Acute Kidney Injury
Diunggah oleh
RohitKumarHak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Acute Kidney Injury
Diunggah oleh
RohitKumarHak Cipta:
Format Tersedia
778
CHAPTER 120 Acute Kidney Injury
120
ACUTE KIDNEY INJURY
BRUCE A. MOLITORIS
DEFINITION
Acute kidney injury (AKI) is a clinical syndrome defined as a functional or
structural kidney abnormality that manifests with an increase in serum creatinine (Cr) of 0.3mg/dL or greater within 48 hours, an increase in serum
Cr of 1.5 or greater times baseline within 7 days or a urine volume less than
0.5mL/kg/hour for 6 hours (Table 120-1).1 Diagnostically, the reduction in
kidney function in AKI is staged according to the maximal rise in serum Cr or
reduction in urine output with oliguria. The use of a 50% change in serum Cr
over baseline should not be used in patients with a very low baseline volume.2
EPIDEMIOLOGY
Most episodes of AKI occur in the hospital, with an incidence of 20% among
all hospitalized patients3 and up to 50% among patients in intensive care
units. AKI is the number one reason for hospital nephrology consult. By
contrast, the incidence of community-acquired AKI is no more than 1%.
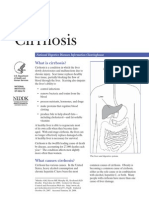
The various causes of AKI are divided broadly into three anatomic categories: prerenal, intrarenal or intrinsic, and postrenal (Fig. 120-1). Each of the
categories represents a unique pathophysiologic process with distinctive
diagnostic parameters and prognosis.
Acute Kidney Injury
Prerenal
(60-70%)
Intrinsic
(25-40%)
Postrenal
(5-10%)
Tubular
cell injury
(80-90%)
Acute
interstitial nephritis
(5-10%)
Acute
glomerulonephritis
(<5%)
Ischemia and inflammation
(sepsis, surgery,
hypoperfusion)
Toxins
Direct: aminoglycosides,
cis-platinum
Vasoconstriction: NSAIDs,
cyclosporine, radiocontrast
FIGURE120-1. Main categories of acute kidney injury. NSAIDs = nonsteroidal anti-inflammatory drugs.
CHAPTER 120 Acute Kidney Injury
779
Glomerulus
TABLE 120-2 COMMON RENAL TUBULAR TOXINS
Vasoconstriction
Afferent
blood
flow
Efferent
Decreased
permeability
Tubule backleak
Tubule
obstruction
Aminoglycosides
Radiocontrast agents
Acyclovir
Cisplatin
Sulfonamides
Methotrexate
Cyclosporine
Tacrolimus
Amphotericin B
Foscarnet
Pentamidine
Ethylene glycol
Toluene
Cocaine
HMG-CoA reductase inhibitors
HMG-CoA = 3-hydroxy-3-methylglutaryl coenzyme A.
FIGURE120-2. Mechanisms of prerenal and intrinsic acute renal injury. See text for
descriptions.
TABLE 120-3 MEDICATIONS ASSOCIATED WITH ACUTE
INTERSTITIAL NEPHRITIS
-LACTAM ANTIBIOTICS
TABLE 120-1 KDIGO ACUTE KIDNEY INJURY
CLASSIFICATION
STAGE
SERUM CREATININE
URINE OUTPUT
1.5-1.9 times baseline
OR
0.3mg/dL (26.5mol/L) increase
<0.5mL/kg/hr for 6-12hr
2.0-2.9 times baseline
<0.5mL/kg/hr for 12hr
3.0 times baseline
OR
Increase in serum creatinine to
4.0mg/dL (353.6mol/L)
OR
Initiation of renal replacement therapy
OR
In patients <18yr, decrease in eGFR to
<35mL/min per 1.73m2
<0.3mL/kg/hr for 24hr
OR
Anuria for 12hr
eGFR = estimated glomerular filtration rate; KDIGO = Kidney Disease Improving Global
Outcomes
Prerenal Azotemia
Prerenal azotemia, which is the most common cause of AKI, is a result of
renal hypoperfusion. It accounts for approximately 60 to 70% of communityacquired and 40% of hospital-acquired cases. Hypoperfusion occurs in
disease states that reduce effective intravascular volume, such as volume
depletion from bleeding over-diuresis, sepsis (Chapter 108), heart failure
(Chapter 58), or liver failure (Chapter 154). Additionally, medications that
act directly to reduce glomerular capillary perfusion, such as angiotensinconverting enzyme (ACE) inhibitors, angiotensin-receptor blockers (ARBs),
and nonsteroidal anti-inflammatory drugs (NSAIDs), also can cause prerenal
AKI. The use of these agents in a patient with underlying renal hypoperfusion
is to be avoided.
Intrinsic Acute Kidney Injury
Intrarenal AKI often results when untreated or untreatable severe hypoperfusion leads to cellular injury and ischemic AKI. The diverse causes of intrinsic
AKI can involve any portion of the renal vasculature, nephron, or interstitium
(Fig. 120-2). Ischemic and septic injury are major causes. Renal toxins, such
as radiocontrast agents and aminoglycosides, also can damage tubules both
directly and indirectly (Table 120-2). Fortunately, AKI does not develop in
every patient exposed to these agents, but elderly patients with diabetes mellitus, hemodynamically unstable patients, and patients with a reduced effective arterial volume (heart failure, burns, cirrhosis, hypoalbuminemia) are
the most susceptible to toxic renal injury. In fact, the incidence of aminoglycoside antibiotic nephrotoxicity increases from 3 to 5% to 30 to 50% in these
high-risk patients.
AKI secondary to injury to the renal interstitium is termed acute interstitial nephritis. Commonly implicated medications for interstitial nephritis
include penicillins, cephalosporins, sulfonamides, and NSAIDs (Table 1203) (Chapter 122). Bacterial and viral infections also can be the causative
Penicillin
Cephalosporins
Ampicillin
Methicillin
Nafcillin
DIURETICS
Furosemide
Hydrochlorothiazide
Triamterene
OTHER ANTIBIOTICS
Sulfonamides
Vancomycin
Rifampin
Acyclovir
Indinavir
NSAIDS
Ibuprofen
Naproxen
Indomethacin
NSAIDs = nonsteroidal anti-inflammatory drugs.
agents. Interstitial nephritis is also associated with a kidney-confined or systemic autoimmune process, such as systemic lupus erythematosus (Chapter
266), Sjgren syndrome (Chapter 268), cryoglobulinemia (Chapter 187),
and primary biliary cirrhosis (Chapter 153).
Postrenal Acute Kidney Injury
Postrenal AKI can occur in the setting of bilateral urinary outflow obstruction
or in a patient with a solitary kidney when a single urinary outflow tract is
obstructed (Chapter 123). Most commonly, this type of outflow obstruction
is observed in patients with prostatic hypertrophy (Chapter 129), prostatic
or cervical cancer (Chapter 199), or retroperitoneal disorders, including
lymphadenopathy. A functional obstruction also can be observed in patients
with a neurogenic bladder. In addition, intraluminal obstruction can be seen
in patients with bilateral renal calculi (Chapter 126), papillary necrosis, blood
clots, and bladder carcinoma, whereas extraluminal obstruction can develop
in connection with retroperitoneal fibrosis, colon cancer, and lymphomas.
Finally, intratubular crystallization of compounds such as uric acid, calcium
oxalate, acyclovir, sulfonamide, and methotrexate, as well as myeloma light
chains, can result in tubular obstruction.
PATHOBIOLOGY
The causes of AKI are diverse, and it can arise from a number of physiologic
insults that injure the kidney and reduce the glomerular filtration rate (GFR).
Decreased kidney perfusion and a reduced GFR can occur with or without
cellular injury; toxic, ischemic, or obstructive injury to the nephron; inflammation and edema of the tubulointerstitium; and a primary glomerular
disease process.
780
CHAPTER 120 Acute Kidney Injury
100
TABLE 120-4 CONDITIONS THAT LEAD TO ISCHEMIC ACUTE
RENAL FAILURE
Large-vessel renal vascular disease
Renal artery thrombosis or embolism,
intraoperative arterial cross-clamping, renal
artery stenosis, cholesterol emboli
Small-vessel renal vascular disease
Impaired renal blood flow
Sepsis, vasculitis, atheroembolism, hemolyticuremic syndrome, malignant hypertension,
scleroderma, preeclampsia, sickle cell
anemia, hypercalcemia, transplant rejection
Cyclosporine, tacrolimus, ACEIs, ARBs,
NSAIDs, radiocontrast agents
ACEIs = angiotensin-converting enzyme inhibitors; ARBs = angiotensin-receptor blockers; NSAIDs
= nonsteroidal anti-inflammatory drugs.
Prerenal Acute Kidney Injury
The precipitating event for prerenal AKI is hypoperfusion of the kidney (see
Fig. 120-2), which can be caused by a reduction in the total or intravascular
fluid volume or disease states associated with normal or even increased total
or intravascular fluid volumes but decrements in effective arterial volume,
such as in sepsis, heart failure, and advanced cirrhosis. Prerenal azotemia is
also divided functionally into volume responsive and nonresponsive azotemia, based on the response to hydration. For example, in severe heart failure
(Chapter 58), additional intravascular volume may not improve kidney perfusion, whereas afterload reduction may improve perfusion by increasing
cardiac output. Early in the course of prerenal AKI, the renal parenchyma
remains intact and functional. During this initial phase, the GFR remains
largely intact because kidney hypoperfusion initiates a neurohormonal
cascade that results in afferent arteriolar dilation and efferent arteriolar constriction, thereby maintaining glomerular perfusion pressure. Because prerenal azotemia is often easily reversible, and mortality rates are low, early
diagnosis and correction of the underlying pathophysiology are of critical
importance. However, without early medical corrective intervention, prerenal azotemia progresses, ischemia worsens, and the resulting injury to tubular
epithelial cells further decreases the GFR. This progression from prerenal
azotemia to ischemic AKI is a continuum that depends on the severity and
duration of the pathophysiologic insult.
Intrarenal Acute Kidney Injury
Intrinsic AKI is classified according to the primary histologic site of injury:
tubules, interstitium, vasculature, or glomerulus. Renal tubular epithelial cell
injury, commonly termed acute tubular necrosis (ATN), occurs more commonly in the setting of ischemia, although the renal tubules also can be
damaged by specific kidney toxins. Ischemia can arise from a number of different clinical scenarios, but the common underlying pathogenesis is reduced
renal blood flow (Table 120-4) with progression from prerenal azotemia to
ischemic AKI in four distinct clinical and cellular phases: initiation, extension, maintenance, and recovery. Each of these phases encompasses distinct
cellular events and declines in GFR as the kidneys respond to the insult and
attempt to maintain and reestablish function (Fig. 120-3).4 The initiation
phase, which marks the transition from prerenal to tubular cell injury and
dysfunction, is characterized by severe cellular depletion of adenosine triphosphate. Renal tubular epithelial cell injury, especially of proximal tubular
cells, is a prominent feature during this phase, but injury to endothelial and
vascular smooth muscle cells also has been documented. During this phase,
extensive signaling between the proximal tubular cells and adjacent endothelial cells results in endothelial dysfunction and an inflammatory endothelial
response.5 Leukocytes of all types play a role in ongoing inflammation and
cell injury. Dendritic cells, macrophages, neutrophils, and lymphocytes have
been shown to play either a detrimental or protective role. The time course
of involvement varies according to the cell type, and changes in macrophage
phenotype from M1 to M2 mediate conversion from a proinflammatory form
to a repair-mediating form.
GFR (%)
Sepsis, hepatorenal syndrome
B
y
er
ov
c
Re
Systemic vasodilation, renal
vasoconstriction
sio
Heart failure, cirrhosis, hepatorenal syndrome,
peritonitis
en
Decreased effective intravascular
volume
t
Ex
Hemorrhage; gastrointestinal, renal, and dermal
losses
na
CONDITION
Intravascular volume depletion
and hypotension
ere
Inflation
MECHANISM
Pr
Maintenance
0
0
Days
FIGURE120-3. Phases of acute kidney injury. GFR = glomerular filtration rate. (From
Sutton TA, Fisher CJ, Molitoris BA. Microvascular endothelial injury and dysfunction
during ischemic acute renal failure. Kidney Int. 2002;62:1539-1549.)
During the extension phase, microvascular congestion with continued
hypoxia and inflammation are most pronounced in the corticomedullary
junction of the kidney, where reperfusion is limited owing to endothelial
dysfunction at the capillary and postcapillary venule levels, with white blood
cell adhesion and rouleaux formation.6 The GFR is at its ebb during the
maintenance phase as cells undergo repair, migration, and proliferation and
as the kidney attempts to reestablish cellular and tubular integrity. Finally,
during the recovery phase, the GFR begins to improve as cellular differentiation continues and normal cellular and organ function returns. Proximal
tubular cells undergo cellular repair, and terminally differentiated epithelial
cells re-express stem cell markers and divide to repopulate the nephron.7 This
last phase is often heralded by increasing urine output.
The S3 segment of the proximal tubule is located in the outer stripe of the
medullary region of the nephron. This region is particularly susceptible to
continued reduced perfusion after injury, and ongoing or worsening hypoxia
results in continued cellular injury. Proximal tubular cell injury during the
initiation phase of renal ischemia is first manifested as bleb formation in the
apical membranes, with loss of the brush border. Proximal tubule cells also
lose the polarity of the surface membrane and the integrity of their tight
junctions. As the injury progresses, both live and necrotic proximal cells
detach and enter the tubular lumen, where they ultimately form casts in the
distal tubule. Casts contribute to a reduction in GFR by obstructing tubular
urine flow, thereby preventing further filtration into that nephron. In addition, loss of the epithelial cell barrier and cell tight junctions allows back-leak
of the glomerular filtrate into the interstitium, thus further compromising
GFR (see Fig. 120-2).
Common agents that can cause direct tubular cell toxicity (see Table
120-2) include the aminoglycoside antibiotics, intravenous radiocontrast
agents, and cisplatin. Other agents such as radiocontrast dyes, NSAIDs, and
cyclosporine induce vasoconstriction and reduce kidney perfusion. Cocaine
and the 3-hydroxy-3-methylglutaryl coenzyme A (HMG-CoA) reductase
inhibitors can damage skeletal muscle and cause rhabdomyolysis (Chapter
113), thereby resulting in the release of myoglobin that is toxic to the tubular
epithelium. Finally, the precipitation of some compounds or their metabolites can cause intratubular obstruction; agents in this category include acyclovir, sulfonamides, ethylene glycol (calcium oxalate metabolite; Chapter
110), methotrexate, and the light chains of multiple myeloma (Chapter 187).
Sepsis is a very common cause of intrinsic AKI. Although the causes of
septic AKI are often multifactorial, ischemia owing to poor microvascular
perfusion is a major factor. Interestingly, proximal tubular cells act as part of
the innate immune system to detect danger-associated molecular patterns
and establish pathogen-associated recognition patterns via toll-like receptors
(TLRs).8 Lipopolysaccharide is a prime example of proximal tubule TLR4mediated uptake that results in subsequent signaling via cytokines and oxidative stress. The resulting histology in humans is patchy involvement of cells
with apoptosis and minimal cellular necrosis that cannot fully explain the
severity of sepsis-induced kidney dysfunction. Coagulation abnormalities of
the microvasculature also play an important role in kidney dysfunction and
ongoing ischemia.
781
CHAPTER 120 Acute Kidney Injury
In AKI caused by the interstitial injury, a mixed inflammatory infiltrate
composed of T lymphocytes, monocytes, and macrophages, is seen. These
inflammatory lesions can be diffuse or patchy in distribution. Occasionally,
granulomas also can be observed, especially in drug hypersensitivity reactions. Acute interstitial nephritis that persists and becomes chronic is characterized by interstitial fibrosis and tubular atrophy, although foci of
inflammatory cells can persist. This process can lead to chronic and even
end-stage kidney disease requiring chronic dialysis.
Vascular causes of intrinsic AKI can include microvascular and macrovascular processes. Classic microvascular disorders, which include thrombotic
thrombocytopenic purpura (Chapter 172), sepsis (Chapter 108), hemolyticuremic syndrome (Chapter 172), and the HELLP syndrome (hemolysis,
elevated liver enzymes, and low platelet count; Chapters 146 and 239), cause
AKI as a result of glomerular capillary thrombosis and microvascular occlusion. Macrovascular disease such as atherosclerosis can cause AKI secondary
to atheroembolization (Chapter 125), especially during or after an invasive
or interventional vascular procedure in a patient with preexisting atherosclerotic disease.
A less common cause of AKI is glomerulonephritis (Chapter 121), which
can be seen in systemic lupus nephritis (Chapter 266), granulomatosis with
polyangiitis (Chapter 270), polyarteritis nodosa (Chapter 270), Goodpasture syndrome (Chapter 121), Henoch-Schnlein purpura (Chapter 270),
and hemolytic-uremic syndrome (Chapter 172). AKI in this setting is termed
rapidly progressive glomerulonephritis and results from direct inflammatory
glomerular or vascular injury.
Postrenal Acute Kidney Injury
Postrenal AKI is caused by obstruction to luminal flow of the glomerular
filtrate. This obstruction results in a relatively complex pathophysiology that
begins with transmission of backpressure to Bowman space of the glomerulus. Intuitively, this backpressure would be expected to reduce the GFR.
However, by dilation of the glomerular afferent arteriole, the GFR remains
largely preserved. Unfortunately, such compensation is only transient, and
the GFR will begin to attenuate if the obstruction is not rapidly relieved. With
continued obstruction for more than 12 to 24 hours, renal blood flow and
intratubular pressure decline and large unperfused and underperfused areas
of the kidney cortex result in a reduction in GFR.
CLINICAL MANIFESTATIONS
AKI, even when advanced, frequently is first diagnosed by abnormalities
observed in a patients laboratory studies and not by any specific symptom
or sign. The clinical manifestations associated with AKI are frequently
protean, occur late in the course, and are often not apparent until kidney
dysfunction has become severe. The clinical findings of AKI also depend on
the stage at which it is diagnosed. Patients with AKI may report symptoms
such as anorexia, fatigue, nausea and vomiting, and pruritus, as well as a
decline in urine output or dark-colored urine. Furthermore, if the patient has
become volume overloaded, shortness of breath and dyspnea on exertion
may be noted.
A thorough physical examination with special emphasis on determination
of volume status and effective arterial volume is essential. If volume overload
is present, jugular venous distention, pulmonary crackles, and peripheral
edema may be found (Chapter 58). Findings such as asterixis, myoclonus, or
a pericardial rub may be seen in severe AKI.
DIAGNOSIS
A systematic approach that considers each of the three major categories in
the pathogenesis of AKI will ensure that an accurate diagnosis and an appropriate therapeutic plan will be achieved. An appropriate diagnostic strategy
is to exclude prerenal and postrenal causes first and then, if needed, begin an
evaluation for possible intrinsic causes.
Laboratory analysis of blood and urine samples of patients with AKI
reveals the level of dysfunction, will frequently suggest a cause, and may also
direct the rapidity with which a specific therapy needs to be instituted. All
patients with clinical findings of AKI should be evaluated with serum measurements of electrolytes, Cr, calcium, and phosphorus; a blood urea nitrogen level; and complete blood count with differential. In addition, urine
studies, including sodium, potassium, chloride, and Cr determinations for
calculation of the fractional excretion of sodium (FENa), are important. The
formula for calculating FENa is as follows:
FE Na =
Urine Na Plasma Cr
100
Plasma Na Urine Cr
TABLE 120-5 FENA VALUES FOR THE VARIOUS CAUSES OF
ACUTE KIDNEY INJURY
CAUSE OF ACUTE
KIDNEY INJURY
FENa
Prerenal
<1%
Intrarenal
Tubular necrosis
Interstitial nephritis
Glomerulonephritis (early)
Vascular disorders (early)
1%
1%
<1%
<1%
Postrenal
1%
BUN-TOSERUM
CREATININE RATIO
>20
<10-15
>20
TABLE 120-6 COMMON URINALYSIS FINDINGS IN ACUTE
KIDNEY INJURY
CAUSE OF ACUTE KIDNEY INJURY
Prerenal
URINALYSIS
Normal or hyaline casts
Intrarenal
Tubular cell injury
Interstitial nephritis
Vascular disorders
Muddy-brown, granular, epithelial casts
Pyuria, hematuria, mild proteinuria,
granular and epithelial casts, eosinophils
Hematuria, marked proteinuria, red blood
cell casts, granular casts
Normal or hematuria, mild proteinuria
Postrenal
Normal or hematuria, granular casts, pyuria
Glomerulonephritis
The numerical value of FENa can be helpful in determining the potential
cause of the AKI (Table 120-5). In some cases, it is better to use FECl because
urinary sodium can be elevated during systemic alkalosis when a high urinary
bicarbonate level obligates the loss of sodium. Urine dipstick and microscopy
(Table 120-6) should be performed on a fresh urine sample because important cellular elements that could indicate potential causes degrade rapidly
with time. Finally, renal ultrasound to determine the presence or absence of
outlet obstruction also should be included in the initial evaluation. Measurement of urine and serum levels of structural biomarkers, such as kidney injury
molecule 1 (KIM-1) and inflammatory markers, such as neutrophil
gelatinaseassociated lipocalin (NGAL) and interleukin 18, may aid in the
diagnosis of AKI, although the data are not yet conclusive.9
Prerenal Azotemia
Prerenal azotemia, which is the most common cause of renal dysfunction,
often can be determined by the patients history. Common historical features
in patients with prerenal azotemia include vomiting, diarrhea, and poor oral
intake. Heart failure can suggest a possible prerenal cause of reduced renal
perfusion from over-diuresis or as exacerbation of the heart failure itself.
Other medications that can attenuate renal perfusion, such as NSAIDs, ACE
inhibitors, and ARBs, can cause prerenal azotemia. Common physical examination findings include tachycardia, systemic or orthostatic hypotension (or
both), and dry mucous membranes.
Laboratory studies in patients with prerenal azotemia demonstrate elevated serum Cr and blood urea nitrogen (BUN) levels. FENa is typically less
than 1%. However, in a patient taking diuretics such as furosemide, FENa may
be greater than 1% even though the patient has prerenal azotemia because of
diuretic-induced natriuresis. For these clinical situations, the fractional excretion of urea can be used and is calculated in similar fashion:
FE urea =
Urine Urea Plasma Cr
100
Plasma Urea Urine Cr
FEurea less than 35% suggests prerenal AKI. Other causes of an FENa greater
than 1% include the presence of a non-reabsorbable solute such as bicarbonate, glucose, or mannitol. Chronic kidney disease, ATN, and late obstructive
nephropathy are also associated with FENa greater than 1%. Therefore, in
these disease states, FENa cannot provide reliable diagnostic information
regarding AKI unless the FENa is less than 1%. Moreover, FEurea has not been
validated for these clinical entities.
Another laboratory parameter to assist in diagnosing prerenal AKI is the
ratio of BUN to serum Cr. Commonly, a patient with prerenal azotemia will
have a ratio of BUN to serum Cr of greater than 20:1.
782
CHAPTER 120 Acute Kidney Injury
Intrarenal Acute Kidney Injury
A history of hypotension or exposure to a nephrotoxin or medication is a
common finding in patients with intrarenal AKI. The nephrotoxin can be a
specific tubular toxin that causes ATN or a medication that causes an allergic
reaction as in acute interstitial nephritis (see Tables 120-2 and 120-3). Physical examination may reveal signs and symptoms of volume depletion or fluid
overload. It is important to remember that ATN often results from a persistent
severe prerenal state and the prerenal state must first be corrected to prevent
ongoing or worsening ATN. Rash may accompany acute interstitial nephritis.
Cholesterol embolism in patients with severe atherosclerotic disease (Chapter
125) may manifest classically as cyanotic digits and AKI; this finding is frequently seen after invasive vascular surgery or an interventional study.
Laboratory studies will demonstrate elevated serum Cr and BUN levels in
intrarenal AKI. ATN and acute interstitial nephritis are frequently associated
with FENa greater than 1, whereas FENa is typically less than 1 in early
radiocontrast-induced AKI, sepsis, glomerulonephritis, and vascular disorders. Peripheral eosinophilia and urinary eosinophils may be present in acute
interstitial nephritis, although the latter are neither sensitive nor specific for
this type of AKI. Urinary eosinophils are also associated with cholesterol
microembolic disease (Chapter 125). Intrarenal AKI has specific urinalysis
findings that can be helpful in making diagnostic and therapeutic decisions
(see Table 120-6).
Postrenal Acute Kidney Injury
A history of prostatic hypertrophy (Chapter 129), prostate cancer (Chapter
201), lymphoma (Chapter 185), cervical cancer (Chapter 199), or retroperitoneal disease often can be found in patients with postrenal AKI. Postrenal
AKI should always be in the differential diagnosis of patients with severe
oliguria (urine output < 450mL/day) or anuria (urine output < 100mL/
day). However, many patients with postrenal AKI are neither oliguric nor
anuric. Beyond an elevation in a patients serum Cr and BUN levels, laboratory studies generally yield benign results. Bladder catheterization can be
both diagnostic and therapeutic in postrenal AKI. However, renal ultrasound
is the diagnostic test of choice, although it may be falsely negative early in
postrenal AKI.
TREATMENT
The cornerstones of therapy for AKI are rapid recognition and correction of
reversible causes such as hypoperfusion, avoidance of any further renal injury,
and correction and maintenance of a normal electrolyte and fluid volume
milieu. Preventive therapy or medical interventions performed during the initiation and extension phases of AKI provide the greatest chance for minimizing
the extent of injury (see Fig. 120-3, lines A and B) and hastening renal recovery
(see Fig. 120-3, line B); interventions provided during the maintenance phase
of AKI have not proved beneficial (see Fig. 120-3, line C). If prerenal AKI is not
addressed early in a patients course or if the patient is seen late in the course,
ATN may occur and markedly increase morbidity and mortality.10
Prerenal azotemia in its early stages often can be rapidly corrected by
aggressive normalization of effective arterial volume, although more care
must be taken during volume resuscitation in patients with a history of heart
failure, cirrhosis, and sepsis. Key approaches include administering volume
(e.g., normal saline) to achieve euvolemia, improving cardiac output by afterload reduction (Chapter 59), or normalizing systemic vascular resistance.
Postrenal AKI secondary to prostatic hypertrophy frequently can be corrected by placement of a bladder catheter. However, outlet obstruction from
a neoplastic process will usually require urologic consultation for consideration of ureteral stenting or placement of a percutaneous nephrostomy tube.
Intrarenal AKI can be the most complex and difficult to treat. AKI caused by
glomerulonephritis (Chapter 121) or vasculitis (Chapters 266 and 270) will
frequently require immunosuppressive therapy. For suspected acute interstitial nephritis, the offending medication must be determined and discontinued; a 2-week tapering course of glucocorticoids, beginning with 1mg/kg of
prednisone (up to 60mg) for 3 days, is commonly recommended despite the
absence of data from randomized trials.
General supportive measures include avoiding any further nephrotoxins
and paying careful attention to the patients fluid balance by monitoring
weight and daily input and output. In addition, serum electrolytes, Cr, and BUN
should be monitored at least daily more frequently if the patients renal function appears to be tenuous. Patients with AKI also should receive a diet low in
sodium, potassium, and protein, which can be liberalized as the patients renal
function improves. A phosphate binder (e.g., calcium acetate [1334mg], lanthanum carbonate [500mg], sevelamer [300 to 1000mg], or aluminum
hydroxide [300 to 600mg] with each meal; see Table 119-4) is also usually
helpful in controlling the serum phosphate level by minimizing the absorption
of dietary phosphate.
Early nephrology consultation will ensure that the patient receives optimal
care. Some patients will warrant urgent hemodialysis because of marked metabolic acidosis unresponsive to sodium bicarbonate infusions; electrolyte
abnormalities, such as hyperkalemia that is unresponsive to medical management; pulmonary edema not responding to diuretic therapy; and uremic symptoms of encephalopathy, seizures, and pericarditis. In the absence of acute
indications, however, when to initiate dialysis in AKI remains unresolved.
For AKI, early initiation of dialysis (Cr level 7.5mg/dL) is no better than
standard dialysis beginning at a Cr level of approximately 10mg/dL.A1 Furthermore, intensive dialytic renal support therapy is no better than standard dialytic therapy, and intermittent hemodialysis and continuous renal replacement
therapy lead to similar clinical outcomes in acute renal failure. However, it is
important to verify that the prescribed dialysis is received and that standardized measures are achieved. Some patientsespecially patients in an increased
catabolic state, trauma patients, and patients receiving glucocorticoidsmay
require dialysis more than three times per week to achieve adequate therapy
(Chapter 131). Neither furosemide nor low-dose dopamine improve outcome,
even though low-dose dopamine may temporarily improve metrics of renal
physiology.
PREVENTION
Given the marked increase in morbidity and mortality associated with AKI,
especially for critically ill patients, potential measures to prevent AKI are
essential. The first step in prevention, however, is being aware of patients who
are at highest risk for AKI because of known kidney disease or comorbid
medical conditions, such as chronic kidney disease, diabetes, hypertension,
nephrotic syndrome, heart failure, age, and peripheral vascular disease.
Of all the risk factors for acquiring AKI, the presence of preexisting chronic
kidney disease is the most predictive. Recent data document a vicious cycle
involving AKI and CKD (Fig. 120-4). Appropriate hospital surveillance
measures include avoiding nephrotoxic medications (e.g., NSAIDs and
aminoglycosides); minimizing diagnostic procedures that require radiocontrast material, especially in the prerenal patient; and careful monitoring of
urinary output with daily determination of serum electrolyte and Cr levels
after any procedures known to induce AKI. Additionally, educating the
patient regarding common nonprescription nephrotoxins such as NSAIDs
can reduce the risk for AKI in outpatients.
Before a potentially nephrotoxic exposure, early consultation with a
nephrologist is warranted for this high-risk group to advise whether a specific
medication or intervention may reduce the risk for AKI or whether an alternative medication or procedure, such as magnetic resonance imaging instead
of computed tomography with intravenous radiocontrast agents, may be preferred. All potential nephrotoxins, such as NSAIDs, should be discontinued
before a potentially nephrotoxic procedure and avoided after it. The patients
volume and hemodynamic status must be maximized both before and after
the event.
In high-risk patients, a renal protective intervention is often instituted
before exposure to the agent. Interventions that may be useful for preventing
AKI associated with intravenous radiocontrast agents include hydration
with intravenous sodium chlorideA2A3 and short-term rosuvastatin (40mg on
admission then 20mg/day or 10mg/day for 2 days before and 3 days after
,
A Vicious Cycle
Elderly/Diabetes mellitus/CKD
Vulnerable
endothelium
Chronic decreased
renal perfusion
Altered renal microvasculature
Attenuation of capillary labyrinth
Renal injury: Decreased
renal blood flow
NSAIDs, radiocontrast,
surgery, infection
Acute kidney injury with
endothelial dysfunction
FIGURE120-4. A vicious cycle exists between acute kidney injury (AKI) and chronic
kidney disease (CKD), with CKD increasing the risk for developing AKI, and AKI accelerating progression of CKD.
the procedure).A4A5 N-Acetylcysteine is no longer recommended for this
purpose.A6
,
PROGNOSIS
Typically, AKI secondary to prerenal causes, if diagnosed and treated early,
has the best prognosis for renal recovery. Patients with prerenal AKI commonly return to their baseline level of renal function and have a mortality rate
of less than 10%. Similarly, patients with postrenal AKI also have a good
prognosis for renal recovery if the outlet obstruction is promptly diagnosed
and definitively treated.
In contrast, patients with intrarenal AKI have a less predictable renal
outcome, and mortality in this group varies between 30 and 80%, depending
on the severity of injury. Higher mortality rates occur in older patients with
hospital-acquired AKI admitted to ICUs. Furthermore, mortality in patients
with AKI is incremental, and seemingly modest increases in serum Cr can
result in marked increases in the mortality rate. Even a rise in serum Cr of
only 0.3mg/dL results in a significantly increased mortality risk.
The clinical course after recovery from ATN is subsequent tubular regeneration with recovery of renal function. However, this outcome is less ensured
in patients with preexisting kidney disease. In addition, given the frequent
systemic nature of their illness, patients with ATN, glomerulonephritis, and
vasculitic causes of AKI may not fully recover to their baseline renal function.11 Recovery is often difficult to quantify using serum creatinine because
muscle wasting alone results in lower creatinine values.12 Patients who have a
severe episode of AKI requiring hemodialysis may not recover their renal
function and may need hemodialysis indefinitely (Chapter 131), especially if
they have a preexisting history of chronic kidney disease.13 AKI hastens progression of chronic kidney disease to end-stage kidney disease and is often the
major factor that causes such progression. It is also important that a nephrologist see most patients with hospital-acquired AKI and follow them in terms of
any progression, hypertension, or other abnormalities.
Grade A References
A1. Jamale TE, Hase NK, Kulkarni M, etal. Earlier-start versus usual-start dialysis in patients with
community-acquired acute kidney injury: a randomized controlled trial. Am J Kidney Dis. 2013;62:
1116-1121.
A2. Koc F, Ozdemir K, Altunkas F, etal. Sodium bicarbonate versus isotonic saline for the prevention
of contrast-induced nephropathy in patients with diabetes mellitus undergoing coronary angiography and/or intervention: a multicenter prospective randomized study. J Investig Med. 2013;61:
872-877.
A3. Brar SS, Aharonian V, Mansukhani P, etal. Haemodynamic-guided fluid administration for the
prevention of contrast-induced acute kidney injury: the POSEIDON randomised controlled trial.
Lancet. 2014;383:1814-1823.
A4. Han Y, Zhu G, Han L, etal. Short-term rosuvastatin therapy for prevention of contrast-induced acute
kidney injury in patients with diabetes and chronic kidney disease. J Am Coll Cardiol. 2014;63:
62-70.
A5. Leoncini M, Toso A, Maioli M, etal. Early high-dose rosuvastatin for contrast-induced nephropathy
prevention in acute coronary syndrome: results from the PRATO-ACS Study (Protective Effect of
Rosuvastatin and Antiplatelet Therapy On contrast-induced acute kidney injury and myocardial
damage in patients with Acute Coronary Syndrome). J Am Coll Cardiol. 2014;63:71-79.
A6. Acetylcysteine for prevention of renal outcomes in patients undergoing coronary and peripheral
vascular angiography: main results from the randomized Acetylcysteine for Contrast-Induced
Nephropathy Trial (ACT). Circulation. 2011;124:1250-1259.
GENERAL REFERENCES
For the General References and other additional features, please visit Expert Consult
at https://expertconsult.inkling.com.
CHAPTER 120 Acute Kidney Injury
GENERAL REFERENCES
1. Kidney Disease: Improving Global Outcomes (KDIGO) Acute Kidney Injury Work Group.
KDIGO clinical practice guide for acute kidney injury. Kidney Int Suppl. 2012;2:1-138.
2. Zeng X, McMahon GM, Brunelli SM, etal. Incidence, outcomes, and comparisons across definitions of AKI in hospitalized individuals. Clin J Am Soc Nephrol. 2014;9:12-20.
3. Susantitaphong P, Cruz DN, Cerda J, etal. World incidence of AKI: a meta-analysis. Clin J Am Soc
Nephrol. 2013;8:1482-1493.
4. Sharfuddin AA, Molitoris BA. Pathophysiology of ischemic acute kidney injury. Nat Rev Nephrol.
2011;7:189-200.
5. Bellomo R, Kellum JA, Ronco C. Acute kidney injury. Lancet. 2012;380:756-766.
6. Molitoris BA. Therapeutic translation in acute kidney injury: the epithelial/endothelial axis. J Clin
Invest. 2014;124:2355-2363.
7. Kusaba T, Lalli M, Kramann R, etal. Differentiated kidney epithelial cells repair injured proximal
tubule. Proc Natl Acad Sci U S A. 2014;111:1527-1532.
783.e1
8. Gomez H, Ince C, De Backer D, etal. A unified theory of sepsis-induced acute kidney injury: inflammation, microcirculatory dysfunction, bioenergetics, and the tubular cell adaptation to injury. Shock.
2014;41:3-11.
9. Parikh CR, Coca SG, Thiessen-Philbrook H, etal. Postoperative biomarkers predict acute kidney
injury and poor outcomes after adult cardiac surgery. J Am Soc Nephrol. 2011;22:1748-1757.
10. Prowle JR, Kirwan CJ, Bellomo R. Fluid management for the prevention and attenuation of acute
kidney injury. Nat Rev Nephrol. 2014;10:37-47.
11. Chawla LS, Eggers PW, Star RA, etal. Acute kidney injury and chronic kidney disease as interconnected syndromes. N Engl J Med. 2014;371:58-66.
12. Prowle JR, Kolic I, Purdell-Lewis J, etal. Serum creatinine changes associated with critical illness
and detection of persistent renal dysfunction after AKI. Clin J Am Soc Nephrol. 2014;9:1015-1023.
13. Stads S, Fortrie G, van Bommel J, etal. Impaired kidney function at hospital discharge and long-term
renal and overall survival in patients who received CRRT. Clin J Am Soc Nephrol. 2013;8:
1284-1291.
783.e2
CHAPTER 120 Acute Kidney Injury
REVIEW QUESTIONS
1. Acute kidney injury is a common disorder in hospitalized patients, occurring in up to 20% of all adult admissions. Within a broad differential,
which particular process is most likely as the cause of acute kidney injury
in hospitalized patients?
A. Outflow obstruction
B. Glomerulonephritis
C. Acute interstitial nephritis
D. Prerenal azotemia
E. Ischemic acute tubular necrosis
Answer: D Up to 50% of patients diagnosed with acute kidney injury in a
hospital setting have prerenal azotemia. It is important to make this diagnosis,
and it usually is a rapidly reversible alteration that is responsive to fluid
therapy, with low morbidity and mortality if treated rapidly and appropriately. However, prerenal azotemia also can lead to ischemic acute tubular
necrosis if it persists or worsens.
2. The diagnosis of prerenal azotemia is made after an appropriate history
and physical examination. What urinary and serum biomarkers can be
used to help confirm the diagnosis of prerenal azotemia?
A. A ratio of BUN to creatinine greater than 20
B. A fractional excretion of sodium less than 1%
C. A bland urine analysis
D. A and B
E. All of the above
Answer: E Prerenal azotemia is an adaptation by the kidney to hypoperfusion without cellular injury. In the prerenal state, the kidney is being inadequately perfused but not yet to a level that results in low cellular ATP and cell
injury. The kidney tries to increase the volume status of the patient by reabsorbing nearly all of the filtered sodium, thereby resulting in a low FENa. Urea
reabsorption is also increased, thereby resulting in the high ratio of BUN to
creatinine.
3. Risk factors for the development of acute kidney injury include all of the
following except?
A. Chronic kidney disease
B. Volume depletion
C. Use of nonsteroidal anti-inflammatory agents
D. Hypertension with blood pressure of 160/100mmHg
E. Nephrotoxins
Answer: D Hypertension causes chronic kidney injury but does not usually
cause acute kidney injury except with malignant hypertension. Of the remaining four risk factors, chronic kidney disease is the most important; the more
severe the chronic kidney disease, the more likely acute kidney injury is to
occur.
4. Serum creatinine is used as a marker of glomerular filtration and therefore
kidney function in patients. Numerous attempts have been made to
develop estimating equations based around serum creatinine and other
serum markers in an attempt to help quantify glomerular filtration rate
without undertaking timely and costly studies. In a patient with acute
kidney injury and either a rising or falling serum creatinine, the calculation
of an eGFR is inappropriate for which of the following reasons?
A. Serum creatinine is not in equilibrium and therefore it is not possible
to calculate eGFR.
B. There may be an alteration in the rate of creatinine released from
muscles in a hospitalized patient.
C. Other factors such as fever, glucocorticoids, or trauma, influence creatinine release.
D. With complete loss of kidney function, the serum creatinine can
rise between 1 and 4mg/dL/day depending on the patients
circumstances.
E. All of the above
Answer: E Although a stable serum creatinine can be used to estimate the
glomerular filtration rate using estimating equations, the equations are reasonably accurate only when the serum creatinine level is stable. Multiple
factors, including fever, glucocorticoids, or trauma, affect the muscle release
of creatine, which is the precursor of serum creatinine.
5. Dialysis for acute kidney injury is a sign of moderate-to-severe injury with
an enhanced morbidity and mortality for the patient. Which of the following is true regarding dialysis for acute kidney injury?
A. Dialysis should be intensive both in frequency and duration to provide
the patient with the most appropriate internal milieu.
B. The major reasons to start dialysis in a patient with acute kidney injury
include acidosis, hyperkalemia, and volume overload.
C. Continuous renal replacement has been shown to have a better
outcome for patients than intermittent hemodialysis.
D. The serum creatinine level at the initiation of dialysis inversely correlates with outcomes in patients with acute kidney injury.
E. Starting dialysis early in patients with sepsis improves outcomes.
Answer: B The patients volume, potassium level, and acid-base status are
major indications for dialysis in AKI. Adequate dialysis is critically important,
but neither increasing the intensity of dialysis nor initiating it earlier improves
outcomes.
Anda mungkin juga menyukai
- ENT Radiology ADokumen64 halamanENT Radiology AMitulsinh M RavaljiBelum ada peringkat
- Renal Case Study Final1Dokumen41 halamanRenal Case Study Final1api-202881815100% (1)
- Secondary Hyperparathyroidism in CKDDokumen52 halamanSecondary Hyperparathyroidism in CKDLee Zhi Yong100% (3)
- Pathophysiology of DiseaseDokumen7 halamanPathophysiology of DiseaseYannah Mae EspineliBelum ada peringkat
- Chirosis HepaticDokumen8 halamanChirosis HepaticCikalHrBelum ada peringkat
- Diabetes TeluguDokumen31 halamanDiabetes TeluguRamesh100% (1)
- Pancytopenia, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsDari EverandPancytopenia, A Simple Guide To The Condition, Diagnosis, Treatment And Related ConditionsBelum ada peringkat
- Cholelithiasis Treatment & ManagementDokumen8 halamanCholelithiasis Treatment & ManagementRayhanun MardhatillahBelum ada peringkat
- Ulcerative ColitisDokumen21 halamanUlcerative Colitismel_chakBelum ada peringkat
- Case Study On Alcoholic Liver DiseaseDokumen20 halamanCase Study On Alcoholic Liver DiseaseHomework PingBelum ada peringkat
- Pathology Polycystic Kidney DiseaseDokumen4 halamanPathology Polycystic Kidney DiseaseOnyedika EgbujoBelum ada peringkat
- Comparing Animal and Plant Cell Structures and FunctionsDokumen30 halamanComparing Animal and Plant Cell Structures and FunctionsNetty BontuyanBelum ada peringkat
- Nephritic SyndromeDokumen24 halamanNephritic SyndromeMuhamed Al Rohani100% (1)
- Acute Kidney Injury - Seminar Lancet 2019Dokumen16 halamanAcute Kidney Injury - Seminar Lancet 2019Giliana P. García AcevedoBelum ada peringkat
- Esophageal VaricesDokumen14 halamanEsophageal VaricesKarla So MejiaBelum ada peringkat
- Malaria MEQDokumen6 halamanMalaria MEQMuvenn KannanBelum ada peringkat
- Upper Gastrointestinal BleedingDokumen24 halamanUpper Gastrointestinal BleedingDr.Sathaporn Kunnathum100% (1)
- Acute Kidney Injury - STUDENTDokumen23 halamanAcute Kidney Injury - STUDENTJbl2328100% (3)
- Mod 7 PoisoningDokumen12 halamanMod 7 Poisoningrez198767% (3)
- Portal HypertensionDokumen65 halamanPortal HypertensionVenu MadhavBelum ada peringkat
- Case Study 26 CKDDokumen15 halamanCase Study 26 CKDapi-247284897100% (3)
- Gallstones: Causes, Symptoms and Treatment of CholelithiasisDokumen7 halamanGallstones: Causes, Symptoms and Treatment of Cholelithiasisjesabel_caraigBelum ada peringkat
- How To Whistle Loud 14 Steps (With Pictures) - WikiHowDokumen4 halamanHow To Whistle Loud 14 Steps (With Pictures) - WikiHowVeselin VasilevBelum ada peringkat
- CHOLEDOCHOLITHIASISDokumen38 halamanCHOLEDOCHOLITHIASISPrecious Cofreros100% (3)
- Anemia in CKD: Ppds Sp1 Divisi Ginjal Hipertensi Bagian Ilmu Penyakit Dalam Rsup Dr. Mohammad Hoesin Palembang 2021Dokumen31 halamanAnemia in CKD: Ppds Sp1 Divisi Ginjal Hipertensi Bagian Ilmu Penyakit Dalam Rsup Dr. Mohammad Hoesin Palembang 2021Richard 151289Belum ada peringkat
- Chronic Kidney DiseaseDokumen49 halamanChronic Kidney Diseasesarguss1471% (7)
- Dr. Rabi Dhakal 1 Year MD Resident Department of PediatricDokumen29 halamanDr. Rabi Dhakal 1 Year MD Resident Department of PediatricRabi Dhakal100% (1)
- Marking of PACESDokumen2 halamanMarking of PACESRohitKumarBelum ada peringkat
- Luria. Higher Cortical Function in ManDokumen653 halamanLuria. Higher Cortical Function in ManAlex Lir100% (2)
- HyponatremiaDokumen21 halamanHyponatremiaselma100% (1)
- Hyponatremia Algorithm GuideDokumen2 halamanHyponatremia Algorithm Guidemina000005100% (1)
- Acute Kidney Injury Review 2017Dokumen20 halamanAcute Kidney Injury Review 2017Eduardo MoraesBelum ada peringkat
- Casestudy Gastric CarcinomaDokumen53 halamanCasestudy Gastric CarcinomaAngelaTrinidadBelum ada peringkat
- Pharmacology Guide for Safe Medication AdministrationDokumen151 halamanPharmacology Guide for Safe Medication Administrationkyuss2100% (4)
- Juvenile Idiopathic Arthritis GuidlineDokumen11 halamanJuvenile Idiopathic Arthritis GuidlineAya Soraya100% (1)
- Lupus NephritisDokumen29 halamanLupus NephritisMuhammad Julpian0% (1)
- Acute Lymphocytic LeukemiaDokumen7 halamanAcute Lymphocytic Leukemiamildred alidon100% (1)
- Acute Kidney InjuryDokumen19 halamanAcute Kidney InjuryAmit Ramrattan0% (1)
- PATHOPHYSIOLOGY OF OSTEOSARCOMaDokumen1 halamanPATHOPHYSIOLOGY OF OSTEOSARCOMakyawBelum ada peringkat
- Kidney TransplantationDokumen14 halamanKidney TransplantationSujith KuttanBelum ada peringkat
- Nursing Board Exam ReviewerDokumen32 halamanNursing Board Exam ReviewerRose Anne Mückl100% (9)
- Common Cases PacesDokumen3 halamanCommon Cases PacesRohitKumarBelum ada peringkat
- Schistosomiasis Case StudyDokumen5 halamanSchistosomiasis Case Studyapi-318749549Belum ada peringkat
- Understanding Stevens-Johnson Syndrome (SJSDokumen53 halamanUnderstanding Stevens-Johnson Syndrome (SJSKathrina CraveBelum ada peringkat
- Chronic Kidney Disease CompilationDokumen33 halamanChronic Kidney Disease CompilationGwen Stefanie Lagrimas ValloyasBelum ada peringkat
- Diverticular Disease of The ColonDokumen38 halamanDiverticular Disease of The Colonapi-19641337Belum ada peringkat
- Crohn's DiseaseDokumen5 halamanCrohn's DiseaseMark CapillanesBelum ada peringkat
- Test Bank For Pathophysiology 8th Edition by MccanceDokumen15 halamanTest Bank For Pathophysiology 8th Edition by Mccanceedwardfrostxpybgdctkr100% (25)
- Case StudyDokumen12 halamanCase Studyapi-242211536100% (1)
- Acute Liver Failure in Adults: Etiology, Clinical Manifestations, and Diagnosis - UpToDateDokumen14 halamanAcute Liver Failure in Adults: Etiology, Clinical Manifestations, and Diagnosis - UpToDateIatros GarciniBelum ada peringkat
- Everything You Need to Know About Pernicious AnemiaDokumen18 halamanEverything You Need to Know About Pernicious Anemiathalafuj100% (1)
- Small Bowel ObstructionDokumen2 halamanSmall Bowel ObstructionSrividya PushpalaBelum ada peringkat
- Diverticular DiseaseDokumen15 halamanDiverticular DiseaseRogie SaludoBelum ada peringkat
- Chole CystDokumen12 halamanChole CystMoch NizamBelum ada peringkat
- Nephrotic SyndromeDokumen35 halamanNephrotic SyndromesudhaBelum ada peringkat
- Initial PE and Labs History Initial Impression: Location &Dokumen1 halamanInitial PE and Labs History Initial Impression: Location &kaydee.arBelum ada peringkat
- Hepatomegaly 1Dokumen5 halamanHepatomegaly 1Bobby ParksBelum ada peringkat
- Choledochal CystDokumen16 halamanCholedochal CystNico HernándezBelum ada peringkat
- Gastric Ulcers: Presented By: Dr. Jawaria Memon & Dr. Deep KumarDokumen31 halamanGastric Ulcers: Presented By: Dr. Jawaria Memon & Dr. Deep KumarDeep KhemaniBelum ada peringkat
- Biliary AtresiaDokumen8 halamanBiliary AtresiaBrooke MauriBelum ada peringkat
- Anatomy & PhysiologyDokumen9 halamanAnatomy & Physiologyrachael80% (5)
- Pathophysiology of Malaria: How Parasite Infection Affects the BodyDokumen20 halamanPathophysiology of Malaria: How Parasite Infection Affects the Bodymelia100% (1)
- Endometriosis: Causes, Symptoms and TreatmentDokumen31 halamanEndometriosis: Causes, Symptoms and TreatmentChauthiran Agamudaiyar100% (1)
- Liver Case StudyDokumen6 halamanLiver Case StudyGhulam MustafaBelum ada peringkat
- Pancretic Cancer Case Study - BurkeDokumen52 halamanPancretic Cancer Case Study - Burkeapi-282999254Belum ada peringkat
- Bladder Cancer Types, Symptoms, Tests & TreatmentDokumen1 halamanBladder Cancer Types, Symptoms, Tests & TreatmentCarmina AguilarBelum ada peringkat
- Diabetic Nephropathy: A GuideDokumen6 halamanDiabetic Nephropathy: A GuideZulfadliZulfadliBelum ada peringkat
- Acute Liver FailureDokumen3 halamanAcute Liver FailureElisabeth F. OjhaBelum ada peringkat
- Glomerulonephritis vs GlomerulopathiesDokumen58 halamanGlomerulonephritis vs GlomerulopathiesRahmailla Khanza Diana FebriliantriBelum ada peringkat
- Gastric CancerDokumen27 halamanGastric Cancermackiecc100% (2)
- Acrf CDokumen70 halamanAcrf CHussain AzharBelum ada peringkat
- Renal Disease: Acute Kidney Injury (AKI)Dokumen5 halamanRenal Disease: Acute Kidney Injury (AKI)api-142637023Belum ada peringkat
- Guide To Resumes & Curricula VitaeDokumen18 halamanGuide To Resumes & Curricula VitaeRohitKumarBelum ada peringkat
- McCombe Et Al. Brain 1987 (CIDP)Dokumen14 halamanMcCombe Et Al. Brain 1987 (CIDP)RohitKumarBelum ada peringkat
- WWW - Healthcare.gov/sbc-Glossary: Important Questions Answers Why This MattersDokumen10 halamanWWW - Healthcare.gov/sbc-Glossary: Important Questions Answers Why This MattersRohitKumarBelum ada peringkat
- Infectious Diseases Consultation ReportDokumen5 halamanInfectious Diseases Consultation ReportRohitKumar100% (1)
- History Taking and Physical Exam Checklist: Introduction To Clinical Medicine IIDokumen16 halamanHistory Taking and Physical Exam Checklist: Introduction To Clinical Medicine IIYukiMaedaBelum ada peringkat
- LymphadenopathyDokumen4 halamanLymphadenopathyRohitKumarBelum ada peringkat
- Epilepsy and SeizuresDokumen37 halamanEpilepsy and SeizuresRohitKumarBelum ada peringkat
- Dengue JournalDokumen4 halamanDengue JournalRohitKumarBelum ada peringkat
- Cardiogenic ShockDokumen9 halamanCardiogenic ShockRohitKumar100% (1)
- Case of Temporal Arteritis...Dokumen14 halamanCase of Temporal Arteritis...RohitKumarBelum ada peringkat
- Cardiogenic ShockDokumen9 halamanCardiogenic ShockRohitKumar100% (1)
- Terapi AntiretroviralDokumen13 halamanTerapi AntiretroviralthiamuthiaBelum ada peringkat
- Bronchial AsthmaDokumen28 halamanBronchial AsthmaRohitKumarBelum ada peringkat
- ART guidelines for HIV-Infected Adults and AdolescentsDokumen122 halamanART guidelines for HIV-Infected Adults and AdolescentsRohitKumarBelum ada peringkat
- ReproductiveDokumen45 halamanReproductiveRohitKumarBelum ada peringkat
- ACG Guideline AcutePancreatitis September 2013Dokumen16 halamanACG Guideline AcutePancreatitis September 2013gorditomaloBelum ada peringkat
- Nejm Journal Alcoholic HepatitisDokumen10 halamanNejm Journal Alcoholic HepatitisRohitKumarBelum ada peringkat
- Patient Satisfaction - ACEPDokumen8 halamanPatient Satisfaction - ACEPRohitKumarBelum ada peringkat
- Emergency Medicine Residents Perception About Patient Safety CultureDokumen4 halamanEmergency Medicine Residents Perception About Patient Safety CultureRohitKumarBelum ada peringkat
- Acute Renal FailureDokumen8 halamanAcute Renal FailureRohitKumarBelum ada peringkat
- HematologyDokumen119 halamanHematologyRohitKumarBelum ada peringkat
- Somatic HybridizationDokumen23 halamanSomatic HybridizationJan VivienelBelum ada peringkat
- Identifying Amino AcidsDokumen8 halamanIdentifying Amino AcidsWahyuniAntariBelum ada peringkat
- Bahasa Inggris: Taking Vital Sign (Injection)Dokumen7 halamanBahasa Inggris: Taking Vital Sign (Injection)iyal09Belum ada peringkat
- Acute Purulent Diseases of Fingers and HandDokumen23 halamanAcute Purulent Diseases of Fingers and Handluckyswiss7776848Belum ada peringkat
- THYMUS PPT Final 7marDokumen15 halamanTHYMUS PPT Final 7marRajesh UgalmugleBelum ada peringkat
- Aiapget2018 Q&ADokumen23 halamanAiapget2018 Q&ASatyam SinghBelum ada peringkat
- Sex and Death Chapter 2Dokumen19 halamanSex and Death Chapter 2arffurBelum ada peringkat
- Lecture (Endocrine System)Dokumen15 halamanLecture (Endocrine System)GerofeBelum ada peringkat
- Christopher MacLeod An Introduction To Practical Neural Networks and Genetic Algorithms For Engineers and Scientists PDFDokumen157 halamanChristopher MacLeod An Introduction To Practical Neural Networks and Genetic Algorithms For Engineers and Scientists PDFayhanhameedBelum ada peringkat
- 10 Urinary BladderDokumen32 halaman10 Urinary BladderMarera DomnicBelum ada peringkat
- Pharmaceutical Sales Medical Devices in Orlando FL Resume Jorge Herrera SotoDokumen3 halamanPharmaceutical Sales Medical Devices in Orlando FL Resume Jorge Herrera SotoJorgeHerraSotoBelum ada peringkat
- Bipap A30 Specification / Part NumbersDokumen2 halamanBipap A30 Specification / Part NumbersDejan ŽujovićBelum ada peringkat
- Contorneo de Hipocamo en RadioterapiaDokumen33 halamanContorneo de Hipocamo en RadioterapiaclaudiaBelum ada peringkat
- 3daybeginners PDFDokumen1 halaman3daybeginners PDFJansen Alonzo BordeyBelum ada peringkat
- CR Lab ReportDokumen6 halamanCR Lab ReportslowteeBelum ada peringkat
- Chapter 10 BloodDokumen43 halamanChapter 10 Bloodemms meBelum ada peringkat
- OBAT-OBATAN YANG MEMPENGARUHI SISTEM KARDIOVASKULERDokumen51 halamanOBAT-OBATAN YANG MEMPENGARUHI SISTEM KARDIOVASKULERQuswah MaharaniBelum ada peringkat
- Advanced Reading Skills III PDFDokumen8 halamanAdvanced Reading Skills III PDFKetheesaran LingamBelum ada peringkat
- (VCE Biology) 2007 Chemology Unit 1 Exam and SolutionsDokumen28 halaman(VCE Biology) 2007 Chemology Unit 1 Exam and SolutionsJustine LyBelum ada peringkat
- Altered Mental State Case ReportDokumen40 halamanAltered Mental State Case ReportnugrahitaBelum ada peringkat
- What Causes Chest Pain When Feelings Are Hurt - Scientific AmericanDokumen5 halamanWhat Causes Chest Pain When Feelings Are Hurt - Scientific AmericangprasadatvuBelum ada peringkat