Am J Clin Nutr 2007 Georgieff 614S 20S
Diunggah oleh
Yusuf Almalik SaputraHak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Am J Clin Nutr 2007 Georgieff 614S 20S
Diunggah oleh
Yusuf Almalik SaputraHak Cipta:
Format Tersedia
Nutrition and the developing brain: nutrient priorities and
measurement13
Michael K Georgieff
KEY WORDS
onate, fetus
Nutrition, brain, development, assessment, ne-
GENERAL PRINCIPLES OF NUTRIENT EFFECTS ON
THE DEVELOPING BRAIN
Nutrients and growth factors regulate brain development during fetal and early postnatal life. The developing brain between
24 and 42 wk of gestation is particularly vulnerable to nutritional
insults because of the rapid trajectory of several neurologic processes, including synapse formation and myelination (for more
extensive reviews, see references 15). Conversely, the young
brain is remarkably plastic and therefore more amenable to repair
after nutrient repletion. On balance, the brains vulnerability to
nutritional insults likely outweighs its plasticity, which explains
why early nutritional insults result in brain dysfunction not only
while the nutrient is in deficit, but also after repletion.
614S
All nutrients are important for neuronal cell growth and
development, but some appear to have greater effects during
the late fetal and neonatal time periods. These include protein,
iron, zinc, selenium, iodine, folate, vitamin A, choline, and
long-chain polyunsaturated fatty acids (13). The effect of
nutrient deficiency or supplementation on the developing
brain is a function of the brains requirement for a nutrient in
specific metabolic pathways and structural components. The
effects are regionally distributed within the brain on the basis
of which areas are rapidly developing at any given time (4).
During late fetal and early neonatal life, regions such as the
hippocampus, the visual and auditory cortices, and the striatum are undergoing rapid development characterized by the
morphogenesis and synaptogenesis that make them functional
(5, 6). The hippocampus that subserves recognition memory
behavior is one of the earliest areas to show cortical-cortical
connectivity and functionality. Furthermore, brain-wide processes such as myelination accelerate during late fetal and
early neonatal life and are vulnerable to deficits of nutrients
that support them. A nutrient that promotes normal brain
development at one time may be toxic at another point in
development. Similarly, a nutrient that promotes normal brain
development at one concentration may be toxic at another.
Several nutrients, including iron, are regulated within a relatively narrow range, where either an excess or a deficiency
induces abnormal brain development. Others have wider
ranges of tolerance.
Nutrients are necessary not only for neurons but also for supporting glial cells. For any given region, early nutritional insults
have a greater effect on cell proliferation, thereby affecting cell
number (7, 8). Later nutritional insults affect differentiation,
including size, complexity, and in the case of neurons, synaptogenesis and dendritic arborization. Microarray analysis of
genomic transcripts from various brain regions in the developing
rat shows an important breakpoint at approximately postnatal
day 7, before which proliferation genes are predominantly expressed (8). After this time point, genes that control differentiation are preferentially expressed. Postnatal day 7 in the rat brain
is roughly equivalent to a late-gestation human fetal brain.
1
From the Department of Pediatrics and Child Development, University
of Minnesota School of Medicine, Minneapolis, MN.
2
Presented at the conference Maternal Nutrition and Optimal Infant
Feeding Practices, held in Houston, TX, February 2324, 2006.
3
Address reprint requests to MK Georgieff, MMC 39, D-136 Mayo Building, 420 Delaware Street SE, Minneapolis, MN 55455. E-mail:
georg001@umn.edu.
Am J Clin Nutr 2007;85(suppl):614S20S. Printed in USA. 2007 American Society for Nutrition
Downloaded from ajcn.nutrition.org by guest on May 4, 2015
ABSTRACT
Nutrients and growth factors regulate brain development during fetal
and early postnatal life. The rapidly developing brain is more vulnerable to nutrient insufficiency yet also demonstrates its greatest
degree of plasticity. Certain nutrients have greater effects on brain
development than do others. These include protein, energy, certain
fats, iron, zinc, copper, iodine, selenium, vitamin A, choline, and
folate. The effect of any nutrient deficiency or overabundance on
brain development will be governed by the principle of timing, dose,
and duration. The ability to detect the specific effects of nutrient
deficiencies is dependent on knowing which area of the brain is
preferentially affected and on having neurologic assessments that
tap into the functions of those specific areas. As examples, proteinenergy malnutrition causes both global deficits, which are testable
by general developmental testing, and area-specific effects on the
hippocampus and the cortex. Iron deficiency alters myelination,
monoamine neurotransmitter synthesis, and hippocampal energy
metabolism in the neonatal period. Assessments of these effects
could include tests for speed of processing (myelination), changes in
motor and affect (monoamines), and recognition memory (hippocampus). Zinc deficiency alters autonomic nervous system regulation and hippocampal and cerebellar development. Long-chain
polyunsaturated fatty acids are important for synaptogenesis, membrane function, and, potentially, myelination. Overall, circuitspecific behavioral and neuroimaging tests are being developed for
use in progressively younger infants to more accurately assess the
effect of nutrient deficits both while the subject is deficient and after
recovery from the deficiency.
Am J Clin Nutr 2007;85(suppl):
614S20S.
615S
NUTRITION AND THE DEVELOPING BRAIN
Nutrients can affect not only neuroanatomy, but also neurochemistry and neurophysiology. Neurochemical alterations include changes in neurotransmitter synthesis, receptor synthesis,
and neurotransmitter reuptake mechanisms (9, 10). Neurophysiologic changes reflect changes in metabolism and signal propagation. The changes across all 3 venues ultimately result in
altered neuronal performance at the time that the nutrient status
is altered. Long-term changes in form and function can occur if
the altered nutrient state changes the trajectory of brain development in a substantive anatomical or neurochemical way, beyond the period where repair can occur.
BRAIN DEVELOPMENT BETWEEN 24 AND 44 WK
AFTER CONCEPTION
NUTRIENTS AND PERINATAL BRAIN CIRCUITRY
As mentioned above, all nutrients are important for brain development, but some appear to have a particularly large effect on
developing brain circuits during the last trimester and early neonatal period (Table 1). The importance of these nutrients has
been established primarily through nutrient deficit studies and
through knowledge of their role in the specific biochemical pathways that underlie neuronal and glial growth and function. A
complete consideration of all nutrient effects on brain development is beyond the scope of this article, but the subject has been
reviewed elsewhere (1 4). Nevertheless, certain nutrients are
commonly deficient in preterm and growth-retarded infants, and
their effects on the developing brain in animals and humans are
presented below.
Protein-energy malnutrition
Protein-energy malnutrition in fetal and early neonatal animal
models reduces neuronal DNA and RNA content and alters the
fatty acid profile (7, 13). Neuropathologically, this results in
lower neuronal number, reduced protein synthesis, and hypomyelination. Brain size is reduced through all of these mechanisms
as the result of changes in structural proteins, growth factor
concentrations, and neurotransmitter production. Ultrastructural
changes include reductions in synapse number and dendritic
Nutrient
Brain requirement for the
nutrient
Protein-energy Cell proliferation, cell
differentiation
Synaptogenesis
Growth factor synthesis
Iron
Myelin
Monoamine synthesis
Neuronal and glial energy
metabolism
Zinc
DNA synthesis
Neurotransmitter release
Copper
Neurotransmitter synthesis,
neuronal and glial energy
metabolism, antioxidant
activity
LC-PUFAs
Synaptogenesis
Myelin
Choline
Neurotransmitter synthesis
DNA methylation
Myelin synthesis
1
Predominant brain circuitry
or process affected by
deficiency
Global
Cortex
Hippocampus
White matter
Striatal-frontal
Hippocampal-frontal
Autonomic nervous system
Hippocampus, cerebellum
Cerebellum
Eye
Cortex
Global
Hippocampus
White matter
LC-PUFAs, long-chain polyunsaturated fatty acids.
arbor complexity (14 19). The cortex and hippocampus appear
to be particularly vulnerable to protein-energy malnutrition (20).
Protein-energy malnutrition in humans between 24 and 44 wk
postconception can occur either in utero or ex utero. Fetal
protein-energy malnutrition results in intrauterine growth retardation and is usually due to maternal hypertension or severe
malnutrition during pregnancy (21). Postnatal malnutrition is
common in sick preterm infants who are fluid restricted or who
do not tolerate high rates of nutrient delivery. Severe or prolonged intrauterine growth retardation results in poor prenatal
head growth associated with poorer developmental outcome (22,
23). In the absence of overt microcephaly, infants with intrauterine growth retardation nevertheless have a 15% rate of mild
neurodevelopmental abnormalities characterized by cognitive
(rather than motor) disabilities (24). Verbal and visual recognition memory systems appear particularly to be vulnerable, which
is consistent with structures that are rapidly developing in this
time period (25, 26).
Iron
Iron is accreted rapidly by the fetus during the last trimester
and is necessary for basic neuronal processes such as myelination, neurotransmitter production, and energy metabolism (9).
The effect of iron deficiency on the developing brain has been
assessed largely in the rat model, where variations in the timing
and severity of the deficiency have helped to elucidate the biochemical, structural, and behavioral effects. Biochemically, fetal
and neonatal iron deficiency results in reduced oxidative metabolism in the hippocampus and frontal cortex (27), elevated intracellular neuronal glutamate concentrations (10), reduced striatal dopamine concentrations (9), and altered fatty acid and
myelin profiles throughout the brain (28). Structurally, dendritic
arbors are truncated in the hippocampus (29), and global and
regional brain masses are reduced while the animals are iron
deficient and after iron repletion (30). Behaviorally, rodents have
Downloaded from ajcn.nutrition.org by guest on May 4, 2015
The human brain undergoes remarkable structural and functional changes between 24 and 44 wk after conception, progressing at the beginning of the third trimester from a smooth bilobed
structure with few gyrations or sulcations to a complex one at
term that morphologically resembles the adult brain (11). The
increase in complexity largely reflects cortical neuronal growth,
differentiation, and synaptic connections. In particular, the
auditory and visual cortices begin to develop rapidly, as do
areas underlying receptive language and higher cognitive
function (5). Myelination begins before term birth as well. Most
importantly, experience-dependent synapse formation occurs before birth and provides a neuronal basis for the fetus to learn. The
hippocampus, which is central to recognition memory processing,
has established most of its connections from the entorhinal cortex
and has begun to send projections through thalamic nuclear structures to the developing frontal cortex (12). These structures and
processes are worth considering because they (and the functions
they serve) are the ones that will be vulnerable to nutritional insults
in this time period.
TABLE 1
Important nutrients during late fetal and neonatal brain development1
616S
GEORGIEFF
long-term deficits in trace recognition memory (31), procedural memory (32), and spatial navigation (33) that indicate
structural and functional abnormalities in the hippocampus
and striatum.
Newborn human infants can have altered iron status as the
result of severe maternal iron deficiency anemia, intrauterine
growth retardation due to maternal hypertension, increased fetal
iron demand for erythropoiesis due to maternal diabetes mellitus,
or lack of fetal iron accretion due to premature birth (34 38). Far
fewer studies have been conducted on the neurologic consequences of perinatal iron deficiency than on classic postnatal
dietary iron deficiency. Infants with cord ferritin concentrations
in the lowest quartile have poorer neurodevelopment at school
age (39). Iron-deficient infants of diabetic mothers have impaired auditory recognition memory processing at birth (40),
whereas iron-deficient premature infants have a higher rate of
abnormal neurologic reflexes at 36 wk postconception (41).
Zinc
Copper
Copper is an essential divalent cation for proteins involved in
brain-energy metabolism, dopamine metabolism, antioxidant
activity, and iron accretion in the fetal and neonatal brain (49
52). Although nutritional copper deficiency does not appear to be
a common clinical problem in the human fetus and neonate, the
neurodevelopmental effects in the developing rodent are striking, both while the animals are copper deficient as pups and after
copper repletion. In particular, the developing cerebellum appears to be particularly at risk in models of gestational copper
deficiency with long-term effects on motor function, balance,
and coordination (53).
Long-chain polyunsaturated fatty acids
Extensive reviews of the effects of long-chain polyunsaturated
fatty acids on the developing brain have been published and will
Other nutrients
Additional nutrients that affect brain and behavior development include iodine and selenium, which mediate their effects
through thyroid hormone metabolism (59, 60); folate and choline, which mediate their effects through one-carbon metabolism, DNA methylation, and neurotransmitter synthesis (61 63);
and vitamins A and B-6. A review of their effects can be found in
reference 1.
CIRCUIT-SPECIFIC ASSESSMENT OF NUTRIENT
EFFECTS ON THE DEVELOPING BRAIN
Ideally, specific nutrient deficiencies would result in a recognizable, characteristic spectrum of neuroanatomical, neurochemical,
and neurophysiologic dysfunction in perinatal humans. Each nutrient would thus have a signature neurodevelopmental effect. Unfortunately, limitations exist that preclude the use of this concept to
generate accurate developmental outcome predictions for preterm
infants, based on neurologic assessment in the newborn period.
Preterm and term infants have limited behavioral expression of the
higher-function cortical activities that are the basis for behaviors
later assessed as intelligence. For example, they are preverbal,
which distinctly limits intellectual reasoning. Furthermore, ongoing
illness can depress brain activity and behavior. Finally, later
catch-up brain growth and the capacity for repair make predictive
assessments difficult.
Nevertheless, neurobehavioral assessments can be performed in infants at or near term that can give insight into
structure and function. Brain size can be estimated either by
occipitofrontal head circumference (assuming no hydrocephalus), computerized axial tomography (CAT), or magnetic
resonance imaging (MRI) scans. Moreover, regional brain
volumes or track size can be measured by structural MRI and
diffusion tensor imaging (DTI) (64, 65). Objective metrics of
brain electrical function can be obtained by electroencephalogram (EEG), auditory brainstem evoked response (ABR), or
event-related potentials (ERPs) (66). The advantage of ERPs
is that activity in response to cognitive stimuli and events,
such as auditory recognition memory, can be assessed (66,
67). Functioning of the hypothalamic-pituitary-adrenal axis
and the autonomic nervous system in response to stressors can
also be measured at this age (68). Finally, limited information
can be obtained from neurologic examination of the infant,
including assessment of neurologic reflexes (41).
Although these measurements are not specifically designed to
assess nutritional effects in the perinatal period, they can be used
Downloaded from ajcn.nutrition.org by guest on May 4, 2015
Fetal and neonatal zinc biology has been assessed in rodent
and primate models. Zinc is a cofactor in enzymes that mediate
protein and nucleic acid biochemistry (42). Fetal zinc deficiency
results in decreased brain DNA, RNA, and protein content (43).
Importantly, insulin-like growth factor I and growth hormone
receptor gene expression are regulated by zinc (44). Neuronally,
presynaptic boutons are dependent on adequate zinc for delivery
of neurotransmitters to the synaptic cleft (45). Structural studies
have shown truncated dendritic arbors and reduced regional
brain mass in the cerebellum, limbic system, and cerebral cortex
(45). Zinc-deficient rats have abnormal cortical electrophysiology (46). The orbitofrontal cortex appears to be particularly
vulnerable. Behaviorally, zinc-deficient rhesus monkeys have
poor short-term memory (47). These effects suggest that zinc is
particularly important for the medial temporal lobe, frontal lobe,
and cerebellar development.
Fetuses of zinc-deficient mothers show decreased fetal movement and heart rate variability, which is suggestive of altered
autonomic nervous system stability (48). Although intelligence
quotient does not seem to be affected, infants born to zincdeficient mothers have decreased preferential looking behavior,
which is indicative of altered hippocampal function.
not be reviewed here (3, 54, 55). Nevertheless, it is important to
note that these fats, particularly docosahexaenoic acid (DHA),
are potent neurobiological agents that affect neuronal membrane
structure, synaptogenesis, and myelination. Studies in preterm humans indicate important benefits for retinal and cognitive development, as indexed by improved electroretinogram activity, visual
acuity, and short-term global developmental outcome after DHA
supplementation of preterm infant formula (56, 57). The effects in
term infants are far less convincing and are substantially underpowered to draw any conclusions (58). DHA supplementation trials
should be considered formula repletion of deficit state studies,
because the fetus normally receives adequate DHA transplacentally,
and breastfed neonates receive DHA in human milk.
617S
NUTRITION AND THE DEVELOPING BRAIN
TABLE 2
The repertoire of neurodevelopmental assessments that can be used in
infants between 36 and 44 wk after conception and the relation to specific
nutritional deficits1
Assessment
Brain region or process
Risk nutrients
Neurologic examination
Whole brain
Whole brain, nervous system
Myelination
Whole brain, nervous system
EEG maturity
Cortex
Stimulated heart rate,
blood pressure,
salivary cortisol
responses
Autonomic nervous system
Protein-energy
Protein-energy
Iron
Protein-energy
Copper
Protein-energy
(LC-PUFAs)
Zinc (Proteinenergy)
OFC
Neurologic reflexes
ABR, ERG
Auditory ERP
HPA axis
Myelination
Synaptic efficacy
Hippocampal function
Global and regional volume
and structure
MR-DTI
Myelin and tract integrity
MR-proton
spectroscopy
Neurochemistry
1
Nutrients with unproven but likely effects based on animal models are
marked in parentheses. EEG; electroencephalogram; LC-PUFAs, long-chain
polyunsaturated fatty acids; HPA, hypothalamic-pituitary-adrenal; ABR, auditory brainstem evoked response; ERG, electroretinogram; ERP, event-related
potential; MRI, magnetic resonance imaging; DTI, diffusion tensor imaging;
OFC, occipitofrontal head circumference.
in such a manner (Table 2). It is important to note that many of
the nutrient deficits will affect similar regions and processes,
making it difficult to obtain a signature effect of any single
TABLE 3
Neurobehavioral and neuroimaging assessments that can be performed to evaluate the effects of neonatal nutrients on general brain development during
the first 6 y of postnatal life1
Neurologic domain
Risk nutrients for
domain
Global function
Protein-energy, iron,
zinc, LC-PUFAs
Myelination
Iron
Behavioral
Age of
reliability
Neuroimaging technique
Bayley Scales
1236 mo
OFC
Any age
WPPSI
Speed of
processing
4 y
4 mo
MR regional volumetrics
ABR, VEP
Newborn and 6 y
Any age
1236 mo
ERP
DTI
Regional MR
After term
Newborn and 6 y
Newborn and 6 y
Actigraph
Any age
LC-PUFAs
Motor function
Protein-energy
Iron
Copper
Bayley Scales
(PDI)
Activity
Coordination
Any age
Any age
Age of reliability
LC-PUFAs, long-chain polyunsaturated fatty acids; WPPSI, Wechsler Preschool and Primary Scale of Intelligence; MR, magnetic resonance; ABR,
auditory brainstem evoked response; VEP, visual evoked potential; ERP, event-related potential; DTI, diffusion tensor imaging; OFC, occipitofrontal head
circumference.
Downloaded from ajcn.nutrition.org by guest on May 4, 2015
MRI (structural)
Iron
LC-PUFAs
Iron (Zinc)
(Choline)
(Proteinenergy)
Protein-energy
(Iron) (Zinc)
(Copper)
Protein-energy
(Iron)
(Copper)
(Iron)
nutrient. The repertoire of assessments expands rapidly after the
neonatal period, particularly at 4 mo of age, when infant behavior
becomes more cortically dominant. By 4 6 mo of age adjusted
for prematurity, the recognition memory system can be assessed
behaviorally by the preferential looking task (69), and both the
explicit and implicit memory systems can be assessed electrophysiologically by using ERPs (70). Speed of processing,
which indexes myelination and synaptic efficacy, can be estimated from ABR and ERPs. Affect and distractiblility,
which at this age index striatal integrity and monoamine neurotransmitter function, can be assessed through direct observation and scoring (71). By the end of the first postnatal year,
more complex reasoning skills can be inferred from the subscales of the Bayley Scales of Infant Development (BSID) and
from specific testing of memory encoding, storage, and retrieval using elicited imitation (72, 73). The recent development of these region- and process-specific assessments for
at-risk newborns and young infants are welcome additions to
the repertoire that has depended on global assessments in the
past. The BSID administered at 12 mo corrected age remains
the most commonly used general assessment in many nutrient
outcome studies because it is widely available, requires little
special equipment, and is easily performed in multicenter
trials. Nevertheless, significant specific neurobehavioral
morbidities can be embedded with a normal Bayley-derived
Developmental Quotient, which can mask potentially important neurologic processing deficits.
More detailed and region-specific interrogation of the infants neurobehavioral repertoire can be conducted as postnatal age increases. The frontal lobes become more testable
by 5 y of age with use of the Cambridge Neuropsychological
Test automated battery (CANTAB), which assesses behaviors
such as strategy switching, executive function, planning,
and working memory (74). The integrity of these behaviors
may ultimately determine success in school performance (75).
By 6 y of age, children can be imaged by MRI scanning
without sedation. Functional MRI becomes a useful tool
for assessing attention, structure-function relations on
618S
GEORGIEFF
TABLE 4
Neurobehavioral and neuroimaging assessments that can be performed to evaluate the effects of neonatal nutrients on cognitive development during the
first 6 y of postnatal life1
Cognitive domain
Explicit-recognition
memory
Working memory
Implicit-procedural
memory
Risk nutrients
for domain
Age of
reliability
Neuroimaging technique
VPC
4 mo
ERP (auditory)
Newborn
DNMS
Elicited imitation
6 mo
12 mo
4 mo
Newborn and 6 y
Protein-energy
Elicited imitation
12 mo
ERP (visual)
MR volume
(hippocampus)
MR volume (prefrontal
cortex)
Iron
CANTAB
4 y
Iron
Priming
4 mo
fMRI
MR volume (striatum)
6 y
Newborn and 6 y
fMRI
Newborn and 6 y
Protein-energy,
iron, zinc
Behavioral
assessment
Age of reliability
Newborn and 6 y
VPC, Visual Paired Comparison (test); ERP, event-related potential; DNMS, Delay Non-Match to Sample (test); MR, magnetic resonance; CANTAB,
Cambridge Neuropsychological Test Automated Battery; fMRI, functional magnetic resonance imaging.
SUMMARY
Fetal and neonatal malnutrition can have global or circuitspecific effects on the developing brain. These effects are based
on the timing and magnitude of the nutrient deficit and on the
brains need for the particular nutrient at the time of the deficit.
It is important to recognize that nutritional effects on the developing brain include not only the provision of specific substrates,
but also the synthesis and activation of growth factors.
Although it would be attractive for each nutrient deficit to have
a signature effect on the brain that could be assessed behaviorally
or through neuroimaging, this is unlikely to occur with the currently available neuroimaging and behavioral techniques, in part
because common nutrient deficiencies in the neonate occur together and affect the same developing brain region. For example,
protein-energy, iron, and zinc malnutrition all affect the developing hippocampus. Ultimately, the attribution of short- and
long-term neurodevelopmental dysfunction to perinatal nutritional status will need to follow specific rules of developmental
neuroscience. The nutrient deficit must be present during the
developmental window when the brain requires that nutrient for
growth and function. Furthermore, the abnormal behavioral
function should be subserved by a brain region or process that is
affected by the nutrient. Usually, a multitier approach from human epidemiology to animal and cellular models will be necessary to provide reasonable scientific evidence of a cause-andeffect association.
TABLE 5
Neurobehavioral and neuroimaging assessments that can be performed to evaluate the effects of neonatal nutrients on affective development during the
first 6 y of postnatal life1
Affective domain
Risk nutrients
for domain
Attention
Iron, zinc
Reactivity (HPA/
ANS)
Iron, zinc
Social interaction
Iron, zinc
Behavioral assessment
Bayley Scales rating
CANTAB
Flanker task
Response to:
Restraint
Separation
Immunization
Spontaneous movement
Bayley Scales rating
Age of
reliability
12 mo
4 y
5 y
Newborn
Any age
12 mo
Neuroimaging technique
Age of reliability
MR volume (prefrontal cortex)
Newborn and 6 y
fMRI
6 y
Salivary cortisol
HR response
Vagal tone
fMRI
Any age
Any age
Any age
6 y
1
MR, magnetic resonance; CANTAB, Cambridge Neuropsychological Test Automated Battery; fMRI, functional magnetic resonance imaging; HPA/
ANS, hypothalamic pituitary adrenal/autonomic nervous system; HR, heart rate.
Downloaded from ajcn.nutrition.org by guest on May 4, 2015
working memory, and implicit memory tasks (76). The behavioral and neuroimaging assessments for general, cognitive, and affective neurobehavioral domains and the corresponding ages of utilization in this population between the
neonatal period and 6 y of age are summarized in Tables 3, 4
and 5.
Unfortunately, the longer the time period between the nutritional deficiency and the subsequent neurobehavioral assessment, the greater the risk that intervening confounding variables
such as postdischarge nutrition, illness, and home environment
will influence the outcome measure (77). Thus, there is a high
premium on further development of neurobehavioral assessments in close temporal proximity to the time of nutritional insult
in the neonatal period. Potential new methods that may be useful
include near infrared spectroscopy (NIRS) and magnetoencephalography (MEG) (78, 79).
NUTRITION AND THE DEVELOPING BRAIN
REFERENCES
25. Gottleib SJ, Biasini FJ, Bray NW. Visual recognition memory in IUGR
and normal birthweight infants. Infant Behav Dev 1998;11:223 8.
26. Pollitt E, Gorman KS. Nutritional deficiencies as developmental risk
factors. In: Nelson CA, ed. Threats to optimal development. The Minnesota Symposia On Child Psychology. Vol 27. Hillsdale, NJ: Erlbaum
Associates, 1994:121 44.
27. deUngria M, Rao R, Wobken JD, Luciana M, Nelson CA, Georgieff MK.
Perinatal iron deficiency decreases cytochrome c oxidase (CytOx) activity in selected regions of neonatal rat brain. Pediatr Res 2000;48:169
76.
28. Beard JL, Wiesinger JA, Connor JR. Pre and postweaning iron deficiency alters myelination in Sptrague-Dawley rats. Dev Neurosci 2003;
5:308 15.
29. Jorgenson LA, Wobken JD, Georgieff MK. Perinatal iron deficiency
alters apical dendritic growth in hippocampal CA-1 pyramidal neurons.
Dev Neurosci 2003;25:41220.
30. Jorgenson LA, Sun M, OConnor M, Georgieff MK. Fetal iron deficiency disrupts the maturation of synaptic function and efficacy in area
CA1 of the developing rat hippocampus. Hippocampus 2005;15:1094
102.
31. McEcheron MD, Cheng AY, Liu H, Connor JR, Gilmartin MR. Perinatal
nutritional iron deficiency permanently impairs hippocampusdependent trace fear conditioning in rats. Nutr Neurosci 2005;8:195
206.
32. Beard JL, Felt BT, Schallert T, Connor JR, Georgieff MK. Moderate iron
deficiency in infancy: biology and behavior in young rats. Behav Brain
Res 2006;171:26170.
33. Felt BT, Lozoff B. Brain iron and behavior of rats are not normalized by
treatment of iron deficiency anemia during early development. J Nutr
1996;126:693701.
34. Chockalingam UM, Murphy E, Ophoven JC, Weisdorf SA, Georgieff
MK. Cord transferrin and ferritin levels in newborn infants at risk for
prenatal uteroplacental insufficiency and chronic hypoxia. J Pediatr
1987;111:283 6.
35. Georgieff MK, Landon MB, Mills MM, et al. Abnormal iron distribution
in infants of diabetic mothers: spectrum and maternal antecedents. J Pediatr 1990;117:455 61.
36. Georgieff MK, Petry CE, Wobken JD, Oyer CE. Liver and brain iron
deficiency in newborn infants with bilateral renal agenesis (Potters
syndrome). Pediatr Pathol 1996;16:509 19.
37. Petry CD, Eaton MA, Wobken JD, Mills MM, Johnson DE, Georgieff
MK. Iron deficiency of liver, heart, and brain in newborn infants of
diabetic mothers. J Pediatr 1992;121:109 14.
38. Rao R, Georgieff MK. Perinatal aspects of iron metabolism. Acta Pediatr
Suppl 2002;91:124 9.
39. Tamura T, Goldenberg RL, Hou J, et al. Cord serum ferritin concentrations and mental and psychomotor development of children at five years
of age. J Pediatr 2002;186:458 63.
40. Siddappa AM, Georgieff MK, Wewerka S, Worwa C, Nelson CA, deRegnier RA. Iron deficiency alters auditory recognition memory in newborn infants of diabetic mothers. Pediatr Res 2004;55:1034 41.
41. Armony-Sivan R, Eidelman A, Lanir A, Sredni D, Yehuda S. Iron status
and neurobehavioral development of premature infants. J Perinatol
2004;24:757 62.
42. Sandstead HH. Zinc: essentiality for brain development and function.
Nutr Rev 1985;43:129 37.
43. Duncan J, Hurley L. Thymidine kinase and DNA polymerase activity in
normal and zinc deficient developing rat embryos. Proc Soc Exp Biol
Med 1978;159:39 43.
44. McNall A, Etherton T, Fosmire G. The impaired growth induced by zinc
deficiency in rats is associated with decreased expression of hepatic
insulin-like growth factor I and growth hormone receptor genes. J Nutr
1995;125:874 9.
45. Frederickson C, Danscher G. Zinc-containing neurons in hippocampus
and related CNS structures. Prog Brain Res 1990;83:71 84.
46. Hesse G. Chronic zinc deficiency alters neuronal function of hippocampal mossy fibers. Science 1979;205:10057.
47. Golub MS, Takeuchi PT, Keen CL, Gershwin E, Hendricks AG, Lonnerdal B. Modulation of behavioral performance of prepubertal monkeys by moderate dietary zinc deprivation. Am J Clin Nutr 1994;60:
238 43.
48. Merialdi M, Caulfield LE, Zavaleta N, Figueroa A, Dominici F, Dipietro
JA. Randomized controlled trial of prenatal zinc supplementation and
Downloaded from ajcn.nutrition.org by guest on May 4, 2015
1. Georgieff MK, Rao R. The role of nutrition in cognitive development. In:
Nelson CA, Luciana M, eds. Handbook in developmental cognitive
neuroscience. Cambridge, MA: MIT Press, 2001:491504.
2. Dobbing J. Vulnerable periods in the developing brain. In: Dobbing J, ed.
Brain, behavior and iron in the infant diet. London, United Kingdom:
Springer, 1990:125.
3. Rao R, Georgieff MK. Early nutrition and brain development. In: Nelson
CA, ed. The effects of early adversity on neurobehavioral development.
Minnesota Symposium on Child Psychology. Vol 31. Hillsdale, NJ:
Erlbaum Associates, 2000:130.
4. Kretchmer N, Beard JL, Carlson S. The role of nutrition in the development of normal cognition. Am J Clin Nutr 1996;63(suppl):997S1001S.
5. Thompson RA, Nelson CA. Developmental science and the media: early
brain development. Am Psychol 2001;56:515.
6. Nelson CA, Bloom FE, Cameron JL, Amaral D, Dahl RE, Pine D. An
integrative, multidisciplinary approach to the study of brain-behavior
relations in the context of typical and atypical development. Dev Psychopathol 2002;14:499 520.
7. Winick M, Rosso P. The effect of severe early malnutrition on cellular
growth of the human brain. Pediatr Res 1969;3:181 4.
8. Stead JD, Neal C, Meng F, et al. Transcriptional profiling of the developing rat brain reveals that the most dramatic regional differentiation in
gene expression occurs postpartum. J Neurosci 2006;26:34553.
9. Beard JL, Connor JR. Iron status and neural functioning. Annu Rev Nutr
2003;23:3158.
10. Rao R, Tkac I, Townsend EL, Gruetter R, Georgieff MK. Perinatal iron
deficiency alters the neurochemical profile of the developing rat hippocampus. J Nutr 2003;133:321521.
11. Pomeroy SL, Ullrich NJ. Development of the nervous system. In: Polin
R, Fox W, Abman S, eds. 3rd ed. Fetal and neonatal physiology. Philadelphia, PA: Saunders, 2004:167598.
12. Seress L. Morphological changes of the human hippocampal formation
from midgestation to early childhood. In: Nelson CA, Luciana M, eds.
Handbook of developmental cognitive neuroscience. Cambridge, MA:
MIT Press, 2001:4558.
13. Winick M, Nobel A. Cellular responses in rats during malnutrition at
various ages. J Nutr 1966;89:300 6.
14. Bass NH, Netsky MG, Young E. Effects of neonatal malnutrition on
developing cerebellum. I. Microchemical and histologic study of cellular
differentiation in the rat. Arch Neurol 1970;23:289 302.
15. Benitez-Bribiesca L, De la Rosa-Alvarez I, Mansilla-Oivares A. Dendritic spine pathology in infants with severe protein-calorie malnutrition.
Pediatrics [serial online] 1999;104:e21. Internet: http://pediatrics.aappublications.org/cgi/content/full/104/2/e21 (accessed 12 December
2006).
16. Jones DG, Dyson SE. The influence of protein restriction, rehabilitation
and changing nutritional status on synaptic development: a quantitative
study in rat brain. Brain Res 1981;208:97111.
17. Wiggens RC, Fuller G, Enna SJ. Undernutrition and the development of
brain neurotransmitter systems. Life Sci 1984;35:208594.
18. Yamamoto N, Saitoh M, Moriuchi A, Nomura M, Okuyama H. Effect of
dietary alpha-linoleate/linoleate balance on brain lipid compositions and
learning ability of rats. J Lipid Res 1987;28:144 51.
19. Nishijima M. Somatomedin-C as a fetal growth promoting factor and
amino acid composition of cord blood in Japanese neonates. J Perinatol
Med 1986;14:163 6.
20. Lee K-H, Kalikoglu A, Ye P, DErcole AJ. Insulin-like growth factor-I
(IGF-I) ameliorates and IGF binding protein-1 (IGFBP-1) exacerbates
the effects of undernutrition on brain growth during early postnatal life:
studies of IGF-I and IGFBP-1 transgenic mice. Pediatr Res 1997;45:
331 6.
21. Low JA, Galbraith RS. Pregnancy characteristics of intrauterine growth
retardation. Obstet Gynecol 1974;44:122 6.
22. Winer EK, Tejani N. Four to seven year evaluation in two groups of small
for gestational age infants. 2nd ed. In: Tejani N, ed. Obstetric events and
developmental sequelae. Boca Raton, FL: CRC Press, 1994:7794.
23. Strauss RS, Dietz WH. Growth and development of term children born
with low birth weight: effects of genetic and environmental factors.
J Pediatr 1998;133:6772.
24. Spinello A, Stronati M, Ometto A, Fazzi E, Lanzi G, Guaschino S. Infant
neurodevelopmental outcome in pregnancies complicated by gestational
hypertension and intrauterine growth retardation. J Perinatol Med 1993;
21:195203.
619S
620S
49.
50.
51.
52.
53.
54.
55.
56.
58.
59.
60.
61.
62.
63.
64.
the development of fetal heart rate. Am J Obstet Gynecol 2004;190:
1106 12.
Prohaska JR, Gybina AA. Rat brain iron concentration is lower following perinatal copper deficiency. J Neurochem 2005;93:698 705.
West EC, Prohaska JR. Cu, Zn-superoxide dismutase is lower and copper chaperone CCS is higher in erythrocytes of copper-deficient rats and
mice. Exp Biol Med (Maywood) 2004;229:756 64.
Gybina AA, Prohaska JR. Increased rat brain cytochrome c correlates
with degree of perinatal copper deficiency rather than apoptosis. J Nutr
2003;133:3361 8.
Prohaska JR, Brokate B. Dietary copper deficiency alters protein levels
of rat dopamine beta-monooxygenase and tyrosine monooxygenase.
Exp Biol Med (Maywood) 2001;226:199 207.
Penland JG, Prohaska JR. Abnormal motor function persists following
recovery from perinatal copper deficiency in rats. J Nutr 2004;134:
1984 8.
Georgieff MK, Innis S. Controversial nutrients in the perinatal period
that potentially affect neurodevelopment: essential fatty acids and iron.
Pediatr Res 2005;57:99R103R.
Simmer K. Long-chain polyunsaturated fatty acid supplementation in
preterm infants (Cochrane Review). Cochrane Data Base Syst Rev 3
2000:CD000376.
San Giovanni JP, Parra-Cabrera S, Colditz GA, Berkey CS, Dwyer JT.
Meta-analysis of dietary essential fatty acids and long-chain polyunsaturated fatty acids as they relate to visual resolution acuity in healthy
preterm infants. Pediatrics 2000;105:1292 8.
OConnor DL, Hall R, Adamkin D, et al. Growth and development in
preterm infants fed long-chain polyunsaturated fatty acids: a prospective, randomized controlled trial. Pediatrics 2001;108:359 71.
Auestad N, Halter R, Hall RT, et al. Growth and development in term
infants fed long-chain polyunsaturated fatty acids: a double-masked,
randomized parallel, prospective, multivariate study. Pediatrics 2001;
108:372 81.
Aghini-Lombardi FA, Pinchera A, Antonangeli T, et al. Mild iodine
deficiency during fetal/neonatal life and neuropsychological impairment
in Tuscany. J Endocrinol Invest 1995;18:5772.
Mitchell JH, Nicol F, Beckett GJ, Arthur JR. Selenoprotein expression
and brain development in preweanling selenium and iodine deficient
rats. J Mol Endocrinol 1998;20:20310.
Ferguson SA, Berry KJ, Hansen DK, Wall KS, White G, Antony AC.
Behavioral effects of prenatal folate deficiency in mice. Birth Defects
Res A Clin Mol Teratol 2005;4:249 52.
Zeisel SH, Niculescu MD. Perinatal choline influences brain structure
and function. Nutr Rev 2006;64:197203.
Chen Z, Schwahn BC, Wu Q, He X, Rozen R. Postnatal cerebellar
defects in mice deficient in methylenetetrahydrofolate reductase. Int J
Dev Neurosci 2005;23:46574.
Peterson BS, Anderson AW, Ehrenkranz R, et al. Regional brain volumes and their later neurodevelopmental correlates in term and preterm
infants. Pediatrics 2003;111:939 48.
65. Seghier ML, Lazeyras F, Zimine S, et al. Combination of event related
fMRI and diffusion tensor imaging in an infant with perinatal stroke.
Neuroimage 2004;21:46372.
66. Nelson CA, Monk CS. The use of event-related potentials in the study of
cognitive development. In: Nelson CA, Luciana M, eds. Handbook in
developmental cognitive neuroscience. Cambridge, MA: MIT Press,
2001:12536.
67. deRegnier RA, Nelson CA, Thomas K, Wewerka S, Georgieff MK.
Neurophysiologic evaluation of auditory recognition memory in healthy
newborn infants and infants of diabetic mothers. J Pediatr 2000;137:
777 84.
68. Davis EP, Townsend E, Gunnar M, et al. Effects of prenatal betamethasone exposure on regulation of stress physiology in healthy premature
infants. Psychoneuroendocrinology 2004;29:1028 36.
69. Fagan JF 3rd, Singer LT, Montie JE, Shepherd PA. Selective screening
device for the early detection of normal or delayed cognitive development in infants at risk for later mental retardation. Pediatrics 1986;78:
1021 6.
70. Stolarova M, Whitney H, Webb S, deRegneir RA, Georgieff MK, Nelson CA. Electrophysiologic brain responses of six-month-old low risk
premature infants. Infancy 2003;4:43750.
71. Angulo-Kinzler RM, Peirano P, Lin E, Garrido M, Lozoff B. Spontaneous motor activity in human infants with iron-deficiency anemia. Early
Hum Dev 2002;66:6779.
72. Bauer PJ. Recalling past events: from infancy to early childhood. Ann
Child Dev 1995;11:2571.
73. Cheatham CL, Bauer PJ, Georgieff MK. Predicting individual differences in recall by infants born preterm and fullterm. Infancy (in press).
74. Luciana M, Nelson CA. Assessment of neuropsychological function
through use of the Cambridge Neuropscyhological Testing Automated
Battery: performance in 4- to 12-year-old children. Dev Neuropsychol
2002;22:595 624.
75. Luciana M, Lindeke L, Georgieff MK, Mills MM, Nelson CA. Neurobehavioral evidence for working memory deficits in school-aged children with histories of neonatal intensive care treatment. Dev Med Child
Neurol 1999;41:52133.
76. Casey BJ, Thomas KM, McCandliss B. Applications of magnetic resonance imaging to the study of development. In: Nelson CA, Luciana M,
eds. Handbook in developmental cognitive neuroscience. Cambridge,
MA: MIT Press, 2001:137 48.
77. Georgieff MK. Intrauterine growth and neurodevelopment. J Pediatr
1998;133:35.
78. Yanowitz TD, Potter DM, Bowen A, Baker RW, Roberts JM. Variability
in cerebral oxygen delivery is reduced in premature neonates exposed to
chorioamnionitis. Pediatr Res 2006;59:299 304.
79. Pihko E, Lauronen L. Somatosensory processing in healthy newborns.
Exp Neurol 2004;190:S27.
Downloaded from ajcn.nutrition.org by guest on May 4, 2015
57.
GEORGIEFF
Anda mungkin juga menyukai
- Cover Modul FCPDokumen3 halamanCover Modul FCPYusuf Almalik SaputraBelum ada peringkat
- 4 Vol. 7 Issue 1 Jan 2016 IJPSR RE 1738 Paper 4Dokumen11 halaman4 Vol. 7 Issue 1 Jan 2016 IJPSR RE 1738 Paper 4Yusuf Almalik SaputraBelum ada peringkat
- Uji Aktifitas Antikanker Ekstrak Etanol Kulit Batang Bruguiera Gymnorhiza Terhadap Sel Meyloma Warsinah, Puji Lestari, TrisnowatiDokumen7 halamanUji Aktifitas Antikanker Ekstrak Etanol Kulit Batang Bruguiera Gymnorhiza Terhadap Sel Meyloma Warsinah, Puji Lestari, TrisnowatiYusuf Almalik SaputraBelum ada peringkat
- Biochemistry of The EyeDokumen38 halamanBiochemistry of The EyeYusuf Almalik SaputraBelum ada peringkat
- Baby Blues & Postpartum Depression PDFDokumen2 halamanBaby Blues & Postpartum Depression PDFYusuf Almalik SaputraBelum ada peringkat
- Efektifitas Ekstrak Biji Srikaya (Annona Squamosa L) Dengan Pelarut Air, Metanol Dan Heksan Terhadap Mortalitas Larva Caplak Boophilus Microplus Secara in VitroDokumen9 halamanEfektifitas Ekstrak Biji Srikaya (Annona Squamosa L) Dengan Pelarut Air, Metanol Dan Heksan Terhadap Mortalitas Larva Caplak Boophilus Microplus Secara in VitroYusuf Almalik SaputraBelum ada peringkat
- Hormon Reproduksi: Dr. Septi Handayani, M.SiDokumen133 halamanHormon Reproduksi: Dr. Septi Handayani, M.SiYusuf Almalik SaputraBelum ada peringkat
- Kul. 6 Respiratory EmegencyDokumen46 halamanKul. 6 Respiratory EmegencyYusuf Almalik SaputraBelum ada peringkat
- Drugs Used in Gastrointestinal DiseasesDokumen44 halamanDrugs Used in Gastrointestinal DiseasesYusuf Almalik Saputra0% (1)
- Shoe Dog: A Memoir by the Creator of NikeDari EverandShoe Dog: A Memoir by the Creator of NikePenilaian: 4.5 dari 5 bintang4.5/5 (537)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDari EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifePenilaian: 4 dari 5 bintang4/5 (5794)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDari EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RacePenilaian: 4 dari 5 bintang4/5 (895)
- The Yellow House: A Memoir (2019 National Book Award Winner)Dari EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Penilaian: 4 dari 5 bintang4/5 (98)
- Grit: The Power of Passion and PerseveranceDari EverandGrit: The Power of Passion and PerseverancePenilaian: 4 dari 5 bintang4/5 (588)
- The Little Book of Hygge: Danish Secrets to Happy LivingDari EverandThe Little Book of Hygge: Danish Secrets to Happy LivingPenilaian: 3.5 dari 5 bintang3.5/5 (400)
- The Emperor of All Maladies: A Biography of CancerDari EverandThe Emperor of All Maladies: A Biography of CancerPenilaian: 4.5 dari 5 bintang4.5/5 (271)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDari EverandNever Split the Difference: Negotiating As If Your Life Depended On ItPenilaian: 4.5 dari 5 bintang4.5/5 (838)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDari EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyPenilaian: 3.5 dari 5 bintang3.5/5 (2259)
- On Fire: The (Burning) Case for a Green New DealDari EverandOn Fire: The (Burning) Case for a Green New DealPenilaian: 4 dari 5 bintang4/5 (74)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDari EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FuturePenilaian: 4.5 dari 5 bintang4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDari EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryPenilaian: 3.5 dari 5 bintang3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnDari EverandTeam of Rivals: The Political Genius of Abraham LincolnPenilaian: 4.5 dari 5 bintang4.5/5 (234)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDari EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaPenilaian: 4.5 dari 5 bintang4.5/5 (266)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDari EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersPenilaian: 4.5 dari 5 bintang4.5/5 (345)
- The Unwinding: An Inner History of the New AmericaDari EverandThe Unwinding: An Inner History of the New AmericaPenilaian: 4 dari 5 bintang4/5 (45)
- Rise of ISIS: A Threat We Can't IgnoreDari EverandRise of ISIS: A Threat We Can't IgnorePenilaian: 3.5 dari 5 bintang3.5/5 (137)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDari EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You ArePenilaian: 4 dari 5 bintang4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Dari EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Penilaian: 4.5 dari 5 bintang4.5/5 (121)
- Her Body and Other Parties: StoriesDari EverandHer Body and Other Parties: StoriesPenilaian: 4 dari 5 bintang4/5 (821)
- Neural Tube DefectsDokumen2 halamanNeural Tube DefectsVijay SluBelum ada peringkat
- Storage ConditionDokumen4 halamanStorage Conditioneshwar_1953Belum ada peringkat
- KVG Medical CollegeDokumen11 halamanKVG Medical CollegepentagoneducationBelum ada peringkat
- Brodil LevoDokumen2 halamanBrodil LevoAziza KhairunBelum ada peringkat
- 2010 Endocrine System ChartDokumen3 halaman2010 Endocrine System ChartAlexander QianBelum ada peringkat
- High Lateral Tension AbdominoplastyDokumen14 halamanHigh Lateral Tension AbdominoplastyAhmad Arbi AninditoBelum ada peringkat
- Anatomy and Physiology Respiratory SystemDokumen7 halamanAnatomy and Physiology Respiratory Systemnoronisa talusobBelum ada peringkat
- Thorax and Lungs SGDokumen2 halamanThorax and Lungs SGDestinee Caple100% (1)
- Navjaat Shishu Suraksha Karyakram: Training ManualDokumen99 halamanNavjaat Shishu Suraksha Karyakram: Training ManualBiswaranjan Padhy100% (1)
- Graseby 3100 Syringe Pump - Service ManualDokumen89 halamanGraseby 3100 Syringe Pump - Service ManualRamanjaneya goud100% (1)
- Oral Wound Healing Efficacy of 1% Myristica Fragrans (Nutmeg) Determined Using MTT Assay: An in Vitro StudyDokumen5 halamanOral Wound Healing Efficacy of 1% Myristica Fragrans (Nutmeg) Determined Using MTT Assay: An in Vitro StudyDeepthi ManjunathBelum ada peringkat
- TRAMADOLDokumen4 halamanTRAMADOLRudie Lee PascualBelum ada peringkat
- Limfoma Kutis Pada Pasien Yang Semula Di DiagnosisDokumen34 halamanLimfoma Kutis Pada Pasien Yang Semula Di DiagnosisChris MulyoBelum ada peringkat
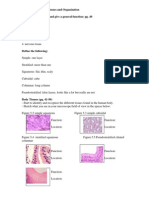
- Human Biology Laboratory 4: Body Tissues and Organization List The 4 Tissue Types and Give A General Function: Pg. 40Dokumen4 halamanHuman Biology Laboratory 4: Body Tissues and Organization List The 4 Tissue Types and Give A General Function: Pg. 40bugyourselfBelum ada peringkat
- Vasoactive Agents in Shock.2Dokumen8 halamanVasoactive Agents in Shock.2Linamaria LozanoBelum ada peringkat
- UKA: When Would I Do It?Dokumen35 halamanUKA: When Would I Do It?neareastspineBelum ada peringkat
- Soccer Programme U19 Pre in SeasonDokumen38 halamanSoccer Programme U19 Pre in SeasonJeffrey Peeko100% (1)
- Smear Layer Final2Dokumen10 halamanSmear Layer Final2bhudentBelum ada peringkat
- High Power Electrosurgery Review Update 2005Dokumen33 halamanHigh Power Electrosurgery Review Update 2005Ana ObradovicBelum ada peringkat
- 2018 - Vitamine D Treatment Guidelines in India - JClinSciResDokumen10 halaman2018 - Vitamine D Treatment Guidelines in India - JClinSciResnagashayana gBelum ada peringkat
- SialodenosisDokumen76 halamanSialodenosisJessica GreenBelum ada peringkat
- Drug Therapy in Pregnancy (Soal)Dokumen6 halamanDrug Therapy in Pregnancy (Soal)Yola FebriyantiBelum ada peringkat
- Cesarean Surgical Techniques - GLOWMDokumen36 halamanCesarean Surgical Techniques - GLOWMOana BalintBelum ada peringkat
- Role, Prospects, and Limitation of HomoeopathyDokumen43 halamanRole, Prospects, and Limitation of HomoeopathyDr.bhagyaBelum ada peringkat
- Neck Pain and Lower Back Pain. Med Clin N Am. 2019.Dokumen14 halamanNeck Pain and Lower Back Pain. Med Clin N Am. 2019.Jose Fernando Diez100% (1)
- Massive Transfusion ProtocolDokumen2 halamanMassive Transfusion ProtocolmukriBelum ada peringkat
- SCOLIOSISDokumen4 halamanSCOLIOSISapi-3822433Belum ada peringkat
- Efficacy and Adverse Events of Oral Isotretinoin For Acne: A Systematic ReviewDokumen10 halamanEfficacy and Adverse Events of Oral Isotretinoin For Acne: A Systematic ReviewFerryGoBelum ada peringkat
- At-Risk and Runaway Youth in Washington State: Outcomes For Youth Admitted To Secure Crisis Residential Centers and Mandatory Chemical Dependency TreatmentDokumen45 halamanAt-Risk and Runaway Youth in Washington State: Outcomes For Youth Admitted To Secure Crisis Residential Centers and Mandatory Chemical Dependency TreatmentWashington State Institute for Public PolicyBelum ada peringkat
- Cardiac GlycosidesDokumen8 halamanCardiac GlycosidesShan Sicat100% (1)