Spinal Cord
Diunggah oleh
Remelou Garchitorena AlfelorDeskripsi Asli:
Hak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Spinal Cord
Diunggah oleh
Remelou Garchitorena AlfelorHak Cipta:
Format Tersedia
Colegio de San Beda - Medicina 2013
Neuroscience 3
SPINAL CORD INJURY AND COMPRESSION
2.
Corticospinal tract, the corticorubrospinal tract, and the
lateral reticulospinal tract - inhibit the antigravity muscles
and facilitate the antagonists.
Cross-Sectional Anatomy of the Spinal Cord
Anatomy of the Spinal Cord
The spinal cord, like the brain, is composed of gray matter and white
matter.
The white matter contains ascending and
descending fiber tracts, while the gray
matter contains neurons of different kinds:
Anterior horns contain mostly
motor neurons
Lateral horns mostly autonomic
neurons, and
Posterior horns mostly
somatosensory neurons
participating in a number of
different afferent pathways
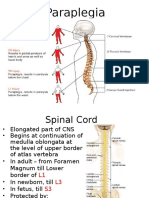
In adults, the spinal cord is shorter than the
vertebral column: it extends from the
craniocervical junction to about the level
between L1 - L2
The segments of the neural tube (primitive
spinal cord) correspond to those of the vertebral
column only up to the third month of gestation,
after which the growth of the spine progressively
outstrips that of the spinal cord.
Nerve roots exit from the spinal canal at the
numerically corresponding levels, so that the
lower thoracic and lumbar roots must travel an
increasingly long distance through the SAS to
reach the intervertebral foramina through which
they exit.
The spinal cord ends as the conus medullaris (or
conus terminalis) at the L1 or L2 level (rarely at
L3).
Below this level, the lumbar sac (theca)contains
only nerve root filaments, the so-called cauda
equina (horses tail)
Motor & Sensory Dermatomes
Dermatome
Specific area in which the spinal nerve travels or controls
Useful in assessment of specific level SCI
Cross-Sectional Anatomy of the Spinal Cord
Major Ascending and Descending Tracts of the Spinal Cord
Ascending Tracts
There are 3 main sensory systems entering the spinal cord:
1. Pain and Temperature lateral spinothalamic tract
2. Proprioceptjon stereognosis medial lemniscus ( fasciculus
gracilis and fasciculus cuneatus)
3. Light touch ventral spinothalamic tract
Descending Tracts 5 ; these systems are important in the postural
control of the limbs.
1. Vestibulospinal tract and the medial reticulospinal tract tend to facilitate motor neurons of antigravity muscles
Page 1
princessczaronne
Colegio de San Beda - Medicina 2013
Neuroscience 3
Dermatomes
C3,4
C3, 4, 5
C5, 6
C7
C8, T1
T4
T10
L1, 2
L3,4
L5
S1
S1, 2
S2,3,4
SPINAL CORD INJURY
motor:shoulder shrug
sensory: top of shoulder
motor: diaphragm
sensory: top of shoulder
motor:elbow flexion
sensory: thumb
motor: elbow, wrist, finger extension
sensory: middle finger
motor: finger abduction & adduction
sensory: little finger
Syndrome of Acute Paraplegia or Quadriplegia Due to Complete Transverse
Lesions of the SC (Transverse Myelopathy)
Trauma ->most frequent cause, but it occurs also as a result of infarction
or hemorrhage and with rapidly advancing compressive, necrotizing,
demyelinative, or inflammatory lesions (transverse myelitis).
Types of Injury
Severe forward flexion injury ;
Hyperextension injury ;
Whiplash injury
High-velocity missile penetrates the vertebral canal and
damages the spinal cord directly;
Indirect consequence of a vascular mechanism.
motor: level of nipple
motor: level of umbilicus
motor: hip flexion
sensory: inguinal crease
motor: quadriceps
sensory: medial thigh, calf
motor: great toe, foot dorsiflexion
sensory: lateral calf
Pathology of Spinal Cord Injury
As a result of squeezing or shearing of the spinal cord, there is
destruction of gray and white matter and a variable amount of
hemorrhage, chiefly in the more vascular central parts -> traumatic
necrosis (are maximal at the level of injury and one or two segments
above and below it)
As a lesion heals, it leaves a gliotic focus or cavitation with variable
amounts of hemosiderin and iron pigment.
Progressive cavitation (traumatic syringomyelia) may develop after an
interval of months or years - > lead to a delayed central or incomplete
transverse cord syndrome.
In most traumatic lesions, the central part of the spinal cord, with its
vascular gray matter, tends to suffer greater injury than the peripheral
parts.
This is the central cervical cord syndrome, also called the
Schneider syndrome
motor: knee flexion
sensory: lateral foot
motor: foot plantar flexion
motor: anal sphincter tone
sensory: perianal
DISEASES OF THE SPINAL CORD
Diseases of the nervous system may be confined to the spinal cord,
where they produce a number of distinctive syndromes.
These syndromes relate to the special physiologic and anatomic features
of the cord, such as its prominent function in sensorimotor conduction
and relatively primitive reflex activity
The main syndromes to be considered are:
1.
a complete or almost complete sensorimotor myelopathy
that involves most or all of the ascending and descending
tracts (transverse myelopathy);
2. a combined painful radicular and transverse cord syndrome;
3. the hemicord (Brown-Sequard) syndrome;
4. a ventral cord syndrome, sparing posterior column function;
5. a high cervicalforamen magnum syndrome;
6. a central cord or syringomyelic syndrome;
7. a syndrome of the conus medullaris;
8.
a syndrome of the cauda equina
In addition, an important distinction is made between lesions within the
cord (intramedullary) and those that compress the cord from without
(extramedullary).
Clinical Effects of Spinal Cord Injury
When the spinal cord is suddenly
and virtually or completely
severed, three disorders of
function are at once evident:
1.
all voluntary movement in parts of the body below the
lesion is immediately and permanently lost;
2. all sensation from the lower (aboral) parts is abolished; and
3. reflex functions in all segments of the isolated spinal cord are
suspended.
The last effect, called spinal shock, involves tendon as well as autonomic
reflexes. It is of variable duration (1 to 6 weeks as a rule but sometimes
far longer)
Less complete lesions of the spinal cord result in little or no spinal shock,
and the same is true of any type of lesion that develops slowly.
Page 2
princessczaronne
Colegio de San Beda - Medicina 2013
Neuroscience 3
Stage of Spinal Shock or Areflexia
The loss of motor function
at the time of injury
1. Tetraplegia -lesions of
the C4-5
2. Paraplegia -lesions of the
thoracic cord
-results in atonic paralysis
of bladder and bowel,
gastric atony, loss of
sensation below a level
corresponding to the
spinal cord lesion,
muscular flaccidity, and
areflexia
As a result of their sudden
separation from higher levels, the neural elements below the lesion fail
to perform their normal function
Disturbance in autonomic function.
Vasomotor tone, sweating, and piloerection in the lower
parts of the body are temporarily abolished.
Systemic hypotension may be severe and contribute to the
spinal cord damage.
The lower extremities lose heat if left uncovered, and they
swell if dependent.
The skin becomes dry and pale, and ulcerations may develop
over bony prominences.
The sphincters of the bladder and the rectum remain
contracted but the detrusor of the bladder and smooth
muscle of the rectum are atonic.
Urine accumulates until the intravesicular pressure is
sufficient to overcome the sphincters; then driblets escape
(overflow incontinence). There is also passive distention of
the bowel, retention of feces, and absence of peristalsis
(paralytic ileus)
Genital reflexes (penile erection, bulbocavernosus reflex,
contraction of dartos muscle) are abolished or profoundly
depressed.
Loss of motor and sensory function above the lesion, coming on years
after the trauma, occurs occasionally and is due to an enlarging cavity in
the proximal segment of the cord ( Syringomyelia)
Transient Cord Injury (Spinal Cord Concussion)
Transient loss of motor and/or sensory function of the spinal cord that
recovers within minutes or hours but sometimes persists for a day or
several days.
Spinal cord concussion from direct impact is observed most frequently in
athletes engaged in contact sports (football, rugby,and hockey).
Progressive Spinal Cord Transection Syndrome
When spinal cord transection syndrome arises gradually rather than
suddenly, e. g., because of a slowly growing tumor, spinal shock does not
arise.
The transection syndrome in such cases is usually partial, rather than
complete.
Progressively severe spastic paraparesis develops below the level of the
lesion, accompanied by a sensory deficit, bowel, bladder, and sexual
dysfunction, and autonomic manifestations (abnormal vasomotor
regulation and sweating, tendency to decubitus ulcers).
Thoracic spinal cord transection syndrome
Transection of the upper thoracic cord spares the upper limbs but
impairs breathing and may also cause paralytic ileus through
involvement of the splanchnic nerves.
Transection of the lower thoracic cord spares the abdominal muscles
and does not impair breathing.
Lumbar spinal cord transection syndrome
Traumatic transection of the spinal cord at lumbar levels often causes
especially severe disturbances because of concomitant damage of the
major supplying artery of the lower spinal cord, the great radicular
artery (of Adamkiewicz).
The result is infarction of the entire lumbar and sacral spinal cord
Epiconus syndrome
Caused by a spinal cord lesion at the L4 to S2 level
Unlike conus syndrome , it is associated with spastic or flaccid paresis of
the lower limbs , depending on the precise level of the lesion.
There is weakness or total paralysis of hip external rotation (L4S1) and
extension (L4L5), and possibly also of knee flexion (L4S2) and flexion and
extension of the ankles and toes (L4S2).
The Achilles reflex is absent, while the knee-jerk reflex is preserved.
The sensory deficit extends from L4 to S5.
The bladder and bowel empty only reflexively; sexual potency is lost, and
male patients often have priapism.
There is transient vasomotor paralysis, as well as a transient loss of
sweating
Stage of Heightened Reflex Activity
This is the more familiar neurologic state that emerges within several
weeks or months after spinal injury.
After a few weeks, the reflex responses to stimulation, which are initially
minimal and unsustained, become stronger and more easily elicitable
and as time passes come to include additional and more proximal
muscles.
Gradually the typical pattern of heightened flexion reflexes emerges:
Dorsiflexion of the big toe (Babinski sign); fanning
of the other toes; and later, flexion or slow
withdrawal movements of the foot, leg, and thigh
with contraction of the tensor fascia lata muscle (
triple flexion).
Retention of urine becomes less complete, and at irregular intervals
urine is expelled by spontaneous contractions of the detrusor muscle.
Reflex defecation also begins
Conus syndrome
Due to a spinal cord lesion at or below S3, is also rare.
It can be caused by spinal tumors, ischemia, or a massive lumbar disk
herniation.
An isolated lesion of the conus medullaris produces the following
neurological deficits:
Detrusor areflexia with urinary retention and overflow incontinence
(continual dripping)
Fecal incontinence
- Impotence
Saddle anesthesia (S3S5) - Loss of the anal reflex
The lower limbs are not paretic, and the Achilles reflex is preserved
(L5S2).
Clinical Effects of Spinal Cord Injury
Any residual symptoms persisting after 6 months are likely to be
permanent, although in a small proportion of patients some return of
function (particularly sensation) is possible
Page 3
princessczaronne
Colegio de San Beda - Medicina 2013
Neuroscience 3
If conus syndrome is produced by a tumor, the lumbar and sacral roots
descending alongside the conus will be affected sooner or later
In such cases, the manifestations of conus syndrome are accompanied
by deficits due to involvement of the cauda equina:weakness of the
lower limbs, and more extensive sensory deficits than are seen in pure
conus syndrome
Cauda equina syndrome
Involves the lumbar and sacral nerve roots, which descend alongside and
below the conus medullaris, and through the lumbosacral subarachnoid
space, to their exit foramina;
a tumor (e. g., ependymoma or lipoma) is the usual cause.
Patients initially complain of radicular pain in a sciatic distribution, and
of severe bladder pain that worsens with coughing or sneezing.
Later, severe radicular sensory deficits, affecting all sensory modalities,
arise at L4 or lower levels.
Lesions affecting the upper portion of the cauda equina produce a
sensory deficit in the legs and in the saddle area.
There may be flaccid paresis of the lower limbs with areflexia; urinary
and fecal incontinence also develop, along with impaired sexual
function.
With lesions of the lower portion of the cauda equina, the sensory
deficit is exclusively in the saddle area (S3S5), and there is no lower limb
weakness, but urination, defecation, and sexual function are impaired.
Tumors affecting the cauda equina, unlike conus tumors, produce slowly
and irregularly progressive clinical manifestations, as the individual
nerve roots are affected with variable rapidity, and some of them may
be spared until late in the course of the illness.
Central Cord Syndrome (Schneider Syndrome) and Cruciate Paralysis
Loss of motor function is characteristically more
severe in the upper limbs than in the lower ones
and particularly severe in the hands.
Bladder dysfunction with urinary retention
occurs in some of cases, and sensory loss is often
slight (hyperpathia over the shoulders and arms
may be the only sensory abnormality).
Damage of the centrally situated gray matter may leave an atrophic,
areflexic paralysis and a segmental loss of pain and thermal sensation
from interruption of crossing pain and thermal fibers.
Etiologies
Retroflexion injuries of the head and neck most common
Hematomyelia
Necrotizing myelitis
Fibrocartilagenous embolism
Infarction due to dissection or compression of the vertebral
artery in the medullary-cervical region
Injuries of the very rostral cervical cord (C1 C2) results in cruciate
paralysis.
Similar to the central cord syndrome except that the weakness is even
more selective, being practically limited to the arms -> a feature that is
attributable to the segregation of corticospinal fibers to the arms
(rostral) and to the legs (caudal) within the pyramidal decussation.
The arm weakness may be asymmetrical or even unilateral; sensory loss
is inconsistent.
Complete paralysis of the arms and legs usually indicates a fracture or
dislocation at C4-C5.
If the legs are paralyzed and the arms can still be abducted and flexed,
the lesion is likely to be at C5-C6
Paralysis of the legs and only the hands indicates a lesion at C6-C7
The level of sensory loss on the trunk, determined by perception of
pinprick, is an accurate guide to the level of the lesion
In all cases of SCI our primary concern is that movement (especially
flexion) of the cervical spine be avoided.
The patient should be placed supine on a firm, flat surface (with one
person assigned, if possible, to keeping the head and neck immobile)
Have the patient remain on the board until a lateral film or a CT or MRI
of the cervical spine has been obtained.
A neurologic examination with detailed recording of motor, sensory, and
sphincter function is necessary to follow the clinical progress of SCI.
If a cervical spinal cord injury is associated with vertebral dislocation,
traction on the neck is necessary to secure proper alignment and
maintain immobilization.
This is best accomplished by use of a halo brace, which, of all the
appliances used for this purpose provides the most rigid external fixation
of the cervical spine.
This type of fixation is usually continued for 4 to 6 weeks, after which a
rigid collar may be substituted.
If a cervical spinal cord injury is associated with vertebral dislocation,
traction on the neck is necessary to secure proper alignment and
maintain immobilization.
This is best accomplished by use of a halo brace, which, of all the
appliances used for this purpose provides the most rigid external fixation
of the cervical spine.
This type of fixation is usually continued for 4 to 6 weeks, after which a
rigid collar may be substituted.
Syndrome of the dorsal root ganglion
Infection of one or more
spinal ganglia by a
neurotropic virus occurs
most commonly in the
thoracic region and causes
painful erythema of the
corresponding
dermatome(s), followed by the formation of a variable number of
cutaneous vesicles.
This clinical picture, called herpes zoster, is associated with very
unpleasant, stabbing pain and paresthesiae in the affected area.
The infection may pass from the spinal ganglia into the spinal cord itself,
but, if it does, it usually remains confined to a small area within the cord.
Involvement of the anterior horns causing flaccid paresis is rare, and
hemiparesis or paraparesis is even rarer.
Electromyography can demonstrate a segmental motor deficit in up to
2/3 of all cases, but, because herpes zoster is usually found in the
thoracic area, the deficit tends to be functionally insignificant, and may
escape the patients notice.
In some cases, the cutaneous lesion is absent (herpes sine herpete).
Herpes zoster is relatively common, with an incidence of 35 cases per
1000 persons per year; immunocompromised individuals (e. g., with
AIDS, malignancy, or immunosuppression) are at elevated risk.
Treatment with topical dermatological medication as well as aciclovir, or
another specific virustatic agent, is recommended.
Even with appropriate treatment, postherpetic neuralgia in the affected
area is a not uncommon complication.
It can be treated symptomatically with various medications, including
carbamazepine and gabapentin.
Examination and Management of the Spine-Injured Patient
The level of the spinal cord and vertebral lesions can be determined
from the clinical findings.
Diaphragmatic paralysis occurs with lesions of the upper three cervical
segments (an unrelated transient arrest of breathing is common in
severe head injury).
Page 4
princessczaronne
Colegio de San Beda - Medicina 2013
Neuroscience 3
Posterior root syndrome
If two or more
adjacent posterior
roots are completely
divided, sensation in
the corresponding
dermatomes is
partially or totally lost.
Incomplete posterior root lesions affect different sensory modalities to
variable extents, with pain sensation usually being most strongly
affected.
Because the lesion interrupts the peripheral reflex arc, the sensory
deficit is accompanied by hypotonia and hyporeflexia or areflexia in the
muscles supplied by the affected roots.
These typical deficits are produced only if multiple adjacent roots are
affected.
Posterior column syndrome
The posterior
columns can be
secondarily
involved by
pathological
processes
affecting the
dorsal root
ganglion cells
and the
posterior roots.
Lesions of the posterior columns typically impair position and vibration
sense, discrimination, and stereognosis; they also produce a positive
Romberg sign, as well as gait ataxia that worsens significantly when the
eyes are closed (unlike cerebellar ataxia, which does not).
Posterior column lesions also often produce hypersensitivity to pain.
Possible causes include vitamin B12 deficiency (e. g., in funicular
myelosis), AIDS-associated vacuolar myelopathy, and spinal cord
compression (e. g., in cervical spinal stenosis).
Tabes dorsalis due to syphilis
Posterior horn syndrome
Can be a clinical manifestation of syringomyelia, hematomyelia, and
some intramedullary spinal cord tumors, among other conditions.
Like posterior root lesions, posterior horn lesions produce a segmental
somatosensory deficit; yet, rather than impairing all sensory modalities
like posterior root lesions, posterior horn lesions spare the modalities
subserved by the posterior columns, i.e., epicritic and proprioceptive
sense.
Only pain and temperature sensation are lost in the corresponding
ipsilateral segments
Loss of pain and temperature sensation with sparing of posterior column
sense is called a dissociated somatosensory deficit.
There may be spontaneous pain (deafferentation pain) in the analgesic
area.
Pain and temperature sensation are intact below the level of the lesion,
as the lateral spinothalamic tract, lying in the anterolateral funiculus, is
undamaged and continues to conduct these modalities centrally.
The most prominently affected fibers are those that originate in
posterior horn cells and conduct coarse pressure, touch, pain, and
temperature sensation; these fibers decussate in the central gray matter
and then ascend in the anterior and lateral spinothalamic tracts.
A lesion affecting them produces a bilateral dissociated sensory deficit in
the cutaneous area supplied by the damaged fibers.
Syringomyelia is characterized by the formation of one or more fluidfilled cavities in the spinal cord; the analogous disease in the brainstem
is called syringobulbia.
The cavities, called syringes, can be formed by a number of different
mechanisms and are distributed in different characteristic patterns
depending on their mechanism of formation.
Some syringes are an expansion of the central canal of the spinal cord,
which may or may not communicate with the fourth ventricle; others are
a hollowing-out of the parenchyma and are separate from the central
canal.
The term hydromyelia is sometimes used loosely for communicating
syringes of the central canal, but it properly refers to an idiopathic,
congenital variant of syringomyelia in which the syrinx communicates
with the subarachnoid space, and should only be used in this sense.
Syringomyelia most commonly affects the cervical spinal cord, typically
producing loss of pain and temperature sensation in the shoulders and
upper limbs.
A progressively expanding syrinx can damage the long tracts of the spinal
cord, producing spastic (para)paresis and disturbances of bladder,
bowel, and sexual function.
Syringobulbia often causes unilateral atrophy of the tongue, hypalgesia
or analgesia of the face, and various types of nystagmus depending on
the site and configuration of the syrinx.
Syndrome of combined lesions of the posterior columns and corticospinal tracts
(funicular myelosis)
Most commonly produced by vitaminB12 deficiency due to a lack of
gastric intrinsic factor (e. g., in atrophic gastritis), and is known in such
cases as subacute combined degeneration, or SCD.
Foci of demyelination are found in the cervical and thoracic regions in
the posterior columns (70- 80%), and somewhat less commonly in the
pyramidal tracts (40 - 50%), while the gray matter is usually spared.
Posterior column damage causes loss of position and vibration sense in
the lower limbs, resulting in spinal ataxia and a positive Romberg sign
(unstable stance with eyes closed).
The accompanying pyramidal tract damage causes spastic paraparesis
with hyperreflexia and bilateral Babinski signs.
Graymatter Syndrome
Damage to the central gray matter of the spinal cord by syringomyelia,
hematomyelia, intramedullary spinal cord tumors, or other processes
interrupts all of the fiber pathways passing through the gray matter.
Page 5
princessczaronne
Colegio de San Beda - Medicina 2013
Neuroscience 3
Anterior Horn Syndrome
Both acute poliomyelitis and spinal muscle atrophy of various types
specifically affect the anterior horn cells, particularly in the cervical and
lumbar enlargements of the spinal cord.
In poliomyelitis (a viral infection), a variable number of anterior horn
cells are acutely and irreversibly lost, mainly in the lumbar region,
causing flaccid paresis of the muscles in the corresponding segments.
Proximal muscles tend to be more strongly affected than distal ones.
The muscles become atrophic and, in severe cases, may be completely
replaced by connective tissue and fat.
It is rare for all of the muscles of a limb to be affected, because the
anterior horn cells are arranged in long vertical columns within the spinal
cord
Pain and temperature sense are largely or completely spared.
The ataxia is severe, because both the posterior columns and the
spinocerebellar tracts are involved; it is evident when the patient tries to
walk, stand, or sit, as well as in the fingernosefinger and heelkneeshin
tests.
The patients gait is uncoordinated, with festination, and also becomes
spastic over time as the pyramidal tracts progressively degenerate.
About half of all patients manifest skeletal deformities such as scoliosis
or pes cavus (the so-called Friedreich foot).
Friedreich ataxia can be diagnosed when the following clinical criteria
are met:
Progressive ataxia of no other known cause, beginning
before age 25 years
Autosomal recessive inheritance
Absent deep tendon reflexes in the lower limbs
Posterior column disturbance
Dysarthria within five years of onset
The diagnosis can be definitively established by underlying genetic
defect, a trinucleotide expansion on Chr 9
Syndrome of the Corticospinal Tracts
Loss of cortical motor neurons is followed by degeneration of the
corticospinal tracts in a number of different diseases, including primary
lateral sclerosis (a variant of amyotrophic lateral sclerosis) and the rarer
form of hereditary spastic spinal paralysis.
The most common subform of this disease is due to a mutation of the
gene for an ATPase of the AAA family on chromosome 2; the disease
appears in childhood and progresses slowly thereafter.
Patients complain initially of a feeling of heaviness, then of weakness in
the lower limbs.
Spastic paraparesis with a spastic gait disturbance gradually develops
and worsens.
The reflexes are brisker than normal.
Spastic paresis of the upper limbs does not develop until much later.
Spinal Cord Hemisection Syndrome (BrownSquard Syndrome)
Rare and usually incomplete; its most common causes are spinal trauma
and cervical disk herniation.
Interruption of the descending motor pathways on one side of the spinal
cord causes an initially flaccid, ipsilateral paresis below the level of the
lesion (spinal shock), which later becomes spastic and is accompanied by
hyperreflexia, Babinski signs, and vasomotor disturbances.
At the same time, the interruption of the posterior columns on one side
of the spinal cord causes ipsilateral loss of position sense, vibration
sense, and tactile discrimination below the level of the lesion.
The ataxia that would normally be caused by the posterior column
lesion cannot be demonstrated because of the coexisting ipsilateral
paresis.
Pain and temperature sensation are spared on the side of the lesion,
because the fibers subserving these modalities have already crossed to
the other side to ascend in the lateral spinothalamic tract, but pain and
temperature sensation are lost contralaterally below the level of the
lesion, because the ipsilateral (crossed) spinothalamic tracts are
interrupted.
Simple tactile sensation is not impaired, as this modality is subserved by
two different fiber pathways: the posterior columns (uncrossed) and the
anterior spinothalamic tract (crossed).
Syndrome of combined involvement of the posterior columns, spinocerebellar
tracts, and (possibly) pyramidal tracts
When the pathological process affects all of these systems, the
differential diagnosis should include spinocerebellar ataxia of Friedreich
type, the axonal form of a hereditary neuropathy (HSMN II), and other
ataxias.
Characteristic clinical manifestations are produced by the lesions in each
of the involved systems.
Friedreich ataxia begins before age 20 with loss of dorsal root ganglion
cells, leading to posterior column degeneration.
The clinical result is an impairment of position sense, two-point
discrimination, and stereognosis, with spinal ataxia and a positive
Romberg sign.
Page 6
princessczaronne
Colegio de San Beda - Medicina 2013
Neuroscience 3
Hemisection of the cord leaves one of these two pathways intact for
tactile sensation on either side of the bodythe contralateral posterior
columns for the side contralateral to the lesion, and the contralateral
anterior spinothalamic tract for the side ipsilateral to it.
Aside from the interruption of the long tracts, the anterior horn cells
may be damaged to a variable extent at the level of the lesion, possibly
causing flaccid paresis.
Irritation of the posterior roots may also cause paresthesiae or radicular
pain in the corresponding dermatomes at the upper border of the
sensory disturbance.
The spine is tender to percussion at the level of the damaged nerve
roots, and the pain is markedly exacerbated by coughing or sneezing.
The pain caused by posterior column involvement is of rheumatic
quality and initially arises at the distal ends of the limbs.
Hyperesthesia is not uncommon in the dermatomes supplied by the
affected nerve roots; this may be useful for clinical localization of the
level of the lesion.
As the spinal cord compression progresses, it eventually leads to bladder
and bowel dysfunction.
Ventrally situated tumors can involve the anterior nerve roots on one or
both sides, causing flaccid paresis, e. g., of the hands (when the tumor is
in the cervical region).
As the tumor grows, it compresses the pyramidal tract, causing spastic
paresis of the ipsilateral lower limb at first, and later of both lower limbs.
Traction on the spinal cord due to stretching of the denticulate ligaments
may further damage the pyramidal tract.
If the compressive lesion is anterolateral to the cord, contralateral pain
and temperature sensation may be
affected.
With ventral as with dorsal tumors, progressive spinal cord compression
eventually leads to bladder and bowel dysfunction.
Intradural INTRAmedullary Tumors
Can be distinguished from extramedullary
tumors by the following clinical features:
They rarely cause radicular pain,
instead causing atypical
(burning, dull) pain of diffuse localization.
Dissociated sensory deficits can be an early finding.
Bladder and bowel dysfunction appear early in the course of
tumor growth.
The sensory level (upper border of the sensory deficit) may
ascend, because of longitudinal growth of the tumor, while
the sensory level associated with extramedullary tumors
generally remains constant, because of transverse growth.
Muscle atrophy due to involvement of the anterior horns is
more common than with extramedullary tumors.
Spasticity is only rarely as severe as that produced by
extramedullary tumors.
SPINAL CORD TUMORS
Complete or partial spinal cord transection syndrome (including conus
syndrome and cauda equina syndrome) is often caused by a tumor.
Spinal cord tumors are classified into three types, based on their
localization
Extradural tumors (metastasis, lymphoma, plasmacytoma)
Intradural extramedullary tumors (meningioma, neurinoma)
Intradural intramedullary tumors (glioma, ependymoma)
Extradural Neoplasms
tend to grow rapidly, often
producing progressively severe
manifestations of spinal cord
compression: spastic paresis of the parts of the body supplied by the
spinal cord below the level of the lesion, and, later, bladder and bowel
dysfunction.
Pain is a common feature.
Dorsally situated tumors mainly cause sensory disturbances; lateral
compression of the spinal cord can produce BrownSquard syndrome
High cervical tumors
can produce bulbar manifestations aswell as fasciculations and
fibrillations in the affected limb.
Extramedullary tumors are much more common overall than
intramedullary tumors.
Tumors at the level of the foramen magnum (meningioma, neurinoma)
often initially manifest themselves with pain, paresthesia, and
hypesthesia in the C2 region (occipital and great auricular nerves). They
can also cause weakness of the sternocleidomastoid and trapezius
muscles (accessory nerve).
Intradural EXTRAmedullary Tumors
Most commonly arise from the vicinity ofthe
posterior roots
They initially produce radicular pain and
paresthesiae.
Later, as they grow, they cause increasing compression of the posterior
roots and the spinal cord, first the posterior columns and then the
pyramidal tract in the lateral funiculus.
The result is a progressively severe spastic paresis of the lower limb, and
paresthesiae (particularly cold paresthesiae) in both lower limbs,
accompanied by a disturbance of both epicritic and proprioceptive
sensation, at first ipsilaterally and then bilaterally.
The sensory disturbance usually ascends from caudal to cranial until it
reaches the level of the lesion.
Dumbbell tumors (or hourglass tumors)
So called because of their unique anatomical configuration
These are mostly neurinomas that arise in the intervertebral foramen
and then grow in two directions: into the spinal canal and outward into
the paravertebral space.
They compress the spinal cord laterally, eventually producing a partial or
complete BrownSquard syndrome.
Ut In Omnibus Glorificetur Deus
Page 7
princessczaronne
Anda mungkin juga menyukai
- Diseases of The Spinal CordDokumen89 halamanDiseases of The Spinal CordLolla SinwarBelum ada peringkat
- UMass Medical School Mind Brain Behavior 1 Spinal Cord Atlas OverviewDokumen11 halamanUMass Medical School Mind Brain Behavior 1 Spinal Cord Atlas Overviewnon_zense100% (1)
- 05 Cardiovascular System PhysiologyDokumen34 halaman05 Cardiovascular System PhysiologyKaye Alyssa EnriquezBelum ada peringkat
- Nerve of The Lower Limb Edited LagiDokumen159 halamanNerve of The Lower Limb Edited Lagifathizu100% (1)
- Peripheral Nerve Injuries Classification and TreatmentDokumen85 halamanPeripheral Nerve Injuries Classification and TreatmentSyed Abudaheer100% (3)
- Anatomy of The SpineDokumen83 halamanAnatomy of The SpineUkhti Nur Zannah83% (6)
- Head, Neck, Limbs OINADokumen17 halamanHead, Neck, Limbs OINAFrancis HenaresBelum ada peringkat
- Muscle Origin Insertion Innervation Action: (Branch of The Brachial Plexus)Dokumen58 halamanMuscle Origin Insertion Innervation Action: (Branch of The Brachial Plexus)sdfs sdfdBelum ada peringkat
- Cranial Neuropathies Guide: Electrodiagnosis and ManagementDokumen74 halamanCranial Neuropathies Guide: Electrodiagnosis and ManagementKevin Woodard100% (1)
- Pain Modulation MechanismsDokumen10 halamanPain Modulation Mechanismssmartie_chaiBelum ada peringkat
- Blood Suppply of Lower LimbDokumen8 halamanBlood Suppply of Lower LimbCamille Magdirila100% (1)
- Anatomy of Spinal CordDokumen47 halamanAnatomy of Spinal CordmayseeBelum ada peringkat
- Anatomy Exam 1 Review - Muscles of the Back, Shoulder, Arm, Forearm & HandDokumen27 halamanAnatomy Exam 1 Review - Muscles of the Back, Shoulder, Arm, Forearm & Handgdubs215Belum ada peringkat
- Posterior Triangle of Neck Anatomy and Clinical ApplicationsDokumen34 halamanPosterior Triangle of Neck Anatomy and Clinical ApplicationssnehalkmBelum ada peringkat
- Cranial Nerve PathwaysDokumen9 halamanCranial Nerve PathwaysbahahahahBelum ada peringkat
- Lumbar and Sacral PlexusDokumen30 halamanLumbar and Sacral PlexusIndah YoulpiBelum ada peringkat
- Internal CapsuleDokumen25 halamanInternal CapsuleMadan KumarBelum ada peringkat
- (K33) Cranial and Spinal NerveDokumen68 halaman(K33) Cranial and Spinal NerveCut Putri Astritd Adelina100% (1)
- Anatomy 1 - Sensory PathwaysDokumen8 halamanAnatomy 1 - Sensory PathwaysAnthony BrownBelum ada peringkat
- Muscles OinaDokumen3 halamanMuscles Oinageldevera100% (1)
- Anatomy and Physiology Notes For Exam 3Dokumen58 halamanAnatomy and Physiology Notes For Exam 3mike921gold100% (2)
- Cerebrum Sulci and Gyri and Circle of WillisDokumen53 halamanCerebrum Sulci and Gyri and Circle of Willisgandhiayu100% (1)
- The Axilla: Norah AlmudawiDokumen14 halamanThe Axilla: Norah AlmudawiF-med440 imamBelum ada peringkat
- Cerebral Palsy AnatomyDokumen5 halamanCerebral Palsy AnatomyIoana irimiaBelum ada peringkat
- DermatomesDokumen12 halamanDermatomesOpe AjaoBelum ada peringkat
- Joints of Lower Limb 2017Dokumen77 halamanJoints of Lower Limb 2017yasrul izadBelum ada peringkat
- NeuroanatomyDokumen72 halamanNeuroanatomyYasar SabirBelum ada peringkat
- The Abdomen: Anatomy and RegionsDokumen10 halamanThe Abdomen: Anatomy and RegionsSiva ShanmugamBelum ada peringkat
- Anatomy of The Shoulder Girdle and Scapulohumeral RhythmDokumen30 halamanAnatomy of The Shoulder Girdle and Scapulohumeral RhythmthwisemanBelum ada peringkat
- Muscles of the Scapula and ShoulderDokumen6 halamanMuscles of the Scapula and ShoulderAndika Anjani AgustinBelum ada peringkat
- Vertebral Arteries, and Their Divisions. Arteries Fuse To Form The Basilar ArteryDokumen6 halamanVertebral Arteries, and Their Divisions. Arteries Fuse To Form The Basilar Arterymurali_bharadwazBelum ada peringkat
- Neuro Anatomy: Ventricular System, Cerebrospinal Fluid and MeningesDokumen13 halamanNeuro Anatomy: Ventricular System, Cerebrospinal Fluid and MeningesNexie100% (1)
- Cranial Nerves Functional ComponentsDokumen7 halamanCranial Nerves Functional ComponentsCoy EnBelum ada peringkat
- The Cardiovascular System: Elaine N. MariebDokumen151 halamanThe Cardiovascular System: Elaine N. Mariebwhiskers qtBelum ada peringkat
- Muscles of The Upper LimbDokumen17 halamanMuscles of The Upper LimbJhanelle S. Dixon-LairdBelum ada peringkat
- Blue Boxes Lower LimbDokumen4 halamanBlue Boxes Lower LimbZllison Mae Teodoro MangabatBelum ada peringkat
- Higher Center - Dr. BarbonDokumen5 halamanHigher Center - Dr. BarbonMelissa SalayogBelum ada peringkat
- Muscle Innervation Chart IIDokumen7 halamanMuscle Innervation Chart IIkimsue9448Belum ada peringkat
- Peripheral Nerve Injury: Relevant Anatomy: Peripheral Neuroanatomy andDokumen7 halamanPeripheral Nerve Injury: Relevant Anatomy: Peripheral Neuroanatomy andJulia SalvioBelum ada peringkat
- The descending pathways that control motor activityDokumen2 halamanThe descending pathways that control motor activityalmastar officeBelum ada peringkat
- Anatomy of Lung, Pleura, Surface MarkingDokumen22 halamanAnatomy of Lung, Pleura, Surface MarkingSandhya SureshBelum ada peringkat
- Upper Limb: Pectoral RegionDokumen13 halamanUpper Limb: Pectoral RegionMariam Alavidze0% (1)
- Lower Limb: Front and Medial Aspect of ThighDokumen8 halamanLower Limb: Front and Medial Aspect of ThighErnie G. Bautista II, RN, MDBelum ada peringkat
- Anatomy of PelvisDokumen40 halamanAnatomy of PelvisGovGeet100% (1)
- Anatomy MnemonicsDokumen2 halamanAnatomy MnemonicsPia Boni0% (1)
- Anatomy of Upper LimbDokumen112 halamanAnatomy of Upper LimbUzma KhanBelum ada peringkat
- The Nervous System: Organization and FunctionsDokumen84 halamanThe Nervous System: Organization and FunctionsAman SharmaBelum ada peringkat
- Muscle Tables of The Upper Extremities From Netter'sDokumen4 halamanMuscle Tables of The Upper Extremities From Netter'sJemarey de RamaBelum ada peringkat
- Dural Venous SinusesDokumen31 halamanDural Venous Sinusesveegeer100% (1)
- Neurology ConferenceDokumen59 halamanNeurology ConferencePGHC100% (4)
- Brain ventricles: cavities within the brainDokumen23 halamanBrain ventricles: cavities within the brainAndrei Scripcaru100% (1)
- Chapter 13: Spinal Cord and Spinal NervesDokumen6 halamanChapter 13: Spinal Cord and Spinal NervesthwisemanBelum ada peringkat
- Yochum and Rowe - Cap 2 PDFDokumen119 halamanYochum and Rowe - Cap 2 PDFRICARDO LOPEZ FLORESBelum ada peringkat
- Biomechanics of Peripheral and Spinal Nerve RootsDokumen86 halamanBiomechanics of Peripheral and Spinal Nerve RootsJawad HassanBelum ada peringkat
- Cardiology: Anatomy of the Heart and MediastinumDokumen13 halamanCardiology: Anatomy of the Heart and MediastinumJennifer SteffiBelum ada peringkat
- Spinal Cord Injury Complications ExplainedDokumen37 halamanSpinal Cord Injury Complications Explainedlim sjBelum ada peringkat
- 19 Spinal CordDokumen8 halaman19 Spinal Cordkarar AhmedBelum ada peringkat
- Neuro ADokumen30 halamanNeuro Akazeem100% (1)
- Spinal Cord Disease by GadisaDokumen128 halamanSpinal Cord Disease by GadisaGadisa DejeneBelum ada peringkat
- ParaplegiaDokumen51 halamanParaplegiaChuah Wei HongBelum ada peringkat
- Chap 8 Prenatal CareDokumen9 halamanChap 8 Prenatal CareRemelou Garchitorena AlfelorBelum ada peringkat
- Trans Congenital MalformationsDokumen10 halamanTrans Congenital MalformationsRemelou Garchitorena AlfelorBelum ada peringkat
- Chapter 3 Congenital Genitourinary AbnormalitiesDokumen4 halamanChapter 3 Congenital Genitourinary AbnormalitiesRemelou Garchitorena AlfelorBelum ada peringkat
- Chapter 2 Maternal AnatomyDokumen9 halamanChapter 2 Maternal AnatomyRemelou Garchitorena Alfelor100% (1)
- BRAIN AND SPINAL CORD TUMORS Table PDFDokumen4 halamanBRAIN AND SPINAL CORD TUMORS Table PDFRemelou Garchitorena Alfelor100% (1)
- PLE Review OBGYN Chap 1 Overview of ObstetricsDokumen2 halamanPLE Review OBGYN Chap 1 Overview of ObstetricsRemelou Garchitorena Alfelor100% (1)
- CASE REPORT ON Bilateral Ectopic PregnancyDokumen29 halamanCASE REPORT ON Bilateral Ectopic PregnancyRemelou Garchitorena AlfelorBelum ada peringkat
- Chronic Kidney Disease in PregnancyDokumen64 halamanChronic Kidney Disease in PregnancyRemelou Garchitorena AlfelorBelum ada peringkat
- Eclampsia in Pediatric PatientDokumen50 halamanEclampsia in Pediatric PatientRemelou Garchitorena AlfelorBelum ada peringkat
- OB Williams Chap 2 Maternal PhysiologyDokumen9 halamanOB Williams Chap 2 Maternal PhysiologyRem Alfelor100% (2)
- PLE Pathology Cell Injury, Cell Death, and AdaptationsDokumen10 halamanPLE Pathology Cell Injury, Cell Death, and AdaptationsRemelou Garchitorena AlfelorBelum ada peringkat
- Hydrocephalus and Anomalies of The CNSDokumen26 halamanHydrocephalus and Anomalies of The CNSRemelou Garchitorena AlfelorBelum ada peringkat
- PLE Reviewer Pathology Inflammation and RepairDokumen15 halamanPLE Reviewer Pathology Inflammation and RepairRemelou Garchitorena AlfelorBelum ada peringkat
- PLE Reviewer Pathology Inflammation and RepairDokumen15 halamanPLE Reviewer Pathology Inflammation and RepairRemelou Garchitorena AlfelorBelum ada peringkat
- OB Williams Chap 2 Maternal AnatomyDokumen7 halamanOB Williams Chap 2 Maternal AnatomyRem Alfelor0% (1)
- Basic Investigation of An Infertile CoupleDokumen53 halamanBasic Investigation of An Infertile CoupleRemelou Garchitorena AlfelorBelum ada peringkat
- Traumatic Brain Injury: Almario G. Jabson MD Section of Neurosurgery Asian Hospital and Medical CenterDokumen38 halamanTraumatic Brain Injury: Almario G. Jabson MD Section of Neurosurgery Asian Hospital and Medical CenterRemelou Garchitorena AlfelorBelum ada peringkat
- Headacheseizures Drterencio TRANSDokumen7 halamanHeadacheseizures Drterencio TRANSRemelou Garchitorena AlfelorBelum ada peringkat
- 10 Medicinal Plants Approved by The DOHDokumen4 halaman10 Medicinal Plants Approved by The DOHAlyssa Jane Gaitan LauBelum ada peringkat
- Brain TumorsDokumen21 halamanBrain TumorsRemelou Garchitorena AlfelorBelum ada peringkat
- Childhood Stroke TransDokumen9 halamanChildhood Stroke TransRemelou Garchitorena AlfelorBelum ada peringkat
- Anemia, Bleeding, ThrombosisDokumen40 halamanAnemia, Bleeding, ThrombosisRemelou Garchitorena AlfelorBelum ada peringkat
- Eac HemaDokumen150 halamanEac HemaRemelou Garchitorena AlfelorBelum ada peringkat
- The MediastinumDokumen61 halamanThe MediastinumRemelou Garchitorena AlfelorBelum ada peringkat
- PartogramDokumen31 halamanPartogramRemelou Garchitorena AlfelorBelum ada peringkat
- RM Name RM Name RM Name RM Name RM Name: Rem AlfelorDokumen1 halamanRM Name RM Name RM Name RM Name RM Name: Rem AlfelorRemelou Garchitorena AlfelorBelum ada peringkat
- History and Pe Sheet ExcelDokumen12 halamanHistory and Pe Sheet ExcelRemelou Garchitorena AlfelorBelum ada peringkat
- Name:: Admitting Diagnosis: Live BabyDokumen2 halamanName:: Admitting Diagnosis: Live BabyRemelou Garchitorena AlfelorBelum ada peringkat
- Clerk - S CensusDokumen2 halamanClerk - S CensusRemelou Garchitorena AlfelorBelum ada peringkat
- Neurosurgey MCQ Collection Part IDokumen35 halamanNeurosurgey MCQ Collection Part IMohammed Ali Aldhahir88% (8)
- PLAB 1700 MCQs Dr. Khalid - S Explanation of 1700 MCQDokumen680 halamanPLAB 1700 MCQs Dr. Khalid - S Explanation of 1700 MCQguzelnor100% (35)
- Dr. Khalid - S Explanation of 1700 MCQ1Dokumen683 halamanDr. Khalid - S Explanation of 1700 MCQ1heba100% (1)
- Brown Sequard SyndromeDokumen20 halamanBrown Sequard SyndromePutu Ariani100% (4)
- Spinal Cord Lesion SymptomsDokumen51 halamanSpinal Cord Lesion SymptomsShirley HernandezBelum ada peringkat
- Spinal Cord InjuriesDokumen51 halamanSpinal Cord Injurieswanglee2000Belum ada peringkat
- Dr. Khalid - S Explanation of 1700 MCQDokumen670 halamanDr. Khalid - S Explanation of 1700 MCQVicky Waran Raj100% (1)
- NEUROSCIENCE SYNOPSISDokumen38 halamanNEUROSCIENCE SYNOPSISJong PetchinBelum ada peringkat
- External & Internal Features of Spinal CordDokumen77 halamanExternal & Internal Features of Spinal CordPatricia Hariramani100% (2)
- Neuro SurgeryDokumen14 halamanNeuro Surgeryapi-3840195100% (4)
- Neurologic Disorders - NCM 102 LecturesDokumen12 halamanNeurologic Disorders - NCM 102 LecturesBernard100% (4)
- UntitledDokumen544 halamanUntitledyenaxoBelum ada peringkat
- Term 2 Fall 2018Dokumen90 halamanTerm 2 Fall 2018Artemio ZavalaBelum ada peringkat
- APNC 520 Exam 10 Study Guide Musculoskeletal DisordersDokumen15 halamanAPNC 520 Exam 10 Study Guide Musculoskeletal DisordersMariaBelum ada peringkat
- Spinal Cord Injuries Anatomy & Pathophysiology: JckingDokumen51 halamanSpinal Cord Injuries Anatomy & Pathophysiology: JckingSatyaRandyBelum ada peringkat
- Acute Treatment of Patients With SpinalDokumen76 halamanAcute Treatment of Patients With SpinalAzmi FarhadiBelum ada peringkat
- Spinal Injury1 2 PPT PDFDokumen60 halamanSpinal Injury1 2 PPT PDFIqra IftikharBelum ada peringkat
- 1700 Questions Not in PLABABLEDokumen131 halaman1700 Questions Not in PLABABLEDaniah Marwan Dawood DAWOODBelum ada peringkat
- Anatomic Localization of Neurological SymptomsDokumen9 halamanAnatomic Localization of Neurological SymptomsTizazu BayihBelum ada peringkat
- Orthopaedic Emergencies GuideDokumen94 halamanOrthopaedic Emergencies GuideZenith100% (1)
- Brown-Séquard Syndrome: Causes and Symptoms of Spinal Cord Hemisection InjuryDokumen4 halamanBrown-Séquard Syndrome: Causes and Symptoms of Spinal Cord Hemisection InjuryDKABelum ada peringkat
- Dr. Ashari Bahar, M.Kes, SP.S, FINS Department of Neurology University of Hasanuddin Makassar 2014Dokumen64 halamanDr. Ashari Bahar, M.Kes, SP.S, FINS Department of Neurology University of Hasanuddin Makassar 2014LIEBERKHUNBelum ada peringkat
- Anatomy and Localization of Spinal Cord Disorders - UpToDate PDFDokumen29 halamanAnatomy and Localization of Spinal Cord Disorders - UpToDate PDFAffan ElahiBelum ada peringkat
- Pathophysiology of Spinal Cord Injury ExplainedDokumen5 halamanPathophysiology of Spinal Cord Injury ExplainedUmar FarooqBelum ada peringkat
- Anatomy of The Spinal CordDokumen50 halamanAnatomy of The Spinal CordAlwi Qatsir AlyaBelum ada peringkat
- Spinal Cord Lesion Learning ModuleDokumen37 halamanSpinal Cord Lesion Learning Moduleเกมกวี MedicalStudentBelum ada peringkat
- Neuroscience FK UPH 2014: Multiple Choice QuestionsDokumen33 halamanNeuroscience FK UPH 2014: Multiple Choice QuestionsSanzuiBelum ada peringkat
- Spinal Cord Q A AnswersDokumen10 halamanSpinal Cord Q A AnswersAlessa Mikkah BaltazarBelum ada peringkat
- Spine Emergencies: Spinal Cord Injury (SCI) - The BasicsDokumen67 halamanSpine Emergencies: Spinal Cord Injury (SCI) - The Basicsditya_madridistasBelum ada peringkat
- Myelopathy: Dr. Astra Dea Simanungkalit, SpsDokumen24 halamanMyelopathy: Dr. Astra Dea Simanungkalit, SpspppkkkBelum ada peringkat