80 118 2 PB PDF
Diunggah oleh
JacobMsangDeskripsi Asli:
Judul Asli
Hak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
80 118 2 PB PDF
Diunggah oleh
JacobMsangHak Cipta:
Format Tersedia
RECONSTRUCTIVE
The Extended Lateral Forehead Flap: Today as Was 50years Ago
Laureen Supit, Gentur Sudjatmiko
Jakarta, Indonesia.
Background: In the era of surgical advances where institutional pride and status resonates with their
progress in the minimal invasives, latest technologies, stem cells, and supermicrosurgeries; some things in
plastic surgery never change. The extended lateral forehad flap (ELFF) was first introduced by Ian
McGregor in 1963 to reconstruct an intraoral defect, he called it the temporal flap. Gillies and Millard each
modified and utilized the flap for patching various facial and intraoral defects and published their
experience a year later. Until today in 2012, the ELFF is still largely useful for the reconstruction of wide
defects post neoplasms ablation in the face or oral region, which would otherwise require distant flaps or
free flaps.
Patients and Methods: Three cases of oral and perioral carcinoma were resected and reconstructed using
the ELFF to cover for: a full-thickness cheek defect including the lip commisure, an inner oral lining, and a
hemipalatal defect.
Results: In all, the flaps were tunneled subcutaneously, and donor area grafted by full-thickness skin. All
flaps survived and functional outcomes are attained in all patients, with acceptable aesthetic results.
Summary: A flap once introduced 49 years ago, is today as consistent and applicable in plastic surgery.
This article is an appraisal to the ELFF, and a reminder to the general plastic surgeons, of the simple yet
versatile role of ELFF in the reconstruction of facial and intraoral defects.
Keywords : Extended lateral forehead flap, temporal flap, intraoral, reconstruction
Pendahuluan: DI era modern dimana sebagian besar institusi berlomba mengembangkan teknologi,
minimal invasif, sel punca, dan supermicrosurgery; beberapa hal dalam bedah plastik tidak berubah.
Extended lateral forehad flap (ELFF) diperkenalkan pertama kali oleh Ian McGregor tahun 1963 untuk
rekonstruksi defek intraoral, dan disebut sebagai temporal flap. Gillies dan Millard memodifikasi
penggunaan flap tersebut untuk berbagai defek wajah dan intraoral. Hingga sekarang ELFF masih sering
digunakan untuk menutup defek luas pasca ablasi tumor daerah wajah atau oral.
Pasien dan Metodologi: Tiga kasus karsinoma pada daerah oral dan perioral direseksi dan
direkonstruksi dengan ELFF: defek full-thickness pada pipi termasuk komisura bibir, lining intra oral, dan
defek hemipalatal.
Hasil : Pada semua kasus dilakukan tunneling flap secara subkutan dan area donor ditutup dengan FTSG.
Semua flap vital dan memiliki hasil secara fungsional dan estetik yang cukup baik.
Ringkasan: Pada semua kasus dilakukan tunneling flap secara subkutan dan area donor ditutup dengan
FTSG. Semua flap vital dan memiliki hasil secara fungsional dan estetik yang cukup baik.
Kesimpulan: Suatu flap yang pertama diperkenalkan 50 tahun lalu, hingga sekarang tetap dapat digunakan
dalam bedah plastik. Artikel ini bertujuan untuk melakukan penilaian ulang kegunaan ELFF, dan sebagai
pengingat bagi ahli bedah plastik secara umum mengenai kegunaan ELFF yang banyak untuk menutup
defek wajah dan intra oral.
Kata Kunci : Extended lateral forehead flap, temporal flap, intraoral, reconstruction
he advent of knowledge and skills in plastic
surgery have introduced what is viewed as
the more-exciting novel procedures such as
micro- and supermicro-surgeries, minimal
invasives, and stem cells. They are certainly
From The Division Of Plastic Reconstructive and
Aesthetic Surgery, University of Indonesia, Cipto
Mangunkusumo Hospital, Jakarta, Indonesia
Presented in 16th IAPS Scientific Meetings In
Sibolangit, North Sumatra, Indonesia.
374
useful and beneficial in some cases. In the field
of reconstructive surgery however, the
applicability of minimal invasive procedures
and stem cells are very limited. And although
microsurgery offers many benefits, such is not
Disclosure: The authors have no financial
interest to declare in relation to the content of this
article.
www.JPRJournal.com
Volume 1 - Number 4 - The Extended Lateral Forehead Flap
always the case, some older and simpler
reconstructive options are still dependable
today. Not because we do not evolve or
advance, but because the basic principles of
plastic surgery stays. It is luring how latest
technologies and techniques help upgrade
institutional pride, but be sure that a
reconstructive decision is not merely based on
trying to catch up with the common hype
among other surgical specialties in which some
has progressed to include even the robotic
technologies.
Reconstruction of postablation defects
of tumor on the facial and intraoral regions is
challenging as the demand of aesthetic and
functional outcomes is high. Several options
including skin grafts, regional flaps, distant
flaps, and free tissue transfers can be
employed. This article discusses the use of a
local flap, the extended lateral forehad
myocutaneous flap (ELFF). It is a versatile
method to reconstruct defect on the face and
mouth. The use of paramedian forehad flap
particularly applicable for the construction of
defected nose is not discussed here and is a
separate subject of its own. The ELFF was first
introduced as temporal flap by Ian McGregor
in 1963 to patch for an intraoral defect.1 Within
the next year, D. Ralph Millard and Sir Harold
Gillies, two historical and influential plastic
surgeons, each modified and published the use
of similar flap for patching various facial and
intraoral defects.2 The increasingly popular
option for head and neck reconstruction by
microsurgery commonly utilizes the radial
forearm or anterolateral thigh free flaps. Their
drawbacks include poor skin color match,
donor site morbidity, excessive tissue bulk, the
need for a specially trained microsurgeon, and
requirement of specific equipments.
The forehead is supplied by four
vascular networks or angiosomes: the left and
right superficial temporal arteries, and the left
and right opthalmic arteries each consisting of
the supraorbital and supratrochlear arteries
(Figure 1).3 The extended lateral forehead flap
is an axial myocutaneous flap supplied by
these vessels. At first, surgeons were worried
of raising forehead flaps beyond the midline,
fearing that by severing two or more successive
t e r r i t o r i e s w o u l d c a u s e a d i s t a l fl a p
compromise. However, a vascular study using
micropaque injections on the superficial
temporal artery in cadavers shows that rich
anastomotic plexus exists between the major
forehead angiosomes linked by the smaller
caliber choke vessels.4,5 This allows the
elevation of an extended forehad muscle and
skin, without the need for flap delay or
prefabrication, with no risk of flap necrosis.
Elevating the whole unit of forehad such as in
ELFF instead of partially will also give a better
conceal of resultant donor defect, as the design
follows the forehead aesthetic units (Figure 2).6
The flap is raised based on either the
right or left superficial temporal artery
transversely across the forehad. Upon
elevation, the ELFF design should encompass
the whole forehad area just below the hairline
up to the upper edge of eyebrows, from one
pedicle reaching the full contralateral forehead
(Figure 3). This is done in order to leave a
donor defect which suits the forehead
aesthethic unit. The flap is elevated just above
the pericranium layer, then shaped as
necessary into the dimensions needed to cover
the primary defect. If any hairbearing part of
the flap will be transferred intraorally, the area
should be epilated otherwise the hair will
continue to grow in the mouth.
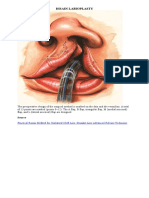
For the tunnel, no extra incision is made
other than the flap design. Flap is tunneled on
the loose connective tissue plane beneath the
base of pedicle. The remaining tunnel is bluntly
dissected in the general direction of the upper
buccal sulcus to reduce the chance of injury to
the facial nerve, until it reaches the defect.
There is generally no risk of strangulation if the
tunnel is made with adequate width. Project
the flap through the tunnel onto the defect.
Area of the flap which will lie within the tunnel
must be marked. Flap is then returned onto a
flat surface and buried area deepithelialized,
before it is finally insetted onto the defect
(Figure 4).
It is best to cover the donor defect by
full-thickness skin graft obtained from the
lower abdominal crease, harvested as a single
one-piece skin to cover the whole defect
surface. Fixation sutures may be done
375
Jurnal Plastik Rekonstruksi - July 2012
circumferentially
aroundasthe
graftand
as immobile
running
pericranial base serves
a rigid
graft bed. To maintain pressure, tie-over
dressing may be applied. Allow 5 days before
the first dressing change.
Similar to non-extended or paramedian
forehead flap, the base of the pedicle is to be
divided three weeks after flap elevation when
engraftment already occurred. The inner
surface of the folded flap base was not
deepithelialized hence will not attach onto the
sutures.
Tacking
suture
is not
required
the
surrounding
tissue
in the
tunnel.
This as
folded
part of pedicle on the temporal area is incised,
skin excess excised, and sutured primarily
(Figure 5). Note the blurry picture of Figure 5,
left: this picture was obtained using a camera
wrapped in a sterile transparent plastic bag.
Compare picture quality to the standard
picture-taking on its right with the same
camera.
Figure( 1.(Vascular+ network+of+ the+ forehad:+(1+ and+ 4)+
The+right+ and+ leV+ supercial+temporal+ arteries,+(2+and+
3)+the+right+and+leV+opthalmic+arteries.
Figure( 2.( The+ facial+ aesthe2c+ units.The+ forehad+ is+
made+of+ one+single+unit,+encompassing+an+area+which+
inadvertently+ suits+ + the+ design+ of+ extended+ lateral+
forehad+ap.
Figure(3.(Red+lines+indicate+the+design+of+the+extended+
forhead+ ap.+ Upper+ border:+ below+ hairline.+ Lower+
border:+above+eyebrows.
Figure( 4.( Illustra2on+ of+ tunneled+ leV+ cheek+area,+ and+
the+ deepithelialized+ part+ of+ forehad+ ap+ to+ lie+ within+
the+tunnel
376
Figure(5.(Three+weeks+aVer+ ap+eleva2on,+base+of+pedicle+divided,+skin+ excess+excised+ and+ sutured+primarily.+The+
new+skin+over+ the+forehead+shows+excellent+take+ of+fullTthickness+graV,+which+typically+happens+to+ the+forehead+
Volume 1 - Number 4 - The Extended Lateral Forehead Flap
Figure(5.(Three+ weeks+aVer+ ap+eleva2on,+base+ of+pedicle+ divided,+skin+excess+excised+ and+sutured+ primarily.+The+
new+skin+over+ the+forehead+shows+excellent+ take+ of+fullTthickness+graV,+which+ typically+happens+ to+the+forehead+
donor+area.
PATIENT AND METHODS
Case 3
Case 1
Female aged 46 years suffered from
mucoepidermoid cancer of the right maxilla
which infiltrated the right palate (Figure 8a).
Hemimaxillectomy was performed, facial
muscles and skin were spared (Figure 8b). A
right pedicled ELFF was used to patch the
palatal defect (Figure 8c), the remaining length
was deepithelialized and used to pack the
maxillary sinus. A coastal bone graft was also
used as a framework to replace the inferior
orbital bone. Functional and aesthetic results
were acceptable (Figure 8d).
55-year-old man with squamous cell
carcinoma on the left lip commisure (Figure
6a). Lesion was widely excised, leaving a full
thickness anterior cheek defect including half
of the left upper and lower lips (Figure 6b). An
ELFF raised with a left temporal pedicle, was
tunneled through the cheek, deepithelialized
on the proximal part to lie within the tunnel
(Figure 6c), folded on the distal side to form
both the inner and outer lining of cheek, as
well as shaped into a new lip commisure
(Figure 6d).
Case 2
50-year-old male had a left buccal
squamous cell carcinoma and underwent a
wide excision which left an intraoral defect of
the left cheek limited to the mucosa. Defect
was reconstructed using a left pedicled ELFF
tunneled through its base and passed along the
cheek to form the buccal inner lining (Figure 7,
left). Flap and grafted donor area healed
satisfactorily (Figure 7, middle). The missing
intraoral mucosa was restored, and ELFF
adapted well to the surrounding tissue (Figure
7, right).
DISCUSSION
The extended forehead flap, a flap once
introduced 49 years ago, is today as consistent
and applicable in plastic surgery as it was back
then. Many years prior to McGregors 1963
publication on the ELFF, Gillies and Millard
stated in their book The Principles and Arts of
Plastic Surgery, that the tint of forehead skin
so exactly matches that of the face and nose
that it must be first choice. With some plastic
juggling, the forehead defect can be
c a m o u fl a g e d e f f e c t i v e l y . 7 T h i s q u o t e
brilliantly summarizes our points of
discussion.
377
Jurnal Plastik Rekonstruksi - July 2012
(a)
(b)
(c)
(d)
Figure( 6.( Case+ 1,+ (a)+ squamous+ cell+ carcinoma+ of+ the+ leV+ commisure,+ (b)+ excised,+ (c)+ reconstructed+ using+ a+
proximally+deepithelialized+and+distally+folded+ELF+ap.+(d)+Final+defect+and+donor+appearance+1+aVer+second+ stage+
surgery.
(a)
(b)
(c)
(d)
Figure(8.+Case+3,+(a)+mucoepidermoid+cancer+inltra2ng+the+right+ palate,+(b)+the+right+maxilla+excised,+(c)+ELFF+used+
to+ pack+the+right+maxillary+defect+ and+ to+ form+the+right+palate,+(d)+forehead+ donor+ 3+ weeks+ aVer+ graVing+during+
pedicle+base+division.
Figure( 7.+ Case+ 2:+ (leV)+ intraoral+ squamousTcell+ carcinoma+ excised+ and+ the+ inner+ lining+ reconstructed+ using+ a+
tunneled+ELFF,+(middle+and+right)+end+results+of+donor+and+ap.+
378
Volume 1 - Number 4 - The Extended Lateral Forehead Flap
As illustrated in the three cases above
(Summarized in Table 1) and some case reports
from overseas,8-10 ELFF has been shown to
adequately provide tissue cover for various
single to multi structural tissue loss of the face
and oral region, which would otherwise
require distant flaps or free flaps. This
relatively simple local flap is specifically useful
in cases of post tumor ablation where
immediate straightforward reconstruction is
warranted, and the tissue must survive
through a series of adjuvant therapies to follow
shortly after. Microsurgery and distant flaps
are alternative options. The advantages and
disadvantages of microsurgery over ELFF are
mentinoned in Table 2. Distant flaps are
technically less complicated than
microsurgery, but still require more planning
and more diversed in anatomy than local flap.
Therefore it is wise to adapt the Occams razor
philosophy: Other things being equal, a
simpler choice is better than a more complex
one.11
All ELFF flaps in the case examples
survived with no partial compromise.
Structures to be reconstructed are adequately
covered with satisfactory restoration of
function. All donor area had a 100 percent graft
take with acceptable aesthetic results. Patients
lost sensation of the forehead, and unable to
perform the expression of raising eyebrows,
but none expressed concerns over these
matters. No facial palsy nor salivary fistula
developed, and skin flaps within the mouth
adapted well into the adjacent mucosa.
Donor site appearance is easily
camouflaged by hair style, hood, or scarf.
Because the flap design follows the forehead
aesthetic unit, even at bare sight without cover,
the face does not seem greatly deformed except
a slight skin step-off above the eyebrows. An
alternative surgical planning is to apply a
tissue expander prior to flap elevation, which
will minimize donor morbidity and leave only
a single-line fine scar near the hairline.12
Table(1.(Summary+of+case+series
Reconstructed Defect
Flap
Donor
Proximally deepithelialized,
tunneled, folded on the distal
FTSG, 100% take
to form inner and outer oral
lining
Complication
Case 1
Full-thickness cheek, and lip
commisure
Case 2
Inner cheek lining
Proximally deepithelialized,
tunneled, placed intraoral
FTSG, 100% take
None
Case 3
Right palate soft tissue
padding of maxilla
Proximally deepithelialized,
tunneled, placed intraoral
FTSG, 100% take
None
None
Table(2.(Advantages+and+disadvantages+of+ELFF
Advantages of ELFF (compared to distant flap or free flap)
1. True replace Like-with Like
2. Less bulky than free flap
3. Smaller risk of vascular compromise
4. Quicker to perform
5. No microsurgery training, equipments, or facility required
6. Reliable in postradiation/palliative reconstructive cases
Disadvantages of ELFF
1. Obvious donor site location
2. Loss of forehead sensation and eyebrow-raise expression
3. Requires a two
379
Jurnal Plastik Rekonstruksi - July 2012
SUMMARY
This article reappraises the extended
lateral forehead flap. It is a reminder to the
general plastic surgeons of a simple yet
versatile role of ELFF for the reconstruction of
facial and intraoral defects, especially in cases
of post tumor ablation where microsurgery,
tissue expansion, and distant flaps seem like a
heftier choice.
Gentur Sudjatmiko, MD
Division of Plastic Surgery
Cipto Mangunkusumo General Hospital, Jakarta.
dr_gentur@yahoo.co.id
REFERENCES
1. McGregor IA. The Temporal Flap in Intra-Oral Cancer:
Its Use in Repairing the Post-Excisional Defect. Br J
Plast Surg 1963;16:318-35.
2. Millard DR, Jr. Forehead Flap in Immediate Repair of
Head, Face and Jaw. Am J Surg 1964;108:508-13.
3. Houseman ND, Taylor GI, Pan WR. The angiosomes of
the head and neck: anatomic study and clinical
applications. Plast Reconstr Surg 2000;105:2287-313.
380
4. Mangold U, Lierse W, Pfeifer G. [The arteries of the
forehead as the basis of nasal reconstruction with
forehead flaps]. Acta Anat (Basel) 1980;107:18-25.
5. Wilson JSP, Breach NM. Forehad skin flaps. In: Strauch
B, Vasconez LO, Hall-Findlay EJ, Lee BT, eds. Grabb's
encyclopedia of flaps: Head and neck. Philadelphia,
USA: Lippincott Williams & Wilkins, 2009:294-300.
6. Baker SR. Flap classification and design. In: Baker SR,
ed. Baker local flaps in facial reconstruction.
Philladelphia, PA: Mosby, 2007:75.
7. Gillies H, Millard DR, Jr. The principles and art of
plastic surgery. Boston: Little, Brown, 1957.
8. Sadhotra LP, Singh M, Raje R. Reconstruction of a
complete palatal defect with a forehead flap: A case
report. Indian J Plastic Surg 2003;36:120-2.
9. Noorman van der Dussen MF. Utilization of the
pedicle of the temporal-forehead-flap to close defects
in the maxilla after tumour surgery. J Maxillofac Surg
1983;11:204-6.
10.Matulic Z, Barlovic M, Mikolji V, Virag M. Tongue
reconstruction by means of the sternocleidomastoid
muscle and a forhead flap. Br J Plast Surg
1978;31:147-51.
11.Bertrand R. History of Western philosophy: Allen &
Unwin, 2000:462-3.
12.Fan J. A new technique of scarless expanded forehead
flap for reconstructive surgery. Plast Reconstr Surg
2000;106:777-85 1995;4:1035-40.
Anda mungkin juga menyukai
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDari EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifePenilaian: 4 dari 5 bintang4/5 (5794)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDari EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You ArePenilaian: 4 dari 5 bintang4/5 (1090)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDari EverandNever Split the Difference: Negotiating As If Your Life Depended On ItPenilaian: 4.5 dari 5 bintang4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDari EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RacePenilaian: 4 dari 5 bintang4/5 (895)
- Grit: The Power of Passion and PerseveranceDari EverandGrit: The Power of Passion and PerseverancePenilaian: 4 dari 5 bintang4/5 (588)
- Shoe Dog: A Memoir by the Creator of NikeDari EverandShoe Dog: A Memoir by the Creator of NikePenilaian: 4.5 dari 5 bintang4.5/5 (537)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDari EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersPenilaian: 4.5 dari 5 bintang4.5/5 (345)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDari EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FuturePenilaian: 4.5 dari 5 bintang4.5/5 (474)
- Her Body and Other Parties: StoriesDari EverandHer Body and Other Parties: StoriesPenilaian: 4 dari 5 bintang4/5 (821)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Dari EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Penilaian: 4.5 dari 5 bintang4.5/5 (121)
- The Emperor of All Maladies: A Biography of CancerDari EverandThe Emperor of All Maladies: A Biography of CancerPenilaian: 4.5 dari 5 bintang4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingDari EverandThe Little Book of Hygge: Danish Secrets to Happy LivingPenilaian: 3.5 dari 5 bintang3.5/5 (400)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDari EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyPenilaian: 3.5 dari 5 bintang3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)Dari EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Penilaian: 4 dari 5 bintang4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDari EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaPenilaian: 4.5 dari 5 bintang4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDari EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryPenilaian: 3.5 dari 5 bintang3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnDari EverandTeam of Rivals: The Political Genius of Abraham LincolnPenilaian: 4.5 dari 5 bintang4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealDari EverandOn Fire: The (Burning) Case for a Green New DealPenilaian: 4 dari 5 bintang4/5 (74)
- The Unwinding: An Inner History of the New AmericaDari EverandThe Unwinding: An Inner History of the New AmericaPenilaian: 4 dari 5 bintang4/5 (45)
- Rise of ISIS: A Threat We Can't IgnoreDari EverandRise of ISIS: A Threat We Can't IgnorePenilaian: 3.5 dari 5 bintang3.5/5 (137)
- The 4 Main Phases of Wound HealingDokumen2 halamanThe 4 Main Phases of Wound HealingJacobMsangBelum ada peringkat
- Contoh Pidato Bahasa Inggris Tentang Perpisahan Sekolah Dan ArtinyaDokumen3 halamanContoh Pidato Bahasa Inggris Tentang Perpisahan Sekolah Dan ArtinyaJacobMsangBelum ada peringkat
- Catatan Harian Seorang Mahasiswa KedokteranDokumen14 halamanCatatan Harian Seorang Mahasiswa KedokteranJacobMsangBelum ada peringkat
- Clinical Anatomy of The Vulva, Vagina, Lower Pelvis, and PerineumDokumen20 halamanClinical Anatomy of The Vulva, Vagina, Lower Pelvis, and PerineumJacobMsangBelum ada peringkat
- Scar RemovalDokumen3 halamanScar RemovalJacobMsangBelum ada peringkat
- When Organs Fail One by OneDokumen6 halamanWhen Organs Fail One by OneJacobMsangBelum ada peringkat
- Anatomical Steps of ThyroidectomyDokumen7 halamanAnatomical Steps of ThyroidectomyJacobMsangBelum ada peringkat
- Video PemeriksaanDokumen8 halamanVideo PemeriksaanJacobMsangBelum ada peringkat
- Craniotomy VS CraniectoyDokumen1 halamanCraniotomy VS CraniectoyJacobMsangBelum ada peringkat
- Nonunion of The Fractured ClavicleDokumen18 halamanNonunion of The Fractured ClavicleJacobMsangBelum ada peringkat
- Wrist Ganglion: Definition and PathologyDokumen8 halamanWrist Ganglion: Definition and PathologyJacobMsangBelum ada peringkat
- Dissertation 7 HeraldDokumen3 halamanDissertation 7 HeraldNaison Shingirai PfavayiBelum ada peringkat
- Contoh Assignment PDFDokumen18 halamanContoh Assignment PDFSiti Fatimah A Salam67% (3)
- Toi Su20 Sat Epep ProposalDokumen7 halamanToi Su20 Sat Epep ProposalTalha SiddiquiBelum ada peringkat
- ISO - 21.060.10 - Bolts, Screws, Studs (List of Codes)Dokumen9 halamanISO - 21.060.10 - Bolts, Screws, Studs (List of Codes)duraisingh.me6602Belum ada peringkat
- 2a Unani Medicine in India - An OverviewDokumen123 halaman2a Unani Medicine in India - An OverviewGautam NatrajanBelum ada peringkat
- Chap9 PDFDokumen144 halamanChap9 PDFSwe Zin Zaw MyintBelum ada peringkat
- Fire Technical Examples DIFT No 30Dokumen27 halamanFire Technical Examples DIFT No 30Daniela HanekováBelum ada peringkat
- PH of Soils: Standard Test Method ForDokumen3 halamanPH of Soils: Standard Test Method ForYizel CastañedaBelum ada peringkat
- Industrial Machine and ControlsDokumen31 halamanIndustrial Machine and ControlsCarol Soi100% (4)
- Hindi ShivpuranDokumen40 halamanHindi ShivpuranAbrar MojeebBelum ada peringkat
- Information Technology Project Management: by Jack T. MarchewkaDokumen44 halamanInformation Technology Project Management: by Jack T. Marchewkadeeps0705Belum ada peringkat
- Getting Returning Vets Back On Their Feet: Ggoopp EennddggaammeeDokumen28 halamanGetting Returning Vets Back On Their Feet: Ggoopp EennddggaammeeSan Mateo Daily JournalBelum ada peringkat
- WinCC Control CenterDokumen300 halamanWinCC Control Centerwww.otomasyonegitimi.comBelum ada peringkat
- Jurnal Ekologi TerestrialDokumen6 halamanJurnal Ekologi TerestrialFARIS VERLIANSYAHBelum ada peringkat
- Intervensi Terapi Pada Sepsis PDFDokumen28 halamanIntervensi Terapi Pada Sepsis PDFifan zulfantriBelum ada peringkat
- 2 AcknowledgementDokumen8 halaman2 AcknowledgementPadil KonamiBelum ada peringkat
- FAO-Assessment of Freshwater Fish Seed Resources For Sistainable AquacultureDokumen669 halamanFAO-Assessment of Freshwater Fish Seed Resources For Sistainable AquacultureCIO-CIO100% (2)
- JP Selecta IncubatorDokumen5 halamanJP Selecta IncubatorAhmed AlkabodyBelum ada peringkat
- List of The Legend of Korra Episodes - Wikipedia PDFDokumen27 halamanList of The Legend of Korra Episodes - Wikipedia PDFEmmanuel NocheBelum ada peringkat
- Pest of Field Crops and Management PracticalDokumen44 halamanPest of Field Crops and Management PracticalNirmala RameshBelum ada peringkat
- LavazzaDokumen2 halamanLavazzajendakimBelum ada peringkat
- Engine Controls (Powertrain Management) - ALLDATA RepairDokumen3 halamanEngine Controls (Powertrain Management) - ALLDATA RepairRonald FerminBelum ada peringkat
- Project Manager PMP PMO in Houston TX Resume Nicolaas JanssenDokumen4 halamanProject Manager PMP PMO in Houston TX Resume Nicolaas JanssenNicolaasJanssenBelum ada peringkat
- Digital SLR AstrophotographyDokumen366 halamanDigital SLR AstrophotographyPier Paolo GiacomoniBelum ada peringkat
- Lesson Plan SustainabilityDokumen5 halamanLesson Plan Sustainabilityapi-501066857Belum ada peringkat
- Footing - f1 - f2 - Da RC StructureDokumen42 halamanFooting - f1 - f2 - Da RC StructureFrederickV.VelascoBelum ada peringkat
- ARC-232, Material Construction 2Dokumen4 halamanARC-232, Material Construction 2danishali1090Belum ada peringkat
- Corvina PRIMEDokumen28 halamanCorvina PRIMEMillerIndigoBelum ada peringkat
- Minuets of The Second SCTVE MeetingDokumen11 halamanMinuets of The Second SCTVE MeetingLokuliyanaNBelum ada peringkat
- Catálogo MK 2011/2013Dokumen243 halamanCatálogo MK 2011/2013Grupo PriluxBelum ada peringkat