Chapter 7 - Health Insurance Administration
Diunggah oleh
Jonathon Cabrera0 penilaian0% menganggap dokumen ini bermanfaat (0 suara)
50 tayangan0 halamanThe information given in this course material is merely for reference. Certain third party terminologies or matter are used only for contextual identification and explanation, without an intention to infringe.
Deskripsi Asli:
Judul Asli
Chapter 7_Health Insurance Administration
Hak Cipta
© Attribution Non-Commercial (BY-NC)
Format Tersedia
PDF, TXT atau baca online dari Scribd
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniThe information given in this course material is merely for reference. Certain third party terminologies or matter are used only for contextual identification and explanation, without an intention to infringe.
Hak Cipta:
Attribution Non-Commercial (BY-NC)
Format Tersedia
Unduh sebagai PDF, TXT atau baca online dari Scribd
0 penilaian0% menganggap dokumen ini bermanfaat (0 suara)
50 tayangan0 halamanChapter 7 - Health Insurance Administration
Diunggah oleh
Jonathon CabreraThe information given in this course material is merely for reference. Certain third party terminologies or matter are used only for contextual identification and explanation, without an intention to infringe.
Hak Cipta:
Attribution Non-Commercial (BY-NC)
Format Tersedia
Unduh sebagai PDF, TXT atau baca online dari Scribd
Anda di halaman 1dari 0
Page 1 of 26
Chapter 7: Health Insurance Administration
Certificate in Health Insurance
Confidentiality statement
This document should not be carried outside the physical and virtual boundaries of TCS and
its client work locations. Sharing of this document with any person other than a TCSer will
tantamount to violation of the confidentiality agreement signed when joining TCS.
Notice
The information given in this course material is merely for reference. Certain third party
terminologies or matter that may be appearing in the course are used only for contextual
identification and explanation, without an intention to infringe.
Certificate in Health Insurance TCS Business Domain Academy
Page 3 of 26
Contents
Chapter - 7 Health Insurance Administration .................................................................... 4
Introduction ...................................................................................................................... 4
7.1 Administration of a Health Insurance ..................................................................... 5
7.2 Governance functions ............................................................................................ 5
7.3 Management Functions ......................................................................................... 5
7.4 Administrative Functions ....................................................................................... 7
7.4.1 Collecting Premium ........................................................................................... 8
7.4.2 Empanelling Providers ....................................................................................... 8
7.4.3 Authorizing admissions ......................................................................................9
7.4.4 Processing of claims ...........................................................................................9
7.4.5 Managing the Funds ........................................................................................ 10
7.4.6 Personnel Management ................................................................................... 11
7.5 Monitoring ........................................................................................................... 12
7.6 Third Party Administrators (TPAs) ....................................................................... 15
7.6.1 Structure of TPA: ............................................................................................. 15
7.6.2 Roles and Responsibilities of a TPA .................................................................. 16
7.6.3 Types of Health Insurance Claims .................................................................... 18
7.6.4 Benefits of TPAs .............................................................................................. 19
7.6.5 Revenue generation for TPAs .......................................................................... 20
7.6.6 Challenges and Scope for TPAs .................................................................... 21
Summary ........................................................................................................................ 22
References ...................................................................................................................... 25
Certificate in Health Insurance TCS Business Domain Academy
Page 4 of 26
Chapter - 7 Health Insurance Administration
Introduction
Managing health insurance scheme is a cumbersome job. It involves various administrative
functions to perform for effective management of the policy. Because of the diversity and
skill set required to perform these functions, various professionals like actuaries, finance
managers, legal managers are hired to do such job. This chapter covers the administrative
aspects of health insurance like activities involved in running a healthcare scheme and
several performance metrics that are used to monitor the scheme.
Learning Objectives
On completion of this chapter, you will understand the:
Administrative system and functions of health insurance
Various performance measurement metrics of insurance schemes
Different skilled professionals required for functioning of a health insurance scheme
Roles and functions of Third Party Administrators (TPAs)
Certificate in Health Insurance TCS Business Domain Academy
Page 5 of 26
7.1 Administration of a Health Insurance
Administering an insurance scheme is a complex task. To begin with, the organiser of the
scheme needs to take responsibility for the scheme. This is the entity that will finally be
accountable for the success or failure of the scheme. Most successful health insurance
schemes have a clear administration.
Administration includes functions like:
Governance functions
Management functions
Administrative functions
Monitoring functions
7.2 Governance functions
Generally this function is performed by a regulator body. And when it comes to the internal
aspects of the company, it is the organizer who performs this role. Proper governance is
essential for functioning of any system. When it comes to the health insurance sector,
primary objective of governance would be to engage all the stakeholders in order to attain a
common goal, which is to provide an affordable healthcare to the entire population. It will
serve the interests of the providers, the community, the insuring companies and the
governments.
It is the organiser who will be deciding which community should be targeted, the overall
design of the scheme and the extent of subsidies that will be made available. They also
monitor the macro indicators like financial status of the scheme, the utilization rates and
any major grievances from the community or providers.
7.3 Management Functions
In the business of insurance there are certain managerial functions that either an organizer
or the insurer would have to perform or might delegate it to another agency. These
management functions can be broadly categorized as:
Certificate in Health Insurance TCS Business Domain Academy
Page 6 of 26
Creating awareness about the health insurance This is an important but often
neglected function. Managers usually assume that people are aware about health
insurance and its complexities. But they have to set aside such pre-conceived
notions and will have to make use of every opportunity available to educate and
enhance the knowledge of customers about health insurance.
Training the staff/community representatives Not only do staff need to be
trained on the policy/ scheme, they should also be given detailed inputs about
health insurance. This is necessary so that they will be able to answer the questions
posed to them by the community.
Negotiating with insurance companies Most insurance companies look at the
scheme from their perspective, i.e. to make profits. So it is essential that the
communitys needs as well as the insurers requirements are also met. Hence it is
important to keep such things in consideration while preparing the policy
document.
Negotiating with providers Providers (hospitals) usually are interested in
increasing their occupancy and profits. Quality of care, access to healthcare and
financial protection is secondary to them usually. Hence, it is imperative that the
insurer negotiates on behalf of the insured community to ensure that people get the
benefits that they have contributed towards.
Fixing the benefit package and the premium This is an important part of the
management function and should be negotiated between the community and the
insurer. A balance has to be maintained between the community needs, technical
requirements and affordability.
Marketing the product Marketing the product is different from creating
awareness on health insurance. It is closely linked, but here the emphasis is on
convincing the community to subscribe to the insurance policy.
Managing risks Any scheme needs to be self-sufficient. For this, moral hazard and
adverse selection need to be minimized. The organizer needs to introduce these
measures so that the scheme is protected against bankruptcy.
Controlling costs Mechanisms to control costs need to be introduced into the
policy right from the beginning. There exist various provider payment mechanisms
that will have to be chosen among in order to achieve that objective.
Controlling fraud Fraud is one of the banes of health insurance, and no country is
spared from this. Fraud can arise from any of the participants in the framework of
Certificate in Health Insurance TCS Business Domain Academy
Page 7 of 26
the health insurance, might be from hospitals and doctors through unnecessary
treatments, from the insured community by ways of falsified claims or from the
insurer by way of accounting malpractices. Measures to prevent fraud, especially by
doctors and hospitals are required. For this the organizer needs to employ medical
officers who will be able to see through the machinations of providers.
Redressing grievances This is yet another important function that is often
neglected. People need to air their grievances associated with the system. It has got
two advantages one, it makes the community feel in control of the scheme. And
two, it gives the insurer insight into the performance of their scheme. Grievances
can be useful in fine-tuning the schemes over time.
Monitoring the policy Mere creation, launch and administration would not serve
the purpose of performance enhancement, there should be a constant monitor on
the system (this will be discussed in detail in the later part of the chapter).
7.4 Administrative Functions
Administration is an important component in the smooth operation of the insurance policy.
Either the insurer or the organizer takes care of these functions. Once the insurance policy
has been designed, it is the responsibility of a team of efficient administrators to implement
the insurance scheme without any hurdles. Any insurance policy will typically involve a large
number of people. Transactions take place at different places at different times. Documents
need to flow smoothly between various stakeholders and financial details of each subscriber
and of the entire policy need to be closely monitored. Hence, it is essential that a good
administrative system is established and the various tasks involved at every stage are
clearly articulated to the team members. Administration can take place with a team within
the insurance company, or within the organizer. It can also be outsourced to Third Party
Administrators (TPAs). These are legal bodies entitled to perform such functions for an
insurance company.
Broadly, the major activities involved in the administration of an insurance scheme can be
listed as follows:
Collecting premium
Empanelling providers
Authorisation of admissions
Processing claims and reimbursements
Certificate in Health Insurance TCS Business Domain Academy
Page 8 of 26
Managing funds
Personnel Management
MIS Reports for Monitoring
7.4.1 Collecting Premium
Premiums are collected from individuals or from groups. Either way, there will be an
Enrolment Form, which the potential insured person is required to fill. The insurer collects
various details of the individual (and his/her family) through the process of filling the
enrolment form. The profile of the members in terms of their age, sex, previous medical
history, pre-existing illnesses, address, etc. are obtained through the enrolment form.
However, in group memberships, there may be just one enrolment form for the entire
group. Here just a list of the members has to be attached to this single form.
The enrolment form and the premium are paid to the insurer who in turn insures the
individual/group. In the case of renewals, there is no need for a new enrolment form. The
insurer issues a policy document that gives the details of the insurance scheme, the
benefits, the validity period, the exclusions and any disclaimers.
The organiser should also maintain financial records of the amounts collected, and the
number of individuals/ families/groups insured as well as their details.
7.4.2 Empanelling Providers
The insurer negotiates with hospitals in the vicinity of the target population for treating
patients under the insurance scheme. The insurers team ascertains the services and
facilities available with the hospital in terms of qualified personnel (doctors, nurses,
pharmacist, laboratory personnel, etc.), diagnostic tools/equipments and infrastructures
like labour room, operation theatre, and separate wards for sick patients/infectious
diseases, etc.
The insurance team would then negotiate the costs that the hospital will charge for the
patients for various procedures and the treatment protocol for various diseases. Once the
treatment procedures and the charges for the majority of the diseases are mutually agreed
and standardized, then that hospital can be empanelled as a Provider under the insurance
scheme. The list of empanelled providers should accompany the policy document, so that
the patient knows where to go when ill.
Certificate in Health Insurance TCS Business Domain Academy
Page 9 of 26
A small team in the hospital will be trained on the terms and administrative procedures
involved in the insurance policy.
7.4.3 Authorizing admissions
When the insured member becomes ill, and seeks medical treatment from an empanelled
provider. In the case of a reimbursement mechanism, there is no need for pre-authorisation.
The patient gets admitted, pays the bill and then gets reimbursed by the insurer. On the
other hand, in the case of a cashless mechanism, if the provider feels that the insured
patient requires admission, then the member is supposed to get a pre-authorization from
the insurer (or a TPA).
7.4.4 Processing of claims
There are two common routes for receiving claims. One is from the provider (in a cashless
system) and the other is from the individual insured patient. In either case, the insurer/TPA
will review the following:
Confirm the identity of patient
Confirm whether the patient had a pre-authorization
Confirm whether the patient was admitted during that period
Assess the diagnosis and the appropriateness of the treatment
Assess the cost of treatment
Figure 1 Process of claims and reimbursements
Certificate in Health Insurance TCS Business Domain Academy
Page 10 of 26
Claims are of two types based on their nature (will be dealt in detail at the end of this
chapter):
Cashless Hospitalization: Here the insurer or the TPA takes care of settling the bills
with the hospital, it is a hassle free process for the policyholder as he/she is not
required to pay anything out-of-pocket and later wait for the reimbursement.
Reimbursement Claim: In this case, initially the policyholder would settle all the
bills with the hospital and latter as per the procedures and policies of the insurance
company submits those bills, which upon scrutiny will be reimbursed by the TPA or
the insurer.
The documents required will vary from scheme to scheme, but usually the minimum
required are:
Copy of policy document
The discharge summary, hospital bill, prescriptions, laboratory reports, medical and
laboratory bills all original documents
If all the documents are acceptable, then the insurer will reimburse the amount to the
insured/provider/organizer.
7.4.5 Managing the Funds
The insurer ideally should have the financial systems to manage the funds received as
premium from the members and keep track of the claims and reimbursements made to
individual members. To put it simply, the insurer receives funds from all the members
initially and then reimburses their expenses from this pool over a period of time as and
Claims Type
Cashless Hospitalization
(Emergency / Planned)
Reimbursement
Claim
Certificate in Health Insurance TCS Business Domain Academy
Page 11 of 26
when claims are received. Hence, the insurer needs to have good systems for fund
management.
The following tasks are involved in the management of funds by the insurer:
Budgeting administrative expenses: The insurer will be incurring administrative
expenses in terms of salaries of personnel, overhead costs like telephone and other
office expenses, etc. It is important that a budget is prepared for these expenses
and they are monitored to see whether they are within the estimates.
Estimation of Cash flow: The insurers main task will be to estimate the cash flow
and estimate the possible outflow of funds. If the
members/providers/intermediaries are expected to send the claims on a monthly
basis, then the insurer should also try to make the cash flow projections on a
monthly basis, taking into account the administrative expenses.
Investing Funds: Depending on the cash flow projections, the unutilised funds
available with the insurer should be invested in banks/other options. The interest
earned from such investments will be a significant income for the insurer and should
be aimed to meet a significant portion of the administrative expenses of the insurer.
7.4.6 Personnel Management
The services of the following personnel are required by the administrative team of the
insurer:
Medical Professionals: The terms of the insurance policy may involve details of
diseases that are covered/ exempted and hence inputs from a doctor are essential
while processing the claims. Moreover, the treatment given to the members and
the costs incurred need to be examined by a qualified medical professional. The
insurer may do well to have broad parameters for monitoring the claims in terms of
the prevailing diseases, incidence of a particular kind of illnesses, average costs for
different categories of procedures, etc.
Actuarial/insurance professional: When the insurance policy is designed, the
company is expected to do an analysis of the historical data with respect to
prevalence of diseases among the insured population, historical data of charges
Certificate in Health Insurance TCS Business Domain Academy
Page 12 of 26
prevailing in the various hospitals/providers, the expected rate of claims, etc. As the
policy gets underway and the company starts receiving the claims, an analysis of
the actual data compared to the earlier estimates shall be done by the
actuarial/insurance professional on a monthly basis to ensure that there is no
malpractice or flaw in the programme. This close monitoring will help design the
policy for subsequent years.
Finance/Programme Manager: The profitability of the insurance programme
depends on the fund management efficiency of the insurer as well. The company
will have invested the unutilised funds in short-term/medium-term deposits and the
interest income is crucial for the programme. So, the finance/ programme manager
should keep track of funds on a regular basis and make suitable investment
decisions. The cash flow projections made at the beginning of the policy period shall
be revisited at least on a monthly basis. The administrative expenses also will have a
bearing on the cash flow of the programme and hence the finance manager will
monitor these expenses as well.
Legal Professional: The insurance policy issued at the beginning of the policy
period is a legal document and hence needs to be drafted according to the existing
laws that cover insurance. The inputs of a legal professional, particularly well-versed
with medico-legal cases, will be useful. Similarly, if there are any disputes regarding
claims and reimbursements between the insurer and the members/providers, one
party may resort to court to settle the disputes. Hence, it is important to keep a
legal professional also as part of the team and get all the documents approved by
her/him.
7.5 Monitoring
The performance of an insurance scheme will be measured on various metrics. The
commonly used indicators/ metrics are:-
Coverage rate - Percentage of people insured with respect to the target population.
Even in some of the best schemes, the coverage rate might reach a maximum of 40
- 50%. Only in mandatory schemes or in social healthcare does the coverage reach
75100%.
Certificate in Health Insurance TCS Business Domain Academy
Page 13 of 26
Renewal rate Proportion of people who were insured in the consecutive year. This
is a good proxy indicator of the quality of the insurance scheme. Good schemes
have a renewal rate of about 50 per cent. This indicates that people are happy with
the scheme and are willing to rejoin it.
Utilization rate - Percentage of people who had accessed healthcare. This depends
on the benefit package. For general hospitalization the rates range from 24%. In
rare cases, it can be as high as 710%.
Claims Ratio - The ratio of the amount of reimbursements made to the total
premium amount received by the provider. This gives a financial overview of the
scheme, whether it is viable or needs to be modified.
Status of the insurance fund A kind of income and expenditure statement,
indicating the cumulative premium amount collected under the scheme,
reimbursements made, the administrative expenses incurred and the interest
income earned.
Certificate in Health Insurance TCS Business Domain Academy
Page 14 of 26
Liquidity Status - The liquid cash available in the insurance fund at the end of every
month (that has not been invested in any instruments/banks). A ratio of this amount
to the average claim amount per month will give us the number of months the fund
can service the claims.
Solvency ratio The assets divided by the liabilities of the scheme. It indicates the
financial strength of the insurance policy and its ability to pay its obligations now
and in the future.
Report of the rejected claims Reasons for rejection and the claim frequency. An
analysis of this report will help the insurer plan an awareness campaign either
among the Members or among the hospitals about the provisions of the insurance
scheme.
Promptness of claims settlement This gives an idea about the efficiency of the
insurer. Many schemes have suffered from delays in reimbursing the patients/
providers leading to loss of the scheme credibility.
Certificate in Health Insurance TCS Business Domain Academy
Page 15 of 26
7.6 Third Party Administrators (TPAs)
Third party administrators (TPAs) are neither healthcare providers nor insurance
companies; they act as intermediaries by bringing all components of healthcare such as
physicians, hospitals, clinics, long-term facilities, and pharmacies together.
A Third Party Administrator is an organization that handles the administrative aspects of a
health insurance company that include processing insurance claims or managing employee
benefit plans of a separate entity.
A TPA can be an entity of an insurance company or an independently operating
organization that handles the outsourced administrative functions of multiple insurance
companies.
7.6.1 Structure of TPA
Figure 2 TPAs in Health Insurance
Certificate in Health Insurance TCS Business Domain Academy
Page 16 of 26
Their services include:
Cashless service at hospitals
Call centre support to policyholders
Medical cost management
Management of claims and reimbursements
List of professionals that TPAs hire for administering such services include:
Medical doctors
Hospital Managers
Insurance Consultants
Legal Experts
Information Technology professionals
Management Consultants
For an effective administration TPAs require skills to:
Develop network
Managing finance
Delivering appropriate healthcare service to its clients
7.6.2 Roles and Responsibilities of a TPA
The basic responsibility of a TPA is to bridge the gap between the insured and the insurer by
providing quality service at an economical cost. In order to provide such services, TPA has to
follow certain best practises like:-
They play a major role in assimilating data for actuarial calculations, because they
are in possession of morbidity data that are linked with individual characteristics
such as age, sex etc.,
TPAs should procure all the relevant information of the policyholders from the
insurers and must issue identity cards to the policyholders which can be furnished to
the hospital authorities prior to availing any hospitalization services.
TPAs should disclose to the clients the healthcare services that it is authorized to
render based on the contract and bring to the notice of the insurer any adverse
report, inconsistencies or material facts that are relevant to the insurance
companys business.
Certificate in Health Insurance TCS Business Domain Academy
Page 17 of 26
A TPA must maintain proper records, documents, evidence and book of all
transactions carried out by it on behalf of an insurance company as per the terms of
agreement. And such records must be preserved at least for certain period of time.
The records that are to be maintained in conformity with the accepted accounting
and professional standards should be made available to the insurance company and
the regulatory bodies as and when required and TPA cannot deny access to these
authorities on any ground.
TPAs should maintain strict confidentiality about the information and records of its
business and about the records of its clients unless required to be produced to an
authority authorized to per use the records or called for by a court of law.
At the time of claim settlement, the TPA should collect all the required documents
pertaining to the claim arising out of the insurance contract concluded by the
insurance company with the policy holder.
The TPA should provide all the required assistance specified under the agreement
and advise to policy holders or claimants or beneficiaries in complying with the
requirements for settlement of claims with the insurance company.
Under no circumstances should a TPA overtly or covertly influence the policyholder
of an insurance company to switch loyalty to some other insurer.
The TPA should not resort to any unethical practise in its dealings with the clients,
like asking a client to suppress information or provide wrong information or
demand a cutback from the claims proceeds.
The TPA should not charge any fee from the policyholders contravening the terms
of the contract.
In case of non-renewal of the contract, revocation or cancellation of the license, the
TPA should hand over all the records, book of accounts, documents and collected
data etc.., to the insurance company immediately.
A TPA is required to prepare an annual report duly authenticated by the directors
and the CEO/ CFO of the company and make it available to the insurance company
as well as the regulatory.
In this context a Network Hospital means a network of hospitals, nursing homes and
healthcare providers approved and empanelled by the company and considered as the
preferred medical centres or establishments.
Certificate in Health Insurance TCS Business Domain Academy
Page 18 of 26
And Cashless Hospitalization means that as a healthcare policyholder, one need not have
to furnish the hospital bills and then get the reimbursement later. On the contrary, the
policyholder will be able to avail of medical services at designated hospitals, and the
concerned TPA will settle the bills.
7.6.3 Types of Health Insurance Claims
With TPAs being introduced into healthcare, the delivery mechanism of insurance has taken
several shapes. Now an insurance policyholder can opt any of these three options:
Get treated in any one of the hospitals by availing cashless facility
Get treated in a network hospital without using the cashless facility
Get treated in a non-network hospital.
Because of these available options, claims can be categorized into three types:
Cashless Hospitalization
Under the cashless hospitalization scheme, the insured is spared the hassle of filling
the claim papers, attaching the supporting documents, submitting the claim and
waiting for the settlement of the claim.
Process of availing cashless hospitalization:
Depending on the need, urgency and status of empanelment of the hospital there are
certain steps that are involved before availing this facility, they are:
Once the health insurance contract is concluded, the insurance company
communicates particulars regarding the insured to the TPA concerned.
On receipt of this information, the TPA will write to the policyholder and advise
him/her on the procedure for obtaining the identification card that will enable
the policyholder to avail of the cashless facility in any of the network hospitals.
Once this is done, the policyholder may face two types of situations, viz.,
planned hospitalization or an unforeseen medical emergency
Planned Hospitalization
In this case, the policyholder needs to undergo following phases:
He/she is required to take pre-admission authorization from the authority
designated for the purpose by the insurance company and then submit in
advance as specified.
Certificate in Health Insurance TCS Business Domain Academy
Page 19 of 26
The designated authority of the company or the TPA upon receiving this
request would examine the request as to whether it would meet the terms and
conditions of the policy, cover limit, exclusion clause etc..,
If all the criteria are met, the designated authority would authorize the
concerned hospital to offer the cashless facility.
In certain cases the authorization maybe rejected for following reasons:
There was a suppression of pre-existing conditions
Recommending physician note contains information about the ailment
Based on the details given by the recommending physician, the ailment falls
under the category of excluded diseases
Unforeseen Emergency
In this case, it is practically infeasible to get the pre-authorization done. Hence there
exists a different process under this scenario.
On admission, the policyholder or his/her authorized representative should notify the
TPA about the whereabouts of the hospital, provisional diagnosis, duration of stay in
the hospital and approximate expenses. This notice has to be served within the
stipulated timeframe as per policys terms and conditions. Thereafter, the TPA will
examine the bill and settle it with the hospital according to the eligibility conditions.
After settling the accounts of the hospital, the TPA will send all the relevant claim
papers to the insurance company to get the reimbursement and the TPA commission
as per the agreement.
7.6.4 Benefits of TPAs
TPAs bring down the claims ratio, by reducing false claims as well as standardizing
treatment costs. Some of the common benefits by introducing TPAs are:
Faster and focused claims management
Lower overhead cost and reduced cost of claims management
Immediate access to highly trained claims administrators
Improved control over claims outcomes
Provision of cashless services at much ease
Certificate in Health Insurance TCS Business Domain Academy
Page 20 of 26
Safeguarding of customer relationships
Protection of brand reputation
Control of possible frauds by the private healthcare providers
7.6.5 Revenue generation for TPAs
The primary revenue for TPAs is the fee charged for managing the claims of the insurance
companies. Such fee is based on the volume and scope of services provided by them and it
usually is a fixed percentage of the premium collected from the enrollees. Apart from this,
TPAs provide many other services to the insurance companies for which the organization
directly pays the fee. Such services include:
Benefit management: While designing group insurance policies and new policies
by the insurance companies, TPAs come handy.
Medical management: It involves a generic follow up of the case and monitor how
treatment is rendered and ensure it is genuine.
Provider network management: It is one of the key tasks of a TPA, where the TPA
negotiates with the providers in terms of quality of care, tariff rates, appointment
and admission policies etc.., before entering into a contract with them to be
empanelled into the provider network. A periodic monitor of the quality and
performance of these providers is also essential.
Claims administration: It involves receiving claims, processing claims and
accepting/rejecting claims based on the terms of the policy. Once the claim is
considered to be genuine and is covered under the benefits of the policy then the
claim is settled which is called as claims adjudication.
Information and data management: Data Analytics is highly essential when it
comes to designing new products. TPAs by the nature of their work have access to
loads of data with which they can generate reports and databases. They act as
inputs for management in analyzing and controlling costs besides helping design
new products.
Certificate in Health Insurance TCS Business Domain Academy
Page 21 of 26
7.6.6 Challenges and Scope for TPAs
Incentives for cost control: The remuneration of TPA would generally be a fixed
percentage of the policy premium. Reimbursements generally are controllable, but
the payments to TPAs for their services are not linked to their effort of controlling
reimbursements. Hence, their remunerations should take into account their efforts
and successes in controlling the costs and reimbursements. In any insurance
system, focus on prevention and promotive services can cut down many costs. TPAs
can play an important role in these areas. However, such mechanisms are not put in
place and their role is not clearly defined. TPAs can offer and organize such services
provided they are incentivized for such efforts.
Educating and improving awareness: In many situations policyholders are not
aware of various conditions and exclusion clauses in insurance policies. As a result,
disputes between policyholders and insurance companies have increased and both
parties have resorted to litigation. Problems arise because of lack of information
and awareness, and an inadequate understanding of various nuances of insurance.
TPAs can play an important role in educating consumers and bringing awareness.
TPAs are the intermediaries between the insurer and the insured and they are in a
position to educate the insurer in such aspects.
Mitigating negative consequences & controlling malpractices in health
insurance: On the demand side, one positive impact of TPAs existence would be on
service utilization. In most situations utilization of high cost speciality care will need
approval and concurrence from TPA. Utilization of such services would be rationed
by restricting direct access to specialists.
Research on data: While dealing with a large number of policyholders TPAs would
be in a position to generate lot of comparable data on utilization of services and
their cost structures. This information can be used to set benchmarks for costs and
quality of care. However, this might take certain time. Understanding cost drivers is
essential in developing and putting in place those drivers.
Certificate in Health Insurance TCS Business Domain Academy
Page 22 of 26
Summary
Administration of health Insurance includes functions like:
Governance functions
Management functions
Administrative functions
Monitoring functions
Governance is generally is performed by a regulator body and when it comes to the
internal aspects of the company, it is the organizer who performs this role
Managerial functions are performed by either an organizer or the insurer or might
delegate it to another agency.
Management functions of a health insurance are:-
Creating awareness about the health insurance
Training the staff/community representatives
Negotiating with insurance companies
Negotiating with providers
Fixing the benefit package and the premium
Marketing the product
Managing risks
Controlling costs
Controlling fraud
Redressing grievances
Monitoring the policy
Administration is an important component in the smooth operation of the
insurance policy. Either the insurer or the organizer takes care of these functions.
Administrative functions in health insurance are:-
Collecting premium
Empanelling providers
Authorisation of admissions
Processing claims and reimbursements
Managing funds
Personnel Management
MIS Reports for Monitoring
Certificate in Health Insurance TCS Business Domain Academy
Page 23 of 26
Claims are classified into two types:-
Cashless Hospitalization
Reimbursement Claim
Managing the fund involves following tasks:-
Budgeting administrative expenses
Estimation of Cash flow
Investing Funds
Different types of professionals in the administrative team are:-
Medical Professionals
Actuarial/insurance professional
Finance/Programme Manager
Legal Professional
Several metrics used to measure the performance of health insurance are:-
Coverage rate
Renewal rate
Utilization rate
Claims Ratio
Status of the insurance fund
Liquidity Status
Solvency ratio
Report of the rejected claims
Promptness of claims settlement
A Third Party Administrator (TPA) is an organization that handles the
administrative aspects of a health insurance company that include processing
insurance claims or managing employee benefit plans of a separate entity.
Network Hospital means a network of hospitals, nursing homes and healthcare
providers approved and empanelled by the company and considered as the
preferred medical centres or establishments.
Cashless Hospitalization means the policyholder will be able to avail of medical
services at designated hospitals, and the concerned TPA will settle the bills.
Types of Health Insurance Claims are:-
Cashless Hospitalization
Planned Hospitalization
Certificate in Health Insurance TCS Business Domain Academy
Page 24 of 26
Unforeseen Emergency
Other Services of a TPA are:-
Benefit management
Medical management
Provider network management
Claims administration
Information and data management
Challenges of a TPA are:-
No Incentives for cost control
Educating and improving awareness
Mitigating negative consequences & controlling malpractices in health
insurance
Research on data
Certificate in Health Insurance TCS Business Domain Academy
Page 25 of 26
References
Ramesh Bhat, Sumesh K Babu, Health Insurance and Third Party Administrators: Issues
and Challenges, Working Paper IIM Ahmedabad, May 2003
IRDA Journal (2003). Data for Health Insurance
Managed Care, International Foundation of Employee Benefit Plans
Dranove D. (2000), The Economic Evolution of American Health Care: From Marcus Welby
to Managed Care, Princeton University Press, New Jersey
Managed care in the public sector, US Department of Health and Human Services
Jonathan Gruber and Helen Levy, The Evolution of Medical Spending Risk, Journal of
Economic Perspectives-Volume 23, Number 4-Fall 2009, Pages 2548
James C. Robinson, The End of Managed Care, American Medical Association
Notice
The information given in this course material is merely for reference. Certain third party
terminologies or matter that maybe appearing in the course are used only for contextual
identification and explanation, without an intention to infringe.
Page 26 of 26
Anda mungkin juga menyukai
- Chapter 6 - Health Insurance SchemesDokumen0 halamanChapter 6 - Health Insurance SchemesJonathon CabreraBelum ada peringkat
- Health Insurance and Risk ManagementDokumen7 halamanHealth Insurance and Risk ManagementPritam BhowmickBelum ada peringkat
- Chapter 8 - Managed Care PlansDokumen0 halamanChapter 8 - Managed Care PlansJonathon CabreraBelum ada peringkat
- Module 2 Insurance EcosystemDokumen52 halamanModule 2 Insurance Ecosystemnivantheking123Belum ada peringkat
- Project Final SolutionDokumen26 halamanProject Final SolutionSohail AfridiBelum ada peringkat
- Literature Review on Insurance Management AutomationDokumen5 halamanLiterature Review on Insurance Management AutomationAncy KalungaBelum ada peringkat
- Functional View of Insurance: Core FunctionsDokumen3 halamanFunctional View of Insurance: Core FunctionsSunil ReddyBelum ada peringkat
- Drive SPRING 2015 Program Mf0018 Insurance and Risk ManagementDokumen12 halamanDrive SPRING 2015 Program Mf0018 Insurance and Risk ManagementRoshan KumarBelum ada peringkat
- AHM 520: Risk Management in Health PlansDokumen17 halamanAHM 520: Risk Management in Health PlansRahul KoulBelum ada peringkat
- Embedded Insurance by Rashmika WijesingheDokumen17 halamanEmbedded Insurance by Rashmika Wijesinghearc chanukaBelum ada peringkat
- Insurance Accounting and Finance: Lecture#4 by Dr. Muhammad UsmanDokumen8 halamanInsurance Accounting and Finance: Lecture#4 by Dr. Muhammad UsmanNoor MahmoodBelum ada peringkat
- Kastur I J Bao Spring 2006Dokumen16 halamanKastur I J Bao Spring 2006Ħøşęħ ÖżįlBelum ada peringkat
- Chapter 3 - Health Insurance ClassificationDokumen0 halamanChapter 3 - Health Insurance ClassificationJonathon CabreraBelum ada peringkat
- RSK4802 Notes To Exam 2021Dokumen61 halamanRSK4802 Notes To Exam 2021bradley.malachiclark11Belum ada peringkat
- Insurance and Risk ManagementDokumen5 halamanInsurance and Risk ManagementPrashant AhujaBelum ada peringkat
- Baf2206 Ahmed PDFDokumen8 halamanBaf2206 Ahmed PDFODUNDO JOEL OKWIRIBelum ada peringkat
- A Report ON Management Thesis - Ii: Under Guidance ofDokumen37 halamanA Report ON Management Thesis - Ii: Under Guidance ofVikas Sharma100% (1)
- Understanding Actuarial Practice - KlugmanDokumen54 halamanUnderstanding Actuarial Practice - Klugmanjoe malor0% (1)
- The Managed Care Answer GuideDokumen33 halamanThe Managed Care Answer Guideron jeremyBelum ada peringkat
- Explore Measurements To Advance The Service Quality of Janashakthi Insurance Life Claims DepartmentDokumen24 halamanExplore Measurements To Advance The Service Quality of Janashakthi Insurance Life Claims DepartmentNuwan KumarasingheBelum ada peringkat
- Insurance and Risk Management (Ranveer)Dokumen9 halamanInsurance and Risk Management (Ranveer)Ranveer Singh RajputBelum ada peringkat
- 9999 Ghausia Insurance Services and Consumer AttitudeDokumen13 halaman9999 Ghausia Insurance Services and Consumer AttitudeiisteBelum ada peringkat
- Customer Satisfaction Insurance Products of ICICI PrudentialDokumen71 halamanCustomer Satisfaction Insurance Products of ICICI Prudentialkarthik_shabby15Belum ada peringkat
- Underwriting Assgment Group 2Dokumen8 halamanUnderwriting Assgment Group 2Elias maphinaBelum ada peringkat
- Surety Structure and OrganisationDokumen12 halamanSurety Structure and Organisation:Lawiy-Zodok:Shamu:-ElBelum ada peringkat
- MF0018Dokumen7 halamanMF0018Pawan Dimri50% (2)
- BAF2206Dokumen7 halamanBAF2206ODUNDO JOEL OKWIRIBelum ada peringkat
- MI Consumer Guide To Health InsuranceDokumen40 halamanMI Consumer Guide To Health InsuranceMichigan NewsBelum ada peringkat
- Consumer Satisfaction with Tata-AIG Life InsuranceDokumen66 halamanConsumer Satisfaction with Tata-AIG Life Insurancetulasinad123100% (1)
- CCE 1 Insurance Laws ®ulations Pravin ShimpiDokumen9 halamanCCE 1 Insurance Laws ®ulations Pravin ShimpiPravin ShimpiBelum ada peringkat
- How Actuaries Help Plan for an Uncertain FutureDokumen12 halamanHow Actuaries Help Plan for an Uncertain FuturePrajakta Kadam67% (3)
- Suggestion and ConclusionDokumen4 halamanSuggestion and ConclusionSidhantha Jain100% (1)
- Internship Report On Bajaj Allianz - 151904489Dokumen60 halamanInternship Report On Bajaj Allianz - 151904489Prakhar100% (1)
- Claim Management in Life InsuranceDokumen55 halamanClaim Management in Life InsuranceSunil RawatBelum ada peringkat
- Managed Care Guide: Understanding Plans, Terms and Your RightsDokumen33 halamanManaged Care Guide: Understanding Plans, Terms and Your RightsHihiBelum ada peringkat
- Insurance Risk Management GuidelinesDokumen32 halamanInsurance Risk Management GuidelinesMohul BasuBelum ada peringkat
- Marketing Mix Insurance SectorDokumen4 halamanMarketing Mix Insurance SectorSantosh Pradhan100% (1)
- 15 Chapter 6Dokumen35 halaman15 Chapter 6Sairaj SankpalBelum ada peringkat
- Q. 15 Insurance Regulatory and Development AuthorityDokumen2 halamanQ. 15 Insurance Regulatory and Development AuthorityMAHENDRA SHIVAJI DHENAKBelum ada peringkat
- Marketing Mix For Insurance IndustryDokumen7 halamanMarketing Mix For Insurance IndustryReema NegiBelum ada peringkat
- Learner Guide 242597Dokumen28 halamanLearner Guide 242597palmalynchwatersBelum ada peringkat
- Ethics in Insurance SectorDokumen24 halamanEthics in Insurance Sectorvishnusharma454Belum ada peringkat
- Summer Training Project Report: in The Partial Fulfillment of The Degree of Master of Business Administration 2009-2010Dokumen62 halamanSummer Training Project Report: in The Partial Fulfillment of The Degree of Master of Business Administration 2009-2010Mahendra ReddyBelum ada peringkat
- Customer Satisfaction On ICICI PrudentialDokumen63 halamanCustomer Satisfaction On ICICI Prudentialmss_singh_sikarwar100% (8)
- Important Role of IRDA in The Insurance Sector in IndiaDokumen2 halamanImportant Role of IRDA in The Insurance Sector in Indiashaheera banuBelum ada peringkat
- Chapter 2 - Health Insurance ConceptsDokumen0 halamanChapter 2 - Health Insurance ConceptsJonathon CabreraBelum ada peringkat
- Daffodil International University Journal of Business and Economics, Vol. 2Dokumen17 halamanDaffodil International University Journal of Business and Economics, Vol. 2hannan000Belum ada peringkat
- Consumer Behaviour and Satisfaction On ICICIDokumen53 halamanConsumer Behaviour and Satisfaction On ICICIMohan RamBelum ada peringkat
- Internship Report: Metlife Alico, BangladeshDokumen38 halamanInternship Report: Metlife Alico, Bangladeshpavel108012Belum ada peringkat
- Designing and Implementing An Effective Health and Safety Management SystemDokumen52 halamanDesigning and Implementing An Effective Health and Safety Management SystemLuis AguilarBelum ada peringkat
- InsuranceDokumen10 halamanInsuranceShriya Vikram ShahBelum ada peringkat
- Insurance Planning and Risk ManagementDokumen52 halamanInsurance Planning and Risk ManagementGouri Pillay67% (3)
- Unit 3 InsuranceDokumen29 halamanUnit 3 InsuranceNikita ShekhawatBelum ada peringkat
- Marketing Mix in Insurance IndustryDokumen4 halamanMarketing Mix in Insurance Industryanon-49388690% (30)
- 2014: Your Ultimate Guide to Mastering Workers Comp Costs: The MINI-BOOK: Reduce Costs 20% to 50%Dari Everand2014: Your Ultimate Guide to Mastering Workers Comp Costs: The MINI-BOOK: Reduce Costs 20% to 50%Belum ada peringkat
- Medical Revenue Cycle Management - The Comprehensive GuideDari EverandMedical Revenue Cycle Management - The Comprehensive GuideBelum ada peringkat
- Textbook of Urgent Care Management: Chapter 9, Insurance Requirements for the Urgent Care CenterDari EverandTextbook of Urgent Care Management: Chapter 9, Insurance Requirements for the Urgent Care CenterBelum ada peringkat
- Textbook of Urgent Care Management: Chapter 20, Strategic Talent Management: Talent Makes All the DifferenceDari EverandTextbook of Urgent Care Management: Chapter 20, Strategic Talent Management: Talent Makes All the DifferenceBelum ada peringkat
- Chapter 11 - Legislations Structure and Trends Across NationsDokumen0 halamanChapter 11 - Legislations Structure and Trends Across NationsJonathon CabreraBelum ada peringkat
- Chapter 10: Fraud Management: Certificate in Health InsuranceDokumen0 halamanChapter 10: Fraud Management: Certificate in Health InsuranceJonathon CabreraBelum ada peringkat
- Chapter 9 - Risk ManagementDokumen0 halamanChapter 9 - Risk ManagementJonathon CabreraBelum ada peringkat
- Chapter 5 - Health Insurance SchemesDokumen0 halamanChapter 5 - Health Insurance SchemesJonathon CabreraBelum ada peringkat
- Chapter 4 - Health Insurance Schemes - GovernmentDokumen0 halamanChapter 4 - Health Insurance Schemes - GovernmentJonathon CabreraBelum ada peringkat
- Chapter 3 - Health Insurance ClassificationDokumen0 halamanChapter 3 - Health Insurance ClassificationJonathon CabreraBelum ada peringkat
- Chapter 1 Introduction To Health InsuranceDokumen0 halamanChapter 1 Introduction To Health InsuranceJonathon CabreraBelum ada peringkat
- Chapter 2 - Health Insurance ConceptsDokumen0 halamanChapter 2 - Health Insurance ConceptsJonathon CabreraBelum ada peringkat
- Zalameda TransactionDokumen1 halamanZalameda TransactionLeslie OngreaBelum ada peringkat
- QropsDokumen35 halamanQropsmuralicgc1544Belum ada peringkat
- Investment Office ANRS: Project Profile On The HONEY Processing PlantDokumen24 halamanInvestment Office ANRS: Project Profile On The HONEY Processing PlantJohn100% (1)
- 11 CaipccaccountsDokumen19 halaman11 Caipccaccountsapi-206947225Belum ada peringkat
- Need & Importance of Capital BudgetingDokumen4 halamanNeed & Importance of Capital BudgetingSrinidhi PnaBelum ada peringkat
- County Times: Sen. Mike MillerDokumen24 halamanCounty Times: Sen. Mike MillerSouthern Maryland OnlineBelum ada peringkat
- Review of financial liabilitiesDokumen3 halamanReview of financial liabilitiesralphalonzo67% (3)
- Auditing Theories and Problems Answer Key Quiz WEEK 1Dokumen10 halamanAuditing Theories and Problems Answer Key Quiz WEEK 1Van MateoBelum ada peringkat
- Financial Accounting I Assignment #1Dokumen8 halamanFinancial Accounting I Assignment #1Sherisse' Danielle WoodleyBelum ada peringkat
- Chapter 332-The Income Tax Act R.e.2022Dokumen104 halamanChapter 332-The Income Tax Act R.e.2022Ishmael OneyaBelum ada peringkat
- Tire City AssignmentDokumen7 halamanTire City AssignmentShivam Kanojia100% (1)
- Bachelor of Business Administration Hons. Islamic BankingDokumen10 halamanBachelor of Business Administration Hons. Islamic BankingSITI NUR AISYAH MD ROSTANBelum ada peringkat
- Journal entries and financial statementsDokumen9 halamanJournal entries and financial statementsFelipe ConcepcionBelum ada peringkat
- Government and Not For Profit Accounting Concepts and Practices 6th Edition Granof Solutions ManualDokumen26 halamanGovernment and Not For Profit Accounting Concepts and Practices 6th Edition Granof Solutions Manualadelarichard7bai100% (27)
- Borrowing CostDokumen12 halamanBorrowing CostKenn Adam Johan Gajudo100% (2)
- Kieso15e Testbank ch13Dokumen48 halamanKieso15e Testbank ch13Nguyễn Văn Tiến50% (2)
- Fabm MidtermDokumen7 halamanFabm MidtermFritzie Mae Ruzhel GuimbuayanBelum ada peringkat
- MBA Finance Interview Questions and Answers 995Dokumen9 halamanMBA Finance Interview Questions and Answers 995Shriya SurekaBelum ada peringkat
- SAP Note For TrainingDokumen25 halamanSAP Note For TrainingRudraraju KrishnaBelum ada peringkat
- Midterm quiz partnership profits ratiosDokumen3 halamanMidterm quiz partnership profits ratiosVia EmbienBelum ada peringkat
- Consolidated Financial Statements HRUM 31march201Dokumen98 halamanConsolidated Financial Statements HRUM 31march201EgaBelum ada peringkat
- GRP 4 (Budget and Fiscal Operations)Dokumen21 halamanGRP 4 (Budget and Fiscal Operations)Carl SallinBelum ada peringkat
- White Paper On Back MoneyDokumen108 halamanWhite Paper On Back MoneyNDTVBelum ada peringkat
- Unit - 4 Capital and Revenue Expenditures and ReceiptsDokumen9 halamanUnit - 4 Capital and Revenue Expenditures and ReceiptsTanyaBelum ada peringkat
- Trial Balance Adjustments Adjusted Trial Balance Income Statement Balance Sheet Account TitlesDokumen1 halamanTrial Balance Adjustments Adjusted Trial Balance Income Statement Balance Sheet Account TitlesRAMIREZ, KRISHA R.Belum ada peringkat
- ORF Presentation On Water Crisis in MumbaiDokumen38 halamanORF Presentation On Water Crisis in MumbaiObserver Research Foundation (ORF), Mumbai100% (2)
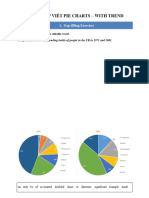
- Pie Charts With TrendDokumen19 halamanPie Charts With TrendHoàng ChiBelum ada peringkat
- Mavoko Water Strategic Plan 2015 - 2020 PDFDokumen50 halamanMavoko Water Strategic Plan 2015 - 2020 PDFDesmond BarongoBelum ada peringkat
- Advanced Accounting Baker Test Bank - Chap012Dokumen67 halamanAdvanced Accounting Baker Test Bank - Chap012donkazotey50% (2)
- Chapter 2 Practice ExamDokumen16 halamanChapter 2 Practice ExamShayma S.h.kBelum ada peringkat