Previews: Stimulation On Demand: Closing The Loop On Deep Brain Stimulation
Diunggah oleh
María Celeste Sánchez SugíaDeskripsi Asli:
Judul Asli
Hak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Previews: Stimulation On Demand: Closing The Loop On Deep Brain Stimulation
Diunggah oleh
María Celeste Sánchez SugíaHak Cipta:
Format Tersedia
Neuron
Previews
Stimulation on Demand: Closing
the Loop on Deep Brain Stimulation
Fernando J. Santos,1 Rui M. Costa,1,* and Fatuel Tecuapetla1,*
1Champalimaud
Neuroscience Programme at Instituto Gulbenkian de Ciencia, Rua da Quinta Grande, 2780-901 Oeiras, Portugal
*Correspondence: ruicosta@fchampalimaud.org (R.M.C.), fatuel.tecuapetla@neuro.fchampalimaud.org (F.T.)
DOI 10.1016/j.neuron.2011.10.004
High-frequency open-loop deep brain stimulation (DBS) has been used to alleviate Parkinsons symptoms for
almost 20 years. In this issue of Neuron, Rosin et al. present a closed-loop real-time approach that improves
DBS and shines light on the etiology of motor symptoms in Parkinsons disease.
In Parkinsons disease (PD), depletion of
dopamine after degeneration of dopaminergic neurons (Carlsson, 1972; Hornykiewicz, 1966), mostly in substantia nigra
pars compacta, leads to a variety of
motor symptoms including bradykinesia,
tremor, and rigidity. This dopamine depletion has consequences for the activity
of cortico-basal ganglia circuits. A wellaccepted view postulates that lack of
dopamine in PD leads to increased
activity of indirect pathway neurons (striatopallidal, which mainly express D2-type
dopamine receptors) and decreased activity of direct pathway neurons (striatonigral, which mostly express D1-type
dopamine receptors) (Albin et al., 1989),
ultimately leading to increased activity
in globus pallidus internus (GPi) and to
overinhibition of thalamus and cortex.
Another view proposes that dopamine
depletion leads to abnormal network oscillations in basal ganglia, which produce
excessive synchrony (Brown, 2003; Goldberg et al., 2004).
Currently, the first approach to alleviate
PD symptoms is the administration of
drugs to restore dopamine, most notably
L-Dopa. However, L-Dopa typically becomes less effective with time. Another
successful approach is the use of high
frequency deep brain stimulation (DBS)
in basal ganglia nuclei, mainly in the subthalamic nucleus (STN), the GPi, or the
thalamus (Wichmann and Delong, 2006).
The first reports of the use of DBS to
treat -PD patients date to 1994 (Limousin
et al., 1995). The paradigms currently used
for DBS are based on continuous stimulation, or open-loop DBS, because the
stimulation pattern and intensity are set
by an external stimulator and adjusted
manually. Although the mechanisms by
which DBS stimulation works are still
under debate, this strategy has helped
more than 55,000 people suffering not
only from PD but also from other motor
disorders (Miller, 2009).
In this issue of Neuron, Rosin, Bergman, and colleagues (Rosin et al., 2011)
develop a new strategy for DBS in the
basal ganglia using a closed-loop paradigm, in which the activity of neurons in
a reference brain area is used as the
trigger for stimulating the target area
(Figure 1). Using primates treated with
MPTP, which causes dopaminergic neuron degeneration and PD-like symptoms
(Burns et al., 1983), the authors compare
the effects of different closed-loop paradigms and standard continuous or openloop DBS protocols in akinesia and pallidal firing properties. These comparisons
show that closed-loop paradigms with
real-time adaptive stimulation have less
undesirable side effects and more clinical
benefits than standard paradigms.
One of the great advantages of closedloop strategies relatively to standard
DBS protocols is the possibility for automatic and constant adaptation to the
dynamics of the disease in each patient
over time. Currently, PD patients that
undergo DBS treatments need to have
periodic medical assistance by a trained
clinician in order to have the stimulation
parameters adjusted to the development
of the disease, and parameters remain
unchanged between adjustments. In this
novel closed-loop DBS paradigm, neuronal spikes recorded in the primary
motor cortex (M1) were used as an online
trigger for stimulation (trains or single
spikes) delivered to the GPi. This paradigm yielded a marked reduction in
akinesia in all four limbs, but most notably
in the contralateral arm to the stimulation
site, as measured by accelerometers.
Importantly, this adaptive closed-loop
DBS successfully triggered a reduction
of pallidal firing rate and a decrease of
oscillatory activity in GPi (Rosin et al.,
2011).
The use of closed-loop DBS with motor
cortex as the reference structure for triggering pallidal stimulation led to a reduction of stimulation frequency and also
to an increase in the variability of the
interstimulus interval when compared
with standard high frequency stimulation.
Could the improvements observed simply
reflect the fact that the stimulation pattern
was of lower frequency and more irregular? In order to demonstrate that the
observed effects were due to the adaptive
closed-loop nature of the stimulation, the
authors performed two experiments. In
one they applied an open-loop stimulation
at low frequency (10 Hz versus standard
DBS at 130 Hz). In another, they applied
a stimulation pattern based on previous
recordings from M1, with the same variability as the online adaptive stimulation
pattern, but unrelated to the ongoing
activity at the moment of the stimulation.
In both cases no relevant improvements
in behavior or neuronal modulation were
observed, strengthening the conclusion
that it was not the statistics of the stimulation pattern that promoted the behavioral
improvements in closed-loop DBS, but
rather the fact that the stimulation pattern
reflected ongoing activity.
This study offers important insights into
how DBS works. Previous studies suggested that there is increased neural activity in the STN of MPTP-treated primates
(Crossman et al., 1985). Accordingly, lesioning the STN in the MPTP primate
Neuron 72, October 20, 2011 2011 Elsevier Inc. 197
Neuron
Previews
A
Open Loop
DBS
Closed Loop
DBS
80ms
delay
130Hz
Recorded
activity
M1
Stimulation train
M1
Stimulation train
GPi
GPi
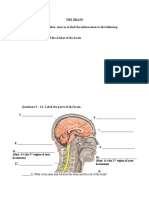
Figure 1. Illustration of an Open-Loop and an Adaptive Closed-Loop Deep Brain Stimulation
(DBS) Paradigm
(A) Standard open-loop high-frequency (130 Hz) DBS consists of continuous stimulation of a target
structure (i.e., internal segment of the globus pallidum, GPi) through an implanted electrode.
(B) Adaptive closed-loop DBS consists of using the online activity of a reference structure (i.e., primary
motor cortex, M1) as a trigger for stimulation of the target structure (i.e., GPi) after a certain delay (i.e.,
80 ms). This results in a lower frequency and more irregular pattern of stimulation and promotes a
substantial reduction of Parkinsonian akinesia compared with standard open-loop DBS protocols, by
adapting the stimulation to the dynamics of cortico-basal ganglia networks.
disorders, like neuropsychiatric disorders. It is becoming increasingly apparent
that several diseases like schizophrenia,
epilepsy, obsessive-compulsive disorders, Tourette syndrome, and depression
could be treated using brain stimulation
(Miller, 2009; Wichmann and Delong,
2006), and the real-time adaptive stimulation paradigm presented here could
also offer significant advantages in the
treatment of the associated symptoms.
Hopefully, future studies in animal models will help disentangle not only how
these pathologies emerge, but also define
the best strategies to improve clinical
outcomes.
REFERENCES
Albin, R.L., Young, A.B., and Penney, J.B. (1989).
Trends Neurosci. 12, 366375.
model reverted the Parkinson-like symptoms (Bergman et al., 1990). Since both
electrical stimulation of STN and STN
lesions produced amelioration of PD
symptoms, it was hypothesized that DBS
leads to decreased activity in STN or
decreased transmission from STN to
GPi, therefore leading to reduced activity
in GPi. Another suggestion has been that
both STN lesions and DBS would disrupt
the pathological oscillations observed in
PD, leading to an improvement in motor
symptoms; this view is supported by
recent studies which suggest that DBS
does not work by inhibiting STN neurons
(Bar-Gad et al., 2004; Carlson et al.,
2010; Gradinaru et al., 2009). Interestingly,
Rosin and colleagues uncovered that
the application of a closed-loop protocol
in which GPi activity triggered GPi
stimulation resulted in a reduction in
pallidal discharge rate with no change in
GPi oscillatory activity, and even in an
increase in oscillatory activity in motor
cortex (Rosin et al., 2011). In this situation,
not only did akinesia in MPTP-treated
primates not improve, but it got worse,
suggesting that the ameliorating effects
of DBS do not stem from reducing GPi
activity, but likely from disrupting pathological oscillatory activity in the basal
ganglia.
These experiments also give invaluable
insight into the mechanisms underlying
the motor symptoms in PD. The fact
that a decrease in GPi discharge rates
with an increase in cortical oscillations
resulted in an aggravation of akinesia,
suggests that motor symptoms in PD are
related to changes in oscillatory activity
in cortico-basal ganglia circuits and not
simply caused by an increase in the firing
rate of GPi as a result of an imbalance
between the activity of the direct and
indirect pathways.
Although this study is very promising, it
opens several questions for future experiments. Which are the optimal parameters
for closed-loop DBS? Can different structures be used as reference or targets?
What kind of signals can be used as
triggers in order to allow for long-term
stability? In this paradigm a single spike
in the reference structure would trigger
stimulation, but it may be difficult to
record M1 spikes during long periods of
time. The use of signals that could be
recorded reliably for longer periods of
time, like local field potential oscillations,
could aid the long-term implementation
of these close-loop strategies. It also
remains to be determined how robust
and stable the ameliorating effects would
be after long-term exposure to such a
treatment.
Furthermore, the approach taken by
the authors can be the starting point to
apply closed-loop DBS strategies to other
198 Neuron 72, October 20, 2011 2011 Elsevier Inc.
Bar-Gad, I., Elias, S., Vaadia, E., and Bergman, H.
(2004). J. Neurosci. 24, 74107419.
Bergman, H., Wichmann, T., and DeLong, M.R.
(1990). Science 249, 14361438.
Brown, P. (2003). Mov. Disord. 18, 357363.
Burns, R.S., Chiueh, C.C., Markey, S.P., Ebert,
M.H., Jacobowitz, D.M., and Kopin, I.J. (1983).
Proc. Natl. Acad. Sci. USA 80, 45464550.
Carlson, J.D., Cleary, D.R., Cetas, J.S., Heinricher,
M.M., and Burchiel, K.J. (2010). J. Neurophysiol.
103, 962967.
Carlsson, A. (1972). Acta Neurol. Scand. Suppl. 51,
1142.
Crossman, A.R., Mitchell, I.J., and Sambrook, M.A.
(1985). Neuropharmacology 24, 587591.
Goldberg, J.A., Rokni, U., Boraud, T., Vaadia, E.,
and Bergman, H. (2004). J. Neurosci. 24, 6003
6010.
Gradinaru, V., Mogri, M., Thompson, K.R., Henderson, J.M., and Deisseroth, K. (2009). Science 324,
354359.
Hornykiewicz, O. (1966). Pharmacol. Rev. 18,
925964.
Limousin, P., Pollak, P., Benazzouz, A., Hoffmann,
D., Le Bas, J.F., Broussolle, E., Perret, J.E., and
Benabid, A.L. (1995). Lancet 345, 9195.
Miller, G. (2009). Science 323, 15541556.
Rosin, B., Slovik, M., Mitelman, R., Rivlin-Etzion,
M., Haber, S.N., Israel, Z., Vaadia, E., and Bergman, H. (2011). Neuron 72, this issue, 370384.
Wichmann, T., and Delong, M.R. (2006). Neuron
52, 197204.
Anda mungkin juga menyukai
- Tmp72e2 TMPDokumen14 halamanTmp72e2 TMPFrontiersBelum ada peringkat
- The Pathophysiology of Motor Symptoms in Parkinson's DiseaseDokumen6 halamanThe Pathophysiology of Motor Symptoms in Parkinson's DiseasegracegozaliBelum ada peringkat
- Role of Preclinical Data in PDDokumen23 halamanRole of Preclinical Data in PDIrving ParraBelum ada peringkat
- Mtanpclbp FinalDokumen12 halamanMtanpclbp FinalSachin AbsBelum ada peringkat
- Biol Psychiatr 2014 Nov 76 (9) 678Dokumen3 halamanBiol Psychiatr 2014 Nov 76 (9) 678drclaudiofernandomedBelum ada peringkat
- Frontal Brain Activity and Cognitive Processing Speed in Multiple SclerosisDokumen8 halamanFrontal Brain Activity and Cognitive Processing Speed in Multiple SclerosisGeo MeBelum ada peringkat
- 10 1016@j Clinph 2019 09 021Dokumen37 halaman10 1016@j Clinph 2019 09 021Jihen FouratiBelum ada peringkat
- 5 - Aerobic Exercise Alters Brain Function and Structure in Parkinson's Disease A Randomized Controlled TrialDokumen14 halaman5 - Aerobic Exercise Alters Brain Function and Structure in Parkinson's Disease A Randomized Controlled TrialGabriel NevesBelum ada peringkat
- Stephan 2006 PlasticityDokumen11 halamanStephan 2006 PlasticityGiuli PanizzoloBelum ada peringkat
- Chiken 2014Dokumen9 halamanChiken 2014dgdgfgfBelum ada peringkat
- Brainsci 09 00005Dokumen8 halamanBrainsci 09 00005Javier Leonardo Rocha BeltranBelum ada peringkat
- Deep Brain Stimulation in 2018Dokumen11 halamanDeep Brain Stimulation in 2018Dhino Armand Quispe SánchezBelum ada peringkat
- Motor Priming in NeurorehabilitationDokumen15 halamanMotor Priming in NeurorehabilitationGhea Mae VillasBelum ada peringkat
- Ni Hms 749680Dokumen32 halamanNi Hms 749680Cristian GhiţăBelum ada peringkat
- Biology ProjectDokumen14 halamanBiology ProjectVittal Rao LBelum ada peringkat
- J NBD 2021 105372Dokumen10 halamanJ NBD 2021 105372bobBelum ada peringkat
- tmp9F14 TMPDokumen24 halamantmp9F14 TMPFrontiersBelum ada peringkat
- Neuro-Cardiac-guided TMSDokumen11 halamanNeuro-Cardiac-guided TMSRafael MoreiraBelum ada peringkat
- BOGGIO Tdcs Alcohol CravingDokumen6 halamanBOGGIO Tdcs Alcohol Cravingexcelencia5Belum ada peringkat
- Grosenick Neuron 2015Dokumen34 halamanGrosenick Neuron 2015AntonellaBelum ada peringkat
- Ambulation and Parkinson DiseaseDokumen22 halamanAmbulation and Parkinson DiseaseDeborah SalinasBelum ada peringkat
- Cognition and Mood in Parkinson's Disease in Subthalamic Nucleus Versus Globus Pallidus Interna Deep Brain Stimulation The COMPARE TrialDokumen10 halamanCognition and Mood in Parkinson's Disease in Subthalamic Nucleus Versus Globus Pallidus Interna Deep Brain Stimulation The COMPARE TrialRicardo GarciaBelum ada peringkat
- Neurostimulation For Stroke RehabilitationDokumen11 halamanNeurostimulation For Stroke Rehabilitationisos.mporei.vevaios.Belum ada peringkat
- Mindfullnes and CongnitionDokumen10 halamanMindfullnes and CongnitionCamila AmorimBelum ada peringkat
- EEG Biofeedback of Low Beta Band Components: Frequency-Specific Effects On Variables of Attention and Event-Related Brain PotentialsDokumen9 halamanEEG Biofeedback of Low Beta Band Components: Frequency-Specific Effects On Variables of Attention and Event-Related Brain PotentialsIshika SharmaBelum ada peringkat
- J Parkreldis 2015 09 028Dokumen4 halamanJ Parkreldis 2015 09 028T.U. Pai João da Caridade & Caboclo FlechasBelum ada peringkat
- Margarita Zachariou Et Al - Sensory Gating and Its Modulation by Cannabinoids: Electrophysiological, Computational and Mathematical AnalysisDokumen12 halamanMargarita Zachariou Et Al - Sensory Gating and Its Modulation by Cannabinoids: Electrophysiological, Computational and Mathematical AnalysisJmasnBelum ada peringkat
- NMDA Receptor Hypofunction Produces Concomitant Firing Rate Potentiation and Burst Activity Reduction in The Prefrontal CortexDokumen6 halamanNMDA Receptor Hypofunction Produces Concomitant Firing Rate Potentiation and Burst Activity Reduction in The Prefrontal CortexCortate15gBelum ada peringkat
- Delayed Plastic Responses To Anodal TDCS in Older Adults. Fujiyama Et Al 2014Dokumen9 halamanDelayed Plastic Responses To Anodal TDCS in Older Adults. Fujiyama Et Al 2014Saray Parra TorróBelum ada peringkat
- Model Responses For Additional SAQ'S PaperDokumen14 halamanModel Responses For Additional SAQ'S PaperYoyo YuBelum ada peringkat
- How Psychotherapy Changes The BrainDokumen5 halamanHow Psychotherapy Changes The BrainTomas SærmarkBelum ada peringkat
- Schulz Gerloff Hummel 2013 Non Invasive Brain Stimulation in Neurological DiseasesDokumen9 halamanSchulz Gerloff Hummel 2013 Non Invasive Brain Stimulation in Neurological DiseasesandreapalmapBelum ada peringkat
- Cholinergic Modulation of Skill Learning and PlasticityDokumen3 halamanCholinergic Modulation of Skill Learning and PlasticityPablo Arenas MancillaBelum ada peringkat
- BHX 055Dokumen13 halamanBHX 055Alfeku CabraBelum ada peringkat
- Irrelevant Stimulus Processing in ADHD: Catecholamine Dynamics and Attentional NetworksDokumen15 halamanIrrelevant Stimulus Processing in ADHD: Catecholamine Dynamics and Attentional NetworksMarie MamatBelum ada peringkat
- Default Mode Network and MeditationDokumen16 halamanDefault Mode Network and MeditationJustin StanleyBelum ada peringkat
- The Utility of Non-Invasive Brain Stimulation in RDokumen10 halamanThe Utility of Non-Invasive Brain Stimulation in RsanagaumiBelum ada peringkat
- Neurophysiological Bio Markers For Drug Development in Schizophrenia. Nat Rev Drug Discov 2008Dokumen16 halamanNeurophysiological Bio Markers For Drug Development in Schizophrenia. Nat Rev Drug Discov 2008Ignacio VarelaBelum ada peringkat
- Transcranial Magnetic Stimulation: Juan Jose Lo Pez-Ibor, Marı A Ine S Lo Pez-Ibor and Jose Ignacio PastranaDokumen7 halamanTranscranial Magnetic Stimulation: Juan Jose Lo Pez-Ibor, Marı A Ine S Lo Pez-Ibor and Jose Ignacio PastranaJ Ignacio PastranaBelum ada peringkat
- PMS, EEG, and Photic StimulationDokumen7 halamanPMS, EEG, and Photic StimulationmarinicamicaBelum ada peringkat
- Neuroplasticity and Non-Invasive Brain Stimulation in The Developing BrainDokumen33 halamanNeuroplasticity and Non-Invasive Brain Stimulation in The Developing BrainRebeca FloresBelum ada peringkat
- Improving Working Memory Exploring The Effect of Transcranial RandomDokumen6 halamanImproving Working Memory Exploring The Effect of Transcranial RandomDanish MujibBelum ada peringkat
- RTMS Gait Parkinsonism Kim2015Dokumen10 halamanRTMS Gait Parkinsonism Kim2015Eduardo Fernández DortaBelum ada peringkat
- How Electroconvulsive Therapy Works - Understanding The Neurobiological Mechanisms - PMCDokumen23 halamanHow Electroconvulsive Therapy Works - Understanding The Neurobiological Mechanisms - PMCSuraj DubeyBelum ada peringkat
- Neurobiology Paper FinalDokumen10 halamanNeurobiology Paper Finalapi-583318017Belum ada peringkat
- NIH Public Access: Author ManuscriptDokumen27 halamanNIH Public Access: Author ManuscriptVictor CarrenoBelum ada peringkat
- Jpts 27 673Dokumen4 halamanJpts 27 673Lazlo SecretBelum ada peringkat
- Pulsed Near Infrared Transcranial and Intranasal Photobiomodulation Significantly Modulates Neural Oscillations: A Pilot Exploratory StudyDokumen11 halamanPulsed Near Infrared Transcranial and Intranasal Photobiomodulation Significantly Modulates Neural Oscillations: A Pilot Exploratory StudyAndré RamosBelum ada peringkat
- Neuro FeedbackDokumen14 halamanNeuro FeedbackMar LindaBelum ada peringkat
- Placebo Article in ArchivesDokumen12 halamanPlacebo Article in ArchivesIsak Isakov100% (2)
- Percutaneous Tibial Nerve Stimulation (PTNS) Efficacy in The Treatment of Lower Urinary Tract Dysfunctions: A Systematic ReviewDokumen11 halamanPercutaneous Tibial Nerve Stimulation (PTNS) Efficacy in The Treatment of Lower Urinary Tract Dysfunctions: A Systematic ReviewMUHAMMMAD FAKHRIBelum ada peringkat
- The Influence of Dopamine On Spatial VisionDokumen7 halamanThe Influence of Dopamine On Spatial VisiontratrBelum ada peringkat
- #6479 Bliem B 2008Dokumen12 halaman#6479 Bliem B 2008marcu_ruxandraBelum ada peringkat
- Papel de La Microglía en La SinapsisDokumen13 halamanPapel de La Microglía en La SinapsisLorena de la FlorBelum ada peringkat
- TMP 13 F2Dokumen16 halamanTMP 13 F2FrontiersBelum ada peringkat
- Toxins: Central Effects of Botulinum Neurotoxin-Evidence From Human StudiesDokumen11 halamanToxins: Central Effects of Botulinum Neurotoxin-Evidence From Human StudiesTameemBelum ada peringkat
- Neuropsychological Rehabilitation, Neuroimaging and Neuropasticity A Clinical CommentaryDokumen11 halamanNeuropsychological Rehabilitation, Neuroimaging and Neuropasticity A Clinical CommentaryRossana Maciel Taboada GarzónBelum ada peringkat
- An Independent Components and Functional Connectivity Analysis of Resting State FMRI Data Points To Neural Network Dysregulation in Adult ADHDDokumen12 halamanAn Independent Components and Functional Connectivity Analysis of Resting State FMRI Data Points To Neural Network Dysregulation in Adult ADHDValentina ScorzoneBelum ada peringkat
- The Properties and Connections of Nerve Cells in Leech Ganglia Maintained in CultureDokumen19 halamanThe Properties and Connections of Nerve Cells in Leech Ganglia Maintained in CultureMaría Celeste Sánchez SugíaBelum ada peringkat
- Requirement of AQP4 For Antidepressive Efficiency of Fluoxetine: Implication in Adult Hippocampal NeurogenesisDokumen14 halamanRequirement of AQP4 For Antidepressive Efficiency of Fluoxetine: Implication in Adult Hippocampal NeurogenesisMaría Celeste Sánchez SugíaBelum ada peringkat
- Hodgkin Katz 1949Dokumen41 halamanHodgkin Katz 1949María Celeste Sánchez SugíaBelum ada peringkat
- Neurobiology of Learning and Memory: Nahid Majlessi, Samira Choopani, Tahereh Bozorgmehr, Zahra AziziDokumen7 halamanNeurobiology of Learning and Memory: Nahid Majlessi, Samira Choopani, Tahereh Bozorgmehr, Zahra AziziMaría Celeste Sánchez SugíaBelum ada peringkat
- Dopaminergic Modulation of Short-Term Synaptic Plasticity at Striatal Inhibitory SynapsesDokumen6 halamanDopaminergic Modulation of Short-Term Synaptic Plasticity at Striatal Inhibitory SynapsesMaría Celeste Sánchez SugíaBelum ada peringkat
- Science:, 1870 (1999) Robert C. Malenka and and Roger A. NicollDokumen6 halamanScience:, 1870 (1999) Robert C. Malenka and and Roger A. NicollMaría Celeste Sánchez SugíaBelum ada peringkat
- Watson 2004Dokumen17 halamanWatson 2004María Celeste Sánchez SugíaBelum ada peringkat
- Nervous System WorksheetDokumen3 halamanNervous System WorksheetaBelum ada peringkat
- Basal Ganglia-KreitzerDokumen51 halamanBasal Ganglia-KreitzerresearchphysioBelum ada peringkat
- Excitable Cells Lecture 2Dokumen34 halamanExcitable Cells Lecture 2stehephBelum ada peringkat
- NCM 106 - Pharmacology Midterms 1M-4M Edited PDFDokumen43 halamanNCM 106 - Pharmacology Midterms 1M-4M Edited PDFKisha Bethel100% (2)
- Brain Bee NotesDokumen10 halamanBrain Bee Notesapi-534972164Belum ada peringkat
- Reviewer On Nervous System Grade VIDokumen4 halamanReviewer On Nervous System Grade VIKent Francis LayaguinBelum ada peringkat
- The Brain: Learning & MemoryDokumen32 halamanThe Brain: Learning & MemoryAkanksha DubeyBelum ada peringkat
- Emotional Resilience - Part 1 The Evolving Brain PDFDokumen10 halamanEmotional Resilience - Part 1 The Evolving Brain PDFPeter Creagh67% (3)
- Neuroanesthesia and Cerebrospinal ProtectionDokumen697 halamanNeuroanesthesia and Cerebrospinal ProtectionUmi KalsumBelum ada peringkat
- Konsep Dasar Ilmu Biokimia Dan Biologi Molekuler Untuk Sistem SarafDokumen31 halamanKonsep Dasar Ilmu Biokimia Dan Biologi Molekuler Untuk Sistem SarafdiandraBelum ada peringkat
- MR IntracranIal menIngIomas!!! Vazno!!!Dokumen5 halamanMR IntracranIal menIngIomas!!! Vazno!!!StefanBelum ada peringkat
- Nervous System of FishDokumen4 halamanNervous System of Fishtalam_06100% (10)
- Roger Sperry: Pioneer of Neuronal Specificity: Essays On Aps Classic PapersDokumen3 halamanRoger Sperry: Pioneer of Neuronal Specificity: Essays On Aps Classic PapersAnderson HenriqueBelum ada peringkat
- Development of RhombencephalonDokumen28 halamanDevelopment of RhombencephalonRamesh KumarBelum ada peringkat
- Speech OutlineDokumen4 halamanSpeech Outlineapi-335645447Belum ada peringkat
- PersonalDevelopment - Q1 - Mod 5 - Powers-of-the-MindDokumen34 halamanPersonalDevelopment - Q1 - Mod 5 - Powers-of-the-MindGene RamirezBelum ada peringkat
- Study Guide Lin 2601Dokumen192 halamanStudy Guide Lin 2601Joanne100% (1)
- Control and Coordination - Class XDokumen5 halamanControl and Coordination - Class XMonika Mehan89% (19)
- SCIENCE ExamDokumen4 halamanSCIENCE ExamLesley AntojadoBelum ada peringkat
- Thalamic Stroke and BehaviourDokumen9 halamanThalamic Stroke and BehaviourparkdhingraBelum ada peringkat
- Grade 10 3rd Quarter Science ReviewerDokumen5 halamanGrade 10 3rd Quarter Science ReviewerZayin DelMundoBelum ada peringkat
- The Brain, Nervous System and Endocrine SystemDokumen13 halamanThe Brain, Nervous System and Endocrine SystemMark Lorenzo A RuizBelum ada peringkat
- Chapter 12 Coordination and ControlDokumen22 halamanChapter 12 Coordination and ControlXaundrae McDonaldBelum ada peringkat
- Disc Vis Lobe Front Et Tempo PDFDokumen12 halamanDisc Vis Lobe Front Et Tempo PDFMarina MaatoukBelum ada peringkat
- Connective TissueDokumen202 halamanConnective TissuePeter ThompsonBelum ada peringkat
- Development of The Nervous SystemDokumen27 halamanDevelopment of The Nervous Systemsalmankhan09215Belum ada peringkat
- Case Study On Meninomyocele (Repaired) PDokumen29 halamanCase Study On Meninomyocele (Repaired) Pcharanjit kaur100% (1)
- The Nervous SystemDokumen25 halamanThe Nervous SystemRoan Angela100% (4)
- SCI Pathophysiology MiculobDokumen1 halamanSCI Pathophysiology MiculobJemina GuenevereBelum ada peringkat
- Sci10 Q3 Module3Dokumen24 halamanSci10 Q3 Module3Jennifer Lomboy50% (2)
- ADHD is Awesome: A Guide to (Mostly) Thriving with ADHDDari EverandADHD is Awesome: A Guide to (Mostly) Thriving with ADHDPenilaian: 5 dari 5 bintang5/5 (3)
- The Age of Magical Overthinking: Notes on Modern IrrationalityDari EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityPenilaian: 4 dari 5 bintang4/5 (30)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeDari EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BePenilaian: 2 dari 5 bintang2/5 (1)
- Love Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)Dari EverandLove Life: How to Raise Your Standards, Find Your Person, and Live Happily (No Matter What)Penilaian: 3 dari 5 bintang3/5 (1)
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionDari EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionPenilaian: 4 dari 5 bintang4/5 (404)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsDari EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsPenilaian: 4 dari 5 bintang4/5 (4)
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisDari EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisPenilaian: 4.5 dari 5 bintang4.5/5 (42)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsDari EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsPenilaian: 5 dari 5 bintang5/5 (1)
- By the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsDari EverandBy the Time You Read This: The Space between Cheslie's Smile and Mental Illness—Her Story in Her Own WordsBelum ada peringkat
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedDari EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedPenilaian: 5 dari 5 bintang5/5 (81)
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsDari EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsPenilaian: 4.5 dari 5 bintang4.5/5 (170)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaDari EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaPenilaian: 4.5 dari 5 bintang4.5/5 (266)
- The Comfort of Crows: A Backyard YearDari EverandThe Comfort of Crows: A Backyard YearPenilaian: 4.5 dari 5 bintang4.5/5 (23)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Dari EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Penilaian: 4.5 dari 5 bintang4.5/5 (110)
- Why We Die: The New Science of Aging and the Quest for ImmortalityDari EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityPenilaian: 4 dari 5 bintang4/5 (5)
- Summary: Limitless: Upgrade Your Brain, Learn Anything Faster, and Unlock Your Exceptional Life By Jim Kwik: Key Takeaways, Summary and AnalysisDari EverandSummary: Limitless: Upgrade Your Brain, Learn Anything Faster, and Unlock Your Exceptional Life By Jim Kwik: Key Takeaways, Summary and AnalysisPenilaian: 5 dari 5 bintang5/5 (8)
- Empath: The Survival Guide For Highly Sensitive People: Protect Yourself From Narcissists & Toxic Relationships. Discover How to Stop Absorbing Other People's PainDari EverandEmpath: The Survival Guide For Highly Sensitive People: Protect Yourself From Narcissists & Toxic Relationships. Discover How to Stop Absorbing Other People's PainPenilaian: 4 dari 5 bintang4/5 (95)
- The Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifeDari EverandThe Courage Habit: How to Accept Your Fears, Release the Past, and Live Your Courageous LifePenilaian: 4.5 dari 5 bintang4.5/5 (253)
- Mindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessDari EverandMindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessPenilaian: 4.5 dari 5 bintang4.5/5 (328)
- Summary: Thinking, Fast and Slow: by Daniel Kahneman: Key Takeaways, Summary & Analysis IncludedDari EverandSummary: Thinking, Fast and Slow: by Daniel Kahneman: Key Takeaways, Summary & Analysis IncludedPenilaian: 4 dari 5 bintang4/5 (61)
- The Obesity Code: Unlocking the Secrets of Weight LossDari EverandThe Obesity Code: Unlocking the Secrets of Weight LossPenilaian: 4 dari 5 bintang4/5 (6)
- The Marshmallow Test: Mastering Self-ControlDari EverandThe Marshmallow Test: Mastering Self-ControlPenilaian: 4.5 dari 5 bintang4.5/5 (60)
- Manipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesDari EverandManipulation: The Ultimate Guide To Influence People with Persuasion, Mind Control and NLP With Highly Effective Manipulation TechniquesPenilaian: 4.5 dari 5 bintang4.5/5 (1412)
- Cult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryDari EverandCult, A Love Story: Ten Years Inside a Canadian Cult and the Subsequent Long Road of RecoveryPenilaian: 4 dari 5 bintang4/5 (45)