Clinical Presentation of Rove Beetle Dermatitis
Diunggah oleh
Wanly SyahrizalDeskripsi Asli:
Hak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Clinical Presentation of Rove Beetle Dermatitis
Diunggah oleh
Wanly SyahrizalHak Cipta:
Format Tersedia
Australasian Medical Journal 2009, 1, 7, 19-24
Clinical Presentation of Rove Beetle Dermatitis
Tahir Mehmood Khan* 1, 3, Mohamad Azmi Hassali 2 , Syed Wasif Gillani 3 & Mohammed Abdul Hameed 3 1 Department of Pharmacy, Island College of technology, Balik Pulau 11000, Penang Malaysia 2 Discipline of Social and Administrative Pharmacy, School of Pharmaceutical Science, Universiti Sains Malaysia, 11800 Penang Malaysia 3 School of Pharmaceutical Science, Universiti Sains Malaysia, 11800 Penang Malaysia Introduction Case Series Among the arthropods, beetles are well known for blistering skin eruptions and commonly known as beetle Date Submitted: 13/07/09 skin dermatitis [1]. Beetles from three families (Meloidae, Date Revised: 21/07/09 Oedemeridae and Staphylinidae) are noted to cause Date Accepted: 01/08/09 vesicant (blistering) lesions [2]. Blister beetle (Meloidae) Published Online: 04/08/09 and Rove beetle (Staphylinidae, sp Paederus) are endemic in Southeast Asia [1]. However, Rove beetles are the Please cite this paper as: Khan T, Hassali M, Gillani S, Hameed largest in this family with over 26000 species world wide M. Clinical presentation of Rove Beetle Dermatitis. AMJ [2]. Rove beetles are small, elongated insects occuring 2009, 1, 7, 19-24. Doi 10.4066/AMJ.2009.77 world wide from 5 mm to 10 mm in length (figure 1) are a Corresponding Author: and found abundantly in tropical areas. In Malaysia rove Tahir Mehmood Khan beetle is abundant in paddy fields (rice fields). Department of Pharmacy, Island College of technology However, blister beetle is more common in Africa, Balik Pulau 11000, Penang Malaysia America and Europe [3]. Rove beetle dermatitis is quite Email: tahir.pks@gmail.com frequent among students in Penang. Many students staying at University Sains Malaysia campus have reported Abstract Rove beetle dermatitis. The main aim of this study is to Objectives: This case series describes new clinical features of report the clinical presentation of rove beetle dermatitis Rove beetle dermatitis and compare the symptoms with previously international Methods: Interviews were conducted with four students at studies. University Sains Malaysia with current or past Rove beetle skin infections. Information on the onset of symptoms, Figure 1 Description of rove beetles complication, treatment and duration of symptoms were recorded. A physician at a local clinic was also interview to describe the challenges in diagnosis and therapy for this condition. Results: This case series describes new features of Rove beetle dermatitis. Redness, swelling, fatigue and localised stretching of the skin were the commonly reported symptoms. However, vibrations, twitching of the skin and difficulty in breathing were new features observed in this study. Three of the four patients were not aware of the aetiology of the condition, antibiotics and topical steroids were prescribed for the management and prevention of secondary infection. Conclusion: Rove beetle dermatitis is a common seasonal endemic in Malaysia, with a higher incidence in the month of Rove beetle (Staphylinidae) September and March. This case series highlights the need for Toxin (paederin) a health literacy program, aimed at informing the public and medical practitioners about the aetiology, symptoms and Method complications of this infection. Face to face interviews were conducted with two Key words: Rove beetle dermatitis, symptoms, case series respondents who had current and previous exposure to Rove beetle dermatitis. Information on the onset of symptoms, complications, treatment and recovery was recorded. Moreover, a physician at a local clinic was also interviewed to ascertain the difficulties in making the diagnosis and the current therapeutic regimen. Ethical clearance was obtained form the research ethics committee of Island College of Technology, Balik Pulau (EA-0109). Informed consent was obtained from the subjects to use the photographs presented in this report. All the pictures (Figure 1, 2 &3) were taken by the research team using a digital camera. Figure 1 was
Clinical Presentation of Rove Beetle Dermatitis among University Students
19
Australasian Medical Journal 2009, 1, 7, 19-24
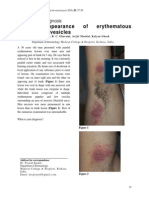
enhanced using adobe photo shop software in order to provide the most suitable image for the Rove beetle. Study location This study was conducted in University Sains Malaysia, Penang. Penang is one of the thirteen states of Malaysia, and comprising of two parts, i.e. Penang Island and Penang mainland. USM is situated in Penang Island; the neighbouring state of Penang is Kedah, is an important rice growing region [4]. Moreover, it is a designated tropical rain forest. Results Two current and two historical cases were reviewed. Of the four cases, three reported infections in the month of March. The other case was observed in the month of September. In Malaysia immediate climatic changes occur in the month of March and September, with the rainy season replacing hot and humid weather. The commonly affected areas observed were exposed parts of the body i.e hand, eye, face, nose and neck. Symptoms reported Frequently reported symptoms were the redness, burning sensation and the pain at the affected site (Figure 2 and Figure 3). In addition to this the stretching of the skin at the affected areas was another commonly reported symptom. The exudates from the lesion was reported on the next day. The lesions were erythematous and edematous, described as linear and whiplash like in appearance. The vesicles generally appeared towards the centre of a plaque. The vesicles frequently turned into pustules. The signs appeared after 24 to 48h of contact with the beetle and last for a week. Details are described in Table 1 and Table 2. Difficulty in breathing was also reported towards the end of the infection (Table 2, Case 2).
Figure 2 Current case
The prime objective in management should be the prevention of secondary infections. Antibiotics, steroidal topical preparations, pain killers and anti-histamines can be beneficial in the prevention of the secondary infections. Recovery is a slow process, two to three weeks is the usual duration of symptoms. However, climatic conditions including high humidity may delay the process of recovery.
Figure 3 Current Cases
A(i) Whiplash Rove Beetle Dermatitis at neck
A(ii)
B(i) Whiplash Rove Beetle Dermatitis on chest demonstrating pustules
A(iii)
Paederin is found on the surface of the beetle and is the agent responsible for the dermatitis. Paederin is a toxic alkaloid, vesicant capable of blocking cell division [8]. The Skin is exposed to Paederin as a result of movement or crawling of the Rove beetle [7,12]. The possible reasons for increase in number of Rove beetles in Penang In Malaysia, Rove beetles are abundant in paddy fields [18]. There are three possible reasons. Firstly heavy flooding in the neighbouring states results in migration of the Rove beetles to the safe areas. Second after the harvest of the rice crop, the field is allowed to dry and the bushes are burned to get rid of pests. The burning of the paddy fields starts in December and continues to February, which may be the reason why the beetles migrate to neighbouring states in search of shelter. The third reason is the thick tropical rain forest of Penang makes an ideal habitat for this pest.
Affected eye and lid
Diagnosis and treatment A general practitioner stated that it is difficult to differentiate Rove beetle dermatitis from other inflammatory skin conditions, without prior experience of managing the infection. The clinical presentations resemble other dermatitis and herpetic infections. Identification of the insect by the patient and the seasonal incidence are the most important clues to the diagnosis.
Clinical Presentation of Rove Beetle Dermatitis among University Students
20
Australasian Medical Journal 2009, 1, 7, 19-24
Table 1 Current cases, two weeks duration Case 1: Dated 05-3-2009 (location of dermatitis: eye) Age of patient 29 years Gender: Male Q. When the symptoms of dermatitis appear? I get early in the morning for pray I feel some pressure on my eye when I lean down I feel that my eye is bouncing and vibrating. Q. Where you slept last night? In my room, at my bed Q. Are you in habit of leaving night lamp ON while sleeping? No, but that day my notebook was ON. Q. What were the initial symptoms? First day 1. My eye was red, and I feel itchy and burning 2. I feel my eye is twitching and pain 3. My skin was stretched Second day 1. There was discharge of fluid from the affected area, look like I put some oil on my eye lid. 2. My eye was swollen Third day 1. The wound was exposed and deep, there was a lesion and yellowish blister was formed. Current status 1. The exposed wound is better now, however still the affected area is red, slightly painful and the skin is stretched. Q. Have you sought some medical attention? Yes, doctor has given me some pain killers, anti-allergy and some cream to apply on wound. On the ninth day lesion healed. Case 2: Dated 12-3-2009 (location of dermatitis: neck[Ai,ii,iii] and chest) figure 3 Age of patient 27 years Gender: Male Q. When the symptoms of dermatitis appear? This morning when I wake up the skin was red. Q. Where you slept last night? I was very tired last night, I sleep at floor. Q. Are you in habit of leaving night lamp ON while sleeping? No, but the day I got this problem the night lamp was ON. Q. What were the initial symptoms? First day 1. I feel that my skin is stretched 2. The affected area was very sensitive and itchy. The itching increase if the affected is touched 3. Small yellow blisters were appearing at night time. Second day 1. When I speak and laugh I feel the affected area is vibrating. 2. Excessive fluid discharges, then I use some talcum powder after that no more. 3. pustules Third day 1. I feel fatigue and dizzy like I will get fever soon. Fourth day 1. I feel better now, it will be ok soon. Q. Have you sought some medical attention? No, my friend he gave me some medicated cream (steroidal) and I am using it form last four days. On the tenth day the lesion healed.
Clinical Presentation of Rove Beetle Dermatitis among University Students
21
Australasian Medical Journal 2009, 1, 7, 19-24
Table 2 Personal experiences of the students with Rove beetle dermatitis in 2008 Case 1: March 2008 (location of dermatitis: Hand) Age of patient 26 years Gender: Male Q. When the symptoms of dermatitis appear? I get early in the morning, nothing was there but immediately in afternoon I noticed that I got a red scar. Q. Where you slept last night? In my room, but I put the mattress on the floor. Q. Are you in habit of leaving night lamp ON while sleeping? No, but that day my notebook was ON. Q. What were the initial symptoms? First day 1. I feel itchy and burning 2. The affected area was red and swollen a little bit Second day 3. There was discharge of fluid from the affected area, the deep wound turned in to lesion and it becomes a bit yellowish. Third day 1. Same condition as second day Q. Have you sought some medical attention? No, I am familiar with this problem it can recover without any medication and I did not like to use a lot of medicines Q. When the wound was recovered? It took around 13 days for the lesion to close. However, the redness remains there. After one month the scaling process started at the wound site. The black colour scalps started to peal off. The pink skin appeared. But the scars still remain. Q. Are you familiar that how this insect looks like? Yes Case 2: Dated September 2008 (location of dermatitis: face, eye, back, nose) Age of patient 32 years Gender: Male Q. When the symptoms of dermatitis appear? This morning when I wake up the skin was red, itchy, stretched and painful. Q. Where you slept last night? I slept on my bed. Q. Are you in habit of leaving night lamp ON while sleeping? Not always sometime. Q. What was the length of the scar? About 3.5 inch Q. Was there any pustule formation? No Q. What were the initial symptoms? First day 1. My face was red, my left eye was swollen 2. My nose was itchy, red and painful 3. I felt difficulty in breathing, I suffer through the rove beetle dermatitis about three times, and when ever I feel difficulty in breathing it is the sign that I got rove beetle dermatitis. Second day 4. The redness turned to lesions and the fluid come through the lesion 5. Unbearable itching and pain Q. Have you sought some medical attention? Yes, I went to see doctor. He gave me paracetamol , anti histamine, Doxycycline (oral), betamethazone and Gentamycine topical cream was given to treat the secondary infection in eye. Q. When the wound was recovered? It took around 15 days for the lesion to close. However, the redness remains there. After 30-35 days the scaling process started at the wound site. The black colour scalps started to peal off. The pink skin appeared. After 5 months the scar vanished totally. Q. Are you familiar that how this insect looks like? No, [An educational session of the respondents was conducted and all the information about the rove beetle and the rove beetle dermatitis was provided to the respondent].
Clinical Presentation of Rove Beetle Dermatitis among University Students
22
Australasian Medical Journal 2009, 1, 7, 19-24
Clinical presentation Slight redness of the affected areas within the first 12-24 hours is usual [8,9,10,11], with the onset of blisters on the 2-4th day followed by pain. [14]. The blister formation may be a response to serine proteases and neutrophil elastase released in in response to Paederin [15, 16]. Following blister formation there is the appearance of linear lesions (that look like whip injuries) and are also known as mirror image or kissing lessons [17]. However, the clinical observations in this study differ from those described in text books. The redness, itching and pain on the affected area were the common symptoms on day one. In addition the swelling, stretching of the skin and vibrations in the affected areas (chest, neck figure 3 and eye figure 2) were other recognised symptoms. The lesion were deep and exposed, exudates from the lesions were commonly reported. A new finding reported by only one individual, was difficulty in breathing. Two possibilities exist; one of the patients was hypersensitive to Paederin. Alternatively as the affected site was the nose and surrounding area that led to the experience of dyspnea, (Table 2, case 2). Unlike, the findings of [8, 10, 11] no one has reported neuralgia, arthralgia and vomiting. However, felling tired and dizzy were the reported by one patient. These new clinical presentations may help further catalogue the known clinical features and assist the general practitioner to make a diagnosis. Recovery occurs within 8- 10 days as the lesions dry and dark scales appear [8,10,11]. After four weeks the black scales start to peal of, exposing new pink skin. After six month the scars vanished (Table 2, case 2), but in one case scars were still apparent after 12 months (Table 2, case 1). However, the scaling process was more rapid in th the case 2 (table 1) on the 8 day the black scale desloughed spontaneously and pink skin appeared. Differential diagnosis and treatment of rove beetle dermatitis Diagnosis of the Rove beetle dermatitis is important. The manifestation of Rove beetle dermatitis may be a clinical conundrum and the differential diagnosis includes herpes simplex, herpes zoster, liquid burns, acute allergic or irritant contact dermatitis, millipede dermatitis and phytophotodermatitis [19]. For effective treatment and accurate diagnosis it is essential that the clinician should thoroughly check the features of the lesions, confirm the presence of kissing lesions, review the incidence of similar cases in the locality, note the seasonal incidence, identify the insect and seek a histopathology report to confirm the diagnosis [20]. No known effective treatment is available. The use anti-histamines and analgesics relieves the sign inflammation. However, the oral and topical use antibiotics, with or without corticosteroids may help prevent secondary infection [21]. of of of to
Factor responsible for the outbreak of Rove beetle dermatitis In addition to burning of stubble in paddy fields, climatic changes also have a vital role in the outbreak of Rove beetle dermatitis. This case series records three cases in the month of March and one only in September. The rainy season starts immediately in February and continues till the end of May, similarly the second wet season starts in September and ends in November [22]. The remaining months are hot. When the rainy seasons start the immediate variations in temperature and humidity are observed, this could be a possible reason for the invasion of the Rove beetles into homes and increased prospect of human infection. [23,24,25]. These findings are consistent with the findings Nandakishore which similarly reported a high incidence of Rove beetle dermatitis in the month of September and March [26,27]. Moreover the use of bright lights at night and in the increased popularity of high rise apartments are the other factors that increase the chance of human contact with Rove beetles [28]. Conclusion Rove beetle dermatitis is a common seasonal endemic in Malaysia, with a higher incidence in the month of September and March. These findings highlight the need of a health literacy program, directed at the public and highlighting the aetiology, symptoms and complications of this infection. Increased public awareness will ultimately assist doctors with the differential diagnosis. Recommendations Though Rove beetle dermatitis does not have an impact on economy in terms of direct cost, the associated morbidity may impact on the local economy. These findings suggest the need for health promotion activities to educate local people about Rove beetle. Moreover, the horticulture department may promote different ways of disposing of stubble in paddy fields. Burning the beetles usual habitat may be one of the reasons for the migration of these pests to neighbouring states.
Reference
1. Nair BKH, Nair TVG .Diseases caused by arthropods. In: Valia R.G., Valia A.R. editors. IADVL Textbook and nd Atlas of Dermatology 2 edition. Mumbai, India: Bhalani publishing house; 2001. p. 340-41. Christmas TI, Nicholls D, Holloway BA, Greig D. Blister beetle dermatosis in New Zealand. N.Z. Med. J. 1987; 100: 51517. Mohanty SK, Dash S. Bone marrow metastasis in Solid tumours. Indian J Pathol Microbiol. Oct 2003; 46 (4):613-16. Socio-Economic & Environmental Research Institute (SERI). (2007) Penang Statistics, 2007 Quarter 2 page th 3. [Online] accessed on 20 march 2008. available from World Wide Web http://www2.seri.com.my/Penang%20Statistics/2007 /Q2-April-June-2007-1.pdf Kerdel-Vegas F, Goihman-Yahr M. Paederus dermatitis. Arch. Derm. 1966; 94: 17585.
2.
3.
4.
5.
Clinical Presentation of Rove Beetle Dermatitis among University Students
23
Australasian Medical Journal 2009, 1, 7, 19-24
6.
7.
8.
9. 10.
11.
12.
13.
14. 15.
16.
17. 18.
19.
20. 21.
22.
23.
Monteith G, Argent C. Whiplash Rove beetles. In: Covacevich J, Davie P, Pearn J (eds). Toxic Plants and Animals. A Guide for Australia. Brisbane: Queensland Museum, 1987; 26771. Ross Piper (2007), Extraordinary Animals: An Encyclopedia of Curious and Unusual Animals, Greenwood Press (August 30, 2007) ISBN-13: 9780313339226. Pages 254-57. Frank, J.H. & K. Kanamitsu. 1987. Paederus, Sensu Lato (Coleoptera: Staphylinidae): Natural History and Medical Importance. J. Med. Entomol. 24: 155191. Millard PT. Whiplash dermatitis produced by the common Rove beetle. Med. J. Aust. 1954; 1: 7414. McCrae, A.W.R. & S.A. Visser. 1975. Paederus (Coleoptera: Staphylinidae) in Uganda. I. Outbreaks, clinical effects, extraction and bioassay of vesicating toxin. Annals of Tropical Medicine and Parasitology. 69: 109-120. Borroni, G, Brazzelli, V., Rosso, R. & M. Pavan. 1991. Paederus fuscipes dermatitis: A histopathological study. The American Journal of Dermatopathology. 13: 467-474. Gary Mullen, (2002) Medical and Veterinary Entomology. Academic Press; 1st edition (September 14, 2002), ISBN-13: 978-0125104517. John ODonel Alexander (1984), Skin eruptions caused by Beetles (Coleoptera). In Arthropods and Human Skin. 1st ed. Berlin/ New York: Springer Verlag;.p.75-85. Southcott RV. Injuries from Coleoptera. Med. J. Aust. 1989; 151: 6549. Liu Z, Shapiro SD, Zhou X, et al: A critical role for neutrophil elastase in experimental bullous pemphigoid. J Clin Invest 2000;105:113123. Liu Z, Zhou X, Shapiro SD, et al: The serpin alpha1proteinase inhibitor is a critical substrate for gelatinase B/MMP-9 in vivo. Cell 2000;102:647 655. Kerdel-Vegas F, Goihman-Yahr M. Paederus dermatitis. Arch.Derm. 1966; 94: 17585. Rahmah E & Norjaiza. (2008)An outbreak of Paederus dermatitis in a primary school, Terengganu, Malaysia Malaysian J Pathol 2008; 30(1) : 53 56 Zargari O, Asadi AK, Fathalikhani F, Panahi M. Paederus dermatitis in northern Iran: A report of 156 cases. Int J Dermatol 2003;42:608-12. Vegas FK, Yahr MG, Venezuela C. Paederus dermatitis. Arch Dermatol 1996;94:175-83. George AO, Hart PD. Outbreak of Paederus dermatitis in southern Nigeria: Epidemiology and dermatology. Int J Dermatol 1990;29:500-1 Weather and Climate in Malaysia, Accessed [online] retrieved from World Wide Web http://www.southtravels.com/asia/malaysia/weath er.html Schofield S. The tale of the Paederus Beetle. http://www.forces.gc.ca/health/information/healt h_promotion/Engraph/BeetleJuice_e.asp accessed on 23.03.2005.
24. Mokhtar N, Singh R, Ghazali W. Paederus dermatitis among medical students in USM, Kelantan. Med J Malaysia 1993;48(4):403-6. 25. Morsy TA, Arafa MA, Younis TA, Mahmoud IA. Studies on Paederus alfierii Koch (Coleoptera: Staphylinidae) with special reference to the medical importance. J Egypt Soc Parasitol 1996;26(2):337- 51 26. Nandakishore. Th, Roslin L, Romita B, Kalkambe KA. (2008) Beetle dermatitis in Manipur JMS Vol 22 No. 1, pp 9-12 27. Claborn DM, Pola JM, Olsa PE, Earhart KC, Sherman SS. (1999) Staphylinid (Rove) beetle dermatitis outbreak in the American Southwest? Mil Med; 164 : 209-13. 28. News Article: Rove Beetle (01/01/2002) INFORMATION ON ROVE BEETLE Majlis Perbandaran Seberang Perai http://www.mpsp.gov.my/includes/Article.asp ?ID=116&Context=2002&Lan=1 accessed on 23.03.2005.
Clinical Presentation of Rove Beetle Dermatitis among University Students
24
Anda mungkin juga menyukai
- Sperm Motility PDFDokumen10 halamanSperm Motility PDFWanly SyahrizalBelum ada peringkat
- Antisperm Antibody Tests Traditional Methods Compared To Elisa PDFDokumen8 halamanAntisperm Antibody Tests Traditional Methods Compared To Elisa PDFWanly SyahrizalBelum ada peringkat
- Testosterone Replacement TherapyDokumen23 halamanTestosterone Replacement TherapyWanly SyahrizalBelum ada peringkat
- Gossypol e infertilidade masculina: os efeitos do gossypol na fertilidade masculinaDokumen2 halamanGossypol e infertilidade masculina: os efeitos do gossypol na fertilidade masculinaWanly SyahrizalBelum ada peringkat
- Femal Sexual 1Dokumen10 halamanFemal Sexual 1Mesgina G-herBelum ada peringkat
- Igf 1 PDFDokumen6 halamanIgf 1 PDFWanly SyahrizalBelum ada peringkat
- Update in Male Infertility PDFDokumen1 halamanUpdate in Male Infertility PDFWanly SyahrizalBelum ada peringkat
- Hypogonadotropic Hypogonadism Revisited: ReviewDokumen8 halamanHypogonadotropic Hypogonadism Revisited: ReviewSintia CahyaniBelum ada peringkat
- Antisperm Antibody Test PDFDokumen9 halamanAntisperm Antibody Test PDFWanly SyahrizalBelum ada peringkat
- Testosteron For LOHDokumen4 halamanTestosteron For LOHWanly SyahrizalBelum ada peringkat
- Phases of The Sexual Response CycleDokumen5 halamanPhases of The Sexual Response CycleWanly SyahrizalBelum ada peringkat
- Semen WashDokumen8 halamanSemen WashPrasmit ShahBelum ada peringkat
- Classification and Definition of Premature Ejaculation: Arie Parnham, Ege Can SerefogluDokumen8 halamanClassification and Definition of Premature Ejaculation: Arie Parnham, Ege Can SerefogluWanly SyahrizalBelum ada peringkat
- Clinical Management of Priapism: A ReviewDokumen8 halamanClinical Management of Priapism: A ReviewWanly SyahrizalBelum ada peringkat
- Kallmann's SyndromeDokumen3 halamanKallmann's SyndromeWanly SyahrizalBelum ada peringkat
- Femal Sexual 1Dokumen10 halamanFemal Sexual 1Mesgina G-herBelum ada peringkat
- Testosteron For LOHDokumen4 halamanTestosteron For LOHWanly SyahrizalBelum ada peringkat
- Estrogen in Male Reproduction FunctionDokumen6 halamanEstrogen in Male Reproduction FunctionWanly SyahrizalBelum ada peringkat
- American Urological Association (AUA) GuidelineDokumen61 halamanAmerican Urological Association (AUA) GuidelineWanly SyahrizalBelum ada peringkat
- Semen WashDokumen8 halamanSemen WashPrasmit ShahBelum ada peringkat
- Images in Pediatric Endocrinology: Adhesion of The Labia Minora in Girls: A Common Disorder That Is Rarely ConsideredDokumen3 halamanImages in Pediatric Endocrinology: Adhesion of The Labia Minora in Girls: A Common Disorder That Is Rarely ConsideredWanly SyahrizalBelum ada peringkat
- Jpem 2012 0004 PDFDokumen3 halamanJpem 2012 0004 PDFWanly SyahrizalBelum ada peringkat
- Periorbital Paederus DermatosisDokumen3 halamanPeriorbital Paederus DermatosisWanly SyahrizalBelum ada peringkat
- 17 Male Infertility - LR1 PDFDokumen42 halaman17 Male Infertility - LR1 PDFsanaBelum ada peringkat
- Semen WashDokumen8 halamanSemen WashPrasmit ShahBelum ada peringkat
- Typhoid FeverDokumen45 halamanTyphoid FeverWanly SyahrizalBelum ada peringkat
- American Urological Association (AUA) GuidelineDokumen61 halamanAmerican Urological Association (AUA) GuidelineWanly SyahrizalBelum ada peringkat
- 13.PhotodermDiagnosis Sudden Appearance of Vesicles in An AdultDokumen3 halaman13.PhotodermDiagnosis Sudden Appearance of Vesicles in An AdultWanly SyahrizalBelum ada peringkat
- Blistering Beetles DermatitisDokumen3 halamanBlistering Beetles DermatitisWanly SyahrizalBelum ada peringkat
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDari EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifePenilaian: 4 dari 5 bintang4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingDari EverandThe Little Book of Hygge: Danish Secrets to Happy LivingPenilaian: 3.5 dari 5 bintang3.5/5 (399)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDari EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryPenilaian: 3.5 dari 5 bintang3.5/5 (231)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDari EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RacePenilaian: 4 dari 5 bintang4/5 (894)
- The Yellow House: A Memoir (2019 National Book Award Winner)Dari EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Penilaian: 4 dari 5 bintang4/5 (98)
- Shoe Dog: A Memoir by the Creator of NikeDari EverandShoe Dog: A Memoir by the Creator of NikePenilaian: 4.5 dari 5 bintang4.5/5 (537)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDari EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FuturePenilaian: 4.5 dari 5 bintang4.5/5 (474)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDari EverandNever Split the Difference: Negotiating As If Your Life Depended On ItPenilaian: 4.5 dari 5 bintang4.5/5 (838)
- Grit: The Power of Passion and PerseveranceDari EverandGrit: The Power of Passion and PerseverancePenilaian: 4 dari 5 bintang4/5 (587)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDari EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaPenilaian: 4.5 dari 5 bintang4.5/5 (265)
- The Emperor of All Maladies: A Biography of CancerDari EverandThe Emperor of All Maladies: A Biography of CancerPenilaian: 4.5 dari 5 bintang4.5/5 (271)
- On Fire: The (Burning) Case for a Green New DealDari EverandOn Fire: The (Burning) Case for a Green New DealPenilaian: 4 dari 5 bintang4/5 (73)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDari EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersPenilaian: 4.5 dari 5 bintang4.5/5 (344)
- Team of Rivals: The Political Genius of Abraham LincolnDari EverandTeam of Rivals: The Political Genius of Abraham LincolnPenilaian: 4.5 dari 5 bintang4.5/5 (234)
- Rise of ISIS: A Threat We Can't IgnoreDari EverandRise of ISIS: A Threat We Can't IgnorePenilaian: 3.5 dari 5 bintang3.5/5 (137)
- The Unwinding: An Inner History of the New AmericaDari EverandThe Unwinding: An Inner History of the New AmericaPenilaian: 4 dari 5 bintang4/5 (45)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDari EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyPenilaian: 3.5 dari 5 bintang3.5/5 (2219)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDari EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You ArePenilaian: 4 dari 5 bintang4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Dari EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Penilaian: 4.5 dari 5 bintang4.5/5 (119)
- Her Body and Other Parties: StoriesDari EverandHer Body and Other Parties: StoriesPenilaian: 4 dari 5 bintang4/5 (821)
- APN 1st Quarter EnewsletterDokumen9 halamanAPN 1st Quarter EnewsletterLukas J. TanBelum ada peringkat
- PGM Calendar of EventsDokumen1 halamanPGM Calendar of EventsPGM Tour (Professional Golf of Malaysia)Belum ada peringkat
- PDC MasterplanDokumen10 halamanPDC MasterplanAbdul Basith Abdul HalimBelum ada peringkat
- Buletin Mutiara Dec # 1 - English, Chinese, TamilDokumen48 halamanBuletin Mutiara Dec # 1 - English, Chinese, TamilChan LilianBelum ada peringkat
- Unesco Heritage Brochure - PenangDokumen6 halamanUnesco Heritage Brochure - PenangDaniel Napitupulu0% (1)
- Malaysian Legal SystemDokumen16 halamanMalaysian Legal SystemPrayveen Raj SchwarzeneggerBelum ada peringkat
- The Future Challenges of Local Authorities in Mala PDFDokumen6 halamanThe Future Challenges of Local Authorities in Mala PDFMuhammad IzwanBelum ada peringkat
- Globetronics Technology BHD - Annual Report 2021Dokumen170 halamanGlobetronics Technology BHD - Annual Report 2021ZeenaBelum ada peringkat
- Apr23 - Vivo E-BrochureDokumen27 halamanApr23 - Vivo E-BrochureMinyiBelum ada peringkat
- Baba and Nyonya at Malacca and PenangDokumen4 halamanBaba and Nyonya at Malacca and PenangRabiatul Adawiyah Ismail0% (3)
- George Town Festival 2017 GuideDokumen41 halamanGeorge Town Festival 2017 GuidefirelightBelum ada peringkat
- Maklumat Pelajar Sesi Julai 2007 (WARISPENJAMIN)Dokumen356 halamanMaklumat Pelajar Sesi Julai 2007 (WARISPENJAMIN)api-3818336Belum ada peringkat
- Landslide Tanjung Bungah, Pulau PinangDokumen18 halamanLandslide Tanjung Bungah, Pulau Pinangkhairi shaariBelum ada peringkat
- PSV Discount IM Clinics List ClinicDokumen1 halamanPSV Discount IM Clinics List ClinicArif izzuddinBelum ada peringkat
- CV Summary for Finance ProfessionalDokumen4 halamanCV Summary for Finance ProfessionalPrakashRajjBelum ada peringkat
- SWM Penang PDFDokumen57 halamanSWM Penang PDFAfifah FauziBelum ada peringkat
- Chap.2 - History of Book PublishingDokumen46 halamanChap.2 - History of Book PublishingNur Aisyah BalqisBelum ada peringkat
- To Heal The SickDokumen1 halamanTo Heal The SickMuhammad Syamsul Bahri GintingBelum ada peringkat
- Naveed Yousaf's CV: Experienced IT ProfessionalDokumen2 halamanNaveed Yousaf's CV: Experienced IT ProfessionalZurina Bt Haji OsmanBelum ada peringkat
- Chee Hong Final ReportDokumen26 halamanChee Hong Final ReportIka Zakaria100% (1)
- Panel Workshop List 2022 - 06 - 01 (14 August)Dokumen14 halamanPanel Workshop List 2022 - 06 - 01 (14 August)Justin LiowBelum ada peringkat
- Msia Nothern Region Travel GuideDokumen56 halamanMsia Nothern Region Travel Guideyusaw618812Belum ada peringkat
- 3 Charter of JusticeDokumen6 halaman3 Charter of JusticeLEE YI XUANBelum ada peringkat
- Bahagian 3.4: Earthworks (Class F)Dokumen11 halamanBahagian 3.4: Earthworks (Class F)RizalFaizBelum ada peringkat
- PenangTouristSurveyReport 2017 PDFDokumen59 halamanPenangTouristSurveyReport 2017 PDFeve limBelum ada peringkat
- Process Engineers - CONCEPT DETAILS (Plating)Dokumen1 halamanProcess Engineers - CONCEPT DETAILS (Plating)vkmsBelum ada peringkat
- Contoh Resume EnglishDokumen3 halamanContoh Resume Englishadyworld93% (14)
- Frequency Radio MalaysiaDokumen3 halamanFrequency Radio MalaysiaMuhammad Hareez Prince NieaBelum ada peringkat
- Penang MapDokumen2 halamanPenang MapYusri BidinBelum ada peringkat
- Buletin Mutiara - Mac #1, 2015Dokumen48 halamanBuletin Mutiara - Mac #1, 2015Chan LilianBelum ada peringkat