Pulp Therapy
Diunggah oleh
fayasyabminJudul Asli
Hak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Pulp Therapy
Diunggah oleh
fayasyabminHak Cipta:
Format Tersedia
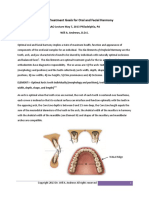
Review Article
Vital pulp therapy using calcium-enriched mixture:
An evidence-based review
Saeed Asgary, Maryam Ahmadyar1
Iranian Center for Endodontic Research, 1Dental Research Center, Research Institute of Dental Sciences, Shahid Beheshti University of
Medical Sciences, Tehran, Iran
Abstract
Worldwide, casecontrol studies have revealed that the treatment outcomes of root canal therapy (RCT) are generally favorable;
however, the overall epidemiological success rate of RCT in the general population is relatively low. On the other hand, vitality
of dental pulp is a key factor in the long-term prognosis of permanent teeth; in recent years, vital pulp therapy (VPT) has
received significant consideration as it has been revealed that the inflamed pulp has the potential to heal. In this review article,
the current best evidence with regard to VPT using calcium-enriched mixture (CEM) cement in human permanent/primary teeth
is discussed. A strategy based on a search using keywords for CEM cement as well as VPT was applied.
Keywords: Calcium-enriched mixture; CEM cement; endodontic; pulp cap; pulpitis; pulpotomy; vital pulp therapy
INTRODUCTION
Dental caries is still one of the most challenging infectious
diseases worldwide; it affects oral/general health as well
as the quality of life. Toothache and infection as the
main sequelae of untreated caries/irreversible pulpitis
are the main reasons for performing root canal therapy
(RCT). [1] Permanent mature teeth with irreversible pulpitis/
carious pulp exposure with/without clinical/radiological
findings of apical periodontitis should be treated by RCT;[2]
management of such teeth is the most common treatment
carried out by dentists.
RCT has been shown to have a good success rate when
carried out correctly.[3] Casecontrol studies have indicated
that the pooled proportion of teeth surviving over 210
years following RCT ranged between 8693%.[4] However,
such studies are mainly carried out under controlled
conditions; therefore, it is not valid to generalize such
results. Moreover, the survival rate of endodontically
treated teeth in comparison to vital teeth, especially
molars, is very low.[5]
Results of epidemiological studies, which comprise<1% of
endodontic literature, are necessary for the evaluation of
treatment outcomes of RCT in the general public.[6] Review
of these studies indicates different success rates of RCT in
various countries, ranging from 35% (Spain)[7] to 7080%
(Sweden, Portugal),[8,9] although the majority of developing/
developed countries (i.e., Iran, Brazil, Turkey, Denmark,
Scotland, and Canada) have reported success rates of
around 50%.[10-15] As an imaginary scenario, by assuming that
one root-treated tooth exists in the mouth of every adult
in a country with an adult population of 100 million, it is
estimated that on an average, 100 million endodontically
treated teeth are present, of which 50 million require
nonsurgical endodontic retreatment (NSER). Results of a
systematic review have revealed that the pooled estimated
success rate of NSER, if carried out by endodontists/
experienced clinicians, is 77%.[16] Assuming that in an
optimal scenario, this country has 2,000 endodontists, all
of whom carried out the necessary NSER treatment on the
failed 50 million teeth, the problem would still remain in
11.5 million teeth. The next option for these teeth is
surgical endodontic retreatment (SER), which has a success
rate of 60%.[17] As a result, the final treatment option
of teeth with failed SER (4.5 million) is extraction. This
imaginary scenario is representative of the inefficiency of
(non)surgical endodontic (re)treatments worldwide, which
may be related to inefficient clinical skills as well as the
complex nature of RCT.
Serious multidimensional (inter)national effort is necessary
for the improvement of the quality of RCT to increase
success rates;[7,10-15] therefore, suggestions of treatment
Access this article online
Address for correspondence:
Quick Response Code:
Prof. Saeed Asgary, Iranian Center for Endodontic Research,
Research Institute of Dental Sciences, Evin, Tehran, Iran.
E-mail: saasgary@yahoo.com
Website:
www.jcd.org.in
Date of submission : 16.04.2012
Review completed : 16.05.2012
Date of acceptance : 01.06.2012
DOI:
10.4103/0972-0707.108173
92
Journal of Conservative Dentistry | Mar-Apr 2013 | Vol 16 | Issue 2
Asgary and Ahmadyar: VPT with CEM cement
options that are simpler/less costly with a higher success
rate are a main priority in dentistry/endodontics.
Many patients are unwilling/unable to pay for necessary
dental treatments; this is directly related to the cost and
inversely related to their level of income/education and
social status.[18,19] It is clear to policy makers of oral health
care that financial difficulty is the main factor preventing the
general population from utilizing oral health-care services.
According to the authors, an attempt should be made to
provide less costly treatment options that are applicable in
the above circumstances. For patients requiring expensive
RCT, if possible, vital pulp therapy (VPT) can be provided as
a less expensive, simple/ethical treatment option.
Biological properties of human dental pulp
The biological roles of pulp tissue consist of nutrition/
sensory/defensive roles, although the most significant is
dentinogenesis (maintenance of physiological vitality of
the dentin).[20] Production of primary dentin occurs during
initial tooth formation, secondary dentin throughout
life, and tertiary dentin in response to various stimuli/
irritations.[21] The pulp is a vascularized connective tissue
consisting of various cells such as fibroblasts/stem cells. [22]
Therefore, the damaged pulp tissue of permanent teeth
has a healing potential similar to other connective tissues.
Weaker stimuli cause stimulation of odontoblasts, which in
turn induces the production of reparative dentin, and the
choice of treatment in such cases is maintenance of vitality
of the damaged odontoblasts. However, odontoblasts lose
their vitality in cases of severe damage; as the adjacent
differentiated odontoblasts cannot replace them, the stem
cells differentiate into odontoblast-like cells.[23]
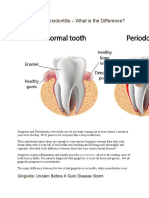
Classification of human dental pulp diseases
The conditions of the pulp that can be identified/
described by using a systematic review include: Clinically
normal pulp, reversible pulpitis, irreversible pulpitis, pulp
necrosis, hyperplastic pulpitis, internal resorption, and
pulp calcification. However, the best diagnostic terms
that represent pulpal health/disease are clinically normal
pulp, pulpitis, and necrosis.[24] The most appropriate term
to use for a dental pulp with inflammation is pulpitis,
although the generally accepted subterms are reversible
and irreversible pulpitis. Irreversible pulpitis is a pulpal
state that is theoretically characterized by mild/severe pain
that lingers after removal of a stimulus, whereas reversible
pulpitis refers to a pulpal state that implies the presence of
mild pulpal inflammation.
Currently, there are no accurate metric methods for
determining the diagnosis of reversible versus irreversible
pulpitis; however, some researchers have tried to correlate
the results of diagnostic tests with types of pulpal
inflammation.[25] As the gold standard is histological
evidence, determination of reversible versus irreversible
pulpitis by using cold testing has low sensitivity, specificity,
and predictive values.[26] Nowadays, differentiating between
reversible/irreversible pulpitis is carried out on an empirical
basis; there is no definitive evidence to support or refute
the use of these terms.[24]
From a clinical point of view, the exposed pulp may be in
one of the following three conditions: Normal pulp without
inflammation (following trauma), reversible pulpitis (after
mechanical exposure), and irreversible pulpitis (following
carious exposure); however, a recent important review
stated It is also not known whether pulps with irreversible
pulpitis are ever truly irreversibly inflamed, that is, could all
pulps with inflammation recover if conservative treatment
strategies were used? This question requires further
research to establish an answer.[24]
Definition/aims of VPT
The aims of VPT include maintenance of vitality of the
dental pulp and stimulation of the remaining pulp tissue for
adequate structural/functional healing of the pulp-dentin
complex.[27] The response of the pulp to direct capping
involves the formation of fibrodentin/reparative dentin
and remineralization of the existing dentin, resulting from
the recruitment of odontoblasts and/or proliferation of
undifferentiated mesenchymal cells, which maybe either
stem cells or dedifferentiated and transdifferentiated
mature cells.[28] Therefore, by the creation of a biological
seal, connection between the pulp and the oral environment
is eliminated and re-entry of pathogens is prevented.
Indications for VPT
Vital primary/permanent teeth with complete/incomplete
root formation after traumatic/mechanical/carious pulp
exposures are suitable candidates for VPT. The most
important factor in success is vitality of the pulp and in
particular the presence of adequate vascularization,
which is necessary for active formation/function of
odontoblasts.[29] In addition, suitable candidates for VPT
include teeth in which an appropriate coronal seal can be
provided, as the prognosis of VPT is significantly reduced in
cases of inadequate coronal seal formation and subsequent
bacterial microleakage.[30] Restorations that require
retention from radicular structures should be treated by
RCT. The presence of a healthy periodontium is necessary
for success of the treatment, as teeth with moderate to
severe periodontal disease are not suitable candidates for
VPT.[31]
Factors effective in the success of VPT
Several factors such as an adequate blood supply, severity
of inflammation, obtaining hemostasis, disinfection of the
exposure/cavity preparation, antibacterial/biocompatibility
properties of pulp-covering agents, provision of an
adequate seal, and the skills of the clinician may affect the
success of VPT.[23,32,33]
Journal of Conservative Dentistry | Mar-Apr 2013 | Vol 16 | Issue 2
93
Asgary and Ahmadyar: VPT with CEM cement
The presence of an adequate blood supply as the most
important factor is required for the maintenance of vitality
of the pulp,[23] which is, in turn, necessary for successful
outcomes via repair/regenerative mechanisms.
Although previous evidence indicates that direct pulp
capping (DPC) may be effective in the treatment of vital
inflamed pulps,[34] it has been reported that the success rate
is reduced in these cases.[35] Therefore it is recommended
to carry out pulpotomy (partial/complete) to create a
wound in an uninflamed location;[33,36] however, this is not
achievable clinically. Alternatively, inflammation of tissue
and healing of pulpal tissue seem to be tightly interlinked;
the inflammatory reaction may be a prerequisite for
the burst of progenitors implicated in pulpal repair/
regeneration.[28]
Control of hemorrhage (to achieve a clot-free pulpal
wound) is necessary for the success of VPT.[37] In addition,
sterilization/disinfection protocols should be followed
as a main principle.[38] Various options available for the
achievement of pulp hemostasis include light mechanical
pressure using a sterile cotton pellet which may be soaked
in saline/hydrogen peroxide/sodium hypochlorite solutions,
although the use of chlorhexidine as an antibacterial/
hemostatic agent is currently suggested.[32]
Another important factor in the success of VPT is the
provision of an adequate seal against bacterial (re)entry, as
a bacterial attack is the cause of failure;[39] if a pulp exposure
is adequately sealed, successful healing with the formation
of a dentin bridge may occur.[38,40]
Pulp-covering agents should provide a suitable environment
and allow regeneration of the pulp-dentin complex. Such
materials should be biocompatible, noncytotoxic, and
antibacterial[41] to induce differentiation of odontoblast
cells.
Similar to all clinical procedures, the skills of the clinician
in carrying out VPT correctly are important. Familiarity with
the principles of clinical decision making, diagnosis, case
selection, access/cavity preparation, and mixing/applying
the capping agent are necessary.
Healing mechanisms of the exposed dental
pulp
Exposure/amputation of a section of the normal pulp is a
process which results in at least short-term inflammation;
in an inflamed pulp, an exposure may well add to the
injury burden of the dental pulp. Initially, in the tissues
adjacent to the exposure site, various amounts of necrotic
tissue, inflammatory cells, and extravascular erythrocytes
can be observed. The initial damage results in the
production of fibrinogen, formation of blood clot, and
94
an acute inflammation accompanied by the presence of
polymorphonuclear leukocytes (PMNs).[42] The production
of mediators by PMNs/macrophages is a significant event
in the successful humoral immune response of the host.[43]
Some particles from the pulp-covering material/dentin
chips may also enter the underlying pulp tissue;[42] hard
tissue formation occurs around dentinal chips. Although the
hemostatic, inflammatory, proliferation, and repair phases
occur in a specific order, it is not possible to specify clearly
the beginnings and ends of these overlapping phases.[44]
The evidence with regard to pulp defense reactions is
similar to the reactions which occur during damage to
other connective tissues with their associated specific/
nonspecific defense mechanisms.[44] Successful elimination
of the causes of pulpitis using VPT results in the successful
treatment of the pulpal wound and creation of a dentin
bridge by regeneration of the pulp-dentin complex.[39,45]
Nowadays, various important studies are being carried out
in the field of pulp-dentin regeneration using molecular
biology and stem cells.[46] Although clinical application of
such techniques is not yet widespread, it appears that the
science of tissue engineering will have highly significant
effects in clinical treatment.
VPT methods
The topic of VPT has received considerable attention in
recent years, in particular with regard to being the most
suitable technique/material.[27,47] In clinical practice, VPT
is categorized as DPC/IPC (IPC: indirect pulp capping)
and miniature/partial/complete pulpotomy.[47-50] Recent
developments in technique/(bio)materials have emerged
in the evolution of the management of caries from G.V.
Black's extension for prevention to minimally invasive
dentistry (MID).[51] In MID during IPC, carious infected
dentin is removed and a pulp-covering (bio)material is
placed onto the remaining affected dentin. Sealing the
lesion with adhesive restorative materials allows healing
of the underlying pulp.[52] During DPC, a pulp-covering (bio)
material is placed directly onto the exposed pulp, which
protects it from further damage and allows healing of the
pulp-dentin complex.[53,54] During a large pulp exposure/
severe pulp inflammation, pulpotomy (miniature/partial/
complete) is carried out. This involves the removal of a
small part/all of the coronal pulp tissue, followed by direct
coverage of the remaining coronal/radicular pulp.[49,55]
CALCIUM-ENRICHED MIXTURE
CEMENT
Calcium-enriched mixture (CEM) cement was introduced to
dentistry as an endodontic filling material (USPTO number:
7,942,961). The major components of the cement powder
are calcium oxide (CaO), sulfur trioxide (SO3), phosphorous
pentoxide (P2O5), and silicon dioxide (SiO2), different from
mineral trioxide aggregate (MTA) and Portland cement
Journal of Conservative Dentistry | Mar-Apr 2013 | Vol 16 | Issue 2
Asgary and Ahmadyar: VPT with CEM cement
(PC).[56,57] The physical properties of this biomaterial,
such as flow, film thickness, and primary setting time are
favorable.[56]
Creation of a three-dimensional seal, acceptable
antimicrobial properties, and biocompatibility are highly
significant in the success of VPT.[58,59] The sealing ability
of CEM is similar to MTA[60] and improves by storage in
phosphate-buffered saline solution.[61] The particle size
of CEM is smaller than MTA;[62] this may be related to its
acceptable sealing properties. It has the ability to promote
hydroxyapatite formation in saline solution[63] and might
promote the process of differentiation in stem cells and
induce hard tissue formation, that is, cementogenesis.[64,65]
Antibacterial properties of CEM, calcium hydroxide
(CH), MTA, and PC have been compared in a number of
studies; the results have shown that CEM has antibacterial
properties similar to CH.[66,67] Comparison of antifungal
properties of CEM and MTA on Candida albicans has shown
that both biomaterials induce complete death of fungal
cells after 24 hours.[68] CEM has an alkaline pH of ~11,
which is important in the antimicrobial properties of this
biomaterial.[56] Several animal studies have shown that in
various forms of VPT treatments, the induction of dentin
bridge formation in CEM was comparable with that in
MTA and superior to that in CH.[69,70] Studies of complete
pulpotomy treatment using CEM, MTA, and CH have shown
that compared to CH, samples in the CEM group exhibited
lower inflammation, improved quality/thickness of calcified
bridge, superior pulp vitality status, and morphology of
odontoblast cells. However, no significant differences
were identified in comparison to MTA.[70] In a study using
the MTT assay on L929 as well as a scanning electron
microscope (SEM) study on human gingival fibroblast
(HGF), the cytotoxicity of CEM was compared with MTA
and intermediate restorative material (IRM); the results
indicated that the cytotoxic potentials of CEM and MTA are
both insignificant and comparable, and both biomaterials
were significantly superior to IRM.[71-73] A recent study
comparing the subcutaneous tissue response to CEM and
MTA in rats showed that unlike MTA, CEM did not induce
any cellular necrosis after one week. After 60 days, levels
of inflammation in the CEM group were significantly lower
than the white/gray MTA groups. Another significant finding
was the presence of dystrophic calcification adjacent to the
biomaterials, which is an indication of their osteo-inductive
potential.[74]
Evidence for VPT with CEM cement
Evidence-based dentistry/endodontics (EBD/EBE) is based
on the best available scientific evidence; the strength of
evidence-based clinical recommendations is classified
according to the existing level of evidence.[75] Randomized
clinical trials as well as systematic reviews (SRs) and metaanalyses provide the highest quality of evidence, followed
by cohort studies, case control studies, case series, and
case reports.[76] Numerous methods/materials have been
proposed for the treatment of exposed dental pulps;
however, many have not been based on current best
evidence, and are unreliable for generalization into the
current clinical practice of dentistry.
FULL/COMPLETE PULPOTOMY WITH
CEM CEMENT
Deciduous molars
Complete pulpotomy treatment of human deciduous molars
is a well-known treatment procedure, which is carried
out following coronal pulp exposure caused by caries/
cavity preparation/trauma. It involves amputation and
removal of the inflamed coronal pulp and maintenance of
uninflamed vital radicular pulp tissue using an appropriate
pulp-covering (bio)material.[77] Recently, a randomized
clinical trial study on the success rates of MTA and CEM in
pulpotomy of deciduous molars with a two-year follow-up
period was published. The results of this trial, which is of
level 1 quality of evidence, indicated that only one tooth
in the CEM group presented with failure, whereas three
teeth in the MTA group were extracted due to pathologic
resorption; however, this difference was not statistically
significant. It was concluded that pulpotomy treatment
of deciduous molars using CEM is an advisable/successful
treatment modality.[78]
Permanent teeth
Open apex
Apexogenesis is considered as the treatment of choice in
vital permanent teeth with incomplete root formation.[79,80]
A rare case of a maxillary incisor with an open apex and
traumatic pulp exposure has been reported; the tooth was
left untreated for one month and then treated by pulpotomy
using CEM. Acceptable clinical/radiographic results were
achieved, including formation of a dentin bridge beneath
CEM and closure of the tooth apex.[81] Another case report
of a permanent molar with an open apex and signs of
irreversible pulpitis showed that complete pulpotomy
using CEM resulted in successful clinical outcomes of
pain relief and radiographic success including apical root
closure.[82] A randomized clinical trial study of permanent
molars with open apices which presented with extensive
caries and signs of reversible/irreversible pulpitis was
carried out on 51 subjects. Results of a follow-up after one
year[85] indicated that complete pulpotomy of the teeth
using MTA and CEM were 100% successful.[83]
Mature molars
A case report of a mature mandibular molar with irreversible
pulpitis and condensing apical periodontitis indicated that
two years after pulpotomy, acceptable clinical/radiographic
results such as formation of normal trabecular bone
structure around the root apices had occurred.[84] In a
Journal of Conservative Dentistry | Mar-Apr 2013 | Vol 16 | Issue 2
95
Asgary and Ahmadyar: VPT with CEM cement
case series study of 12 permanent mature molars with
irreversible pulpitis, CEM was used for pulpotomy, and
resulted in complete success at a follow-up after16 months.
It was also shown that to enable improved regeneration,
the pulp-dentin complex had isolated itself by forming a
calcified bridge.[45] In a multicenter randomized clinical trial
in 23 medical centers linked to five medical universities in
Iran, pulpotomy treatment of mature permanent molar
teeth with irreversible pulpitis using CEM and MTA were
examined. The results of this trial indicated that pulpotomy
treatment carried out by trained dentists can result in
successful control of pain[85] and high rates of clinical/
radiographic success (> 92%) during a follow-up after
oneyear.[86,87]
DPC WITH CEM CEMENT
Deciduous molars
There is controversy amongst pediatric dentists regarding
DPC treatment of human deciduous molars with CH;[88]
however, many investigations have found that postoperative
pulpal pathosis can be attributed not to the capping agent,
but to later microbial microleakage at the dentin/pulp
interface.[89] A recent randomized clinical trial study has
shown that CEM and MTA exhibit similar and acceptable
outcomes in DPC treatment of human deciduous molars.[90]
Permanent teeth
DPC is one of the best known clinical treatments available,
whereby connection between the exposed pulp and oral
cavity is eliminated using appropriate materials.[47] A case
report of a mature first mandibular molar with symptomatic
irreversible pulpitis/apical periodontitis demonstrated
favorable clinical/radiographic outcomes such as complete
resolution of the apical lesion at a follow-up after 15
months.[91] Recent DPC outcomes of prospective randomized
controlled/clinical trials carried out on 32 permanent teeth
that were orthodontically planned for extraction have
shown that under immunohistochemical examinations,
thickness of dentinal bridge beneath CEM was higher than
MTA at various time intervals; pulp inflammation was also
lower in the CEM groups.[92] In addition, expression of
fibronectin/tenascin in the CEM groups were higher than
the MTA groups during both time intervals; however, the
above differences were not statistically significant.[93]
IPC WITH CEM CEMENT
Permanent teeth
Currently, the concept of complete caries removal is being
challenged for permanent teeth. IPC decreases the risk of
pulp exposure, reduces the substrate for bacteria, prevents
lesion development and promotes a physiological reaction
in the pulp-dentin complex. Once cariogenic flora is isolated
from their nutritional supply by an effective coronal seal,
96
they perish/become inactive. An interesting case report
of IPC treatment with CEM of a mature symptomatic first
mandibular molar with irreversible pulpitis associated with
apical periodontitis demonstrated favorable clinical and
radiographic outcomes such as complete resolution of
symptoms and healing of the apical lesion at 15 months
follow-up. [94]
SUCCESS CRITERIA
The clinician can assess outcomes of the treatment
by compiling the information collected from clinical/
radiographic signs. Excluding low-level sensitivity and
short-term pain during the initial 1-2 weeks after VPT, lack/
relief of pain is one of the criteria for success.[53] In general,
increased bone density is not a sign of failure,[95] although
elimination of periapical lesions and a positive response to
electric/thermal pulp testing after VPT are signs of success
of the treatment.[87] Although the most accurate method
of assessment is by histological examination of the pulpdentin complex, it is apparent that this is only possible in
laboratory/animal studies and cases of extraction of the
human tooth.[40]
Prognosis
There is general consensus that in pulp exposure of
mature/immature permanent teeth, VPT by DPC/pulpotomy
(complete/incomplete) is an alternative treatment for
healthy uninflamed pulps (normal pulp or reversible
pulpitis).[96,97] Results of a number of recent histological
studies have shown that even in cases of irreversible pulpitis,
VPT using endodontic biomaterials has a satisfactory
success rate.[40,45,98] An interesting recent systematic review
revealed that the success rate of VPT was up to 99%; this
provides an important evidence that permanent teeth with
cariously exposed pulps can be successfully managed by
VPT.[47]
The success of VPT is based on the healing capacity of
the normal/inflamed dental pulp; it has been reported
that aging of the pulp reduces the chance of success.[99]
However, recent studies have revealed the weakness of
evidence regarding the effects of age and status of the root
apex on treatment outcomes of VPT.[47]
Placement of an adequate coronal seal is necessary for
ensuring success of most endodontic treatments.[10,30]
Prognosis of VPT is reasonably high if a bacteria-tight
coronal restoration is placed.[100]
Policy making
Based on the best current evidence[85-87], VPT treatment
of teeth by complete pulpotomy using CEM has been
introduced by the Iranian Ministry for Health and Medical
Education in public health-care centers; this has resulted in
Journal of Conservative Dentistry | Mar-Apr 2013 | Vol 16 | Issue 2
Asgary and Ahmadyar: VPT with CEM cement
saving many teeth which would otherwise be unnecessarily
extracted. Oral health-care policy makers have officially
announced that nearly2 million teeth are extracted
annually in public health-care centers in Iran. Therefore, it
is believed that by the generalization of this technique, it is
possible to save many of these teeth.
CONCLUSION
13.
14.
15.
16.
Results of epidemiological studies demonstrate that the
success rate of RCT is alarmingly low worldwide.
Maintenance of vitality of the pulp with the aim of extending
the lifespan of vital teeth is a proven concept.
17.
18.
19.
20.
Carrying out VPT (apexogenesis) in vital immature teeth
with open apices is an inevitable choice of treatment.
Carious pulp exposure/irreversible pulpitis can be treated
by VPT; therefore, carrying out VPT in mature/immature
permanent/primary vital teeth is a logical priority in
modern dentistry.
The highest level of current best evidence has revealed that
CEM cement is a suitable endodontic biomaterial for VPT
treatments of primary molars as well as mature/immature
permanent teeth with reversible/irreversible pulpitis.
2.
3.
4.
5.
6.
7.
8.
9.
10.
11.
12.
22.
23.
24.
25.
26.
27.
28.
REFERENCES
1.
21.
Boykin MJ, Gilbert GH, Tilashalski KR, Shelton BJ. Incidence of
endodontic treatment: A 48-month prospective study. J Endod
2003;29:806-9.
European Society of Endodontology. Quality guidelines for endodontic
treatment: Consensus report of the European Society of Endodontology.
Int Endod J 2006;39:921-30.
Kojima K, Inamoto K, Nagamatsu K, Hara A, Nakata K, Morita I, et al.
Success rate of endodontic treatment of teeth with vital and nonvital
pulps. A meta-analysis. Oral Surg Oral Med Oral Pathol Oral Radiol
Endod 2004;97:95-9.
Ng YL, Mann V, Gulabivala K. Tooth survival following non-surgical
root canal treatment: A systematic review of the literature. Int Endod J
2010;43:171-89.
Caplan DJ, Cai J, Yin G, White BA. Root canal filled versus non-root
canal filled teeth: A retrospective comparison of survival times. J Public
Health Dent 2005;65:90-6.
Eriksen H, Kirkevang L, Petersson K. Endodontic epidemiology and
treatment outcome: General considerations. Endod Topics 2002;2:1-9.
Jimnez-Pinzn A, Segura-Egea JJ, Poyato-Ferrera M, Velasco-Ortega E,
Ros-Santos JV. Prevalence of apical periodontitis and frequency of rootfilled teeth in an adult Spanish population. Int Endod J 2004;37:167-73.
Frisk F, Hugoson A, Hakeberg M. Technical quality of root fillings and
periapical status in root filled teeth in Jnkping, Sweden. Int Endod J
2008;41:958-68.
Marques MD, Moreira B, Eriksen HM. Prevalence of apical periodontitis
and results of endodontic treatment in an adult, Portuguese population.
Int Endod J 1998;31:161-5.
Asgary S, Shadman B, Ghalamkarpour Z, Shahravan A, Ghoddusi J,
Bagherpour A, et al. Periapical status and quality of root canal fillings and
coronal restorations in Iranian population. Iran Endod J 2010;5:74-82.
Siqueira JF Jr, Ras IN, Alves FR, Campos LC. Periradicular status
related to the quality of coronal restorations and root canal fillings in a
Brazilian population. Oral Surg Oral Med Oral Pathol Oral Radiol Endod
2005;100:369-74.
Sunay H, Tanalp J, Dikbas I, Bayirli G. Cross-sectional evaluation of
the periapical status and quality of root canal treatment in a selected
29.
30.
31.
32.
33.
34.
35.
36.
37.
38.
39.
40.
41.
42.
43.
44.
population of urban Turkish adults. Int Endod J 2007;40:139-45.
Kirkevang LL, rstavik D, Hrsted-Bindslev P, Wenzel A. Periapical
status and quality of root fillings and coronal restorations in a Danish
population. Int Endod J 2000;33:509-15.
Saunders WP, Saunders EM. Prevalence of periradicular periodontitis
associated with crowned teeth in an adult Scottish subpopulation. Br
Dent J 1998;185:137-40.
Dugas NN, Lawrence HP, Teplitsky PE, Pharoah MJ, Friedman S.
Periapical health and treatment quality assessment of root-filled teeth in
two Canadian populations. Int Endod J 2003;36:181-92.
Ng YL, Mann V, Gulabivala K. Outcome of secondary root canal treatment:
A systematic review of the literature. Int Endod J 2008;41:1026-46.
Kvist T, Reit C. Results of endodontic retreatment: A randomized
clinical study comparing surgical and nonsurgical procedures. J Endod
1999;25:814-7.
Kanli A, Kanbur NO, Dural S, Derman O. Effects of oral health behaviors
and socioeconomic factors on a group of Turkish adolescents.
Quintessence Int 2008;39:E26-32.
Gilbert GH, Duncan RP, Shelton BJ. Social determinants of tooth loss.
Health Serv Res 2003;38:1843-62.
Mjr IA, Sveen OB, Heyeraas KJ. Pulp-dentin biology in restorative
dentistry. Part 1: Normal structure and physiology. Quintessence Int
2001;32:427-46.
Linde A, Goldberg M. Dentinogenesis. Crit Rev Oral Biol Med 1993;4:679728.
Rosa V, Botero TM, Nr JE. Regenerative endodontics in light of the
stem cell paradigm. Int Dent J 2011;61 Suppl 1:23-8.
Ricketts D. Management of the deep carious lesion and the vital pulp
dentine complex. Br Dent J 2001;191:606-10.
Levin LG, Law AS, Holland GR, Abbott PV, Roda RS. Identify and define
all diagnostic terms for pulpal health and disease states. J Endod
2009;35:1645-57.
Garfunkel A, Sela J, Ulmansky M. Dental pulp pathosis. Clinicopathologic
correlations based on 109 cases. Oral Surg Oral Med Oral Pathol
1973;35:110-7.
Hyman JJ, Cohen ME. The predictive value of endodontic diagnostic
tests. Oral Surg Oral Med Oral Pathol 1984;58:343-6.
Zhang W, Yelick PC. Vital pulp therapy-current progress of dental pulp
regeneration and revascularization. Int J Dent 2010;2010:856087.
Goldberg M, Smith AJ. Cells and extracellular matrices of dentin and
pulp: Abiological basis for repair and tissue engineering. Crit Rev Oral
Biol Med 2004;15:13-27.
Ohshima H, Yoshida S. The relationship between odontoblasts and
pulp capillaries in the process of enamel-and cementum-related dentin
formation in rat incisors. Cell Tissue Res 1992;268:51-63.
Demarco FF, Rosa MS, Tarquinio SB, Piva E. Influence of the restoration
quality on the success of pulpotomy treatment: A preliminary
retrospective study. J Appl Oral Sci 2005;13:72-7.
Stanley HR. Pulp capping: Conserving the dental pulpcan it be done?
Is it worth it? Oral Surg Oral Med Oral Pathol 1989;68:628-39.
Hilton TJ. Keys to clinical success with pulp capping: A review of the
literature. Oper Dent 2009;34:615-25.
Mjr IA. Pulp-dentin biology in restorative dentistry. Part 7: The exposed
pulp. Quintessence Int 2002;33:113-35.
Cox CF, Bergenholtz G. Healing sequence in capped inflamed dental
pulps of Rhesus monkeys (Macaca mulatta). Int Endod J 1986;19:113-20.
Mjr IA, Tronstad L. The healing of experimentally induced pulpitis. Oral
Surg Oral Med Oral Pathol 1974;38:115-21.
Sbay RK, Suzuki S, Kaya H, Cox CF. Human pulp response after partial
pulpotomy with two calcium hydroxide products. Oral Surg Oral Med
Oral Pathol Oral Radiol Endod 1995;80:330-7.
Matsuo T, Nakanishi T, Shimizu H, Ebisu S. A clinical study of direct pulp
capping applied to carious-exposed pulps. J Endod 1996;22:551-6.
Witherspoon DE. Vital pulp therapy with new materials: New directions and
treatment perspectivespermanent teeth. Pediatr Dent 2008;30:220-4.
Kakehashi S, Stanley HR, Fitzgerald RJ. The effects of surgical exposures
of dental pulps in germ-free and conventional laboratory rats. Oral Surg
Oral Med Oral Pathol 1965;20:340-9.
Eghbal MJ, Asgary S, Baglue RA, Parirokh M, Ghoddusi J. MTA
pulpotomy of human permanent molars with irreversible pulpitis. Aust
Endod J 2009;35:4-8.
Modena KC, Casas-Apayco LC, Atta MT, Costa CA, Hebling J, Sipert
CR, et al. Cytotoxicity and biocompatibility of direct and indirect pulp
capping materials. J Appl Oral Sci 2009;17:544-54.
Hrsted P, El Attar K, Langeland K. Capping of monkey pulps with Dycal
and a Ca-eugenol cement. Oral Surg Oral Med Oral Pathol 1981;52:531-53.
Kokkas A, Goulas A, Stavrianos C, Anogianakis G. The role of cytokines
in pulp inflammation. J Biol Regul Homeost Agents 2011;25:303-11.
Tziafas D. Basic mechanisms of cytodifferentiation and dentinogenesis
Journal of Conservative Dentistry | Mar-Apr 2013 | Vol 16 | Issue 2
97
Asgary and Ahmadyar: VPT with CEM cement
45.
46.
47.
48.
49.
50.
51.
52.
53.
54.
55.
56.
57.
58.
59.
60.
61.
62.
63.
64.
65.
66.
67.
68.
69.
70.
71.
72.
73.
74.
98
during dental pulp repair. Int J Dev Biol 1995;39:281-90.
Asgary S, Ehsani S. Permanent molar pulpotomy with a new endodontic
cement: A case series. J Conserv Dent 2009;12:31-6.
Chai Y, Slavkin HC. Prospects for tooth regeneration in the 21stcentury:
A perspective. Microsc Res Tech 2003;60:469-79.
Aguilar P, Linsuwanont P. Vital pulp therapy in vital permanent teeth with
cariously exposed pulp: A systematic review. J Endod 2011;37:581-7.
Barrieshi-Nusair KM, Qudeimat MA. A prospective clinical study of
mineral trioxide aggregate for partial pulpotomy in cariously exposed
permanent teeth. J Endod 2006;32:731-5.
Asgary S, Ahmadyar M. Can miniature pulpotomy procedure improve
treatment outcomes of direct pulp capping? Med Hypotheses
2012;78:283-5.
JOE Editorial Board. Vital pulp therapy: An online study guide. J Endod
2008;34:E103-6.
Murdoch-Kinch CA, McLean ME. Minimally invasive dentistry. J Am Dent
Assoc 2003;134:87-95.
Fuks AB. Vital pulp therapy with new materials for primary teeth: New
directions and treatment perspectives. J Endod 2008;34:S18-24.
Mente J, Geletneky B, Ohle M, Koch MJ, Friedrich Ding PG, Wolff D, et
al. Mineral trioxide aggregate or calcium hydroxide direct pulp capping:
An analysis of the clinical treatment outcome. J Endod 2010;36:806-13.
Asgary S, Parirokh M, Eghbal MJ, Ghoddusi J, Eskandarizadeh A. SEM
evaluation of neodentinal bridging after direct pulp protection with
mineral trioxide aggregate. Aust Endod J 2006;32:26-30.
Fong CD, Davis MJ. Partial pulpotomy for immature permanent teeth, its
present and future. Pediatr Dent 2002;24:29-32.
Asgary S, Shahabi S, Jafarzadeh T, Amini S, Kheirieh S. The properties
of a new endodontic material. J Endod 2008;34:990-3.
Asgary S, Eghbal MJ, Parirokh M, Ghoddusi J, Kheirieh S, Brink F.
Comparison of mineral trioxide aggregate's composition with Portland
cements and a new endodontic cement. J Endod 2009;35:243-50.
Costa CA, Hebling J, Hanks CT. Current status of pulp capping with
dentin adhesive systems: A review. Dent Mater 2000;16:188-97.
Mohammadi Z, Dummer PM. Properties and applications of calcium
hydroxide in endodontics and dental traumatology. Int Endod J
2011;44:697-730.
Asgary S, Eghbal MJ, Parirokh M. Sealing ability of a novel endodontic
cement as a root-end filling material. J Biomed Mater Res A 2008;87:706-9.
Ghorbani Z, Kheirieh S, Shadman B, Eghbal M, Asgary S. Microleakage
of CEM cement in two different media. Iran Endod J 2008;4:87-90.
Soheilipour E, Kheirieh S, Madani M, Akbarzadeh Baghban A, Asgary S.
Particle size of a new endodontic cement compared to Root MTA and
calcium hydroxide. Iran Endod J 2009;4:112-6.
Asgary S, Eghbal MJ, Parirokh M, Ghoddusi J. Effect of two storage
solutions on surface topography of two root-end fillings. Aust Endod J
2009;35:147-52.
Asgary S, Eghbal MJ, Ehsani S. Periradicular regeneration after
endodontic surgery with calcium-enriched mixture cement in dogs. J
Endod 2010;36:837-41.
Nosrat A, Seifi A, Asgary S. Regenerative endodontic treatment
(revascularization) for necrotic immature permanent molars: A review
and report of two cases with a new biomaterial. J Endod 2011;37:562-7.
Hasan Zarrabi M, Javidi M, Naderinasab M, Gharechahi M. Comparative
evaluation of antimicrobial activity of three cements: New endodontic
cement (NEC), mineral trioxide aggregate (MTA) and Portland. J Oral
Sci 2009;51:437-42.
Asgary S, Kamrani FA. Antibacterial effects of five different root canal
sealing materials. J Oral Sci 2008;50:469-74.
Kangarlou A, Sofiabadi S, Yadegari Z, Asgary S. Antifungal effect of
Calcium Enriched Mixture (CEM) cement against Candida Albicans. Iran
Endod J 2009;4:101-5.
Asgary S, Eghbal MJ, Parirokh M, Ghanavati F, Rahimi H. A comparative
study of histologic response to different pulp capping materials and a
novel endodontic cement. Oral Surg Oral Med Oral Pathol Oral Radiol
Endod 2008;106:609-14.
Tabarsi B, Parirokh M, Eghbal MJ, Haghdoost AA, Torabzadeh H, Asgary
S. A comparative study of dental pulp response to several pulpotomy
agents. Int Endod J 2010;43:565-71.
Ghoddusi J, Tavakkol Afshari J, Donyavi Z, Brook A, Disfani R,
Esmaeelzadeh M. Cytotoxic effect of a new endodontic cement and mineral
trioxide aggregate on L929 line culture. Iran Endod J 2008;3:17-23.
Asgary S, Moosavi SH, Yadegari Z, Shahriari S. Cytotoxic effect of MTA
and CEM cement in human gingival fibroblast cells. Scanning electronic
microscope evaluation. N Y State Dent J 2012;78:51-4.
Mozayeni M, Salem Milani A, Alim Marvasti L, Asgary S. Cytotoxicity of
new ceramic enriched mixture (CEM) compared with MTA and IRM. Aust
Endod J 2012;38:70-5.
Parirokh M, Mirsoltani B, Raoof M, Tabrizchi H, Haghdoost AA.
Comparative study of subcutaneous tissue responses to a novel rootend filling material and white and grey mineral trioxide aggregate. Int
Endod J 2011;44:283-9.
75. Available from: http://ebd.ada.org/About.aspx. [Last accessed on 2012
Apr 1]
76. Torabinejad M, Bahjri K. Essential elements of evidenced-based
endodontics: Steps involved in conducting clinical research. J Endod
2005;31:563-9.
77. Camp JH. Overviews of pediatric-endodontics. Alpha Omegan
1991;84:26-7.
78. Malekafzali B, Shekarchi F, Asgary S. Treatment outcomes of pulpotomy
in primary molars using two endodontic biomaterials. A 2-year
randomised clinical trial. Eur J Paediatr Dent 2011;12:189-93.
79. Kontham UR, Tiku AM, Damle SG, Kalaskar RR. Apexogenesis of a
symptomatic mandibular first permanent molar with calcium hydroxide
pulpotomy. Quintessence Int 2005;36:653-7.
80. Bishop BG, Woollard GW. Modern endodontic therapy for an
incompletely developed tooth. Gen Dent 2002;50:252-6; quiz 257-8.
81. Nosrat A, Asgary S. Apexogenesis treatment with a new endodontic
cement: A case report. J Endod 2010;36:912-4.
82. Nosrat A, Asgary S. Apexogenesis of a symptomatic molar with calcium
enriched mixture. Int Endod J 2010;43:940-4.
83. Nosrat A, Seifi A, Asgary S. Pulpotomy in caries-exposed immature
permanent molars using calcium-enriched mixture cement or mineral
trioxide aggregate: A randomized clinical trial. Int J Paediatr Dent 2012.
84. Asgary S. Calcium-enriched mixture pulpotomy of a human permanent
molar with irreversible pulpitis and condensing apical periodontitis. J
Conserv Dent 2011;14:90-3.
85. Asgary S, Eghbal MJ. The effect of pulpotomy using a calcium-enriched
mixture cement versus one-visit root canal therapy on postoperative
pain relief in irreversible pulpitis: A randomized clinical trial. Odontology
2010;98:126-33.
86. Asgary S, Eghbal M, Ghoddusi J, Yazdani S. One-year results of vital
pulp therapy in permanent molars with irreversible pulpitis: An ongoing
multicenter, randomized, non-inferiority clinical trial. Clin Oral Investig
2012.
87. Asgary S, Eghbal MJ. Treatment outcomes of pulpotomy in permanent
molars with irreversible pulpitis using biomaterials: A multi-center
randomized controlled trial. Acta Odontol Scand 2012.
88. Kopel HM. Considerations for the direct pulp capping procedure in
primary teeth: A review of the literature. ASDC J Dent Child 1992;59:141-9.
89. Kopel HM. The pulp capping procedure in primary teeth "revisited".
ASDC J Dent Child 1997;64:327-33.
90. Fallahinejad Ghajari M, Asgharian Jeddi T, Iri S, Asgary S. Direct
pulp-capping with calcium enriched mixture in primary molar teeth: A
randomized clinical trial. Iran Endod J 2010;1:1-4.
91. Asgary S, Homayounfar N. Periapical Healing After Direct Pulp Capping
With Calcium-Enriched Mixture Cement: A Case Report. Oper Dent
2012.
92. Zarrabi MH, Javidi M, Jafarian AH, Joushan B. Histologic assessment of
human pulp response to capping with mineral trioxide aggregate and a
novel endodontic cement. J Endod 2010;36:1778-81.
93. Zarrabi MH, Javidi M, Jafarian AH, Joushan B. Immunohistochemical
expression of fibronectin and tenascin in human tooth pulp capped with
mineral trioxide aggregate and a novel endodontic cement. J Endod
2011;37:1613-8.
94. Torabzadeh H, Asgary S. Indirect pulp therapy in a symptomatic mature
molar using CEM cement. J Conserv Dent 2012;16:83-6.
95. Hrsted-Bindslev P, Lvschall H. Treatment outcome of vital pulp
treatment. Endod Topics 2002;2:24-34.
96. Dumsha T, Hovland E. Considerations and treatment of direct and
indirect pulp-capping. Dent Clin North Am 1985;29:251-9.
97. Cvek M, Lundberg M. Histological appearance of pulps after exposure
by a crown fracture, partial pulpotomy, and clinical diagnosis of healing.
J Endod 1983;9:8-11.
98. Chueh LH, Chiang CP. Histology of Irreversible pulpitis premolars treated
with mineral trioxide aggregate pulpotomy. Oper Dent 2010;35:370-4.
99. Cohen S, Hargreaves K, editors. Pathway of the Pulp. 9thed.St. Louis:
CV Mosby; 2006.
100. Trope M, McDougal R, Levin L, May KN Jr, Swift EJ Jr. Capping the
inflamed pulp under different clinical conditions. J Esthet Restor Dent
2002;14:349-57.
How to cite this article: Asgary S, Ahmadyar M. Vital pulp
therapy using calcium-enriched mixture: An evidence-based
review. J Conserv Dent 2013;16:92-8.
Source of Support: Nil, Conflict of Interest: None declared.
Journal of Conservative Dentistry | Mar-Apr 2013 | Vol 16 | Issue 2
Anda mungkin juga menyukai
- Apert N CrouzonDokumen13 halamanApert N CrouzonfayasyabminBelum ada peringkat
- Contoh Kasus AutisDokumen3 halamanContoh Kasus AutisfayasyabminBelum ada peringkat
- Oral ScrerenDokumen9 halamanOral Screrenfayasyabmin100% (1)
- The Individually Prepared Transpalatal Arch (TPA) : Valentin Moutaftchiev, Alexander MoutaftchievDokumen4 halamanThe Individually Prepared Transpalatal Arch (TPA) : Valentin Moutaftchiev, Alexander MoutaftchievfayasyabminBelum ada peringkat
- Sag 34 1 10 0309 11 PDFDokumen8 halamanSag 34 1 10 0309 11 PDFfayasyabminBelum ada peringkat
- Sag 34 1 10 0309 11 PDFDokumen8 halamanSag 34 1 10 0309 11 PDFfayasyabminBelum ada peringkat
- The Yellow House: A Memoir (2019 National Book Award Winner)Dari EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Penilaian: 4 dari 5 bintang4/5 (98)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDari EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifePenilaian: 4 dari 5 bintang4/5 (5795)
- Shoe Dog: A Memoir by the Creator of NikeDari EverandShoe Dog: A Memoir by the Creator of NikePenilaian: 4.5 dari 5 bintang4.5/5 (537)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDari EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FuturePenilaian: 4.5 dari 5 bintang4.5/5 (474)
- Grit: The Power of Passion and PerseveranceDari EverandGrit: The Power of Passion and PerseverancePenilaian: 4 dari 5 bintang4/5 (588)
- On Fire: The (Burning) Case for a Green New DealDari EverandOn Fire: The (Burning) Case for a Green New DealPenilaian: 4 dari 5 bintang4/5 (74)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDari EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryPenilaian: 3.5 dari 5 bintang3.5/5 (231)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDari EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RacePenilaian: 4 dari 5 bintang4/5 (895)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDari EverandNever Split the Difference: Negotiating As If Your Life Depended On ItPenilaian: 4.5 dari 5 bintang4.5/5 (838)
- The Little Book of Hygge: Danish Secrets to Happy LivingDari EverandThe Little Book of Hygge: Danish Secrets to Happy LivingPenilaian: 3.5 dari 5 bintang3.5/5 (400)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDari EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersPenilaian: 4.5 dari 5 bintang4.5/5 (345)
- The Unwinding: An Inner History of the New AmericaDari EverandThe Unwinding: An Inner History of the New AmericaPenilaian: 4 dari 5 bintang4/5 (45)
- Team of Rivals: The Political Genius of Abraham LincolnDari EverandTeam of Rivals: The Political Genius of Abraham LincolnPenilaian: 4.5 dari 5 bintang4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDari EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyPenilaian: 3.5 dari 5 bintang3.5/5 (2259)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDari EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaPenilaian: 4.5 dari 5 bintang4.5/5 (266)
- The Emperor of All Maladies: A Biography of CancerDari EverandThe Emperor of All Maladies: A Biography of CancerPenilaian: 4.5 dari 5 bintang4.5/5 (271)
- Rise of ISIS: A Threat We Can't IgnoreDari EverandRise of ISIS: A Threat We Can't IgnorePenilaian: 3.5 dari 5 bintang3.5/5 (137)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDari EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You ArePenilaian: 4 dari 5 bintang4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Dari EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Penilaian: 4.5 dari 5 bintang4.5/5 (121)
- Her Body and Other Parties: StoriesDari EverandHer Body and Other Parties: StoriesPenilaian: 4 dari 5 bintang4/5 (821)
- Uprighting of Lower MolarsDokumen10 halamanUprighting of Lower Molarssolodont1Belum ada peringkat
- NDS Study Club Brochure v4Dokumen9 halamanNDS Study Club Brochure v4Hamed KarimiBelum ada peringkat
- Booklet - e 1 - 2013Dokumen101 halamanBooklet - e 1 - 2013Dani AedoBelum ada peringkat
- s41415 023 5624 0 LibreDokumen6 halamans41415 023 5624 0 LibreAZWATEE BINTI ABDUL AZIZBelum ada peringkat
- Coricama c17 en CatalogueDokumen232 halamanCoricama c17 en CatalogueBernythefly axcBelum ada peringkat
- Da Costa 2013, A Meta Analysis of The Most Indicated Preparation Design For Porcelain Laminate VeneersDokumen7 halamanDa Costa 2013, A Meta Analysis of The Most Indicated Preparation Design For Porcelain Laminate VeneersAaron MarroBelum ada peringkat
- A Retrospective Comparison of Two Protocols For Correction of Skeletal Class III Malocclusion in Prepubertal ChildrenDokumen11 halamanA Retrospective Comparison of Two Protocols For Correction of Skeletal Class III Malocclusion in Prepubertal ChildrenMariana SantosBelum ada peringkat
- Pitts Et Al 2019 Early Childhood Caries IAPD Bangkok Declaration. IJPDDokumen3 halamanPitts Et Al 2019 Early Childhood Caries IAPD Bangkok Declaration. IJPDThaliaBelum ada peringkat
- A Survey On Oral Health Attitude, Awareness and Behaviour of Dental StudentsDokumen5 halamanA Survey On Oral Health Attitude, Awareness and Behaviour of Dental StudentsazizahBelum ada peringkat
- The Coronally Advanced Flap in Combination With Platelet-Rich Fibrin (PRF) and Enamel Matrix Derivative in The Treatment of Gingival Recession: A Comparative StudyDokumen15 halamanThe Coronally Advanced Flap in Combination With Platelet-Rich Fibrin (PRF) and Enamel Matrix Derivative in The Treatment of Gingival Recession: A Comparative StudyAnsh Veer ChouhanBelum ada peringkat
- Gingivitis Vs PeriodontitisDokumen2 halamanGingivitis Vs Periodontitisandreas kevinBelum ada peringkat
- Facebow Tech Spec Gen LRDokumen1 halamanFacebow Tech Spec Gen LRrojBelum ada peringkat
- Andrews, Will - Scientific Treatment Goals For Oral and Facial HarmonyDokumen7 halamanAndrews, Will - Scientific Treatment Goals For Oral and Facial Harmonykarol yanacBelum ada peringkat
- New Microsoft Office Word DocumentDokumen3 halamanNew Microsoft Office Word DocumentAtulsanapBelum ada peringkat
- Effect of Lip Bumpers On MandibularDokumen4 halamanEffect of Lip Bumpers On MandibularMaria SilvaBelum ada peringkat
- Upto HistoryDokumen70 halamanUpto HistoryAnil Sukumaran33% (3)
- Tsoukaki 2012Dokumen8 halamanTsoukaki 2012Marina JoelBelum ada peringkat
- Davidovitch1995 PDFDokumen6 halamanDavidovitch1995 PDFRahulLife'sBelum ada peringkat
- The Evaluation of The Nasolabial Angle in Iraqi Subject With Class I, II and III Skeletal Relationship (Comparative Study)Dokumen5 halamanThe Evaluation of The Nasolabial Angle in Iraqi Subject With Class I, II and III Skeletal Relationship (Comparative Study)Rebin AliBelum ada peringkat
- Lec 8 3rd Class PDFDokumen4 halamanLec 8 3rd Class PDFBrandon AviciiBelum ada peringkat
- RPD M C Q With AnswersDokumen23 halamanRPD M C Q With Answersيارا حسين81% (16)
- Orthodontic Treatment: Patient Information LeafletDokumen2 halamanOrthodontic Treatment: Patient Information LeafletRakan KhtoomBelum ada peringkat
- Efektivitas Pasta Gigi Herbal Dan Non-Herbal Terhadap Penurunan Plak Gigi Anak Usia 12-14 TahunDokumen7 halamanEfektivitas Pasta Gigi Herbal Dan Non-Herbal Terhadap Penurunan Plak Gigi Anak Usia 12-14 Tahunfadhilah nurBelum ada peringkat
- Dentaltrauma: Lewis C. JonesDokumen8 halamanDentaltrauma: Lewis C. JonesHusni mubarakBelum ada peringkat
- Managing Geriatric PatientsDokumen8 halamanManaging Geriatric PatientsSarah KahilBelum ada peringkat
- Surveyors &surveying Inrpd: Presented By: Annesha K. Konwar Mds Ii ND YearDokumen82 halamanSurveyors &surveying Inrpd: Presented By: Annesha K. Konwar Mds Ii ND YearArchita KureelBelum ada peringkat
- Class 7 Work Book Answers Page 16Dokumen2 halamanClass 7 Work Book Answers Page 16Gaurav SethiBelum ada peringkat
- Cavity PrepDokumen10 halamanCavity PrepShruti GolaiBelum ada peringkat
- Ferrari Et Al 2017 JDentDokumen29 halamanFerrari Et Al 2017 JDentAli Al-QaysiBelum ada peringkat
- MOH Exam Paper C PDFDokumen7 halamanMOH Exam Paper C PDFmidhun0% (1)