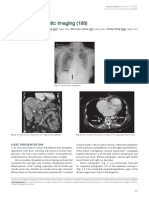
Reversed Carvallo's Sign
Diunggah oleh
rxrkDeskripsi Asli:
Hak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Reversed Carvallo's Sign
Diunggah oleh
rxrkHak Cipta:
Format Tersedia
16 Coumel P. Supraventricular tachycardias. In: Krikler DM, Godwin JF, eds. Cardiac arrhythmias.
London: WB Saunders,
1975:116-143
17 Marquez-Montes J, Rufilanchas JJ, Esteve-Alderete JJ, Mendez
J, Ugarte J, Rodriguez E, et al. Tratamiento quirurgico en 24
pacientes con sindrome de Wolff-Parkinson-White y taquicardias: diagnostic0 topografico de 10s haces de Kent y evaluation de
resultados. Rev Esp Cardiol 1981; 34:271-281
18 Josephson ME, Horowitz LN, Farshidi A, Spear JF, Kastor JA,
Moore EN. Recurrent sustained ventricular tachycardia: 2.
Endocardia mapping. Circulation 1978; 57:440447
19 Janse MJ, Van Capelle FJL, Anderson RH, Touboul P, Billette J.
Electrophysiology and structure of the atrioventricular node of
the isolated rabbit heart. In: Wellens HJJ, Lie KI, et al, eds. The
conduction system ofthe heart. Leiden: Stenfert & Kroese, 1976:
296-315
Reversed Rivero-Carvallo's Sign in
Right-Sided Hypertrophic
Obstructive Cardiomyopathy*
Kyozo Ishikawa, M. D . , E C . C . P ; Fukiyo Hirata, M . D . ;
Shunkichi Hirata, M . D . ; and Masarnichi lshikawa, M.D
An 18-year-old patient had right-sided hypertrophic
obstructive cardiomyopathy. His case was quite unique in
that the intensity of the systolic murmur was apparently
decreased during the inspiratory phase and increased during the expiratory phase (reversed Rivera-Carvalloi sign).
ypertrophic cardiomyopathy is classically associated
with predominant left-sided obstruction, but cases of
isolated and dominant right ventricular outflow obstruction
(RVO) have been described.14 I t is usually expected that the
*From the Kyorin University School of Medicine, Second Department of Internal Medicine, Tokyo, Japan.
Reprint requests: D1: Ishikawa, Kyorin University, 6-20 Shinkawa,
Mitaka City, Tokyo, lapan
Expiration
systolic m u r m u r resulting from subpulmonic stenosis in RVO
may b e increased in intensity during t h e inspiratory phase
and decreased during t h e expiratory phase (Rivero-Carvallo's
sign). T h e present patient with RVO in hypertrophic cardiornyopathy was quite unique in that the intensity of the
systolic m u r m u r was apparently decreased during t h e inspiratory phase and increased during the expiratory phase
(reversed Rivero-Carvallo's sign).
The patient, an 18-year-old man, was referred to us for cardiac
evaluation because of cardiac murmur. He had been in good health
and asymptomatic. He had never experienced chest pain or any kind
of unconsciousness. Examination revealed a grade 316 systolic
murmur with late systolic accentuation. This systolic murmur
became louder on expiration and quieter on inspiration (Fig 1).
Intracardiac phonocardiogram recorded in the right ventricular
outflow portion apparently demonstrated that the systolic murmur
became louder on expiration than on inspiration (Fig 2). Cardiac
catheterization revealed no intracardiac shunts, and a systolic
gradient of 7 mm Hg was recorded between the right ventricular
inflow and outflow tracts (Fig3). The pulmonary artery pressure was
1718 mm Hg. No pressure gradient was recorded in the left
ventricular cavity. Electrocardiograms showed right axis deviation
and right ventricular hypertrophy (Fig 4).
A selective angiogram with right ventricular injection revealed
protrusion of the interventricular septum into the right ventricular
outflow tract. Left ventricular obstruction was not demonstrated by
the left ventricular angiogram. Echocardiography demonstrated a
thick interventricular septum (27 mm) but did not reveal systolic
fluttering of the pulmonary valve, which was considered to be
characteristic of RV0.3.4
The data from t h e cardiac catherization and angiography
demonstrated t h e presence of isolated RVO. T h e systolic
pressure gradient within the right ventricle was slight in
degree (7 m m Hg) b u t apparently nonartifactual. D u r i n g t h e
cardiac catheterization, t h e pressure recordings within t h e
right ventricle were carefully repeated several times, reveal-
Inspiration
FIGURE
1. Respiratory change in the intensity of systolic murmur. During expiration the intensity of the
systolic murmur was increased whereas its intensity was markedly decreased during inspiration.
Reversed Riveco-Carvallo's Sign (lshikawa eta/)
Downloaded From: http://journal.publications.chestnet.org/ on 12/12/2015
matim
Expiration
FIGURE
2. Intracardiac phonocardiography recorded in the outflow tract ofthe right ventricle. ?he systolic
murmur became louder on expiration than on inspiration.
ing the constant existence of a systolic pressure gradient
within the right ventricle. It seems most likely that the
systolic murmur in the present case originated from subpulmonic stenosis due to RVO. The question then arises as to
why the systolic murmur became louder in expiration and
not in inspiration. In cases where the systolic murmur is from
a right-sided origin, its intensity would tend to be increased
in inspiration, which is commonly understood as RiveroCarvallo's sign. However, the systolic murmur in the present
case apparently increased in expiration, which is
diametrically opposite to Ftivero-Cwallo's sign. The precise
mechanism responsible for such a "reversed Rivero-Carvallo's sign" remains unclear. However, it is tempting to
speculate that an increase in the venous return into the right
ventricle in inspiration may dilate the dimensions of the right
ventricle as well as the obstructed portion of the right
PA
ventricular o u a o w tract. As a result, the systolic murmur
originating from the RVO may b e decreased. Such a reversed
Rivero-Cwallo's sign has never been described previously
in ~ u b l i s h e dcases with RV0.14
The degree of the right intraventricular systolic pressure
daerences in a number of RVO collected from published
reports was found to vary from 7 to 118 mm Hg.' It would
appear that the distensibility of the obstructed portion may
b e ereater in mild cases than in more severe cases. Consequently, in mild cases such as the present case, an increase in
the venous return in inspiration might dilate the obstructed
portion with a resultant decrease in the intensity of the
systolic murmur. On the other hand, in severe cases, the
hstensibility and dilatation of the obstructed portion could
not be expected to decrease the systolic murmur to such an
extent.
RV
RA
FIGURE
3. Right heart catheterization. The pressure was continuously recorded while the catheter tip was
being slowly drawn from the pulmonary artery to the right atrium. n e r e was a slight but clearly apparent
pressure gradient between the right ventricular outflow portion and inflow portion.
CHEST 1 83 I 4 1 Aprfl, 1983
Downloaded From: http://journal.publications.chestnet.org/ on 12/12/2015
6QS
VI
v
2
v
3
v
4
1/2
112
112
v
5
I t is possible b u t not certain that, with advancing severity
of this disease, the intensity of t h e systolic m u r m u r might
vary from inspiratory decrease to inspiratory increase. However, long-term follow-up observations will b e required to
confirm t h e validity of such a hypothesis.
1 Lockhart A. Charpentier S, Bourdarias JP, Ismail MB, Ourbak P,
Scebat L. Right ventricular involvement in obstructive cardiomyopathies; haemodynamic studies in 13 cases. Br Heart J
1966; 28:122
2 Momw AG, Fisher RD, Fogarty TJ. Isolated hypertrophic
obstruction to right ventricular outflow: clinical, hemodynamic,
and angiographic findings before and after operative treatment.
Am Heart J 1969; 77:814
3 Cardiel EA, Alonso M, Delcan JL, Menarguez L: Echocardiographic sign of right-sided hypertrophic obstructive cardiomyopathy. Br Heart J 1978; 40:1321
4 Kishimoto C, Kaburagi T, Takayam S, Kanyu I, Yokoyama S,
Ekatsu Y: A case of hypertrophic obstructive cardiomyopathy
with isolated obstruction to the right ventricular outflow: the
echocardiographic findings. J Cardiography 1980; 10:881
Azathioprine-Associated
Pulmonary Dysfunction*
Michael J. Krowka, M.D.t; Richard I . Breuer, M.D.S;and
Thomas]. Kehoe, M.D.5
We present a case of azathioprine-associated alveolitis
diagnosed by gallium-67 scanning and transbronchial biopsy. I h e patient denied respiratory symptoms, exhibited
spiking fevers, and had normal chest roentgenograms.
Allopurinol inhibition of a z a t h i o p ~ emetabolism may have
been a contributing factor.
ulmonary toxicity of immunosuppressive and cytotoxic
agents has been recently reviewed.'.' Respiratory dysfunction is usually characterized by dyspnea, cough, abnormal pulmonary function tests, and chest roentgenographic
-
*From the Department of Medicine, Evanston Hospital, Northwestern University Medical School, Evanston, Illinois.
tResident in Internal Medicine.
$Associate Professor, Division of Gastroenterology.
%AssociateAttending. Division of Pulmonary Medicine.
696
Downloaded From: http://journal.publications.chestnet.org/ on 12/12/2015
v6
F I G U R E4. Electrocardiogram showing right
axis deviation and right ventricular hypertrophy.
changes in a febrile patient. Early detection of such toxicity,
prior to chest roentgenographic abnormalities, has been
described and may have a significant impact o n morbidity
and ~ n o r t a l i t y .We
~ describe a patient with azathioprinerelated pulmonary dysfunction characterized by normal
findings o n c h e s t r o e n t g e n o g r a m a n d a b n o r m a l galli~m-67(~~G
lung
a ) scan.
A 35-year-old man was admitted for evaluation of intermittent
fever (39.4OC). Crohn's disease had been diagnosed when he was
aged 17. Four bowel operations performed because of obstruction or
fistulas resulted in an ileostomy in 1970. Subsequent medical
therapy included a two-month trial of azulfidine because of radiologic demonstration ofileal recurrence two years prior to admission.
Kidney stones were passed in 1971, 1972, and 1979. Stone analysis
indicated 90 percent urate in each instance. Allopurinol therapy was
begun two years prior to admission and continued at doses ranging
from 100 to 200 mglday. Eight months prior to admission, ileal
obstruction resolved with tube decompression and initiation of
prednisone therapy, 60 mg/day. The prednisone was decreased to 20
mg/day, but four months later bleeding from the ileum recurred.
Azathioprine, 50 mgtday, along with prednisone, 40 mg/day, successfully controlled the bleeding. By one month prior to admission,
prednisone had been reduced to 40 mg every other day and
azathioprine had been increased to 125 mg/day. At no time did the
patient complain of respiratory difficulties.
Physical examination indicated blood pressure of 120180 mm Hg
without orthostatic changes. Temperature was 39.1C orally, respirations 18 per minute, with a regular pulse rate of SO per minute. The
chest was clear to auscultation and percussion. Cardiac examination
was within normal limits. Abdominal examination was significant for
mild, &se tenderness without rebound or hepatosplenomegaly.
There was no adenopathy, and the neurologic examination was
normal.
Fever workup included cultures of induced sputum, urine, blood,
spinal fluid, and bone marrow. All were negative. Chest roentgenograms were normal. The WBC was elevated to 15,50O/cu mm, with
65 percent polymorphonuclear leukocytes and no eosinophils.
Atypical lymphocytes were not seen on the peripheral smear.
Antinuclear antibody and rheumatoid factor titers were less than
1:20. Lymphocyte stimulation, immune complex, and complement
studies were not done. Hepatorenal function was normal, and the
urinalysis was unremarkable. Forty-eight hours after admission,
azathioprine and allopurinol therapy was stopped, and prednisone
administration continued at 40 mg/day. AGCascan obtained to locate
a possible abdominal abscess was unremarkable. However, both
lungs demonstrated spectacular uptake at 6, 24, and 48 hours after
A z a t h i i n e - W a t e d Pulmonary Dysfunction (Krowke et al)
Anda mungkin juga menyukai
- Reversed Rlvero-Carvallo's Sign in Right-Sided Hypertrophic Obstructive CardiomyopathyDokumen3 halamanReversed Rlvero-Carvallo's Sign in Right-Sided Hypertrophic Obstructive CardiomyopathySergio RodriguezBelum ada peringkat
- Echo Case Ao RegurgDokumen3 halamanEcho Case Ao Regurgdgina8800Belum ada peringkat
- A Case Report of Pseudo Wellenssyndrome in Patient WithpulmonaryembolismDokumen5 halamanA Case Report of Pseudo Wellenssyndrome in Patient WithpulmonaryembolismIJAR JOURNALBelum ada peringkat
- Massive Pulmonary Embolism: A Case Report and Review of LiteratureDokumen6 halamanMassive Pulmonary Embolism: A Case Report and Review of LiteratureCATHERINE SIENNA ALTARBelum ada peringkat
- Department of Internal Medicine Ii and Phthysiatry: - Rajkumar Subasaravanan Subgroup "12"Dokumen57 halamanDepartment of Internal Medicine Ii and Phthysiatry: - Rajkumar Subasaravanan Subgroup "12"Suba Saravanan 12Belum ada peringkat
- Xrayand ElectrocardiogramDokumen104 halamanXrayand ElectrocardiogramdrelvBelum ada peringkat
- Severe Pulmonary Arterial Hypertension Due To Angiostrongylosus VasorumDokumen4 halamanSevere Pulmonary Arterial Hypertension Due To Angiostrongylosus VasorumPutri AfrindaBelum ada peringkat
- Epsilon WaveDokumen3 halamanEpsilon WaveMiguel SilvaBelum ada peringkat
- EBSTEIN'S ANOMALY Dhini - Maju 17 Juli 2014Dokumen29 halamanEBSTEIN'S ANOMALY Dhini - Maju 17 Juli 2014Azizi PranokoBelum ada peringkat
- Journal of Arrhythmia: Case ReportDokumen2 halamanJournal of Arrhythmia: Case ReportMusafa WidagdoBelum ada peringkat
- EKG Self Study GuideDokumen26 halamanEKG Self Study GuideDadank Zeand ThOmankBelum ada peringkat
- 3 Heart InternetNewDokumen55 halaman3 Heart InternetNewCoral Srinivasa RamaluBelum ada peringkat
- Assignment: Applied MedicineDokumen15 halamanAssignment: Applied MedicineKhadija BakhtawarBelum ada peringkat
- T 20 CardiologyDokumen51 halamanT 20 Cardiologydrkhalid12100% (3)
- Effect of Right Ventricular Function and Pulmonary Pressures On Heart Failure PrognosisDokumen7 halamanEffect of Right Ventricular Function and Pulmonary Pressures On Heart Failure PrognosisMatthew MckenzieBelum ada peringkat
- TUGAS Ventricular Septal DefectDokumen8 halamanTUGAS Ventricular Septal DefectMohammad NafisBelum ada peringkat
- Aortic Atresia With Normally Developed Left Ventricle in A Young AdultDokumen3 halamanAortic Atresia With Normally Developed Left Ventricle in A Young AdultUmmul HidayahBelum ada peringkat
- Heart EditDokumen51 halamanHeart EditCoral Srinivasa Ramalu100% (1)
- Basics of ECG (Dr. MD Kalimuddin)Dokumen53 halamanBasics of ECG (Dr. MD Kalimuddin)CloudySkyBelum ada peringkat
- Week 3 (CH 7 Dysrhythmias)Dokumen26 halamanWeek 3 (CH 7 Dysrhythmias)Sarah ChadnickBelum ada peringkat
- Pacemaker Related RHFDokumen4 halamanPacemaker Related RHFFaQihuddin AhmadBelum ada peringkat
- Aortic Stenosis AmendillaDokumen31 halamanAortic Stenosis AmendillaVadim BursacovschiBelum ada peringkat
- Patent Ductus Arteriosus Presenting in Old Age: Chi-Ling Hang, and Thompson SullebargerDokumen3 halamanPatent Ductus Arteriosus Presenting in Old Age: Chi-Ling Hang, and Thompson SullebargerQuindo Isaac Santana FontalvoBelum ada peringkat
- Jugular Venous Pressure: Congestive Heart FailureDokumen5 halamanJugular Venous Pressure: Congestive Heart FailureKrisSentosaBelum ada peringkat
- 1 Mitral Stenosis: InstructionDokumen8 halaman1 Mitral Stenosis: Instructionrashid.scribdBelum ada peringkat
- Top 100 ECG CasesDokumen212 halamanTop 100 ECG Casessoha.s.tumsa7Belum ada peringkat
- EKG Self Study GuideDokumen40 halamanEKG Self Study GuideArgee AlonsabeBelum ada peringkat
- Idiopathic Fascicular LV Tachycardia Case Report - Kadek Agus Putra - Edit 1Dokumen8 halamanIdiopathic Fascicular LV Tachycardia Case Report - Kadek Agus Putra - Edit 1putra udayanaBelum ada peringkat
- Pearls in CardiologyDokumen65 halamanPearls in CardiologyAmber MerrittBelum ada peringkat
- ECG - Dilated HypertrophiedDokumen19 halamanECG - Dilated Hypertrophiedyusuf fathoniBelum ada peringkat
- Straight Back Syndrome: Brit. Heart 614Dokumen6 halamanStraight Back Syndrome: Brit. Heart 614SaZa KarrarBelum ada peringkat
- Pi Is 0002934312004901Dokumen2 halamanPi Is 0002934312004901MuliaDharmaSaputraHutapeaBelum ada peringkat
- Acute Myocardial Infarction-Part II: ABC of Clinical ElectrocardiographyDokumen4 halamanAcute Myocardial Infarction-Part II: ABC of Clinical ElectrocardiographyAbdulkarim AlmansoorBelum ada peringkat
- Nikus2017 PDFDokumen11 halamanNikus2017 PDFAngie AlonsoBelum ada peringkat
- Case 3485Dokumen7 halamanCase 3485Hand SanitizerBelum ada peringkat
- CardioDokumen146 halamanCardiobbdddBelum ada peringkat
- Criss-Cross Heart With Double-Outlet Right VentricleDokumen4 halamanCriss-Cross Heart With Double-Outlet Right Ventriclejuana lopezBelum ada peringkat
- Pericardial Disease: Adel Hasanin Ahmed 1Dokumen5 halamanPericardial Disease: Adel Hasanin Ahmed 1Shaz ChindhyBelum ada peringkat
- AR Yang Komplikasi Menjadi Gagal Jantung PDFDokumen5 halamanAR Yang Komplikasi Menjadi Gagal Jantung PDFFitriani AlawiyahBelum ada peringkat
- Cardiac LipomDokumen4 halamanCardiac LipomCiprian MarianBelum ada peringkat
- Coronary Arteriovenous Fistula: ImageDokumen1 halamanCoronary Arteriovenous Fistula: Imagealex mihneaBelum ada peringkat
- 2016-Clin Nucl Med-Hu-4176787Dokumen3 halaman2016-Clin Nucl Med-Hu-4176787LH HuBelum ada peringkat
- Aranda 1998Dokumen5 halamanAranda 1998Sarly FebrianaBelum ada peringkat
- Article Heart-2001-Lindström-31-8Dokumen9 halamanArticle Heart-2001-Lindström-31-8dgina8800Belum ada peringkat
- Myocardial InfarctionDokumen5 halamanMyocardial InfarctionDaniel CiubatiiBelum ada peringkat
- Jugular Venous PressureDokumen5 halamanJugular Venous PressureYusran YusoffBelum ada peringkat
- Velocity of Blood Flow in Normal Human Venae CavaeDokumen11 halamanVelocity of Blood Flow in Normal Human Venae CavaeNguyen Huynh SonBelum ada peringkat
- Lapkas Pediatrik NLDokumen31 halamanLapkas Pediatrik NLHannaTashiaClaudiaBelum ada peringkat
- UMS Medical Short Cases Records 1st EditionDokumen36 halamanUMS Medical Short Cases Records 1st EditionHendraDarmawan67% (3)
- SMJ 59 279Dokumen5 halamanSMJ 59 279Faradiba MaricarBelum ada peringkat
- Pulmonary HypertensionDokumen63 halamanPulmonary HypertensionChrishan Shivanthan100% (4)
- Lead Avr PDFDokumen9 halamanLead Avr PDFsiddharthBelum ada peringkat
- ST Elevation in Lead aVR and Its Association With Clinical OutcomesDokumen4 halamanST Elevation in Lead aVR and Its Association With Clinical OutcomesshendyBelum ada peringkat
- Jugular Venous PressureDokumen9 halamanJugular Venous Pressuremoh86-Belum ada peringkat
- DR Abdulkareem Al Othman Valvular HDDokumen10 halamanDR Abdulkareem Al Othman Valvular HDDarawan MirzaBelum ada peringkat
- 1077 CMCNCHDokumen11 halaman1077 CMCNCHمحمد عقيليBelum ada peringkat
- Cardio 2Dokumen2 halamanCardio 2Erika De JesusBelum ada peringkat
- Cardiovascular ExaminationDokumen13 halamanCardiovascular ExaminationBitu JaaBelum ada peringkat
- Science Olympiad Anatomy & Physiology 2014Dokumen2 halamanScience Olympiad Anatomy & Physiology 2014Alicia Hyland82% (11)
- Nureal Control and CoordinationDokumen16 halamanNureal Control and CoordinationthushyanthBelum ada peringkat
- 2012 Digestive System in ManDokumen52 halaman2012 Digestive System in ManhueymeyBelum ada peringkat
- QTR 2 Module 1 From Cell To OrganismDokumen8 halamanQTR 2 Module 1 From Cell To OrganismNick Bantolo91% (11)
- Acute Heart Failure For Nurse FinalDokumen21 halamanAcute Heart Failure For Nurse FinalAnonymous AZNHObw8Belum ada peringkat
- EndocrineDokumen6 halamanEndocrineShreyasi PatankarBelum ada peringkat
- Cardiac Arrhythmia From Guyton's BookDokumen10 halamanCardiac Arrhythmia From Guyton's BookNadhirah Mohamad NohBelum ada peringkat
- 11 Lung PathologyDokumen7 halaman11 Lung PathologycarlgangcaBelum ada peringkat
- Echo 20190914164646458Dokumen2 halamanEcho 20190914164646458Gigi DajoyagBelum ada peringkat
- Case StudyDokumen4 halamanCase Studyllyryc100% (1)
- Saliva - A Diagnostic ToolDokumen30 halamanSaliva - A Diagnostic ToolPrathusha UmakhanthBelum ada peringkat
- A Nursing Student Cast Study (Revised) A Case Study of Erratic ParasitismDokumen19 halamanA Nursing Student Cast Study (Revised) A Case Study of Erratic ParasitismDenie BoyonasBelum ada peringkat
- Human Reproduction - Part 1Dokumen22 halamanHuman Reproduction - Part 1NickOoPandeyBelum ada peringkat
- Anatomy and PhysiologyDokumen3 halamanAnatomy and PhysiologyJade AltarejosBelum ada peringkat
- C40 - RATNA UMI AZIZAH - G41172240 - Prak 2Dokumen3 halamanC40 - RATNA UMI AZIZAH - G41172240 - Prak 2Ratna Umi AzizahBelum ada peringkat
- 35 AnswersDokumen7 halaman35 AnswersJasmine Nicole EnriquezBelum ada peringkat
- Learners Material Module 1 Respiratory ADokumen27 halamanLearners Material Module 1 Respiratory AJelly FloresBelum ada peringkat
- EndocrineDokumen70 halamanEndocrinehamidBelum ada peringkat
- MRCP High YieldDokumen6 halamanMRCP High Yieldchia2011Belum ada peringkat
- Hypothyroidism - StatPearls - NCBI BookshelfDokumen10 halamanHypothyroidism - StatPearls - NCBI BookshelfKarla CordobaBelum ada peringkat
- 10 EncephalopathyDokumen18 halaman10 EncephalopathyAbdullah ShiddiqBelum ada peringkat
- Screening of Breast CancerDokumen19 halamanScreening of Breast CancerIncredible DivineBelum ada peringkat
- Graves' Disease: Bella I. Putri 16-025Dokumen29 halamanGraves' Disease: Bella I. Putri 16-025anon_414347743Belum ada peringkat
- The Immune System 2013Dokumen31 halamanThe Immune System 2013api-202513022Belum ada peringkat
- CHAP 10 FORM 4 BiologyDokumen8 halamanCHAP 10 FORM 4 BiologyCrescentiaBelum ada peringkat
- Glomerular Disease: Acute Nephritic Syndrome Nephrotic Syndrome Chronic GlomerulonephritisDokumen18 halamanGlomerular Disease: Acute Nephritic Syndrome Nephrotic Syndrome Chronic GlomerulonephritisironBelum ada peringkat
- Cognitive NeuroscienceDokumen42 halamanCognitive NeuroscienceDiya Saher100% (1)
- Management of Thyroid DisordersDokumen53 halamanManagement of Thyroid DisordersAnityo S AthmadjaBelum ada peringkat
- Biology Worksheet On Excretory SystemDokumen5 halamanBiology Worksheet On Excretory SystemDhruv Nair IX ABelum ada peringkat
- Session #41 SAS - AnaPhy (Lab) (Agdana, Nicole Ken)Dokumen5 halamanSession #41 SAS - AnaPhy (Lab) (Agdana, Nicole Ken)Nicole Ken AgdanaBelum ada peringkat