Journal
Diunggah oleh
Robertus ElvantoraHak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Journal
Diunggah oleh
Robertus ElvantoraHak Cipta:
Format Tersedia
International Journal of Reproduction, Contraception, Obstetrics and Gynecology
Ahmad SN et al. Int J Reprod Contracept Obstet Gynecol. 2016 Jun;5(6):1874-1878
www.ijrcog.org
pISSN 2320-1770 | eISSN 2320-1789
DOI: http://dx.doi.org/10.18203/2320-1770.ijrcog20161681
Research Article
Evaluating condom catheter balloon tamponade in non-traumatic
postpartum haemorrhage resistant to medical management
Syed Nawaz Ahmad*, Sunita Seth, Shefali Agarwal, Swati Choudhary
Department of Obstetrics and Gynecology, Deen Dayal Upadhyay Hospital, New Delhi, India
Received: 26 March 2016
Revised: 01 May 2016
Accepted: 13 May 2016
*Correspondence:
Dr. Syed Nawaz Ahmad,
E-mail: dr.syednawaz@gmail.com
Copyright: the author(s), publisher and licensee Medip Academy. This is an open-access article distributed under
the terms of the Creative Commons Attribution Non-Commercial License, which permits unrestricted non-commercial
use, distribution, and reproduction in any medium, provided the original work is properly cited.
ABSTRACT
Background: Obstetric haemorrhage remains the most important cause of maternal mortality worldwide accounting for
25% of maternal deaths annually. The aim of the study was to evaluate efficacy of a condom catheter assembly for
uterine tamponade in the management of non-traumatic postpartum haemorrhage (PPH).
Methods: It was a prospective interventional study done in a tertiary care hospital in New Delhi, India. Thirty three
women with intractable PPH unresponsive to medical management were managed by uterine balloon tamponade
using a condom-catheter assembly prior to surgical intervention.
Results: The catheter successfully controlled haemorrhage in 31 out of 33 patients. In both the failed cases,
hysterectomy was required. Among the failed cases there was one maternal death due to sepsis and multi-organ
dysfunction syndrome (MODS). In cases where the balloon was successful, it was removed around 24 hours later and
no further bleeding or complication was observed.
Conclusions: Placement of a condom catheter balloon can successfully treat non-traumatic PPH refractory to medical
management. It is simple, inexpensive, easily, available and in those with successful placement no procedure related
morbidity was observed. The potential for it to be used by inexperienced operators in areas with limited resources
makes it a useful tool in management of PPH.
Keywords: Postpartum haemorrhage, Condom catheter balloon, Non-traumatic
INTRODUCTION
Obstetric haemorrhage remains the most important cause of
maternal mortality worldwide accounting for 25% of
maternal deaths annually. It is estimated that worldwide one
woman dies every four minutes due to postpartum
haemorrhage with an average yearly incidence of about
1,40,000 women deaths.1 Of the numerous causes of
postpartum haemorrhage, uterine atony is the commonest,
complicating 1 in 20 pregnancies. However, death from
PPH can largely be avoided through proper prevention,
diagnosis and management.2 Doumouchtsis SK et al in a
systematic review to identify all the studies evaluated the
success rates of treatment of PPH with uterine balloon
tamponade, uterine compression sutures, pelvic
devascularisation and arterial embolization.3 The
cumulative outcomes showed success rates of 84% (95%
CI, 77.5%-88.80%) for balloon tamponade. It was
concluded that balloon tamponade was the least invasive
and most rapid remedy for PPH management and should
be considered as the first step following failure of
medical therapy.
Condom catheter is a cheap and easily available
alternative to catheters like Sengstaken Blakemore tube
and Bakri balloon which are commonly used for
tamponade in post-partum haemorrhage. This prospective
study was planned to evaluate the utility of condom
catheter tamponade in non-traumatic PPH after failure of
medical management.
June 2016 Volume 5 Issue 6
Page 1874
Ahmad SN et al. Int J Reprod Contracept Obstet Gynecol. 2016 Jun;5(6):1874-1878
METHODS
Our study was a prospective interventional study
conducted at a tertiary care multi-speciality government
hospital of New Delhi, India from May 2013 to June
2014. All patients who delivered either vaginally or by
Caesarean section and developed non-traumatic
postpartum haemorrhage not responding to medical
management were included in this study.
The procedure was performed without additional
anaesthesia. First, bleeding due to local trauma or
retained tissue in the uterus was excluded. Blood loss was
estimated by visual method including use of calibrated
mops and suction apparatus. A condom was tied over the
distal end of the Foley's catheter with a silk thread.
Condom-catheter assembly was inserted into the uterine
cavity with a sponge holding forceps after introduction of
sims speculum into the vagina and holding cervical lips
with sponge holding forceps. Condom was inflated with
appropriate volume of normal saline (250 to 500ml) till
bleeding was arrested and balloon was visible through the
cervical canal. Outer end of Foley's catheter was clamped
and tied with silk thread. Bleeding was observed for next
15minutes. If bleeding stopped, tamponade was
continued for next 12-24hrs. Oxytocin infusion was
continued until 12 to 24 hours in the postoperative period.
After 12-24 hours, if the uterine fundus remained at the
same level and no bleeding was seen through the cervix,
balloon was removed. Oxytocin infusion (20 U in 500ml
Normal Saline) was started half an hour before deflation,
if not already on flow. The balloon was deflated slowly
(at the rate of 15 to 20 ml per minute) but not removed
until next 30 minutes, in case need for re-inflation arose.
Oxytocin infusion was continued during deflation. If the
patient did not bleed for next 30 minutes, the catheter
balloon assembly was removed and oxytocin infusion
continued according to clinical assessment, for a
maximum of 6 hours.
Statistical analysis was done using simple measures like
mean, median etc.
RESULTS
9.1%
6.1%
A+ C
A+Placental
bed
C
6.1%
9.1%
69.7%
Placental bed
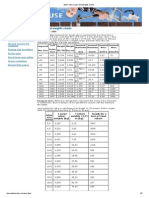
All women included in the study had primary PPH.
Atonicity (A) of the uterus was the cause in 23 (69.7%),
bleeding placental bed in 3 (9.1%), atonicity with
coagulopathy in 3 (9.1%), atonicity with bleeding placental
bed in 2 (6.1%) and only coagulopathy(C) in 2 (6.1%)
(Figure 1).
In 31 patients (93.9%), condom catheter balloon
successfully controlled bleeding and no additional
intervention was required at the time of deflation. The
mean time taken to arrest bleeding after the application of
the condom catheter balloon tamponade was 6.66 minutes
[Median (IQR) = 6 (5 - 8); 95% CI = 5.871 7.268] (Table
1).
The mean volume of fluid used to create tamponade was
381.06 ml [Median (IQR) = 400(300-450); 95% CI =
352.275 409.845] (Table 2).
On an average the condom catheter tamponade was
placed in situ for 19.94 hours [Median (IQR) = 21 (16
24); 95% CI = 18.578 21.302] (Figure 2).
Table 1: The mean time taken to arrest bleeding after
the application of the condom catheter balloon
tamponade.
Time taken
NA
1 5 min
6 10 min
>10 min
Total
Mean SD
Median (IQR)
95% CI
Frequency
2
8
21
2
33
6.66 1.98
6 (5 8)
5.871 7.268
Percentage
6.1%
24.2%
63.6%
3.0%
100%
Table 2: The mean volume of fluid used to create
tamponade.
Volume of fluid
<300 ml
300 - 400 ml
400 - 500 ml
Total
Mean SD
Median (IQR)
95% CI
Frequency Percentage
5
15.2%
16
48.5%
12
36.4%
33
100%
381.06 81.18
400 (300 - 450)
352.275 - 409.845
Every patient received 10 to 20 units of oxytocin infusion.
Thirty one (93.9%) patients received intramuscular
methylergometrine (0.2mg) injection in the range of 0 to 3
doses (average 2.45). Two (6.1%) women who didnt
receive methylergometrine had contraindication for the
same. All but one patient received PGF2 alpha (250
microgram) injection in the range of 0 to 5 doses (average of
3.21). All but one woman received PGE1 1000 micrograms
(five 200 microgram tablets) per rectum.
Figure 1: Causes of PPH.
International Journal of Reproduction, Contraception, Obstetrics and Gynecology
Volume 5 Issue 6 Page 1875
Ahmad SN et al. Int J Reprod Contracept Obstet Gynecol. 2016 Jun;5(6):1874-1878
NA
6.1%
12.1%
<15hrs
15-20 hrs
48.5%
33.3%
>20 hrs
Figure 2: Duration of tamponade.
Average blood loss per patient due to PPH in the study was
1.48 litres (SD 0.46; 95% CI 1.314-1.643). All 33 patients
were transfused with blood or blood products or both.
Average whole blood/packed cell transfusions received by
the patients in the study was 3.09 1.355 units (range 1-7 ,
total 102 units), 1.73 units of FFP (range 0 to 14; total 57
units) and 1.09 units of platelets ( range 0 to8; total 36 units).
The mean duration of hospital stay was 8.88 days.
Twenty nine women (87.9%) were followed up at 6weeks
postpartum. None of them had any clinical symptoms or
signs of endometritis.
In two patients in whom condom catheter balloon
tamponade failed to attain haemostasis, hysterectomy was
done. One of these two patients had multiple high risk
factors including anaemia, antepartum eclampsia,
deranged coagulation profile and was shifted to surgical
intensive care unit where she expired due to sepsis and
multi-organ dysfunction.
DISCUSSION
In the study period, 12460 deliveries took place of which
184 patients developed non-traumatic PPH. Thirty three
patients were enrolled for the study and 23 of those patients
(69.7%) had atonicity as the only cause for PPH while the
other ten had a combination of factors such as coagulopathy
and bleeding from the placental bed along with atonic
uterus. Twenty three (69.7%) patients had pre-existing risk
factors for PPH such as jaundice, anaemia, preeclampsia etc.
As shown in our study, in 31 out of 33 patients (93.9%),
condom catheter balloon successfully controlled bleeding
and no additional intervention was required [95% CI 79.4
99.3]. Tindell K et al conducted a systemic analysis to
evaluate the effectiveness of various types of uterine balloon
tamponade in the management of PPH in resource poor
settings.4 The studies used various types of uterine balloon
tamponade, including condom catheter (number of women
=193), Foleys catheter (n =5), and Sengstaken-Blakemore
oesophageal catheter (n = 1). In these studies, uterine
balloon tamponade successfully treated intractable PPH in
234 out of 241 women. Akhter S et al evaluated the
efficacy of hydrostatic condom catheter to control PPH
due to atonicity and morbid placental adhesions in 23
patients.5 The condom was inflated with 250 to 500 ml of
normal saline and was kept in situ for 24 to 48 hours. In
all 23 cases bleeding was successfully controlled. No
patient needed further intervention and no intrauterine
infection was documented. Thapa K et al in their
prospective study successfully applied condom catheter
tamponade in 14 patients with varying degrees of PPH
not controlled with pharmacological measures.6 The
Foleys - condom catheter tamponade stopped bleeding in
all the cases and no complications were encountered.
Condous GS et al evaluated the tamponade test in the
management of massive PPH in 16 patients and success
was met with in 14 (87.5%) of them.7 Two (12.5%) gave
negative tamponade test and hence underwent
laparotomy. This diagnostic test rapidly identified
patients with PPH who required a laparotomy. Rathore
AM et al in their prospective study conducted from 2009
to 2012 at Maulana Azad Medical College New Delhi
India, studied the efficacy of condom catheter tamponade
in the management of non-traumatic PPH resistant to
medical therapy in 18 patients with a success rate of
94%.8 Lydia R et al successfully managed four cases of
massive PPH due to uterine atony using condom catheter
balloon tamponade.9
The mean volume of fluid used to create tamponade and
stop bleeding was 381.06 81.18ml which was comparable
to the studies by Akhtar S et al (mean reported fluid
volume 336.4 ml) and Rather SY et al (mean reported
volume 342.8ml).5,10 The maximum volume of fluid used
in the study was 500ml. Till date the maximum volume of
fluid a condom catheter can hold has not been described, so
the end point for fluid inflation was till the bleeding stopped
and not the upper capacity limit as is the case with other
balloon devices like Sengstaken-Blakemore, Foleys
catheter Bakri balloon and Rusch urological catheter, all of
which have a defined upper limit. Since these devices can
hold a limited volume of fluid before they burst, for example
30ml for Foleys balloon, 500ml for Bakri balloon and
250ml for the gastric balloon of Sengstaken-Blakemore
tube, the tamponade test can be falsely be labelled as
negative though these devices can prove useful in cases of
small uteri as in post-abortal cases and secondary PPH.
In our study the mean time taken to arrest bleeding after the
application of the balloon tamponade was 6.66 1.98
minutes which was comparable to the study by Rathore AM
et al (6.06 minutes).8 While waiting for arrest of
haemorrhage, simultaneous arrangements can be done to
proceed to surgical measures. So waiting for 10 - 15 minutes
for the haemorrhage to stop while patient and operation
theatre are prepared for laparotomy can be justified, when
weighed against the radical procedures like hysterectomy.
Hence guarded wait can prevent radical procedures, more
importantly so in primiparous women, and the much
valuable uteri can be salvaged.
Average blood loss in this study was 1.48 litres which was
comparable to the study by Rathore AM.8 Since blood loss
estimation was done by visual method methods using
International Journal of Reproduction, Contraception, Obstetrics and Gynecology
Volume 5 Issue 6 Page 1876
Ahmad SN et al. Int J Reprod Contracept Obstet Gynecol. 2016 Jun;5(6):1874-1878
calibrated mops, it was subject to error. Blood loss
estimation by the suction apparatus in cases of caesarean
section would have been more objective, but often liquor
suction and blood suction were done with the same
apparatus which lead to inaccuracies in the blood loss
estimation even by this method.
In our study the condom catheter tamponade was placed in
situ for a mean duration of 19.94 3.84 hours. Minimum
duration for which condom catheter balloon tamponade was
left in situ was 13 hours and the maximum was 24 hours. In
the study by Rathore AM and Thapa K duration of
tamponade was between 24 to 28 hours.6,8 The tamponade
duration in our study was determined by the factors as the
hemodynamic condition of the patient, correction of
coagulation abnormality, availability of senior obstetrician,
availability of senior anaesthetist. The shorter duration of
tamponade in our study can imply that an attempt at earlier
deflation of the tamponade can be made, though further
studies are needed to recommend a specific duration for the
tamponade. Although condom catheter tamponade was
deflated at an early interval compared to other studies,
haemorrhage didnt resume in any patient. Though no major
complications have been reported by any study group with
the longer duration of the tamponade, the shorter duration
may reduce the morbidity due to longer duration, if any
proved in future.
Except for febrile morbidity in five patients in our study, no
major short-term complication was noted in any patient.
Among these five, cause of febrile morbidity was unknown
in one patient only. In the remaining four; respiratory
infection in one, urinary tract infection in two and
thrombophelebitis at venipuncture site in one patient were
identified as the cause. None of the patients had any
complaints and no complications like endometritis were
noted at six weeks follow up. Long-term complications like
development of ashermans syndrome, dysmenorrhoea,
oligomenorrhoea or problems with future conception and
fertility were not evaluated due to time constraints of the
study.
Few technical difficulties that were encountered in our study
included expulsion, in one patient who was asthmatic, and
abnormally tight tie of the condom over the Foleys catheter
leading to inflation failure in one patient.
In the setting of failure of medical management and when
other options are not available, especially in low-resource
settings, condom catheter balloon is a potential and
promising remedy available. It is simple, cheap, easily
available, effective and even a trained midwife can apply it.
It fits uterine contours naturally and no special technique as
in case of uterine packing is needed. It can be used in cases
of atonic uterus as well as PPH due to other causes although
studies involving larger groups of patients are needed to
further investigate this use. Further result in terms of arrest
of haemorrhage is available immediately. Even if it fails,
application of condom tamponade can buy us time to
prepare the patient for other surgical procedures. . In
resource-poor countries such as ours, where a majority of
deliveries take place at peripheral health centres, there is a
continuing need to develop low cost methods requiring
minimal skill to stem the morbidity and mortality arising out
of postpartum complications.
Limitations of the study include small sample size. Also the
impact of condom catheter tamponade on long term
outcomes like development of Ashermans syndrome,
menstrual disturbances, development of pelvic inflammatory
diseases in future, future fertility were not studied due to
short duration of the study.
CONCLUSION
Uterine tamponade using condom catheter balloon to
manage non-traumatic PPH is a fairly good procedure
with a definite advantage over other tamponade
procedures with respect to the cost, the expertise, and
availability. It also has the admirable advantage of
preservation of uterus and hence the future menstrual
function, fertility and conception when compared to the
radical procedures like hysterectomy. It is advantageous
over other surgical procedures like compression sutures
and devascularisation in terms of the cost effectiveness,
the ease of the procedure and the duration of hospital
stay, provided haemostasis is attained.
Funding: No funding sources
Conflict of interest: None declared
Ethical approval: The study was approved by the
Institutional Ethics Committee
REFERENCES
1.
2.
3.
4.
5.
6.
7.
Abouzahn C. Global burden of maternal death and
disability. Br Med Bull. 2003;67:1-11.
Karoshi M, Keith L. Challenges in managing
postpartum haemorrhage in resource- poor countries.
Clin Obstet Gynecol. 2009;52:285-98.
Doumouchtsis SK, Papageoeghiou AT, Arulkumaran
S. Systematic review of conservative management of
postpartum haemorrhage: what to do when medical
management
fails.
Obstet
Gynecol
Surv
2007;62(8):540-7.
Tindell K Garfinkel R, Abu-Hayder E, Ahn R, Burke
T, Conn K. Uterine balloon tamponade for the
treatment of postpartum haemorrhage in resourcepoor settings: a systematic review. Br J Obstet
Gynecol. 2012;120(1):5-14.
Akhter S, Begum MR, Kabir Z, Rashid M, Laila TR,
Zabeen F. Use of a condom to control massive
postpartum haemorrhage. Med Gen Med.
2003;5(3):38.
Thapa K, Malla B, Pandey S, Amatya S. Intrauterine
condom tamponade in management of postpartum
haemorrhage. J Nepal Health Res Counc. 2010;8:19.
Condous GS, Arulkumaran S, Symonds I, Chapman
R, Sinha A, Razvi K. The tamponade test in the
International Journal of Reproduction, Contraception, Obstetrics and Gynecology
Volume 5 Issue 6 Page 1877
Ahmad SN et al. Int J Reprod Contracept Obstet Gynecol. 2016 Jun;5(6):1874-1878
8.
management of massive postpartum haemorrhage.
Obstet Gynecol. 2003;101:767-72.
Rathore AM, Gupta S, Manaktala U, Gupta S,
Dubhey C, Khan AM. Uterine tamponade using
condom catheter balloon in the management of nontraumatic postpartum haemorrhage. J Obstet
Gynaecol Res. 2012;38:1162.
9.
Airede LR, Nnadi DC. The use of condom catheter
for the treatment of postpartum haemorrhage. Trop
Doct. 2008;38:84-6.
10. Rather SY, Qadir A, Parveen S, Jabeen F. Use of
condom to control intractable PPH. JK Science.
2010;12(3):127-9.
Cite this article as: Ahmad SN, Seth S, Agarwal S,
Choudhary S. Evaluating condom catheter balloon
tamponade in non-traumatic postpartum haemorrhage
resistant to medical management. Int J Reprod
Contracept Obstet Gynecol 2016;5:1874-8.
International Journal of Reproduction, Contraception, Obstetrics and Gynecology
Volume 5 Issue 6 Page 1878
Anda mungkin juga menyukai
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDari EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifePenilaian: 4 dari 5 bintang4/5 (5795)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDari EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You ArePenilaian: 4 dari 5 bintang4/5 (1091)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDari EverandNever Split the Difference: Negotiating As If Your Life Depended On ItPenilaian: 4.5 dari 5 bintang4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDari EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RacePenilaian: 4 dari 5 bintang4/5 (895)
- Grit: The Power of Passion and PerseveranceDari EverandGrit: The Power of Passion and PerseverancePenilaian: 4 dari 5 bintang4/5 (588)
- Shoe Dog: A Memoir by the Creator of NikeDari EverandShoe Dog: A Memoir by the Creator of NikePenilaian: 4.5 dari 5 bintang4.5/5 (537)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDari EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersPenilaian: 4.5 dari 5 bintang4.5/5 (345)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDari EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FuturePenilaian: 4.5 dari 5 bintang4.5/5 (474)
- Her Body and Other Parties: StoriesDari EverandHer Body and Other Parties: StoriesPenilaian: 4 dari 5 bintang4/5 (821)
- The Emperor of All Maladies: A Biography of CancerDari EverandThe Emperor of All Maladies: A Biography of CancerPenilaian: 4.5 dari 5 bintang4.5/5 (271)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Dari EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Penilaian: 4.5 dari 5 bintang4.5/5 (121)
- The Little Book of Hygge: Danish Secrets to Happy LivingDari EverandThe Little Book of Hygge: Danish Secrets to Happy LivingPenilaian: 3.5 dari 5 bintang3.5/5 (400)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDari EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyPenilaian: 3.5 dari 5 bintang3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)Dari EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Penilaian: 4 dari 5 bintang4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDari EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaPenilaian: 4.5 dari 5 bintang4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDari EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryPenilaian: 3.5 dari 5 bintang3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnDari EverandTeam of Rivals: The Political Genius of Abraham LincolnPenilaian: 4.5 dari 5 bintang4.5/5 (234)
- Exxonmobil Interview Questions and AnswersDokumen60 halamanExxonmobil Interview Questions and Answersrajkamal eshwar100% (3)
- On Fire: The (Burning) Case for a Green New DealDari EverandOn Fire: The (Burning) Case for a Green New DealPenilaian: 4 dari 5 bintang4/5 (74)
- The Unwinding: An Inner History of the New AmericaDari EverandThe Unwinding: An Inner History of the New AmericaPenilaian: 4 dari 5 bintang4/5 (45)
- Afloat 2Dokumen256 halamanAfloat 2Matthaios SkantrzourakisBelum ada peringkat
- Rise of ISIS: A Threat We Can't IgnoreDari EverandRise of ISIS: A Threat We Can't IgnorePenilaian: 3.5 dari 5 bintang3.5/5 (137)
- Lecture-8: Identification of The Suspect: Attributing Cyber Conduct To A PersonDokumen22 halamanLecture-8: Identification of The Suspect: Attributing Cyber Conduct To A Personreputation.com.ngBelum ada peringkat
- Enron Case StudyDokumen23 halamanEnron Case StudyJayesh Dubey100% (1)
- Home Work: Novendra Dery ElvantoraDokumen8 halamanHome Work: Novendra Dery ElvantoraRobertus ElvantoraBelum ada peringkat
- Data Univariat: StatisticsDokumen5 halamanData Univariat: StatisticsRobertus ElvantoraBelum ada peringkat
- Crosstabs Kadar Kolesterol Dengan Kadar HDLDokumen2 halamanCrosstabs Kadar Kolesterol Dengan Kadar HDLRobertus ElvantoraBelum ada peringkat
- Jurnal KustaDokumen14 halamanJurnal KustaRobertus ElvantoraBelum ada peringkat
- Home Work: Novendra Dery ElvantoraDokumen5 halamanHome Work: Novendra Dery ElvantoraRobertus ElvantoraBelum ada peringkat
- Scientific Writing: How To Create, and FormDokumen42 halamanScientific Writing: How To Create, and FormRobertus ElvantoraBelum ada peringkat
- Penyakit Degeneratif: Resti AraniaDokumen61 halamanPenyakit Degeneratif: Resti AraniaRobertus ElvantoraBelum ada peringkat
- Measure Surface Texture and Lead Angle of ShaftsDokumen7 halamanMeasure Surface Texture and Lead Angle of Shaftsshivam daveBelum ada peringkat
- Solid State Broadband High Power Amplifier: 1 - 30 MHZ / 50 WattsDokumen3 halamanSolid State Broadband High Power Amplifier: 1 - 30 MHZ / 50 Wattskhanafzaal2576Belum ada peringkat
- The Learning Principle PRINTDokumen5 halamanThe Learning Principle PRINTnurulBelum ada peringkat
- JOURNAL REVIEW Government Policy of Indonesia To Managing Demographic Bonus and Creating Indonesia Gold in 2045Dokumen5 halamanJOURNAL REVIEW Government Policy of Indonesia To Managing Demographic Bonus and Creating Indonesia Gold in 2045albertus amandaruBelum ada peringkat
- 2012 Nike Football Clinic 4Dokumen2 halaman2012 Nike Football Clinic 4Bruno ChuBelum ada peringkat
- Single and Multistage Steam Jet Ejectors: TorinoDokumen12 halamanSingle and Multistage Steam Jet Ejectors: TorinoSuman SenapatiBelum ada peringkat
- Impact of Phragmanthera Capitata (Sprenge.) Balle On Pod and Beans Production of Two Cocoa Clones in Nkoemvone Seed Fields (South Cameroun) - JBES @scribdDokumen9 halamanImpact of Phragmanthera Capitata (Sprenge.) Balle On Pod and Beans Production of Two Cocoa Clones in Nkoemvone Seed Fields (South Cameroun) - JBES @scribdInternational Network For Natural SciencesBelum ada peringkat
- TestDokumen4 halamanTestAlina DushachenkoBelum ada peringkat
- BM 2 Operations Management and TQM NewDokumen9 halamanBM 2 Operations Management and TQM NewEly GragasinBelum ada peringkat
- Steel Rebar Sizes and Weights ChartsDokumen2 halamanSteel Rebar Sizes and Weights ChartsNadiah Abdul RahamanBelum ada peringkat
- 2000 - VAICTM-an Accounting Tool For IC Management - Ante PulicDokumen13 halaman2000 - VAICTM-an Accounting Tool For IC Management - Ante PulicIklima RahmaBelum ada peringkat
- Commercial InvoiceDokumen4 halamanCommercial InvoiceHenry SilvaBelum ada peringkat
- Lipsey and Chrystal Economics 11th Edition Free: Page 1 / 3Dokumen3 halamanLipsey and Chrystal Economics 11th Edition Free: Page 1 / 3MahmoudElbehairy100% (1)
- Major and Minor TriadsDokumen16 halamanMajor and Minor TriadsSAYIBelum ada peringkat
- Av1 OnDokumen7 halamanAv1 OnLê Hà Thanh TrúcBelum ada peringkat
- Open CVDokumen11 halamanOpen CVXavier Ibarra CorteBelum ada peringkat
- Tos-Teacher-Made-Test-Group-3Dokumen10 halamanTos-Teacher-Made-Test-Group-3Maestro MotovlogBelum ada peringkat
- The Metal Oxide FETDokumen7 halamanThe Metal Oxide FETSitty GuBelum ada peringkat
- ReadingDokumen3 halamanReadingMuhamad IbrohimBelum ada peringkat
- 曼昆《经济学原理第三版》宏观分册原版中英文双语PPT课件Chap 25Dokumen76 halaman曼昆《经济学原理第三版》宏观分册原版中英文双语PPT课件Chap 25Jia Wei MiaoBelum ada peringkat
- Module II - Value Chain AnalysisDokumen72 halamanModule II - Value Chain AnalysisloganathprasannaBelum ada peringkat
- Simulation of CO2 Capture Using MEA Scrubbing A Flowsheet Decomposition Method PDFDokumen13 halamanSimulation of CO2 Capture Using MEA Scrubbing A Flowsheet Decomposition Method PDFSuprio KamalBelum ada peringkat
- EE 421-Digital System Design-Dr. Shahid Masud-Updated PDFDokumen4 halamanEE 421-Digital System Design-Dr. Shahid Masud-Updated PDFUbaid UmarBelum ada peringkat
- AttentionDokumen26 halamanAttentionKarn KunteBelum ada peringkat
- FRENCH Grade 6 UnlockedDokumen50 halamanFRENCH Grade 6 UnlockedWainaina MuriukiBelum ada peringkat
- Two Square TEAM 82 - LondonCRUDokumen53 halamanTwo Square TEAM 82 - LondonCRUAsankanathBelum ada peringkat