Chronic Follicular Conjunctivitis
Diunggah oleh
Tiodora Wike Ds0 penilaian0% menganggap dokumen ini bermanfaat (0 suara)
124 tayangan7 halamanChronic follicular conjunctivitis is a mild type of chronic inflammation associated with follicular hyperplasia, predominantly involving the lower eyelid. There are several etiological types including infective, toxic, chemical, and allergic. Allergic conjunctivitis is characterized by itching and can be seasonal or perennial. Signs include conjunctival injection, edema, clear discharge, and papillae formation. Treatment involves antihistamines, mast cell stabilizers, and short term steroid drops under supervision.
Deskripsi Asli:
Hak Cipta
© © All Rights Reserved
Format Tersedia
DOCX, PDF, TXT atau baca online dari Scribd
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniChronic follicular conjunctivitis is a mild type of chronic inflammation associated with follicular hyperplasia, predominantly involving the lower eyelid. There are several etiological types including infective, toxic, chemical, and allergic. Allergic conjunctivitis is characterized by itching and can be seasonal or perennial. Signs include conjunctival injection, edema, clear discharge, and papillae formation. Treatment involves antihistamines, mast cell stabilizers, and short term steroid drops under supervision.
Hak Cipta:
© All Rights Reserved
Format Tersedia
Unduh sebagai DOCX, PDF, TXT atau baca online dari Scribd
0 penilaian0% menganggap dokumen ini bermanfaat (0 suara)
124 tayangan7 halamanChronic Follicular Conjunctivitis
Diunggah oleh
Tiodora Wike DsChronic follicular conjunctivitis is a mild type of chronic inflammation associated with follicular hyperplasia, predominantly involving the lower eyelid. There are several etiological types including infective, toxic, chemical, and allergic. Allergic conjunctivitis is characterized by itching and can be seasonal or perennial. Signs include conjunctival injection, edema, clear discharge, and papillae formation. Treatment involves antihistamines, mast cell stabilizers, and short term steroid drops under supervision.
Hak Cipta:
© All Rights Reserved
Format Tersedia
Unduh sebagai DOCX, PDF, TXT atau baca online dari Scribd
Anda di halaman 1dari 7
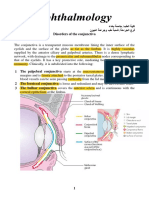
CHRONIC FOLLICULAR CONJUNCTIVITIS
It is a mild type of chronic catarrhal conjunctivitis associated with follicular hyperplasia,
predominantly
involving the lower lid.
Etiological types
1. I nfective chronic follicular conjunctivitis is essentially a condition of 'benign folliculosis'
with a superadded mild infection. Benign folliculosis, also called 'School folliculosis', mainly
affects school children. This condition usually occurs as a part of generalized lymphoid
hyperplasia of the upper respiratory tract (enlargement of adenoids and tonsils) seen at this age.
It may be associated with malnutrition, constitutional disorders and unhygienic conditions. In
this condition, follicles are typically arranged in parallel rows in the lower palpebral conjunctiva
without any associated conjunctival hyperaemia (Fig.4.18).
2. Toxic type of chronic follicular conjunctivitis is seen in patients suffering from molluscum
contagiosum. This follicular conjunctivitis occurs as a response to toxic cellular debris
desquamated into the conjunctival sac from the molluscum contagiosum nodules present on the
lid margin (the primary lesion).
3. Chemical chronic follicular conjunctivitis. It is an irritative follicular conjunctival response
which occurs after prolonged administration of topical medication. The common topical
preparations associated with chronic follicular conjunctivitis are: idoxuridine (IDU), eserine,
pilocarpine, DFP and adrenaline.
4. Chronic allergic follicular conjunctivitis. A true allergic response is usually papillary.
However, a follicular response is also noted in patients with 'contact dermoconjunctivitis'.
Allergic conjunctivitis
HistoryThe main feature of allergic conjunctivitis is itching. Both eyes usually are affected
and there may be a clear discharge. There may be a family history of atopy or recent contact with
chemicals or eye drops. Similar symptoms may have occurred in the same season in previous
years. It is important to differentiate between an acute allergic reaction and a more long term
chronic allergic eye disease.
ExaminationThe conjunctivae are diffusely injected and may be oedematous (chemosis). The
discharge is clear and stringy. Because of the fibrous septa that tether the eyelid (tarsal)
conjunctivae, oedema results in round swellings (papillae). When these are large they are
referred to as cobblestones.
ManagementTopical antihistamine and vasoconstrictor eye drops provide short term relief.
Eye drops that prevent degranulation of mast cells also are useful, but they may need to be used
for several weeks or months to achieve maximal effect. Oral antihistamines may also be used,
particularly the newer compounds that cause less sedation. Topical steroids are effective but
should not be used without regular ophthalmological supervision because of the risk of steroid
induced cataracts and glaucoma, which may irreversibly
ALLERGIC CONJUNCTIVITIS
It is the inflammation of conjunctiva due to allergic or hypersensitivity reactions which may be
immediate (humoral) or delayed (cellular). The conjunctiva is ten times more sensitive than the
skin to allergens.
Types
1. Simple allergic conjunctivitis
_ Hay fever conjunctivitis
_ Seasonal allergic conjunctivitis (SAC)
_ Perennial allergic conjunctivitis (PAC)
2. Vernal keratoconjunctivitis (VKC)
3. Atopic keratoconjunctivitis (AKC)
4. Giant papillary conjunctivitis (GPC)
5. Phlyctenular keratoconjunctivitis (PKC)
6. Contact dermoconjunctivitis (CDC)
Simple Allergic Conjunctivitis
It is a mild, non-specific allergic conjunctivitis characterized by itching, hyperaemia and mild
papillary response. Basically, it is an acute or subacute urticarial reaction.
Etiology
It is seen in following forms:
1. Hay fever conjunctivitis. It is commonly associated with hay fever (allergic rhinitis). The
common allergens are pollens, grass and animal dandruff.
2. Seasonal allergic conjunctivitis (SAC). SAC is a response to seasonal allergens such as grass
pollens. It is of very common occurrence.
3. Perennial allergic conjunctivitis (PAC) is a response to perennial allergens such as house dust
and mite. It is not so common.
Pathology
Pathological features of simple allergic conjunctivitis comprise vascular, cellular and
conjunctival
responses.
1. Vascular response is characterised by sudden and extreme vasodilation and increased
permeability of vessels leading to exudation.
2. Cellular response is in the form of conjunctival infiltration and exudation in the discharge of
eosinophils, plasma cells and mast cells producing histamine and histamine-like substances.
3. Conjunctival response is in the form of boggy swelling of conjunctiva followed by increased
connective tissue formation and mild papillary hyperplasia.
Clinical picture
Symptoms include intense itching and burning sensation in the eyes associated with watery
discharge and mild photophobia.
Signs.
(a) Hyperaemia and chemosis which give a swollen juicy appearance to the conjunctiva.
(b) Conjunctiva may also show mild papillary reaction.
(c) Oedema of lids.
Diagnosis
Diagnosis is made from : (1) typical symptoms and signs; (2) normal conjunctival flora; and (3)
presence of abundant eosinophils in the discharge.
Treatment
1. Elimination of allergens if possible.
2. Local palliative measures which provide immediate relief include:
i. Vasoconstrictors like adrenaline, ephedrine, and naphazoline.
ii. Sodium cromoglycate drops are very effective
in preventing recurrent atopic cases.
iii. Steroid eye drops should be avoided. However, these may be prescribed for short duration in
severe and non-responsive patients.
3. Systemic antihistaminic drugs are useful in acute cases with marked itching.
4. Desensitization has been tried without much rewarding results. However, a trial may be given
in recurrent cases.
VERNAL KERATOCONJUNCTIVITIS (VKC) OR SPRING CATARRH
It is a recurrent, bilateral, interstitial, self-limiting, allergic inflammation of the conjunctiva
having a periodic seasonal incidence.
Etiology
It is considered a hypersensitivity reaction to some exogenous allergen, such as grass pollens.
VKC is thought to be an atopic allergic disorder in many cases, in which IgE-mediated
mechanisms play an important role. Such patients may give personal or family history of other
atopic diseases such as hay fever, asthma, or eczema and their peripheral blood shows
eosinophilia and inceased serum IgE levels. Predisposing factors
1. Age and sex. 4-20 years; more common in boys than girls.
2. Season. More common in summer; hence the name spring catarrh looks a misnomer. Recently
it is being labelled as 'Warm weather conjunctivitis'.
3. Climate. More prevalent in tropics, less in temperate zones and almost non-existent in cold
climate.
Pathology
1. Conjunctival epithelium undergoes hyperplasia and sends downward projections into the
subepithelial tissue.
2. Adenoid layer shows marked cellular infiltration by eosinophils, plasma cells, lymphocytes
and histiocytes.
3. Fibrous layer shows proliferation which later on undergoes hyaline changes.
4. Conjunctival vessels also show proliferation, increased permeability and vasodilation.
All these pathological changes lead to formation of multiple papillae in the upper tarsal
conjunctiva.
Clinical picture
Symptoms. Spring catarrh is characterised by marked burning and itching sensation which is
usually intolerable and accentuated when patient comes in awarm humid atmosphere. Itching is
more marked with palpebral form of disease. Other associated symptoms include: mild
photophobia, lacrimation, stringy (ropy) discharge and heaviness of lids.
Signs of vernal keratoconjunctivitis can be described in following three clinical forms:
1. Palpebral form. Usually upper tarsal conjunctiva of both eyes is involved. The typical lesion is
may hypertrophy to produce cauliflower like excrescences of 'giant papillae'. Conjunctival
changes are associated with white ropy discharge. characterized by the presence of hard, flat
topped, papillae arranged in a 'cobble-stone' or 'pavement
stone', fashion (Fig. 4.20). In severe cases, papillae may hypertrophy to produce cauliflower like
excrescences of 'giant papillae'. Conjunctival changes are associated with white ropy discharge.
Fig. 4.20. Palpebral form of vernal keratoconjunctivitis
2. Bulbar form. It is characterised by: (i) dusky red triangular congestion of bulbar conjunctiva in
palpebral area; (ii) gelatinous thickened accumulation of tissue around the limbus; and (iii)
presence of discrete whitish raised dots along the limbus (Tranta's spots) (Fig. 4.21).
3. Mixed form. It shows combined features of both palpebral and bulbar forms (Fig. 4.22).
Vernal keratopathy. Corneal involvement in VKC may be primary or secondary due to
extension of limbal lesions. Vernal keratopathy includes following 5 types of lesions:
1. Punctate epithelial keratitis involving upper cornea is usually associated with palpebral form
of disease. The lesions always stain with rose bengal and invariably with fluorescein dye.
2. Ulcerative vernal keratitis (shield ulceration) presents as a shallow transverse ulcer in upper
part of cornea. The ulceration results due to epithelial macroerosions. It is a serious problem
which may be complicated by bacterial keratitis.
3. Vernal corneal plaques result due to coating of bare areas of epithelial macroerosions with a
layer of altered exudates (Fig. 4.23).
4. Subepithelial scarring occurs in the form of a ring scar.
5. Pseudogerontoxon is characterised by a classical cupids bow outline.
Fig. 4.21. Bulbar form of vernal keratoconjunctivitis
Fig. 4.22. Artist's diagram of mixed form of vernal
keratoconjunctivitis.c
Fig. 4.23. Vernal corneal plaque.
Clinical course of disease is often self-limiting and usually burns out spontaneously after 5-10
years.
Differential diagnosis. Palpebral form of VKC needs to be differentiated from trachoma with
pre-dominant
papillary hypertrophy (see page 67).
Treatment
A. Local therapy
1. Topical steroids. These are effective in all forms of spring catarrh. However, their use should
be minimised, as they frequently cause steroid induced glaucoma. Therefore, monitoring of
intraocular pressure is very important during steroid therapy. Frequent instillation (4 hourly) to
start with (2 days) should be followed by maintenance therapy for 3-4 times a day for 2 weeks.
Commonly used steroid solutions are of fluorometholone medrysone, betamethasone or
dexamethasone. Medrysone and fluorometholone are safest of all these.
2. Mast cell stabilizers such as sodium cromoglycate (2%) drops 4-5 times a day are quite
effective in controlling VKC, especially atopic cases. It is mast cell stabilizer. Azelastine eye
drops are also effective in controlling VKC.
3. Topical antihistaminics are also effective.
4. Acetyl cysteine (0.5%) used topically has mucolytic properties and is useful in the treatment of
early plaque formation.
5. Topical cyclosporine (1%) drops have been recently reported to be effective in severe
unresponsive cases.
B. Systemic therapy
1. Oral antihistaminics may provide some relief from itching in severe cases.
2. Oral steroids for a short duration have been recommended for advanced, very severe,
nonresponsive cases.
C. Treatment of large papillae. Very large (giant) papillae can be tackled either by :
_ Supratarsal injection of long acting steroid or
_ Cryo application
_ Surgical excision is recommended for extraordinarily large papillae.
D. General measures include :
_ Dark goggles to prevent photophobia.
_ Cold compresses and ice packs have soothing effects.
_ Change of place from hot to cold area is recommended for recalcitrant cases.
E. Desensitization has also been tried without much rewarding results.
F. Treatment of vernal keratopathy
_ Punctate epithelial keratitis requires no extra treatment except that instillation of steroids
should be increased.
_ A large vernal plaque requires surgical excision by superficial keratectomy.
_ Severe shield ulcer resistant to medical therapy may need surgical treatment in the form of
debridment, superficial keratectomy, excimer laser therapeutic kerateotomy as well as amniotic
membrane transplantation to enhance reepithelialization.
Anda mungkin juga menyukai
- Allergic Eye Diseases MSRDokumen11 halamanAllergic Eye Diseases MSRnafilBelum ada peringkat
- Conjunctivitis, Allergic: Author: Parag A Majmudar, MD, Fellowship Co-Director, Department of OphthalmologyDokumen7 halamanConjunctivitis, Allergic: Author: Parag A Majmudar, MD, Fellowship Co-Director, Department of OphthalmologyDicki Pratama HolmesBelum ada peringkat
- Ocular Allergy Esen Karamursel Akpek, MDDokumen8 halamanOcular Allergy Esen Karamursel Akpek, MDAndri SaputraBelum ada peringkat
- Vernal ConjungtivitisDokumen34 halamanVernal ConjungtivitisNadine WangBelum ada peringkat
- Allergic Conjunctivitis: History Is ImportantDokumen17 halamanAllergic Conjunctivitis: History Is ImportantAnnisa RahimBelum ada peringkat
- Tjo 51 45Dokumen10 halamanTjo 51 45Bryan SocorroBelum ada peringkat
- The Conjunctiva: Lecture One DR - Ali.a.taqiDokumen56 halamanThe Conjunctiva: Lecture One DR - Ali.a.taqiJorge Esteban Novelo PavíaBelum ada peringkat
- Diseases of The ConjunctivaDokumen18 halamanDiseases of The Conjunctivadykesu1806Belum ada peringkat
- Laporan Kasus Keratokonjungtivitis Atopik Dengan Limbal Stem Cell Deficiency - ViorasusiDokumen10 halamanLaporan Kasus Keratokonjungtivitis Atopik Dengan Limbal Stem Cell Deficiency - Viorasusimade dharmaBelum ada peringkat
- Referat KonjungtivitisDokumen21 halamanReferat KonjungtivitisWyendae CliquersBelum ada peringkat
- Konjungtivitis Dan KeratitisDokumen117 halamanKonjungtivitis Dan KeratitisResti Puteri ApriyuslimBelum ada peringkat
- The ConjunctivaDokumen63 halamanThe ConjunctivaMariam QaisBelum ada peringkat
- Vernal Keratoconjunctivitis: - Dr. Zulfiqar AliDokumen30 halamanVernal Keratoconjunctivitis: - Dr. Zulfiqar AliAsad FrazBelum ada peringkat
- Eye Emergency: DR Abdelmoniem SaeedDokumen63 halamanEye Emergency: DR Abdelmoniem SaeedYousef Al-AmeenBelum ada peringkat
- 2013 Article 19-VKC PDFDokumen16 halaman2013 Article 19-VKC PDFmentariBelum ada peringkat
- ConjunctivaDokumen10 halamanConjunctivawissam salimBelum ada peringkat
- CD 2Dokumen14 halamanCD 2Amira AlmutairiBelum ada peringkat
- Laporan Kasus Pada An.A Dengan Konjungtivitis Unspecified Di Poliklinik Mata Rsud SumedangDokumen15 halamanLaporan Kasus Pada An.A Dengan Konjungtivitis Unspecified Di Poliklinik Mata Rsud SumedangEvaliaRahmatPuzianBelum ada peringkat
- The ConjungtivaDokumen111 halamanThe ConjungtivaLuvita Amallia SyadhatinBelum ada peringkat
- Allaergic Conjunctivitis PathophysiologyDokumen25 halamanAllaergic Conjunctivitis PathophysiologyRabiu Hassan MusaBelum ada peringkat
- CONJUNCTIVITISDokumen67 halamanCONJUNCTIVITISNauli Panjaitan86% (7)
- Conjunctiva Anatomy and PhysiologyDokumen101 halamanConjunctiva Anatomy and PhysiologyPurva KeswaniBelum ada peringkat
- Allergic ConjunctivitisDokumen6 halamanAllergic ConjunctivitisLetisha RahmadinaBelum ada peringkat
- ABC of Red EyeDokumen5 halamanABC of Red Eyeakmar887Belum ada peringkat
- Types of ConjunctivitisDokumen20 halamanTypes of ConjunctivitisAnonymous 9lmlWQoDm8Belum ada peringkat
- Jurnal KeratitisDokumen2 halamanJurnal Keratitisanggun pratissaBelum ada peringkat
- Vernal Keratoconjunctivitis: Mast Cell StabilizersDokumen1 halamanVernal Keratoconjunctivitis: Mast Cell StabilizersIntan MayangsariBelum ada peringkat
- Conjunctivitis 1Dokumen28 halamanConjunctivitis 1Nrs Sani Sule MashiBelum ada peringkat
- 6 - 7 ConjunctivaDokumen16 halaman6 - 7 ConjunctivaMariam QaisBelum ada peringkat
- OpthaDokumen5 halamanOpthavarun2k6Belum ada peringkat
- Conjunctivitis: by PGMI Jasleen MonrealDokumen77 halamanConjunctivitis: by PGMI Jasleen MonrealJade MonrealBelum ada peringkat
- FinalDokumen105 halamanFinalBharath BalagaBelum ada peringkat
- Pemicu 2 "Ada Apa Dengan Mataku?": Adrian Pratama - 405100018 - Blok PenginderaanDokumen82 halamanPemicu 2 "Ada Apa Dengan Mataku?": Adrian Pratama - 405100018 - Blok PenginderaanRilianda SimbolonBelum ada peringkat
- Conjunctivitis - Dita LSDokumen17 halamanConjunctivitis - Dita LSMeBelum ada peringkat
- KeratitisDokumen26 halamanKeratitisHIDAYATUL RAHMIBelum ada peringkat
- Ophthalmology - Diseases of ConjunctivaDokumen11 halamanOphthalmology - Diseases of ConjunctivajbtcmdtjjvBelum ada peringkat
- High Fever, Maculopapular Rash, Perianal Desquamation, and Conjunctivitis in A 3-Year-Old BoyDokumen8 halamanHigh Fever, Maculopapular Rash, Perianal Desquamation, and Conjunctivitis in A 3-Year-Old BoyTri ApriastiniBelum ada peringkat
- Mata Merah, Visus Normal - 1Dokumen51 halamanMata Merah, Visus Normal - 1nashqonashBelum ada peringkat
- Conjunctivitis - AAFPDokumen23 halamanConjunctivitis - AAFP21613284Belum ada peringkat
- Allergic ConjunctivitisDokumen3 halamanAllergic ConjunctivitisMarisa SukoBelum ada peringkat
- Red EyesDokumen3 halamanRed EyesirijoaBelum ada peringkat
- Mata MerahDokumen119 halamanMata MerahAzwanHamdiBelum ada peringkat
- Simposium Flamicort ALLERGI Mar-2015Dokumen58 halamanSimposium Flamicort ALLERGI Mar-2015Sastra WijayaBelum ada peringkat
- Mutia Skenario B Blok 19Dokumen8 halamanMutia Skenario B Blok 19Mutia AgustriaBelum ada peringkat
- Focus: Chronic Allergic Eye DiseaseDokumen2 halamanFocus: Chronic Allergic Eye DiseaseBal QieshBelum ada peringkat
- Jurnal Mulya Dita ParamitaDokumen12 halamanJurnal Mulya Dita ParamitamulyaditaBelum ada peringkat
- 2 EczemaDokumen5 halaman2 Eczemaحسين طاهر حاتم طاهرBelum ada peringkat
- ConjunctivaDokumen85 halamanConjunctivaMuhammad AboAlasaadBelum ada peringkat
- Red Eye Differential DiagnosisDokumen70 halamanRed Eye Differential DiagnosisAdetz HaedetzBelum ada peringkat
- Viral Conjunctivitis AlgorithmDokumen8 halamanViral Conjunctivitis AlgorithmRobert Selvin MBelum ada peringkat
- Viral Keratitis: Current ConceptsDokumen8 halamanViral Keratitis: Current ConceptsDini MayrisdayaniBelum ada peringkat
- BlepharitisDokumen15 halamanBlepharitisLatoya ShopBelum ada peringkat
- Vesicular Palmoplantar EczemaDokumen16 halamanVesicular Palmoplantar EczemakcipitBelum ada peringkat
- Vernal Keratoconjunctivitis (VKC)Dokumen19 halamanVernal Keratoconjunctivitis (VKC)api-3742497Belum ada peringkat
- Adult BlepharitisDokumen11 halamanAdult BlepharitistrisnatersinandaBelum ada peringkat
- Practical Insights into Atopic DermatitisDari EverandPractical Insights into Atopic DermatitisKwang Hoon LeeBelum ada peringkat
- Folliculitis, A Simple Guide To the Condition, Treatment And Related DiseasesDari EverandFolliculitis, A Simple Guide To the Condition, Treatment And Related DiseasesBelum ada peringkat
- Systemic Inflammatory Disease and the EyeDari EverandSystemic Inflammatory Disease and the EyePenilaian: 5 dari 5 bintang5/5 (3)
- Winter Defeated: Your Subtitle Goes HereDokumen5 halamanWinter Defeated: Your Subtitle Goes HereTiodora Wike DsBelum ada peringkat
- Flower Daffodil Array: Your Subtitle Goes HereDokumen5 halamanFlower Daffodil Array: Your Subtitle Goes HereTiodora Wike DsBelum ada peringkat
- Awan BiruDokumen5 halamanAwan BiruTiodora Wike DsBelum ada peringkat
- Bola BolaDokumen5 halamanBola BolaTiodora Wike DsBelum ada peringkat
- ANJINGDokumen5 halamanANJINGTiodora Wike DsBelum ada peringkat
- Stormy: Add Your Topic HereDokumen5 halamanStormy: Add Your Topic HereTiodora Wike DsBelum ada peringkat
- Someone Like YouDokumen10 halamanSomeone Like YouTiodora Wike DsBelum ada peringkat
- Definition: in Hyperopia, There Is A Discrepancy Between The Refractive Power and Axial Length of The EyeDokumen109 halamanDefinition: in Hyperopia, There Is A Discrepancy Between The Refractive Power and Axial Length of The EyeTiodora Wike DsBelum ada peringkat
- Pemeriksaan Fisik VaskulerDokumen25 halamanPemeriksaan Fisik VaskulerTiodora Wike Ds100% (3)
- KochDokumen3 halamanKochJared NyakambaBelum ada peringkat
- MCQ's For TrainingDokumen52 halamanMCQ's For TrainingYalvant YadavBelum ada peringkat
- 336 ScabiesDokumen2 halaman336 ScabiesrozanfikriBelum ada peringkat
- Expanded Immunization Program EpiDokumen22 halamanExpanded Immunization Program EpiGirome BairaBelum ada peringkat
- CH13 Ninenth Standard NCERT BOOKDokumen26 halamanCH13 Ninenth Standard NCERT BOOKPrash ShanthBelum ada peringkat
- Antibody Diversity:Variable Joining Sites and Somatic MutationsDokumen11 halamanAntibody Diversity:Variable Joining Sites and Somatic MutationsFemi Mega LestariBelum ada peringkat
- List of Human DiseasesDokumen11 halamanList of Human DiseasesRavi PrakashBelum ada peringkat
- Full Download Test Bank For Cellular and Molecular Immunology 8th Edition Abul K Abbas Download PDF Full ChapterDokumen34 halamanFull Download Test Bank For Cellular and Molecular Immunology 8th Edition Abul K Abbas Download PDF Full Chapterbowgebachelorqcja694% (18)
- L30 - FPSC Paper Mill Colony C38/1, Gurdwara Road, Siddheshwar LucknowDokumen4 halamanL30 - FPSC Paper Mill Colony C38/1, Gurdwara Road, Siddheshwar LucknowShamsuddin ShamsBelum ada peringkat
- Annex 6 Whole Cell Pertussis WHO TRS 941, 2007Dokumen33 halamanAnnex 6 Whole Cell Pertussis WHO TRS 941, 2007at_sehly2458Belum ada peringkat
- Fimmu 10 01078Dokumen24 halamanFimmu 10 01078ArieBelum ada peringkat
- HPV Vaccine Powerpoint PresentationDokumen18 halamanHPV Vaccine Powerpoint Presentationkristia destiBelum ada peringkat
- Needle Stick Injury Lesson PlanDokumen16 halamanNeedle Stick Injury Lesson PlanJyoti Sidhu100% (1)
- 8th Grade Health Powerpoint On Hiv and Aids (STDS)Dokumen9 halaman8th Grade Health Powerpoint On Hiv and Aids (STDS)Ryan JohnstonBelum ada peringkat
- Solowska Et Al DX and MGT of COVID Vaccine ReactionsDokumen31 halamanSolowska Et Al DX and MGT of COVID Vaccine ReactionsJoshua TamayoBelum ada peringkat
- Secondary SyphilisDokumen2 halamanSecondary SyphilisRoberto López MataBelum ada peringkat
- Virulence Factors of Streptococcus PyogenesDokumen6 halamanVirulence Factors of Streptococcus PyogenesAmador GielasBelum ada peringkat
- Derma - Verruca Plana and VulgarisDokumen22 halamanDerma - Verruca Plana and VulgarisAbigail RamirezBelum ada peringkat
- Nursing Management of Anti Fungal DrugsDokumen25 halamanNursing Management of Anti Fungal DrugsJennyDaniel100% (1)
- leptospirosis钩体Dokumen29 halamanleptospirosis钩体russonegroBelum ada peringkat
- Parvo BrochureDokumen2 halamanParvo BrochureDumapis RichardBelum ada peringkat
- Causes of Disease Mark SchemeDokumen3 halamanCauses of Disease Mark SchemerkblsistemBelum ada peringkat
- Pathogenesis and Clinical Aspects of Rheumatoid Arthritis: Ivan Padjen, Cem Gabay, Daniel AletahaDokumen83 halamanPathogenesis and Clinical Aspects of Rheumatoid Arthritis: Ivan Padjen, Cem Gabay, Daniel AletahaPankaj VatsaBelum ada peringkat
- Zika Virus FactsheetDokumen2 halamanZika Virus Factsheetfriska_arianiBelum ada peringkat
- Pneumonia Dan TB ParuDokumen55 halamanPneumonia Dan TB ParuNitya Manggala JayaBelum ada peringkat
- 10.1007/978 3 662 46410 6Dokumen522 halaman10.1007/978 3 662 46410 6Francisco Ibañez Irribarra100% (1)
- Acute Interstitial NephritisDokumen36 halamanAcute Interstitial NephritisosaqerBelum ada peringkat
- Wuchereria Bancrofti, Brugia Malayi, Brugia TimoriDokumen3 halamanWuchereria Bancrofti, Brugia Malayi, Brugia TimoriJurel GaoatBelum ada peringkat
- InternationalCertificate DeepikaDokumen1 halamanInternationalCertificate Deepikasrikanth1kBelum ada peringkat
- Canine BabesiosisDokumen10 halamanCanine BabesiosisIonuț Gabriel ȚoleaBelum ada peringkat