Anti-HIV Therapeutic Research - Institute of Human Virology
Diunggah oleh
Man LorJudul Asli
Hak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Anti-HIV Therapeutic Research - Institute of Human Virology
Diunggah oleh
Man LorHak Cipta:
Format Tersedia
Anti-HIV Therapeutic Research: Institute of Human Virology
CLINCAL CARE AND
RESEARCH
Division Overview
Site
Directory
Faculty
Search the Site
IHV > Research:Anti-HIV Therapeutic Research
ANTI-HIV THERAPEUTIC RESEARCH
Clinical Trials
Associated Faculty
Anti-HIV Therapeutic Research
Lab Head
Assistant Professor Olga Latinovic, PhD
Clinics
Assistant Professor Alonso Heredia, PhD
Social Entrepreneurship (PDF)
JACQUES Initiative
Focus of our work is the CCR5 chemokine receptor that plays a crucial
role in HIV-1 infection and as such offers an important potential
therapeutic target [Fig.1]. We have established methods to quantify
CCR5 density and to evaluate its impact on virus infectivity in
spreading/single cycle infection and direct virus-cell fusion assays.
Using low doses of the drug Rapamycin, a CCR5 suppressor, we
demonstrate decreased R5 HIV-1 infectivity and enhanced potency of
entry inhibitors. Our data show that Rapamycin reduction of CCR5
density restores sensitivity of drug-resistant R5 HIV-1 to fusion inhibitor
Enfuvirtide,T-20, (Antimicrobial Reagents and Chemotherapy, 2007) and
to the new generation of entry inhibitors-CCR5 antagonists (Antiviral
Research, 2009; Clinical Medicine: Therapeutics, 2009).
Robert Redfield, MD
We found that Rapamycin induced reduction of CCR5 density in
lymphocytes increased sensitivity to Vicriviroc (VCV) in VCV-resistant strains, inhibiting production by ~ 90% (PNAS,
2008). Novel Beta-lactamase (BlaM) entry assay revealed the differences in the activity between CCR5 antagonist
sensitive and CCR5 antagonist resistant virus. In the case of CCR5 antagonist sensitive virus, we observed complete
inhibition in cell lines with high and physiological CCR5 levels. In the case of the resistant virus, there is no inhibition in
higher CCR5 expressive cells, but in cells with physiological expression of CCR5, we do observe susceptibility to
CCR5 antagonist resistant virus.
As an alternative anti-viral therapy approach, we currently employ the CCR5 antibodies in order to determine the affinity
of resistant virus Envelope in cases when it is free versus occupied CCR5 site by the CCR5 antagonists. Looking for
the mechanism of resistant to CCR5 antagonists viruses [Fig. 2], we found out that interaction between the antagonists
occupied CCR5 and the CCR5 antibody is more potent than inhibition provided by CCR5 antibody per se. HIV-1 strains
resistant to the only clinically approved CCR5 antagonist Maraviroc (MVC, Fig. 3) generally remain CCR5 tropic, but
gain the ability to use drug-bound CCR5. We demonstrate that MVCresistant HIV-1 loses the ability to use MVC-bound
CCR5 at low surface CCR5 densities, suggesting a lower affinity for antagonist-bound CCR5 compared to free CCR5.
In accordance, antibodies directed against the second extracellular loop (ECL2) of CCR5 had greater antiviral activity
in MVC-bound than in MVC-free CCR5 infection of cell lines. However, in primary peripheral blood lymphocytes
(PBLs), a dichotomy in antibody efficacy became evident. ECL2 CCR5 mAbs HGS004 and HGS101, inhibited PBL
infection by MVC resistant HIV-1 more potently with MVC-bound than with free CCR5. In addition, HGS004 and
HGS101, but not the other mAbs, restored the antiviral activity of MVC against resistant virus in PBLs. Both, HGS004
and HGS101, currently in clinical development, could help overcome MVC Resistance (Virology, 2011).
In addition, we demonstrate that the CCR5 antibody HGS004 and the CCR5 antagonist Maraviroc have potent antiviral
synergy against R5 HIV-1, translating into dose reductions of >10-fold for Maraviroc and >150-fold for HGS004 (AIDS,
2011). These data, together with the high barrier of resistance to HGS004, suggest that combinations of Maraviroc and
HGS004 could provide effective preventive and therapeutic strategies against R5 HIV-1.
Figure 1
Therapeutic opportunities for inhibition of HIV-1 entry
http://www.ihv.org/research/anti_hiv.html[28/10/2557 3:36:38]
Anti-HIV Therapeutic Research: Institute of Human Virology
HIV-1 entry is mediated by the viral Env protein, which comprises the glycoproteins gp120 and gp41 arranged in
trimeric spikes on the viral surface. Entry encompasses three steps: CD4 binding, coreceptor binding and fusion. The
viral gp120 first binds to CD4, causing a repositioning of the variable loops V1/V2 and V3 and thereby exposing the
bridging sheet and forming a coreceptor binding site. Upon coreceptor binding, conformational changes in gp120 and
gp41 lead to the insertion of gp41 fusion peptide into the cell membrane. Subsequent conformational changes result in
the formation of a six-helix bundle, with the HR2 domains folding back and packing into grooves on the outside of the
triple-stranded HR1 domains. This brings the fusion peptide and transmembrane region of gp41 in close proximity,
forming a fusion pore that allows transfer of the viral core into the cell. Each step on HIV-1 entry can be targeted by
inhibitors currently approved or in clinical development. CD4 binding is targeted by ibalizumab (formerly TNX-355), a
humanized monoclonal antibody that binds to CD4. Coreceptor binding is blocked by small-molecule CCR5 antagonists
(Maraviroc and Vicriviroc) and by CCR5 antibodies (PRO-140 and HGS-004). Finally, the formation of a six-helix
bundle, and thereby fusion, is prevented by enfuvirtide. Figure 1. adapted from Melikyan GB, Retrovirology, 2008.
Figure 2
Model for Maraviroc mechanism of resistance
Maraviroc binds to the transmembrane region of CCR5, thereby inducing confomational changes that cannot be
recognized by R5 HIV-1 gp120. One mechanism of resistance involves changes in HIV-1 Env that permit recognition of
Maraviroc-bound CCR5. As such, resistant viruses are not blocked by increasing Maraviroc doses. Figure 2. adapted
from M. Westby, Curr Opin HIV AIDS, 2007.
http://www.ihv.org/research/anti_hiv.html[28/10/2557 3:36:38]
Anti-HIV Therapeutic Research: Institute of Human Virology
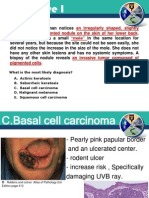
Figure 3
Model for maraviroc mechanism of action
Binding of HIV-1 gp120 to CD4 exposes the bridging sheet and creates a coreceptor binding site. In the absence of
Maraviroc, the bridging sheet and the base of V3 interact with the N-terminus of CCR5, while more distal regions of V3
interact with extracellular loops (mainly ECL2). Binding of Maraviroc to the transmembrane region of CCR5 locks CCR5
in a conformation that does not recognize the distal regions of V3. Figure 3. adapted from Soriano V. et al, AIDS, 2008.
Hotline
The Institute of Human Virology, 725 West Lombard Street, Baltimore MD 21201
http://www.ihv.org/research/anti_hiv.html[28/10/2557 3:36:38]
Anda mungkin juga menyukai
- Shoe Dog: A Memoir by the Creator of NikeDari EverandShoe Dog: A Memoir by the Creator of NikePenilaian: 4.5 dari 5 bintang4.5/5 (537)
- Benign Skin TumoursDokumen7 halamanBenign Skin TumoursMan LorBelum ada peringkat
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDari EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifePenilaian: 4 dari 5 bintang4/5 (5794)
- Calendar July 2016 LandscapeDokumen1 halamanCalendar July 2016 LandscapeMan LorBelum ada peringkat
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDari EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RacePenilaian: 4 dari 5 bintang4/5 (895)
- Bowen's Disease: Understanding The SkinDokumen6 halamanBowen's Disease: Understanding The SkinMan LorBelum ada peringkat
- The Yellow House: A Memoir (2019 National Book Award Winner)Dari EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Penilaian: 4 dari 5 bintang4/5 (98)
- Calendar September 2016 LandscapeDokumen1 halamanCalendar September 2016 LandscapeMan LorBelum ada peringkat
- Grit: The Power of Passion and PerseveranceDari EverandGrit: The Power of Passion and PerseverancePenilaian: 4 dari 5 bintang4/5 (588)
- Frizzell - Handbook of PathophysiologyDokumen973 halamanFrizzell - Handbook of PathophysiologyididgamaBelum ada peringkat
- The Little Book of Hygge: Danish Secrets to Happy LivingDari EverandThe Little Book of Hygge: Danish Secrets to Happy LivingPenilaian: 3.5 dari 5 bintang3.5/5 (400)
- History: A 65-Year-Old Man Presented To TheDokumen3 halamanHistory: A 65-Year-Old Man Presented To TheMan LorBelum ada peringkat
- The Emperor of All Maladies: A Biography of CancerDari EverandThe Emperor of All Maladies: A Biography of CancerPenilaian: 4.5 dari 5 bintang4.5/5 (271)
- LCE-24C100F (K) LCE-24C100F (N) LCE-24C100F (R) LCE-24C100F (S) : Instruction ManualDokumen20 halamanLCE-24C100F (K) LCE-24C100F (N) LCE-24C100F (R) LCE-24C100F (S) : Instruction ManualMan LorBelum ada peringkat
- Never Split the Difference: Negotiating As If Your Life Depended On ItDari EverandNever Split the Difference: Negotiating As If Your Life Depended On ItPenilaian: 4.5 dari 5 bintang4.5/5 (838)
- Skin CutDokumen9 halamanSkin CutMan LorBelum ada peringkat
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDari EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyPenilaian: 3.5 dari 5 bintang3.5/5 (2259)
- Case Hematology + Genetics I: Β Thalassemia/Hbe DiseaseDokumen1 halamanCase Hematology + Genetics I: Β Thalassemia/Hbe DiseaseMan LorBelum ada peringkat
- On Fire: The (Burning) Case for a Green New DealDari EverandOn Fire: The (Burning) Case for a Green New DealPenilaian: 4 dari 5 bintang4/5 (74)
- Skin-All For FriendDokumen10 halamanSkin-All For FriendMan LorBelum ada peringkat
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDari EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FuturePenilaian: 4.5 dari 5 bintang4.5/5 (474)
- Proteins Practice QuizDokumen5 halamanProteins Practice Quizafaflotfi_155696459Belum ada peringkat
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDari EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryPenilaian: 3.5 dari 5 bintang3.5/5 (231)
- Lipids 31 2012 NotesDokumen20 halamanLipids 31 2012 Notesapi-178321548Belum ada peringkat
- Team of Rivals: The Political Genius of Abraham LincolnDari EverandTeam of Rivals: The Political Genius of Abraham LincolnPenilaian: 4.5 dari 5 bintang4.5/5 (234)
- 1907 - Cibenza DP100 CasablancaMC-shortDokumen38 halaman1907 - Cibenza DP100 CasablancaMC-shortMuhammad Farrukh HafeezBelum ada peringkat
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDari EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaPenilaian: 4.5 dari 5 bintang4.5/5 (266)
- Alternate Phosphorylation-O-GlcNAc Modification On Human Insulin IRSs - A Road Towards Impaired Insulin Signaling in Alzheimer and DiabetesDokumen19 halamanAlternate Phosphorylation-O-GlcNAc Modification On Human Insulin IRSs - A Road Towards Impaired Insulin Signaling in Alzheimer and DiabeteswaqarchemistBelum ada peringkat
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDari EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersPenilaian: 4.5 dari 5 bintang4.5/5 (345)
- Glyoxylate CycleDokumen8 halamanGlyoxylate Cyclerahul pBelum ada peringkat
- KilomikronDokumen17 halamanKilomikronsolgraBelum ada peringkat
- The Unwinding: An Inner History of the New AmericaDari EverandThe Unwinding: An Inner History of the New AmericaPenilaian: 4 dari 5 bintang4/5 (45)
- Histone Deacetylases Transcriptional Control, and Cancer.Dokumen16 halamanHistone Deacetylases Transcriptional Control, and Cancer.jose_gladiusBelum ada peringkat
- Rise of ISIS: A Threat We Can't IgnoreDari EverandRise of ISIS: A Threat We Can't IgnorePenilaian: 3.5 dari 5 bintang3.5/5 (137)
- Protein IDokumen52 halamanProtein INusmir LisičićBelum ada peringkat
- Antibody Structure and Function PDFDokumen8 halamanAntibody Structure and Function PDFJay JaswaniBelum ada peringkat
- Biochemistry ProblemDokumen5 halamanBiochemistry ProblemJnanendra SenguptaBelum ada peringkat
- Vitamin A FinalDokumen64 halamanVitamin A FinalLiaqat HussainBelum ada peringkat
- GlycolysisDokumen51 halamanGlycolysisKazar ProbusBelum ada peringkat
- 1 Digestion and AbsorptionDokumen12 halaman1 Digestion and AbsorptionJared Dela cruzBelum ada peringkat
- Lactobaciluss LactisDokumen12 halamanLactobaciluss LactisHary Peace LoveerBelum ada peringkat
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDari EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You ArePenilaian: 4 dari 5 bintang4/5 (1090)
- Protein Chemistry Section ExamDokumen9 halamanProtein Chemistry Section ExamJoelBelum ada peringkat
- Level of Organisation of Protein StructureDokumen18 halamanLevel of Organisation of Protein Structureyinghui94Belum ada peringkat
- Chapter 23 Lippincott BiochemistryDokumen44 halamanChapter 23 Lippincott BiochemistryMeysam SajjadiBelum ada peringkat
- Atrovas Dan Feno FibrateDokumen9 halamanAtrovas Dan Feno FibrateGalih Antona SinatriaBelum ada peringkat
- Human Nutrition, NotesDokumen470 halamanHuman Nutrition, NotesruthBelum ada peringkat
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Dari EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Penilaian: 4.5 dari 5 bintang4.5/5 (121)
- Laporan TATDokumen12 halamanLaporan TATHARPIANELIBelum ada peringkat
- Chapter 2 - Basics of EnzymesDokumen40 halamanChapter 2 - Basics of EnzymesSakinah MuhamadBelum ada peringkat
- Criteria For Purity of Enzyme PreparationDokumen24 halamanCriteria For Purity of Enzyme Preparationshabana75% (4)
- Shikimic Acid Pathway: By: Resane Ma. JannelleDokumen14 halamanShikimic Acid Pathway: By: Resane Ma. JannelleMA. JANNELLE P. RESANEBelum ada peringkat
- Protien ChipDokumen5 halamanProtien ChipPallav SinghBelum ada peringkat
- Vaxa - UltraNanno Product Data SheetDokumen4 halamanVaxa - UltraNanno Product Data SheetLuan NguyenBelum ada peringkat
- Is It So Bad To Eat Only PizzaDokumen2 halamanIs It So Bad To Eat Only PizzaNicholasBelum ada peringkat
- Her Body and Other Parties: StoriesDari EverandHer Body and Other Parties: StoriesPenilaian: 4 dari 5 bintang4/5 (821)
- Phospholipid and Sphingosine SynthesisDokumen2 halamanPhospholipid and Sphingosine SynthesisAlliah Mae LumanogBelum ada peringkat
- (IB Biology) 1.3 Membrane StructureDokumen25 halaman(IB Biology) 1.3 Membrane StructureYiwei HeBelum ada peringkat
- Hema 2Dokumen35 halamanHema 2Angela ReyesBelum ada peringkat
- Source: Data Obtained From Robert Mcgilvery, Biochemistry: A Functional Approach, 1970, W. B. Saunders.Dokumen8 halamanSource: Data Obtained From Robert Mcgilvery, Biochemistry: A Functional Approach, 1970, W. B. Saunders.Ayaan AliBelum ada peringkat