Major Complication of Cirrhosis
Diunggah oleh
Alya Putri KhairaniHak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Major Complication of Cirrhosis
Diunggah oleh
Alya Putri KhairaniHak Cipta:
Format Tersedia
Alya Putri Khairani | 130110110220 | A4
Major Complication of Cirrhosis
The clinical course of patients with
advanced Cirrhosis is often
complicated by a number of important
sequelae that can occur regardless of
the underlying cause of the Liver
Disease
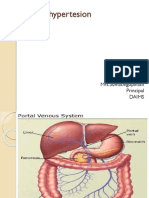
PORTAL HYPERTENSION
DEFINITON
Defined as the elevation of the hepatic venous pressure gradient (HVPG) to >5 mmHg. Portal hypertension is
caused by a combination of two simultaneously occurring hemodynamic processes:
1. Increased intrahepatic resistance to the passage of blood flow through the liver due to cirrhosis and
regenerative nodules
2. Increased splanchnic blood flow secondary to vasodilatation (vasodilatory substances, most importantly
Nitric Oxide Synthase) within the splanchnic vascular bed
CLASSIFICATION
The causes of portal hypertension are usually subcategorized as prehepatic, intrahepatic, and posthepatic
Prehepatic
Affecting the portal venous system before it enters the liver; they include Portal vein thrombosis and Splenic vein
thrombosis. Posthepatic
Encompass those affecting the Hepatic veins and venous drainage to the heart; they include BCS, Venoocclusive
disease, and Chronic right-sided cardiac congestion
Intrahepatic
Represented by the major forms of Cirrhosis
Postsinusoidal causes include venoocclusive disease
Presinusoidal causes include congenital hepatic fibrosis and schistosomiasis
Sinusoidal causes are related to cirrhosis from various causes
CLINICAL FEATURES
Physical findings in cirrhosis that might suggest the presence of portal hypertension include muscle wasting, spider
angiomata, jaundice, abdominal collateral vessels, and an altered mental status
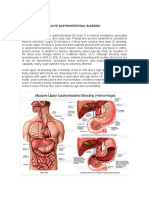
The three primary complications of portal hypertension are Gastroesophageal Varices with Hemorrhage,
Ascites, and Hypersplenism.
Alya Putri Khairani | 130110110220 | A4
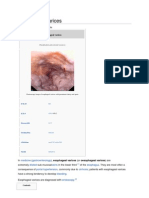
So, in endoscopy, we will find: esophageal or gastric varices, with the development of ascites along with peripheral
edema, or with an enlarged spleen with associated reduction in platelets and white blood cells on routine
laboratory testing
* Gastroesophageal Varices with Hemorrhage
Approximately 515% of cirrhotics per year develop varices, and it is estimated that the majority of
patients with cirrhosis will develop varices over their lifetime. Furthermore, it is anticipated that roughly
one-third of patients with varices will develop hemorrhage
Several factors predict the risk of bleeding, including the severity of cirrhosis (Childs class); the height of
wedged-hepatic vein pressure; the size of the varix; the location of the varix; and certain endoscopic
stigmata, including red wale signs, hematocystic spots, diffuse erythema, bluish color, cherry-red spots, or
white-nipple spots
DIAGNOSIS
Presence of thrombocytopenia; the appearance of an enlarged spleen; or the development of ascites,
encephalopathy and/or esophageal varices with or without bleeding
Interventional radiologic procedures can be performed to determine wedged and free hepatic vein
pressures that will allow for the calculation of a wedged-to-free gradient, which is equivalent to the portal
pressure. The average normal wedged-to-free gradient is 5 mmHg, and patients with a gradient >12
mmHg are at risk for variceal hemorrhage
PREVENTION AND MANAGEMENT
Nonselective -blockers (propranolol, nadolol, and timolol) are the
cornerstone of long-term management in patients with portal
hypertension.
The use of -blockers in patients with cirrhosis is limited by their sideeffect profile, which includes hypotension, fatigue, lethargy, depression,
and dyspnea in patients with associated
pulmonary disease. Due to concomitant diseases such as reactive airway
disease, congestive heart failure, bradycardia, and heart block, 1520% of
patients are unable to take -blockers.
In patients who are candidates for -blocker therapy, dose titration
should be adjusted to patient tolerance
2 SPLENOMEGALY & HYPERSPLENISM
Congestive splenomegaly
Clinical features: presence of an enlarged spleen on physical examination and the development of
thrombocytopenia and leukopenia in patients who have cirrhosis
Some patients will have fairly significant left-sided and left upper quadrant abdominal pain related to an
enlarged and engorged spleen
Hypersplenism with the development of thrombocytopenia is a common feature of patients with cirrhosis and is
usually the first indication of portal hypertension
3 ASCITES
Five major factors are involved in the pathogenesis of
cirrhotogenic
DEFINITION
ascites:
Portal hypertension,
Hypoalbuminemia,
Sodium
The
accumulation
of fluid within
the peritoneal cavity
retention, Water retention, and increased lymph formation.
PATHOGENESIS
Development
of Cirrhotogenic
{) Intrahepatic
resistance Ascites
{) Portal pressure +
Vasodilatation of the Splanchnic arterial system = {)
Production of Splanchnic
lymph.
Vasodilating factors such as nitric oxide Causing activation
of the Renin-Angiotensin-Aldosterone system with the
development of Hyperaldosteronism Sodium retention
The renal effects of {) Aldosterone Sodium retention
Alya Putri Khairani | 130110110220 | A4
Sodium retention fluid accumulation and expansion of the extracellular fluid volume Formation of peripheral
Edema and Ascites.
Hypoalbuminemia and reduced plasma oncotic pressure also contribute to the loss of fluid from the vascular
compartment into the
peritoneal cavity. Hypoalbuminemia is due to decreased synthetic function in a cirrhotic liver.
CLINIAL FINDINGS
In abdominal girth that is often accompanied by the development of peripheral edema. The development
of ascites is often insidious
Hepatic hydrothorax may contributing to respiratory symptoms
Patients with massive ascites are often malnourished and have muscle wasting and excessive fatigue and
weakness
DIAGNOSIS
Abdominal imaging
Bulging flanks, fluid wave, or may have the presence of shifting dullness.
This is determined by taking patients from a supine position to lying on either their left or right side and
noting the movement of the dullness top percussion
Diagnostic paracentesis be performed to characterize the fluid, include the determination of total protein
and albumin content, blood cell counts with differential, and cultures. In the appropriate setting, amylase
may be measured and cytology performed
4 SPONTANEOUS BACTERIAL PERITONITIS
DEFINITION
A common and severe complication of ascites characterized by spontaneous infection of the ascitic fluid without an
intraabdominal source
ETIOLOGY & PATHOGENESIS
Bacterial translocation is the presumed mechanism for development of SBP, with gut flora traversing the intestine
into mesenteric lymph nodes, leading to bacteremia and seeding of the ascitic fluid. The most common organisms
are Escherichia coli and other gut bacteria; however, gram-positive bacteria, including Streptococcus viridans,
Staphococcus aureus, and Enterococcus sp., can also be found
DIAGNOSIS
Fluid sample has an absolute neutrophil count >250/mm3
Bedside cultures should be obtained when ascitic fluid is tapped
May present with fever, altered mental status, elevated white blood cell count, and abdominal pain or
discomfort, or they may present without any of these features
Peritoneal taps are important for making the diagnosis
TREATMENT
Use of a third-generation cephalosporin such as cefotaxime or ceftazidime, given at a dosage of 2 g/8 h. Other
third-generation cephalosporins, such as ceftizoxime or ceftriaxone, are also suitable antibiotics. The
cephalosporins have been shown to be as effective
as, if not more effective than, combinations of ampicillin and an aminoglycoside
5 HEPATORENAL SYNDROME
DEFINITION
Characterized by functional kidney failure in patients with end-stage liver disease. It results in intense renal
vasoconstriction without any other identifiable kidney pathology
Type 1 hepatorenal syndrome
Characterized by rapid and progressive impairment of renal function defined by a doubling the initial serum
creatinine to a level higher than 2.5 mg/dL or a 50% reduction of the initial 24-hour creatinine clearance to
a level lower than 20 mL/min in less than 2 weeks
Alya Putri Khairani | 130110110220 | A4
Type 2 hepatorenal syndrome
Impairment in renal function (serum creatinine > 1.5 mg/dL) that does not meet the criteria for type 1.
Prerenal failure is a preischemic state and may lead to ischemic tubular necrosis
PATHOGENESIS
Cirrhosis Activation of the Renin-Angiotensin and sympathetic nervous systems {) Levels of renin,
aldosterone, and norepinephrine.
If undergo diuresis successfully () Levels of renin, aldosterone, norepinephrine, and antidiuretic
hormone
In patients with end-stage liver disease complicated by hepatorenal syndrome () Systemic vascular
resistance and splanchnic arteriolar vasodilation
and norepinephrine
() Levels of renin, aldosterone, antidiuretic hormone,
DIFFERENTIAL DIAGNOSIS
Acute tubular necrosis and other forms of renal disease such as glomerulonephritis and vasculitis
CLINICAL FINDINGS
TREATMENT
Preventive measures
Hepatorenal syndrome develops in patients with systemic
bacterial infections (ie, spontaneous bacterial peritonitis or
severe alcoholic hepatitis, or both), and it is important to
provide prophylactic treatment
to guard against its development. This includes the
administration of IV albumin (1.5 g/kg) at the time of
diagnosis of spontaneous bacterial peritonitis or sepsis, and
another dose of albumin (1.0 g/kg) after 48 hours of
antibiotic treatment
Vasopressor therapy
Accumulating data suggest that combination therapy with
midodrine and octreotide may be effective and safe. The
rationale for such therapy is that midodrine is a systemic
vasoconstrictor and addresses the question of inappropriate
vasodilation, and octreotide is an inhibitor of endogenous
vasodilators
6 HEPATIC ENCEPHALOPATHY
DEFINITION
An alteration in mental status and cognitive function occurring in the presence of liver failure. In acute liver injury
with fulminant hepatic failure, the development of encephalopathy is a requirement for a diagnosis of fulminant
failure. Encephalopathy is much more commonly seen in patients with chronic liver disease
PATHOGENESIS
Alya Putri Khairani | 130110110220 | A4
Although the precise pathogenesis of hepatic
encephalopathy is unknown, accumulation of nitrogenous
products derived from the gut can have adverse effects on
brain function and is believed to play a major role
CLINICAL FINDINGS
Physical examination
Fetor hepaticus; this is a pungent breath odor caused
by the breakdown products of sulfur-containing amino
acids such as cysteine and methionine and consisting of
dimethyl sulfides methanethiol and ethanethiol
Asterixis or a metabolic flapping tremor
Focal neurologic abnormalities such as increased deep
tendon reflexes, unilateral or bilateral Babinski sign, and
other findings such as ataxia,
dysarthria, tremor, or myopathy, usually with longstanding
chronic systemic shunting
Mental status changes
TREATMENT
7 MALNUTRITION IN CIRRHOSIS
Because the liver is principally involved in the regulation of protein
and energy metabolism in the body, it is not surprising that
patients with advanced liver disease are commonly malnourished.
Once patients become cirrhotic, they are more catabolic, and
muscle protein is
Metabolized
8 ABNORMALITIES IN COAGULATION
There is decreased synthesis of clotting factors and impaired
clearance of anticoagulants. In addition, patients may have
thrombocytopenia from hypersplenism due to portal hypertension.
Vitamin Kdependent clotting factors are Factors II, VII, IX, and X.
Vitamin K requires biliary excretion for its subsequent absorption; thus, in patients with chronic cholestatic
syndromes, vitamin K absorption is frequently diminished.
More commonly, the synthesis of vitamin Kdependent clotting factors is diminished because of a decrease in
hepatic mass, and under these circumstances administration of parenteral vitamin K does not improve the clotting
factors or the prothrombin time. Platelet function is often abnormal in patients with chronic liver disease, in
addition to decreases in platelet levels due to hypersplenism.
Alya Putri Khairani | 130110110220 | A4
9 BONE DISEASE IN CIRRHOSIS
Osteoporosis is common in patients with chronic cholestatic liver disease because of malabsorption of vitamin D
and decreased calcium ingestion. The rate of bone resorption exceeds that of new bone formation in patients with
cirrhosis resulting in bone loss
10 HEMATOLOGIC ABNORMALITIES IN CIRRHOSIS
Numerous hematologic manifestations of cirrhosis are present, including anemia from a variety of causes including
hypersplenism, hemolysis, iron deficiency, and perhaps folate deficiency from malnutrition. Macrocytosis is a
common abnormality in red blood cell morphology seen in patients with chronic liver disease, and neutropenia may
be seen as a result of hypersplenism
References:
Harrison Internal Medicine 17th edition
Current Diagnosis and Treatment in Gastroenterology, Hepatology, and
Endoscopy
Anda mungkin juga menyukai
- Hepatorenal Syndrome: Causes, Tests, and Treatment OptionsDari EverandHepatorenal Syndrome: Causes, Tests, and Treatment OptionsPenilaian: 4.5 dari 5 bintang4.5/5 (2)
- Portal Hypertension, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsDari EverandPortal Hypertension, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsBelum ada peringkat
- JURNAL Ascites PDFDokumen9 halamanJURNAL Ascites PDFican_parlenteBelum ada peringkat
- Portal HypertensionDokumen11 halamanPortal Hypertensionsaeid seyedraoufiBelum ada peringkat
- Presented By: Medicine Unit 1Dokumen95 halamanPresented By: Medicine Unit 1Abdullah Muceddidi100% (1)
- Approach To Acute Upper Gastrointestinal Bleeding in Adults - UpToDateDokumen48 halamanApproach To Acute Upper Gastrointestinal Bleeding in Adults - UpToDateDũng Hoàng Nghĩa TríBelum ada peringkat
- AscitesDokumen36 halamanAscitesmiki0% (1)
- Pathohysiology of Ascites: Waleed Al-HamoudiDokumen36 halamanPathohysiology of Ascites: Waleed Al-Hamoudiarina31Belum ada peringkat
- B.SC Nursing Medical Surgical Nursing - I Unit: Iv - Nursing Management of Patients With Disorders of Digestive System Portal HypertensionDokumen32 halamanB.SC Nursing Medical Surgical Nursing - I Unit: Iv - Nursing Management of Patients With Disorders of Digestive System Portal HypertensionPoova RagavanBelum ada peringkat
- Ascites: Pathogenesis and Clinical ApproachDokumen34 halamanAscites: Pathogenesis and Clinical ApproachPooja ShashidharanBelum ada peringkat
- Portal Hypotension: Clinical AssignmentDokumen8 halamanPortal Hypotension: Clinical AssignmentM shayan JavedBelum ada peringkat
- Prepared by Inzar Yasin Ammar LabibDokumen47 halamanPrepared by Inzar Yasin Ammar LabibJohn Clements Galiza100% (1)
- UGIB HanifDokumen90 halamanUGIB HanifHanif KhairudinBelum ada peringkat
- Ascites: Fredric D. GordonDokumen15 halamanAscites: Fredric D. GordonNancy Mac Lean BalboaBelum ada peringkat
- AscitesascitesDokumen15 halamanAscitesascitesKevinJuliusTanadyBelum ada peringkat
- Esophageal VaricesDokumen9 halamanEsophageal VaricesErina WahyuniBelum ada peringkat
- Portal HypertensionDokumen13 halamanPortal HypertensionCiprian BoesanBelum ada peringkat
- Done By: Dana Othman: AscitesDokumen28 halamanDone By: Dana Othman: Ascitesraed faisalBelum ada peringkat
- AscitesDokumen5 halamanAscitesEeshuAomBelum ada peringkat
- Portal HypertensionDokumen13 halamanPortal HypertensionEmmaBelum ada peringkat
- Ascitis PDFDokumen17 halamanAscitis PDFLeonardo MagónBelum ada peringkat
- Ascites: Pathogenesis and Therapeutic Principles: Søren Møller, Jens H. Henriksen & Flemming BendtsenDokumen10 halamanAscites: Pathogenesis and Therapeutic Principles: Søren Møller, Jens H. Henriksen & Flemming BendtsenAWw LieyaBelum ada peringkat
- Portal HypertensionDokumen65 halamanPortal HypertensionVenu MadhavBelum ada peringkat
- Portal HypertensionDokumen41 halamanPortal Hypertensionams_1234100% (2)
- Prepared by Inzar Yasin Ammar LabibDokumen47 halamanPrepared by Inzar Yasin Ammar LabibdiaBelum ada peringkat
- Lower Gastrointestinal Bleeding (LGIB)Dokumen41 halamanLower Gastrointestinal Bleeding (LGIB)api-196413370% (1)
- Di Lucio NalDokumen8 halamanDi Lucio NalElisabeth Correa De GanteBelum ada peringkat
- Ascitis ImportanteDokumen17 halamanAscitis Importantedanyescalerapumas24Belum ada peringkat
- Presentation Liver CirrhosisDokumen26 halamanPresentation Liver CirrhosisFaye Dominique Roxas PalmaresBelum ada peringkat
- Liver Cirrhis Due To Upper Gi BleedingDokumen5 halamanLiver Cirrhis Due To Upper Gi BleedingNathaniel BudayBelum ada peringkat
- Portal HypertensionDokumen23 halamanPortal HypertensionSumathi Gopinath100% (1)
- HcirhosisDokumen11 halamanHcirhosisChetendra IndoliaBelum ada peringkat
- W J C M P R: Orld Ournal of Urrent Edical and Harmaceutical EsearchDokumen3 halamanW J C M P R: Orld Ournal of Urrent Edical and Harmaceutical EsearchVivi DeviyanaBelum ada peringkat
- Gi BleedingDokumen22 halamanGi BleedingAndreea GociuBelum ada peringkat
- GI Bleeding-1Dokumen38 halamanGI Bleeding-1Ibsa ShumaBelum ada peringkat
- Liver CirrhosisDokumen8 halamanLiver CirrhosisDiana DeciuBelum ada peringkat
- Pa Tho Physiology of Liver Cirrhosis - MercyDokumen7 halamanPa Tho Physiology of Liver Cirrhosis - Mercymersenie_TheovercomerBelum ada peringkat
- Upper GIB Lecture and Presentation.Dokumen75 halamanUpper GIB Lecture and Presentation.Williams Emmanuel AdeyeyeBelum ada peringkat
- AscitesDokumen32 halamanAscitesIsaac MwangiBelum ada peringkat
- Ascitis RefractariaDokumen11 halamanAscitis RefractariaGiselle L. AlcaláBelum ada peringkat
- HDA UPTODATE Approach To Acute Upper Gastrointestinal Bleeding in AdultsDokumen12 halamanHDA UPTODATE Approach To Acute Upper Gastrointestinal Bleeding in AdultsLeoberto Batista Pereira SobrinhoBelum ada peringkat
- Hepatorenal Syndrome - UpToDateDokumen26 halamanHepatorenal Syndrome - UpToDateAssault AmphibiansBelum ada peringkat
- NCP CKD From CaneDokumen74 halamanNCP CKD From CaneSheela Khrystyn LeeBelum ada peringkat
- Sirosis Hepatis: Sigit Widyatmoko Fakultas Kedokteran UMSDokumen66 halamanSirosis Hepatis: Sigit Widyatmoko Fakultas Kedokteran UMSArif Rahman DmBelum ada peringkat
- Acute Gastrointestinal Bleeding Upper GI BleedingDokumen18 halamanAcute Gastrointestinal Bleeding Upper GI BleedingAldwin AyuyangBelum ada peringkat
- Renal SyndromeDokumen13 halamanRenal SyndromeAndreas KristianBelum ada peringkat
- Hematemesis Melena (Upper Gi Bleeding)Dokumen134 halamanHematemesis Melena (Upper Gi Bleeding)Mardoni Efrijon100% (1)
- PBLDokumen22 halamanPBLOmar AhmedBelum ada peringkat
- Dr. S.P. Hewawasam (MD) Consultant Gastroenterologist/Senior Lecturer in PhysiologyDokumen33 halamanDr. S.P. Hewawasam (MD) Consultant Gastroenterologist/Senior Lecturer in PhysiologyAjung SatriadiBelum ada peringkat
- Esophageal VaricesDokumen12 halamanEsophageal VaricesgemergencycareBelum ada peringkat
- 58 Lower Gastrointestinal BleedDokumen4 halaman58 Lower Gastrointestinal BleedLuphly TaluvtaBelum ada peringkat
- Portal HypertensionDokumen23 halamanPortal HypertensionSumathi GopinathBelum ada peringkat
- Massive Upper Gastrointestinal HemorrhageDokumen73 halamanMassive Upper Gastrointestinal HemorrhageDONALD UNASHEBelum ada peringkat
- Cirrhosis in Adults - Overview of Complications, General Management, and PrognosisDokumen24 halamanCirrhosis in Adults - Overview of Complications, General Management, and PrognosisAhraxazel Galicia ReynaBelum ada peringkat
- Upper GI Bleed - SymposiumDokumen38 halamanUpper GI Bleed - SymposiumSopna ZenithBelum ada peringkat
- Approach To UGI BleedDokumen18 halamanApproach To UGI BleedBiji GeorgeBelum ada peringkat
- Clinical Portal Hyoer TensionDokumen8 halamanClinical Portal Hyoer TensionAhmed ImranBelum ada peringkat
- Acute Liver Failure 2012Dokumen47 halamanAcute Liver Failure 2012nancy voraBelum ada peringkat
- 21 Ascitis PDFDokumen11 halaman21 Ascitis PDFlupiBelum ada peringkat
- Portal Vein Thrombosis, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsDari EverandPortal Vein Thrombosis, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsBelum ada peringkat
- Iccu / Cicu: Patients Heart Attacks Unstable Angina Cardiac DysrhythmiaDokumen4 halamanIccu / Cicu: Patients Heart Attacks Unstable Angina Cardiac DysrhythmiaAlya Putri KhairaniBelum ada peringkat
- Uric Acid and Its MetabolismDokumen3 halamanUric Acid and Its MetabolismAlya Putri KhairaniBelum ada peringkat
- Pericardium:: AnatomyDokumen4 halamanPericardium:: AnatomyAlya Putri KhairaniBelum ada peringkat
- Histogenesis of BoneDokumen6 halamanHistogenesis of BoneAlya Putri KhairaniBelum ada peringkat
- Kinesiology of Shoulder ComplexDokumen7 halamanKinesiology of Shoulder ComplexAlya Putri KhairaniBelum ada peringkat
- Bleeding: Blood VesselDokumen2 halamanBleeding: Blood VesselAlya Putri KhairaniBelum ada peringkat
- Anatomy of Oral RegionDokumen6 halamanAnatomy of Oral RegionAlya Putri KhairaniBelum ada peringkat
- Herpes VirusesDokumen6 halamanHerpes VirusesAlya Putri KhairaniBelum ada peringkat
- Clobetasol Propionate and Urea CreamDokumen4 halamanClobetasol Propionate and Urea CreamAlya Putri KhairaniBelum ada peringkat
- Leptospira SP.: Leptospira Are Spiral Bacteria (Spirochaete) in The Family of LeptospiraceaeDokumen3 halamanLeptospira SP.: Leptospira Are Spiral Bacteria (Spirochaete) in The Family of LeptospiraceaeAlya Putri KhairaniBelum ada peringkat
- Congenital SyphilisDokumen4 halamanCongenital SyphilisAlya Putri Khairani100% (1)
- Influenza: Laboratory FindingsDokumen6 halamanInfluenza: Laboratory FindingsAlya Putri KhairaniBelum ada peringkat
- Physiology of MastigationDokumen3 halamanPhysiology of MastigationAlya Putri KhairaniBelum ada peringkat
- Components of Breast MilkDokumen2 halamanComponents of Breast MilkAlya Putri KhairaniBelum ada peringkat
- Hemolytic Anemia: MorphologyDokumen10 halamanHemolytic Anemia: MorphologyAlya Putri KhairaniBelum ada peringkat
- The Body Fluid CompartmentsDokumen6 halamanThe Body Fluid CompartmentsAlya Putri KhairaniBelum ada peringkat
- Differential Diagnosis of WheezingDokumen3 halamanDifferential Diagnosis of WheezingAlya Putri KhairaniBelum ada peringkat
- Nevada Sagebrush Archives For 03152016Dokumen10 halamanNevada Sagebrush Archives For 03152016The Nevada SagebrushBelum ada peringkat
- 14.ergonomic Workstation Design For Science Laboratory (Norhafizah Rosman) PP 93-102Dokumen10 halaman14.ergonomic Workstation Design For Science Laboratory (Norhafizah Rosman) PP 93-102upenapahangBelum ada peringkat
- Disaster Triage Forgotten Lessons in Pandemic Covid-19 Management - Dr. Yogi Prabowo, SpOT (K)Dokumen23 halamanDisaster Triage Forgotten Lessons in Pandemic Covid-19 Management - Dr. Yogi Prabowo, SpOT (K)Clara EverlastBelum ada peringkat
- Material Safety Data Sheet of Bee VenomDokumen2 halamanMaterial Safety Data Sheet of Bee VenommnemonicsBelum ada peringkat
- Freed TestimonyDokumen12 halamanFreed TestimonyCasey SeilerBelum ada peringkat
- Single Cases Efim 2012Dokumen56 halamanSingle Cases Efim 2012Careca Santacruz CarrascoBelum ada peringkat
- Bowel Preparation For Pediatric Colonoscopy AnakDokumen8 halamanBowel Preparation For Pediatric Colonoscopy AnakrantaikarbonBelum ada peringkat
- Lacosamide TreatmentDokumen13 halamanLacosamide TreatmentawinsyBelum ada peringkat
- Lab Values and Vital Signs PDFDokumen4 halamanLab Values and Vital Signs PDFmike_steven12Belum ada peringkat
- Presentasi Tentang RokokDokumen9 halamanPresentasi Tentang Rokokjugumon_46Belum ada peringkat
- 2012 NeoReviews DiscDokumen22 halaman2012 NeoReviews DiscgtheofanopoulosBelum ada peringkat
- Bronchopneumonia PP 2003Dokumen31 halamanBronchopneumonia PP 2003Rizky FadhilaBelum ada peringkat
- Abg Analysis ReviewerDokumen21 halamanAbg Analysis ReviewerAyiessa_AJBelum ada peringkat
- Endocrinologists Clinic Schedule 2019Dokumen1 halamanEndocrinologists Clinic Schedule 2019ranBelum ada peringkat
- NCV Findings in Lower LimbsDokumen30 halamanNCV Findings in Lower LimbsKarthik BhashyamBelum ada peringkat
- Direction: Kurnihayati, M.PDDokumen28 halamanDirection: Kurnihayati, M.PDKurnihayati MuklasBelum ada peringkat
- 50 Studies - Every - Obstetrician - Gynecologist - Should - Know - First - EditionDokumen321 halaman50 Studies - Every - Obstetrician - Gynecologist - Should - Know - First - EditionMiryam Diaz100% (1)
- Fixation of Mandibular Fractures With 2.0 MM MiniplatesDokumen7 halamanFixation of Mandibular Fractures With 2.0 MM MiniplatesRajan KarmakarBelum ada peringkat
- The Blue People of Troublesome CreekDokumen9 halamanThe Blue People of Troublesome Creekapi-3173246110% (1)
- Medical Biotech Pharmaceutical Sales in Kansas City MO Resume James DebrickDokumen2 halamanMedical Biotech Pharmaceutical Sales in Kansas City MO Resume James DebrickJamesDebrickBelum ada peringkat
- Atria Risk Score - Jaha 2013Dokumen11 halamanAtria Risk Score - Jaha 2013LR NesBelum ada peringkat
- Final Pediatric Basic Life SupportDokumen26 halamanFinal Pediatric Basic Life SupportMohamed Ghanem100% (2)
- Autopsy Toxicology Origins: New Suicide Modalities: The Use of Helium As An Oxygen Displacement AgentDokumen1 halamanAutopsy Toxicology Origins: New Suicide Modalities: The Use of Helium As An Oxygen Displacement AgentAluísio RomaBelum ada peringkat
- McqsDokumen14 halamanMcqsBushra Mahboob100% (1)
- Salinan SLIDE - Cairan Amnion Dan Oligo - ObgynDokumen6 halamanSalinan SLIDE - Cairan Amnion Dan Oligo - ObgynariniBelum ada peringkat
- Practical Algorithms in Pediatric GastroenterologyDokumen4 halamanPractical Algorithms in Pediatric GastroenterologyHitesh Deora0% (1)
- STSurg NumntDokumen11 halamanSTSurg NumntrohiBelum ada peringkat
- Sample CCMSADokumen8 halamanSample CCMSAVasantha Eswaraka0% (1)
- Type 2 Diabetes Final DraftDokumen14 halamanType 2 Diabetes Final DraftAbbie HillsBelum ada peringkat
- PTC Course ManualDokumen64 halamanPTC Course Manualaditya brahmantio sujakaBelum ada peringkat