Hernia
Diunggah oleh
Franciscus BuwanaHak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Hernia
Diunggah oleh
Franciscus BuwanaHak Cipta:
Format Tersedia
Hernia
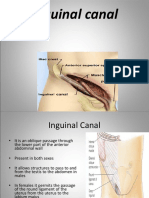
Inguinal Hernia
Shirin Towfigh, MD, and Leigh Neumayer, MD, MS
OVERVIEW
Inguinal hernia repair remains the most common general surgical
procedure in the United States, with over 800,000 performed annually. It has a long history, and thus a wide variety of techniques have
been described. The goals of inguinal hernia repair, however, remain
the same for all techniques: to provide long-lasting, secure closure of
the pelvic floor defect, reduce pain, and improve quality of life. In
modern-day repair, recurrence after hernia repair has remained fairly
low. A concerning trend is the increase in chronic pain seen after
inguinal hernia repair. Though mesh implantation has been associated with this trend, most believe that chronic pain is a result of
surgical technique, difficulty with identification of hernia anatomy,
and other unknown patient factors. In this chapter, we review diagnosis of inguinal hernias among adults, common procedures for
inguinal hernia repair and their expected outcomes, and the issue of
chronic postinguinal herniorrhaphy pain.
DIAGNOSIS
Patients with inguinal hernias may present with complaints of a
painless bulge, pain in the groin without a bulge, or some variation
in between. It is very important to accurately document the preoperative symptoms and confirm that they are consistent with an inguinal hernia. Some patients may have other causes for their symptoms,
such as epididymitis, testicular pain, or endometriosis. Symptoms
from an inguinal hernia may include a burning or pinching sensation
in the groin. The pain may radiate into the scrotum, labia, or vagina,
down the leg, or around the back. They may have worsening pain
with prolonged sitting, prolonged standing, bending, coughing,
straining, getting out of a car, or toward the end of the day. Lying flat
almost always results in improvement of their symptoms. Women
may also report worse pain during their menses. Obstructive symptoms may include bloatedness, nausea, and vomiting.
Inguinal hernias are most commonly seen in men and are of the
indirect typethat is, the result of a patent processus vaginalis. These
hernias typically present with a bulge in the groin that may extend
into the scrotum or labia. A less common variant, an interstitial
hernia, dissects within the oblique muscle layers and presents with
an oblong bulge extending superolaterally. Direct hernias are a result
of weakness in the transversalis fascia and are more commonly seen
in older males. Femoral hernias are rare and typically seen in women,
as their pelvis is broad and the femoral space is wider. This compares
to the narrow pelvis of males where the myoaponeurosis attaches at
a different angle, resulting in downward forces merging onto a larger
myopectineal orifice of Fruchaud (Figure 1).
Hernia development is considered to be due to genetic factors as
well as acquired factors. Patients with inguinal hernias have been
shown to have a higher proportion of immature type III collagen as
compared to type I collagen. Patients with a family history of hernia
are four times more likely to have an inguinal hernia. Medical diseases that have been associated with a higher risk of inguinal hernia
include aneurysmal disease, other collagen disorders, hiatal hernia,
and sleep apnea. In addition, it is commonly believed, though never
scientifically proven, that increases in abdominal pressure contribute
to the development of hernia. Such activities include straining due
to constipation or prostatic hypertrophy, chronic cough or clearing
of the throat, and heavy lifting as part of a daily job. Exercise has been
shown to have a protective effect on hernia development. It is important to control for these risk factors preoperatively in order to
improve outcomes after hernia repair.
Diagnosis of a hernia is based primarily on physical exam. The
patient is examined in the standing position to allow for gravity to
accentuate any findings. Standing alone may demonstrate a bulge,
and attempts should be made to reduce it. In men, the examiners
digit is used to follow the spermatic cord cephalad into the inguinal
canal by using the redundancy of the scrotal skin. There, the internal
ring may be entered, and also the direct space can be examined for
weakness. A cough or valsalva by the patient may be necessary if the
initial exam is not diagnostic. The femoral space is examined by
pressing medially in the groin just cephalad to the pubic bone. In
women, the inguinal exam is often not as obvious, because many do
not have a palpable bulge, defect, or reducible mass. If that is the case,
the examiner may be able to elicit pain while pressing at the internal
ring. This is suggestive of a hernia as the cause of the patients pain,
and further workup may be necessary. Femoral hernias, when palpable on examination, present as bulges below (caudad) the inguinal
ligament. The bulge can be found just medial to the femoral pulse
and frequently feels like a lipoma or lymph node. The differential
diagnosis for a mass in this location must include femoral hernia.
If the exam is suggestive of a hernia, such as pain or mild fullness
at the internal ring, without palpable mass or defect, and the history
is also suggestive of a hernia, then radiologic studies may be considered before proceeding to surgery. These include ultrasound, herniogram, computed tomographic (CT) scan, or magentic resonance
imaging (MRI). All of these studies can be performed in dynamic
mode, with valsalva, to accentuate small hernias.
INGUINAL HERNIA REPAIR
Repair of the inguinal hernia should be timed to provide the most
benefit to the patient and the least risk from the procedure. It was
considered at one time that all inguinal hernias should be repaired
531
Downloaded from ClinicalKey.com at Universitas Kristen Duta Wacana on March 19, 2016.
For personal use only. No other uses without permission. Copyright 2016. Elsevier Inc. All rights reserved.
532
Inguinal Hernia
FIGURE 1 Female pelvis (left)
and male pelvis (right). (From
Drake RL, Vogl AW, Mitchell AWM,
et al: Grays atlas of anatomy,
Philadelphia, 2007, Churchill
Livingstone.)
to reduce the morbidity and mortality associated with potential
incarceration or strangulation. Based on two prospective clinical
trials in men with asymptomatic or minimally symptomatic inguinal
hernias, the option of watchful waiting has been shown to be of low
risk. In one trial, the risk of incarceration among patients randomized to the watchful waiting arm was calculated as 0.18% per year.
No patient had a strangulated hernia during the trial period (2-4.5
years). In the second trial, only males age 55 and over were enrolled.
Among this population, patients in the watchful waiting trial were
more likely to suffer from a debilitating medical complication such
as stroke or heart attack, thus rendering them poor candidates for
elective inguinal hernia repair in the future. However, there were no
hernia-related complications during the watchful waiting period. A
commonly accepted practice now is to offer elective inguinal hernia
repair to patients physically fit for surgery and to patients with symptomatic inguinal hernias. The timing of the repair is rarely urgent
unless there is a known incarceration episode. In those at higher risk
for perioperative complications or for minimally symptomatic
patients not wishing to undergo repair at this time, watchful waiting
is considered a safe option.
Femoral hernias, unlike other inguinal hernias, are associated
with a much higher risk of incarceration or strangulation. One third of
all femoral hernias are repaired emergently, compared to 6% of all
inguinal hernias. Thus, repair is recommended for all patients with
femoral hernias.
Tissue Repair
The technique of nonmesh or tissue repair dates back to ancient
Egypt. Hundreds of techniques have been described since. Though
mesh repair has become the standard in the United States, tissue
repair remains the primary technique across the world and is growing
in its application in the United States due to the increased concern
with chronic pain. Tissue repair is considered to be superior to mesh
repair in terms of chronic pain, though most studies show that acute
postoperative pain and hernia recurrence are significantly worse
when mesh is not used. Tissue repair is indicated for patients at risk
for mesh infection, such as with a strangulated hernia requiring
bowel resection. Also, it should be considered for patients at higher
risk for chronic pain, such as women and those who present with a
history of chronic pain.
The type of tissue repair and its outcome is dependent on technique and surgeon experience. No single technique is considered to
be superior. The surgeon should be familiar with at least one or two
techniques and perfect them in order to have the best outcome. All
tissue repairs share a similar concept: closure of the defect and reinforcing the pelvic floor. A relaxing incision is often incorporated to
reduce the tension on the repair. Repairs are performed with permanent suture.
The Marcy repair is a primary closure of the internal ring defect
alone, without any further reinforcement of the pelvic floor. It is most
often used for children because the recurrence rate is considered too
high among adults.
The Bassini and McVay repairs involve opening the pelvic floor
transversely and reducing all preperitoneal contents and the hernia
sac back into the abdominal cavity. It is not necessary to resect the
hernia sac if it can be successfully reduced. For the Bassini repair, one
reapproximates the tissues by sewing the conjoint tendon to the
inguinal ligament. For the McVay repair, the conjoint tendon is
sutured to Coopers ligament, thus patching the femoral space as well.
Then, at the level of the femoral vein, a transition suture is used to
continue the approximation from the conjoint tendon to the inguinal
ligament. The suture line for both repairs starts medially at the anterior rectus fascia overlying the pubic tubercle and ends laterally at
the internal ring. Suturing is in interrupted fashion using permanent
suture. Care must be taken not to entrap the ilioinguinal, iliohypogastric, and genitofemoral nerve branches. The external oblique is
then closed over this repair.
The Shouldice repair involves step-by-step layered closure of the
pelvic floor. Pelvic floor dissection is similar to the Bassini and McVay
(Figure 2, A). Classically, the cremasteric muscle is resected, including
the genital branch of the genitofemoral nerve. For the hernia repair,
starting medially at the pubic tubercle, the lower edge of transversalis
fascia is sutured in running fashion to the underside of the upper
edge, with partial thickness bites of the transversus abdominis and
internal oblique (Figure 2, B). This continues laterally. At the internal
ring, the proximal stump of cremasteric muscle enveloping the spermatic cord is included, and the suture line is reversed (Figure 2, C).
In this second suture line, full-thickness bites of the upper edge of
the transversalis fascia is sutured to the inguinal ligament below
(Figure 2, D). Once completed medially, this suture end is tied to the
tail of the first suture line. The third suture line begins laterally at the
internal ring. The external oblique just above the inguinal ligament
is sutured to partial-thickness bites of the internal oblique from the
superior flap (Figure 2, E). This is continued medially toward the
anterior rectus fascia overlying the pubic tubercle and reversed for
the fourth and final suture line, which involves another layer of
external oblique from the lower edge sewn to the internal oblique of
the superior flap (Figure 2, F). To prevent ptosis of the testicle, the
distal end of the cremasteric muscle stump is sutured to the anterior
rectus fascia at the pubic tubercle or included in the external ring
closure.
Mesh Repair
The gold standard in the United States involves implantation of
mesh. It has been shown to provide a secure repair with little or no
tension, as compared with tissue repair. Also, since most patients have
Downloaded from ClinicalKey.com at Universitas Kristen Duta Wacana on March 19, 2016.
For personal use only. No other uses without permission. Copyright 2016. Elsevier Inc. All rights reserved.
533
H ERNI A
int. oblique
int. oblique
ext. oblique
ext. oblique
iliohypogastric
nerve
ilioinguinal nerve
ilioinguinal
nerve
iliohypogastric
nerve
spermatic cord
epigastric vessels
epigastric vessels
spermatic cord
flap of int. oblique,
trans. abdominus,
transversalis fascia
stump of cremasteric
muscle
stump of cremasteric
muscle
flap of ext. oblique
(reflected back)
shelving border
of inguinal lig.
spermatic veins in
cord space of Bogros transversalis
fascia
(under trans. fascia)
flap of ext. oblique
(reflected back)
spermatic
cord
transversalis
fascia
shelving border
of inguinal lig.
iliohypogastric
nerve
ext. oblique
ext. oblique
iliohypogastric
nerve
ilioinguinal nerve
ilioinguinal
nerve
spermatic cord
2nd line of repair
stump of
cremasteric muscle
flap of int. oblique,
trans. abdominus,
transversalis fascia
spermatic cord
flap of int. oblique,
trans. abdominus,
transversalis fascia
flap of ext. oblique
(reflected back)
spermatic transversalis
cord
fascia
shelving
border of
inguinal lig.
spermatic
cord
1st line shelving border
of sutures of inguinal lig.
ext. oblique
ext. oblique
int. oblique
ilioinguinal nerve
ilioinguinal nerve
int. oblique
iliohypogastric
nerve
3rd line of repair
spermatic cord
3rd line of repair
iliohypogastric
nerve
spermatic cord
4th line of
repair
2nd line of
repair
flap of ext. oblique
(reflected back)
spermatic
cord
flap of ext. oblique
(reflected back)
shelving
border of
inguinal lig.
spermatic
flap of ext. oblique
cord
(reflected back)
FIGURE 2 Shouldice hernia repair. A, Splitting of the transversalis fascia from the internal ring to the pubic crest as far as desired. B, First
suture line continues to tack the lateral flap of transversalis fascia to the transversalis fascia lying medially beneath the rectus, transversus
abdominis, and internal oblique muscles. C, Reconstruction of the internal ring incorporating transversalis fascia and the proximal stump of
cremasteric muscle. D, Second suture line carrying the previously established medial flap of tissue to the curved or shelving edge of the
inguinal ligament. E, The undersurface of the external oblique close to inguinal ligament is now in this third line of sutures being tacked over the
internal oblique. F, The fourth line of sutures tacks more of the lower flap of the external oblique over the internal oblique. (From Shouldice EB:
The Shouldice repair for groin hernias, Surgical Clinics of North America 83:11631187, 2003.)
Downloaded from ClinicalKey.com at Universitas Kristen Duta Wacana on March 19, 2016.
For personal use only. No other uses without permission. Copyright 2016. Elsevier Inc. All rights reserved.
534
Inguinal Hernia
intrinsically weak pelvic floor tissue or may have a wide defect with
absent tissue, the implant can augment the security of repair by
bolstering the muscles or bridging the defect. Hernia recurrence rates
using mesh implantation are typically under 5% nationally and are
reported by experts to be less than 1%. This compares to recurrence
after elective tissue repair, which may reach as high as 15% to 20%,
depending on the patient characteristics and surgical technique
performed. There are a multitude of hernia mesh biomaterials and
techniques that have been developed. Outcomes are variable and
dependent on surgeon technique and expertise. No single repair is
considered to be superior. For the best outcome, it is important that
the surgeon be informed about the risks and benefits of each implant
and to know the correct surgical technique recommended for the
chosen mesh biomaterial.
The onlay patch repair, reported by Lichtenstein and modified by
Amid, is one of the most commonly performed inguinal hernia
repairs with mesh. After the hernia sac and fat are reduced, flat mesh,
8 15cm or 3 6 inches, is sutured in running fashion starting
inferomedially at the anterior rectus fascia over the pubic tubercle
and continuing along the ilioinguinal ligament, stopping at the internal ring. A few interrupted sutures are placed at the superior edge of
the mesh. Care is taken to place sutures only in conjoint tendon and
anterior rectus fascia, as the iliohypogastric nerve runs through the
internal oblique muscle layer and can be entrapped if sutures are
placed through this muscle. A lateral slit in the mesh accommodates
the spermatic cord or round ligament. The round ligament can be
sacrificed in most women, so a slit may not be necessary. In the Amid
modification of this repair, the tails of the mesh are sutured to each
other laterally at the level of the inguinal ligament, thus forming a
three-dimensional tunnel for the recreated internal ring (Figure 3).
This conforms to the contour of the pelvis and has lower risk of ring
tightness as compared to the keyhole technique. The lateral tails of
the mesh are tucked under the external oblique. For large indirect
hernias, some advocate narrowing the internal ring with absorbable
suture. For direct hernias, it is recommended to imbricate the
Iliohypogastric n.
External oblique
aponeurosis
Internal oblique m.
and aponeurosis
Iliolinguinal n.
External
spermatic v.
Genital branch
of genitofemoral n.
Pubic tubercle
FIGURE 3 Amid modification of Lichtenstein open inguinal hernia
repair with mesh. Mesh is sized to overlap with pubic tubercle,
inguinal ligament, and conjoint tendon, typically 3 6 inches. Note the
interrupted sutures or staples placed in conjoint tendon, with care
not to entrap iliohypogastric nerve. Laterally, the tails of the mesh are
secured to each other and the inguinal ligament with a single suture
or staple. (Image courtesy of PK Amid, MD.)
redundant transversalis fascia, using absorbable sutures prior to
placing the onlay patch.
The multi-institutional European TIMELI trial compared the traditional Lichtenstein repair with sutures to a similar repair spraying
fibrin glue to anchor the mesh. Patients had body mass index (BMI)
under 35kg/m2 and nonscrotal, nonincarcerated inguinal hernias.
Results showed no significant difference in recurrence between the
two groups (0.94% overall). The patients with fibrin glue had significantly lower moderate to severe pain or groin discomfort at 12
months (8.1% vs 14.8%). More experience is being gained with nonsuture techniques of mesh repair using tissue glue or implanting
self-adhering mesh.
The mesh plug technique was introduced to reduce the amount
of dissection necessary and thus reduce postoperative pain. Plugs are
variable in their construction. They are typically placed through the
defect after highly dissecting out the hernia sac and confirming wide
retromuscular dissection free of retroperitoneal fat. Some plugs have
an outer leaflet that can be positioned in this retromuscular space,
essentially resulting in a small sublay repair. Other plugs are developed as a space occupying implant, thus requiring an onlay mesh
repair with a second flat patch of mesh.
The sandwich repair, such as that pioneered by Gilbert, involves
a two-layer mesh repair. The anterior leaflet of this mesh is placed as
an onlay, similar to the Lichtenstein repair. It may or may not require
suturing. Gilbert recommends only an anchoring stitch placed medially. The posterior leaflet of the mesh is placed in the retromuscular,
preperitoneal space, providing a sublay repair. With this repair, it is
important that the hernia sac is dissected highly and that the retromuscular preperitoneal space is widely dissected free of all fat and
adhesions in order to accommodate this mesh.
Since mesh implantation induces an inflammatory process in the
groin, chronic pain and postoperative swelling can be greater with
this procedure than with tissue repair. Recent studies are suggesting
a lower inflammatory response and less postoperative chronic pain
and swelling with lightweight mesh biomaterials, defined as weighing
less than 40g/m2. The recurrence rate of these products may be
slightly higher than that of normal-weight mesh, also referred to as
heavyweight mesh, defined as weighing 90g/m2 or greater. One study
reports a 3% absolute increase in hernia recurrence rate when using
lightweight mesh.
Laparoscopic repair is growing in popularity as more surgeons are
gaining experience with the preperitoneal anatomy and the surgical
technique. It has been associated with shorter recovery time and less
postoperative pain. The learning curve is high and directly related to
outcome. Expert surgeons with experience performing 250 or more
laparoscopic cases can provide this repair to their patients with lower
complication rates and lower recurrence rates as compared to the
open repair. Laparoscopic repair involves dissection of the peritoneal
sac and preperitoneal fat from the posterior abdominal wall and
pelvic floor. The dissection can be performed totally extraperitoneally (TEP) or transabdominally with a preperitoneal dissection
(TAPP). No single technique is considered superior, and the outcome
is dependent on surgical technique and surgeon experience. It is
important, however, that the surgeon performing the TEP technique
also be facile with the TAPP technique, because conversion from TEP
to TAPP may be necessary due to adhesions, scarring, large hernia,
or other confounding factors.
The principles of laparoscopic technique include safely reducing
the peritoneal hernia sac without injuring the external iliac vessels,
bladder, or intraperitoneal organs. For this reason, most large scrotal
hernias and some incarcerated hernias are not performed laparoscopically. The mesh is placed retromuscularly and extraperitoneally.
It is important that the dissection be complete and wide, examining
all three potential areas of hernia development in the myopectineal
orifice: indirect, direct, and femoral spaces. Also, spermatic cord
lipomas should be carefully dissected off prior to mesh placement.
This may not be as evident during laparoscopic dissection as with an
open dissection. The mesh size used is 10 15cm or 4 6 inches.
Downloaded from ClinicalKey.com at Universitas Kristen Duta Wacana on March 19, 2016.
For personal use only. No other uses without permission. Copyright 2016. Elsevier Inc. All rights reserved.
H ERN I A
535
For most indirect hernias, the mesh can be placed without fixation
or with the use of tissue glue alone. For direct hernias, the mesh
should provide wide overlap medially and be fixed with permanent
fixation. When using a fixation device, care should be taken not to
injure the bladder inferomedially; external iliac vessels, genitofemoral
nerves, and lateral femoral cutaneous nerves inferolaterally; and the
ilioinguinal and iliohypogastric nerves superolaterally.
For patients with large scrotal hernias, with loss of pelvic floor
domain, or with bilateral inguinal hernias that are not amenable to
laparoscopic repair, the Stoppa repair is a tension-free technique that
can offer long-lasting repair. It is also known as a giant prosthetic
reinforcement of the visceral sac. Essentially, it is a wide preperitoneal
repair that involves implantation of a flat piece of mesh from left to
right anterior superior iliac spine in the transverse dimension and
from mid-anterior rectus muscle to sacrum in the longitudinal
dimension. It can also be modified for unilateral hernias.
CHRONIC POSTINGUINAL
HERNIORRHAPHY PAIN
Surgical techniques for inguinal hernia repair have advanced rapidly
in the past few decades. With the introduction of mesh implantation
in the 1980s, average hernia recurrence rates have dramatically
reduced. Recurrence rates are now less than 5% overall and less than
1% as reported by most experts. Thus, most of the efforts toward
advancement of hernia repair have been concentrated on developing
techniques and biomaterials that reduce operating time, reduce surgical incision length and dissection, and reduce postoperative pain
and recovery time.
We are now dealing with the phenomenon of chronic postinguinal herniorrhaphy groin pain, or inguinodynia. Chronic pain, defined
as persistent pain lasting longer than 3 months postoperatively, is
reported to be 15% to 33%. Three percent of patients suffer from
severe debilitating pain. With over 800,000 inguinal hernia repairs
performed annually in the United States, a large number of patients
are suffering from pain due to their operation. A recent hernia database using the Caroline Comfort Scale for preoperative and postoperative evaluation of patients followed patients for up to 2 years
postoperatively. Results showed that young patients and women are
at highest risk for chronic pain. It is important to carefully evaluate
the symptoms of all patients preoperatively, counsel patients about
the risk of chronic pain as part of the informed consent process, and
tailor the surgical plan and technique to meet the patients specific
needs.
The four main causes of chronic postoperative pain include
hernia recurrence, mesh-related pain, nerve-related pain, and infection. Patients with chronic pain after hernia repair may suffer from
one or a combination of these causes.
Hernia recurrence, if not obvious from exam and history, can be
confirmed by radiologic studies if necessary. These patients typically
complain of recurrence of their preoperative pain. Their pain may
be activity-related. The pain is relieved when lying flat. Some may
have new pain due to a missed femoral hernia or a new direct inguinal hernia. Repair of the recurrent hernia will treat this problem.
Patients with mesh-related pain may have pain due to a persistent
inflammatory reaction to the mesh. In most patients, the inflammation associated with mesh resolves with time. In a small subset, the
inflammatory reaction persists, resulting in swelling and chronic pain
in the affected area. CT scan or MRI may show an abnormal inflammatory reaction in the groin that is not typical of postoperative
changes after mesh repair. In most patients, antiinflammatory treatments such as ice packs, nonsteroidal antiinflammatory medications,
or steroid injections may relieve their discomfort. In rare cases, the
mesh must be removed.
A more common mesh-related complication is termed meshoma,
and it is due to the folding or balling of mesh (Figure 4). This is
perceived by the patient as a mass in the groin and can sometimes
FIGURE 4 Meshoma (ball of mesh) folded, with ilioinguinal nerve
entrapped within its fold (at 5:00 position).
be felt on exam. The patient typically has pain with hip flexion.
Activities such as sitting, driving, and bending are uncomfortable. It
is not unusual for the patient to prefer to stand or to slouch back
when sitting, with ipsilateral leg extended. Radiologic studies may
confirm this diagnosis by showing a thickened pelvic floor or a
foreign body mass with adjacent mass effect, such as distortion of the
bladder. Removal of the mesh is the only treatment for this problem.
Neuropathic pain may be due to direct nerve injury at the time
of hernia surgery, ingrowth of the mesh into a nerve, entrapment of
the nerve by suture, fixation material, scar tissue or a fold in the mesh
(see Figure 4), or impingement on the nerve from the mass effect of
a meshoma. These patients typically have a burning pain or electrical
shooting sensation in the dermatome of the affected nerve. Any
external pressure from belts, jeans, or underpants causes discomfort.
Diagnostic testing includes a local nerve block. Treatment may
include serial nerve blocks, topical lidocaine patch, nerve ablation, or
neurectomy. The mesh may or may not need to be removed.
An active infection of the mesh will present with purulent drainage from the wound or a fluid collection around mesh implant. In
some patients, their mesh can be seeded from bacteremia, such as
tooth infection. They may present with a chronic infection, resulting
in pain and intermittent swelling in the groin. They may also have
associated constitutional symptoms such as fever, night sweats,
fatigue, or joint pain. Radiologic study may show an inflammatory
reaction, thickening of the soft tissue, or a fluid collection with or
without gas. Antibiotics alone will improve their symptoms. In most
cases, mesh removal is necessary.
Regardless of the cause of the chronic pain, it is important that
the surgeon address this issue in a timely manner. Urologists and pain
management specialists may also be consulted to help address the
patients needs. Early treatment of the cause of chronic pain provides
the best outcome.
Suggested Readings
Alfieri S, Amid PK, Campanelli G, et al: International guidelines for prevention and management of post-operative chronic pain following inguinal
hernia surgery, Hernia 15:3949, 2011.
Amid PK: Lichtenstein tension-free hernioplasty: its inception, evolution, and
principles, Hernia 8:17, 2004.
Campanelli G, Pascual MH, Hoeferlin A, et al: Randomized, controlled,
blinded trial of Tisseel/Tissucol for mesh fixation in patients undergoing
Lichtenstein technique for primary inguinal hernia repair. Results of the
TIMELI trial, Ann Surg 255(4):650657, 2012.
Downloaded from ClinicalKey.com at Universitas Kristen Duta Wacana on March 19, 2016.
For personal use only. No other uses without permission. Copyright 2016. Elsevier Inc. All rights reserved.
Fitzgibbons RJ Jr, Giobbie-Hurder A, Gibbs JO, et al: Watchful waiting vs
repair of inguinal hernia in minimally symptomatic men: a randomized
prospective clinical trial, JAMA 295(3):285292, 2006.
Neumayer L, Giobbie-Hurder A, Jonasson O, et al: Open mesh versus laparoscopic mesh repair of inguinal hernia, N Engl J Med 350:18191827, 2004.
ODwyer PJ, Norrie J, Alani A, et al: Observation or operation for patients
with asymptomatic inguinal hernia: A randomized clinical trial, Ann Surg
244(2):167173, 2006.
Shouldice EB: The Shouldice repair for groin hernias, Surg Clin North Am
83:11631187, 2003.
Simons MP, Aufenacker T, Bay-Nielsen M, et al: European Hernia Society
guidelines on the treatment of inguinal hernia in adult patients, Hernia
13:343403, 2009.
Downloaded from ClinicalKey.com at Universitas Kristen Duta Wacana on March 19, 2016.
For personal use only. No other uses without permission. Copyright 2016. Elsevier Inc. All rights reserved.
Anda mungkin juga menyukai
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDari EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryPenilaian: 3.5 dari 5 bintang3.5/5 (231)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Dari EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Penilaian: 4.5 dari 5 bintang4.5/5 (119)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDari EverandNever Split the Difference: Negotiating As If Your Life Depended On ItPenilaian: 4.5 dari 5 bintang4.5/5 (838)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDari EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaPenilaian: 4.5 dari 5 bintang4.5/5 (265)
- The Little Book of Hygge: Danish Secrets to Happy LivingDari EverandThe Little Book of Hygge: Danish Secrets to Happy LivingPenilaian: 3.5 dari 5 bintang3.5/5 (399)
- Grit: The Power of Passion and PerseveranceDari EverandGrit: The Power of Passion and PerseverancePenilaian: 4 dari 5 bintang4/5 (587)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDari EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyPenilaian: 3.5 dari 5 bintang3.5/5 (2219)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDari EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifePenilaian: 4 dari 5 bintang4/5 (5794)
- Team of Rivals: The Political Genius of Abraham LincolnDari EverandTeam of Rivals: The Political Genius of Abraham LincolnPenilaian: 4.5 dari 5 bintang4.5/5 (234)
- Rise of ISIS: A Threat We Can't IgnoreDari EverandRise of ISIS: A Threat We Can't IgnorePenilaian: 3.5 dari 5 bintang3.5/5 (137)
- Shoe Dog: A Memoir by the Creator of NikeDari EverandShoe Dog: A Memoir by the Creator of NikePenilaian: 4.5 dari 5 bintang4.5/5 (537)
- The Emperor of All Maladies: A Biography of CancerDari EverandThe Emperor of All Maladies: A Biography of CancerPenilaian: 4.5 dari 5 bintang4.5/5 (271)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDari EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You ArePenilaian: 4 dari 5 bintang4/5 (1090)
- Her Body and Other Parties: StoriesDari EverandHer Body and Other Parties: StoriesPenilaian: 4 dari 5 bintang4/5 (821)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDari EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersPenilaian: 4.5 dari 5 bintang4.5/5 (344)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDari EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RacePenilaian: 4 dari 5 bintang4/5 (890)
- CASE PRESENTATION Nadhirah RahimDokumen60 halamanCASE PRESENTATION Nadhirah RahimNadhirah Rahim100% (1)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDari EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FuturePenilaian: 4.5 dari 5 bintang4.5/5 (474)
- The Unwinding: An Inner History of the New AmericaDari EverandThe Unwinding: An Inner History of the New AmericaPenilaian: 4 dari 5 bintang4/5 (45)
- The Yellow House: A Memoir (2019 National Book Award Winner)Dari EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Penilaian: 4 dari 5 bintang4/5 (98)
- On Fire: The (Burning) Case for a Green New DealDari EverandOn Fire: The (Burning) Case for a Green New DealPenilaian: 4 dari 5 bintang4/5 (73)
- 3-Inguinal Canal PDFDokumen58 halaman3-Inguinal Canal PDFN A0% (1)
- Exam of Scrotal SwellingDokumen8 halamanExam of Scrotal Swellingprasanth bylapudiBelum ada peringkat
- Usmle Step1 MCQ Study Online Questions ReviewDokumen13 halamanUsmle Step1 MCQ Study Online Questions ReviewfrabziBelum ada peringkat
- Cryptorchidism: Undescended TestisDokumen9 halamanCryptorchidism: Undescended TestisemirilejlaBelum ada peringkat
- Heart Lung Abdomen ExamDokumen1 halamanHeart Lung Abdomen ExamJOUO20009167Belum ada peringkat
- Matary Operative 2011 PDFDokumen125 halamanMatary Operative 2011 PDFjd4730Belum ada peringkat
- Surgery PracticalsDokumen24 halamanSurgery PracticalsAparna DeviBelum ada peringkat
- HERNIADokumen34 halamanHERNIAAtiqah ShahBelum ada peringkat
- Atlas of General SurgeryDokumen620 halamanAtlas of General SurgeryzeparionBelum ada peringkat
- Recfognizing Interstitiil and Air Space DiseaseDokumen2 halamanRecfognizing Interstitiil and Air Space DiseaseFranciscus BuwanaBelum ada peringkat
- Tetanus PDFDokumen26 halamanTetanus PDFFranciscus BuwanaBelum ada peringkat
- 1 s2.0 S0021915008005315Dokumen6 halaman1 s2.0 S0021915008005315Franciscus BuwanaBelum ada peringkat
- Genetics / Newborn / Chromosomal DisorderDokumen2 halamanGenetics / Newborn / Chromosomal DisorderFranciscus BuwanaBelum ada peringkat
- Cmanagement of Tremor, Chorea, Dystonia, Myoclonus and AtaxiaDokumen89 halamanCmanagement of Tremor, Chorea, Dystonia, Myoclonus and AtaxiaFranciscus BuwanaBelum ada peringkat
- Bronchiolitis ObliteranDokumen8 halamanBronchiolitis ObliteranFranciscus BuwanaBelum ada peringkat
- LiverDokumen2 halamanLiverFranciscus BuwanaBelum ada peringkat
- Cardiovascular DiseaseDokumen2 halamanCardiovascular DiseaseFranciscus BuwanaBelum ada peringkat
- RespiratoryDokumen2 halamanRespiratoryFranciscus BuwanaBelum ada peringkat
- EncephalitisDokumen3 halamanEncephalitisFranciscus BuwanaBelum ada peringkat
- Thoracic RadiculopathyDokumen6 halamanThoracic RadiculopathyFranciscus BuwanaBelum ada peringkat
- Brain VascularisationDokumen33 halamanBrain VascularisationFranciscus BuwanaBelum ada peringkat
- PediatricsDokumen2 halamanPediatricsFranciscus BuwanaBelum ada peringkat
- Urologi JKMDokumen80 halamanUrologi JKMFranciscus BuwanaBelum ada peringkat
- Urologi JKMDokumen80 halamanUrologi JKMFranciscus BuwanaBelum ada peringkat
- Gagal GinjalDokumen44 halamanGagal GinjalFranciscus BuwanaBelum ada peringkat
- Childhood psoriasis literature reviewDokumen9 halamanChildhood psoriasis literature reviewFranciscus BuwanaBelum ada peringkat
- VERTIGO (Compatibility Mode)Dokumen28 halamanVERTIGO (Compatibility Mode)Franciscus BuwanaBelum ada peringkat
- NYERI KEPALA: PENGELOLAAN YANG TEPATDokumen39 halamanNYERI KEPALA: PENGELOLAAN YANG TEPATFranciscus BuwanaBelum ada peringkat
- Osteoarthritis FFDokumen4 halamanOsteoarthritis FFPutra DhyatmikaBelum ada peringkat
- Pharmacotherapy of Parkinson DISEASE3 PDFDokumen53 halamanPharmacotherapy of Parkinson DISEASE3 PDFFranciscus BuwanaBelum ada peringkat
- Pain (: Nociceptic and Neuropathic) Nociceptic and Neuropathic)Dokumen50 halamanPain (: Nociceptic and Neuropathic) Nociceptic and Neuropathic)Franciscus BuwanaBelum ada peringkat
- Comparation Effect of Azitromycin Gel With Clindamycin in Patient With AcneDokumen10 halamanComparation Effect of Azitromycin Gel With Clindamycin in Patient With AcneFranciscus BuwanaBelum ada peringkat
- Use Oral Contraceptive For Management of Acne Vulgaris Pratical Consideration in Real Word PracticeDokumen7 halamanUse Oral Contraceptive For Management of Acne Vulgaris Pratical Consideration in Real Word PracticeFranciscus BuwanaBelum ada peringkat
- Comparation Effect of Azitromycin Gel With Clindamycin in Patient With AcneDokumen10 halamanComparation Effect of Azitromycin Gel With Clindamycin in Patient With AcneFranciscus BuwanaBelum ada peringkat
- Demographic Characteristic and Risk Factor in Turki Patient With Anogenital WartsDokumen6 halamanDemographic Characteristic and Risk Factor in Turki Patient With Anogenital WartsFranciscus BuwanaBelum ada peringkat
- Intracranial Infection in Neonatus and ChildrenDokumen12 halamanIntracranial Infection in Neonatus and ChildrenMichael WijayaBelum ada peringkat
- Acute Ureteric Colic Ultrasound As The InitialDokumen4 halamanAcute Ureteric Colic Ultrasound As The InitialFranciscus BuwanaBelum ada peringkat
- Parasites Causing Neurosensory Complaints PDFDokumen44 halamanParasites Causing Neurosensory Complaints PDFFranciscus BuwanaBelum ada peringkat
- Irfan's Shukar BookDokumen56 halamanIrfan's Shukar BookHina MalikBelum ada peringkat
- Male Genitalia FlashcardsDokumen10 halamanMale Genitalia Flashcardsaznknight323Belum ada peringkat
- Stoppa Forgotten SurgeryDokumen4 halamanStoppa Forgotten SurgeryGuilherme Kazuo OgawaBelum ada peringkat
- 0301omar Yusef Kudsi - Robotic Hernia Surgery - A Comprehensive Illustrated Guide-Springer International Publishing - Springer (2020)Dokumen25 halaman0301omar Yusef Kudsi - Robotic Hernia Surgery - A Comprehensive Illustrated Guide-Springer International Publishing - Springer (2020)ravikanthBelum ada peringkat
- Hernias: Mark A. Malangoni, Michael J. RosenDokumen28 halamanHernias: Mark A. Malangoni, Michael J. RosenHenryOeiBelum ada peringkat
- Confidential Attorney Client CommunicationDokumen15 halamanConfidential Attorney Client CommunicationPatrice AllenBelum ada peringkat
- Inguinal Hernia in A Spitz DogDokumen3 halamanInguinal Hernia in A Spitz DogDaniela VidalBelum ada peringkat
- Stoppa ModificadoDokumen6 halamanStoppa ModificadomvortopediaBelum ada peringkat
- Male Genitals and Inguinal Area-WordDokumen5 halamanMale Genitals and Inguinal Area-Wordmalyn1218Belum ada peringkat
- Step 2 CasesDokumen0 halamanStep 2 CasesSergio VillaBelum ada peringkat
- Abd Wall - Inguinal Reg. - Upnm7 - 210218Dokumen38 halamanAbd Wall - Inguinal Reg. - Upnm7 - 210218Gx NavinBelum ada peringkat
- Hernia InguinalDokumen11 halamanHernia InguinalFernando BurgoaBelum ada peringkat
- CSP - Groin LumpDokumen39 halamanCSP - Groin LumpAnnisa SakilaBelum ada peringkat
- MCQ Bedah Dasar UNAS JuliDokumen51 halamanMCQ Bedah Dasar UNAS Julifaris nagibBelum ada peringkat
- (MediNotes) HerniaDokumen1 halaman(MediNotes) HerniaMuh PaturBelum ada peringkat
- WJR 8 656Dokumen13 halamanWJR 8 656aldosaputraBelum ada peringkat
- Question Bank: Chapterwise (Wbuhs)Dokumen188 halamanQuestion Bank: Chapterwise (Wbuhs)Saikat MondalBelum ada peringkat
- Abstract's BookDokumen167 halamanAbstract's BookandreaBelum ada peringkat
- Umesh Singh. TLTK-47Dokumen5 halamanUmesh Singh. TLTK-47HẢI HOÀNG THANHBelum ada peringkat
- Ospe Answers 88Dokumen88 halamanOspe Answers 88ShreyaBelum ada peringkat