Therapeutic Hypothermia Paper Jenna Spotts
Diunggah oleh
api-301727553Deskripsi Asli:
Judul Asli
Hak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Therapeutic Hypothermia Paper Jenna Spotts
Diunggah oleh
api-301727553Hak Cipta:
Format Tersedia
Running head: therapeutic hypothermia
Therapeutic Hypothermia
Jenna M. Spotts
Cedar Crest College
therapeutic hypothermia
2
Abstract
Therapeutic hypothermia is an intervention that is becoming more widely used in patients who
have cardiac or brain injuries. The purpose of therapeutic hypothermia is to decrease the chance
of a patient acquiring neural damage. Therapeutic hypothermia helps to decrease the metabolic
rate of the brain and decreases cerebral edema. The two most common types of therapeutic
hypothermia being used are surface cooling and endovascular cooling, endovascular is the more
invasive of the two methods however shivering is more common with surface cooling. As with
any intervention there are complications to therapeutic hypothermia, the most common being
shivering. Prior to cooling a patient lab tests are done and medications are administered. One of
the most important interventions to complete during the cooling process is to monitor the
patients temperature. For therapeutic hypothermia to be widely accepted education is a very
important aspect for continuing the use of the protocol. Therapeutic hypothermia is highly
beneficial to the patient because the chance of survival and hospital discharge is increased.
Keywords: Code Chill, Therapeutic Hypothermia, Therapeutic Hypothermia Cardiac,
Therapeutic Hypothermia Traumatic Brain Injury
therapeutic hypothermia
3
Therapeutic Hypothermia
Therapeutic hypothermia is the intentional cooling of a patients body temperature to
protect the brain and help with return of spontaneous circulation. Therapeutic hypothermia is
beneficial to the patient because the chance of survival and hospital discharge is increased. There
are two common methods, surface and endovascular. The main complication of therapeutic
hypothermia is shivering, however magnesium sulfate can be administered to help with the
shivering.
Pathophysiology
Therapeutic hypothermia is an intervention that is used in patients with cardiac, brain,
and spinal injuries, and hemorrhaging (Wright, 2005). As stated by Wright (2005), therapeutic
hypothermia is the cooling of a persons body temperature to less than thirty-six degrees Celsius
in a controlled setting. It is taught that hyperthermia is highly detrimental to the brain because an
increase in temperature will increase the metabolic demand of the brain as well as the
intracranial pressure (Wright, 2005). Wright (2005) states that along with keeping the body at
thirty six to thirty seven degrees Celsius for neuroprotection, it helps to intentionally cool the
body down to avoid more injury to the brain. Hypothermia helps to protect the brain by
inhibiting the massive depolarization that occurs, thus inhibiting the release of glutamate and
aspartate, and therefore maintains the stabilization of the blood-brain barrier and in turn prevents
cell death (Wright, 2005).
According to Varon and Acosta (2008), a study performed by Bigelow and McBernie
(1953) found that therapeutic hypothermia is beneficial to the heart and brain. Varon and Acosta
(2008) also discussed another study from Rosomoff and Gilbert (1955) that showed a direct
correlation between body temperature, brain volume, and intracranial pressure. It was found that
therapeutic hypothermia
the cooling of body temperature reduced the cerebral consumption of oxygen, metabolic rate
decreases, and blood flow is reduced (Varon & Acosta, 2008). The decrease in metabolic rate
allows for a decrease of carbon dioxide and lactate build-up (Wright, 2005).
Why and when a protocol is needed
According to Dixon and Keasling (2014) due to neurologic injury after a traumatic brain
injury or cardiac arrest, patients have an increased risk of death. With the use of therapeutic
hypothermia cerebral edema, inflammation, and cerebral metabolic rate are reduced; this in turn
reduces cell death because the brain cells are preserved (Dixon & Keasling, 2014). Dixon and
Keasling (2014) stated that there were two studies that help to push therapeutic hypothermia into
a protocol, these studies showed that therapeutic hypothermia helped to increase the patients
chances with a good outcome and in both studies the mortality rate was lower for those who
were in the hypothermia group.
The Advanced Life Support Task Force of the International Liaison Committee on
Resuscitation recommended that hospitals use therapeutic hypothermia on unconscious patients
with spontaneous return of circulation after ventricular fibrillation cardiac arrest (Dixon &
Keasling, 2014). The American Heart Association recommended that all patients who
experienced a cardiac arrest should have therapeutic hypothermia (Dixon & Keasling, 2014). The
American Heart Association recommended that therapeutic hypothermia be included with the
intervention of percutaneous coronary intervention for patients with an ST-segment elevated
myocardial infarction, the reason behind this is that a study showed that patients who underwent
both interventions had an increased survival rate (Dixon & Keasling, 2014). According to Dixon
and Keasling (2014) a protocol is necessary to improve the neurologic function along with
reduced mortality rates in patients after a cardiac arrest.
therapeutic hypothermia
5
Medications and diagnostic studies
Magnesium sulfate is found to be beneficial during the process of therapeutic
hypothermia, the benefits are reduction of shivering, enhances the cooling rates of the patients
due to vasodilation, and are said to have neuroprotective effects (Cushman, Warren, & Livesay,
2007).
Prior to starting therapeutic hypothermia a complete blood count, liver enzymes and
chemistries, pregnancy tests, electrocardiogram, and cranial computed tomography are
completed (Guluma, Hemmen, Olsen, Rapp, & Lyden, 2006). The patient is then given buspirone
prior to placing the catheter, and then a loading dose of meperidine is given and then the cooling
begins (Guluma, Hemmen, Olsen, Rapp, & Lyden, 2006).
Assessments and interventions
Interventions of therapeutic hypothermia are to monitor the patients temperature (Dixon
& Keasling, 2014). This intervention is highly important due to the patient being rapidly cooled
down and rewarmed (Dixon & Keasling, 2014). According to Dixon and Keasling (2014) the
ways to monitor body temperature during therapeutic hypothermia are esophageal, blood,
bladder, tympanic, and rectal.
Education is a very important intervention for therapeutic hypothermia, without
education there is a barrier to providing effective care (Dixon & Keasling, 2014). To overcome
this obstacle, the staff were given evidenced based research articles to show the necessity of
therapeutic hypothermia as well as informing the staff on what therapeutic hypothermia is
(Dixon & Keasling, 2014).
therapeutic hypothermia
6
Types of cooling
The two most common types of cooling methods that are used are surface and
endovascular (Dixon & Keasling, 2014). Dixon and Keasling (2014) stated that endovascular is
shown to cool the patient more quickly and have more accurate temperatures versus surface,
however endovascular is more expensive and requires a special invasive catheter. Surface
cooling takes longer, approximately two to eight hours, but is a simple procedure (Varon &
Acosta, 2008).
Surface cooling can be done through ice packs, circulating water blankets, and cold-water
immersion, however the side effect of shivering is more common in this scenario (Varon &
Acosta, 2008). Endovascular cooling occurs when a chilled saline solution is run through a
percutaneously set intravascular catheter (Varon & Acosta, 2008).
Complications of therapeutic hypothermia
Complications that were discussed were cardiac irritability, decreased clearance rate of
staphylococcal bacteremia, and ventricle fibrillation with deep hypothermia; deep hypothermia is
where the body temperature is decreased to less than thirty degrees Celsius (Varon & Acosta,
2008).
A common side effect of therapeutic hypothermia is shivering (Varon & Acosta, 2008).
Shivering is stated to increase body temperature and oxygen consumption (Varon & Acosta,
2008). Hypotension is another side effect that is treated with intravascular fluids (Varon &
Acosta, 2008). Varon and Acosta (2008) state that the side effect of hypotension and shivering
can be avoided if the patient is sedated properly and the correct neuromuscular blockers are
administered. Other side effects of therapeutic hypothermia are dysrhythmias and coagulopathies
(Varon & Acosta, 2008). It was reported that some patients experienced a decrease in the ability
therapeutic hypothermia
to fight off bacterial infections, and other patients had an increase in their leukocyte count; this
count was found to only be increased for the first twenty-four hours after therapeutic
hypothermia (Varon & Acosta, 2008).
Other complications of therapeutic hypothermia are hypokalemia, decreased stroke
volume, decreased contractility, and bradycardia (Wright, 2005). These are important end organ
cardiovascular complications to watch for because these complications can lead to decreased
cardiac output, increased systemic vascular resistance, and vasoconstriction (Wright, 2005).
According to Wright (2005) there are pulmonary complications such as tachypnea, atelectasis,
acute respiratory distress syndrome, pneumonia, and decreased cough reflex. Wright (2005)
states that another significant complication is rebound hyperemia and cerebral edema, this
happens during the rewarming stage, it was also noted that some patients experience an increase
in intracranial pressure. Due to the decrease in body temperature the patients can also experience
nephrogenic diabetes insipidus due to the decrease in enzymatic activity in the renal tubules
(Wright, 2008). Nephrogenic diabetes insipidus can be a problem because the treatment is
antidiuretic hormone, and during the cooling process the body is desensitized to both synthetic
and endogenous antidiuretic hormone (Wright, 2008).
Outcomes improved by the initiated protocol
According to Cushman, Warren, and Livesay (2007) the patients in the presented study
had an increase in survival rate, a majority of the patients were discharged home, and other
patients were either placed into a rehabilitation center or a skilled nursing facility. The nurses in
this study feel as though a protocol was formed that made a difference in the lives of patients, the
study showed that along with an increase in survival rate, the neurologic recovery was increased
(Cushman, Warren, & Livesay, 2008).
therapeutic hypothermia
It was found that patients who underwent percutaneous coronary intervention along with
therapeutic hypothermia the myocardial reperfusion injury is reduced which increases the
patients chances for a hospital discharge (Dixon & Keasling, 2014).
Conclusion
Therapeutic hypothermia is found to be beneficial to patients who have cardiac or brain
injuries. Therapeutic hypothermia is the cooling of a patients body in a controlled setting to
decrease the chance of neural injury. The chances of survival are increased when this
intervention is used. The two most common types of cooling were discussed. Shivering is a
common side effect of therapeutic hypothermia.
therapeutic hypothermia
9
References
Cushman, L., Warren, M., & Livesay, S. (2007). Bringing research to the bedside: The role of
induced hypothermia in cardiac arrest. Critical Care Nursing Quaterly, 30(2). Pages 143153.
Dixon, M., & Keasling, M. (2014). Development of a therapeutic hypothermia protocol:
Implementation for postcardiac arrest STEMI patients. Critical Care Nursing Quaterly,
37(4). Pages 377-383.
Guluma, K., Hemmen, T., Olsen, S., Rapp, K., & Lyden, P. (2006). A trial of therapeutic
hypothermia via endovascular approach in awake patients with acute ischemic strokes:
Methodology. Academic Emergency Medicine, 13. Pages 820-827.
Varon, J., & Acosta, P. (2008). Therapeutic hypothermia: Past, present, and future. Chest, 133(5).
Pages 1267-1274.
Wright, J. (2005). Therapeutic hypothermia in traumatic brain injury. Critical Care Nursing
Quaterly, 28(2). Pages 150-161.
Anda mungkin juga menyukai
- The Yellow House: A Memoir (2019 National Book Award Winner)Dari EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Penilaian: 4 dari 5 bintang4/5 (98)
- Acute Care MapDokumen11 halamanAcute Care Mapapi-301727553Belum ada peringkat
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDari EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifePenilaian: 4 dari 5 bintang4/5 (5795)
- Jenna Spotts Ebs PosterDokumen1 halamanJenna Spotts Ebs Posterapi-301727553Belum ada peringkat
- Shoe Dog: A Memoir by the Creator of NikeDari EverandShoe Dog: A Memoir by the Creator of NikePenilaian: 4.5 dari 5 bintang4.5/5 (537)
- Concept MapDokumen22 halamanConcept Mapapi-3017275530% (1)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDari EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FuturePenilaian: 4.5 dari 5 bintang4.5/5 (474)
- Epidemiological StudyDokumen6 halamanEpidemiological Studyapi-301727553Belum ada peringkat
- Grit: The Power of Passion and PerseveranceDari EverandGrit: The Power of Passion and PerseverancePenilaian: 4 dari 5 bintang4/5 (588)
- Apa PaperDokumen8 halamanApa Paperapi-301727553Belum ada peringkat
- On Fire: The (Burning) Case for a Green New DealDari EverandOn Fire: The (Burning) Case for a Green New DealPenilaian: 4 dari 5 bintang4/5 (74)
- Aging PaperDokumen16 halamanAging Paperapi-301727553Belum ada peringkat
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDari EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryPenilaian: 3.5 dari 5 bintang3.5/5 (231)
- Process RecordingDokumen13 halamanProcess Recordingapi-301727553Belum ada peringkat
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDari EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RacePenilaian: 4 dari 5 bintang4/5 (895)
- Jenna Spotts: Languages SoftwareDokumen2 halamanJenna Spotts: Languages Softwareapi-301727553Belum ada peringkat
- Never Split the Difference: Negotiating As If Your Life Depended On ItDari EverandNever Split the Difference: Negotiating As If Your Life Depended On ItPenilaian: 4.5 dari 5 bintang4.5/5 (838)
- Reflective PaperDokumen13 halamanReflective Paperapi-301727553100% (2)
- The Little Book of Hygge: Danish Secrets to Happy LivingDari EverandThe Little Book of Hygge: Danish Secrets to Happy LivingPenilaian: 3.5 dari 5 bintang3.5/5 (400)
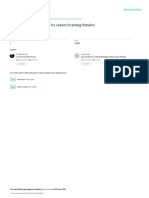
- Hormonal Imbalance and Its Causes in Young Females: January 2015Dokumen6 halamanHormonal Imbalance and Its Causes in Young Females: January 2015figgernaggotBelum ada peringkat
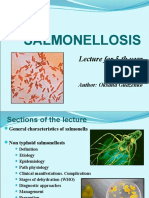
- Salmonellosis 2021Dokumen36 halamanSalmonellosis 2021mehrshad Farahpour Gp5Belum ada peringkat
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDari EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersPenilaian: 4.5 dari 5 bintang4.5/5 (345)
- CytopathologyDokumen19 halamanCytopathologyማላያላም ማላያላም100% (2)
- Black Seedd 30mlDokumen1 halamanBlack Seedd 30mlKalinix DigitalBelum ada peringkat
- The Unwinding: An Inner History of the New AmericaDari EverandThe Unwinding: An Inner History of the New AmericaPenilaian: 4 dari 5 bintang4/5 (45)
- Webinar 10 12 17 PDFDokumen73 halamanWebinar 10 12 17 PDFDanielaGarciaBelum ada peringkat
- Team of Rivals: The Political Genius of Abraham LincolnDari EverandTeam of Rivals: The Political Genius of Abraham LincolnPenilaian: 4.5 dari 5 bintang4.5/5 (234)
- Diagnosis and Management of Treatment Refractory HypothyroidismDokumen17 halamanDiagnosis and Management of Treatment Refractory HypothyroidismMerlyn AngelinaBelum ada peringkat
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDari EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyPenilaian: 3.5 dari 5 bintang3.5/5 (2259)
- MethottexateDokumen104 halamanMethottexateFarha Elein KukihiBelum ada peringkat
- Hypocalcemia: Author: Christopher B Beach, MD, FACEP, FAAEM, Associate Professor and ViceDokumen65 halamanHypocalcemia: Author: Christopher B Beach, MD, FACEP, FAAEM, Associate Professor and ViceronelnBelum ada peringkat
- Research Proposal DoneDokumen8 halamanResearch Proposal DoneLoveu GoBelum ada peringkat
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDari EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaPenilaian: 4.5 dari 5 bintang4.5/5 (266)
- NP4 ExamDokumen14 halamanNP4 ExamArnie Jude CaridoBelum ada peringkat
- The Emperor of All Maladies: A Biography of CancerDari EverandThe Emperor of All Maladies: A Biography of CancerPenilaian: 4.5 dari 5 bintang4.5/5 (271)
- Blood Component TherapyDokumen8 halamanBlood Component TherapyquerokeropiBelum ada peringkat
- TURP SyndromeDokumen13 halamanTURP SyndromeWindy Ari WijayaBelum ada peringkat
- Rise of ISIS: A Threat We Can't IgnoreDari EverandRise of ISIS: A Threat We Can't IgnorePenilaian: 3.5 dari 5 bintang3.5/5 (137)
- Gosssypiboma: Dr. B.V AmruthavalliDokumen3 halamanGosssypiboma: Dr. B.V AmruthavalliInternational Organization of Scientific Research (IOSR)Belum ada peringkat
- Lips Diseases and Its Management: Classification of Lip DisordersDokumen17 halamanLips Diseases and Its Management: Classification of Lip DisordersSubhash VermaBelum ada peringkat
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDari EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You ArePenilaian: 4 dari 5 bintang4/5 (1090)
- ImplementDokumen17 halamanImplementkrissy100% (3)
- Junal PDFDokumen8 halamanJunal PDFAneu DwiBelum ada peringkat
- Neonatal SepsisDokumen8 halamanNeonatal SepsisPrabiñKhadkaBelum ada peringkat
- Agrypnia Excitata and Obstructive Apnea in A Patient With Fatal Familial Insomnia From ChinaDokumen5 halamanAgrypnia Excitata and Obstructive Apnea in A Patient With Fatal Familial Insomnia From ChinaDayana VieiraBelum ada peringkat
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Dari EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Penilaian: 4.5 dari 5 bintang4.5/5 (121)
- OCD Lecture NotesDokumen4 halamanOCD Lecture NotesAustin Higgins67% (3)
- 1768-Article Text-8493-1-10-20230604Dokumen6 halaman1768-Article Text-8493-1-10-20230604Maya azrianiBelum ada peringkat
- 12 Lead Electrocardiogram (Ecg) Placement: Module DescriptionDokumen11 halaman12 Lead Electrocardiogram (Ecg) Placement: Module DescriptionHanna La MadridBelum ada peringkat
- Anxiety DisorderDokumen44 halamanAnxiety DisorderKemal AmanoBelum ada peringkat
- Avascular NecrosisDokumen58 halamanAvascular Necrosischatree100% (4)
- Cardiology FMDokumen25 halamanCardiology FMtrushaBelum ada peringkat
- PacemakerDokumen24 halamanPacemakerLAWKUSH KUMARBelum ada peringkat
- Tetanus Neonatorum LectureDokumen11 halamanTetanus Neonatorum LectureJackBelum ada peringkat
- HaemoptysisDokumen22 halamanHaemoptysisminci sensei100% (5)
- Droplet Infection: Tuberkulosis (TB) ParuDokumen2 halamanDroplet Infection: Tuberkulosis (TB) ParuMiiniieBelum ada peringkat
- Her Body and Other Parties: StoriesDari EverandHer Body and Other Parties: StoriesPenilaian: 4 dari 5 bintang4/5 (821)
- Acute Mesenteric IschemiaDokumen46 halamanAcute Mesenteric Ischemiashita febrianaBelum ada peringkat
- Lecture 1 - Principles of Newborn ResuscitationDokumen29 halamanLecture 1 - Principles of Newborn ResuscitationShane Lim GarciaBelum ada peringkat