Amputation Levels
Diunggah oleh
Rachel Caldito0 penilaian0% menganggap dokumen ini bermanfaat (0 suara)
39 tayangan11 halamanAmputaiton
Hak Cipta
© © All Rights Reserved
Format Tersedia
DOC, PDF, TXT atau baca online dari Scribd
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniAmputaiton
Hak Cipta:
© All Rights Reserved
Format Tersedia
Unduh sebagai DOC, PDF, TXT atau baca online dari Scribd
0 penilaian0% menganggap dokumen ini bermanfaat (0 suara)
39 tayangan11 halamanAmputation Levels
Diunggah oleh
Rachel CalditoAmputaiton
Hak Cipta:
© All Rights Reserved
Format Tersedia
Unduh sebagai DOC, PDF, TXT atau baca online dari Scribd
Anda di halaman 1dari 11
1-Amputation Levels
Amputation levels above the knee are shown in Figure 1. These
levels include the following:
Hemipelvectomy is the loss of any part of the ilium, ischium, and
pubis.
Hip disarticulation is the loss of all of the femur. The
hemipelvectomy and hip disarticulation procedures are usually
done in cases of malignant tumors, extensive gangrene, massive
trauma, or advanced infection.
Short transfemoral amputations occur when lessthan !" of
femoral length is present. A larger weight bearing surface can be
created if femoral transaction can be done at the level of the lesser
trochanter. This level retains the femoral head and neck and the
greater trochanter, resulting in improved prosthetic fit. The number
of transfemoral amputations has declined since the 1#$%s. This
decline is due to improved surgical techni&ues and better
preoperative assessment of vascular status.
Medium tansfemoral amputations occur when between ! and
'%" of femoral length is present. (deally, tansfemoral limbs should
be at least ) inches or 1% cm above the lower end of the femur to
allow room for the prosthetic knee. (n a transfemoral amputation,
both anterior and posterior muscular surfaces are well vasculari*ed+
therefore, e&ual flaps are fashioned.
A rotationplasty is applicable to patients who have a malignant
tumor in the middle or distal femur. (t is also done in cases of
,FF-. A rotationsplasty involves an osteotomy in the proximal
third of the femur, distal to the lesser trochanter, and in the
proximal part of the tibia, distal to the tibial tuberosity. The foot is
rotated 1$%. and the tibia reattached to the remaining femur. The
foot is fit into the prosthesis and acts as a knee /oint. ,rosthetically,
this amputation has the advantage of preserving the anatomic ankle
/oint, which acts as a knee /oint, and a long lever arm for better
prosthesis control. The rotationsplasty procedure is illustrated in
Figure 0.
Long transfemoral amputations occur when more than '%" of
femoral length is present but not capable of end bearing. A
transfemoral amputation is depicted in Figure 111).
In a supracondylar amputation, the patella may be left for better
end bearing. 2owever, the area created between the end of the
femur and the patella may delay healing.
A knee disarticulation amputation offers good weight distribution
and retains a long, powerful, muscle 3 stabili*ed femoral lever arm.
(n addition, the thigh muscles are completely preservfed, thereby
ensuring good muscular balance. This amputation maintains the
femoral length in growing children by preserving the growth
potential of the distal femoral epiphysis. 2owever, the knee
disarticulation amputation yields a noncosmetic socket because of
the need for an external /oint mechanism and resulting difficulty
with swing1phase control. 4nee disarticulation amputation is often
performed on the patient who will not become a prosthetic walker.
This amputation avoids the possibility of knee flexion contractures
and provides an excellent platform for sitting and transfers.
Transtibial amputation levels are depicted in Figure . These
include the flowing:
A very short transtibial amputation occurs when less than 0%" of
tibial length is present. This amputation may result from trauma
and is usually not done as an elective procedure. A very short
transtibial amputation results in a small1moment arm, making knee
extension difficult. 5oment arms are further described in 6hapter
!, 78iomechanics (mplications of ,rosthetic and 9rthosis7.
A standard transtibial amputation occurs when between 0% and
!%" of tibial length is present. An elective amputation in the
middle third of the tibia, regardless of measured length, provides a
well1padded and biomechanically sufficient lever arm. At least $
cm of tibia is re&uired below the knee /oint for optimal fitting of a
prosthesis.
A long transtibial amputation occurs when more than !%" of
tibital length is present. This amputation is not advised because of
poor blood supply in the distal leg.
The level of tibial transaction should be as long as possible
between the tibial tubercle and the /unction of the middle and distal thirds
of the tibia. A long posterior flap for transtibial amputations is
advantageous because it is well vasculari*ed and provides an excellent
weight1bearing surface. (n addition, the scar is on the anterior border, an
area that is sub/ect to less weight bearing. The deep calf musculature is
often thinned to reduce the bulk of the posterior flap.
(n a transtibial amputation, the fibula is transected 1 to 0 cm shorter
than the tibia to avoid distal fibula pain. (f the fibula is transected at the
same length as the tibia, the patient senses that the fibula is too long,
which may cause pain over the distal fibula. (f the fibula is cut too short,
a more conical shape, rather than the desired cylindrical 3 shape residual
limb results. The cylindrical shape is better suited for total contact
prosthetic fitting techni&ues. A bevel is placed on the anterior distal tibia
to minimi*e tibial pain on weight bearing. To avoid a painful neuroma, a
collection of axons and fibrous tissue, nerves should be identified, drawn
down, severed, and allowed to retract at least to ! cm away from the
areas of weight1bearing pressure.
A Syme amputation was named for :ames syme, a noted ;niversity of
<dinburg surgeon, in the mid11$%%s. This amputation is an ankle
disarticulation in which the heel pad is kept for good weight bearing. The
=yme amputation results in a residual limb that possesses good function
due to the long lever arm to control the prosthesis and the ability to
ambulate without the prosthesis.
Associated problems with the =yme amputation include an
unstable heel flap, development of neuromas of the posterior tibial nerve,
and poor cosmesis. ,erformed properly, the residual limb is ideally suited
for weight bearing and lasts virtually the life of the patient.
The bulky residual limb that results from a =yme amputation may
be streamlined by trimming the remaining metaphyseal flares of the tibia
and fibula
oot amputations levels are depicted in Figure ). These include
the following:
A transmetatarsal amputation >T5A? may be performed for
deformities resulting from trauma to the toes, infection or gangrene
due to frostbite, diabetes, arteriosclerosis, or autoimmune
circulatory connective tissue disorders. There are approximately
1%,%%% T5As a year in the ;nited =tates, with a failure rate of
about %". 9f all the amputations done in the ;nited 4ingdom,
this amputation has the highest failure rate. This high failure rate is
due to a combination of substantial loss of weight1bearing areas on
the neuropathic foot and the decreased foot length available to
generate a plantarflexor moment. As a result, the remaining tissues
bear an increased load. This amputation should b elimited to
patients with an intact posterior tibial pulse, a warm foot, and
locali*ation of osteomyelitis or gangrene to the phalanges. A dorsal
incision is made through the mid1to proximal metatarsal shafts. A
long, thick, myocutaneous plantar flap including the flexor tendons
is used, with closure of this flap onto the dorsum of the foot. The
transmetatarsal procedure is depicted in Figure. 110%.
The Lisfranc amputation is done at the tarsometatarsal /oint and
involves a disarticulation of all five metatatarsal and digitis.
The !hopart amputation, at the talonavicular and clacaneocuboid
/oints, involves a disarticulation through the midtarsal /oint leaving
only the clacaneus and talus. 8oth the @isfranc and 6hopart
amputations were introduced before blood transfusions and
antibiotics were available. They were planned as diarticulations to
be performed as rapidly as possible. These amputations often result
in an e&uines and varus deformity due to the pull of the
plantarflexors and loss of dorsiflexor and peroneal muscles. (n
addition, a distal sensitive end often leads to skin breakdown.
There is much less indication for their use today.
A trransphalangeal >toe disarticulation? amputation is done at the
metatarsophalangeal /oint. Toe disarticulations result in
biomechnical deficiencies. Amputation of the great toe affects
push1off during fast walking and running+ as a result, patients with
,A- often have a nonpropulsive gait pattern. (f the base of the
proximal phalanx with the insertion of the flexor hallucis brevis
issaved, stability is enhanced. =econd1digit amputation results in
severe hallux valgus.
"halangeal or partial toe amputation involves excision of any part
of one or more toes. The lesser toes serve little function in patients
with ischemic ,A-. As a result, gait is not markedly affected with
amputation of the lessor toes. ,rosthesis is usually not necessary
for teo amputations.
(n general, as much viable tissue as possible shouldbe preserved
after hand in/ury and partial amputation. This view must, however, be
tempered with an appreciation of what will remain functional. The
retention of a finger or part of one which is anaesthetic, cold and stiff
dose no service to the patient and will actively discourage use of the hand
and ability to work and, even after amputation, pain and a lack of desire
to return to normal function will persist.
#-$pper limb levels of amputation
Amputation of %igits
Benerally the level will be determined by the degree of in/ury fig.!.
(f the in/ury is solely to the index or little finger, useful function is
unlikely unless one and a half phalanges are still present. <ven at this
level initial acceptance of this limited loss by the patient is often
transmuted into a desire for cosmesis and later amputation is re&uested.
The best cosmesis is achieved by amputation through the metacarpal
shaft with suitable beveling.This, however, reduces the span of the hand
and power of the grip and it may be better in largey manual workers to
amputate through the metacarpophalangeal /oint.
The long and ring fingers are best amputated through whatever
level will leave a mobile and comfortable stump. <ven a very short
stump, for example the proximal phalanx, may have some definite
functional value and in the half1closed position be at least cosmetically
acceptable. Amputations of either of these fingers in which the metatarsal
ray is excised for cosmetic reasons may seriously disturb function and are
seldom desirable.
As much of the thumb as can be must be preserved for as long as
possible. Any stump covered with sensititive skin may be of great value.
&rist disarticulation
(ndications for wrist disarticulation are rare but usually related to severe
trauma to the hand with considerable loss of tissue and loss of sensation.
Any tissue with sensation should be preserved. <ven carpal bones and
remnants of metacarpals, providing they are covered by viable skin, may
be useful as the wrist extensors and flexor may be preserved as well.
The orearm
The usual indications for amputation through the forearm are for
severe trauma affecting the wrist and hand and occasionally it is used as
treatment for chronic sepsis or tumour of the hand.
(deally as with other amputations, the stump should be as long as
possible. A too distal amputation, however, whilst having the advantage
of a long lever and ease of fitting, often suffers from cold and cyanotic
skin with little subcutaneous and muscular tissue covering the bone ends.
Therefore the ideal distance is 1Ccm measured from the olecranon in the
average adult and this roughly corresponds to the /unction of the proximal
two1thirds and the distal one1third of the forearm.
9ccasionally the extent of the trauma or disease affecting the hand
and forearm may be too great to allow a useful below1elbow stump to be
fashioned. (n the past conventional treatment would have been to
amputate at the level of the distal humerus but as a result of the recent
improvements in prosthetic design, disarticulation at the elbow is
preferable. (t looks as though it will be possible, by retaining the bulbous
stump, to have a self1retaining socket and a better /oint in the future.
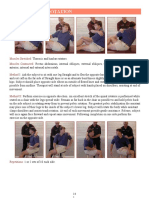
Techni&ue. The skin flaps will often be determined by whatever
skin is available but where possible &ual anterior and posterior flaps
should be made the incisions beginning at the level of the humeral
epicondyles and extending distally ) cm beyond the point of the
olecranon posteriorly and to point /ust distal to the insertion of the biceps
anteriorly.
Amputation through the Humerus
The commonest indication is severe truma of the forearm.
9ccasionally this amputation may be used for sepsis or malignant
tumours. As elsewhere in the upper limb the level may be determined by
factors beyond the surgeonDs control. The ideal is 1%cm above the elbow
/oint, which leaves room for the elbow mechanism in the prosthesis and
provides the best length of stump for fitting. Above this level as long a
stump as possible should be retained.
Amputation through the 'eck of the Humerus
This operation does not leave the patient with any functional stump
and should not be performed when it is possible to leave a humeral stump
extending to three finger breadths below the anterior axillary fold. This is
the critical minimal length to which an upper limb.
,rosthesis can be fitted. (t the amputation is being performed for
malignant tumour at the lower end of the humerus there is no alternative
but diarticulation at the shoulder /oint. To leave the humeral head in situ
when it is permitted on pathological grounds, however, produces a better
cosmetic appearance, particularly when wearing clothes, by preserving
the rounded contour of the shoulder.
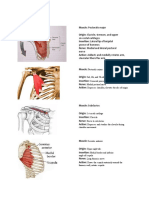
Shoulder disarticulation
The arm completely lost
ore(uarter Amputation
6lavicle, scapula, and arm are excised. This amputation is rarely
performed and is indicated only for malignant tumours around the
shoulder /oint, particularly where the tumour has spread into the
surrounding muscles so that the less mutilating procedures of
disarticulation of the shoulder or amputation through the neck of the
humerus are no longer practicable.
Fig .1 above knee levels of amputation
Fig. 0 Eotationplasty
Fig. transtibial >below knee? amputation
Fig.) foot amputation levels
Fig.! upper limb amputation levels
Anda mungkin juga menyukai
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDari EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RacePenilaian: 4 dari 5 bintang4/5 (895)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDari EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifePenilaian: 4 dari 5 bintang4/5 (5794)
- The Impact of Frequent Injections For Hematopoietic Growth Factor Support On Patients Receiving Chemotherapy An Observational StudyDokumen6 halamanThe Impact of Frequent Injections For Hematopoietic Growth Factor Support On Patients Receiving Chemotherapy An Observational StudyRachel CalditoBelum ada peringkat
- Why The Fair Innings Argument Is Not Persuasive: Michael M RivlinDokumen6 halamanWhy The Fair Innings Argument Is Not Persuasive: Michael M RivlinRachel CalditoBelum ada peringkat
- 2052 3211 6 1 PDFDokumen2 halaman2052 3211 6 1 PDFRachel CalditoBelum ada peringkat
- BMC NursingDokumen5 halamanBMC NursingRachel CalditoBelum ada peringkat
- NG2 Cells, A New Trail For Alzheimer 'S Disease Mechanisms?: Research Open AccessDokumen13 halamanNG2 Cells, A New Trail For Alzheimer 'S Disease Mechanisms?: Research Open AccessRachel CalditoBelum ada peringkat
- Heart Failure (HF), Also Known As Chronic Heart Failure (CHF), Is When The Heart Is Unable To PumpDokumen1 halamanHeart Failure (HF), Also Known As Chronic Heart Failure (CHF), Is When The Heart Is Unable To PumpRachel CalditoBelum ada peringkat
- Knowledge About The Administration and Regulation of High Alert Medications Among Nurses in Palestine: A Cross-Sectional StudyDokumen17 halamanKnowledge About The Administration and Regulation of High Alert Medications Among Nurses in Palestine: A Cross-Sectional StudyRachel CalditoBelum ada peringkat
- Germany RequirementsDokumen1 halamanGermany RequirementsRachel CalditoBelum ada peringkat
- Talk That Talk (Rihanna Song)Dokumen2 halamanTalk That Talk (Rihanna Song)Rachel CalditoBelum ada peringkat
- Growth Hormone (GH) or Somatotropin, Also Known As Human Growth Hormone (HGH or HGH)Dokumen1 halamanGrowth Hormone (GH) or Somatotropin, Also Known As Human Growth Hormone (HGH or HGH)Rachel CalditoBelum ada peringkat
- BLS-ACLS Sched 2H2018 PDFDokumen1 halamanBLS-ACLS Sched 2H2018 PDFRachel CalditoBelum ada peringkat
- ResignationDokumen2 halamanResignationRachel CalditoBelum ada peringkat
- BiochemDokumen2 halamanBiochemRachel CalditoBelum ada peringkat
- Shoe Dog: A Memoir by the Creator of NikeDari EverandShoe Dog: A Memoir by the Creator of NikePenilaian: 4.5 dari 5 bintang4.5/5 (537)
- Grit: The Power of Passion and PerseveranceDari EverandGrit: The Power of Passion and PerseverancePenilaian: 4 dari 5 bintang4/5 (588)
- The Yellow House: A Memoir (2019 National Book Award Winner)Dari EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Penilaian: 4 dari 5 bintang4/5 (98)
- The Little Book of Hygge: Danish Secrets to Happy LivingDari EverandThe Little Book of Hygge: Danish Secrets to Happy LivingPenilaian: 3.5 dari 5 bintang3.5/5 (400)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDari EverandNever Split the Difference: Negotiating As If Your Life Depended On ItPenilaian: 4.5 dari 5 bintang4.5/5 (838)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDari EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FuturePenilaian: 4.5 dari 5 bintang4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDari EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryPenilaian: 3.5 dari 5 bintang3.5/5 (231)
- Rise of ISIS: A Threat We Can't IgnoreDari EverandRise of ISIS: A Threat We Can't IgnorePenilaian: 3.5 dari 5 bintang3.5/5 (137)
- The Emperor of All Maladies: A Biography of CancerDari EverandThe Emperor of All Maladies: A Biography of CancerPenilaian: 4.5 dari 5 bintang4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDari EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaPenilaian: 4.5 dari 5 bintang4.5/5 (266)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDari EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersPenilaian: 4.5 dari 5 bintang4.5/5 (345)
- On Fire: The (Burning) Case for a Green New DealDari EverandOn Fire: The (Burning) Case for a Green New DealPenilaian: 4 dari 5 bintang4/5 (74)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDari EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyPenilaian: 3.5 dari 5 bintang3.5/5 (2259)
- Team of Rivals: The Political Genius of Abraham LincolnDari EverandTeam of Rivals: The Political Genius of Abraham LincolnPenilaian: 4.5 dari 5 bintang4.5/5 (234)
- The Unwinding: An Inner History of the New AmericaDari EverandThe Unwinding: An Inner History of the New AmericaPenilaian: 4 dari 5 bintang4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDari EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You ArePenilaian: 4 dari 5 bintang4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Dari EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Penilaian: 4.5 dari 5 bintang4.5/5 (121)
- Her Body and Other Parties: StoriesDari EverandHer Body and Other Parties: StoriesPenilaian: 4 dari 5 bintang4/5 (821)
- Syndactyly 1Dokumen13 halamanSyndactyly 1AminullahBelum ada peringkat
- A) Biphalangeal Fifth Toe PDFDokumen4 halamanA) Biphalangeal Fifth Toe PDFericdgBelum ada peringkat
- LESSON PLAN - Beauty Care-Foot SpaDokumen7 halamanLESSON PLAN - Beauty Care-Foot SpaGwen SalabsabBelum ada peringkat
- CTS Employees Compensation Insurance PolicyDokumen21 halamanCTS Employees Compensation Insurance Policynivasshaan0% (1)
- Amputatii PiciorDokumen21 halamanAmputatii PiciorAloexandru All IonBelum ada peringkat
- Automation of Shoe Last Modification andDokumen80 halamanAutomation of Shoe Last Modification andVijay UB100% (1)
- Swanson Toe ReplacementDokumen19 halamanSwanson Toe ReplacementJacob DoughertyBelum ada peringkat
- Oina SummaryDokumen37 halamanOina SummaryC1 - RAZALAN NICKA JOYBelum ada peringkat
- Partial Foot AmputationDokumen38 halamanPartial Foot AmputationVandana SinghBelum ada peringkat
- DR Anurag TalesraDokumen5 halamanDR Anurag Talesraapi-200677911Belum ada peringkat
- Kay SPJ: Cleft Hand, in Green DP (Ed) : Green's Operative Hand Surgery. Philadelphia, Pa, Churchill Livingston, 1999, PP 402-414Dokumen75 halamanKay SPJ: Cleft Hand, in Green DP (Ed) : Green's Operative Hand Surgery. Philadelphia, Pa, Churchill Livingston, 1999, PP 402-414Héctor Pando SánchezBelum ada peringkat
- Msu-Celp P 1 Certificate of English Language Proficiency: Ractice TestDokumen29 halamanMsu-Celp P 1 Certificate of English Language Proficiency: Ractice TestminiseviBelum ada peringkat
- Physical and Medical Standards: Appendix A General InstructionsDokumen22 halamanPhysical and Medical Standards: Appendix A General InstructionssreyasBelum ada peringkat
- Yamamoto 2016Dokumen7 halamanYamamoto 2016Stefanie LoiseBelum ada peringkat
- Foot JournalDokumen13 halamanFoot Journalay100% (1)
- Sept 2019 RecallsDokumen18 halamanSept 2019 RecallsAbdullah Mohammad Ibne HaiderBelum ada peringkat
- Lecture Activities No. 6 Skeletal System: Guide Questions AnswersDokumen13 halamanLecture Activities No. 6 Skeletal System: Guide Questions AnswersPrancheska Abigayle Peneyra SantiagoBelum ada peringkat
- 411 419Dokumen9 halaman411 419Afif MansorBelum ada peringkat
- Hallux VarusDokumen18 halamanHallux VarusSneha SutharBelum ada peringkat
- Diabetic Foot: The Orthopedic Surgery Angle:, T. Leemrijse, P.-A. DeleuDokumen16 halamanDiabetic Foot: The Orthopedic Surgery Angle:, T. Leemrijse, P.-A. DeleuDewi Sartika100% (1)
- Active Isolated Stretching The Mattes Method 151 184Dokumen38 halamanActive Isolated Stretching The Mattes Method 151 184Nazareth Varas AlonsoBelum ada peringkat
- Agnikarma Criticle ReviewDokumen158 halamanAgnikarma Criticle Reviewrauol100% (4)
- A Review Article On Mode of Action of PadabhyangaDokumen5 halamanA Review Article On Mode of Action of PadabhyangaEditor IJTSRDBelum ada peringkat
- Daftar Nama Anatomi Inggris-LatinDokumen58 halamanDaftar Nama Anatomi Inggris-LatinFelicia NikeBelum ada peringkat
- Clinical Presentation of Diabetic FootDokumen13 halamanClinical Presentation of Diabetic FootMehek BatraBelum ada peringkat
- The Toepro Foot/Ankle Exercise PlatformDokumen2 halamanThe Toepro Foot/Ankle Exercise PlatformelproedrosBelum ada peringkat
- Clinical Cases and Osces in SurgeryDokumen278 halamanClinical Cases and Osces in SurgeryTristan Greene100% (5)
- 5 Deformities of Lower Limb NCBDokumen82 halaman5 Deformities of Lower Limb NCBShiv Ram100% (1)
- 11 Tibia & Fibula (A)Dokumen29 halaman11 Tibia & Fibula (A)idaramaBelum ada peringkat
- Top of The Foot Pain and Swelling TreatmentDokumen13 halamanTop of The Foot Pain and Swelling TreatmentNyanLinKyawBelum ada peringkat