10-11 Treatment of Hypertension
Diunggah oleh
Hanif Gandoh0 penilaian0% menganggap dokumen ini bermanfaat (0 suara)
35 tayangan11 halamandrug treatment of hyperlipidimea
Hak Cipta
© © All Rights Reserved
Format Tersedia
PDF, TXT atau baca online dari Scribd
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen Inidrug treatment of hyperlipidimea
Hak Cipta:
© All Rights Reserved
Format Tersedia
Unduh sebagai PDF, TXT atau baca online dari Scribd
0 penilaian0% menganggap dokumen ini bermanfaat (0 suara)
35 tayangan11 halaman10-11 Treatment of Hypertension
Diunggah oleh
Hanif Gandohdrug treatment of hyperlipidimea
Hak Cipta:
© All Rights Reserved
Format Tersedia
Unduh sebagai PDF, TXT atau baca online dari Scribd
Anda di halaman 1dari 11
Treatment of Hypertension
Pharmacology Team 430
Done By:
Hatem Al Ansari
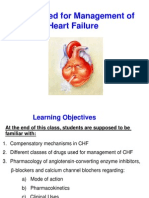
Overview & Physiology
Hypertension:
Hypertension is the most common cardiovascular disease ( 24% in USA)
Cause damage to blood vessels in kidney, heart & brain
Increase incidence of renal failure, coronary disease, stroke and heart failure.
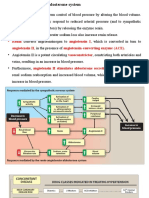
MECHANISMS FOR CONTROLLING BLOOD PRESSURE
Cardiac output and peripheral resistance are controlled mainly by two overlapping control mechanisms: the
baroreflexes, which are mediated by the sympathetic nervous system, and the renin-angiotensin-aldosterone
system. The 2 mechanisms in detail:
l
Increased blood pressure
vasoconstriction and increased cardiac output.
This prompts a reflex response of increased sympathetic and decreased
parasympathetic output to the heart and vasculature,
pressure-sensitive neurons (baroreceptors in the aortic arch and carotid sinuses)
send fewer impulses to cardiovascular centers in the spinal cord.
Fall in blood pressure
A. Baroreceptors and the sympathetic nervous system
Increase of blood pressure
Increase of blood volume
This increased secretion leads to salt & water retention
some of angiotensin II vasconstricts the vessels and the rest travels to the adrenal cortex
to increase thesecretion of aldestrone
converts angiotensinogen to angiotensin I, which is then converted to angiotensin II (
Potent Vasoconstrictor)
Baroreceptors in the kidney respond to reduced arterial pressure (and to sympathetic
stimulation of -adrenoceptors) by releasing renin
B. Renin-angiotensin-aldosterone system
Summary of the physiology:
D
Blood pressure is determined by:
1- Blood volume
2- Cardiac output ( rate &
contractility )
3- Peripheral resistance
Classification of antihypertensive
1-Diuretics
hydrochlorothiazide
furosemide
Uses: diuretics may be adequate in mild to moderate
hypertension.
2-Drugs acting on the renin -angiotensin - aldosterone system
A) Angiotensin-converting enzyme inhibitors (ACEI)
enalapril
captopril (prototype)
ramipril
lower blood pressure.
decrease cardiac output
decrease volume of blood
cause sodium and water loss
RENIN-ANGIOTENSIN ALDOSTERONNE SYSTEM
ACE inhibitors Block the enzyme that cleaves angiotensin I to form the potent
vasoconstrictor angiotensin II &Stop the rate of bradykinin inactivation. ( Decrease
Sympatehtic activity)
ACE inhibitors also decrease the secretion of
aldosterone, resulting in decreased sodium and
water retention ( decrease Blood pressure)
reduce the rate of bradykinin inactivation.
(leads to Vasodilation)
MOA
MOA
Important points about ACEI:
- The antihypertensive effect of ACE inhibitors Results primarily from vasodilatation ( reduction of
peripheral resistance ) with little change in cardiac output; a fall in aldosterone production may also
contribute to decrease
-ACE inhibitors are particularly effective when hypertension results from excess renin production
(renovascular hypertension)
Pharmacokinetics:
Captopril, enalapril and ramipril .
All are rapidly absorbed from GIT after oral administration.
Food reduce their bioavailability.
Enalapril , ramipril are prodrugs, converted to the active
metabolite in the liver
Have a long half-life & given once daily
Enalaprilat is the active metabolite of enalapril given by i.v. route in hypertensive
emergency.
Therapeutic uses
- Treatment of heart failure.
-Treatment of essential hypertension and hypertension in patients with:
chronic renal disease
Ischemic heart disease.
diabetes
ADVERSE EFFECTS:
1- Acute renal failure, especially in patients with renal artery stenosis.
2- Hyperkalemia, especially in patients with renal insufficiency or diabetes.
3- severe hypotension in hypovolemic patients (due to diuretics, salt restriction or gastrointestinal fluid loss)
4- Dry cough sometimes with wheezing
5- Angioneurotic edema ( swelling in the nose , throat, tongue, larynx)
6- Dysgeusia ( reversible loss or altered taste )
7- Skin rash and fever.
8- Proteinuria (excess of serum proteins in the urine) and neutropenia (low number of neutrophils).
Effects 4 & 5 may be caused by inhibition of bradykinin metabolism which accumulates in bronchial mucosa. (
use and NSAID to treat these effects)
Effects 6, 7, & 8 occur only in the use of Captopril because it contains sulfhydryl group in its molecule.
Contraindications
During the second and third trimesters of pregnancy due to the risk of: fetal hypotension, anuria (means non
passage of urine), renal failure, and malformations. (ACE inhibitors are teratogenic).
Renal artery stenosis. ( Because ACE inhibitors cause renal failure)
Drug interactions
With potassium-sparing diuretics. (they are weak antihypertensive when used alone, but provide an additive
hypotension effect when combined with diuretics).
With NSAIDs ( they impair ACE inhibitors hypotensive effects by blocking bradykinin mediated vasodilation)
B) Angiotensin receptor blockers
losartan
valsartan
irbesartan
losartan Valsartan
Orally effective
Has a potent active metabolite.
Long half-life, taken once daily.
Can not cross BBB
Has no active metabolites.
- As losartan in side effects and contraindications.
Both have the same Clinical uses as ACEI.
MOA:
Extremely potent competitive blockers of the AT 1 receptor.
Leads to a block of action of angiotensin II
Advantages compared with ACE inhibitors:
No effect on bradykinin (more selective), so they have the advantage of not causing the adverse effects
of ACE inhibitors such as cough & angioedema.
Produce more complete inhibition of angiotensin, because there are other enzymes (not only ACE) that
can generate angiotensin.
Adverse Effects:
Same as ACE inhibitors except for cough, wheezing, and angioedema.
Contraindications:
Same as ACE inhibitors.
3-Calcium Channel blockers:
They are divided into three classes.
Dihydropyridine group
(nifedipine, nicardipine ,
amlodipine)
Verapamil Diltiazem
act mainly on smooth muscle and
used as vasodilators
act more on the myocardium and
used as antiarrhythmic drug
has intermediate effect.(act on both
smooth muscles & myocardium)
MOA:
Block the influx of calcium through calcium channels resulting in:
1-Peripheral vasodilatation
2- Decrease cardiac contractility
Both effects 1 & 2 lower blood pressure
Pharmacokinetics:
given orally and intravenous injection
well absorbed from G.I.T
Verapamil and nifedipine are highly bound to plasma protiens (more than 90%) while diltiazem is less (70-80%)
Note: Both ACE inhibitors & angiotensin receptor blockers are teratogenic (fetotoxic) meaning that they are
harmful to the fetus. That is why they contraindicated in the last 2 trimesters pregnancy
Therapeutic uses
Treatment of chronic hypertension with oral preparation
Nicardipine can be given by I.V. route & used in hypertensive emergency
ADVERSE EFFECTS
Verapamil Diltiazem Nifedipine
Headache , Flushing
, Hypotension
Headache, Flushing,
Hypotension
Headache ,
Flushing,
Hypotension
Peripheral edema
(ankle edema)
Peripheral edema
(ankle edema)
Peripheral edema
(ankle edema)
Cardiac depression,
A-V block ,
bradycardia
Cardiac depression ,
A-V block ,
bradycardia
Tachycardia
Constipation
4- VASODILATORS
Vasodilators
Drug Hdralazine Minoxidil Diazoxide Sodium nitropruside
Site of action Arteriodilator Arteriodilator Arteriodilator Arteriodilator &
venodilator
MOA Direct Opening of
potassium channels
in smooth muscle
membranes by
minoxidil sulfate
( active metabolite)
Opening of
potassium channels
Release of nitric oxide (
NO)
Route of admin Oral Oral Rapid IV IV infusion
Therapeutic Uses Moderate -severe
hypertension.
Moderate -severe
hypertension.
Hypertensive
emergency
Hypertensive
emergency
Uses in
combination with
In combination
with diuretic & -
blockers
Hypertensive
pregnant woman
Baldness Treatment of
hypoglycemia due to
insulinoma
Severe heart failure
Adverse effects Hypotension, reflex tachycardia, palpitation, angina, salt and water
retention ( edema)
Severe hypotension
Specific adverse
effects
lupus
erythematous
like syndrome
Hypertrichosis
(abnormal hair
growth) .
Contraindicated
in females
Inhibit insulin
release from
cells of the
pancreas
causing
hyperglycemia
Contraindicated
in diabetics
1.Methemoglobinduring
infusion
2. Cyanide toxicity
3. Thiocyanate toxicity
4.Nausea, vomiting,
headache, palpitations
which disappear when
infusion is stopped
5.Cyanide accumulation
cause (cyanide
poisoning metabolic
acidosis, arrhythmias,
severe hypotension and
death)
Important points:
Both Sodium thiosulphate &hydroxocobolamine are used to prevent cyanide poisoning
Sodium thiosulphate increases metabolism of cyanide to thiocyanate (which is less toxic).
hydroxocobolamine combines with cyanide to form cyanocobolamine (nontoxic)
Thiocyanate accumulation cause thiocyanate toxicity (in renal disease) manifested as weakness, psychoses, muscle spasms
and convulsions.
Note:
Nitroprusside is poisonous if given orally because of its hydrolysis to cyanide
Nitroprusside is metabolized rapidly (half-life of minutes) and requires continuous infusion to maintain its hypotensive
action.
5- Drugs acting on sympathetic system
Review questions
1- A 45-year-old man has recently been diagnosed with hypertension and started on monotherapy designed to
reduce peripheral resistance and prevent NaCl and water retention. He has developed a persistent cough. Which of
the following drugs would have the same benefits but would not cause cough?
A) Losartan.
B) Nifedipine.
C) Prazosin.
D) Propranolol.
2- Which one of the following drugs may cause a precipitous fall in blood pressure and fainting on initial
administration?
A. Atenolol.
B. Hydrochlorothiazide.
C. Nifedipine.
D. Prazosin.
E. Verapamil.
3- Which one of the following antihypertensive drugs can precipitate a hypertensive crisis following abrupt cessation
of therapy?
A. Clonidine.
B. Diltiazem.
C. Enalapril.
D. Losartan.
E. Hydrochlorothiazide.
Adrenoreceptor blocking agents Centrally acting adrenergic drugs
- adrenoceptors blockers
(Propranolol,atenolol)
-ADRENOCEPTOR
BLOCKERS
(prazosin)
Clonidine - methyldopa
Used in mild to
moderate hypertension.
In severe cases used in
combination with other
drugs.
May take two weeks
for optimal therapeutic
response
They lower blood
pressure by :
1- Decreasing cardiac
output.
2- Decreasing renin
release.
block - receptors in
arterioles and venules
reduce blood pressure
by decreasing both
afterload & preload
This 2-agonist diminishes
central adrenergic outflow.
Clonidine does not
decrease renal blood flow
or glomerular filtration
and, therefore, is useful in
the treatment of
hypertension complicated
by renal disease.
2 agonist is converted to
methyl norepinephrine
centrally to diminish the
adrenergic outflow from
the C.N.S. This lead to
reduced total peripheral
resistance, and a decreased
blood pressure.
Correct answer = A. The cough is an adverse effect of an ACE inhibitor. Losartan is
an ARB that will have the same beneficial effects as an ACE inhibitor but will not
produce a cough. The other drugs also do not cause this side effect.
Correct answer = D. Prazosin produces first-dose hypotension, presumably by
blocking 1-receptors. This effect is minimized by initially giving the drug in small,
divided doses. The other agents do not have this adverse effect.
Correct answer = A. Increased sympathetic nervous system activity occurs
if clonidine therapy is abruptly stopped after prolonged administration.
Uncontrolled elevation in blood pressure can occur. Patients should be
slowly weaned from clonidine while other antihypertensive medications
are initiated. The other drugs on the list do not produce this phenomenon.
4- A 48-year-old hypertensive patient has been successfully treated with a thiazide diuretic for the last 5 years. Over
the last 3 months, his diastolic pressure has steadily increased, and he has been started on an additional
antihypertensive medication. He complains of several instances of being unable to achieve an erection and that he is
no longer able to complete three sets of tennis. The second antihypertensive medication is most likely which one of
the following?
A. Captopril.
B. Losartan.
C. Minoxidil.
D. Metoprolol.
E. Nifedipine.
Correct answer = D. The side effect profile of -blockers, such as metoprolol, are
characterized by interference with sexual performance and decreased exercise tolerance.
None of the other drugs is likely to produce this combination of side effects.
Anda mungkin juga menyukai
- Antianginal DrugsDokumen19 halamanAntianginal DrugsAnusha ZubairBelum ada peringkat
- Hepatorenal Syndrome, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsDari EverandHepatorenal Syndrome, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsBelum ada peringkat
- Pharmacology 3 - Management of Heart FailureDokumen59 halamanPharmacology 3 - Management of Heart Failurealbatros000Belum ada peringkat
- Anoosha Roll#21Dokumen19 halamanAnoosha Roll#21Anusha ZubairBelum ada peringkat
- Cardiotonic DrugsDokumen67 halamanCardiotonic DrugsLady Mae Ramos100% (1)
- ACE InhibitorsDokumen26 halamanACE Inhibitorsali mohammedBelum ada peringkat
- ACE INHIBITORS & ARBsDokumen31 halamanACE INHIBITORS & ARBsMaria khurshidBelum ada peringkat
- Antihypertensive & Antianginal DrugsDokumen5 halamanAntihypertensive & Antianginal Drugsdomememe1Belum ada peringkat
- Drugs Used in HF IIDokumen40 halamanDrugs Used in HF IIJamal LudinBelum ada peringkat
- Vasodilators by Hiren PatelDokumen28 halamanVasodilators by Hiren PatelHiren_Patel_2427Belum ada peringkat
- 10 and 11 Treatment of Hypertension and AnginaDokumen10 halaman10 and 11 Treatment of Hypertension and AnginaBrandon AviciiBelum ada peringkat
- Pharmacotherapy of Hypertention TerbaruDokumen45 halamanPharmacotherapy of Hypertention TerbarulisaBelum ada peringkat
- Lecture 1 antihypertensionSDSDokumen7 halamanLecture 1 antihypertensionSDSSara AbbasBelum ada peringkat
- Treatment of Hypertension: Antihypertensive AgentsDokumen4 halamanTreatment of Hypertension: Antihypertensive AgentsHanif GandohBelum ada peringkat
- Congestive Heart Failure: CardiacDokumen36 halamanCongestive Heart Failure: CardiacHUZAIFA YAMAANBelum ada peringkat
- Pharmacology: Unit VIIIDokumen92 halamanPharmacology: Unit VIIIChristian Laraya AlayonBelum ada peringkat
- Lec 2 Heart Failure, Angina and Arryth2Dokumen19 halamanLec 2 Heart Failure, Angina and Arryth2Adel AlomarBelum ada peringkat
- Anti HypretensivesDokumen18 halamanAnti HypretensivesLeena AlateeqBelum ada peringkat
- Ishac M2 Cardio Antihypertensives 2010Dokumen16 halamanIshac M2 Cardio Antihypertensives 2010Franchesca LugoBelum ada peringkat
- Anti HypretensivesDokumen18 halamanAnti HypretensivesLeena AlateeqBelum ada peringkat
- Pharmacotherapy of Hypertension: Dr. R. Jamuna Rani MD, Professor & HOD, Department of PharmacologyDokumen24 halamanPharmacotherapy of Hypertension: Dr. R. Jamuna Rani MD, Professor & HOD, Department of PharmacologyshyamkattiBelum ada peringkat
- Anti Hypertensive 20191211Dokumen35 halamanAnti Hypertensive 20191211helloitsmenadBelum ada peringkat
- Anti HypertensivesDokumen21 halamanAnti HypertensivesDivya RanasariaBelum ada peringkat
- HypertensionDokumen54 halamanHypertensionBadri KarkiBelum ada peringkat
- Congestive Cardiac FailureDokumen27 halamanCongestive Cardiac FailureKrupasagar Pn PalegarBelum ada peringkat
- HypertensionDokumen36 halamanHypertensionmohamedahmedf12345678Belum ada peringkat
- Antihypertensive Drugs RTDokumen41 halamanAntihypertensive Drugs RTMaherBelum ada peringkat
- Drugs Affecting The Cardiovascular SystemDokumen70 halamanDrugs Affecting The Cardiovascular SystemRayne Bonifacio100% (2)
- Anti Hypertensive Drugs - ACE InhibitorDokumen16 halamanAnti Hypertensive Drugs - ACE InhibitorApurba Sarker Apu100% (1)
- Drugs For Congestive Heart FailureDokumen46 halamanDrugs For Congestive Heart Failuresultan khabeeb100% (1)
- Chapter 17 Cardiovascular DrugsDokumen35 halamanChapter 17 Cardiovascular Drugsaisyahasrii_Belum ada peringkat
- CardiotonicsDokumen21 halamanCardiotonicsmohsen mirdamadiBelum ada peringkat
- Pharmacology of Cardiac Diseases MINEDokumen3 halamanPharmacology of Cardiac Diseases MINEMitu Miressa تBelum ada peringkat
- Cardio Lab MedsDokumen11 halamanCardio Lab MedsDianne Erika MeguinesBelum ada peringkat
- CVS (HF, HTN) PharmacologyDokumen99 halamanCVS (HF, HTN) PharmacologyCherenet TomaBelum ada peringkat
- Anti - ArrhythmicsDokumen5 halamanAnti - ArrhythmicsAnabeth F. PungtilanBelum ada peringkat
- Study Guide For Final Pharmacology HypertensionDokumen39 halamanStudy Guide For Final Pharmacology HypertensionAlejandro Daniel Landa MoralesBelum ada peringkat
- ACE Inhibitors: Medications To Control Blood PressureDokumen3 halamanACE Inhibitors: Medications To Control Blood PressurekBelum ada peringkat
- PharmaDokumen8 halamanPharma2022105340Belum ada peringkat
- AntiHypertensives (Autosaved)Dokumen64 halamanAntiHypertensives (Autosaved)UsamaBelum ada peringkat
- 1 Antihypertensive DrugsDokumen14 halaman1 Antihypertensive DrugsReda SoBelum ada peringkat
- 11A Drugs Acting On The Cardiovascular SystemDokumen85 halaman11A Drugs Acting On The Cardiovascular SystemJaps De la CruzBelum ada peringkat
- Inhibitors of AngiotensinDokumen37 halamanInhibitors of AngiotensinBoyu GrtrBelum ada peringkat
- HYPERTENSIONDokumen5 halamanHYPERTENSIONRajesh RamanBelum ada peringkat
- Beta Blockers and Calcium Channel BlockersDokumen34 halamanBeta Blockers and Calcium Channel Blockersnevena.stankovic986Belum ada peringkat
- Cholinergic System: e CarbamatesDokumen26 halamanCholinergic System: e CarbamatesAcai BoncaiBelum ada peringkat
- Cardiovascular Drugs (Veterinary Pharmacology)Dokumen44 halamanCardiovascular Drugs (Veterinary Pharmacology)DR Muhammad Abdul BasitBelum ada peringkat
- CVS PharmacologyDokumen60 halamanCVS PharmacologyGølà Sèèñàà–baale irraaBelum ada peringkat
- Antihypertensive Pharmacologic Agents: Nr33 K Burger, Msed, MSN, RN, CneDokumen28 halamanAntihypertensive Pharmacologic Agents: Nr33 K Burger, Msed, MSN, RN, CneLopez JoeBelum ada peringkat
- Management of Heart Failure: OutlineDokumen27 halamanManagement of Heart Failure: OutlineBoetik AlifiaBelum ada peringkat
- Angiotensin I Angiotensin II, Angiotensin-Converting Enzyme (ACE) - Vasoconstrictor Angiotensin II Stimulates Aldosterone SecretionDokumen11 halamanAngiotensin I Angiotensin II, Angiotensin-Converting Enzyme (ACE) - Vasoconstrictor Angiotensin II Stimulates Aldosterone SecretionAbdullah asadBelum ada peringkat
- Drugs Acting On Cardiovascular System-FinalsDokumen125 halamanDrugs Acting On Cardiovascular System-FinalsPrincess C. SultanBelum ada peringkat
- Pharmacological-Management-of-HypertensionDokumen35 halamanPharmacological-Management-of-Hypertensiontf.almutairi88Belum ada peringkat
- Cardiac Medication LectureDokumen23 halamanCardiac Medication LectureilikeedsheeranBelum ada peringkat
- Antihypertensive Drugs ٠١١٦٥٨Dokumen10 halamanAntihypertensive Drugs ٠١١٦٥٨mohnad806mBelum ada peringkat
- Hypertension TejaDokumen64 halamanHypertension TejaAnushka MaheshwariBelum ada peringkat
- Vasodilators 1233318450814478 3Dokumen29 halamanVasodilators 1233318450814478 3Nehal AmjadBelum ada peringkat
- Heart Failure New SlidesDokumen41 halamanHeart Failure New SlidesjawadBelum ada peringkat
- Ectopic Pregnancy OSCEDokumen4 halamanEctopic Pregnancy OSCEPatrick BayuBelum ada peringkat
- GOLD 2020 POCKET GUIDE Ver1.0 - FINAL WMVDokumen53 halamanGOLD 2020 POCKET GUIDE Ver1.0 - FINAL WMVRupesh MohandasBelum ada peringkat
- Abnormarlities On Physical Examination in A Patient With HepatosplenomegalyDokumen7 halamanAbnormarlities On Physical Examination in A Patient With HepatosplenomegalyHanif GandohBelum ada peringkat
- Ovarian Hyperstimulation SyndromeDokumen3 halamanOvarian Hyperstimulation SyndromeHanif GandohBelum ada peringkat
- Contraception - Updates: Mr. Wu Pin Ms. Nur SakinahDokumen66 halamanContraception - Updates: Mr. Wu Pin Ms. Nur SakinahHanif GandohBelum ada peringkat
- Engaging Adolescent-Headss FrameworkDokumen28 halamanEngaging Adolescent-Headss FrameworkHanif GandohBelum ada peringkat
- CF Obstructive UropathyDokumen1 halamanCF Obstructive UropathyHanif GandohBelum ada peringkat
- CCD - Ectopic Pregnancy HafyzDokumen29 halamanCCD - Ectopic Pregnancy HafyzHanif GandohBelum ada peringkat
- CCD InfertilityDokumen26 halamanCCD InfertilityHanif GandohBelum ada peringkat
- Investigation of Muscle WeaknessDokumen6 halamanInvestigation of Muscle WeaknessHanif GandohBelum ada peringkat
- CCD Obstetric GynecologyDokumen43 halamanCCD Obstetric GynecologyHanif GandohBelum ada peringkat
- Introduction To Beta Lactam AntibioticsDokumen31 halamanIntroduction To Beta Lactam AntibioticsVishaal BhatBelum ada peringkat
- OG Short CasesDokumen33 halamanOG Short CasesHanif GandohBelum ada peringkat
- Retropharyngeal AbscessDokumen8 halamanRetropharyngeal AbscessHanif Gandoh100% (1)
- BurnsDokumen9 halamanBurnsHanif GandohBelum ada peringkat
- FEVER HanifDokumen3 halamanFEVER HanifHanif GandohBelum ada peringkat
- ImpetigoDokumen21 halamanImpetigoHanif GandohBelum ada peringkat
- NASA's Flying Laboratory Studies Impact of Air Pollution 2008on ArcticDokumen41 halamanNASA's Flying Laboratory Studies Impact of Air Pollution 2008on ArcticHanif GandohBelum ada peringkat
- Health Information SystemsDokumen18 halamanHealth Information SystemsHanif Gandoh100% (2)
- Differences Between Benign and Malignant TumourDokumen5 halamanDifferences Between Benign and Malignant TumourHanif GandohBelum ada peringkat
- COLD CHAIN & VaccinationDokumen40 halamanCOLD CHAIN & VaccinationHanif GandohBelum ada peringkat
- Microbiology Table 1.23123Dokumen8 halamanMicrobiology Table 1.23123Hanif GandohBelum ada peringkat
- Commed OSCE Tutorial For Dummies 2Dokumen7 halamanCommed OSCE Tutorial For Dummies 2Hanif GandohBelum ada peringkat
- Pulmonary Tuberculosis HanifDokumen24 halamanPulmonary Tuberculosis HanifHanif GandohBelum ada peringkat
- PBL Peptic UlcerDokumen1 halamanPBL Peptic UlcerHanif GandohBelum ada peringkat
- Cardiac Rhytmn AbnormalitiesDokumen13 halamanCardiac Rhytmn AbnormalitiesHanif GandohBelum ada peringkat
- Treatment of Hypertension: Antihypertensive AgentsDokumen4 halamanTreatment of Hypertension: Antihypertensive AgentsHanif GandohBelum ada peringkat
- Mock1 8thmarch CompDokumen36 halamanMock1 8thmarch Compdr_zafarBelum ada peringkat
- Diuretics Table (Pharma)Dokumen4 halamanDiuretics Table (Pharma)Hanif GandohBelum ada peringkat
- The Effect of Tobacco Use On Oral HealthDokumen8 halamanThe Effect of Tobacco Use On Oral HealthRivandy HolilBelum ada peringkat
- CS Form 86 Physical and Medical Health and RecordDokumen1 halamanCS Form 86 Physical and Medical Health and RecordHONEY JADE OMAROLBelum ada peringkat
- 2015 To 2019 Super Speciality Dissertation Topics PDFDokumen35 halaman2015 To 2019 Super Speciality Dissertation Topics PDFJoseph John Crasto100% (4)
- Renal Calculi: Ahmednagar Homoeopathic Medical College & Hospital AhmednagarDokumen15 halamanRenal Calculi: Ahmednagar Homoeopathic Medical College & Hospital AhmednagarSuhas IngaleBelum ada peringkat
- Low-Cost Breath AnalyzerDokumen20 halamanLow-Cost Breath AnalyzeradnanBelum ada peringkat
- Above Knee AmputationDokumen8 halamanAbove Knee AmputationAbdul Ghafoor SajjadBelum ada peringkat
- Cure Gum Disease Naturally Heal and Prevent AmazonindsjzoDokumen6 halamanCure Gum Disease Naturally Heal and Prevent Amazonindsjzocafechild05Belum ada peringkat
- Pregnancy TestDokumen13 halamanPregnancy TestAbdirahman YznBelum ada peringkat
- Abortion Using Misoprostol Pills: Before SmaDokumen1 halamanAbortion Using Misoprostol Pills: Before SmaAhmad Shah SyedBelum ada peringkat
- nsg-320cc Care Plan 1Dokumen14 halamannsg-320cc Care Plan 1api-509452165Belum ada peringkat
- Pregnancy PlannerDokumen75 halamanPregnancy PlannerDaniza LanyonBelum ada peringkat
- Breast Cancer in MenDokumen14 halamanBreast Cancer in MenNyawBelum ada peringkat
- 12 Drugs Acting On The Cardiovascular SystemDokumen5 halaman12 Drugs Acting On The Cardiovascular SystemJAN CAMILLE LENONBelum ada peringkat
- Mod DescriptionsDokumen9 halamanMod DescriptionsGuilherme CoutinhoBelum ada peringkat
- My Trip To The Hospital - A Coloring BookDokumen0 halamanMy Trip To The Hospital - A Coloring Bookili_thBelum ada peringkat
- Perineal CareDokumen32 halamanPerineal CareKasnha100% (1)
- Research Article Respiratory RelatedDokumen3 halamanResearch Article Respiratory RelatedRizza Faye BalayangBelum ada peringkat
- Apollo Fertility IUI IVF Clinic and Dr. Lakshmi Krishna Leela GynecologistDokumen6 halamanApollo Fertility IUI IVF Clinic and Dr. Lakshmi Krishna Leela GynecologistPrabha SharmaBelum ada peringkat
- Exercise No. 26 The Blood GroupsDokumen8 halamanExercise No. 26 The Blood GroupsPATRICIA ROSE SORIANOBelum ada peringkat
- Closed Fracture OsDokumen23 halamanClosed Fracture OsDiana Lita SBelum ada peringkat
- Adorio Partograph ScenarioDokumen2 halamanAdorio Partograph Scenariojonathan liboonBelum ada peringkat
- Wound Debridement-FinalDokumen3 halamanWound Debridement-FinaljessicagrepoBelum ada peringkat
- SimMan 3G BrochureDokumen8 halamanSimMan 3G BrochureDemuel Dee L. BertoBelum ada peringkat
- Outstanding Academician Aileen Guzman-BanzonDokumen1 halamanOutstanding Academician Aileen Guzman-BanzonwiltechworksBelum ada peringkat
- Hyper Calc Emi ADokumen31 halamanHyper Calc Emi AFatima SajidBelum ada peringkat
- Drug Management of Thyroid DiseaseDokumen22 halamanDrug Management of Thyroid DiseaseHassan.shehri100% (6)
- Giraffe Blood CirculationDokumen9 halamanGiraffe Blood Circulationthalita asriandinaBelum ada peringkat
- Dentist Hong Kong Jain SmithDokumen31 halamanDentist Hong Kong Jain SmithcheriesandeepBelum ada peringkat
- Prosta LacDokumen16 halamanProsta LacantoniofacmedBelum ada peringkat
- OT Relevance RMTDokumen12 halamanOT Relevance RMTFredy RamoneBelum ada peringkat