Placenta Previa (Clinical Features, Diagnosis, and Course)
Diunggah oleh
Muhammad AzwanJudul Asli
Hak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Placenta Previa (Clinical Features, Diagnosis, and Course)
Diunggah oleh
Muhammad AzwanHak Cipta:
Format Tersedia
Placenta previa (Clinical features, diagnosis, and course)
INTRODUCTION
1. Placenta previa refers to presence of placental tissue that extends over or
lies proximate to internal cervical os. Sequelae include potential for severe
bleeding and preterm birth, as well as the need for cesarean delivery.
2. Placenta previa should be suspected in any woman beyond 20 weeks of
gestation who presents with painless vaginal bleeding. For women who
have not had 2nd trimester ultrasound examination, antepartum bleeding
after 20 weeks of gestation should prompt sonographic determination of
placental location before digital vaginal examination is performed because
palpation of placenta can cause severe hemorrhage.
PREVALENCE AND RISK FACTORS
1. In systematic review including 58 observational studies of placenta previa,
prevalence ranged from 3.5 to 4.6 per 1000 births. The prevalence is
several-fold higher early in gestation, but most of these cases resolve
before delivery.
2. Purported risk factors, some of which are interdependent.
A. Previous placenta previa
B. Previous cesarean delivery
C. Multiple gestation
D. Multiparity
E. Advanced maternal age
F. Infertility treatment
G. Previous abortion
H. Previous intrauterine surgical procedure
I. Maternal smoking
J. Maternal cocaine use
K. Male fetus
L. Non-white race
3. There is paucity of data regarding the prevalence of placenta previa in twin
pregnancies. In a retrospective study of natural history of placenta previa in
twins, the prevalence of placenta previa in twins was similar to that in
singleton pregnancies. However, dichorionic twins had statistically
increased risk of placenta previa compared with monochorionic twins (OR
3.3) or singleton gestations (OR 1.5).
PATHOGENESIS
1. The pathogenesis of placenta previa is unknown. One hypothesis is
that presence of areas of suboptimal endometrium in upper uterine cavity
due to previous surgery or pregnancies promotes implantation of
trophoblast in, or unidirectional growth of trophoblast toward, the lower
uterine cavity. Another hypothesis is that particularly large placental
surface area, as in multiple gestations or in response to reduced
uteroplacental perfusion, increases likelihood that the placenta will cover or
encroach upon cervical os.
PATHOPHYSIOLOGY
1. Placental bleeding is thought to occur when gradual changes in cervix and
lower uterine segment apply shearing forces to inelastic placental
attachment site, resulting in partial detachment. Vaginal examination or
coitus can also disrupt intervillous space and cause bleeding. Bleeding is
primarily maternal, but fetal bleeding can occur if fetal vessel is disrupted.
CLINICAL FEATURES
1.
Ultrasound presentation and course
A. 1 to 6% of pregnant women display sonographic evidence of placenta
previa between 10 and 20 weeks of gestation when they undergo
obstetrical ultrasound for assessment of gestational age, fetal anatomic
survey, or prenatal diagnosis. The majority of these women are
asymptomatic and 90% of these early cases resolve. Two theories have
been put forth to account for resolution of previa.
i.
The lower uterine segment lengthens from 0.5 cm at 20 weeks of
gestation to > 5 cm at term. Development of lower uterine
segment relocates stationary lower edge of placenta away from
internal os.
ii.
Progressive unidirectional growth of trophoblastic tissue toward
fundus within relatively stationary uterus results in upward
migration of placenta. This phenomenon has been termed
trophotropism.
B. Placental atrophy may explain why portion of placenta that
sonographically appeared to cover cervix resolves.
C. The later in gestation the previa persists, the more likely it will
be present at delivery. In one series of 714 placenta previa in
singleton gestations with liveborn infant 25 weeks of gestation,
previa was present at delivery in 12% of those identified at 15 to 19
weeks, 34% of those identified at 20 to 23 weeks, 49% of those
identified at 24 to 27 weeks, 62% of those identified at 28 to 31 weeks,
and 73% of those identified at 32 to 35 weeks. The likelihood of
resolution by the time of delivery is also high in twin gestations, and
also dependent on gestational age of diagnosis. If previa persists with
advancing gestational age, it is less likely to resolve.
D. The distance the placenta extends over internal cervical os is
the best predictor of placenta previa at delivery. However,
available data correlating gestational age, millimeters of extension over
cervical os, and outcome are insufficient to make precise predictions.
Based on available data, at 18 to 23 weeks of gestation, distance of at
least 14 to 15 mm appears to be associated with 20% risk of placenta
previa at delivery, and when distance is at least 25 mm, 40 to 100% of
previas will be present at delivery. In the 3rd trimester, distance over 20
mm is highly predictive of persistence. An anterior placenta previa
appears to resolve more often and more quickly than posterior placenta
previa.
2.
Bleeding
A. In 2nd half of pregnancy, the characteristic clinical presentation is
painless vaginal bleeding, which occurs in 70 to 80% of cases. An
additional 10 to 20% of women present with both uterine contractions
and bleeding, which is similar to presentation of abruptio placenta.
B. In approximately 33% of affected pregnancies, initial bleeding episode
occurs prior to 30 weeks of gestation; this group is more likely to
require blood transfusions and is at greater risk of preterm delivery and
perinatal mortality than women whose bleeding begins later in
gestation. An additional 33% of patients become symptomatic between
30 and 36 weeks, while most of the remaining patients have their first
bleed after 36 weeks. About 10% of women reach term without
3.
bleeding.
C. For individual patient, it is not possible to predict whether bleed will
occur, nor gestational age, volume, or frequency of bleeding. Authors
have reported that placentas that cover os bleed earlier and more than
placentas that are proximate to os, placentas near os have greater risk
of bleeding if placental edge is thick (> 1 cm), and identification of
echo-free space in placental edge covering internal os or cervical
length 3 cm are predictive of hemorrhage. Although the magnitude
of risk may differ according to previa characteristics, all patients with
placentas covering or in close proximity to cervical os are at risk of
significant antepartum, intrapartum, and postpartum bleeding. Further
study of patient-specific risk factors for bleeding is needed.
Associated conditions
A. Placenta previa has been associated with increased risk of several
other pregnancy complications. The most serious and best supported of
these complications is placenta accreta.
B. Placenta accreta
i.
Placenta accreta complicates 1 to 5% of pregnancies with placenta
previa and unscarred uterus. The presence of placenta previa and
one or more cesarean delivery scars places woman at very high
risk for placenta accreta and need for cesarean hysterectomy: one
previous cesarean birth (11 to 25%), two previous cesarean births
(35 to 47%), three previous cesarean births (40%), and 4
previous cesarean births (50 to 67%).
ii.
In one large series, composite maternal morbidity in women with
placenta previa and 0, 1, 2, or 3 prior cesarean deliveries was 15,
23, 59, and 83%, and almost all of excess composite maternal
morbidity in women with prior cesarean was related to
complications associated with placenta accreta.
C. Preterm labor and rupture of membranes
i.
Antepartum bleeding from any cause is risk factor for preterm labor
and PROM.
D. Malpresentation
i.
The large volume of placenta in lower portion of uterine cavity
predisposes fetus to assume non-cephalic presentation. Noncephalic presentation at delivery is also related to increased risk of
delivery before term, when non-cephalic presentations are more
common.
E. Intrauterine growth restriction
i.
An increased risk of IUGR has been reported by several, but not all,
investigators, and remains controversial. If reduction in fetal growth
occurs, it is likely to be mild or due to confounding factors.
F. Vasa previa and velamentous umbilical cord
i.
Vasa previa and velamentous umbilical cord insertion are
uncommon, but when present they are often associated with
placenta previa.
G. Congenital anomalies
i.
Population-based cohort studies have reported an increase in
overall rate of neonatal congenital anomalies in pregnancies
complicated by placenta previa, but no single anomaly or
syndrome was associated with disorder.
H. Amniotic fluid embolism
i.
A large population-based cohort study reported strong association
between placental pathology, such as placenta previa, and
amniotic fluid embolism.
DIAGNOSIS
1. Placenta previa should be suspected in any woman beyond 20 weeks of
gestation who presents with vaginal bleeding. For women who have not
had second or third trimester ultrasound examination, antepartum bleeding
should prompt sonographic determination of placental location before
digital vaginal examination is performed because palpation of placenta can
cause severe hemorrhage.
2. The diagnosis of placenta previa is based on identification of placental
tissue covering internal cervical os on imaging study, typically ultrasound.
TAU is performed as initial examination; if it shows placenta previa or
findings are uncertain, TVU should be performed to better define placental
position.
3. If placental edge covers internal os, placenta is labeled previa. If placental
edge is < 2 cm from, but not covering, internal os, placenta is labeled as
low-lying. Placenta previa should be described by distance (millimeters)
that placenta covers internal cervical os. A low lying placenta should be
described by distance (millimeters) between internal cervical os and
inferior edge of placenta.
4.
Ultrasonography
A. Transabdominal
i.
TAU is used for initial placental localization. The sonographic
diagnosis of placenta previa requires identification of echogenic
homogeneous placental tissue covering or proximate to internal
cervical os (distance > 2 cm from os excludes diagnosis of previa).
Sagittal, parasagittal, and transverse sonographic views should be
obtained with patient's bladder partially full.
ii.
Specific points that should be appreciated when performing
sonographic examination for placenta previa.
1. An over-distended bladder can compress anterior lower uterine
segment against posterior lower uterine segment to give
appearance of previa. The diagnosis of placenta previa should
not be made without confirming placental position after patient
has emptied bladder. Care should be taken to not make
diagnosis of placenta previa when lower uterine segment is
contracting, which commonly occurs after woman empties her
bladder.
2. A previa can be missed near term if fetal head is low in pelvis
since acoustic shadowing from or compression of placental
tissue by fetal skull may obscure placental location. In these
cases, cervix may be better visualized by placing patient in
Trendelenburg position and/or gently pushing fetal head
cephalad.
3. The sonographic diagnosis of complete central previa is readily
made since the placenta is centered over cervix and placental
tissue is imaged anterior and posterior to cervix. Complete noncentral previas, particularly when lateral, are more difficult to
confirm. Transverse views at and above internal cervical os
should facilitate accurate diagnosis.
4. The placental location may also be obscured by hematoma or
lower uterine segment contraction.
iii.
The overall false positive rate of TAU for diagnosis of placenta
previa is high (up to 25%), so diagnosis should be confirmed by
TVU unless previa is clearly central.
B. Transvaginal
i.
RCT and prospective comparative studies have established superior
performance of TVU over TAU for diagnosis of placenta previa. TAU
is performed as initial examination; if it shows placenta previa or
findings are uncertain, TVU should be performed to better define
placental position. TVU generally provides a clearer image of
relationship of edge of placenta to internal cervical os than TAU. In
one study of 100 suspected cases, sensitivity, specificity, and PPV
and NPV of TVU for diagnosis of placenta previa were 87.5, 98.8,
93.3, 97.6%.
ii.
TVU can be performed safely in patients with previa since optimal
position of vaginal probe for visualization of internal os is 2 to 3 cm
away from cervix and angle between cervix and vaginal probe is
sufficient to prevent probe from inadvertently slipping into cervical
canal.
iii.
Translabial (transperineal) ultrasound imaging is alternative
technique that provides excellent images of cervix and placenta.
The use of 3D ultrasound may also improve accuracy.
5. Magnetic resonance imaging (MRI)
A. MRI is well-suited to assessment of placental-cervical relationships
because of differing magnetic resonance characteristics of two tissues.
However, it is not used for diagnosis of placenta previa because of its
high cost, limited availability, and well-established safety and accuracy
of TVU. MRI is most useful for diagnosis of complicated placenta previa,
such as previa-accreta and previa-percreta.
DIFFERENTIAL DIAGNOSIS
1. Exclusion of placenta accreta
A. When placenta previa is diagnosed, the possibility of placenta previaaccreta/percreta should be considered. The normal interface between
placenta and bladder is characterized by hypoechoic boundary that
represents myometrium and normal retroplacental myometrial
vasculature. When placenta accreta is present, this hypoechoic
boundary is lost and placenta appears contiguous with bladder wall. On
ultrasound, intraplacental sonolucent spaces (lacunar flow) may be
observed adjacent to involved uterine wall. The diagnosis of placenta
accreta is reviewed in detail separately.
MORBIDITY AND MORTALITY
1. Maternal
A. Placenta previa increases risk of APH (RR 9.8), IPH (RR 2.5), and PPH
2.
(RR 1.9). For this reason, women with placenta previa are more likely to
receive blood transfusions (12 vs. 0.8% without previa) and undergo
postpartum hysterectomy, uterine/iliac artery ligation, or embolization
of pelvic vessels to control bleeding (2.5 vs. 0% without previa). The
risk is particularly high in those with previa-accreta.
B. Rapid, significant loss of intravascular volume can lead to
hemodynamic instability, decreased oxygen delivery, decreased tissue
perfusion, cellular hypoxia, organ damage, and death. The maternal
mortality rate associated with placenta previa is < 1% in resource-rich
countries, but remains high in resource-poor countries where maternal
anemia, lack of medical resources, and home births are common.
Neonatal
A. Neonatal morbidity and mortality rates in pregnancies complicated by
placenta previa have fallen over the past few decades because of
improvements in obstetrical management (antenatal corticosteroids,
delayed delivery when possible), liberal use of cesarean delivery, and
improved neonatal care. The principal causes of neonatal morbidity and
mortality are related to preterm delivery, rather than anemia,
hypoxia, or growth restriction.
B.
A retrospective cohort study of live births in the US (1989 to 1991 and
1995 to 1997) included over 61,000 singleton pregnancies complicated
by placenta previa and delivered by cesarean birth after 24 weeks of
gestation. During this period, the neonatal mortality rate was 10.7 per
1000 live births with placenta previa compared to 2.5 per 1000 live
births in non-previa pregnancies (RR 4.3).
RECURRENCE
1. Placenta previa recurs in 4 to 8% of subsequent pregnancies.
SUMMARY AND RECOMMENDATIONS
1. Placenta previa should be suspected in any woman beyond 20 weeks of
gestation who presents with painless vaginal bleeding. For women who
have not had a second trimester ultrasound examination, antepartum
bleeding after 20 weeks of gestation should prompt sonographic
determination of placental location before digital vaginal examination is
performed because palpation of the placenta can cause severe
hemorrhage.
2. Previous placenta previa, previous cesarean deliveries, and multiple
gestations are major risk factors for placenta previa.
3. The distance from the placental edge to the internal cervical os is the best
predictor of placenta previa at delivery, but available data correlating
gestational age, millimeters of extension over the cervical os, and outcome
are insufficient to make precise predictions.
4. The characteristic clinical presentation is painless vaginal bleeding, which
occurs in 70 to 80% of cases. An additional 10 to 20% of women present
with both uterine contractions and bleeding, which is similar to the
presentation of abruptio placenta. In approximately one-third of affected
pregnancies, the initial bleeding episode occurs prior to 30 weeks of
gestation.
5. Some conditions that may be associated with placenta previa include
placenta accreta, malpresentation, preterm labor or premature rupture of
6.
the membranes, vasa previa and velamentous insertion of umbilical cord.
The diagnosis of placenta previa is based upon identification of placental
tissue covering or proximate to internal cervical os on TVU.
Anda mungkin juga menyukai
- Shoe Dog: A Memoir by the Creator of NikeDari EverandShoe Dog: A Memoir by the Creator of NikePenilaian: 4.5 dari 5 bintang4.5/5 (537)
- The Yellow House: A Memoir (2019 National Book Award Winner)Dari EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Penilaian: 4 dari 5 bintang4/5 (98)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDari EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifePenilaian: 4 dari 5 bintang4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingDari EverandThe Little Book of Hygge: Danish Secrets to Happy LivingPenilaian: 3.5 dari 5 bintang3.5/5 (400)
- Grit: The Power of Passion and PerseveranceDari EverandGrit: The Power of Passion and PerseverancePenilaian: 4 dari 5 bintang4/5 (588)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDari EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FuturePenilaian: 4.5 dari 5 bintang4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDari EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryPenilaian: 3.5 dari 5 bintang3.5/5 (231)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDari EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RacePenilaian: 4 dari 5 bintang4/5 (895)
- Team of Rivals: The Political Genius of Abraham LincolnDari EverandTeam of Rivals: The Political Genius of Abraham LincolnPenilaian: 4.5 dari 5 bintang4.5/5 (234)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDari EverandNever Split the Difference: Negotiating As If Your Life Depended On ItPenilaian: 4.5 dari 5 bintang4.5/5 (838)
- The Emperor of All Maladies: A Biography of CancerDari EverandThe Emperor of All Maladies: A Biography of CancerPenilaian: 4.5 dari 5 bintang4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDari EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaPenilaian: 4.5 dari 5 bintang4.5/5 (266)
- On Fire: The (Burning) Case for a Green New DealDari EverandOn Fire: The (Burning) Case for a Green New DealPenilaian: 4 dari 5 bintang4/5 (74)
- The Unwinding: An Inner History of the New AmericaDari EverandThe Unwinding: An Inner History of the New AmericaPenilaian: 4 dari 5 bintang4/5 (45)
- Rise of ISIS: A Threat We Can't IgnoreDari EverandRise of ISIS: A Threat We Can't IgnorePenilaian: 3.5 dari 5 bintang3.5/5 (137)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDari EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersPenilaian: 4.5 dari 5 bintang4.5/5 (345)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDari EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyPenilaian: 3.5 dari 5 bintang3.5/5 (2259)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDari EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You ArePenilaian: 4 dari 5 bintang4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Dari EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Penilaian: 4.5 dari 5 bintang4.5/5 (121)
- Her Body and Other Parties: StoriesDari EverandHer Body and Other Parties: StoriesPenilaian: 4 dari 5 bintang4/5 (821)
- Junior Science Book 3 Answers PDFDokumen36 halamanJunior Science Book 3 Answers PDFpololaperez0% (2)
- MCN ExamDokumen10 halamanMCN ExamYaj CruzadaBelum ada peringkat
- Delivery of Baby (Actual, Assist, and Cord Care)Dokumen3 halamanDelivery of Baby (Actual, Assist, and Cord Care)Jasmin AdoraBelum ada peringkat
- Extraembryonic MembraneDokumen41 halamanExtraembryonic MembraneDangkoBelum ada peringkat
- Maternal and Child Nursing Answers and RationaleDokumen94 halamanMaternal and Child Nursing Answers and RationaleAnn Michelle Tarrobago100% (1)
- Anatomy and PhysiologyDokumen10 halamanAnatomy and PhysiologyLiwayway Bayoca LozanoBelum ada peringkat
- Case Presentation Placenta PreviaDokumen37 halamanCase Presentation Placenta PreviaJasmin Sabna100% (2)
- 16.4 Human Repro Notes 1r0bthiDokumen5 halaman16.4 Human Repro Notes 1r0bthisalmasomaBelum ada peringkat
- NCM 107 - LM 7 Assessing Blood Loss, Identifying LOCHIADokumen8 halamanNCM 107 - LM 7 Assessing Blood Loss, Identifying LOCHIAJewel Ramos GalinatoBelum ada peringkat
- DR Chaitra Srinivas Project PDF 2012 PDFDokumen121 halamanDR Chaitra Srinivas Project PDF 2012 PDFNavdeep SohiBelum ada peringkat
- The Placenta BDokumen48 halamanThe Placenta BLulano MbasuBelum ada peringkat
- Cytomegalovirus in Pregnancy - GLOWMDokumen24 halamanCytomegalovirus in Pregnancy - GLOWMLearta Asani VeliuBelum ada peringkat
- Quiz 5 Test BankDokumen37 halamanQuiz 5 Test BankOnyeka O AniyedeBelum ada peringkat
- NCM109 RLE 1st Term ReviewerDokumen40 halamanNCM109 RLE 1st Term ReviewerCarelle Faith Serrano AsuncionBelum ada peringkat
- (T6) How Do Characteristics Pass From One Generation To AnotherDokumen103 halaman(T6) How Do Characteristics Pass From One Generation To AnotherTiara MasseyBelum ada peringkat
- Study of Calcified Placenta and Its Correlation WithDokumen4 halamanStudy of Calcified Placenta and Its Correlation Withcut normaya putriBelum ada peringkat
- The Effect of Drugs On PregnancyDokumen26 halamanThe Effect of Drugs On PregnancyVictoria MarionBelum ada peringkat
- Maternal & Child Nursing Bullets (Nle & Nclex)Dokumen38 halamanMaternal & Child Nursing Bullets (Nle & Nclex)Richard Ines Valino95% (22)
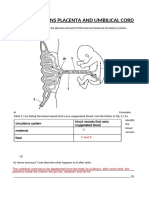
- Igcse Questions Placenta and Umbilical CordDokumen3 halamanIgcse Questions Placenta and Umbilical CordFabriV9Belum ada peringkat
- Intrapartal Complications: Problems With The PowerDokumen10 halamanIntrapartal Complications: Problems With The PowerkeinwayBelum ada peringkat
- Roles and Responsibility As A Nurse in Delivery RoomDokumen6 halamanRoles and Responsibility As A Nurse in Delivery RoomMay 마이100% (8)
- ReadingsDokumen3 halamanReadingsYori Nicole Martine CuyosBelum ada peringkat
- Temporal Expression of Genes Involved in Folate Metabolism and Transport During Placental Development, Preeclampsia and Neural Tube DefectsDokumen9 halamanTemporal Expression of Genes Involved in Folate Metabolism and Transport During Placental Development, Preeclampsia and Neural Tube DefectsMauro Porcel de PeraltaBelum ada peringkat
- 2023 UA Paper Solved by HannanDokumen47 halaman2023 UA Paper Solved by HannanHannan syedBelum ada peringkat
- Iufd Lesson PlanDokumen21 halamanIufd Lesson PlanBupe LwitaBelum ada peringkat
- Placental Therapy: An Insight To Their Biological and Therapeutic PropertiesDokumen7 halamanPlacental Therapy: An Insight To Their Biological and Therapeutic PropertiesIkaSugihartatikBelum ada peringkat
- 3F Intranatal NotesDokumen5 halaman3F Intranatal NotesAlyssa Claire TumulakBelum ada peringkat
- Tinjauan Pustaka Persalinan NormalDokumen31 halamanTinjauan Pustaka Persalinan NormalNurul Fathia Shafira AmiantiBelum ada peringkat
- Abruptio PlacentaDokumen20 halamanAbruptio PlacentaHizkia Mangaraja Hasiholan LimBelum ada peringkat
- Chemical Equilibrium: - HENRI LE CHÂTELIER (1850-1936)Dokumen48 halamanChemical Equilibrium: - HENRI LE CHÂTELIER (1850-1936)Ghida Al Hajj ChehadeBelum ada peringkat