Orthopedic Assessment Sample PDF
Diunggah oleh
Syahrani SaidDeskripsi Asli:
Judul Asli
Hak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Orthopedic Assessment Sample PDF
Diunggah oleh
Syahrani SaidHak Cipta:
Format Tersedia
4
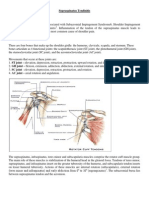
Orthopedic Assessment in Massage Therapy
Figure 11.7: Finger MCP flexion (A), PIP flexion (B), DIP flexion (C), and MCP, PIP, and DIP extension (D).
BOX: 11.2 CAPSULAR PATTERNS FOR DISTAL UPPER EXTREMITY
Elbow
Flexion more limited than extension
Forearm Radioulnar joints
Pronation and supination usually equally limited
Wrist
Flexion and extension equally limited.
Possible slight limitation in radial and ulnar deviation
Figure 11.8: Finger MCP abduction (A) and adduction (B).
Thumb CMC joint
Abduction most limited
Extension limited after abduction
Fingers
In the metacarpophalangeal (MCP), proximal interphalangeal (PIP), and distal interphalangeal (DIP) joints,
flexion and extension occur in the sagittal plane (Figure
11.7). Movement at the MCP joint occurs as the finger
is brought toward the anterior surface of the palm from
anatomical position. Returning the finger to anatomical position is extension in the MCP; hyperextension is
movement past full extension. Average range of motion
for MCP flexion is 900; hyperextension is approximately
300 with more passive motion possible than active.
Movement at the PIP and DIP joints occurs as the tip
of the finger is brought toward the anterior surface of the
palm in flexion. The finger is in full extension in anatomical position and ordinarily there is no additional range of
extension available. Average range of motion for finger
flexion at the PIP joint is 1000; average range of motion at
the DIP joint is 850900.
Abduction and adduction at the MCP joint occurs in
the frontal plane (Figure 11.8). Abduction is different for
the four fingers because finger abduction is movement
away from the midline of the hand versus the midline of
the body.4 Adduction is the return to anatomical position.
No range of motion values for adduction or abduction are
usually calculated at the MCP joint.
Thumb MCP & IP joints
Flexion more limited than extension
Capsular patterns
Range of motion testing in the elbow, forearm, wrist,
and hand requires evaluation at several articulations.
It is important to consider the role of the joint capsule
Fingers MCP, PIP, & DIP joints
Flexion limited most, followed by extension
when assessing joint function. Pathological problems
in the capsule, such as fibrosis, may be visible with the
joints capsular pattern. The capsular pattern is a pattern of movement restriction that is characteristic to each
individual joint. It is present in both active and passive
motion. Capular patterns are represented by a sequential
listing of the movements from most likely to least likely
limited. See the description of capsular patterns for this
region in Box 11.2.
ACTIVE RANGE OF MOTION
In the history, the practitioner identifies movements or
positions that cause pain or discomfort. This information
is used to guide more detailed evaluation of active movements using the single-plane motions described above.
Active movements employ contractile tissues, while also
moving inert tissues in the process. Pain during active
movement indicates problems in either the contractile
or inert tissues associated with that movement. Further
testing with passive motion and manual resistance helps
clarify the tissues at fault.
When performing active range-of-motion (AROM)
Chapter 11 Elbow, Forearm, Wrist, & Hand
BOX 11.3: MUSCLE ACTIONS OF THE ELBOW, FOREARM, & WRIST
Elbow
Flexion
Extension
brachialis
Triceps brachii
biceps brachii
Anconeus
brachioradialis
pronator teres
extensor carpi radialis longus
exor carpi radialis
exor carpi ulnaris
Forearm
Wrist
Pronation
Supination
pronator teres
biceps brachii
pronator quadratus
supinator
Flexion
exor carpi radialis
Extension
extensor carpi radialis longus
exor carpi ulnaris
extensor carpi radialis brevis
palmaris longus
extensor carpi ulnaris
exor digitorum supercialis
extensor digitorum
exor digitorum profundus
Wrist
Radial Deviation
Ulnar Deviation
extensor carpi radialis longus
extensor carpi ulnaris
extensor carpi radialis brevis
exor carpi ulnaris
extensor pollicis longus
extensor pollicis brevis
exor carpi radialis
abductor pollicis longus
evaluations, consider the position of the limb to ensure
that the target tissues are engaged. For example, active
elbow flexion and extension are usually evaluated with
the client in a vertical (either seated or standing) position. When the client actively flexes the elbow (by lifting
the forearm toward the upper arm), the elbow flexors
are engaged concentrically. When the elbow returns to
anatomical position it is not the elbow extensors that are
responsible for the action, but the elbow flexors as they
employ an eccentric contraction. Engaging the elbow
extensors requires a change in body position or in the
way resistance to the movement is offered.
Active movement is commonly stopped near the
end range of motion by stretching antagonistic muscles.
Other factors that could prematurely limit active movement in this region include ligamentous or capsular
damage, muscle contractures, pain from nerve compression or tension, tendinosis, tenosynovitis, fibrous cysts,
or joint disorders such as arthritis. Identifying structures
involved in active movement and comparing those with
results from passive movement and manual resistive tests
helps identify the cause of movement restriction.
To perform AROM evaluations, refer to the step-by-
step instructions in Chapter 3. Also review the guidelines
of how to interpret the results from these tests in the
same section. The muscles engaged to perform actions of
the elbow, forearm, wrist, and hand are listed in Boxes
11.35. Other muscles may also contribute to the motion
and subsequent dysfunction. When performing the tests,
motions the practitioner suspects may be painful should
be reserved for the end of the evaluation process.
PASSIVE RANGE OF MOTION
During passive range-of-motion (PROM) evaluations
inert tissues are moved, but the contractile tissues are not
engaged. Pain during passive movement predominantly
implicates inert tissues as the cause. Pain from contractile
tissues could occur at the end range of passive movement
as the antagonistic muscles are stretched, although it
would be those tissues that concentrically contract in the
opposite direction of the movement.
Passive motion is performed after active for several
reasons. When active movement is performed first, movement restrictions due to pain are established without
causing additional discomfort. The client will not move
Chapter 11 Elbow, Forearm, Wrist, & Hand
Figure 11.26: The elbow flexion test.
flexion of the thumb, because these are primary motions
of the adductor pollicis muscle. Weakness of this muscle
is more specifically tested with the Froments sign discussed in the section on Guyons canal syndrome.
Special Tests
Elbow Flexion Test
The client is standing or seated and brings both elbows
into full flexion with the forearms supinated and the wrists
hyperextended (Figure 11.26). The client should adopt the
position on both sides at the same time so a comparison
with the unaffected side can be made. If symptoms are
reproduced within about 60 seconds, compression of the
ulnar nerve in the cubital tunnel is likely.66, 67
Explanation: The position puts tensile stress on the
ulnar nerve while decreasing space within the cubital
tunnel. If the condition is present, these actions aggravate the clients symptoms. Note the similarity of this test
position to the upper limb tension test #4. The variation
of adding shoulder abduction makes this test more sensitive.
Froments sign
See Guyons Tunnel Syndrome.
Upper limb tension test #4
See Nerve Compression and Tension Pathologies near
end of chapter.
Differential Evaluation
Guyons tunnel syndrome, thoracic outlet syndrome,
carpal tunnel syndrome, other regions of ulnar nerve
compression or tension, systemic disease, space-occupying lesions in the elbow, ligament damage in the elbow,
cervical radiculopathy, myofascial trigger point referral,
diabetic neuropathy, osteophytes in the elbow region.
Suggestions for Treatment
Relieving compression on the affected nerve is the primary
goal of treatment. Encourage the client to eliminate activi-
19
ties that keep the elbow flexed for long periods or apply
pressure to the cubital tunnel (leaning on the elbows, for
example). Splints that keep the elbows in extension are
helpful for people who sleep with the elbows in flexion.
Even low levels of compression, if left on the nerve for
long periods, can require a lengthy period of rehabilitation to restore normal function. If conservative measures
are not successful, surgery is sometimes performed. A
common surgical procedure involves moving the ulnar
nerve to a different location so it is not compressed within
the tunnel.
Massage is helpful for cubital tunnel syndrome
because a primary cause is muscular hypertonicity in
the flexor carpi ulnaris (FCU). Techniques such as deep
stripping or massage with active engagement help reduce
overall tension in the muscles and decrease compression
on the ulnar nerve. Particular caution should be observed
in applying pressure to the flexor carpi ulnaris near the
region of ulnar nerve entrapment so as not to aggravate
the pathology.
PRONATOR TERES SYNDROME
The symptoms of pronator teres syndrome (PTS) can
be identical to those of carpal tunnel syndrome because
they are both peripheral median nerve compression
syndromes. Some suggest that PTS is under-diagnosed
because carpal tunnel syndrome has received more attention.43
Characteristics
PTS develops from compression of the median nerve
by the pronator teres muscle. It is sometimes referred to
as pronator syndrome. According to Wertsch,68 the term
pronator syndrome also includes median nerve compression by other structures in the elbow such as the ligament
of Struthers or the bicipital aponeurosis (lacertus fibrosus).
As the median nerve passes the elbow it runs between
the two heads of the pronator teres muscle, where the
nerve may be compressed (Figure 11.27). Compression
can be due to muscle hypertonicity or fibrous bands
within the muscle pressing on the nerve.69, 70 In some cases
pressure is placed on the nerve by anatomical anomalies, such as the nerve traveling deep to both heads of
the pronator teres.71 In this situation, the nerve may be
compressed against the ulna by the pronator teres muscle
itself.
PTS results from repetitive motions that cause hypertonicity in the pronator teres. Occupational activities such
as hammering, cleaning fish, or performing any activity
that requires continual manipulation of tools can cause
overuse of the pronator teres.72 The hypertonicity then
causes nerve compression and the symptoms are felt in
the median nerve distribution in the anterior forearm and
hand (Figures 11.45). Women are affected more than men,
but the reason why is not clear.
20
Orthopedic Assessment in Massage Therapy
tor teres syndrome, but AIN involvement is also called
anterior interosseous nerve syndrome.75 AIN syndrome
rarely produces sensory symptoms because the nerve is
almost exclusively composed of motor fibers.43 If the AIN
is compressed it shows up clinically as motor weakness
in the index finger and thumb, making it difficult to form
a pinch grip with those two digits (see description of the
pinch grip test below).76
lacertus fibrosus
superficial head
deep head
median nerve
Figure 11.27: Anterior view of the left elbow showing the two heads of
the pronator teres muscle. The median nerve runs between the two heads
and is compressed in this region in pronator teres syndrome. (3-D anatomy
image courtesy of Primal Pictures Ltd. www.primalpictures.com).
Most symptoms of nerve compression radiate distal to
the site of compression. Aching forearm pain and paresthesia along with pain in the median nerve distribution in
the hand is likely to be PTS and should not be assumed to
indicate carpal tunnel syndrome.73 In some cases, nerve
compression pain can radiate proximal to the site of compression. All potential sites of compression should be
considered in the differential evaluation process.74
While PTS and carpal tunnel syndrome both affect
the median nerve and have similar symptoms, there are
distinct differences. PTS pain is exacerbated by repetitive elbow flexion and symptoms occur in the forearm
as well as the hand. Carpal tunnel syndrome is aggravated by wrist movements and pain is not experienced as
much in the forearm. In both cases, atrophy is possible in
the thenar muscles of the hand, which are innervated by
branches from the median nerve. The median nerve can
be compressed in more than one location. There could be
carpal tunnel compression and pronator teres compression simultaneously (see the double or multiple crush
phenomenon described in Chapter 2).
Another cause of median nerve compression near the
pronator teres involves a fibrous band from the biceps
brachii muscle. This band connects the distal portion
of the biceps brachii to the ulna on the forearm and is
called the lacertus fibrosus or bicipital aponeurosis. The
median nerve runs under the lacertus fibrosus and may
be compressed by it, particularly during strong repetitive
contractions of the biceps brachii.43
In some cases, pronator teres compression pathologies
affect the anterior interosseous nerve (AIN) and not the
median nerve. The AIN branches off the median nerve
as it passes between the two heads of the pronator teres.
Some authors consider AIN compression part of prona-
History
The client reports aching, shooting, or sharp, electricaltype pain, as well as paresthesia in the median nerve
distribution of the hand. These symptoms might be
felt in the anterior forearm as well. Pain is aggravated
when performing activities that use the pronator teres
muscle against resistance, such as using a screwdriver
or hand-held power tool.72, 77 Ask about repetitive elbow
movements that aggravate symptoms.
Clients with carpal tunnel syndrome often report night
pain; those with PTS generally do not.43 Prolonged wrist
flexion during sleep aggravates carpal tunnel syndrome
because it decreases the space in the carpal tunnel and
presses on the median nerve. Because wrist flexion does
not affect the pronator teres muscle, this wrist position
does not increase nerve compression symptoms in PTS.
Observation
There are no prominent visual indicators of pronator
teres syndrome. Nerve compression may cause atrophy
of the forearm and hand muscles supplied by the median
nerve (see Nerve Compression and Tension Pathologies
at the end of the chapter for muscles supplied by the
median nerve). If only one hand is symptomatic, it should
be compared with the opposite side to determine differences in muscle size. The muscles of the thenar eminence
(fleshy bundle of muscles on the thumb side of the hand)
are likely to show signs of atrophy when compared to the
unaffected side.
Palpation
Tenderness and hypertonicity are common in the forearm
flexor muscles and the pronator teres muscle. Symptoms
are aggravated when palpating the pronator teres, as
pressure is increased in the region of nerve compression.
Range-of-Motion and Resistance Testing
AROM: Active motion without resistance rarely causes
discomfort in any direction unless the condition is
advanced. There may be slight discomfort at the end of
active supination if the wrist is hyperextended and the
supination is performed with the elbow extended. Pain
or discomfort with this maneuver is due to simultaneous
stretching of the pronator teres and the median nerve,
which pulls the nerve taut against the dense muscular
fibers. Symptoms present if active motions are performed
against resistance (holding a heavy implement in the
hand during motion, for example).
Chapter 11 Elbow, Forearm, Wrist, & Hand
21
Figure 11.28: The pronator teres test.
Figure 11.29: The pinch grip test. Image shows inability to prevent the
PROM: Passive supination can produce pain if the wrist is
hyperextended and the elbow is extended, due to simultaneous stretching of the pronator teres and the median
nerve.
MRT: Pain might be felt during resisted pronation of
the forearm and possibly during resisted elbow flexion.
Weakness may be evident in the flexors of the hand or
fingers, due to impairment of motor signals from the
median nerve.
nerve near the elbow. This test is similar to Froments sign,
although motor signals in different nerves are tested.
Explanation: The anterior interosseous nerve innervates the flexor digitorum profundus muscle that flexes
the DIP joint of the index finger. This muscle is also necessary to hold the finger in a normal pinch grip without
hyperextending the DIP joint. If the nerve is compressed,
impaired motor signals causes muscle weakness.
Special Tests
Pronator Teres Test
The client is standing with the elbow in 900 of flexion.
The practitioner places one hand on the clients elbow for
stabilization and the other hand grasps the clients hand
in a handshake position. The client holds this position as
the practitioner attempts to supinate the clients forearm
(forcing the client to contract the pronator muscles). While
holding the resistance against pronation, the practitioner
extends the clients elbow (Figure 11.28). If this motion
reproduces the clients pain or discomfort there is a good
chance of median nerve compression by the pronator
teres. The client should keep the elbow relaxed during
the test, because holding the elbow firmly in flexion will
not allow elbow extension.
Explanation: The pronator teres is engaged in an isometric contraction, which increases compression of the
median nerve. Once the pronator teres is contracted and
the elbow is extended, the contracted muscle is forcefully
lengthened, producing greater potential nerve compression.
Pinch Grip Test
This test is specific to anterior interosseous nerve syndrome. The client firmly pinches the tips of the thumb
and index finger together (Figure 11.29). If the client is
unable to do this without hyperextending the DIP joint of
the index finger, anterior interosseous nerve motor signals
could be impaired due to proximal compression of the
index finger DIP joint from extending during pinch grip.
Differential Evaluation
Carpal tunnel syndrome, other median nerve entrapment
sites, cervical radiculopathy, thoracic outlet syndrome,
tumors or space-occupying lesions of the anterior elbow,
medial epicondylitis, medial apophysitis (little league
elbow), myofascial trigger point referrals, diabetic neuropathy.
Suggestions for Treatment
The primary focus of treatment is reducing compression
on the median nerve. If the primary pathology is hypertonicity of the pronator teres, the condition is easier to
address than if there are other anatomical considerations.
Massage is helpful, as it can be directly applied to the pronator teres muscle. Static compression methods are used
to treat myofascial trigger point activity aggravating the
surrounding muscles. Deep stripping or pin-and-stretch
methods are also helpful.
Traditional treatment includes splints or braces that
are used to change elbow biomechanics and reduce compression on the affected nerve. Stretching methods are
valuable to decrease nerve compression by improving
flexibility in the pronator teres.
BOX 11.9: CLINICAL NOTES
Pronator teres dysfunction:
The pronator teres can be a common cause of
median nerve entrapment. Due to its function it
may also be involved in medial epicondylitis.
32
Orthopedic Assessment in Massage Therapy
medial brachial
cutaneous nerve
C6
C6
T1
C7
C8
radial nerve
medial antebrachial
cutaneous nerve
C5
Figure 11.44: Dermatomes of the upper extremity (Mediclip image copy-
lateral antebrachial
cutaneous nerve
right, 1998 Williams & Wilkins. All Rights Reserved).
General Neuromuscular Disorders
In many cases, soft-tissue dysfunctions occur that are not
given a specific name. Adequate assessment determines
the most likely tissues involved and takes into account
pathologies that may or may not have specific titles. The
following three sections provide an overview of general
soft-tissue disorders when they occur in the elbow, forearm, wrist, and hand. Chapter 4 provides a thorough
discussion of the pathological process of nerve compression and tension, hypertonicity, myofascial trigger points,
and muscle strains in any region of the body. Chapter
4 also includes the history, observation, palpation, and
relevant tests sections of assessment for these conditions.
Unique assessment procedures and/or specialized information on these conditions as they occur in the elbow,
forearm, wrist, and hand are provided below.
median nerve
radial nerve
radial nerve
ulnar nerve
C
Figure 11.45: Cutaneous innervation of the upper extremity in the anterior arm (A) posterior arm (B) dorsal hand (C) and palmar hand (D).
NERVE COMPRESSION & TENSION PATHOLOGIES
Nerve compression or tension pathologies produce symptoms in the elbow, forearm, wrist, or hand from either a
cervical radiculopathy (spinal nerve root compression)
or a peripheral neuropathy (peripheral upper extremity
nerve injury). There are numerous locations in the distal
upper extremity where peripheral neuropathies could
occur; many are discussed as discrete conditions earlier
in the chapter. Other common regions where nerve compression might occur in the elbow, forearm, wrist, and
hand are listed in Box 11.11.
Sensory symptoms from a radiculopathy may also
be felt in the distal upper extremity and are experienced
within the dermatome associated with that nerve root
(Figure 11.44). Sensory symptoms of peripheral neuropathy are felt in the region of cutaneous innervation for
the nerve affected (Figure 11.45). Peripheral neuropathies cause motor dysfunction and produce weakness in
the muscles innervated by the affected nerve (Box 11.12).
Consult Chapter 4 for a thorough discussion of what to
look for in the history, observation, and palpation sections when evaluating nerve compression and tension
pathologies.
BOX: 11.11 REGIONS OF POSSIBLE NERVE ENTRAPMENT
Radial and Posterior Interosseous Nerves
The spiral groove on the posterior aspect of the humerus
Under the supinator muscle in the radial tunnel
Median and Anterior Interosseous Nerves
Under the bicipital aponeurosis (lacertus fibrosus)
Beneath the Ligament of Struthers
The carpal tunnel
Ulnar Nerve
In the cubital tunnel
In Guyons tunnel
Chapter 11 Elbow, Forearm, Wrist, & Hand
33
BOX: 11.12 MUSCLES INNERVATED BY THE RADIAL, MEDIAN, & ULNAR NERVES
Radial Nerve
Main Trunk
Brachialis
Triceps brachii
Anconeus
Brachioradialis
Extensor carpi radialis longus
Posterior Interosseous Branch
Supinator
Extensor carpi radialis brevis
Extensor digiti minimi
Extensor carpi ulnaris
Extensor digitorum
Extensor indicis
Abductor pollicis longus
Extensor pollicis brevis
Extensor pollicis longus
Median Nerve
Main Trunk
Flexor carpi radialis
Pronator teres
Palmaris longus
Flexor digitorum superficialis
Abductor pollicis brevis
Opponens pollicis
Flexor pollicis brevis (superficial head)
Lumbricales (1st & 2nd)
Anterior Interosseous Branch
Flexor pollicis longus
Flexor digitorum profundus (lateral part)
Pronator quadratus
Range-of-Motion and Resistance Testing
AROM: Active movement may produce pain if the affected
nerve is stretched. In some cases movements may also
compress the nerve causing exacerbation of symptoms.
Consider the biomechanics of each motion and how it
affects the nerve being evaluated.
PROM: The same principles apply as for active motion.
MRT: In nerve compression or tension pathologies, the
affected nerve causes weakness in the muscles it innervates. Manual resistive tests evaluate muscle strength and
are important for determining weakness levels in nerve
pathologies. Depending on the location of the compression pathology, weakness may be apparent in some or all
of the muscles innervated by the affected nerve. The more
proximal the compression site, the greater the number of
muscles affected (Figure 11.46). A list of primary upper
extremity motor nerves and the muscles they innervate
is provided in Box 11.12. Table 1 at the end of the chapter
provides a chart of muscles, their resisted actions, and
potentially affected nerves or nerve roots.
Muscle 2
Muscle 1
Proximal end of nerve
Distal end of nerve
Compression Site A
Compression Site B
Muscle 3
Figure 11.46: Muscles affected by different regions of nerve compression. If compression occurs at Site A, muscles 1, 2, & 3 are affected. If it
occurs at Site B, only muscles 2 and 3 are affected.
Ulnar Nerve
Ulnar nerve
Adductor pollicis
Abductor digiti minimi
Opponens digiti minimi
Flexor digiti minimi brevis
Flexor digitorum profundus (medial part)
Flexor carpi ulnaris
Lumbricales (3rd & 4th)
Palmaris brevis
Palmar interossei
Dorsal interossei
Flexor pollicis brevis (deep head)
Special Tests
Upper limb tension tests (ULTTs) evaluate symptoms in
neural tension or compression pathologies. There are four
common ULTTs; the first two test the median nerve, the
radial is tested by the third, and the fourth tests the ulnar.
The numbering of these tests is not consistent in medical
texts; in this text they are numbered ULTT 14. To avoid
confusion in treatment notes, identify the ULTT used by
the nerve being stressed during the test. For example,
treatment notes might state, ULTT #2 with median nerve
bias.
General instructions: The practitioner performs a
series of movements that gradually increase tension on
the nerve. Symptoms, if present, will increase as movements are added. Movements are performed in the order
listed with each test. During testing, ask the client about
changes in symptoms after each movement. Once the
client experiences symptoms, it is not necessary to complete the remainder of the movements, especially if the
symptoms are strong.
Upper Limb Tension Test #1 (Median nerve bias)
The client is in a supine position. The practitioner stands
facing the clients head on the testing side. The clients
elbow is flexed at the beginning of the test. The final
position of the shoulder in ULTT #1 is contraindicated if
shoulder instability is present (Figure 11.47)
Test Movements
1.
Shoulder is brought into depression.
2.
Arm is abducted to about 1100.
3.
Forearm is supinated.
4.
Wrist and fingers are hyperextended.
5.
Shoulder is laterally rotated.
6.
Elbow is extended.
7.
Neck is contralaterally flexed.
36
Orthopedic Assessment in Massage Therapy
Figure 11.51 Myofascial trigger point referral patterns: Biceps brachii (A), Brachialis (B), Brachioradialis (C), Extensor carpi radialis brevis (D),
Extensor carpi radialis longus (E), Extensor carpi ulnaris (F), Extensor digitorum (G), Supinator (H), Flexor carpi radialis (I), Flexor carpi ulnaris (J), Flexor
digitorum profundus & superficialis (K), Flexor pollicis longus (L), Palmaris longus (M), Pronator teres (N). (Images courtesy of Mediclip, copyright 1998
Williams & Wilkins. All rights reserved)..
Chapter 11 Elbow, Forearm, Wrist, & Hand
37
Figure 11.52 Myofascial trigger point referral patterns: Triceps brachii (A, B), Adductor pollicis (C). (Images courtesy of Mediclip, copyright 1998
Williams & Wilkins. All rights reserved)..
TABLE 1: WEAKNESS WITH MANUAL RESISTIVE TEST POSSIBLE NERVE INVOLVEMENT
MUSCLE
RESISTED ACTION
POSSIBLE NERVE INVOLVEMENT IF ACTION WEAK
Abductor pollicis brevis
thumb abduction
median (C7-C8)
Abductor pollicis longus
thumb abduction
radial (C7-C8)
Adductor pollicis
thumb adduction
ulnar (C8-T1)
Anconeus
elbow extension
radial (C6-C8)
Biceps brachii
elbow flexion
musculocutaneous (C5-C6)
Brachialis
elbow flexion
musculocutaneous (C5-C6)
Brachioradialis
elbow flexion
radial (C5-C6)
Extensor carpi radialis brevis
wrist extension
radial (C7-C8)
Extensor carpi radialis longus
wrist extension
radial (C6-C7)
Extensor carpi ulnaris
wrist extension
radial (C7-C8)
Extensor digitorum
finger extension (MCP joint)
radial (C7-C8)
Extensor pollicis brevis
thumb extension
radial (C7-C8)
Extensor pollicis longus
thumb extension
radial (C7-C8)
Flexor carpi radialis
wrist flexion
median (C6-C7)
Flexor carpi ulnaris
wrist flexion
ulnar (C7-T1)
Flexor digitorum profundus
finger flexion (DIP joint)
median (C8-T1)
Flexor digitorum superficialis
finger flexion (PIP joint)
median (C8-T1)
Flexor pollicis longus
thumb flexion
median (C7-C8)
Palmaris longus
wrist flexion
median (C7-C8)
Pronator quadratus
forearm pronation
median (C7-C8)
Pronator teres
forearm pronation
median (C7-C8)
Supinator
forearm supination
radial (C6-C7)
Triceps brachii
elbow extension
radial (C6-C8)
38
Orthopedic Assessment in Massage Therapy
TABLE 2: JOINTS, ASSOCIATED MOTIONS, PLANES OF MOTION IN ANATOMICAL POSITION, AXIS OF ROTATION, AND AVERAGE RANGE OF MOTION
Joint
Elbow
Forearm
Wrist
Thumb (CMC)
Thumb (MCP)
Thumb (IP)
Finger (MCP)
Finger (PIP)
Finger (DIP)
Motion
Plane of Motion
Axis of Rotation
Avg. ROM (degrees)
Flexion
Sagittal
Medial-lateral
150
Extension
Sagittal
Medial-lateral
Pronation
Transverse
Vertical
80
Supination
Transverse
Vertical
80
Flexion
Sagittal
Medial-lateral
80
Extension
Sagittal
Medial-lateral
70
Radial Deviation
Frontal
Anterior-posterior
20
Ulnar Deviation
Frontal
Anterior-posterior
30
Flexion
Frontal
Anterior-posterior
15 (CMC & MCP)
Extension
Frontal
Anterior-posterior
20 (CMC & MCP)
Abduction
Sagittal
Medial-lateral
70 (CMC & MCP)
Adduction
Sagittal
Medial-lateral
Flexion
Frontal
Anterior-posterior
15 (CMC & MCP)
Extension
Frontal
Anterior-posterior
20 (CMC & MCP)
Abduction
Sagittal
Medial-lateral
70 (CMC & MCP)
Adduction
Sagittal
Medial-lateral
Flexion
Frontal
Anterior-posterior
80
Extension
Frontal
Anterior-posterior
Flexion
Sagittal
Medial-lateral
90
Extension
Sagittal
Medial-lateral
30
Abduction
Frontal
Anterior-posterior
Adduction
Frontal
Anterior-posterior
Flexion
Sagittal
Medial-lateral
100
Extension
Sagittal
Medial-lateral
Flexion
Frontal
Anterior-posterior
85-90
Extension
Frontal
Anterior-posterior
*Average range-of-motion values are either 0 or not usually calculated
Chapter 11 Elbow, Forearm, Wrist, & Hand
39
T
Elb
ow
f
Fin lexi
on
kle
te
ste
st
Fro
in
te
m
st
en
ts
Go
sig
lfe
n
r
Ph s elb
ale
ow
n
t
Pin s te est
s
ch
t
Pr grip
on
te
st
at
or
Te
t
e
nn
re
st
is
es
elb
t
Te
o
w
th
er
t
e
Tin ed m st
el
s s edia
nn
ign
UL
er
TT
ve
#1
s tr
UL
es
TT
st
#2
es
t
UL
TT
#
UL 3
TT
#4
PR
MR
OM
AR
OM
TABLE 3: QUICK REFERENCE TABLE FOR CONDITION ASSESSMENT
Carpal Tunnel Syndrome
Cubital Tunnel Syndrome
De Quervains Tenosynovitis
Ganglion Cyst
Guyons Canal Syndrome
Lateral Epicondylitis
Medial Epicondylitis
Muscle Strains
Muscular Hypertonicity
Nerve Compression & Tension
Olecranon Bursitis
Pronator Teres Syndrome
Radial Tunnel Syndrome
Trigger Finger
Notes
1.
2.
3.
4.
5.
6.
7.
8.
9.
Cyriax J. Textbook of Orthopaedic Medicine Volume One:
Diagnosis of Soft Tissue Lesions. Vol 1. 8th ed. London:
Bailliere Tindall; 1982.
Hislop H, Montgomery J. Daniels and Worthinghams Muscle
Testing. Philadelphia: W.B. Saunders; 2002.
Berryman Reese N, Bandy WD. Joint Range of Motion and
Muscle Length Testing. Philadelphia: W.B. Saunders Co.;
2002.
Neumann DA. Kinesiology of the Musculoskeletal System.
St. Louis: Mosby; 2002.
Kendall F, Kendall-McCreary E, Geise-Provance P. Muscles:
Testing and Function. 4th ed. Baltimore: Williams & Wilkins;
1993.
Shaffer K, Shaffer J. Dupuytren Contracture. eMedicine [web
page]. 4-28-04. Available at: www.emedicine.com. Accessed
February 7, 2005.
Ravid M, Dinai Y, Sohar E. Dupuytrens disease in diabetes
mellitus. Acta Diabetol Lat. May-Aug 1977;14(3-4):170-174.
Attali P, Ink O, Pelletier G, et al. Dupuytrens contracture,
alcohol consumption, and chronic liver disease. Arch Intern
Med. Jun 1987;147(6):1065-1067.
Burge P, Hoy G, Regan P, Milne R. Smoking, alcohol and the
10.
11.
12.
13.
14.
15.
16.
17.
risk of Dupuytrens contracture. J Bone Joint Surg Br. Mar
1997;79(2):206-210.
Benson LS, Williams CS, Kahle M. Dupuytrens contracture. J
Am Acad Orthop Surg. Jan-Feb 1998;6(1):24-35.
McFarlane RM. On the origin and spread of Dupuytrens
disease. J Hand Surg [Am]. 2002;27(3):385-390.
Zerajic D, Finsen V. Dupuytrens disease in Bosnia and
Herzegovina. An epidemiological study. BMC Musculoskelet
Disord. Mar 29 2004;5(1):10.
Silman AJ, Pearson JE. Epidemiology and genetics of
rheumatoid arthritis. Arthritis Res. 2002;4 Suppl 3:S265272.
Gabriel SE, Crowson CS, OFallon WM. The epidemiology of
rheumatoid arthritis in Rochester, Minnesota, 1955-1985.
Arthritis Rheum. Mar 1999;42(3):415-420.
Lee DM, Weinblatt ME. Rheumatoid arthritis. Lancet. Sep 15
2001;358(9285):903-911.
Rattray F, Ludwig L. Clinical Massage Therapy:
Understanding, Assessing and Treating over 70 Conditions.
Toronto: Talus Incorporated; 2000.
Neumeister M, Nguyen M. Rheumatoid Hand. eMedicine
[web page]. 11-17-2004. Available at: www.emedicine.com.
Anda mungkin juga menyukai
- Article - Evaluating The Efficacy of Drama Therapy in Teaching Social Skills To Children With Autism Spectrum DisordersDokumen20 halamanArticle - Evaluating The Efficacy of Drama Therapy in Teaching Social Skills To Children With Autism Spectrum DisordersDespina Kalaitzidou100% (3)
- Hip Adductor RehabilitationDokumen4 halamanHip Adductor RehabilitationOscar NgBelum ada peringkat
- Trunk Stabilization ProgramDokumen20 halamanTrunk Stabilization ProgramLate ArtistBelum ada peringkat
- Hand and Upper Extremity Review for NBCOT ExamDokumen59 halamanHand and Upper Extremity Review for NBCOT ExamJenny RajanBelum ada peringkat
- Selected Bibliography On DreamingDokumen29 halamanSelected Bibliography On DreamingkayarBelum ada peringkat
- TECH 524 - Palpation II (Castellucci) 9 2015Dokumen12 halamanTECH 524 - Palpation II (Castellucci) 9 2015Robert StraubBelum ada peringkat
- Chronic Pain ACTDokumen8 halamanChronic Pain ACTRan AlmogBelum ada peringkat
- William C. Cottrell, MD AbstractDokumen4 halamanWilliam C. Cottrell, MD AbstractmalaBelum ada peringkat
- Videofluoroscopic Swallowing StudiesDokumen25 halamanVideofluoroscopic Swallowing StudiesPriisciilla Vicencio100% (1)
- Adrenal Fatigue WebDokumen2 halamanAdrenal Fatigue Webfractalmonkey2Belum ada peringkat
- PNF SimplifiedDokumen3 halamanPNF SimplifiedsaswepakBelum ada peringkat
- Rotator Cuff Injury RehabilitationDokumen29 halamanRotator Cuff Injury RehabilitationArko duttaBelum ada peringkat
- The Correlation Between Parenting Style and Child StuntingDokumen15 halamanThe Correlation Between Parenting Style and Child StuntingMonica RaharjoBelum ada peringkat
- Shoulder Application SolutionsDokumen3 halamanShoulder Application SolutionsDBelum ada peringkat
- TCM Acupuncture and Acupressure Effects on LaborDokumen17 halamanTCM Acupuncture and Acupressure Effects on Laboramilyapradita100% (1)
- The Physics of Feldenkrais: Part 2: No Strain, No GainDokumen9 halamanThe Physics of Feldenkrais: Part 2: No Strain, No GainvkBelum ada peringkat
- Neuromuscular Electrical Stimulation For Treatment of Muscle Impairment Critical Review and Recommendations For Clinical PracticeDokumen76 halamanNeuromuscular Electrical Stimulation For Treatment of Muscle Impairment Critical Review and Recommendations For Clinical PracticeCleuton Braga LandreBelum ada peringkat
- Narrative Exposure Therapy (NET) : For Full Information About The NET Procedure See The ManualDokumen9 halamanNarrative Exposure Therapy (NET) : For Full Information About The NET Procedure See The ManualUncynical MailBelum ada peringkat
- Adhd ArticleDokumen6 halamanAdhd Articleapi-115513756Belum ada peringkat
- Survival StrategiesDokumen8 halamanSurvival StrategiesDr Jitender SinghBelum ada peringkat
- What Is A Migraine Headache - CourseDokumen14 halamanWhat Is A Migraine Headache - CourseKARL PASCUABelum ada peringkat
- MobilisationDokumen97 halamanMobilisationMegha Patani100% (1)
- Dr. Muhammad Ali-ur-Rasheed: Lecturer, Department of Physiotherapy. Sargodha Medical CollegeDokumen89 halamanDr. Muhammad Ali-ur-Rasheed: Lecturer, Department of Physiotherapy. Sargodha Medical CollegeRukhma NoorBelum ada peringkat
- Shoulder Assessment: Ayesha RazzaqDokumen47 halamanShoulder Assessment: Ayesha RazzaqayeshaBelum ada peringkat
- Aaos 2002Dokumen120 halamanAaos 2002Yusufa ArdyBelum ada peringkat
- Elbow Rehabilitation - SpringerLinkDokumen35 halamanElbow Rehabilitation - SpringerLinkasdfBelum ada peringkat
- Patient Health ProfileDokumen4 halamanPatient Health ProfileChristopher WuBelum ada peringkat
- 18-Abduction of Infant ChildDokumen5 halaman18-Abduction of Infant ChildakositabonBelum ada peringkat
- Somatosensory System OverviewDokumen16 halamanSomatosensory System OverviewRamadhan OdiestaBelum ada peringkat
- Supraspinatus TendinitisDokumen7 halamanSupraspinatus Tendinitismilananand100% (1)
- Merchant of DeathDokumen9 halamanMerchant of DeathHowardBelum ada peringkat
- Shoulder PDFDokumen11 halamanShoulder PDFteresaioana100% (1)
- Cadac J-Type User ManualDokumen200 halamanCadac J-Type User ManualPaulo FeijãoBelum ada peringkat
- Caffeine ADHDDokumen7 halamanCaffeine ADHDTim GiordaniBelum ada peringkat
- Lisdexamfetamine For Adhd in Adults New Medicine RecommendationDokumen4 halamanLisdexamfetamine For Adhd in Adults New Medicine RecommendationVinicius Piazza FerreiraBelum ada peringkat
- Brachial Plexus Neuritis Following HPV VaccinationDokumen3 halamanBrachial Plexus Neuritis Following HPV Vaccinationkiedd_04100% (1)
- Beighton Hypermobility ScoreDokumen6 halamanBeighton Hypermobility ScoreluckyBelum ada peringkat
- Screendem P KIrwan SpondyloarthropathyDokumen1 halamanScreendem P KIrwan SpondyloarthropathyMilos DjuricBelum ada peringkat
- Posture Pro posts on posture, performance and posturologyDokumen15 halamanPosture Pro posts on posture, performance and posturologyVlad PadinaBelum ada peringkat
- A System Based' Approach To Risk Assessment of The Cervical Spine Prior ToDokumen9 halamanA System Based' Approach To Risk Assessment of The Cervical Spine Prior ToRudolfGerBelum ada peringkat
- Transversus Abdominis Plane (Tap) BlockDokumen6 halamanTransversus Abdominis Plane (Tap) BlockSuresh KumarBelum ada peringkat
- Orthopedic Assessment Sample PDFDokumen11 halamanOrthopedic Assessment Sample PDFDuppala Sateesh KumarBelum ada peringkat
- Stiff Elbow PP Nov 14Dokumen35 halamanStiff Elbow PP Nov 14BekBelum ada peringkat
- President's Address: Trick MovementsDokumen3 halamanPresident's Address: Trick MovementsDr. Rushikesh K. Joshi100% (1)
- The Slump Test: Examining Spinal Pain and Range of MotionDokumen5 halamanThe Slump Test: Examining Spinal Pain and Range of MotionNahu SteinmannBelum ada peringkat
- Shoulder ExamDokumen24 halamanShoulder ExamMuhammad FahmyBelum ada peringkat
- MFR Functional TestingDokumen0 halamanMFR Functional TestingasloocltBelum ada peringkat
- Elbow Arthritis and Removal of Loose Bodies and SpursDokumen11 halamanElbow Arthritis and Removal of Loose Bodies and SpurspuchioBelum ada peringkat
- Naskah Publikasi Fix PDFDokumen15 halamanNaskah Publikasi Fix PDFDedy williantoBelum ada peringkat
- 6 Elbow and WristDokumen76 halaman6 Elbow and Wristalinaziyad3Belum ada peringkat
- Tendon Transfers For Thumb Opposition: Alexander Y. Shin, MD, and Khiem D. Dao, MDDokumen17 halamanTendon Transfers For Thumb Opposition: Alexander Y. Shin, MD, and Khiem D. Dao, MDFernando Martín Arce AlvaBelum ada peringkat
- Assignment 14a Final PaperDokumen11 halamanAssignment 14a Final Paperapi-665233380Belum ada peringkat
- 08 Lumbar Fusion PP OrthoDokumen17 halaman08 Lumbar Fusion PP Orthoapi-547492718Belum ada peringkat
- Case Report Presentation - TFCCDokumen3 halamanCase Report Presentation - TFCCapi-414663729Belum ada peringkat
- Aco102 085dDokumen2 halamanAco102 085dDonny HendrawanBelum ada peringkat
- ScoliosesDokumen10 halamanScolioseschandiwalaBelum ada peringkat
- Radial Nerve PalsyDokumen10 halamanRadial Nerve PalsyMahardika PutraBelum ada peringkat
- ReferatDokumen7 halamanReferatMuh Arya SaputraBelum ada peringkat
- Anatomy and Management of Radial Nerve PalsyDokumen61 halamanAnatomy and Management of Radial Nerve PalsyDenoson PalsonBelum ada peringkat
- Boehnke - Dorsal Scapular Nerve SyndromeDokumen7 halamanBoehnke - Dorsal Scapular Nerve Syndromekeeley_holderBelum ada peringkat
- Dr. Ashish Research ProposalDokumen14 halamanDr. Ashish Research ProposalShobhit RaoBelum ada peringkat
- Week 5 Category 1: Simple Mechanic Case Activity 2 (1&2)Dokumen5 halamanWeek 5 Category 1: Simple Mechanic Case Activity 2 (1&2)api-508474347Belum ada peringkat
- Tendon Transfers For Lateral Pinch: Albert A. Weiss, MD, and Scott H. Kozin, MDDokumen11 halamanTendon Transfers For Lateral Pinch: Albert A. Weiss, MD, and Scott H. Kozin, MDFernando Martín Arce AlvaBelum ada peringkat
- Ankle:: The Two Most Important Ankle Motions (Dorsiflexion and Plantarflexion) Are Assessed and TreatedDokumen6 halamanAnkle:: The Two Most Important Ankle Motions (Dorsiflexion and Plantarflexion) Are Assessed and TreatedGuillaumeBanvilleBelum ada peringkat
- Pi Is 2212628718300215Dokumen5 halamanPi Is 2212628718300215Proactive physiotherapyBelum ada peringkat
- An Overview of Facilitated Stretching - Robert E. McAtee - A-9Dokumen9 halamanAn Overview of Facilitated Stretching - Robert E. McAtee - A-9Tito AlhoBelum ada peringkat
- Maintaining Joint Range of MotionDokumen27 halamanMaintaining Joint Range of MotionKiko KikoBelum ada peringkat
- Halbert Sma 1994Dokumen6 halamanHalbert Sma 1994Irsa SevenfoldismBelum ada peringkat
- Cebu (Velez) General Hospital Department of PediatricsDokumen4 halamanCebu (Velez) General Hospital Department of PediatricsJanelle Estrabela GargaritanoBelum ada peringkat
- Abo IncompatabilityDokumen3 halamanAbo Incompatabilityx483xDBelum ada peringkat
- University in Saudi Arabia PDFDokumen98 halamanUniversity in Saudi Arabia PDFHafiz Iqbal MaulanaBelum ada peringkat
- PreviewpdfDokumen481 halamanPreviewpdfAdams BrunoBelum ada peringkat
- A Survey of Stent Designs PDFDokumen11 halamanA Survey of Stent Designs PDFGabriel Lopez BarajasBelum ada peringkat
- Opd SchedDokumen20 halamanOpd SchedFergie DeactBelum ada peringkat
- AnatoFisio VestibularDokumen17 halamanAnatoFisio VestibularRocío YáñezBelum ada peringkat
- Cruise Ship Health Care Guidelines PrepDokumen8 halamanCruise Ship Health Care Guidelines PrepMaxMusterBelum ada peringkat
- Thesis: Attitude Towards Acupuncture Therapy in ChildrenDokumen21 halamanThesis: Attitude Towards Acupuncture Therapy in Childrenobiero peterBelum ada peringkat
- Exchange TransfusionDokumen13 halamanExchange TransfusionSaba WaheedBelum ada peringkat
- Allied HospitalDokumen6 halamanAllied HospitalMalik Mubeen 007Belum ada peringkat
- 2015 Movement DisordersDokumen567 halaman2015 Movement DisordersAndreea Raluca CimpoiBelum ada peringkat
- A Case Report of Ureteric Calculus Treated With Homoeopathic Medicine, Hydrangea Arborescens 30Dokumen7 halamanA Case Report of Ureteric Calculus Treated With Homoeopathic Medicine, Hydrangea Arborescens 30Baru Chandrasekhar RaoBelum ada peringkat
- Hyphema 140917144203 Phpapp02thsDokumen20 halamanHyphema 140917144203 Phpapp02thsYuda Arie DharmawanBelum ada peringkat
- Sepsis Power Point Slide Presentation - The Guidelines - Implementation For The FutureDokumen25 halamanSepsis Power Point Slide Presentation - The Guidelines - Implementation For The Futuremontie13Belum ada peringkat
- Variants of NormalDokumen9 halamanVariants of NormalFaizah HannyBelum ada peringkat
- ProspectusDokumen92 halamanProspectusAnwer SaidBelum ada peringkat
- South Maine HMO AncillaryDokumen81 halamanSouth Maine HMO AncillaryMaine Trust For Local NewsBelum ada peringkat
- GingivectomyDokumen51 halamanGingivectomyWendy JengBelum ada peringkat
- ADEA CAAPID InstructionsDokumen10 halamanADEA CAAPID Instructionsshyam05_narainBelum ada peringkat
- Baba Farid University of Health Sciences, Sadiq Road, Faridkot Ph. 01639-256232, 256236 Advt. No 06/2020 VacanciesDokumen4 halamanBaba Farid University of Health Sciences, Sadiq Road, Faridkot Ph. 01639-256232, 256236 Advt. No 06/2020 VacanciesSinghTarunBelum ada peringkat
- Bicon Catalog 2012Dokumen68 halamanBicon Catalog 2012Bicon Implant InaBelum ada peringkat