(OS 213) LEC 02 Cardinal Symptoms of Heart Disease (A)
Diunggah oleh
Yavuz DanisJudul Asli
Hak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
(OS 213) LEC 02 Cardinal Symptoms of Heart Disease (A)
Diunggah oleh
Yavuz DanisHak Cipta:
Format Tersedia
OS 213: Cardiovascular System
LEC 02: CARDINAL SYMPTOMS OF HEART DISEASE
Exam 1 | Dr. Donato Maraon | September 24, 2012
OUTLINE
Common Cardiac Symptomatology
A.
Chest Pain
1. Attributes of Pain
2. Definitions
3. Chronic Recurrent Chest Pain Syndrome
4. Acute Chest Pain Syndrome
5. Case Discussion
B.
Dyspnea
C.
Palpitations
D. Edema
E.
Cyanosis
F.
Syncope
II. Importance of History and PE
The lecture is similar from block Bs Lecture but we changed the formatting though kasing ang gulo nung topic. So if
mas naguluhan kayo sorry.
Some changes:
1. All the symptomatology are now under common cardiac symptomatology.
2. Differentials for chest pain have been divided into chronic and acute.
I. COMMON CARDIAC SYMPTOMATOLOGY
Symptoms: complaints of the patient (most common complaint: pain); Includes chest pain, dyspnea,
palpitations, edema, cyanosis, syncope
Signs: doctors objective findings and observations
A. CHEST PAIN
Chest pain: most common but not exhaustive - can be caused by other factors such as hypertension
ATTRIBUTES OF PAIN (PPQRSTO)
Provocative what provokes/triggers the pain
o
Is it precipitated by effort (exertional)?
At what time does it appear? When you are trying to get up, moving the body, etc
Palliative what relieves/palliates the pain
Medications, therapy, etc
Quality the nature of the pain
Sharp, burning, pricking, stabbing, strangulating, oppressing, ache similar to muscle ache, etc.
Region/Radiation location (primary region where the pain is felt), central region, how wide the coverage is
and where the pain radiates or is worst
o
Central precordial pain where does it radiate? Back? Leg?
Hard to interview Filipinos doon, diyan vague descriptions of location
Severity intensity: mild, moderate, severe
o
May use a scale from 0 to 10 (worst)
Give open-ended questions
Timing
o
Onset abrupt, worse at start, insidious, builds up/gradual
Ian, Aca, Hannah
UPCM 2016A: XVI, Walang
Kapantay!
1 of
14
OS 213: Cardiovascular System
LEC 02: CARDINAL SYMPTOMS OF HEART DISEASE
Exam 1 | Dr. Donato Maraon | September 24, 2012
Duration how long does it last: few seconds, minutes, hours
Frequency once every month, once every 2 years, etc.; avoid using phrases such as rarely,
o
sometimes
Other associated symptoms important to be able to identify the etiology
o
Nausea and vomiting, cold sweats, palpitations, co-morbidities and other risk factors, etc.
Always observe while you are examining (these might give you clues on the symptoms of the patient)
DEFINITIONS
From 2015 Block B:
Spontaneous: comes and goes, not related to effort
Rest: pain gradually subsides when the effort is eliminated
Nitrates: coronary vasodilators; this as a palliative factor is characteristic of myocardial ischemia.
Fastest acting- sublingual nitrates
Diffuse: not more than one fingerbreadth
Time: anything exceeding 20 minutes is associated with myocardial infarction
Severe: acute coronary syndrome
CHRONIC RECURRENT CHEST PAIN SYNDROME
DDX
1. CARDIAC ETIOLOGY: Classic AnginaA
Fixed arterial stenosis causing symptoms, usually while exerting self
o
Quality of chest pain of aortic stenosis is the same as that of angina
Imbalance in myocardial oxygen demand outstripping the supply
In anemics, the same amount of oxygen will be distributed to the tissues as normal if there is increase in
Cardiac Output or if there is increase in Oxygen Extraction Rate in the tissues.
American Heart Association (AHA): "a medical term for chest pain or discomfort due to coronary heart
o
disease."
o
Chronic angina- myocardial ischemia
Nocturnal angina- provoked during sleep
2014: chest pain due to temporary myocardial ischemia, usually secondary to coronary atherosclerosis
2014 trans: Less than 15-20 minutes unstable coronary syndrome, if greater than 30 minutes, acute
Ian, Aca, Hannah
UPCM 2016A: XVI, Walang
Kapantay!
2 of
14
OS 213: Cardiovascular System
LEC 02: CARDINAL SYMPTOMS OF HEART DISEASE
Exam 1 | Dr. Donato Maraon | September 24, 2012
2. CARDIAC ETIOLOGY: Atypical Angina/Angina PectorisA
the chest discomfort of myocardial ischemia is a visceral discomfort that is usually described as a heaviness,
pressure, or squeezing (Harrisons 17th Edition page 87).
While at rest or while having atypical workload
Table 1. Differentiating the quality of angina
TYPICAL
FEATURES
ATYPICAL
FEATURES
DIABETICS
Heaviness
(vague ache in
the chest)
Squeezing
Constricting
Strangling
builds up
over time
Burning
Stabbing
Pin Pricking
May have
paresthesia/
change in
sensorium, will
describe things
differently
Coronary Artery Diseases (CAD)
most common etiology for coronary insufficiency
common
symptom
IS
ANGINA.
ANGINA
(http://www.nhlbi.nih.gov/health/health-topics/topics/angina/)
The aforementioned features are usually the basis for the determination of typical or atypical angina. In some
references this is based on three classic signs:
is
symptom
not
disease!
(1) substernal chest discomfort with a characteristic quality pressure /squeezing/heaviness an
o
duration
o
(2) provoked by exertion or emotional stress
(3) relieved by rest or nitroglycerin.
Typical angina if it has all these three signs and atypical if it has two.
Angina symptoms resemble those of a heart attack. However, angina symptoms usually last only one to
five minutes, while chest pain from a heart attack may last for hours. Angina symptoms normally diminish after
resting or taking angina medications. Heart attack symptoms do not improve with rest, and angina medication will
not reduce heart attack chest pain
Angina (definition) chest pain caused by restricted blood flow to the heart (called ischemia). It often occurs
when you are under emotional or physical stress, such as exercise. When the heart doesn't get enough oxygen from
the coronary arteries, you feel a squeezing chest pain or pressure across your chest that usually goes away after you
stop the activity. The most common cause of angina is hardening of the arteries (atherosclerosis). (www.umm.edu)
Usual Distribution of Myocardial Ischemia
Retrosternal chest pain
Ian, Aca, Hannah
UPCM 2016A: XVI, Walang
Kapantay!
3 of
14
OS 213: Cardiovascular System
LEC 02: CARDINAL SYMPTOMS OF HEART DISEASE
Exam 1 | Dr. Donato Maraon | September 24, 2012
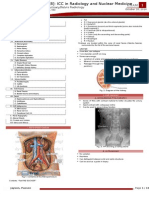
Central chest radiates to neck and jaw (angina dentis- dental pain); more commonly down the left arm
(following dermatomal distribution)
Can also radiate to right arm (for right coronary problems), epigastrium, or back.
Dermatomal origin of heart involved (hence different areas of referred pain
Tooth Ache and throat ache can also be a sign of MI up to the neck and into the jaw.
Figure 1. Usual Distribution of ischemic chest pain: dermatomal distribution of the heart
*epigastrium: may suggest right coronary artery involvement
3. CARDIAC ETIOLOGY: Mitral Valve Prolapse
An abnormal systolic ballooning of part of the mitral valve into the left atrium, resulting in a floppy leaky valve.
o
Younger patients usually have this instead of coronary insufficiency
Usually stays as it is, without hemodynamic deterioration of the valve or stroke
2-5% of people, especially the females commonly seen in the clinics
Not very life threatening, but is associated with mitral regurgitation in the United States.
Table 2. Chronic Recurrent Chest Pain Syndromes: Cardiac Differentials*
Atypical Angina should be
Mitral Valve Prolapse
Classic Angina
distinguished from nonaffects 5% of females
cardiac chest pain**
During effort/ exertion(e.g.
Spontaneous/cold
Spontaneous
walking or during very hot or
weather(mechanism is
very cold weather); due to
vasocontriction/ coronary
demand for oxygen (demand
vasospasm = supply type of
P
type)
angina rather than demand type),
pain at night
Rest / nitrates(diagnostic if chest
pain goes away in a few minutes)
Nitrates
Variable (TYPICAL: Squeezing,
constricting, pin pricking,
stabbing tightness, pressure,
heaviness, strangling,vague
chest discomfort)
basta mabigat
SEVERE: parang may hollow
blocks sa chest
Variable(burning, pricking,
stabbing pain; found in diabetics
and the elderly; itis not life
threatening)
Ian, Aca, Hannah
Spontaneous (can be
incapacitatingneed to use a Bblocker)
Variable(diagnosis is based on
echocardiography)
UPCM 2016A: XVI, Walang
Kapantay!
4 of
14
OS 213: Cardiovascular System
LEC 02: CARDINAL SYMPTOMS OF HEART DISEASE
Exam 1 | Dr. Donato Maraon | September 24, 2012
Classic Angina
R
Retrosternal/ precordial(diffuse
pain, more centrallylocated)
Mild to moderate*** (stable =
same level of intensity for some
time now)
1-30 min
Typically <15-20 mins
If > 20 mins. = Myocardial
Infarction (MI)
Risk factors (i.e. Age: M>55/45*,
F>65/55*, 5 most common risk
factors: Smoking, DM,
hypertension, dyslipidemia,
genetic predisposition)
Associated factors: obesity,
stress
Atypical Angina should be
distinguished from noncardiac chest pain**
Retrosternal (not typical ; maybe
different in location); especially
with diabetics, they usually
present with atypical angina
Mild to moderate
Mitral Valve Prolapse
affects 5% of females
Left anterior, variable(can be
under the breast)
Mild severe(not life threatening
but pain is incapacitating)
1-30 mins
Maybe 2-3 mins
Mins hours
Also w/ CSAP
(Chronic Stable Angina Pectoris;
higher risk in diabetic patients
and in women, presence of at
least 1 risk factor for coronary
disease)
Young female(oftentimes the
complication is benign)
*These are just common diseases (other diseases may present with similar pain/symptoms)
**We should not dismiss the complaint just because it is atypical
***The Canadian Cardiovascular Society (CCS) grading of angina pectoris was described in the medical literature in
1976. This grading system of the severity of effort angina has been accepted throughout the world over the past 30
years.
Table 3. Canadian Cardiovascular Society Grading of Angina Pectoris
Grade
Description
Grade I
Ordinary physical activity does not cause angi
na, such as walking and climbing stairs. Angi
na with strenuous or rapid or prolonged
exertion at work or recreation. (least
bothersome)
Grade I
I
Slight limitation of ordinary activity. Walking
or climbing stairs rapidly, walking uphill,
walking or stair climbing after meals, or in
cold, or in wind, or under emotional stress, or
only during the few hours after awakening.
Walking more than two blocks on the level
and climbing more than one flight of ordinary
stairs at a normal pace and in normal
conditions (provoked by more than usual to
usual activities)
Grade I
II
Marked limitation of ordinary physical activity.
Walking
one or two blocks on the level and climbing o
ne flight of stairs in normal conditions and at
normal pace (provoked by less than usual
activities)
Grade I
V
Inability to carry on any physical activity with
out discomfort,
anginal syndrome may be present at rest (dis
abling or severe, pain at rest)
References:Campeau Lucien. Grading of angina pectoris. Circulation 197654:5223 http://www.ccs.ca/download/position_statements/
Grading%20of%20Angina.pdf
4. GI ETIOLOGY: ESOPHAGEAL, GASTRIC, BILIARY
Table 4. Chronic Recurrent Chest Pain Syndromes: GI differentials
Ian, Aca, Hannah
UPCM 2016A: XVI, Walang
Kapantay!
5 of
14
OS 213: Cardiovascular System
LEC 02: CARDINAL SYMPTOMS OF HEART DISEASE
Exam 1 | Dr. Donato Maraon | September 24, 2012
Esophageal
Gastric
Biliary
Acid Reflux Disease
Gastric/Peptic Ulcer
Gallbladder stones
Feed (a common provoking factor), exercise,
supine/lying down after a meal (due to reflux;
especially if patient has hiatal hernia or weak
GI sphincter; Gastroesophageal reflux:
HEARTBURN)
Drinking, proton pump inhibitors, antacids,
burping,(H2 blocker/proton pump inhibitors
decrease acidity of gastric secretions) pain
is due to acid going back to the esophagus,
SLN
Fasting(or 2hrs after eating);
e.g. peptic ulcer
Feeding (precipitated
by high fat meals;
spastic)
Feeding, Rx (antacids: H2
blockers, proton pump
inhibitors)
Spontaneous,Rx(antis
pasmodics,
antiparasympathomim
etic agents)
Variable (burning, lower part of the chest;
angina-like)
Variable (hunger- like pain;
gnawing pain/discomfort)
Colicky, crampy or
spastic/painful
Substernal(may radiate to the epigastrium;
visceral ache)
Epigastrium/ lower sternum
Right upper quadrant
but can radiate to
chest and shoulder
Mild - severe
Mild moderate; severe(may
imply persistence of a
perforation if severe)
Mild, severe
5-60 min
earlier)
Hours(1.5 hrs or longer after a
meal; antacids for immediate
relief)
Min-hrs
Angina-like(esophageal spasms also
manifested but not relieved by nitrates)
Epigastric pain
4 Fs (risk factors of
gallstones: fat,
female, fertile, forty),
nausea and vomiting
(usually not relieved
Your notes here:
5. OTHER ETIOLOGY: PLEURAL, MSK, FUNCTIONAL
Table 5. Chronic Recurrent Chest Pain Syndromes: Other differentials
Pleural (more diffuse) or
Musculoskeletal (felt almost by
Pulmonary (acute pericarditis,
everyone unless sedentary)
pneumonia)
P
Respiration (deep breaths);
coughing; pleural
inflammation(acute pleuritis,
asthma)
Analgesics (anti-inflammatory,
narcotics)
Variable (sharp, more localized
pain)
Variable (wherever pathology
is, esp. Left/ Right chest, back)
Mild severe (unequal
breathing; leaning on one side
to protect the hurting area
dependent if acute)
Variable(until inflammation
abates)
Cough & fever (because
inflammation involved), cough
associated pain
T
O
Ian, Aca, Hannah
Change in Position, upon
application of pressure, upon
motion; elicit tenderness; may be
recurrent; may also be associated
with cough
Rest, Rx (analgesics and/or nonsteroidals because its an
inflammation)
Variable
(dull muscle type
pain, depends on position and
motion)
Variable
Functional* (psychosomatic)
Supratentorial; Stress: all in the
head no organic basis;
psychiatric (especially Borderline
Personality)
Relaxation; psychiatric intervention;
extensive workup; deliberate thought
on diagnosisreally depends on
history
Variable (but can be distressing
especially if unknown etiology)
Substernal
Mild severe
Mild severe
Variable
Hours
Tietzes Syndrome acute
costochondritis; inflammation of
costal cartilages (costochondral
and sternocostal junction),
tenderness and sharp localized
Da Costas(soldiers heart) most
severe; in soldiers sent to war
patient with profound psycho
somatizations (loss of motivation,
energy lack, chest pains, vague
UPCM 2016A: XVI, Walang
Kapantay!
6 of
14
OS 213: Cardiovascular System
LEC 02: CARDINAL SYMPTOMS OF HEART DISEASE
Exam 1 | Dr. Donato Maraon | September 24, 2012
Pleural (more diffuse) or
Pulmonary (acute pericarditis,
pneumonia)
Musculoskeletal (felt almost by
everyone unless sedentary)
Functional* (psychosomatic)
pain (a few points in the chest)
symptoms)
- more common in females beyond -may require psychiatric care;
forty; PE evoke tenderness by
circulatory neurastemia
touching chest pain
*Functional aka supratentorial (its all in the mind): but its symptoms is as real as those with organic symptoms
Your notes here:
Table 6. Chronic Recurrent Chest Pain Syndromes: Summary
Differential
Provocative
Palliative
Other
Angina
During effort
Rest, sublingual nitrates
Mins
Coronary disease
risk factors
Esophageal
Feeding, exercise,
supine position
Burping, drinking, SLN
Mins
Angina like
GI
Fasting
Food, Antacids
Mins
Epigastric pain
Biliary
Feeding
Spontaneous, Rx
Mins
Crampy, colicky
Pleural, Pulmonary
Respiration, cough
Analgesics
Var.
Assoc.
with cough and
fever
Musculo-skeletal
Position, motion,
pressure
Analgesics, (muscle
relaxants)
Var.
Tietzes syndrome
Functional
Stress
Relaxation
Var.
Da Costas
syndrome
Few modern doctors are equipped to recognize the subtle cases of angina, largely because they are ignorant of these
details or unwilling to invest time in history takingOf the million coronary angiograms done in 1993, 200,000
revealed normal coronary arteriesHad Levines teachings been heeded, few if any of the patients would have been
subjected
to
such
a
costly
and
invasive
procedure
Frequent reliance on a so-called work-upIs testimony to lack of clinical skills
-Bernard Lown, MD (1985 Nobel Peace Prize)
Point of Emphasis: History and PE matter.
ACUTE CHEST PAIN SYNDROME DDX
Table 7. Acute Chest Pain Syndromes
Common
Clinical Clues
Causes
ACS: Acute
MI*
ACS:
Unstable
Angina*
Acute
Pulmonary
Embolism*
Dissecting
aortic
aneurysm*
Prior angina, risk factors,
>20minutes, crescendo
Dyspnea, clear lung fields (this is not
a pulmonary problem, its a vascular
problem), Deep Vein Thrombosis is a
risk factors
Unequal phases- radial, brachial,
femoral
You can hear regurgitations
Ian, Aca, Hannah
UPCM 2016A: XVI, Walang
Kapantay!
7 of
14
OS 213: Cardiovascular System
LEC 02: CARDINAL SYMPTOMS OF HEART DISEASE
Exam 1 | Dr. Donato Maraon | September 24, 2012
Common
Causes
Clinical Clues
Acute
Pericarditis
Pleuritic (aggravated when leaning
forward or taking deep breaths),
central chest, anterior friction rub
Acute
Pneumonia
Pleuritic, cough
After alcohol,
gnawing
Acute Gastritis
Acute
Pancreatitis
Nausea and
vomiting
Acute
Cholecystitis
Acute visceral
problems
(abdomen)
After alcohol,
gallstones
Jaundice
Nausea, vomiting, cold sweat
*Three diseases associated with chest pain that would require immediate attention (life threatening). These Big
Three diseases can be ruled out by CV angiogram (however relying on this test can make your mental capacities
deteriorate (Maranon, 2011; basing from Lown)
**Acute Coronary Syndrome (ACS): Acute MI and Unstable Angina. Unstable Angina is without necrosis (thus is
diagnosed after MI is ruled out)
***Sometimes nausea and vomiting together with diffused pain can be a manifestation of acute MI (respect these
symptoms!)
Fixed obstruction kind can result to unstable angina.
o
Intensity
Frequency
What provokes it
Acute coronary syndrome results from plaque rupture
o
Necrosis is present in acute MI. Acute thrombosis occurs.
Diagnostic of necrosis: Enzymes.
Acute MI is ruled out if there is no evidence of myocardial necrosis, negative for EKG changes, and no
characteristic pain. If enzyme tests negative, then it is unstable angina.
Lethal
Acute MI, Unstable Angina, Acute Pulmonary Embolism, Dissecting Aortic Aneurysm
Unstable Angina
more severe, more frequent, needs ICU confinement; crescendo angina (increasing intensity/
worsening pattern, unlike in classic and atypical angina), must monitor angina within the first month because it
can head south to this
Dissecting Aortic Aneurysm
aorta tears; aortic insufficiency murmurs are heard on PE; the pain is more severe at the outset and it
radiates to the back and the butt (depending on the extent of the aneurysm)
Ian, Aca, Hannah
UPCM 2016A: XVI, Walang
Kapantay!
8 of
14
OS 213: Cardiovascular System
LEC 02: CARDINAL SYMPTOMS OF HEART DISEASE
Exam 1 | Dr. Donato Maraon | September 24, 2012
o
patients feel like theyre going to die (20% die at initial pain); unequal pulses depending on the levels
of compromise of aortic branches
Proximal aortic dissection
manifests as chest pain
Acute pulmonary embolism
shortness of breath, clear lung fields (a problem of perfusion, not ventilation), oxygen desaturation/
hypoxemia, pleuritic, pulmonary hypertension- related, RV cannot compensate: Right heart failure. Pneumonia=
crackles,
Acute pericarditis- pericardial rub
Acute pneumonia
febrile
episode
with
pleuritic
pain;
inspiratory
pleuritic
rub
CASE DISCUSSION
Case 2
The pain usuallyCase
occurs
1
The patient is a 40F with
during exertion but
pain Do
on exertion,
In chest
this case:
not use endoscopy unless the patient does
sometimes at rest or after
usually after washing
not
respond
to
medications/
treatment
fatty meals. It is relieved
clothes
by nitrates or rest or
sometimes
by belching
Diagno
Upper extremity effort (musculoskeletal
sis pain); can also be due to angina BUT the
Diagno multiple etiologies: biliary, esophageal,
type of effort is important.
B. DYSPNEA
sis atypical angina (Be open minded of other
Definition:
The patient
possible etiologies. Do not Caveat
be limitedInto
angina, effort
as light as walking
can is not necessarily in distress but is
shortness
of breath
what is being discussed. )
cause the pain. suffering
The kind from
of effort
will
characterize the pain.
TWO MAIN
TYPES of
OFparsimony:
DYSPNEA:simplest
CARDIAC
Caveat
The concept
wayAND
to
PULMONARY
explain (only one disease)
Table 8. Differentiating cardiac and pulmonary dyspnea
Cardiac
Pulmonary
Usually from congestive heart failure or
Obstructive pulmonary airway
angina, but these do not include edema
syndromes, e.g. asthma
Progressive and occurs on exertion
Progressive (chronic: COPD or end stage
lung disease)
Progressive: takes more effort at the outset,
On exertion
then less and less in time until it occurs at
episodic (bronchial asthma, which has
rest
reversible, intermittent causes)
2015: RHD, MI or cardiomegaly
Late
Immediate, can happen earlier on
Orthopnea
unless in cases of acute mitral valve
regurgitation
Relieved by sitting orstanding
Expectorate:
relieved by sputum production & cough
PND** (Paroxysmal reduction of central venous pooling
Nocturnal Dyspnea) 2015: when patient is supine, there is
2015:expectorating phlegm, blood
Cardiac Asthma
pulmonary congestion due to increased
blood flow to the lungs
Cough
Late symptom
Early prominent symptom
Ascending (from the feet up)
Ascending(only in a R-sided failure or RV
Edema
Biventricular- from Left heart failure (CAD)
heart failure from pulmonary
hypertension core pulmonare)
*To differentiate the different forms of dyspnea, be detailed as possible, since symptoms are similar for both the
cardiac and pulmonary types
OTHER TYPES OF DYSPNEA SYNDROMES
Orthopnea - dyspnea when in supine; difficulty breathing in supine position, late sign
Paroxymal nocturnal dyspnea** - episodes of sudden dyspnea and orthopnea that awaken the patient from sleep,
usually one or two hours after going to bed, when you sleep, get up and youre out of breath
Trepopnea dyspnea when lying on side/lateral decubitus position, can occur due to heart failure or pulmonary
conditions or disease states
Ian, Aca, Hannah
UPCM 2016A: XVI, Walang
Kapantay!
9 of
14
OS 213: Cardiovascular System
LEC 02: CARDINAL SYMPTOMS OF HEART DISEASE
Exam 1 | Dr. Donato Maraon | September 24, 2012
Platypnea dyspnea when upright usually due to a diaphragmatic problem; differentials: hepatopulmonary syndrome
due to pulmonary shunting, diaphragmatic mismatch
Treponea and Platypnea are issues with changing perfusion-ventilation ratios and congenital diaphragm problems
Non cardiac causes of dyspnea: Dyspnea may be caused by severe anemia and hypoxia, which are not exclusively
cardiac or pulmonary causes
Caveat
Case 1
Diagnos
is
Caveat
Case 2
Diagnos
is
Caveat
Doc, madali po akong mapagod
easy fatigue vs. exertional dyspnea
difference in vernacular: tire easily (easy
fatigue) versus out of breath (exertional
dyspnea)
Differentiate between pathologic and
physiologic
Easy fatigue: effort intolerance due to
low cardiac output
Exertionaldyspnea: congestive heart
failure
Pathologic if the symptom is not age/
appropriate
Doc, hinihingal po ako kahit walang
ginagawa, saka mayroon ho akong kaba,
nahihilo ako, at nanlalamig, at lagi akong
hinang-hina
hyperventilation syndrome
The case may appear non-specific but
these signs are characteristic of
hyperventilation syndrome, which may be
a normal thing and would require patient
to blow into rebreathing bag
Dyspnea may be normal or abnormal depending upon the situation. Therefore, we need to elicit more information from
the patient during the history taking. Remember that cardiac and pulmonary symptoms may always be
present on exertion, orthopnea, PND, cough, and edema. Proper diagnosis entails a good history taking which
involves the clear characterization of the symptoms and correct understanding of the patients descritption of cardiopulmonary symptoms.
C. PALPITATION
Definition: Awareness/sensation of ones heartbeat
Can be:
o Singlet (skipped beats)
o Rapid succession of palpitations (tachyarrhythmia)
o How to differentiate? Ask the patient to tap on the table following the rhythm of his/her perceived heartbeat
Can develop during exercise
Not always tachycardia or bradycardia
Table 9. Differentiating functional and organic palpitations
Functional
Start
Gradual
End
Gradual
Trigger
Stress
Rate
<<100
Other Symptoms
Organic/ Pathologic
Sudden
Sudden
None
>>100 (they can have
supraventricular or ventricular
tachycardias occurring and
because of that, extremely rapid
rate)
Anxiety (a little bit of tremulousness, stage fright)
* Many complain about this!
2015: although there are some
bradycardic palpitations)
Chest tightness, shortness of
breath, syncope
Caveat
Case 1
Diagno
sis
Doc, lagi po akong kinakabahan
You can only come to a diagnosis if you ask the
patient further. Ask: Ano pong ibig niyong sabiing
kinakabahan?[Do not suggest an answer. If you
Ian, Aca, Hannah
UPCM 2016A: XVI, Walang
Kapantay!
10 of
14
OS 213: Cardiovascular System
LEC 02: CARDINAL SYMPTOMS OF HEART DISEASE
Exam 1 | Dr. Donato Maraon | September 24, 2012
Caveat
are prone to suggest, give multiple choices.
Let the patient explain what s/he means
D. GENERALIZED EDEMA
characterized by an (abnormal) accumulation of water (actually an accumulationof salt, whichbringswaterwith it)
generally PAINLESS
Table 10. Differentiating the different types of edema
Cause
Description
Renal
Descending
Hypoalbuminic states: puffy eyelids (periorbital edema) and face,
especially in nephrotic syndrome
Hypervolemia, acute renal failure
Two types: Acute renal failure and nephrotic syndrome
Hepatic, systemic
Centrifugal
Starts in the abdomen (ascites) due to portal hypertension
As secondary compensatory mechanism, you get it in your feet
next
Cardiac and Pulmonary
Ascending
(Dependent edema)
Feet first, bilateral then upward, may evolve to anasarca
(generalized edema)
Heart failure (L&R for cardiac, R sided for pulmonary)
Caveat
Case 1
Diagno
sis
Caveat
This 74F has been having bilateral ankle swelling
for the past month, she can hardly walk
Ankle Arthritis
Check first if there is pain since arthritis and gout
are usually painful. Edema is painless.
E. CYANOSIS
Definition: bluish color of the skin and mucous membranes resulting from an increased quantity of reduced
hemoglobin (i.e., deoxygenated hemoglobin) or of hemoglobin derivatives (e.g., methemoglobin or sulfhemoglobin)
in the small blood vessels of those tissues. (Harrisons 18 thed)
Common locations: in the mucous membranes (of the mouth), nail beds, conjunctivae
Pathophysiology:
o Increase in the quantity of venous blood as a result of dilation of the venules and venous ends of the capillaries
~OR~
o Reduction in the saturation of arterial blood (SaO2) in the capillary blood
o Leads to increase in the quantity of reduced hemoglobin in mucocutaneous vessels
Cyanosis becomes apparent when concencentrations of reduced hemoglobin in capillary blood exceeds 40g/L (4g/dL)
At least 5 grams per cell or greater (of desaturation):
o It is the absolute, rather than the relative, quantity of reduced hemoglobin that is important in producing
cyanosis (Harrisons, 18th ed)
Thus, cyanosis is more appreciated in a polycythemic person rather than an anemic person
Anemic patient w hemoglobin at 8, O2 saturation of 75% due to pulmonary disease desaturation is of 8 = 2
not cyanotic because degree of deoxyhemoglobin is only 2
o Patient with hemoglobin of 16, 75% saturated or 4 is not yet cyanotic (you need more desaturation for
cyanosis to manifest)
It is easier to see desaturation or cyanosis
o In a polycythemic person
o In fair skinned people than dark skinned (skin color matters)
o Better detected in nail beds and malar prominences in fairer skinned persons
o In mucous membranes than nail beds
Table 11. DeoxyHb Concentration that cause Cyanosis
DeoxyHb
Concentration
Normal
5 g/dl
Met Hbanemia (Abnormal Hb)
1.5 g/dl
*congenital or acquired, from abnormal Hg or drugs (nitrates)
*usually in toxic concentrations and hemoglobinopathies
Sulf Hb (Abnormal Hb)
0.5 g/dl
Met-Hb and Sulf-Hb arise from hemoglobin congenital problems and toxicities (nitrate poisoning)
Can be congenital or acquired
PATTERNS OF CYANOSIS: CENTRAL OR
PERIPHERAL
Table 12. Differentiating central and peripheral cyanosis
Central
Peripheral
Ian, Aca, Hannah
UPCM 2016A: XVI, Walang
Kapantay!
11 of
14
OS 213: Cardiovascular System
LEC 02: CARDINAL SYMPTOMS OF HEART DISEASE
Exam 1 | Dr. Donato Maraon | September 24, 2012
Sirs words:
Desaturated centrally
O2 saturation is low due
to a cardiac pulmonary
condition
The arterial blood has low
oxygen level (hypoxemia
leading to arterial
oxygendesaturation from
the aortadeoxyhemoglobin).
Cyanosis is observed both
in mucous membranes
(mouth, lips, palpebral
conjunctiva and
especially under the
tongue) and nailbeds
Happens with congenital
heart disease, heart
failure, pulmonary edema
Sirs words:
Caused by something
in the periphery
(vasoconstriction, cold
weather)
There is
vasoconstriction
(demonstrated by
touching ice), arterial
venous occlusions,
hemostasis and arterial
blood has normal
oxygen level (normal
saturation)
But for some reason,
cutaneous blood flow
slows down and
decreases, and the
tissues extract more
oxygen from the blood
There is an increase in
venous deoxygenated
blood in the capillaries,
and only the nailbeds
are cyanotic
This phenomenon can be attributed to:
Vasospasm (Raynauds phenomenon- characterized by the focal vasoconstricted state of the
arteries), ex. Digital arteries
A thrombus, embolus or a normal response to a cold environment or anxiety
It could also be PDA: Patent Ductus Arteriosus wherein the deoxygenated blood flows to the lower
extremities (only the lower extremities are cyanotic, the upper extremities and oral mucosa look normal)
Polycythemic (with Hb<20) get cyanotic earlier than anemic.
Caveat
Case 1
The toes were cyanotic but her fingers
were not
Diagn Differential cyanosis from PDA
osis Reverse PDA
There is a right to left shunting of blood
past the subclavian artery, and the
upper extremities are spared
Note that PDA is a left to right shunt
Review: Patent Ductus Arteriosus
Ductus Arteriosus: Communication between the aorta and the pulmonary artery ligamentum arteriosum
Patent DA: The ductus arteriosus still persists as a vessel leading from the bifurcation of the pulmonary artery to the
aorta just distal to the left subclavian artery instead of closing after birth
In adult patients with PDA, pulmonary pressures are normal and a gradient and shunt from aorta to pulmonary artery
persist throughout the cardiac cycle.
Pulmonary pressure is 1/6 of the systemic circulation. Blood from the left heart goes upward (fingers), mixed blood
goes downward (feet).
Differential cyanosis from PDA
o May be due to preferential shunting of blood to the feet via the patent ductus arteriosus (PDA).
o Differential diagnosis include:
Diabetes and Eisenmenger syndrome- patients with a large communication between the two circulations at
the aortopulmonary, ventricular or atrial levels and directional or predominantly right to left shunts because of
high resistance and obstructive pulmonary hypertension
Severe pulmonary vascular disease results in reversal of flow through the ductus, unoxygenated blood is
shunted to the descending aorta, and the toes, but not the fingers, become cyanotic and clubbed termed
differential cyanosis.
F. SYNCOPE
Syncope is the relatively abrupt loss of consciousness(2015: brief, seconds to a few minutes and due to decreased
blood flow in the brain), with or without a short prodrome.
Presyncope dizziness
Some people develop syncope after dizziness
Doc nahihilo akowhat type? Characterize and describe!
Table
13. Types
of Dizziness
Ian, Aca,
Hannah
UPCM 2016A: XVI, Walang
Kapantay!
12 of
14
OS 213: Cardiovascular System
LEC 02: CARDINAL SYMPTOMS OF HEART DISEASE
Exam 1 | Dr. Donato Maraon | September 24, 2012
Vertigo
Disequilibrium
sensation
of
spinning
or the
room is
spinning
Syncope/ Near
Syncope
less than vertigo,
passing out
may be ear problems/ (2015: near
vestibular or the CNS/ faintness, about
central connections in to pass out,
the brain (2015:
light
sense of imbalance;
headedness),
mild kind of vertigo;
metabolic
problem with
sometimes
proprioceptors,
(hypoglycemia
stereognosis;
but thats not
unsteady gait)
our topic since
this is cardio)
Stokes Adams
Types and causes of cardiogenic syncope
Stokes-Adams/ cardiac (syncope)- sudden cessation of
cardiac function and effective CO, complete heart block;
bradycardia(from complete heart block)causing loss of
consciousness
Vasovagal/Common
faintaka
neurocardiogenic
syncope(2015: Neurologic cause with prodrome(flashes of
light, weakness and cold clammy sweat), more benign;
interaction of cardiac mechanoreceptors as well as paraand sympathetic receptors; vasodepressor or inhibitor. Can
be prevented because there are warning signs)
Table 14. Qualities of syncope
Vasovagal(the common faint e.g. in the heat)
Onset
Sudden
With short prodrome (stomachache, dimming of vision,
lightheadedness); close to hyperventilation; position
dependent, aka common faint
End
Asymptomatic, (2015: no post ictus,
pt has no memory of occurrence)
Usually no post ictus (post seizure) except for a few
brief jerks sometimes
Duration
Seconds (or else the patient will be
dead)
Minutes to hours, relieved by lying down (blood goes
to head)
Table 15. Other Causes of Syncope-like Episodes (DDx)
Absence seizures
Situational(2015: preand post-ictal stages,
weak and sleepy upon
revival, non convulsive
seizures)
Cough syncope
Situational (2015: benign
and common in elderly,
loss of consciousness
after coughing bout due
to increased vagal
stimulation)
Post micturition
Situational (2015: benign
syndrome
and common in elderly,
pt is woken up by an urge
to urinate and losses
consciousness upon
micturition)
Carotid sinus
Passing out when shaving
hypersensitivity
(2015: when the patient
turns his heador wears a
tight collared shirt)
Hyperventilation
2015: Due to hypocapnia
syndrome
leading to loss of
consciousness
Hypoglycemia
2015: through intake of
oral hypoglycemics such
as glibenclamide,
metformin, insulin and
comistamil
Caveat:
Case 1
Diagnosis
Caveat
Doc, nahihilopo ako then loses consciousness
Trauma
Determine the differentials (this patient had trauma (head injury))
Temporal order is important (hitting head then getting up and fainting vs fainting and then falling and
hitting head)
II. IMPORTANCE OF HISTORY AND PE
Table 16. Importance of Hx and PE
Crombie, 1963
History and PE accounts for 88% of patient diagnosis
Hampton, 1975
History=82%
PE= 9%
Saundler, 1980
History=56%
PE= 15%
Sapira, 1990
History=90%
PE= 9%
Ian, Aca, Hannah
UPCM 2016A: XVI, Walang
Kapantay!
13 of
14
OS 213: Cardiovascular System
LEC 02: CARDINAL SYMPTOMS OF HEART DISEASE
Exam 1 | Dr. Donato Maraon | September 24, 2012
Looking at the more recent values, we can see that we can still arrive at a diagnosis with history and PE. Between the
two, history is important!
Remember the importance of history taking (and PE) so we can prove this guy wrong: "Doctors pour drugs of
which they know little, to cure diseases of which they know less, into human beings of whom they know nothing".
Voltaire
END OF TRANSCRIPTION
Ian: Hi block A! One last module, then SEMBREAK na! Yehey! :)
Aca: Aca: Heaven in a wild flower. Also, Im currently in a post-Awkward (season 2) high. Matty please, please be the one! [cc: DOMS] They wont get to
read this, but happy happy birthday to my beloved batchmate, Blessie! I love you, sis Also to the sizzling hot and awesome Patrick (super miss na kita
) and lastly, belated happy birthday to one of the sausage masters, Lee! Kevin, awesome job, man. Sexy mo! Hi sisses and brods, AFTG! XVI: Walang
Kapantay! Hi you!
Hannah: Kamustamus Kalabasa naman sa minigreetings?! Hahaha! Sorry guys! We did our best but we guess our best was the best.
(vangagaboomboomangpakalakapeg!)
Ian, Aca, Hannah
UPCM 2016A: XVI, Walang
Kapantay!
14 of
14
Anda mungkin juga menyukai
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDari EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifePenilaian: 4 dari 5 bintang4/5 (5794)
- A Durable Ultrasound Phantom For Trainees Using Common MaterialsDokumen7 halamanA Durable Ultrasound Phantom For Trainees Using Common MaterialsYavuz DanisBelum ada peringkat
- The Yellow House: A Memoir (2019 National Book Award Winner)Dari EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Penilaian: 4 dari 5 bintang4/5 (98)
- TI Analog HandbookDokumen101 halamanTI Analog HandbookJenory DenemyBelum ada peringkat
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDari EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryPenilaian: 3.5 dari 5 bintang3.5/5 (231)
- LogmakDokumen2 halamanLogmakYavuz DanisBelum ada peringkat
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDari EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RacePenilaian: 4 dari 5 bintang4/5 (895)
- Radio 25 E1 Lec 10 MSK RadiologyDokumen3 halamanRadio 25 E1 Lec 10 MSK RadiologyYavuz DanisBelum ada peringkat
- The Little Book of Hygge: Danish Secrets to Happy LivingDari EverandThe Little Book of Hygge: Danish Secrets to Happy LivingPenilaian: 3.5 dari 5 bintang3.5/5 (400)
- (OS 213) LEC 03 Review of Normal Lung Structure and FunctionDokumen8 halaman(OS 213) LEC 03 Review of Normal Lung Structure and FunctionYavuz DanisBelum ada peringkat
- Shoe Dog: A Memoir by the Creator of NikeDari EverandShoe Dog: A Memoir by the Creator of NikePenilaian: 4.5 dari 5 bintang4.5/5 (537)
- 2016 May - NCDokumen36 halaman2016 May - NCYavuz DanisBelum ada peringkat
- Never Split the Difference: Negotiating As If Your Life Depended On ItDari EverandNever Split the Difference: Negotiating As If Your Life Depended On ItPenilaian: 4.5 dari 5 bintang4.5/5 (838)
- (Os 213) Lec 05.2 Drugs For RtiDokumen1 halaman(Os 213) Lec 05.2 Drugs For RtiYavuz DanisBelum ada peringkat
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDari EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FuturePenilaian: 4.5 dari 5 bintang4.5/5 (474)
- (OS 213) LEC 13 Paragonimus Westermani (A)Dokumen4 halaman(OS 213) LEC 13 Paragonimus Westermani (A)Yavuz DanisBelum ada peringkat
- Grit: The Power of Passion and PerseveranceDari EverandGrit: The Power of Passion and PerseverancePenilaian: 4 dari 5 bintang4/5 (588)
- (OS 213) LEC36 CVS Course SummaryDokumen12 halaman(OS 213) LEC36 CVS Course SummaryYavuz DanisBelum ada peringkat
- (OS 213) LEC 03 Review of Normal Lung Structure and FunctionDokumen8 halaman(OS 213) LEC 03 Review of Normal Lung Structure and FunctionYavuz DanisBelum ada peringkat
- The Emperor of All Maladies: A Biography of CancerDari EverandThe Emperor of All Maladies: A Biography of CancerPenilaian: 4.5 dari 5 bintang4.5/5 (271)
- (Os 213) Pictotrans Ws 02 - Ecg Skills Enhancement (A)Dokumen16 halaman(Os 213) Pictotrans Ws 02 - Ecg Skills Enhancement (A)Yavuz DanisBelum ada peringkat
- On Fire: The (Burning) Case for a Green New DealDari EverandOn Fire: The (Burning) Case for a Green New DealPenilaian: 4 dari 5 bintang4/5 (74)
- (OS 213) LEC 15 Surgery For Peripheral Vascular Diseases I (B)Dokumen8 halaman(OS 213) LEC 15 Surgery For Peripheral Vascular Diseases I (B)Yavuz DanisBelum ada peringkat
- Team of Rivals: The Political Genius of Abraham LincolnDari EverandTeam of Rivals: The Political Genius of Abraham LincolnPenilaian: 4.5 dari 5 bintang4.5/5 (234)
- 5 Medicine OSCE Collection: By: Fatimah Al-IbrahimDokumen69 halaman5 Medicine OSCE Collection: By: Fatimah Al-IbrahimJim JordenBelum ada peringkat
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDari EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaPenilaian: 4.5 dari 5 bintang4.5/5 (266)
- Diagnostic Procedures in Ophthalmology Full ColourDokumen488 halamanDiagnostic Procedures in Ophthalmology Full ColourAnquito100% (4)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDari EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersPenilaian: 4.5 dari 5 bintang4.5/5 (344)
- (OS 213) LEC 15 Pneumonia (B) - 1Dokumen7 halaman(OS 213) LEC 15 Pneumonia (B) - 1Yavuz DanisBelum ada peringkat
- Rise of ISIS: A Threat We Can't IgnoreDari EverandRise of ISIS: A Threat We Can't IgnorePenilaian: 3.5 dari 5 bintang3.5/5 (137)
- (Os 213) Lec 09 TB Dots (A)Dokumen2 halaman(Os 213) Lec 09 TB Dots (A)Yavuz DanisBelum ada peringkat
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDari EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyPenilaian: 3.5 dari 5 bintang3.5/5 (2259)
- (OS 213) LEC 10 Rheumatic Fever and RHD (B)Dokumen6 halaman(OS 213) LEC 10 Rheumatic Fever and RHD (B)Yavuz DanisBelum ada peringkat
- (OS 213) LAB 03 Paragonimus Westermani (A)Dokumen3 halaman(OS 213) LAB 03 Paragonimus Westermani (A)Yavuz DanisBelum ada peringkat
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDari EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You ArePenilaian: 4 dari 5 bintang4/5 (1090)
- (OS 213) LEC 03 Drugs Acting On The Respiratory System (1) - 1Dokumen16 halaman(OS 213) LEC 03 Drugs Acting On The Respiratory System (1) - 1Yavuz DanisBelum ada peringkat
- RADIO 250 (8) LEC 08 Genitourinary Pelvis RadiologyDokumen14 halamanRADIO 250 (8) LEC 08 Genitourinary Pelvis RadiologyYavuz DanisBelum ada peringkat
- (OS 213) CASE 01 Case PresentationsDokumen3 halaman(OS 213) CASE 01 Case PresentationsYavuz DanisBelum ada peringkat
- The Unwinding: An Inner History of the New AmericaDari EverandThe Unwinding: An Inner History of the New AmericaPenilaian: 4 dari 5 bintang4/5 (45)
- (OS 213) LAB 03 Paragonimus Westermani (B) - 2Dokumen3 halaman(OS 213) LAB 03 Paragonimus Westermani (B) - 2Yavuz DanisBelum ada peringkat
- Radio 250 (8) Lec 05 Gi RadiologyDokumen11 halamanRadio 250 (8) Lec 05 Gi RadiologyYavuz Danis100% (1)
- (OS 213) LEC 09 Physical Diagnosis of The Respiratory System (B) - 2Dokumen8 halaman(OS 213) LEC 09 Physical Diagnosis of The Respiratory System (B) - 2Yavuz DanisBelum ada peringkat
- (OS 213) LEC 11 Viral and Fungal Diseases of The Lung (A)Dokumen7 halaman(OS 213) LEC 11 Viral and Fungal Diseases of The Lung (A)Yavuz DanisBelum ada peringkat
- RADIO 250 (8) LEC 09 Musculoskeletal RadiologyDokumen4 halamanRADIO 250 (8) LEC 09 Musculoskeletal RadiologyYavuz DanisBelum ada peringkat
- RADIO 250 (8) LEC 11 Introduction To Interventional RadiologyDokumen6 halamanRADIO 250 (8) LEC 11 Introduction To Interventional RadiologyYavuz DanisBelum ada peringkat
- Radio 250 E1 Lec 01 Intro To Radiology and RadioprotectionDokumen6 halamanRadio 250 E1 Lec 01 Intro To Radiology and RadioprotectionYavuz DanisBelum ada peringkat
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Dari EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Penilaian: 4.5 dari 5 bintang4.5/5 (121)
- (OS 213) LEC 10 Rheumatic Fever and RHD (B)Dokumen6 halaman(OS 213) LEC 10 Rheumatic Fever and RHD (B)Yavuz DanisBelum ada peringkat
- Gallop RhythmDokumen2 halamanGallop RhythmMuhammad SulamanBelum ada peringkat
- Cardiovascular DiseaseDokumen33 halamanCardiovascular Diseasejoyce lakshmanBelum ada peringkat
- Normal Adult 12-Lead ECGDokumen2 halamanNormal Adult 12-Lead ECGIlonaBelum ada peringkat
- Wide QRS Complex TachyarrhythmiaDokumen36 halamanWide QRS Complex TachyarrhythmiaMaruliBelum ada peringkat
- Chest Pain Protocol For ER DoctorsDokumen4 halamanChest Pain Protocol For ER DoctorsSaleh Abu wardaBelum ada peringkat
- Atrial Myxoma As A Cause of Stroke: Case Report and DiscussionDokumen4 halamanAtrial Myxoma As A Cause of Stroke: Case Report and DiscussionNaveedBelum ada peringkat
- Cardiac Emergency PDFDokumen45 halamanCardiac Emergency PDFnikenBelum ada peringkat
- Acute Medicine 4th EdDokumen660 halamanAcute Medicine 4th EdEmmanuel Ortiz100% (4)
- Revascularization in Stable Coronary Artery Disease Review BMJDokumen17 halamanRevascularization in Stable Coronary Artery Disease Review BMJucicardiocovid ocgnBelum ada peringkat
- Penyakit-Penyakit Jantung Kongenital.: M.S.GanesanDokumen63 halamanPenyakit-Penyakit Jantung Kongenital.: M.S.GanesanSyukri SamsudinBelum ada peringkat
- Her Body and Other Parties: StoriesDari EverandHer Body and Other Parties: StoriesPenilaian: 4 dari 5 bintang4/5 (821)
- All Past Rounds Cardio MCQs AlexandriaDokumen37 halamanAll Past Rounds Cardio MCQs AlexandriaMahmoud Abouelsoud100% (1)
- Sas 27Dokumen2 halamanSas 27Leaflor Ann ManghihilotBelum ada peringkat
- ECG Masters' Collection Volume 2Dokumen218 halamanECG Masters' Collection Volume 2Илија Радосављевић100% (1)
- Localization On ECG: Myocardial Ischemia / Injury / InfarctionDokumen56 halamanLocalization On ECG: Myocardial Ischemia / Injury / InfarctionduratulfahliaBelum ada peringkat
- CVS Examination 3rd MBDokumen30 halamanCVS Examination 3rd MBsnowlover boyBelum ada peringkat
- 3 Manifestasi Klinik StrokeDokumen35 halaman3 Manifestasi Klinik StrokeDea100% (1)
- CV of Invited Speaker: Title Prof. Mr. Mrs. Ms. Nationality Indonesia Position: OrganizationDokumen3 halamanCV of Invited Speaker: Title Prof. Mr. Mrs. Ms. Nationality Indonesia Position: OrganizationKM Habil SBelum ada peringkat
- Ecg Quick Guide PDFDokumen7 halamanEcg Quick Guide PDFansarijavedBelum ada peringkat
- Medical Case StudiesDokumen39 halamanMedical Case Studieszozo002Belum ada peringkat
- Bol U Grudima - 2Dokumen41 halamanBol U Grudima - 2Nenad RadosavljevićBelum ada peringkat
- Clinical Trials in Hypertension PDFDokumen674 halamanClinical Trials in Hypertension PDFmildariantyBelum ada peringkat
- Critical Limb IschemiaDokumen11 halamanCritical Limb IschemiaAmalia Hendar PangestutiBelum ada peringkat
- ACLS 2015 Algorithm and Anesthesia ACLS PDFDokumen14 halamanACLS 2015 Algorithm and Anesthesia ACLS PDFTaufiqurrahman RizkiBelum ada peringkat
- Daftar PustakaDokumen3 halamanDaftar PustakaFaisal RahmanBelum ada peringkat
- The ECG Made Easy by John R. HamptonDokumen1 halamanThe ECG Made Easy by John R. HamptonLpBelum ada peringkat
- Clinical Indications, Treatment and Current PracticeDokumen14 halamanClinical Indications, Treatment and Current PracticefadmayulianiBelum ada peringkat
- Xavier University-Ateneo de CagayanDokumen3 halamanXavier University-Ateneo de CagayanMariano MarbellaBelum ada peringkat
- MKSAP 17 Audio Companion 2015 - PDF File - Cardiology PDFDokumen68 halamanMKSAP 17 Audio Companion 2015 - PDF File - Cardiology PDFPaul StatoBelum ada peringkat
- Percussion FindingsDokumen12 halamanPercussion FindingsMonica JamesBelum ada peringkat
- Chapter 27 - Management of Patients With Dysrhythmias and ConductionDokumen8 halamanChapter 27 - Management of Patients With Dysrhythmias and ConductionMichael Boado100% (1)