Allergic Conjunctivitis
Diunggah oleh
Endah Jona SariHak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Allergic Conjunctivitis
Diunggah oleh
Endah Jona SariHak Cipta:
Format Tersedia
Allergic Conjunctivitis &Vernal Keratoconjunctivitis
(VKC)
SIGNS AND SYMPTOMS
Itching and conjunctival injection are the two hallmarks of an allergic reaction. Also definitive is a lack of
palpable preauricular lymph nodes, since palpable preauricular nodes signify viral infection. The eyelids may
be swollen and red, and you may also see papillae of the palpebral conjunctiva. In most cases, patients
will report a history of seasonal or other allergies.
Seasonal allergies typically produce a thin, watery discharge and do not involve the cornea. If the patient
exhibits thick, ropy discharge with severe itching and corneal involvement, it is most likely VKC rather
than a seasonal allergy. VKCs prevalence is higher in the warmer climates. Onset is typically between the ages
of three and 25 years. Males are typically more affected than females.
The important clinical signs of VKC include large conjunctival papillae on the back of the superior
tarsus, Horner-Trantas dots (gelatinous, white clumps of degenerated eosinophils at the superior
limbus), areas of superficial punctate keratitis (SPK) and, in severe cases, well demarcated, sterile,
superiorly located corneal shield ulcers.
PATHOPHYSIOLOGY
An allergic response is an unwarranted over-reaction of the bodys immune system to foreign substances
known as allergens, which the body wrongly perceives as a potential threat. The response can be innate or
acquired. The presence of an allergen on the conjunctiva initiates two simultaneous immune responses,
one caused by the release of so-called pre-formed inflammatory mediators such as histamine from
mast cells, and the other by the production of arachidonic acid and its conversion into so-called newly-
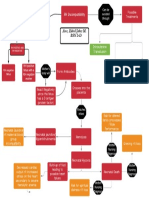
formed mediators such as prostaglandins (see Tracing the Complex Path of Allergic Reactions, on
next page). Pre-formed mediators are released immediately upon exposure; newly-formed mediators are
delayed roughly eight to 24 hours.
In mast cell degranulation, the allergen attracts and binds to an antibody known as immunoglobulin E
(abbreviated as IgE), then adheres to mast cells and causes them to degranulate, like a key opening a
lock. This discharges the pre-formed mediators. Their effects can be either direct, indirect or a
combination of the two.
Two important mediators released from mast cells, histamine and bradykinin, immediately begin to
stimulate nerve endings called nociceptors, creating the sensation of itching. Both also increase vascular
permeability and vasodilation; this causes the clinical signs of redness and conjunctival injection.
Meanwhile, other mediators released from mast cells send out chemical signals that attract both red and
white blood cells to the area. Once these cells arrive, they easily reach the conjunctival surface by moving
through the dilated and highly permeable capillaries.
The bodys other defense mechanism, referred to as the arachidonic acid cascade, produces three newly-
formed inflammatory mediatorsprostaglandins, thromboxanes and leukotrieneswhich are
collectively known as eicosanoids.
Virtually all cells contain a phospholipid layer within their cell walls. Any disruption or threat signals the cell
to convert phospholipids into arachidonic acid. When arachidonic acid interacts with two enzymes known as
cyclooxygenase and lipoxygenase, it is metabolized into eicosanoids. An allergens presence initiates the
arachidonic acid cascade both within conjunctival epithelial cells and also within mast cells as they degranulate.
Much like histamine and bradykinin, prostaglandins directly stimulate nerve endings to produce
sensations of itching and pain, and also increase vascular permeability and vasodilation. Leukotrienes
primarily attract macrophages (white blood cells).
MANAGEMENT
Management of both allergic conjunctivitis and VKC is primarily aimed at alleviating symptoms. The most
effective but least practical treatment is to prevent exposure to the allergen. Since this is not usually possible,
instruct patients to frequently use cold compresses, artificial tears and ointments to soothe, lubricate and wash
away the allergens. Also recommend that patients use a topical decongestant such as naphazoline or
phenylephrine as needed. These drugs cause vasoconstriction, retarding the release of the chemical
mediators into the tissues from the blood stream. This reduces hyperemia, chemosis and other
symptoms.
Mast cell stabilizers such as Alomide and Crolom help prevent the onset of allergic reactions by blocking
the adherence of the IgE-allergen compound to the mast cell. Treat patients with a history of recurrent
seasonal allergies using a mast cell stabilizer q.i.d. for four weeks in advance of allergy season. Patanol
(olopatadine 0.1%) combines mast cell stabilization with an antihistamine to offer therapy that is for both acute
and chronic symptoms. The effects last eight hours, allowing for b.i.d. rather than q.i.d. dosing.
In moderate to severe cases, recommend one or more of the following, used from two to four times per day as
needed: a topical medication such as Patanol or Livostin, oral antihistamines such as Benadryl, or a topical non-
steroidal anti-inflammatory drug (Acular, Voltaren or Profenal). In extremely symptomatic cases, use a topical
steroid such as Vexol, Flarex or Alrex q.i.d.
Only prostaglandins and thromboxanes are produced when cyclooxygenase interacts with arachidonic acid.
Leukotrienes, by contrast, are produced from the break-down of arachidonic by lipoxygenase. This leads to an
interesting distinction in anti-inflammatory treatment. Non-steroidal drugs prevent the formation of
cyclooxygenase but not lipoxygenase, thus they have virtually no effect on the production of leukotrienes. As a
result, non-steroidals are useful in reducing itching and conjunctival injection but not very helpful in ridding the
eye of excess immune cells. But because steroids inhibit the production of arachidonic acid itself, they reduce
the production of all three eicosanoids. This is why we must use steroids to treat any inflammatory conditions
characterized by a build-up of immune cells, such as chalazia, uveitis or corneal infiltrates.
VKC patients who present with shield ulcers also need aggressive cycloplegia (atropine 1%, homatropine 5%
or scopolamine 0.25%, b.i.d.) and a topical antibiotic (Tobrex, Ciloxan Ocuflox or Polytrim) q4-6h. To reduce
the interaction between the lid and cornea, provide a low-water content soft lens as a bandage lens. When the
corneal lesion has re-epithelialized, begin topical steroid therapy.
Newer anti-histamines, such as dual-action olopatadine hydrochloride 0.1% (Patanol) b.i.d. as well as
emedastine difumarate 0.5% (Emadine) q.i.d. have been seen to be very effective. A recently developed steroid,
loteprednol etabonate (Alrex) q.i.d. is specifically marketed for the management of allergic conjunctivitis.
CLINICAL PEARLS
Educate patients with a history of seasonal allergic conjunctivitis about how to avoid exposure to
substances that precipitate symptoms, and recommend prophylactic treatment with a mast cell
stabilizer. If effective, maintain this therapy for the duration of the season.
Follow-up with patients on non-steroidal medicines in one to two weeks after the start of therapy. See
patients on topical steroids no later than one week after the start of therapy, and monitor their IOP
routinely for the duration of the therapy. Re-examine patients treated for shield ulceration every one to
three days.
Mast cell degranulation only occurs in allergic reactions, but the arachidonic acid cascade occurs after
any threatening event, such as bacterial infection, surgery or accidental trauma.
Follow up with patients placed on topical medications after one week, with close monitoring thereafter
Anda mungkin juga menyukai
- Gluco TrackDokumen2 halamanGluco TrackEndah Jona SariBelum ada peringkat
- J Neurol Neurosurg Psychiatry 2013 Makin JNNP 2012 303645Dokumen9 halamanJ Neurol Neurosurg Psychiatry 2013 Makin JNNP 2012 303645Endah Jona SariBelum ada peringkat
- Skenario A Blok 16Dokumen4 halamanSkenario A Blok 16Endah Jona SariBelum ada peringkat
- Antibiotik Dan Analgetik Type of Infection Antibiotic of ChoiceDokumen4 halamanAntibiotik Dan Analgetik Type of Infection Antibiotic of ChoiceEndah Jona SariBelum ada peringkat
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDari EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifePenilaian: 4 dari 5 bintang4/5 (5782)
- Shoe Dog: A Memoir by the Creator of NikeDari EverandShoe Dog: A Memoir by the Creator of NikePenilaian: 4.5 dari 5 bintang4.5/5 (537)
- The Little Book of Hygge: Danish Secrets to Happy LivingDari EverandThe Little Book of Hygge: Danish Secrets to Happy LivingPenilaian: 3.5 dari 5 bintang3.5/5 (399)
- The Yellow House: A Memoir (2019 National Book Award Winner)Dari EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Penilaian: 4 dari 5 bintang4/5 (98)
- On Fire: The (Burning) Case for a Green New DealDari EverandOn Fire: The (Burning) Case for a Green New DealPenilaian: 4 dari 5 bintang4/5 (72)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDari EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RacePenilaian: 4 dari 5 bintang4/5 (890)
- The Emperor of All Maladies: A Biography of CancerDari EverandThe Emperor of All Maladies: A Biography of CancerPenilaian: 4.5 dari 5 bintang4.5/5 (271)
- Team of Rivals: The Political Genius of Abraham LincolnDari EverandTeam of Rivals: The Political Genius of Abraham LincolnPenilaian: 4.5 dari 5 bintang4.5/5 (234)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDari EverandNever Split the Difference: Negotiating As If Your Life Depended On ItPenilaian: 4.5 dari 5 bintang4.5/5 (838)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDari EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FuturePenilaian: 4.5 dari 5 bintang4.5/5 (474)
- Grit: The Power of Passion and PerseveranceDari EverandGrit: The Power of Passion and PerseverancePenilaian: 4 dari 5 bintang4/5 (587)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDari EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryPenilaian: 3.5 dari 5 bintang3.5/5 (231)
- Rise of ISIS: A Threat We Can't IgnoreDari EverandRise of ISIS: A Threat We Can't IgnorePenilaian: 3.5 dari 5 bintang3.5/5 (137)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDari EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaPenilaian: 4.5 dari 5 bintang4.5/5 (265)
- The Unwinding: An Inner History of the New AmericaDari EverandThe Unwinding: An Inner History of the New AmericaPenilaian: 4 dari 5 bintang4/5 (45)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDari EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersPenilaian: 4.5 dari 5 bintang4.5/5 (344)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDari EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyPenilaian: 3.5 dari 5 bintang3.5/5 (2219)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDari EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You ArePenilaian: 4 dari 5 bintang4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Dari EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Penilaian: 4.5 dari 5 bintang4.5/5 (119)
- Her Body and Other Parties: StoriesDari EverandHer Body and Other Parties: StoriesPenilaian: 4 dari 5 bintang4/5 (821)
- Moh731 TemplateDokumen2 halamanMoh731 TemplateSemeeeJuniorBelum ada peringkat
- The SARS-CoV-2 Genome, Its Variants and Their Various Way of ImmunizationDokumen7 halamanThe SARS-CoV-2 Genome, Its Variants and Their Various Way of ImmunizationInternational Journal of Innovative Science and Research TechnologyBelum ada peringkat
- HIV Book 2012-2013Dokumen761 halamanHIV Book 2012-2013Rodolfo Martinez100% (1)
- Basic Concept Map - RH IncompatibilityDokumen1 halamanBasic Concept Map - RH IncompatibilityTechnoShindoBelum ada peringkat
- Flow Cytometry Clearllab 10c Panel Marker Selection Whitepaper Including Case StudyDokumen8 halamanFlow Cytometry Clearllab 10c Panel Marker Selection Whitepaper Including Case StudyHam BoneBelum ada peringkat
- High Sensitivity CRP - IMMULITE and IMMULITE 1000 - Rev 06 DXDCM 09017fe980297730-1538194293759Dokumen36 halamanHigh Sensitivity CRP - IMMULITE and IMMULITE 1000 - Rev 06 DXDCM 09017fe980297730-1538194293759Deqsa Corporativo0% (1)
- 20 Mechanisms of Injury from COVID VaccinesDokumen2 halaman20 Mechanisms of Injury from COVID Vaccinespantufo100% (1)
- AB BIOINNOVATIONS, Inc. Announces A Ground-Breaking Alternative To AntibioticsDokumen2 halamanAB BIOINNOVATIONS, Inc. Announces A Ground-Breaking Alternative To AntibioticsPR.comBelum ada peringkat
- 3 Year Old With Persistent Cough Diagnosed With AsthmaDokumen1 halaman3 Year Old With Persistent Cough Diagnosed With AsthmaAngie MandeoyaBelum ada peringkat
- 18 ACVVR FinalDokumen58 halaman18 ACVVR FinalElison J PanggaloBelum ada peringkat
- Allergic Conjunctivitis in NigeriaDokumen5 halamanAllergic Conjunctivitis in NigeriaStephen OguntoyeBelum ada peringkat
- Igra PDFDokumen3 halamanIgra PDFDenada Florencia LeonaBelum ada peringkat
- Hematology Review Notes Dela Cruz TopicDokumen22 halamanHematology Review Notes Dela Cruz TopicShienna Rose Ann ManaloBelum ada peringkat
- Pemphigus Diseases ExplainedDokumen23 halamanPemphigus Diseases ExplainedPutkurBelum ada peringkat
- Chikungunya VirusDokumen11 halamanChikungunya VirusEvelyn Chacon JohnsonBelum ada peringkat
- Norsu Health Declaration Form 1 September 2022Dokumen1 halamanNorsu Health Declaration Form 1 September 2022Joshua Allen AjetoBelum ada peringkat
- Ophthalmia NeonatorumDokumen30 halamanOphthalmia NeonatorumManish ShresthaBelum ada peringkat
- VaccineDokumen72 halamanVaccineSiddharth Shekhar SinghBelum ada peringkat
- RadioimmunoassayDokumen35 halamanRadioimmunoassayRekha ChaudharyBelum ada peringkat
- 7 Medicine RheumatologyDokumen28 halaman7 Medicine RheumatologyAmitBelum ada peringkat
- HypersensitivityDokumen12 halamanHypersensitivityDwi TyoBelum ada peringkat
- Curative SARS-CoV-2 Test Results ReportDokumen1 halamanCurative SARS-CoV-2 Test Results ReportAxel BolanosBelum ada peringkat
- Harvard Medical School Controlling Your AllergiesDokumen57 halamanHarvard Medical School Controlling Your Allergiesjennieval100% (1)
- Transfusion Medicine Handbook Third Edition 2016Dokumen172 halamanTransfusion Medicine Handbook Third Edition 2016Nur Rahmat Wibowo100% (1)
- MD3 Immunology Final Exam ReviewDokumen28 halamanMD3 Immunology Final Exam Reviewdavid100% (1)
- RevalidaDokumen5 halamanRevalidaHawkins FletcherBelum ada peringkat
- EsplenomegaliaDokumen24 halamanEsplenomegaliaJhonatan Efraín López CarbajalBelum ada peringkat
- ArchRheumatol 32 21Dokumen5 halamanArchRheumatol 32 21indriBelum ada peringkat
- Role of Substance P Neuropeptide in Inflammation WDokumen12 halamanRole of Substance P Neuropeptide in Inflammation WGandhis Apri WidhayantiBelum ada peringkat
- Acute Poststreptococcal GlomerulonephritisDokumen69 halamanAcute Poststreptococcal GlomerulonephritisJirran CabatinganBelum ada peringkat