Chapter II - Thesis Breast Cancer
Diunggah oleh
roxannefourteenHak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Chapter II - Thesis Breast Cancer
Diunggah oleh
roxannefourteenHak Cipta:
Format Tersedia
9
Chapter II
REVIEW OF RELATED LITERATURE
This chapter embodies literatures and studies, published, unpublished and
posted online, of local and foreign locale, found in books, journal, magazines and similar
periodicals as well in Internet websites which in essence are supportive of the theme of
the study at hand.
Foreign Literature
Each woman's breast cancer risk may be higher or lower, depending upon
several factors, including family history, genetics, age of menstruation, and other factors
that have not yet been identified. While breast cancer is less common at a young age
(i.e., in their thirties), younger women tend to have more aggressive breast cancers than
older women, which may explain why survival rates are lower among younger women.
All women are at risk for developing breast cancer. The older a woman is, the greater
her chances of developing breast cancer. Approximately 77% of breast cancer cases
occur in women over 50 years of age (http://www.imaginis.com/breast-health/breastcancer-statistics-on-incidence-survival-and-screening-2).
Dramatically, one-third of breast cancer deaths could be decreased if detected
and treated early. In a worldwide context, this means that 400,000 lives could be saved
every year (Danaei et al., 2005). The World Health Organization (WHO, 2009) has
suggested that two components of early detection have been shown to improve cancer
mortality: Educationto help people recognize early signs of cancer and seek prompt
medical attention for symptoms and Screening programsto identify early cancer or
pre-cancer before signs are recognizable, including mammography for breast cancer. In
the UK and US, effective education and screening could save between 12 to 37 lives
per day, respectively (http://www.worldwidebreastcancer.com/learn/breast-cancer-statis
tics-worldwide/).
10
According to Microsoft Encarta Encyclopedia (2007), treatment of breast
cancer depends on a womans age and health as well as the type, extent, and location
of the tumor, and if the cancer has remained in the breast or has spread to other parts
of the body. Treatment may include surgery, radiation, chemotherapy, hormone
therapy, or a combination of treatments.
Removal of a cancerous tumor by surgery cures one-third of all breast cancers
that are detected early. If only the lump and some surrounding breast tissue are
removed, leaving most of the breast intact, the procedure is called a partial
mastectomy, or lumpectomy. In a simple mastectomy, only the affected breast is
removed. When the breast and other tissues surrounding it are removed, the
operation is termed a radical mastectomy. Doctors have found that radical
mastectomies do not improve patient survival rates, and therefore are rarely worth the
significant changes that they impose on the female body. Many women choose to
have breast reconstruction surgery right after a mastectomy to restore the breasts
appearance.
In some cases, doctors recommend radiation therapy in addition to surgery to
treat cancer that has not spread beyond the breast. Radiation therapy uses highenergy rays or particles that destroy cancer cells that may remain in the breast, chest
wall, or underarm area after surgery
In chemotherapy, a patient receives cancer-fighting drugs intravenously to
destroy breast cancer cells that have spread to other organs. Chemotherapy may be
given in addition to surgery to reduce the risk that breast cancer will recur. It also may
be used as the primary treatment for women with more advanced cases of breast
cancer. In these cases, high doses of chemotherapy kill cancer cells, but they also kill
stem cells, blood-producing cells in the bone marrow. Some women in advanced
stages of breast cancer may undergo chemotherapy followed by a bone-marrow
transplant to restore healthy stem cells, although it is not yet clear whether this
procedure helps prolong a womans survival.
11
Hormone therapy exploits some of the chemicals the body naturally produces.
For example, some breast cancer cells thrive on the hormone estrogen, which is
produced in the ovaries. Hormone therapy slows the growth of such cells by
preventing them from using estrogen. One of the drugs employed in endocrine
therapy ]is tamoxifen, which prevents breast cancer from recurring. It may also
prevent new cancers from forming in the other breast. Tamoxifens chemical cousin,
raloxifene, has shown similar results in preliminary studies. The most radical forms of
hormone therapy are the removal of the ovaries by surgery or the virtual destruction of
the ovaries by radiation treatments to prevent these organs from secreting estrogen.
Research into breast cancer treatment and prevention is ongoing. A number of
drugs are under investigation for treating breast cancer. One of the newest forms of
breast cancer treatments is a monoclonal antibody called trastuzumab, marketed
under the brand name Herceptin. This drug targets cells that overproduce HER-2, a
protein implicated in about one-third of all breast cancer cases.
Women with a family history of breast cancer may choose to undergo genetic
testing to determine if they carry mutated forms of the BRCA1 or BRCA2 genes. There
is no way to know for sure if a woman who carries these genes will develop breast
cancer, but statistics show that about 50 to 60 percent of women with these mutations
will develop the disease by the age of 70. Although there is no surefire way to prevent
breast cancer, women who test positively for these genes may elect to take
precautions that may lower their risk of developing the disease. For example, they
may decrease the level of fat and alcohol in their diets and eat more fruits and
vegetablesfoods that have been shown to decrease an individuals risk of
developing most types of cancer. Recent studies show that in women who are at very
high risk for breast cancer, prophylactic mastectomies significantly lower this risk. In
this procedure, surgeons remove both breasts before any signs of breast cancer are
detected to remove the vulnerable tissue before cancer can take hold.
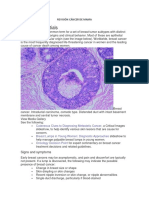
Each breast has 15 to 20 sections called lobes (Panno, 2005). Within each lobe
are many smaller lobules. Lobules end in dozens of tiny bulbs that can produce milk.
12
Thin tubes, called ducts, link all the lobes, lobules, and bulbs. These ducts lead to the
nipple in the center of a dark area of skin called the areola. There are no muscles in the
breast, but muscles lie under each breast and cover the ribs. The breasts also contain
blood vessels and vessels for the lymphatic system, which consists of many lymph
nodes found throughout the body. Many lymph nodes are found near the breast, under
the arm, above the collarbone, and in the chest. The most common type of breast
cancer is ductal carcinoma, which begins in the lining of the ducts. The second type
occurs in the lobes and is called lobular carcinoma.
Breast cancer or malignant breast neoplasm is cancer origination from breast
tissue, most commonly from the inner lining of milk ducts or the lobules that supply the
ducts with milk (Sariego, 2010). Cancers originating from ducts are known as ductal
carcinomas; those originating from lobules are known as lobular carcinomas. Breast
cancer is a disease of humans and other mammals; while the overwhelming majority
cases in humans are women, men can also develop breast cancer (US NIH, 2011).
Breast cancer is more than 100 times more common in women than breast
cancer in men, although males tend to have poorer outcomes due to delays in diagnosis
(NCI, 2010; Buchholz, 2009). The size, stage, rate of growth, and other characteristics
of the tumor determine the kinds of treatment. Treatment may include surgery, drugs
(hormonal therapy and chemotherapy), radiation and/or immunotherapy (Florescu et al.,
2011).
According to Diab, Ellege, and Clark (2000), as cited by Overcash and Balducci
(2003), breast cancer in older women is thought to be less aggressive, with a larger
percentage of estrogen-receptor (ER) positive cells and more favorable. The major risk
factor for breast cancer is age older than 60 years (McCarthy et al., 1998). Additionally,
breast cancer is an important diagnostic consideration even if the older woman has no
family history of the disease. Many other risk factors have been identified including first
degree relative with breast cancer diagnosed when younger than 40, postmenopausal
body mass index greater than 35, menopause at 55 or older, menarche before the age
of 12 (Collaborative Group on Hormonal Factors in Breast Cancer, 1997).
13
Hormone replacement therapy (HRD) with estrogen has been implicated in postmenopausal women as a risk factor for breast cancer (Clemons and Goss, 2001). The
combination of estrogen-progesterone therapy may cause a rise in a cancer risk, which
is more than for estrogen alone. It has been shown, however that the breast cancers
found in women taking HRT may have a low biologic aggressiveness (Holli, Isola and
Cuzick, 1998).
The association between fat intake and breast cancer remains controversial.
Recent studies have also been unable to confirm any association between fruit and
vegetable consumption and breast cancer risk (Smith-Warner, Spiegelman and Yaun,
2001).
After the breast cancer has been diagnosed, the healthcare team will
recommend treatment. There are five standard treatment options for breast cancer:
surgery, chemotherapy, targeted therapies, radiation, and hormonal therapy (Stephan,
2011).
Surgery. The goals of breast cancer surgery are to remove the cancerous tissue
and to analyze it for type, grade, size, hormonal status, and possible metastasis (if the
cancer has spread). There are both diagnostic and therapeutic surgeries, as well as
reconstruction options.
Removal of a cancerous tumor by surgery cures one-third of all breast cancers
that are detected early. If only the lump and some surrounding breast tissue are
removed, leaving most of the breast intact, the procedure is called a partial
mastectomy, or lumpectomy. In a simple mastectomy, only the affected breast is
removed. When the breast and other tissues surrounding it are removed, the
operation is termed a radical mastectomy. Doctors have found that radical
mastectomies do not improve patient survival rates, and therefore are rarely worth the
significant changes that they impose on the female body. Many women choose to
have breast reconstruction surgery right after a mastectomy to restore the breasts
appearance (Microsoft Encarta Encyclopedia, 2007).
14
Radiation therapy. In some cases, doctors recommend radiation therapy in
addition to surgery to treat cancer that has not spread beyond the breast. Radiation
therapy uses high-energy rays or particles that destroy cancer cells that may remain in
the breast, chest wall, or underarm area after surgery (Microsoft Encarta
Encyclopedia, 2007). Cancer cells grow and divide much more quickly than healthy
cells, and their internal functions are not well organized. This makes them more
susceptible to damage from radiation treatment, and therefore less able to repair
themselves and recover. That is the reason that they are destroyed by the radiation
(Stephan, 2011).
Chemotherapy. A patient receives cancer-fighting drugs intravenously to
destroy breast cancer cells that have spread to other organs. Chemotherapy may be
given in addition to surgery to reduce the risk that breast cancer will recur. It also may
be used as the primary treatment for women with more advanced cases of breast
cancer. In these cases, high doses of chemotherapy kill cancer cells, but they also kill
stem cells, blood-producing cells in the bone marrow. Some women in advanced
stages of breast cancer may undergo chemotherapy followed by a bone-marrow
transplant to restore healthy stem cells, although it is not yet clear whether this
procedure helps prolong a womans survival (Microsoft Encarta Encyclopedia,
2007).
Cancer is uncontrolled cell growth, and chemotherapy targets rapidly diving cells
throughout your body. Chemotherapy is considered systemic therapy because, like
systemic
(metastatic)
cancer,
it
goes
everywhere
in
your
body's
systems.
Chemotherapy is used to kill cancer cells and prevent recurrence (Stephan, 2011).
Hormonal therapy. Hormonal therapy exploits some of the chemicals the body
naturally produces. For example, some breast cancer cells thrive on the hormone
estrogen, which is produced in the ovaries. Hormone therapy slows the growth of such
cells by preventing them from using estrogen. One of the drugs employed in endocrine
therapy is tamoxifen, which prevents breast cancer from recurring. It may also prevent
new cancers from forming in the other breast. Tamoxifens chemical cousin, raloxifene,
15
has shown similar results in preliminary studies. The most radical forms of hormone
therapy are the removal of the ovaries by surgery or the virtual destruction of the
ovaries by radiation treatments to prevent these organs from secreting estrogen
(Microsoft Encarta Encyclopedia, 2007).
Breast cancers are frequently dependent on estrogen for their growth. Antiestrogen hormone therapy starves tumor cells of the estrogen they need to grow,
resulting in cancer cell death. This type of therapy may be delivered before surgery, or
at the same time as radiation. You may need to take hormonal therapy for five years
after you're finished with primary treatment to prevent the cancer from coming back
(Stephan, 2011).
Targeted Biologic Therapies. These are drugs that can be added to
chemotherapy, to target specific cancer cells. Herceptin, Avastin, and Tykerb are all
approved for use as targeted therapies for breast cancer (Stephan, 2011).
Research into breast cancer treatment and prevention is ongoing. A number of
drugs are under investigation for treating breast cancer. One of the newest forms of
breast cancer treatments is a monoclonal antibody called trastuzumab, marketed
under the brand name Herceptin. This drug targets cells that overproduce HER-2, a
protein implicated in about one-third of all breast cancer cases ((Microsoft Encarta
Encyclopedia, 2007).
Stephan (2008), a breast cancer survivor, shares her thoughts and experiences
on the disease. According to her, a diagnosis of breast cancer is a great shock. Women
report that they fear breast cancer more than heart disease, even though they have a
better chance of surviving breast cancer, and dying of stroke or heart failure. Breast
cancer has been with us since the early Egyptians, and fear of this disease as well as
the treatments for it, seems to be inherent in women all across the world.
Some of the normal emotions a breast cancer patient experiences at diagnosis
are: fear, shock; denial; depression; sadness; anxiety; stress; guilt; loneliness,
(alienation); and hopelessness.
As the patient begins to deal with diagnosis and
treatment, the body will be reacting to emotions as well as surgery and drugs.
16
When the patients have accepted their diagnosis, they may be facing other
emotional concerns. The loss of a breast, or part of a breast, has an impact that goes
beyond the physical fact. If aggressive treatment is required, it might have long-term
impact on their health.
The patients can improve their emotional health and reduce their physical
symptoms with good coping strategies. A study published in the Journal of Psychosocial
Oncology reports that women who get help with pain and emotional distress have lower
levels of anxiety, fatigue and depression. Following are some ways to cope with
emotions: communicate with family and friends; maintain intimacy (if patient has a
partner); visit with a counselor or spiritual director; join a support group; express your
needs and ask for help; report symptoms to healthcare team; keep a log of medical
visits, save test results, keep receipts; educate yourself about your cancer and
treatments; exercise; and make plans for a crisis (http://breastcancer.about.com/od/diag
nosis/a/emotion s_coping.htmp).
Guided imagery is a technique that uses the breast patients mind and senses to
help her connect to her body, guiding her overall self into a relaxed and centered state
(Stephan, 2011). Breast cancer patients may use guided imagery for stress relief, pain
management, and to promote better sleep. An instructor, audio tape, or written script
helps guide her to focus her imagination and engage her senses (smell, sight, touch,
hearing, taste) to mentally re-create a safe, welcoming, restful place.
It may be a familiar place with positive memories, good fragrances, pleasant
views, or soothing sounds. She may move around within this safe place, in her mind,
becoming relaxed and feeling more in control. Her breathing can become regular and
slow, helping panic and stress subside. The benefits of guided imagery are relaxation,
lower blood pressure, lower stress levels and pain management. Guided imagery is
used in plenty of other situations, other than breast cancer treatment, such as in people
who need to lose weight, quit smoking, or achieve a goal (http://breastcancer.about.
com/od/lifeduring treatment/qt/guided_imagery.htm).
17
According to Carvalho and Stewart (2009), feeling tired is a common complaint.
But the fatigue that comes from breast cancer treatment is commonly described by
women as a tired feeling like one they have never before experienced. It is a chemical,
radiating tiredness that feels much different than anything patient may have felt before.
Fatigue varies for each individual, but it is safe to say that this is one of the major
complaints for those receiving radiation and chemotherapy treatments. It truly is a
tiredness that is felt at a much deeper level. It is a combination of being physically
drained of energy and emotionally and psychologically challenged with the everyday
reality of breast cancer treatments.
Balancing the breast cancer patients work life and her personal life becomes
more difficult in a world that already requires her to multitask in order to get through the
day. Now fatigue plays a major role. She has to slow down, prioritize, and perhaps give
up many of her day-to-day activities and responsibilities during her breast cancer
treatments. It is a temporary problem but offers many challenges to women of all ages.
In order to prioritize, she has to know what is important to her. There is no judgment
allowed, but only an identification of how to work with optimizing her time and balancing
her personal and work life, whether it is caring for her children or elderly parents, or her
volunteer commitments. Saying no to her usual activities takes practice and may be
difficult, but conserving energy will help her cope with the general loss of energy that
accompanies breast cancer treatment (http://www.netplaces.com/living-with-breast-can
cer/going-through-treatment/dealing-with-fatigue.htm).
As more is learned about lifestyle risk factors for breast cancer, there's one clear
downside: Patients who are diagnosed with the disease may blame themselves for not
having minimized such risk factors long ago (Lee-Frye, 2008). According to the
American Cancer Society (2008), lifestyle factors that increase a woman's risk for breast
cancer include having postmenopausal hormone therapy, also known as hormone
replacement therapy; consuming more than one alcoholic beverage per day; being
overweight, obese or too physically inactive; short-term or no breastfeeding; and not
having children or having had them later in life.
18
For example, in a 2007 issue of Stanford Medicine Magazine, journalist Amy
Adams (2008) discussed her increased risk of breast cancer due to having children later
in life. Adams implied that, should she be diagnosed with breast cancer, she might feel
responsible to some degree. Adams wrote, "... Where our breasts are concerned,
nothing can overcome all of those years spent in school, shunning motherhood in favor
of a bright illustrious future career."
Almost all patients who are newly diagnosed with cancer will run through a list of
could-haves and should-haves. But with regard to breast cancer, there are science,
social norms and sexuality to help create a lengthy list of places to point the finger. It
may be hard for women diagnosed with breast cancer to avoid asking, "Why did this
have to happen to me?" But it's best -- for them and their families -- to avoid getting
stuck in the blame game.
In a study presented at the 2007 conference of the American Psychosocial
Society (Romero, 2007), women were asked about breast cancer self-blame at an
average of 21 months post-diagnosis. Nearly 70% blamed themselves for not having
gotten sufficient exercise; 57% said they hadn't eaten proper foods; and more than 30%
focused on their decision to take oral contraceptives.
These modern lifestyle choices (Mayo Clinic Staff, 2008) are frequent areas of
recriminations among women diagnosed with breast cancer. According to a commentary
published in The New England Journal of Medicine by Porter (2008), "modernized"
lifestyles have increased breast cancer rates in industrialized countries.
While women most often seem to blame themselves for their cancer diagnosis,
there are other places to point the finger (Friedman, et al., 2008). The media has
reported that everything from environmental pollution to indoor lighting could be
contributing to the increase in breast cancer.
Families aren't immune to the breast cancer blame game. A mother's exposure
during pregnancy to the drug diethylstilbestrol, or DES, used during the 1950s and 60s,
is known to increase a daughter's breast cancer risk. And some women may even feel
19
angry with their parents for passing down a genetic risk factor for the disease. Others
may blame a spouse for encouraging them to wait to have kids.
Although there are no exact figures, some women also blame God or some
higher power for their cancer diagnosis. But, more commonly, women seek solace in
religion. According to one study, women who mention religion in their online support
group postings (Shaw et al., 2008) seem to express more positive emotions, a higher
level of engagement in their health care and a greater sense of well-being.
Although temporarily assigning blame is a normal and even healthy way to cope
with a breast cancer diagnosis, studies show that women who blame themselves report
poorer quality of life during and after their cancer experience than those who avoid
protracted self-blame. Assigning blame can also impact familial relationships, especially
if there's a genetic history of breast cancer. Male relatives who carry the breast cancer
mutation may feel particularly guilty, at least according to one study of men who tested
positive for the mutation. Opening the lines of communication about this issue can be
helpful for family members, whether male or female. In addition, seeking genetic
counseling can help families with a strong history of breast cancer learn more about
their risks.
According to the Duffy et al. (2008) of University of Michigan Comprehensive
Cancer Center, placing blame is a common behavior among people with any type of
cancer. But it's an avoidance behavior. It can limit an individual's ability to move on and
take action to deal with the diagnosis, emotionally and medically.
It's important not to feel guilty for blaming someone or something. Wanting to
hold someone (even if it's you) accountable is understandable. But it's not a place to
stop or get stuck. Blame can be a barrier to supportive familial relationships and to a
healthy attitude regarding breast cancer treatment. Women who feel that their lifestyle
choices may be responsible for their cancer should remember that we don't fully
understand the factors involved -- particularly in the case of the individual woman.
There's no foolproof way to move from population-based risk factor data -- a business of
statistics and averages -- to the case of unique individuals. While it makes sense to do
20
what we can with what we know, it's important to recognize that our knowledge of risk
and cause is fragmentary. And the biggest risk factor -- age -- is something none of us
can control. According to New York's Cedars-Sinai Health System (2008), "Over 70% of
breast cancers occur in women who have no identifiable risk factor other than age." But
there's been relatively little study of the impact of increased life expectancy on breast
cancer rates.
Several studies suggest that oncologists should talk with their patients about
blame issues. If your doctor doesn't bring up this topic, don't hesitate to ask questions
about what might be responsible for a breast cancer diagnosis. If thoughts about blame
become intrusive or seem to be interfering with a positive attitude about treatment,
mention this to a physician or a counselor who can provide additional coping
mechanisms. Communication with family and friends is also important. The American
Cancer Society encourages newly diagnosed patients to share their regrets and
concerns with loved ones, and for patients to allow their loved ones to do the same. In
addition, patients may find it helpful to join a support group whether online or in person.
These groups can allow women with breast cancer to talk about blame in a safe
environment.
Foreign Studies
The aim of Goodwin, Zhang and Ostirs (2004P) study is to assess the effect of a
prior diagnosis of depression on the diagnosis, treatment, and survival of older women
with breast cancer. Retrospective analysis of records from Surveillance, Epidemiology
and End Results (SEER) and Medicare claims. A total of 24,696 women aged 67 to 90
diagnosed with breast cancer between 1993 and 1996 and included in the SEER
Medicare linked database were studied.
A total of 1,841 of the 24,696 women (7.5%) had been given a diagnosis of
depression sometime in the 2 years before the diagnosis of breast cancer. There was
no difference in tumor size or stage at diagnosis between depressed and nondepressed
women. Women diagnosed with depression were less likely to receive treatment
21
generally considered definitive (59.7% vs 66.2%, P<.0001), and this difference
remained after controlling for age, ethnicity, comorbidity, and SEER site.
Also, women with a prior diagnosis of depression had a higher risk of death
(hazard ratio=1.42; 95% confidence interval= 1.13-1.79) after controlling for other
factors that might affect survival. The higher risk of death associated with a prior
diagnosis of depression was also seen in analyses restricted to women who received
definitive treatment. Women with a recent diagnosis of depression are at greater risk for
receiving non-definitive treatment and experience worse survival after a diagnosis of
breast cancer, but differences in treatment do not explain the worse survival.
Another study (Reddick et al., 2005) examined the influence of coping with pain
on depression, anxiety, and fatigue among women with breast cancer. The study
theorized that breast cancer treatment can have a profound influence on a woman's
physical, psychological, social, and spiritual well-being. Anxiety, depression, anger,
fatigue, and fear of recurrence are common responses to a diagnosis of breast cancer
and undergoing breast cancer treatment. Women develop their own coping strategies
for the pain and other effects of treatment. However, it is unclear whether there is a
relationship between adaptation to pain and psychological distress during breast cancer
treatment.
Findings from the present study reveal that breast cancer patients who have
better pain coping strategies also have lower levels of anxiety, fatigue and depression.
These results suggest that pain coping interventions may reduce fatigue and
psychological distress among women with breast cancer.
A 2006 study, conducted by researchers at Dartmouth Medical School, as cited
by Tremblay (2009), found that nearly half of the 236 newly diagnosed breast cancer
patients in the study experienced emotional symptoms and distress that were clinically
significant. This means that these patients, rather than having a passing case of the
blues, meet established screening criteria for severe emotional distress or psychiatric
disorders.
22
Some of the conditions that a breast cancer patient may experience include:
severe emotional distress; major depression; post-traumatic stress disorder (PTSD);
and generalized anxiety disorder (GAD).
Stppler (2011) cited a study presented at the Fourth AACR Conference on the
Science of Cancer Health Disparities in September 2011 which revealed an association
between psychological stress and one of the most aggressive types of breast cancer.
The study was performed on 989 women with breast cancer. Two to three
months after diagnosis, the women were asked to rate their degree of anxiety, fear, and
isolation. These self-reported stress scores were higher for black and Hispanic women
than in white women. Further, those women who reported having higher levels of stress
tended to have more aggressive tumors (defined as being negative for the presence of
estrogen receptors, meaning that therapies designed to block the effects of estrogen will
not be effective) than those with lower stress levels. The association between stress
level and aggressive tumors was strongest in black and Hispanic women.
To clarify whether stress levels influence a tumor's aggressiveness, it would be
necessary to interview women about their psychosocial stressors prior to their
developing cancer, ideally over a period of years. Since most women do not develop
breast cancer, a very large population of women would need to be interviewed, perhaps
yearly, about their psychological stress levels (American Association for Cancer
Research [AACR], 2011).
These women could be followed over a period of years, and those who develop
breast cancer could be further studied to determine if high psychologically stressed
women developed the most aggressive breast cancer types. Currently, there is no good
data that psychological stress is a cause of the most aggressive types of breast cancer
(http://www.medicinenet.com/ script/main/art.asp?articlekey=149787).
Local Literature
The 1998 Philippine Cancer Facts and Estimates revealed that the breast is the
number one cancer site among Filipino women. The 1998 estimates showed that about
23
26 for every 100,000 Filipino women are at risk of having breast cancer. Breast cancer
is the most common cancer disease and the leading cause of cancer deaths among
Filipino women in the country today. The same document showed that in 1998 about
9,325 Filipino women were diagnosed of breast cancer and about 3,057 have
succumbed to death because of it (National Statistical Coordination Board Fact Sheet
(2002).
According to Buban (2001), breast cancer becomes a survivable disease where
women have access to education about their own health and where there is more
effective detection and treatment programs. Even though the world is waking up to the
realization that cases of breast cancer are steadily increasing (worldwide rates have
increased by 26 percent since 1980), mortality rates in some countries are declining. In
fact, the countries with the highest number of new cases annually have seen significant
declines in mortality rates, according to a study conducted at the Roswell Park Cancer
Institute in the 1990s. These are the United States, the United Kingdom and Canada.
Sadly, this trend in mortality is not evident in the Philippines which in 1998 still
ranks ninth in the world and first in Asia with 9,000 cases. But this figure was clearly
way off the mark and with no new data, we can just infer how many Filipino women
today have this disease, reports Dr. Diana Cua, a breast surgeon and oncologist at the
Makati Medical Center.
Despite the growing number of Filipino women developing this disease, Dr. Cua
laments that a lot of them are not undergoing mammography screening which they
should take once a year. One factor is the cost of examination and another is the
availability. The facilities are offered mostly by private hospitals and the process is
considered painful by many patients, observes Dr. Cua.
Lagman-Dy (2001) reports that breast cancer is the most common cancer in
pregnant and postpartum women with a three percent incidence rate. The natural
engorgement during pregnancy and lactation may hinder detection of discreet masses
and early detection of breast cancer. Delays in diagnosis are common, with an average
reported delay of 5 to 15 months from the onset of symptoms. Because of these delay,
24
cancers are typically detected at a later stage than in a non-pregnant, age-matched
population.
To detect breast cancer, pregnant and lactating women should practice selfexamination and undergo a breast examination as part of the routine prenatal
examination. If an abnormality is suspected, diagnostic approaches such as breast
ultrasound and mammography may be used. With proper shielding, mammography
poses little risk of radiation exposure to the fetus. Since about 25 percent of
mammograms in pregnancy may be negative in the presence of cancer, a biopsy is
essential for the diagnosis of any palpable mass. Diagnosis may be safely
accomplished with a fine-needle aspiration or excisional biopsy under local anesthesia.
Biopsy and mastectomy can be well tolerated by mother and fetus with only a
one percent risk of spontaneous abortion following general anesthesia. Chemotherapy
has not been shown to cause congenital malformation when given after the first
trimester, but may be associated with premature labor and fetal wastage. In a study
involving 163 patients given chemotherapy in the first semester, there were 19 cases of
fetal malformations (10.4 percent). Data on the immediate and long-term effects of
chemotherapy on the fetus are limited. Radiation therapy, if indicated, should be
withheld until after delivery since it may be harmful to the fetus at any stage of
development.
Local Studies
The study of Cope (2004) aimed to analyze the cultural beliefs and health
practices of women with breast cancer. The study was conducted on six breast cancer
patients. The findings of the study were: the 6 patients believed in 5 of 16 cultural
beliefs regarding diagnosis; 4 out of 11 cultural beliefs on treatment; 5 out of 12 cultural
beliefs on nursing care; 5 out of 8 cultural beliefs on survival; and 6 out of 13 cultural
beliefs on spirituality.
The study concluded that: 1) the breast cancer patients have no personal history
of previous serious disease and family health history is not conclusive for cancer; 2) the
25
cancer patients have practiced a healthy lifestyle; 3) the cancer patients have had
immovable painless lump on the right breast the size of which is consistent with Stage II
and Stage III cancer of the breast; and 4) the cultural beliefs practiced by the patients
are few with regards to diagnosis, treatment nursing care, survival and spirituality.
Identifying the stressors, coping strategies, and reflections of female breast
cancer survivors from the time of diagnosis up to treatment was the goal of Rufino et
al.s (2004) study. The researchers interviewed nine women who have undergone
mastectomy and treatment. A descriptive research design was used, in addition a semistructured questionnaire for in-depth interview was utilized to cover the variables.
After the data had been gathered, the researchers identified the themes from the
data as follows: the respondents seem to be somewhat confused or rather unsure of
what their illness really is; most of the respondents are religious; all had a support
network of family and friends; all had a practical approach to their illness; all found time
for recreation; all of them see breasts as mere appendage only; all of them were afraid
how their body will react to the medication; because of the side-effects, they couldn't do
the things that they used to do; most of the respondents feel that there was a change in
the way they communicated; most respondents are worriers, and all of them saw a
benefit from their illness.
In her study, Santos (2001) aimed to describe the emotions and concerns of
Filipino middle-aged female breast cancer patients. It focused on their initial reaction,
their emotions months/years after their diagnosis, their present concerns and reported
reasons for experiencing such. Eleven breast cancer patients were interviewed with the
use of an interview guide. Data gathered were then analyzed qualitatively. From this,
patterns and themes were produced.
Results showed that initial reactions experienced by breast cancer patients were
generally the same. These emotions differed only after a certain lapse of time. The
differences were due to the respondents' perception and outlook toward cancer.
Emotions such as shock, depression, anxiety, fear, guilt, denial, anger, acceptance, and
hope were exhibited. Concerns regarding their loved ones, role as a mother, financial
26
stability, health, recurrence, midlife, discrimination, and physical appearance emerged.
However, these concerns varied due to their age, ages of their children, and their socioeconomic status.
The exploratory study of Gomez (2000) examines what social support women
diagnosed with breast cancer need and what they actually receive from the
perspectives of the women themselves (n=30), their family caregivers (n=20) and
medical healthcare providers (n=5).
The results of the study generated similar taxonomies of social support from
viewpoints of the women and their family caregivers. The types of social support
needed by women diagnosed with breast cancer are emotional, spiritual, financial,
physical, informational and political support. The interviews with medical healthcare
providers came up with four (4) categories of support: emotional, financial, physical and
informational.
Data further revealed that the women generally receive what social support the
respondents perceive women with breast cancer should have. The main source of
support is the family. However, families are not expected to provide informational and
political support. The former is primarily sought from the doctor, while the latter, from
high-ranking officials. Among married breast cancer patients, the husband is considered
the most supportive. For the single and widowed women, the siblings and the children
were chosen, respectively. Other people who compose the social network providing
support to the diagnosed women are her relatives, employer and co-workers, neighbors,
and religious group.
Synthesis
The foregoing literature and studies presented an overall picture of breast cancer
and its treatments. As well, they discussed the effects of the disease and therapy
thereof involving social and emotional aspects.
A review of the studies cited reveal that there are similarities with and differences
from the current study. The study at hand deals with the socio-economic effects of
27
breast cancer and its treatments as well the adaptation strategies employed by the
respondents to cope with these effects. The locale of the study is Cavite province,
particularly in selected hospitals, to wit: Bautista Hospital, Cavite Medical Center, Divine
Grace Hospital, DLSU Medical Center, and Gen. Emilio Aguinaldo Memorial Hospital. A
total of 25 breast cancer patients or 5 each hospital will participate in the study.
Compared to the study of Cope (2004), the latters aim was to analyze the
cultural beliefs and health practices of women with breast cancer. The study was
conducted on six breast cancer patients. On the other hand, the study of Rufino et al.
(2004) identified the stressors, coping strategies and reflections of female breast cancer
survivors from the time of diagnosis up to treatment. The researchers interviewed nine
women who have undergone mastectomy and treatment.
In the study of Santos (2001), eleven Filipino middle-aged breast cancer patients
were interviewed to describe their emotions and concerns focusing on their initial
reaction, their emotions months/years after their diagnosis, their present concerns and
reported reasons for experiencing such.
Finally, the exploratory study of Gomez (2000) examined what social support
women diagnosed with breast cancer need and what they actually receive from the
perspectives of the women themselves (n=30), their family caregivers (n=20) and
medical healthcare providers (n=5).
Anda mungkin juga menyukai
- Hormone Therapy: Current Drugs for Treating Breast Cancer – What You Must KnowDari EverandHormone Therapy: Current Drugs for Treating Breast Cancer – What You Must KnowPenilaian: 5 dari 5 bintang5/5 (1)
- Breast Cancer: A Comprehensive Resource for Women and FamiliesDari EverandBreast Cancer: A Comprehensive Resource for Women and FamiliesBelum ada peringkat
- Bukidnon State UniversityDokumen106 halamanBukidnon State UniversityfLOR_ZIANE_MAEBelum ada peringkat
- Breast Cancer: The BasicsDokumen5 halamanBreast Cancer: The BasicsJamie CabreraBelum ada peringkat
- Re As DingsDokumen4 halamanRe As DingsMei-mei ZhuangBelum ada peringkat
- Breast Cancer FinalDokumen68 halamanBreast Cancer Finalapi-400333454Belum ada peringkat
- Pathophysiology Breast CancerDokumen3 halamanPathophysiology Breast CancerNathalie kate petallarBelum ada peringkat
- Endometrial Cancer: A Comprehensive Resource for Patients and FamiliesDari EverandEndometrial Cancer: A Comprehensive Resource for Patients and FamiliesBelum ada peringkat
- Breast CancerDokumen29 halamanBreast CancerSherly CanceritaBelum ada peringkat
- Anti-cancer Living: Women’s Must-Have Guide on Reducing Cancer Risk and Surviving Breast CancerDari EverandAnti-cancer Living: Women’s Must-Have Guide on Reducing Cancer Risk and Surviving Breast CancerBelum ada peringkat
- Reading Passage 'Breast Cancer'Dokumen2 halamanReading Passage 'Breast Cancer'DheyaKarina100% (1)
- Fast Facts On Breast CancerDokumen8 halamanFast Facts On Breast CancerTety KarmilaBelum ada peringkat
- Breast CancerDokumen8 halamanBreast CancerJeyser T. Gamutia100% (1)
- Breast Cancer (Reaction Paper)Dokumen2 halamanBreast Cancer (Reaction Paper)Maria Angela Del GallegoBelum ada peringkat
- Twelve Major Cancers: Fact SheetDokumen7 halamanTwelve Major Cancers: Fact SheetSCRUPEUSSBelum ada peringkat
- Breast CancerDokumen3 halamanBreast Cancerjames garciaBelum ada peringkat
- WOMEN'S HEALTH 2019with VIDEODokumen73 halamanWOMEN'S HEALTH 2019with VIDEOAurora Doris BatagaBelum ada peringkat
- CopyofovariancancerpaperDokumen7 halamanCopyofovariancancerpaperapi-310316770Belum ada peringkat
- Breast CancerDokumen10 halamanBreast CancerMaha RaniBelum ada peringkat
- Breast CancerDokumen11 halamanBreast CancerRock'nRoll Buddies100% (2)
- Vdocuments - MX Biology Investigatory Project Class Xii Breast CancerDokumen14 halamanVdocuments - MX Biology Investigatory Project Class Xii Breast CancerPooja TikaniaBelum ada peringkat
- Ca MamaeDokumen7 halamanCa MamaeKevin RadittyaBelum ada peringkat
- Breast Cancer Medical Surgical NursingDokumen5 halamanBreast Cancer Medical Surgical NursingKath RubioBelum ada peringkat
- Chapter One: 1.1 BackgroundDokumen74 halamanChapter One: 1.1 Backgroundcadnaan144Belum ada peringkat
- 1.page de Garde 2Dokumen8 halaman1.page de Garde 2Lu SuznBelum ada peringkat
- Breast Cancer - StatPearls - NCBI BookshelfDokumen10 halamanBreast Cancer - StatPearls - NCBI BookshelfCARDIO 2019Belum ada peringkat
- Review ArticleDokumen24 halamanReview ArticleGeetika PremanBelum ada peringkat
- Understanding Lumpectomy: A Treatment Guide for Breast CancerDari EverandUnderstanding Lumpectomy: A Treatment Guide for Breast CancerBelum ada peringkat
- Album de InglesDokumen8 halamanAlbum de Ingles夢於נмᷓBelum ada peringkat
- Cherry Kraft Invasive Ductal Carcinoma Case PresentationDokumen7 halamanCherry Kraft Invasive Ductal Carcinoma Case Presentationapi-279084200Belum ada peringkat
- Breast CancerDokumen7 halamanBreast CancerDeepankar Srigyan100% (1)
- Jonathan Bland Pathophysiology Professor Lori Mcgowan: 1 Running Header: Cervical, Ovarian, and Uterine CancerDokumen4 halamanJonathan Bland Pathophysiology Professor Lori Mcgowan: 1 Running Header: Cervical, Ovarian, and Uterine CancerjonBelum ada peringkat
- American Cancer SocietyDokumen40 halamanAmerican Cancer Societybrunna_pultzBelum ada peringkat
- Breast CancerDokumen5 halamanBreast Cancerbobtaguba100% (1)
- Introduction To Breast CancerDokumen4 halamanIntroduction To Breast CancerEzzati AizaBelum ada peringkat
- Breast Cancer: Practice EssentialsDokumen11 halamanBreast Cancer: Practice EssentialsRayhanun MardhatillahBelum ada peringkat
- Breast CancerDokumen27 halamanBreast Cancerrikshya k c100% (3)
- Lesson Plan: Breast Cancer and Environment: ObjectivesDokumen8 halamanLesson Plan: Breast Cancer and Environment: ObjectivesMara KathrinaBelum ada peringkat
- What Is Breast CancerDokumen20 halamanWhat Is Breast CancerKesyaBelum ada peringkat
- Breast Disease: Diagnosis and Pathology, Volume 1Dari EverandBreast Disease: Diagnosis and Pathology, Volume 1Adnan AydinerBelum ada peringkat
- Ijpt 309Dokumen10 halamanIjpt 309Earthjournal PublisherBelum ada peringkat
- Breast Cancer: Estrogen Estrogen Estrogen EstrogenDokumen13 halamanBreast Cancer: Estrogen Estrogen Estrogen EstrogenMarde Cabucos Phillip BonachitaBelum ada peringkat
- Breast CancerDokumen15 halamanBreast CancerDwiKamaswariBelum ada peringkat
- Breast Cancer Prevention: Steps to Protect Your Health: Course, #5Dari EverandBreast Cancer Prevention: Steps to Protect Your Health: Course, #5Belum ada peringkat
- Inflammatory Breast CancerDokumen6 halamanInflammatory Breast CancerHafsa ShafiqueBelum ada peringkat
- Breast Cancer (Research Paper)Dokumen12 halamanBreast Cancer (Research Paper)Katrina Arnaiz100% (3)
- Medication and Lifestyle May Lower Breast Cancer Risk: by Jane E. BrodyDokumen3 halamanMedication and Lifestyle May Lower Breast Cancer Risk: by Jane E. BrodySabirBelum ada peringkat
- Pharmacotherapy of Oncologic DisordersDokumen31 halamanPharmacotherapy of Oncologic DisordersWeliam Jhay Coyme100% (1)
- Ung Thư VúDokumen16 halamanUng Thư VúVăn LêBelum ada peringkat
- Multifactorial DiseaseDokumen17 halamanMultifactorial Diseasepratibha mishraBelum ada peringkat
- TB During Pregnancy: Midwifery Study Program Karawang Bandung Health Polytechnic 2017Dokumen16 halamanTB During Pregnancy: Midwifery Study Program Karawang Bandung Health Polytechnic 2017Fontanella DwiputriBelum ada peringkat
- Breast Cancer2Dokumen16 halamanBreast Cancer2hasan100% (1)
- Course Work EssayDokumen12 halamanCourse Work EssayKanza NajamBelum ada peringkat
- Revisión Cáncer de MamaDokumen19 halamanRevisión Cáncer de MamaCAROLINA CHUMACERO BERMEOBelum ada peringkat
- Screening Mammograms: Questions and Answers: Key PointsDokumen9 halamanScreening Mammograms: Questions and Answers: Key PointsInternational Business TimesBelum ada peringkat
- Breast Cancer Term PaperDokumen86 halamanBreast Cancer Term Papersusy mary thomasBelum ada peringkat
- Breast Cancer - DZMEDokumen6 halamanBreast Cancer - DZMEMarife CompraBelum ada peringkat
- Common Cancer and Risk Factors AssignmentDokumen18 halamanCommon Cancer and Risk Factors AssignmentAzharBelum ada peringkat
- Kanker PayudaraDokumen11 halamanKanker PayudaracahyaaBelum ada peringkat
- One Sentence Strategy PDFDokumen1 halamanOne Sentence Strategy PDFroxannefourteenBelum ada peringkat
- 2016-2017 Wedding PackageDokumen7 halaman2016-2017 Wedding PackageroxannefourteenBelum ada peringkat
- Pte Prep Tips-Compiled From Expat ThreadsDokumen12 halamanPte Prep Tips-Compiled From Expat ThreadsDARSHANBelum ada peringkat
- Wedding Budget ChecklistDokumen2 halamanWedding Budget ChecklistroxannefourteenBelum ada peringkat
- Chapter I - Thesis Breast CancerDokumen6 halamanChapter I - Thesis Breast CancerroxannefourteenBelum ada peringkat
- Chapter III - Thesis Breast CancerDokumen5 halamanChapter III - Thesis Breast CancerroxannefourteenBelum ada peringkat
- Comprehensive Nclex Exam Answer KeyDokumen12 halamanComprehensive Nclex Exam Answer KeyAmy93% (15)
- 50 Item Gastrointestinal Health Problems Test Drill KeysDokumen14 halaman50 Item Gastrointestinal Health Problems Test Drill KeysmervilynBelum ada peringkat
- Chapter IV - Thesis Breast CancerDokumen13 halamanChapter IV - Thesis Breast CancerroxannefourteenBelum ada peringkat
- NCLEX-RN Gastrointestinal Health Problems Test DrillDokumen9 halamanNCLEX-RN Gastrointestinal Health Problems Test DrillAko Si PisangBelum ada peringkat
- 40 Items Comprehensive NCLEX ReviewDokumen9 halaman40 Items Comprehensive NCLEX ReviewChristina CollinsBelum ada peringkat
- Colorectal CancerDokumen69 halamanColorectal Cancerroxannefourteen100% (1)
- Staff Data FormDokumen2 halamanStaff Data Formroxannefourteen67% (3)
- Letter of AuthorizationDokumen1 halamanLetter of AuthorizationAngelito Motas PobleteBelum ada peringkat
- Brain CancerDokumen33 halamanBrain Cancermynoidanh19Belum ada peringkat
- Delcaration Form by The Sponsoring FacilityDokumen1 halamanDelcaration Form by The Sponsoring FacilityDr-Usman Khan100% (1)
- Applicant Declaration FormDokumen1 halamanApplicant Declaration FormroxannefourteenBelum ada peringkat
- Cryptosporidiosis in Ruminants: Update and Current Therapeutic ApproachesDokumen8 halamanCryptosporidiosis in Ruminants: Update and Current Therapeutic ApproachesDrivailaBelum ada peringkat
- Turkey Book 03 Internal Medicine PDFDokumen47 halamanTurkey Book 03 Internal Medicine PDFPreaisBelum ada peringkat
- Anti Diare SGDokumen17 halamanAnti Diare SGludoy03Belum ada peringkat
- Managing Tumor Lysis Syndrome.2Dokumen4 halamanManaging Tumor Lysis Syndrome.2Caballero X CaballeroBelum ada peringkat
- Ready Reckoner For Class Room 08-01-2020Dokumen70 halamanReady Reckoner For Class Room 08-01-2020yoBelum ada peringkat
- Temporal Bone Radiology ReadyDokumen136 halamanTemporal Bone Radiology Readyadel madanyBelum ada peringkat
- Pertussis - Not Just For Kids: Clinical PracticeDokumen8 halamanPertussis - Not Just For Kids: Clinical PracticeMihaela-Alexandra PopBelum ada peringkat
- Sas 39Dokumen2 halamanSas 39Sistine Rose LabajoBelum ada peringkat
- Hospital Infections PDFDokumen794 halamanHospital Infections PDFJOSEPH APPIAHBelum ada peringkat
- Sodium Bicarbonate: PresentationDokumen3 halamanSodium Bicarbonate: Presentationmadimadi11Belum ada peringkat
- Presidential Theme: 66 (LXVI) Annual Conference of Indian Orthopaedic AssociationDokumen17 halamanPresidential Theme: 66 (LXVI) Annual Conference of Indian Orthopaedic AssociationnipundaveBelum ada peringkat
- Microbiology: Pathogenic Gram-Positive Cocci (Streptococcus)Dokumen26 halamanMicrobiology: Pathogenic Gram-Positive Cocci (Streptococcus)Shuler0071Belum ada peringkat
- YS Curodont Sell Sheet - 8.5x11 - FINAL 1Dokumen1 halamanYS Curodont Sell Sheet - 8.5x11 - FINAL 1lucian hahaianuBelum ada peringkat
- 2) Megaloblastic AnemiaDokumen17 halaman2) Megaloblastic AnemiaAndrea Aprilia100% (1)
- Finish LineDokumen3 halamanFinish LineSgBelum ada peringkat
- 4.1 Fixator Extern Circular IlizarovDokumen10 halaman4.1 Fixator Extern Circular IlizarovTudorica AdrianBelum ada peringkat
- Canine Influenza FactsDokumen5 halamanCanine Influenza FactsWIS Digital News StaffBelum ada peringkat
- Perineal Techniques During The Second Stage of Labour For Reducing Perineal Trauma (Review)Dokumen118 halamanPerineal Techniques During The Second Stage of Labour For Reducing Perineal Trauma (Review)Ppds ObgynBelum ada peringkat
- Chapter 2Dokumen4 halamanChapter 2Lawrence LuceñoBelum ada peringkat
- An Essay On The End-Of-Life Care in ChildrenDokumen4 halamanAn Essay On The End-Of-Life Care in ChildrenThinashe MaswahuBelum ada peringkat
- Ptj/pzaa 200Dokumen39 halamanPtj/pzaa 200Yenie YenBelum ada peringkat
- Dental Management of The Patient With HIVAIDS 2002Dokumen6 halamanDental Management of The Patient With HIVAIDS 2002drkameshBelum ada peringkat
- Pedia ADCONDokumen24 halamanPedia ADCONRaul MangrobangBelum ada peringkat
- Prof Norhayati RMC KPJUCDokumen18 halamanProf Norhayati RMC KPJUCtheskywlkrBelum ada peringkat
- Dade InnovinDokumen7 halamanDade InnovinchaiBelum ada peringkat
- 09 ITLS PretestDokumen6 halaman09 ITLS PretestArlanosaurus100% (2)
- Abiraterone Acetate Plus Prednisone Versus Placebo Abiratetone LancetDokumen9 halamanAbiraterone Acetate Plus Prednisone Versus Placebo Abiratetone LancetMahesh TamhaneBelum ada peringkat
- Abtahi 2020Dokumen9 halamanAbtahi 2020Rati Ramayani AbidinBelum ada peringkat
- 2021 Va Ers DataDokumen1.788 halaman2021 Va Ers DataasdasdasdBelum ada peringkat
- Clinical EnzymologyDokumen23 halamanClinical EnzymologyKishore KaranBelum ada peringkat