Gravity FAIRER
Diunggah oleh
Josh GreerHak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Gravity FAIRER
Diunggah oleh
Josh GreerHak Cipta:
Format Tersedia
Magnetic Resonance Imaging 19 (2001) 929 935
Gravity-dependent perfusion of the lung demonstrated with the
FAIRER arterial spin tagging method
Shella D. Keilholza, Jack Knight-Scottb, John M. Christopherb,
Vu M. Maic, Stuart S. Berr a,b,*
a
Engineering Physics Program, School of Engineering, University of Virginia, Charlottesville, VA 22908, USA
b
Department of Radiology, University of Virginia Health Sciences Center, Charlottesville, VA 22908, USA
c
Department of Radiology, Beth Israel Deaconess Medical Center and Harvard Medical School, Boston, MA 02215, USA
Received 11 January 2001; accepted 17 June 2001
Abstract
Magnetic resonance imaging of lung perfusion using an arterial spin tagging (AST) sequence called flow sensitive alternating inversion
recovery with an extra RF pulse (FAIRER) was performed in the left and right lateral positions in five volunteers. Coronal slices were
obtained and the average intensity of each lung was measured. In both positions, an increase in the intensity of the dependent lung was found
(229% for left lateral, 40% for right lateral). No change was seen along an isogravitational plane. Lung volumes were measured in each
position to account for the compression of the lungs by the heart. This effect was found to be symmetric and did not contribute to the
perfusion gradient. This demonstrates that AST is sensitive to gravity-dependent perfusion gradients in the lung. 2001 Elsevier Science
Inc. All rights reserved.
Keywords: Lung MRI; Pulmonary perfusion; Gravity-dependent perfusion
1. Introduction
The effects of gravity are greater in the pulmonary circulation than in the rest of the body because the pressures in
the left atrium and pulmonary artery are much lower than
systemic vascular pressures. At total lung capacity in the
upright position, typical pulmonary arterial pressure ranges
from 4 cm H2O at the top of the lung to 34 cm H2O at the
bottom. The higher arterial pressure increases the transmural pressure, which distends the tubes and lowers resistance
to flow. This leads to an increase in perfusion in the dependent part of the lung [1].
Although recent magnetic resonance imaging (MRI)
studies have successfully imaged lung perfusion using both
exogenous contrast enhancement and arterial spin tagging
(AST) [6 8], scintigraphy is the gold standard clinical
method for imaging lung perfusion in obstructive pulmonary disease [25]. Compared to scintigraphy, MRI offers
* Corresponding author. Tel.: 1-804-924-5096; fax: 1-804-9249435.
E-mail address: berr@virginia.edu (S.S. Berr).
the advantages of high spatial resolution and no ionizing
radiation. An additional advantage of AST is that no exogenous contrast agent is needed. Instead, magnetically labeled blood water is used as an endogenous, freely diffusible tracer. This reduces both the expense of the exam and
the risk to the patient.
An increase in perfusion in the direction of gravity has
been observed in the supine position using positron emission tomography (PET) [9]. Contrast-enhanced MRI has
also been successful in demonstrating the gravitational dependence of perfusion in the supine and prone positions
[10]. Recent work by Mai et al [6] suggests that similar
gravitational effects influence the image intensity in a perfusion weighted image obtained by AST. In this study we
investigated the sensitivity of a noninvasive arterial spin
tagging method called flow sensitive alternating inversion
recovery with an extra RF-pulse (FAIRER) [6,7,11] to gravitational perfusion changes in subjects placed in a lateral
position. FAIRER has been shown to be capable of measuring pulmonary perfusion quantitatively [12]. These perfusion variations are of interest because they may help us
understand the complex interaction of gravity, anatomy, and
microvascular pressure that controls perfusion in the lung,
0730-725X/01/$ see front matter 2001 Elsevier Science Inc. All rights reserved.
PII: S 0 7 3 0 - 7 2 5 X ( 0 1 ) 0 0 4 1 6 - 7
930
S.D. Keilholz et al. / Magnetic Resonance Imaging 19 (2001) 929 935
which may in turn lead to greater understanding of chronic
lung diseases such as asthma and emphysema.
2. Materials and Methods
All experiments were performed on a Magnetom VISION 1.5 T MR imaging system (Siemens Medical Systems, Iselin, NJ, USA) with maximum gradient strengths
and slew rates of 25 mT/m and 83 mT/m/s, respectively. A
four-element receiver body phased array coil was used for
all images. Five volunteers (one male and four females)
were imaged using procedures approved by the University
of Virginia Human Investigation Committee. Subjects with
narrow shoulders were chosen to facilitate imaging in the
lateral position. Ages ranged from 24 to 43, with a mean age
of 30.2. Informed consent was obtained before each study.
All volunteers were studied in both the left and right lateral
position. One was imaged twice, first as part of a preliminary study and later to obtain additional slices, and data
from both sessions were used in this study. All were nonsmokers.
Subjects were positioned in the lateral position, and localizer images of the lung were acquired in the transverse,
coronal, and sagittal planes, using a FLASH sequence with
the following parameters: TE 6 ms, TR 15 ms, flip angle 30,
slice thickness 10 mm, FOV 450 mm, matrix size 128 phase
encode steps (zero filled to 256) by 256 readout steps, 1
acquisition. These images were used to choose posterior
coronal slices, avoiding the heart, where flow causes significant artifacts. One to three slices were chosen, depending
on the thickness of the subjects chest and the position of the
heart. Each slice was then imaged with the FAIRER perfusion sequence, using a half Fourier acquisition single shot
turbo spin echo (HASTE) readout and the following parameters: effective TE 36 ms, interecho time 4.5 ms, matrix size
128 phase encode steps (zero filled to 256) by 256 readout
steps, slice thickness 10 mm, FOV 500 mm, 1 acquisition.
We routinely use an FOV of 500 mm for lung studies
because it allows us to accommodate subjects with large
torsos without introducing wraparound into the image. Cardiac triggered tag and control images were acquired in a
single breathhold of approximately 10 seconds at end-expiration, when the SNR of the lungs is greatest due to the
increased density of the tissue. Complex subtraction of the
real and imaginary parts of the tag image signal from the
control image signal was used to obtain the magnitude
perfusion image. Immediately after the completion of the
perfusion sequence, the subject was asked to lie on the
opposite side and the procedure was repeated. A water
phantom was also imaged using the same protocol to assess
the effects of surface coil inhomogeneity.
The cardiac triggering scheme used with the FAIRERHASTE sequence is shown in Fig. 1. Acquisition of the
image was triggered by the R-wave of the cardiac QRS
complex. The delay after the R-wave, TECG, was set to 500
Fig. 1. Representation of the cardiac triggering scheme. TI is chosen to be
the length of one heart cycle so that the tag and acquisition occur at the
same point in the cardiac cycle. This reduces motion artifacts. Tecg, the
delay between the R-wave and the tagging pulse, is chosen to place the
image tag and acquisition in diastole.
ms to place the image acquisition in diastole. The inversion
time, TI, was set to the length of one heart cycle (750 to
1100 ms). This caused the inversion preparation and the
image acquisition to occur at the same point in the cardiac
cycle, ensuring that the imaging and reinversion slices were
centered at the same location. It also allowed sufficient time
for the inflow of tagged spins.
For each volunteer, the average intensity of the whole
lung was measured using standard analysis software on the
Siemens scanner. A cursor was used to trace the outer edge
of the lung, avoiding artifacts caused by motion of the
diaphragm, and the program returned an average intensity
value for the region enclosed. The intensity of the noise was
measured by using the same program to draw a roughly
circular area in a region as far from the tissue as possible.
Signal to noise ratios (SNR) from the left and right lungs
were calculated and compared for each slice using a paired
t-test with 0.05. A p value of less than 0.01 was
considered significant. Two intensity profiles across each
slice were also measured, one parallel to the spine and
approximately isogravitational, and another along the direction of gravity, and the results were compared.
To help separate volume effects from perfusion effects,
we measured the volume of each lung in one subject in both
lateral positions and in the supine position by taking contiguous, 10 mm slices through the entire lung. The area of
the lung in each slice was measured, and the slice areas were
totaled to give an area for the entire lung that was proportional to the volume of the lung.
3. Results
Mai et al. [6] have shown what appears to be a gravitydependent perfusion gradient in the supine position in
FAIRER-HASTE images. To verify that the gradient is
indeed due to gravity, we examined sagittal slices from both
the supine and prone positions (Fig. 2). As expected, the
region of maximum enhancement moved from the posterior
portion of the lung to the anterior portion. An isogravitational coronal slice (Fig. 3) shows no perfusion gradient. In
the left lateral position, a large difference in intensity in the
S.D. Keilholz et al. / Magnetic Resonance Imaging 19 (2001) 929 935
Fig. 2. (a) Sagittal slice taken in the supine position. Increased intensity is
visible in the posterior parts of the lung. (b) Sagittal slice taken in the prone
position. Increased intensity is now visible in the anterior region of the lung.
perfusion-weighted image was observed between the left
and right lungs (Fig. 4a). To quantify these differences,
eleven coronal slices from the five volunteers were analyzed
(Fig. 5a). The average right (up gravity) lung SNR for all
slices was 4.8 1.1, while the average for the left (down
gravity) lung was 15.8 6.0, an increase of 229%. The
average ratio of left lung SNR to right lung SNR was 3.3
0.9. The difference between the two ratios was significant
(p 0.0001).
In the right lateral position, a much smaller difference in
931
Fig. 3. Coronal slice taken in supine position. No perfusion gradient is
visible. The dark bands in the right lung may correspond to the divisions
between lobes.
intensity was observed (Fig. 4b). Eleven coronal slices were
analyzed (Fig. 5b). The average left (up gravity) lung SNR
for all slices was 6.7 3.1, while the average right (down
gravity) lung SNR was 9.4 3.4, an increase of 40%. The
average ratio of right lung SNR to left lung SNR was 1.5
0.4. The paired t-test found a significant difference (p
0.0015). The results for coronal slices in the left and right
lateral positions are summarized in Table 1.
Transverse slices were also obtained from some volunteers (Fig. 6). The results were similar to those obtained
from the coronal slices. Three slices were analyzed from the
left lateral position, and two from the right lateral (Fig. 7).
Fig. 4. (a) Demonstration of a perfusion gradient in the left lateral position. The left lung has higher intensity than the right lung in both parenchyma and
vessels. (b) Demonstration of a perfusion gradient in the right lateral position. The right lung has higher intensity than the left lung, though the difference
is not as pronounced as in (a). The bright band at the bottom of the right lung is caused by incomplete subtraction of the diaphragm due to respiratory motion.
932
S.D. Keilholz et al. / Magnetic Resonance Imaging 19 (2001) 929 935
Fig. 5. (a) A comparison of average SNR for the left (white) and right (black) lungs from coronal slices in the left lateral position. The numbers along the
x-axis indicate the volunteers from whom the images were obtained. (b) A comparison of average SNR for the left (white) and right (black) lungs from coronal
slices in the right lateral position. The difference is much smaller than in the left lateral position.
The average ratio of upper lung SNR to lower lung SNR
was 4.2 1.7 in the left lateral position and 2.1 0.7 in the
right lateral position. No t-test was run due to the small
sample size. The results are summarized in Table 2.
Profiles were measured along an isogravitational line for
both coronal and transverse slices (Figs. 8a and 9a) and
compared to profiles measured along the gravitationally
dependent line (Figs. 8b and 9b). The isogravitational profiles were relatively constant, as would be expected.
Table 1
Comparison of the average SNR of left and right lungs in left and right
lateral positions for coronal slices
Left Lateral
Right Lateral
Right Lung
Left Lung
Ratio
4.8 1.1
9.4 3.4
15.8 6.0 3.3 0.9
6.7 3.1 1.5 0.4
Percent Difference
229%
40%
No statistically significant difference in sensitivity between the upper and lower coils was found when imaging
the water phantom. The SNR for region of the phantom
nearest the upper coil was 1.3% greater than the SNR for the
part of the phantom nearest the lower coil.
The results of our lung volume measurements showed
that the compression of the left lung by the heart in the left
lateral position was equal to the compression of the right
lung by the heart in the right lateral position, as summarized
in Table 3.
4. Discussion
Systemic arterial pressure is measured with reference to
the pressure at the level of the heart. In the lungs of a
normal, upright subject, the arterial pressure falls by 1 cm
H2O for each centimeter above the left atrium and rises by
S.D. Keilholz et al. / Magnetic Resonance Imaging 19 (2001) 929 935
933
Fig. 6. (a) Transverse slice demonstrating increased perfusion in the left lung in the left lateral position. (b) Transverse slice showing increased perfusion in
the right lung in the right lateral position. Again, the increase is not as pronounced as in (a).
1 cm H2O for each centimeter below the left atrium. As a
consequence, the pulmonary perfusion of a normal subject
can be divided into three zones. In the highest portion of the
lung, alveolar pressure exceeds both the venous and arterial
pressures and no flow occurs. This area is small or nonexistent in normal lungs. In the next lower zone, pulmonary
arterial pressure exceeds alveolar pressure and perfusion is
regulated by the compression of the capillaries by the alveolar pressure. In the lowest part of the lung, both arterial and
venous pressures exceed alveolar pressure, and perfusion is
regulated by the transmural pressure [1]. Similar differences
in pulmonary arterial pressure exist in the supine position,
and the associated perfusion gradients have been observed
[9,10].
Mai et al. [6] have demonstrated what appears to be a
gravity-dependent perfusion gradient in the supine position
using FAIRER-HASTE. To further test the sensitivity of
FAIRER-HASTE and complete our survey of the effects of
gravity on pulmonary perfusion, we examined perfusion in
the lateral positions. In addition to the usual differences in
pulmonary arterial pressure, other effects that may contribute to perfusion variations in a lateral position include
changes in the orientation of the heart and the blood vessels,
compression of the lungs, and preferential flow due to the
nearly vertical position of the main pulmonary arteries. It is
interesting to note that in our results, no perfusion gradient
is observed across either lung. Rather, the lower lung is
more intense than the upper. This difference in intensity is
more pronounced in the left lateral position, which may be
due to a volumetric effect caused by the compression of the
lung by the heart or a geometric effect caused by the
individuals anatomy.
It is well known from x-ray examinations that the heart
changes position rather dramatically when a patient is
moved from an upright to a lateral position. We surmised
that the position of the heart causes a change in the volume
of the lung so that in the left lateral position we see both
compression and gravitational effects, while in the right
lateral position we see only the gravitational effects. This
volume effect is similar to the increased perfusion seen in
images taken at end-expiration, compared to those taken at
end-inspiration. Since the volumes were consistent, this
implies that the difference observed in the gradient between
left and right laterals is not due to compression of the lung
by the heart. Though we only studied volume measurements
from one subject, nuclear medicine experiments corroborate
our findings [13]. The possibility remains that in the lateral
position, the distortion of the pulmonary arteries by the
Table 2
Comparison of the average SNR of the left and right lungs in left and
right lateral positions for transverse slices
Fig. 7. Comparison of average SNR for left (white) and right (black) lungs
from transverse slices in the left lateral (a) and right lateral (b) positions.
Again, the difference in SNR between the lungs is larger in the left lateral
position.
Left Lateral
Right Lateral
Right Lung
Left Lung
Ratio
3.7 4.1
9.1 8.7
12.2 7.4 4.2 1.7
4.6 2.8 2.1 0.7
Percent Difference
235%
99%
934
S.D. Keilholz et al. / Magnetic Resonance Imaging 19 (2001) 929 935
Table 3
Comparison of the volume of the left and right lungs in three positions.
The change in volume corresponds to the compression of the lung by
the heart. The compression of the left lung in the left lateral position is
approximately equal to the compression of the right lung in the right
lateral position
Left Lateral
Right Lateral
Supine
Fig. 8. (a) Intensity profile for an isogravitational line in a left lateral
coronal slice. The spike near 100 corresponds to the bright band caused by
motion of the diaphragm. No gradient is apparent. (b) Intensity profile for
a gravity-dependent line in a left lateral coronal slice. The difference in
intensity between the left and right lungs is clearly shown.
change in the hearts orientation may lead to preferential
flow to one side or the other. The pulmonary trunk begins at
the right ventricle and splits into the left and right pulmonary arteries, which carry blood to the left and right lungs.
It is possible that, as the heart shifts position, the junction of
the trunk and the two arteries becomes distorted, changing
the characteristics of the blood flow pattern. This type of
distortion could also happen in the smaller arteries of the
lungs, since our method only measures regional perfusion
rather than total lung perfusion.
Right Lung (cm3)
Left Lung (cm3)
Total (cm3)
1570
1230
1270
1190
1510
1050
2760
2740
2320
There are several nuclear medicine studies that examined
perfusion in the lateral position [14 19], but they neither
confirm nor rule out the difference in the perfusion gradient
between the right and left lateral position that we observed.
Two studies dealt only with the right lateral position [14,15]
and one did not distinguish between left and right lateral
positions [16]. Of those that studied both left and right
lateral positions, one looked at perfusion only in the right
lung [17] and another had different subjects studied in each
position [18]. Only in one study was a subject studied in
both positions [19]. It did not show a significant difference
in the perfusion gradient in the two positions. However, the
sample size was very small (n 1).
Another possibility is that the difference between the
perfusion gradient in the two positions may be due to our
measurement method in some way we cannot yet explain.
AST studies acquire slightly different information than nuclear studies. For example, in the papers cited above, perfusion effects were separated from volume effects by dividing the perfusion signal by the regional alveolar volume. In
AST, the volume effects contribute. However, we have
found no indication that the volume effects contribute differently in the left and right lateral positions. Also, we
examine perfusion from a single slice of the lung, while the
nuclear studies obtained data for the whole lung. Perhaps a
regional perfusion difference is involved.
These results demonstrate FAIRERs sensitivity to perfusion changes in the lung. The results also suggest that
subject positioning may be influential in MR perfusion
studies of the lung using AST. A drawback of AST lung
imaging is that the SNR is low, particularly in the anterior
portions of the lung. Positioning the patient so that the area
of interest is down-gravity may increase SNR and improve
visibility of perfusion defects.
Acknowledgments
Fig. 9. (a) Intensity profile for an isogravitational line in a left lateral
transverse slice. No intensity gradient is apparent. (b) Intensity profile for
a gravity-dependent line in a left lateral transverse slice. The intensity on
the left is higher than that on the right, though the profile is complicated by
the inclusion of flow artifacts from major vessels.
This work was supported in part by an NIH grant R21
CA89633 (SSB), and a Department of Defense NDSEG
Fellowship (SDK). The authors thank Talissa Altes, MD,
for her assistance.
S.D. Keilholz et al. / Magnetic Resonance Imaging 19 (2001) 929 935
References
[1] Berne RM, Levy MN. Physiology. Mosby-Year Book Inc. St. Louis,
MO. 1993.
[2] Orphanidou D, Hughes JMB, Myers MJ, Al-Suhali AR, Henderson B.
Tomography of regional ventilation and perfusion using krypton 81m
in normal subjects and asthmatic patients. Thorax 1986;41:54251.
[3] West JB, Dollery CT. Distribution of blood flow and ventilationperfusion ratio in the lung, measured with radioactive CO2. J Appl
Physiol 1960;15:40510.
[4] Ball WC, Stewart PB, Newsham LGS, Bates DV. Regional pulmonary function studies with 133xenon. J Clin Invest 1962;41:519 31.
[5] Treppo S, Mijailovich SM, Venegas JG. Contributions of pulmonary
perfusion and ventilation to heterogeneity in V(A)/Q measured by
PET. J Appl Physiol 1997;82:116376.
[6] Mai VM, Hagspiel KD, Christopher JM, et al. Perfusion imaging of
the human lung using flow-sensitive alternating inversion recovery
with an extra radiofrequency pulse (FAIRER). Magn Reson Imag
1999;17:355 61.
[7] Mai VM, Berr SS. MR perfusion imaging of pulmonary parenchyma
using pulsed arterial spin labeling techniques: FAIRER and FAIR.
JMRI 1999;9:4837.
[8] Hatabu H, Gaa J, Kim D, Li W, Prasad PV, Edelman RR. Pulmonary
perfusion: qualitative assessment with dynamic contrast-enhanced
MRI using ultra-short TE and inversion recovery turboFLASH. Magn
Reson Med 1996;36:503 8.
[9] Brudin LH, Rhodes CG, Valind SO, Jones T, Hughes JMB. Interrelationships between regional blood flow, blood volume, and ventilation in supine humans. J Appl Physiol 1994;76:120510.
[10] Stock KW, Chen Q, Levin D, Hatabu H, Edelman RR. Demonstration
of gravity-dependent lung perfusion with contrast-enhanced magnetic
resonance imaging. JMRI 1999;9:557 61.
935
[11] Mai VM, Knight-Scott J, Kallmes DF, et al. Quantification of steadystate perfusion rates using flow-sensitive alternating inversion recovery with an extra radiofrequency pulse (FAIRER). Proceedings of the
6th ISMRM (Abstracts), Sydney, Australia; 1998:1215.
[12] Mai VM, Chen Q, Edelman RR. Absolute quantification of pulmonary perfusion rates using flow-sensitive alternating inversion
recovery with an extra radiofrequency pulse (FAIRER). Proceedings of the 8th ISMRM, Abstract number 171, Denver, Colorado;
2000.
[13] Kaneko K, Milic-Emili J, Dolovich MB, Dawson A, Bates DV.
Regional distribution of ventilation and perfusion as a function of
body position. J Appl Physiol 1966;21:76777.
[14] Landmark SJ, Knopp TJ, Rehder K, Sessler AD. Regional pulmonary
perfusion and V/Q in awake and anesthetized-paralyzed man. J Appl
Physiol 1977;43:9931000.
[15] Chevrolet JC, Martin JG, Flood R, Martin RR, Engel LA. Topographical ventilation and perfusion distribution during IPPB in the lateral
posture. Am Rev Resp Dis 1978;118:84754.
[16] Bhuyan U, Peters AM, Gordon I, Davies H, Helms P. Effects of
posture on the distribution of pulmonary ventilation and perfusion in
children and adults. Thorax 1989;44:480 4.
[17] Tanaka M, Fujii T, Hirayama J, Okubo S, Sekiguchi M. Estimation of
pulmonary hypertension by perfusion lung scintigraphy: gravitational
effect of postural changes between the lateral decubitus positions. Eur
J Nucl Med 1990;17:320 6.
[18] Amis TC, Jones HA, Hughes JMB. Effect of posture on inter-regional
distribution of pulmonary perfusion and VA/Q ratios in man. Resp
Physiol 1984;56:169 82.
[19] Kaneko K, Milic-Emil J, Dolovich MB, Dawson A, Bates DV. Regional distribution of ventilation and perfusion as a function of body
position. J Appl Physiol 1966;21:76777.
Anda mungkin juga menyukai
- MRI Clinical Application 1Dokumen17 halamanMRI Clinical Application 1Alberto AlbertoBelum ada peringkat
- IHD Vitamin CDokumen17 halamanIHD Vitamin CFarrah ErmanBelum ada peringkat
- 3D Transthoracic Echocardiography Provides Accurate Cross-Sectional Area of The RV Outflow Tract - 1Dokumen3 halaman3D Transthoracic Echocardiography Provides Accurate Cross-Sectional Area of The RV Outflow Tract - 1Thumper KatesBelum ada peringkat
- Atlas of Cardiovascular Computed Tomography - Imaging Companion To Braunwald's Heart Disease, 1E (2010) (PDF) (UnitedVRG) PDFDokumen270 halamanAtlas of Cardiovascular Computed Tomography - Imaging Companion To Braunwald's Heart Disease, 1E (2010) (PDF) (UnitedVRG) PDFboghezloredanaBelum ada peringkat
- Ijcc 4 098Dokumen9 halamanIjcc 4 098ASIK1144Belum ada peringkat
- 心脏超声基础知识(超声心动图基础知识)Dokumen12 halaman心脏超声基础知识(超声心动图基础知识)Xin HuangBelum ada peringkat
- Ngo 2016Dokumen11 halamanNgo 2016Carlos Daniel AliagaBelum ada peringkat
- Echo 6Dokumen10 halamanEcho 6Indera VyasBelum ada peringkat
- Lobo 2018Dokumen9 halamanLobo 2018Carlos Daniel AliagaBelum ada peringkat
- LN3Dokumen6 halamanLN3Haseeb QuadriBelum ada peringkat
- Quantification of Stenotic Mitral Valve Area With Magnetic Resonance Imaging and Comparison With Doppler UltrasoundDokumen5 halamanQuantification of Stenotic Mitral Valve Area With Magnetic Resonance Imaging and Comparison With Doppler UltrasoundRyanBelum ada peringkat
- 1 s2.0 S0735109786800183 Main PDFDokumen252 halaman1 s2.0 S0735109786800183 Main PDFdangthieuhoiBelum ada peringkat
- CT Angiography of The Lower Extremities The Peripheral Vascular System Presents Unique Imaging ChallengesDokumen7 halamanCT Angiography of The Lower Extremities The Peripheral Vascular System Presents Unique Imaging ChallengesDavid Puyó100% (1)
- Article PDFDokumen7 halamanArticle PDFOscarBelum ada peringkat
- Reifferscheid 2011Dokumen9 halamanReifferscheid 2011Carlos Daniel AliagaBelum ada peringkat
- M-Mode Echocardiography in DogsDokumen10 halamanM-Mode Echocardiography in DogsTactvisBelum ada peringkat
- Role of Transesophageal Echocardiography (Tee) in Cardiac SurgeryDokumen35 halamanRole of Transesophageal Echocardiography (Tee) in Cardiac SurgeryIJAR JOURNALBelum ada peringkat
- Derivation of Respiratory Signals From Multilead EDokumen12 halamanDerivation of Respiratory Signals From Multilead EFelipe Cavalcante da SilvaBelum ada peringkat
- The Potential For Undertaking Slow CT Using A Modern CT ScannerDokumen7 halamanThe Potential For Undertaking Slow CT Using A Modern CT ScannerAndreas RonaldBelum ada peringkat
- Mitral Valve Annular Downsizing Forces: Implications For Annuloplasty Device DevelopmentDokumen8 halamanMitral Valve Annular Downsizing Forces: Implications For Annuloplasty Device Developmentdiana25Belum ada peringkat
- 41-Article Text-73-1-10-20200503Dokumen6 halaman41-Article Text-73-1-10-20200503kusumayoga 16Belum ada peringkat
- Diagnostic Ultrasound For The Detection of Atherosclerotic Changes Inside Femoral Arteries of Lower LimbDokumen4 halamanDiagnostic Ultrasound For The Detection of Atherosclerotic Changes Inside Femoral Arteries of Lower LimbInternational Jpurnal Of Technical Research And ApplicationsBelum ada peringkat
- Imaging in Acute Respiratory Distress Syndrome: ReviewDokumen13 halamanImaging in Acute Respiratory Distress Syndrome: ReviewIva SeptianingsihBelum ada peringkat
- Original Article: Serratus Plane Block: A Novel Ultrasound-Guided Thoracic Wall Nerve BlockDokumen7 halamanOriginal Article: Serratus Plane Block: A Novel Ultrasound-Guided Thoracic Wall Nerve Blockandrew herringBelum ada peringkat
- Cavotricuspid Isthmus: Anatomy, Electrophysiology, and Long-Term OutcomeDokumen5 halamanCavotricuspid Isthmus: Anatomy, Electrophysiology, and Long-Term Outcomeapi-26166949Belum ada peringkat
- A Study and Optimization of Lumbar Spine X-Ray ImagingDokumen12 halamanA Study and Optimization of Lumbar Spine X-Ray ImagingMatt ParkmanBelum ada peringkat
- Pi Is 0894731703010198Dokumen5 halamanPi Is 0894731703010198Nag Mallesh RaoBelum ada peringkat
- Ultrasonographic Diagnosis of Median Arcuate Ligament Syndrome: A Report of Two CasesDokumen4 halamanUltrasonographic Diagnosis of Median Arcuate Ligament Syndrome: A Report of Two CasesMaria IszlaiBelum ada peringkat
- Inhomogeneities in Wall Stress Measured by Microergometry in The Heart Muscle in SituDokumen12 halamanInhomogeneities in Wall Stress Measured by Microergometry in The Heart Muscle in SituKiki D. RestikaBelum ada peringkat
- Effects of Incentive Spirometry On Respiratory Motion in Healthy Subjects Using Cine Breathing Magnetic Resonance ImagingDokumen6 halamanEffects of Incentive Spirometry On Respiratory Motion in Healthy Subjects Using Cine Breathing Magnetic Resonance ImagingNavajeevan PanthiBelum ada peringkat
- Two-Dimensional Cardiothoracic Ratio For Evaluation of Cardiac Size in German Shepherd DogsDokumen8 halamanTwo-Dimensional Cardiothoracic Ratio For Evaluation of Cardiac Size in German Shepherd DogsWerner AlbuquerqueBelum ada peringkat
- Hexeberg 1993Dokumen4 halamanHexeberg 1993CARLOS FRANCISCO MANTILLA MONTALVOBelum ada peringkat
- Electrocardiography: Selection The Positions Measuring LocationsDokumen14 halamanElectrocardiography: Selection The Positions Measuring LocationsSivaRaman JayaramanBelum ada peringkat
- Chest 1975 Capone 577 82Dokumen8 halamanChest 1975 Capone 577 82ativonBelum ada peringkat
- Influence of Cardiomegaly On Disordered Breathing During Exercise in Chronic Heart FailureDokumen8 halamanInfluence of Cardiomegaly On Disordered Breathing During Exercise in Chronic Heart FailurenadiaBelum ada peringkat
- Thoracic Ultrasound and Integrated ImagingDari EverandThoracic Ultrasound and Integrated ImagingFrancesco FelettiBelum ada peringkat
- Recurent EpistaxisDokumen3 halamanRecurent EpistaxisFongmeicha Elizabeth MargarethaBelum ada peringkat
- Cardiac Radiosurgery (CyberHeart™) For Treatment of Arrhythmia: Physiologic and Histopathologic Correlation in The Porcine ModelDokumen28 halamanCardiac Radiosurgery (CyberHeart™) For Treatment of Arrhythmia: Physiologic and Histopathologic Correlation in The Porcine ModelCureusBelum ada peringkat
- Hypertonic Saline Attenuates Cord Swelling and Edema in Experimental Cord Injury - Experimental (2009) PDFDokumen7 halamanHypertonic Saline Attenuates Cord Swelling and Edema in Experimental Cord Injury - Experimental (2009) PDFCoal CoalyBelum ada peringkat
- Intracardiac Echocardiography2Dokumen12 halamanIntracardiac Echocardiography2Salah AttaBelum ada peringkat
- Ce (Ra1) F (T) PF1 (Bmak) Pfa (Ak) PF2 (Pag)Dokumen4 halamanCe (Ra1) F (T) PF1 (Bmak) Pfa (Ak) PF2 (Pag)Jozhy Nugraha MahmudaBelum ada peringkat
- Electrical Impedance Tomography: Eduardo L.V. Costa, Raul Gonzalez Lima and Marcelo B.P. AmatoDokumen7 halamanElectrical Impedance Tomography: Eduardo L.V. Costa, Raul Gonzalez Lima and Marcelo B.P. Amatojorgeluis.unknownman667Belum ada peringkat
- Acquiring 4D Thoracic CT Scans Using A Multislice Helical MethodDokumen16 halamanAcquiring 4D Thoracic CT Scans Using A Multislice Helical MethodAndreas RonaldBelum ada peringkat
- Basic Physics of B-ModeDokumen12 halamanBasic Physics of B-ModeEd ShieldsBelum ada peringkat
- Erven 2011Dokumen8 halamanErven 2011Jussara FerreiraBelum ada peringkat
- Monte Carlo HeterogeneitiesDokumen6 halamanMonte Carlo HeterogeneitiesRamses HerreraBelum ada peringkat
- Broadband Discrete-Level Excitations For Improved Extraction of Information in Bioimpedance MeasurementsDokumen15 halamanBroadband Discrete-Level Excitations For Improved Extraction of Information in Bioimpedance MeasurementsThành PhạmBelum ada peringkat
- JurnalDokumen16 halamanJurnalsamuelionardiBelum ada peringkat
- Bondgraph Published CardioVascular 5Dokumen24 halamanBondgraph Published CardioVascular 5AhmedBelum ada peringkat
- 1 s2.0 S0741521495702881 MainDokumen12 halaman1 s2.0 S0741521495702881 MainRonald VillaBelum ada peringkat
- Manual Vibration Increases Expiratory Flow Rate Via Increased Intrapleural Pressure in Healthy Adults: An Experimental StudyDokumen5 halamanManual Vibration Increases Expiratory Flow Rate Via Increased Intrapleural Pressure in Healthy Adults: An Experimental StudyManuel Jesús Torres CaterianoBelum ada peringkat
- Echo Guidelines For Chamber QuantificationDokumen24 halamanEcho Guidelines For Chamber QuantificationOnon EssayedBelum ada peringkat
- Gambar Slowctlewis2009Dokumen12 halamanGambar Slowctlewis2009Andreas RonaldBelum ada peringkat
- Application Note - Pulmonary Hypertension and The VevoDokumen5 halamanApplication Note - Pulmonary Hypertension and The VevoVisualSonicsBelum ada peringkat
- Tema Seminar BiofluidicaDokumen2 halamanTema Seminar BiofluidicaClaudia MimiBelum ada peringkat
- Ajr 11 6559Dokumen4 halamanAjr 11 6559g1381821Belum ada peringkat
- Articol 2Dokumen6 halamanArticol 2Silviu Iulian FilipiucBelum ada peringkat
- Current Techniques in Canine and Feline NeurosurgeryDari EverandCurrent Techniques in Canine and Feline NeurosurgeryAndy ShoresBelum ada peringkat
- Hemodynamic Disorders Omar GhaziDokumen19 halamanHemodynamic Disorders Omar GhaziSawsan Z. JwaiedBelum ada peringkat
- Liver PathophysiologyDokumen19 halamanLiver PathophysiologyЮлия ЦыгановаBelum ada peringkat
- Quarter 2 Summative Test in ScienceDokumen4 halamanQuarter 2 Summative Test in ScienceSharmaine RamirezBelum ada peringkat
- BRS Anatomy - Intro Flashcards by Grace Caldwell - BrainscapeDokumen10 halamanBRS Anatomy - Intro Flashcards by Grace Caldwell - BrainscapeCarmela MarianoBelum ada peringkat
- Skin, Anaesthesia, Radiology and PsychiatryDokumen209 halamanSkin, Anaesthesia, Radiology and PsychiatryDrChauhanBelum ada peringkat
- Chapter 16Dokumen10 halamanChapter 16missy23pap50% (2)
- 4 Building A Fundation For Bagua - A Dynamic Stepping SystemDokumen91 halaman4 Building A Fundation For Bagua - A Dynamic Stepping Systemvincraig100% (2)
- Lec 1disorders of Vascular Flow and ShockDokumen91 halamanLec 1disorders of Vascular Flow and ShockMohid AhmedBelum ada peringkat
- Complication of Hemodialysis and Their ManagementDokumen52 halamanComplication of Hemodialysis and Their ManagementRetno SumaraBelum ada peringkat
- MCQ Exam EntDokumen26 halamanMCQ Exam EntDr-Firas Nayf Al-Thawabia0% (1)
- MCQ General Surgery DR ZahidDokumen49 halamanMCQ General Surgery DR Zahidhassanenterprises9907Belum ada peringkat
- Updated Physiology and Pathophysiology of CSF Circulation - The Pulsatile Vector TheoryDokumen18 halamanUpdated Physiology and Pathophysiology of CSF Circulation - The Pulsatile Vector TheorysavitageraBelum ada peringkat
- The Wonder Book On The AtmosphereDokumen342 halamanThe Wonder Book On The AtmosphereHadia Altaf Malik100% (1)
- Obstetrics & Gynaecology Terminal Sept 2022Dokumen11 halamanObstetrics & Gynaecology Terminal Sept 2022STEP TO MEDICOSBelum ada peringkat
- Milagon Matta BrochureDokumen7 halamanMilagon Matta BrochurePaul KlussmannBelum ada peringkat
- Anterior Abdominal Wall - Dr. Bea (KK)Dokumen3 halamanAnterior Abdominal Wall - Dr. Bea (KK)Karen EstavilloBelum ada peringkat
- Medical Terminology - Cardiovascular SystemDokumen4 halamanMedical Terminology - Cardiovascular SystemDenisse PortillaBelum ada peringkat
- Circulation and Gas Exchange: For Campbell Biology, Ninth EditionDokumen116 halamanCirculation and Gas Exchange: For Campbell Biology, Ninth EditionMahnoor AnjumBelum ada peringkat
- Just Go With The FlowDokumen2 halamanJust Go With The FlowIRIS50% (2)
- Daflon 500Dokumen3 halamanDaflon 500Shambhu SinghBelum ada peringkat
- Cardiovascular SystemDokumen26 halamanCardiovascular SystemGaurav SinghBelum ada peringkat
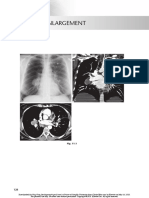
- Hilar EnlargementDokumen19 halamanHilar EnlargementGriggrogGingerBelum ada peringkat
- FS 5 Activity Multiple ChoiceDokumen5 halamanFS 5 Activity Multiple ChoiceFritzy Gwen BabaBelum ada peringkat
- Transport of Oxygen and Carbon DioxideDokumen45 halamanTransport of Oxygen and Carbon DioxideNamithaBelum ada peringkat
- Ultrasound Evaluation of Renal Artery StenosisDokumen19 halamanUltrasound Evaluation of Renal Artery Stenosisroentgen169100% (1)
- Vascular EmergencyDokumen324 halamanVascular EmergencyAhmed Aboud100% (1)
- Rapid Pathology Pathology Textbook For Medical StudentsDokumen89 halamanRapid Pathology Pathology Textbook For Medical Studentsyennqing100% (1)
- 6 Best Homeopathic Medicines For Swollen Ankles - Homeopathy at DrHomeoDokumen9 halaman6 Best Homeopathic Medicines For Swollen Ankles - Homeopathy at DrHomeovivek khannaBelum ada peringkat
- DVTDokumen6 halamanDVTNader Smadi100% (1)
- Standard First AidDokumen96 halamanStandard First AidahCURSED100% (9)