Scrotal Mass
Diunggah oleh
Amelia Alresna0 penilaian0% menganggap dokumen ini bermanfaat (0 suara)
55 tayangan6 halamanbh
Hak Cipta
© © All Rights Reserved
Format Tersedia
PDF, TXT atau baca online dari Scribd
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen Inibh
Hak Cipta:
© All Rights Reserved
Format Tersedia
Unduh sebagai PDF, TXT atau baca online dari Scribd
0 penilaian0% menganggap dokumen ini bermanfaat (0 suara)
55 tayangan6 halamanScrotal Mass
Diunggah oleh
Amelia Alresnabh
Hak Cipta:
© All Rights Reserved
Format Tersedia
Unduh sebagai PDF, TXT atau baca online dari Scribd
Anda di halaman 1dari 6
Evaluation of Scrotal Masses
JEFFREY D. TIEMSTRA, MD, and SHAILENDRA KAPOOR, MD
Department of Family Medicine, University of Illinois at Chicago College of Medicine, Chicago, Illinois
Scrotal masses can represent a wide range of medical issues, from benign congenital conditions to life-threatening
malignancies and acute surgical emergencies. Having a clear understanding of scrotal anatomy allows the examiner
to accurately identify most lesions. Benign lesions such as hydroceles and varicoceles are often found incidentally by
the patient or physician on routine examination. Epididymitis is bacterial in origin, readily diagnosed on physical
examination, and treated with antibiotics. Indirect inguinal hernias usually are palpable separate from the normal
scrotal contents and are a surgical emergency if strangulation is suspected based on symptoms of abdominal pain,
tenderness, and nonreducibility. Testicular swelling may be caused by orchitis, cancer, or testicular torsion. Orchitis
is usually viral in origin, subacute in onset, and may be accompanied by systemic illness. Testicular carcinomas are
more gradual in onset; the testis will be nontender on examination. Testicular torsion has an acute onset, often with
no antecedent trauma; the involved testis may be retracted and palpably rotated, and will be tender on examination.
The swollen testis is always a true emergency. Although history and examination may suggest the diagnosis, testicular
torsion can be reliably conrmed only with color Doppler ultrasonography, which must be obtained immediately. If
torsion is suspected, surgical consultation should be obtained concurrently with ultrasonography, because the abil-
ity to successfully salvage the affected testis declines dramatically after six hours of torsion. (Am Fam Physician.
2008;78(10):1165-1170. Copyright 2008 American Academy of Family Physicians.)
S
crotal masses can occur from infancy
to old age, with the various causes
distributed widely across the age
spectrum. Causes range from inci-
dental ndings of little clinical signicance
to conditions that can cause permanent dis-
ability or death. Fortunately, with a careful
history and physical examination, physi-
cians can usually identify those patients with
potentially serious conditions. Because of the
possibility of emergent and life-threatening
causes, and because a swollen scrotum is
usually of great concern to patients, imme-
diate evaluation is always required.
Scrotal masses are best categorized by their
anatomic origin. Because the anatomy of the
scrotum is easy to appreciate on physical
examination, identifying normal anatomy
by inspection and palpation will usually lead
to an accurate differential diagnosis of most
scrotal masses (Figure 1). Figure 2 illustrates
the normal anatomy of the scrotum, and
Table 1 classies causes of scrotal masses by
anatomic origin.
Causes of Scrotal Swelling
SKIN
Any lesion of the skin may occur on the skin
of the scrotum. Sebaceous cysts commonly
occur on the scrotum of adults, typically pre-
senting as painless, slowly growing nodules
in the skin. Occasionally such lesions become
infected, in which case they will be erythem-
atous and tender. They can be palpated in the
dermal layer and are freely mobile and sepa-
rate from the testes and spermatic cord.
Squamous cell carcinoma of the scrotal
skin is primarily an occupational illness.
Although it used to be common among
chimney sweeps, the disease is now fairly
rare because the risks of exposure to occupa-
tional carcinogens have been recognized, and
use of protective clothing and equipment has
become routine. However, squamous cell car-
cinoma of the scrotal skin is seen on occasion,
and has been reported in a variety of indus-
trial occupations, such as textile milling and
metalworking. Scrotal carcinoma has also
been cited as a complication of PUVA (pso-
ralen plus ultraviolet A) therapy for psoriasis.
The frequency of scrotal carcinoma increases
with age, peaking around 75 years of age. It
typically presents as a raised papule or plaque
that progressively enlarges and ulcerates.
1,2
TUNICA VAGINALIS AND PROCESSUS VAGINALIS
During fetal development, the processus
vaginalis testis forms as an extension of
Downloaded from the American FamilyPhysician Web site at www.aafp.org/afp. Copyright 2008 American Academyof FamilyPhysicians. For the private, noncommercial
use of one individual user of the Web site. All other rightsreserved. Contact copyrights@ aafp.org for copyright questionsand/or permission requests.
Scrotal Masses
1166 American Family Physician www.aafp.org/afp Volume 78, Number 10
November 15, 2008
the peritoneum, descending into the scrotum and sur-
rounding the testis. With complete descent of the testis,
the surrounding tunica vaginalis testis separates from
the processus vaginalis testis. A hydrocele is a collec-
tion of uid in either the tunica vaginalis or a persis-
tent processus vaginalis. Hydroceles are common in
newborns, but often disappear within the rst year of
life. However, a hydrocele may appear at any age as a
painless, unilateral scrotal swelling of acute or insidious
onset. On examination, a hydrocele is uctuant, ovoid,
SORT: KEY RECOMMENDATIONS FOR PRACTICE
Clinical recommendation
Evidence
rating References
Any patient reporting swelling of the scrotum should be evaluated immediately. A careful physical
examination should include identication of the normal anatomic structures of the scrotum, and
transillumination of any mass.
C 16-18
If testicular torsion is suspected, emergent surgical consultation with or without Doppler
ultrasonography should be obtained. Surgery for testicular torsion must be performed within six
hours of the onset of pain to maximize the odds of salvaging the testis.
B 15, 19-21
Color Doppler ultrasonography is the test of choice for immediate evaluation of scrotal masses. B 25-29
A = consistent, good-quality patient-oriented evidence; B = inconsistent or limited-quality patient-oriented evidence; C = consensus, disease-
oriented evidence, usual practice, expert opinion, or case series. For information about the SORT evidence rating system, go to http://www.aafp.
org/afpsort.xml.
Diagnosing Scrotal Masses
Figure 1. Algorithm of the likely diagnoses of a scrotal mass based on physical examination ndings.
Swelling of the skin
Rule out squamous
cell carcinoma
Irregular, enlarging;
occupational risk
Sebaceous cyst
Smooth, cystic,
stable in size
Swelling of the spermatic cord
Swelling extends
to inguinal ring
Indirect inguinal hernia
Smooth, transilluminates
Hydrocele; consider
ultrasonography to conrm
Bag of worms texture
Varicocele
Swelling of the epididymis
Nodule, stable in size Diffusely swollen,
tender, acute onset
Epididymitis
Spermatocele; consider
ultrasonography to conrm
Swelling of the testis
Nontender, gradual onset
Transilluminates
Hydrocele obscuring
testis; order ultra-
sonography to conrm
Solid
Suspect testicular
carcinoma; order ultra-
sonography or referr
Tender, onset < 24 hours
Torsion versus orchitis
Emergent surgical referral
NOTE: Emergent surgical referral should be strongly considered for any acutely painful scrotum when testicular torsion is a possibility. If testicular tor-
sion is not suspected, ultrasonography may be performed to conrm the diagnosis.
Scrotal Masses
November 15, 2008
Volume 78, Number 10 www.aafp.org/afp American Family Physician 1167
and nontender. Hydroceles in the tunica vaginalis may
obscure the adjacent testis, whereas hydroceles arising
from a persistent processus vaginalis are palpated above
the testis along the spermatic cord. Transillumination
(shining a light through the swelling) demonstrates
light transmission through the uid-lled hydrocele,
compared with nontransmission or limited transmis-
sion through the solid testis.
3
Hydroceles may develop
in adulthood as a result of lymphatic obstruction by dis-
eases such as lariasis, and are common in areas where
such infection is endemic.
4
A persistent processus vaginalis may lead to a hydro-
cele or an indirect inguinal hernia. Inguinal hernias
can also present at any age. Indirect inguinal hernias
follow the path of the processus vaginalis through the
internal inguinal ring and into the scrotum. Although
the persistent processus vaginalis is congenital, symp-
tomatic indirect inguinal hernias may develop at any
age. Patients may present with scrotal swelling that
uctuates in size, and may note increased swelling with
Valsalva-type maneuvers. On palpation, the indirect
inguinal hernia may be felt as a swelling extending up
Table 1. Causes of Scrotal Lesions by Anatomic Origin
Anatomic origin Lesion/condition Onset/progression
Pain/
tenderness
Aggravating/alleviating factors,
associated symptoms
Skin Sebaceous cyst Acute/chronic, stable No
Squamous cell
carcinoma
Chronic, progressive No
Tunica vaginalis
testis
Hydrocele Acute/chronic, stable No Transilluminates
Hematocele Acute, caused by trauma Yes Does not transilluminate well
Processus
vaginalis testis
Indirect inguinal
hernia
Acute/chronic, stable or
progressive
No; yes if
strangulated
May enlarge with Valsalva-type maneuvers;
size may uctuate
Hydrocele Chronic, stable No
Pampiniform
plexus
Varicocele Chronic, stable No Bag of worms consistency
Epididymis Epididymitis Acute, progressive Yes May have symptoms of urinary tract infection
Spermatocele Chronic, stable No
Testis Testicular torsion Acute, progressive Yes Elevation of testis may aggravate pain;
abnormal testicular lie; cremasteric reex
usually absent
Appendix testis
torsion
Acute, stable Yes Blue dot sign
Orchitis Acute, self-limited Yes Elevation of testis may relieve pain, may
have systemic symptoms of viral illness
Testicular cancer Chronic, progressive No
Figure 2. Anatomy of the scrotum.
Spermatic cord
Vas deferens
Pampiniform
plexus
Epididymis
Testis (covered
by visceral
layer of tunica
vaginalis testis)
Cremaster
muscle
and fascia
Appendix of
epididymis
Appendix
of testis
Parietal layer of
tunica vaginalis testis
I
L
L
U
S
T
R
A
T
I
O
N
B
Y
T
O
D
D
B
U
C
K
Scrotal Masses
1168 American Family Physician www.aafp.org/afp Volume 78, Number 10
November 15, 2008
the spermatic cord to the inguinal ring. Inguinal her-
nias often enlarge with the Valsalva maneuver, and can
be reduced by the examiner unless the hernias are incar-
cerated. In contrast, patients with hydroceles will have a
palpably normal spermatic cord and inguinal ring above
the swollen area. About one third of patients referred for
surgery for a palpable inguinal hernia have a nonpalpa-
ble contralateral hernia as well, so ultrasound imaging
should be considered in these patients.
5,6
Strangulated indirect inguinal hernias present as acute
painful masses, often accompanied by abdominal com-
plaints such as pain, nausea, and vomiting. The hernia
is typically rm and tender, and is usually not reducible.
Strangulated hernias are a surgical emergency.
7
Hematoceles are typically a result of direct trauma to
the scrotum (including iatrogenic trauma from aspira-
tion of a hydrocele), although idiopathic cases have been
reported. Patients usually present following trauma with
pain and an acute scrotal swelling similar to a hydrocele,
although not transilluminating well. Hematoceles can
mimic testicular torsion and epididymitis.
TESTES
Testicular tumors are the most common malignant
tumors encountered in men 25 to 35 years of age. His-
tologic classication of these tumors is complex, and
includes seminomas, choriocarcinoma, and a variety of
teratomas, or germ cell tumors. Most palpable testicular
tumors in adults are malignant, although 80 percent of
nonpalpable testicular lesions are benign.
8
Children with
testicular tumors are more likely to have benign lesions,
with 20 to 40 percent being benign.
9,10
On examination,
the testis is enlarged, nontender, has a rm consistency,
and does not transilluminate. In seminomas, the testic-
ular surface is smooth and the consistency is uniform,
whereas teratomas may be more irregular. Urgent evalu-
ation and referral are indicated.
11-14
Torsion of the testis is most common in males 10 to
25 years of age. Most torsions occur during sleep, with
scrotal trauma accounting for less than 10 percent of
cases.
15
Patients typically present with sudden onset
of painful testicular swelling. The pain radiates to the
inguinal and hypogastric areas and may be accompa-
nied by nausea and vomiting. The testis will be tender
and swollen, and is often high in the scrotum because
of shortening of the spermatic cord with torsion.
15
The
position of the epididymis varies depending on the
degree of rotation, but will be in the normal posterior
position with 360 rotation. The cremasteric reex is
usually absent, and elevation of the testes may aggravate
the pain.
15
Suspected torsion is a surgical emergency;
the testicular salvage rate for detorsion is 90 percent
if performed within six hours of symptom onset, but
drops to 50 percent after 12 hours, and to only 10 per-
cent after 24 hours.
15-22
The presentation of torsion of the appendix testis
may be identical to that of testicular torsion. On physi-
cal examination, however, a hard, tender nodule at the
superior aspect of the testis may be palpated just beneath
the skin, often with a bluish discoloration (i.e., the blue
dot sign).
Orchitis can occur when organisms travel up the vas
deferens from the urinary tract, or it can be caused by
systemic infections; potential pathogens include chla-
mydia, salmonella, mumps, brucellosis, and tubercu-
losis. In addition to a painful swollen testis, patients
may have fever and other systemic signs and symptoms.
Unlike the pain of testicular torsion, the pain of orchitis
is usually relieved by elevation of the testes.
23
EPIDIDYMIS
Epididymitis, acute infection of the epididymis, is usu-
ally caused by sexually transmitted diseases or common
genitourinary pathogens, including gonorrhea and chla-
mydia. Patients typically have subacute onset of pain
and swelling, sometimes with associated urinary tract
symptoms, and on examination have a diffusely swollen,
tender epididymis distinct from the testis.
23
A spermatocele is a retention cyst of the epididymis.
The patient usually presents with a soft nodule in the
head of the epididymis. On examination, a swelling can
be felt above and behind the testes, distinct from the tes-
tes; typically it does not transilluminate.
23
PAMPINIFORM PLEXUS
A varicocele is a dilation of the pampiniform venous
plexus along the spermatic cord. It is more common in
tall, thin men and usually occurs on the left side. Patients
may be asymptomatic or may complain of a dull, drag-
ging discomfort on the affected side. Palpation reveals
the classic bag of worms along the spermatic cord. The
mass disappears when the patient lies down and reap-
pears when the patient stands. Because varicoceles may
contribute to lower sperm counts in some men, they
should be considered in infertility evaluations.
22,23
Diagnostic Evaluation
HISTORY AND PHYSICAL EXAMINATION
Because of potential emergencies (e.g., testicular torsion)
and potentially life-threatening diseases (e.g., testicular
carcinoma), any patient with a new or changing scro-
tal mass should be evaluated immediately in the ofce
Scrotal Masses
November 15, 2008
Volume 78, Number 10 www.aafp.org/afp American Family Physician 1169
or emergency department. Key features of the history
include timing of onset, progression, trauma, aggravating
and alleviating factors, pain, and genitourinary and sys-
temic symptoms (Table 1). Careful physical examination
should include attention to the location of the swelling
in relation to the normal anatomic structures within the
scrotum, and transillumination to check for testicular
masses. Patients with suspected torsion should be evalu-
ated emergently by a urologist, because surgery must be
performed immediately to maximize the likelihood of
salvaging the testis.
DOPPLER ULTRASONOGRAPHY
Ultrasonography with color Doppler imaging has become
the accepted standard for evaluation of the acutely swol-
len scrotum. Ultrasonography will readily conrm the
diagnosis in extratesticular masses, such as hydrocele,
spermatocele, and varicocele. For the swollen testis,
ultrasonography usually demonstrates normal paren-
chyma in cases of torsion and orchitis, and a heteroge-
neous appearance in carcinoma (Figure 3). In such cases,
color Doppler ultrasonography is essential because it
will show decreased blood ow in testicular torsion, nor-
mal or increased ow in carcinoma, and increased ow
in orchitis. For testicular torsion, color Doppler ultra-
sonography has a sensitivity of 86 to 88 percent and a
specicity of 90 to 100 percent. When testicular torsion
is suspected, emergent surgical consultation should be
obtained before ultrasonography is performed, because
surgical exploration as soon as possible is critical to sal-
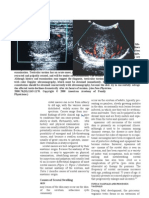
Figure 3. Ultrasound images of a patient with mixed germ cell tumor of the right testis. Longitudinal views of the testes
show (A) the heterogeneous nature of the tumor parenchyma on the right compared with (B) the normal parenchyma
on the left. Color Doppler images show normal blood ow on (C) the right longitudinal and (D) left transverse views.
A B
C D
Scrotal Masses
1170 American Family Physician www.aafp.org/afp Volume 78, Number 10
November 15, 2008
vaging the testis and should not be delayed for imaging
unless the diagnosis is in doubt.
24-30
OTHER IMAGING
Radionuclide imaging is accurate in diagnosing testicu-
lar torsion but, because of the time delay involved, is not
often employed. Computed tomography and magnetic
resonance imaging can be used when carcinoma is sus-
pected if ultrasonography is inconclusive, and are also
used for staging testicular tumors.
25
The Authors
JEFFREY D. TIEMSTRA, MD, is an associate professor of clinical family medi-
cine at the University of Illinois at Chicago College of Medicine. Dr. Tiem-
stra received his medical degree from Rush University Medical College in
Chicago, and completed a residency in family medicine at the University of
Texas Southwestern Medical School in Dallas.
SHAILENDRA KAPOOR, MD, is a third-year resident in family medicine at
the University of Illinois at Chicago College of Medicine. Dr. Kapoor received
his medical degree from Thanjavur Medical College in Tamilnadu, India.
Address correspondence to Jeffrey D. Tiemstra, MD, Dept. of Family
Medicine (M/C 663), University of Illinois at Chicago, 1919 W. Taylor St.,
Chicago, IL 60612 (e-mail: jtiemstr@uic.edu). Reprints are not available
from the authors.
Author disclosure: Nothing to disclose.
REFERENCES
1. de la Brassinne M, Richert N. Genital squamous-cell carcinoma after
PUVA therapy. Dermatology. 1992;185(4):316-318.
2. Fay HT. Risk factors in scrotal epithelioma. J R Soc Med. 1978;71(10):
741-747.
3. Davenport M. ABC of general paediatric surgery. Inguinal hernia, hydro-
cele, and the undescended testis. BMJ. 1996;312(7030):564-567.
4. Tobian AA, Tarongka N, Baisor M, Bockarie M, Kazura JW, King CL. Sen-
sitivity and specicity of ultrasound detection and risk factors for larial-
associated hydroceles. Am J Trop Med Hyg. 2003;68(6):638-642.
5. Kraft BM, Kolb H, Kuchuk B, et al. Diagnosis and classication of ingui-
nal hernias. Surg Endosc. 2003;17(12):2021-2024.
6. van den Berg JC, de Valois JC, Go PM, Rosenbusch G. Detection of groin
hernia with physical examination, ultrasound, and MRI compared with
laparoscopic ndings. Invest Radiol. 1999;34(12):739-743.
7. Bax T, Sheppard BC, Crass RA. Surgical options in the management of
groin hernias. Am Fam Physician. 1999;59(4):893-906.
8. Carmignani L, Gadda F, Gazzano G, et al. High incidence of benign testic-
ular neoplasms diagnosed by ultrasound. J Urol. 2003;170:1783-1786.
9. Ross JH, Rybicki L, Kay R. Clinical behavior and a contemporary manage-
ment algorithm for prepubertal testis tumors: a summary of the Prepu-
bertal Testis Tumor Registry. J Urol. 2002;168(4 pt 2):1675-1678.
10. Shukla AR, Woodard C, Carr MC, et al. Experience with testis sparing
surgery for testicular teratoma. J Urol. 2004;171(1):161-163.
11. Horwich A, Shipley J, Huddart R. Testicular germ-cell cancer [pub-
lished correction appears in Lancet. 2006;367(9520):1398]. Lancet.
2006;367(9512):754-765.
12. Shelley MD, Burgon K, Mason MD. Treatment of testicular germ-cell
cancer: a Cochrane evidence-based systematic review. Cancer Treat Rev.
2002;28(5):237-253.
13. Hartmann JT, Kanz L, Bokemeyer C. Diagnosis and treatment of patients
with testicular germ cell cancer. Drugs. 1999;58(2):251-281.
14. Frank IN, Graham SD, Nabors WL. Urologic and male genital cancers. In:
Holleb AI, Fink DJ, Murphy GP, eds. American Cancer Society Textbook
of Clinical Oncology. Atlanta, Ga.: The Society; 1991:283-287.
15. Kadish HA, Bolte RG. A retrospective review of pediatric patients with
epididymitis, testicular torsion, and torsion of testicular appendages.
Pediatrics. 1998;102(1 pt 1):73-76.
16. Ringdahl E, Teague L. Testicular torsion. Am Fam Physician. 2006;74(10):
1739-1743.
17. Galejs LE. Diagnosis and treatment of the acute scrotum. Am Fam Physi-
cian. 1999;59(4):817-824.
18. Prater JM, Overdorf BS. Testicular torsion: a surgical emergency. Am
Fam Physician. 1991;44(3):834-840.
19. Lewis AG, Bukowski TP, Jarvis PD, Wacksman J, Sheldon CA. Evalua-
tion of acute scrotum in the emergency department. J Pediatr Surg.
1995;30(2):277-281.
20. Knight PJ, Vassy LE. The diagnosis and treatment of the acute scrotum
in children and adolescents. Ann Surg. 1984;20(5):664-673.
21. Granados EA, Caicedo P, Garat JM. Testicular torsion after 12 hours. III
[Spanish]. Arch Esp Urol. 1998;51(10):978-981.
22. Pillai SB, Besner GE. Pediatric testicular problems. Pediatr Clin North
Am. 1998;45(4):813-830.
23. Krieger JN. Epididymitis, orchitis, and related conditions. Sex Transm
Dis. 1984;11(3):173-181.
24. Akin EA, Khati NJ, Hill MC. Ultrasound of the scrotum. Ultrasound Q.
2004;20(4):181-200.
25. Schalamon J, Ainoedhofer H, Schleef J, Singer G, Haxhija EQ, Hllwarth
ME. Management of acute scrotum in childrenthe impact of Doppler
ultrasound. J Pediatr Surg. 2006;41(8):1377-1380.
26. Karmazyn B, Steinberg R, Kornreich L, et al. Clinical and sonographic
criteria of acute scrotum in children: a retrospective study of 172 boys.
Pediatr Radiol. 2005;35(3):302-310.
27. Lamm WW, Yap TL, Jacobsen AS, Teo HJ. Colour Doppler ultrasonog-
raphy replacing surgical exploration for acute scrotum: myth or reality?
Pediatr Radiol. 2005;35(6):597-600.
28. Paltiel HJ, Connolly LP, Atala A, Paltiel AD, Zurakowski D, Treves ST.
Acute scrotal symptoms in boys with an indeterminate clinical presenta-
tion: comparison of color Doppler sonography and scintigraphy. Radiol-
ogy. 1998;207(1):223-231.
29. Coley BD, Frush DP, Babcock DS, et al. Acute testicular torsion: com-
parison of unenhanced and contrast-enhanced power Doppler US,
color Doppler US, and radionuclide imaging. Radiology. 1996;199(2):
441-446.
30. Herbener TE. Ultrasound in the assessment of the acute scrotum. J Clin
Ultrasound. 1996;24(8):405-421.
Anda mungkin juga menyukai
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDari EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryPenilaian: 3.5 dari 5 bintang3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Dari EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Penilaian: 4.5 dari 5 bintang4.5/5 (120)
- Grit: The Power of Passion and PerseveranceDari EverandGrit: The Power of Passion and PerseverancePenilaian: 4 dari 5 bintang4/5 (588)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDari EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaPenilaian: 4.5 dari 5 bintang4.5/5 (266)
- The Little Book of Hygge: Danish Secrets to Happy LivingDari EverandThe Little Book of Hygge: Danish Secrets to Happy LivingPenilaian: 3.5 dari 5 bintang3.5/5 (399)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDari EverandNever Split the Difference: Negotiating As If Your Life Depended On ItPenilaian: 4.5 dari 5 bintang4.5/5 (838)
- Shoe Dog: A Memoir by the Creator of NikeDari EverandShoe Dog: A Memoir by the Creator of NikePenilaian: 4.5 dari 5 bintang4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerDari EverandThe Emperor of All Maladies: A Biography of CancerPenilaian: 4.5 dari 5 bintang4.5/5 (271)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDari EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifePenilaian: 4 dari 5 bintang4/5 (5794)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDari EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyPenilaian: 3.5 dari 5 bintang3.5/5 (2259)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDari EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersPenilaian: 4.5 dari 5 bintang4.5/5 (344)
- Rise of ISIS: A Threat We Can't IgnoreDari EverandRise of ISIS: A Threat We Can't IgnorePenilaian: 3.5 dari 5 bintang3.5/5 (137)
- Team of Rivals: The Political Genius of Abraham LincolnDari EverandTeam of Rivals: The Political Genius of Abraham LincolnPenilaian: 4.5 dari 5 bintang4.5/5 (234)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDari EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You ArePenilaian: 4 dari 5 bintang4/5 (1090)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDari EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RacePenilaian: 4 dari 5 bintang4/5 (895)
- Her Body and Other Parties: StoriesDari EverandHer Body and Other Parties: StoriesPenilaian: 4 dari 5 bintang4/5 (821)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDari EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FuturePenilaian: 4.5 dari 5 bintang4.5/5 (474)
- Day 11 Histopathology of Male Genital DisordersDokumen26 halamanDay 11 Histopathology of Male Genital DisordersMuhammad RamadhanBelum ada peringkat
- The Unwinding: An Inner History of the New AmericaDari EverandThe Unwinding: An Inner History of the New AmericaPenilaian: 4 dari 5 bintang4/5 (45)
- The Yellow House: A Memoir (2019 National Book Award Winner)Dari EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Penilaian: 4 dari 5 bintang4/5 (98)
- On Fire: The (Burning) Case for a Green New DealDari EverandOn Fire: The (Burning) Case for a Green New DealPenilaian: 4 dari 5 bintang4/5 (73)
- Varicocele-Healing PDFDokumen42 halamanVaricocele-Healing PDFmusag100% (1)
- MED 2.2 Examination of The Male GenitaliaDokumen7 halamanMED 2.2 Examination of The Male Genitaliaelleinas100% (1)
- Medad Andrology Special Note NMT13 PDFDokumen70 halamanMedad Andrology Special Note NMT13 PDFSelim TarekBelum ada peringkat
- Testicular Examination Report BrianDokumen13 halamanTesticular Examination Report BrianKarlBalmeraBelum ada peringkat
- UrologyDokumen35 halamanUrologymiansk100% (1)
- Cornea and Sclera III Common DisordersDokumen83 halamanCornea and Sclera III Common DisordersAmelia AlresnaBelum ada peringkat
- TB ResistantDokumen64 halamanTB ResistantAmelia AlresnaBelum ada peringkat
- JNC 8Dokumen14 halamanJNC 8amiwahyuniBelum ada peringkat
- Agility Project Manage M NTDokumen8 halamanAgility Project Manage M NTAmelia AlresnaBelum ada peringkat
- Evaluation of A Method For Improving The Detection of Hepatocellular CarcinomaDokumen7 halamanEvaluation of A Method For Improving The Detection of Hepatocellular CarcinomaAmelia AlresnaBelum ada peringkat
- XP02 LimitationsDokumen4 halamanXP02 LimitationsdnudnuBelum ada peringkat
- Comparison of Efficacy, Safety, and Cost-Effectiveness of Various Statins in Dyslipidemic Diabetic PatientsDokumen8 halamanComparison of Efficacy, Safety, and Cost-Effectiveness of Various Statins in Dyslipidemic Diabetic PatientsAmelia AlresnaBelum ada peringkat
- Daftar PustakaDokumen4 halamanDaftar PustakaAmelia AlresnaBelum ada peringkat
- Cardiac Cirrhosis and Congestive HepatopathyDokumen4 halamanCardiac Cirrhosis and Congestive HepatopathyAmelia AlresnaBelum ada peringkat
- Medical AnthropologieDokumen10 halamanMedical AnthropologieAmelia AlresnaBelum ada peringkat
- Jadwal Saraf DR Ida EditDokumen18 halamanJadwal Saraf DR Ida EditPutri Nisrina HamdanBelum ada peringkat
- English-Sub HTMLDokumen1 halamanEnglish-Sub HTMLAmelia AlresnaBelum ada peringkat
- Komp Ot MDokumen5 halamanKomp Ot MAmelia AlresnaBelum ada peringkat
- DpusDokumen10 halamanDpusAmelia AlresnaBelum ada peringkat
- S 1Dokumen1 halamanS 1Amelia AlresnaBelum ada peringkat
- Minggu Ke-Tanggal Senin Selasa: Nama Minggu 1 - 2 Minggu 3 - 4 Minggu 5 - 6Dokumen3 halamanMinggu Ke-Tanggal Senin Selasa: Nama Minggu 1 - 2 Minggu 3 - 4 Minggu 5 - 6Amelia AlresnaBelum ada peringkat
- Anemia in ChildrenDokumen10 halamanAnemia in ChildrenAnastasio DiazBelum ada peringkat
- P 1165Dokumen10 halamanP 1165Amelia AlresnaBelum ada peringkat
- Daftar PustakaDokumen1 halamanDaftar PustakaAmelia AlresnaBelum ada peringkat
- Breast CancerDokumen38 halamanBreast CancerojoayodeleBelum ada peringkat
- DafpusDokumen7 halamanDafpusAmelia AlresnaBelum ada peringkat
- Hands WashingDokumen9 halamanHands WashingAmelia AlresnaBelum ada peringkat
- Gus156 Slide Scrotal SwellingsDokumen31 halamanGus156 Slide Scrotal SwellingsAmelia AlresnaBelum ada peringkat
- Kripto DR YeppyDokumen8 halamanKripto DR YeppyAmelia AlresnaBelum ada peringkat
- Lirik LaguDokumen1 halamanLirik LaguAmelia AlresnaBelum ada peringkat
- Anafilaksis DewasaDokumen7 halamanAnafilaksis DewasaAmelia AlresnaBelum ada peringkat
- Lirik LaguDokumen1 halamanLirik LaguAmelia AlresnaBelum ada peringkat
- Lirik LaguDokumen1 halamanLirik LaguAmelia AlresnaBelum ada peringkat
- Lirik LaguDokumen1 halamanLirik LaguAmelia AlresnaBelum ada peringkat
- MALE REPRODUCTIVE PROBLEMS 2021 With NotesDokumen35 halamanMALE REPRODUCTIVE PROBLEMS 2021 With NotesNikky SilvestreBelum ada peringkat
- Sample Surgery QuestionsDokumen98 halamanSample Surgery QuestionspandaBelum ada peringkat
- Varicocele and Testicular PainDokumen7 halamanVaricocele and Testicular PainseptaayuBelum ada peringkat
- ClinicalDokumen121 halamanClinicalArwa QishtaBelum ada peringkat
- Varicocele and InfertilityDokumen9 halamanVaricocele and InfertilityGrigore PopaBelum ada peringkat
- TolitsDokumen42 halamanTolitsAzela TuzonBelum ada peringkat
- Color Doppler Ultrasound Diagnosis of VaricoceleDokumen2 halamanColor Doppler Ultrasound Diagnosis of VaricoceleSehat SerasiBelum ada peringkat
- Scrotal SwellingDokumen40 halamanScrotal Swellingeirene simbolonBelum ada peringkat
- Canadian Undergraduate Urology Curriculum (Canuuc) : Scrotal ConditionsDokumen63 halamanCanadian Undergraduate Urology Curriculum (Canuuc) : Scrotal ConditionswhidiBelum ada peringkat
- Scrotal SwellingDokumen30 halamanScrotal Swellingumi muzayyanaBelum ada peringkat
- 11 I January 2023Dokumen4 halaman11 I January 2023IJRASETPublicationsBelum ada peringkat
- VaricoceleDokumen3 halamanVaricoceleMandy ChengBelum ada peringkat
- Testicle UltrasoundDokumen5 halamanTesticle UltrasoundJan Karl Roelhsen AngelesBelum ada peringkat
- SpermatoceleDokumen6 halamanSpermatoceleDae AhmadBelum ada peringkat
- Printable Version - Approval Reference No - 60247630Dokumen2 halamanPrintable Version - Approval Reference No - 60247630sohaibkhaled5858Belum ada peringkat
- VaricoceleDokumen1 halamanVaricoceleshailesh284Belum ada peringkat
- Varicocele and Male Infertility Evidence in The Era of Assisted Reproductive Technology 2161 038X 3 E114Dokumen3 halamanVaricocele and Male Infertility Evidence in The Era of Assisted Reproductive Technology 2161 038X 3 E114quickdannyBelum ada peringkat
- Surgery Illustrated - Surgical Atlas: Microsurgical VaricocelectomyDokumen8 halamanSurgery Illustrated - Surgical Atlas: Microsurgical Varicocelectomynugroho akhbarBelum ada peringkat
- Varicocele PresentasiDokumen22 halamanVaricocele PresentasiRini Oyien WulandariBelum ada peringkat
- Causes of Painless Scrotal Swelling in Children and Adolescents - UpToDateDokumen15 halamanCauses of Painless Scrotal Swelling in Children and Adolescents - UpToDateLeoberto Batista Pereira SobrinhoBelum ada peringkat
- ScrotalswellingDokumen82 halamanScrotalswellingNajihah MuhammadBelum ada peringkat
- "Oral Questions in Clinical Surgery" Case 1. LipomaDokumen19 halaman"Oral Questions in Clinical Surgery" Case 1. LipomaSherif Magdi100% (3)
- Surgical Management of Male Infertility: An Update: Monica Velasquez, Cigdem TanrikutDokumen13 halamanSurgical Management of Male Infertility: An Update: Monica Velasquez, Cigdem TanrikutIrvan PutraBelum ada peringkat
- Fundamental Research in Electrical Engineering: ArticleDokumen16 halamanFundamental Research in Electrical Engineering: ArticlepriyanBelum ada peringkat