Etiology and Pathogenesis of Preeclampsia: Current Concepts: Ajog Reviews
Diunggah oleh
tapayanaJudul Asli
Hak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Etiology and Pathogenesis of Preeclampsia: Current Concepts: Ajog Reviews
Diunggah oleh
tapayanaHak Cipta:
Format Tersedia
AJOG REVIEWS
Etiology and pathogenesis of preeclampsia: Current concepts
Gustaaf A. Dekker, MD, PhD, and Baha M. Sibai, MD
Amsterdam, The Netherlands, and Memphis, Tennessee
The etiology of preeclampsia is unknown. At present, 4 hypotheses are the subject of extensive investigation,
as follows: (1) Placental ischemiaIncreased trophoblast deportation, as a consequence of ischemia, may
inflict endothelial cell dysfunction. (2) Very low-density lipoprotein versus toxicity-preventing activityIn compensation for increased energy demand during pregnancy, nonesterified fatty acids are mobilized. In women
with low albumin concentrations, transporting extra nonesterified fatty acids from adipose tissues to the liver
is likely to reduce albumins antitoxic activity to a point at which very-low density lipoprotein toxicity is expressed. (3) Immune maladaptationInteraction between decidual leukocytes and invading cytotrophoblast
cells is essential for normal trophoblast invasion and development. Immune maladaptation may cause shallow invasion of spiral arteries by endovascular cytotrophoblast cells and endothelial cell dysfunction mediated by an increased decidual release of cytokines, proteolytic enzymes, and free radical species. (4)
Genetic imprintingDevelopment of preeclampsia-eclampsia may be based on a single recessive gene or a
dominant gene with incomplete penetrance. Penetrance may be dependent on fetal genotype. The possibility
of genetic imprinting should be considered in future genetic investigations of preeclampsia. (Am J Obstet
Gynecol 1998;179:1359-75.)
Key words: Preeclampsia, endothelium, etiology, immune, gene
Shallow endovascular cytotrophoblast invasion in the
spiral arteries and endothelial cell dysfunction are 2 key
features in the pathogenesis of preeclampsia, yet the etiology of preeclampsia is still unknown. Currently, 4 hypotheses are favored: placental ischemia, very low-density
lipoproteins versus toxicity preventing activity, immune
maladaptation, and genetic imprinting. For the sake of
clarity, these 4 hypotheses are described separately; however, it should be stressed that these 4 hypotheses are not
mutually exclusive but probably interactive.
Before discussing the pros and cons of these 4 hypotheses, we will briefly review the literature on uteroplacental circulation, vascular tone regulation in normal
pregnancy, and pathogenesis of the clinical syndrome.
Uteroplacental circulation
During the early weeks of gestation, cytotrophoblast
cells stream out of the tips of the anchoring villi and penetrate the trophoblast shell and the overlying syncytiotrophoblast to form cytotrophoblast columns that develop
into the cytotrophoblast shell. Trophoblast cells continue
to migrate into the decidua and eventually colonize the
placental beds myometrium. When the cytotrophoblast
From the Division of Maternal-Fetal Medicine, Department of Obstetrics
and Gynaecology, Free University Hospital, Amsterdam, and the
Division of Maternal-Fetal Medicine, Department of Obstetrics and
Gynecology, University of Tennessee, Memphis.
Reprint requests: Baha M. Sibai, MD, Department of Obstetrics and
Gynecology, 853 Jefferson Ave, Suite E102, Memphis, TN 38103.
Copyright 1998 by Mosby, Inc.
0002-9378/98 $5.00 + 0 6/1/86764
shell contacts the spiral arteries openings, trophoblast
cells stream into their lumina, where they form intraluminal plugs.1-3 Endovascular trophoblast cells replace
the endothelium of spiral arteries and then invade the
media, with resulting destruction of the medial elastic,
muscular, and neural tissue. Trophoblast cells become incorporated into the vessel wall, and in the final stages the
endothelial lining is reconstituted.1-3 Zhou et al4 demonstrated that endovascular cytotrophoblasts normally
transform their adhesion receptor phenotype so as to resemble the endothelial cells they replace, and they were
subsequently successful in demonstrating that
preeclampsia is associated with a failure of cytotrophoblasts to mimic a vascular adhesion phenotype.
Vascular changes may actually precede trophoblast invasion, suggesting that interstitial trophoblast plays a role
in inducing early disruption (probably by secreting proteolytic enzymes).3 These physiologic changes create a
low-resistance arteriolar system and an absence of maternal vasomotor control, which allows the dramatic increase in blood supply to the growing fetus. During early
stages of implantation, cytotrophoblast plugs may act as
valves regulating blood flow in the intervillous space and
protect the embryo from forceful maternal blood flow.
Results of color Doppler studies suggest that the presence of continuous intervillous space flow in the first
trimester is associated with a complicated pregnancy outcome and that a true intervillous space blood flow is established only by about 12 weeks gestation in normal
pregnancies.4-6
In preeclampsia and some cases of intrauterine growth
1359
1360 Dekker and Sibai
restriction (IUGR), physiologic changes in the spiral arteries are confined to the decidual portion of the arteries; about 30% to 50% of the placental beds spiral arteries escape entirely from endovascular trophoblast
invasion.1, 2, 7 Myometrial segments remain anatomically
intact and undilated, and adrenergic nerve supply to the
spiral arteries remains intact.2, 7 Intraluminal cytotrophoblast in spiral arteries is often identified in
preeclampsia and IUGR, unlike in normal pregnancies.2, 7
Many vessels are occluded by atherosis, with an accumulation of lipid-laden macrophages and a perivascular
mononuclear cell infiltrate. Acute atherosis and the associated thrombosis may cause placental infarctions.
Lipoprotein-a deposition is often found in association
with atherosis.8
Vascular endothelial growth factor (VEGF) and the vascular adhesion phenotype of invading cytotrophoblasts.
VEGF, a growth factor involved in angiogenesis, with a
specific action on endothelial cells, is widely expressed at
the fetomaternal interface.9 On implantation, expression is dominant in the uterine epithelial cells.
Subsequently, expression increases in the decidual
macrophages, which remain the principal source of
VEGF. First-trimester human intermediate and extravillous trophoblast has been found to express the flt receptor for VEGF. VEGF is up-regulated by hypoxia10; neovascularization induced by hypoxia corrects tissue
oxygenation, and VEGF release will be down-regulated.
This homeostatic mechanism may have particular relevance in the first trimester when oxygen tension of trophoblast villi is particularly low.4-6, 10-12 VEGF may be involved in inducing the expression of endothelial markers
by invading cytotrophoblasts. VEGF has been shown to
induce the expression of those integrins on endothelial
cells that are associated with angiogenic invasion; these
integrins are the same as those described by Zhou et al4
as being part of the de novo expression of endothelial
characteristics by invading cytotrophoblasts.
Decidual extracellular matrix and cell surface adhesion
molecules. During invasion, trophoblast cells are not cytolytic but secrete enzymes that affect the extracellular
matrix. Immunohistochemical studies have localized
plasminogen activator, as well as metalloproteinases,
which include collagenases within the extravillous trophoblast.3, 13, 14 Metalloproteinase activity is influenced
by a variety of mediators. Secretion of metalloproteinases
is plasmin dependent but is inhibited by -human chorionic gonadotropin, which would favor an autocrine regulatory system. However, interleukin-l (IL-1) is stimulatory, and because trophoblast cells release IL-1 and also
express the IL-1 receptor, there may be an autocrine
stimulatory loop.15 Another potential candidate for stimulation of type IV collagenase is tumor necrosis factor-
(TNF-).3
Cell migration is dependent on adhesion to extracellu-
November 1998
Am J Obstet Gynecol
lar matrix proteins for anchorage and traction. In addition to mediating adhesion, extracellular matrix binding
to specific transmembrane receptors also affects cell
growth and differentiation.16, 17 Also, trophoblast behavior during implantation is influenced by decidual extracellular matrix proteins.18, 19 Cells bind to extracellular
matrix proteins by appropriate surface receptors called
adhesion molecules.20 The 4 major families of adhesion
molecules are integrins, cadherins, immunoglobulin superfamily, and selectins. E-Cadherin is involved in differentiation of cytotrophoblast into syncytiotrophoblast,21
whereas integrins mediate adhesion to the extracellular
matrix.20 Integrins are transmembrane glycoproteins
consisting of noncovalently associated - and -subunits.22 Integrin ligand specificity is determined by combination of the various - and -subunits.22-26 Thus onset
of migratory or invasive behavior of trophoblast is associated with a shift in integrin expression, thereby changing the binding tendency of trophoblast from a basal
lamina (laminin) to a stromal type (fibronectin) of matrix.3, 27-31
Integrin switching by invasive cytotrophoblasts is abnormal in preeclampsia. Invading trophoblast within the
placental bed of preeclamptic patients fails to down-regulate 4 and to make the switch from 6 to 5 and 1 integrin subunits.25, 27-30 Pijnenborg et al32 observed lower
trophoblast attachment on the extracellular matrix proteins fibronectin and vitronectin in preeclamptic pregnancies. This probably reflects differences in trophoblast
integrin expression. In contrast, Divers et al33 failed to
find any difference in trophoblast integrin expression between normal and preeclamptic pregnancies. The abnormal cytotrophoblast differentiation in preeclampsia is
not necessarily a primary feature. An alternative explanation is an abnormal interaction between trophoblast and
decidual lymphoid cells.31 In a monkey model hypoxia
was demonstrated to be associated with increased invasion.34 However, it is uncertain whether this phenomenon is mediated by a direct effect of hypoxia on cytotrophoblast integrin expression or reflects increased VEGF
action.4
Vascular tone
In normal pregnancy there is an 8-fold to 10-fold increase in prostacyclin. Thromboxane A2 (TxA2) biosynthesis is also increased throughout normal pregnancy;
the net result, however, is a biologic dominance of
prostacyclin over TxA2.35, 36 The dominance of prostacyclin provides an explanation for vascular refractoriness
to angiotensin II in normal pregnancy, although its role
as a circulating hormone is still controversial because of
its evanescent nature.35-37 However, prostaglandins may
not be the major vasodilators of pregnancy.38, 39 A number of peptide regulatory factors (cytokines, binding proteins, growth factors) released in an appropriate cortico-
Volume 179, Number 5
Am J Obstet Gynecol
steroid environment play an integral part in this mediation.40-42 Nitric oxide is probably an important messenger, but certainly not the only one, in inducing vasodilation in normal pregnancy.42-47 In pregnant animals
chronic inhibition of nitric oxide synthesis reverses refractoriness to angiotensin and vasopressin and eventually produces a preeclampsia-like syndrome.48 Nitric
oxide is probably not the only explanation for the
marked vasodilatation of normal pregnancy. Pascoal and
Umans49 recently provided strong evidence for the presence of an endothelium-derived hyperpolarizing vasodilatory factor in causing pregnancy-associated vasorelaxation.
Nitric oxide is more important than prostacyclin in
maintaining low vascular tone in fetoplacental vessels.50-52 Immunohistochemical studies to localize endothelial nitric oxide synthetase in term placentae found
strong staining patterns in syncytiotrophoblast and absence of staining in endothelial cells of small fetoplacental vessels and the cytotrophoblast.53 Negligible nitric
oxide production in the placental bed is unlikely to contribute substantially to uteroplacental vasodilation.54
Additionally, recent studies found significantly higher inducible nitric oxide synthetase activity in basal plate and
villous tissue compared with the activity of endothelial nitric oxide synthetase.54, 55
Pathogenesis of preeclampsia
In preeclampsia, absence of normal stimulation of the
renin-angiotensin system, despite hypovolemia, and increased vascular sensitivity to angiotensin II and norepinephrine can be explained by a biologic dominance of
TxA2 over prostacyclin.35-37, 56, 57 A reduction in urinary
excretion of prostacyclin metabolites precedes the development of clinical disease, whereas TxA2 biosynthesis is
increased in preeclampsia.58 Increased TxA2 production
in preeclampsia is largely derived from platelets35 and
the placenta.59 Placental prostacyclin production is reduced.60 Although the increased TxA2-to-prostacyclin
ratio allows an explanation for vasoconstriction, platelet
destruction, and reduced uteroplacental blood flow, evidence is mounting that preeclampsia is not simply a state
of prostacyclin deficiency.57, 61 Increased levels of factor
VIIIrelated antigen, total and cellular fibronectin,
thrombomodulin, endothelin, growth factor activity, a
disturbance of the tissue plasminogen activator/plasminogen activator inhibitor balance, and the prostacyclin/TxA2 balance all support the hypothesis that a more
global endothelial cell dysfunction is intimately involved
in the pathogenesis of preeclampsia.62-73 Morphologic
evidence of endothelial cell injury is provided by
glomerular endotheliosis and ultrastructural changes in
the placental bed, uterine boundary vessels, and other
parts of the circulation.74-76 In in vitro experiments
preeclamptic sera do not cause actual endothelial cell
Dekker and Sibai 1361
damage but rather activate specific endothelial cell metabolic pathways,77 which may be related to the disturbances in vascular function encountered in vivo.78
Results of studies on actual nitric oxide production in
preeclampsia have yielded controversial results: Plasma
nitrite and nitrate levels have been found to be decreased, unchanged, and increased as compared with the
levens in normotensive control subjects.79-84 However,
the best indicator (in vivo) of overall nitric oxide production is the steady-state urinary excretion of nitrites, and
Davidge et al85 found urinary excretion, but not plasma
levels, of these nitric oxide metabolites to be decreased
in preeclampsia. Plasma concentrations of endogenous
nitric oxide synthetase inhibitors are raised in patients
with preeclampsia as compared with the levels in patients
with normal pregnancies or patients with gestational hypertension.86, 87 Nitric oxide donors cause a significant
decrease in uterine artery resistance in patients with an
elevated uterine artery resistance index.88
In preeclampsia, endothelial cell dysfunction and
platelet aggregation precede the increase in thrombin
and fibrin formation.89, 90 An inadequate production of
either antiaggregatory prostacyclin or nitric oxide, or
both, provides an attractive hypothetical explanation for
surface-mediated platelet activation occurring on the
inner lining of spiral arteries. Platelets adhere to and release and dense granule constituents, specifically, TxA2
and serotonin, contributing to platelet aggregation and
inducing fibrin formation. Zeeman and Dekker61 suggested that if there are still intact endothelial cells left in
the spiral arteries the increased platelet-derived serotonin levels91 may interact with endothelial S1 receptors,
which may induce a partial recovery of endothelial
prostacyclin and nitric oxide release.92 Local prostacyclin
may stimulate the uteroplacental renin-angiotensin system and thus induce the release of angiotensin II, which
may improve uteroplacental perfusion by increasing maternal blood pressure (perfusion pressure) and by forming an extra stimulus for prostacyclin and nitric oxide release by the uteroplacental vessels.61, 93
In preeclampsia and IUGR the fetoplacental unit is
also characterized by a prostacyclin/TxA2 imbalance.94
Concerning fetoplacental nitric oxide synthesis, Morris
et al54 found syncytiotrophoblast nitric oxide release, as
judged by nitric oxide synthetase activity, to be decreased
in preeclampsia as compared with normal placentas.
Wang et al95 found no differences in nitric oxide production, as judged by nitrite levels, between normal and
preeclamptic placentas. Ghabour et al96 reported that
syncytiotrophoblast endothelial nitric oxide synthetase
immunostains appeared primarily apical in location and
diffuse in distribution in preeclamptic placentas but primarily basal and punctate in normal placentas. In the villous trophoblast differentiation of cytotrophoblast into
syncytiotrophoblast is associated with endothelial nitric
1362 Dekker and Sibai
oxide synthetase expression.97 Thus alterations in endothelial nitric oxide synthetase expression in
preeclamptic placentas may be a result of placental damage and repair processes rather than the primary mediator.
Etiology of preeclampsia
Endothelial cell activation or dysfunction appears to
be the central theme in the pathogenesis of preeclampsia, but what causes these endothelial changes in
preeclampsia? Four hypotheses are currently the subject
of extensive investigation. For the sake of clarity these hypotheses are described separately; however, it should be
stressed that they are not mutually exclusive but probably
interactive.
Placental ischemia. According to the Oxford group of
researchers, preeclampsia is a 2-stage placental disease.
The first stage is the process that affects the spiral arteries
and results in a deficient blood supply to the placenta.
The second stage encompasses the effects of the ensuing
placental ischemia on both the fetus and the
mother.98-100 Syncytiotrophoblast microvillous membranes from normal and preeclamptic placentas were
found to suppress endothelial cell proliferation to a similar extent and disrupted endothelial monolayers to form
a honeycomb-like pattern.98 Deportation of placental tissue, a feature also present in normal pregnancy, is increased in established preeclampsia. Although deportation of intact trophoblasts could, at least in theory, exert
a systemic effect by impairing the substantial pulmonary
nitric oxide production, it is (according to the Oxford
group) the increased microdeportation of syncytiotrophoblast microvillous membrane particles that is probably more related to the systemic endothelial cell dysfunction
in preeclampsia.99, 100 The increased syncytiotrophoblast
deportation in preeclampsia is probably explained by the
presence of syncytial sprouts that may be elongated on
long pedicles.99 Cytotrophoblast proliferation and formation of these outgrowth lesions of syncytiotrophoblast
may represent evidence of placental repair mechanisms.
Preeclampsia is associated with glycogen accumulation in
syncytiotrophoblast,101 which could be another expression of increased syncytiotrophoblast deportation and increased cytotrophoblast proliferation. Placental villous
cytotrophoblasts produce TxA2, the amount decreasing
as they mature into syncytiotrophoblasts.102 Tsukimori et
al103 found a syncytiotrophoblast factor that was cytotoxic to endothelial cells to be present in preeclamptic
placentas but not in normal ones.
Placental ischemia as the cause of endothelial cell dysfunction in preeclampsia is an attractive concept, but several concerns are conceivable that may dispute its validity. First, if placental ischemia is the actual cause of
endothelial cell dysfunction, one would expect a closer
November 1998
Am J Obstet Gynecol
correlation between the presence of maternal and fetal
components of the disease. However, this is not the usual
finding in clinical practice. Next, the chronology of the
maternal components of the syndrome appear not to fit
with the placental ischemia hypothesis. The findings of
some recent studies suggest that endothelial cell involvement is already present in the first trimester,104, 105 which
is difficult to reconcile with the first conceivable stages of
placental ischemia. The normal environment for trophoblast in the first trimester is low in oxygen,10-12 and
this relative hypoxia is likely to be of physiologic importance because signs of increased intervillous flow are associated with adverse pregnancy outcome.6 Low oxygen
also affects trophoblast function later in pregnancy, and
the fact that hypoxia-induced syncytiotrophoblast and cytotrophoblast changes in third-trimester placentas resemble the histologic changes in preeclampsia suggests
that the placenta may indeed be relatively hypoxic in the
end stage of a preeclamptic pregnancy.106 The basic
problem with the Oxford hypothesis is the fact that the
studies are confined to patients with established disease.
Thus increased syncytiotrophoblast deportation, which is
of pivotal importance in this hypothesis, is likely to be
just a feature of end-stage disease. Nevertheless, this phenomenon might be clinically relevant because it could be
involved in causing the extreme refractory hypertension
and vasospasm, which are so common in the terminal
stages of severe preeclampsia-eclampsia.
Very low-density lipoproteins (VLDL) versus toxicitypreventing activity. In preeclampsia, circulating free fatty
acids (FFA) are already increased 15 to 20 weeks before
the onset of clinical disease.107 Sera from preeclamptic
women have both a higher ratio of FFA to albumin and
increased lipolytic activity resulting in enhanced endothelial cell uptake of FFA, which are further esterified
into triglycerides.108, 109 Among the FFA, oleic, linoleic,
and palmitic acids have been found to be increased by
37%, 25%, and 25%, respectively. Linoleic acid reduces
thrombin-stimulated prostacyclin release by 30% to 60%
and oleic acid by 10% to 30%, whereas palmitic acid has
no effect. Incubation with linoleic acid reduces endothelial cyclic guanosine monophosphate levels by 70% and
the ability to inhibit platelet aggregation by 10% to
45%.110 Plasma albumin exists as several isoelectric
species, which range from isoelectric point (pI) 4.8 to pI
5.6. The more FFA are bound to albumin, the lower the
pI. Plasma albumin exerts a toxicity-preventing activity if
it is in the pI 5.6 form. Because higher ratios of FFA to albumin cause a shift from the pI 5.6 to the pI 4.8 form of
albumin, patients with preeclampsia will have lower
amounts of protective toxicity-preventing acivity (pI 5.6)
than normotensive pregnant women. A low ratio of toxicity-preventing activity to VLDL would result in cytotoxicity and triglyceride accumulation in endothelial cells.111
Volume 179, Number 5
Am J Obstet Gynecol
According to Arbogast et al,111 pregnancy increases energy demands, which are reflected by increasing VLDL
concentrations throughout pregnancy. In women with
low albumin concentrations, the burden of transporting
extra FFA from adipose tissue to the liver is likely to reduce the concentration of toxicity-preventing activity to a
point at which VLDL toxicity is expressed, leading to endothelial cell injury.
Similar to the concerns with regard to the placental ischemia hypothesis, it is difficult to reconcile an exaggerated energy demand occurring so early that it will cause a
severe VLDL/toxicity-preventing activity imbalance and
subsequently endothelial cell dysfunction in the first
trimester. Thus FFA and endothelial cell triglyceride accumulation are early and probably very relevant features
in preeclampsia, but they are not necessarily caused by
an exaggerated energy demand.111, 112 Increased FFA levels and endothelial cell triglyceride accumulation in
preeclampsia may reflect cytokine-mediated oxidative
stress, caused by either ischemia-reperfusion mechanisms or activated leukocytes, or both.113
Immune maladaptation. In humans, organ transplants
will be rejected if there are differences between donor
and recipient with respect to major histocompatibility
complex (MHC) genes (ie, human leukocyte antigens
[HLA]). It has been found that trophoblast cells in contact with maternal blood are negative for MHC class I
and II alloantigens, whereas those in contact with maternal tissue are often MHC class I positive. Hence firsttrimester syncytiotrophoblast and noninvasive villous cytotrophoblast do not express MHC class I alloantigens,
but rather the extravillous cytotrophoblast at the tips of
the cell columns and in spiral arteries is MHC class I positive.ll4-ll7 The HLA class I gene family encodes cell-surface glycoproteins that include the highly polymorphic
transplantation molecules HLA-A, HLA-B, and HLA-C,
which show widespread tissue expression and function in
the presentation of autologous peptide antigens to T
cells. At least 3 additional class I genes (HLA-E, HLA-F,
and HLA-G, known as nonclassical [class Ib] genes) have
been identified that are highly homologous to classical
HLA genes. HLA-E and HLA-F are expressed in many
fetal and adult tissues. By contrast, HLA-G is only expressed by the extravillous trophoblast at the maternofetal interface, where classical class I and II antigens are absent; this restricted expression suggests that HLA-G plays
a role in the immune tolerance of the semiallogenic fetus
by the mother.114-117 An important feature of HLA-G is
that its gene locus appears to exhibit a very limited degree of polymorphism, which is not likely to affect unduly the sequence of expressed proteins. However, van
der Ven and Ober118 presented evidence of many distinctive alleles in the African-American population and the
presence of subtle HLA-G mutations in African-
Dekker and Sibai 1363
American neonates with IUGR, which appears to contrast with the finding that HLA-G shows very little polymorphism in Caucasian persons.
The decidua contains an abundance of cells of bone
marrow origin as is demonstrable by their cell surface
antigen expression (CD45). These antigens are designated by their CD number, an arbitrary number assigned
to each Cluster of Differentiation. In the late secretory
phase of the endometrium an unusual population expressing CD56, a marker of peripheral blood large granular lymphocytes, becomes dominant. These uterine
large granular leukocytes resemble natural killer (NK)
cells but do not express such strong NK cell activity as peripheral blood NK cells. About 75% of decidual cells express CD45, reflecting their bone marrow origin (ie, 45%
uterine large granular leukocytes, 19% macrophages,
and 8% T cells). As pregnancy progresses, the number of
macrophages and T cells remains constant but the number of uterine large granular leukocytes declines dramatically.119-121
Cells of the NK lineage, such as uterine large granular
leukocytes, kill target cells that are deficient in MHC expression rather than recognizing the presence of foreign
MHC. This is the basis of the missing self hypothesis for
NK cytolysis.122-124 Therefore simple lack of classical class
I molecules on trophoectoderm and later on invading cytotrophoblast would seem to be inadequate to explain
their protection from NK(-like) cells. The presence of a
nonpolymorphic nonclassical class I antigen, HLA-G,
on the surface of invasive cytotrophoblast cells may be an
explanation for this conundrum.125 HLA-G is indeed capable of inhibiting NK activity of uterine large granular
leukocytes against trophoblast cells at the maternofetal
interface.114, 120, 123 Thus the remarkable absence of regular HLA expression and the presence of HLA-G on invasive cytotrophoblast are likely to be of pivotal significance in protecting trophoblast from effective maternal
immune recognition or cytotoxic attack.115-117
Throughout gestation, extravillous cytotrophoblast cells
retain the ability to up-regulate HLA-G expression.
Apparently they must avoid maternal immune surveillance constantly. In contrast, cytotrophoblast cells only
express invasive characteristics transiently (ie, only in
early gestation are they characterized by enhanced metalloproteinase expression and integrin switching).126
Colbern et al127 observed a lower level of messenger ribonucleic acid for HLA-G in chorionic tissue in
preeclampsia than in normal pregnancy. However, normalization to messenger ribonucleic acid for cytokeratin
revealed that this was caused by a smaller number of trophoblast cells present in preeclamptic placentas, thus
showing that these findings were only a reflection of the
well-established reduced trophoblast invasion in
preeclampsia. Recent studies suggest that extravillous
1364 Dekker and Sibai
trophoblast cells also express HLA-C. It may be that the
coordinated expression of both HLA-G and HLA-C is required to provide a set of trophoblast HLA class I molecules, which act together for optimal NK recognition and
to prevent lysis by these cells.114, 116
An alternative biologic role for uterine large granular
lymphocytes and other decidual CD56 cells has recently
been consideredthat trophoblast growth and invasion
may be dependent on appropriate cytokines being produced by these cells in response to HLA-G expressed on
cytotrophoblast cells.128 Hence decidual leukocyte activity could actually be beneficial to trophoblast growth and
function by a phenomenon named immunotrophism.129
In addition, colony-stimulating factors are produced by
decidual macrophages and by the developing placenta itself. The amount increases with implantation.130 Colonystimulating factors stimulate the endometrial
macrophage population, trophoblast human placental
lactogen, and human chorionic gonadotropin synthesis
and thus appear to be intimately involved in decidual trophoblast interactions during early pregnancy.131 Several
cytokines are now known to be integral to early pregnancy development. Granulocyte-macrophage colonystimulating factor (GM-CSF), IL-1, TNF-, interferon(IFN-), and colony-stimulating factor-1 (CSF-1) have all
been implicated in blastocyst attachment and in trophoblast implantation, proliferation, and invasion.
Because TNF-, IFN-, IFN-, IFN-, and transforming
growth factor (TGF)-l are produced in the uteroplacental unit and inhibit trophoblast deoxyribonucleic acid
synthesis, they may take part in regulating trophoblast
growth. Conversely, IL-1, GM-CSF, and IL-6 are thought
to have trophoblast growth-stimulating effects. It should
be emphasized that the majority of these cytokine effects
occur in a close and complex interaction with corticosteroids and prostaglandins.l19, 132-134
In 1986, 2 distinct and mutually inhibitory types of Thelper cells were described.135 The first type of cell,
termed Th1, secretes IL-2, IFN-, and lymphotoxin. This
contrast with Th2 cells, which secrete IL-4, IL-4, IL-6, and
IL-10.136 Th1 cytokines are associated with cell-mediated
immunity and delayed hypersensitivity reactions, whereas
Th2 cytokines foster antibody responses and allergic reactions. Because Th1 cytokines are considered to be
harmful to pregnancy and Th2 cytokines (IL-10) can
down-regulate production of Th1 cytokines, it has been
proposed that successful pregnancy is a Th2 phenomenon.137 This hypothesis is consistent with the observation
that cell-mediated autoimmune conditions such as
rheumatoid arthritis are often improved during pregnancy, whereas disorders associated with autoantibodies
may be worsened by pregnancy.138 Several substances
such as prostaglandin E2, TGF-, GM-CSF, and IL10139-141 play a part in the immunoendocrine network in
pregnancy maintenance. PGE2 has many immunosup-
November 1998
Am J Obstet Gynecol
pressive properties, including the inhibition of all cells of
the immune system.140 IL-10 potentially has 2 mechanisms by which it may inhibit immune function: (1) directly as a cytokine synthesis inhibitory factor and (2) indirectly as an inducer of adrenocorticotropic hormone.
Although these data are intriguing, they must be considered in light of the successful reproduction of IL-10
knock-out mice.142
In addition to cytokines, fetal and placental growth is
at least partially regulated by insulin-like growth factors
(IGF) and insulin-like growth factorbinding proteins
(IGFBP-1 or placental protein 12). Trophoblast substances such as human placental lactogen stimulate an
increasing production of IGF-I by the maternal liver,
whereas, on the other hand, IGF-I binding to trophoblast
cells changes during trophoblast differentiation.143 Fetal
and maternal IGF-I levels are positively correlated with
fetal weight. IGFBP-1, which is produced by decidual
stromal cells, impairs trophoblast growth by inhibiting
IGF-I. Another explanation may be that IGFBP-1 also
contains an integrin arginineglycineaspartic acid
recognition sequence that can bind to the 4D1 integrin
(fibronectin receptor).144 The presence of elevated maternal levels of IGFBP-1, at 16-24 weeks gestation, in future preeclampsia and IUGR suggests that decidual overproduction of IGFBP-1 may be at least partially involved
in the causation of abnormal placentation.143-145 In contrast, de Groot et al146 found midtrimester plasma
IGFBP-1 concentrations to be significantly lower in
women who later had preeclampsia compared with control subjects with normal pregnancies. At the moment it
is not clear whether these contradictory findings can be
explained by assay differences.
Epidemiologic evidence suggests that immune mechanisms ought to be involved in the etiology of preeclampsia.147-149 Genuine preeclampsia is primarily a disease of
first pregnancies. A previous normal pregnancy is associated with a markedly lowered incidence of preeclampsia.
Even a previous abortion provides some protection.
Multiparitys protective effect, however, is lost with
change of partner; thus preeclampsia may be a problem
of primipaternity rather than primigravidity.148 In a recent article Trupin et al149 studied 5068 nulliparous and
5800 multiparous women, 573 of whom had new partners. The preeclampsia incidence in nulliparous women
(3.2%) and multiparous women with changed paternity
(3%) was found to be similar, as contrasted with the significantly lower incidence of preeclampsia (1.9%) in
multiparous women with no change in partners.
Analogous to altered paternity, artificial donor insemination and oocyte donation result in an increased incidence of preeclampsia.150 Additionally, the length of
time of unprotected sexual cohabitation before conception appears to be inversely related to the incidence of
pregnancy-induced hypertensive disorders.151 There are
Volume 179, Number 5
Am J Obstet Gynecol
numerous reports of immunologic phenomena in
preeclampsia. Beginning early in the second trimester,
women in whom preeclampsia develops later have a significantly lower proportion of T-helper cells compared
with the proportion in those women who remain normotensive.152 Antibodies against endothelial cells have
been found in 50% of women with preeclampsia versus
15% of control women.153 Deposition of immunoglobulins (IgM), complement (C3), and fibrin has been noted
in the walls of preeclamptic spiral arteries, especially in
acute atherosis, in which substantial granular deposits of
IgM can often be seen. Immunologic pathogenesis of
acute atherosis is suggested by morphologic similarities
to lesions seen in allograft rejection.154 However, acute
atherosis usually occurs in those arteries that have not
undergone physiologic changes mediated by trophoblast
invasion; thus, if a transplantation analogy is pursued, it
is necessary to consider that the fetus is rejecting the
mother.154
What is the link between immune maladaptation and
endothelial cell activation in preeclampsia? The decidua
contains an abundance of cells of bone marrow origin.
These cells, when activated, can release a host of mediators that may interact with endothelial cells.
Elastase. Activated neutrophils release elastase and
other toxic proteases, which can destroy the integrity of
endothelium. Plasma elastase levels are significantly
higher in preeclampsia than in normal pregnancy and
correlate with elevated levels of endothelin and factor
VIIIrelated antigen, supporting their involvement in
causing endothelial cell dysfunction in preeclampsia.
The number of elastase-positive decidual neutrophils is
significantly greater in preeclampsia than in normal
pregnancies and correlates with plasma uric acid.155, 156
Cytokines. So far, most cytokine research has been concerned with TNF and IL-1 because their endothelial effects resemble changes described in preeclampsia. TNF
and IL-1 enhance the generation of thrombin, plateletactivating factor, factor VIIIrelated antigen, and plasminogen activator inhibitor-l, endothelial cell permeability, and expression of intercellular adhesion molecule-1
(ICAM-1) and vascular cell adhesion molecule-1 (VCAM1) and increase inducible nitric oxide synthetase activity
and levels of a variety of prostaglandins, at the same time
that endothelial nitric oxide synthetase activity is downregulated.157, 158 So far, most studies reported found an
increase in TNF- levels in preeclampsia, although it is
still controversial whether this increase in TNF- occurs
after the syndrome is detected clinically and whether this
increase only occurs in preeclamptic pregnancies complicated by IUGR.159-161 TNF- detection is problematic
as a result of a short half-life and possible interference of
its soluble receptors. It may be deceptive to draw conclusions from plasma TNF levels. Soluble TNF receptors are
more reliable markers for TNF activity. There are 2 spe-
Dekker and Sibai 1365
cific receptors for TNF- of 75 and 55 kd molecular
weight (p75 and p55, respectively). Each can be shed as
soluble protein that specifically binds TNF. Levels of
soluble TNF receptors are known to increase after an increase in TNF-, bind TNF-, and thus provide a protective mechanism against excessive TNF- production.
Because TNF receptors have a longer half-life than TNF, they are footprints of TNF- activity. The p55 and
p75 soluble TNF receptor levels are significantly elevated
in preeclampsia as compared with uncomplicated pregnancy.162, 163 Thus the rise in TNF- levels reported in
preeclampsia is probably real.164 The source of this excessive production may be activated (decidual) leukocytes or the placenta itself, because syncytiotrophoblast
contains TNF- messenger ribonucleic acid.165
Preeclampsia shows some aspects of an acute-phase response, which may be caused by the elevated IL-6 levels.166 Changes in plasma proteins, which include increases in plasma ceruloplasmin, l-antitrypsin, and
haptoglobin, hypoalbuminemia, and reduced plasma
transferrin are characteristic of an acute-phase reaction,
as are certain alterations in complement activity in
preeclamptic sera. Also, Il-6 has definite effects on endothelial cells such as increased permeability, stimulation
of platelet-derived growth factor synthesis, and impairment of prostacyclin synthesis. Oxygen free radicals are
known to induce endothelial IL-6 synthesis. Il-6 production is thought to be integrally related to TNF-. Whereas
IL-6 has direct negative feedback on TNF- production,
its production in decidua and trophoblast is increased by
TNF-a and IL-1.167 IFN- levels are increased in
preeclampsia.168 IFN- up-regulates endothelial cell
ICAM-1 expression and IL-6 synthesis, which may be another explanation for the increased plasma IL-6 levels in
preeclampsia. IL-8 and GM-CSF levels have been found
to be similar in normal and preeclamptic pregnancies.166
Dysfunctional endothelial cells undergo activation
with production of cell surface proteins that mediate adherence of inflammatory cells. This inductive process is
mediated by cytokines produced by inflammatory cells
and activated endothelial cells. A number of so-called
leukocyte-endothelial adhesion molecules have been
identified, including E-selectin, VCAM-1, and ICAM-1.
ICAM-1 and VCAM-1 have a wide tissue distribution,
whereas E-selectin is only expressed by endothelial cells.
Preeclampsia is associated with increased maternal
serum levels of soluble VCAM-1, E-selectin, and probably
also ICAM-1.168, 169 This increase may be an early
event.168 The increased IL-6 and IL-1 receptor antagonist
(reflecting increased IL-1 concentrations) levels in
preeclampsia correlate with elevated VCAM-1 concentrations.166 The increase in these soluble cell adhesion molecules reflects increased expression of these molecules
on endothelial cells and thereby explains leukocyte activation in preeclampsia.156 Abnormal endothelial
1366 Dekker and Sibai
cellleukocyte interaction in preeclampsia is confined to
maternal circulation, as is demonstrated by similar expression of cell adhesion molecules in placental vessels
and elastase levels in fetal plasma in preeclampsia as
compared with normal pregnancy.156, 170
Oxygen free radicals. Preeclampsia is associated with
oxidative stress, defined as an imbalance between prooxidant and antioxidant forces in favor of prooxidants,
leading to potential cell or tissue damage.171 Oxygen free
radicals can lead to the formation of lipid peroxides.
Once lipid peroxidation is initiated, it becomes self-propagating. According to some investigators, oxidized lowdensity lipoproteins may have a half-life of 3 hours in the
circulatory system, suggesting the still controversial possibility that they may function as circulating compounds.171-173 Because lipid peroxides, measured as stable lipid peroxide metabolites,172 are increased above
nonpregnant levels in normal pregnancy, it seems that
even normal pregnancy induces a certain degree of oxidative stress. Lipid peroxide levels are further increased
in preeclampsia and correlate with an increase in blood
pressure but not with perinatal outcome.174-178
Preeclamptic lesions of decidual vessels resemble atherosclerotic lesions, both showing fibrinoid necrosis of the
vessel wall and accumulation of lipid-laden foam cells, a
hallmark of oxidized low-density lipoproteins.173, 174, 179
Some,180 but not all,181 investigators found titers of IgG
autoantibody to oxidized low-density lipoproteins to be
increased in preeclampsia.
Activated leukocytes may provide one of the major
sources of oxygen free radicals in preeclampsia.
Additionally, activated leukocytes may, by producing certain cytokines, irreversibly convert endothelial cell xanthine dehydrogenase to xanthine oxidase, thus causing
endothelial release of oxygen free radicals.182-184 Oxygen
free radicals and elastase may work synergistically in causing endothelial cell damage.182, 185, 186 The placenta is
another source of free radical species in preeclampsia;
placental lipid peroxide production correlates with the
increased placental production of TxA2.175 Metabolism
of arachidonic acid generates oxygen free radicals by
both lipoxygenase and cyclooxygenase pathways, but the
cyclooxygenase pathway generates >1000 times more superoxide than the lipoxygenase pathway.187 Walsh175 hypothesized that neutrophils could be activated as they circulate through the intervillous space by lipid peroxide
generated by trophoblast cells. Increased lipid peroxide
has also been observed in platelets and red blood cells.188
Free radical species cause a type of endothelial cell dysfunction that is similar to changes seen in preeclampsia.174, 175 Lipid peroxides stimulate prostaglandin H synthase but inhibit prostacyclin synthase; therefore
increased lipid peroxide levels in preeclampsia favor production of platelet-derived TxA2 above vascular prostacyclin synthesis. Free radical species impair endothelial cell
November 1998
Am J Obstet Gynecol
nitric oxide production and inhibit macrophage inducible nitric oxide synthetase.189, 190 Lipid peroxides
alter capillary permeability to proteins186 and may thus
be involved in causing edema and proteinuria.175 Lipid
peroxides trigger thrombosis by increasing thrombin
generation and endothelial plasminogen activator inhibitor-1 release while at the same time decreasing antithrombin and endothelial tissue plasminogen activator
release.191 Lipid peroxides alter cell membrane fluidity
by increasing incorporation of cholesterol, oxidized fatty
acids, and low-density lipoproteins. In preeclampsia this
phenomenon has been described for platelets, erythrocytes, and trophoblast cells.188, 192 This may partially explain why incubation of endothelial cells with sera from
preeclamptic women increases the endothelial cell content of triglycerides, which results in a disturbance of endothelial cell physiologic characteristics.77, 108, 113
Antioxidants are a diverse family of compounds designed to prevent overproduction of and damage caused
by free radical species. The picture in preeclampsia is
complex, but it is apparent that the disease cannot be
characterized as a state of global antioxidant deficiency.193 One apparent paradox of the oxidative stress
theory of preeclampsia concerns the antioxidant function of uric acid.183, 194 In preeclampsia the ability of
plasma to scavenge aqueous radicals is markedly augmented, and most of this increase is caused by the increase in uric acid.193, 194 Thus, although increased xanthine oxidase activity may contribute to oxidative stress in
preeclampsia, hyperuricemia itself may serve a protective
role as antioxidant.194
Vitamin E is the major lipid-soluble antioxidant.
According to Wang et al,36 maternal concentration ratios
of antioxidant vitamin E to lipid peroxides and prostacyclin to TxA2 favor the antioxidant activity of vitamin E
and the vasodilator effects of prostacyclin with advancing
gestation in normotensive pregnancy, whereas in severe
preeclampsia the lipid peroxide levels are increased and
the vitamin E levels are decreased; this imbalance correlates with the imbalance of increased TxA2 and decreased prostacyclin177 and with the increase in blood
pressure.195 Several authors did not find decreased vitamin E levels in preeclampsia.178, 193, 196
Generation of highly toxic radicals, such as OH, that
initiate lipid peroxidation and reactions causing propagation of lipid peroxidation require the presence of a
low-molecular-weight pool of iron or other transition
metals. Thus a critical group of antioxidants is those designed to bind metal ions in forms that will not generate
free radical species, including transferrin, albumin, and
ceruloplasmin.197, 198 When brain tissue is homogenized
in a buffer solution, endogenous lipids undergo rapid
peroxidation as a result of transition metals released
from cells. The ability of small amounts of serum to inhibit this peroxidation provides an assay for serum an-
Volume 179, Number 5
Am J Obstet Gynecol
tioxidant activity. Peroxidation is inhibited by several
iron-chelating agents; thus the assay has a predilection
for antioxidants that function by sequestering
metals.197-199 Using this assay, Davidge et al199 found an
increased serum antioxidant capacity during uncomplicated pregnancy, whereas the antioxidant capacity in
preeclampsia was found to be reduced by 50%.
Erythrocyte glutathione levels and glutathione peroxidase activity, another lipid peroxide scavenger system,
are increased in preeclampsia in comparison with normal pregnancy; this increase may represent a compensatory response.176 Tissue glutathione peroxidase levels
may be different from erythrocyte levels. Indeed, Walsh
and Wang200 found decreased glutathione peroxidase
levels in placentas from preeclamptic pregnancies as
compared with normotensive pregnancies.
Ascorbic acid, -tocopherol, and -carotene are potent
antioxidant nutrients. Ascorbic acid has been described
as the major front-line water-soluble antioxidant.
Ascorbic acid levels are significantly decreased in patients with mild and severe preeclampsia, whereas -tocopherol and -carotene levels are significantly decreased
only in severe preeclampsia.201 Thus, in preeclampsia,
antioxidant nutrients may be used to a greater extent to
counteract free radical-mediated cell disturbances, resulting in a reduction in antioxidant plasma levels. Watersoluble antioxidant nutrients may initially be consumed,
followed by lipid-soluble antioxidants. Diminished serum
metal-binding antioxidant capacity and placental antioxidants may be of special importance in allowing initiation
and propagation of lipid peroxidation in preeclampsia.175, 194, 199
The hypothesis that cytokines, especially TNF-, may
contribute to oxidative stress in preeclampsia was reviewed by Stark.202 Mitochondrial injury is the first detectable effect of TNF- in cultured cell lines, whereas
some studies found preeclampsia to be associated with a
very similar type of mitochondrial damage.74-76 Oxidative
disequilibrium in preeclampsia is probably closely linked
with cytokine activity, particularly TNF-. Antioxidants
selectively inhibit TNF- release because they control the
oxidation-reduction status of glutathione peroxidase,
which is of major importance as an endogenous modulator of TNF- production. In mitochondria, TNF- subverts part of the electron flow to release oxygen free radicals with subsequent lipid peroxide formation. If these
are not removed with subsequent efficient reduction of
the oxidized glutathione peroxidase, serious toxic effects
ensue.
Immune maladaptation is an attractive hypothesis to
explain several of the well-known epidemiologic features
of preeclampsia. It should be emphasized that although
there is no doubt that patients with preeclampsia manifest immunopathologic characteristics, the question remains as to whether such immunologic abnormality
Dekker and Sibai 1367
causes or results from preeclampsia. Immunoglobulin,
immune complex, complement, and fibrin deposits in
decidual vessels may be the effect of occluded vessels
rather than the cause; analogous results described in
chorionic villous tissue may have resulted from placental
ischemia, and the IgM, IgG, and complement deposits in
glomeruli in preeclampsia also are not direct proof for
an immunologic pathogenesis of these lesions. The immune maladaptation hypothesis is, of course, not mutually exclusive with the placental ischemia hypothesis.
Immune maladaptation may be the cause of abnormal
implantation and thus evoke placental ischemia.
Moreover, placental ischemia provides an alternative explanation for the cytokine changes203 and oxidative
stress seen in preeclampsia. Placental cells express erythropoietin, which is the prototype molecule for transcriptional regulation by hypoxia in mammals. TNF-
and IL-1 have deoxyribonucleic acid sequences that are
homologous or nearly homologous to the hypoxia-responsive enhancer element of the erythropoietin gene,
thus providing a potential but as of yet untested molecular link between placental hypoxia and stimulation of cytokine production.203
Preeclampsia as a genetic disease
Severe preeclampsia and eclampsia have a familial tendency. Chesley et al204 found a 26% incidence of
preeclampsia in daughters of women with preeclampsia
but only an 8% incidence in the daughters-in-law.
Published reports are consistent with a relatively common allele acting as a major gene conferring susceptibility to preeclampsia. The development of preeclampsia
may be based on a single recessive gene or a dominant
gene with incomplete penetrance. Multifactorial inheritance is another possibility.205, 206 The principal reason
for suspecting the existence of a maternal gene as the
sole explanation for preeclampsia is data showing a lack
of concordance for susceptibility in a small sample (n =
10) of monozygous twins.207 The increased prevalence of
preeclampsia in daughters born to an eclamptic mother,
as opposed to a noneclamptic pregnancy of the same
mother, could indicate an influence of the fetal genotype
on susceptibility to preeclampsia.205, 206 An example of
the impact of the fetal genotype on preeclampsia is the
association between HELLP (hemolysis, elevated liver enzymes, and low platelets) syndrome and a rare fetal metabolic disorder208 and the increased incidence of
preeclampsia in cases of fetal chromosomal abnormalities (for example, triploid and trisomy 13).209
Arngrimsson et al210 provided epidemiologic evidence
that the genetic predisposition to preeclampsia may be
related to implantation and placentation.
Conflicting data have been reported regarding the involvement of HLA antigens. Several studies revealed an
increased HLA compatibility between patients and their
1368 Dekker and Sibai
mates.205 Kilpatrick et al211 found a significant association between HLA-DR4 and preeclampsia. However, association of preeclampsia with HLA-DR4 has now been excluded by detailed genetic analysis of restriction
fragment polymorphisms of HLA-DR4 in informative
pedigrees; the association probably indicates an underlying tendency to autoimmune disease with which HLADR4 is linked.212, 213 In contrast, Peterson et al214 observed that mothers with HLA haplotypes A23/29, B44,
and DR7 are at a higher risk for development of
preeclampsia and IUGR than mothers without such haplotypes. Humphrey et al215 studied HLA-G deletion polymorphisms in preeclamptic pedigrees and controls and
concluded that there is no detectable relationship between susceptibility to preeclampsia or being born of a
preeclamptic pregnancy and the HLA genotype.
However, as mentioned earlier, Van der Ven and 0ber118
demonstrated the presence of subtle HLA-G mutations
in African-American neonates with IUGR.
An amino substitution in the angiotensinogen gene on
chromosome 1 (the presence of threonine rather than
methionine at residue 235 [T235] in the protein) has
been suggested to correlate with the risk of preeclampsia
but not with the risk of HELLP syndrome.216 Other studies found no association between the T235 allele and
preeclampsia217, 218 and suggested that the T235 allele
has more to do with a tendency for high blood pressure
to develop rather than with preeclampsia.219 Genetic alterations in angiotensin II receptors are currently studied because changes in their expression may be involved
in regulating vasodilation in uteroplacental and fetoplacental vessels.220, 221 Involvement of (genetic) TNFmediated mitochondrial dysfunction in the etiology of
preeclampsia158, 203 is supported by the increased incidence of severe preeclampsia in a family with a failure of
the reduced nicotinamide adenine dinucleotide
ubiquinone oxidoreductase step in the mitochondrial
electron chain.222 Furui et al223 observed reduced expression of mitochondrial genes in placental dysfunction
in preeclamptic pregnancies. Chen et al158 demonstrated
the presence of an increased TNF- messenger ribonucleic acid expression in leukocytes from women with
preeclampsia as compared with women with normal
pregnancies and nonpregnant women. This high expression of TNF- may be associated with the TNF-1 allele,
whose frequency is markedly increased in preeclampsia.158
Opinion on whether placental antigens or the fetal genetic component is more relevant in the etiology of
preeclampsia may be moving toward genetic (rather than
immunologic) interpretation. According to Haig,224 a
genetic conflict can be said to exist between maternal
and fetal genes. Maternal and fetal genomes perform different roles during development. Heritable paternal,
rather than maternal, imprinting of the genome is neces-
November 1998
Am J Obstet Gynecol
sary for normal development of trophoblast and extraembryonic membranes.224 This is clearly revealed in
aberrant development of human conceptuses with abnormal ratios of maternal-to-paternal genomes (a complete hydatidiform mole is a good example). Most complete moles are diploid (with both sets of chromosomes
paternally derived) and are associated with a relatively
high incidence of severe early-onset preeclampsia.
Principally, parental imprinting refers to a parent-of-origin dependent expression of a subset of autosomal loci,
independent of the sex of the offspring. McCowan and
Becroft225 reported on the association of BeckwithWiedemann syndrome and preeclampsia. Overexpression
of the IGF-2 gene during development may be the cause of
excessive growth associated with the BeckwithWiedemann syndrome. It is interesting that the IGF-2
gene is subject to parental imprinting in humans.226
Animal experiments suggest that gene imprinting is also
involved in placental HLA expression.227
According to the genetic conflict theory, fetal genes
will be selected to increase nutrient transfer to the fetus,
and maternal genes will be selected to limit transfers in
excess of some maternal optimum. The phenomenon of
genomic imprinting means that a similar conflict exists
within fetal cells between genes that are maternally derived and genes that are paternally derived. Haig224
stresses the fact that endovascular trophoblast invasion
has 3 consequences: (1) The fetus gains direct access to
its mothers arterial blood. Therefore a mother cannot
reduce the nutrient content of blood reaching the placenta without reducing the nutrient supply to her own
tissues. (2) The volume of blood reaching the placenta
becomes largely independent of control by the local maternal vasculature. (3) The placenta is able to release
hormones and other substances directly into the maternal circulation. The conflict hypothesis predicts that placental factors (fetal genes) will act to increase maternal
blood pressure, whereas maternal factors will act to reduce blood pressure. It also suggests that the mother reduces vascular resistance early in pregnancy to ration
fetal nutrients and that subsequent physiologic increase
in vascular resistance represents the changing balance
of power as the fetus grows larger. A corollary is that placental factors contribute to an increase in maternal cardiac output. Placental factors have an opportunity to
preferentially increase nonplacental resistance because
uteroplacental arteries are highly modified and unresponsive to vasoconstrictors.224 Intrinsic effects of a high
maternal systemic blood pressure are ultimately beneficial to the fetus. Thus Haigs conflict hypothesis224 predicts that fetal genes will enhance maternal blood flow
through the intervillous space by increasing maternal
blood pressure (perfusion pressure). Maternal blood
pressures form a continuum so that the dividing line between normotensive and hypertensive pregnancies is ar-
Dekker and Sibai 1369
Volume 179, Number 5
Am J Obstet Gynecol
bitrary. The conflict hypothesis predicts that a mothers
position on this continuum is determined by the balance
between fetal factors increasing blood pressure and maternal factors decreasing blood pressure. This mechanism may be operative in gestational hypertension, in
which fetal prognosis is known to be good.224 In contrast,
in preeclampsia the hypertension results from vasoconstriction rather than increased cardiac output. A hypoxic
placenta may release cytotoxic factors that damage maternal endothelial cells98-102 and thus cause vasoconstriction and an increase in maternal blood pressure. In this
situation small increments in the birth weight of semistarved fetuses may often have caused major increases in
subsequent survival despite substantial costs to the
mother. Thus endothelial cell dysfunction may have
evolved as a high-risk fetal strategy to increase nonplacental resistance when the uteroplacental blood supply
of a fetus is inadequate.
Underlying disorders associated with preeclampsia
Chronic hypertension, diabetes, and obesity predispose women to the development of preeclampsia.228-230
The link between obesity and preeclampsia is complex;
many mechanisms may be involved. Obesity is characterized by expanded blood volume, increased cardiac output, and hypertension. Elevated cardiac output with compensatory vasodilatation may expose capillary beds to
systemic pressures and increased flow, eventually leading
to endothelial cell dysfunction characteristic of
preeclampsia.231 Obesity is also associated with increased
lipid availability, increased delivery of FFA to tissues,
higher cholesterol and triglyceride levels, insulin resistance, and hyperinsulinemia.232, 233 Women with
preeclampsia are relatively insulin resistant and hyperinsulinemic during pregnancy, as well as months after delivery.234 These metabolic changes may, at least theoretically, cause a derangement of the VLDL/toxicity-preventing
activity balance. High insulin levels may also directly cause
hypertension, by increased sympathetic activity or increased tubular sodium resorption.235, 236 High insulin
levels in obesity may also aggravate cytokine-mediated oxidative stress.237 The combination of insulin resistance
and compensatory hyperinsulinemia may be part of a
cluster of abnormalities, the so-called syndrome X, including some degree of glucose intolerance, increased
triglyceride levels, decreased high-density lipoprotein
cholesterol levels, hypertension, hyperuricemia, smaller,
denser low-density lipoprotein particles, and higher circulating levels of plasminogen activator inhibitor-1,
which is more frequent in adults who themselves had
growth restruction at birth.233, 236
Severe early-onset preeclampsia is also associated with
a high incidence of underlying disorders such as protein
S deficiency, activated protein C resistance [factor V mu-
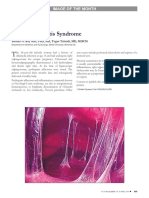
Fig 1. Hypothesis on genesis of preeclampsia, in which most previously discussed concepts are integrated. EC, Endothelial cell;
CTB, cytotrophoblast; STB, syncytiotrophoblast; CK, cytokine.
tation], hyperhomocysteinemia, and anticardiolipin antibodies, which may cause a more aggressive accelerated
course of the disease by inducing an abnormal interaction between endothelial cells, platelets, leukocytes, and
plasmatic coagulation and fibrinolytic factors.228
Unifying hypothesis (Fig 1)
Endothelial cell dysfunction appears to be the final
common pathway in the pathogenesis of preeclampsia,
yet the etiology of the disease remains obscure. Genetic
factors are involved; however, it is likely that there is not 1
major preeclampsia gene but several genetic factors that
are associated with maternal susceptibility. Placental ischemia and increased syncytiotrophoblast deportation
probably represent an end-stage disease phenomenon,
actually very similar to that predicted by the conflict hypothesis, in which it is stated that endothelial cell damage may have evolved as a high-risk fetal strategy to increase nonplacental resistance when the uteroplacental
blood supply to a fetus is inadequate.224 Immune maladaptation and the genetic conflict hypothesis are the hypotheses that are congruous with data on the effects of
changing partners and the protective effect of sperm exposure. Presence of an abundance of decidual leukocytes
and the complex cytokine network underlines the pivotal
impact of a correct fetal (paternal)-maternal interaction.
1370 Dekker and Sibai
Cytokine-mediated oxidative stress, caused by immune
maladaptation or a genetic conflict, fits with data on cytokines, oxidative stress, lipid changes, and the type and
chronologic sequence of endothelial cell dysfunction in
preeclampsia.
REFERENCES
1. Khong TY, De Wolf F, Robertson WB, Brosens I. Inadequate
maternal vascular response to placentation in pregnancies
complicated by pre-eclampsia and by small-for-gestational age
infants. Br J Obstet Gynaecol 1986;93:1049-59.
2. Pijnenborg R, Anthony J, Davey DA, Rees A, Tiltman A,
Vercruysse L, et al. Placental bed spiral arteries in the hypertensive disorders of pregnancy. Br J Obstet Gynaecol
1991;98:648-55.
3. Pijnenborg R. The placental bed. Hypertens Pregnancy
1996;15:7-23.
4. Zhou Y, Damsky CH, Fisher SJ. Preeclampsia is associated with
failure of human cytotrophoblasts to mimic a vascular adhesion phenotype. J Clin Invest 1997;99:2152-64.
5. Meuris S, Nagy AM, Delogne-Desnoeck J, Jurkovic D, Jauniaux
E. Temporal relationship between the human chorionic gonadotropin peak and the establishment of intervillous blood
flow in early pregnancy. Hum Reprod 1995;10:947-50.
6. Jaffe R, Dorgan A, Abramowicz JS. Color Doppler imaging of
the uteroplacental circulation in the first trimester: value in
predicting pregnancy failure or complication. Am J
Roentgenol 1995;164:1255-8.
7. Meekins JW, Pijnenborg R, Hanssens M, McFadyen IR, van
Assche A. A study of placental bed spiral arteries and trophoblast invasion in normal and severe pre-eclamptic pregnancies. Br J Obstet Gynaecol 1994;101:669-74.
8. Meekins JW, Pijnenborg R, Hanssens M, van Assche A,
McFadyen IR. Immunohistochemical detection of lipoprotein(a) in the wall of placental bed spiral arteries in normal
and severe pre-eclamptic pregnancies. Placenta 1994;15:51124.
9. Charnock Jones DS, Sharkey AM, Boocock CA, Ahmed A,
Plevin R, Ferrara N, et al. Vascular endothelial growth factor receptor localization and activation in human trophoblast and
choriocarcinoma cells. Biol Reprod 1994;51:524-30.
10. Wheeler T, Elcock CL, Anthony FW. Angiogenesis and the placental environment. Placenta 1995;16:289-96.
11. Rodesch F, Simon P, Donner C, Jauniaux E. Oxygen measurements in endometrial and trophoblastic tissues during early
pregnancy. Obstet Gynecol 1992;80:283-5.
12. Jauniaux E, Jurkovic D, Campbell S, Hustin J. Doppler ultrasonographic features of the developing placental circulation:
correlation with anatomic findings. Am J Obstet Gynecol
1992;166:585-7.
13. Hofmann GE, Glatsein I, Schatz F, Heller D, Deligdisch L.
Immunohistochemical localization of urokinase-type plasminogen activator and the plasminogen activator inhibitors 1 and 2
in early human implantation sites. Am J Obstet Gynecol
1994;170:671-6.
14. Moll UM, Lane BL. Proteolytic activity of first trimester human
placenta: localization of interstitial collagenase in villous and
extravillous trophoblast. Histochemistry 1990;94:555-60.
15. Librach CL, Feigenbaum SL, Bass KE, Cui TY, Verastas N,
Sadovsky Y, et al. Interleukin-l regulates human cytotrophoblast metalloproteinase activity and invasion in vitro. J Biol
Chem 1994;269:17125-31.
16. Hay ED. Collagen and other matrix glycoproteins in embryogenesis. In: Hay ED, editor. Cell biology of extracellular matrix.
New York: Plenum; 1991. p. 419-62.
17. Lin CQ, Bisell MJ. Multifaceted regulation of cell differentiation by extracellular matrix. FASEB J 1993;7:737-4.
18. Graham CH, Lala PK. Mechanism of control of trophoblast invasion in situ. J Cell Physiol 1991;148:228-34.
19. Aplin JD, Charlton AK, Ayad S. An immunohistochemical
November 1998
Am J Obstet Gynecol
20.
21.
22.
23.
24.
25.
26.
27.
28.
29.
30.
31.
32.
33.
34.
35.
36.
37.
38.
39.
40.
41.
study of human endometrial extracellular matrix during the
menstrual cycle and first trimester of pregnancy. Cell Tissue
Res 1988;253:231-40.
Hynes RO. The impact of molecular biology on models for cell
adhesion. BioEssays 1994;16:663-9.
Coutifaris C, Kao L, Sehdev HM, Chin U, Babalola G. ECadherin expression during the differentiation of trophoblasts. Development 1991;113:767-7.
Loke YW, King A. Trophoblast interaction with extracellular
matrix. In: Loke YW, King A, editors. Human implantation: cell
biology and immunology. New York: Cambridge University
Press; 1995. p. 151-79.
Hynes RO. Integrinsversatility, modulation, and signaling in
cell adhesion. Cell 1992;69:11-25.
Aplin JD. Expression of integrin 64 in human trophoblast
and its loss from extravillous cells. Placenta 1993;14:203-15.
Damsky CH, FitzGerald ML, Fisher SJ. Distribution patterns of
extracellular matrix components and adhesion receptors are
intricately modulated during first trimester cytotrophoblast differentiation along the invasive pathway, in vivo. J Clin Invest
1992;89:210-22.
Burrows TD, King A, Loke YW. Expression of integrins by
human trophoblast and differential adhesion to laminin or fibronectin. Hum Reprod 1993;8:475-84.
Burrows TD, King A, Loke YW. Expression of adhesion molecules by endovascular trophoblast and decidual endothelial
cells: implications for vascular invasion during implantation.
Placenta 1994;15:21-33.
Damsky CH, Librach C, Lim KH, FitzGerald ML, McMaster
MT, Janatpour M, et al. Integrin switching regulates normal
trophoblast invasion. Development 1994;120:3657-66.
Zhou Y, Damsky CH, Chiu K, Roberts JM, Fisher SJ.
Preeclampsia is associated with abnormal expression of adhesion molecules by invasive cytotrophoblasts. J Clin Invest
1993;91:950-60.
Fisher SJ, Damsky CH. Human cytotrophoblast invasion. Semin
Cell Biol 1993;4:183-8.
Loke YW, King A. Clinical implications of defective implantation. In: Loke YW, King A, editors. Human implantation: cell
biology and immunology. New York: Cambridge University
Press, 1995; p. 224-36.
Pijnenborg R, Luyten C, Vercruysse L, Van Assche FA.
Attachment and differentiation in vitro of trophoblast from
normal and preeclamptic human placentas. Am J Obstet
Gynecol 1996;175:30-6.
Divers MJ, Bulmer JN, Miller D, Lilford RJ. Beta 1 integrins in
third trimester human placentae: no differential expression in
pathological pregnancies. Placenta 1995;16:245-60.
Zhou Y, Chiu K, Brescia RJ, Combs CA, Katz MA, Kitzmiller JL,
et al. Increased depth of trophoblast invasion after chronic
constriction of the lower aorta in rhesus monkeys. Am J Obstet
Gynecol 1993;169:224-9.
Meagher EA, FitzGerald GA. Disordered eicosanoid formation
in pregnancy-induced hypertension. Circulation 1993;88;132433.
Wang Y, Walsh SW, Guo J, Zhang J. Maternal levels of prostacyclin, thromboxane, vitamin E and lipid peroxides throughout
normal pregnancy. Am J Obstet Gynecol 1991;165:1690-4.
Gant NF, Daley GI, Chand S, Whalley PJ, MacDonald PC. A
study of angiotensin-II pressor response throughout primigravid pregnancy. J Clin Invest 1973;52:2682-9.
Conrad KP, Colpoys MC. Evidence against the hypothesis that
prostaglandins are the vasodepressor agents of pregnancy. J
Clin Invest 1986;77:236-45.
Mukaddam Daher S, Moutquin JM, Gutkowska BJ, Nuwayhid
BS, Quillen EW Jr. Effects of prostaglandin inhibition on the
renal function curve during ovine pregnancy. Am J Obstet
Gynecol 1994;171:599-607.
Fay TN, Grudzinskas JG. Human endometrial peptides: a review of their potential role in implantation and placentation.
Hum Reprod 1991;6:1311-26.
Daunter B. Immunology of pregnancy: towards a unifying hypothesis. Eur J Obstet Gynecol Reprod Biol 1992;43:81-95.
Dekker and Sibai 1371
Volume 179, Number 5
Am J Obstet Gynecol
42. Morris NH, Eaton BM, Dekker G. Nitric oxide, the endothelium, pregnancy and pre-eclampsia. Br J Obstet Gynaecol
1996;103:4-15.
43. van Buren GA, Yang D, Clark KE. Estrogen-induced uterine vasodilatation is antagonized by L-nitroarginine methyl ester, an
inhibitor of nitric oxide synthesis. Am J Obstet Gynecol
1992;167:828-33.
44. Weiner CP, Lizasoain I, Baylis SA, Knowles RG, Charles IG,
Moncada S. Induction of calcium-dependent nitric oxide synthases by sex hormones. Proc Natl Acad Sci U S A 1994;91:
5212-6.
45. Conrad KP, Joffe GM, Kruszyna H, Kruszyna R, Rochntitryp P,
Chavez JE, et al. Identification of increased nitric oxide biosynthesis during pregnancy in rats. FASEB J 1993;7:566-71.
46. Chu ZM, Beilin LJ. Nitric oxidemediated changes in vascular
reactivity in pregnancy in spontaneously hypertensive rats. Br J
Pharmacol 1993;110:1184-8.
47. Ahokas RA, Mercer BM, Sibai BM. Enhanced endothelium-derived relaxing factor activity in pregnant spontaneously hypertensive rats. Am J Obstet Gynecol 1991;165:801-7.
48. Molnar M, Suto T, Toth T, Hertelendy F. Prolonged blockade
of nitric oxide synthesis in gravid rats produces sustained hypertension, proteinuria, thrombocytopenia and intrauterine
growth retardation. Am J Obstet Gynecol 1994;170:1458-66.
49. Pascoal IF, Umans JG. Effect of pregnancy on mechanisms of
relaxation in human omental microvessels. Hypertension
1996;28:183-7.
50. Myatt L, Brewer A, Langdon G, Brockman DE. Attenuation of
the vasoconstrictor effects of thromboxane and endothelin by
nitric oxide in the human fetal-placental circulation. Am J
Obstet Gynecol 1992;166:224-30.
51. Myatt L, Brockman DE, Langdon G, Pollock JS. Constitutive
calcium-dependent isoform of nitric oxide synthase in the
human placental villous vascular tree. Placenta 1993;14:37383.
52. Myatt L, Brockman DE, Eis AL, Pollock JS. Immunohistochemical
localization of nitric oxide synthase in the human placenta.
Placenta 1993;14:487-95.
53. Buttery LDK, McCarthy A, Springall DR, Sullivan MHF, Elder
MG, Michel T, et al. Endothelial nitric oxide synthase in the
human placenta: regional distribution and proposed regulatory role at the fetomaternal interface. Placenta 1994;15:25765.
54. Morris NH, Sooranna SR, Learmont JG, Poston L, Ramsey B,
Pearson JD, et al. Nitric oxide synthase activities in placental
tissue from normotensive, preeclamptic and growth retarded
pregnancies. Br J Obstet Gynaecol 1995;102:711-4.
55. Toth M, Kukor Z, Romero R, Hertelendy F. Nitric oxide synthase in first-trimester human placenta: characterization and
subcellular distribution. Hypertens Preg 1995;14:287-300.
56. Baker PN, Broughton Pipkin F, Symonds EM. Platelet angiotensin II binding sites in normotensive and hypertensive
women. Br J Obstet Gynaecol 1991;98:436-40.
57. Friedman SA. Preeclampsia: a review of the role of
prostaglandins. Obstet Gynecol 1988;71:122-37.
58. FitzGerald DJ, Rocki W, Murray R, Mayo G, FitzGerald GA.
Thromboxane A2 synthesis in pregnancy-induced hypertension. Lancet 1990;335:751-4.
59. Walsh SW. Preeclampsia: an imbalance in placental prostacyclin and thromboxane production. Am J Obstet Gynecol
1985;152:335-40.
60. Woodworth SH, Li X, Lei ZM, Rao CV, Yussman MA, Spinnato
JA II, et al. Eicosanoid biosynthetic enzymes in placental and
decidual tissues from preeclamptic pregnancies: increased expression of thromboxane-A2 synthase gene. J Clin Endocrinol
Metab 1994;78:1225-31.
61. Zeeman GG, Dekker GA. Pathogenesis of preeclampsia: a hypothesis. Clin Obstet Gynecol 1992;35:317-37.
62. Friedman SA, de Groot CJM, Taylor RN, Golditch BD, Roberts
JM. Plasma cellular fibronectin as a measure of endothelial involvement in preeclampsia and intrauterine growth retardation. Am J Obstet Gynecol 1994;170:838-41.
63. Hsu CD, Iriye B, Johnson TRB, Witter FR, Hong SF, Chan DW.
64.
65.
66.
67.
68.
69.
70.
71.
72.
73.
74.
75.
76.
77.
78.
79.
80.
81.
82.
83.
84.
85.
86.
Elevated circulating thrombomodulin in severe preeclampsia.
Am J Obstet Gynecol 1993;169:148-9.
Friedman SA, Schiff E, Emeis JJ, Dekker GA, Sibai BM.
Biochemical corroboration of endothelial involvement in severe preeclampsia. Am J Obstet Gynecol 1995;172:202-3.
de Boer K, Lecander I, ten Cate JW, Borm JJJ, Treffers PE.
Placental-type plasminogen activator inhibitor in preeclampsia. Am J Obstet Gynecol 1988;158:518-22.
de Groot CJM, Taylor RN. The role of endothelium in pregnancy and pregnancy-related diseases. Curr Obstet Med
1993;2:107-37.
Roberts JM, Taylor RN, Goldfien A. Endothelial cell activation
as a pathogenetic factor in preeclampsia. Semin Perinatol
1991;15:86-93.
Roberts JM, Taylor RN, Goldfien A. Clinical and biochemical
evidence of endothelial cell dysfunction in the pregnancy syndrome preeclampsia. Am J Hypertens 1991;4:700-8.
Kamoi K, Sudo N, Ishibashi M, Yamaji T. Plasma endothelin-1
levels in patients with pregnancy-induced hypertension. N Engl
J Med 1990;323:1486-7.
Nova A, Sibai BM, Barton JR, Mercer BM, Mitchell MD.
Maternal plasma level of endothelin is increased in preeclampsia. Am J Obstet Gynecol 1991;165:724-7.
Taylor RN, Varma M, Teng NH, Roberts JM. Women with
preeclampsia have higher plasma endothelin levels than
women with normal pregnancies. J Clin Endocrinol Metab
1990;71:1675-7.
Kraayenbrink AA, Dekker GA, van Kamp GJ, van Geijn HP.
Endothelial vasoactive mediators in preeclampsia. Am J Obstet
Gynecol 1993;169:160-5.
Barton JR, Sibai BM, Whybrew WD, Mercer BM. Urinary endothelin-l: not a useful marker for preeclampsia. Am J Obstet
Gynecol 1993;168:599-601.
Shanklin DR, Sibai BM. Ultrastructural aspects of preeclampsia. I. Placental bed and uterine boundary vessels. Am J Obstet
Gynecol 1989;161:735-41.
Shanklin DR, Sibai BM. Ultrastructural aspects of preeclampsia. II. Mitochondrial changes. Am J Obstet Gynecol
1990;163:943-53.
Barton JR, Hiett AK, OConnor WN, Nissen SE, Greene JW.
Endomyocardial ultrastructural findings in preeclampsia. Am J
Obstet Gynecol 1991;165:389-91.
Endresen MJ, Tosti E, Lorentzen B, Henriksen T. Sera of
preeclamptic women are not cytotoxic to endothelial cells in
culture. Am J Obstet Gynecol 1995;172:196-201.
McCarthy AL, Woolfson RG, Raju SK, Poston L. Abnormal endothelial cell function of resistance arteries from women with
preeclampsia. Am J Obstet Gynecol 1993;168:1323-30.
Friedman SA, Lubarsky SL, Ahokas RA, Nova A, Sibai BM.
Preeclampsia and related disorders: clinical aspects and relevance of endothelin and nitric oxide. Clin Perinatol
1995;22:343-55.
Davidge ST, Billiar TR, Roberts JM. Plasma nitrites and nitrates,
stable end products of nitric oxide, are elevated in women with
preeclampsia. Hypertens Pregn 1994;13:344.
Cameron IT, van Papendorp CL. Relationship between nitric
oxide synthesis and increase in systolic blood pressure in
women with hypertension in pregnancy. Hypertens Pregn
1993;12:85-92.
Curtis NE, Gude NM, King RG, Marriott PJ, Rook TJ,
Brennecke SP. Nitric oxide in normal human pregnancy and
preeclampsia. Hypertens Pregn 1995;14:339-49.
Lyall F, Young A, Greer IA. Nitric oxide concentrations are increased in the fetoplacental circulation in preeclampsia. Am J
Obstet Gynecol 1995;173:714-8.
Brown MA, Tibben E, Zammit VC, Cario GM, Carlton MA.
Nitric oxide excretion in normal and hypertensive pregnancies. Hypertens Pregn 1995;14:319-26.
Davidge ST, Stranko CP, Roberts JM. Urine but not plasma nitric oxide metabolites are decreased in women with preeclampsia. Am J Obstet Gynecol 1996;174:1008-13.
Vallance P, Collier J. Biology and clinical relevance of nitric
oxide. BMJ 1994;309:453-7.
1372 Dekker and Sibai
87. Fickling SA, Williams D, Vallance P, Nussey SS, Whitley GS.
Plasma concentrations of endogenous inhibitor of nitric oxide
synthesis in normal pregnancy and pre-eclampsia. Lancet
1993;342:242-3.
88. Ramsay B, de Belder A, Campbell S, Moncada S, Martin JF. A
nitric oxide donor improves uterine artery diastolic blood flow
in normal early pregnancy and in women at high risk of preeclampsia. Eur J Clin Invest 1994;24:76-8.
89. Ballegeer VC, Spitz B, De Baene LA, van Assche AF, Hidajar M,
Criel AM. Platelet activation and vascular damage in gestational hypertension. Am J Obstet Gynecol 1992;166:629-33.
90. Halligan A, Bonnar J, Sheppard B, Darling M, Walshe J.
Haemostatic, fibrinolytic and endothelial variables in normal
and pre-eclamptic pregnancies. Br J Obstet Gynaecol
1994;101:488-92.
91. Middelkoop CM, Dekker GA, Kraayenbrink AA, Popp-Snijders
C. Platelet-poor plasma serotonin in normal and preeclamptic
pregnancy. Clin Chem 1993;39:1675-8.
92. Vanhoutte PM. Serotonergic antagonists and vascular disease.
Cardiovasc Drugs Ther 1990;4:7-12.
93. de Jong CLD, Dekker GA, Sibai BM. The renin-angiotensin-aldosterone system in preeclampsia: a review. Clin Perinatol
1991;18:1-29.
94. Mitsuhashi N, Kuwabara Y. Prostaglandin biosynthesis in the
umbilical artery and its relation to fetal growth. Asia Oceania J
Obstet Gynaecol 1994;20:111-4.
95. Wang Y, Walsh SW, Parnell R, Han J. Placental production of
nitric oxide and endothelin in normal and preeclamptic pregnancies. Hypertens Pregn 1994;13:171-8.
96. Ghabour MS, Eis ALW, Brockman DE, Pollock JS, Myatt L.
Immunohistochemical characterization of placental nitric
oxide synthase expression in preeclampsia. Am J Obstet
Gynecol 1995;173:687-94.
97. Eis ALW, Brockman DE, Pollock JS, Myatt L. Immunohistochemical localization of endothelial nitric oxide synthase in
human villous and extravillous trophoblast populations and expression during syncytiotrophoblast formation in vitro.
Placenta 1995;16:113-26.
98. Smarason AK, Sargent IL, Starkey PM, Redman CWG. The effect of placental syncytiotrophoblast microvillous membranes
from normal and pre-eclamptic women on the growth of endothelial cells in vivo. Br J Obstet Gynaecol 1993;100:943-9.
99. Sargent IL, Johansen M, Chua S, Redman CWG. Clinical experience: isolating trophoblasts from maternal blood. Ann N Y
Acad Sci 1994;731:154-61.
100. Chua S, Wilkins T, Sargent I, Redman C. Trophoblast deportation in pre-eclamptic pregnancy. Br J Obstet Gynaecol
1991;98:973-9.
101. Arkwright PD, Rademacher TW, Dwek RA, Redman CWG.
Preeclampsia is associated with an increase in trophoblast
glycogen content and glycogen synthase activity, similar to that
found in hydatidiform moles. J Clin Invest 1993;91:2744-53.
102. Ding Z, Rowe J, Sinosich M, Saunders DM, Gallery EDM.
Secretion of vasoactive substances by cultured human villous
cytotrophoblasts. Hypertens Pregn 1994;13:352-7.
103. Tsukimori K, Ishida K, Maeda H, Koyanagi T, Nakano H. The
placenta as possible source of the factor causing endothelial
cell injury in preeclampsia. Hypertens Pregn 1994;13:358.
104. Lockwood CJ, Peters JH. Increased plasma levels of ED1(+) cellular fibronectin precede the clinical signs of preeclampsia.
Am J Obstet Gynecol 1990;162:358-62.
105. Taylor RN, Heilbron DC, Roberts JM. Growth factor activity in
the blood of women in whom preeclampsia develops is elevated from early pregnancy. Am J Obstet Gynecol
1990;163:1839-44.
106. Cross JC. Trophoblast function in normal and preeclamptic
pregnancy. Fetal Matern Med Rev 1996;8:57-66.
107. Lorentzen B, Endresen MJ, Clausen T, Henriksen T. Fasting
serum free fatty acids and triglycerides are increased before 20
weeks of gestation in women who later develop preeclampsia.
Hypertens Pregn 1994;13:103-9.
108. Endresen MJ, Lorentzen B, Henriksen T. Increased lipolytic activity and high ratio of free fatty acids to albumin in sera from
November 1998
Am J Obstet Gynecol
109.
110.
111.
112.
113.
114.
115.
116.
117.
118.
119.
120.
121.
122.
123.
124.
125.
126.
127.
128.
129.
130.
women with preeclampsia leads to triglyceride accumulation in
cultured endothelial cells. Am J Obstet Gynecol 1992;167:4407.
Endresen MJ, Lorentzen B, Henriksen T. Increased lipolytic activity of sera from pre-eclamptic women due to the presence of
a lysophospholipase. Scand J Clin Lab Invest 1993;53:733-9.
Endresen MJ, Tosti E, Heimli H, Lorentzen B, Henriksen T.
Effects of free fatty acids found increased in women who develop pre-eclampsia on the ability of endothelial cells to produce prostacyclin, cGMP and inhibit platelet aggregation.
Scand J Clin Lab Invest 1994;54:549-57.
Arbogast BW, Leeper SC, Merrick RD, Olive KE, Taylor RN.
Hypothesis: which plasma factors bring about disturbance of
endothelial function in pre-eclampsia? Lancet 1994;343:340-1.
Lorentzen B, Drevon CA, Endresen MJ, Henriksen T. Fatty acid
pattern of esterified and free fatty acids in sera of women with
normal and pre-eclamptic pregnancy. Br J Obstet Gynaecol
1995;102:530-7.
Sattar N, Gaw A, Packard CJ, Greer IA. Potential pathogenic
roles of aberrant lipoprotein and fatty acid metabolism in
preeclampsia. Br J Obstet Gynaecol 1996;103:614-20.
Loke YW, King A. Immunology of human placental implantation: clinical implications of our current understanding. Mol
Med Today 1997;Apr:153-9.
Sargent IL. Maternal and fetal immune responses during pregnancy. Exp Clin Immunogenet 1993;10:85-102.
Carosella ED, Dausset J, Kirszenbaum M. HLA-G revisited.
Immunol Today 1996;17:407-9.
Shorter SC, Starkey PM, Ferry BL, Clover LM, Sargent IL,
Redman CWG. Antigenic heterogeneity of human cytotrophoblast and evidence for the transient expression of MHC
class I antigens distinct from HLA-G. Placenta 1993;14:571-82.
van der Ven K, Ober C. HLA-G polymorphisms in African
Americans. J Immunol 1994;153:5628-33.
Starkey PM. The decidua and factors controlling placentation.
In: Redman CWG, Sargent LL, Starkey PM, editors. The
human placenta. Oxford (United Kingdom): Blackwell
Scientific Publications; 1993. p. 362-413.
Saito S, Nishikawa K, Morii T, Enomoto M, Narita N, Motoyoshi
K, et al. Cytokine production by CD16 CD56 bright natural
killer cells in human pregnancy decidua. Int Immunol
1993;5:559-63.
Deniz G, Christmas SE, Brew R, Johnson PM. Phenotypic and
functional cellular differences between human CD3(-) decidual and peripheral blood leukocytes. J Immunol
1994;152:4255-61.
Klein J, Ohuigin C. The conundrum of nonclassical major histocompatibility complex genes. Proc Natl Acad Sci U S A
1994;91:6251-2.
Chumbley G, King A, Robertson K, Holmes N, Loke YW.
Resistance of HLA-G and HLA-A2 transfectants to lysis by decidual NK cells. Cell Immunol 1994;155:312-22.
Ljunggren HG, Karre K. In search of the missing self MHC
molecules and NK cell recognition. Immunol Today
1990;11:237-44.
Jurisicova A, Casper RF, MacLusky NJ, Mills GB, Librach CL.
HLA-G expression during preimplantation human embryo development. Proc Natl Acad Sci U S A 1996;93:161-5.
McMaster MT, Librach CL, Zhou Y, Lim KH, Janatpour MJ,
DeMars R, et al. Human placental HLA-G expression is restricted to differentiated cytotrophoblasts. J Immunol
1995;154:3771-8.
Colbern GT, Chiang MH, Main EK. Expression of the nonclassic histocompatibility antigen HLA-G by preeclamptic placenta. Am J Obstet Gynecol 1994;170:1244-50.
King A, Balendran N, Wooding P, Carter NP, Loke YW. CD3
leukocytes present in the human uterus during early placentation: phenotypic and morphologic characterization of the
CD56++ population. Dev Immunol 1991;1:169-90.
Wegmann TG. Maternal T cells promote placental growth and
prevent spontaneous abortion. Immunol Lett 1988;17:297302.
Shorter SC, Vince GS, Starkey PM. Production of granulocyte-
Volume 179, Number 5
Am J Obstet Gynecol
131.
132.
133.
134.
135.
136.
137.
138.
139.
140.
141.
142.
143.
144.
145.
146.
147.
148.
149.
150.
151.
152.
153.
154.
colony stimulating factor at the materno-foetal interface in
human pregnancy. Immunology 1992;75:468-74.
Giudice LC. Growth factors and growth modulators in human
uterine endometrium: their potential relevance to reproductive medicine. Fertil Steril 1994;61:1-17.
Aoki K, Kajiura S, Matsumoto Y, Ogasawara M, Okada S,
Yagami Y, et al. Preconceptional natural-killer-cell activity as a
predictor of miscarriage. Lancet 1995;345:1340-2.
Clark DA. Cytokines, decidua, and early pregnancy. Oxf Rev
Reprod Biol 1993;15:83-111.
Giudice LC. Growth factors and growth modulators in human
uterine endometrium: their potential relevance to reproductive medicine. Fertil Steril 1994;61:1-17.
Mosmann TR, Cherwinski H, Bond MW. Two types of murine
helper T cell clone. I. Definition according to profiles of lymphokine activities and secreted proteins. J Immunol
1986;136:2348-57.
Mosmann TR, Moore KW. The role of Il-10 in cross-regulation
of Thl and Th2 responses. Immunol Today 1991;12:A49-53.
Wegmann TG, Lin H, Guilbert L, Mosmann TR. Bidirectional
cytokine interactions in the maternal-fetal relationship: is successful pregnancy a Th2 phenomenon? Immunol Today
1993;15:353-6.
Varner MW. Autoimmune disorders and pregnancy. Semin
Perinatol 1991;15:238-50.
Cadet P, Rady PL, Tyring SK, Yandell RB, Hughes TK.
Interleukin-10 messenger ribonucleic acid in human placenta:
implications of a role for interleukin-10 in fetal allograft protection. Am J Obstet Gynecol 1995;173:25-9.
Goodwin JS, Ceuppens J. Regulation of the immune response
by prostaglandins. J Clin Immunol 1983;3:295-315.
Lin H, Mosmann TR, Guilbert L, Tuntipopipat S, Wegmann
TG. Synthesis of T helper 2-type cytokines at the maternal fetal
interface. J Immunol 1993;151:4562-73.
Kuhn R, Lohler J, Rennick D. Interleukin-10-deficient mice develop chronic enterocolitis. Cell 1993;75:263-74.
Jones JI, Clemmons DR. Insulin-like growth factors and their
binding proteins: biological actions. Endocr Rev 1995;16:3-34.
Jones JI, Gockerman A, Busby WH, Wright G, Clemmons DR.
Insulin-like growth factor binding protein 1 stimulates cell migration and binds to the 51 integrin by means of its arg-glyasp sequence. Proc Natl Acad Sci U S A 1993;90:10553-7.
Milio LA, Hu J, Douglas GC. Binding of insulin-like growth factor I to human trophoblast cells during differentiation in vitro.
Placenta 1994;15:641-51.
de Groot CJM, OBrien TJ, Taylor RN. Biochemical evidence of
impaired trophoblastic invasion of decidual stroma in women
destined to have preeclampsia. Am J Obstet Gynecol
1996;175:24-9.
Redman CWG. Immunology of preeclampsia. Semin Perinatol
1991;15;257-62.
Robillard PY, Hulsey TC, Alexander GR, Keenan A, de Caunes
F, Papiernik E. Paternity patterns and risk of preeclampsia in
the last pregnancy in multiparae. J Reprod Immunol 1993;24:112.
Trupin LS, Simon LP, Eskenazi B. Change in paternity: a risk
factor for preeclampsia in multiparas. Epidemiology
1996;7:240-4.
Serhal PF, Craft IL. Oocyte donation in 61 patients. Lancet
1989;1:1185-7.
Robillard PY, Hulsey TC, Perianin J, Janky E, Miri EH,
Papiernik E. Association of pregnancy-induced hypertension
with duration of sexual cohabitation before conception.
Lancet 1994;344:973-5.
Bardeguez AD, McNerney R, Frieri M, Verma UL, Tejani N.
Cellular immunity in preeclampsia: alterations in T-lymphocyte
subpopulations during early pregnancy. Obstet Gynecol
1991;77:859-62.
Rappaport VJ, Hirata G, Kim Yap H, Jordan SC. Anti-vascular
endothelial cell antibodies in severe preeclampsia. Am J Obstet
Gynecol 1990;162:138-46.
Labarrere C. Acute atherosis. A histopathological hallmark of
immune aggression? Placenta 1988;9:95-108.
Dekker and Sibai 1373
155. Butterworth BH, Greer IA, Liston WA, Haddad NG, Johnston
TA. Immunocytochemical localization of neutrophil elastase in
term placenta decidua and myometrium in pregnancy-induced
hypertension. Br J Obstet Gynaecol 1991;98:929-33.
156. Greer IA, Leask R, Hodson BA, Dawes J, Kilpatrick DC, Liston
WA. Endothelin, elastase, and endothelial dysfunction in
preeclampsia. Lancet 1991;337:558.
157. Yoshizumi M, Perrella MA, Burnett JC Jr, Lee MET. Tumor
necrosis factor downregulates an endothelial nitric oxide synthase mRNA by shortening its half-life. Circ Res 1993;73:205-9.
158. Chen G, Wilson R, Wang SH, Zheng HZ, Walker JJ, McKillop
JH. Tumour necrosis factor-alpha (TNF-) gene polymorphism
and expression in preeclampsia. Clin Exp Immunol
1996;104:154-9.
159. Kupferminc MJ, Peaceman AM, Wigton TR, Rehnberg KA,
Socol ML. Tumor necrosis factor-alpha is elevated in plasma
and amniotic fluid of patients with severe preeclampsia. Am J
Obstet Gynecol 1994;170:1752-7.
160. Schiff E, Friedman SA, Baumann P, Sibai BM, Romero R.
Tumor necrosis factor-alpha in pregnancies associated with
preeclampsia or small-for-gestational-age newborns. Am J
Obstet Gynecol 1994;170:1224-9.
161. Meekins JW, McLaughlin PJ, West DC, McFadyen IR, Johnson
PM. Endothelial cell activation by tumour necrosis factor-alpha
(TNF-alpha) and the development of pre-eclampsia. Clin Exp
Immunol 1994;98:110-4.
162. Kupferminc MJ, Peaceman AM, Aderka D, Wallach D, Peyser
MR, Lessing JB, et al. Soluble tumor necrosis factor receptors
in maternal plasma and second-trimester amniotic fluid. Am J
Obstet Gynecol 1995;173:900-5.
163. Stark M, Jones SJ, Johansen K, Blake L, Shaw R. Tumour necrosis factor. Lancet 1995;345:648-9.
164. Vince GS, Starkey PM, Austgulen R, Kwiatkowski D, Redman
CWG. Interleukin-6, tumour necrosis factor and soluble tumour necrosis factor receptors in women with pre-eclampsia.
Br J Obstet Gynaecol 1995;102:20-5.
165. Kupferminc MJ, Peaceman AM, Wigton TR, Tamura RK,
Rehnberg KA, Socol ML. Immunoreactive tumor necrosis factor-alpha is elevated in maternal plasma but undetected in amniotic fluid in the second trimester. Am J Obstet Gynecol
1994;171:976-9.
166. Greer IA, Lyall F, Perera T, Boswell F, Macara LM. Increased
concentrations of cytokines, interleukin-6 and interleukin-1 receptor antagonist in plasma of women with preeclampsia: a
mechanism for endothelial dysfunction? Obstet Gynecol
1994;84:937-40.
167. Silver RM, Schwinzer B, McGregor JA. Interleukin-6 levels in
amniotic fluid in normal and abnormal pregnancies:
preeclampsia, small-for-gestational-age fetus, and premature
labor. Am J Obstet Gynecol 1993;169:1101-5.
168. Toohey JS, Morgan MA, Yaziri ND, Yousefi S, de Veciana M,
Lien J. Longitudinal plasma ICAM-1 & IFN- in pre-eclampsia.
Hypertens Pregn 1994;13:319.
169. Lyall F, Greer IA, Boswell F, Macara LM, Walker JJ. The cell adhesion molecule, VCAM-1, is selectively elevated in serum in
pre-eclampsia: does this indicate the mechanism of leukocyte
activation? Br J Obstet Gynaecol 1994;101:485-7.
170. Lyall F, Greer IA, Boswell F, Young A, Macara LM, Jeffers MD.
Expression of cell adhesion molecules in placentae from pregnancies complicated by pre-eclampsia and intrauterine growth
retardation. Placenta 1995;16:579-87.
171. Cheeseman KH, Slater TF. An introduction to free radical biochemistry. Br Med Bull 1993;49:481-93.
172. Holley AE, Cheeseman KH. Measuring free radical reactions in
vivo. Br Med Bull 1993;49:494-505.
173. Esterbauer H, Wg G, Puhl H. Lipid peroxidation and its role
in atherosclerosis. Br Med Bull 1993;49:566-76.
174. Hubel CA, Roberts JM, Taylor RN, Musci TJ, Rogers GM,
McLaughlin MK. Lipid peroxidation in pregnancy: new perspectives on preeclampsia. Am J Obstet Gynecol
1989;161:1025-34.
175. Walsh SW. Lipid peroxidation in pregnancy. Hypertens Pregn
1994;13:1-31.
1374 Dekker and Sibai
176. Dekker GA, Kraayenbrink AA. Oxygen free radicals in
preeclampsia. Am J Obstet Gynecol 1991;164:273.
177. Wang Y, Walsh SW, Guo J, Zhang J. The imbalance between
thromboxane and prostacyclin in preeclampsia is associated
with an imbalance between lipid peroxides and vitamin E in
maternal blood. Am J Obstet Gynecol 1991;165:1695-700.
178. Uotila JT, Tuimala RJ, Aarnio TM. Findings on lipid peroxidation and antioxidant function in hypertensive complications of
pregnancy. Br J Obstet Gynaecol 1993;100:270-6.
179. Kloner RA, Przyklenk K, Whittaker P. Deleterious effects of oxygen radicals in ischemia/reperfusion, resolved and unresolved
issues. Circulation 1989;80:115-27.
180. Branch DW, Mitchell MD, Miller E, Palinski W, Wiztum JL. Preeclampsia and serum antibodies to oxidized low-density
lipoprotein. Lancet 1994;343:645-6.
181. Armstrong VW, Wieland E, Diedrich F, Renner A, Rath W,
Kreuzer H, et al. Serum antibodies to oxidised low-density
lipoprotein in pre-eclampsia and coronary heart disease [letter]. Lancet 1994;343;1570.
182. Friedl HP, Till GO, Ryan US, Ward PA. Mediator-induced activation of xanthine oxidase in endothelial cells. FASEB J
1989;3:2512-8.
183. Becker BF. Towards the physiological function of uric acid.
Free Radic Biol Med 1993;14:615-31.
184. Phan SH, Gannon DE, Varani J, Ryan US, Ward PA. Xanthine
oxidase activity in rat pulmonary artery endothelial cells and its
modulation by activated neutrophils. Am J Pathol 1989;134:
1201-11.
185. Ward PA. Mechanisms of endothelial cell killing by H2O2 or
products of activated neutrophils. Am J Med 1991;91:89S-94S.
186. Varani J, Ginsburg I, Schuger L, Gibbs DF, Bromberg J,
Johnson KJ, et al. Endothelial cell killing by neutrophils: synergistic interaction of oxygen products and proteases. Am J
Pathol 1989;135:435-8.
187. Higgs GA, Vane JR. Inhibition of cyclooxygenase and lipoxygenase. Br Med Bull 1983;39:265-70.
188. Garzetti GG, Tranquilli AL, Cugini AM, Mazzanti L, Cester N,
Romanini C. Altered lipid composition, increased lipid peroxidation, and altered fluidity of the membrane as evidence of
platelet damage in preeclampsia. Obstet Gynecol 1993;81:33740.
189. Katusic ZS, Vanhoutte PJM. Superoxide anion and endothelial
regulation of arterial tone. Semin Perinatol 1991;15:30-3.
190. Yang X, Cai B, Sciacca RR, Cannon PJ. Inhibition of inducible
nitric oxide synthase in macrophages by oxidized low-density
lipoproteins. Circ Res 1994;74:318-28.
191. Kugiyama K, Sakamoto T, Misumi I, Sugiyama S, Ohgushi M,
Ogawa H, et al. Transferable lipids in oxidized low-density
lipoprotein stimulate plasminogen activator inhibitor-1 and inhibit tissue-type plasminogen activator release from endothelial cells. Circ Res 1993;73:335-43.
192. Cester N, Mazzanti L, Benedetti G, Cugini AM, Rabini RA,
Tranquilli AL, et al. Pregnancy-induced hypertension: observations on chemical-physical properties of syncytiotrophoblast
plasma membranes from human placentae. Clin Exp
Hypertens [B] Hypertens Pregn 1988;B7:57-66.
193. Uotila JT, Kirkkola AL, Rorarius M, Tuimala RJ, Metsa-Ketela T.
The total peroxyl radical-trapping ability of plasma and cerebrospinal fluid in normal and preeclamptic parturients. Free
Radic Biol Med 1994;16:581-90.
194. Many A, Hubel CA, Roberts JM. Hyperuricemia and xanthine
oxidase in preeclampsia, revisited. Am J Obstet Gynecol
1996;174:288-91.
195. Jain SK, Wise R. Relationship between elevated lipid peroxides,
vitamin E deficiency and hypertension in preeclampsia. Mol
Cell Biochem 1995;151:33-8.
196. Rebelo I, Carvalho-Guerra F, Pereira-Leite L, Quintanilha A.
Comparative study of lactoferrin and other markers of inflammatory stress between preeclamptic and normal pregnancies.
Eur J Obstet Gynecol Reprod Biol 1996;64:167-73.
197. Aust SD, Koppenol WH. Transition metals in oxidative stress:
November 1998
Am J Obstet Gynecol
198.
199.
200.
201.
202.
203.
204.
205.
206.
207.
208.
209.
210.
211.
212.
213.
214.
215.
216.
217.
218.
219.
220.
an overview. In: Davies KJA, editor. Oxidative damage and repair: chemical, biological and medical aspects. Oxford (United
Kingdom): Pergamon Press; 1990. p. 802-7.
Halliwell B, Gutteridge JMC, Cross CE. Free radicals, antioxidants, and human disease: where are we now? J Lab Clin Med
1992;119:598-620.
Davidge ST, Hubel CA, Brayden RN, Capeless EC, McLaughlin
MK. Sera antioxidant activity in uncomplicated and preeclamptic pregnancies. Obstet Gynecol 1992;79:897-901.
Walsh SW, Wang Y. Deficient glutathione peroxidase activity in
preeclampsia is associated with increased placental production
of thromboxane and lipid peroxides. Am J Obstet Gynecol
1993;169:1456-61.
Mikhail MS, Anyaegbunam A, Garfinkel D, Palan PR, Basu J,
Romney SL. Preeclampsia and antioxidant nutrients: decreased plasma levels of reduced ascorbic acid, alpha-tocopherol, and beta-carotene in women with preeclampsia. Am J
Obstet Gynecol 1994;171:150-7.
Stark JM. Pre-eclampsia and cytokine induced oxidative stress.
Br J Obstet Gynaecol 1993;100:105-9.
Conrad KP, Benyo DF. Placental cytokines and the pathogenesis of preeclampsia. Am J Reprod Biol 1997;37:240-9.
Chesley LC, Annitto JE, Cosgrove RA. The familial factor in
toxemia of pregnancy. Obstet Gynecol 1968;32:303-11.
Cooper DW, Brennecke SP, Wilton AN. Genetics of preeclampsia. Hypertens Pregn 1993;12:1-23.
Arngrimsson R, Bjornsson S, Geirsson RT, Bjornsson H, Walker
JJ, Snaedal G. Genetic and familial predisposition to eclampsia
and pre-eclampsia in a defined population. Br J Obstet
Gynaecol 1990;97:762-9.
Thornton JC, Onwude JL. Pre-eclampsia: discordance among
identical twins. BMJ 1991;303:1241-2.
Wilcken B, Leung KC, Hammond J, Kamath R, Leonard JV.
Pregnancy and fetal long-chain 3-hydroxyacyl coenzyme: a dehydrogenase deficiency. Lancet 1993;341:407-8.
Boyd PA, Lindenbaum RH, Redman C. Preeclampsia and trisomy 13: a possible association. Lancet 1987;2:397-9.
Arngrimsson R, Connor JM, Geirsson RT, Brennecke S, Cooper
DW. Is genetic susceptibility for pre-eclampsia and eclampsia
associated with implantation failure and fetal demise? Lancet
1994;343:1643-4.
Kilpatrick DC, Gibson F, Livingston J, Liston WA. Preeclampsia
is associated with HLA-DR4 sharing between mother and fetus.
Tissue Antigens 1990;35:178-81.
Wilton AN, Barendse WJ, Donald JA, Marshall P, Trudinger B,
Gallery EDM, et al. HLA-DRB types in pre-eclampsia and
eclampsia. Tissue Antigens 1991;38:137-41.
Hayward C, Livingstone J, Holloway S, Liston WA, Brock DJH.
An exclusion map for pre-eclampsia: assuming autosomal recessive inheritance. Am J Hum Genet 1992;50:749-57.
Peterson RDA, Tuck-Muller CM, Spinnato JA, Peevy K, Giattina
K, Hoff C. Short communication: an HLA-haplotype associated
with preeclampsia and intrauterine growth retardation. Am J
Reprod Immunol 1994;31:177-9.
Humphrey KE, Harrison GA, Cooper DW, Wilton AN,
Brennecke SP, Trudinger BJ. HLA-G deletion polymorphisms
and preeclampsia/eclampsia. Br J Obstet Gynaecol 1995;
102:707-10.
Ward K, Hata A, Jeunemaitre X, Helin C, Nelson L, Namikawa
C, et al. A molecular variant of angiotensinogen associated with
preeclampsia. Nat Genet 1993;4:59-61.
Morgan L, Baker P, Broughton-Pipkin F, Kalsheker N.
Preeclampsia and the angiotensinogen gene. Br J Obstet
Gynaecol 1995;102:489-90.
Wilton AN, Kaye JA, Guo G, Brennecke SP, Cooper DW. Is angiotensinogen a good candidate gene for preeclampsia?
Hypertens Pregn 1995;14:251-60.
Herrera VLM, Ruiz-Opazo N. Beyond genetic markers: hypertension genes. J Hypertens 1994;12:847-56.
Cox BE, Word RA, Rosenfeld CR. Angiotensin II receptor characteristics and subtype expression in uterine arteries and my-
Dekker and Sibai 1375
Volume 179, Number 5
Am J Obstet Gynecol
221.
222.
223.
224.
225.
226.
227.
228.
ometrium during pregnancy. J Clin Endocrinol Metab
1996;81:49-58.
Knock GA, Sullivan MHF, McCarthy A, Elder MG, Polak JM,
Wharton J. Angiotensin II (AT-1) vascular binding sites in
human placentae from normal-term, preeclamptic and growth
retarded pregnancies. J Pharmacol Exp Ther 1994;271:100715.
Torbergsen T, Oian P, Mathiesen E, Borud O. Preeclampsia: a
mitochondrial disease? Acta Obstet Gynecol Scand 1989;
68:145-8.
Furui T, Kurauchi O, Tanaka M, Mizutani S, Ozawa T, Tomoda
Y. Decrease in cytochrome c oxidase and cytochrome oxidase
subunit I messenger RNA levels in preeclampsia pregnancies.
Obstet Gynecol 1994;84:283-8.
Haig D. Genetic conflicts in human pregnancy. Q Rev Biol
1993;68:495-532.
McCowan LME, Becroft DMO. Beckwith-Wiedemann syndrome, placental abnormalities, and gestational proteinuric
hypertension. Obstet Gynecol 1994;83:813-7.
Ekstrom TJ. Parental imprinting and the IGF2 gene. Horm Res
1994;42:176-81.
Kanbour-Shakir A, Zhang X, Rouleau A, Armstrong DT, Kunz
HW, Macpherson TA, et al. Gene imprinting and major histocompatibility complex class I antigen expression in the rat placenta. Proc Natl Acad Sci U S A 1990;87:444-8.
Dekker GA, de Vries JIP, Doelitzsch PM, Huijgens PC, von
Blomberg BME, Jakobs C, et al. Underlying disorders associ-
229.
230.
231.
232.
233.
234.
235.
236.
237.
ated with severe early-onset preeclampsia. Am J Obstet Gynecol
1995;173:1042-8.
Reiter L, Brown MA, Whitworth JA. Hypertension in pregnancy: the incidence of underlying renal disease and essential
hypertension. Am J Kidney Dis 1994;24:883-7.
Sibai BM, Gordon T, Thom E, Caritis SN, Klebanoff M,
McNellis D, et al. Risk factors for preeclampsia in healthy nulliparous women: a prospective multicenter study. Am J Obstet
Gynecol 1995;172:642-8.
Easterling TR, Benedetti TJ, Schmucker BC, Millard SP.
Maternal hemodynamics in normal and preeclamptic pregnancies: a longitudinal study. Obstet Gynecol 1990;76:1061-9.
Unger RH. Perspectives in diabetes: lipotoxicity in the pathogenesis of obesity-dependent NIDDM. Diabetes 1995;44:863-70.
Reaven GM. Pathophysiology of insulin resistance in human
disease. Physiol Rev 1995;75:473-85.
Fuh MM, Yin CS, Pei D, Sheu WH, Jeng CY, Chen YI, et al.
Resistance to insulin-mediated glucose uptake and hyperinsulinemia in women who had preeclampsia during pregnancy.
Am J Hypertens 1995;8:768-71.
Julius S, Jamerson K. Sympathetics, insulin resistance and coronary risk in hypertension: the chicken-and-egg question. J
Hypertens 1994;12:495-502.
Stern MP. Perspectives in diabetes: diabetes and cardiovascular
disease. The common soil hypothesis. Diabetes 1995;44:369-74.
Cunningham JM, Green IC. Cytokines, nitric oxide and insulin
secreting cells. Growth Regul 1994;4:173-80.
Anda mungkin juga menyukai
- 1477 7827 5 6 PDFDokumen14 halaman1477 7827 5 6 PDFKaleb Rudy HartawanBelum ada peringkat
- Why Is Placentation Abnormal in Preeclampsia?Dokumen8 halamanWhy Is Placentation Abnormal in Preeclampsia?cecilliacynthiaBelum ada peringkat
- GGHFDGHDHJJ 7549gfh NDokumen8 halamanGGHFDGHDHJJ 7549gfh NthBelum ada peringkat
- Molecular Mechanism of ImplantationDokumen19 halamanMolecular Mechanism of ImplantationAbunu TilayeBelum ada peringkat
- M 105Dokumen8 halamanM 105midwfjessica4Belum ada peringkat
- Fournier 2011Dokumen9 halamanFournier 2011Nofi NurinaBelum ada peringkat
- Regulation of Blastocyst Formation.Dokumen24 halamanRegulation of Blastocyst Formation.christopher LopezBelum ada peringkat
- Immunology of PreeclampsiaDokumen13 halamanImmunology of PreeclampsiaRohmantuah_Tra_1826Belum ada peringkat
- Kaufmann-2004-Aspects of Human Fetoplacental V PDFDokumen13 halamanKaufmann-2004-Aspects of Human Fetoplacental V PDFNguyễn Cao VânBelum ada peringkat
- Early Development of The Human Placenta and Pregnancy ComplicationsDokumen9 halamanEarly Development of The Human Placenta and Pregnancy ComplicationsSherilinne Quiles LópezBelum ada peringkat
- Artigo Endocytosis in The Placenta An Undervalued Mediator of Placental TransferDokumen7 halamanArtigo Endocytosis in The Placenta An Undervalued Mediator of Placental TransferSarah Saene da Silva NoiaBelum ada peringkat
- Mechanisms of Disease: I S E PDokumen9 halamanMechanisms of Disease: I S E Plupiz717Belum ada peringkat
- Endometrial Receptivity BiomarkersDokumen19 halamanEndometrial Receptivity BiomarkersEndriana Gak Endut EndutBelum ada peringkat
- 10 1016@j Ajog 2019 07 010 PDFDokumen13 halaman10 1016@j Ajog 2019 07 010 PDFDaniel GamarraBelum ada peringkat
- Dr. Diah Rumekti hadiatiAPCGS JogjaDokumen25 halamanDr. Diah Rumekti hadiatiAPCGS JogjacirererereBelum ada peringkat
- Funcion Endocrina de La Placenta HumanaDokumen30 halamanFuncion Endocrina de La Placenta HumanaSofia RossoBelum ada peringkat
- Reproductive Biology and EndocrinologyDokumen4 halamanReproductive Biology and EndocrinologyAnditha Namira RSBelum ada peringkat
- Section 1: Cellular AdaptationsDokumen30 halamanSection 1: Cellular Adaptationshaddi awanBelum ada peringkat
- Section 1: Cellular AdaptationsDokumen30 halamanSection 1: Cellular AdaptationsElena PoriazovaBelum ada peringkat
- Inflammatory Networks in The Control of Spermatogenesis: Chronic Inflammation in An Immunologically Privileged Tissue?Dokumen23 halamanInflammatory Networks in The Control of Spermatogenesis: Chronic Inflammation in An Immunologically Privileged Tissue?Bobby's SetyabudiBelum ada peringkat
- Sjogrensyndromecme1 151224004322Dokumen56 halamanSjogrensyndromecme1 151224004322Andreea StaicuBelum ada peringkat
- The Coagulation System in ChildrenDokumen7 halamanThe Coagulation System in ChildrenlastrironauliBelum ada peringkat
- Cme Reviewarticle: The Role of Genes in The Development of Mullerian AnomaliesDokumen9 halamanCme Reviewarticle: The Role of Genes in The Development of Mullerian Anomaliesapi-54418266Belum ada peringkat
- CH 5 Implantation, Placental Dev (Part1)Dokumen36 halamanCH 5 Implantation, Placental Dev (Part1)Tengku Chairannisa PutriBelum ada peringkat
- Role of The Monocyte-Macrophage System in Normal Pregnancy and PreeclampsiaDokumen17 halamanRole of The Monocyte-Macrophage System in Normal Pregnancy and PreeclampsiadavidBelum ada peringkat
- Gyne. FertilizationDokumen10 halamanGyne. FertilizationdorquinloveBelum ada peringkat
- Placental Origins of PEDokumen7 halamanPlacental Origins of PENi Wayan Ana PsBelum ada peringkat
- Endocrinology of Ectopic PregnancyDokumen16 halamanEndocrinology of Ectopic PregnancyJulian Andres CastroBelum ada peringkat
- Molecular Mechanism of ImplantationDokumen5 halamanMolecular Mechanism of Implantationarunnene2Belum ada peringkat
- Pregnancy (Group1)Dokumen10 halamanPregnancy (Group1)Gustavo PerezBelum ada peringkat
- Ruiz-Iraztorza Et Al (2010) - Antiphospholipid SyndromeDokumen13 halamanRuiz-Iraztorza Et Al (2010) - Antiphospholipid SyndromextraqrkyBelum ada peringkat
- Vascular Endothelium: An Integrator of Pathophysiologic Stimuli in AtherosclerosisDokumen4 halamanVascular Endothelium: An Integrator of Pathophysiologic Stimuli in AtherosclerosisNithin CBelum ada peringkat
- 1st, 2nd & 3rdweeksDokumen9 halaman1st, 2nd & 3rdweeksPristine KrBelum ada peringkat
- Gestational Trophoblastic NeoplasiaDokumen18 halamanGestational Trophoblastic NeoplasiaTanuj sai kumarBelum ada peringkat
- EportfolioDokumen7 halamanEportfolioapi-344036469Belum ada peringkat
- Pulmonary Hypertension Advances in Pathogenesis and TreatmentDokumen12 halamanPulmonary Hypertension Advances in Pathogenesis and Treatmentbdalcin5512Belum ada peringkat
- Vol IDokumen273 halamanVol IReza ParkerBelum ada peringkat
- Uterine Fibroids: Review ArticleDokumen12 halamanUterine Fibroids: Review ArticleDusty SandBelum ada peringkat
- Defense Mechanisms of the GingivaDokumen249 halamanDefense Mechanisms of the GingivaAssssssBelum ada peringkat
- Early Conceptus Growth andDokumen7 halamanEarly Conceptus Growth andJunlianty UnhyBelum ada peringkat
- Fetal-Placental DisordersDari EverandFetal-Placental DisordersNicholas S. AssaliPenilaian: 5 dari 5 bintang5/5 (1)
- ArtiDokumen4 halamanArtiNur Laila FaizahBelum ada peringkat
- Etiology, Clinical Manifestations, and Prediction of Placental AbruptionDokumen9 halamanEtiology, Clinical Manifestations, and Prediction of Placental AbruptionKadije OanaBelum ada peringkat
- A Microphysiological Model of Human Trophoblast Invasion During ImplantationDokumen18 halamanA Microphysiological Model of Human Trophoblast Invasion During ImplantationLucas HeBelum ada peringkat
- Final - Artic Ro Imf&Gd ModifDokumen8 halamanFinal - Artic Ro Imf&Gd ModifAnonymous eson90Belum ada peringkat
- Meyer Et Al. 2004Dokumen15 halamanMeyer Et Al. 2004Aline Freitas de MeloBelum ada peringkat
- Update On Mechanisms of Ultrafiltration FailureDokumen5 halamanUpdate On Mechanisms of Ultrafiltration Failurerodrigoch2009Belum ada peringkat
- Fast Facts: Myelofibrosis: Reviewed by Professor Ruben A. MesaDari EverandFast Facts: Myelofibrosis: Reviewed by Professor Ruben A. MesaBelum ada peringkat
- Fisiologi HaidDokumen66 halamanFisiologi HaidRizna AriyaniBelum ada peringkat
- In Vitro Spheroid Model of Placental Vasculogenesis: Does It Work?Dokumen12 halamanIn Vitro Spheroid Model of Placental Vasculogenesis: Does It Work?constantinilieBelum ada peringkat
- Tumor Cell Interaction with Lymphatic Vessels in Cancer Progression and MetastasisDokumen10 halamanTumor Cell Interaction with Lymphatic Vessels in Cancer Progression and MetastasisChetan PatilBelum ada peringkat
- 2008 - Huppertz - The Anatomy of The Normal PlacentaDokumen8 halaman2008 - Huppertz - The Anatomy of The Normal Placentaиick LooяBelum ada peringkat
- Blois Et Al 2011 ProofsDokumen8 halamanBlois Et Al 2011 ProofsGabriela BarrientosBelum ada peringkat
- Mammary GlandDokumen7 halamanMammary Glanddaitya99Belum ada peringkat
- Vmi2011 757194Dokumen13 halamanVmi2011 757194Ahmad SolihinBelum ada peringkat
- Lancet FQ PDFDokumen14 halamanLancet FQ PDFYesenia HuertaBelum ada peringkat
- Placenta in PreeclampsiaDokumen20 halamanPlacenta in PreeclampsiaRania MousaBelum ada peringkat
- Immunology of EndometriosisDokumen19 halamanImmunology of EndometriosisMairunzi EziBelum ada peringkat
- Perspectives: Extracellular Vesicles: Biology and Emerging Therapeutic OpportunitiesDokumen11 halamanPerspectives: Extracellular Vesicles: Biology and Emerging Therapeutic OpportunitiesYanan ZhangBelum ada peringkat
- Post-Caesarean Rectus Sheath HaematomaDokumen4 halamanPost-Caesarean Rectus Sheath HaematomatapayanaBelum ada peringkat
- DIC in PregnancyDokumen41 halamanDIC in PregnancytapayanaBelum ada peringkat
- Jadwal BiccmDokumen4 halamanJadwal BiccmtapayanaBelum ada peringkat
- GTG 56 PDFDokumen24 halamanGTG 56 PDFKadelsy BristolBelum ada peringkat
- Appendicitis 130421042532 Phpapp02Dokumen32 halamanAppendicitis 130421042532 Phpapp02Rabie'ahBahananBelum ada peringkat
- Maternal Collapse During PregnancyDokumen57 halamanMaternal Collapse During PregnancytapayanaBelum ada peringkat
- Diagnosis and Management of Ectopic Pregnancy: Europe PMC Funders GroupDokumen20 halamanDiagnosis and Management of Ectopic Pregnancy: Europe PMC Funders GrouptapayanaBelum ada peringkat
- Prenatal Diagnosis Down SyndromDokumen36 halamanPrenatal Diagnosis Down SyndromtapayanaBelum ada peringkat
- Dengue Virus Infection Pathogenesis - UpToDateDokumen28 halamanDengue Virus Infection Pathogenesis - UpToDatetapayanaBelum ada peringkat
- Appendicitis 130421042532 Phpapp02Dokumen32 halamanAppendicitis 130421042532 Phpapp02Rabie'ahBahananBelum ada peringkat
- Hypoxia. 2. Hypoxia Regulates Cellular Metabolism: William W. Wheaton and Navdeep S. ChandelDokumen10 halamanHypoxia. 2. Hypoxia Regulates Cellular Metabolism: William W. Wheaton and Navdeep S. ChandeltapayanaBelum ada peringkat
- Maternal HipoksiaDokumen15 halamanMaternal HipoksiatapayanaBelum ada peringkat
- 3 SEPSIS MATERNAL - Yudianto B. SaroyoDokumen31 halaman3 SEPSIS MATERNAL - Yudianto B. SaroyotapayanaBelum ada peringkat
- SOP Green CodeDokumen2 halamanSOP Green CodetapayanaBelum ada peringkat
- Use of Chemotherapy During Human PregnancyDokumen9 halamanUse of Chemotherapy During Human PregnancytapayanaBelum ada peringkat
- Anemia During PregnancyDokumen8 halamanAnemia During Pregnancyekaseptiani312Belum ada peringkat
- Update of Fetal Growth Restriction: I Nyoman Suetri TapayanaDokumen44 halamanUpdate of Fetal Growth Restriction: I Nyoman Suetri TapayanatapayanaBelum ada peringkat
- ImplanonDokumen52 halamanImplanontapayanaBelum ada peringkat
- Coiling IndexDokumen3 halamanCoiling IndextapayanaBelum ada peringkat
- CTG HaDokumen15 halamanCTG HaNabila SaribanunBelum ada peringkat
- Amnioinfusion Guide: Functions, Indications, Procedures"TITLE"All about Amnioinfusion - What it is, When Used, Process" TITLE"Complete Amnioinfusion Overview - Definition, Benefits, RisksDokumen16 halamanAmnioinfusion Guide: Functions, Indications, Procedures"TITLE"All about Amnioinfusion - What it is, When Used, Process" TITLE"Complete Amnioinfusion Overview - Definition, Benefits, RiskstapayanaBelum ada peringkat
- Amenorrhea: An Approach To Diagnosis and ManagementDokumen8 halamanAmenorrhea: An Approach To Diagnosis and ManagementtapayanaBelum ada peringkat
- Placental Secretion of Interleukin-1 and Interleukin-1 Receptor Antagonist in Preeclampsia: Effect of Magnesium SulfateDokumen10 halamanPlacental Secretion of Interleukin-1 and Interleukin-1 Receptor Antagonist in Preeclampsia: Effect of Magnesium SulfatetapayanaBelum ada peringkat
- Breech DeliveryDokumen6 halamanBreech DeliveryNyoman TapayanaBelum ada peringkat
- Fitz Hugh Curtis SyndromeDokumen1 halamanFitz Hugh Curtis SyndrometapayanaBelum ada peringkat
- Afamin Serum Concentrations Are Associated With Insulin Resistance and Metabolic Syndrome in PCOSDokumen7 halamanAfamin Serum Concentrations Are Associated With Insulin Resistance and Metabolic Syndrome in PCOStapayanaBelum ada peringkat
- A Blinded Randomized Controlled Trial of High Dose Vit D Supplementation To Reduce Recurrence of BV PDFDokumen13 halamanA Blinded Randomized Controlled Trial of High Dose Vit D Supplementation To Reduce Recurrence of BV PDFtapayanaBelum ada peringkat
- Kegels Exercise Could Reduce The Incidence of Postpartum Urinary Stress IncontinenceDokumen3 halamanKegels Exercise Could Reduce The Incidence of Postpartum Urinary Stress IncontinencetapayanaBelum ada peringkat
- The Presence of Multipel Gestational Sacs Confers A Higher Live Birth Rate in Women With Infertility Who Achieve A Positive Pregnancy Test After Fresh and Frozen Embryo TransferDokumen6 halamanThe Presence of Multipel Gestational Sacs Confers A Higher Live Birth Rate in Women With Infertility Who Achieve A Positive Pregnancy Test After Fresh and Frozen Embryo TransfertapayanaBelum ada peringkat
- Immunosero Notes 2Dokumen20 halamanImmunosero Notes 2Rakim MikarBelum ada peringkat
- Corneal Graft Rejection Causes and Risk FactorsDokumen72 halamanCorneal Graft Rejection Causes and Risk FactorsGaurav shuklaBelum ada peringkat
- MHC Class I and II Antigens Present Foreign Antigens to T CellsDokumen16 halamanMHC Class I and II Antigens Present Foreign Antigens to T CellssharanBelum ada peringkat
- Specific Immunity. FINALDokumen29 halamanSpecific Immunity. FINALLUZVIMINDA GORDOBelum ada peringkat
- Q1. What Is Vaccine?: Vaccinology Lecture NotesDokumen31 halamanQ1. What Is Vaccine?: Vaccinology Lecture Notesحوراء موجد هادي غاويBelum ada peringkat
- Immunology MCQDokumen50 halamanImmunology MCQAbdallah Essam Al-Zireeni96% (131)
- NonClassical MHC Class I PDFDokumen12 halamanNonClassical MHC Class I PDFRobMarvinBelum ada peringkat
- 3353 FullDokumen11 halaman3353 Fullsekoslava85Belum ada peringkat
- The ORF8 Protein of SARS-CoV-2 Mediates Immune Evasion Through Potently Downregulating MHC-IDokumen41 halamanThe ORF8 Protein of SARS-CoV-2 Mediates Immune Evasion Through Potently Downregulating MHC-IZerohedge71% (7)
- CD Marker HandbookDokumen47 halamanCD Marker HandbookSteph Vee100% (1)
- Lec 9Dokumen16 halamanLec 9moh2002medicineBelum ada peringkat
- ImmunologyDokumen29 halamanImmunologySadia ShafiqueBelum ada peringkat
- HLA Typing: Understanding the Human Leukocyte Antigen SystemDokumen27 halamanHLA Typing: Understanding the Human Leukocyte Antigen SystemCsn VittalBelum ada peringkat
- Test 3 Study Guide INNATE DEFENSES A&P2Dokumen13 halamanTest 3 Study Guide INNATE DEFENSES A&P2Sarah C. SnooksBelum ada peringkat
- Immunology - Website QuestionsDokumen100 halamanImmunology - Website QuestionsMohammed AlMujaini75% (12)
- White Blood CellDokumen21 halamanWhite Blood CellAnonymous 0C4OZmRBelum ada peringkat
- IMMUNITY: A Concise Guide to Innate and Acquired ImmunityDokumen190 halamanIMMUNITY: A Concise Guide to Innate and Acquired ImmunityFathima100% (1)
- Chapter 2 - AntigenDokumen6 halamanChapter 2 - AntigenAngelica Joy GonzalesBelum ada peringkat
- Epitope Predictions: AbbreviationsDokumen19 halamanEpitope Predictions: AbbreviationsRasha Samir SryoBelum ada peringkat
- Immune Mechanisms in Type 1 Diabetes: Maja Wa Llberg and Anne CookeDokumen9 halamanImmune Mechanisms in Type 1 Diabetes: Maja Wa Llberg and Anne CookeJosé Fernández MejíaBelum ada peringkat
- Score Report - Immunology & Serology at Free Online Quiz SchoolDokumen29 halamanScore Report - Immunology & Serology at Free Online Quiz SchoolThomas GiangBelum ada peringkat
- Biochimica Et Biophysica Acta: Dilip Shrestha, Mark A. Exley, György Vereb, János Szöll Ősi, Attila JeneiDokumen14 halamanBiochimica Et Biophysica Acta: Dilip Shrestha, Mark A. Exley, György Vereb, János Szöll Ősi, Attila JeneiLeandro CarreñoBelum ada peringkat
- Janeways Immunobiology 9Th Edition Murphy Test Bank Full Chapter PDFDokumen44 halamanJaneways Immunobiology 9Th Edition Murphy Test Bank Full Chapter PDFJamesWellsoeic100% (9)
- MHC ModuleDokumen17 halamanMHC ModuleK-idol LiveBelum ada peringkat
- Immunological BioinformaticsDokumen332 halamanImmunological BioinformaticsDiana GabrielaBelum ada peringkat
- A Novel Multiplexed 11 Locus HLA Full Gene Amplification Assay Using Next Generation Sequencing-LijoDokumen13 halamanA Novel Multiplexed 11 Locus HLA Full Gene Amplification Assay Using Next Generation Sequencing-Lijorajasereddy1275Belum ada peringkat
- Immunology: Overview (Moses Franklyn Dumbuya)Dokumen69 halamanImmunology: Overview (Moses Franklyn Dumbuya)Moses DumbuyaBelum ada peringkat
- Report From The National Institute of Allergy and Infectious Diseases Workshop On Drug AllergyDokumen12 halamanReport From The National Institute of Allergy and Infectious Diseases Workshop On Drug AllergyHusni mubarakBelum ada peringkat
- Etiology and Pathogenesis of Preeclampsia: Current Concepts: Ajog ReviewsDokumen17 halamanEtiology and Pathogenesis of Preeclampsia: Current Concepts: Ajog ReviewstapayanaBelum ada peringkat
- T Cell Maturation, Activation and DifferentiationDokumen65 halamanT Cell Maturation, Activation and DifferentiationChanDan RjBelum ada peringkat