1.oestrogen and Immunomodulation - New Mechanisms That Impact On Peripheral and Central Immunity
Diunggah oleh
drindrasJudul Asli
Hak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
1.oestrogen and Immunomodulation - New Mechanisms That Impact On Peripheral and Central Immunity
Diunggah oleh
drindrasHak Cipta:
Format Tersedia
Available online at www.sciencedirect.
com
Oestrogen and immunomodulation: new mechanisms that impact
on peripheral and central immunity
Suchita Nadkarni and Simon McArthur
The regulation of the immune response to infection or tissue
damage is a complex interplay of multiple factors, but it has
long been recognised that steroid hormones can exert powerful
modulatory effects at all levels of the innate and adaptive
immune systems. Although most attention has been paid to
glucocorticoids given their widespread clinical use, it is
becoming increasingly clear that sex steroid hormones, and in
particular the principle female sex steroid oestrogen, exerts
potent effects upon the immune response. In this review, we
will discuss the latest findings on the impact of oestrogen upon
various cellular components of the immune system, and how
this hormone can offer new opportunities to pharmacologically
harness the immune response.
Addresses
Department of Biochemical Pharmacology, William Harvey Research
Institute, Barts and the London School of Medicine, Charterhouse
Square, London EC1M 6BQ, UK
Corresponding authors: Nadkarni, Suchita (s.nadkarni@qmul.ac.uk) and
McArthur, Simon (s.mcarthur@qmul.ac.uk)
Current Opinion in Pharmacology 2013, 13:576581
This review comes from a themed issue on Immunomodulation
Edited by Catherine Godson and Mauro Perretti
For a complete overview see the Issue and the Editorial
Available online 31st May 2013
1471-4892/$ see front matter, # 2013 Elsevier Ltd. All rights
reserved.
http://dx.doi.org/10.1016/j.coph.2013.05.007
Innate immunity
Following exposure to infection or tissue damage, there is
a rapid mobilisation and extravasation of neutrophils,
effectively serving as the first arm of the immune
response. Excessive or inappropriate neutrophil accumulation, or a failure in their removal by macrophages, can
induce significant damage to otherwise healthy tissue,
which can lead to both acute and chronic inflammatory
diseases. Restricting neutrophil recruitment is therefore
one of the most important ways in which oestrogen can
regulate the immune response in humans [1], as well as a
wide variety of acute [2,3] and chronic [4,5] animal
inflammatory models. A number of recent studies have
focused on the role of oestrogen in the regulation of
neutrophil recruitment, by two principle mechanisms
of action: namely the control of neutrophil chemotaxis
and the modulation of neutrophilendothelial cell interactions.
Current Opinion in Pharmacology 2013, 13:576581
Oestrogen has been shown to decrease production of the
major neutrophil chemoattractants CXCL1, CXCL2 and
CXCL3 at inflammatory sites in rodent models of intestinal [4,6], lung [3,5,6] and vascular [7] injury, an action
which directly led to decreased neutrophil accumulation.
Similarly, oestradiol has been shown to limit release of the
potent neutrophil chemoattractant CXCL8 from human
monocytes ex vivo [8]. The recruitment and extravasation
of neutrophils not only requires exposure to chemoattractant agents but also involves a series of critical interactions between neutrophils themselves and endothelial
cells. Oestrogen, or its mimetics such as resveratrol, have
recently been shown to limit adhesion of both human and
rodent neutrophils to activated endothelial cell monolayers under shear stress conditions in vitro [911] and to
vascular endothelial cells in vivo [9], directly limiting
neutrophil transmigration and tissue infiltration. Our
own studies have confirmed that this action of oestrogen
is mediated through the rapid upregulation of the wellknown anti-inflammatory protein annexin A1 on neutrophils, and that removal of this protein by either immunoneutralisation or genetic deletion abated the regulatory
effects of oestrogen upon neutrophil extravasation both in
vitro and in vivo [9], see Figure 1.
Further studies have extended the idea that oestrogen
can directly influence neutrophil activation, with both
human and rodent cells having been shown to respond to
the hormone through a reduction in oxidative metabolism
[12], a feature of potentially great importance, given that
excessive oxidative damage is the principal mechanism
whereby over-exuberant neutrophil accumulation can
injure healthy tissues. These studies support by our
recent work showing oestrogen induces a distinct
CD62Llow/anti-inflammatory neutrophil phenotype [9].
The vast majority of extravasated cells undergo apoptosis
in situ. Removal of these effete cells by monocytes and
macrophages is of critical importance for inflammatory
resolution, as apoptotic cells can rapidly progress into
secondary necrosis and become potent sources of inflammation in their own right. Phagocytic clearance of apoptotic neutrophils aids resolution not only through the
removal of potential pro-inflammatory stimuli, but
through the induction of an alternatively activated
phenotype in the phagocyte itself, accompanied by the
induction of cytokines such as IL-10 and TGFb [13].
Mice specifically lacking oestrogen receptor alpha (ERa)
expression in cells of the myeloid lineage [14!] showed
both a defect in inflammatory cell clearance by
www.sciencedirect.com
Oestrogen and immunity Nadkarni and McArthur 577
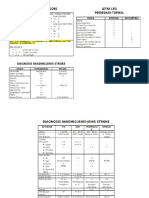
Figure 1
Neutrophil
Oestrogen induces
externalisation of Annexin A1
to the surface of the
neutrophil
Oestrogen binds to its receptor
TNF
IL-1
IL-6
CXCL1,2 3
Oestrogen
NFB
Annexin A1 inhibits
neutrophil adhesion to the
endothelial cell, preventing
potentially harmful
inflammation
IB
Target Tissue
Current Opinion in Pharmacology
Oestrogen and the neutrophil. This figure focuses on the direct effects of oestrogen upon the neutrophil, and how oestrogen can influence neutrophil
chemoattraction through actions in target tissues. In particular, the relative roles of NFkB and annexin A1 are highlighted.
macrophages, and a failure in macrophage phenotypic
conversion from classically to alternatively activated
forms. A further study revealed that oestrogen limits the
numbers of classical macrophages in atherosclerotic lesions
in monkeys fed a high cholesterol diet [15], together
suggesting an important endogenous role for oestrogen.
Oestrogen has been shown to markedly attenuate the
release of pro-inflammatory mediators such as TNFa,
IL-1b and IL-6 from both neutrophils and macrophages
in rats [16], mice [17] and humans [18!!]. Intriguingly, a
number of recent studies have identified the inhibition of
NFkB signalling by oestrogen as lying at the heart of both
these actions and in the reduction of chemokine release
from injured tissues. Oestrogen has been shown to both
enhance production [7] and limit degradation following
phosphorylation of the endogenous NFkB inhibitor
IkBa [18!!], acting via regulation of the microRNAs
let-7a and miR-125b [18!!]. Together, these actions limit
levels of NFkB nuclear translocation and hence prevent
the transcription of pro-inflammatory cytokine and chemokine genes.
www.sciencedirect.com
Together, these studies have revealed a number of
important ways through which oestrogen can regulate
the innate immune response, whether by modulation
of cytokine and chemokine production through interactions with NFkB signalling, or by direct induction of
pro-resolution phenotypes in neutrophils and macrophages through annexin A1 or ERa respectively. We
suggest that these identified mechanisms highlight the
important role of oestrogen in innate immunity, and make
a compelling case for further study of the regulatory roles
the hormone plays in the response to injury and infection.
Adaptive immunity
Balance in the immune system is tightly regulated by
concerted interactions between the professional antigen
presenting cells, dendritic cells (DCs), and T and B
lymphocytes. Dysregulation of this tolerant state can lead
to a variety of pathologies including the failure to recognise self-antigens appropriately, leading to autoimmune
diseases. Oestrogens association with the adaptive
immune system is evident through its ability to modulate
a variety of immune responses and expression of its
Current Opinion in Pharmacology 2013, 13:576581
578 Immunomodulation
receptors, ERa and ERb on T and B cells, as well as DCs
[19,20], suggesting that this hormone can regulate their
responses.
Autoimmune diseases such as rheumatoid arthritis (RA),
multiple sclerosis (MS) and systemic lupus erythematosus (SLE), can be used to highlight the distinct role
oestrogens can play on cells of the adaptive immune
system. For example, women who suffer from MS and
RA can undergo remission during pregnancy at a time
when oestrogen levels are high, but experience disease
relapse post-partum [21,22]. On the other hand, women
who suffer from SLE experience cyclical changes in their
disease during the menstrual cycle, with a worsening of
symptoms correlating with high oestrogen levels during
the cycle [23]. This differential role of oestrogen in
autoimmune diseases could be dependent on whether
the disease is B-cell mediated (such as SLE) or T cell
mediated (such as RA and MS).
Oestrogens detrimental role in SLE may be due to the
appearance of auto-antibodies against ERa; auto-antibodies targeting this receptor are capable of interfering
with T cell homeostasis, promoting their apoptosis [24].
Furthermore, oestrogen has been shown to increase antiDNA antibodies and maintain B cell survival and activation via the up-regulation of CD22 and SHP-1, resulting in decreased signalling through the B cell receptor and
subsequent induction of auto-reactive B cells [25].
Further studies have added to these findings, suggesting
the oestrogen is responsible for promoting systemic
inflammation through the induction of B cell activating
factor (BAFF) and interferon-inducible genes [26]. SLE
patients experience augmented serum levels of the type-I
interferon, IFNa, as well as over-expression of IFNarelated genes [27]. Plasmacytoid DCs (pDC) are a subset
of DC that respond to viral infections and produce IFNa
via the toll-like receptors TLR-7 and TLR-9. A recent
study has shown that oestrogen, via ERa, is capable of
promoting TLR-7/9-induced IFNa release, suggesting a
potential mechanism as to why oestrogen could be
adverse in SLE [28].
Contrary to its pathogenic effects on B cells in SLE,
oestrogen can induce a protective state in B cells in the
mouse model of multiple sclerosis, experimental autoimmune encephalitis (EAE). Administration of oestrogen
to EAE mice depleted of protective regulatory T cells
(Tregs, see below) can still induce a protective response.
Here, the authors suggest that in the absence of Tregs,
compensatory pathways are activated, resulting in the
augmentation of oestrogen-induced regulatory B cells,
with enhanced secretion of the anti-inflammatory cytokine, IL-10 [29].
DCs are professional antigen presenting cells (APC),
meaning that they are capable of processing antigen
Current Opinion in Pharmacology 2013, 13:576581
and presenting them to T cells, a process that instigates
the immune response. For this reason, DCs are often
described as bridging the gap between the innate and
adaptive immune system. The efficient presentation of
antigen relies on expression of MHC II. A recent paper
has demonstrated that oestrogen, via ERa, is capable of
promoting DC differentiation and MHC II expression, by
upregulating the transcription factor, IRF4 [30]. Oestrogen also promotes a tolerogenic phenotype in DC [31!!]
by upregulating the necessary markers for antigen presentation, as well as inhibitory molecules such as the
programme cell-death ligands, PD-L1 and PD-L2.
Additionally, oestrogen is capable of promoting the
release of the regulatory cytokines, IL-10 and TGFb,
while attenuating the release of IL-12 and ameliorating
EAE [31!!].
Tregs are a subset of T cells capable of inducing immune
tolerance, by dampening down pro-inflammatory
responses (reviewed elsewhere [32]). The role of oestrogen in immune tolerance has been further characterised
in pregnancy, where foetalmaternal tolerance is
mediated by Tregs, with an enrichment of Tregs at the
foetalmaternal interface [33]. Aberrations in the number
of Tregs and their suppressive capacity can lead to
pregnancy complications including pre-eclampsia [34]
and spontaneous abortion [35]. Oestrogen is capable of
inducing Tregs in vitro and promoting their proliferation
via the PI3K/AKT signalling pathway with a concomitant
augmentation in their suppressive capacity [36], and of
mediating Treg suppression by promoting perforin-dependent killing of effector cells [37].
Oestrogens ability to maintain immune tolerance is not
just dependent on the induction of Tregs, and its effects
have broader implications on other T cell subtypes. For
example, oestrogen has been shown to inhibit pro-inflammatory Th1 and Th17 cytokines, including IFNg, TNFa
and IL-17, in EAE, acting specifically via ERa [38!]. In
addition to inhibiting pathogenic T cells, oestrogen has
been found to limit the migration of pathogenic T cells to
the central nervous system in EAE. However, the authors
of these findings suggest that oestrogen does not directly
modulate chemokine expression on the T cell, but rather
modulates adhesion molecule expression on the endothelium, which in turn can influence T cell migration [39].
Taken together, these recent studies highlight diseasespecific actions of oestrogen within the adaptive immune
response.
Central immunity
It is a little recognised fact, but both male and female
brains are steroidogenic organs associated with a basal
production of oestrogen and that, more importantly, localised upregulation of oestrogen synthesis is one of the first
responses to brain injury [40]. Whilst many studies have
investigated a role for oestrogen as a neuroprotective
www.sciencedirect.com
Oestrogen and immunity Nadkarni and McArthur 579
agent in neurodegenerative disease [41], fewer have
directly considered its role as a regulator of the immune
cells of the brain, the microglia and astrocytes, and their
actions in neuroinflammatory disease. Several recent studies have, however, suggested that oestrogen may suppress inflammatory cytokine and chemokine gene activity
within the rodent brain under basal conditions or following traumatic injury [42,43], indicating a potential action
of the hormone upon inflammatory glia.
Whilst astrocytes are not developmentally related to
myeloid or lymphoid cells, they play an important role
in central nervous system immunity, and are fully capable
of producing and responding to inflammatory mediators.
Multiple studies have shown, moreover, that astrocytes
are potently regulated by oestrogen with the steroid
inhibiting cytokine and chemokine production in response
to both viral [44] and bacterial [45] challenge. Additionally,
astrocyte-specific deletion of ERa prevented the protective
Figure 2
Inhibit
neutrophilendothelium
interactions
Reduce
oxidative
metabolism
Promote IFN
release in SLE
Decrease neutrophil
chemoattractants
Induction of
tolerogenic DC
CH3
OH
Oestrogen
HO
Inhibition of Th1 and
Th17 cells
Maintenance of
B cell survival
in SLE
Induction of
regulatory T
cells in vitro
Enhance
apoptotic cell
clearance
Promote
macrophage
alternative
activation
Induction of
regulatory B
cells in EAE
Current Opinion in Pharmacology
Oestrogen and the immune system. This figure summarises how oestrogen can influence the phenotype and behaviour of cells of the innate and
adaptive immune system, modulating the activity of virtually every cell type involved.
www.sciencedirect.com
Current Opinion in Pharmacology 2013, 13:576581
580 Immunomodulation
effects of oestrogen in a murine model of multiple sclerosis
[46]. As with neutrophils and macrophages, these actions of
oestrogen appear to be mediated largely through modulation of NFkB signalling and the inhibition of p65 nuclear
translocation [47], further reinforcing the importance of this
signalling pathway in the actions of oestrogen upon the
immune system.
Microglia have been more closely studied in terms of their
response to oestrogen, with many of their responses akin to
those of peripheral macrophages. For example, oestrogen
has been recently shown to inhibit accumulation of microglia following rat cerebral artery occlusion, through the
prevention of CCL2 and CCL5 secretion [48]. Similarly,
treatment of microglia with oestrogen has been shown to
prevent LPS-induced secretion of the pro-inflammatory
cytokines IL-1b and TNFa via activation of both ERa and
ERb [49], confirming a potent anti-inflammatory action of
the hormone. Evidence is accumulating that oestrogen is
not only anti-inflammatory, but may actually promote
resolution within the brain, as treatment of microglia with
oestrogen has been shown to potentiate their clearance of
apoptotic cells [50], an action vital for the efficient termination of an inflammatory reaction.
Conclusion
In this review we have identified several emerging mechanisms whereby oestrogen can affect the function of the
innate, adaptive and central immune systems, features
that are common to multiple components of these systems (summarised in Figure 2). In particular, oestrogen
has clearly been shown to interact with NFkB signalling
to limit inflammatory activity, along with accumulating
evidence for a role of the hormone in regulating the antiinflammatory/pro-resolution protein annexin A1. Whilst it
must be borne in mind that actions of oestrogen in one
cell type may not necessarily be transferable to another,
these pathways represent enticing new therapeutic targets, and reveal an opportunity to exploit this powerful
hormone to develop novel anti-inflammatory treatments.
Acknowledgements
We would like to thank Dr Neil Dufton for the illustrations in this review.
This review was supported by the British Heart Foundation (PG/09/060)
and The Wellcome Trust (086867/Z/08/Z).
References and recommended reading
Papers of particular interest, published within the period of review,
have been highlighted as:
! of special interest
!! of outstanding interest
3.
Shih H-C, Huang M-S, Lee C-H: Estrogen augments the protection
of hypertonic saline treatment from mesenteric ischemiareperfusion injury. Shock (Augusta, Ga.) 2011, 35:302-307.
4.
Sheh A, Ge Z, Parry NMA, Muthupalani S, Rager JE, Raczynski AR,
Mobley MW, McCabe AF, Fry RC, Wang TC et al.: 17b-Estradiol
and tamoxifen prevent gastric cancer by modulating
leukocyte recruitment and oncogenic pathways in
Helicobacter pylori-infected INS-GAS male mice. Cancer Prev
Res (Phil PA) 2011, 4:1426-1435.
5.
Yang S-J, Chen H-M, Hsieh C-H, Hsu J-T, Yeh C-N, Yeh T-S,
Hwang T-L, Jan Y-Y, Chen M-F: Akt pathway is required for
oestrogen-mediated attenuation of lung injury in a rodent
model of cerulein-induced acute pancreatitis. Injury 2011,
42:638-642.
6.
Doucet D, Badami C, Palange D, Bonitz RP, Lu Q, Xu D-Z,
Kannan KB, Colorado I, Feinman R, Deitch EA: Estrogen receptor
hormone agonists limit trauma hemorrhage shock-induced
gut and lung injury in rats. PLoS ONE 2010, 5:e9421.
7.
Xing D, Oparil S, Yu H, Gong K, Feng W, Black J, Chen Y-F,
Nozell S: Estrogen modulates NFkB signaling by enhancing
IkBa levels and blocking p65 binding at the promoters of
inflammatory genes via estrogen receptor-b. PLoS ONE 2012,
7:e36890.
8.
Pioli PA, Jensen AL, Weaver LK, Amiel E, Shen Z, Shen L, Wira CR,
Guyre PM: Estradiol attenuates lipopolysaccharide-induced
CXC chemokine ligand 8 production by human peripheral
blood monocytes. J. Immunol 2007, 179:6284-6290.
9.
Nadkarni S, Cooper D, Brancaleone V, Bena S, Perretti M:
Activation of the annexin A1 pathway underlies the protective
effects exerted by estrogen in polymorphonuclear leukocytes.
Arterioscler Thromb Vasc Biol 2011, 31:2749-2759.
10. Rius C, Abu-Taha M, Hermenegildo C, Piqueras L, CerdaNicolas J-M, Issekutz AC, Estan L, Cortijo J, Morcillo EJ, Orallo F
et al.: Trans- but not cis-resveratrol impairs angiotensin-IImediated vascular inflammation through inhibition of NF-kB
activation and peroxisome proliferator-activated receptorgamma upregulation. J Immunol (Baltimore, MD.: 1950) 2010,
185:3718-3727.
11. Szabo A, Hartmann P, Varga R, Janvari K, Lendvai Z, Szalai I,
Gomez I, Varga G, Greksa F, Nemeth I et al.: Periosteal
microcirculatory action of chronic estrogen supplementation
in osteoporotic rats challenged with tourniquet ischemia. Life
Sci 2011, 88:156-162.
12. Golecka-Bakowska M, Mierzwinska-Nastalska E, Bychawska M:
Influence of hormone supplementation therapy on the incidence
of denture stomatitis and on chemiluminescent activity of
polymorphonuclear granulocytes in blood of menopausal-aged
women. Eur J Med Res 2010, 15(Suppl 2):46-49.
13. Savill J, Dransfield I, Gregory C, Haslett C: A blast from the past:
clearance of apoptotic cells regulates immune responses. Nat
Rev Immunol 2002, 2:965-975.
14. Ribas V, Drew BG, Le JA, Soleymani T, Daraei P, Sitz D,
!
Mohammad L, Henstridge DC, Febbraio MA, Hewitt SC et al.:
Myeloid-specific estrogen receptor alpha deficiency impairs
metabolic homeostasis and accelerates atherosclerotic
lesion development. Proc Natl Acad Sci U S A 2011, 108:1645716462.
This study demonstrates a critical role for ERa in signalling oestrogens
immune functions by elegant myeloid-specific receptor deletion.
15. Sophonsritsuk A, Appt SE, Clarkson TB, Shively CA, Espeland MA,
Register TC: Differential effects of estradiol on carotid artery
inflammation when administered early versus late after
surgical menopause. Menopause (New York, N.Y.) 2013.
1.
MacNeil LG, Baker SK, Stevic I, Tarnopolsky MA: 17b-Estradiol
attenuates exercise-induced neutrophil infiltration in men. Am
J Physiol Regulat Integr Compar Physiol 2011, 300:R1443-R1451.
16. Yu H-P, Hwang T-L, Hsieh P-W, Lau Y-T: Role of estrogen
receptor-dependent upregulation of P38 MAPK/heme
oxygenase 1 in resveratrol-mediated attenuation of intestinal
injury after trauma-hemorrhage. Shock (Augusta, Ga.) 2011,
35:517-523.
2.
Chandrasekaran VRM, Periasamy S, Liu L-L, Liu M-Y: 17bEstradiol protects against acetaminophen-overdose-induced
acute oxidative hepatic damage and increases the survival
rate in mice. Steroids 2011, 76:118-124.
17. Toyoda Y, Miyashita T, Endo S, Tsuneyama K, Fukami T,
Nakajima MYT: Estradiol and progesterone modulate
halothane-induced liver injury in mice. Toxicol Lett 2011,
204:17-24.
Current Opinion in Pharmacology 2013, 13:576581
www.sciencedirect.com
Oestrogen and immunity Nadkarni and McArthur 581
18. Murphy AJ, Guyre PM, Pioli PA: Estradiol suppresses NF-kappa
!! B activation through coordinated regulation of let-7a and miR125b in primary human macrophages. J Immunol (Baltimore,
Md.: 1950) 2010, 184:5029-5037.
This study clarifies the mechanism whereby oestrogen affects NFkB
signalling leading to its effects on cytokine and chemokine release.
19. Pierdominici M, Maselli A, Colasanti T, Giammarioli AM,
Delunardo F, Vacirca D, Sanchez M, Giovannetti A, Malorni W,
Ortona E: Estrogen receptor profiles in human peripheral blood
lymphocytes. Immunol Lett 2010, 132:79-85.
20. Sapino A, Cassoni P, Ferrero E, Bongiovanni M, Righi L,
Fortunati N, Crafa P, Chiarle R, Bussolati G: Estrogen receptor
alpha is a novel marker expressed by follicular dendritic cells
in lymph nodes and tumor-associated lymphoid infiltrates. Am
J Pathol 2003, 163:1313-1320.
21. Ostensen M, Villiger PM: The remission of rheumatoid arthritis
during pregnancy. Semin Immunopathol 2007, 29:185-191.
22. Vukusic S, Hutchinson M, Hours M, Moreau T, CortinovisTourniaire P, Adeleine P, Confavreux C, The Pregnancy in Multiple
Sclerosis Group: Pregnancy and multiple sclerosis (the PRIMS
study): clinical predictors of post-partum relapse. Brain 2004,
127:1353-1360.
23. Shabanova SS, Ananieva LP, Alekberova ZS, Guzov II: Ovarian
function and disease activity in patients with systemic lupus
erythematosus. Clin Exp Rheumatol 2008, 26:436-441.
24. Colasanti T, Maselli A, Conti F, Sanchez M, Alessandri C,
Barbati C, Vacirca D, Tinari A, Chiarotti F, Giovannetti A et al.:
Autoantibodies to estrogen receptor alpha interfere with T
lymphocyte homeostasis and are associated with disease
activity in systemic lupus erythematosus. Arthritis Rheum 2012,
64:778-787.
25. Grimaldi CM, Jeganathan V, Diamond B: Hormonal regulation of B
cell development: 17 beta-estradiol impairs negative selection
of high-affinity DNA-reactive B cells at more than one
developmental checkpoint. J Immunol 2006, 176:2703-2710.
26. Venkatesh J, Yoshifuji H, Kawabata D, Chinnasamy P,
Stanevsky A, Grimaldi CM, Cohen-Solal J, Diamond B: Antigen is
required for maturation and activation of pathogenic anti-DNA
antibodies and systemic inflammation. J Immunol 2011,
186:5304-5312.
27. Bennett L, Palucka AK, Arce E, Cantrell V, Borvak J, Banchereau J,
Pascual V: Interferon and granulopoiesis signatures in
systemic lupus erythematosus blood. J Exp Med 2003,
197:711-723.
28. Seillet C, Laffont S, Tremollieres F, Rouquie N, Ribot C, Arnal JF,
Douin-Echinard V, Gourdy P, Guery JC: The TLR-mediated
response of plasmacytoid dendritic cells is positively
regulated by estradiol in vivo through cell-intrinsic estrogen
receptor alpha signaling. Blood 2012, 119:454-464.
29. Subramanian S, Yates M, Vandenbark AA, Offner H: Oestrogenmediated protection of experimental autoimmune
encephalomyelitis in the absence of Foxp3+ regulatory T cells
implicates compensatory pathways including regulatory B
cells. Immunology 2011, 132:340-347.
30. Carreras E, Turner S, Frank MB, Knowlton N, Osban J, Centola M,
Park CG, Simmons A, Alberola-Ila J, Kovats S: Estrogen receptor
signaling promotes dendritic cell differentiation by increasing
expression of the transcription factor IRF4. Blood 2010,
115:238-246.
31. Papenfuss TL, Powell ND, McClain MA, Bedarf A, Singh A,
!! Gienapp IE, Shawler T, Whitacre CC: Estriol generates
tolerogenic dendritic cells in vivo that protect against
autoimmunity. J Immunol 2011, 186:3346-3355.
This study highlights oestrogens ability to induce tolerogenic DC by
promoting IL-10 and TGFb release, leading to the amelioration of EAE.
34. Toldi G, Saito S, Shima T, Halmos A, Veresh Z, Vasarhelyi B, Rigo J
Jr, Molvarec A: The frequency of peripheral blood CD4+
CD25high FoxP3+ and CD4+ CD25- FoxP3+ regulatory T cells
in normal pregnancy and pre-eclampsia. Am J Reprod Immunol
2012, 68:175-180.
35. Lee SK, Kim JY, Hur SE, Kim CJ, Na BJ, Lee M, Gilman-Sachs A,
Kwak-Kim J: An imbalance in interleukin-17-producing T and
Foxp3(+) regulatory T cells in women with idiopathic recurrent
pregnancy loss. Hum Reprod 2011, 26:2964-2971.
36. Prieto GA, Rosenstein Y: Oestradiol potentiates the
suppressive function of human CD4 CD25 regulatory T cells by
promoting their proliferation. Immunology 2006, 118:58-65.
37. Valor L, Teijeiro R, Aristimuno C, Faure F, Alonso B, de Andres C,
Tejera M, Lopez-Lazareno N, Fernandez-Cruz E, SanchezRamon S: Estradiol-dependent perforin expression by human
regulatory T-cells. Eur J Clin Invest 2011, 41:357-364.
38. Lelu K, Laffont S, Delpy L, Paulet PE, Perinat T, Tschanz SA,
!
Pelletier L, Engelhardt B, Guery JC: Estrogen receptor alpha
signaling in T lymphocytes is required for estradiol-mediated
inhibition of Th1 and Th17 cell differentiation and protection
against experimental autoimmune encephalomyelitis. J
Immunol 2011, 187:2386-2393.
This study identifies that oestrogen signalling via hematopoetic cellexpression of ERa leads to the inhibition of Th1 and Th17 cells and confers
protection from EAE.
39. Lelu K, Delpy L, Robert V, Foulon E, Laffont S, Pelletier L,
Engelhardt B, Guery J-C: Endogenous estrogens, through
estrogen receptor a, constrain autoimmune inflammation in
female mice by limiting CD4+ T-cell homing into the CNS. Eur J
Immunol 2010, 40:3489-3498.
40. Saldanha CJ, Duncan KA, Walters BJ: Neuroprotective actions
of brain aromatase. Front Neuroendocrinol 2009, 30:106-118.
41. Gillies GE, McArthur S: Estrogen actions in the brain and the
basis for differential action in men and women: a case for sexspecific medicines. Pharmacol Rev 2010, 62:155-198.
42. Akabori H, Moeinpour F, Bland KI, Chaudry IH: Mechanism of the
anti-inflammatory effect Of 17beta-estradiol on brain following
trauma-hemorrhage. Shock (Augusta, Ga.) 2010, 33:43-48.
43. Sarvari M, Hrabovszky E, Kallo I, Solymosi N, Toth K, Liko I, Szeles J,
Maho S,MolnarB,LipositsZ:Estrogensregulateneuroinflammatory
genesviaestrogenreceptorsaandbinthefrontalcortexofmiddleaged female rats. J Neuroinflamm 2011, 8:82.
44. Rubio N, Cerciat M, Unkila M, Garcia-Segura LM, Arevalo M-A: An in
vitro experimental model of neuroinflammation: the induction of
interleukin-6 in murine astrocytes infected with Theilers murine
encephalomyelitis virus, and its inhibition by oestrogenic
receptor modulators. Immunology 2011, 133:360-369.
45. Cerciat M, Unkila M, Garcia-Segura LM, Arevalo M-A: Selective
estrogen receptor modulators decrease the production of
interleukin-6 and interferon-gamma-inducible protein-10 by
astrocytes exposed to inflammatory challenge in vitro. Glia
2010, 58:93-102.
46. Spence RD, Hamby ME, Umeda E, Itoh N, Du S, Wisdom AJ,
Cao Y, Bondar G, Lam J, Ao Y et al.: Neuroprotection mediated
through estrogen receptor-alpha in astrocytes. Proc Natl Acad
Sci U S A 2011, 108:8867-8872.
47. Giraud SN, Caron CM, Pham-Dinh D, Kitabgi P, Nicot AB:
Estradiol inhibits ongoing autoimmune neuroinflammation
and NFkappaB-dependent CCL2 expression in reactive
astrocytes. Proc Natl Acad Sci U S A 2010, 107:8416-8421.
48. Dang J, Mitkari B, Kipp M, Beyer C: Gonadal steroids prevent
cell damage and stimulate behavioral recovery after transient
middle cerebral artery occlusion in male and female rats. Brain
Behav Immun 2011, 25:715-726.
32. Josefowicz SZ, Lu LF, Rudensky AY: Regulatory T cells:
mechanisms of differentiation and function. Annu Rev Immunol
2012, 30:531-564.
49. Smith JA, Das A, Butler JT, Ray SK, Banik NL: Estrogen or estrogen
receptor agonist inhibits lipopolysaccharide induced microglial
activation and death. Neurochem Res 2011, 36:1587-1593.
33. Aluvihare VR, Kallikourdis M, Betz AG: Regulatory T cells
mediate maternal tolerance to the fetus. Nat Immunol 2004,
5:266-271.
50. McArthur S, Gillies GE: Peripheral vs. central sex steroid
hormones in experimental Parkinsons disease. Front
Endocrinol 2011, 2:82.
www.sciencedirect.com
Current Opinion in Pharmacology 2013, 13:576581
Anda mungkin juga menyukai
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDari EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifePenilaian: 4 dari 5 bintang4/5 (5794)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDari EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You ArePenilaian: 4 dari 5 bintang4/5 (1090)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDari EverandNever Split the Difference: Negotiating As If Your Life Depended On ItPenilaian: 4.5 dari 5 bintang4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDari EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RacePenilaian: 4 dari 5 bintang4/5 (895)
- Grit: The Power of Passion and PerseveranceDari EverandGrit: The Power of Passion and PerseverancePenilaian: 4 dari 5 bintang4/5 (588)
- Shoe Dog: A Memoir by the Creator of NikeDari EverandShoe Dog: A Memoir by the Creator of NikePenilaian: 4.5 dari 5 bintang4.5/5 (537)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDari EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersPenilaian: 4.5 dari 5 bintang4.5/5 (344)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDari EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FuturePenilaian: 4.5 dari 5 bintang4.5/5 (474)
- Her Body and Other Parties: StoriesDari EverandHer Body and Other Parties: StoriesPenilaian: 4 dari 5 bintang4/5 (821)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Dari EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Penilaian: 4.5 dari 5 bintang4.5/5 (121)
- The Emperor of All Maladies: A Biography of CancerDari EverandThe Emperor of All Maladies: A Biography of CancerPenilaian: 4.5 dari 5 bintang4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingDari EverandThe Little Book of Hygge: Danish Secrets to Happy LivingPenilaian: 3.5 dari 5 bintang3.5/5 (399)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDari EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyPenilaian: 3.5 dari 5 bintang3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)Dari EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Penilaian: 4 dari 5 bintang4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDari EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaPenilaian: 4.5 dari 5 bintang4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDari EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryPenilaian: 3.5 dari 5 bintang3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnDari EverandTeam of Rivals: The Political Genius of Abraham LincolnPenilaian: 4.5 dari 5 bintang4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealDari EverandOn Fire: The (Burning) Case for a Green New DealPenilaian: 4 dari 5 bintang4/5 (73)
- The Unwinding: An Inner History of the New AmericaDari EverandThe Unwinding: An Inner History of the New AmericaPenilaian: 4 dari 5 bintang4/5 (45)
- Rise of ISIS: A Threat We Can't IgnoreDari EverandRise of ISIS: A Threat We Can't IgnorePenilaian: 3.5 dari 5 bintang3.5/5 (137)
- (Springer) Cancer Immunology A Translational Medicine ContextDokumen633 halaman(Springer) Cancer Immunology A Translational Medicine ContextManoj PandreBelum ada peringkat
- Patient Satisfaction Evaluation On Hospitals Comparison Study Between Accredited and Non Accredited Hospitals in JordanDokumen18 halamanPatient Satisfaction Evaluation On Hospitals Comparison Study Between Accredited and Non Accredited Hospitals in JordandrindrasBelum ada peringkat
- Kriteria StrokeDokumen2 halamanKriteria StrokedrindrasBelum ada peringkat
- Hormonal Modulation of The Immune System - A Spotlight On The Role of ProgestogeDokumen7 halamanHormonal Modulation of The Immune System - A Spotlight On The Role of ProgestogedrindrasBelum ada peringkat
- Reference Ida MPASIDokumen2 halamanReference Ida MPASIdrindrasBelum ada peringkat
- 4.immunologic Disorders of The Female and Male Reproductive TractDokumen6 halaman4.immunologic Disorders of The Female and Male Reproductive TractdrindrasBelum ada peringkat
- 4.immunologic Disorders of The Female and Male Reproductive TractDokumen6 halaman4.immunologic Disorders of The Female and Male Reproductive TractdrindrasBelum ada peringkat
- Hormonal Modulation of The Immune System - A Spotlight On The Role of ProgestogeDokumen7 halamanHormonal Modulation of The Immune System - A Spotlight On The Role of ProgestogedrindrasBelum ada peringkat
- Estrogen Metabolism and AutoimmunityDokumen5 halamanEstrogen Metabolism and AutoimmunitypebripulunganBelum ada peringkat
- GALS AssessmentDokumen46 halamanGALS AssessmentdrindrasBelum ada peringkat
- GALS AssessmentDokumen46 halamanGALS AssessmentdrindrasBelum ada peringkat
- Ru Ella 2013Dokumen25 halamanRu Ella 2013Ruben NatarîșBelum ada peringkat
- Neurolint 13 00051 v3Dokumen10 halamanNeurolint 13 00051 v3Juan Carlos ConsuegraBelum ada peringkat
- Widoasti Putri Utami - 22010120410005 PDFDokumen20 halamanWidoasti Putri Utami - 22010120410005 PDFdevaBelum ada peringkat
- Autoimmune Hepatitis - A Guide For Practicing Clinicians - G. Hirschfield, Et. Al., (Humana, 2012) WWDokumen246 halamanAutoimmune Hepatitis - A Guide For Practicing Clinicians - G. Hirschfield, Et. Al., (Humana, 2012) WWIulian MunteanuBelum ada peringkat
- Chapter 2 Systemic Response To Injury and Metabolic Support PDFDokumen28 halamanChapter 2 Systemic Response To Injury and Metabolic Support PDFGian Carlo RabagoBelum ada peringkat
- Patogenesis Dan DD CTCLDokumen18 halamanPatogenesis Dan DD CTCLBayu HBelum ada peringkat
- 2022 - CCR8 Treg Cells in Tumor Tissues With Long-Lasting MemoryDokumen12 halaman2022 - CCR8 Treg Cells in Tumor Tissues With Long-Lasting Memory1262615286Belum ada peringkat
- Unit 1-Lecture 3 Intro To Immuno-Acquired ImmunityDokumen65 halamanUnit 1-Lecture 3 Intro To Immuno-Acquired ImmunityBecky GoodwinBelum ada peringkat
- Cover LetterDokumen2 halamanCover LetterkhaledBelum ada peringkat
- Atresia BilieerDokumen9 halamanAtresia BilieerSolo UpdateBelum ada peringkat
- Int Endodontic J - 2022 - Alsamahi - Type 2 Diabetes and The Clinically Normal Pulp An in Vitro StudyDokumen12 halamanInt Endodontic J - 2022 - Alsamahi - Type 2 Diabetes and The Clinically Normal Pulp An in Vitro StudyAKSBelum ada peringkat
- 7 (1) - Van Der Houwen-2022-Immunopathogenesis of Behcet's Disease and Treatment ModalitiesDokumen11 halaman7 (1) - Van Der Houwen-2022-Immunopathogenesis of Behcet's Disease and Treatment Modalitieskueiying.suBelum ada peringkat
- miRNA AlergenosDokumen76 halamanmiRNA AlergenosJosue BarralBelum ada peringkat
- T Cells & Autoimmunity, s3Dokumen21 halamanT Cells & Autoimmunity, s3LiaAriestaBelum ada peringkat
- Chinese Medicine 2Dokumen23 halamanChinese Medicine 2Tim SchlankBelum ada peringkat
- Resolving The Paradox of Colon CancerDokumen25 halamanResolving The Paradox of Colon CancerFranciscoGarciaBelum ada peringkat
- ACPN AbstractsDokumen21 halamanACPN AbstractsPediatric NephrologyBelum ada peringkat
- Cluster of Differentiation Antigen PosterDokumen1 halamanCluster of Differentiation Antigen PosterReeti R. Bhat100% (1)
- Autoimmune Disease MechanismsDokumen6 halamanAutoimmune Disease MechanismsHaliunaa BattulgaBelum ada peringkat
- Immunobiology: 1 Week To Check With Me. Follow The Syllabus's Guidelines!!Dokumen9 halamanImmunobiology: 1 Week To Check With Me. Follow The Syllabus's Guidelines!!Kay YgBelum ada peringkat
- Intl Journal of Cancer - 2014 - Lakritz - Beneficial Bacteria Stimulate Host Immune Cells To Counteract Dietary and GeneticDokumen12 halamanIntl Journal of Cancer - 2014 - Lakritz - Beneficial Bacteria Stimulate Host Immune Cells To Counteract Dietary and GeneticTrang MốcBelum ada peringkat
- Vitamin D: Modulator of The Immune SystemDokumen15 halamanVitamin D: Modulator of The Immune SystemJosé Antonio Silva NetoBelum ada peringkat
- Ar 3595Dokumen54 halamanAr 3595suryasanBelum ada peringkat
- Brain Immunology and Immunotherapy in Brain TumoursDokumen14 halamanBrain Immunology and Immunotherapy in Brain TumoursAnonymous QLadTClydkBelum ada peringkat
- DAVENPORT 2023 ERH-2022 - 0397.R2 - Proof - HiDokumen32 halamanDAVENPORT 2023 ERH-2022 - 0397.R2 - Proof - HiTeresa RibaltaBelum ada peringkat
- 03.immune InflamationDokumen11 halaman03.immune InflamationVARUN BHARADWAJ .MBelum ada peringkat
- NRDPUlcerative Colitis PDFDokumen21 halamanNRDPUlcerative Colitis PDFLuminita HutanuBelum ada peringkat
- The Risks vs. Benefits of Face Masks - Is There An Agenda - Children's Health DefenseDokumen7 halamanThe Risks vs. Benefits of Face Masks - Is There An Agenda - Children's Health DefenseAndrew LatorcaiBelum ada peringkat
- Immunology of Pediatric HIV InfectionDokumen51 halamanImmunology of Pediatric HIV InfectionPotafingersBelum ada peringkat