Dr. Kirti Kumsowar - 6
Diunggah oleh
Diah Ayu SulistyowatiHak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Dr. Kirti Kumsowar - 6
Diunggah oleh
Diah Ayu SulistyowatiHak Cipta:
Format Tersedia
Case Report
Ocular prosthesis: Patient rehabilitation - A Case Reprot
Kirti Somkuwar, Robin Mathai, *Panambily Jose
Department of Prosthodontics, * Department of Oral Medicine, Peoples College of Dental Sciences & Research Centre, Peoples Campus Bhanpur, Bhopal - 462037 (M.P.)
Abstract:
The loss of the facial structures can have a physical, social and psychological impact on those affected .Maxillofacial prostheses which restore and replace stomatognathic and associated facial structures with artificial substitutes, aim to improve the patient aesthetics, restore and maintain health of the remaining structures and consequently provide physical and mental well being. Accurate impressions of these tissues facilitate a close adaptation of the custom prosthesis to the tissue bed resulting in better potential for movement by the patient. Treatment of such cases includes implants and acrylic eye prosthesis. Due to economic factors it may not be advisable in all patients. A custom-made ocular prosthesis is a good alternative. A case of a custom-made ocular acrylic prosthesis is presented here, which had acceptable fit, retention and esthetics.
Key Words: Maxillofacial prosthesis, stomatognathic, scleral shell prosthesis. Introduction:
The disfigurement associated with the loss of an eye can cause significant physical and emotional problems (Lubkin & Solan, 1990). The rehabilitation of a patient who has suffered the psychological trauma of an ocular loss requires a prosthesis that will provide the optimum cosmetic and functional result. Refinement in the details of custom made ocular construction has produced a superior restoration delivered more readily. An ocular prosthetic does not provide vision; this would be a visual prosthetic. Someone with an ocular prosthesis is totally blind on the affected side and has monocular (one sided) vision which affects depth perception. The Scleral Shell Prosthesis is a thin hard acrylic shell-like artificial eye. This type of eye prosthesis is worn over a damaged, disfigured eye or eviscerated globe. The Shell Prosthesis covers the entire surface of the eye, restoring it to a natural appearance. In most cases, there is no surgery involved in obtaining the Scleral Shell Prosthesis. The fitting process involves making an impression of the cosmetically blemished eye. This will allow the Ocularist to create an anatomically correct and comfortable prosthesis. An impression fit shell will also provide maximum comfort, movement, and wearing time.
----------------------------------------------------------------------------Corresponding Author: Dr.Kirti Somkuwar, Old jail complex Arera hills, Jhangribad, Bhopal-462004, M.P. Phone No : 9981833467 E-mail .: kirtisomkuwar@gmail.com, Peoples Journal of Scientific Research 21
Before starting the design of the prosthesis, it is essential to assess the psychological component in order to gain the confidence of the patient, in addition to a detailed medical history that includes the condition that led to the excision and enucleation in order to alert the possibility of recurrence (Cain, 1982).
A Brief History of Ocular Prosthesis:
The art of making artificial eyes has been practiced since ancient times. Egyptian priests made the first ocular prosthesis, called Ectblepharons, as early as the 5th century BC. In those days, artificial eyes were made of enameled metal or painted clay and attached to cloth and worn outside the socket. The first in-socket artificial eye made in the th 15 century was made of gold with coloured enamel. In the latter part of the 16th century, the Venetian glass artisans discovered a formula that could be tolerated inside the eye socket. These early glass eyes were crude, uncomfortable to wear and very fragile. Today the vast majority of patients all around the world wear ocular prosthesis made of acrylic. Several techniques have been used in fitting and fabricating artificial eyes. Empirically fitting a stock eye, modifying a stock eye by making an impression of the ocular defect (Taicher et al, 1985), and the custom eye technique (Benson, 1977) are the most commonly used techniques. The fabrication of a custom acrylic resin eye provides more esthetic and gives precise results
Vol.2(2), July 2009
Ocular prosthesis: Patient rehabilitation--------------------------------------K Somkuwar, R Mathai & P Jose
because an impression establishes the defect contours, and the iris and the sclera are custom fabricated and painted. Keeping these in mind we at the Department of Prosthodontics, Peoples College of Dental Sciences & Research Centre successfully rehabilitated a patient for an ocular prosthesis of which the case description is as follows:
Case report:
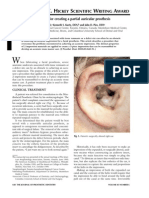
A 62 year old female patient reported in the Department of Prosthodontics, with the chief complaint of difference in colour with the present artificial eye and its impingement while she was wearing it during the night (Fig. I). She had lost her right eye as a result of an episode of chickenpox at the age of 6-7 years. She had her first artificial eye constructed at the age of 25years. Since then she has changed her prosthesis thrice and the one which she was wearing at the time of presenting to our Depratment was 2 years old.
Fig. II: Photograph showing the ocular defect of the patient.
Procedure:
Primary impression: Sykes (1996) used medium viscosity polyvinyl siloxane impression material. A modification of the technique described by Taicher et al (1985) was performed by Sykes. We used the same basic technique in this case. The patients eye socket was coated with a thin layer of vaseline and an impression was made using medium body addition silicone impression material (Fig. III). Impression was made by injecting the material first into the depth below the upper eye lid and then into the lower .This was done so as to record the proper extensions of the defect. After that the whole eye socket was filled with material and the patient was asked to close her eye so that the excess material could flow
Fig. I: Photograph showing patient with previous prosthesis.
On examination of the defective eye socket it was found that she had a defect with a shrunken orbit and intact tissue bed (Fig. II).
Overview of construction:
Armamentarium & material included light, medium and putty consistency (additional polyvinyl siloxane) impression material (Manufacturer: Coltane/ Whaledent AG, Switzerland), the dispensing gun with a fine tip and Vaseline.
Peoples Journal of Scientific Research 22
Fig. III: Photograph showing Primary impression of the patient eye socket. Vol.2(2), July 2009
Ocular prosthesis: Patient rehabilitation--------------------------------------K Somkuwar, R Mathai & P Jose
out. Patient was then asked to move her eye to the right then to the left, then up and down and finally in a circular motion, so that the functional impression of the defect could be obtained . The impression was then retrieved when it had completely set. This impression was then invested to obtain a primary sectional cast. (Fig. IV).
Fig. VI: Photograph showing final impression of the tissue bed.
Fig. IV: Photograph showing how Primary impression was invested for special tray fabrication.
as a wash material. By this the whole extent of the defect was recorded, keeping in mind the various movements as mentioned earlier so as to achieve a functional impression of the tissue bed (Fig.VI). Acrylic sprue was attached to the tray handle to act as a sprue channel for pouring modelling wax into the mold space later on. This impression was then poured in the same manner as the primary impression except keeping in mind the handle length and position ( Fig.VII).
Fig.V: Photograph showing Special tray fabricated to make final Impression
The first half of sectional cast was poured while keeping the impression surface facing upwards and after which the indexing of the first pour was done so as to allow orientation of the second half. After complete setting the two halves of the cast were separated and a special tray with clear acrylic was fabricated, finished and polished (Fig. V). Secondary impression: This impression was made using soft putty consistency polyvinyl siloxane and light body addition silicone impression material. Firstly the gross extent of the defect was recorded with soft putty and the final impression was then made using light body
Peoples Journal of Scientific Research 23
Fig. VII: Photograph showing final impression invested from wax pattern fabrication.
Then the two halves of casts were separated and the final impression retrieved so as to keep the mold space ready for wax pattern fabrication for which molten wax was poured into the secondary cast through the sprue channel (Fig.VIII). When the wax had set the cast was separated and the wax pattern was retrieved and carved.
Vol.2(2), July 2009
Ocular prosthesis: Patient rehabilitation--------------------------------------K Somkuwar, R Mathai & P Jose
Fig. X: Photograph showing wax pattern trial. Fig.VIII: Photograph showing fabricated wax pattern.
Fig. IX: Photograph showing stock eye from which section of the iris was taken.
Fig. XI: Photograph showing iris placement.
The selection of the iris for the patient was done by trimming and modifying a commercially available stock eye which had almost matching resemblance to her unaffected natural eye (Fig. IX).
Wax pattern trial
First of all the fullness of the both palpabre and the eye socket was checked along with the extensions, this was confirmed by asking the patient to close her eyes and patient was inspected from the profile view. During tryin the iris was placed keeping in mind the symmetry with the iris of the adjacent unaffected right natural eye of the patient. To achieve this exact location, a micro tape was secured on the fore head and the midline of face was marked along with the position of the natural iris while she was looking straight ahead to a distant object (Fig. X).
Peoples Journal of Scientific Research 24
The distance was measured from the midline to the centre of the pupil of the natural eye and the same distance to the left side was marked and engraved into the wax pattern. The pattern was taken out and keeping this position in mind, the iris was placed and adjusted according to the horizontal and vertical axis (Fig.XI). Also her eye movements were checked for symmetry and function and it was found that the wax tryin moved and synchronised in harmony with the patients natural eye movements. This gave a realistic feeling and instilled confidence in the patient. Flasking After the trial of wax pattern the secondary impression cast was trimmed about the size of the flask. On to this the wax pattern was sealed and the whole assembly invested as in the case of a complete denture laboratory procedures. A handle was attached to the iris which
Vol.2(2), July 2009
Ocular prosthesis: Patient rehabilitation--------------------------------------K Somkuwar, R Mathai & P Jose
Fig. XII: Photograph showing wax pettern invested with handle attachment (acrylic stick)
porosities and gives a good finish to the prosthesis. We used long curing cycle of 4-6 hours so as to prevent the presence of any residual monomer in the prosthesis which is very essential.It prevents any untoward irritation or sensitivity and thereby rejection of the prosthesis by the patient. The eye socket is extremely sensitive and the residual conjuctiva and related structures react to any surface roughness and irregularities. Final finishing and polishing of the prosthesis Finished prosthesis requires a highly polished surface which would have a glass like finish to provide maximum adaptation and overall success of the prosthesis (Fig.XIV).
was made of cold cure acrylic so as to prevent the displacement of the iris during dewaxing. Dewaxing The second pour was poured in such a way that the handle attached to the iris was embedded into the plaster of the counter flasking. Then the dewaxing was done after the final set, taking care so that there was complete wax elimination from the mold space.
Fig. XIII: Photograph showing dewaxing of flasked wax pattern.
Fig.XIV:Photograph showing finished prothesis with characterization.
Packing and flasking This step is the most important, as it involves the characterisation of the prosthesis before packing with tooth coloured heat cured polymethylmethacrylate of appropriate shade, matching with the colour of the sclera of normal eye of the patient. A thin layer of heat cured clear acrylic was spread evenly in and around the iris. The characterisation is done so as to achieve the vitality necessary to give it a life like appearance and blend with the patients natural appearance and cosmetics. After the characterisation, the mold was packed with heat cured tooth coloured acrylic resin of appropriate shade and kept for bench curing to enable complete polymerisation and prevention of any excess unreacted monomer. This enables the minimisation of
Peoples Journal of Scientific Research 25
Fig.XV: Photograph with finished ocular prosthesis in place. Vol.2(2), July 2009
Ocular prosthesis: Patient rehabilitation--------------------------------------K Somkuwar, R Mathai & P Jose
implant replacements. Also, as discussed above, the esthetic and functional outcome of the prosthesis was far better than the stock ocular prosthesis (Cain, 1982). Although the patient cannot see with this prosthesis, it has definitely restored her self-esteem and allowed her to confidently face the world.
Bibliography:
1. Benson P: The fitting and fabrication of a custom resin artificial eye. The Journal of Prosthetic Dentistry, 1977; 38(5):532-538. 2. Cain JR: Custom Ocular Prosthetic. The Journal of Prosthetic Dentistry, 1982; 48(6):690-694. 3. Doshi PJ, Aruna B: Prosthetic management of patient with ocular defect. The Journal of Indian Posthodontic Society, 2005 :5(1): 37-38. 4. Lubkin V, Sloan S: Enucleation and psychic trauma. Advances in Ophthalmic Plastic and Reconstructive Surgery, 1990; 8:259-262. 5. Sykes LM: Custom made ocular prosthesis: A clinical report. The Journal of Prosthetic Dentistry, 1996;75(1): l-3. 6. Taicher S, Steinberg HM, Tubiana I, Sela M: Modified stock-eye ocular prosthesis. The Journal of Prosthetic Dentistry, 1985; 54(1):95-98. 7. Trawnik J R: Dallas eye Prosthetics cited from www.dallaeye.net.
Fig.XVI:Photograph showing pa tient profile view of finshed prosthesis.
. . . .
The final outcome of the prosthesis was ascertained from the satisfied look on the face of the patient and from the follow up a week later. (Fig. XV & XVI). The patient was given instruction for wearing the prosthesis and its home care protocol which is given below: Prosthesis should be handeled with care and with clean hands. Removal of Acrylic prosthesis during night is ideal. It should be soaked in an antibacterial solution to kill the surface bacteria. Routine polishing of prosthesis should be done every year to prevent deposition of protein and bacteria. Children and those living in arid climates require polishing every six month.
Discussion: A well-made and properly planned ocular prosthesis maintains its orientation when patient performs various movements. With the development of newer materials the socket can be finely recorded on which custom made ocular acrylic prosthesis (Sykes, 1996) can be fabricated with exact fit and esthetics although the prosthetic rehabilitation may be enhanced with the use of implants, can coordinate the movements with natural eye, as they are not always possible or feasible. More, over the use of stock ocular prosthesis of appropriate size and colour cannot be neglected, a custom made ocular prosthesis provide better results functionally as well as aesthetically (Doshi & Aruna, 2005).
Conclusion:
The use of custom-made ocular prosthesis has been a boon to the patients who cannot afford for the
Peoples Journal of Scientific Research 26 Vol.2(2), July 2009
Anda mungkin juga menyukai
- Eye For An Eye: Ocular Prosthesis - A Case ReportDokumen8 halamanEye For An Eye: Ocular Prosthesis - A Case ReportSkAliHassanBelum ada peringkat
- ManuscriptDokumen3 halamanManuscriptAbhishek Kumar GuptaBelum ada peringkat
- Ocular Prosthesis BhavanDokumen58 halamanOcular Prosthesis BhavanDrkvpratheep Pratheep100% (1)
- JSD 2 56Dokumen5 halamanJSD 2 56Swapnil RastogiBelum ada peringkat
- Ocular ProsthesisDokumen3 halamanOcular ProsthesisAmar BhochhibhoyaBelum ada peringkat
- An Innovative Technique For Fabricating A CustomMade Ocular Prosthesis in A Pediatric Patient A Case ReportDokumen4 halamanAn Innovative Technique For Fabricating A CustomMade Ocular Prosthesis in A Pediatric Patient A Case ReportInternational Journal of Innovative Science and Research TechnologyBelum ada peringkat
- Sculpting The Eye Prosthetic Rehabilitation FollowDokumen5 halamanSculpting The Eye Prosthetic Rehabilitation Followisichelichukwutem3Belum ada peringkat
- Ocular ProsthesisDokumen80 halamanOcular ProsthesisPriyaAgrawalBelum ada peringkat
- Orbital ProsthesisDokumen5 halamanOrbital ProsthesisdrsmritiBelum ada peringkat
- IJISRT20JAN543Dokumen3 halamanIJISRT20JAN543International Journal of Innovative Science and Research TechnologyBelum ada peringkat
- Partial Auricular ProsthesisDokumen4 halamanPartial Auricular ProsthesisdrsmritiBelum ada peringkat
- A Simplified Method For The Fabrication of Obturator:a Case ReportDokumen4 halamanA Simplified Method For The Fabrication of Obturator:a Case ReportinventionjournalsBelum ada peringkat
- Management of Phthisis Bulbi Patient with Scleral Cover Shell ProsthesisDokumen4 halamanManagement of Phthisis Bulbi Patient with Scleral Cover Shell ProsthesisOliver GiroudBelum ada peringkat
- Technique for Fabricating Temporary Ocular ProsthesisDokumen8 halamanTechnique for Fabricating Temporary Ocular ProsthesisDeepthi Rajesh100% (1)
- Management of Hyper-Mobile Tissue With A Modified Combine Technique of Zafrulla and HobkrikDokumen5 halamanManagement of Hyper-Mobile Tissue With A Modified Combine Technique of Zafrulla and HobkrikIJAR JOURNALBelum ada peringkat
- Impression Techniques For Occular Prosthesis - ReviewDokumen9 halamanImpression Techniques For Occular Prosthesis - ReviewIJAR JOURNALBelum ada peringkat
- Bridging The Gap: Interim Prosthetic Rehabilitation For Oro-Cutaneous Fistula Post Cancer SurgeryA Case ReportDokumen5 halamanBridging The Gap: Interim Prosthetic Rehabilitation For Oro-Cutaneous Fistula Post Cancer SurgeryA Case ReportInternational Journal of Innovative Science and Research TechnologyBelum ada peringkat
- A Prosthodontic Rehabilitation of A Partial Maxillectomy Patient With Hollow Bulb ObturatorDokumen4 halamanA Prosthodontic Rehabilitation of A Partial Maxillectomy Patient With Hollow Bulb ObturatorDentist HereBelum ada peringkat
- Case Report - Complete Denture - 2Dokumen4 halamanCase Report - Complete Denture - 2Astri Ggamjong Xiao LuBelum ada peringkat
- Managing Flabby RidgesDokumen6 halamanManaging Flabby RidgesRiya KvBelum ada peringkat
- IJPRDDEC2013EYEPROSTHESISDokumen6 halamanIJPRDDEC2013EYEPROSTHESISSahana RangarajanBelum ada peringkat
- A New Clinical Approach in Fabrication of Closed Hollow Bulb Obturator: A Case ReportDokumen4 halamanA New Clinical Approach in Fabrication of Closed Hollow Bulb Obturator: A Case ReportDr. Ravi Sagar Singh ShahiBelum ada peringkat
- Innovative Rehabilitation Approach Spectacle-Retained Orbital Prosthesis For Post-Mucormycosis Orbital DefectDokumen5 halamanInnovative Rehabilitation Approach Spectacle-Retained Orbital Prosthesis For Post-Mucormycosis Orbital DefectInternational Journal of Innovative Science and Research TechnologyBelum ada peringkat
- Ocular ProsthesisDokumen28 halamanOcular ProsthesisrajaniBelum ada peringkat
- History of Artificial EyeDokumen3 halamanHistory of Artificial EyeNadja SansaronaBelum ada peringkat
- Artificial Eye Seminar ReportDokumen16 halamanArtificial Eye Seminar ReportKeerthan GowdaBelum ada peringkat
- The Biotransfer Approach: The Use of An Alveolar Cast Die For The Fabrication of The Emergence Profile On Implant-Supported Interim RestorationsDokumen4 halamanThe Biotransfer Approach: The Use of An Alveolar Cast Die For The Fabrication of The Emergence Profile On Implant-Supported Interim RestorationsClaudioBelum ada peringkat
- Rehabilitation of A Complex Oro-Facial Defect by Modified Prosthetic ApproachDokumen3 halamanRehabilitation of A Complex Oro-Facial Defect by Modified Prosthetic ApproachBharat KhemaniBelum ada peringkat
- Fabrication of A Custom Ocular Prosthesis: Case ReportDokumen4 halamanFabrication of A Custom Ocular Prosthesis: Case ReportIa HidaryaBelum ada peringkat
- Nasal Prosthesis - A Case ReportDokumen4 halamanNasal Prosthesis - A Case ReportInternational Organization of Scientific Research (IOSR)Belum ada peringkat
- Surgical Obturator: Squamous Cell Carcinoma of Right Maxilla (Upper Jaw) Invading Bone. Patient WillDokumen12 halamanSurgical Obturator: Squamous Cell Carcinoma of Right Maxilla (Upper Jaw) Invading Bone. Patient WillDrRanjeet Kumar ChaudharyBelum ada peringkat
- 1st Article - Vikas AggarwalDokumen4 halaman1st Article - Vikas AggarwalSai VyshuBelum ada peringkat
- Baru Mata 2Dokumen29 halamanBaru Mata 2Ichsan DiazBelum ada peringkat
- CSE Artificial Eye REPORTDokumen18 halamanCSE Artificial Eye REPORTVaibhav TiwariBelum ada peringkat
- Dr. Kirti Kumsowar - 6Dokumen2 halamanDr. Kirti Kumsowar - 6Zoya AfzalBelum ada peringkat
- Positioning Magnets On A Multiple/Sectional Maxillofacial ProsthesisDokumen7 halamanPositioning Magnets On A Multiple/Sectional Maxillofacial Prosthesisڣـڕٱټـي آڵـھـۈئBelum ada peringkat
- 2011 Article 99Dokumen4 halaman2011 Article 99ali baridiBelum ada peringkat
- Customized Thermoplast Retentive Aid For Partial Auricular Prosthesis-A Case ReportDokumen9 halamanCustomized Thermoplast Retentive Aid For Partial Auricular Prosthesis-A Case ReportIJAR JOURNALBelum ada peringkat
- DR Fabio RossiDokumen3 halamanDR Fabio RossiMohsin Habib100% (1)
- Mold Making For Orbital ProsthesisDokumen4 halamanMold Making For Orbital ProsthesisdrsmritiBelum ada peringkat
- Effective Suction-Imporession For Retentive Mand Dentture PDFDokumen24 halamanEffective Suction-Imporession For Retentive Mand Dentture PDFFaheemuddin MuhammadBelum ada peringkat
- Ansari 1997Dokumen4 halamanAnsari 1997SkAliHassanBelum ada peringkat
- Prosthetic Rehabilitation of Maxillectomy Patient With Telescopic DenturesDokumen6 halamanProsthetic Rehabilitation of Maxillectomy Patient With Telescopic DenturesVero AngelBelum ada peringkat
- Ophthalmology and Clinical Research: ClinmedDokumen10 halamanOphthalmology and Clinical Research: Clinmedhafidh akbarBelum ada peringkat
- Prosthodontic Management of Flabby Ridge From Modified Impression To DentureDokumen14 halamanProsthodontic Management of Flabby Ridge From Modified Impression To DenturePhoebe David100% (1)
- PDF 338Dokumen7 halamanPDF 338ali baridiBelum ada peringkat
- Impression Techniques in Removable Partial DentureDokumen8 halamanImpression Techniques in Removable Partial DentureLama Nahed100% (2)
- An Innovative Technique For Acrylisation To Fabricate Hollow Bulb Obturator Using Chlorinated Polyvinyl Chloride (CPVC) PipeDokumen8 halamanAn Innovative Technique For Acrylisation To Fabricate Hollow Bulb Obturator Using Chlorinated Polyvinyl Chloride (CPVC) PipeIJAR JOURNALBelum ada peringkat
- A Procedure For Relining A Complete or Removable Partial Denture Without The Use of WaxDokumen3 halamanA Procedure For Relining A Complete or Removable Partial Denture Without The Use of WaxKarthikmds ElangovanBelum ada peringkat
- Vis AnteDokumen16 halamanVis AntejochigBelum ada peringkat
- Straumann Pro Arch DR EskanDokumen3 halamanStraumann Pro Arch DR EskanShyam BhatBelum ada peringkat
- Construction of An Orbital Prosthesis Using Magnets For RetentionDokumen12 halamanConstruction of An Orbital Prosthesis Using Magnets For RetentionjoephinBelum ada peringkat
- Materials Used in Maxillofacial ProsthesisDokumen88 halamanMaterials Used in Maxillofacial ProsthesisAkanksha MahajanBelum ada peringkat
- Materials Used in Maxillofacial ProsthesisDokumen88 halamanMaterials Used in Maxillofacial ProsthesisAmit Shivrayan60% (5)
- ITP2Dokumen42 halamanITP2Mehak JainBelum ada peringkat
- Customized Scale Aids Iris Orientation in Ocular ProsthesisDokumen4 halamanCustomized Scale Aids Iris Orientation in Ocular ProsthesisRajsandeep SinghBelum ada peringkat
- A Hollow Bulb ObturatorDokumen6 halamanA Hollow Bulb ObturatorrekabiBelum ada peringkat
- Ijms 23 01049Dokumen14 halamanIjms 23 01049Manjeev GuragainBelum ada peringkat
- Welcome To MEGA PDFDokumen9 halamanWelcome To MEGA PDFRüdiger TischbanBelum ada peringkat
- Child Oral HealthDokumen7 halamanChild Oral HealthManjeev GuragainBelum ada peringkat
- Sdarticle PDFDokumen9 halamanSdarticle PDFManjeev GuragainBelum ada peringkat
- Sdarticle PDFDokumen10 halamanSdarticle PDFManjeev GuragainBelum ada peringkat
- Influence of Parents' Oral HealthDokumen8 halamanInfluence of Parents' Oral HealthManjeev GuragainBelum ada peringkat
- Even More ScaredDokumen108 halamanEven More ScaredManjeev GuragainBelum ada peringkat
- Sdarticle PDFDokumen2 halamanSdarticle PDFManjeev GuragainBelum ada peringkat
- Titanium Framework Removable Partial Denture Used ForDokumen4 halamanTitanium Framework Removable Partial Denture Used ForManjeev GuragainBelum ada peringkat
- Hypersensitivity To Temporary Soft Denture LinersDokumen3 halamanHypersensitivity To Temporary Soft Denture LinersManjeev GuragainBelum ada peringkat
- SdarticleDokumen3 halamanSdarticleManjeev GuragainBelum ada peringkat
- Reliability, Validity, and Utility of Various Occlusal Measurement Methods and TechniquesDokumen7 halamanReliability, Validity, and Utility of Various Occlusal Measurement Methods and TechniquesManjeev GuragainBelum ada peringkat
- 9 PDFDokumen6 halaman9 PDFManjeev GuragainBelum ada peringkat
- Sdarticle PDFDokumen3 halamanSdarticle PDFManjeev GuragainBelum ada peringkat
- Sdarticle PDFDokumen8 halamanSdarticle PDFManjeev GuragainBelum ada peringkat
- DisclaimerDokumen2 halamanDisclaimerManjeev GuragainBelum ada peringkat
- Sdarticle PDFDokumen4 halamanSdarticle PDFManjeev GuragainBelum ada peringkat
- Luzerne Jordan, Washington, D. CDokumen2 halamanLuzerne Jordan, Washington, D. CManjeev GuragainBelum ada peringkat
- President'S Address: Detroit, MichDokumen2 halamanPresident'S Address: Detroit, MichManjeev GuragainBelum ada peringkat
- Luzerne Jordan, Washington, D. CDokumen2 halamanLuzerne Jordan, Washington, D. CManjeev GuragainBelum ada peringkat
- 10 PDFDokumen9 halaman10 PDFManjeev GuragainBelum ada peringkat
- 8 PDFDokumen13 halaman8 PDFManjeev GuragainBelum ada peringkat
- Analyzing Partial Denture StressesDokumen5 halamanAnalyzing Partial Denture StressesManjeev GuragainBelum ada peringkat
- 5Dokumen9 halaman5Manjeev GuragainBelum ada peringkat
- 12 PDFDokumen6 halaman12 PDFManjeev GuragainBelum ada peringkat
- 5Dokumen9 halaman5Manjeev GuragainBelum ada peringkat
- President'S Address: Detroit, MichDokumen2 halamanPresident'S Address: Detroit, MichManjeev GuragainBelum ada peringkat
- Centric Position Dental DocumentDokumen3 halamanCentric Position Dental DocumentManjeev GuragainBelum ada peringkat
- Abraham E-I. Lazarus,: New York, N. IDokumen5 halamanAbraham E-I. Lazarus,: New York, N. IManjeev GuragainBelum ada peringkat
- Wilfrid Hall Terrell, Calif.: ExaminationDokumen25 halamanWilfrid Hall Terrell, Calif.: ExaminationManjeev GuragainBelum ada peringkat