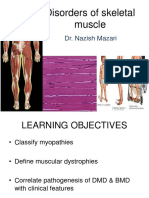
Muscle: Duchenne Muscular Dystrophy
Diunggah oleh
Micke RodriguezJudul Asli
Hak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Muscle: Duchenne Muscular Dystrophy
Diunggah oleh
Micke RodriguezHak Cipta:
Format Tersedia
27.05.
2015
muscle
Muscle diseases
type I (red) slow twitch muscle fibbers (numerous
mitochondria and much more of myoglobin); more
enzymes for Krebs cycle (aerobic oxidation) than
in fast twitch; almost unstained for alkaline ATPaze
reaction
type II (white) fast twitch muscle fibbers; faster
stronger contraction; Embden-Meyerhof pathway of
glycolysis (anaerobic); androgenic steroids cause their
hypertrophy, and disuse results in their selective atrophy
In humans no muscle composed exclusively of one
fibber type, but proportions vary from muscle to muscle
and from person to person (genetically determined).
Muscular dystrophy
disease characterised by progressive weakness of the
voluntary muscle
caused by primary muscle degeneration or by nervous
system involvement
primary muscular degeneration hereditary/familial;
relentlessly progressive
morphology:
degeneration of muscle fibers
regenerative activity
progressive fibrosis
infiltration of the muscle with fatty tissue
no inflammation
Duchenne Muscular Dystrophy (1)
(proressive muscular dystrophy//DMD)
non-inflammatory myopathy
severe, progressive and fatal, appears before the age of
4
inherited, X-linked, DMD and Becker muscular dystrophy
(BMD) occurs in 1/3,500 males (almost like cystic
fibrosis)
the Duchenne-Becker gene (one of the largest known
human genes 2x106 base pairs) located on the
chromosome X
27.05.2015
Duchenne Muscular Dystrophy (2)
boys suffer from progressive degeneration of muscles
(mainly the pelvic and shoulder girdles)
caused by deficiency of dystrophin (a cytoskeleton
protein located on the cytoplasmic face of the plasma
membrane, which linked to by an integral membrane
protein; play role in mechanical properties and flexibility
during contraction and relaxation)
DMD - no dystrophin
BMD - smaller then normal amount of dystrophin
DMD 33% new mutations
33% mutations in mother
33% family disease (more then one generation)
Duchenne Muscular Dystrophy (3)
pathology:
relentless degeneration
prolonged efforts to repair and regeneration
progressive fibrosis
progressively decreasing number of muscle fibers +
fibro-fatty connective tissue
early development of endomysial fibrosis
Duchenne Muscular Dystrophy (4)
Duchenne Muscular Dystrophy (5)
clinical diagnosis
elevelated of creatine kinase levels in the blood +
muscle biopsy (morphologica changes observed even in
utero)
prenatal diagnosis (DNA analysis and/or elevated
serum creatine kinase levels found in up to 75% of
carrier mothers)
clinical features:
normal growth within 1 year of life by the age of 18
months 50% of patients fail to walk proximal muscle
weakness and pseudohypertrophy of the calf muscles
striking tendency to form contractures when immobilized
for short time period
more then 90% affected boys are chair-bound by the age
of 11 years
patients are bedridden by the age of 15
decreased intelligence (20% are significantly retarded)
death occurs at the mean age of 17 years respiratory
inssuficiency and cardiac arrythmia
Becker Muscular Dystrophy
Myotonic Dystrophy (1)
milder form of DMD
later onset
at the age of 12, all patients are still walking
95% survive beyond the age of 21
the most common form of adult muscle dystrophia
sustained muscle contraction and rigitity (myotonia) +
progressive muscular weakness and wasting
incidence 14/100,000
gene responsible for the disease 19q13.3 (novel
cyclic AMP-depended protein kinase excitability of
sarcolemma becouse of abnormal forsorylation of ion
channels) in most cases descenceded from one
original mutaion
aticipation aerlier age of onset and increasing
severity of symptoms in successive generations
unstable genomic segment (CCG repeats)
27.05.2015
Myotonic Dystrophy (2)
pathology:
highly variable changes even in one patient
atrophy of type I fibers with hypertrophy of type II fibers
internally situated nuclei
ring fibers in ATPase reaction
necrosis and regeneration are not prominent
Myotonic Dystrophy (3)
clinic:
three types:
congenital
only in offspring of women who themselves exhibit symptoms of myotonic dystrophy
newborns with muscle weakness but myotonia is inconspicious or absent (appears
later)
mental retardation
classic adult onset
muscle weakness and stiffness principally in the distal limbs
facial and jaw muscles always affected (severe ptosis)
additionally cataracts and personality deterioration
some patients have smoth muscle involvement (GI, gallbladder, uterus, arrthmias)
minimal symptoms with late onset
CONGENITAL MYOPATHIES
abnormalities confined to type I fibers
type I fibers predominance (better to say: failure of type II fibers to
develop)
muscles do not show active degeneration no serum creatine kinase
elevation
CONGENITAL MYOPATHIES
Central core disease
congenital hypotonia + proximal muscle weakness
decreased deep tendom reflexes
delayed motor development
sporadid or AR or AD
muscle strenght never becoms normal
pathology:
predominance of type I fibers
central zone degeneration (loss of membranous organelles with or without
disorganization of myofibrillar architecture) [like in active denervating
conditions; but no evidence of such process]
periphery is unremarkable
CONGENITAL MYOPATHIES
Rod (Nemaline) myopathy
tangled/threadlike mass inclusions within muscle fibers
rod-shaped structures
group of diseases:
congenital (hypotonia, deleyed motor milestones, variable sevirity +
kyphoscoliosis; in some involvement of face, pharynx, and neck)
later-onset (childhood and adult; some muscle degeneration + elevation
of creatine kinase)
CONGENITAL MYOPATHIES
Central nuclear myopathy (myotubular myopathy)
group of diseases
AR, AD, X-linked
in severe cases death in neanatal period becouse of respiratory
insufficiency
pathology:
predominance of type I fibers
rod-shaped structures (inclusions arising from Z line)
27.05.2015
INFLAMMATORY MYOPATHIES
a. dermatomyositis
b. polymyositis
c. inclusion body myositis
Pathogenesis:
autoimmune origin:
follow viral infections
detected autoantibodies
muscle cell injury causwed by cytotoxic lymphocytes or complementmediated microangiopathy
INFLAMMATORY MYOPATHIES
dermatomyosistis:
lymphoid infiltration (mainly B cells)
high ratio of CD4+/CD8+ cells
proximity of helper T cells to B cells and macrophages
paucity of lymphocytes in uninvolved muscle fibers
injury produced primarly by complement-mediated cytotoxic antibodies
direct against the microvasculature of skeletal muscle tissue
ischemia of individual muscle fibers, microinfarcts, and secondary
inflammation
INFLAMMATORY MYOPATHIES
polymyosistis and inclusion body myosistis
direct muscle damage by cytotoxic T cells
no microangiopathy
healthy muscle fibbers surrounded by T cell (CD8+) and macrophages
degeneration of muscle fibber (express MHC-I Ag on sarcolemma)
MIASTENIA GRAVIS
Myasthenia gravis (2)
Autoimmune disease blockage and
destruction of acetylcholine receptors
(AChR) of motor end plate by
autoantibodies (IgG, may cross the
placenta).
Additionally, anti-AChR antibodies fix
complement and lead to direct injury to the
postsynaptic membrane.
Myasthenia gravis (3)
MORPHOLOGY:
no specific abnormalities on gross examination or LM
Sometimes focal collections of lymphocytes
(lymphorrhages).
In severe cases sometimes diffuse changes with type 2 fiber
atrophy.
Immunohistochemistry: IgG and complement components
on the motor end plate.
Electron microscope: damage of the motor end plate with
the loss of the normally complex folds.
27.05.2015
Myasthenia gravis (4)
CLINICAL FEATURES:
muscle weakness that is aggravated by repeated
contraction
muscles with the smallest motor units are affected first, most
typically ocular muscles (bilateral ptosis, diplopia) - only
ocular problems in 20% of patients.
In others, diasease progresses: facial muscles, limb girdle
muscles, and respiratory muscles.
Progression usually slow, respiratory muscles involvement
5-20 years after the onset.
Sensory and autonomic functions NOT affected.
Untreated, 40% of patients will die within 10 years.
Inherited and developmental diseases
Osteogenesis imperfecta
Osteopetrosis
Cleidocranial dysplasia (dysostosis)
Achondroplasia
Fibroosseus diseases
Cherubism
Osteogenesis imperfecta
symptoms when child learns to walk fragile as a china doll
thin, bulging skull and blue sclera, defness (mulitiple farctures)
hypermobile joints and thin translucent skin and heart valve defects
associated with dentinogenesis imperfecta (mainly deciduous
dentition)
in OI type I because of hypolpalsia of the dentine and pulp, the teeth
are misshapen and bluish yellow
four types:
type I most common (blue sclera, bone fragility and deafness)
type II most severe (bone factures in utero)
type III some defects visible at birth but latter progressive deformities
occur; growth retardation; common the teeth abnormalities
type IV similar to type I, but sclerae are normal; colagen forms delicate
thin fibrils (improper cross-linking)
Myasthenia gravis (6)
TREATMENT:
anticholinesterases.
in crisis situations (i.e. when respiratory function is
compromised) high-dosage corticosteroids, plasma
exchange.
Thymectomy is indicated remmision in many patients,
esp. in young women with recent onset of MG and thymic
hyperplasia.
Osteogenesis imperfecta
brittle bone disease
hereditary disease (heterogeneous group)
defective collagen type I synthesis (lower amount of procollagen
OI type I)
deletions and mutations of collagen type I gene OI type II, III, and
IV
characterized by generalized osteoporosis with slender bones
( tendency for pathologic fractures; they heal sometimes exuberant
callus formation)
the long bones have narrow and poorly formed cortices composed
by immature, woven bone
Osteopetrosis
(marble bone disease/Albers-Schnberg bone disease)
excessive density (blocklite) of all bones (but mechanically weak)
with marrow cavity obliteration ( anemia)
failure of bone remodelling (osteoclastic activity)
retention of the primary spongiosum with cartilage cores
lack of funnelization of the metaphysis
thickened cortex
thickened cortices with reduced marrow cavities, persistence of
woven bone and lack of lamellar bone, almost always cartilage core
could be observed
delayed teeth eruption
27.05.2015
Osteopetrosis
tooth extraction commonly followed by osteomyelitis
long bones have Erlenmeyer flask (widened metaphysis
and diaphysis)
on x-ray no distinction between cortical and medullary bone;
almost invisible tooth roots
mandible more common involved then maxilla
two types:
Cleidocranial dysplasia
(dysostosis)
many bones abnormalities, mainly skull, jaw and clavicles (lack)
with dental abnormalities
AD
flat skull, prominent frontal, parietal and occipital bones,
opened fontanelles and sutures
high and narrow arched palate with underdevelopment of maxilla
retained deciduous teeth and or non-erupted permanent dentition
supernumerary teeth (mandibular premolar and incisor region)
early in life (AR), multiple fractures with early death (before puberty)
benign (AD), sometimes with mild symptoms and very late diagnosis
Achondroplasia
the most common form of dwarfism (F = 125 cm, and M = 131 cm)
no mental retardation, and normal average life span
abnormal endochondral ossification (defect/absence of the zone
of provisional ossification of the cartilage in the epiphyses and the
skull base middle third of the face is retrusive)
but intramembranous ossification is undisturbed and periosteum
function is normal bones are very short but thick
the trunk and skull (sometimes large) of normal size but the
extremities are extremely short; sometimes severe kyphoscoliosis
develops
AD or fresh mutations (most common)
Fibrous dysplasia of the bone (1)
Etiology unknown developmental defect?
Disorganized mixture of fibrous and osseus
elements in the interior
of affected bones
FIBROOSSEUS LESIONS
Fibrous dysplasia of the bone (2a)
monostotic
more common than polyostotic
2nd and 3rd decade, M=F
most frequently extremities > ribs > skull (jaws
maxilla > mandible)
usually present at childhood or adolescents
In 5% of patients McCune-Albright syndrome
(bone lesions + skin pigmentation + endocrine
abnormalities)
27.05.2015
Fibrous dysplasia of the bone (2b)
presentation:
painless asymmetric enlargement of poorly
circumscribed mass even on x-ray (may mimic a
cyst)
usually placed more buccally than lingually or
palatally
maxillary masses (distal to the canine fossa) often
lead
to extension to the sinus, zygomatic processus, and
floor of the orbit
mandible masses (molar and premolar region)
they may lead to tooth abnormalities
Fibrous dysplasia of the bone (2c)
Fibrous dysplasia of the bone (2d)
morphology:
replacement of normal bone by fibrous tissue
(sometimes more cellular or plenty of thick
collagen bundles) with islands of trabeculae of
metaplastic bone (irregular shape, coarse-fibred
woven bone with varying amounts of osteoid
in jaw lesion could be more variable than in long
bones with spheroidal areas of calcification
resembling cementum
osteclastic and osteoblastic activity may be seen
Cherubism (1)
polyostotic
F:M = 3:1
25% of patients have exhibit disease in more than half of
the skeleton including facila bones
mainly in long bones (lower extremities) than in skull
vertebrae, ribs
and pelvis
involve one bone segmentally or one side of the body
diagnosed in childhood (pathologic fractures of deformed
bones),
accompanied (sometimes) by caf au lait spots (coast of
Maine)
Albright syndrome (endocrine disfunction
acromegaly, Cushing syndrome, hyperthyroidism,
vitamin D-resistant rickets)
rare disease, AD, M:F = 2:1
at the age of 2-4 years, painless usually asymmetric
enlargement of mandible (less often maxilla) that stops
at the age of 7, then regression of face deformity occurs
characteristically chubby face (fullness of the chicks
and enlarged submandibular lymph nodes) is observed
eyes upturn to heavens (visible rim of sclera beneath the
iris)
premature loss of deciduous teeth with failure of
development of many permanent ones
on x-rays multiple radiolucent sharply demarcated
lesions
Cherubism (2)
Osteomyelitis
morphology:
- cellular and vascular fibrous tissue containing
multinucleated giant cells
differs from the inflammation of the long
bones:
usually a localized condition
associtaed with periodontal infection
usually involves otherwise healthy adults
often caused by anaerobes
27.05.2015
acute suppurative (rarefying) osteomyelitis
now rare
adult males
presented with pain, swelling, paresthesia of the lip, pyrexia, and
mobility of the teeth, trismus
following teeth infection (mixed flora, but St. aureus is a rare
factor) or local trauma
mandible is predisposed for it
risk factors: DM, leukaemia, bone diseases (osteopetrosis,
Pagets disease, radiation-damage)
tissue necrosis develops because of thrombosis in surrounding
blood supply, then marrow cavity is filled with pus (sometimes
with sequestrum)
latter granulation tissue is developing
x-rays: lytic bone destruction (after one week) and later
periosteal bone formation
focal sclerosing osteomyelitis
(condensing/sclerosing osteitis)
a special type of chronicc osteomyelitis
at the apex of the tooth (first permanent
molar)
patients usually before the age of 20
usually asymptomatic
bone reaction to periodontal infection
fibrosed marrow with some lymphocytes and
plasma cells and local increased thickness of
bone trabeculae
chronic suppurative (rarefying) osteomyelitis
may follow an acute osteomyelitis or start as
chronic from the beginning (tuberculosis,
syphilis or actinomycosis, but all of those are
now rare)
symptoms are more insidious
marrow cavity contains granulation tissue
rather than pus
diffuse sclerosing osteomyelitis
also a special type of chronic ostemyoelitis
as focsal sclerosis osteomyleitis but occurs in
patients with widespread periodontitis
occurs in elderly patients (blacks)
often bilateral, mandible or maxilla
sometimes with fistulas formation
chronic osteomyelitis with proliferative
periostitis
radiation osteomyelitis
(osteoradionecrosis)
(Garres osteomyelitis; periostitis ossificans)
radiation induced occlusion of the vessels
asymptomatic bone necrosis rapid
spread of infection form surrounding
structures painful necrosis of the bone
exclusively in mandible
children and young adults
spread of inflammation (apical, soft tissue,
mechanical irritation) with a proliferation
reaction of the periosteum (visible on x-rays)
27.05.2015
chemical osteomytelitis
now rare
associated with phosphorus and mercury
poisons
pulse granuloma/vegetable granuloma
chronic periostitis associated with hyaline
bodies (ring-shaped) accompanied by
giant cells
Bone diseases
METABOLIC AND ENDOCRINE
BONE DISAESES
OSTEOPOROSIS
osteoporosis
decreased bone strength
reduction in the bone mass (density) increasing porosity of the
skeleton fractures (1.5 mln fractures a year in USA), mainly:
vertebral and hip
in USA affects > 10 mln patients (8 mln and 2 mln ), but
additional 18 mln have decreased bone mass
Def:
reduction in the bone mass (density) or the presence of fragility
fractures
most women meet criteria by the age 70 to 80
27.05.2015
osteoporosis
osteoporosis
Consequences:
in USA about 300,000 hip fractures a year
(about 14% of risk for 50-year-old white individual and about 5%
risk for same ; related African Americans have a half risk rate)
deep vein thrombosis
Pulmonary embolism (20-50%)
5-20% mortality (in 12 months after surgery)
vertebral crush fractures 700,000 a year (less clinically
significant, some asymptomatic) multiple height loss, kyphosis,
secondary pain, altered biomechanics of the back, pulmonary
restrictive diseases (thoracic) or abdominal symptoms such as
constipation, distension and early satiety (lumbar region)
wrist fractures about 250,000 a year
other (e.g. humerus, pelvis) fractures 300.000 a year
10
27.05.2015
osteoporosis
Primary:
Postmenopausal
Senile
Secondary:
Endocrine dis:
Hyperparathyroidisms
Hypo/hyperthyroidisms
Hypogonadism
Pituitary tu.
DM type 1
Addisons disease
Neoplasia:
Multiple myeloma
carcinomatosis
Secondary (cd):
drugs:
Anticoagulants
Chemotherapy
Corticosteroids
Anticonvulsants
Alcohol
GI diseases:
Malnutrition
Malabsorption
Hepatic insufficiency
Deficiency of vit C/D
idiopathic
osteoporosis
peak bone density early adulthood (it could be stable during age
30 to 45, latter we observe - imbalance between the bone resorption
and formation) according to genes, life-style, nutrition
heritability responds to from 50 to 80% for bone density,
candidate genes:
vit. D rec.
type I collagen
estrogen rec.
IL-6
IGF-I
locus on chr. 11 associated with high bone mass (extreme bone mass in
patients with mutation LRP5 [ LDL receptor related protein])
osteoporosis
Miclellaneous:
- Osteogenesis imperfecta
- Immobilisation
- Pulmonanry diseases
- Homocystynuria
- Anemia
Other causes:
dementia
Parkinsons disease
multiple sclerosis
osteoporosis
hormones that have influence on bone remodeling:
estrogens
androgens
vit. D
PTH
and produced locally
IGF-I and II
TGF-
PTHrP
ILs
prostaglandins
TNF
and cytokines (RANK, and osteoprotegerin ligand)
osteoporosis
other causes:
inadequate calcium intake during growth
in adult life inadequate calcium intake (recommended 1000-1200 mg/d;
<400mg/d detrimental for skeleton) secondary hyperparathyroidism
vit D deficiency (elderly, living in northern latitudes, poor nutrition,
malabsorption, chronic liver disease, chronic kidney disease) compensatory
hyperparathyroidism
estrogen function cessation
physical activity (inactivity, bed rest and paralysis versus athletes)
chronic diseases (nutrition + reduced physical activity + factors influencing
bone remodeling)
Medication
cigarette smoking ( toxic effect on osteoblasts; modifying estrogen
activity; and secondary effects: respiratory illnesses, frailty, decreased
exercise, poor nutrition and medication [eg. glucocorticoids])
osteoporosis
morphology:
in trabecular bone, if the osteoclasts penetrate trabeculae, they
leave no template for new born formation to occur ( rapid bone
loss)
in cortical bone, increased activation of remodeling creates more
porous bone
micro-fractures (collapse of vertebrae)
thinned cortex
Haversian systems widened
estrogen levels secretion of IL-1 (stimulator of osteoclast
recruitment and activity)
11
27.05.2015
rickets and osteomalacia
deficiency or resistance to vitamin D
failure of mineralization of bone and cartilage
enamel hypoplasia, increased width of predentine, large amounts of
interglobular dentine
delayed dentition, severe dental caries, enamel defects
lack of growth of vertical ramus of the mandible
Bone diseases
RICKETS/OSTEOMALACIA
PARATHYROID GLANDS:
ANATOMY AND PHYSIOLOGY
- the parathyroids arise from the third and
fourth branchial clefts
- 3 or 4 but 5 or 6 too
- each 3-4 mm and weigh 35 mg each
Primary hyperthyroidism
is a common clinical problem
1 person in 1000 will need parathyroid
surgery during his or her lifetime
Patient with MEN I has about an 85%
lifetime chance of getting primary
hyperparathyroidism;
with MEN II has about a 20% chance
(usually hyperplasias).
HYPERPARATHYROIDISM
("stone and bone disease")
PRIMARY HYPERPARATHYROIDISM due to disease of the
parathyroid glands.
80-85%... parathyroid "adenoma" ("single gland disease")
10-15%... parathyroid "hyperplasia" ("multiple gland disease",
usually all four glands)
maybe 1%... parathyroid carcinoma (I think this traditional number is
high)
<1%... iatrogenic seeding causing lots of little glands:
hypercalcemia caused by production of parathyroid-hormone-like
activity (PTH-rP) by cancers (eg. squamous lung cancer)
"pseudohyperparathyroidism"
Primary hyperthyroidism
Symptoms and signs:
Elevated serum calcium on routine screening (most common
now)
Mental changes (depression, psychosis)
kidney stones (the commonest presentation in the past)
nephrocalcinosis (metastatic calcification in the tubular
basement membranes with eventual damage to the tubules)
bone changes (first osteomalacia, then widespread involvement
of the skeleton by increased osteoclastic activity especially in the
centers of trabeculae; finally cystic lesions variously known as
"osteitis fibrosa cystica", "von Recklinghausen's disease of
bone", or "brown tumors." All this heals after the
hyperparathyroidism is fixed.)
most extreme: Calciphylaxis (metastatic calcification of the skin,
with horrible ulcers and breakdown)
12
27.05.2015
Primary hyperthyroidism
Symptoms and signs:
gastric ulcers (5%; hypercalcemia from any cause enhances
gastrin secretion)
hypertension (50%, cured by parathyroid surgery only if the
kidney is undamaged)
pancreatitis (occasionally)
pseudogout (occasionally)
13
Anda mungkin juga menyukai
- Transverse Myelitis, A Simple Guide To The Condition, Treatment And Related DiseasesDari EverandTransverse Myelitis, A Simple Guide To The Condition, Treatment And Related DiseasesPenilaian: 5 dari 5 bintang5/5 (1)
- 1 - Skeletal Muscle DisordersDokumen32 halaman1 - Skeletal Muscle DisordersGarrett ZajicekBelum ada peringkat
- 08.01.24 Dr. Helal, DMD, CPD-2Dokumen60 halaman08.01.24 Dr. Helal, DMD, CPD-2Minhajul IslamBelum ada peringkat
- Muscle Disease For PhysiosDokumen46 halamanMuscle Disease For PhysiosKrishna KanthBelum ada peringkat
- Neuromuscular dis د.رشاد عبدالغنيDokumen47 halamanNeuromuscular dis د.رشاد عبدالغنيMohammad Belbahaith100% (1)
- Mod9Week7 - PA 3306 - Oct 2&3Dokumen64 halamanMod9Week7 - PA 3306 - Oct 2&3komal sheikhBelum ada peringkat
- Arthritis 180325095830 PDFDokumen77 halamanArthritis 180325095830 PDFHesoca HuxBelum ada peringkat
- Als Med Surg Group 2Dokumen17 halamanAls Med Surg Group 2David MharkBelum ada peringkat
- Skeletal Muscle Pathology For Second Year Dental Students: by Dr. Ioannis G. KoutlasDokumen8 halamanSkeletal Muscle Pathology For Second Year Dental Students: by Dr. Ioannis G. KoutlasnaglaramdanBelum ada peringkat
- Disorders of Skeletal MuscleDokumen31 halamanDisorders of Skeletal Muscleapi-19916399Belum ada peringkat
- Myopathy: By: Rey MartinoDokumen16 halamanMyopathy: By: Rey Martinorey martinoBelum ada peringkat
- Systematic PathologyDokumen119 halamanSystematic Pathologypatricemuza69Belum ada peringkat
- 22 Disorders of Skeletal Muscle by DR NazishDokumen41 halaman22 Disorders of Skeletal Muscle by DR NazishAhmed YTBelum ada peringkat
- Kelainan Neuromuskuler: Dr. Luhu A. Tapiheru, SP.S Fakultas Kedokteran Universitas Muhammadiyah MedanDokumen84 halamanKelainan Neuromuskuler: Dr. Luhu A. Tapiheru, SP.S Fakultas Kedokteran Universitas Muhammadiyah MedandanieliqbalBelum ada peringkat
- Diseases of The MuscleDokumen51 halamanDiseases of The MuscleGianina RafaelBelum ada peringkat
- Cell and Tissue InjuryDokumen60 halamanCell and Tissue InjurydesiBelum ada peringkat
- Approach To Myopathy by AnkitDokumen83 halamanApproach To Myopathy by AnkitankitBelum ada peringkat
- CBT Ortho 1Dokumen45 halamanCBT Ortho 1putri umepalBelum ada peringkat
- Pathology Muskulo SkletalDokumen68 halamanPathology Muskulo SkletalwilliamBelum ada peringkat
- Muscular Dystrophy NoteDokumen6 halamanMuscular Dystrophy NoteMd. Sherajul HaqueBelum ada peringkat
- Osteoartritis Dan GoutDokumen66 halamanOsteoartritis Dan GoutReioctabianoBelum ada peringkat
- Disturbances of Growth Asnan Sphinx 6 PDFDokumen20 halamanDisturbances of Growth Asnan Sphinx 6 PDFmina hishamBelum ada peringkat
- 7 Soft Tissue Tumor-Muscular DystrophyDokumen23 halaman7 Soft Tissue Tumor-Muscular DystrophyDikpal BikramBelum ada peringkat
- Classification of Disorders of Musculoskeletal System (MSK) : Presented By: Siti Sarah Maha Dewi Bong Jen NeeDokumen69 halamanClassification of Disorders of Musculoskeletal System (MSK) : Presented By: Siti Sarah Maha Dewi Bong Jen NeeBONG AIKCHINGBelum ada peringkat
- Assesment Rheumatoid ArthritisDokumen39 halamanAssesment Rheumatoid ArthritisKlinik SakuramedicaBelum ada peringkat
- FinalDokumen87 halamanFinalSanjiv GoyalBelum ada peringkat
- Biochemistry-Musculoskeletal DisorderDokumen17 halamanBiochemistry-Musculoskeletal DisorderSyifa SalsabilaBelum ada peringkat
- Pathology Lecture SeriesDokumen168 halamanPathology Lecture SeriesButch DumdumBelum ada peringkat
- Epidemiology, Genetics, PathophysiologyDokumen18 halamanEpidemiology, Genetics, PathophysiologySutapa PawarBelum ada peringkat
- Osteoarthritis (Oa) : Prakash Thakulla InternDokumen48 halamanOsteoarthritis (Oa) : Prakash Thakulla InternPrakash ThakullaBelum ada peringkat
- Bone Disorders PPT Part 4 of 4Dokumen28 halamanBone Disorders PPT Part 4 of 4Mister CrabsBelum ada peringkat
- NewGeneral Pathology2Dokumen305 halamanNewGeneral Pathology2Tahir AzizBelum ada peringkat
- (K25) Path - Musculosceletal FK Part 2Dokumen69 halaman(K25) Path - Musculosceletal FK Part 2Virginia JawaBelum ada peringkat
- Complications of FractureDokumen19 halamanComplications of FractureEsome Sharma100% (1)
- JointsDokumen68 halamanJointsLaine ZeeBelum ada peringkat
- MyopathyDokumen47 halamanMyopathySOUMYADEEP BHUINYABelum ada peringkat
- Rheumatology: Osteoarthritis Rheumatoid Arthritis: Dr. Meg-Angela Christi AmoresDokumen25 halamanRheumatology: Osteoarthritis Rheumatoid Arthritis: Dr. Meg-Angela Christi AmoresNinaBelum ada peringkat
- OSTEOARTHRITISDokumen29 halamanOSTEOARTHRITISValabhoju Bindu MadhaviBelum ada peringkat
- NewGeneral Pathology2Dokumen305 halamanNewGeneral Pathology2Tahir AzizBelum ada peringkat
- Cell InjuryDokumen132 halamanCell InjuryAboubakar Moalim Mahad moh'dBelum ada peringkat
- Polymyositis DermatomyositisDokumen2 halamanPolymyositis DermatomyositisTay Woo ChiaoBelum ada peringkat
- MuscolskeletalDokumen74 halamanMuscolskeletalsamar yousif mohamedBelum ada peringkat
- 病理國考複習 PDFDokumen61 halaman病理國考複習 PDFAnonymous ZUQcbcBelum ada peringkat
- Cellular Responses To Stress and Toxic Insults: Adaptation, Injury, and DeathDokumen26 halamanCellular Responses To Stress and Toxic Insults: Adaptation, Injury, and DeathHusam ShawaqfehBelum ada peringkat
- Screenshot 2022-11-29 at 1.52.52 PMDokumen13 halamanScreenshot 2022-11-29 at 1.52.52 PMf267wbmdfkBelum ada peringkat
- Common Bone Disorders: Bone and Cartilage Deterioration Is A Natural Process As We AgeDokumen28 halamanCommon Bone Disorders: Bone and Cartilage Deterioration Is A Natural Process As We Ageluckyswiss7776848Belum ada peringkat
- Myopathy: Continuing Education ActivityDokumen15 halamanMyopathy: Continuing Education ActivityHerry GunawanBelum ada peringkat
- Myotonic Dystrophy Type I (Steinert's Disease)Dokumen3 halamanMyotonic Dystrophy Type I (Steinert's Disease)Mohan KrishabiBelum ada peringkat
- Collagen Presentation 2Dokumen8 halamanCollagen Presentation 2Sanjay VeerasammyBelum ada peringkat
- Myopathies: Presenter: DR Edom G/medhin (IMR3) Moderator: DR Teklil Hagos (Consultant Neurologist) July 23 /2021Dokumen48 halamanMyopathies: Presenter: DR Edom G/medhin (IMR3) Moderator: DR Teklil Hagos (Consultant Neurologist) July 23 /2021Meseret Hamer ZewdieBelum ada peringkat
- Anaphy Lec DiseaseDokumen8 halamanAnaphy Lec DiseaseJules ConcepcionBelum ada peringkat
- OsteoarthritisDokumen40 halamanOsteoarthritiskylieverBelum ada peringkat
- Osteogenesis Imperfecta, AMCDokumen6 halamanOsteogenesis Imperfecta, AMCmakananlezatBelum ada peringkat
- Class 2Dokumen65 halamanClass 2hari dharshanBelum ada peringkat
- Osteomyelitis: Pediatric Surgery Department Andreev D.ADokumen83 halamanOsteomyelitis: Pediatric Surgery Department Andreev D.AlimeddyBelum ada peringkat
- IT 1 Introduction Blok 22 - PRMDokumen18 halamanIT 1 Introduction Blok 22 - PRMApriyani Supia DewiBelum ada peringkat
- UU 5 1997psikotropikaDokumen85 halamanUU 5 1997psikotropikaMeilina PutriBelum ada peringkat
- Muscular DystrophiesDokumen36 halamanMuscular DystrophiesAbdullah AzamBelum ada peringkat
- 2011 Spring SURGERY III BY Ismail Answere: Past Papers Question andDokumen11 halaman2011 Spring SURGERY III BY Ismail Answere: Past Papers Question andDerranMorganBelum ada peringkat
- Necrosis and Cellualr AdaptationDokumen56 halamanNecrosis and Cellualr AdaptationEs SarveshBelum ada peringkat
- Book PDFDokumen186 halamanBook PDFLuis CcenchoBelum ada peringkat
- Obstetric by 10 Teachers Chapter 8Dokumen25 halamanObstetric by 10 Teachers Chapter 8FerasBelum ada peringkat
- Hirschsprung Disease (Congenital Aganglionic Megacolon) : PathophysiologyDokumen2 halamanHirschsprung Disease (Congenital Aganglionic Megacolon) : PathophysiologyDiane Mary S. Mamenta100% (1)
- Dilation and CurettageDokumen2 halamanDilation and CurettageElisse GarciaBelum ada peringkat
- JSS MoUDokumen88 halamanJSS MoUchetanhiremathBelum ada peringkat
- Corticosteroids 24613Dokumen33 halamanCorticosteroids 24613NOorulain HyderBelum ada peringkat
- TumorDokumen8 halamanTumorputyCeria86Belum ada peringkat
- Malaika Nakupenda MalaikaDokumen11 halamanMalaika Nakupenda MalaikaMuhidin Issa MichuziBelum ada peringkat
- 1-History of Surgery in UkraineDokumen16 halaman1-History of Surgery in UkraineErdemBelum ada peringkat
- Exercises in Epidemiology Applying Principles and MethodsDokumen266 halamanExercises in Epidemiology Applying Principles and MethodsVivin Fitriana91% (11)
- Test ExpositionDokumen9 halamanTest ExpositionFatimatuz Zahro'Belum ada peringkat
- THORACENTESISDokumen9 halamanTHORACENTESISJohn Ray J. PaigBelum ada peringkat
- Pemeriksaan Colok DuburDokumen9 halamanPemeriksaan Colok DuburRidwan Hadinata SalimBelum ada peringkat
- Approach To Patients EULARDokumen35 halamanApproach To Patients EULARstuckinbedBelum ada peringkat
- Physiology of The PancreasDokumen4 halamanPhysiology of The PancreasClayton VerBerkmösBelum ada peringkat
- Multidisciplinary Patient Care Navigator To Help Patients at Brinton Lake - Crozer-Keystone Health System - PADokumen2 halamanMultidisciplinary Patient Care Navigator To Help Patients at Brinton Lake - Crozer-Keystone Health System - PAnbmyersBelum ada peringkat
- Giant Cell Lesions of The Jaws: DR Syeda Noureen IqbalDokumen61 halamanGiant Cell Lesions of The Jaws: DR Syeda Noureen IqbalMuhammad maaz khanBelum ada peringkat
- Arab Board Final 2018 - 2Dokumen12 halamanArab Board Final 2018 - 2lonsilord17Belum ada peringkat
- Malignancy Yield of Testis PathologyDokumen7 halamanMalignancy Yield of Testis PathologyadolfoBelum ada peringkat
- Total Glossectomy For Tongue CancerDokumen10 halamanTotal Glossectomy For Tongue CancerRajan KarmakarBelum ada peringkat
- PTW PresentationDokumen44 halamanPTW PresentationGina RBelum ada peringkat
- Telus Health - Care Centres Elite Preventative Health Assessment 2021Dokumen2 halamanTelus Health - Care Centres Elite Preventative Health Assessment 2021sergii volodarskiBelum ada peringkat
- Revised Proposal Water TreatmentDokumen13 halamanRevised Proposal Water TreatmentBryan Henson CarreonBelum ada peringkat
- Airway Management - DR Dedi SpAnDokumen120 halamanAirway Management - DR Dedi SpAnBagus Abdillah WinataBelum ada peringkat
- Tawam Gen InfoDokumen10 halamanTawam Gen InfoiknowvskiBelum ada peringkat
- Drug Use During Pregnancy and LactationDokumen50 halamanDrug Use During Pregnancy and LactationJuveria Fatima75% (4)
- Power Guard 818 MSDSDokumen4 halamanPower Guard 818 MSDSPowerGuardSealersBelum ada peringkat
- Creatine Kinase. by AsifDokumen10 halamanCreatine Kinase. by AsifharisBelum ada peringkat
- Kardex: Diet: Interventions IVF (Indicate Date and Time Started) Room Number: 313Dokumen2 halamanKardex: Diet: Interventions IVF (Indicate Date and Time Started) Room Number: 313kuro hanabusaBelum ada peringkat
- (23933356 - Romanian Journal of Rhinology) Sphenoid Rhinosinusitis Associated With Abducens Nerve Palsy - Case ReportDokumen6 halaman(23933356 - Romanian Journal of Rhinology) Sphenoid Rhinosinusitis Associated With Abducens Nerve Palsy - Case ReportFoppy PuspitasariBelum ada peringkat