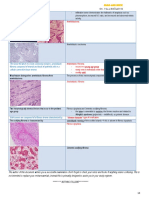
Nonsquamous Cell Malignant Tumours of The Oral Cavity: An Overview
Diunggah oleh
ranggadrDeskripsi Asli:
Judul Asli
Hak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Nonsquamous Cell Malignant Tumours of The Oral Cavity: An Overview
Diunggah oleh
ranggadrHak Cipta:
Format Tersedia
C
L I N I C A L
R A C T I C E
Nonsquamous Cell Malignant Tumours
of the Oral Cavity: An Overview
Tom Daley, DDS, MSc, FRCD(C)
Mark Darling, BChD, MSc (Dent), MSc (Med), MChD
A b s t r a c t
Many malignant tumours other than squamous cell carcinoma may present in the oral cavity. Melanomas of the oral
cavity are usually pigmented, aggressive tumours associated with a poor prognosis. Neoplasms of the minor
salivary glands have a greater tendency to be malignant than those of the major glands, and some exhibit a predilection for occurring in the mouth. Many types of connective tissue malignant tumours (sarcomas) may arise in the
mouth, including soft-tissue cancers and lesions of hematologic cells such as lymphoma, whereas osteosarcoma is
the most common malignancy of the hard tissues found in the mouth. Cancers from distant organs such as breast,
lung and prostate may metastasize to the oral cavity. This paper presents a brief overview of nonsquamous cell oral
cancers, with emphasis on those most likely to be encountered by the practising dentist.
MeSH Key Words: diagnosis, differential; mouth neoplasms/epidemiology; mouth neoplasms/pathology
J Can Dent Assoc 2003; 69(9):57782
This article has been peer reviewed.
lthough squamous cell carcinoma accounts for
approximately 90%1 to 94%2 of malignant
tumours of the oral cavity, many other types of
malignant lesions, including melanoma, carcinomas of the
salivary glands, sarcomas of soft and hard connective
tissues, and metastatic cancers, are also encountered. The
clinical presentation of these lesions, their treatment and
the prognosis is highly variable, depending on the type of
tumour, its histologic variant and grade, and the extent of
spread at the time of biopsy. Table 1 lists the more common
of these oral cancers. Any of these nonsquamous cell
cancers may be encountered by the practising dentist.
Selected entities are briefly reviewed in this article.
Melanoma
Melanoma is a malignant tumour of the melanocytes,
the cells that produce brown pigmentation in the epithelia.
Consequently, most (though not all) melanomas appear as
irregular brown to black pigmentation of the affected area.
Although lesions may be flat and painless during the early
stages, there is often associated nodularity, induration and
ulceration at the time of biopsy. The palate and maxillary
gingiva of middle-aged and older adults, men more often
than women, are the most common sites for oral
Journal of the Canadian Dental Association
melanoma.3 Rapid growth, bone invasion and metastasis to
adjacent lymph nodes or distant organs are characteristic of
this aggressive cancer. Microscopically, the tumours consist
of theques and sheets of malignant cells, usually containing
melanin pigmentation, invading both the epithelium and
(eventually) the underlying connective tissues. Diagnosis of
nonpigmented melanomas can be confirmed immunohistochemically. Treatment is radical surgery, including block
removal of portions of the jaws when bone is involved.
Regional lymph node dissection may be necessary. The
prognosis is poor,1 with 10-year survival less than 30%.2
Salivary Gland Carcinomas
The oral cavity contains hundreds of minor salivary
glands below the oral epithelium as well as 3 pairs of major
salivary glands. Although malignant tumours may be seen
anywhere that salivary glands occur, they have a predilection for the slope of the hard palate and the soft palate and
occur only rarely in the lower lip. Proportionately more
malignant tumours occur in the minor salivary glands than
in the major glands.
There are many types of salivary gland cancers4
(Table 2), but most are too rare to warrant review. The most
common malignant tumours of the intraoral salivary glands
October 2003, Vol. 69, No. 9
577
Daley, Darling
Table 1 Oral cancers other than squamous cell carcinoma
Cells or tissue of origin
Cancer name
Usual age group
Prognosis
Melanocytes
Melanoma
Adults
Very poor
Salivary glands
Many types
Adults
Good to poor
Fibroblasts
Fibrosarcoma
Malignant fibrous histiocytoma
Young adults
Older adults
Intermediate to poor
Intermediate to poor
Myofibroblasts
Myofibrosarcoma
Adults
Intermediate to poor
Fat cells
Liposarcoma
Adults
Intermediate to poor
Skeletal muscle
Rhabdomyosarcoma
Children and adolescents
Intermediate
Smooth muscle
Leiomyosarcoma
Adults
Poor
Peripheral nerves
Neurosarcoma
Malignant granular cell tumour
Young adults
Adults
Very poor to poor
Poor
Synovial cells
Synovial sarcoma
Adolescents and young adults
Poor
Endothelial cells
Angiosarcoma
AIDS-related Kaposis sarcoma
Classic Kaposis sarcoma
Elderly people
Young adults
Elderly men
Very poor
Poor
Good
Lymphocytes
Lymphoma
Adults and children
Good, intermediate or poor
Plasma cells
Plasmacytoma
Multiple myeloma
Adults
Older adults
Good to intermediate
Poor to very poor
Bone cells
Osteosarcoma
Parosteal osteosarcoma
Children and young adults
Children and adults
Intermediate to poor
Good
Cartilage cells
Chondrosarcoma
Adults
Intermediate
Odontogenic cells
Various carcinomas and sarcomas
Adults
Poor
Metastatic tumours
Breast, lung, prostate, kidney, thyroid
Leukemic infiltrate
Adults
Children and adults
Very poor
Variable
Table 2 Carcinomas of the salivary glands
Relative intraoral
frequency
Prognosis
Mucoepidermoid
carcinoma
Common
Good
Adenoid cystic carcinoma
Common
Intermediate
to poor
Polymorphous low-grade
adenocarcinoma
Common
Good
Acinic cell carcinoma
Rare
Good to
intermediate
Carcinoma ex pleomorphic
adenoma
Rare
Poor
Uncommon
Poor
Epithelial myoepithelial
carcinoma
Rare
Intermediate
Clear cell carcinoma
Rare
Intermediate
Salivary duct carcinoma
Rare
Poor
Basal cell adenocarcinoma
Rare
Intermediate
Undifferentiated carcinoma
Rare
Poor
Very rare
Variable
Tumour
Adenocarcinoma
Others
578
October 2003, Vol. 69, No. 9
are mucoepidermoid carcinoma, adenoid cystic carcinoma
and polymorphous low-grade adenocarcinoma.
Mucoepidermoid Carcinoma
Mucoepidermoid carcinoma is most often a low-grade
lesion composed of well-differentiated mucous cells and
epidermoid cells, often forming cystic spaces but invading
adjacent tissues without encapsulation. It occurs over a wide
age range in both males and females, including children.
A typical low-grade lesion presents as a fluctuant, bluish,
poorly defined, painless and slow-growing subepithelial
mass, sometimes mimicking a mucocele or mucous retention cyst (Figs. 1a and 1b). Treatment is by surgical excision, and the prognosis for low-grade lesions is excellent,
with a cure rate of over 90%.2 Intermediate-grade lesions
are more aggressive, whereas high-grade lesions, although
rare, carry a grave prognosis.5
Adenoid Cystic Carcinoma
Perineural invasion is a hallmark of adenoid cystic
carcinoma, which is composed of masses of basaloid
neoplastic myoepithelial cells containing occasional ductal
structures and typically forming a cribriform growth
pattern. It usually presents as a slowly growing, firm,
poorly defined, subepithelial mass, sometimes associated
Journal of the Canadian Dental Association
Nonsquamous Cell Malignant Tumours of the Oral Cavity
Others
Other malignant tumours of the
salivary gland are listed in Table 2,
along with their prognoses. These are
usually seen in the parotid or
submandibular glands and uncommonly or rarely affect the oral cavity.4
Soft-Tissue Sarcomas
Malignant tumours arising from
the connective tissues, including
any of the connective tissues of
the maxillofacial complex, are
called sarcomas. Oral sarcomas
include fibrosarcoma, liposarcoma,
rhabdomyosarcoma, leiomyosarcoma,
angiosarcoma, neurosarcoma8 and
malignant tumours of the hematologic
tissues such as lymphoma,9 myeloma
and leukemia.2 Most of these are rarely
encountered in the oral cavity, but
some are more frequent. Most types
of sarcomas appear clinically as
Figure 2a: Kaposis sarcoma in a 28-yearFigure 2b: Microscopically, the tumours
subepithelial nodules of variable
old HIV-positive man who presented with
were composed of sheets of spindle-shaped
growth rate, forming infiltrating
multifocal flat to nodular purple lesions of
endothelial cells associated with hemthe facial skin and oral mucous
orrhage. (Hematoxylin and eosin, 200.)
masses that may be associated with
membranes. Facial (black arrow), palatal
ulceration. Microscopic examination
and tongue (white arrow) lesions are
is necessary for diagnosis since the
illustrated.
clinical characteristics are too vague
with pain or paresthesia related to the perineural invasion.6
for precise recognition. Microscopy of soft-tissue sarcomas
is sometimes difficult, and adjunctive immunohistochemiPalatal lesions may exhibit bone invasion and destruction.
cal studies may be required for better definition. Treatment
Middle-aged and older individuals are affected most often.
ranges from local surgical excision to a combination of
Treatment is by surgical excision with or without therapeusurgery, radiation and chemotherapy. The prognosis
tic radiation, but recurrence is common, and distant metasdepends on the type, histologic variant and grade, and stage
tases may occur late in the disease process. Short-term
of the tumour.8 The more common soft-tissue sarcomas are
(5-year) prognosis is good (70%), but long-term survival
reviewed here.
(to 20 years) is poor (20% to 30%), a reflection of the
Malignant Fibrous Histiocytoma
tumours persistence and recurrence.2
Cells producing malignant fibrous histiocytomas
exhibit
both fibroblastic and histiocytic characteristics on
Polymorphous Low-Grade Adenocarcinoma
microscopic
examination. There are a variety of growth
Polymorphous low-grade adenocarcinoma is a lowpatterns, the most characteristic being the presence of
grade malignant tumour seen most often at the junction of
swirled fascicles of spindle-shaped cells with associated
the hard and soft palate in older men and women.
vascularity and polygonal cells or giant cells.8 Most such
Clinically, it presents as a slow-growing, painless mass that
tumours occur in older individuals as firm, pink, occasionmay erode adjacent bone. Microscopically, it is composed
ally ulcerated subepithelial masses that may be painful.
Treatment is by radical surgical excision. Recurrence and
of both ductal and myoepithelial elements exhibiting a varimetastasis occur in about 40% of cases,2 and death may
7
ety of growth patterns and invading adjacent tissues. Wide
ensue.
surgical excision is the treatment of choice. Local recurrence is reported in up to 17% of cases,1 metastasis to
AIDS-related Kaposis Sarcoma
regional lymph nodes is uncommon (less than 10% of
The AIDS epidemic has brought a new type of
Kaposis
sarcoma, which occurs only in HIV-infected
cases), and death from the tumour is rare.
Figure 1a: Mucoepidermoid carcinoma in a
61-year-old man who presented with a
painless, slowly growing, slightly bluish
mass of the soft palate.
Journal of the Canadian Dental Association
Figure 1b: Microscopic examination showed
well-differentiated mucous cells (m) and
epidermoid cells (e), with cyst formation,
characteristic of low-grade mucoepidermoid
carcinoma. (Hematoxylin and eosin, 200.)
October 2003, Vol. 69, No. 9
579
Daley, Darling
Figure 3a: Lymphoma in a 79-year-old
woman who presented with a rubbery,
painless mass that was moulded to
accommodate the buccal surface of her
upper denture.
Figure 3b: A biopsy showed the presence of
sheets of atypical lymphocytes infiltrating
and displacing the normal tissues. Here, the
tumour is strangling a peripheral nerve (n)
seen across the centre of the photomicrograph. (Hematoxylin and eosin, 200.)
persistently and may become so large
that they interfere with oral function.
The cancer invades the jaw bones,
causing loosening or exfoliation of
teeth. Widespread dissemination to
other organs and lymph nodes is
common. Microscopically, the tumours
are composed of sheets of spindle cells
associated with hemorrhage and
hemosiderin. Diagnosis may be
assisted by vascular markers, which are
identified immunohistochemically.
Treatment is usually palliative, involving radiation and chemotherapy to
control but not cure the growth.
Affected patients usually die of other
causes, such as disseminated infections,
before succumbing to the Kaposis
sarcoma.
Non-Hodgkins Lymphoma
Non-Hodgkins lymphomas occurring in the mouth usually present as
red or purple extranodal rubbery
Figure 4b: A biopsy of the lesion showed a
Figure 4a: Osteosarcoma in a 36-year-old
masses, most commonly occurring on
malignant bone-producing tumour (arrow)
woman who complained of discomfort and
the palatal mucosa, buccal vestibule or
characteristic of osteosarcoma. (Hematoxylin
pain of the left posterior mandible. A mobile
and eosin, 300.)
second molar was extracted, but the
gingiva in middle-aged and older
symptoms did not resolve. The radiograph
patients. Lymphoma may also present
illustrates a poorly defined radiolucency
within the jaw bones, producing a
with vague internal radiopacities.
ragged radiolucency with vague pain
or paresthesia and eventual cortical
expansion or perforation (or both).
There may be associated enlargement
of the cervical lymph nodes, and the
patient may have symptoms such as
fatigue, weight loss and night sweats.
Biopsy is necessary to establish a diagnosis of non-Hodgkins lymphoma and
to further characterize the specific type,
Figure 5: Metastatic disease in a 32-yearFigure 4c: Parosteal osteosarcoma in a 34usually by identification of immunohisold woman who complained of paresthesia
year-old woman in whom a painless, bony,
tochemical markers or gene rearrangeof the right lower lip and chin. A radiohard, progressively enlarging nodule of the
ment studies (or both). Determining
graph revealed multifocal radiolucencies
maxillary alveolus developed. A radiograph
mimicking periapical disease (arrows), but
showed an exophytic radiopaque mass
the specific type of non-Hodgkins
the teeth were vital. A biopsy showed
extending from the cortical bone and not
lymphoma is extremely important
metastatic breast carcinoma.
involving the trabecular bone. Microscopic
because lymphomas exhibit a wide
examination revealed a well-differentiated
osteosarcoma.
range of aggressiveness and response
to treatment.9 In 85% of cases, oral
lymphomas are composed of masses of B cells (small, large or
individuals. The oral and maxillofacial region is commonly
both)2 in a diffuse or follicular pattern associated with interaffected by this malignant tumour of the endothelial cells,
mediate-grade malignant behaviour (Figs. 3a and 3b).
which has a strong etiologic association with human
10
Treatment
for intermediate-grade and high-grade lesions
herpesvirus 8. It presents initially as multifocal purple
consists of radiation with or without multiagent chemothermacules that soon develop into painful, bleeding, someapy, whereas low-grade lesions may not be treated at all. The
times necrotic nodular masses on the skin and oral mucous
prognosis depends on the specific type of lymphoma and the
membranes (Figs. 2a and 2b). These lesions grow
580
October 2003, Vol. 69, No. 9
Journal of the Canadian Dental Association
Nonsquamous Cell Malignant Tumours of the Oral Cavity
Table 3 Examples of very rare oral cancers
Alveolar soft parts sarcoma
Ewings sarcoma
Hodgkins disease (Hodgkins lymphoma)
Acute disseminated Langerhans cell histiocytosis
(LettererSiwe disease)
Mycosis fungoides
T cell lymphomas
Merkle cell carcinoma
Primitive neuroendocrine tumour
Neuroblastoma
Malignant triton tumour
Malignant teratoma
Inflammatory pseudotumour/sarcoma
extent of spread, with median survival of 8 to 10 years
or more for low-grade tumours but 60% mortality within
5 years for high-grade lesions.2 Burkitts lymphoma, a
high-grade tumour seen more commonly in Africa than in
North America, has a predilection for the head and neck in
children.1
Neurofibrosarcoma
Neurofibrosarcomas, also known as malignant peripheral nerve sheath tumours, malignant schwannomas
and neurosarcomas, account for about 10% of soft-tissue
sarcomas, and approximately half of these lesions occur in
the setting of neurofibromatosis type 1 (NF1). Neurofibrosarcomas occur only rarely in the head and neck region
and are most common in young adults (mean age 40 to
46 years). The mean age of occurrence in patients with
neurofibromatosis is 29 to 36 years, although such lesions
have been described in younger patients.11 Malignant
transformation usually occurs in association with a large,
diffuse neurofibroma in cases of NF1. In the oral regions,
the mandible, lips and buccal mucosa are most commonly
involved. The tumours present as rapidly enlarging masses,
sometimes with associated pain. Radiographs may show
widening of the inferior alveolar canal, with or without
destruction of surrounding bone and involvement of the
inferior alveolar nerve. Microscopically the tumour shows
fascicles of atypical spindle-shaped cells, which may resemble those of fibrosarcoma but which are usually more irregular, with wavy or comma-shaped nuclei. Some less cellular
myxoid areas may also be seen. Positive immunostaining
for S100 protein is often helpful, but a definitive diagnosis
of neural origin is often difficult.2 The prognosis for
patients with neurofibrosarcoma arising de novo is about
50% for 5-year survival, whereas it is 15% for neurofibrosarcoma arising in cases of neurofibromatosis.2
Hard-Tissue Sarcomas
Osteosarcoma and chondrosarcoma of the jaws are the
2 types of hard-tissue malignant tumours that occur in the
Journal of the Canadian Dental Association
mouth. Malignant odontogenic tumours involving hardtissue production (dentin, enamel) are extremely rare.
Osteosarcoma
Malignancy of bone-forming cells may occur in the
maxilla or the mandible. Jaw osteosarcoma usually affects
adolescents and young to middle-aged adults of both sexes;
either jaw may be affected, but there is a predilection for
the mandible.12 Osteosarcoma presents as a moderate- to
fast-growing, asymmetric, often painful enlargement of the
bone with invasion of the antrum in maxillary lesions.
Teeth may become loose or displaced. Radiographically,
there may be widening of the periodontal ligament in the
early stages, associated with irregular mixed radiolucency or
radiopacity. In some cases there is a sunburst periosteal
reaction as the tumour mass expands through cortical bone.
Microscopically, there are masses of polygonal or spindleshaped cells associated with highly variable amounts of
osteoid, some of which is calcified (Figs. 4a and 4b). The
tumour is invasive and may hematogenously metastasize to
distant sites such as lung and brain. Treatment is by radical
surgical resection. Adjuvant chemotherapy may also be
effective in reducing the risk of death. The prognosis for
affected patients is poor, with 5-year survival rates ranging
from 30% to 50%.2
Osteosarcoma sometimes arises from the cortex rather
than from cells deep within the bone. These juxtacortical
osteosarcomas (Fig. 4c), most commonly of the parosteal
type, present as exophytic, hard, slow-growing masses.
They are typically better differentiated than intrabony
tumours, and the prognosis is good with local surgical
excision.2
Chondrosarcoma
Chondrosarcomas are rare, slow-growing cartilageforming tumours that usually occur in the maxilla of
middle-aged and older individuals, but which are sometimes observed in young patients. Radical surgical excision
is the treatment of choice. Short-term (5-year) prognosis is
good, but recurrence is common, and the long-term
prognosis is variable and depends on a variety of factors.1,2
Metastatic Tumours
Tumours from other organs and body parts may metastasize to the jaw bones and oral soft tissues by either the
lymphatic or blood vascular systems. Metastatic tumours
may present in adults as one or more soft-tissues nodules,
which are painless but which have persistent growth. They
may eventually induce painful ulceration of the soft tissues.
More commonly, metastases present within the jaws,
especially the posterior mandible (Fig. 5). They are often
discovered when teeth become loose or painful; in such
cases, radiography will show one or more irregular, motheaten radiolucencies. Unilateral numbness of the chin is a
October 2003, Vol. 69, No. 9
581
Daley, Darling
frequent symptom of mandibular metastatic lesions. Some
tumours, such as prostatic carcinoma and some breast carcinomas, may induce bone formation, producing a mixed
opaque and lucent radiographic appearance. Carcinomas
metastasize to the jaws far more frequently than sarcomas
do. The most common metastatic tumours found in the
oral tissues are carcinoma of lung and adenocarcinoma of
breast, prostate, kidney and thyroid.1 Metastasis to the
maxillofacial region is a grave prognostic sign, suggesting
disseminated metastasis. Most patients die within 1 year.2
Other Cancers
Cancers arising from the odontogenic apparatus are
very rare.13 The most common is ameloblastic carcinoma,
which occurs in older individuals, causing destruction of
the jaw, usually the posterior mandible. The prognosis is
poor. The discussion of other odontogenic carcinomas and
sarcomas13 is beyond the scope of this paper.
Other malignant tumours (Table 3) rarely affect the
oral regions.
7. Regezi JA, Zarbo RJ, Stewart JC, Courtney RM. Polymorphous lowgrade adenocarcinoma of minor salivary gland. A comparative histologic
and immunohistochemical study. Oral Surg Oral Med Oral Pathol 1991;
71(4):46975.
8. Weiss SW, Goldblum JR. Enzinger and Weisss soft tissue tumors.
4th ed. St Louis: Mosby; 2001. Ch. 15, 25.
9. Harris NL, Jaffe ES, Stein H, Banks PM, Chan JK, Cleary ML, and
others. A revised European-American classification of lymphoid
neoplasms: a proposal from the International Lymphoma Study Group.
Blood 1994; 84(5):136192.
10. Flaitz CM, Jin YT, Hicks MJ, Nichols CM, Wang YW, Su IJ. Kaposis
sarcoma-associated herpesvirus-like DNA sequences (KSHV/HHV-8) in
oral AIDS-Kaposis sarcoma. A PCR and clinicopathologic study.
Oral Surg Oral Med Oral Pathol Oral Radio Endod 1997; 83(2):25964.
11. Allen CM, Miloro M. Gingival lesion of recent onset in a patient with
neurofibromatosis. Oral Surg Oral Med Oral Pathol Oral Radio Endod
1997; 84(6):5957.
12. Bennett JH, Thomas G, Evans AW, Speight PM. Osteosarcoma of the
jaws: a 30-year retrospective review. Oral Surg Oral Med Oral Pathol Oral
Radio Endod 2000; 90(3):32332.
13. Sciubba JJ, Fantasia JE, Kahn LB. Tumors and cysts of the jaws.
Washington: AFIP; 2001. p. 768, Ch. 6.
Conclusions
Dental personnel cannot be expected to know the
details of all types of cancers that may affect the maxillofacial region. They should, however, be aware that such
lesions exist and should have some knowledge of those that
are most likely to be encountered. C
Acknowledgement: The authors with to thank Dr. G.P. Wysocki for
contributing the photomicrographs.
Dr. Daley is professor and chair of oral pathology, department of
pathology, division of oral pathology, University of Western Ontario,
London, Ontario.
Dr. Darling is assistant professor, oral pathology, department of oral
pathology, division of oral pathology, University of Stellenbosch,
Cape Town, South Africa.
Correspondence to: Dr. Tom Daley, Department of Pathology,
University of Western Ontario, London, ON N6A 5C1. E-mail:
tdaley@uwo.ca.
The authors have no declared financial interests.
References
1. Sapp JP, Eversole LR, Wysocki GP. Contemporary oral and maxillofacial pathology. St Louis: Mosby; 1997. p. 174, 18993, 4034.
2. Neville BW, Damm DD, Allen CM, Bouquot JE. Oral & maxillofacial
pathology. 2nd ed. Philadelphia: WB Saunders Co; 2002. p. 356,
37680, 42030, 48090, 51724, 57480, 5823.
3. Gorsky M, Epstein JB. Melanoma arising from the mucosal surfaces of
the head and neck. Oral Surg Oral Med Oral Pathol Oral Radio Endod
1998; 86(6):7159.
4. Dardick I. Color atlas/text of salivary gland tumor pathology.
New York: Igaku-Shoin Medical Publishers Inc; 1996. Ch. 1624.
5. Auclair PL, Goode RK, Ellis GL. Mucoepidermoid carcinoma of
intraoral salivary glands. Evaluation and application of grading criteria in
143 cases. Cancer 1992; 69(8):202130.
6. van der Wal JE, Snow GB, van der Waal I. Intraoral adenoid cystic
carcinoma. The presence of perineural spread in relation to site, size, local
extension, and metastatic spread in 22 cases. Cancer 1990; 66(9):20313.
582
October 2003, Vol. 69, No. 9
Journal of the Canadian Dental Association
Anda mungkin juga menyukai
- Download 12,000 Shed PlansDokumen27 halamanDownload 12,000 Shed PlansRadu_IS100% (2)
- Medical CertificationDokumen4 halamanMedical CertificationranggadrBelum ada peringkat
- Anatomy 090819Dokumen30 halamanAnatomy 090819Vaishnavi GourabathiniBelum ada peringkat
- Book of Lost Spells (Necromancer Games)Dokumen137 halamanBook of Lost Spells (Necromancer Games)Rodrigo Hky91% (22)
- PPC2000 Association of Consultant Architects Standard Form of Project Partnering ContractDokumen5 halamanPPC2000 Association of Consultant Architects Standard Form of Project Partnering ContractJoy CeeBelum ada peringkat
- Malignant Epithelial Non-Odontogenic Tumors 2Dokumen11 halamanMalignant Epithelial Non-Odontogenic Tumors 2samamustafa.2003Belum ada peringkat
- Neoplasia (II) : Department of Pathology, Sun Yat-Sen UniversityDokumen138 halamanNeoplasia (II) : Department of Pathology, Sun Yat-Sen UniversityleyreaBelum ada peringkat
- Aruns PL - Ade FinalDokumen9 halamanAruns PL - Ade FinaldrarunsinghBelum ada peringkat
- Oral SCCDokumen10 halamanOral SCCيونس حسينBelum ada peringkat
- Neoplasms Ear CanalDokumen12 halamanNeoplasms Ear CanalannaBelum ada peringkat
- Sheet 11 PDFDokumen16 halamanSheet 11 PDFHanin AbukhiaraBelum ada peringkat
- Squamous Cell Carcinoma-Well DifferentiatedDokumen4 halamanSquamous Cell Carcinoma-Well DifferentiatedYukankolmi OyoBelum ada peringkat
- Skin Cancers: Assistant Larisa PoroshinaDokumen42 halamanSkin Cancers: Assistant Larisa PoroshinaMed PoxBelum ada peringkat
- Salivary Gland Tumors: 1. AdenomasDokumen18 halamanSalivary Gland Tumors: 1. AdenomasMahammed Ahmed BadrBelum ada peringkat
- Randall 1996Dokumen21 halamanRandall 1996agita kartika sariBelum ada peringkat
- HEAD AND NECK 1.robbins & Cotran Pathologic Basis of Disease ReviewerDokumen14 halamanHEAD AND NECK 1.robbins & Cotran Pathologic Basis of Disease ReviewerSeff Causapin100% (1)
- Current Controversies in The Management of Malignant Parotid TumorsDokumen8 halamanCurrent Controversies in The Management of Malignant Parotid TumorsDirga Rasyidin LBelum ada peringkat
- Practice Essentials: View Media GalleryDokumen8 halamanPractice Essentials: View Media GallerywzlBelum ada peringkat
- Common Malignant Salivary Gland Epithelial TumorsDokumen39 halamanCommon Malignant Salivary Gland Epithelial TumorsJesús De Santos AlbaBelum ada peringkat
- 1 Tmu - JD - 039Dokumen4 halaman1 Tmu - JD - 039Hasan BlackBelum ada peringkat
- 1 Tmu - JD - 039 PDFDokumen4 halaman1 Tmu - JD - 039 PDFKristina SabuBelum ada peringkat
- Soft Tissue TumorDokumen67 halamanSoft Tissue TumorVincentius Michael WilliantoBelum ada peringkat
- Malignant Melanoma of Oral Cavity PDFDokumen3 halamanMalignant Melanoma of Oral Cavity PDFahmed shimalBelum ada peringkat
- Basal Cell Carcinoma - Pathophysiology and ManagementDokumen6 halamanBasal Cell Carcinoma - Pathophysiology and ManagementReylan Garcia0% (1)
- Slide 15 Diseases of Salivary Glands IIDokumen64 halamanSlide 15 Diseases of Salivary Glands IIJustDen09100% (1)
- Jurnal 1Dokumen8 halamanJurnal 1LuthfianaBelum ada peringkat
- Clinical Case CAPDokumen82 halamanClinical Case CAPIna GargBelum ada peringkat
- Parotid Gland Tumor Case ReportDokumen4 halamanParotid Gland Tumor Case ReportmitaBelum ada peringkat
- Oral Cancer MADE EASYDokumen19 halamanOral Cancer MADE EASYMohammedBelum ada peringkat
- Clinically, These Lesions All Form Pinkish Nodules Unless The Surface Has Been InjuredDokumen28 halamanClinically, These Lesions All Form Pinkish Nodules Unless The Surface Has Been Injuredreal_septiady_madrid3532Belum ada peringkat
- Oral and Maxillofacial Surgery/fifth Year: The Natural History of Oral SCCDokumen25 halamanOral and Maxillofacial Surgery/fifth Year: The Natural History of Oral SCCAbdullah Muhammed khaleel HassanBelum ada peringkat
- Neoplasia 1Dokumen14 halamanNeoplasia 1Omar MaanBelum ada peringkat
- Lec. 8 Malignant Bone TumorsDokumen17 halamanLec. 8 Malignant Bone Tumorsنور كاضمBelum ada peringkat
- Odontogenic Tumor: Oral PathologyDokumen17 halamanOdontogenic Tumor: Oral PathologyJoker KillerBelum ada peringkat
- Intraoral Benign TumorsDokumen4 halamanIntraoral Benign TumorsSaman SadeghiBelum ada peringkat
- Squamous Cell Carcinoma of the Oral Cavity: Etiology, Clinical Features, Diagnosis and ManagementDokumen5 halamanSquamous Cell Carcinoma of the Oral Cavity: Etiology, Clinical Features, Diagnosis and ManagementNuman QureshiBelum ada peringkat
- Davars LOM Vol 2Dokumen163 halamanDavars LOM Vol 2Sridhar SriBelum ada peringkat
- Conjunctival Pigmented LesionsDokumen0 halamanConjunctival Pigmented LesionsBhartendu AgarwalBelum ada peringkat
- Bone tm3Dokumen57 halamanBone tm3ZakiyahulfahdwBelum ada peringkat
- PA 29 Testicular TumorsDokumen46 halamanPA 29 Testicular TumorsFangBelum ada peringkat
- Skin Cancer Types, Risk Factors, Diagnosis & TreatmentDokumen53 halamanSkin Cancer Types, Risk Factors, Diagnosis & TreatmentMohammadSAL-RawashdehBelum ada peringkat
- Head and Neck: Salivary Gland Tumors: An OverviewDokumen12 halamanHead and Neck: Salivary Gland Tumors: An OverviewVanessa MordiBelum ada peringkat
- Servix Squamous Intraepithelial Lesion (SIL) Squamous Intraepithelial Lesion (SIL) Is The Abnormal Growth of Squamous Cells OnDokumen6 halamanServix Squamous Intraepithelial Lesion (SIL) Squamous Intraepithelial Lesion (SIL) Is The Abnormal Growth of Squamous Cells OnJenylia HapsariBelum ada peringkat
- Fibrosarcoma Differential DiagnosisDokumen10 halamanFibrosarcoma Differential DiagnosisdmdsahBelum ada peringkat
- CH15 Patho D&R AgamDokumen11 halamanCH15 Patho D&R AgamBio CheBelum ada peringkat
- Referat Bedah - QuwDokumen14 halamanReferat Bedah - QuwSaniaty TuankottaBelum ada peringkat
- Oral Pathology Lec - 1Dokumen11 halamanOral Pathology Lec - 1مصطفى محمدBelum ada peringkat
- Giant Cell Lesions of Oral CavityDokumen4 halamanGiant Cell Lesions of Oral CavityPreetam PatnalaBelum ada peringkat
- Tumor of The EyeDokumen40 halamanTumor of The EyeGustiAngriAngalanBelum ada peringkat
- Data SCC From InternetDokumen3 halamanData SCC From InternetristaniatauhidBelum ada peringkat
- Malignant NeoplasmsDokumen59 halamanMalignant NeoplasmsRosa Gusmi PutriBelum ada peringkat
- Basal Cell CarcinomaDokumen1 halamanBasal Cell CarcinomaMuhammad Alief FahrenBelum ada peringkat
- Managing Malignant Melanoma: Learning Objectives: After Reading This Article, The Participant Should Be AbleDokumen15 halamanManaging Malignant Melanoma: Learning Objectives: After Reading This Article, The Participant Should Be AbleDian Ariska SBelum ada peringkat
- 8 Diseases of Infancy and ChildhoodDokumen23 halaman8 Diseases of Infancy and ChildhoodBalaji DBelum ada peringkat
- Tumores OdontogenicDokumen17 halamanTumores OdontogenicrachmaniabudiatiBelum ada peringkat
- Case StudyDokumen18 halamanCase StudyKristine Joy RevañoBelum ada peringkat
- Publications 011Dokumen4 halamanPublications 011utamiBelum ada peringkat
- Case Report: Primary Malignant Melanoma of Maxilla: Report of A Case With DiscussionDokumen5 halamanCase Report: Primary Malignant Melanoma of Maxilla: Report of A Case With DiscussionGina Kristina NanginBelum ada peringkat
- Soft Tissues PathologyDokumen53 halamanSoft Tissues PathologyWz bel DfBelum ada peringkat
- Cancer of The PenisDokumen6 halamanCancer of The PenisPaul CenabreBelum ada peringkat
- Malignant Tumors: Dr.N.Govindrajkumar Reader Dept - Oral &maxillo Facial PathologyDokumen50 halamanMalignant Tumors: Dr.N.Govindrajkumar Reader Dept - Oral &maxillo Facial PathologypriyaBelum ada peringkat
- Diseases of The Salivary GlandDokumen14 halamanDiseases of The Salivary Glandsaurabhv89Belum ada peringkat
- Tumor Suzne Zlijezde AAODokumen4 halamanTumor Suzne Zlijezde AAOJovan PopovićBelum ada peringkat
- Salivary Gland Cancer: From Diagnosis to Tailored TreatmentDari EverandSalivary Gland Cancer: From Diagnosis to Tailored TreatmentLisa LicitraBelum ada peringkat
- 2012 11 03 Raphael Chee Radiotherapy in Cervix and UterineDokumen29 halaman2012 11 03 Raphael Chee Radiotherapy in Cervix and UterineranggadrBelum ada peringkat
- PDFDokumen70 halamanPDFranggadrBelum ada peringkat
- Guidelines For Glaucoma PDFDokumen69 halamanGuidelines For Glaucoma PDFhelviaseptariniBelum ada peringkat
- Figo Igcs StagingDokumen88 halamanFigo Igcs StagingranggadrBelum ada peringkat
- Guidelines For Medical Practitioners On Certificates Certifying Illness 2011Dokumen3 halamanGuidelines For Medical Practitioners On Certificates Certifying Illness 2011ranggadrBelum ada peringkat
- Benign & Malignant Tumours of Oral CavityDokumen11 halamanBenign & Malignant Tumours of Oral CavityranggadrBelum ada peringkat
- Cervical CancerDokumen60 halamanCervical CancerNova Yuli PrasetyoBelum ada peringkat
- Cervical Cancer: Prevention, Diagnosis, and TherapeuticsDokumen23 halamanCervical Cancer: Prevention, Diagnosis, and TherapeuticsranggadrBelum ada peringkat
- PDFDokumen25 halamanPDFTruly GracevaBelum ada peringkat
- Dentistry Spid Oral Cancer 1039Dokumen5 halamanDentistry Spid Oral Cancer 1039ranggadrBelum ada peringkat
- PDFDokumen57 halamanPDFranggadrBelum ada peringkat
- Handbook On Medical Certification of Death: Prepared For: Registered Nurses (Extended Class)Dokumen33 halamanHandbook On Medical Certification of Death: Prepared For: Registered Nurses (Extended Class)ranggadrBelum ada peringkat
- PDFDokumen25 halamanPDFTruly GracevaBelum ada peringkat
- 08Dokumen7 halaman08ranggadrBelum ada peringkat
- TerminologyDokumen7 halamanTerminologyranggadrBelum ada peringkat
- 31752Dokumen19 halaman31752ranggadrBelum ada peringkat
- Medical Certificate Guidelines June 2012Dokumen3 halamanMedical Certificate Guidelines June 2012wudthipanBelum ada peringkat
- Guidelines Medical Certificates ReportsDokumen36 halamanGuidelines Medical Certificates ReportsranggadrBelum ada peringkat
- Medical certificates standardsDokumen15 halamanMedical certificates standardsranggadrBelum ada peringkat
- Medcert July 2010Dokumen15 halamanMedcert July 2010ranggadrBelum ada peringkat
- 66 240 1 PBDokumen7 halaman66 240 1 PBranggadrBelum ada peringkat
- HB CodDokumen65 halamanHB CodranggadrBelum ada peringkat
- Medical AspectsDokumen75 halamanMedical AspectsranggadrBelum ada peringkat
- AKUPUNCTUR VS ONDANSETRONDokumen7 halamanAKUPUNCTUR VS ONDANSETRONDiyah RahmawatiBelum ada peringkat
- Journal of Orthopaedic Surgery and Research: Tibial Shaft Fractures in Football PlayersDokumen5 halamanJournal of Orthopaedic Surgery and Research: Tibial Shaft Fractures in Football PlayersranggadrBelum ada peringkat
- Achot 2012 6 499 505Dokumen7 halamanAchot 2012 6 499 505ranggadrBelum ada peringkat
- 978 951 44 8360 8Dokumen179 halaman978 951 44 8360 8ranggadrBelum ada peringkat
- Orthopaedics and Traumatology: Skeletal Traction TechniquesDokumen33 halamanOrthopaedics and Traumatology: Skeletal Traction TechniquesranggadrBelum ada peringkat
- Cloud Security Training and Awareness Programs For OrganizationsDokumen2 halamanCloud Security Training and Awareness Programs For OrganizationsdeeBelum ada peringkat
- Rock Laboratory PricelistDokumen1 halamanRock Laboratory PricelistHerbakti Dimas PerdanaBelum ada peringkat
- Echt Er Nacht 2014Dokumen8 halamanEcht Er Nacht 2014JamesBelum ada peringkat
- DBIRS SyllabusDokumen2 halamanDBIRS SyllabusAshitosh KadamBelum ada peringkat
- Activities/Assessments 2:: Determine The Type of Sampling. (Ex. Simple Random Sampling, Purposive Sampling)Dokumen2 halamanActivities/Assessments 2:: Determine The Type of Sampling. (Ex. Simple Random Sampling, Purposive Sampling)John Philip Echevarria0% (2)
- 740 (Q50, V40, Awa 4Dokumen10 halaman740 (Q50, V40, Awa 4rawat2583Belum ada peringkat
- Self Healing Challenge - March 2023 Workshop ThreeDokumen16 halamanSelf Healing Challenge - March 2023 Workshop ThreeDeena DSBelum ada peringkat
- 1651 EE-ES-2019-1015-R0 Load Flow PQ Capability (ENG)Dokumen62 halaman1651 EE-ES-2019-1015-R0 Load Flow PQ Capability (ENG)Alfonso GonzálezBelum ada peringkat
- History of English Prose PDFDokumen21 halamanHistory of English Prose PDFMeisyita QothrunnadaBelum ada peringkat
- Financial Services : An OverviewDokumen15 halamanFinancial Services : An OverviewAnirudh JainBelum ada peringkat
- Temptations in MinistryDokumen115 halamanTemptations in MinistryJoseph Koech100% (1)
- Dryers in Word FileDokumen5 halamanDryers in Word FileHaroon RahimBelum ada peringkat
- PS Neo HSK2LCD ICON LED RF Keypad v1 0 Installation Guide R001 en FR Es PoDokumen40 halamanPS Neo HSK2LCD ICON LED RF Keypad v1 0 Installation Guide R001 en FR Es Po7seguridadBelum ada peringkat
- Administrations whose CoCs are accepted for CECDokumen1 halamanAdministrations whose CoCs are accepted for CECGonçalo CruzeiroBelum ada peringkat
- Indian ChronologyDokumen467 halamanIndian ChronologyModa Sattva100% (4)
- Recent Developments in Ultrasonic NDT Modelling in CIVADokumen7 halamanRecent Developments in Ultrasonic NDT Modelling in CIVAcal2_uniBelum ada peringkat
- MMADDokumen2 halamanMMADHariharan SBelum ada peringkat
- WBC Study Reveals God's NatureDokumen11 halamanWBC Study Reveals God's NatureSherwin Castillo DelgadoBelum ada peringkat
- CE ProblemDokumen5 halamanCE ProblemJho FBelum ada peringkat
- Management and Breeding of Game BirdsDokumen18 halamanManagement and Breeding of Game BirdsAgustinNachoAnzóateguiBelum ada peringkat
- NewTrendsInLeadershipandManagement ArikkokDokumen32 halamanNewTrendsInLeadershipandManagement Arikkoksocofem288Belum ada peringkat
- Philip Larkin: The Art of Poetry 30Dokumen32 halamanPhilip Larkin: The Art of Poetry 30Telmo RodriguesBelum ada peringkat
- Joel Werner ResumeDokumen2 halamanJoel Werner Resumeapi-546810653Belum ada peringkat
- Math-149 MatricesDokumen26 halamanMath-149 MatricesKurl Vincent GamboaBelum ada peringkat
- D2DDokumen2 halamanD2Dgurjit20Belum ada peringkat
- What Are Universities ForDokumen19 halamanWhat Are Universities ForBikash Ranjan MishraBelum ada peringkat