complicated by persistent oligoarticular
juvenile idiopathic arthritis; lessons to be learned. Pediatr Rheumatol
Online J 2011, 9:13.
Gubinelli E, Angelo C, Pacifico V: A case of dystrophic epidermolysis
bullosa improved with etanercept for concomitant psoriatic arthritis. Am
J Clin Dermatol 2010, 11:5354.
Fewtrell MS, Allgrove J, Gordon I, Brain C, Atherton D, Harper J, Mellerio JE,
Martinez AE: Bone mineralization in children with epidermolysis bullosa.
Br J Dermatol 2006, 154:959962.
Martinez AE, Mellerio JE: Osteopenia and osteoporosis in epidermolysis
bullosa. Dermatol Clin 2010, 28:353355.
Bruckner AL, Bedocs LA, Keiser E, Tang JY, Doernbrack C, Arbuckle HA,
Berman S, Kent K, Bachrach LK: Correlates of low bone mass in children
Goldschneider et al. BMC Medicine 2014, 12:178
http://www.biomedcentral.com/1741-7015/12/178
127.
128.
129.
130.
131.
132.
133.
134.
135.
136.
137.
138.
139.
140.
141.
142.
143.
144.
145.
146.
147.
148.
149.
150.
with generalized forms of epidermolysis bullosa. J Am Acad Dermatol
2011, 65:10011009.
Lacativa PG, Farias ML: Osteoporosis and inflammation. Arq Bras Endocrinol
Metabol 2010, 54:123132.
Tilg H, Moschen AR, Kaser A, Pines A, Dotan I: Gut, inflammation and
osteoporosis: basic and clinical concepts. Gut 2008, 57:684694.
Levis S, Theodore G: Summary of AHRQs comparative effectiveness
review of treatment to prevent fractures in men and women with low
bone density or osteoporosis: update of the 2007 report. J Manag Care
Pharm 2012, 18:S115. discussion S13.
Noguera A, Ros JB, Pava C, Alcover E, Valls C, Villaronga M, Gonzlez E:
Bisphosphonates, a new treatment for glucocorticoid-induced osteoporosis
in children. J Pediatr Endocrinol Metab 2003, 16:529536.
Gandrud LM, Cheung JC, Daniels MW, Bachrach LK: Low-dose intravenous
pamidronate reduces fractures in childhood osteoporosis. J Pediatr
Endocrinol Metab 2003, 16:887892.
Falcini F, Trapani S, Ermini M, Brandi ML: Intravenous administration of
alendronate counteracts the in vivo effects of glucocorticoids on bone
remodeling. Calcif Tissue Int 1996, 58:166169.
Chou R, Qaseem A, Snow V, Casey D, Cross JT Jr, Shekelle P, Owens DK,
Clinical Efficacy Assessment Subcommittee of the American College of
Physicians, American College of Physicians, American Pain Society Low Back
Pain Guidelines Panel: Diagnosis and treatment of low back pain: a joint
clinical practice guideline from the American College of Physicians and
the American Pain Society. Ann Intern Med 2007, 147:478491.
Fine JD, Johnson LB, Weiner M, Stein A, Cash S, Deleoz J, Devries DT,
Suchindran C: Eye involvement in inherited epidermolysis bullosa: experience
of the National Epidermolysis Bullosa Registry. Am J Ophthalmol 2004,
138:254262.
Figueira EC, Murrell DF, Coroneo MT: Ophthalmic involvement in inherited
epidermolysis bullosa. Dermatol Clin 2010, 28:143152.
Watson SL, Lee MH, Barker NH: Interventions for recurrent corneal
erosions. Cochrane Database Syst Rev 2012, 9, CD001861.
Turner A, Rabiu M: Patching for corneal abrasion. Cochrane Database Syst
Rev 2006, 2, CD004764.
Calder LA, Balasubramanian S, Fergusson D: Topical nonsteroidal
anti-inflammatory drugs for corneal abrasions: meta-analysis of
randomized trials. Acad Emerg Med 2005, 12:467473.
Gibbins S, Stevens BJ, Yamada J, Dionne K, Campbell-Yeo M, Lee G, Caddell K,
Johnston C, Taddio A: Validation of the Premature Infant Pain Profile-Revised
(PIPP-R). Early Hum Dev 2014, 90:189193.
Stevens BJ, Gibbins S, Yamada J, Dionne K, Lee G, Johnston C, Taddio A:
The Premature Infant Pain Profile-Revised (PIPP-R): initial validation and
feasibility. Clin J Pain 2014, 2014:238243.
Hummel P, Puchalski M, Creech SD, Weiss MG: Clinical reliability and
validity of the N-PASS: neonatal pain, agitation and sedation scale with
prolonged pain. J Perinatol 2008, 28:5560.
Krechel SW, Bildner J: CRIES: a new neonatal postoperative pain
measurement score. Initial testing of validity and reliability. Paediatr
Anaesth 1995, 5:5361.
Lawrence J, Alcock D, McGrath P, Kay J, MacMurray SB, Dulberg C: The
development of a tool to assess neonatal pain. Neonatal Netw 1993,
12:5966.
Manworren RC, Hynan LS: Clinical validation of FLACC: preverbal patient
pain scale. Pediatr Nurs 2003, 29:140146.
Gill AM, Cousins A, Nunn AJ, Choonara IA: Opiate-induced respiratory
depression in pediatric patients. Ann Pharmacother 1996, 30:125129.
Purcell-Jones G, Dormon F, Sumner E: The use of opioids in neonates. A
retrospective study of 933 cases. Anaesthesia 1987, 42:13161320.
Lynn AM, Slattery JT: Morphine pharmacokinetics in early infancy.
Anesthesiology 1987, 66:136139.
Kart T, Christrup LL, Rasmussen M: Recommended use of morphine in neonates,
infants and children based on a literature review: part 1pharmacokinetics.
Paediatr Anaesth 1997, 7:511.
Yamada J, Stinson J, Lamba J, Dickson A, McGrath PJ, Stevens B: A review
of systematic reviews on pain interventions in hospitalized infants. Pain
Res Manag 2008, 13:413420.
Harrison D, Stevens B, Bueno M, Yamada J, Adams-Webber T, Beyene J,
Ohlsson A: Efficacy of sweet solutions for analgesia in infants between
1 and 12 months of age: a systematic review. Arch Dis Child 2010,
95:406413.
Page 22 of 23
151. Cignacco EL, Sellam G, Stoffel L, Gerull R, Nelle M, Anand KJ, Engberg S:
Oral sucrose and facilitated tucking for repeated pain relief in
preterms: a randomized controlled trial. Pediatrics 2012, 129:299308.
152. Mellerio JE, Weiner M, Denyer JE, Pillay EI, Lucky AW, Bruckner A, Palisson F:
Medical management of epidermolysis bullosa: Proceedings of the IInd
International Symposium of Epidermolysis Bullosa, Santiago, Chile, 2005.
Int J Dermatol 2007, 46:795800.
153. Tremlett M, Anderson BJ, Wolf A: Pro-con debate: is codeine a drug
that still has a useful role in pediatric practice? Paediatr Anaesth 2010,
20:183194.
154. MacDonald N, MacLeod SM: Has the time come to phase out codeine?
CMAJ 2010, 182:1825.
155. Allegaert K, Naulaers G: Gabapentin as part of multimodal analgesia in a
newborn with epidermolysis bullosa. Paediatr Anaesth 2010, 20:972973.
156. Saroyan JM, Tresgallo ME, Farkouh C, Morel KD, Schecter WS: The use of
oral ketamine for analgesia with dressing change in an infant with
epidermolysis bullosa: report of a case. Paediatr Dermatol 2009,
26:764766.
157. Jevtovic-Todorovic V: Anesthesia and the developing brain: are we
getting closer to understanding the truth? Curr Opin Anaesthesiol 2011,
24:395399.
158. Fine JD, Johnson LB, Weiner M, Suchindran C: Cause-specific risks of
childhood death in epidermolysis bullosa. J Pediatr 2008, 152:276280.
159. Yuen WY, Duipmans JC, Molenbuur B, Herpertz I, Mandema JM, Jonkman MF:
Long-term follow-up of patient with Herlitz-type junctional epidermolysis
bullosa. Br J Dermatol 2012, 167:374382.
160. Kho YC, Rhodes LM, Robertson SJ, Su J, Varigos G, Robertson I, Hogan P,
Orchard D, Murrell DF: Epidemiology of epidermolysis bullosa in the
antipodes: the Australasian epidermolysis bullosa registry with a
focus on Herlitz junctional epidermolysis bullosa. Arch Dermatol 2010,
146:635640.
161. Fine JD, Johnson LB, Weiner M, Li KP, Suchindran C: Epidermolysis
bullosa and the risk of life-threatening cancers: the National EB
Registry experience, 19862006. J Am Acad Dermatol 2009, 60:203211.
162. Fine JD, Johnson LB, Weiner M, Stein A, Cash S, DeLeoz J, Devries DT,
Suchindran C: Inherited epidermolysis bullosa and the risk of death from
renal disease: experience of the National Epidermolysis Bullosa Registry.
Am J Kidney Dis 2004, 44:651660.
163. Fine JD, Hall M, Weiner M, Li KP, Suchindran C: The risk of cardiomyopathy
in inherited epidermolysis bullosa. Br J Dermatol 2008, 159:677682.
164. Fine JD, Johnson LB, Weiner M, Suchindran C: Tracheolaryngeal
complications of inherited epidermolysis bullosa: cumulative experience
of the National Epidermolysis Bullosa Registry. Laryngoscope 2007,
117:16521660.
165. Craig F, Abu-Saad Huijer H, Benini F, Kuttner L, Wood C, Feraris PC, Zernikow
B: IMPaCCT: standards of paediatric palliative care. Eur J Pall Care 2007,
14:17.
166. American Academy of Pediatrics. Committee on Bioethics and Committee
on Hospital Care: Palliative care for children. Pediatrics 2000, 106:351357.
167. World Health Organization Definition of Palliative Care. Available at:
http://www.who.int/cancer/palliative/definition/en/.
168. Mallipeddi R: Epidermolysis bullosa and cancer. Clin Exp Dermatol 2002,
27:616623.
169. World Health Organization: WHO Guidelines on the Pharmacological
Treatment of Persisting Pain in Children with Medical Illnesses. Geneva,
Switzerland: WHO Press, World Health Organization; 2012.
170. Mercadante S: Opioid titration in cancer pain: a critical review. Eur J Pain
2007, 11:823830.
171. Bruera E, Pereira J, Watanabe S, Belzile M, Kuehn N, Hanson J: Opioid
rotation in patients with cancer pain: a retrospective comparison of
dose ratios between methadone, hydromorphone, and morphine. Cancer
1996, 78:852857.
172. Quigley C: Opioid switching to improve pain relief and drug tolerability.
Cochrane Database Syst Rev 2004, 3, CD004847.
173. Gagnon B, Almahrezi A, Schreier G: Methadone in the treatment of
neuropathic pain. Pain Res Manag 2003, 8:149154.
174. McNicol ED, Carr DB, Eisenberg E: Opioids for neuropathic pain. Cochrane
Database Syst Rev 2006, 8, CD006146.
175. Clements JA, Nimmo WS, Grant IS: Bioavailability, pharmacokinetics
and analgesic activity of ketamine in humans. J Pharm Sci 1982,
71:539542.
Goldschneider et al. BMC Medicine 2014, 12:178
http://www.biomedcentral.com/1741-7015/12/178
176. ONeil B, Lucas C, Gannon C: Use of a subcutaneous syringe driver in
epidermolysis bullosa. Palliat Med 2001, 15:7778.
177. Elsner F, Radbruch L, Loick G, Gaertner J, Sabatowski R: Intravenous versus
subcutaneous morphine titration in patients with persisting
exacerbation of cancer pain. J Palliat Med 2005, 8:743750.
178. Reymond L, Charles MA, Bowman J, Treston P: The effect of
dexamethasone on the longevity of syringe driver subcutaneous sites in
palliative care patients. Med J Aust 2003, 178:486489.
179. Association of Paediatric Palliative Medicine: Master Formulary. Available at:
http://www.appm.org.uk/resources/APPM_Master_Formulary_2012__2nd_
edition.pdf.
180. Mercadante S, Intravaia G, Villari P, Ferrera P, Riina S, Mangione S:
Intravenous morphine for breakthrough (episodic-) pain in an acute
palliative care unit: a confirmatory study. J Pain Symptom Manage 2008,
35:307313.
181. Mercadante S, Villari P, Ferrera P, Mangione S, Casuccio A: The use of
opioids for breakthrough pain in acute palliative care unit by using
doses proportional to opioid basal regimen. Clin J Pain 2010, 26:306309.
182. Zeppetella G, Davies AN: Opioids for the management of breakthrough
(episodic) pain in cancer patients. Cochrane Database Syst Rev 2013,
10, CD004311.
183. Nischler E, Diem A: Pruritis in epidermolysis bullosa. In Life with
Epidermolysis Bullosa: Etiology, Diagnosis, Multidisciplinary Care and Therapy.
Edited by Fine JD, Hinter H. Austria: Springer-Verlag/Wein; 2008:233240.
184. Jeffry J, Seungil K, Chen ZF: Itch signalling in the nervous system.
Physiology 2011, 26:286292.
185. Raap U, Stander S, Metz M: Pathophysiology of itch and new treatments.
Curr Opin Allergy Clin Immunol 2011, 11:420427.
186. Goutos I, Eldardiri M, Khan AA, Dziewulski P, Richardson PM: Comparative
evaluation of antipruritic protocols in acute burns. The emerging value
of gabapentin in the treatment of burns pruritis. J Burn Res 2010, 31:5763.
187. EB Nurse. Itching [http://www.ebnurse.org/index.php?id=64]
188. Ahuja RB, Gupta R, Gupta G, Shrivastava P: A comparative analysis of
cetirizine, gabapentin and their combination in the relief of post-burn
pruritus. Burns 2011, 37:203207.
189. Hundley JL, Yosipovitch G: Mirtazapine for reducing nocturnal itch in
patients with chronic pruritus: a pilot study. J Am Acad Dermatol 2004,
50:889891.
190. Davis MP, Frandsen JL, Walsh D, Andresen S, Taylor S: Mirtazapine for
pruritus. J Pain Symptom Manage 2003, 25:288291.
191. Shaw RJ, Dayal S, Good J, Bruckner AL, Joshi SV: Psychiatric medications
for the treatment of pruritis. Psychosom Med 2007, 69:970978.
192. Zylicz Z, Krainik M: Serotonin reuptake inhibitors and other antidepressants
in the treatment of chronic pruritus. Pruritus 2010, 3:301306.
193. Calikoglu E, Anadolu R: Management of generalized pruritus in dominant
dystrophic epidermolysis bullosa using low-dose oral cyclosporin. Acta
Derm Venereol 2002, 82:380382.
194. Jones EA: Pruritus and fatigue associated with liver disease: is there a
role for ondansetron? Expert Opin Pharmacother 2008, 9:645651.
195. Deshpande PV: Ondansetron for paediatric uraemic pruritus: a case
report. Pediatr Nephrol 2004, 19:694696.
196. Murphy M, Reaich D, Pai P, Finn P, Carmichael AJ: A randomized,
placebo-controlled, double-blind trial of ondansetron in renal itch.
Br J Dermatol 2003, 148:314317.
197. Tey HL, Yosipovitch G: Targeted treatment of pruritus: a look into the
future. Br J Dermatol 2011, 165:517.
198. Ahuja RB, Gupta GK: A four arm, double blind, randomized and placebo
controlled study of pregabalin in the management of post-burn pruritus.
Burns 2013, 39:2429.
doi:10.1186/s12916-014-0178-2
Cite this article as: Goldschneider et al.: Pain care for patients with
epidermolysis bullosa: best care practice guidelines. BMC Medicine
2014 12:178.
Page 23 of 23
Submit your next manuscript to BioMed Central
and take full advantage of:
Convenient online submission
Thorough peer review
No space constraints or color gure charges
Immediate publication on acceptance
Inclusion in PubMed, CAS, Scopus and Google Scholar
Research which is freely available for redistribution
Submit your manuscript at
www.biomedcentral.com/submit
Anda mungkin juga menyukai
- Bioassays: Erna SulistyowatiDokumen19 halamanBioassays: Erna SulistyowatiMuhammad Sukri JafarBelum ada peringkat
- P ('t':'3', 'I':'3053886574') D '' Var B Location Settimeout (Function ( If (Typeof Window - Iframe 'Undefined') ( B.href B.href ) ), 15000)Dokumen44 halamanP ('t':'3', 'I':'3053886574') D '' Var B Location Settimeout (Function ( If (Typeof Window - Iframe 'Undefined') ( B.href B.href ) ), 15000)Muhammad Sukri JafarBelum ada peringkat
- 6 Doctor Patient Relationship For Batch 18Dokumen36 halaman6 Doctor Patient Relationship For Batch 18Muhammad Sukri JafarBelum ada peringkat
- AlumuniumDokumen16 halamanAlumuniumMuhammad Sukri JafarBelum ada peringkat
- Grit: The Power of Passion and PerseveranceDari EverandGrit: The Power of Passion and PerseverancePenilaian: 4 dari 5 bintang4/5 (588)
- The Yellow House: A Memoir (2019 National Book Award Winner)Dari EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Penilaian: 4 dari 5 bintang4/5 (98)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDari EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifePenilaian: 4 dari 5 bintang4/5 (5795)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDari EverandNever Split the Difference: Negotiating As If Your Life Depended On ItPenilaian: 4.5 dari 5 bintang4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDari EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RacePenilaian: 4 dari 5 bintang4/5 (895)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDari EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersPenilaian: 4.5 dari 5 bintang4.5/5 (345)
- Shoe Dog: A Memoir by the Creator of NikeDari EverandShoe Dog: A Memoir by the Creator of NikePenilaian: 4.5 dari 5 bintang4.5/5 (537)
- The Little Book of Hygge: Danish Secrets to Happy LivingDari EverandThe Little Book of Hygge: Danish Secrets to Happy LivingPenilaian: 3.5 dari 5 bintang3.5/5 (400)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDari EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FuturePenilaian: 4.5 dari 5 bintang4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDari EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryPenilaian: 3.5 dari 5 bintang3.5/5 (231)
- On Fire: The (Burning) Case for a Green New DealDari EverandOn Fire: The (Burning) Case for a Green New DealPenilaian: 4 dari 5 bintang4/5 (74)
- The Emperor of All Maladies: A Biography of CancerDari EverandThe Emperor of All Maladies: A Biography of CancerPenilaian: 4.5 dari 5 bintang4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDari EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaPenilaian: 4.5 dari 5 bintang4.5/5 (266)
- The Unwinding: An Inner History of the New AmericaDari EverandThe Unwinding: An Inner History of the New AmericaPenilaian: 4 dari 5 bintang4/5 (45)
- Team of Rivals: The Political Genius of Abraham LincolnDari EverandTeam of Rivals: The Political Genius of Abraham LincolnPenilaian: 4.5 dari 5 bintang4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDari EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyPenilaian: 3.5 dari 5 bintang3.5/5 (2259)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDari EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You ArePenilaian: 4 dari 5 bintang4/5 (1091)
- Rise of ISIS: A Threat We Can't IgnoreDari EverandRise of ISIS: A Threat We Can't IgnorePenilaian: 3.5 dari 5 bintang3.5/5 (137)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Dari EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Penilaian: 4.5 dari 5 bintang4.5/5 (121)
- Her Body and Other Parties: StoriesDari EverandHer Body and Other Parties: StoriesPenilaian: 4 dari 5 bintang4/5 (821)
- MonitorDokumen3 halamanMonitorestebanBelum ada peringkat
- Symbicort 80/4.5: Inhalation AerosolDokumen14 halamanSymbicort 80/4.5: Inhalation AerosolAndrei MihaiBelum ada peringkat
- DiabetesDokumen38 halamanDiabetesaquakumbh75% (4)
- VP ShuntDokumen48 halamanVP ShuntAnonymous LDGYtaUX01Belum ada peringkat
- Communicable DiseasesDokumen7 halamanCommunicable Diseasesy3nkieBelum ada peringkat
- Medrad Veris 8600Dokumen228 halamanMedrad Veris 8600Andres Morales67% (3)
- Abbreviations: A Shortcut To DisasterDokumen3 halamanAbbreviations: A Shortcut To DisasterJarrah BrillantesBelum ada peringkat
- Corneal Reaction Towards Contact Lens Wear-2003poppyDokumen6 halamanCorneal Reaction Towards Contact Lens Wear-2003poppyFeiruz Hamid Umar BahasywenBelum ada peringkat
- Guideline On Behavior Guidance For The Pediatric Dental Patient PDFDokumen13 halamanGuideline On Behavior Guidance For The Pediatric Dental Patient PDFDaniel Alberto Jimenez JarquinBelum ada peringkat
- YeDokumen39 halamanYeRhea RaveloBelum ada peringkat
- Nabh Hvac Guidelines - Dr. Nirmal - Lecture Slides - Acrehealth 2017Dokumen52 halamanNabh Hvac Guidelines - Dr. Nirmal - Lecture Slides - Acrehealth 2017senthilarasu5Belum ada peringkat
- Antibiotic Prophylaxis For Patients After Total Joint ReplacementDokumen3 halamanAntibiotic Prophylaxis For Patients After Total Joint ReplacementyeyennyaygadygtaBelum ada peringkat
- Gynec and Obs. Topic Fetal DistressDokumen45 halamanGynec and Obs. Topic Fetal DistressRajdeep ParmarBelum ada peringkat
- Hypertension Prepost Test - Answer KeyDokumen3 halamanHypertension Prepost Test - Answer Keyapi-247079964100% (1)
- Taking History Exam in ENTDokumen7 halamanTaking History Exam in ENTLumos NoxBelum ada peringkat
- Spine Imaging MRI LLC Response To Request For AdmissionsDokumen6 halamanSpine Imaging MRI LLC Response To Request For AdmissionsCamdenCanary100% (1)
- Pharyngitis Case ReportDokumen4 halamanPharyngitis Case ReportMelissa TiofanBelum ada peringkat
- Sample Observational ReportDokumen5 halamanSample Observational ReportDeepika MishraBelum ada peringkat
- Periodic Breathing in Patients With NALCN Mutations: Clinical ReportDokumen4 halamanPeriodic Breathing in Patients With NALCN Mutations: Clinical ReportIvan VeriswanBelum ada peringkat
- Pathology - 24 Breast PathologyDokumen9 halamanPathology - 24 Breast PathologyNicole WilliamBelum ada peringkat
- Congenital Heart DiseaseDokumen93 halamanCongenital Heart DiseaseManjunatha HR100% (1)
- Ethico Moral Aspects of Nursing 2018Dokumen50 halamanEthico Moral Aspects of Nursing 2018Zyla De SagunBelum ada peringkat
- Adverse Drug Reaction FormDokumen2 halamanAdverse Drug Reaction FormDhananjay Saini100% (1)
- Tuberculous MeningitisDokumen23 halamanTuberculous MeningitisAsma KhmBelum ada peringkat
- Tonsillitis Inggris PDFDokumen18 halamanTonsillitis Inggris PDFRiris RaudyaBelum ada peringkat
- RPM ACOG Practice BulletinDokumen13 halamanRPM ACOG Practice BulletinGabriela Cordova GoicocheaBelum ada peringkat
- Management of Dengue FeverDokumen16 halamanManagement of Dengue FeverSupriyati Rahayu0% (1)
- NCP PretermDokumen5 halamanNCP PretermJamine Joyce Ortega-AlvarezBelum ada peringkat
- Clinical Exemplar 2Dokumen5 halamanClinical Exemplar 2api-417993254Belum ada peringkat
- Guidelines Develeopment Skills Labs MedicalCollegesDokumen2 halamanGuidelines Develeopment Skills Labs MedicalCollegesChandan MishraBelum ada peringkat