A Fixed Guide Flange Appliance For Hemimandibulectomy
Diunggah oleh
Rohan Grover0 penilaian0% menganggap dokumen ini bermanfaat (0 suara)
119 tayangan4 halamanguide flange
Judul Asli
A Fixed Guide Flange Appliance for Hemimandibulectomy
Hak Cipta
© © All Rights Reserved
Format Tersedia
PDF, TXT atau baca online dari Scribd
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen Iniguide flange
Hak Cipta:
© All Rights Reserved
Format Tersedia
Unduh sebagai PDF, TXT atau baca online dari Scribd
0 penilaian0% menganggap dokumen ini bermanfaat (0 suara)
119 tayangan4 halamanA Fixed Guide Flange Appliance For Hemimandibulectomy
Diunggah oleh
Rohan Groverguide flange
Hak Cipta:
© All Rights Reserved
Format Tersedia
Unduh sebagai PDF, TXT atau baca online dari Scribd
Anda di halaman 1dari 4
A fixed guide flange appliance for
patients after a hemimandibulectomy
Santosh Nelogi, MDS,
a
Ramesh Chowdhary, MDS,
b
Maheshwari Ambi, BDS,
c
and Prachi Kothari, MDS
d
KLE VK Institute of Dental Science, Karnataka, India; S. Nijalingappa
Institute of Dental Sciences, Gulbarga, India
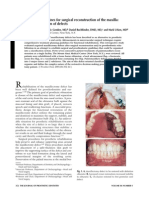
Oral carcinoma destroys structures, including the maxilla and mandible, which often require surgical management and
rehabilitation. Poor tissue support after mandibular reconstruction in patients with hemimandibular defects hinders the
reconstruction of functional and stable mandibular guide ange prostheses. The fabrication and use of a xed guide ange
prosthesis for rehabilitating patients with hemimandibular defects is described. The device permitted the use of the same
prosthesis for both the functional and mechanical correction of mandibular deviation and is indicated where the fabrication
of other appliances is contraindicated because of the compromised oral and physical state of the patient. (J Prosthet Dent
2013;110:429-432)
Oral cancer is the eighth most
common carcinoma worldwide,
1-5
de-
stroys tissue, which often requires resec-
tioninvolving the mandible, maxilla, oor
of the mouth, and tongue, and which
may adversely affect an individuals
mental health.
6-9
After mandibular
resection, patients experience the loss
of a proprioceptive sense of occlusion
and the absence of the muscles of
mastication on the surgical side, result-
ing in signicant rotation of the man-
dible upon closure, with the mandible
deviating toward the surgical side
(medial).
7,8,10-12
Treatment of the deviated mandible
starts with early corrective mandibular
movement therapy, including physi-
otherapeutic stretching exercises.
7,13,14
Various designs of prostheses used to
guide the mandible into centric oc-
clusion have been described.
7-22
A
removable guide ange prosthesis
cannot be retained intraorally if only
a few teeth remain in the sectioned
mandible. Retention can be further
compromised by radiation and surgical
scarring, which limits mouth opening
and functional vestibule depth such
that placement and removal of the
guide ange prosthesis is impossible
for the patient,
13
leading to further
occlusion problems.
13,7,20
Therefore, to
overcome the problems of the remov-
able design, a xed prosthesis that
would prevent scar contraction by
keeping muscles in the stressed condi-
tion and at the same time provide
corrective and masticatory functions
is indicated.
10,11
A technique using a
xed mandibular guide ange appli-
ance has been designed for the pros-
thetic management of patients after a
hemimandibulectomy.
TECHNIQUE
1. Make maxillary and segmented
mandibular impressions in elastomeric
impression material (Aquasil Ultra
Soft Putty; Aquasil Ultra LV Wash;
Dentsply Intl) andpour casts withType III
dental stone (Kalastone; Kalabahi Pvt
Ltd).
2. Articulate the maxillary and
mandibular casts at a reasonable centric
relationship with occlusion recording
wax (Dental Wax; Carmel Group Inc).
3. Place orthodontic tooth separa-
tors (Elstico Separador; Dental Morelli
Ltd) interdentally around one of the
mandibular posterior teeth so as to
create interdental space.
4. Adapt the prefabricated ortho-
dontic molar band (3M Unitek) of the
proposed tooth size on the prepared
mandibular cast (Fig. 1).
5. Bend a wrought wire (KC Smith
and Co) 1 mm thick and 5 cm long in
the shape of a U (with right angle
bends) with a tube 10 mm in length
occupying the base of the U, which
freely rotates around the wire (Fig. 2).
6. Adjust the height of the U-sha-
ped loop with a tube on a mounted
mandibular cast with a preadjusted
band in such a manner that the tube
will be placed horizontally at the level
of the buccal surface of maxillary
posterior teeth when the teeth are in
articulation. After conrming the po-
sition, solder a U-shaped loop (Den-
taurum Dental Technology) to the
preadjusted band (Figs. 3, 4).
a
Reader, Department of Prosthetic Dentistry, KLE VK Institute of Dental Science.
b
Professor, Department of Prosthetic Dentistry, S. Nijalingappa Institute of Dental Sciences.
c
Lecturer, Department of Prosthetic Dentistry, KLE VK Institute of Dental Science.
d
Postgraduate student, Department of Prosthetic Dentistry, KLE VK Institute of Dental Science.
Nelogi et al
7. Further adjust the band with
a soldered U-shaped loop with the
tube positioned medially and laterally
depending on the extent of the mandib-
ular deviation (Fig. 4).
8. Sterilize the appliance with dry
heat before cementing it to the pre-
pared site.
9. Remove the separators placed in
the patients mouth and place the
molar band with the U loop and eval-
uate for efcacy. Any adjustment in
angulation (medially, laterally) of the
U-shaped loop in relation to the molar
band is done at this stage so that
it guides the mandible in centric
occlusion with less strain on the patient
(Figs. 5, 6).
10. Once the t and function of
the appliance are conrmed with the
least possible strain on the patient,
cement it to the proposed tooth. The
design of the xed guide ange with
a U-shaped loop is adjusted in such
a way that it will not traumatize the
maxillary teeth and gingiva during
function (Fig. 7).
DISCUSSION
The mandibular guide ange pros-
thesis is commonly used and has been
the subject of many studies.
7,12-20
Sahin et al
18
and Chalian et al
19
advocated the fabrication of a cast
metal guidance prosthesis with sup-
porting and retentive anges for a pa-
tient after a mandibulectomy. The
authors claimed that the patient was
able to achieve a functional intercuspal
position after the insertion of the
prosthesis but that mastication was
limited to vertical movement only. Joshi
et al
20
described the fabrication of a
mandibular guide ange prosthesis and
suggested that a removable prosthesis
was an effective alternative for most
patients with mandibular defects,
considering the poor prognosis, dif-
culty in deciding on the use of the
implant, and economic feasibility. The
prosthesis described by Koumjian and
Firtell
21
was modied with a Herbst
appliance; the disadvantage of this
technique was the occasional separa-
tion of the tube and plunger at
maximum jaw opening. Prencipe et al
22
described a technique by simply insert-
ing and removing the guide ange.
The xed guide ange appliance
mentioned here consists of a molar
band with a U loop, which is cemented
to the tooth. The U loop of the xed
guide ange extends superiorly and
diagonally along the buccal surface of
1 Mandibular cast with molar band adapted to prepared
tooth.
2 U loop with tube.
3 U loop soldered to preadjusted band.
430 Volume 110 Issue 5
The Journal of Prosthetic Dentistry Nelogi et al
the maxillary premolar and molar teeth.
The stainless steel tube at the base of
the U loop glides the mandible into
centric occlusion, thereby reducing
mandibular deviation and allowing
for the normal vertical and horizontal
overlap of the remaining dentition
(Figs. 6, 7).
The xed guide ange presented
here prevents the deviation of the
mandible toward the surgical side and
serves to minimize radiation scarring by
keeping the tissue in a stressed condi-
tion; stretching the tissues during heal-
ing minimizes the amount of scarring
within the area.
7,14
The proposed xed guide ange
is recommended for those patients
with signicant mandibular resection
(Fig. 8) who have limited mouth
opening ability resulting from tissue
scarring and who lack the motor skills
to manage a removable prosthesis
(Fig. 9).
The technique is proposed only
when the remaining teeth are peri-
odontally sound enough to bear the
angular pull of muscles and masti-
catory forces. The xed guide ange
prosthesis proposed is functional, aes-
thetic, comfortable, and easy to fabri-
cate and repair; it also allows better
hygiene maintenance.
After the placement of a xed
mandibular guide ange prosthesis,
the patient must be evaluated for any
strain or pain in the temporoman-
dibular joints and muscles every 6
hours for the rst 72 hours after
cementation. The patient is further
recalled after 6, 12, and 28 days to
evaluate the efcacy of the xed guide
ange appliance and to ensure that
no misalignment or migration of the
maxillary tooth/teeth adjacent to the
loop has occurred in the remaining
dentition.
SUMMARY
The proposed guide ange is a
simple alternative to the existing
removable mandibular guide ange
prosthesis. The guide ange consists of
a molar band with a U loop, which is
cemented to one of the mandibular
teeth. Disadvantages include the pos-
sible migration of maxillary teeth adja-
cent to the loop. Further research
should focus on determining the inu-
ence of the xed guide ange on the
maxillary teeth and on any long-term
adverse effects of its use.
4 Fixed appliance guide ange.
5 Occlusal view of cemented xed guide ange.
6 Fixed guide ange showing position and level of loop at
time of articulation.
November 2013 431
Nelogi et al
REFERENCES
1. Petersen PE. Strengthening the prevention of
oral cancer: the WHO perspective. Commu-
nity Dent Oral Epidemiol 2005;33:397-9.
2. Pisani P, Bray F, Parkin DM. Estimates of the
world-wideprevalenceof cancer for 25sites inthe
adult population. Int J Cancer 2002;97:72-81.
3. Jemal A, Thomas A, Murray T, Thun M.
Cancer statistics, 2002. CA Cancer J Clin
2002;52:23-47.
4. Silverman S. Demographics and
occurrence of oral and pharyngeal
cancers. The outcomes, the trends, the
challenge. J Am Dent Assoc
2001;132(suppl):7S-11S.
5. Silverberg E, Boring CC, Squires TS. Cancer
statistics, 1990. CA Cancer J Clin 1990;40:
9-26.
6. Logemann JA, Bytell DE. Swallowing disor-
ders in three types of head and neck surgical
patients. Cancer 1979;44:1095-105.
7. Beumer J III, Curtis TA, Marunick MT. Maxil-
lofacial rehabilitation. In: Prosthodontic and
surgical consideration. St Louis: Ishiyaku,
EuroAmerica; 1996. p. 113-24, 184-8.
8. Taylor TD. Clinical maxillofacial prosthetics.
Chicago: Quintessence; 1997. p. 171-88.
9. Tjellstrom A, Jansson K, Branemark PI. Cranio-
facial defects in advanced osseontegration sur-
gery. In: Worthington P, Brnemark PI, editors.
Advanced osseointegration surgery: applica-
tions in the maxillofacial region. Chicago:
Quintessence; 1992. p. 263-312.
10. Olson ML, Shedd DP. Disability and rehabili-
tation in head and neck cancer patients after
treatment. Head Neck Surg 1978;1:52-8.
11. Curtis DA, Plesh O, Miller AJ, Curtis TA,
Sharma A, Sehweitzer RL, et al.
A comparison of masticatory function with
or without reconstruction of the mandible.
Head Neck 1997;19:287-96.
12. Aramany MA, Myers EN. Intermaxillary xa-
tion following mandibular resection.
J Prosthet Dent 1977;37:437-44.
13. Schneider RL, Taylor TD. Mandibular resec-
tion guidance prostheses: a literature review.
J Prosthet Dent 1986;55:84-6.
14. Robinson JE, Rubright WC. Use of a guide
plane for maintaining the residual fragment
in partial or hemimandibulectomy. J Prosthet
Dent 1964;14:992-9.
15. Moore DJ, Mitchell DL. Rehabilitating
dentulous hemimandibulectomy patients.
J Prosthet Dent 1976;35:202-6.
16. Fattore L, Marchmont-Robinson H, Crinzi RA,
Edmonds DC. Use of a two-piece Gunning
splint as a mandibular guide appliance for a
patient treated for ameloblastoma. Oral Sur-
gery Oral Med Oral Pathol 1988;66:662-5.
17. Hasanreisoglu U, Utasli S, Gurbuz A.
Mandibular guidance prosthesis following
resection procedures: three case reports. Eur J
Prosthodont Restor Dent 1992;1:69-72.
18. Sahin N, Hekimoglu C, Aslan Y. The fabrication
of cast metal guidance ange prostheses for
a patient with segmental mandibulectomy: a
clinical report. J Prosthet Dent 2005;93:217-20.
19. Chalian VA, Drane JB, Standish SM. Maxil-
lofacial prosthetics multidisciplinary practice.
Baltimore: Williams & Wilkins; 1972. p. 148.
20. Joshi PR, Saini GS, Shetty P, Bhat SG. Pros-
thetic rehabilitation following segmental
mandibulectomy. J Ind Prosthodont Soc
2008;8:108-11.
21. Koumjian JH, Firtell DN. An appliance to
correct mandibular deviation in a dentulous
patient with a discontinuity defect. J Prosthet
Dent 1992;67:833-4.
22. Prencipe MA, Durval E, De Salvador A,
Tatini C, Roberto B. Removable partial
prosthesis (RPP) with acrylic resin ange for
the mandibular guidance therapy.
J Maxillofac Oral Surg 2009;8:19-21.
Corresponding author:
Dr Santosh Nelogi
House #1, l.i.g. Phase III
Adarsh Nagar, Gulbarga, Karnatka
INDIA
E-mail: santrodent@rediffmail.com
Copyright 2013 by the Editorial Council for
The Journal of Prosthetic Dentistry.
7 Denitive intraoral result.
8 Panoramic radiographic view showing mandibular discontinuity defect.
9 Intraoral view showing mandibular deviation toward
resected side.
432 Volume 110 Issue 5
The Journal of Prosthetic Dentistry Nelogi et al
Anda mungkin juga menyukai
- MCQs in Oral Surgery: A comprehensive reviewDari EverandMCQs in Oral Surgery: A comprehensive reviewPenilaian: 5 dari 5 bintang5/5 (6)
- Short ImplantsDari EverandShort ImplantsBoyd J. TomasettiBelum ada peringkat
- A Fixed Guide Flange Appliance For Patients Af Ter A HemimandibulectomyDokumen4 halamanA Fixed Guide Flange Appliance For Patients Af Ter A HemimandibulectomyKrupali JainBelum ada peringkat
- Fabrication of Conventional Complete Dentures For A Left Segmental MandibulectomyDokumen4 halamanFabrication of Conventional Complete Dentures For A Left Segmental MandibulectomyIndrani DasBelum ada peringkat
- Articol Pentru Teme 14-18Dokumen9 halamanArticol Pentru Teme 14-18Diamanta Yalomit CirsteaBelum ada peringkat
- Tooth-Supported Telescopic Prostheses in Compromised Dentitions - A Clinical ReportDokumen4 halamanTooth-Supported Telescopic Prostheses in Compromised Dentitions - A Clinical Reportpothikit100% (1)
- Prosthodontic Rehabilitation Using Attachment Retained Overdenture - Case ReportsDokumen7 halamanProsthodontic Rehabilitation Using Attachment Retained Overdenture - Case ReportsIOSRjournalBelum ada peringkat
- The Socket-Shield Technique To Support The Buccofacial Tissues at Immediate Implant Placement PDFDokumen7 halamanThe Socket-Shield Technique To Support The Buccofacial Tissues at Immediate Implant Placement PDFAhmed Mohammed Saaduddin SapriBelum ada peringkat
- SJDS 34100 103Dokumen4 halamanSJDS 34100 103Andi Sry PermatasariBelum ada peringkat
- Biologically Oriented Preparation Technique For SurgicallyDokumen6 halamanBiologically Oriented Preparation Technique For SurgicallyAbdelrahman Galal100% (1)
- Telescopic Overdenture: A Case Report: C. S. Shruthi, R. Poojya, Swati Ram, AnupamaDokumen5 halamanTelescopic Overdenture: A Case Report: C. S. Shruthi, R. Poojya, Swati Ram, AnupamaRani PutriBelum ada peringkat
- Chapter 14 - Unilateral Subperiosteal ImplantsDokumen55 halamanChapter 14 - Unilateral Subperiosteal ImplantsKomal TalrejaBelum ada peringkat
- Pps 2Dokumen5 halamanPps 2Hendy NurahadiBelum ada peringkat
- Management of Supraerupted TeethDokumen4 halamanManagement of Supraerupted TeethankitbudhirajaBelum ada peringkat
- Chung2010 PDFDokumen12 halamanChung2010 PDFsmritiBelum ada peringkat
- Gigi Tiruan GasketDokumen5 halamanGigi Tiruan GasketGus BasyaBelum ada peringkat
- Prosthetic Rehabilitation of Maxillectomy Patient With Telescopic DenturesDokumen6 halamanProsthetic Rehabilitation of Maxillectomy Patient With Telescopic DenturesVero AngelBelum ada peringkat
- Restoration of Edentulous Maxillae With OverdenturesDokumen29 halamanRestoration of Edentulous Maxillae With OverdenturesCostina BolboriciBelum ada peringkat
- 2016 Article 143Dokumen7 halaman2016 Article 143Andrea TokumotoBelum ada peringkat
- BDJ Volume 201 Issue 6 2006 (Doi 10.1038/sj - bdj.4814041) Chee, W Jivraj, S - Treatment Planning of The Edentulous MandibleDokumen9 halamanBDJ Volume 201 Issue 6 2006 (Doi 10.1038/sj - bdj.4814041) Chee, W Jivraj, S - Treatment Planning of The Edentulous MandibleahmadBelum ada peringkat
- Rehab of Severley Worn Dentition-Using Fixed and RemovableDokumen0 halamanRehab of Severley Worn Dentition-Using Fixed and RemovableFaheemuddin MuhammadBelum ada peringkat
- A Countdown To Orthognathic SurgeryDokumen5 halamanA Countdown To Orthognathic SurgeryhaneefmdfBelum ada peringkat
- Awais AssignmentDokumen3 halamanAwais AssignmentMuhammad AwaisBelum ada peringkat
- Full Mouth Rehabilitation of The Patient With Severly Worn Out Dentition A Case Report.Dokumen5 halamanFull Mouth Rehabilitation of The Patient With Severly Worn Out Dentition A Case Report.sivak_198100% (1)
- Management of Impacted Maxillary Canines Using Mandibular AnchorageDokumen4 halamanManagement of Impacted Maxillary Canines Using Mandibular AnchoragedrsankhyaBelum ada peringkat
- Oh 2010Dokumen5 halamanOh 2010gbaez.88Belum ada peringkat
- ArticleDokumen4 halamanArticleDrRahul Puri GoswamiBelum ada peringkat
- Prosthodontic Rehabilitation With Onlay Removable Partial Denture: A CaseDokumen7 halamanProsthodontic Rehabilitation With Onlay Removable Partial Denture: A CasePhanQuangHuyBelum ada peringkat
- Root Perforation Associated With The Use of A Miniscrew Implant Used For Orthodontic AnchorageDokumen11 halamanRoot Perforation Associated With The Use of A Miniscrew Implant Used For Orthodontic AnchorageSALAHEDDINE BLIZAKBelum ada peringkat
- Precision Attachments For The 21st CenturyDokumen6 halamanPrecision Attachments For The 21st CenturyMohsin Habib67% (3)
- Edéntulo Tota Superior HíbridaDokumen7 halamanEdéntulo Tota Superior HíbridaAlexis BenitesBelum ada peringkat
- AJODONovember2016Dokumen13 halamanAJODONovember2016garciadeluisaBelum ada peringkat
- Unconventional Fixed Partial Denture: A Simple Solution For Aesthetic RehabilitationDokumen4 halamanUnconventional Fixed Partial Denture: A Simple Solution For Aesthetic RehabilitationAdvanced Research PublicationsBelum ada peringkat
- Kaldenbach Carina Articol EPI Engleza PDFDokumen9 halamanKaldenbach Carina Articol EPI Engleza PDFFlorin UngureanuBelum ada peringkat
- Prosthodontics PDFDokumen27 halamanProsthodontics PDFزهراء فاضل اجبير فعيل100% (1)
- Conservative Mangement of Tilted AbutmentsDokumen3 halamanConservative Mangement of Tilted Abutmentsrayavarapu sunilBelum ada peringkat
- Implant Overdenture ComplicationsDokumen5 halamanImplant Overdenture ComplicationsAdina UlaruBelum ada peringkat
- Jap 2 58Dokumen3 halamanJap 2 58joephinBelum ada peringkat
- Rotational Versus ConventionalDokumen7 halamanRotational Versus ConventionalKhaleda ShafiraBelum ada peringkat
- 10 1016@j Prosdent 2015 05 010 PDFDokumen5 halaman10 1016@j Prosdent 2015 05 010 PDFammarkochiBelum ada peringkat
- Aula EduinaDokumen7 halamanAula EduinaJoão S NetoBelum ada peringkat
- Sectional RPDDokumen5 halamanSectional RPDTejas KhaireBelum ada peringkat
- The Size of Occlusal Rest Seats PreparedDokumen7 halamanThe Size of Occlusal Rest Seats PreparedPatra PrimadanaBelum ada peringkat
- Forced EruptionDokumen4 halamanForced Eruptiondrgeorgejose7818Belum ada peringkat
- Hybrid Prosthesis for Tooth RetentionDokumen4 halamanHybrid Prosthesis for Tooth RetentionGowriKrishnaraoBelum ada peringkat
- RestorationDokumen5 halamanRestorationFathira AiniBelum ada peringkat
- Boneceramic Graft Regenerates Alveolar Defects But Slows Orthodontic Tooth Movement With Less Root ResorptionDokumen10 halamanBoneceramic Graft Regenerates Alveolar Defects But Slows Orthodontic Tooth Movement With Less Root Resorptionplayer osamaBelum ada peringkat
- En-Masse Protraction of Mandibular Posterior Teeth Into Missing Mandibular Lateral Incisor Spaces Using A Fixed Functional ApplianceDokumen12 halamanEn-Masse Protraction of Mandibular Posterior Teeth Into Missing Mandibular Lateral Incisor Spaces Using A Fixed Functional ApplianceNingombam Robinson SinghBelum ada peringkat
- Bedrossian Treatment Planning The Maxilla PDFDokumen11 halamanBedrossian Treatment Planning The Maxilla PDFSitiKhadijahBelum ada peringkat
- Canine Impaction Different MethodsDokumen11 halamanCanine Impaction Different MethodsMSHBelum ada peringkat
- Guerrero 1997Dokumen10 halamanGuerrero 1997Deyvid Gustavo Capelo RiosBelum ada peringkat
- Use of Implants in The Pterygoid Region For Prosthodontic TreatmentDokumen4 halamanUse of Implants in The Pterygoid Region For Prosthodontic TreatmentSidhartha KumarBelum ada peringkat
- Use of Implants in The Pterygoid RegionDokumen4 halamanUse of Implants in The Pterygoid RegionManjulika TysgiBelum ada peringkat
- 4353 17293 1 PBDokumen2 halaman4353 17293 1 PBSwagata DebBelum ada peringkat
- Tretment PlanningDokumen6 halamanTretment PlanningAkshay Gajakosh0% (1)
- A Classification System of DefectsDokumen12 halamanA Classification System of DefectsPrana SkyaBelum ada peringkat
- 2007 - Intrusion of Overerupted Molars byDokumen7 halaman2007 - Intrusion of Overerupted Molars byTien Li AnBelum ada peringkat
- Prosthetic Rehabilitation of Mandibular Defects With Fixed-Removable Partial Denture Prosthesis Using Precision Attachment - A Twin Case ReportDokumen17 halamanProsthetic Rehabilitation of Mandibular Defects With Fixed-Removable Partial Denture Prosthesis Using Precision Attachment - A Twin Case ReportIvy MedBelum ada peringkat
- Treatment Planning Single Maxillary Anterior Implants for DentistsDari EverandTreatment Planning Single Maxillary Anterior Implants for DentistsBelum ada peringkat
- Maxillary Major ConnectorsDokumen20 halamanMaxillary Major ConnectorsRohan GroverBelum ada peringkat
- Retainers and Connectors in Fixed Partial DenturesDokumen1 halamanRetainers and Connectors in Fixed Partial DenturesRohan GroverBelum ada peringkat
- LD Gingival RetractionDokumen39 halamanLD Gingival RetractionRohan GroverBelum ada peringkat
- Pi I 0022391385906407Dokumen7 halamanPi I 0022391385906407Rohan GroverBelum ada peringkat
- Gag Reflex Isdh 2009 No Patient Idppt1374Dokumen38 halamanGag Reflex Isdh 2009 No Patient Idppt1374Rohan GroverBelum ada peringkat
- Management of Compromised RidgeDokumen5 halamanManagement of Compromised RidgeBindu Madhavi PaladuguBelum ada peringkat
- Inhibition of Polymerization of Polyvinyl Siloxanes byDokumen4 halamanInhibition of Polymerization of Polyvinyl Siloxanes byRohan GroverBelum ada peringkat
- Anterior Key Method For Indexing Orbital ProsthesesDokumen4 halamanAnterior Key Method For Indexing Orbital ProsthesesRohan GroverBelum ada peringkat
- Occlusal Rehabilitation of A Patient With Dentinogenesis ImperfectaDokumen4 halamanOcclusal Rehabilitation of A Patient With Dentinogenesis ImperfectaRohan GroverBelum ada peringkat
- Attachment Procedures: Attachments in DentistryDokumen7 halamanAttachment Procedures: Attachments in DentistryRohan GroverBelum ada peringkat
- Sps 24188Dokumen10 halamanSps 24188Rohan GroverBelum ada peringkat
- DR Narendra Basutkar M.D.S (Prosthodontics)Dokumen42 halamanDR Narendra Basutkar M.D.S (Prosthodontics)Rohan GroverBelum ada peringkat
- GlossectomyDokumen68 halamanGlossectomyRohan GroverBelum ada peringkat
- Centric Relation Concepts and ControversiesDokumen51 halamanCentric Relation Concepts and ControversiesRohan Grover100% (11)
- Deser DsfdsDokumen93 halamanDeser DsfdsNaresh TeresBelum ada peringkat
- Precision AttachmentsDokumen92 halamanPrecision AttachmentsRohan Grover100% (3)
- Alveolar Bone - VandyDokumen80 halamanAlveolar Bone - VandyRohan GroverBelum ada peringkat
- 03 02 ARTICOL Classification System For Partial EdentulismDokumen13 halaman03 02 ARTICOL Classification System For Partial EdentulismRohan GroverBelum ada peringkat
- AmalgamDokumen60 halamanAmalgamRohan GroverBelum ada peringkat
- Maxillary Sinus Disease - Power Point PresentationDokumen45 halamanMaxillary Sinus Disease - Power Point PresentationRohan Grover100% (1)
- Try in of Waxed Up DenturesDokumen58 halamanTry in of Waxed Up DenturesRohan Grover100% (1)
- Maxillary LandmarksDokumen30 halamanMaxillary LandmarksRajsandeep Singh86% (14)
- Casting Procedures and Casting DefectsDokumen70 halamanCasting Procedures and Casting DefectsRohan Grover100% (1)
- Maxillary LandmarksDokumen30 halamanMaxillary LandmarksRajsandeep Singh86% (14)
- MRI Guide: History, Fundamentals, ApplicationsDokumen22 halamanMRI Guide: History, Fundamentals, ApplicationsRohan GroverBelum ada peringkat
- Basic Removable Appliances DesignDokumen160 halamanBasic Removable Appliances DesignRohan Grover100% (1)
- Management of Patient's Gag Reflex in Making Alginate ImprDokumen2 halamanManagement of Patient's Gag Reflex in Making Alginate Imprapi-3710948Belum ada peringkat
- Flexibility Is Our Strength: Making Millions Smile ™Dokumen41 halamanFlexibility Is Our Strength: Making Millions Smile ™Rohan GroverBelum ada peringkat
- Gag Reflex Isdh 2009 No Patient Idppt1374Dokumen38 halamanGag Reflex Isdh 2009 No Patient Idppt1374Rohan GroverBelum ada peringkat
- Gtbr2016 Main TextDokumen214 halamanGtbr2016 Main TextRaimundo Isidro MachavaBelum ada peringkat
- Guide To Environmental Microbiological MonitoringDokumen29 halamanGuide To Environmental Microbiological MonitoringzyrtylBelum ada peringkat
- Acute Pain Abdomen in Surgical PracticeDokumen34 halamanAcute Pain Abdomen in Surgical PracticedrakashnardeBelum ada peringkat
- How To Measure Frailty in Your PatientsDokumen1 halamanHow To Measure Frailty in Your PatientsZahra'a Al-AhmedBelum ada peringkat
- Wet Cell and Radial DeviceDokumen21 halamanWet Cell and Radial DeviceChava Chavous100% (1)
- Boaz Gobera (NsambyaHospitalReport2021)Dokumen62 halamanBoaz Gobera (NsambyaHospitalReport2021)GOBERA BOAZBelum ada peringkat
- A Pain Education ProgrammeDokumen13 halamanA Pain Education Programmeapi-244230664Belum ada peringkat
- MacroMinerals: Calcium, Phosphorus, Potassium, Sodium, Chloride, and MagnesiumDokumen9 halamanMacroMinerals: Calcium, Phosphorus, Potassium, Sodium, Chloride, and MagnesiumDerek AtienzaBelum ada peringkat
- Part I سنه القمله 2016Dokumen20 halamanPart I سنه القمله 2016Aloah122346Belum ada peringkat
- Nursing Care Plan #1 Assessment Explanation of The Problem Goal/Objective Intervention Rational EvaluationDokumen10 halamanNursing Care Plan #1 Assessment Explanation of The Problem Goal/Objective Intervention Rational EvaluationmalindaBelum ada peringkat
- Cannabis Phenolics and Their BioactivitiesDokumen44 halamanCannabis Phenolics and Their BioactivitiesTomislav ĆurićBelum ada peringkat
- EXP 6 - Fecal Coliform Test - StudentDokumen8 halamanEXP 6 - Fecal Coliform Test - StudentAbo SmraBelum ada peringkat
- Vocational Rehabilitation Programs for People with DisabilitiesDokumen44 halamanVocational Rehabilitation Programs for People with DisabilitiesKannappa Shetty MudiyanuruBelum ada peringkat
- Nat Ag Winter Wheat in N Europe by Marc BonfilsDokumen5 halamanNat Ag Winter Wheat in N Europe by Marc BonfilsOrto di CartaBelum ada peringkat
- Epidemiology SlidesDokumen30 halamanEpidemiology SlidesHongMingBelum ada peringkat
- ER Nurse CVDokumen5 halamanER Nurse CVLopezDistrict FarmersHospitalBelum ada peringkat
- Cellular Detox Smoothies PDFDokumen20 halamanCellular Detox Smoothies PDFRuth Engelthaler100% (2)
- 1.4.2 Making VaccinesDokumen21 halaman1.4.2 Making VaccinesVikas Viki0% (1)
- Module 4 Visual ImpairmentDokumen61 halamanModule 4 Visual ImpairmentMina Agarwal100% (5)
- Cardiovascular Embryology StagesDokumen109 halamanCardiovascular Embryology StagesBir Singh100% (1)
- Human Induced HazardDokumen56 halamanHuman Induced HazardMaria Flor Pabelonia100% (3)
- Budwig Cancer GuideDokumen116 halamanBudwig Cancer GuideStanley ChanBelum ada peringkat
- Book of Vile DarknessDokumen25 halamanBook of Vile Darknessv0idless100% (2)
- Shift work effects on doctors' healthDokumen4 halamanShift work effects on doctors' healthHalilGutajBelum ada peringkat
- Tugas Jurnal PaliatifDokumen11 halamanTugas Jurnal PaliatifSiti Wahyuningsih100% (1)
- Unit - 10 - General Characters and Classification of Fungi by Dr. Kirtika PadaliaDokumen38 halamanUnit - 10 - General Characters and Classification of Fungi by Dr. Kirtika PadalianucleophilicmishraBelum ada peringkat
- Coronavirus British English Intermediate b1 b2 GroupDokumen4 halamanCoronavirus British English Intermediate b1 b2 GroupAngel AnitaBelum ada peringkat
- Medscape Physician Compensation Report 2023 - Your Income Vs Your Peers'Dokumen8 halamanMedscape Physician Compensation Report 2023 - Your Income Vs Your Peers'David J ShinBelum ada peringkat
- Soal BAHASA INGGRIS - X - KUMER - PAKET 2Dokumen13 halamanSoal BAHASA INGGRIS - X - KUMER - PAKET 2Agus SuhendraBelum ada peringkat
- Hardy-Weinberg Practice Problems 2017 ANSWER KEY PDFDokumen3 halamanHardy-Weinberg Practice Problems 2017 ANSWER KEY PDFzairaaa999Belum ada peringkat