Guide to Acute, Chronic Wounds: Types, Causes, Healing
Diunggah oleh
Bayu Mario GintingDeskripsi Asli:
Judul Asli
Hak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Guide to Acute, Chronic Wounds: Types, Causes, Healing
Diunggah oleh
Bayu Mario GintingHak Cipta:
Format Tersedia
Wound Types
Acute Wounds
Acute wounds can occur from traumatic abrasions, lacerations, and superificial skin and soft tissue injuries.1 Acute wounds tend to heal spontaneously without complications through the four phases of wound healing which are hemostasis, inflammation, proliferation, and maturation.
Chronic Wounds
The problem of chronic wounds...
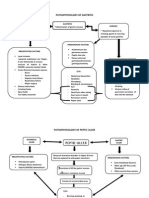
Chronic wounds are wounds that fail to heal within a six-to-twelve week period of best clinical practice.2 They are a challenge to both healthcare professionals and patients because they last a long time, causing a loss of body image and making the person more susceptible to infection. Several factors can impair the normal healing process such as infection, necrotic tissue, impaired tissue perfusion and steroids.3 Chronic wounds can occur anywhere on the body including the lower extremities. They are commonly referred to as diabetic foot ulcers, venous stasis ulcers and pressure ulcers. Chronic wounds fail to progress through an organized, orderly and timely sequence of wound repair. The patients involved may have other pre-existing medical conditions such as diabetes mellitus that could contribute to the non-healing, chronic wound. It is important to determine the underlying etiology of the chronic wound and identify the factors that interfere with the healing process such as malnutrition, poor glucose control, excessive pressure to an area, anemia and persistent edema. Elderly patients who are experiencing a chronic wound may have multiple medical conditions that necessitate a non-surgical approach to wound healing. Acceleration of wound closure is important for individuals with chronic wounds because they are at risk for infection, and these wounds can interfere with activities of daily living.
The common types of chronic wounds are as follows:
Diabetic Foot Ulcers (DFU)Diabetic foot ulcers are a significant problem on a global basis. Approximately 15% of people with diabetes will develop a foot ulcer and it is estimated that more than half of these will experience a second ulcer. Diabetic foot ulcers occur most commonly due to neuropathy (loss of sensation in the lower extremity) and peripheral vascular disease. Neuropathy can occur partially as a complication of prolonged glucose elevation.4 Failure of diabetic foot ulcers to heal may result in amputation. The main reasons for diabetic foot ulcers failing to heal are two-fold. The first is because the person with the foot ulcer continues to walk on the ulcer causing irritation and skin breakdown. They may also have some type of foreign body enter the skin and be unaware of this happening. For the healing process to take place, these wounds usually must have weight redistributed away from the wound in what is known as offloading. Specialty shoes and devices are available to assist with this process. The second main reason that these ulcers fail to heal is related to poor diabetes control. Uncontrolled blood sugar can prevent the body from healing itself by interfering with various healing processes. In addition to blood sugar control, management of diabetic wounds includes prevention of weight bearing (off loading), debridement of devitalized tissue, prevention of infection and local wound management.
1.
2.
Venous UlcersVenous Ulcers are the most common and costly chronic wound ulcer seen in the United States and affect women three times more often than men. The prevalence of lower limb ulcers ranges from 0.12% to 0.32% of the general population.5 Patients experiencing venous ulcers suffer from the inability to heal and the high rate of reoccurrence at 72%.5 Venous ulcers can cause
pain, limit activities of daily living and negatively impact quality of life.
Venous ulcers can be caused by damaged or leaky venous valves, or a faulty calf muscle pump action which causes sustained high venous pressure known as venous hypertension. These ulcers are usually located around the medial malleolus and are accompanied by edema or swelling of the affected leg, large amounts of drainage, and often have a scaly type of skin condition known as dermatosis. It is important to note that not all leg ulcers are venous in origin particularly those ulcers located above or below the gaiter and ankle region. People with venous insufficiency sometimes report having had a blood clot in the affected limb. Due to the interruption of blood flow back to the heart, pooling of blood is seen in the limb that sometimes results in swelling. Eventually, protein from blood vessels can leak into the tissue and cause an ulcer to form. A cornerstone of treatment for venous ulcers beyond local ulcer management is the use of sustained compression in order to decrease the edema by wrapping the legs to promote blood flow back to the heart. Pressure UlcersPressure ulcers are also known as decubitus ulcers or bed sores and have a psychologic, physiologic and economic impact on the individual. Pressure ulcers can result from immobility and can occur in persons that are bed ridden, who have had a spinal cord injury, or are in a wheelchair. Prevalence and incidence across all care settings varies, ranging from 0.4% to 38% in general acute care, 2.2% to 23.9% in long-term care, and 0% to 17% in home care.6 The tissue injury that occurs sometimes is a result of sustained pressure to a bony prominence area such as the hip or heel. The sustained pressure prevents adequate blood flow and causes the tissue to die. The wounds often fail to heal for a variety of reasons. One main reason is that pressure is not relieved from the wound. Special mattresses, bed and seating cushions are designed to help to relieve pressure to allow better blood flow to the injured area. Other reasons for these wounds to fail to heal often have to do with other underlying medical conditions that affect individuals, such as poor nutrition and incontinence, shear and friction. Pressure ulcer management includes pressure relief/pressure reduction, proper positioning, prevention of infection and local wound management.
3.
Types of wounds
Wound, sewn with four stitches
A laceration to the leg
An abrasion Open Open wounds can be classified according to the object that caused the wound. The types of open wound are: Incisions or incised wounds, caused by a clean, sharp edged object such as a !nife, a ra"or or a glass splinter. #ncisions which in$ol$e only the epider%is are legally classified as cuts, rather than wounds. Lacerations, irregular wounds caused by a blunt i%pact to soft tissue that lies o$er hard tissue &e.g. laceration of the s!in co$ering the s!ull' or tearing of s!in and other tissues such as caused by childbirth. (acerations %ay show bridging, as connecti$e tissue or blood $essels are flattened against the underlying hard surface. The ter% laceration is co%%only %isused in reference to injury with sharp objects, which would not display bridging &connecti$e tissue and blood $essels are se$ered'. Abrasions &gra"es', superficial wounds in which the top%ost layer of the s!in &the epider%is' is scraped off. Abrasions are often caused by a sliding fall onto a rough surface. Puncture wounds, caused by an object puncturing the s!in, such as a nail or needle. Penetration wounds, caused by an object such as a !nife entering the body Gunshot wounds, caused by a bullet or si%ilar projectile dri$ing into or through the body. There %ay be two wounds, one at the site of entry and one at the site of e)it, such is generally !nown as a through and through. #n a %edical conte)t, stab wounds and gunshot wounds are considered %ajor wounds. Closed *losed wounds ha$e fewer categories, but are just as dangerous as open wounds. The types of closed wounds are: Contusions, %ore co%%only !nown as bruises, caused by blunt force trau%a that da%ages tissue under the s!in. Hematomas, also called blood tu%ors, caused by da%age to a blood $essel that in turn causes blood to collect under the s!in. Crushing injuries, caused by a great or e)tre%e a%ount of force applied o$er a long period of ti%e.
Healing To heal a wound, the body underta!es a series of actions collecti$ely !nown as the wound healing process. Infection +acterial infection of wound can i%pede the healing process and lead to life threatening co%plications. ,cientists at ,heffield -ni$ersity ha$e identified a way of using light to rapidly detect the presence of bacteria. They are de$eloping a portable !it in which specially designed %olecules e%it a light signal when bound to bacteria. *urrent laboratory based detection of bacteria can ta!e hours or e$en days..1/ Cultural history 0ro% the *lassical 1eriod to the 2edie$al 1eriod, the body and the soul were belie$ed to be inti%ately connected, based on se$eral theories put forth by the philosopher 1lato. Wounds on the body were belie$ed to correlate with wounds to the soul and $ice $ersa3 wounds were seen as an outward sign of an inward illness. Thus, a %an who was wounded physically in a serious way was said to be hindered not only physically but spiritually as well. #f the soul was wounded, that wound %ay also e$entually beco%e physically %anifest, re$ealing the true state of the soul..2/ Wounds were also seen as writing on the 4tablet4 of the body. Wounds gotten in war, for e)a%ple, told the story of a soldier in a for% which all could see and understand, and the wounds of a %artyr told the story of their faith..2/
Anda mungkin juga menyukai
- Decubitus UlcerDokumen8 halamanDecubitus UlcerDanilo EspinoBelum ada peringkat
- Decubitus UlcerDokumen14 halamanDecubitus Ulcerayman100% (3)
- The Impact of Pressure Ulcers: Bony Sacrum Coccyx Heels Hips Elbows Knees Ankles CraniumDokumen48 halamanThe Impact of Pressure Ulcers: Bony Sacrum Coccyx Heels Hips Elbows Knees Ankles CraniumVanessa Camille DomingoBelum ada peringkat
- Non Healing UlcersDokumen36 halamanNon Healing UlcersIniya RajendranBelum ada peringkat
- Decubitus UlcerDokumen30 halamanDecubitus UlcerZgama AbdulrahmanBelum ada peringkat
- Bed SoresDokumen15 halamanBed Soresver_at_work100% (1)
- Assessing and Classifying Pressure SoresDokumen7 halamanAssessing and Classifying Pressure SoresAnnette Baines100% (1)
- What Is Pressure Ulcer?: Signs and SymptomsDokumen6 halamanWhat Is Pressure Ulcer?: Signs and Symptomsshenecajean carajayBelum ada peringkat
- Fracture: Signs and SymptomsDokumen6 halamanFracture: Signs and SymptomsKaran MauryaBelum ada peringkat
- Types of Wounds and Phases of HealingDokumen6 halamanTypes of Wounds and Phases of HealingAsniah Hadjiadatu AbdullahBelum ada peringkat
- Clinical Procedures for Safer Patient Wound CareDokumen50 halamanClinical Procedures for Safer Patient Wound CareJan Oliver Yares100% (2)
- Oral Ondansetron For Gastroenteritis in A Pediatric Emergency DepartmentDokumen7 halamanOral Ondansetron For Gastroenteritis in A Pediatric Emergency DepartmentshaerizzeBelum ada peringkat
- A Wound Is A Break in The Continuity of A Tissue of The BodyDokumen6 halamanA Wound Is A Break in The Continuity of A Tissue of The BodyChristine Katherine LibuitBelum ada peringkat
- Venous Ulcer: Irene Dorthy Santoso, Hanny Nilasari, Shannaz Nadia YusharyahyaDokumen13 halamanVenous Ulcer: Irene Dorthy Santoso, Hanny Nilasari, Shannaz Nadia YusharyahyaIntan CahyaBelum ada peringkat
- PE1Dokumen23 halamanPE1abbynoreen2Belum ada peringkat
- Cellulitis ThesisDokumen8 halamanCellulitis Thesisgbvjc1wy100% (2)
- Pressure UlcersDokumen5 halamanPressure UlcersAmna AliBelum ada peringkat
- Pressure Ulcers- Surgery i March 2019Dokumen63 halamanPressure Ulcers- Surgery i March 2019daniyfondoBelum ada peringkat
- Skin IntegrityDokumen56 halamanSkin IntegrityneehoshiBelum ada peringkat
- Bed Sore 48Dokumen45 halamanBed Sore 48Sedaka DonaldsonBelum ada peringkat
- Prosthesis TopicDokumen16 halamanProsthesis Topicjack sparrowBelum ada peringkat
- Plasmid Curing Response of Staphylococcus Aureus From Wound and High Vaginal SwabDokumen94 halamanPlasmid Curing Response of Staphylococcus Aureus From Wound and High Vaginal SwabElufisan TemidayoBelum ada peringkat
- What Are The Three Types of Wound Healing? Define Each TypeDokumen2 halamanWhat Are The Three Types of Wound Healing? Define Each TypeKing Aldus ConstantinoBelum ada peringkat
- 2 Skin-IntegrityDokumen74 halaman2 Skin-IntegrityFlourence ZafranBelum ada peringkat
- Decision Summary: Decision Memo For Electrostimulation For Wounds (CAG-00068N)Dokumen28 halamanDecision Summary: Decision Memo For Electrostimulation For Wounds (CAG-00068N)omboBelum ada peringkat
- The Diabetic Foot: Current Problems in SurgeryDokumen30 halamanThe Diabetic Foot: Current Problems in SurgeryBolivar IseaBelum ada peringkat
- Prevent Pressure Ulcers with Proper Skin Care, Repositioning and Support SurfacesDokumen6 halamanPrevent Pressure Ulcers with Proper Skin Care, Repositioning and Support SurfacesasuratosBelum ada peringkat
- Hips Back Ankles Buttocks HeelsDokumen13 halamanHips Back Ankles Buttocks Heelsفرزدق الحسيناويBelum ada peringkat
- Wounds: DR - Mohanned A LshalahDokumen4 halamanWounds: DR - Mohanned A Lshalahjohana_6647Belum ada peringkat
- Stasis Dermatitis: An Overview of Its Clinical Presentation, Pathogenesis, and ManagementDokumen12 halamanStasis Dermatitis: An Overview of Its Clinical Presentation, Pathogenesis, and ManagementNydia OngaliaBelum ada peringkat
- Question Answer of Surgery Mbbs Supplementary 1st Paper CDokumen296 halamanQuestion Answer of Surgery Mbbs Supplementary 1st Paper CShivam AgarwalBelum ada peringkat
- Types of WoundsDokumen4 halamanTypes of WoundsHanarisha Putri AzkiaBelum ada peringkat
- First Aid Notes: Wounds, Bleeding, and Chest InjuriesDokumen40 halamanFirst Aid Notes: Wounds, Bleeding, and Chest InjuriesGo andWatchBelum ada peringkat
- Bleeding & WoundsDokumen28 halamanBleeding & WoundsSemo SupraBelum ada peringkat
- CAPE Biology Unit 2 ProjectDokumen13 halamanCAPE Biology Unit 2 ProjectAudi Sweetangel0% (1)
- It Does More Than Help Save LivesDokumen14 halamanIt Does More Than Help Save LivesJade ElleneBelum ada peringkat
- Complications From Fractures. Information and Treatment - PatientDokumen11 halamanComplications From Fractures. Information and Treatment - PatientBahy A. El-agouzBelum ada peringkat
- ReportDokumen30 halamanReportNeisha Halil VillarealBelum ada peringkat
- DR Mohit Gulati (PT)Dokumen62 halamanDR Mohit Gulati (PT)Shubha DiwakarBelum ada peringkat
- SJMCR 3111056 1058 PDFDokumen3 halamanSJMCR 3111056 1058 PDFDicky HardiBelum ada peringkat
- 45 Necrotising FasciitisDokumen17 halaman45 Necrotising FasciitisJasna MeenangadiBelum ada peringkat
- Review of Literature-1Dokumen39 halamanReview of Literature-1soumya ranjan ranaBelum ada peringkat
- The Dangers of Faecal Incontinence in The At-Risk PatientDokumen6 halamanThe Dangers of Faecal Incontinence in The At-Risk PatientRicardo BalauBelum ada peringkat
- Pressure Ulcers and Decubitus Patients: Iliadis Christos, Mihalache Anca, Dimitriadou AlexandraDokumen3 halamanPressure Ulcers and Decubitus Patients: Iliadis Christos, Mihalache Anca, Dimitriadou AlexandraerpublicationBelum ada peringkat
- Medicinal Plants for Wound Healing ReviewDokumen11 halamanMedicinal Plants for Wound Healing ReviewyraghavendraBelum ada peringkat
- The Investigation of Wound Healing DisordersDokumen15 halamanThe Investigation of Wound Healing DisordersRadulescu IonelaBelum ada peringkat
- Casestudy OsteomyelitisDokumen52 halamanCasestudy OsteomyelitisMJ Amarillo84% (19)
- NCM 109 LP2Sabio Jeanette B.Dokumen20 halamanNCM 109 LP2Sabio Jeanette B.Alyssa DagandanBelum ada peringkat
- Wound CareDokumen27 halamanWound Carepedrovsky702Belum ada peringkat
- Skin Integrity Wound CareDokumen93 halamanSkin Integrity Wound CarePaul DeliyosBelum ada peringkat
- PBL 4Dokumen4 halamanPBL 4Victor VBelum ada peringkat
- Diabetic FoootDokumen34 halamanDiabetic Foootsiakonihmat433Belum ada peringkat
- Wound AssessmentDokumen14 halamanWound AssessmentMah ShawdBelum ada peringkat
- A Stroke or Cerebrovascular Accident and CellulitisDokumen3 halamanA Stroke or Cerebrovascular Accident and CellulitisCjhay Polintan ParasoBelum ada peringkat
- The Care and Treatment of Skin and Soft Tissue Infections Among Injection Drug Users in The Community SettingDokumen22 halamanThe Care and Treatment of Skin and Soft Tissue Infections Among Injection Drug Users in The Community Settingapple.scotch.fool3550Belum ada peringkat
- Examples of Side Effects of Over-The-Counter Medicines: Acetaminophen TylenolDokumen4 halamanExamples of Side Effects of Over-The-Counter Medicines: Acetaminophen Tylenolまあく めんでず おるびりあBelum ada peringkat
- KalonchoeDokumen11 halamanKalonchoeCeleste MitchellBelum ada peringkat
- 4 Wounds and Wound CareDokumen25 halaman4 Wounds and Wound Caredoc-fahad aftabBelum ada peringkat
- Giatric NurseDokumen5 halamanGiatric NurseKim TanBelum ada peringkat
- UrethroplastyDokumen9 halamanUrethroplastyBayu Mario GintingBelum ada peringkat
- QSAR Modeling TechniquesDokumen35 halamanQSAR Modeling TechniquesBayu Mario GintingBelum ada peringkat
- Antibacterial Activity of Persea Cordata Stem BarksDokumen3 halamanAntibacterial Activity of Persea Cordata Stem BarksBayu Mario GintingBelum ada peringkat
- Antibacterial Activity Litsea glutinosa BarkDokumen3 halamanAntibacterial Activity Litsea glutinosa BarkBayu Mario GintingBelum ada peringkat
- Multan MushtaqDokumen53 halamanMultan MushtaqBayu Mario GintingBelum ada peringkat
- Molecular Virology - Moses P. AdogaDokumen178 halamanMolecular Virology - Moses P. AdogaDavid Orjuela100% (5)
- bc5d49f144e358e334336a6d3e691b08Dokumen5 halamanbc5d49f144e358e334336a6d3e691b08Bayu Mario GintingBelum ada peringkat
- Viral Skin Infections - RaRaDokumen15 halamanViral Skin Infections - RaRaBayu Mario GintingBelum ada peringkat
- English Days, Months, and Date.Dokumen2 halamanEnglish Days, Months, and Date.Bayu Mario GintingBelum ada peringkat
- Hannah RainaDokumen1 halamanHannah RainaBayu Mario GintingBelum ada peringkat
- Traumatic AmputationDokumen5 halamanTraumatic AmputationBayu Mario GintingBelum ada peringkat
- Pokemon Bayu MarioDokumen1 halamanPokemon Bayu MarioBayu Mario GintingBelum ada peringkat
- KARONESEDokumen6 halamanKARONESEBayu Mario GintingBelum ada peringkat
- JesusDokumen35 halamanJesusBayu Mario GintingBelum ada peringkat
- Neonatal-Perinatal Infections An UpdateDokumen215 halamanNeonatal-Perinatal Infections An Updatebromean.cubitos-0qBelum ada peringkat
- Nanoparticles in Drug Loading Encapsulation and Adsorption-2019-03-31-20-59 PDFDokumen3 halamanNanoparticles in Drug Loading Encapsulation and Adsorption-2019-03-31-20-59 PDFsara castro olayaBelum ada peringkat
- Snakebite First Aid PosterDokumen1 halamanSnakebite First Aid Postervet mhmdBelum ada peringkat
- Pathophysiology of Some GI DisordersDokumen5 halamanPathophysiology of Some GI Disordersghee05Belum ada peringkat
- Maxillary Orthognathic Procedures - PPT / Orthodontic Courses by Indian Dental AcademyDokumen53 halamanMaxillary Orthognathic Procedures - PPT / Orthodontic Courses by Indian Dental Academyindian dental academyBelum ada peringkat
- Essential Newborn Care (Enc) & Delivery Room ProtocolsDokumen95 halamanEssential Newborn Care (Enc) & Delivery Room ProtocolsEyySiEffVeeBelum ada peringkat
- Racism in Medicine: Shifting the Power from Physician to PatientDokumen3 halamanRacism in Medicine: Shifting the Power from Physician to PatientSophieBelum ada peringkat
- Fasting and Natural Diet - GoldsteinDokumen119 halamanFasting and Natural Diet - GoldsteinJavier100% (1)
- Sara Resume For PortfolioDokumen3 halamanSara Resume For Portfolioapi-662320589Belum ada peringkat
- Wuhan Lab Caught Deleting Files Proving Fauci Funding: - Story At-A-GlanceDokumen11 halamanWuhan Lab Caught Deleting Files Proving Fauci Funding: - Story At-A-GlanceTomBelum ada peringkat
- AdvaGenix Letter To MoCo 8 18Dokumen2 halamanAdvaGenix Letter To MoCo 8 18DCOH EditorBelum ada peringkat
- Chp9 Sclera DiseasesDokumen23 halamanChp9 Sclera DiseasesUchyIntamBelum ada peringkat
- Emerging Zoonoses: I. W. FongDokumen255 halamanEmerging Zoonoses: I. W. FongfdfdfdfBelum ada peringkat
- Postbasicbscnursingbook PDFDokumen216 halamanPostbasicbscnursingbook PDFSamjhana NeupaneBelum ada peringkat
- 2010, Opdam NJMDokumen6 halaman2010, Opdam NJMLucasBelum ada peringkat
- Purulent Diseases of Lungs and PleuraDokumen60 halamanPurulent Diseases of Lungs and PleuraBob BlythBelum ada peringkat
- 1107398b-09a0 - Salaam Health Claim FormDokumen2 halaman1107398b-09a0 - Salaam Health Claim FormFarhan Ali100% (1)
- Rapid Communication: Spontaneous Abortions and Policies On COVID-19 mRNA Vaccine Use During PregnancyDokumen14 halamanRapid Communication: Spontaneous Abortions and Policies On COVID-19 mRNA Vaccine Use During PregnancyStéphane BoucherBelum ada peringkat
- Marik Covid Protocol SummaryDokumen2 halamanMarik Covid Protocol Summarysimodino100% (6)
- A45 - Varanasi Lab-3 Varanasi Lab-3: Patientreportscsuperpanel - General - Panel - Analyte - SC (Version: 6)Dokumen4 halamanA45 - Varanasi Lab-3 Varanasi Lab-3: Patientreportscsuperpanel - General - Panel - Analyte - SC (Version: 6)Akash Kumar NigamBelum ada peringkat
- Nursing Process: Mr. Binu Babu M.Sc. (N) Assistant Professor Mrs. Jincy Binu M.Sc. (N) LecturerDokumen83 halamanNursing Process: Mr. Binu Babu M.Sc. (N) Assistant Professor Mrs. Jincy Binu M.Sc. (N) LecturerSAJIDA100% (1)
- Curriculum Vitae SteffyDokumen4 halamanCurriculum Vitae Steffyapi-551787505Belum ada peringkat
- Research BSN3G SetA Group1FINALDokumen75 halamanResearch BSN3G SetA Group1FINALRachelle DelantarBelum ada peringkat
- Fetal Growth Restriction FGRDokumen57 halamanFetal Growth Restriction FGRDewa Made Sucipta PutraBelum ada peringkat
- AAHA Canine Vaccination GuidelinesDokumen23 halamanAAHA Canine Vaccination GuidelinesRaniah DahlanBelum ada peringkat
- Patient Admission (Penerimaan Pasien)Dokumen4 halamanPatient Admission (Penerimaan Pasien)Juan KrismanaBelum ada peringkat
- Job Stress and Mental Health Among PolicDokumen9 halamanJob Stress and Mental Health Among PolicJay GalangBelum ada peringkat
- Global Leprosy StrategyDokumen36 halamanGlobal Leprosy StrategyBlue PielagoBelum ada peringkat
- Stress Testing of Drug SubstancesDokumen29 halamanStress Testing of Drug SubstancesMr. HIMANSHU PALIWALBelum ada peringkat
- Viral Triggering of Anti-NMDA Receptor Encephalitis in a ChildDokumen4 halamanViral Triggering of Anti-NMDA Receptor Encephalitis in a ChildPyaePhyoAungBelum ada peringkat