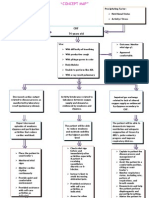
Fluid Volume Excess CRF
Diunggah oleh
Dana Fajardo RezanoHak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Fluid Volume Excess CRF
Diunggah oleh
Dana Fajardo RezanoHak Cipta:
Format Tersedia
Medical Diagnosis: Renal Failure Problem: Fluid Volume Excess RT Decreased Glomerular Filtration Rate and Sodium Retention
Assessment Subjective: (none) Objective: Patient manifested: Edema Hypertension Weight gain Pulmonary congestion (SOB, DOB) Oliguria Distended jugular vein Changes in mental status Patient may manifest: Nursing Diagnosis Fluid Volume Excess R/T decrease Glomerular filtration Rate and sodium retention Scientific Explanation Renal disorder impairs glomerular filtration that resulted to fluid overload. With fluid volume excess, hydrostatic pressure is higher than the usual pushing excess fluids into the interstitial spaces. Since fluids are not reabsorbed at the venous end, fluid volume overloads the lymph system and stays in the interstitial spaces leading the patient to have edema, weight gain, pulmonary congestion and HPN at the same time due to decrease GFR, nephron hyperthrophized leading to decrease ability of the kidney to concentrate urine and impaired excretion of fluid thus leading to Planning Short Term: After 4-8 hours of nursing interventions, patient will demonstrate behaviors to monitor fluid status and reduce recurrence of fluid excess Interventions 1. Establish rapport Rationale 1. To assess precipitating and causative factors. 2. To obtain baseline data 3. To obtain baseline data Long Term: The patient shall have manifested stabilized fluid volume AEB balance I & O, normal VS, stable weight, and free from signs of edema. Evaluation Short Term: The patient shall have demonstrated behaviors to monitor fluid status and reduce recurrence of fluid excess
2. Monitor and record vital signs 3. Assess possible risk factors
Long Term: After 3 days of nursing intervention the patient will manifest stabilize fluid volume AEB balance I & O, normal VS, stable weight, and free from signs of edema.
4. Monitor and record vital signs.
4. To note for presence of nausea and vomiting 5. To prevent fluid overload and monitor intake and output 6. To monitor fluid retention and evaluate degree of excess
5. Assess patients appetite
6. Note amount/rate of fluid intake from all sources
7. Compare current weight gain with admission or previous stated weight
7. For presence of crakles or congestion
www.NursesLabs.com
oliguria/anuria.
8. Auscultate breath sounds 9. Record occurrence of dyspnea 10. Note presence of edema. 11. Measure abdominal girth for changes. 12. Evaluate mentation for confusion and personality changes. 13. Observe skin mucous membrane. 14. Change position of client timely.
8. To evaluate degree of excess 9. To determine fluid retention 10. May indicate increase in fluid retention 11. May indicate cerebral edema.
12. To evaluate degree of fluid excess.
13. To prevent pressure ulcers. 14. To monitor fluid and electrolyte imbalances 15. To lessen fluid retention and overload.
15. Review lab data like BUN, Creatinine, Serum electrolyte. 16. Restrict sodium and fluid intake if indicated
16. To monitor kidney function and fluid
www.NursesLabs.com
17. Record I&O accurately and calculate fluid volume balance 18. Weigh client
retention. 17. Weight gain indicates fluid retention or edema. 18. Weight gain may indicate fluid retention and edema. 19. To conserve energy and lower tissue oxygen demand. 20. To promote wellness.
19. Encourage quiet, restful atmosphere. 20. Promote overall health measure.
www.NursesLabs.com
Anda mungkin juga menyukai
- Fluid Volume ExcessDokumen4 halamanFluid Volume ExcessTamil Villardo100% (2)
- NCP - Fluid RetentionDokumen3 halamanNCP - Fluid RetentionMichelle Teodoro100% (1)
- NCP - Altered Tissue PerfusionDokumen2 halamanNCP - Altered Tissue PerfusionLeigh Kristel Andrion0% (1)
- Actual NCPDokumen3 halamanActual NCPMabz BoholBelum ada peringkat
- Activity Intolerance Related To AmeniaDokumen1 halamanActivity Intolerance Related To AmeniaSiti Syazana Mohamad MogriBelum ada peringkat
- NCP For Risk of Infectiong R/T Indwelling Catheter Post PartumDokumen1 halamanNCP For Risk of Infectiong R/T Indwelling Catheter Post PartumJared Mabulay100% (1)
- Nursing Care Plan: Date/ Time Assessment Nursing Diagnosis Planning Intervention Evaluatio NDokumen2 halamanNursing Care Plan: Date/ Time Assessment Nursing Diagnosis Planning Intervention Evaluatio NnananaBelum ada peringkat
- Fluid Volume Excess NCPDokumen3 halamanFluid Volume Excess NCPAfia TawiahBelum ada peringkat
- Compartment Syndrome NCP (PAIN)Dokumen2 halamanCompartment Syndrome NCP (PAIN)eunica16Belum ada peringkat
- NCP Ineffective Tissue PerfusionDokumen2 halamanNCP Ineffective Tissue PerfusionYasminGianneDeOcampoBarizoBelum ada peringkat
- NCP Activity Intolerance Related To Decreased in Oxygen SupplyDokumen3 halamanNCP Activity Intolerance Related To Decreased in Oxygen SupplyKyle Stephen TancioBelum ada peringkat
- Deficit)Dokumen2 halamanDeficit)Lee DeeBelum ada peringkat
- Ineffective Airway ClearanceDokumen2 halamanIneffective Airway ClearancePatrick Arvin Ballesteros BarcarseBelum ada peringkat
- Ineffective Airway ClearanceDokumen6 halamanIneffective Airway ClearanceBenly Grace Rebuyon MosquedaBelum ada peringkat
- NCP - Excessive Fluid VolumeDokumen4 halamanNCP - Excessive Fluid VolumeryanBelum ada peringkat
- Healthcare - Nursing Care Plan - Excess Fluid VolumeDokumen4 halamanHealthcare - Nursing Care Plan - Excess Fluid VolumeBenjamin CañalitaBelum ada peringkat
- NCPDokumen3 halamanNCPJezza RequilmeBelum ada peringkat
- Risk For Acute ConfusionDokumen2 halamanRisk For Acute ConfusionChar PereaBelum ada peringkat
- Short Term: Independent: Independent: Short TermDokumen2 halamanShort Term: Independent: Independent: Short TermAndre ImperialBelum ada peringkat
- Impaired Urinary EliminationDokumen3 halamanImpaired Urinary EliminationDenise Republika100% (1)
- NCPDokumen9 halamanNCPYesha Mae MartinBelum ada peringkat
- Nursing Care Plan Renal FailureDokumen2 halamanNursing Care Plan Renal FailureMark Jason Rabadan100% (1)
- Chronic Renal Failure Nursing Care PlanDokumen6 halamanChronic Renal Failure Nursing Care PlanRuva Oscass JimmyBelum ada peringkat
- Impaired Skin IntegrityDokumen3 halamanImpaired Skin IntegrityAubrey SungaBelum ada peringkat
- Fluid Volume DeficitDokumen2 halamanFluid Volume DeficitRuby AnneBelum ada peringkat
- Impaired Urinary EliminationDokumen2 halamanImpaired Urinary EliminationMatty-b AskalaniBelum ada peringkat
- Concept Map - Abby !Dokumen2 halamanConcept Map - Abby !Abegail Abaygar100% (3)
- NCP FVDDokumen1 halamanNCP FVDsisjing88510Belum ada peringkat
- NCP Tissue PerfusionDokumen2 halamanNCP Tissue PerfusionNiña Montejo Ealdama100% (1)
- Nursing Care Plan: Assessment Diagnosis Planning Interventions Rationale EvaluationDokumen1 halamanNursing Care Plan: Assessment Diagnosis Planning Interventions Rationale EvaluationJhevilin RM100% (1)
- NCP - Deficient Fluid VolumeDokumen2 halamanNCP - Deficient Fluid VolumerobbychuaBelum ada peringkat
- TB, Ineffectivbe Breathing PatternsDokumen1 halamanTB, Ineffectivbe Breathing PatternsnikkilyceeBelum ada peringkat
- Nursing Care Plan - 1 AlyanaDokumen1 halamanNursing Care Plan - 1 AlyanaKen100% (1)
- NCP 1Dokumen1 halamanNCP 1hsiriaBelum ada peringkat
- Nursing Care PlanDokumen4 halamanNursing Care PlanKath RubioBelum ada peringkat
- Medical Diagnosis: Chronic Kidney Disease Stage 5 Patient's NameDokumen4 halamanMedical Diagnosis: Chronic Kidney Disease Stage 5 Patient's NameHadeer Mahmoud Abuslima100% (1)
- NCP HyperthermiaDokumen1 halamanNCP HyperthermiaPastor James PacadaljenBelum ada peringkat
- Deficient Fluid Volume (Vanene)Dokumen7 halamanDeficient Fluid Volume (Vanene)jajalerBelum ada peringkat
- Tissue PerfusionDokumen2 halamanTissue PerfusionMichael John LeandichoBelum ada peringkat
- Nursing Care Plan Priorities: Risk For InjuryDokumen6 halamanNursing Care Plan Priorities: Risk For InjuryPauling FrezBelum ada peringkat
- Nursing Care Plan ExampleDokumen5 halamanNursing Care Plan ExampleBrittanyBelum ada peringkat
- FAELDONEA, PJ - Nursing Care PlanDokumen6 halamanFAELDONEA, PJ - Nursing Care PlanPatricia Jean Faeldonea100% (1)
- Fluid Volume Deficit BatuDokumen2 halamanFluid Volume Deficit Batumecz26Belum ada peringkat
- NCP - Fluid Volume ExcessDokumen2 halamanNCP - Fluid Volume ExcessIngrid Sasha Fong100% (4)
- MGH 8 - Ihd - NCPDokumen12 halamanMGH 8 - Ihd - NCPSesinando Niez Quilao Jr.100% (1)
- NCP For Ruptured AppendicitisDokumen2 halamanNCP For Ruptured AppendicitisJansen Arquilita RiveraBelum ada peringkat
- Fluid Volume DeficitDokumen3 halamanFluid Volume Deficitprickybiik100% (1)
- NCP 1Dokumen5 halamanNCP 1Denisse Shazz Mae MaretBelum ada peringkat
- A Renal Failure (NCP)Dokumen2 halamanA Renal Failure (NCP)Julie Aranda Hapin100% (1)
- NCP - Excess Fluid Volume (Aortic Stenosis)Dokumen3 halamanNCP - Excess Fluid Volume (Aortic Stenosis)Daniel Vergara Arce100% (3)
- 1 Fluid Volume Excess Chronic Renal Failure Nursing Care PlansDokumen3 halaman1 Fluid Volume Excess Chronic Renal Failure Nursing Care PlansMichael Baylon DueñasBelum ada peringkat
- NCP DMDokumen21 halamanNCP DMKate ManalastasBelum ada peringkat
- NCP For Nephrotic SyndromeDokumen2 halamanNCP For Nephrotic SyndromeLee Jenny100% (5)
- C C C C C C C C C C C C C C C C C C C C C C C C C C C C C C C CDokumen5 halamanC C C C C C C C C C C C C C C C C C C C C C C C C C C C C C C CMichaela ArellanoBelum ada peringkat
- Excess Fluid Volume - Nursing Diagnosis & Care Plan - NurseslabsDokumen8 halamanExcess Fluid Volume - Nursing Diagnosis & Care Plan - NurseslabsEricsonMitraBelum ada peringkat
- NCP Format 3 (CKD Chronic Kidney Disease DM Diabetes Mellitus Nephropathy)Dokumen4 halamanNCP Format 3 (CKD Chronic Kidney Disease DM Diabetes Mellitus Nephropathy)John Christopher Celestino100% (10)
- NCPDokumen15 halamanNCPCamille PinedaBelum ada peringkat
- Fluid Imbalance (NCP)Dokumen9 halamanFluid Imbalance (NCP)Putry RainismBelum ada peringkat
- NCP Liver CirrosisDokumen2 halamanNCP Liver CirrosisRosebud RoseBelum ada peringkat
- Excess Fluid VolumeDokumen3 halamanExcess Fluid VolumeStephanie Joy EscalaBelum ada peringkat
- Melvin D. Fabra: Objective - Aspiring To Obtain A Position As A Call Center Representative in A DynamicDokumen2 halamanMelvin D. Fabra: Objective - Aspiring To Obtain A Position As A Call Center Representative in A DynamicDana Fajardo RezanoBelum ada peringkat
- CA 2 Nres Exam & Answers 2014Dokumen5 halamanCA 2 Nres Exam & Answers 2014Dana Fajardo RezanoBelum ada peringkat
- Diagnostic and Laboratory ProcedureDokumen4 halamanDiagnostic and Laboratory ProcedureDana Fajardo RezanoBelum ada peringkat
- General Physical AssessmentDokumen2 halamanGeneral Physical AssessmentDana Fajardo RezanoBelum ada peringkat
- Benign Prostatic HyperplasiaDokumen18 halamanBenign Prostatic HyperplasiaDana Fajardo Rezano0% (1)
- JMDokumen45 halamanJMDana Fajardo RezanoBelum ada peringkat
- Students Name - Kendrick Joel Fernandes ROLL NO. 8250 Semester Vi Subject - Turnaround Management Topic-Industrial SicknessDokumen15 halamanStudents Name - Kendrick Joel Fernandes ROLL NO. 8250 Semester Vi Subject - Turnaround Management Topic-Industrial SicknesskarenBelum ada peringkat
- 12-List of U.C. Booked in NGZ Upto 31032017Dokumen588 halaman12-List of U.C. Booked in NGZ Upto 31032017avi67% (3)
- ICT Authority Legal NoticeDokumen13 halamanICT Authority Legal NoticeICT AUTHORITYBelum ada peringkat
- Coles Stategic AssessmentDokumen10 halamanColes Stategic AssessmentRichardBelum ada peringkat
- Rationale of Labour Welfare To Employers and EmployeesDokumen20 halamanRationale of Labour Welfare To Employers and Employeesajit yadav100% (1)
- IHE ITI Suppl XDS Metadata UpdateDokumen76 halamanIHE ITI Suppl XDS Metadata UpdateamBelum ada peringkat
- Frost Academy All Boys SchoolDokumen361 halamanFrost Academy All Boys Schoolcam UyangurenBelum ada peringkat
- Account StatementDokumen12 halamanAccount StatementbadramostuBelum ada peringkat
- Making Electric Vehicles ProfitableDokumen18 halamanMaking Electric Vehicles ProfitablevjslkumarBelum ada peringkat
- Drishti IasDokumen36 halamanDrishti Ias23010126269Belum ada peringkat
- RJSC - Form VII PDFDokumen4 halamanRJSC - Form VII PDFKamruzzaman SheikhBelum ada peringkat
- ILO Report On Disability and Labour India - 2011wcms - 229259Dokumen56 halamanILO Report On Disability and Labour India - 2011wcms - 229259Vaishnavi JayakumarBelum ada peringkat
- Republic of The Philippines: Paulene V. Silvestre Personal DevelopmentDokumen3 halamanRepublic of The Philippines: Paulene V. Silvestre Personal DevelopmentPau SilvestreBelum ada peringkat
- Chapter 1Dokumen25 halamanChapter 1Aditya PardasaneyBelum ada peringkat
- Articles On Philippine Obligation and ContractsDokumen114 halamanArticles On Philippine Obligation and ContractsKriz Batoto100% (1)
- APD6 Spec T20X en RevaDokumen10 halamanAPD6 Spec T20X en RevaKarla MartinsBelum ada peringkat
- Notice: Agency Information Collection Activities Proposals, Submissions, and ApprovalsDokumen2 halamanNotice: Agency Information Collection Activities Proposals, Submissions, and ApprovalsJustia.comBelum ada peringkat
- Topic 4 Qualitative Lectures 3Dokumen28 halamanTopic 4 Qualitative Lectures 3JEMABEL SIDAYENBelum ada peringkat
- Sample Information For Attempted MurderDokumen3 halamanSample Information For Attempted MurderIrin200Belum ada peringkat
- C Programming Bit Bank U-1, U-2Dokumen17 halamanC Programming Bit Bank U-1, U-2HariahBelum ada peringkat
- Organic Agriculture Gr12 - Module2.final For StudentDokumen20 halamanOrganic Agriculture Gr12 - Module2.final For Studentapril jean cahoyBelum ada peringkat
- Kohn v. Hollywood Police, Einhorn, Knapp, Perez, Sheffel, Cantor, BlattnerDokumen30 halamanKohn v. Hollywood Police, Einhorn, Knapp, Perez, Sheffel, Cantor, Blattnerkohn5671Belum ada peringkat
- Lecture 1. Introducing Second Language AcquisitionDokumen18 halamanLecture 1. Introducing Second Language AcquisitionДиляра КаримоваBelum ada peringkat
- Monthly Film Bulletin: 1T1IcqDokumen12 halamanMonthly Film Bulletin: 1T1IcqAlfred_HitzkopfBelum ada peringkat
- Listening Test Sweeney Todd, Chapter 4: 1 C. Zwyssig-KliemDokumen3 halamanListening Test Sweeney Todd, Chapter 4: 1 C. Zwyssig-KliemCarole Zwyssig-KliemBelum ada peringkat
- Business Communication and Behavioural StudiesDokumen10 halamanBusiness Communication and Behavioural StudiesBhujangam NaiduBelum ada peringkat
- Problem+Set+ 3+ Spring+2014,+0930Dokumen8 halamanProblem+Set+ 3+ Spring+2014,+0930jessica_1292Belum ada peringkat
- Nonfiction Reading Test The Coliseum: Directions: Read The Following Passage and Answer The Questions That Follow. ReferDokumen3 halamanNonfiction Reading Test The Coliseum: Directions: Read The Following Passage and Answer The Questions That Follow. ReferYamile CruzBelum ada peringkat
- WK5 SR MOD001074 Grundy 2006 PDFDokumen18 halamanWK5 SR MOD001074 Grundy 2006 PDFadwiyahBelum ada peringkat
- Enter Pre NaurDokumen82 halamanEnter Pre NaurNeha singhalBelum ada peringkat