PHG
Diunggah oleh
Aulia Maghfira Kusuma WardhaniHak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
PHG
Diunggah oleh
Aulia Maghfira Kusuma WardhaniHak Cipta:
Format Tersedia
Journal of Dental Herald
Journal of Dental Herald
www.dherald.in
(January 2015) Issue:1, Vol.:2
E ISSN No. : 2348 1331
P ISSN No. : 2348 134X
Case Report
Primary Herpetic Gingivostomatitis - Detailed Review And Report Of A Case
Cheranjeevi Jayam1, Anila Bandlapalli2, Kapil Rajiv Sharma3, Deepak Chauhan4
1
Lecturer, Department of Pedodontics,Himachal Pradesh Government Dental College, Shimla, Himachal Pradesh.
Senior Lecturer, Department of Conservative Dentistry & Endodontics,Himachal College of Dental Sciences, Himachal Pradesh.
3
Professor & H.O.D, Himachal Pradesh Government Dental College, Shimla, Himachal Pradesh.
4
Lecturer, Department of Pedodontics,Himachal Pradesh Government Dental College, Shimla, Himachal Pradesh.
2
Abstract
Primary Herpetic Gingivostomatitis(PHG) is a common infection of oral mucosa in children due to viral origin. PHG is accompanied with several
prodromal symptoms like fever, anorexia, irritability, malaise and headache. Intraorally there is severe stomatitis (inflammation of oral mucosa),
presence of several pin point vesicles that rupture to give raise to ulcers.Several oral conditions occur commonly that resemble PHG leading to
wrong diagnosis of the condition. Improper diagnosis can lead to improper treatment planning in children.The authors propose a treatment
algorithm for management of PHG.
Key Words
Primary Herpetic Gingivostomatitis, HSV 1, teething, acyclovir.
Introduction
Primary Herpetic Gingivostomatitis (PHG) is a common
infection of oral mucosa in children due to viral origin. It is
referred to as primary because the oral manifestation of disease
commonly occursduring the 1stepisode of Herpes simplex
virus (Herpes hominis virus, type I and II, with type I more
common). Other terms used to describe this condition is canker
sores.[1] About 1% of primary care consultations are for cold
sores. In US, 57.7% of population is infected with HSV-1.[2]
Worldwide, the rate of infection is over 85% after levels of
passively acquired maternal antibodies have diminished;
infants and young children are at increased risk for acquiring
infections.
After an incubation period of 3-7 days, the symptoms of the
disease start to appear. Virus enters epithelial lining of oral
mucosa and starts to replicate. Further these epithelial cells full
of virions breakdown pouring out their contents. Now newly
formed virions are free to invade neighbouring cells or
transmit to new sites or infect other people.[3] PHG is
accompanied with several prodromal symptoms like fever,
anorexia, irritability, malaise and headache. Intraorally there is
severe stomatitis (inflammation of oral mucosa), presence of
several pin point vesicles that rupture to give raise to ulcers.
These ulcers are usually covered by a yellow-grey membrane,
several in number, pinpoint in size. There is presence of linear
gingival erythema of gums, coated tongue, presence of plaque
due to ensuing improper oral hygiene and halitosis. Other
findings include halitosis, drooling saliva and refusal to drink
are usual concomitant findings.[4]
Quick Response Code
Case Report
A 2 year old child was accompanied by parents to the clinic.
The accompanying mother complained of inability/refusal of
the child to consume food from past 3 days. On general
examination, the child appeared to be malnourished. Weight
and height of the child did not coincide with Indian Standard
height-weight charts. The child was lethargic, irritated and not
oriented (must have occurred due absence of food intake from
past 3 days), severe halitosis (must have occurred due to lack of
oral hygiene), and pyrexia. Intraoral examination revealed
severe gingivitis (marginal, papillary and attached gingiva)
with linear marginal erythema characteristic of the disease
(Figure 1). Other regions of the mouth especially the upper
and lower lip was also erythematous with multiple ulcers
(Figure 2). The tongue showed peculiar strawberry
appearance (may be due to malnutrition and ensuing vitamin
deficiency) with several coalesced areas of depapillation and
ulcers (Figure 3). There was presence of pinpoint multiple
ulcerations in the gingiva and buccal mucosa also (Figure 4).
The ulcer was covered with grey-yellow membrane and
surrounded by a small area of inflammation. Palpation of the
small ulcers and surrounding region was painful.
Address For Correspondence:
Dr Cheranjeevi Jayam, Lecturer,
Department of Pedodontics,
Himachal Pradesh Government Dental College,
Shimla,
Himachal Pradesh.
Email:cheranjeevij@gmail.com,
chiru_jayam@rediffmail.com
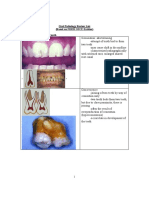
Figure 1 - Linear Gingival Erythema With Acute Gingivitis Which Are Pathognomonic Of
Herpetic Gingivostomatitis.
Journal of Dental Herald (January 2015 Issue:1, Vol.:2).
011
isolation of child from other children were also ascertained.
Proper oral hygiene maintenance by gentle brushing and;
warm and salt water rinses 4-5 times daily was advised.
Nutritional guidelines were given taking care of daily caloric
intake as well as instructions regarding abstinence from spicy
and sour food.
Figure 2 - Erythematous Lips With Multiple Pin Point Ulcers.
Figure 3 - Strawberry Appearance Of Tongue With Several Coalesced Areas Of Depapillation
And Ulcers.
Figure 4 - Pinpoint Multiple Ulcerations In The Gingiva And Buccal Mucosa.
Diagnosis
Based on history, symptoms, and signs - a diagnosis of Primary
herpetic gingivostomatitis was ascertained.
Treatment
The patient was hospitalised immediately to treat for severe
dehydration immediately. Prescription of acyclovir to treat
infection, paracetamol to treat pyrexia was done. Topical
application of glycerine to oral mucosa was advised to
alleviate painful ulcers. Mother was instructed regarding care
of patient and hygiene practices to decrease the chances of
spread of infection to mother as well. Instructions regarding
Journal of Dental Herald (January 2015 Issue:1, Vol.:2).
Discussion
Herpetic gingivostomatitis is a highly contagious disease of
children. The general course is 10-14 days, although it is a selflimiting disease; it can cause several complications in children
and especially individuals with weak immunity. Viral
shedding can occur up to 60 hours after the onset of
symptoms.[5] Exchange of oral secretions can lead to
transmission of organisms from a child to other children.
Sharing of cups, baby bottles, nipples, spoons, plates, teething
toys or even mouth touching or kissing can easily lead to
spread of infection. All this accounts to higher infectious rate
of HSV among children. Reactivation of the dormant virus can
occur, often precipitated by factors such as sun exposure,
s t r e s s , i l l n e s s , m e n s e s , f e v e r, o r i m m u n e
suppression.Especially it is common to see sudden epidemics
in schools or day care centres. There are several complications
of untreated herpes virus-, viz Simplex keratitis- Constant touching of lesions and eye
can relocate organisms from oral cavity to eyes. It is
characterised by conjunctivitis, uveitis, (red eyes, watering
eyes), callousness to light and in severe cases can lead to
blindness. [6]
Genital lesions- Characterised by presence of painful
ulcers on genitals. HSV-1 can also be transferred to the
genitals through oral sex when mouth sores are present,
causing genital sores.
Herpes Zoster-Virus involving trigeminal neuralgia can
lead to neuralgias.
Bell's palsy- Bell's palsy is paralysis of facial muscles
affecting facial nerve.
Recurrent infections can lead to herpes labialis.[7]
Recurrent lesions at same site may sometimes alsoleads to
atrophy and scarring.
Secondary bacterial infection like impetigo may also
occur.
Several oral conditions occur commonly that resemble PHG
leading to wrong diagnosis of the condition. Improper
diagnosis can lead to improper treatment planning. The
conditions that mimic PHG are1. Teething- Teething is a common condition that occurs
during childhood. Symptoms of teething are similar to
PHG such as inability to eat, fever, irritation, lethargy.
Also, a milder form of PHG occurs when there is presence
of residual maternal antibodies leading to wrong diagnosis;
hence dismissed as teething problem because of absence of
classical signs of PHG in such cases.[8]
2. Aphthous stomatitis- Can be differentiated by presence of
lesions only in non-keratinizsed mucosa. There is no
history of vesicles and no prodromal symptoms.[9]
3. Herpangina- caused by Coxsackie A virus. This condition
is differentiated by presence of ulcers in soft palate and
anterior pillar of the mouth.[10]
4. Chickenpox- Caused by Varicella zoster. Presence of
vesicular rash mainly on head and body.
012
Table 1- Authors Propose A New Treatment Algorithm For Management Of Phg
1.
Maintenance of hydration levels.
2.
Treatment of infection.
3.
Treatment of other symptoms.
4.
Maintenance of oral hygiene.
5.
Maintenance of proper nutrition.
6.
Prevention of spread to health care worker.
7.
Prevention of spread to care giver.
8.
Prevention of spread to other children.
4.
5. Chronic elemental mercury poisoning- Characterised by
severe inflammation of gums and oral mucosa. It is
differentiated by presence of additional neurological
problems like tremors, paraesthesia and psychiatric
problems like forgetfulness & mood disturbances.
6. Hand, foot, and mouth disease- Caused by Coxsackie viral
disease. This is differentiated by presence intra-oral and
extra-oral vesicles over other parts of body.
7. Stevens-Johnson Syndrome/ Erythema multiformeDifferentiated by presence of bothintra & oral lesions.
8. Impetigo.
Laboratory Investigations
Commonly used investigations are full blood count, culture
testsand serological tests.
1. In addition to the clinical picture associated with PHGS, a
complete blood count may reveal leucocytosis or
neutropenia associated with viral infections.
2. Culture of herpes simplex virus Isolation of the HSV-1
virus can be done using cell culture techniques.
Commercial kits are available. Careful swabbing of lesions
can be done with careful effort not to invoke trauma on
painful lesions.
3. Serology assaysAn indirect immunofluorescence
antibody test can be performed. newer fluorescent staining
or monoclonal antibodies can be performed.
4. Immunoassay techniques such as enzyme immunoassay
(EIA) or (ELISA) can identify viral DNA.
5. Rapid detection based on polymerase chain reaction (PCR)
is available when required (e.g., immunocompromised
patients, severe infection).[5]
6. Nucleic acid probes.
5.
6.
7.
8.
hours) can be given to children at home for mild to
moderate pain. Viscous lidocaine (2%) can be prescribed
for topical application using a Q-tip, providing a local
anaesthetic lasting approximately 10-15 minutes. Overthe-counter topical anaesthetics in gel form contain 20%
benzocaine and may be helpful for those with a minimal
number of lesions. Glyoxide, a topical preparation
available over the counter, contains glycerine and
peroxide. It is soothing to the mucous membranes. Aspirin
is not used since this is a known viral infection.
Maintenance of proper Nutrition- Counselling regarding
nutrition and maintenance of healthy diet is advised.
Offering soft and cold foods like ice cream& non-citrus
juices can be beneficial. However, the child is asked to
refrain from spicy and sour foods that can cause irritation
of ulcers. Infants should be breast fed or formula fed as
normal to maintain sufficient calories.
Maintenance of oral hygiene- Emphasis is given on oral
hygiene; although it is difficult to brush teeth, mechanical
plaque removal by gentle tooth brushing is advised
augmented with chemical plaque control (salt & warm
water rinse; chemical mouthwashes are not advised
because of fear of ingestion in children and irritation).
Absence of maintaining good oral hygiene can lead to
worsening of symptoms. If there is presence of space
maintainers or other appliances in mouth, cleaning of them
should be emphasized.
Prevention of spread to care giver- Give advice to reduce
the risk of transmission to caregiver. To avoid the HSV-1
virus avoid kissing or touching the face of an infected
individual. Cleaning of hands after contact with oral fluids
of affected child should be done. Proper general hygiene
has to be maintained.[13,14]
Prevention of spread to health care worker- Herpetic
whitlow is infection of limbs. Before the introduction of
universal precautions and the widespread use of gloves,
health care providers like physicians, dentists, nurses and
attendants were at risk of contracting HSV. Proper aseptic
precautions and barrier techniques should be utilized like
use of isolation rooms; hand washing, disposable gloves
and clothing must be emphasized.
Supportive nursing care for pain and fever are part of the
management process.
Treatment
The authors propose a treatment algorithm for management of
PHG (Table 1).
Nonpharmacologic comfort measures may include ageappropriate distraction techniques, cutaneous stimulation, and
the presence of significant caregivers to hold or rock children.
1. Maintenance of hydration levels - Depending upon level of
dehydration, child is fed orally by mixing one-half
teaspoon of salt in one cup of water. If the child refuses to
drink, they have to be admitted to hospital for rehydration.
2. Treatment of infection-Acyclovir interferes with DNA
synthesis, thereby inhibiting viral replication. Acyclovir 15
mg/kg five times a day for seven days. Usual modes of
dispensing is suspension- 200 mg/5 ml for young
children,5% acyclovir lotions, IV dosage of acyclovir is
250 mg/m2 every 8 hours are also available.Side effects of
acyclovir may include anorexia , nausea, vomiting and
diarrhoea, hypersensitivity and nephrotoxicity.[11, 12]
3. Treatment of other symptoms-Acetaminophen (10-15
mg/kg every 4 hours) or ibuprofen (10 mg/kg every 6
References
1. Kolokotronis A, Doumas S. Herpes simplex virus
infection, with particular reference to the progression and
complications of primaryherpetic gingivostomatitis. Clin
Microbiol Infect. 2006 Mar;12(3):202-11.
2. Xu F, Sternberg MR, Kottiri BJ, et al. Trends in herpes
simplex virus type 1 and type 2 seroprevalence in the
United States. JAMA. 2006 Aug 23;296(8):964-73.
3. Arduino PG, Porter SR. Herpes Simplex Virus Type 1
infection: overview on relevant clinico-pathological
features.J Oral Pathol Med. 2008 Feb;37(2):107-21.
4. Chandrasekar PH. Identification and treatment of herpes
lesions. Adv Wound Care. 1999 Jun;12(5):254-62.
5. Vogel JL, Kristie TM; The dynamics of HCF-1 modulation
Journal of Dental Herald (January 2015 Issue:1, Vol.:2).
013
of herpes simplex virus chromatin during initiation of
infection. Viruses. 2013 May 22;5(5):1272-91.
6. Mohan RP, Verma S, Singh U, et al. Acute primary herpetic
gingivostomatitis. BMJ Case Rep. 2013 Jul 8;2013.
7. Cunningham A, Griffiths P, Leone P, et al. Current
management and recommendations for access to antiviral
therapy of herpes labialis. J Clin Virol. 2012 Jan;53(1):611.
8. David L. King, William Steinhauer, Franklin GarciaGodoy, et al. Pediatric dentistry march/April, 1992 volume
14, number 2. p84.
9. Fatahzadeh M. Recurrent oral herpes:diagnosis
&management. J N JDent Assoc.2012;83(4):24-6.
10. Parrott, Rh; Wolf, Si, Nudelman, J, et al (August 1954).
"Clinical and laboratory differentiation between
herpangina and infectious (herpetic) gingivostomatitis.".
Pediatrics 14 (2): 1229.
11. Opstelten W, Neven AK, Eekhof J. Treatment and
prevention of herpes labialis. Can Fam Physician. 2008
Dec;54(12):1683-7.
12. Rahimi H, Mara T, Costella J, et al; Effectiveness of
antiviral agents for the prevention of recurrent herpes
labialis: a systematic review and meta-analysis. Oral Surg
Oral Med Oral Pathol Oral Radiol. 2012 May;113(5):61827.
13. Noonan V, Lerman MA, Woo SB, et al. Acute primary
herpetic gingivostomatitis. J Mass Dent Soc.
2014;63(2):51.
14. Stoopler ET, Balasubramaniam R. Topical and systemic
therapies for oral and perioral herpes simplex virus
infections. J Calif Dent Assoc. 2013 Apr;41(4):259-62.
Source of Support : Nill, Conflict of Interest : None declared
Journal of Dental Herald (January 2015 Issue:1, Vol.:2).
014
Anda mungkin juga menyukai
- Channel TV RumahDokumen1 halamanChannel TV RumahAulia Maghfira Kusuma WardhaniBelum ada peringkat
- Dentj 38 3 07Dokumen5 halamanDentj 38 3 07vil66Belum ada peringkat
- Dental JournalDokumen6 halamanDental JournalAulia Maghfira Kusuma WardhaniBelum ada peringkat
- Avoiding and Managing The Failure of Conventional Crowns and BridgesDokumen6 halamanAvoiding and Managing The Failure of Conventional Crowns and BridgesAulia Maghfira Kusuma WardhaniBelum ada peringkat
- Dental JournalDokumen6 halamanDental JournalAulia Maghfira Kusuma WardhaniBelum ada peringkat
- HttpsDokumen1 halamanHttpsAulia Maghfira Kusuma WardhaniBelum ada peringkat
- Dental JournalDokumen6 halamanDental JournalAulia Maghfira Kusuma WardhaniBelum ada peringkat
- Atrofi MukosaDokumen59 halamanAtrofi MukosaFaiza LailiyahBelum ada peringkat
- Iki LoDokumen10 halamanIki LoAulia Maghfira Kusuma WardhaniBelum ada peringkat
- PHGDokumen4 halamanPHGAulia Maghfira Kusuma WardhaniBelum ada peringkat
- Pit & Fisur Sealant GuideDokumen40 halamanPit & Fisur Sealant GuideDianita Rahma100% (1)
- WiresDokumen24 halamanWiresAulia Maghfira Kusuma WardhaniBelum ada peringkat
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDari EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifePenilaian: 4 dari 5 bintang4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingDari EverandThe Little Book of Hygge: Danish Secrets to Happy LivingPenilaian: 3.5 dari 5 bintang3.5/5 (399)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDari EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryPenilaian: 3.5 dari 5 bintang3.5/5 (231)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDari EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RacePenilaian: 4 dari 5 bintang4/5 (894)
- The Yellow House: A Memoir (2019 National Book Award Winner)Dari EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Penilaian: 4 dari 5 bintang4/5 (98)
- Shoe Dog: A Memoir by the Creator of NikeDari EverandShoe Dog: A Memoir by the Creator of NikePenilaian: 4.5 dari 5 bintang4.5/5 (537)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDari EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FuturePenilaian: 4.5 dari 5 bintang4.5/5 (474)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDari EverandNever Split the Difference: Negotiating As If Your Life Depended On ItPenilaian: 4.5 dari 5 bintang4.5/5 (838)
- Grit: The Power of Passion and PerseveranceDari EverandGrit: The Power of Passion and PerseverancePenilaian: 4 dari 5 bintang4/5 (587)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDari EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaPenilaian: 4.5 dari 5 bintang4.5/5 (265)
- The Emperor of All Maladies: A Biography of CancerDari EverandThe Emperor of All Maladies: A Biography of CancerPenilaian: 4.5 dari 5 bintang4.5/5 (271)
- On Fire: The (Burning) Case for a Green New DealDari EverandOn Fire: The (Burning) Case for a Green New DealPenilaian: 4 dari 5 bintang4/5 (73)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDari EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersPenilaian: 4.5 dari 5 bintang4.5/5 (344)
- Team of Rivals: The Political Genius of Abraham LincolnDari EverandTeam of Rivals: The Political Genius of Abraham LincolnPenilaian: 4.5 dari 5 bintang4.5/5 (234)
- Rise of ISIS: A Threat We Can't IgnoreDari EverandRise of ISIS: A Threat We Can't IgnorePenilaian: 3.5 dari 5 bintang3.5/5 (137)
- The Unwinding: An Inner History of the New AmericaDari EverandThe Unwinding: An Inner History of the New AmericaPenilaian: 4 dari 5 bintang4/5 (45)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDari EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyPenilaian: 3.5 dari 5 bintang3.5/5 (2219)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDari EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You ArePenilaian: 4 dari 5 bintang4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Dari EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Penilaian: 4.5 dari 5 bintang4.5/5 (119)
- Her Body and Other Parties: StoriesDari EverandHer Body and Other Parties: StoriesPenilaian: 4 dari 5 bintang4/5 (821)
- Herpes Labialis During PregnancyDokumen3 halamanHerpes Labialis During Pregnancyhendra cahyaditaBelum ada peringkat
- Oral Pathology Review List For NDEB With PicsDokumen75 halamanOral Pathology Review List For NDEB With PicsBookwyrm AddictBelum ada peringkat
- Topic - 8Dokumen29 halamanTopic - 8Cynthia GBelum ada peringkat
- Oral Pathology in The Pediatric PatientDokumen149 halamanOral Pathology in The Pediatric PatientDuOBelum ada peringkat
- Jaypee's Dental Dictionary (2009) (PDF) (UnitedVRG)Dokumen619 halamanJaypee's Dental Dictionary (2009) (PDF) (UnitedVRG)baselrehawiBelum ada peringkat
- Primary Herpetic Gingivostimatitis 2019Dokumen4 halamanPrimary Herpetic Gingivostimatitis 2019HeinzBelum ada peringkat
- Clinical Features of PeriodontitisDokumen36 halamanClinical Features of Periodontitislenami_91Belum ada peringkat
- Pemphigus Vulgaris 1Dokumen3 halamanPemphigus Vulgaris 1Yeni PuspitasariBelum ada peringkat
- OMIC 311 Lecture 17 Human Papilloma, Herpes, Hepatits VirusDokumen51 halamanOMIC 311 Lecture 17 Human Papilloma, Herpes, Hepatits VirusMaryam XABelum ada peringkat
- ICD Poli Gigi RevisiDokumen4 halamanICD Poli Gigi Revisiarsel dalungBelum ada peringkat
- Pediatrics (Toronto Notes For PDA 2004)Dokumen70 halamanPediatrics (Toronto Notes For PDA 2004)Worawut PhromwangBelum ada peringkat
- Non-Plaque Induced GingivitisDokumen30 halamanNon-Plaque Induced GingivitisDentist AymanBelum ada peringkat
- Oral Pathology: Dr. Rafil Hameed RasheedDokumen60 halamanOral Pathology: Dr. Rafil Hameed RasheedAhmed NajmBelum ada peringkat
- Modern Approaches To The Treatment of Viral Stomatitis in ChildrenDokumen5 halamanModern Approaches To The Treatment of Viral Stomatitis in ChildrenCentral Asian StudiesBelum ada peringkat
- Pedo2013 14Dokumen189 halamanPedo2013 14Vladimir Argirovic100% (4)
- Acute Gingival Infections: Necrotizing Ulcerative Gingivitis: Classification: 1. Acute. 2. SubacuteDokumen19 halamanAcute Gingival Infections: Necrotizing Ulcerative Gingivitis: Classification: 1. Acute. 2. SubacuteaizawachoiBelum ada peringkat
- Case #1: Case Study Assignment Assignment #3Dokumen10 halamanCase #1: Case Study Assignment Assignment #3api-536664543Belum ada peringkat
- A 25yr Old Male Presented With Skin Rash Involving Both Hands and Feet For 2 DaysDokumen234 halamanA 25yr Old Male Presented With Skin Rash Involving Both Hands and Feet For 2 DaysAli LashhabBelum ada peringkat
- Malassezia Furfur An-An Ap-Ap Naturally Found On The SkinDokumen48 halamanMalassezia Furfur An-An Ap-Ap Naturally Found On The SkinNikki ValerioBelum ada peringkat
- Acute Herpetic Gingivostomatitis: Causes, Symptoms and TreatmentDokumen14 halamanAcute Herpetic Gingivostomatitis: Causes, Symptoms and Treatmentapoorv jainBelum ada peringkat
- Alimentary Tract Pathology LGL 1 Oral and Salivary (WPS)Dokumen68 halamanAlimentary Tract Pathology LGL 1 Oral and Salivary (WPS)jwan ahmedBelum ada peringkat
- Hand, Foot, and Mouth Disease and Herpangina - UpToDateDokumen42 halamanHand, Foot, and Mouth Disease and Herpangina - UpToDateFer45Belum ada peringkat
- Viral Infections: Presented By: Fatimah Zahraa Ahmed Supervised By: DR - RafilDokumen31 halamanViral Infections: Presented By: Fatimah Zahraa Ahmed Supervised By: DR - Rafilfatimah zahraaBelum ada peringkat
- Daftar Penyakit Gigi Dan MulutDokumen10 halamanDaftar Penyakit Gigi Dan MulutbudiBelum ada peringkat
- Viral Ds. QuesDokumen6 halamanViral Ds. QuesArchanaBelum ada peringkat
- Anatomy and Disorders of the Oral CavityDokumen24 halamanAnatomy and Disorders of the Oral CavityMuhammad SalmanBelum ada peringkat
- Herpes Viruses: Clinical FeaturesDokumen4 halamanHerpes Viruses: Clinical FeaturesMoka MohsenBelum ada peringkat
- Lesi Multipel Akut (Infeksi Virus & Bakteri)Dokumen19 halamanLesi Multipel Akut (Infeksi Virus & Bakteri)Icha AnviniBelum ada peringkat
- Gingival Diseases PerioDokumen56 halamanGingival Diseases PerioFourthMolar.com100% (1)
- Questions From The Section On General and Special VirologyDokumen21 halamanQuestions From The Section On General and Special VirologytiffylolaBelum ada peringkat