Acute Kidney Injury in ICU/CCM Board Review
Diunggah oleh
AzmachamberAzmacare0 penilaian0% menganggap dokumen ini bermanfaat (0 suara)
56 tayangan69 halamanCritical care Board review
Judul Asli
Acute Kidney Injury in ICU/CCM Board review
Hak Cipta
© © All Rights Reserved
Format Tersedia
PDF, TXT atau baca online dari Scribd
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniCritical care Board review
Hak Cipta:
© All Rights Reserved
Format Tersedia
Unduh sebagai PDF, TXT atau baca online dari Scribd
0 penilaian0% menganggap dokumen ini bermanfaat (0 suara)
56 tayangan69 halamanAcute Kidney Injury in ICU/CCM Board Review
Diunggah oleh
AzmachamberAzmacareCritical care Board review
Hak Cipta:
© All Rights Reserved
Format Tersedia
Unduh sebagai PDF, TXT atau baca online dari Scribd
Anda di halaman 1dari 69
Acute k|dney In[ury:
Lva|uanon and Management
naro|d M. Szer||p, MD IAC, ICC, IASN, INkI
Un|vers|ty of North 1exas nea|th Sc|ence Center
D|sc|osure
CranL SupporL:
SpecLral ulagnosucs, Lll Lllly
Cb[ecnves
Aer Lhls course, you wlll be able Lo:
! SLaLe Lhe consensus denluon of Akl
! ulscuss Lhe epldemlology of Akl
! Lxplaln Lhe morLallLy assoclaLed wlLh Akl
! ldenufy Lhe cause of Akl
! ApproprlaLely LreaL Akl
Acute k|dney In[ury: AkIN dehn|non
Added time frame " rise in creatinine 0.3 mg/dl over 48 hours
Less than 0.3 ml/kg/h
(Risk)
(Injury)
(Failure)
AkIN Cr|ter|a:
1hese crlLerla should be applled ln Lhe conLexL of Lhe
cllnlcal presenLauon and followlng adequaLe uld
resusclLauon when appllcable
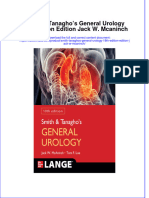
Dehn|ng AkI
120
40
80
0
GFR
(mL/min)
0 2 4 6 8
4
Days
2
0
6
Serum
Creatinine
(mg/dL)
Dehn|ng AkI
Biomarkers
Conceptua| Mode| for AkI
Complications
Normal
Increased
Risk
Damage GFR
Kidney
Failure
Death
Susceptibility
Staging
Age Volume Diabetes NSAID
Insult and Injury
Acute kena| Ia||ure
50%
Complete recovery No recovery
40%
10%
Acute Renal Failure
Death
50%
Function stable Function regresses
10% 90%
Incomplete Recovery
ESRD
Coca SG, et al Kid Intern. 2012; 81:242
CKD
ESRD
AkI: A ma[or cause of CkD
Lp|dem|o|ogy of AkI |n the ICU
13-70 lCu pauenLs develop Akl (Akln crlLerla)
lncldence ls lncreaslng
Plgher aculLy of lllness
lncreased recognluon
1-4 of pauenLs wlll requlre 881
Sepsls ls Lhe leadlng cause of Akl ln Lhe lCu
Morb|d|ty and Morta||ty of AkI
1he worse Lhe ln[ury Lhe longer Lhe lCu sLay
1he greaLer Lhe sLage Lhe worse of Lhe morLallLy
SLage 1 (8lsk) " 88 2.4
SLage 2 (ln[ury) " 88 4.13
SLage 3 (lallure) " 88 6.37
need for 881 " 44-33 morLallLy
Cllgurlc >> non-ollgurlc
1ranslenL lncreases (< 48 h) are assoclaLed wlLh
beuer ouLcomes
Prevention is best therapy
Morb|d|ty and Morta||ty of AkI
MorLallLy llkely skewed by Lhe overwhelmlng
predomlnance of A1n ln Lhe populauon
unclear lf rlses ln creaunlne from lnLersuual or
glomerular causes are assoclaLed wlLh slmllar
ouLcomes
1he greaLer Lhe amounL of volume overload Lhe
worse Lhe ouLcome
uesnon 1
A 36 year old 70 kg man ls admlued Lo Lhe lCu wlLh
resplraLory fallure secondary Lo pneumonla. Pe ls lnLubaLed.
8ecause of hypoLenslon unresponslve Lo lnLravenous ulds he
ls begun on noreplnephrlne uLraLed Lo keep hls MA > 63. Pls
creaunlne was 0.9 mg/dl on admlsslon Lo Lhe lCu. 24 hours
laLer hls creaunlne ls 1.3 mg/dl. Pe has made 400 cc of urlne.
WhaL ls Lhe sLage Akl does he have?
A. SLage 1
8. SLage 2
C. SLage 3
u. SLage 4
L. unable Lo deLermlne from daLa glven
AcuLe kldney
lnsumclency
Spurlous re-renal
8enal
(AcuLe kldney ln[ury)
osL-renal
volume depleuon
CPl
PepaLorenal syndrome
1ubules
ureLeral
8ladder ouLleL
Medlcauons
Assay lnLerference
8habdomyolysls
lmmunologlc
1hrombouc
Sepsls,Shock
1oxlns
Medlcauons
lnfecuons
AcuLe 1ubular
ln[ury
AcuLe
Clomerular
ln[ury
AcuLe
lnLersuual
ln[ury
k|dney In[ury:
0
10
20
30
40
50
Pre-renal Nephrotoxins Post-Op Multifactorial Reno-vascular Obstruction
Etiology
ATN
k|dney In[ury:
Approach to the panent
P&, charL revlew " look for clues Lo volume
sLaLus, sepsls, hearL fallure, nephroLoxlns
Make ow charL
urlnalysls, urlne chemlsLrles
8ule ouL obsLrucuon
8enal 8x when ln doubL
uesnon 2
A 64 year old woman ls admlued Lo Lhe lCu wlLh sepuc
shock. She requlres vasopressors Lo supporL her blood
pressure. She ls noLed Lo become ollgo-anurlc and on day
2 renal replacemenL Lherapy ls begun.
WhaL are Lhe chances LhaL she wlll be dlscharged wlLh
normal renal funcuon?
A. 80
8. 60
C. 40
u. 20
L. 0
k|dney In[ury: Autoregua|non
Shifted to
right in
patients with
sustained
hypertension
k|dney In[ury: re-rena|
n|story
hys|ca|
! CrLhosLasls
! ury mucous membranes
! llaL neck velns
! Skln Lenung
! vomlung
! ularrhea
! olyurla
! h/o CPl
k|dney In[ury: ILNa
lracuonal excreuon of a subsLance ls Lhe
percenLage of a freely lLered subsLance LhaL
appears ln Lhe urlne
1hus lL ls a measure of Lubular lnLegrlLy
ln volume depleuon Lhe kldney should be holdlng
on Lo sodlum lf Lhe Lubules are funcuonal -- lLna
< 1
ulmculL Lo lnLerpreL ln Lhe face of dlureucs,
mannlLol or ln polyurla
k|dney In[ury: ILNa
ulureucs:
lracuonal excreuon urea may be beuer marker
of pre-renal sLaLe (< 33)
Low lena can be seen ln conLrasL nephropaLhy
or sodlum avld sLaLes ln whlch sodlum LransporL
capaclLy of Lhe Lubule has been revved up.
U
Na
x V
P
Na
U
Creat
x V
P
Creat
k|dney In[ury
Pre-Renal Renal Failure
Management
! Intravascular volume repletion
! Crystalloid
AkI: nepato-rena| syndrome
LxLreme form of pre-renal fallure
Pepauc fallure (acuLe or chronlc)
AsclLes usually presenL
ullauon of splanchnlc vasculaLure (nC)
vasoconsLrlcuon of renal vessels (A2, endoLhelln)
AkI: nepato-rena| syndrome
8lslng creaunlne >1.3 (desplLe volume repleuon/
dlsconunuauon of dlureucs)
1ype 1 " rapld course
1ype 2 " chronlc course
< 30 88C/hpf -- < 300mg proLeln/24h
no oLher posslble cause
usually ollgurlc
usually low lL
na
Because of decreased muscle mass creatinine
usually low. Estimating equations often over
estimate GFR. Measure creatinine clearance
k|dney In[ury: Intr|ns|c
Acute Intrinsic Renal Failure
AIN ATN AGN
Medication
Post-infectious
Vasculitis
Sepsis
Toxins
Hypotension
k|dney In[ury:
A1N:k|sk Iactors
Acute Tubular Necrosis Risk factors
Volume depletion
Renal insufficiency
Elderly
Use of NSAIDs
Diabetes
k|dney In[ury: A1N
n|story
! renal Loxlns
lv conLrasL
amlnoglycosldes
rhabdomyolysls
amphoLerlcln
vancomycln
! hypoLenslon
! sepsls
Laboratory I|nd|ngs
! 8un/Creaunlne = 10:1
! urlne CsmolallLy =
lsoLhenurlc
! urlne Sodlum > 20 meq/L
! lena > 1
! urlnalysls " dlrLy brown
granular casLs, 81L cells
Rule out Volume depletion and obstruction
Perazella M A et al. CJASN 2010;5:402-408
2010 by American Society of Nephrology
k|dney In[ury: Ur|ne Sed|ment |n A1N
Renal Tubular Epithelial Cell
Muddy Granular Casts
k|dney In[ury
Acute Tubular Necrosis
Oliguric
Non-Oliguric
< 400 ml/day > 400 ml/day
Mortality greater with oliguria
Converting oliguric to non-oliguric kidney injury w/o benefit
Acute 1ubu|ar Necros|s
C||n|ca| Character|sncs
Characteristic Oliguric ATN Non-Oliguric ATN
Incidence 41% 59%
Toxin-induced 8% 30%
UV (ml/24h) < 400 1,280 + 75
U
Na
(mEq/L) 68 + 6 50 + 5
FE
Na
(%) 6.8 + 1.4 3.1 + 0.5
Dialysis required 84% 26%
Mortality 50% 25%
uesnon 3
A 72 year old man presenLs Lo Lhe emergency deparLmenL wlLh
abdomlnal paln, nausea and dluse foul smelllng dlarrhea for 2
days. Pe [usL compleLed a course of anubloucs for an upper
resplraLory lnfecuon. Cn exam he appears acuLely lll and has
marked abdomlnal Lenderness. uesplLe recelvlng 3 llLers of 0.9
naCl hls blood pressure ls 80/42mmPg and noreplnephrlne ls
sLarLed and he ls Lransferred Lo Lhe lCu. Pls urlne ouLpuL ls 20 cc/h
over Lhe nexL 3 hours.
Whlch of Lhe followlng would besL predlcL LhaL he wlll develop Akl?
A. granular casLs and renal Lubular cells on u/A
8. lena >1
C. elevaLed urlne nCAL
u. lacLaLe > 4 mmol/L
kena| Ia||ure |n the ICU
When should you obtain renal consult
Mehta RL et al. Am Med J 2002;113:456
Late consultation associated with lower creatinine and higher urine output
k|dney In[ury
Ischemic Acute Tubular Necrosis Time course
Creatinine plateaus 7-10 days
Polyuric phase 10-14 days
Recovery 14-21 days
khabdomyo|ys|s
llndlngs
Muscle Lenderness
Ck
Pyperkalemla
PyperphosphaLemla
Pypocalcemla
Pypercalcemla
(recovery)
urlne dlp posluve for
blood
Muscle ln[ury
1raumauc ln[ury
ressure ln[ury (drug Cu)
Cver-exeruon
Pyperpyrexla
1oxln
Alcohol
Cocalne
SLauns
vlral/8acLerlal
lnammaLory
MeLabollc
Pypokalemla
PypophosphaLemla
1hyrold dlsease
khabdomyo|ys|s: treatment
0.9 sallne (Lhe earller Lhe beuer)
naPCC
3
(?)
AkI: Intra-abdom|na| hypertens|on
lncreaslngly recognlzed ln lCu semng
osL abdomlnal surgery
1rauma
8urns
lschemlc bowel
ancreauus
Masslve asclLes
Intra-abdominal Pressure (IAP)
! Intravesicular pressure
! Measured in mm Hg at end expiration
! Supine position
! Transducer zeroed at mid-axillary line
! Absence of muscle contraction
Grade 1: IAP 12-15 mm Hg
Grade 2: IAP 16-20 mm Hg
Grade 3: IAP 21-25 mm Hg
Grade 4: IAP > 25 mm Hg
Ventilatory difficulty
AKI
Gut ischemia
kad|ocontrast Nephropathy: k|sk Iactors
auenL 8elaLed
reexlsung renal lnsumclency
ulabeLes melllLus
lnLravascular volume depleuon
8educed cardlac ouLpuL
ConcomlLanL nephroLoxlns (nSAlus)
rocedure relaLed
lncreased dose of radloconLrasL
Muluple procedures wlLhln 72 hours
lnLra-arLerlal admlnlsLrauon
1ype of radloconLrasL
red|cnon Score for CIN
Mehran R et al. J Am Coll Cardiol. 51:1419, 2006
Acute k|dney In[ury:
kad|ocontrast Nephropathy
Time Course
Creatinine rises in 24-48 h
Peaks in 5 days
Recovery begins 5-7 days
Distinguish from cholesterol emboli
revennon of Acute kena| Ia||ure:
kad|ocontrast Nephropathy
# Avoid contrast when possible
# Stop NSAID
# ? D/C ACE/ARB
# Use low/iso-osmolar contrast
# IV saline/bicarbonate cautiously
# Limit dose of contrast
# ? Acetylcysteine (cant hurt)
kena| Ia||ure: management
Management of Acute Renal Failure
Remove all offending agents
Avoid hyperkalemia
Avoid Volume overload
Post-hoc analysis of FACTT trial showed
that positive fluid balance worsened outcomes
Dose all meds appropriately
? High protein diet
Renal replacement therapy
kena| Ia||ure |n the ICU:
1|m|ng of rena| rep|acement therapy
Whlle Lhere ls lncreaslng recognluon of Lhe value of
earller dlalysls, Lhe publlshed consensus, and Lhe
pracuce ln many cenLers aL presenL, ls sull Lo apply
dlalysls Lo relauvely lll raLher Lhan Lo relauvely
healLhy pauenLs.
Teschan PE et al: Ann Int Med 1960;53:992
Ind|canons for Acute nemod|a|ys|s
uremla (sympLomauc azoLemla)
nausea/vomlung
Change ln menLal sLaLus
Selzures
erlcardlus
Pyperkalemla
MeLabollc acldosls
volume overload
Not treatable by
medical means
These are complications
of kidney injury
Lar|y vs Late Intervennon:
No well-powered randomized controlled trials
The VA/NIH Acute Renal Failure Trial Network. N Engl J Med 2008;10.1056/NEJM
Renal Failure in the ICU:
Intensive Vs Conventional Therapy
Renal Failure in the ICU:
Intensive Vs Conventional Therapy
Survival
Inadequate Adequate
kk1: Connnuous moda||nes
CvvP ---- hemolLrauon (convecuve clearance)
CvvPu -- hemodlalysls (dluslve clearance)
CvvPu - hemodlalLrauon
SLLu (Pybrld) SusLalned low emclency dlalysls
Major advantage of continuous modalities is
the ability to remove excess volume
Interm|uent vs Connnuous 1herapy
Time
Ckk1 Vs InD
Bagshaw SM et al. Crit Care Med 36:610, 2008
kena| Ia||ure:
Acute Intersnna| Nephr|ns
urug lnduced
lnfecuons
MallgnanL cell lnvaslon
Sarcold
Collagen vascular dlsease
ldlopaLhlc
kena| Ia||ure:
Acute Intersnna| Nephr|ns
!-lactams NSAIDs
Fever,Rash, Eosinophilia 80 % 19 %
Eosinophiluria
83 % 13 %
Duration of drug
2-60 days Days-months
Nephrotic syndrome
< 1 % 83 %
Most common agent
Methicillin Fenoprofen
kena| Ia||ure:
Acute Intersnna| Nephr|ns
ulagnosls
Classlc 1rlad
8ecognlzed oendlng agenL
usually requlres renal 8x
kena| Ia||ure:
Acute Intersnna| Nephr|ns
Urinary Eosinophils: Wrights stain
kena| Ia||ure:
Acute Intersnna| Nephr|ns
1reaLmenL
SLop oendlng agenL
ulalysls
SLerolds
uesnon 4
A 24 y/o lv drug abuser presenLs wlLh fever and
hypoLenslon. Pe ls admlued Lo Lhe lCu wlLh a dlagnosls
of sepuc shock. Pe ls sLarLed on anubloucs and
vasopressors. Pls urlne ouLpuL ls 10 cc/h and hls
creaunlne ls rlslng.
Whlch of Lhe followlng has been shown Lo lmprove
ouLcome?
A. AdmlnlsLrauon of hlgh dose loop dlureuc
8. nephrology consulLauon
C. lnluauon of early dlalysls
u. ually lnLermluenL dlalysls
L. Conunuous dlalysls
kena| Ia||ure:
kena| Vascu|ar D|sease
vacullus
11 (8x "plasmapheresls)
PuS (e. coll) (8x "?ecullzamab)
ulC
Scleroderma (LreaL wlLh ACL-l)
re-eclampsla
MallgnanL hyperLenslon
CholesLerol emboll
Thrombotic
microangiopathy
kena| Ia||ure:
Acute G|omeru|onephr|ns
vascullus
osL lnfecuous
Collagen vascular dlsease
AnCA posluve vasculludes
Wegeners (CranulomaLosls wlLh polyangllus)
Mlcroscoplc olyarLerlus
CoodpasLeurs syndrome
kena| Ia||ure:
Acute G|omeru|onephr|ns
LaboraLory analysls
! 8un:Creaunlne 10:1
! urlne CsmolallLy > 300 mosm/kg
! urlne na < 10 meq/L
! urlnalysls
! 88Cs (dysmorphlc)/88C casLs
! roLelnurla
ked 8|ood Ce|| Cast
Dysmorph|c ked 8|ood Ce||s
kena| Ia||ure
Post-renal Renal Failure: etiology
Intratubular
! crystals (urate, acyclovir, indinavir, methotrexate)
! proteins (myeloma)
Extrarenal
! ureter (single kidney or bilateral)
! stone
! papilla, tumor
! Bladder
! Urethra
kena| Ia||ure: tubu|ar obstrucnon
AcuLe uraLe nephropaLhy (Lumor lysls)
reclplLauon of urlc acld ln Lhe Lubules
Leukemlas/lymphomas (usually posL Lherapy)
reLreaL wlLh allopurlnol/rasburlcase (alkallnlzauon)
8asburlcase/ulds /loop dlureucs/881
MeLhoLrexaLe
Clucarpldase/ulds
kena| Ia||ure: tubu|ar obstrucnon
Urate deposition in collecting ducts
kena| Ia||ure
Post-renal Renal Failure
History
Very young
Elderly males
History single kidney
History pelvic or intraabdominal cancer
Leukemia/lymphoma
Anuria or frequent small volumes
kena| Ia||ure
Post-renal Renal Failure -- Dx
Renal Ultarsound
kena| Ia||ure
Post-renal Renal Failure -- Treatment
Foley catheter
Ureteral stents
Antegrade nephrostomy tubes
Summary
Akl ln Lhe lCu
8ule ouL pre-renal and posL-renal causes
lncreases morLallLy
lrequenL cause of Cku
Sepsls ls commonesL cause
uose all drugs approprlaLely
Larly renal consulLauon
8enal replacemenL
Larly LreaLmenL may be beuer
no role for lnLenslve LreaLmenL
no beneL C881 over lPu
revennon |s best po||cy
uesnons
Anda mungkin juga menyukai
- Quality Safety Complications/Pulmonary Board ReviewDokumen135 halamanQuality Safety Complications/Pulmonary Board ReviewAzmachamberAzmacareBelum ada peringkat
- HAP/Pulmonary Board ReviewDokumen80 halamanHAP/Pulmonary Board ReviewAzmachamberAzmacareBelum ada peringkat
- Acid Base Disorders/Pulmonary Board ReviewDokumen75 halamanAcid Base Disorders/Pulmonary Board ReviewAzmachamberAzmacareBelum ada peringkat
- Bronch IP/Pulmonary Board ReviewDokumen73 halamanBronch IP/Pulmonary Board ReviewAzmachamberAzmacareBelum ada peringkat
- CAP/Pulmonary Board ReviewDokumen64 halamanCAP/Pulmonary Board ReviewAzmachamberAzmacareBelum ada peringkat
- Mycobacterium/Pulmonary Board ReviewDokumen59 halamanMycobacterium/Pulmonary Board ReviewAzmachamberAzmacareBelum ada peringkat
- SEEK/Pulmonary Board ReviewDokumen101 halamanSEEK/Pulmonary Board ReviewAzmachamberAzmacare100% (1)
- Unusual Lung Infect Bronch & CF/Pulmonary Board ReviewDokumen87 halamanUnusual Lung Infect Bronch & CF/Pulmonary Board ReviewAzmachamberAzmacareBelum ada peringkat
- Cellular Biology and Immunology/Pulmonary Board ReviewDokumen68 halamanCellular Biology and Immunology/Pulmonary Board ReviewAzmachamberAzmacareBelum ada peringkat
- Thromboembolic Disease/Pulmonary Board ReviewDokumen60 halamanThromboembolic Disease/Pulmonary Board ReviewAzmachamberAzmacareBelum ada peringkat
- Pulmonary Hypertension/Pulmonary Board ReviewDokumen66 halamanPulmonary Hypertension/Pulmonary Board ReviewAzmachamberAzmacareBelum ada peringkat
- Vasculitis & Alveolar Hemorrhage/Pulmonary Board ReviewDokumen62 halamanVasculitis & Alveolar Hemorrhage/Pulmonary Board ReviewAzmachamberAzmacareBelum ada peringkat
- COPD - I/Pulmonary Board ReviewDokumen68 halamanCOPD - I/Pulmonary Board ReviewAzmachamberAzmacare100% (1)
- Asthma/Pulmonary Board ReviewDokumen66 halamanAsthma/Pulmonary Board ReviewAzmachamberAzmacareBelum ada peringkat
- Unusual and Uncommon Pulmonary Disorder/pulmonary Board ReviewDokumen68 halamanUnusual and Uncommon Pulmonary Disorder/pulmonary Board ReviewAzmachamberAzmacareBelum ada peringkat
- Mediastinal & Other Neoplasms/Pulmonary Board ReviewDokumen86 halamanMediastinal & Other Neoplasms/Pulmonary Board ReviewAzmachamberAzmacareBelum ada peringkat
- Diffues Lung Disease I/Pulmonary DBoard ReviewDokumen184 halamanDiffues Lung Disease I/Pulmonary DBoard ReviewAzmachamberAzmacare100% (1)
- SEEK/Pulmonary Board ReviewDokumen102 halamanSEEK/Pulmonary Board ReviewAzmachamberAzmacare100% (2)
- Copd /pulmonary Board ReviewDokumen68 halamanCopd /pulmonary Board ReviewAzmachamberAzmacareBelum ada peringkat
- Diffuse Lung Disease II/Pulmonary Board ReviewDokumen181 halamanDiffuse Lung Disease II/Pulmonary Board ReviewAzmachamberAzmacareBelum ada peringkat
- Sleep Science Polysomnography/Pulmonary Board ReviewDokumen154 halamanSleep Science Polysomnography/Pulmonary Board ReviewAzmachamberAzmacareBelum ada peringkat
- Sleep Disorders - I/Pulmonary Board ReviewDokumen87 halamanSleep Disorders - I/Pulmonary Board ReviewAzmachamberAzmacareBelum ada peringkat
- Sleep Disorders II/Pulmonary Board ReviewDokumen106 halamanSleep Disorders II/Pulmonary Board ReviewAzmachamberAzmacareBelum ada peringkat
- SEEK/Pulmonary Board ReviewDokumen34 halamanSEEK/Pulmonary Board ReviewAzmachamberAzmacareBelum ada peringkat
- Exercise Testing/Pulmonary Board ReviewDokumen42 halamanExercise Testing/Pulmonary Board ReviewAzmachamberAzmacareBelum ada peringkat
- Pleural Diseases I & II/Pulmonary Board ReviewDokumen181 halamanPleural Diseases I & II/Pulmonary Board ReviewAzmachamberAzmacareBelum ada peringkat
- Ethics/Pulmonary Board ReviewDokumen43 halamanEthics/Pulmonary Board ReviewAzmachamberAzmacareBelum ada peringkat
- Women's Issues in Pulmonary Medicine/Pulmonary Board ReviewDokumen67 halamanWomen's Issues in Pulmonary Medicine/Pulmonary Board ReviewAzmachamberAzmacareBelum ada peringkat
- Eosinophilic Lung Disease/Pulmonary Board ReviewDokumen51 halamanEosinophilic Lung Disease/Pulmonary Board ReviewAzmachamberAzmacareBelum ada peringkat
- PFT Excercise Testing Case Studies/pulmonary Board ReviewDokumen64 halamanPFT Excercise Testing Case Studies/pulmonary Board ReviewAzmachamberAzmacareBelum ada peringkat
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDari EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifePenilaian: 4 dari 5 bintang4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingDari EverandThe Little Book of Hygge: Danish Secrets to Happy LivingPenilaian: 3.5 dari 5 bintang3.5/5 (400)
- Shoe Dog: A Memoir by the Creator of NikeDari EverandShoe Dog: A Memoir by the Creator of NikePenilaian: 4.5 dari 5 bintang4.5/5 (537)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDari EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RacePenilaian: 4 dari 5 bintang4/5 (895)
- The Yellow House: A Memoir (2019 National Book Award Winner)Dari EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Penilaian: 4 dari 5 bintang4/5 (98)
- The Emperor of All Maladies: A Biography of CancerDari EverandThe Emperor of All Maladies: A Biography of CancerPenilaian: 4.5 dari 5 bintang4.5/5 (271)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDari EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryPenilaian: 3.5 dari 5 bintang3.5/5 (231)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDari EverandNever Split the Difference: Negotiating As If Your Life Depended On ItPenilaian: 4.5 dari 5 bintang4.5/5 (838)
- Grit: The Power of Passion and PerseveranceDari EverandGrit: The Power of Passion and PerseverancePenilaian: 4 dari 5 bintang4/5 (588)
- On Fire: The (Burning) Case for a Green New DealDari EverandOn Fire: The (Burning) Case for a Green New DealPenilaian: 4 dari 5 bintang4/5 (74)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDari EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FuturePenilaian: 4.5 dari 5 bintang4.5/5 (474)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDari EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaPenilaian: 4.5 dari 5 bintang4.5/5 (266)
- The Unwinding: An Inner History of the New AmericaDari EverandThe Unwinding: An Inner History of the New AmericaPenilaian: 4 dari 5 bintang4/5 (45)
- Team of Rivals: The Political Genius of Abraham LincolnDari EverandTeam of Rivals: The Political Genius of Abraham LincolnPenilaian: 4.5 dari 5 bintang4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDari EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyPenilaian: 3.5 dari 5 bintang3.5/5 (2259)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDari EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You ArePenilaian: 4 dari 5 bintang4/5 (1090)
- Rise of ISIS: A Threat We Can't IgnoreDari EverandRise of ISIS: A Threat We Can't IgnorePenilaian: 3.5 dari 5 bintang3.5/5 (137)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDari EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersPenilaian: 4.5 dari 5 bintang4.5/5 (344)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Dari EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Penilaian: 4.5 dari 5 bintang4.5/5 (121)
- Her Body and Other Parties: StoriesDari EverandHer Body and Other Parties: StoriesPenilaian: 4 dari 5 bintang4/5 (821)
- Lab 8 Bi309Dokumen8 halamanLab 8 Bi309SanahKumarBelum ada peringkat
- Basuki B Purnomo Department of Urology Medical School Brawijaya University/Saiful Anwar Hospital MalangDokumen44 halamanBasuki B Purnomo Department of Urology Medical School Brawijaya University/Saiful Anwar Hospital MalangChangi RenandaBelum ada peringkat
- HematuriaDokumen24 halamanHematuriaHawania IIBelum ada peringkat
- Sistem Perkemihan: Indargairi Universitas Mega RezkyDokumen46 halamanSistem Perkemihan: Indargairi Universitas Mega RezkyMaria GabrielaBelum ada peringkat
- Excretion MCQ Assignment: Also Visit Us At: Also Visit Us atDokumen3 halamanExcretion MCQ Assignment: Also Visit Us At: Also Visit Us atPriyanshu YadavBelum ada peringkat
- Audit October 2020Dokumen23 halamanAudit October 2020shyaka jean claudeBelum ada peringkat
- 00 NephrologyDokumen98 halaman00 Nephrologyeryxsp0% (1)
- Lecture Urinary System of AnimalsDokumen38 halamanLecture Urinary System of Animals1kshitiz ThakurBelum ada peringkat
- AUBFDokumen32 halamanAUBFAndrei Tumarong AngoluanBelum ada peringkat
- Urinary SystemDokumen99 halamanUrinary SystemHarshika KDGBelum ada peringkat
- Anatomy and Physiology NotesDokumen4 halamanAnatomy and Physiology NotesTristan Arambulo100% (1)
- Handout Finals AnaphyDokumen26 halamanHandout Finals AnaphyALEXANDRA SAN PEDROBelum ada peringkat
- Applied Nutrition: Nutritional Consideration in The Prevention and Management of Renal Disease - VIIDokumen28 halamanApplied Nutrition: Nutritional Consideration in The Prevention and Management of Renal Disease - VIIHira KhanBelum ada peringkat
- Smith Tanaghos General Urology 19Th Edition Edition Jack W Mcaninch Full Download ChapterDokumen38 halamanSmith Tanaghos General Urology 19Th Edition Edition Jack W Mcaninch Full Download Chapterjeffrey.dunaway695100% (6)
- LANGMANS Chapter 15 Development of The Urinary SystemDokumen3 halamanLANGMANS Chapter 15 Development of The Urinary SystemMerryl BastilloBelum ada peringkat
- Chapter 26Dokumen7 halamanChapter 26jess waldenBelum ada peringkat
- Nursing Care PlanDokumen2 halamanNursing Care Planmjoie_baby6568470100% (6)
- Urology HydronephrosisDokumen31 halamanUrology Hydronephrosisaarm1990100% (1)
- Obstructive Uropathy 2Dokumen10 halamanObstructive Uropathy 2jollyannealonzoBelum ada peringkat
- Gambaran Anatomi Dan Histologi Ginjal Dan Vesika Urinaria PADA MUSANG LUWAK (Paradoxurus Hermaphroditus) DI PULAU TIMORDokumen11 halamanGambaran Anatomi Dan Histologi Ginjal Dan Vesika Urinaria PADA MUSANG LUWAK (Paradoxurus Hermaphroditus) DI PULAU TIMORSaadatulBelum ada peringkat
- (Mebooksfree Net) Oxf&tex&uro&sur&1stDokumen1.201 halaman(Mebooksfree Net) Oxf&tex&uro&sur&1stMohammadSAL-Rawashdeh100% (2)
- Kidney Stones - K.S. GopiDokumen4 halamanKidney Stones - K.S. GopiMahmood MuftiBelum ada peringkat
- Overview of RENAL: Dr. Wilson Arthur Zein, M. BiomedDokumen34 halamanOverview of RENAL: Dr. Wilson Arthur Zein, M. BiomedAnnisBelum ada peringkat
- Urine AnalysisDokumen69 halamanUrine AnalysisAffan ElahiBelum ada peringkat
- ACVR and ECVDI Consensus Statement For The Standardization of The AbdominalDokumen14 halamanACVR and ECVDI Consensus Statement For The Standardization of The AbdominalErick RamosBelum ada peringkat
- Urinary Tract Infection UTI and Dementia FactsheetDokumen10 halamanUrinary Tract Infection UTI and Dementia FactsheettoobaziBelum ada peringkat
- GGK PKMRS PugerDokumen12 halamanGGK PKMRS Pugersyamsul arifinBelum ada peringkat
- NephrologyDokumen7 halamanNephrologyYT ShortsBelum ada peringkat
- Stones, Urinary Stones or Renal Calculi. As Aforementioned, It Is Quite Vague andDokumen4 halamanStones, Urinary Stones or Renal Calculi. As Aforementioned, It Is Quite Vague andChristian Salunga SangalangBelum ada peringkat
- URINARY TRACT INFECTION - FinalDokumen86 halamanURINARY TRACT INFECTION - FinalShreyance Parakh100% (2)