Introduction
Diunggah oleh
Nantini Gopal0 penilaian0% menganggap dokumen ini bermanfaat (0 suara)
9 tayangan2 halamanIntroduction
Hak Cipta
© © All Rights Reserved
Format Tersedia
DOCX, PDF, TXT atau baca online dari Scribd
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniIntroduction
Hak Cipta:
© All Rights Reserved
Format Tersedia
Unduh sebagai DOCX, PDF, TXT atau baca online dari Scribd
0 penilaian0% menganggap dokumen ini bermanfaat (0 suara)
9 tayangan2 halamanIntroduction
Diunggah oleh
Nantini GopalIntroduction
Hak Cipta:
© All Rights Reserved
Format Tersedia
Unduh sebagai DOCX, PDF, TXT atau baca online dari Scribd
Anda di halaman 1dari 2
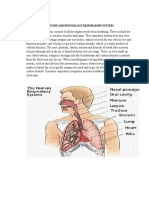
Introduction
A pheochromocytoma is a rare, catecholamine-secreting tumor derived from chromaffin cells.
When such tumors arise outside of the adrenal gland, they are termed extra-adrenal
pheochromocytomas, or paragangliomas. (See the images below.) Because of excessive
catecholamine secretion, pheochromocytomas may precipitate life-threatening hypertension or
cardiac arrhythmias. If the diagnosis of a pheochromocytoma is overlooked, the consequences
can be disastrous, even fatal; however, if a pheochromocytoma is found, it is potentially
curable.
[1]
Axial, T2-weighted magnetic resonance imaging (MRI) scan showing large left suprarenal mass of high signal
intensity on a T2-weighted image. The mass is a pheochromocytoma.
Abdominal computed tomography (CT) scan demonstrating left suprarenal mass of soft-tissue attenuation
representing a paraganglioma
The term pheochromocytoma (in Greek, phios means dusky, chroma means color, and cytoma
means tumor) refers to the color the tumor cells acquire when stained with chromium salts. Roux
performed the first surgical resection of a pheochromocytoma in Lausanne, Switzerland in 1926.
Later the same year, Charles Mayo performed the first surgical resection in the United States.
[2]
In a study by Paraby et al, severe hypertension was associated with 5 of 35 pheochromocytoma
resections (14.3%), compared with 2 of 106 nonpheochromocytoma adrenal tumor resections
(1.9%), and there was a significant increase in the need for intraoperative hypertensive treatment
in the pheochromocytoma patients. In the study, the researchers investigated whether significant
differences exist between perioperative hemodynamic changes arising from laparoscopic
adrenalectomy for pheochromocytomas and those stemming from the use of the procedure for
other types of adrenal tumors. The study included 34 patients who underwent laparoscopic
adrenalectomy for pheochromocytomas (total resections = 35) and 104 patients who underwent
the laparoscopic adrenalectomy for other tumors (total resections = 106).
[3]
Despite the greater occurrence of hypertension in the pheochromocytoma group, the
investigators found no instances of transient or persistent systolic blood pressure of greater than
220 mm Hg in either group and noted no significant differences in recovery room hemodynamic
parameters, frequency of persistent hypotension, or occurrence of heart rates greater than
120/min between the 2 groups.
Over 90% of pheochromocytomas are located within the adrenal glands, and 98% are within the
abdomen. Extra-adrenal pheochromocytomas develop in the paraganglion chromaffin tissue of
the sympathetic nervous system. They may occur anywhere from the base of the brain to the
urinary bladder. Common locations for extra-adrenal pheochromocytomas include the organ of
Zuckerkandl (close to origin of the inferior mesenteric artery), bladder wall, heart, mediastinum,
and carotid and glomus jugulare bodies
3
.
1. Waguespack SG, Rich T, Grubbs E, et al. A Current Review of the Etiology, Diagnosis, and
Treatment of Pediatric Pheochromocytoma and Paraganglioma. J Clin Endocrinol Metab. Mar 9
2010;[Medline].
2. Sheps SG, Jiang NS, Klee GG, van Heerden JA. Recent developments in the diagnosis and
treatment of pheochromocytoma. Mayo Clin Proc. Jan 2010;65(1):88-95. [Medline].
3. Parnaby CN, Serpell MG, Connell JM, et al. Perioperative haemodynamic changes in patients
undergoing laparoscopic adrenalectomy for phaeochromocytomas and other adrenal tumours.
Surgeon. Feb 2010;8(1):9-14. [Medline].
Anda mungkin juga menyukai
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDari EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RacePenilaian: 4 dari 5 bintang4/5 (895)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDari EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifePenilaian: 4 dari 5 bintang4/5 (5794)
- Ten N Sjs ReviewDokumen5 halamanTen N Sjs ReviewNantini GopalBelum ada peringkat
- Differential Diagnosis of Gastric CarcinomaDokumen3 halamanDifferential Diagnosis of Gastric CarcinomaNantini GopalBelum ada peringkat
- Figure 1. Origin of Hydatidiform Mole. The Hydatidiform Mole Most Frequently Results From The Fertilization of An Oocyte Without Active NucleusDokumen2 halamanFigure 1. Origin of Hydatidiform Mole. The Hydatidiform Mole Most Frequently Results From The Fertilization of An Oocyte Without Active NucleusNantini GopalBelum ada peringkat
- Basic Science of Articular Cartilage and Osteoarthritis: Andrew D. Pearle, MD, Russell F. Warren, MD, Scott A. Rodeo, MDDokumen12 halamanBasic Science of Articular Cartilage and Osteoarthritis: Andrew D. Pearle, MD, Russell F. Warren, MD, Scott A. Rodeo, MDNantini GopalBelum ada peringkat
- NEJM 347 p0340Dokumen7 halamanNEJM 347 p0340Nantini GopalBelum ada peringkat
- DSADokumen7 halamanDSANantini GopalBelum ada peringkat
- DivingDokumen5 halamanDivingNantini GopalBelum ada peringkat
- Shoe Dog: A Memoir by the Creator of NikeDari EverandShoe Dog: A Memoir by the Creator of NikePenilaian: 4.5 dari 5 bintang4.5/5 (537)
- Grit: The Power of Passion and PerseveranceDari EverandGrit: The Power of Passion and PerseverancePenilaian: 4 dari 5 bintang4/5 (588)
- The Yellow House: A Memoir (2019 National Book Award Winner)Dari EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Penilaian: 4 dari 5 bintang4/5 (98)
- The Little Book of Hygge: Danish Secrets to Happy LivingDari EverandThe Little Book of Hygge: Danish Secrets to Happy LivingPenilaian: 3.5 dari 5 bintang3.5/5 (400)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDari EverandNever Split the Difference: Negotiating As If Your Life Depended On ItPenilaian: 4.5 dari 5 bintang4.5/5 (838)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDari EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FuturePenilaian: 4.5 dari 5 bintang4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDari EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryPenilaian: 3.5 dari 5 bintang3.5/5 (231)
- Rise of ISIS: A Threat We Can't IgnoreDari EverandRise of ISIS: A Threat We Can't IgnorePenilaian: 3.5 dari 5 bintang3.5/5 (137)
- The Emperor of All Maladies: A Biography of CancerDari EverandThe Emperor of All Maladies: A Biography of CancerPenilaian: 4.5 dari 5 bintang4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDari EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaPenilaian: 4.5 dari 5 bintang4.5/5 (266)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDari EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersPenilaian: 4.5 dari 5 bintang4.5/5 (345)
- On Fire: The (Burning) Case for a Green New DealDari EverandOn Fire: The (Burning) Case for a Green New DealPenilaian: 4 dari 5 bintang4/5 (74)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDari EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyPenilaian: 3.5 dari 5 bintang3.5/5 (2259)
- Team of Rivals: The Political Genius of Abraham LincolnDari EverandTeam of Rivals: The Political Genius of Abraham LincolnPenilaian: 4.5 dari 5 bintang4.5/5 (234)
- The Unwinding: An Inner History of the New AmericaDari EverandThe Unwinding: An Inner History of the New AmericaPenilaian: 4 dari 5 bintang4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDari EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You ArePenilaian: 4 dari 5 bintang4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Dari EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Penilaian: 4.5 dari 5 bintang4.5/5 (121)
- Her Body and Other Parties: StoriesDari EverandHer Body and Other Parties: StoriesPenilaian: 4 dari 5 bintang4/5 (821)
- Anatomy and PhysiologyDokumen37 halamanAnatomy and PhysiologyJamesMarcoMBelum ada peringkat
- LactationDokumen24 halamanLactationJenyl Bajado100% (1)
- Liv 6Dokumen1 halamanLiv 6ray72roBelum ada peringkat
- Anatomy and Physiology Respiratory SystemDokumen7 halamanAnatomy and Physiology Respiratory Systemnoronisa talusobBelum ada peringkat
- Massaging Auricular PointsDokumen2 halamanMassaging Auricular PointsCarissa Nichols100% (5)
- Chronic Kidney Disease Pathophysiology Schematic DiagramDokumen3 halamanChronic Kidney Disease Pathophysiology Schematic Diagramnursing concept maps100% (5)
- An Act of KindnessDokumen4 halamanAn Act of KindnessKai Xuen LooBelum ada peringkat
- PhysiologyDokumen15 halamanPhysiology221618Belum ada peringkat
- Animal Tissue NotesDokumen20 halamanAnimal Tissue NotesSahejBelum ada peringkat
- MCQ Questions End of Module EndocrineDokumen9 halamanMCQ Questions End of Module EndocrineAlif Akmal100% (2)
- Lecture On The Histology of Cerebrum and Meninges by Dr. RoomiDokumen20 halamanLecture On The Histology of Cerebrum and Meninges by Dr. RoomiMudassar Roomi100% (1)
- Normal Value For Urine TestDokumen2 halamanNormal Value For Urine TestMarcellino NernereBelum ada peringkat
- Gross Anatomy of LungsDokumen8 halamanGross Anatomy of LungsAriguna WijayaBelum ada peringkat
- Pain ControlDokumen313 halamanPain ControlBlueSaga100% (1)
- Zollinger Case StudyDokumen53 halamanZollinger Case StudyGLYDEL CORDEROBelum ada peringkat
- HEALTH ASSESSMENT!!!Digestive SystemDokumen24 halamanHEALTH ASSESSMENT!!!Digestive Systemapi-19885395100% (1)
- Summative PracticeDokumen42 halamanSummative PracticeDewi SallehBelum ada peringkat
- AnaPhy Lab Exercise 24-41Dokumen6 halamanAnaPhy Lab Exercise 24-41Angelyka Cabalo50% (2)
- Chapter 30Dokumen3 halamanChapter 30Grant ParkBelum ada peringkat
- Tumors and Cancers Endocrine Glands - Blood - Marrow - LymphDokumen231 halamanTumors and Cancers Endocrine Glands - Blood - Marrow - LymphAndré Jason MendesBelum ada peringkat
- What Is GravesDokumen3 halamanWhat Is GravesSynoyk AnunciacionBelum ada peringkat
- Presentation JaundiceDokumen49 halamanPresentation JaundiceVinoth KumarBelum ada peringkat
- Unit 5. Interaction and HealthDokumen11 halamanUnit 5. Interaction and Healthtamarita90Belum ada peringkat
- Revision QuestionsDokumen11 halamanRevision QuestionsxilcomBelum ada peringkat
- Acute Kidney Injury and Chronic Kidney DiseaseDokumen59 halamanAcute Kidney Injury and Chronic Kidney Diseasesho bartBelum ada peringkat
- Pathophysiology of Breast CancerDokumen3 halamanPathophysiology of Breast Cancerpauline mangadaBelum ada peringkat
- Anatomy and Physiology-NotesDokumen6 halamanAnatomy and Physiology-NotesAkirah Jewelle JaenBelum ada peringkat
- Kidney Quiz - Path Exam 3Dokumen15 halamanKidney Quiz - Path Exam 3tatti9990% (1)
- Electrophysiological Properties of Cardiac MyocytesDokumen39 halamanElectrophysiological Properties of Cardiac Myocytesapi-19916399Belum ada peringkat
- OmrDokumen39 halamanOmrabhijeetBelum ada peringkat