Protocol Picior
Diunggah oleh
Ioana Temeliescu Ex ZamfirDeskripsi Asli:
Hak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Protocol Picior
Diunggah oleh
Ioana Temeliescu Ex ZamfirHak Cipta:
Format Tersedia
Red Flags for Potential Serious Conditions in Patients with Knee, Leg, Ankle or Foot Problems Medical Screening
for the Knee, Leg, Ankle or Foot Region
Condition Fractures1-4 Red Flag Data obtained during Interview/History History of recent trauma: crush injury, MVA, falls from heights, or sports injuries Osteoporosis in the elderly Age > 55 years old History of type II diabetes History of ischemic heart disease Smoking history Sedentary lifestyle Co-occurring intermittent claudication Recent surgery, malignancy, pregnancy, trauma, or leg immobilization Red Flag Data obtained during Physical Exam Joint effusion and hemarthorsis Bruising, swelling, throbbing pain, and point tenderness over involved tissues Unwillingness to bear weight on involved leg Unilaterally cool extremity (may be bilateral if aorta is site of occlusion) Prolonged capillary refill time (>2 sec) Decreased pulses in arteries below the level of the occlusion Prolonged vascular filling time Ankle Brachial index < 0.90 Calf pain, edema, tenderness, warmth Calf pain that is intensified with standing or walking and relieved by rest and elevation Possible pallor and loss of dorsalis pedis pulse History of blunt trauma, crush Severe, persistent leg pain that is intensified with injury - or stretch applied to involved muscles Recent participation in a rigorous, Swelling, exquisite tenderness and palpable unaccustomed exercise or tension/hardness of involved compartment training activity Paresthesia, paresis, and pulselessness History of recent infection, surgery, Constant aching and/or throbbing pain, joint or injection swelling, tenderness, warmth Coexisting immunosuppressive May have an elevated body temperature disorder History of recent skin ulceration or Pain, skin swelling, warmth and an advancing, abrasion, venous insufficiency, irregular margin of erythema/reddish streaks CHF, or cirrhosis Fever, chills, malaise and weakness History of diabetes mellitus
Peripheral Arterial Occlusive Disease5-9
Deep Vein Thrombosis10,11,17
Compartment Syndrome12-14
Septic Arthritis15
Cellulitis16
References: 1. Judd DB, Kim DH. Foot fractures misdiagnosed as ankle sprains. Am Fam Physician. 2002;68:785-794. 2. Hatch RL, Hacking S. Evaluation and management of toe fractures. Am Fam Physician. 2002;68:2413-2418. 3. Hasselman CT, et al. Foot and ankle fractures in elderly white woman. J of Bone Joint Surg. 2003;85:820-824. 4. Rammelt S, Zwipp H. Calcaneus fractures: facts, controversies, and recent developments. Injury. 2004;35:443-461. 5. Boyko EJ, et al. Diagnostic utility of the history and physical examination for peripheral vascular disease among patients with diabetes mellitus. Journal of Clinical Epidemiology. 1997;50:659-668. 6. McGee SR, Boyko EJ. Physical examination and chronic lower-extremity ischemia: a critical review. Arch Intern Med. 1998;158:1357-1364. 7. Halperin, JL. Evaluation of patients with peripheral vascular disease. Thrombosis Research. 2002;106:V303-11. 8. Hooi JD, Stoffers HE, Kester AD, et al. Risk factors and cardiovascular diseases associated with asymptomatic peripheral occlusive vascular disease. Scand J Prim Health Care. 1998;16:177-182. 9. Leng, GC, et al. Use of ankle brachial pressure index to predict cardiovascular events and death: a cohort study. BMJ. 1996;313:1440-79. 10. Constans J, et al. Comparison of four clinical prediction scores for the diagnosis of lower limb deep venous thrombosis in outpatients. Amer J Med. 2003;115:436-440. 11. Bustamante S, Houlton, PG. Swelling of the leg, deep venous thrombosis and the piriformis syndrome. Pain Res Manag. 2001;6:200-203. 12. Bourne RB, Rorabeck CH. Compartment syndromes of the lower leg. Clin Orthop. 1989;240:97-104. 13. Swain R. Lower extremity compartment syndrome: when to suspect pressure buildup. Postgraduate Medicine. 1999:105. 14. Ulmer T. The clinical diagnosis of compartment syndrome of the lower leg: are clinical findings predictive of the disorder. Orthop Trauma. 2002;16:572-577. 15. Gupta MN, et al. A prospective 2-year study of 75 patients with adult-onset septic arthritis. Rheumatology. 2001;40:24-30. 16. Stulberg D, Penrod M, Blatny R: Common bacterial skin infections. Am Fam Physician. 2002; 66:119-124. 17. Riddle DL, et al. Diagnosis of lower-extremity deep vein thrombosis in outpatients with musculoskeletal disorders: a national survey study of physical therapists. Phys Ther. 2004; 84 (8): 717-728.
Robert Klingman PT, Joe Godges PT KP SoCal Ortho PT Residency
KNEE/LEG/ANKLE/FOOT SCREENING QUESTIONNAIRE
NAME: ________________________________________ Medical Record #: _________________________ DATE: _____________
Yes 1. Have you recently experienced a trauma, such as a vehicle accident, a fall from a height, or a sports injury? 2. Have you recently had a fever? 3. Have you recently taken antibiotics or other medicines for an infection? 4. Have you had a recent surgery? 5. Have you had a recent injection to one or more of your joints? 6. Have you recently had a cut, scrape, or open wound? 7. Do you have diabetes? 8. Have you been diagnosed as having an immunosuppressive disorder? 9. Do you have a history of heart trouble? 10. Do you have a history of cancer? 11. Have you recently taken a long car ride, bus trip, or plane flight? 12. Have you recently been bedridden for any reason? 13. Have you recently begun a vigorous physical training program? 14. Do you have groin, hip, thigh or calf aching or pain that increases with physical activity, such as walking or running? 15. Have you recently sustained a blow to your shin or any other trauma to either of your legs?
No
Joe Godges DPT
KP SoCal Ortho PT Residency
Normal Gait Mechanics
Normal Gait Patterns Have Two Major Periods: 1. Double Limb Support: a) weight loading b) weight unloading 2. Single Limb Support: a) stance phase of ipsilateral side b) swing phase of contralateral side
DOUBLE LIMB SUPPORT WEIGHT UNLOADING: Phases: Trailing foot is rolling off floor when heel rises when 1st MTP rolls off floor Pre-Swing Max. plantarflexion (20 o) Flexes to approx. 40o Flexes to approx. 0o (neutral) Less anterior rotation Begin anterior elevation Aligned towards wt. loading leg
Terminal Stance: Pre-Swing:
Joint Motions: Ankle Knee Hip Pelvis Trunk
Terminal Stance Heel rise Full extension Max. extension (20o) Relative anterior rotation Posterior depression Aligned between legs
WEIGHT LOADING: Phases:
Weight is transferred to contralateral leg Initial Contact: Loading Response: when heel contacts floor when sole of foot contacts floor
Joint Motions Ankle Knee Hip Pelvis Trunk
Initial Contact Neutral Knee extended Flexed 25o Level Aligned between legs
Loading Response Plantarflexes 10o Knee flexes 15o Stable 25o flexion Relative abduction Lateral drop to swing leg Aligned towards wt. bearing leg
Joe Godges DPT
Anda mungkin juga menyukai
- Physical Therapy ProtocolsDokumen852 halamanPhysical Therapy Protocolspickach83% (6)
- 01MedicalScreening KneeLegAnkleandFootRegions PDFDokumen1 halaman01MedicalScreening KneeLegAnkleandFootRegions PDFShaun TylerBelum ada peringkat
- Physical Therapy Protocols For Ankle and Foot ConditionsDokumen116 halamanPhysical Therapy Protocols For Ankle and Foot ConditionstinadasilvaBelum ada peringkat
- Physical Therapy Protocols - Knee ConditionsDokumen120 halamanPhysical Therapy Protocols - Knee Conditionssayles4174100% (1)
- Physical Therapy Protocols For The Conditions of Hip RegionDokumen50 halamanPhysical Therapy Protocols For The Conditions of Hip RegionAnita GajariBelum ada peringkat
- Ankle PainnDokumen4 halamanAnkle PainngoodlucksonkiloBelum ada peringkat
- Musculoskeletal TraumaDokumen70 halamanMusculoskeletal Traumavincee_08Belum ada peringkat
- 2the Limping Child-JoaDokumen51 halaman2the Limping Child-JoaQasem RababahBelum ada peringkat
- Limping 12.10.2018Dokumen32 halamanLimping 12.10.2018Emily Eresuma100% (1)
- History Taking Orthopaedics CompleteDokumen6 halamanHistory Taking Orthopaedics CompletenorisahnirishBelum ada peringkat
- Diabetic Foot, Diabetic Foot Ulcer & Diabetic Foot Care: Prepared by Munirah Supervised by DR NaqibDokumen49 halamanDiabetic Foot, Diabetic Foot Ulcer & Diabetic Foot Care: Prepared by Munirah Supervised by DR NaqibAfifah SelamatBelum ada peringkat
- RHEUMATOID ARTHRITIS DR DON J SCOTT BERIN G BHMS (MEDICAL OFFICER) PDFDokumen6 halamanRHEUMATOID ARTHRITIS DR DON J SCOTT BERIN G BHMS (MEDICAL OFFICER) PDFDr-Don JamesScott BerinGraceBelum ada peringkat
- Total Knee Replacement: Done By: Sajeda Moha'dDokumen27 halamanTotal Knee Replacement: Done By: Sajeda Moha'dlolo223Belum ada peringkat
- Part IIDokumen64 halamanPart IIhussainBelum ada peringkat
- HistoryandPhysicalExamDokumen105 halamanHistoryandPhysicalExamsilentscream0618Belum ada peringkat
- Robert J. Snyder, DPM, MSC, Cws Professor and Director of Clinical Research Barry University SPMDokumen108 halamanRobert J. Snyder, DPM, MSC, Cws Professor and Director of Clinical Research Barry University SPMddBelum ada peringkat
- Prepared By: Edwin Jonathan A. Manlapas, DDM, R.NDokumen726 halamanPrepared By: Edwin Jonathan A. Manlapas, DDM, R.NQuolette ConstanteBelum ada peringkat
- Coxa PlanaDokumen9 halamanCoxa PlanaRegine BlanzaBelum ada peringkat
- Closed Fracture of Midshaft Femur FracturesDokumen33 halamanClosed Fracture of Midshaft Femur FracturesLana AdilaBelum ada peringkat
- Sudden Onset Leg PainDokumen16 halamanSudden Onset Leg PainNafisNomanBelum ada peringkat
- Concomitant PAD and CADDokumen96 halamanConcomitant PAD and CADric_vir_014Belum ada peringkat
- 58 Cases History and Physical Exam BookDokumen102 halaman58 Cases History and Physical Exam BookeleazarmdBelum ada peringkat
- Red FlagsDokumen2 halamanRed FlagsHeidiBelum ada peringkat
- Osteoarthritis 2018Dokumen71 halamanOsteoarthritis 2018title1989Belum ada peringkat
- TetrapareseDokumen38 halamanTetraparesemariamunsriBelum ada peringkat
- FMcase 10Dokumen14 halamanFMcase 10Ryan TownsendBelum ada peringkat
- Prosthesis in Below Knee Amputation and Gait TrainingDokumen34 halamanProsthesis in Below Knee Amputation and Gait TrainingSonal Khera100% (1)
- Fever PresentationDokumen10 halamanFever Presentationapi-555392359Belum ada peringkat
- Popliteal Artery Entrapement SyndromeDokumen29 halamanPopliteal Artery Entrapement SyndromeShahzaib AslamBelum ada peringkat
- Musculoskeletal TraumaDokumen63 halamanMusculoskeletal Traumarobby pardiansyahBelum ada peringkat
- Musculoskeletal Disorders Care of Client With Fall 2005Dokumen41 halamanMusculoskeletal Disorders Care of Client With Fall 2005mara5140100% (3)
- Clinical Examination of The Knee: DR John EbnezarDokumen95 halamanClinical Examination of The Knee: DR John EbnezarsandeepBelum ada peringkat
- Knee Pain Answers by Tessa LaiDokumen3 halamanKnee Pain Answers by Tessa LaitessalaiBelum ada peringkat
- Development of Shoulder Rehabilitation GuidelinesDokumen3 halamanDevelopment of Shoulder Rehabilitation GuidelinessugoimanBelum ada peringkat
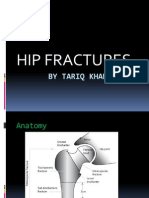
- Hip Fractures: by Tariq KhanDokumen42 halamanHip Fractures: by Tariq KhanKamran Khan KhalilBelum ada peringkat
- Case Presentations in Arterial DiseaseDari EverandCase Presentations in Arterial DiseasePenilaian: 5 dari 5 bintang5/5 (1)
- Plantar Heel Pain, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsDari EverandPlantar Heel Pain, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsBelum ada peringkat
- The Good Foot Book: A Guide for Men, Women, Children, Athletes, Seniors - EveryoneDari EverandThe Good Foot Book: A Guide for Men, Women, Children, Athletes, Seniors - EveryoneBelum ada peringkat
- Correct Your Pelvis and Heal Your Back-pain: The Self-Help Manual for Alleviating Back-Pain and Other Musculo-Skeletal Aches and PainsDari EverandCorrect Your Pelvis and Heal Your Back-pain: The Self-Help Manual for Alleviating Back-Pain and Other Musculo-Skeletal Aches and PainsBelum ada peringkat
- ABC of Orthopaedics and TraumaDari EverandABC of Orthopaedics and TraumaKapil SugandBelum ada peringkat
- Polymyalgia Rheumatica, A Simple Guide To The Condition, Treatment And Related DiseasesDari EverandPolymyalgia Rheumatica, A Simple Guide To The Condition, Treatment And Related DiseasesPenilaian: 5 dari 5 bintang5/5 (2)
- Posterior Tibial Tendon Dysfunction, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsDari EverandPosterior Tibial Tendon Dysfunction, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsPenilaian: 5 dari 5 bintang5/5 (1)
- Correct Your Pelvis and Heal your Back-Pain: The Self-Help Manual for Alleviating Back-Pain and other Musculo-Skeletal Aches and PainsDari EverandCorrect Your Pelvis and Heal your Back-Pain: The Self-Help Manual for Alleviating Back-Pain and other Musculo-Skeletal Aches and PainsBelum ada peringkat
- The Perrin Technique 2nd edition: How to diagnose and treat chronic fatigue syndrome/ME and fibromyalgia via the lymphatic drainage of the brainDari EverandThe Perrin Technique 2nd edition: How to diagnose and treat chronic fatigue syndrome/ME and fibromyalgia via the lymphatic drainage of the brainPenilaian: 5 dari 5 bintang5/5 (1)
- Exercise Physiology for the Pediatric and Congenital CardiologistDari EverandExercise Physiology for the Pediatric and Congenital CardiologistBelum ada peringkat
- Orthopedics Notes for Medical StudentsDari EverandOrthopedics Notes for Medical StudentsPenilaian: 4.5 dari 5 bintang4.5/5 (3)
- Sports Injuries of the Foot: Evolving Diagnosis and TreatmentDari EverandSports Injuries of the Foot: Evolving Diagnosis and TreatmentBelum ada peringkat
- The Thoracic Outlet Syndrome, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsDari EverandThe Thoracic Outlet Syndrome, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsBelum ada peringkat
- Postural Tachycardia Syndrome: A Concise and Practical Guide to Management and Associated ConditionsDari EverandPostural Tachycardia Syndrome: A Concise and Practical Guide to Management and Associated ConditionsNicholas GallBelum ada peringkat
- Hip Osteonecrosis A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsDari EverandHip Osteonecrosis A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsBelum ada peringkat
- The Return of The Facelift: Accessing The Healing Power of The Vagus Nerve by Stanley RosenbergDokumen1 halamanThe Return of The Facelift: Accessing The Healing Power of The Vagus Nerve by Stanley RosenbergIoana Temeliescu Ex ZamfirBelum ada peringkat
- Cjo Journal Revised-2Dokumen32 halamanCjo Journal Revised-2Ioana Temeliescu Ex ZamfirBelum ada peringkat
- Acceptable Usage Policy Acknowledgement v1 3Dokumen1 halamanAcceptable Usage Policy Acknowledgement v1 3Ioana Temeliescu Ex ZamfirBelum ada peringkat
- Psoas PDF 1Dokumen17 halamanPsoas PDF 1Ioana Temeliescu Ex ZamfirBelum ada peringkat
- Teste UmarDokumen30 halamanTeste UmarIoana Temeliescu Ex Zamfir100% (2)
- Joe Godges PT, Robert Klingman PT Loma Linda U DPT Program Kpsocal Ortho PT ResidencyDokumen3 halamanJoe Godges PT, Robert Klingman PT Loma Linda U DPT Program Kpsocal Ortho PT ResidencyIoana Temeliescu Ex ZamfirBelum ada peringkat
- Normal Gait Mechanics: Weight UnloadingDokumen4 halamanNormal Gait Mechanics: Weight UnloadingIoana Temeliescu Ex ZamfirBelum ada peringkat
- 2011 Japanese RoundtableDokumen6 halaman2011 Japanese RoundtableIoana Temeliescu Ex ZamfirBelum ada peringkat
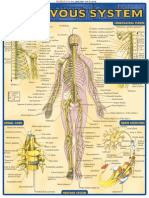
- Study Nervous SystemDokumen2 halamanStudy Nervous SystemIoana Temeliescu Ex Zamfir100% (4)
- Today's Physical Therapist:: A Comprehensive Review of A 21st-Century Health Care ProfessionDokumen140 halamanToday's Physical Therapist:: A Comprehensive Review of A 21st-Century Health Care ProfessionVishal ParnerkarBelum ada peringkat
- Declaratie: Subsemnata (Ul) Reprezentant Legal Al SCDokumen1 halamanDeclaratie: Subsemnata (Ul) Reprezentant Legal Al SCIoana Temeliescu Ex ZamfirBelum ada peringkat
- Angle Grinder Gws 7 100 06013880f0Dokumen128 halamanAngle Grinder Gws 7 100 06013880f0Kartik ParmeshwaranBelum ada peringkat
- Virtual Assets Act, 2022Dokumen18 halamanVirtual Assets Act, 2022Rapulu UdohBelum ada peringkat
- SyncopeDokumen105 halamanSyncopeJohn DasBelum ada peringkat
- Famous Little Red Book SummaryDokumen6 halamanFamous Little Red Book SummaryMatt MurdockBelum ada peringkat
- Toh MFS8B 98B 003-11114-3AG1 PDFDokumen92 halamanToh MFS8B 98B 003-11114-3AG1 PDFDmitry NemtsoffBelum ada peringkat
- Seabank Statement 20220726Dokumen4 halamanSeabank Statement 20220726Alesa WahabappBelum ada peringkat
- 2 To 20 Years - Girls Stature-For-Age and Weight-For-Age PercentilesDokumen1 halaman2 To 20 Years - Girls Stature-For-Age and Weight-For-Age PercentilesRajalakshmi Vengadasamy0% (1)
- Data Sheet Eldar Void SpinnerDokumen1 halamanData Sheet Eldar Void SpinnerAlex PolleyBelum ada peringkat
- DFo 2 1Dokumen15 halamanDFo 2 1Donna HernandezBelum ada peringkat
- All Day Breakfast: .Served With Cappuccino or Espresso or Lime Juice or TeaDokumen7 halamanAll Day Breakfast: .Served With Cappuccino or Espresso or Lime Juice or TeaBryan KuoKyBelum ada peringkat
- BLP#1 - Assessment of Community Initiative (3 Files Merged)Dokumen10 halamanBLP#1 - Assessment of Community Initiative (3 Files Merged)John Gladhimer CanlasBelum ada peringkat
- Ci Thai RiceDokumen4 halamanCi Thai RiceMakkah Madina riceBelum ada peringkat
- Elpodereso Case AnalysisDokumen3 halamanElpodereso Case AnalysisUsama17100% (2)
- To Find Fatty Material of Different Soap SamplesDokumen17 halamanTo Find Fatty Material of Different Soap SamplesRohan Singh0% (2)
- 1B20 40Dokumen4 halaman1B20 40Electrival TcatallerBelum ada peringkat
- Modern School For SaxophoneDokumen23 halamanModern School For SaxophoneAllen Demiter65% (23)
- Network Fundamentas ITEC90Dokumen5 halamanNetwork Fundamentas ITEC90Psychopomp PomppompBelum ada peringkat
- Dominion Wargame RulesDokumen301 halamanDominion Wargame Rules4544juutf100% (4)
- General Chemistry 2 Q1 Lesson 5 Endothermic and Exotheric Reaction and Heating and Cooling CurveDokumen19 halamanGeneral Chemistry 2 Q1 Lesson 5 Endothermic and Exotheric Reaction and Heating and Cooling CurveJolo Allexice R. PinedaBelum ada peringkat
- 07 GDL Web-Site 04 (2021-2022) For 15284Dokumen2 halaman07 GDL Web-Site 04 (2021-2022) For 15284ABCDBelum ada peringkat
- Facebook: Daisy BuchananDokumen5 halamanFacebook: Daisy BuchananbelenrichardiBelum ada peringkat
- (Campus of Open Learning) University of Delhi Delhi-110007Dokumen1 halaman(Campus of Open Learning) University of Delhi Delhi-110007Sahil Singh RanaBelum ada peringkat
- Disclosure To Promote The Right To InformationDokumen11 halamanDisclosure To Promote The Right To InformationnmclaughBelum ada peringkat
- ALE Manual For LaserScope Arc Lamp Power SupplyDokumen34 halamanALE Manual For LaserScope Arc Lamp Power SupplyKen DizzeruBelum ada peringkat
- Maritime Academy of Asia and The Pacific-Kamaya Point Department of AcademicsDokumen7 halamanMaritime Academy of Asia and The Pacific-Kamaya Point Department of Academicsaki sintaBelum ada peringkat
- GE 7 ReportDokumen31 halamanGE 7 ReportMark Anthony FergusonBelum ada peringkat
- Hydraulic Mining ExcavatorDokumen8 halamanHydraulic Mining Excavatorasditia_07100% (1)
- A Noble Noose of Methods - ExtendedDokumen388 halamanA Noble Noose of Methods - ExtendedtomasiskoBelum ada peringkat
- Trade MarkDokumen2 halamanTrade MarkRohit ThoratBelum ada peringkat
- Case Study - Kelompok 2Dokumen5 halamanCase Study - Kelompok 2elida wenBelum ada peringkat