Güder & Rutten FH Ea - (Epub) Chronic Obstructive Pulmonary ... Diagnosis and Treatment European Journal of Heart Failure 27 Oktober 2014
Diunggah oleh
Naela RizqiJudul Asli
Hak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Güder & Rutten FH Ea - (Epub) Chronic Obstructive Pulmonary ... Diagnosis and Treatment European Journal of Heart Failure 27 Oktober 2014
Diunggah oleh
Naela RizqiHak Cipta:
Format Tersedia
REVIEW
European Journal of Heart Failure (2014)
doi:10.1002/ejhf.183
Chronic obstructive pulmonary disease
in heart failure: accurate diagnosis
and treatment
Glmisal Gder1,2,3, Susanne Brenner2,3, Stefan Strk2,3,
Arno Hoes1, and Frans H. Rutten1*
1 Julius
Center for Health Sciences and Primary Care, University Medical Center Utrecht, Utrecht, The Netherlands; 2 Comprehensive Heart Failure Center, University of
Wrzburg, Wrzburg, Germany; and 3 Department of Internal MedicineCardiology, University Hospital Wrzburg, Germany
Received 4 July 2014; revised 8 September 2014; accepted 12 September 2014
Coincidence of COPD and heart failure (HF) is challenging as both diseases interact on multiple levels with each other, and thus impact
significantly on diagnosis, disease severity classification, and choice of medical therapy. The current overview aims to educate caregivers
involved in the daily management of patients with HF and (possibly) concurrent COPD in how to deal with clinically relevant issues such as
interpreting spirometry, the potential role of extensive pulmonary function testing, and finally, the potential beneficial, but also detrimental
effects of medication used for HF and COPD on either disease.
..........................................................................................................
Heart failure
COPD misdiagnosis
Severity classification
Introduction
A 60 year old man (110 kg, 170 cm) consults his general practitioner (GP) because of progressive dyspnoea on minimal exertion.
The patient is an active smoker (40 pack-years) with a history
of diabetes type 2, obesity, hyperlipidaemia, and hypertension. He
reported a weight gain of 4 kg within the last 3 days. At clinical
examination the GP detects increased jugular venous pressure, pulmonary expiratory wheezing, a broadened and sustained apex beat
in the lateral decubitus position, ankle oedema, and a high systolic
blood pressure of 180 mmHg. The forced expiratory volume in
1 s/forced vital capacity ratio (FEV1 /FVC) measured by a hand-held
spirometer is 0.60 post-bronchodilator and thus would be compatible with pulmonary obstruction as seen in COPD. The reversibility
of the FEV1 value, 15 min after salbutamol inhalation, lies in the grey
zone, i.e. 9%.
This scenario describes a common dilemma in everyday clinical
practice. Does this patient have COPD, heart failure (HF), or both?
In order to arrive at an accurate diagnosis, the recent guidelines
on HF and COPD both emphasize not to rely on the assessment
...........................................................
Keywords
of clinical symptoms only, but recommend additional investigations
aiming to detect structural or functional cardiac or pulmonary
abnormalities.1,2 In many previously published studies, a patient
recall of suffering from COPD was deemed sufficient for the diagnosis of COPD.3 However, even with spirometry, a misdiagnosis
and over-rating of COPD severity is likely in patients with HF,
because HF on its own may mimic an obstructive pattern compatible with COPD.4 More importantly, current guidelines advocate
the same COPD/HF therapy in patients with co-morbid COPD and
HF without acknowledging the lack of accurate evidence on bronchodilator therapy in patients with severe HF.1,2 Specific information on defining COPD and COPD severity grading in the presence
of HF is also not given.1,2
The current review takes a pragmatic approach in that it aims to
educate doctors and nurses involved in the daily management of
patients with HF and/or COPD in how to deal with some clinically
relevant issues that have not been addressed in depth by previous
reviews. This includes a detailed discussion on the diagnostic
approach of how to establish and grade COPD in patients with
HF, and the potential beneficial but also detrimental effects of
*Corresponding author. Julius Center for Health Sciences and Primary Care, University Medical Center Utrecht, PO Box 85060, Stratenum 6.131, 3508 AB Utrecht, The
Netherlands. Tel: +31 88 7568193, Fax: +31 88 7569028, E-mail: F.H.Rutten@umcutrecht.nl
2014 The Authors
European Journal of Heart Failure 2014 European Society of Cardiology
The definition of chronic
obstructive pulmonary disease
Chronic obstructive pulmonary disease is defined as persistent
airflow limitation that is progressive over time and, if diagnosed by
the GOLD criteria (global strategy for the diagnosis, management,
and prevention of chronic obstructive pulmonary disease), requires
a post-bronchodilator ratio of the forced expiratory volume in
1 s (FEV1 ) to the forced vital capacity (FVC) <0.7.1 This criterion
is adequate in clear-cut cases with severe obstruction, but may
be problematic in borderline cases, when the strictly defined
ratio reaches its limits of diagnostic certainty.5 Application of
the strict ratio in older persons has been repeatedly criticized
for not acknowledging the age-associated physiological decline
of the FEV1 /FVC ratio, thus risking overdiagnosis of COPD in
this population.6 Alternatively, an age- and sex-adjusted approach
was proposed employing the lower limit of normal (LLN) of the
FEV1 /FVC ratio, but the superiority of the LLN over the GOLD
definition has not generally been accepted.5 Diagnosing COPD
using the LLN threshold also has considerable shortcomings. There
are several equations (and thresholds) available. resulting in a lack
of consistency,7 and the LLN approach has poor accuracy in the
early stages of COPD.
A validated consensus diagnosis of an expert panel of pulmonologists using all diagnostic information, including extensive pulmonary function testing, physical examination, patients medical
history, and smoking status, may be viewed as the current reference standard for the diagnosis of COPD in the research setting.8
Adequate reporting of the procedure of the panel, however, is
required.9
When compared with an expert panel of pulmonologists who
used the comprehensive information from spirometry, but also
from body box and diffusion measurements, LLN was inferior to
the GOLD definition.10 Compared with such an expert panel, a
diagnosis based on the GOLD definition was more sensitive but
less specific, and better predicted future exacerbations than the
LLN approach in clinically stable elderly patients aged 65 years or
over and suspected of COPD.10 Thus, both a fixed FEV1 /FVC ratio
and the LLN approach appear to be insufficient as a single criterion
for the diagnosis of COPD, especially in early COPD. Although
the GOLD guidelines acknowledge these limitations of the current
definition, they still adhere to the fixed ratio for its simplicity and
applicability to a broader, worldwide range of caregivers.1
In conclusion: especially in borderline cases, the commonly
used fixed ratio of FEV1 /FVC as measured with spirometry, and the
LLN approach both bear the risk of over- and underdiagnosing true
COPD, respectively. A gold standard for diagnosing COPD is lacking, but may be best approached by a validated consensus diagnosis
of an expert panel of pulmonologists in the research setting.8 For
routine clinical practice, consultation of a pulmonologist in unclear
cases or repeated pulmonary function testing would be both a pragmatic and an adequate approach.
........................................................................................................................................................................
medication used for HF and COPD on either condition, in both
the acute and non-acute setting.
G. Gder et al.
Concurrence of heart failure
and chronic obstructive
pulmonary disease
Chronic obstructive pulmonary disease and HF are common
diseases of the elderly,11 although COPD develops on average
10 years earlier than HF (>55 vs. >65 years).1,2 Both conditions
can be consideredat least partlyas premature organ ageing,
with profound systemic effects and a chronic progressive course
impacting heavily on exercise tolerance and health-related quality
of life. Both conditions share non-specific, but very common symptoms such as breathlessness and fatigue, and cigarette smoking as
a major risk factor. It is estimated that >90% of cases with COPD
in the Western world are due to cigarette smoking.12 Interestingly,
in patients with HF, the proportion of patients with COPD had
a smoking history less often than would be expected. Some of
these studies reported prevalence rates of never-smokers as high
as 2050%, 4,13,14 which may raise the suspicion of overdiagnosis
of COPD in patients with HF (Table 1).
In recent years, systemic inflammation has increasingly been
recognized as another important common pathway for both
conditions.15 Systemic inflammation expressed by increased
levels of cytokines, such as tumour-necrosis factor (TNF)-,
interleukin-1 (IL-1), and IL-6, might accelerate and perpetuate
disease progression and exacerbation of both diseases.16 Hence,
systemic low-grade inflammation is regarded more and more
as a critical link between pulmonary disease and cardiovascular
conditions.15 The significance of each disease to the development
of the other is, however, still unanswered.16 Also other inflammatory conditions such as rheumatoid arthritis and inflammatory
bowel diseases are associated with COPD,17,18 but the associations
are much weaker than in HF (prevalence rates 48% vs. 25%,
respectively).17 19
Moreover, although in 60% of patients with heart failure with
reduced ejection fraction (HFrEF) an ischaemic cause can be
detected in coronary angiography2 and both CAD and COPD
share the same risk factors as smoking and low-grade inflammation,
the prevalence of CAD or a history of myocardial infarction
was similar between HF patients with and without COPD,4,14,20
indicating that an additional risk factor may influence the high
co-incidence of COPD and HF.
In conclusion: smoking and low-grade systemic inflammation
seem the most important common risk factors for the concurrence
of COPD and HF but do not entirely explain the high co-incidence
of both conditions.
Prevalence of chronic obstructive
pulmonary disease in patients
with heart failure
Published estimates on the prevalence of COPD in patients with
HFrEF varied considerably among studies, ranging from 8% to 52%.
Differences in these rates may be due to numerous factors such as
geographical region, age and sex distribution, urban environment,
2014 The Authors
European Journal of Heart Failure 2014 European Society of Cardiology
Accurate diagnosis and treatment of COPD in HF
Table 1 Prevalence of concurrent chronic obstructive pulmonary disease as spirometrically defined by a
post-bronchodilator forced expiratory volume in 1 s/forced vital capacity ratio <70% assessed in patients with heart
failure.
Beta-blocker
use, % (differences
in patients
with or without
COPD)
...........................................................................................................................................
First author,
year,
reference no.
HF
phenotype
Time point
of measurements
Iversen, 200814
532
Mixed
13 days after
hospitalization for
acute HF
Mascarenhas, 200822
223
309
186
HFpEF, (LVEF 45%)
HFrEF, (LVEF <45%)
HFrEF (LVEF <45%)
Apostolovic, 201113
Macchia, 201120
Boschetto, 201224
Stable HF, outpatients
department
174
HFrEF (LVEF<45%)
Stable HF, outpatients
department
201
HFrEF (LVEF 40%)
Stable, outpatients
department
118 Mixed (mean LVEF 40%) Stable HF, outpatients
department
Steinacher, 201226
89
Mixed (3% HFpEF)
Brenner, 20134
272
HFrEF (LVEF <40%)
619
HFrEF (LVEF <40%)
Begh, 201325
124
HFeEF
Minasian, 201323
187
HFrEF (LVEF <40%)
Minasian, 201321
116
HFrEF (LVEF <40%)
Stable, outpatients
department
35 days after
hospitalization for
acute HF
Stable, outpatients
department
Stable, outpatients
department
Stable, outpatients
department
Stable, outpatients
department
Prevalence Prevalence of
of COPDa never-smokers
in patients
with COPD
35%b
41%b
31%b
39%
27.6%
37%
30%
44%
20%
29% (no)
No specification, 49% in
the total cohort
54%
87% (no)
No specification for
GOLD-COPD
0%, >10 pack-years of
smoking was an
inclusion criterion
No specification for
GOLD-COPD
Not mentioned
19%
100% no)
83% (no)
98% (no)
92% (no)
28%
91% (no)
83% (no)
32
0%, >10 pack-years of
smoking was an
inclusion criterion
5%
34
6%
34%
92% (no information
on differences)
91% (no information
on differences)
and smoking prevalence of the study population, but importantly
also depend on the diagnostic criteria and definition of COPD
applied, and whether patients underwent spirometry while in
a euvolaemic and stable condition of HF.19 Surprisingly, only a
few studies included spirometry to determine the presence of
COPD (Table 1).4,13,14,20 26 Most studies relied rather on medical
recordings or patients self-report to diagnose COPD.19 Reliable
estimates of the prevalence of COPD in a representative sample
of HF patients in a stable situation with preserved ejection fraction
(HFpEF) are still lacking.27
There are major concerns about interpreting pulmonary function testing in patients with HF when based solely on the FEV1 /FVC
ratio. HF may induce restrictive pulmonary changes (proportional
reduction in lung volumes) due to enlargement of the heart,
.........................................
FEV1 , forced expiratory volume in 1 s; FVC, forced vital capacity; HF, heart failure; HFpEF heart failure with preserved ejection fraction; HFrEF, heart failure with reduced
ejection fraction.
a COPD prevalence in patients with HF according to the GOLD definition (post-bronchdilator FEV /FVC ratio <0.7).
1
b Exclusion of GOLD stage I patients (FEV >80% of predicted).
1
2014 The Authors
European Journal of Heart Failure 2014 European Society of Cardiology
pulmonary congestion, or pleural effusion, andin long-standing
HF with repetitive decompensationsfibrotic alterations of the
pulmonary interstitium.28 Obesity is another frequent cause of
such externally induced pulmonary restriction.29 In stable HFrEF,
both FEV1 and FVC are reduced on average by 20% compared
with age-, sex-, and height-matched controls from the general
population, thus, fortunately, not affecting the FEV1 /FVC ratio.30
Occasionally, however, HF may reduce the FEV1 /FVC ratio by causing a larger reduction in FEV1 than in FVC, and thus produce an
obstructive ventilatory pattern in spirometry.5 Importantly, pulmonologists often only consider intrabroncheolar obstruction as
a cause for reduction in FEV1 /FVC, while extrabroncheolar (fluid)
and attenuated thoracic muscle function (both of which often occur
in HF patients) can cause such a reduction as well.31,32 In a study
Alternatives to diagnose chronic
obstructive pulmonary disease
in heart failure
Body plethysmography results can improve the diagnostic accuracy
of detecting COPD. Determining the ratio of residual volume
and total lung capacity (RV/TLC) is worthwhile,4 because COPD
is very often accompanied by air-trapping and hyperinflation.36
Hyperinflation (high RV/TLC ratio) is a valid indicator of true
COPD, especially in patients with decompensated HF.4 Hence,
before considering long-term bronchodilator therapy in patients
with HF and suspected COPD, comprehensive pulmonary function
testing should be considered.
In conclusion: hyperinflation (high RV/TLC ratio) is a valid
indicator of true COPD in patients with HF, even when performed
when patients were recently decompensated.
........................................................................................................................................................................
conducted in patients with stable HFrEF, i.v. infusion of 1 L of
saline over 30 min resulted in a decreased FEV1 and FEV1 /VC ratio,
without a substantial change in VC, while the same procedure in
healthy subjects did not result in substantial changes in any of these
three measurements.33 Saline infusion results in fluid extravasation
in the lungs in HF patients, but not in healthy subjects. Therefore,
especially in acutely decompensated HF patients, and in HF patients
with chronic pulmonary fluid overload, congestion of the lung may
provoke mechanical obstruction of the bronchi by increased interstitial fluid pressure. This results in a reduction of both FEV1 and
FVC, but to a larger extent of FEV1 , with a reduction of the
FEV1 /FVC ratio as a result.28,31,32,34,35 After re-compensation of HF,
airway conduction may improve or even normalize.4,34,35 Thus, in
unstable HF patients with pulmonary congestion, the FEV1 /FVC
ratio may comply with the GOLD criteria for COPD (FEV1 /FVC
<0.7) in the absence of true COPD, with, as a result, false-positive
COPD diagnosis.35
A study assessing patients hospitalized for symptomatic HF 13
days after admission found a prevalence of COPD based on the
GOLD criteria (FEV1 /FVC <0.7) of 31% in patients with HFrEF,
and of 41% in patients with HFpEF.14 Another study investigating
patients with established HFrEF by repeat pulmonary function
testing showed that the prevalence of COPD in the cohort
changed over time, with a prevalence rate of 19% at 35 days
after admission for acute decompensation, and only a rate of
9% at 6 months after discharge, when the majority of patients
were in a stable phase and considered euvolaemic.4 These studies
clearly illustrate that COPD may be overdiagnosed in patients with
HF when based on spirometry performed when HF patients are
(recently) decompensated or not euvolaemic.
In conclusion: overdiagnosis of COPD in HF is very likely when
spirometry is performed when HF patients are unstable. Based
on studies performed in stable HF, the prevalence of COPD
defined according to a post-dilatory value of FEV1 /FVC <70%
varies between 9% and 44% (Table 1), depending on population
characteristics, the timing of pulmonary function testing, and the
method or definition applied to diagnose COPD.
G. Gder et al.
Table 2 Grading of severity of airflow limitation in
chronic obstructive pulmonary diseas based on
post-bronchodilator forced expiratory volume in 1 s as
a percentage of predicted values
Stage
Severity
Post-bronchodilator
FEV1 % of predicted level
................................................................
GOLD 1
GOLD 2
GOLD 3
GOLD 4
Mild
Moderate
Severe
Very severe
80%
50 to <80%
30 to <50%
<30 %
Adapted from Vestbo et al.1
Severity grading of COPD according to the GOLD guidelines (postbronchodilator FEV1 /FVC ratio <0.7).
FEV1 , forced expiratory volume in 1 s; FVC, forced vital capacity.
Severity grading of chronic
obstructive pulmonary disease
in the presence of heart failure
Until recently, severity of COPD was graded on the reduction of
FEV1 . This approach results in overestimation of COPD severity in
patients with HFrEF, because HF itself causes a 20% reduction in
FEV1 (Table 2).30 Because FEV1 poorly correlates with symptoms
and the risk of exacerbations in COPD, the international guidelines
on COPD introduced a new severity classification system, incorporating symptom load and history of exacerbations in combination
with FEV1 reduction.1 Patients with COPD can thus be classified
into four groups (AD) and treated according to severity grade
as specified in Figure 1. Breathlessness may be assessed with the
Modified British Medical Research Council (mMRC) questionnaire
or the COPD Assessment Test (CAT).1
These questionnaires cannot discriminate between cardiac- and
pulmonary-induced breathlessness and physical limitations. Moreover, exacerbations of COPD might be confused with or triggered
by episodes of cardiac decompensation. Thus, the new severity
classification system for COPD can also be expected to mediate
over-rating the severity of COPD and consequently overtreatment
with inhaled pulmonary drugs when patients have not only COPD,
but also HF.
In conclusion: because HF itself reduces FEV1 and causes dyspnoea and functional limitations, overestimation of the severity of
COPD is likely in those with concomitant HF and COPD.
Cardiac asthma: the alternative
diagnosis
The term asthma cardiale was first mentioned in the literature
>180 years ago and was thought to distinguish bronchial asthma
from the clinical picture seen in acutely decompensated HF.37 The
main trigger of expiratory obstruction with the clinical sign of
wheezing in asthma is an allergen, while in acutely decompensated
HF abrupt pulmonary congestion with increased interstitial fluid
2014 The Authors
European Journal of Heart Failure 2014 European Society of Cardiology
Accurate diagnosis and treatment of COPD in HF
D
D
Alternative choices:
Long-acting anticholinergic + long-acting beta2-agonist
Long-acting anticholinergic + phosphodiesterase-4 inhibitor
Long-acting beta-2 agonist + phosphodiesterase-4 inhibitor
Inhaled corticosteroid + long-acting anticholinergic +
long-acting beta2-agonist
Inhaled corticosteroid + long-acting anticholinergic +
phosphodiesterase-4 inhibitor
Long-acting anticholinergic + long-acting beta2-agonist
Long-acting anticholinergic + phosphodiesterase-4 inhibitor
Short-acting anticholinergic
OR
Short-acting beta2-agonist
Recommended first-line therapies:
A
A
Long-acting anticholinergic
OR
Long-acting beta2-agonist
Alternative choices:
Alternative choice:
Long-acting anticholinergic
Long-acting beta2-agonist
Short-acting anticholinergic + short-acting beta2-agonist
Long-acting anticholinergic + long-acting beta2-agonist
mMRC < 2
CAT < 10
2/year
Inhaled corticosteroid + long-acting beta2-agonist
+ / OR
Long-acting anticholinergic
Alternative choices:
Recommended first-line therapies:
FEV1 50%
Recommended first-line therapies:
C
C
B
B
Exacerbation frequency
Inhaled corticosteroid + long-acting beta2-agonist
OR
OR
Long-acting anticholinergic
< 2/year
Spirometry
FEV1 < 50%
Recommended first-line therapies:
mMRC 2
CAT 10
Symptoms and quality of life
Figure 1 Proposed grading scheme: patients are allocated to groups AD according to the forced expiratory volume in 1 s (FEV1 ) % of
pressure causes external, mechanical obstruction and reactive
spasms of the bronchi.38 Wheezing is technically produced by
narrowing or obstruction of the bronchi. A study that defined
cardiac asthma as the presence of wheezing at initial presentation
found a prevalence of 35% in patients with acute HF.39 Interestingly,
this prevalence is comparable with the overestimated prevalence
of COPD found in most of the studies conducted in HF based on
spirometry when patients were unstable (Table 1).
In conclusion: cardiac asthma is a clinical picture based on
externally induced pulmonary obstruction of cardiac origin, and
wheezing may be present in one-third of patients with acutely
decompensated HF.
The use of beta-blockers may
result in over-diagnosing chronic
obstructive pulmonary disease
Only a few studies have assessed the effect of beta-blockers on
spirometry in patients with HF,40 44 and in even fewer patients
with HF and coincident COPD (Table 3).45 47
..............................................................
predicted level, the number of COPD exacerbations within the last 12 months, and symptoms. Symptoms are assessed using either the
Modified Medical Research Council Dyspnea Scale (mMRC) or the COPD Assessment Test (CAT). The mMRC contains five categories that
describe incremental symptom severity (0 = breathlessness only at strenuous exercise, 1 = dyspnoea when hurrying on level ground or
walking up a slight hill, 2 = walking more slowly than people of the same age because of dyspnoea on level ground, 3 = dyspnoea after walking
100 yards or after a few minutes on level ground. 4 = dyspnoea when dressing). The CAT assesses eight questions on typical symptoms of
daily life with COPD. Each question is rated from 0 to 5 points according to severity of symptoms. Questions refer to coughing frequency,
phlegm production, angina pectoris, dyspnoea uphill, limitations at daily activities, functionally fixed to domestic environment due to dypsnoea,
sleep disturbances, and physical energy. Adapted from Vestbo et al.1
2014 The Authors
European Journal of Heart Failure 2014 European Society of Cardiology
In fact, the effects of beta-blocker intake on spirometry results
vary considerably, according to the beta-blocker type used (cardioselective vs. non-selective), duration of beta-blocker treatment,
dose applied, and underlying diseases.48 50 Still, it appears that
beta-blockers primarily reduce FEV1 but not FVC. Agostoni et al.
were the first who addressed this question in a randomized
controlled trial (RCT) and showed in a crossover design of 15
patients with HF without COPD that carvedilol, a non-selective
beta-blocker, did not change FEV1 or VC when compared with
placebo. Data were reported without information about whether
bronchodilators were administered.40 Later the same study group
showed that carvedilol inhibited the post-bronchodilator increase
of FEV1 with salbutamol but not the increase of FVC when compared with bisoprolol, 2 months after beta-blocker initiation in 53
patients with HF.42 Intake of beta-blockers also reduced FEV1 significantly in 35 patients with HF, but without substantial effects
on FVC within 12 months of follow-up.41 The largest cohort that
addressed this question was derived from the CIBIS elderly RCT.
In this study, bisoprolol use was associated with significantly higher
levels of FEV1 (50 mL) than carvedilol after 12 weeks of treatment.
G. Gder et al.
Table 3 Effects of beta-blockers on resting spirometry in patients with heart failure only, and in patients with heart
failure and chronic obstructive pulmonary disease
Study design, n,
HF
Studied
Effects on
First author,
study duration
phenotype
beta-blocker
spirometry
year,
refence no.
...........................................................................................................................................
HF
Agostoni, 200240 RCT double blind, crossover HFrEF <40%, COPD
Carvedilol vs. placebo
Difference between carvedilol and
study, n = 15, 4 months
excluded
placebo: no effects on FEV1 , VC,
DLCO
beta-blocker use
Cohort study, n = 35 with
HFrEF <40%, COPD
Carvedilol (n =11),
Difference between baseline and
Witte, 200541
PFT on 12 months
excluded
bisoprolol (n = 24)
follow-up (n = 35): FEV1 , 84%
(19)% to 79 (21)% (P <0.01); FVC.
follow-up
no effects. No difference between
both beta-blockers
Agostoni, 200742 RCT, double blind crossover HF with NYHA II or LVEF Carvedilol vs. isoprolol
Difference between carvedilol and
study, n = 53, 2 months
<45%; severe COPD
bisoprolol: FEV1 (L): 2.71 vs.
2.83 L (P = 0.03); VC, no effects.
excluded
Analyses refer to
post-bronchodilator values
Difference between carvedilol and
Dungen, 201143 RCT, open label, n = 714 with HF with NYHA II or LVEF Carvedilol (n = 365) vs.
PFT, 12 weeks
<45%
bisoprolol (n = 349)
bisoprolol: FEV1 . +50 mL
(P = 0.03) for bisoprolol; FVC, not
reported
HF + COPD
HFrEF <40% and COPD
Bisoprolol (n = 14) vs
Difference between bisoprolol and
Hawkins, 200945 RCT, placebo controlled,
n = 27, 4 months
GOLD 2, 3
placebo (n = 13)
placebo: FEV1 , 70 vs. 120 mL
(P<0.05); FEV1
post-salbutamol, 90 vs. 20 mL
(P<0.05). No change on VC, RV,
TLC, PEF
Jabbour, 201146 RCT, open label, triple
HF (mean LVEF 37%), COPD Carvedilol, bisoprolol and
Difference for FVC: no effects in all
crossover study, n = 51,
GOLD 2, 3, 16 HF only 35
metoprolol succinate
subgroups. Difference between
each 6 weeks
CHF + COPD
bisoprolol vs. carvedilol, CHF,
FEV1 , +120 ml for bisoprolol
(P = 0.02); CHF + COPD, FEV1 ,
+150 mL for bisoprolol (P = 0.01)
Difference between metoprolol
vs. carvedilol: total group, FEV1 , +
80 mL for metoprolol (P = 0.04)
Bisoprolol vs. metoprolol: no
difference
Carvedilol (n = 31) vs.
Change in FEV1 between baseline
Lainscak, 201147 RCT, open label, n = 63, 46 HFrEF (LVEF <40%) and
weeks after up-titration
COPD GOLD 2
bisoprolol (n = 32)
and follow-up: bisoprolol, 1561 to
1698 mL (P = 0.046); carvedilol,
1704 to 1734 mL (P = 0.44). No
between-group difference for
FEV1 FVC: no effects
In patients with HF and COPD, beta-blocker-induced reduction of FEV1 might be even stronger. In an RCT conducted
by Hawkins et al., FEV1 was reduced between baseline and 4
months of follow-up with bisoprolol (70 mL) but not with placebo
(+120 mL).45 Another RCT that compared carvedilol with bisoprolol could show an increase of FEV1 by 137 mL for bisoprolol after
................
All studies were performed in patients with HF when in a stable phase of their disease.
CHF, congestive heart failure; DLCO, diffusing capacity of the lung for carbon monoxide; FEV1 , forced expiratory volume in 1 s; FVC, forced vital capacity; HF, heart failure;
HFrEF, heart failure with reduced ejection fraction; PEF, peak expiratory flow; PFT, pulmonary function test; RCT, randomized controlled trial; TLC, total lung capacity; VC,
vital capscity.
6 weeks of treatment but no change for carvedilol.47 In a triple
crossover RCT, the non-selective beta-blocker carvedilol reduced
FEV1 by 150 mL when compared with bisoprolol in patients with
HF and COPD and by 80 mL when compared with metoprolol. No
significant difference was seen between patients on bisoprolol vs.
2014 The Authors
European Journal of Heart Failure 2014 European Society of Cardiology
metoprolol succinate.46 Of note, in all of the mentioned studies,
there was no effect on (F)VC (Table 3).
Thus, use of beta-blockers could result in a reduction of the
FEV1 /FVC ratio and subsequently in overdiagnosing of COPD.42
Importantly, however, beta-blockers were well tolerated in these
studies (>90% continuation within 1 year of follow-up41 ).
Multiple observational studies in patient with COPD suggest that
(cardioselective) beta-blockers reduce the risk of all-cause death
and exacerbations, even in the subpopulation without overt cardiac
disease.51 Most importantly, guidelines on HF and COPD both
recommend cardioselective beta-blockers in patients with HFrEF
with or without co-morbid COPD.1,2
In conclusion: beta-blockers might induce bronchoconstriction,
i.e. reduce FEV1 somewhat without an effect on FVC and thus
facilitate overdiagnosis of COPD when a FEV1 /FVC cut-off-based
definition is applied. Irrespective of this fact, beta-blockers are
well tolerated by COPD patients and beta1-selective beta-blockers
are recommended in any patient with HFrEF with or without
concurrent COPD.
Reversibility testing in patients
with heart failure
An increase of >12% or >200 mL in the baseline FEV1 after
inhalation of a bronchodilator (usually a beta-2-agonist) is an
accepted positive bronchodilator response indicating reversibility
of obstruction.52 A recent study conducted in 116 patients with
stable chronic HFrEF and no history of asthma or COPD detected
a pre-bronchodilator airway obstruction in 55%.21 After administration of bronchodilators (400 g of salbutamol and 80 g of ipratropium), FEV1 and the FEV1 /FVC ratio, but not the FVC, increased
slightly but significantly: pre- vs. post-bronchodilator FEV1 /FVC
0.68 0.8 vs. 0.71 0.8, P<0.001. In 22%, post-bronchodilator
FEV1 /FVC values increased to >0.7, thus reducing the percentage of patients with obstruction to 33%.21 Patients with HFrEF
and clinical signs of pulmonary congestion (n = 16) more often had
a FEV1 /FVC <0.7 after bronchodilation than the remaining 100
HF patients without such signs (56% vs. 30%, P = 0.04).21 Moreover, 9 out of 39 patients with persisting pulmonary obstruction
after administration of bronchodilators and therefore spirometrically confirmed COPD, had a positive reversibility testing due
to an increase of FEV1 >200 mL and >12% of baseline values. It is
unclear whether these patients had a true asthmatic component
or whether the reversibility in any way was related to HF. Interestingly, all 116 HF patients experienced amelioration of shortness of
breath shortly after the administration of salbutamol.21
In conclusion: a reversible obstructive pattern in spirometry is
common in stable HFrEF, and a short-acting beta2-agonist applied
during spirometry resulted in immediate symptom relief.
Bronchodilators in heart failure:
beneficial or detrimental?
Beta-2-agonists may increase heart rate,53 worsen cardiac
function, and might decrease potassium levels, thus facilitating
........................................................................................................................................................................
Accurate diagnosis and treatment of COPD in HF
2014 The Authors
European Journal of Heart Failure 2014 European Society of Cardiology
hypokalaemia-induced arrhythmias and tachycardias, as well as
sudden cardiac death.53 56
Theoretically, however, short-term use of beta-2-agonists may
also exert positive effects in acutely decompensated HF, and
in subjects presenting with wheezing, since they may reduce
pulmonary congestion by increasing transepithelial sodium and
chloride transport, as shown in animal models.53,57,58 In addition,
small sized studies showed that short-term use of beta-2-agonists
increases FEV1 ,59 improves peripheral oxygen delivery,53 increases
cardiac index, and decreases systemic vascular resistance, even
in stable patients with HFrEF.53 So in acutely decompensated HF,
short-acting bronchodilators may result in immediate symptom
relief, and bridge the time gap until i.v. diuretics and nitrates start
working. On the other hand, the described adverse effects of
beta-2 agonists may limit even the short-term use in both acutely
decompensated and stable HF.
The ongoing Study to Understand Mortality and Morbidity in
COPD (SUMMIT) is a four-armed study investigating the effect
of a beta-2 agonist (vilanterol) and an inhalative corticosteroid
(fluticasone furoate) as monotherapy and combined vs. placebo
specifically in COPD patients who have established cardiovascular diseases (CAD, peripheral arterial disease, previous stroke or
myocardial infarction, or diabetes mellitus with target organ disease), or if older than 60 years have treatment for two of the
following cardiovascular risk factors: hypertension, diabetes mellitus, hypercholesterolaemia, or treatment for peripheral arterial
disease.60 Importantly, even in the controlled setting of this trial,
patients with severe HF (NYHA IV), and those with an LVEF <30%,
or an implantable cardioverter defibrillator (ICD), were excluded.
The primary bronchodilator therapy48 recommended in patients
with co-morbid HF and COPD is a long-acting anticholinergic
(e.g. tiotropium bromide), as its cardiovascular risk seems to be
more favourable than the risk of long-acting beta-2-agonists.61
However, because patients with underlying cardiac disease are
largely under-represented in RCTs in COPD patients, it is unclear
whether long-acting anticholinergics may be safely used in those
with cardiac disease, including HF. Several large observational
studies with long follow-up periods indicated that long-acting
anticholinergics may be associated with the same cardiovascular
event risk as long-acting beta-2-agonists in patients with cardiac
disease.62,63 The question remains of whether we should prioritize
either a long-acting anticholinergic or a long-acting beta-2-agonist
in patients with HF and true COPD. Although not formally
evidence-based, it may be assumed that in addition to the mentioned side effects, beta-agonists may exert beta-blocker-opposing
effects on cardiac remodelling in the long term. Thus, on a theoretical basis, maybe long-acting anticholinergics should be preferred
over long-acting beta-agonists, but both pulmonary drug classes
should be used under close follow-up.
In conclusion: bronchodilators may improve symptoms in HF
in the short term, even in the absence of COPD, but negative cardiovascular side effects may prevail during long- or even
short-term therapy. When patients need bronchodilation for pulmonary symptom improvement and reduction of the risk of exacerbations, long-acting anticholinergics seem to be preferred over
beta-2-agonists in patients with concurrent HF, although both drugs
Other pulmonary medication
prescribed in chronic obstructive
pulmonary disease
Inhaled or oral corticosteroids are recommended in COPD
patients with GOLD stage 3 or 4.1 Apart from the known adverse
metabolic effects in cardiovascular diseases, corticosteroids are
also known to induce sodium and water retention, and may therefore cause worsening of HF.64 Although the risk is thought to be
rather low with inhaled corticosteroids, prescription of corticosteroids in patients with HF should be considered carefully.
The xanthine derivative theophylline is regarded as a secondchoice bronchodilator in COPD. Theophylline has, however, only
a small therapeutic range and may accumulate easily, especially in
older patients with HF.65 As toxic alterations may also include fatal
arrhythmias, theophylline should preferably be avoided in patients
with HF.
How to manage our case?
Coming back to our patient at the beginning of this review.
What would be the most appropriate diagnostic and therapeutic
approach?
As the patient is obviously decompensated, diuretics are indicated. Bronchodilator therapy with (short-acting) salbutamol might
provide immediate relief of dyspnoea and could therefore be considered as short-term therapy to bridge the time till the diuretics
take effect. Evidence for such an approach is, however, scarce and
has not been proven to be prognostically beneficial.66 Moreover,
one has to consider the risk of tachyarrhythmias, and therefore
low dosing with monitoring of heart rate and rhythm seems mandatory. After initial stabilization, the underlying cause and severity of
HF should be evaluated and medication initiated or optimized as
recommended by the current HF guidelines. The patient should be
encouraged to stop smoking and in the meanwhile considered as
suspected of having COPD. A complete pulmonary function test
should be performed months later when the patient is euvolaemic.
Until COPD is then firmly established, any pulmonary therapy must
be considered experimental.
Conclusions
In patients with HF, a (post-dilatory) FEV1 /FVC ratio <0.7 is insufficient to diagnose true COPD. Because of the potential risk of detrimental effects of bronchodilators in cardiac patients, and in order
to prevent unnecessary polypharmacy, long-acting bronchodilators
should only be started or maintained in subjects with true COPD.
Inhalative therapy should be preferred over oral, as systemic effects
........................................................................................................................................................................................................................
were related to severe side effects especially in patients with underlying cardiovascular diseases.
In any case, after initiation of bronchodilators, physicians should
carefully monitor symptom improvements and side effects in
patients with HF, and eventually consider drug discontinuation.
G. Gder et al.
are less if therapy is applied locally. A complete pulmonary function
test executed under stable, euvolaemic conditions is a mandatory
prerequisite to establish definitely a diagnosis of COPD. In patients
with co-morbid COPD and HF, accurate severity grading of COPD
is not feasible with currently advocated scores. Adequately powered randomiszd trials are needed to establish the best treatment
approach in patients with concurrent COPD and HF.
Funding
G.G. was supported by a fellowship grant from the Medical Faculty of the University of Wrzburg (Habilitationsstipendium). This
work was supported by grants from the German Ministry of Education and Research (BMBF), Berlin, Germany [BMBF 01EO1004;
Comprehensive Heart Failure Center Wrzburg].
Conflict of interest: none declared.
References
1. Vestbo J, Hurd SS, Agusti AG, Jones PW, Vogelmeier C, Anzueto A, Barnes PJ,
Fabbri LM, Martinez FJ, Nishimura M, Stockley RA, Sin DD, Rodriguez-Roisin
R. Global strategy for the diagnosis, management, and prevention of chronic
obstructive pulmonary disease: GOLD executive summary. Am J Respir Crit Care
Med 2013;187:347365.
2. McMurray JJ, Adamopoulos S, Anker SD, Auricchio A, Bohm M, Dickstein K, Falk
V, Filippatos G, Fonseca C, Gomez-Sanchez MA, Jaarsma T, Kober L, Lip GY,
Maggioni AP, Parkhomenko A, Pieske BM, Popescu BA, Ronnevik PK, Rutten FH,
Schwitter J, Seferovic P, Stepinska J, Trindade PT, Voors AA, Zannad F, Zeiher A,
Bax JJ, Baumgartner H, Ceconi C, Dean V, Deaton C, Fagard R, Funck-Brentano
C, Hasdai D, Hoes A, Kirchhof P, Knuuti J, Kolh P, McDonagh T, Moulin C, Reiner
Z, Sechtem U, Sirnes PA, Tendera M, Torbicki A, Vahanian A, Windecker S, Bonet
LA, Avraamides P, Ben Lamin HA, Brignole M, Coca A, Cowburn P, Dargie H,
Elliott P, Flachskampf FA, Guida GF, Hardman S, Iung B, Merkely B, Mueller C,
Nanas JN, Nielsen OW, Orn S, Parissis JT, Ponikowski P. ESC guidelines for the
diagnosis and treatment of acute and chronic heart failure 2012: the Task Force
for the Diagnosis and Treatment of Acute and Chronic Heart Failure 2012 of
the European Society of Cardiology. Developed in collaboration with the Heart
Failure Association (HFA) of the ESC. Eur J Heart Fail 2012;14:803869.
3. Hawkins NM, Virani S, Ceconi C. Heart failure and chronic obstructive pulmonary disease: the challenges facing physicians and health services. Eur Heart
J 2013;34:27952807.
4. Brenner S, Guder G, Berliner D, Deubner N, Frohlich K, Ertl G, Jany B,
Angermann CE, Stork S. Airway obstruction in systolic heart failureCOPD
or congestion? Int J Cardiol 2013;168:19101916.
5. Hansen JE, Sun XG, Wasserman K. Spirometric criteria for airway obstruction:
use percentage of FEV1/FVC ratio below the fifth percentile, not <70%. Chest
2007;131:349355.
6. Hardie JA, Buist AS, Vollmer WM, Ellingsen I, Bakke PS, Morkve O. Risk of
over-diagnosis of COPD in asymptomatic elderly never-smokers. Eur Respir J
2002;20:11171122.
7. Marks GB. Are reference equations for spirometry an appropriate criterion for
diagnosing disease and predicting prognosis? Thorax 2012;67:8587.
8. Moons KG, Grobbee DE. When should we remain blind and when should our
eyes remain open in diagnostic studies? J Clin Epidemiol 2002;55:633636.
9. Bertens LC, Broekhuizen BD, Naaktgeboren CA, Rutten FH, Hoes AW, van
Mourik Y, Moons KG, Reitsma JB. Use of expert panels to define the reference
standard in diagnostic research: a systematic review of published methods and
reporting. PLoS Med 2013;10:e1001531.
10. Guder G, Brenner S, Angermann CE, Ertl G, Held M, Sachs AP, Lammers JW, Zanen P, Hoes AW, Stork S, Rutten FH. GOLD or lower limit
of normal definition? A comparison with expert-based diagnosis of chronic
obstructive pulmonary disease in a prospective cohort-study. Respir Res 2012;
13:13.
11. Rutten FH, Cramer MJ, Grobbee DE, Sachs AP, Kirkels JH, Lammers JW, Hoes
AW. Unrecognized heart failure in elderly patients with stable chronic obstructive
pulmonary disease. Eur Heart J 2005;26:18871894.
2014 The Authors
European Journal of Heart Failure 2014 European Society of Cardiology
12. US Surgeon General. The health consequences of smoking. Chronic obstructive lung disease. A report of the Surgeon General Rockville, MD: US Department of Health and Human Services; Public Health Service; 1984 [http://www.
surgeongeneral.gov/library/reports/index.html], DHHS (PHS) 84-50205. 1984.
13. Apostolovic S, Jankovic-Tomasevic R, Salinger-Martinovic S, DjordjevicRadojkovic D, Stanojevic D, Pavlovic M, Stankovic I, Putnikovic B, Kafedzic S,
Catovic S, Tahirovic E, Dungen HD. Frequency and significance of unrecognized
chronic obstructive pulmonary disease in elderly patients with stable heart
failure. Aging Clin Exp Res 2011;23:337342.
14. Iversen KK, Kjaergaard J, Akkan D, Kober L, Torp-Pedersen C, Hassager C,
Vestbo J, Kjoller E. Chronic obstructive pulmonary disease in patients admitted
with heart failure. J Intern Med 2008;264:361369.
15. Sin DD, Man SF. Why are patients with chronic obstructive pulmonary disease at
increased risk of cardiovascular diseases? The potential role of systemic inflammation in chronic obstructive pulmonary disease. Circulation 2003;107:15141519.
16. Sevenoaks MJ, Stockley RA. Chronic obstructive pulmonary disease, inflammation and co-morbiditya common inflammatory phenotype? Respir Res
2006;7:70.
17. Dougados M, Soubrier M, Antunez A, Balint P, Balsa A, Buch MH, Casado
G, Detert J, El-Zorkany B, Emery P, Hajjaj-Hassouni N, Harigai M, Luo SF,
Kurucz R, Maciel G, Mola EM, Montecucco CM, McInnes I, Radner H, Smolen
JS, Song YW, Vonkeman HE, Winthrop K, Kay J. Prevalence of comorbidities in rheumatoid arthritis and evaluation of their monitoring: results of
an international, cross-sectional study (COMORA). Ann Rheum Dis 2014;73:
6268.
18. Whitehead WE, Palsson OS, Levy RR, Feld AD, Turner M, Von Korff M. Comorbidity in irritable bowel syndrome. Am J Gastroenterol 2007;102:27672776.
19. Hawkins NM, Petrie MC, Jhund PS, Chalmers GW, Dunn FG, McMurray JJ.
Heart failure and chronic obstructive pulmonary disease: diagnostic pitfalls and
epidemiology. Eur J Heart Fail 2009;11:130139.
20. Macchia A, Rodriguez Moncalvo JJ, Kleinert M, Comignani PD, Gimeno G,
Arakaki D, Laffaye N, Fuselli JJ, Massolin HP, Gambarte J, Romero M, Tognoni
G. Unrecognised ventricular dysfunction in COPD. Eur Respir J 2011;39:
5158.
21. Minasian AG, van den Elshout FJ, Dekhuijzen PN, Vos PJ, Willems FF, van den
Bergh PJ, Heijdra YF. Bronchodilator responsiveness in patients with chronic
heart failure. Heart Lung 2013;42:208214.
22. Mascarenhas J, Lourenco P, Lopes R, Azevedo A, Bettencourt P. Chronic
obstructive pulmonary disease in heart failure. Prevalence, therapeutic and
prognostic implications. Am Heart J 2008;155:521525.
23. Minasian AG, van den Elshout FJ, Dekhuijzen PN, Vos PJ, Willems FF, van den
Bergh PJ, Heijdra YF. COPD in chronic heart failure: less common than previously
thought? Heart Lung 2013;42:365371.
24. Boschetto P, Fucili A, Stendardo M, Malagu M, Parrinello G, Casimirri E, Potena
A, Ballerin L, Fabbri LM, Ferrari R, Ceconi C. Occurrence and impact of
chronic obstructive pulmonary disease in elderly patients with stable heart failure.
Respirology 2013;18:125130.
25. Beghe B, Verduri A, Bottazzi B, Stendardo M, Fucili A, Balduzzi S, Leuzzi C, Papi A,
Mantovani A, Fabbri LM, Ceconi C, Boschetto P. Echocardiography, spirometry,
and systemic acute-phase inflammatory proteins in smokers with COPD or CHF:
an observational study. PLoS One 2013;8:e80166.
26. Steinacher R, Parissis JT, Strohmer B, Eichinger J, Rottlaender D, Hoppe UC,
Altenberger J. Comparison between ATS/ERS age- and gender-adjusted criteria
and GOLD criteria for the detection of irreversible airway obstruction in chronic
heart failure. Clin Res Cardiol 2012;101:637645.
27. Rutten FH, Cramer MJ, Lammers JW, Grobbee DE, Hoes AW. Heart failure and
chronic obstructive pulmonary disease: an ignored combination? Eur J Heart Fail
2006;8:706711.
28. Kee K, Naughton MT. Heart failure and the lung. Circ J 2010;74:25072516.
29. Melo LC, Silva MA, Calles AC. Obesity and lung function: a systematic review.
Einstein (Sao Paulo) 2014;12:120125.
30. Guder G, Rutten FH, Brenner S, Angermann CE, Berliner D, Ertl G, Jany B,
Lammers JW, Hoes AW, Stork S. The impact of heart failure on the classification
of COPD severity. J Card Fail 2012;18:637644.
31. Faggiano P. Abnormalities of pulmonary function in congestive heart failure. Int J
Cardiol 1994;44:18.
32. Dimopoulou I, Daganou M, Tsintzas OK, Tzelepis GE. Effects of severity
of long-standing congestive heart failure on pulmonary function. Respir Med
1998;92:13211325.
33. Puri S, Dutka DP, Baker BL, Hughes JM, Cleland JG. Acute saline infusion reduces
alveolarcapillary membrane conductance and increases airflow obstruction in
patients with left ventricular dysfunction. Circulation 1999;99:11901196.
34. Light RW, George RB. Serial pulmonary function in patients with acute heart
failure. Arch Intern Med 1983;143:429433.
........................................................................................................................................................................................................................
Accurate diagnosis and treatment of COPD in HF
2014 The Authors
European Journal of Heart Failure 2014 European Society of Cardiology
35. Petermann W, Barth J, Entzian P. Heart failure and airway obstruction. Int J Cardiol
1987;17:207209.
36. Puente-Maestu L, Stringer WW. Hyperinflation and its management in COPD.
Int J Chron Obstruct Pulmon Dis 2006;1:381400.
37. Hope J. A Treatise on the Diseases of the Heart and Great Vessels, 3rd ed. Philadelphia,
PA: Lea and Blanchard; 1839. pp466471.
38. Tanabe T, Rozycki HJ, Kanoh S, Rubin BK. Cardiac asthma: new insights into an
old disease. Expert Rev Respir Med 2013;6:705714.
39. Jorge S, Becquemin MH, Delerme S, Bennaceur M, Isnard R, Achkar R, Riou
B, Boddaert J, Ray P. Cardiac asthma in elderly patients: incidence, clinical
presentation and outcome. BMC Cardiovasc Disord 2007;7:16.
40. Agostoni P, Guazzi M, Bussotti M, De Vita S, Palermo P. Carvedilol reduces the
inappropriate increase of ventilation during exercise in heart failure patients. Chest
2002;122:20622067.
41. Witte KK, Clark AL. Beta-blockers and inspiratory pulmonary function in chronic
heart failure. J Card Fail 2005;11:112116.
42. Agostoni P, Contini M, Cattadori G, Apostolo A, Sciomer S, Bussotti M, Palermo
P, Fiorentini C. Lung function with carvedilol and bisoprolol in chronic heart
failure: is beta selectivity relevant? Eur J Heart Fail 2007;9:827833.
43. Dungen HD, Apostolovic S, Inkrot S, Tahirovic E, Topper A, Mehrhof F, Prettin C,
Putnikovic B, Neskovic AN, Krotin M, Sakac D, Lainscak M, Edelmann F, Wachter
R, Rau T, Eschenhagen T, Doehner W, Anker SD, Waagstein F, Herrmann-Lingen
C, Gelbrich G, Dietz R. CIBIS-ELD investigators and Project Multicentre Trials in
the Competence Network Heart Failure Titration to target dose of bisoprolol
vs. carvedilol in elderly patients with heart failure: the CIBIS-ELD trial. Eur J Heart
Fail 2011;13:670680.
44. Agostoni P, Palermo P, Contini M. Respiratory effects of beta-blocker therapy in
heart failure. Cardiovasc Drugs Ther 2009;23:377384.
45. Hawkins NM, MacDonald MR, Petrie MC, Chalmers GW, Carter R, Dunn FG,
McMurray JJ. Bisoprolol in patients with heart failure and moderate to severe
chronic obstructive pulmonary disease: a randomized controlled trial. Eur J Heart
Fail 2009;11:684690.
46. Jabbour A, Macdonald PS, Keogh AM, Kotlyar E, Mellemkjaer S, Coleman CF, Elsik
M, Krum H, Hayward CS. Differences between beta-blockers in patients with
chronic heart failure and chronic obstructive pulmonary disease: a randomized
crossover trial. J Am Coll Cardiol 2010;55:17801787.
47. Lainscak M, Podbregar M, Kovacic D, Rozman J, von Haehling S. Differences between bisoprolol and carvedilol in patients with chronic heart failure and chronic obstructive pulmonary disease: a randomized trial. Respir Med
2011;105(Suppl 1):S44S49.
48. Hawkins NM, Petrie MC, Macdonald MR, Jhund PS, Fabbri LM, Wikstrand
J, McMurray JJ. Heart failure and chronic obstructive pulmonary disease
the quandary of beta-blockers and beta-agonists. J Am Coll Cardiol 2011;57:
21272138.
49. Salpeter SR, Ormiston TM, Salpeter EE, Poole PJ, Cates CJ. Cardioselective
beta-blockers for chronic obstructive pulmonary disease: a meta-analysis. Respir
Med 2003;97:10941101.
50. Le Jemtel TH, Padeletti M, Jelic S. Diagnostic and therapeutic challenges in patients
with coexistent chronic obstructive pulmonary disease and chronic heart failure.
J Am Coll Cardiol 2007;49:171180.
51. Rutten FH, Zuithoff NP, Hak E, Grobbee DE, Hoes AW. Beta-blockers may
reduce mortality and risk of exacerbations in patients with chronic obstructive
pulmonary disease. Arch Intern Med 2010;170:880887.
52. Pellegrino R, Viegi G, Brusasco V, Crapo RO, Burgos F, Casaburi R, Coates A, van
der Grinten CP, Gustafsson P, Hankinson J, Jensen R, Johnson DC, MacIntyre N,
McKay R, Miller MR, Navajas D, Pedersen OF, Wanger J. Interpretative strategies
for lung function tests. Eur Respir J 2005;26:948968.
53. Maak CA, Tabas JA, McClintock DE. Should acute treatment with inhaled beta
agonists be withheld from patients with dyspnea who may have heart failure?
J Emerg Med 2013;40:135145.
54. Salpeter SR. Cardiovascular safety of beta(2)-adrenoceptor agonist use in
patients with obstructive airway disease: a systematic review. Drugs Aging
2004;21:405414.
55. Mettauer B, Rouleau JL, Burgess JH. Detrimental arrhythmogenic and sustained
beneficial hemodynamic effects of oral salbutamol in patients with chronic
congestive heart failure. Am Heart J 1985;109:840847.
56. Cazzola M, Page CP, Calzetta L, Matera MG. Pharmacology and therapeutics of
bronchodilators. Pharmacol Rev 2012;64:450504.
57. Saldias FJ, Comellas A, Ridge KM, Lecuona E, Sznajder JI. Isoproterenol improves
ability of lung to clear edema in rats exposed to hyperoxia. J Appl Physiol (1985)
1999;87:3035.
58. Mutlu GM, Sznajder JI. beta(2)-Agonists for treatment of pulmonary edema: ready
for clinical studies? Crit Care Med 2004;32:16071608.
10
..........................
59. Uren NG, Davies SW, Jordan SL, Lipkin DP. Inhaled bronchodilators increase
maximum oxygen consumption in chronic left ventricular failure. Eur Heart J
1993;14:744750.
60. Vestbo J, Anderson J, Brook RD, Calverley PM, Celli BR, Crim C, Haumann B,
Martinez FJ, Yates J, Newby DE. The Study to Understand Mortality and Morbidity
in COPD (SUMMIT) study protocol. Eur Respir J 2013;41:10171022.
61. Michele TM, Pinheiro S, Iyasu S. The safety of tiotropiumthe FDAs conclusions.
N Engl J Med 2010;363:10971099.
62. Vogelmeier C, Hederer B, Glaab T, Schmidt H, Rutten-van Molken MP, Beeh
KM, Rabe KF, Fabbri LM. Tiotropium versus salmeterol for the prevention of
exacerbations of COPD. N Engl J Med 2011;364:10931103.
63. Gershon A, Croxford R, Calzavara A, To T, Stanbrook MB, Upshur R,
Stukel TA. Cardiovascular safety of inhaled long-acting bronchodilators in
G. Gder et al.
individuals with chronic obstructive pulmonary disease. JAMA Intern Med
2013;173:
11751185.
64. Wei L, MacDonald TM, Walker BR. Taking glucocorticoids by prescription
is associated with subsequent cardiovascular disease. Ann Intern Med. 2004;
141:764770.
65. Greenberger PA, Cranberg JA, Ganz MA, Hubler GL. A prospective evaluation of
elevated serum theophylline concentrations to determine if high concentrations
are predictable. Am J Med 1991;91:6773.
66. Dharmarajan K, Strait KM, Lagu T, Lindenauer PK, Tinetti ME, Lynn J, Li SX,
Krumholz HM. Acute decompensated heart failure is routinely treated as a
cardiopulmonary syndrome. PLoS One 2014;8:e78222.
2014 The Authors
European Journal of Heart Failure 2014 European Society of Cardiology
Anda mungkin juga menyukai
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDari EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifePenilaian: 4 dari 5 bintang4/5 (5794)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDari EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You ArePenilaian: 4 dari 5 bintang4/5 (1090)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDari EverandNever Split the Difference: Negotiating As If Your Life Depended On ItPenilaian: 4.5 dari 5 bintang4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDari EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RacePenilaian: 4 dari 5 bintang4/5 (895)
- Grit: The Power of Passion and PerseveranceDari EverandGrit: The Power of Passion and PerseverancePenilaian: 4 dari 5 bintang4/5 (588)
- Shoe Dog: A Memoir by the Creator of NikeDari EverandShoe Dog: A Memoir by the Creator of NikePenilaian: 4.5 dari 5 bintang4.5/5 (537)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDari EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersPenilaian: 4.5 dari 5 bintang4.5/5 (344)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDari EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FuturePenilaian: 4.5 dari 5 bintang4.5/5 (474)
- Her Body and Other Parties: StoriesDari EverandHer Body and Other Parties: StoriesPenilaian: 4 dari 5 bintang4/5 (821)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Dari EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Penilaian: 4.5 dari 5 bintang4.5/5 (121)
- The Emperor of All Maladies: A Biography of CancerDari EverandThe Emperor of All Maladies: A Biography of CancerPenilaian: 4.5 dari 5 bintang4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingDari EverandThe Little Book of Hygge: Danish Secrets to Happy LivingPenilaian: 3.5 dari 5 bintang3.5/5 (400)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDari EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyPenilaian: 3.5 dari 5 bintang3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)Dari EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Penilaian: 4 dari 5 bintang4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDari EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaPenilaian: 4.5 dari 5 bintang4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDari EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryPenilaian: 3.5 dari 5 bintang3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnDari EverandTeam of Rivals: The Political Genius of Abraham LincolnPenilaian: 4.5 dari 5 bintang4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealDari EverandOn Fire: The (Burning) Case for a Green New DealPenilaian: 4 dari 5 bintang4/5 (73)
- The Unwinding: An Inner History of the New AmericaDari EverandThe Unwinding: An Inner History of the New AmericaPenilaian: 4 dari 5 bintang4/5 (45)
- Rise of ISIS: A Threat We Can't IgnoreDari EverandRise of ISIS: A Threat We Can't IgnorePenilaian: 3.5 dari 5 bintang3.5/5 (137)
- Ucmc DepartmentsDokumen39 halamanUcmc DepartmentsAllen ZhuBelum ada peringkat
- Introduction To Clinical Psychology Notes 1Dokumen83 halamanIntroduction To Clinical Psychology Notes 1Paulo Miguel GernaleBelum ada peringkat
- APL 10 April 2017Dokumen24 halamanAPL 10 April 2017Naela RizqiBelum ada peringkat
- Plasma Cortisol Levels in DyspepsiaDokumen17 halamanPlasma Cortisol Levels in Dyspepsiasitnuciana_123Belum ada peringkat
- Bleeding Disorders PDFDokumen92 halamanBleeding Disorders PDFNaela RizqiBelum ada peringkat
- Causes of Interruption of Radiotherapy in Nasopharyngeal Carcinoma Patients in TaiwanDokumen5 halamanCauses of Interruption of Radiotherapy in Nasopharyngeal Carcinoma Patients in TaiwanNaela RizqiBelum ada peringkat
- Randomized Trial of Radiotherapy Versus Concurrent Chemoradiotherapy Followed by Adjuvant Chemotherapy in PatientsDokumen9 halamanRandomized Trial of Radiotherapy Versus Concurrent Chemoradiotherapy Followed by Adjuvant Chemotherapy in PatientsNaela RizqiBelum ada peringkat
- Jurnal RokokDokumen9 halamanJurnal RokokNaela RizqiBelum ada peringkat
- Form Permintaan BarangDokumen66 halamanForm Permintaan BarangNaela RizqiBelum ada peringkat
- Anemias PharmacotherapyDokumen27 halamanAnemias Pharmacotherapy1108010091Belum ada peringkat
- Bone Health GuidelinesDokumen34 halamanBone Health GuidelinesNaela RizqiBelum ada peringkat
- Biotech PPT Gene TherapyDokumen13 halamanBiotech PPT Gene TherapyNaela RizqiBelum ada peringkat
- Captopril ApplicationDokumen7 halamanCaptopril ApplicationNaela RizqiBelum ada peringkat
- Appropriate Use of Benzathine Penicillin G For Treatment of SyphilisDokumen2 halamanAppropriate Use of Benzathine Penicillin G For Treatment of SyphilisNaela RizqiBelum ada peringkat
- 5-Step Plan To Treat Constipation in Psychiatric PatientsDokumen7 halaman5-Step Plan To Treat Constipation in Psychiatric PatientsNaela RizqiBelum ada peringkat
- Stroke 1998 Yamaguchi 12 7Dokumen7 halamanStroke 1998 Yamaguchi 12 7Naela RizqiBelum ada peringkat
- 1 Ajg2010409aDokumen7 halaman1 Ajg2010409aAryaldy ZulkarnainiBelum ada peringkat
- 1398943904MS Ijbpas 2014 1756Dokumen10 halaman1398943904MS Ijbpas 2014 1756Naela RizqiBelum ada peringkat
- Citicoline (Qureshi)Dokumen15 halamanCiticoline (Qureshi)Lalalala Gabriella KristianiBelum ada peringkat
- Perinatal GLDokumen264 halamanPerinatal GLNaela RizqiBelum ada peringkat
- Prinsip Terapi GinjalDokumen1 halamanPrinsip Terapi GinjalNaela RizqiBelum ada peringkat
- Citicoline (Qureshi)Dokumen15 halamanCiticoline (Qureshi)Lalalala Gabriella KristianiBelum ada peringkat
- BHIVA Pregnancy Guidelines Update 2014Dokumen78 halamanBHIVA Pregnancy Guidelines Update 2014meliabudiBelum ada peringkat
- BoneguidelinesDokumen206 halamanBoneguidelineskrishnanoelleBelum ada peringkat
- Perinatal GLDokumen264 halamanPerinatal GLNaela RizqiBelum ada peringkat
- Clin Kidney J 2013 Hadjiyannakos 164 8Dokumen5 halamanClin Kidney J 2013 Hadjiyannakos 164 8Naela RizqiBelum ada peringkat
- Pustaka 1Dokumen587 halamanPustaka 1Naela RizqiBelum ada peringkat
- KelesuanDokumen6 halamanKelesuanNaela RizqiBelum ada peringkat
- Pustaka 3Dokumen5 halamanPustaka 3Naela RizqiBelum ada peringkat
- Antiepilepsy Drugs: Pharmacodynamics and Principles of Drug SelectionDokumen22 halamanAntiepilepsy Drugs: Pharmacodynamics and Principles of Drug SelectionNaela RizqiBelum ada peringkat
- Pustaka 2Dokumen13 halamanPustaka 2Naela RizqiBelum ada peringkat
- In Car WhoDokumen27 halamanIn Car WhoNaela RizqiBelum ada peringkat
- 792Dokumen527 halaman792MarcNicaBelum ada peringkat
- Beaumont Job Shadow All Interview Ty NoteDokumen12 halamanBeaumont Job Shadow All Interview Ty Noteapi-358423274Belum ada peringkat
- (2015) Extemporaneous Formulation 2015Dokumen80 halaman(2015) Extemporaneous Formulation 2015DanielaGarciaBelum ada peringkat
- Complied Date of MO - JharkhandDokumen59 halamanComplied Date of MO - JharkhandShiwali SinghBelum ada peringkat
- PMLS PRESENTATION (Lesson 3&4) (10.5 × 9 CM)Dokumen4 halamanPMLS PRESENTATION (Lesson 3&4) (10.5 × 9 CM)Rhygn SarmientoBelum ada peringkat
- LPL - Pasricha Diagnostics & Ultrasound Clinic: Patientreportscsuperpanel - SP - General - Template01 - SC (Version: 7)Dokumen3 halamanLPL - Pasricha Diagnostics & Ultrasound Clinic: Patientreportscsuperpanel - SP - General - Template01 - SC (Version: 7)isw1707Belum ada peringkat
- Delta Sigma Theta Sorority, Inc. Jacksonville Alumnae ChapterDokumen7 halamanDelta Sigma Theta Sorority, Inc. Jacksonville Alumnae ChaptermortensenkBelum ada peringkat
- Quality Tools Medical LaboratoryDokumen32 halamanQuality Tools Medical LaboratorySergio Cabrera CalzadillaBelum ada peringkat
- Dietschi Poste IDokumen12 halamanDietschi Poste IAxelJaraBelum ada peringkat
- 3 Lifespan CH 3 Prenatal DevelopmentDokumen23 halaman3 Lifespan CH 3 Prenatal DevelopmentJoseph Barnes100% (1)
- SOPIEDokumen16 halamanSOPIEshing_1987Belum ada peringkat
- Compliance Program Guidance Manual 7341.002 PDFDokumen45 halamanCompliance Program Guidance Manual 7341.002 PDFpopatlilo2Belum ada peringkat
- Ayurveda MD Panchakarma Academics DissertationDokumen38 halamanAyurveda MD Panchakarma Academics DissertationManish KubawatBelum ada peringkat
- Munro 2007Dokumen17 halamanMunro 2007Jose RodriguezBelum ada peringkat
- Kundalini YogaDokumen3 halamanKundalini YogaHoutan Afkhami100% (4)
- Field Demonstration ScriptDokumen3 halamanField Demonstration ScriptRizabelle Halang HernaezBelum ada peringkat
- Breathing and KiDokumen10 halamanBreathing and KiYuri DittrichBelum ada peringkat
- Leave and Joining Time Rules: National Seeds Corporation Limited (A Government of India Undertaking)Dokumen26 halamanLeave and Joining Time Rules: National Seeds Corporation Limited (A Government of India Undertaking)Rojan MathewBelum ada peringkat
- Organization Name: Al-Shifa Trust Eye Hospital, GT Road, RawalpindiDokumen4 halamanOrganization Name: Al-Shifa Trust Eye Hospital, GT Road, RawalpindiTahseen FatimaBelum ada peringkat
- Epidemiological Characteristics, Safety and Efficacy of Medical Cannabis inDokumen7 halamanEpidemiological Characteristics, Safety and Efficacy of Medical Cannabis inDanielBelum ada peringkat
- National Detector Dog Manual PDFDokumen268 halamanNational Detector Dog Manual PDFBorgy EscalanteBelum ada peringkat
- General Anxiety Remedies in HomeopathyDokumen5 halamanGeneral Anxiety Remedies in Homeopathyvijay kumarBelum ada peringkat
- 302333KW PDFDokumen19 halaman302333KW PDFdhineshBelum ada peringkat
- Experience of Dental Caries in Mother/child Pairs: Association Between Risk Indicators and Dental CariesDokumen8 halamanExperience of Dental Caries in Mother/child Pairs: Association Between Risk Indicators and Dental CariesRisky Anita OktavianiBelum ada peringkat
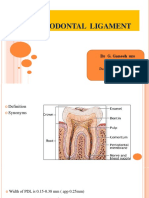
- Periodontal Ligament: Ganesh Ganji 2 Year PGDokumen34 halamanPeriodontal Ligament: Ganesh Ganji 2 Year PGNareshBelum ada peringkat
- Uji Fagositosis PDFDokumen11 halamanUji Fagositosis PDFEno PauzahBelum ada peringkat
- 123Dokumen10 halaman123Aryan SanezBelum ada peringkat
- What Is AsomatognosiaDokumen10 halamanWhat Is AsomatognosiaNedima DzaferagicBelum ada peringkat