Jurnal Aarabi
Diunggah oleh
rizkyHak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Jurnal Aarabi
Diunggah oleh
rizkyHak Cipta:
Format Tersedia
Received: 21 Jun.
2008
Accepted: 11 Mar. 2008
Original Article
Health care personnel compliance with standards of eye and face protection
and mask usage in operating rooms
Akram Aarabi*, Effat Kordi**, Hassan Farahmand*,
Farzaneh Gholami*, Soheila Bakhtiari*
Abstract
Background: Personal protection equipments (PPEs) should be easily accessible to decrease contact with infecting factors
and also should be used purposefully to effectively keep the health care personnel in a safe distance from the patient blood
and body fluid which can easily infect the operating rooms personnel. This study aimed to find the operating rooms' personnel compliance with standards of two PPE items, mask and eye/face protection and the effective factors on their compliance.
Methods: This was a descriptive correlative study. Sampling method was simple and 250 operating room personnel were
selected. Data were collected by a questionnaire consisting of three parts; demographic characteristics and standards usage
of mask and eye/face protection. Participants were divided into four groups of perfect, favorable, relatively acceptable and
deficient based on their scores of their compliance with standards in the second and third parts of the questionnaire.
Results: The favorable compliance with standard usage of mask and eye/face protection was 33.9% and 46.4%, respectively. Participants said that lack of mask and eye/face protection was the main effective factor for their compliance. There was
no significant relationship between work place and educational degree, and the personnel's compliance with standard usage
of eye/face protection and mask.
Conclusion: Compliance with standard usage of mask is not acceptable and is almost in agreement with other studies. The
important point is that there is no significant difference between personnel's compliance with standard usage of mask and
eye/face protection in high risk and low risk environments.
Key words: Compliance with standards, personal protection equipments, effective factors, operating room personnel
IJNMR 2008; 13(2): 59-64
nfection control is a major issue in hospital
environment especially operating rooms. It
has two sides: patient and health care personnel. In the personnel side, two issues should
be considered: transferring infection from personnel and to the personnel. Infection control
has been studied with various approaches, one
of which is Personal protection equipments
(PPEs) that consider both transferring from and
to personnel. PPEs include mask, gloves,
eye/face protection and gown.1
Mayhall (2004) says that some strategies are
needed to reduce the professional contact with
infective factors. These strategies include developing knowledge, changing habits, and improving PPE qualities. PPEs should be easily accessible and purposefully used to effectively provide a safe distance between the patient blood
and body fluid and health care personnel. The
health care personnel should be taught how to
use PPEs and it should be assured that they are
using the PPEs correctly.2 Operating room
* MSc, Department of Operating Room Nursing, School of Nursing and Midwifery, Isfahan University of Medical Sciences, Isfahan, Iran.
** BSc, Manager of Operating Room, Al-Zahra Hospital, Isfahan University of Medical Sciences, Isfahan, Iran.
Correspondence to: Akram Aarabi MSc.
E-mail: aarabi@nm.mui.ac.ir
Research Article of Isfahan University of Medical Sciences, No: 286039
IJNMR/ Spring 2008; Vol 13, No 2.
59
www.mui.ac.ir
Health care personnel compliance with operating room standards
personnel are in danger of being infected by
patient's blood and body fluid splash. The main
risk factor in this regard is their behavior in the
operating rooms, how they deal with minimum
infection, how they wash their hands and how
cautious they are in general.3 Phippen (2000)
suggests that the eye/face protection must be
used wherever there is a possibility of blood
and body fluid splash.4 However, some personnel do not follow this rule for some reasons.
Based on the researcher experiences, an effective factor in usage of eye/face protection is
dealing with dangerous blood diseases such as
AIDS or hepatitis and in other cases personnel
do not find it necessary to use the eye/face protection. All hospital personnel who participate
in operations or c-section should be cautious
about skin contact with mucous membrane and
it is necessary to use mask and eye protection
during all operations which can transfer the infected components or pieces of bones.5 Angelillo et al (1999) in a study on 216 operating room
personnel in 16 hospitals reported that just 38%
were using the PPEs (gloves, mask, eyes protection) appropriately and based on standards.3 In
Iran, Motamed et al, on a study on 54 health
care personnel in two hospitals in Mazandaran
in 2006, reported favorable usage of PPEs and
hand washing. But, he reported that the participants knowledge of PPEs especially eye/face
protection was low except about wound by
needles, contact with vaginal secretions, usage
of mask and gown and cleaning the splashed
blood.6 Nursing services have played an effective role in health care services by keeping high
professional standards.7
Considering the potential danger of working
in an operating room without PPEs, this study
aimed to find the operating rooms' personnel
compliance with the standards of using mask
and eye/face protection in selected hospitals
administered by the Isfahan University of Medical Sciences. Also, the effective factors on their
compliance with these standards were investigated. It is hoped that by finding the effective
factors on the compliance with standards of using mask and eye/face protection, we can im-
Arabi et al
prove the situation and make it closer to the
standard level.
Methods
This was a descriptive correlative study. The
research population included all the operating
room personnel working under the Isfahan
University of Medical Sciences. The sample included 250 personnel selected by simple method. The sample size was calculated based on a
pilot study on 13 operating room personnel in
Al-Zahra hospital with p = 25% and accuracy of
0.07 (d).
The inclusion criteria included working in
operating rooms with education level of nursing diploma, operating room college degree,
anesthesia college degree, bachelor degree or
Master in nursing.
Data were collected by a questionnaire made
by the researcher based on the standards of using PPEs cited in Waikato (DHB) in February
2006.1 This questionnaire measured the usage of
mask and eye/face protection separately. The
first section of the questionnaire included demographic data and the second section included two parts, one on standard usage of
mask and the other on eye/face protection.
Since for the personnel of anesthesia just mask
is important, these personnel were studies just
for mask. Data were analyzed using SPSS software and descriptive and inferential statistics
(U-Mann Whitney and Spearman correlation
coefficient).
Since the questionnaire was made based on
DHB standards, questions were formed in a
standard form. Also, to assure the structure of
questions, the content validity was obtained
with the help of several faculty members of the
Faculty of Nursing and Midwifery. To check the
reliability of the questionnaire, re-test was used.
The questionnaire was completed by 13 personnel twice and the correlation coefficient between questions was calculated 0.53 and the
reliability obtained 0.69.
Results
Two hundred and fifty participants included
60
IJNMR/ Spring 2008; Vol 13, No 2.
www.mui.ac.ir
Health care personnel compliance with operating room standards
Arabi et al
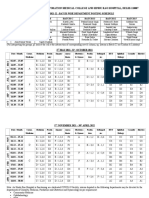
Table 1. Compliance with standards of using mask in risky and less risky operating rooms
Work Place Risky
Compliance with standards
No(%)
Less Risky
No(%)
Total
No(%)
Deficient
16(6.5)
4(1.6)
20(8.1)
Relatively acceptable
81(32.9)
22(8.9)
103(41.9)
Favorable
61(24.8)
22(8.9)
83(33.7)
Perfect
35(14.2)
5(2)
40(16.3)
Total
193(78.5)
53(21.5)
246(100)
131 operating room personnel (scrubbing) and
109 anesthesia personnel. As it was mentioned,
the data of compliance with standards of mask
usage were from all 250 subjects, but the data
related to eye/face protection usage were from
141 (because the rest were working just in anesthesia and didn't need eye/face protection). Results are shown in table 1 and 2. The highest
rate of compliance with standards was relatively acceptable compliance (104 participants,
41.9%). Also, the highest frequency belonged to
using mask (225 participants, 91.46%). From
demographic data, two characteristic of work
place in operating room and educational level
was considered for correlation with compliance
with standards. Operating rooms were divided
into risky and less risky based on the dangers of
transferring infection to personnel, which
means in those operating rooms where the possibility of splash of blood and body fluid is
more, such as orthopedic, women, heart, emergency, jaw and face and nerves considered risky
and other operating rooms were less risky.
U-Mann Whitney test
Z = 0.046, p = 0.96
In this field, most personnel working in risky
places were using masks relatively standard
(32.9%).
The relation of compliance with standards of
using mask and the educational level showed
that the highest frequency belongs to the personnel with relatively acceptable compliance
and a college degree (31.2%).
The frequency distribution of compliance
with standards of using eye/face protection
showed that the highest frequency belongs to
those with favorable and perfect compliance
respectively (46.4% and 30%) and just 13 personnel had deficient compliance with standards. Also, the highest frequency belonged to
using eye/face protection (42.42%). From the
demographic data, the relation between work
place and educational degree with the personnel's compliance with standards were considered and the highest frequency belongs to
those working in risky operating rooms and
having a college degree (37% and 32.1%).
Table 2. Compliance with standards of using eye/face protection in risky and less risky operating
rooms
Less Risky
Total
U-Mann Whitney test
Work Place Risky
Compliance with standards
No(%)
No(%)
No(%)
Deficient
9(6.5)
4(2.9)
13(9.4)
Relatively acceptable
12(8.7)
8(5.8)
20(14.5)
Favorable
51(37)
13(9.4)
64(46.4)
Perfect
27(19.6)
14(10.1)
41(29.7)
Total
99(71.7)
39(28.3)
138(100)
IJNMR/ Spring 2008; Vol 13, No 2.
Z = 0.046, p = 0.96
61
www.mui.ac.ir
Health care personnel compliance with operating room standards
Discussion
In this research, the range of compliance with
standards was very small. If we consider a wider range, we can add the personnel with favorable compliance to the perfect ones. Larson et al
(1999) say that even the best surgery masks
cannot cover the face in a way that the air cannot sneak into the edges.8 Therefore, this study
considers the favorable compliance with standards and the perfect one in one group. Thus,
the total number of personnel, who had acceptable usage of mask, is half of the sample. The
effective factors on personnel's compliance with
standards of using masks can be divided into
three categories based on the subjects:
1) Mask quality related factors including being
bothered by mask lint, elastic straps, nose skin
sensitivity, and bad smell of some masks. Rivera et al (2000) about using low quality cheap
masks in some health centers found that some
health centers use N-90 masks because they
are cheaper, so that they can reduce expenses,
but studies show that these masks are not
good to be used even once and therefore personnel have to change several masks per day
and this makes the expenses increase and not
decrease.9
2) Factors related to using mask: 46 subjects
said that lack of mask is the main reason for
not changing mask after each procedure. In
mask usage standards, it is warned in big
fonts that masks should not be kept around
the neck when it is not used.1 Considering the
reasons that 26 participants mentioned for
why they keep the mask around their neck
(which include the need for immediate use of
mask, habit, forgetfulness), it seems that education is necessary to remove these factors
and improve the compliance with this standard. Rothrock et al (2003) write that mask
should be enough big to cover the nose,
mouth, lower jaw and facial hair.10 Five participants mentioned breathing problems as the
reason they do not follow this standard,
which seems to be a ridiculous excuse. In
mask using standards it is mentioned that to
remove the mask, the front part should not be
touched but used the straps.1 Nine partici-
Arabi et al
pants mentioned that the factors for not following this standard include not being used
to it, being negligent, not believing in it and
lack of knowledge about standards, which all
can be changed and improved by education.
In the standards of using mask it is mentioned
that personnel should not go to work when
they catch a cold.1 Ninety nine participants
said that the reason they do not follow this
standard is that the authorities do not consider their cold important. It is usual in Iranian
hospitals that personnel who have cold work
in the operating rooms while being cautious
of some specific principles including using
two masks over each other, working in a peripatetic position rather than scrub, none of
which are in agreement with standards.
3) Factors related to mask usage style in scopy:
in mask usage standards it is mentioned that
during scopy operations, masks should be effectively used just like other operations.1 The
replies of 13 participants implied that they
thought of using masks during scopy because
of the patient's safety and not their own safety. They mentioned some reasons such as low
risk of infection for the patient why they
didn't follow this standard. This can also be
fixed by education.
The relation of compliance with standards
and two demographic items of work place and
educational level were studies. Rothrock et al
(2003) about the effective role of mask in risky
operating rooms says that mask is important
not only for protecting the patient from infection, but also protecting the operating room
personnel from the potential infections due to
blood and body fluid; especially in the cause of
mask, personnel's protection is concerned more
than patients.10 U-Mann Whitney test showed
no significant relation between compliance with
standards and working place. It means that
working in risky or less risky operating rooms
was not related to compliance with standards of
mask usage. In regard with the educational degree, it seems that the different number of participants in various levels of education made
this relation insignificant (there were more college degrees than others). Roup 1999 believes
62
IJNMR/ Spring 2008; Vol 13, No 2.
www.mui.ac.ir
Health care personnel compliance with operating room standards
that literacy has little role in effective factors of
personnel's safety care. He mentioned some key
components of protection, safety and effective
use of PPEs, a significant one of which is educating personnel and follow-ups.11
The data collected about compliance with
standards of using eye/face protection show
that most participants' compliance with standards were favorable and perfect respectively
and just 13 participants' compliance with standards were deficient. Akdoman et al (1999) in a
study on 597 health care personnel in operating
rooms reported their compliance with standards of using protective glasses, 32% and eyeprotections, 24%.13 The researcher made three
categories of all factors introduced by the personnel as obstacles of their compliance with
standards of using eye/face protection:
1) Factors related to correct use of eye/face protection: The most frequent reason was lack of
eye/face protections, then shortage of
eye/face protections, type of surgery, and
emergency operations. The researcher investigated the issue of lack of eye/face protection
and found that all the personnel of the selected hospitals received an eye/face protection at least once; in Al-Zahra hospital, recycle
type was also distributed. Some participants
believed that using eye/face protection during surgeries with infections is necessary. In
the standards of using eye/face protections, it
is mentioned that all personnel who are involved in orthopedic and women surgeries
should use them all the time.1 It means that
using eye/face protection is not limited to infection surgeries or patients with infection.
Four participants, mentioned emergency operations as the reason of not following these
standards, and 1 participant mentioned lack
of time as the reason. According to Rothrock
et al (2003), during emergency operations (but
not always) or during the work in emergency
rooms using eye/face protection is necessary.10 One participants mentioned wearing
eye-glasses as the obstacle to follow the standards. Buster (2006) introduced different
types of eye/face protections, some of which
are designed for those wearing eye-glasses.1
Arabi et al
Fortunately, eye/face protections are available
in operating rooms in Al-Zahra hospital and it
is not difficult to provide them for other hospitals.
2) Factors related to eye/face protections maintenance: In the standards of using eye/face
protections, it is mentioned that recycle types
should be demolished after being used once
and the usual ones should be washed after being used each time and if they are too messy
to be cleaned, should be demolished.1 Ten
participants mentioned lack of eye/face protections as the reason for reusing the recycle
types. This case seems to need education.
3) Factors related to the quality of eye/face protections include being heavy, foggy glasses,
discomfort around the ears and improper
sight: The factor, foggy glasses, was reported
by 5 personnel. Although a few personnel
mentioned the low quality of eye/face protections as the reason for not following the standard rules, it should be paid attention and
solved, because the quality of a product
strongly affects its usage. To prevent discomfort of the holders around the ears, the elastic
types can be used.
Regarding the relation between compliance
with standards of eye/face protections usage
and the risk of work place in operating rooms,
Rothrock et al (2003) say that using eye/face
protections in orthopedic operating rooms is
absolutely necessary.10 Also, in the standards of
using eye/face protections, it is mentioned that
in those operating rooms where the possibility
of blood and body fluid splash is high, eye/face
protections must be used.1 More than two third
of participants in this study working in risky
operating rooms and 39 personnel working in
less risky operating rooms. The highest frequency belonged to those working in risky operating rooms and their compliance with standards was favorable and then perfect. The reason for this high number is that most participants in the study were working in risky operating rooms. The number of personnel with deficient and relatively deficient compliance with
standards was higher in this group as well. Finally, because this relation was not significant,
IJNMR/ Spring 2008; Vol 13, No 2.
63
www.mui.ac.ir
Health care personnel compliance with operating room standards
we resulted that compliance with standards of
eye/face protections usage is not related to how
risky is the operating rooms. In other words,
personnel's behavior is the same in risky and
less risky operating rooms.
The relation of compliance with standards of
eye/face protections usage and educational level followed the same pattern. The highest frequency belonged to the personnel with college
degree whose compliance with standards was
Arabi et al
favorable and perfect. Because the number of
participants with a college degree was 40 personnel more than those with bachelor degrees,
probably the high frequency of them in all four
groups from deficit to perfect compliance in
participants with college degree was related to
this difference.
The researchers declare that have no conflict of
interest in this study and they have surveyed
under the research ethics.
References
1. Wiseman B. Procedure: Serious and Sentinel Event Review. Hamilton: Waikato district health board; 2005. p. 1-10.
2. Glen MC. Epidemiology and Infection control. 3rd ed. New York: Lippincott Williams and Wilkins 2004. p. 1453.
3. Angelillo IF, Mazziotta A, Nicotera G. Nurses and hospital infection control: knowledge, attitudes and behaviour of
Italian operating theatre staff. Journal of hospital infection 1999; 42(2): 105-12.
4. Phippen ML, Wells M. Patient care during operative and invasive procedures. Philadelphia: W.B.Saunders; 2000. p.
713.
5. Ibrahimzadeh S. A study of nurses' knowledge about hospital infections control and prevention. Quarterly of Nurse,
scientific news of Gilan faculty of nursing and midwifery 2001. 12(43-4): 29.
6. Motamed N, BabaMahmodi F, Khalilian A, Peykanheirati M, Nozari M. Knowledge and practices of health care
workers and medical students towards universal precaustions in hospitals in Mazandaran Province. East Mediterr
Health J 2006; 12: 653-61.
7. Makkiabadi Z. First aid health care by nurses. Behdasht Jahan 2002; 15(1-2): 63-5.
8. Larson EL. APIC guideline for handwashing and hand antisepsis in health care settings. Am J Infect Control 1995;
23(4): 251-69.
9. Rivera P, Louther J, Mohr J, Campbell A, DeHovitz J, Sepkowitz KA. Does a cheaper mask save money? The cost
of implementing a respiratory personal protective equipment program. Infect Control Hosp Epidemiol 1997; 18(1):
24-7.
10. Roup BJ. OSHA's new standard: exposure to bloodborne pathogens. AAOHN J 1993; 41(3): 136-42.
11. McEwen RJD, Smith D, Editors. Alexanders Care of the Patient in Surgery. 12th ed. St Louis: Mosby-Year Book,
Inc; 2003. p. 720.
12. Akduman D, Kim LE, Parks RL, L'Ecuyer PB, Mutha S, Jeffe DB, et al. Use of personal protective equipment and
operating room behaviors in four surgical subspecialties: personal protective equipment and behaviors in surgery.
Infect Control Hosp Epidemiol 1999; 20(2): 110-4.
13. Abdollahzadeh Mahlani F, Moghadasian S, Ghorbanian N. Use of personal protective equipment and operating
room behaviors in three surgical sub-specialties. ThPeC7463. Proceeding of the 15th International Conference on
AIDS. 2004 Jul 11-16; Bangkok, Thailand. p. 15.
64
IJNMR/ Spring 2008; Vol 13, No 2.
www.mui.ac.ir
Anda mungkin juga menyukai
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDari EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryPenilaian: 3.5 dari 5 bintang3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Dari EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Penilaian: 4.5 dari 5 bintang4.5/5 (121)
- Grit: The Power of Passion and PerseveranceDari EverandGrit: The Power of Passion and PerseverancePenilaian: 4 dari 5 bintang4/5 (588)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDari EverandNever Split the Difference: Negotiating As If Your Life Depended On ItPenilaian: 4.5 dari 5 bintang4.5/5 (838)
- The Little Book of Hygge: Danish Secrets to Happy LivingDari EverandThe Little Book of Hygge: Danish Secrets to Happy LivingPenilaian: 3.5 dari 5 bintang3.5/5 (400)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDari EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaPenilaian: 4.5 dari 5 bintang4.5/5 (266)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDari EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifePenilaian: 4 dari 5 bintang4/5 (5794)
- Rise of ISIS: A Threat We Can't IgnoreDari EverandRise of ISIS: A Threat We Can't IgnorePenilaian: 3.5 dari 5 bintang3.5/5 (137)
- Her Body and Other Parties: StoriesDari EverandHer Body and Other Parties: StoriesPenilaian: 4 dari 5 bintang4/5 (821)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDari EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You ArePenilaian: 4 dari 5 bintang4/5 (1090)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDari EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyPenilaian: 3.5 dari 5 bintang3.5/5 (2259)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDari EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersPenilaian: 4.5 dari 5 bintang4.5/5 (345)
- Shoe Dog: A Memoir by the Creator of NikeDari EverandShoe Dog: A Memoir by the Creator of NikePenilaian: 4.5 dari 5 bintang4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerDari EverandThe Emperor of All Maladies: A Biography of CancerPenilaian: 4.5 dari 5 bintang4.5/5 (271)
- Team of Rivals: The Political Genius of Abraham LincolnDari EverandTeam of Rivals: The Political Genius of Abraham LincolnPenilaian: 4.5 dari 5 bintang4.5/5 (234)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDari EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RacePenilaian: 4 dari 5 bintang4/5 (895)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDari EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FuturePenilaian: 4.5 dari 5 bintang4.5/5 (474)
- Sarms 1 - The Ultimate Guide To SarmsDokumen4 halamanSarms 1 - The Ultimate Guide To SarmsHumbert Gym ColombinaBelum ada peringkat
- On Fire: The (Burning) Case for a Green New DealDari EverandOn Fire: The (Burning) Case for a Green New DealPenilaian: 4 dari 5 bintang4/5 (74)
- The Yellow House: A Memoir (2019 National Book Award Winner)Dari EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Penilaian: 4 dari 5 bintang4/5 (98)
- Lastearthdistro PDFDokumen24 halamanLastearthdistro PDFleonabrahamzapruderBelum ada peringkat
- The Unwinding: An Inner History of the New AmericaDari EverandThe Unwinding: An Inner History of the New AmericaPenilaian: 4 dari 5 bintang4/5 (45)
- Legal MedDokumen42 halamanLegal Medaisajane_rmt100% (6)
- DewormingDokumen48 halamanDewormingJulie Ann Escartin80% (5)
- Neurotransmitters & NeuromodulatorsDokumen41 halamanNeurotransmitters & Neuromodulatorsafiwahyu100% (1)
- CH 11 Admission, Discharge, Transfers & ReferralsDokumen14 halamanCH 11 Admission, Discharge, Transfers & ReferralsNilakshi Barik Mandal100% (1)
- Nasya Treatment: DefinitionDokumen4 halamanNasya Treatment: DefinitionkaukabBelum ada peringkat
- Pharma QuestionsDokumen13 halamanPharma QuestionsSarah Mae SinceroBelum ada peringkat
- TheraSuit BrochureDokumen8 halamanTheraSuit BrochureMhmd IrakyBelum ada peringkat
- Anthelmintic DrugsDokumen35 halamanAnthelmintic DrugsRamla KashifBelum ada peringkat
- A Descoberta de Diferentes Tipos de Muco Cervical e o Método de Ovulação Billings Erik OdebladDokumen31 halamanA Descoberta de Diferentes Tipos de Muco Cervical e o Método de Ovulação Billings Erik OdebladClaudioeTatiane MacedoBelum ada peringkat
- Sds Methode LimitationsDokumen8 halamanSds Methode LimitationsorinadeesfuerzoBelum ada peringkat
- Doctors Order Form D4Dokumen1 halamanDoctors Order Form D4Marielle ChuaBelum ada peringkat
- 36450378Dokumen109 halaman36450378Seiba PerezBelum ada peringkat
- IonnyDokumen4 halamanIonnyLu KaBelum ada peringkat
- Virtual Long Bone DissectionDokumen2 halamanVirtual Long Bone Dissectionapi-438665079Belum ada peringkat
- XareltofinalDokumen2 halamanXareltofinalMuniba NasimBelum ada peringkat
- Simultaneous Determination of Methylparaben + Propylparaben + Hidrocortisone Topical Cream PDFDokumen7 halamanSimultaneous Determination of Methylparaben + Propylparaben + Hidrocortisone Topical Cream PDFNájla KassabBelum ada peringkat
- Role, Prospects, and Limitation of HomoeopathyDokumen43 halamanRole, Prospects, and Limitation of HomoeopathyDr.bhagyaBelum ada peringkat
- Acceleration of Tibial Fracture Healing by Non Invasive Low Intensity UltrasoundDokumen9 halamanAcceleration of Tibial Fracture Healing by Non Invasive Low Intensity UltrasoundRinto Sapta Andreas SimanjuntakBelum ada peringkat
- Carte PsihiatrieDokumen9 halamanCarte PsihiatrieInna CazacliuBelum ada peringkat
- Teratogenic ItyDokumen8 halamanTeratogenic ItyValentin IanaBelum ada peringkat
- Introduction To SpineDokumen29 halamanIntroduction To Spinebmahmood1Belum ada peringkat
- Leaflet of Bach Therapy PDFDokumen2 halamanLeaflet of Bach Therapy PDFPrakash VerekarBelum ada peringkat
- Interns 2016 DistributionDokumen13 halamanInterns 2016 DistributionKashish ChawlaBelum ada peringkat
- Contract For External SupervisionDokumen2 halamanContract For External SupervisionMarkTLFBelum ada peringkat
- Name: Shafiq Ur Rahman Class No. 36 BSN Year-Iii, Semester-Vi Topic: "Reflection On Subject of Mental Health Nursing"Dokumen3 halamanName: Shafiq Ur Rahman Class No. 36 BSN Year-Iii, Semester-Vi Topic: "Reflection On Subject of Mental Health Nursing"Shafiq Ur RahmanBelum ada peringkat
- Long-Term Prediction of Functional Outcome After Stroke Using Single Items of The Barthel Index at Discharge From Rehabilitation CentreDokumen7 halamanLong-Term Prediction of Functional Outcome After Stroke Using Single Items of The Barthel Index at Discharge From Rehabilitation CentretitinBelum ada peringkat
- Minimalist Shoes Running Intervention Can Alter The Plantar Loadingdistribution and Deformation of Hallux Valgus A Pilot StudyDokumen7 halamanMinimalist Shoes Running Intervention Can Alter The Plantar Loadingdistribution and Deformation of Hallux Valgus A Pilot StudyGourgen GevorgyanBelum ada peringkat
- Neural Tube DefectsDokumen2 halamanNeural Tube DefectsVijay SluBelum ada peringkat