Bronchiolitislast Edited
Diunggah oleh
regarskid0 penilaian0% menganggap dokumen ini bermanfaat (0 suara)
24 tayangan14 halamanBronchiolitislast Edited
Hak Cipta
© © All Rights Reserved
Format Tersedia
DOCX, PDF, TXT atau baca online dari Scribd
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniBronchiolitislast Edited
Hak Cipta:
© All Rights Reserved
Format Tersedia
Unduh sebagai DOCX, PDF, TXT atau baca online dari Scribd
0 penilaian0% menganggap dokumen ini bermanfaat (0 suara)
24 tayangan14 halamanBronchiolitislast Edited
Diunggah oleh
regarskidBronchiolitislast Edited
Hak Cipta:
© All Rights Reserved
Format Tersedia
Unduh sebagai DOCX, PDF, TXT atau baca online dari Scribd
Anda di halaman 1dari 14
BRONCHIOLITIS
Presentators : Febi Putri Lestari and Maulida Septianita
Day, Date : Tuesday, March 26
th
2013
Supervisor : dr. Wisman Dalimunthe, Sp.A(K)
CHAPTER 1
INTRODUCTION
1.1. Background
Bronchiolitis is an infection of the bronchioles, the small air passages in the lungs, it
is common in children less than 2 years of age and is the leading cause of serious lower
respiratory illness in infants.
1
Bronchiolitis occurs in association with viral infections (Respiratory Syncytial Virus;
RSV, in around 75% of cases) and is seasonal, with peak prevalence in the winter months
(November to March) when such viruses are widespread in the community. Hayden reported
that RSV infection causes bronchiolitis around 45%-90% and causes pneumonia around
40%.
2
Re-infection during a single season is possible. Children with underlying medical
problems (prematurity, cardiac disease or underlying respiratory disease) are more
susceptible to severe disease and so have higher rates of hospitalisation. In preterm infants
less than six months of age, admission rate with acute bronchiolitis is 6.9% with admission to
intensive care more frequent in such patients.
3
Twenty percent of infants with bronchiolitis (40-50% of those hospitalised) proceed
to a grumbling, sometimes protracted, respiratory syndrome of persistent cough and recurrent
viral induced wheeze. Ongoing symptoms may relate to continuing inflammation and
temporary cilial dysfunction. An association between acute bronchiolitis and later respiratory
morbidity is recognized.
3
According to the World Health Organization bulletin,
an estimated 150 million new
cases occur annually; 11-20 million (7-13%) of these cases are severe enough to require
hospital admission. Worldwide, 95% of all cases occur in developing countries.
4
1.2. Objective
The aim of this study is to explore more about the theoritical aspects on
bronchiolitis, and to integrate the theory and application of bronchiolitis case in daily
life.
CHAPTER 2
LITERATURE REVIEW
2.1. Definition
Bronchiolitis is a viral lower respiratory tract infection (VlRI) in a child <24 months
of age, it is characterized by acute inflammation, edema and necrosis of epithelial cells lining
small airways, increased mucus production, and bronchospasm. Signs and symptoms such as
rhinitis, tachypnea, wheezing, cough, crackles, use of accessory muscles, and/or nasal
flaring.
5
The authors of University of Nottingham study derived a consensus definition of a
seasonal viral illness characterized by fever, nasal discharge, and dry, wheezy cough. On
examination there are fine inspiratory crackles and/or high-pitched expiratory wheeze.
7
2.2. Etiology
Most cases of bronchiolitis result from a viral pathogen, such as Respiratory Syncytial
virus (RSV), parainfluenza virus, influenza virus, or adenovirus. The virus that causes it is
spread from person to person through direct contact with nasal secretions, airborne droplets,
and fomites.
4
These droplets are transmitted to hands and fingers, and self inoculation then
occurs with transmission of virus into the eyes or nose, which act us portals to the respiratory
tract.
11
RSV is the most commonly isolated agent in 75% of children younger than 2 years
who are hospitalized for bronchiolitis.
4
Human metapneumovirus (hMPV) is thought to be
the next most common cause of bronchiolitis. Some severe cases of bronchiolitis have also
been reported associated with co-infection of hMPV with RSV.
1
RSV incubation period
before the onset of symptoms appears to be in the range of 3 to 8 days.
11
The viral shedding
in nasal secretions continues for 6-21 days after symptoms develop.
4
RSV continues to be
shed from the respiratory tract for an average of 9 days in children younger than 1 year of
age. Among infants infected with human immunodeficiency virus, RSV is shed for a median
of 30 days.
10
In general, only infant older than 1 month develop the clinical syndrome of
bronchiolitis.
10
Nearly 70% of infants are infected in their first year of life and about half of
these children are re-infected in the next season. Throughout life everyone is re-infected
multiple times. It has been shown in experimental settings, when human volunteers were re-
infected multiple times with the same virus strain (at short time intervals of 4, 8, 14, 20 and
26 months), that each challenge resulted in infection in at least one fourth of the subjects. Re-
infection occurred despite the presence of high levels of neutralizing antibodies. This clearly
demonstrates that immune memory established during natural infection is incomplete.
6
RSV causes yearly epidemics of respiratory disease during the winter season in
moderate climates and during the wet season in tropical regions. RSV infections widely vary
in disease severity, causing a broad range of symptoms varying from a mild cold to severe
lower respiratory tract (LRT) disease. About 3% of infants that are infected with RSV require
hospitalization, mostly due to respiratory failure or feeding problems.
6
Risk factor for the development of bronchiolitis include low levels of antibodies in
cord blood, gender, birth month, absence of or minimal breastfeeding, crowded living
conditions, being a twin or triplet, and low socioeconomic status.
10
Premature (gestational
age less than 37 weeks), low birth weight, age under 12 weeks, congenital heart disease,
chronic lung disease (cystic fibrosis, bronchopulmonary dysplasia and underlying lung
anomalies), immunocompromised state, and congenital or anatomical defects of the airway
are risk factors for severe disease.
1
Age is a significant factor in the severity of infection: The younger the patient is, the
more severe the infection tends to be, as measured by the lowest oxygen saturation. Infants
younger than 6 months are most severely affected, owing to their smaller, more easily
obstructed airways and their decreased ability to clear secretions.
4
Intrauterine cigarette-smoke exposure may impair in utero airway development or
alter the elastic properties of the lung tissue. Second-hand cigarette smoke (eg, by a parent or
family member) in the postnatal period compounds the severity of RSV bronchiolitis in
infants.
4
2.3. Epidemiology
According to the World Health Organization bulletin,
an estimated 150 million new
cases occur annually; 11-20 million (7-13%) of these cases are severe enough to require
hospital admission. Worldwide, 95% of all cases occur in developing countries.
4
Among
infants hospitalized for 1 week, 45% become infected, and infection is related to the duration
of hospitalization.
10
About 3% of all infants less than a year old are admitted to hospital with
bronchiolitis.
3
About 75% of cases of bronchiolitis occur in children younger than 1 year and 95% in
children younger than 2 years. Incidence peaks in those aged 2-8 months.
4
In large urban
populations, the peak age incidence of RSV bronchiolitis is at 2 months; in more rural setting
it often appears later.
10
Infants younger than 6 months are most severely affected, owing to
their smaller, more easily obstructed airways and their decreased ability to clear secretions.
4
Bronchiolitis occurs as much as 1.25 times more frequently in males than in females;
the exact reason for this difference is unknown.
Death is 1.5 times more likely in males. Race
and low socioeconomic status may adversely affect outcome in patients with acute
bronchiolitis. In one study,RSV bronchiolitis seemed to be more severe in white children than
in black children.
4
2.4. Pathogenesis and Pathophysiology
Bronchioles are small airways (< 2 mm in diameter) and lack cartilage and submucosal
glands. The terminal bronchiole, a 16th-generation airway, is the final conducting airway that
terminates in the respiratory bronchioles. The acinus (ie, the gas exchange unit of the lung)
consists of respiratory bronchioles, the alveolar duct, and alveoli. The bronchiolar lining
consists of surfactant-secreting Clara cells and neuroendocrine cells, which are the source of
bioactive products such as somatostatin, endothelin, and serotonin.
4
Bronchiolar injury and the consequent interplay between inflammatory and
mesenchymal cells can lead to diverse pathologic and clinical syndromes. The effects of
bronchiolar injury include the following increased mucus secretion, bronchial obstruction and
constriction, alveolar cell death, mucus debris, viral invasion, air trapping, atelectasis,
reduced ventilation that leads to ventilation-perfusion mismatch, labored breathing.
4
Complex immunologic mechanisms play a role in the pathogenesis of bronchiolitis.
Type 1 allergic reactions mediated by immunoglobulin E (IgE) may account for some
clinically significant bronchiolitis. Infants who are breastfed with colostrum rich in
immunoglobulin A (IgA) appear to be relatively protected from bronchiolitis. Necrosis of the
respiratory epithelium is one of the earliest lesions in bronchiolitis and occurs within 24 hours
of acquisition of infection. Cytokines and chemokines, released by infected respiratory
epithelial cells, amplify the immune response by increasing cellular recruitment into infected
airways. Interferon and interleukin (IL)4, IL-8, and IL-9 are found in high concentrations in
respiratory secretions of infected patients.
4
Proliferation of goblet cells results in excessive mucus production, whereas epithelial
regeneration with nonciliated cells impairs elimination of secretions. Lymphocytic infiltration
may result in submucosal edema.
4
As a result of the edema of the airway wall and the
accumulation of mucus and cellular debris, many peripheral airways are narrowed, and some
are partially and other total occluded.
10
Airway obstruction was due to epithelial and inflammatory cell debris mixed with
fibrin, mucus, and edema fluid but not to bronchial smooth muscle constriction. Smooth
muscle constriction appears to have little role in the pathogenic process, which may explain
the limited benefit from bronchodilator therapy observed in some clinical trials.
4
The mechanics of respiration are abnormal. The infant breathes at high lung volume,
and resting end expiratory lung volume (functional residual capacity) is elevated. Dynamic
compliance is decreased, in part because the infant is breathing at higher lung volume and
hence on a stiffer portion of the volume-pressure curve of the lung, and in part because of the
uneven distribution of resistances within the lung. The decrease in compliance and increase in
resistant result in increases work of breathing. Serious alteration in gas exchange occur as a
result of the airway obstruction and patchy distribution of atelectasis. Arterial hypoxemia
develops as a result of mismatching of pulmonary ventilation and perfussion.
10
Infants are affected most often because of their small airways, high closing volumes,
and insufficient collateral ventilation. Recovery begins with regeneration of bronchiolar
epithelium after 3-4 days; however, cilia do not appear for as long as 2 weeks. Mucus plugs
are predominantly removed by macrophages.
4
2.5. Diagnosis
The diagnosis of bronchiolitis is based on clinical presentation, the patients age, seasonal
occurrence, and findings from the physical examination. When all of these are consistent with
the expected diagnosis of bronchiolitis, few laboratory studies are necessary.
Tests are
typically used to exclude other diagnoses (eg, bacterial pneumonia, sepsis, or congestive
heart failure) or to confirm a viral etiology and determine required infection control for
patients admitted to the hospital. Severely ill children may have dual viral infections.
4
The diagnosis should be suspected in any infant under the age of 2 years who presents
with nasal discharge and wheezy cough in the presence of fine inspiratory crackles and/or
high-pitched expiratory wheeze, even in the absence of fever.
1
Bronchiolitis typically has a coryzal phase for two to three days which precedes the
onset of other symptoms. In the first 72 hours of the illness, infants with bronchiolitis may
deteriorate clinically before symptom improvement.
Infants younger than 1 month may
present as hypothermic.
4
Severe cases progress to respiratory distress with poor feeding,
lethargy, history of apnoea, tachypnea, nasal flaring, retractions, cyanosis, oxygen saturation
94% or less.
1
Table 1. Assessment of severity bronchiolitis
Mild Moderate Severe
Respiratory
Rate
Normal to slightly
increased
Increased Markedly increased RR>
70 (<6 months),
RR>60 (6-12 months),
RR>40 (>12 months)
Respiratory
Effort
Mild chest wall
retraction
Tracheal tug, Nasal
flare, Moderate chest
wall retraction
Marked chest wall
retraction, Nasal flare,
Grunting
Oxygen
Saturations
No supplemental
oxygen requirement
O2 saturations >95%
Saturations 90-95% Saturations <90% may
not be corrected by O2
Feeding Normal to slightly
decreased
50 75% of normal
feeds
<50% of feeds, unable to
feed
Apnoea Nil May have brief episodes May have increasing
episodes
The type and frequency of diagnostic tests used for bronchiolitis, such as viral
detection and radiographs, vary markedly among clinicians. As stated in the AAP guideline,
results of evidence-based reviews have not supported a role for any diagnostic tests in the
management of routine cases of bronchiolitis.
7
According to a survey of hospital-based pediatricians, the most common tests are
rapid viral antigen testing of nasopharyngeal secretions for respiratory syncytial virus (RSV),
arterial blood gas (ABG) analysis (in severely ill patients, especially those requiring
mechanical ventilation), white blood cell (WBC) count with differential, C-reactive protein
(CRP) level, and chest radiography. Other common tests are pulse oximetry, blood culture,
urine analysis and culture, and cerebrospinal fluid (CSF) analysis and culture. Urine specific
gravity may provide useful information regarding fluid balance and possible dehydration.
Serum chemistries are not affected directly by the infection but may aid in gauging severity
dehydration.
7
Rapid viral antigen tests have variable sensitivity and specificity depending on the test
and when they are used during the respiratory season. These tests detect the RSV antigen in
epithelial cells from nasopharyngeal secretions, bronchoalveolar lavage fluid, or lung tissue.
They are performed by using either direct immunofluorescent antibody (IFA) staining or an
enzyme-linked immunosorbent assay (ELISA). With adequate sampling, IFA staining
requires 2-6 hours for processing and is 90% sensitive and specific. ELISA requires 30
minutes for processing and is 85-90% sensitive as compared with viral culture. Although
ELISA is somewhat quicker and easier to interpret because it yields a more objective
endpoint, the IFA technique may be preferable, in that it permits determination of the number
of epithelial cells recovered and thereby can verify the adequacy of the sample.
4
The WBC count range from 5000-24,000 cell/mm
3
. In patients with elevated WBC
counts, there is a preponderance of polimorphonuclear leukocytes and band forms.
10
Pulse oximetry is performed in almost every child who presents with acute
bronchiolitis. Suggested guidelines for lower limits of acceptable oxygen saturation levels for
bronchiolitis have included 90% and 94% as well as 92%. Transcutaneous oxygen saturation
is a good indicator of the severity of bronchiolitis. It correlates best with tachypnea; however,
it correlates poorly with wheezing and retractions. Patients with persistent resting oxygen
saturations below 92% in room air require a period of observation and possible
hospitalization.
4
Chest radiographs are not routinely necessary.If clinically indicated, they should
include anteroposterior (AP) and lateral views. Chest radiography is most useful in excluding
unexpected congenital anomalies or other conditions, it may also yield positive evidence of
alternative diagnoses (eg, lobar pneumonia, congestive heart failure, or foreign body
aspiration). Findings from chest radiography in individuals with bronchiolitis are variable.
Hyperinflation is usually present (see the image below), and 20-30% of chest radiographs
show lobar infiltrates, atelectasis, or both. Other findings may include bronchial wall
thickening, air trapping, flattened diaphragm, increased AP diameter, peribronchial cuffing,
tiny nodules, linear opacities, and patchy alveolar opacities. Opacities on radiographs do not
suggest bacterial pneumonia and incorrectly lead to inappropriate treatment with antibiotics.
4
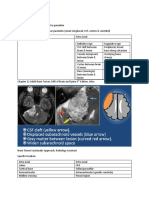
Immunohistochemistry of autopsy lung specimens
from a 15-month-old patient with an untreated RSV
infection (72). Immunostaining for RSV antigens
(a) revealed infection of the bronchiolar epithelium in
a near circumferential pattern sparing the basal cells.
The basal cells can restore the epithelium, but in the
process may lead to mucus metaplasia and
remodeling of airways. In addition to infection of the
polarized ciliated epithelium, it appears that other cell
types, potentially including intraepithelial DCs, can
be infected (arrows point to the projections of
irregularly shaped RSV-infected cells that are thought
to be DCs, based on morphology). Immunostaining
for CD1a_ DCs
(b) showed that they are not prominent in the lung
parenchyma during infection, but when present can
have a distinctive morphology with multiple
projections that can extend beyond the apical or basal
boundary of the columnar epithelium. CD69_
monocytes were the major cell type present in
peribronchiolar infiltrates. However, CD3_ T cells
also were abundant and, while most of them appeared
to be double negative for CD4 and CD8, many were
positive
for CD8 immunostaining (c). In panels a to c, L
indicates airway lumen; in panel c, the lower lumen is
occluded with debris and immune
cells.
Figure 1. Chest radiography of bronchiolitis 1. A chest radiography revealing lung
hyperinflation with a flattened diaphragm and bilateral atelectasis in the right apical and left
basal regions in a 16-day-old infant with severe bronchiolitis.
Electrocardiography (ECG) or echocardiography should be reserved for those few
children who display arrhythmias or cardiomegaly.
In rare situations, such as severe
immunodeficiency or a strong history of possible foreign body aspiration, bronchoscopy may
be indicated for diagnostic bronchoalveolar lavage or therapeutic foreign body removal.
4
2.6. Differential Diagnosis
A number of other conditions can mimic acute bronchiolitis. Pulmonary causes of
bronchiolitis like symptoms include asthma, bronchopneumonia, pertussis, congenital lung
disease, cystic fibrosis or inhaled foreign body. Non-pulmonary causes include CHD, sepsis
or severe metabolic acidosis, tracheoesophageal fistula, gastroesophageal reflux.
3
Other causes of chest retraction and airway obstruction must be ruled out be careful
physical and radiographic examination. These include obstruction of the nasopharynx by
hypertrophied adenoids or a retropharyngeal abscess; laryngeal obstruction caused by
abnormalities of the larynx, croup, a foreign body, and lobar emphysema. Occasionally,the
hypernea of metabolic disorders such as salicylate poisoning mimics bronchiolitis.If
salicylate have been given, measurements of pH, oxygent saturation, salicylate levels, and
serum electrolytes aid in making the proper diagnosis. Congestive heart failure secondary to
a congenital malformation or viral myocarditis may manifest clinical findings very similar to
those of brochiolitis, and the palpable liver and spleen found frequently in infants with
brochiolitis may contribute to the confusion. A history of normal growth and development
and the absence of a cardiac murmur assist in the diagnosis. Infants with cardiac disease often
develop congestive heart failure during viral infections,and the two conditions may conexist.
The lung disease of cystic fibrosis may present as acute brochiolitis.
10
2.7. Treatment
Carefull monitoring and good supportive care remain the cornerstones of
management. For those without an underlying immunodeficiency, RSV infections are self
limiting, and management is aimed at providing adequate support until the illness resolves.
Monitoring is principally directed toward the detection of apnea, hypoxia, and exhaustion.
Supportive care is directed an alleviating hypoxia, providing adequate fluids, and preventing
exhaustion by relieving hypoxia and minimal handling.
11
Mild bronchiolitis is often treated at home. For infants wih mild respiratory
distress,careful observation and adequate fluid administration are appropriate.Infants with
moderate of severe respiratory distress should usually be hospitalized. The aims of hospital
treatment are: 1.to support the infant; 2.to detect and treat possible complications; 3.to
prevent the spread of infection to other patients and to staff; 4.to treath with specific antiviral
agents in indicated.
10
Controversies in the treatment of bronchiolitis concern:1.the use bronchodilators;
2.the use of corticosteroids.; 3.the use of antiviral agents; 4.unfortunatelythe use of
antibiotics. Supportive care for hospitalized infants with bronchiolitis includes the
administration of oxygen and the appropriate fluids, careful monitoring to detect hypoxemia,
apnea and respiratoy failure; and attention to temperature regulation.
10
Oxygen is indicated to maintain saturations > 90%.
4
Apply oxygen only if saturations
are persistently below 90%.
11
The target range saturation oxygen is 92-96%. Continuous
monitoring is recommended if supplemental oxygen is required. If supplemental oxygen is
not needed, every 4 hour oxygen saturation monitoring may be used. Consider maintaining
higher oxygen saturations for patients with: fever, acidosis, hemoglobinopathy, chronic lung
disease, significant cardiac disease, or prematurity. Oxygen can preferably via a humidified
circuit : nasal cannula up to 2 l.p.m. flow and head box for higher requirements.
4
Infants with bronchiolitis are mildly dehydrated because of decreased fluid intake and
increased fluid losses from fever and tachypnea. Accordingly, it is vital to maintain adequate
hydration. Avoid excessive fluid administration, because this may promote interstitial edema
formation, particularly if a component of inappropriate antidiuretic hormone release is
present.
7
Oral therapy is preferred, smaller and more frequent feeds either by breast or bottle-
feed, calculated to a 2nd to 3rd hourly. Peroral feeds are recommended if patients are stable
with RR < 80/minute. Thickening feeds with 1-2 teaspoons of cereal/ounce of formula or
breast milk has been shown to decrease the risk of aspiration and is recommended. Continued
breastfeeding should be encouraged. Nasogastric/Orogastric feeds are an effective and safe
method if used appropriately. It is indicated in those who are unable to take sufficient oral
intake to maintain or correct hydration status, has a persistent RR > 80/minute, vomiting,
decreased oxygen saturation to < 90% despite supplemental oxygen during feedings, or
marked work of breathing during feeds.
8
Intravenous fluids indicated if child is vomiting or has severe respiratory distress,
which may be worsened by enteral feeds. The IV line are 0.45% saline (as concentration) and
5% dextrose with 10mmol KCl per 500mls, then give 75% maintenance and Check UEs
within 24 hours of commencing, in particular to monitor for hyponatraemic fluid overload.
Parenteral therapy may be necessary in patients who are unable to take fluids by mouth or
who have a respiratory rate higher than 70 breaths/min. Nasal saline drops and frequent
suctioning, especially prior to feeding, is useful.
8
Medications have a limited role in the management of bronchiolitis. In
immunocompetent patients with large number of trials have not found drug therapy to be of
significant benefit, so do not routinely prescribe bronchodilators, antibiotics or steroids.
7
Bronchodilators including nebulised epinephrine, a trial of 6 actuations of a
salbutamol MDI, administered via spacer may be tried on the advice of senior medical staff
but if no clinical improvement ensues in 20 minutes it should not be continued. Albuterol is
not typically beneficial. If a patient has a strong family history of asthma or a component of
bronchospasm, albuterol may be helpful. A trial of albuterol should be discontinued if no
response is noted after an initial dose. Patients who respond to albuterol may have
undiagnosed asthma.
8
Steroids (inhaled or oral) systematic review, no evidence of benefit acutely or in
preventing future wheezing.3 However, in a patient with a strong family history of asthma or
a past history of wheezing/asthma, steroids may be beneficial particularly if a patient is
deteriorating. Patients who respond to steroids may have undiagnosed asthma.
8
Ribavirin not routinely recommended. Ribavirin, an anti-viral administered in a
negative flow room via aerosolized particles, may be indicated for highrisk patients with
severe RSV bronchiolitis or for patients at risk for severe RSV bronchiolitis and requires
pediatric critical care consultation. Ribavirin may be considered for patients with the
following characteristics: Complicated congenital heart disease, immunocompromised
bronchopulmonary dysplasia (BPD), multiple congenital anomalies, metabolic disease,
chronic lung disease (CLD), neurologic disease.
8
Antibiotics, in controlled trials show not indicated routinely. RSV immunoglobulin not
routinely recommended too. Physiotherapy, no evidence to support the use of chest
physiotherapy.
7
Table 2. Summary of Recent Evidence for Therapies Used for Bronchiolitis
2.8. Prevention
The prevention of RSV infection has been accelerated in recent years by the trials of
RSV immune globulin administered intravenously monthly in doses of 750 mg to high risk
infants and of intramuscular palivizumab, a humanized respiratory monoclonal antibody that
has demonstrated considerable efficacy in preventing the hospitalization of high risk infants.
It is known commercially as synagis, is administered IM at a dose of 15 mg/kg every 30 days,
and is distributed in 100 mg lyophilized vials.
10
2.9. Prognosis
Hospitalization is required in as many 2% of cases (mostly patients younger than 6
months). Overall, the mortality in children hospitalized for bronchiolitis in different series
ranges from 0.2% to 7%. Morbidity and mortality from RSV mostly occur in children
younger than 2 years. Other high-risk infants and children include premature infants younger
than 6 months, infants and children with underlying pulmonary or cardiac disease, and those
an immune deficiency.
4
Although bronchiolitis has been identified as a risk factor for asthma, this does not
necessarily imply causation. Children already predisposed to asthma may be more likely to
wheeze when exposed to RSV or other respiratory infectious or allergic stimuli. On the other
hand, it is postulated that RSV infection may predispose an individual to later bronchospasm
by selective promotion of specific subsets of helper T cells.
4
Multiple studies have shown that children, including febrile infants younger than 8
weeks, with confirmed RSV infection have a lower risk of serious bacterial infections or
secondary bacterial superinfection than controls (eg, 0% vs 2.7% for bacteremia, and 2% vs
14% for urinary tract infection. The risk of concurrent bacterial infections is low.
4
Discharge criteria for patients with bronchiolitis is stable and improving, oxygen
saturation maintained >92% in air for period of 8-12 hours, including a period of sleep,
feeding adequately (more than 2/3 normal feeds), family confident in their ability to manage.
8
Anda mungkin juga menyukai
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDari EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifePenilaian: 4 dari 5 bintang4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingDari EverandThe Little Book of Hygge: Danish Secrets to Happy LivingPenilaian: 3.5 dari 5 bintang3.5/5 (399)
- Ecr2019 C-0304Dokumen14 halamanEcr2019 C-0304regarskidBelum ada peringkat
- Ecr2017 C-2712Dokumen14 halamanEcr2017 C-2712regarskidBelum ada peringkat
- Critical ValueDokumen17 halamanCritical ValueregarskidBelum ada peringkat
- Brain Tumor - IntraExtra AxialDokumen6 halamanBrain Tumor - IntraExtra AxialregarskidBelum ada peringkat
- Prkacin 2018Dokumen1 halamanPrkacin 2018regarskidBelum ada peringkat
- Choledochal CystsDokumen26 halamanCholedochal CystsregarskidBelum ada peringkat
- Reference Management for Medical PapersDokumen37 halamanReference Management for Medical PapersregarskidBelum ada peringkat
- Kuo 2017Dokumen35 halamanKuo 2017regarskidBelum ada peringkat
- Critical Value (EDIT)Dokumen8 halamanCritical Value (EDIT)regarskidBelum ada peringkat
- Mon 11-30 Neuroimaging Pearls For The Primary Care Provider - 0Dokumen25 halamanMon 11-30 Neuroimaging Pearls For The Primary Care Provider - 0regarskidBelum ada peringkat
- Panduan Penelitian NHS 2013Dokumen28 halamanPanduan Penelitian NHS 2013regarskidBelum ada peringkat
- Choledochal CystsDokumen6 halamanCholedochal CystsregarskidBelum ada peringkat
- Pharmacology Aspect of Antimalaria - 2009Dokumen48 halamanPharmacology Aspect of Antimalaria - 2009regarskidBelum ada peringkat
- Panduan Penelitian NHS 2013 LampiranDokumen19 halamanPanduan Penelitian NHS 2013 LampiranrosidahhanumBelum ada peringkat
- Physical Examination Generalised StatusDokumen10 halamanPhysical Examination Generalised StatusregarskidBelum ada peringkat
- Lapkas Lalala FixDokumen36 halamanLapkas Lalala FixregarskidBelum ada peringkat
- Faktor-Faktor Yang Mempengaruhi BelajarDokumen21 halamanFaktor-Faktor Yang Mempengaruhi BelajarregarskidBelum ada peringkat
- THE LASIK REPORT - A Call For The Discontinuation of A Harmful ProcedureDokumen11 halamanTHE LASIK REPORT - A Call For The Discontinuation of A Harmful Procedurebrentahanson100% (1)
- Lapkas Anak Febi c3-4Dokumen17 halamanLapkas Anak Febi c3-4regarskidBelum ada peringkat
- Night Vision GoogleDokumen1 halamanNight Vision GoogleregarskidBelum ada peringkat
- Vulgaris Gene Found Information SheetDokumen4 halamanVulgaris Gene Found Information SheetregarskidBelum ada peringkat
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDari EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryPenilaian: 3.5 dari 5 bintang3.5/5 (231)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDari EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RacePenilaian: 4 dari 5 bintang4/5 (894)
- The Yellow House: A Memoir (2019 National Book Award Winner)Dari EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Penilaian: 4 dari 5 bintang4/5 (98)
- Shoe Dog: A Memoir by the Creator of NikeDari EverandShoe Dog: A Memoir by the Creator of NikePenilaian: 4.5 dari 5 bintang4.5/5 (537)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDari EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FuturePenilaian: 4.5 dari 5 bintang4.5/5 (474)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDari EverandNever Split the Difference: Negotiating As If Your Life Depended On ItPenilaian: 4.5 dari 5 bintang4.5/5 (838)
- Grit: The Power of Passion and PerseveranceDari EverandGrit: The Power of Passion and PerseverancePenilaian: 4 dari 5 bintang4/5 (587)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDari EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaPenilaian: 4.5 dari 5 bintang4.5/5 (265)
- The Emperor of All Maladies: A Biography of CancerDari EverandThe Emperor of All Maladies: A Biography of CancerPenilaian: 4.5 dari 5 bintang4.5/5 (271)
- On Fire: The (Burning) Case for a Green New DealDari EverandOn Fire: The (Burning) Case for a Green New DealPenilaian: 4 dari 5 bintang4/5 (73)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDari EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersPenilaian: 4.5 dari 5 bintang4.5/5 (344)
- Team of Rivals: The Political Genius of Abraham LincolnDari EverandTeam of Rivals: The Political Genius of Abraham LincolnPenilaian: 4.5 dari 5 bintang4.5/5 (234)
- Rise of ISIS: A Threat We Can't IgnoreDari EverandRise of ISIS: A Threat We Can't IgnorePenilaian: 3.5 dari 5 bintang3.5/5 (137)
- The Unwinding: An Inner History of the New AmericaDari EverandThe Unwinding: An Inner History of the New AmericaPenilaian: 4 dari 5 bintang4/5 (45)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDari EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyPenilaian: 3.5 dari 5 bintang3.5/5 (2219)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDari EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You ArePenilaian: 4 dari 5 bintang4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Dari EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Penilaian: 4.5 dari 5 bintang4.5/5 (119)
- Her Body and Other Parties: StoriesDari EverandHer Body and Other Parties: StoriesPenilaian: 4 dari 5 bintang4/5 (821)
- Pediatric Nursing - Respiratory DisordersDokumen9 halamanPediatric Nursing - Respiratory Disordershasan ahmdBelum ada peringkat
- 10 Quiz of PneumoniaDokumen3 halaman10 Quiz of PneumoniaTatyannah Alexa MaristelaBelum ada peringkat
- Welcome RSVDokumen32 halamanWelcome RSVapi-260357356Belum ada peringkat
- Presentation URTI& LRTI - G1Dokumen134 halamanPresentation URTI& LRTI - G1Aniq Zahran MasomBelum ada peringkat
- Bronchiolitis Management French GDL ICM 23Dokumen21 halamanBronchiolitis Management French GDL ICM 23Adynna TévinaBelum ada peringkat
- An Evaluation of Chest Physiotherapy in The Management of Acute Bronchiolitis Changing Clinical Practice PDFDokumen6 halamanAn Evaluation of Chest Physiotherapy in The Management of Acute Bronchiolitis Changing Clinical Practice PDFbuku fisioBelum ada peringkat
- Effectiveness of nebulized N-acetylcysteine in treating children with acute bronchiolitisDokumen4 halamanEffectiveness of nebulized N-acetylcysteine in treating children with acute bronchiolitisIvan VeriswanBelum ada peringkat
- Bronchiolitis FdneDokumen27 halamanBronchiolitis FdneRonit ChandBelum ada peringkat
- Asthma Clinical Care GuidelinesDokumen17 halamanAsthma Clinical Care GuidelinesWalaa MoustafaBelum ada peringkat
- AAH v2 Acute AsthmaDokumen81 halamanAAH v2 Acute AsthmaEssa SmjBelum ada peringkat
- 1 Topic 1 - Differential Diagnosis of Pneumonia in Children. Complications of Pneumonia ... (PDFDrive)Dokumen164 halaman1 Topic 1 - Differential Diagnosis of Pneumonia in Children. Complications of Pneumonia ... (PDFDrive)Dara PitraBelum ada peringkat
- Pediatric Noninvasive Ventilation: Cathy HautDokumen7 halamanPediatric Noninvasive Ventilation: Cathy HautsiputamaliaputriBelum ada peringkat
- Case Study 3 BronchiolitisDokumen3 halamanCase Study 3 Bronchiolitisarifqighaffur95Belum ada peringkat
- Buckinghamshire Pathways and Leaflets PDFDokumen10 halamanBuckinghamshire Pathways and Leaflets PDFAlexa SienesBelum ada peringkat
- Jurnal 7 BronkiolitisDokumen7 halamanJurnal 7 BronkiolitisIrsanti sasmitaBelum ada peringkat
- Child - Bronchiolitis NCPDokumen2 halamanChild - Bronchiolitis NCPjoeti80% (5)
- Jurnal AsmaDokumen11 halamanJurnal AsmaAi Siti Rika FauziahBelum ada peringkat
- Treating RSV Pneumonitis in InfantsDokumen6 halamanTreating RSV Pneumonitis in InfantsIja Lourice RosalBelum ada peringkat
- Lecture 8, Nursing Care of The Child With Respiratory Dysfunction and Renal Disorders 2Dokumen48 halamanLecture 8, Nursing Care of The Child With Respiratory Dysfunction and Renal Disorders 2مهند الرحيليBelum ada peringkat
- Pem Quiz: Respiratory Emergencies Peter S. Auerbach, MDDokumen3 halamanPem Quiz: Respiratory Emergencies Peter S. Auerbach, MDPhanVHBelum ada peringkat
- Virology Respiratory VirusesDokumen6 halamanVirology Respiratory VirusesHisham ChomanyBelum ada peringkat
- Oral Dexamethasone For Bronchiolitis A Randomized TrialDokumen9 halamanOral Dexamethasone For Bronchiolitis A Randomized TrialhwelpBelum ada peringkat
- Status Asthmaticus Case StudyDokumen18 halamanStatus Asthmaticus Case Studygeorgeloto12Belum ada peringkat
- Effectiveness of thoracic-abdominal rebalancing technique for acute viral bronchiolitisDokumen9 halamanEffectiveness of thoracic-abdominal rebalancing technique for acute viral bronchiolitisrebeca paulinoBelum ada peringkat
- Nej Me 030052Dokumen2 halamanNej Me 030052BahrunBelum ada peringkat
- Acute Respiratory Infections in Children: Causes and BurdenDokumen16 halamanAcute Respiratory Infections in Children: Causes and BurdenDesi Riana PurbaBelum ada peringkat
- Pediatric Fundamental Critical Care SupportDokumen811 halamanPediatric Fundamental Critical Care SupportSofi De Leon85% (20)
- Cao Et Al-2013-Cochrane Database of Systematic ReviewsDokumen30 halamanCao Et Al-2013-Cochrane Database of Systematic ReviewsIRMÃOS FOREVERBelum ada peringkat
- Clinical Profile of Acute BronchiolitisDokumen4 halamanClinical Profile of Acute BronchiolitisInternational Journal of Innovative Science and Research TechnologyBelum ada peringkat
- The Wheezing Infant: Airway Problems in ChildrenDokumen4 halamanThe Wheezing Infant: Airway Problems in ChildrenDenise DelaneyBelum ada peringkat