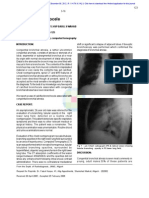
Section II - Chest Radiology: Figure 1A
Diunggah oleh
Haluk AlibazogluJudul Asli
Hak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Section II - Chest Radiology: Figure 1A
Diunggah oleh
Haluk AlibazogluHak Cipta:
Format Tersedia
Section II Chest Radiology
Figure 1A
32. You are shown a PA chest radiograph and CT image (Figures 1A and 1B) from a 51-year-old man with shortness of breath. What is the MOST LIKELY diagnosis? A. B. C. D. Pulmonary alveolar proteinosis Cardiogenic pulmonary edema Idiopathic pulmonary fibrosis Pneumocystis carinii pneumonia
Diagnostic In-Training Exam 2006
Section II Chest Radiology
Figure 1B
American College of Radiology
Section II Chest Radiology
Question #32 Findings: Chest radiograph demonstrates bilateral perihilar opacities. High resolution CT scan demonstrates bilateral thin walled cysts, ground glass and reticular opacities Rationales: A. Incorrect. The most common radiographic manifestation of pulmonary alveolar proteinosis is ground glass and air space opacities which are located in a perihilar distribution such as in this case. The presence of ground glass opacities on the CT scan is consistent with pulmonary alveolar proteinosis. However, septal thickening is not prominent. The combination of ground glass opacities and septal thickening is sometimes referred to crazy paving, an appearance most commonly seen in pulmonary alveolar proteinosis. The CT also demonstrates the presence of multiple relatively thin walled cysts. Such cysts are not a feature of pulmonary alveolar proteinosis. B. Incorrect. Although the standard radiograph is somewhat suggestive of the butterfly or bats wing pattern identified in cardiogenic pulmonary edema, the heart is not enlarged and there is no evidence of Kerley B lines or pleural effusions. Multiple thin walled cysts are not a feature of congestive heart failure. C. Incorrect. IPF occurs in patients between 50 and 70 years old. Radiographic findings include reticular opacities in the peripheral distribution at the lung bases. Thus, the presence of perihilar disease in our case along with absence of disease in the subpleural basilar location lead us away from the diagnosis. D. Correct. In patients with PCP, the chest radiograph classically demonstrates bilateral often perihilar reticular and ground glass opacification which may eventually become confluent and produce air space consolidation within several days. Cysts are visible on chest radiographs in 10% of patients although they are appreciated far more commonly on HRCT scans (33%). Cysts may occur in the acute or post infective period and range in number, size, shape and distribution. They are commonly multiple and have a predilection for the upper lobes. Spontaneous pneumothorax may be a feature of PCP infection and occurs in approximately 35% of patients with cysts.
Diagnostic In-Training Exam 2006
Section II Chest Radiology
Figure 2A
33. You are shown two images from a high-resolution CT (Figures 2A and 2B) of the chest of a 40year-old female smoker with a 1-year history of increasing shortness of breath. What is the MOST LIKELY diagnosis? A. B. C. D. Centrilobular emphysema Lymphangioleiomyomatosis Langerhans cell histiocytosis Lymphocytic interstitial pneumonia
American College of Radiology
Section II Chest Radiology
Figure 2B
Diagnostic In-Training Exam 2006
Section II Chest Radiology
Question #33 Findings: Diffuse cystic lung disease. Lungs are uniformly involved with no evidence of architectural distortion. Rationales: A. Incorrect. Centrilobular emphysema which occurs in smokers is recognized by the presence of multiple lucencies which are predominant in the upper lobes. Characteristically these areas of centrilobular emphysema do not have well defined walls and therefore can be differentiated from cysts. Upper lobe predominance is a key feature and differs from the test case in which there is diffuse involvement. B. Correct. Lymphangioleiomyomatosis. This disease occurs in young to middle-aged women of reproductive age. It is characterized by the presence of cysts with well-defined thin walls measuring 1-2 mm in diameter. The distribution is usually diffuse and other features of interstitial lung disease or fibrosis are notably absent, i.e. reticulation, small nodules, honeycombing and traction bronchiectasis. There is no evidence of architectural distortion. C. Incorrect. Langerhans cell histiocytosis does occur in smokers but is characterized by a number of different features. Nodules up to 1 cm in diameter are common. These nodules frequently cavitate and in the end state of the disease a cystic pattern can be noted. However, a purely cystic pattern is extremely unusual. Upper lobe involvement predominates, and the bases, particularly the costophrenic angles are free of disease, a feature which is not present in the test case. D. Incorrect. CT features of lymphoid interstitial pneumonia include ground glass attenuation, centrilobular and subpleural lung nodules with thickening of the interlobular septa and peribronchovascular interstitium. Perivascular cysts are seen in a minority of cases. Most of these CT features are not present in the test case. The cysts are diffuse and not perivascular in location.
American College of Radiology
Section II Chest Radiology
Figure 3A
Figure 3B
7 American College of Radiology
Section II Chest Radiology
Figure 3C
34. You are shown three CT images (Figures 3A, 3B, and 3C) of a 59-year-old man with cough and stridor. What is the MOST LIKELY diagnosis? A. B. C. D. Squamous cell papilloma Carcinoid Adenoid cystic carcinoma Tracheobronchopathia osteochondroplastica
Diagnostic In-Training Exam 2006
Section II Chest Radiology
Question #34 Findings: Irregular soft tissue mass with diffuse infiltration of the tracheal wall extending into the bronchial walls of the right lung (better seen on lung windows). This irregular mass is associated with lymphadenopathy and infiltration of adjacent mediastinal fat. Rationales: A. Incorrect. The most common benign tracheal tumor, this lesion usually manifests as a smooth, wellcircumscribed, soft tissue lesion measuring less than 2 cm. This would not be an appropriate choice for this irregular mass with extension along the tracheobronchial tree with lymphadenopathy. B. Incorrect. These also tend to be well-defined, smooth, round lesions. Carcinoid tumors arise from neuroendocrine cells and may calcify. They may enhance vigorously with intravenous contrast. The lack of enhancement and diffuse infiltration of the tracheobronchial walls make carcinoid tumor highly unlikely. C. Correct. Adenoid cystic tumors represent the most common salivary gland tumor of the trachea. These lesions tend to grow slowly and spread submucosally. Formerly known as cylindromas because of their tendency to create castes of the tracheal tree, adenoid cystic carcinomas have been reclassified so as not to be confused with benign disease. Treatment is surgical resection which can be challenging because of this tumors tendency to spread perineurally and escape radiologic detection. D. Incorrect. Though the imaging might suggest an inflammatory or infectious tracheal process because of the long-segment of airway involvement, tracheobronchopathia osteochondroplastica (TOP) would not be a likely diagnosis here. The lack of calcification and preferential involvement of the posterior membrane would not allow for TOP to be the preferred diagnosis.
American College of Radiology
Section II Chest Radiology
Figure 4
35. You are shown a CT image (Figure 4) of a 63-year-old man who underwent heart transplantation for ischemic cardiomyopathy two years ago. What is the MOST LIKELY diagnosis? A. B. C. D. Bronchiolitis obliterans Post-transplant lymphoproliferative disease Cryptogenic organizing pneumonia Bronchogenic carcinoma
10
American College of Radiology
Section II Chest Radiology
Question #35 Rationales: A. Incorrect. More commonly seen after lung transplantation, bronchiolitis obliterans usually is radiographically occult. When it is seen, it may be seen as areas of air-trapping or mosaic attenuation. Other reported findings include bronchiectasis and septal line thickening. Solitary nodule is not a finding of bronchiolitis obliterans. B. Incorrect. Post-transplant lymphoproliferative disease (PTLD) (after infection) is one of the most common explanations for a solitary pulmonary nodule in the post-transplanted patient. The imaging features include one or more smooth nodules or areas of consolidation with air bronchograms. A single, spiculated nodule would be an unusual manifestation of PTLD. C. Incorrect. Cryptogenic organizing pneumonia (CPO) is another finding that may be encountered in the post-transplant patient. COP may present with peripheral consolidations (similar to chronic eosinophilic pneumonia) or may present in a nodular form. The nodular form tends to have air bronchograms. A solitary nodule with spiculation would be highly unlikely for COP. In fact, a biopsy of this nodule would likely be repeated if COP was the pathologic diagnosis, in order to exclude inadequate sampling as biopsy of the area adjacent to a neoplasm will result in a pathologic diagnosis of COP. D. Correct. As transplant patients are living longer, it has become well-accepted that transplant immunosuppression results in an increased risk of solid-organ tumors, especially in smokers. In this patient, smoking had contributed to his ischemic cardiomyopathy. Radiologic features of these neoplasms are similar to the features in a non-transplant patient. If this CT were reviewed without the transplant history, bronchogenic neoplasm would lead the differential diagnosis. This lesion was biopsied and this suspicion was confirmed.
Diagnostic In-Training Exam 2006
11
Section II Chest Radiology
Figure 5A
Figure 5B
36. You are shown a CT image (Figure 5A) and two images from an F-18 FDG (fluorodeoxyglucose) PET scan (Figure 5B) of a 71-year-old man. What is the MOST LIKELY diagnosis? A. B. C. D. Benign nodule Stage I lung cancer Stage II lung cancer Stage IV lung cancer
12
American College of Radiology
Section II Chest Radiology
Question #36 Findings: A small irregularly marginated uncalcified nodule on CT shows intense activity on FDG PET scan. In addition, there is a large focus of intense activity in the region of the right adrenal gland. Rationales: A. Incorrect. Benign nodules may show uptake on FDG PET scan, but rarely this intense. Benign etiology does not explain adrenal activity. B. Incorrect. Without the adrenal activity, this would be typical of Stage I lung cancer. C. Incorrect. There is no adjacent nodal activity to suggest T1or2 N1 disease.
D. Correct. The adrenal gland is one of the most common sites of metastasis from bronchogenic carcinoma and may be seen in otherwise Stage I disease. This tumor is T1N0M1 or Stage IV.
Diagnostic In-Training Exam 2006
13
Section II Chest Radiology
Figure 6
37. You are shown a PA chest radiograph (Figure 6) of a 54-year-old woman with shortness of breath and cough. What is the MOST LIKELY diagnosis? A. B. C. D. Miliary tuberculosis Pulmonary alveolar microlithiasis Lymphangitic carcinomatosis Idiopathic pulmonary hemosiderosis
14
American College of Radiology
Section II Chest Radiology
Question #37 Rationales: A. Incorrect. Miliary TB represents diffuse hematogenous spread of the tuberculin bacillus throughout the lungs. The radiographic appearance is that of tiny 1-2 mm nodules throughout the lungs. Our case has much more numerous micronodules than seen in miliary TB. B. Correct. Correct. Pulmonary alveolar microlithiasis (PAM) is a rare condition of uncertain etiology. The chest radiograph shows numerous very fine micronodules throughout both lungs, more so in the middle and lower lung zones. The radiographic findings have been described as that of a sand-storm like appearance. Our case has classic features seen in PAM. C. Incorrect. Lymphangitic carcinomatosis is characterized by metastatic tumor involvement of the lymphatic system. The typical chest radiographic findings include reticulonodular or linear opacities, septal lines and mediastinal or hilar adenopathy. These features are absent in our case. D. Incorrect. Idiopathic pulmonary hemosiderosis is a rare disease of unknown etiology. It most commonly occurs in children in their first decade of life. It is seen as diffuse airspace opacities following an episode of acute hemorrhage. As the blood products break down, there is deposition of hemosiderin into the pulmonary interstitium and lymphatics. Thus, the radiographic findings following repeated bouts of bleeding appear as a reticular pattern. These features are absent in our case.
Diagnostic In-Training Exam 2006
15
Section II Chest Radiology
38. For which of the following is obtaining a definitive diagnosis with needle biopsy MOST DIFFICULT? A. Hamartoma B. Healed granuloma C. Lymphoma D. Metastatic carcinoma Question #38 Rationales: A, C and D are Incorrect. B is Correct. Percutaneous needle biopsy is most commonly used to biopsy intrathoracic or parenchymal lesions. Either 22Gauge needles or 20 Gauge core biopsy needles are utilized. Percutaneous needle biopsy is most commonly used to establish a diagnosis of malignancy. The sensitivity for diagnosis of malignancy (primary and metastatic) is about 85 95%. Diagnosis of Lymphoma and Hamartoma is a little more difficult and sensitivity is in the range of 50 65%. However, histologic diagnosis of benign lesions such as granuloma is far more difficult. In general, granulomas that are active can be diagnosed by needle biopsy by demonstrating a positive culture. However, healed granulomas contain necrotic material and far fewer inflammatory cells. Thus, scant cellularity and minimal number of organisms in a healed granuloma result in far fewer definitive diagnoses than Lymphoma, Hamartoma and Metastasis.
16
American College of Radiology
Section II Chest Radiology
39. Which one of the following is MOST frequently involved in fibrosing mediastinitis? A. B. C. D. Pulmonary artery Aorta Left common carotid artery Bronchial artery
Question #39 Rationales: A is Correct. Fibrosing mediastinitis is a rare disorder characterized by chronic inflammation and fibrosis of mediastinal soft tissues. There are many causes of fibrosing mediastinitis. The most frequently implicated process is infection, of which Histoplasma capsulatum is the most common cause. Complications of fibrosis within the mediastinum lead to encasement and compression of mediastinal structures. Those that are particularly involved include superior vena cava, trachea and bronchi, and pulmonary artery and veins. Aorta and great vessel involvement is extremely rare. B, C and D are Incorrect.
Diagnostic In-Training Exam 2006
17
Section II Chest Radiology
40. Concerning inverse square law in chest fluoroscopy, if the patients entrance dose is 20 mGy/min with the source-to-skin distance (SSD) of 65 cm and source-to-image distance (SID) of 90 cm. How much does the entrance dose change if the SID is increased to 120 cm while maintaining similar SSD? A. B. C. D. Increases by a factor of approximately 1.3 Remains unchanged Decreases by a factor of approximately 2 Increases by a factor of approximately 1.8
Question #40 Rationales: A. Incorrect. See correct answer. B. Incorrect. See correct answer. C. Incorrect. See correct answer. D. Correct. According to the inverse square law, if the exposure-rate from a source is X1 at distance d1, the exposure rate X2 at another distance d2 will be X2=X1(d1/d2)2. Therefore, Increasing the SID requires an increased output from the X-ray tube. Using the inverse square law, you have two equations, (Xpatient90/X90)=(d90/d65)2 and (Xpatient120/X120)=(d120/d65)2. A constant dose rate is necessary at the image intensifier at any SID since auto brightness control is being used so X90=X120. So when you plug this into the equations and rearrange, you get (Xpatient120/Xpatient90)=(120/90)2 1.8.
18
American College of Radiology
Section II Chest Radiology
41. A. B. C. D. Which one of the following is MOST LIKELY to be associated with small cell carcinoma? Brachial plexopathy Hypoglycemia Hyponatremia Pupillary constriction
Question #41 Rationales: A, B and D are Incorrect. C is Correct. Small cell carcinoma is a form of lung cancer. It accounts for 15 20% of all lung cancers. It is characterized by rapid growth, early metastasis and extremely poor prognosis. It is associated with paraneoplastic syndromes, including Cushings syndrome and inappropriate ADH secretion. Inappropriate ADH secretion results in hyponatremia. Hypoglycemia, Brachial plexopathy and pupillary constriction are not clinical features of small cell carcinoma. The most common tumor responsible for hypoglycemia in the thorax is Solitary fibrous tumor of the pleura. Brachial plexopathy and pupillary constriction are more likely to occur with superior sulcus tumor.
Diagnostic In-Training Exam 2006
19
Section II Chest Radiology
42. Concerning pulmonary veno-occlusive disease, which of the following are characteristic CT findings? A. B. C. D. Enlarged left atrium and diffuse interstitial edema Enlarged left atrium and normal lung parenchyma Normal-sized left atrium and normal lung parenchyma Normal-sized left atrium and diffuse interstitial edema
Question #42 Rationales: A, B and C are Incorrect. D is Correct. Pulmonary venoocclusive disorder is a rare disorder characterized by obliteration of small pulmonary veins. This leads to pulmonary hypertension. The causes are many and include viral infections, inhaled toxins and immune complex deposition within the lung to name a few. Diagnosis is suggested in a patient with pulmonary hypertension when radiographic features demonstrate enlarged pulmonary arteries, diffuse interstitial edema and small to normal sized left atrium.
20
American College of Radiology
Section II Chest Radiology
43. A. B. C. D. Kerley B lines represent which one of the following? Dilated peripheral pulmonary veins Distended capillaries Distended lymphatics Thickened interlobular septa
Question #43 Rationales: A, B and C are Incorrect. D is Correct. Kerley B lines are short horizontal lines that are visible on chest radiograph adjacent to the costophrenic sulcus. They are approximately 1 to 2 cm long and are noted to extend to the pleural surface. They represent thickened interlobular septa and are visible in patients with lymphangitic carcinomatosis and pulmonary edema.
Diagnostic In-Training Exam 2006
21
Section II Chest Radiology
44. A. B. C. D. Which one of the following injuries is indicated by the dependent viscera sign? Bronchial fracture Diaphragmatic rupture Pulmonary laceration Traumatic aortic tear
Question #44 Rationales: A. Incorrect B. Correct. Tear in the diaphragm results in herniation of viscera (bowel and solid organs) into the thoracic cavity. As the injured diaphragm no longer supports these structures posteriorly, they fall to a dependent position against the posterior ribs. Hence, the dependent viscera sign is observed in patients with diaphragmatic injury when they lie supine for a CT scan. C. Incorrect D. Incorrect
22
American College of Radiology
Section II Chest Radiology
45. A. B. C. D. Which one of the following entities can be expected to cause a pneumothorax? Boerhaaves syndrome Desquamative interstitial pneumonia Metastatic osteogenic sarcoma Ruptured bronchus within 1 cm of the carina
Question #45 Rationales: A. Incorrect. Boerhaaves syndrome represents perforation of esophagus following severe episodes of vomiting. In this instance, pneumomediastinum rather than pneumothorax is the expected consequence. B. Incorrect. Recurrent pneumothorax may be associated with chronic infiltrative lung disease of any cause, but the prevalence is particularly high in two diseases; Langerhans cell histiocytosis (histiocytosis x) and lymphangioleiomyomatosis. Both of these entities are characterized by the presence of multiple lung cysts which may rupture through the visceral pleura causing a complicating pneumothorax. However, pneumothorax may be seen as a complication of the late stages of other types of infiltrative lung diseases that are associated with fibrosis and honeycombing. Desquamative interstitial pneumonia is not characterized by the presence of cysts. High resolution CT frequently demonstrates ground glass and alveolar opacities more marked in the mid and lower lung zones. Fibrosis and honeycombing are not features and the disease responds to steroid therapy. C. Correct. Malignant neoplasms, particularly metastatic sarcoma, are occasional causes of spontaneous pneumothorax. The most common tumor type is metastatic osteogenic sarcoma. The mechanism for the development of pneumothorax is not clear, but it may be related to the presence of cavitation and subsequent rupture into the pleural space. The presence of a spontaneous pneumothorax in a child in the setting of a primary osteogenic sarcoma should prompt a CT examination to search for the presence of metastatic disease. D. Incorrect. Pneumothorax which is unresponsive to chest tube drainage can be a feature of a ruptured bronchus which is sustained following blunt trauma usually in high speed motor vehicle accidents. However, the rupture must occur at a site in the bronchus which is contained within the mediastinal pleura. Thus tears close to the carina produce pneumomediastinum rather than pneumothorax.
Diagnostic In-Training Exam 2006
23
Section II Chest Radiology
46. Concerning cystic fibrosis, which one is TRUE? A. B. C. D. Bronchiectasis is more severe in the lower lobes. Sodium and chloride levels are elevated in the sweat. It is heritable by dominant transmission. The lung volumes are small.
Question #46 Rationales: A. Incorrect. Bronchiectasis-- identified as parallel lines or as ring shadows larger than the accompanying pulmonary arteryusually is widespread on radiographs but tends to affect mainly the upper lobes. B. Correct. True statement. The Sweat Test is one of the ways that diagnosis of Cystic fibrosis is made. C. Incorrect. Cystic fibrosis is a relatively common hereditary disorder of recessive transmission. The disease is the most common lethal genetically transmitted disease among whites with an estimated incidence in this group of 1 per 2,000 to 3,000 live births. D. Incorrect. Hyperinflation is seen in about 80% of adult patients and tends to involve mainly the lower lobes.
24
American College of Radiology
Section II Chest Radiology
47. A. B. C. D. Concerning solitary pulmonary nodules, which one is TRUE? Considered benign if stable for 1 year Defined as a lesion that measures less than 2 cm Metastasis is the most common cause Presence of fat is indicative of benign etiology
Question #47 Rationales: A, B and C are Incorrect. D is correct. Solitary pulmonary nodule is defined as a well circumscribed round or oval lesion measuring less than 3 cm in diameter. About half of the lesion are proven to be benign, about 40% are proven to be primary lung carcinoma and only about 10% are proven to be metastasis. A number of criteria have been described to help differentiate benign from malignant nodules. However, none have proven to be of very specific except presence of fat is suggestive of a benign lesion. Also, benign lesions have a doubling time of less than 1 month or greater than 16 months. Thus, nodules that are stable for over a 2 year period are considered benign.
Diagnostic In-Training Exam 2006
25
Section II Chest Radiology
48. A film cassette spot film is taken of the chest of a supine patient with an under-table tube on a fluoroscopic system. How does the spot film image taken with an under-table fluoroscopy system differ from a typical properly exposed PA chest radiography film performed using an upright Bucky with similar kVp and cassette? A. The spot film will have significantly lower noise. B. The longer exposure time will cause increased cardiac motion blurring for the spot film image. C. A larger difference in image size is seen between anterior and posterior structures in spot film image. D. The spot film yields lower entrance dose to patient. Question #48 Rationales: A. Incorrect. Since both films are properly exposed and are using the same cassette, equivalent number of photons will be absorbed to produce the images, and they should have equivalent levels of noise. B. Incorrect. The exposure time for the spot film should be shorter due to the shorter source-film distance. C. Correct. The shorter source-to-image distance with the fluoroscopic system will result in a wider beam divergence, and a larger difference in image magnification of structures on the posterior side of the patient versus the anterior side. D. Incorrect. Because of the shorter source-to-image distance, the entrance dose for spot film will be greater than chest radiography.
26
American College of Radiology
Section II Chest Radiology
49. A. B. C. D. Which finding is characteristic of sarcoidosis? Anterior mediastinal adenopathy Basilar reticular opacities Peribronchovascular nodules Random nodules
Question #49 Rationales: A. Incorrect. Bilateral hilar and right paratracheal adenopathy is common. Anterior mediastinal adenopathy / mass usually signify Lymphoma or Thymoma. B. Incorrect. The disease in sarcoidosis tends to be predominantly upper lobe in distribution. C. Correct. Peribronchovascular or perilymphatic nodules are typically seen in patients with sarcoidosis. Nodules in sarcoidosis are also noted in the subpleural location and along the interlobular septa. D. Incorrect. Random nodules usually represent hematogenous metastasis or miliary infection, such as Tuberculosis.
Diagnostic In-Training Exam 2006
27
Section II Chest Radiology
50. A. B. C. D. Concerning the left superior vena cava, how does it communicate with the heart? Enters the left atrium via the pulmonary veins Enters the left atrium via the coronary sinus Enters the right atrium via the sinus of Valsalva Enters the right atrium via the coronary sinus
Question #50 Rationales: A. Incorrect. B. Incorrect. The left superior vena cava drains into the right atrium via the coronary sinus. C. Incorrect. The sinus of Valsalva is at the root of the aorta. D. Correct. The left superior vena cava (SVC) drains into the right atrium via the coronary sinus. A left-sided SVC, a normal anatomic variant, is found in 0.3% of normal individuals. 80% of such individuals also have a right-sided SVC and 60% have a left BCV connecting to the right and left SVCs.
28
American College of Radiology
Section II Chest Radiology
51. A. B. C. D. Concerning eosinophilic lung disease, which one is TRUE? Blood eosinophilia is necessary to make the diagnosis. It can be caused by drugs, such as sulfonamides. Chronic eosinophilic pneumonia is characterized by central opacities. Lofflers syndrome is characterized by peripheral opacities.
Question #51 Rationales: B & D ARE BOTH CORRECT A. Incorrect. Blood eosinophilia is not necessary to make the diagnosis of eosinophilic lung disease. The term pulmonary eosinophilia, synonymous with pulmonary infiltration with eosinophilia, describes a group of diseases in which blood and/or tissue eosinophilia affects major airways and lung parenchyma. B. Correct. True statement. Eosinophilic lung diseases are a group of pulmonary disorders that are characterized by abundant eosinophils in the pulmonary opacities. They are classified into groups with and without a specific cause. The specific causes include drugs, such as sulfonamides, parasites, and fungi. C. Incorrect. Chronic eosinophilic pneumonia has classic radiographic and chest CT findings of peripheral, nonsegmental, homogenous alveolar opacities, often with air bronchograms. D. Correct. Lofflers syndrome is characterized by blood eosinophilia, absence of or mild symptoms and signs (cough, fever, and dyspnea), one or more nonsegmental mixed interstitial and alveolar pulmonary opacities that are transitory or migratory, and spontaneous clearing of the opacities.
Diagnostic In-Training Exam 2006
29
Section II Chest Radiology
52. Which one of the following is characteristic of acute pulmonary emboli on CT angiography? A. Thickened, narrowed pulmonary arteries B. Pulmonary artery webs C. Central filling defect within the pulmonary arteries D. Mosaic perfusion of the lung parenchyma Question #52 Rationales: A. Incorrect. B. Incorrect. Webs are seen with chronic emboli and represent residual thrombus or scarring in a recanalized vessel. Occasionally, these may calcify. They are much easier to see on angiography or coronal reconstructions of pulmonary embolism protocol CT. C. Correct. The railroad track sign or doughnut sign (with the clot centrally and contrast peripherally) is a direct sign of acute pulmonary embolus on CT. Chronic pulmonary embolus tends to be eccentric. Occasionally, acute pulmonary embolus may be eccentric. The margin with the lumen, in these cases, tends to be convex as compared to chronic pulmonary embolus which has a flat or concave margin to the lumen. D. Incorrect. Mosaic attenuation or perfusion is a finding more commonly seen with chronic emboli. The vessels in the darker regions are attenuated and the darker regions do not demonstrate air-trapping.
30
American College of Radiology
Section II Chest Radiology
53. Which one of the following radiographic features is seen with allergic bronchopulmonary aspergillosis? A. B. C. D. Air crescent sign Central bronchiectasis Halo sign Pleural thickening
Question #53 Rationales: A, C and D are incorrect. B is correct. Allergic bronchopulmonary aspergillosis is a complex hypersensitivity reaction to aspergillus organisms colonizing the bronchial lumen. The inflammatory reaction results in cellular infiltration and release of proteolytic enzymes which produce tissue damage in the bronchial wall. Excessive mucus production leads to mucoid impaction of the airways. The radiographic hallmark is central bronchiectasis. Air-crescent sign, pleural thickening, and halo sign are not features of allergic bronchopulmonary aspergillosis.
Diagnostic In-Training Exam 2006
31
Section II Chest Radiology
54. Which one of the following conditions demonstrates air-trapping on expiratory high resolution CT scan? A. B. C. D. Churg-Strauss syndrome Goodpastures syndrome Scimitar syndrome Swyer-James syndrome
Question #54 Rationales: A. Incorrect. It is a necrotizing vasculitis that is characterized clinically by asthma, fever and eosinophilia. Radiographic manifestation includes bilateral patchy consolidations but not air-trapping. B. Incorrect. It is an autoimmune disorder of unknown etiology that is characterized by repeated episodes of pulmonary hemorrhage. No air-trapping is noted. C. Incorrect. Also known as congenital pulmonary venolobar syndrome. It is a congenital anomaly that consists of hypoplasia of the right lung and the right pulmonary artery. There is anomalous venous drainage of the right lung into systemic venous system, usually below the diaphragm into the inferior vena cava. No air-trapping is noted. D. Correct. The syndrome is believed to be initiated by a viral bronchiolitis in childhood. It is characterized by hyperlucent lobe or lung. The hyperlucency is due to bronchiolar obliteration and this results in air-trapping on expiratory CT scan.
32
American College of Radiology
Section II Chest Radiology
55. Which one of the following mediastinal landmarks is likely to be obliterated by a bronchogenic cyst? A. B. C. D. Anterior junction line Psterior junction line Azygoesophageal interface Descending aortic interface
Question #55 Rationales: C. Correct. Bronchogenic cysts are congenital lesions that result from an abnormality of budding of the tracheobronchial tree during embryologic development. They are most commonly found in the subcarinal location and thus there presence in this location will cause obliteration of the azygoesophageal interface. Azygoesophageal interface is formed by the interposition of the aerated lung and the lateral wall of the azygous vein and esophagus. A, B and D Incorrect. Anterior and Posterior junction lines are longitudinal opacities that are formed by the close apposition of the visceral and parietal layers of the pleura of both the lungs as they come together anteriorly and posteriorly to the mediastinum. Descending aortic interface is formed by the juxtaposition of the aerated lung and the soft tissue of the left lateral margin of the descending thoracic aorta.
Diagnostic In-Training Exam 2006
33
Section II Chest Radiology
56. A. B. C. D. Concerning asbestosis, which one of the following is an expected manifestation? Increased lung volume Upper lung nodules Bronchiectasis Pleural effusions
Question #56 Rationales: A. Incorrect. Very common in the later stages of asbestosis. B. Incorrect. Upper lung nodules are typical of silicosis and granulomatous disease, not asbestosis. C. Incorrect. This is the most common early manifestation of asbestosis and is best demonstrated by high resolution CT. With time, these progress to a coarse reticular pattern. D. Correct. Pleural plaques and pleural effusions are common findings in asbestosis.
34
American College of Radiology
Section II Chest Radiology
57. A. B. C. D. Which one is MOST likely to cause hoarseness? Anterior mediastinal mass Aorto-pulmonary window mass Right hilar mass Subcarinal mass
Question #57 Rationales: A. Incorrect B. Correct. It is situated between the aortic arch and the left pulmonary artery. The space contains mediastinal fat, ductus ligament, nodes and the left recurrent laryngeal nerve. Thus, mass in this location can involve the left recurrent laryngeal nerve resulting in vocal cord abnormalities, including hoarseness. C. Incorrect D. Incorrect
Diagnostic In-Training Exam 2006
35
Anda mungkin juga menyukai
- Pneumothorax Concept Map: Diagnostic TestsDokumen1 halamanPneumothorax Concept Map: Diagnostic TestsJoshua Villarba80% (5)
- TCCC-MP Test Answer Key 140602Dokumen16 halamanTCCC-MP Test Answer Key 140602samfarmer333100% (2)
- Final Oral Revalida Internal Medicine Compilation 1Dokumen45 halamanFinal Oral Revalida Internal Medicine Compilation 1Joel SaluBelum ada peringkat
- Chest Tube ModuleDokumen37 halamanChest Tube ModuleEdison Reyes100% (1)
- 06 ChestDokumen16 halaman06 ChestANAS ALIBelum ada peringkat
- A Case of Pulmonary Tuberculosis With Multiple Nodules Mimicking Lung MetastasesDokumen4 halamanA Case of Pulmonary Tuberculosis With Multiple Nodules Mimicking Lung MetastasesKusuma IntanBelum ada peringkat
- Bronquiolite DiagnosticoDokumen14 halamanBronquiolite DiagnosticoFrederico PóvoaBelum ada peringkat
- Jurnal Radiologi TBDokumen7 halamanJurnal Radiologi TBrian00019Belum ada peringkat
- SGL5 - HaemoptysisDokumen73 halamanSGL5 - HaemoptysisDarawan MirzaBelum ada peringkat
- Pi Is 00960217166003657Dokumen15 halamanPi Is 00960217166003657Jesicca SBelum ada peringkat
- Pulmonary Pseudotumoral Tuberculosis in An Old Man: A Rare PresentationDokumen3 halamanPulmonary Pseudotumoral Tuberculosis in An Old Man: A Rare PresentationNurhasanahBelum ada peringkat
- Journal Radiologi 3Dokumen14 halamanJournal Radiologi 3WinayNayBelum ada peringkat
- Types of CAMDokumen7 halamanTypes of CAMjojolilimomoBelum ada peringkat
- High Resolution CT of The Lungs: Technique, Indications and FindingsDokumen9 halamanHigh Resolution CT of The Lungs: Technique, Indications and FindingsHari Baskar SBelum ada peringkat
- Approach To Interstitial Lung DiseasesDokumen38 halamanApproach To Interstitial Lung DiseasesmeawchiBelum ada peringkat
- Asthma and Lung MassDokumen4 halamanAsthma and Lung MassAzmachamberAzmacareBelum ada peringkat
- Bronchogenic Malignancy and Metastatic Disease: Hilar MassesDokumen4 halamanBronchogenic Malignancy and Metastatic Disease: Hilar MassesTira SariBelum ada peringkat
- Case 16797Dokumen7 halamanCase 16797eduardoBelum ada peringkat
- Radiology RoundsDokumen30 halamanRadiology RoundsKelum BuddhikaBelum ada peringkat
- Radiological Signs (Shënja Radiologjike) - 1Dokumen122 halamanRadiological Signs (Shënja Radiologjike) - 1Sllavko K. KallfaBelum ada peringkat
- Jurnal Radio Inggris TalDokumen17 halamanJurnal Radio Inggris TalimamattamamiBelum ada peringkat
- An Unusual Presentation of Multiple Cavitated Lung Metastases From Colon CarcinomaDokumen4 halamanAn Unusual Presentation of Multiple Cavitated Lung Metastases From Colon CarcinomaGita AmeliaBelum ada peringkat
- Pneumo Cist IsDokumen6 halamanPneumo Cist IsAlexei RobuBelum ada peringkat
- Jurnal 2Dokumen0 halamanJurnal 2Seftiana SaftariBelum ada peringkat
- Imaging of Solitary and Multiple Pulmonary NodulesDokumen75 halamanImaging of Solitary and Multiple Pulmonary NodulesAnshulVarshneyBelum ada peringkat
- Bronchiolitis A Practical Approach For The General RadiologistDokumen42 halamanBronchiolitis A Practical Approach For The General RadiologistTara NareswariBelum ada peringkat
- MUCORMYCOSISDokumen37 halamanMUCORMYCOSISSK MOMTAZUL KARIMBelum ada peringkat
- Pulmonary Tuberculosis: Parenchymal DiseaseDokumen5 halamanPulmonary Tuberculosis: Parenchymal DiseaseSekar Indah SBelum ada peringkat
- The Solitary Pulmonary NoduleDokumen8 halamanThe Solitary Pulmonary NoduleRafa IsaacBelum ada peringkat
- Esti2012 E-0066Dokumen40 halamanEsti2012 E-0066nistor97Belum ada peringkat
- Lung Cancer in ChildDokumen4 halamanLung Cancer in Childtonirian99Belum ada peringkat
- Articulo 20 de OctubreDokumen6 halamanArticulo 20 de OctubreAlba PalaciosBelum ada peringkat
- Jrcollphyslond146949 0029bDokumen7 halamanJrcollphyslond146949 0029bArun JadhavBelum ada peringkat
- The Radiologic Appearance of Lung Cancer: Review Article Peter B. O'donovan, MDDokumen12 halamanThe Radiologic Appearance of Lung Cancer: Review Article Peter B. O'donovan, MDAdrianus KevinBelum ada peringkat
- Neu Motor AxDokumen6 halamanNeu Motor AxZay SiagBelum ada peringkat
- Interstitial Lung DiseaseDokumen4 halamanInterstitial Lung DiseasedewimarisBelum ada peringkat
- Journal Reading: TuberculosisDokumen44 halamanJournal Reading: Tuberculosisnurza yeyeniBelum ada peringkat
- Solitary Pulmonary Nodule (SPN (Dokumen59 halamanSolitary Pulmonary Nodule (SPN (mahmod omerBelum ada peringkat
- Radiological Signs (Shënja Radiologjike) - 1Dokumen122 halamanRadiological Signs (Shënja Radiologjike) - 1Sllavko K. KallfaBelum ada peringkat
- Tuberculosis: A Benign Impostor: Cher H. Tan Dimitrios P. Kontoyiannis Chitra Viswanathan Revathy B. IyerDokumen7 halamanTuberculosis: A Benign Impostor: Cher H. Tan Dimitrios P. Kontoyiannis Chitra Viswanathan Revathy B. IyerElza Astri SafitriBelum ada peringkat
- Journal ReadingDokumen42 halamanJournal Readingnurza yeyeniBelum ada peringkat
- Letter TO THE Editor: Secondary Organizing Pneumonia After Varicella-Zoster Virus Infection: A Rare AssociationDokumen3 halamanLetter TO THE Editor: Secondary Organizing Pneumonia After Varicella-Zoster Virus Infection: A Rare AssociationfatimiahmastaBelum ada peringkat
- Malignant Mesothelioma ImagingDokumen22 halamanMalignant Mesothelioma ImagingFatya WelinsaBelum ada peringkat
- Adenosquamous Carcinomaof The Lung: Two Cases ReportDokumen5 halamanAdenosquamous Carcinomaof The Lung: Two Cases ReportIJAR JOURNALBelum ada peringkat
- International Journal of Cancer and Clinical ResearchDokumen5 halamanInternational Journal of Cancer and Clinical ResearchDenny SutantoBelum ada peringkat
- Case 1: Recurrent Pneumonia in A 15-Year-Old Girl: Article Figures & Data Info & Metrics CommentsDokumen7 halamanCase 1: Recurrent Pneumonia in A 15-Year-Old Girl: Article Figures & Data Info & Metrics CommentsJoshua MendozaBelum ada peringkat
- TB and Lung CancerDokumen26 halamanTB and Lung CanceraprinaaaBelum ada peringkat
- PDF To WordDokumen17 halamanPDF To Wordanisa ghinaBelum ada peringkat
- The Many Faces of Cryptogenic Organizing Pneumonia (COP)Dokumen7 halamanThe Many Faces of Cryptogenic Organizing Pneumonia (COP)Miguel Angel GarciaBelum ada peringkat
- Kak Rifda Ppds ParuDokumen6 halamanKak Rifda Ppds ParuAsdar Raya RangkutiBelum ada peringkat
- Radiologicalfeaturesofbronchogeniccarcinoma 160608214533Dokumen135 halamanRadiologicalfeaturesofbronchogeniccarcinoma 160608214533Abdi KumalaBelum ada peringkat
- A 56 Year Old Woman With Multiple Pulmonary CystsDokumen8 halamanA 56 Year Old Woman With Multiple Pulmonary CystsAchmad Dodi MeidiantoBelum ada peringkat
- OverviewDokumen2 halamanOverviewAlexa DivaBelum ada peringkat
- SGL6 - CoughDokumen63 halamanSGL6 - CoughDarawan MirzaBelum ada peringkat
- 521 FullDokumen11 halaman521 FulljhordyafsBelum ada peringkat
- Direpub 2063 OnlineDokumen9 halamanDirepub 2063 OnlinephobicmdBelum ada peringkat
- Chest ThesisDokumen6 halamanChest Thesiskcfxiniig100% (1)
- Lung Abscess Bronchiectasis TuberculosisDokumen19 halamanLung Abscess Bronchiectasis Tuberculosisajjju02Belum ada peringkat
- Short Case 9Dokumen192 halamanShort Case 9Dr Gurunandini AcharBelum ada peringkat
- Lesiones Cavitarias - Chest - Sper BuenoDokumen11 halamanLesiones Cavitarias - Chest - Sper BuenoMary CogolloBelum ada peringkat
- Radiology 111Dokumen51 halamanRadiology 111Sherika A. BurgessBelum ada peringkat
- Jurnal TB RadiologiDokumen41 halamanJurnal TB RadiologiDesi AdiyatiBelum ada peringkat
- 11 - Less Common Pulmonary Diseases - Live Session RecordingDokumen21 halaman11 - Less Common Pulmonary Diseases - Live Session RecordingjimmyneumologiaBelum ada peringkat
- Chest X Rays Made EasyDokumen3 halamanChest X Rays Made EasyHaluk AlibazogluBelum ada peringkat
- Cardiac RadiologyDokumen10 halamanCardiac RadiologyHaluk AlibazogluBelum ada peringkat
- ABC of Reading Chest XrayDokumen1 halamanABC of Reading Chest Xraykrisnochura100% (3)
- Websites For Review of RadiologyDokumen1 halamanWebsites For Review of RadiologyHaluk AlibazogluBelum ada peringkat
- Chest X-Ray InterpretationDokumen3 halamanChest X-Ray InterpretationHaluk AlibazogluBelum ada peringkat
- Chest X Ray InterpretationDokumen2 halamanChest X Ray InterpretationHaluk AlibazogluBelum ada peringkat
- Chest X-Ray InterpretationDokumen3 halamanChest X-Ray InterpretationHaluk AlibazogluBelum ada peringkat
- Innovation and Development in Indian HealthcareDokumen29 halamanInnovation and Development in Indian HealthcareSahana BoseBelum ada peringkat
- TechTips FastSpectDokumen2 halamanTechTips FastSpectHaluk AlibazogluBelum ada peringkat
- Cardiac Radiology.Dokumen13 halamanCardiac Radiology.Haluk AlibazogluBelum ada peringkat
- Basic Interpretation of CXRDokumen84 halamanBasic Interpretation of CXRHaluk AlibazogluBelum ada peringkat
- Printer Sony Upd75mdDokumen2 halamanPrinter Sony Upd75mdHaluk AlibazogluBelum ada peringkat
- Medical Surgical Nursing Assignment - 2Dokumen147 halamanMedical Surgical Nursing Assignment - 2Sonali Sengar0% (1)
- pg36-37 of Pneumothorax Case StudyDokumen2 halamanpg36-37 of Pneumothorax Case Studyikemas100% (1)
- NCM 112 Lesson1Dokumen9 halamanNCM 112 Lesson1Trisha LopezBelum ada peringkat
- Atls Spanish POST TESTDokumen12 halamanAtls Spanish POST TESTScribdTranslations100% (1)
- Early and Persistent Hemothorax and PneumothoraxDokumen7 halamanEarly and Persistent Hemothorax and Pneumothoraxtri_budi_20Belum ada peringkat
- The Modified First Updated CapsuleDokumen132 halamanThe Modified First Updated Capsuleyasser.yasser.yaBelum ada peringkat
- TEST BANK Chapter 21Dokumen6 halamanTEST BANK Chapter 21Louise Lorraine TaculodBelum ada peringkat
- PneumothoraxDokumen11 halamanPneumothoraxmrinmayee deshmukhBelum ada peringkat
- Meconium Aspiration Syndrome, Management ofDokumen9 halamanMeconium Aspiration Syndrome, Management ofGinaJaraBelum ada peringkat
- Radiology: Discussion PaperDokumen12 halamanRadiology: Discussion PaperMadhu SowmithaBelum ada peringkat
- Chapter 27: Alterations of Pulmonary Function Power-Kean Et Al: Huether and Mccance'S Understanding Pathophysiology, Second Canadian EditionDokumen13 halamanChapter 27: Alterations of Pulmonary Function Power-Kean Et Al: Huether and Mccance'S Understanding Pathophysiology, Second Canadian EditionmonicaBelum ada peringkat
- Pulmonary Bleb: On This PageDokumen6 halamanPulmonary Bleb: On This PageYaumul RobbiBelum ada peringkat
- Medical Surgical Nursing Review 1Dokumen422 halamanMedical Surgical Nursing Review 1jeshemaBelum ada peringkat
- Pneumothorax, Tension and TraumaticDokumen24 halamanPneumothorax, Tension and TraumaticSatria WibawaBelum ada peringkat
- Kumpulan POMRDokumen26 halamanKumpulan POMRIMN Wiranta PrasetyajiBelum ada peringkat
- Respiratory CytologyDokumen45 halamanRespiratory CytologytheintrovBelum ada peringkat
- MCQ RespiratoryDokumen15 halamanMCQ Respiratoryanaphysioforyou100% (1)
- Basic Interpretation of CXRDokumen84 halamanBasic Interpretation of CXRHaluk AlibazogluBelum ada peringkat
- Procedures ThoracentesisDokumen4 halamanProcedures ThoracentesisPatty MArivel ReinosoBelum ada peringkat
- Year 3 Surgery Posting Sylabbus 2008Dokumen29 halamanYear 3 Surgery Posting Sylabbus 2008davidwee1987Belum ada peringkat
- Surgery TCVS SGD Guide KKDokumen7 halamanSurgery TCVS SGD Guide KKFu Xiao ShanBelum ada peringkat
- Chapter 20 REVIEW OF THORACIC IMAGINGDokumen8 halamanChapter 20 REVIEW OF THORACIC IMAGINGZahra Margrette SchuckBelum ada peringkat
- 10 Respiratory System 2Dokumen120 halaman10 Respiratory System 2rosalyn gaboniBelum ada peringkat
- Hyperbaric Soft Tissue RadionecrosisDokumen13 halamanHyperbaric Soft Tissue Radionecrosisina permata dewiBelum ada peringkat
- ADivP 02 (A) MedDokumen357 halamanADivP 02 (A) MedSamo PecanBelum ada peringkat
- Fundamentals of Chest RadiologyDokumen119 halamanFundamentals of Chest RadiologyAlexandra DîrțuBelum ada peringkat