Im Fuo Trans
Diunggah oleh
Ryan PanHak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Im Fuo Trans
Diunggah oleh
Ryan PanHak Cipta:
Format Tersedia
Module No.
[SUBJECT]
[LECTURE
TITLE]
[Lecturer]
DD Month 2016
Outline
1.
1.
1.
2.
1.
2.
Heading 1
Heading 2
Heading 3
Heading 1
Heading 2
Heading 2
1.
Heading 3
2.
Heading 3
Proportion of caused by intraabdominal abscesses and
tumors lessearlier detection by CT and UTZ
IE is less frequent because blood culture and 2D-echo
techniques have improved
HIV unknown four decades ago
Types of FUO
Classic FUO
LEGEND
Lecture Powerpoint, Audio, Textbook
Temp >38.0C (>100.4F) on several occasions;
Duration of fever of >3 weeks
3 outpatient visits or 3 days in the hospital without elucidation
of a cause or 1 week of "intelligent and invasive" ambulatory
investigation
temperature of >38.0C (>100.4F) develops on several
occasions in a hospitalized patient who is receiving acute
care and in whom infection was not manifest or incubating on
admission.
3 days of investigation, including at least 2 days' incubation of
cultures, is the minimum requirement for this diagnosis
Fever of Unknown Origin(FUO)
Febrile Illness
Nosocomial FUO
Definition
Fever of Unknown Origin (FUO) is defined as any febrile illness
without initially obvious etiology. Most would be resolved before
diagnosis or is used to lead on a diagnosis. FUO excludes immunecompromised patients because they require an entirely different
diagnostic and therapeutic approach.
Accordingly, FUO is now defined as:
1. Fever >38C (101F) on at least two occasions
2. Illness duration of 3 weeks
3. No known immune-compromised state
4. Diagnosis that remains uncertain after a thorough history-taking,
physical examination, and the following obligatory investigations:
determination of erythrocyte sedimentation rate (ESR) and Creactive protein (CRP) level; platelet count; leukocyte count and
differential; measurement of levels of hemoglobin, electrolytes,
creatinine, total protein, alkaline phosphatase, alanine
aminotransferase,
aspartate
aminotransferase,
lactate
dehydrogenase, creatine kinase, ferritin, antinuclear antibodies, and
rheumatoid factor; protein electrophoresis; urinalysis; blood
cultures (n = 3); urine culture; chest x-ray; abdominal
ultrasonography; and tuberculin skin test (TST).
Most febrile illness:
1. Resolve before a diagnosis can be made or
2. Develop distinguishing charactereristics that lead to diagnosis
FUO should be reserved for prolonged febrile illnesses WITHOUT an
established etiology despite intensive evaluation and diagnostic testing
Historical Causes of FUO
Hippocrates: excess of yellow bile
Middle Ages (5th-15thcenturies): demonic possession
(encephalitis?)
18thCentury: Friction associated with the flow of blood
through the vascular system and from fermentation and
putrefaction occurring in the blood and intestines
Originally defined by Petersdorfand Beeson in 1961 as:
temperatures of >38.3C (>101F) on several occasions;
a duration of fever of >3 weeks; and
failure to reach a diagnosis despite 1 week of inpatient
investigation
Etiology and Epedemiology
NeutropenicFUO
temperature of >38.0C (>100.4F) on several occasions in a
patient whose neutrophil count is <500/L or is expected to fall
to that level in 12 days
a specific cause is not identified after 3 days of investigation,
including at least 2 days' incubation of cultures
HIV-associated FUO
temperature of 38.0C (100.4F) on several occasions over
a period of >3 weeks for outpatients or >3 days for
hospitalized patients with HIV infection
appropriate investigation over 3 days, including 2 days'
incubation of cultures, reveals no source
Classic FUO Definition
o
o
o
o
o
o
o
o
o
o
Temp >38.3C (>101F) on at least two (2) occasions;
Illness duration of 3 weeks
No known immunocompromised state
Diagnosis that remains uncertain after a thorough historytaking, PE, and the following obligatory investigations:
ESR and CRP level
CBC with platelet count
Electrolytes, creatinine total protein alkaline phosphatase,
alanine
aminotransferase,
aspartate
aminotransferase lactate dehydrogenase, creatinekinase,
ferritin
ANA and RF
protein electrophoresis
Urinalysis
Blood cultures (n=3) and urine culture
Chest x-ray and abdominal UTZ
and tuberculin skin test (TST)
Classic FUO
remember that FUO is far more often caused
by an atypical presentation of a rather common
disease than by a very rare disease.
Signs and Symptoms:
Endocarditis
Diverticulitis
Vertebral osteomyelitis
EPTB
The range of FUO etiologies has evolved over time as a result of changes
in the spectrum of diseases causing FUO, the widespread use of
antibiotics, and the availability of new diagnostic techniques.
Increase in diagnostic failure rate is due to the establishment of the
diagnosis prior to the 3 weeks illness duration even with advanced
technological screening techniques (CT and MRI). Also, a patient with
FUO but without a diagnosis has less aggressive diagnostic approach and
is relevant with recurrent fever (repeated episodes of fever interspersed
with fever-free intervals of at least 2 weeks and apparent remission of the
underlying disease) would have <50% etiologic diagnosis.
Classic Causes of FUO
In Western Countries
Insert picture here
Infectious Causes of FUO
Bacterial (non-specific)
Transcribed by: [TRANSERS]
Checked by: [TRANSHEAD]
Abdominal abscess (liver, splenic, psoas, etc)
Adnexitis, appendicitis, cholecystitis, tubo-ovarian abscess,
pyometra
Intracranial abscess, sinusitis, dental abscess
Page 1 of 6
[SUBJECT]
[Lecture Title]
Chronic pharyngitis, tracheobronchitis, lung abscess
Septic
jugular
phlebitis,
mycoticaneurysm,
endocarditis, intravenous catheter infection, vascular
graft infection
Wound infection, osteomyelitis, infected joint prosthesis,
pyelonephritis, prostatitis
Lung abscess, liver abscess, renal abscess
Tuberculosis
(including
EPTB),Mycobacterium
aviumcomplex, syphilis, Q fever, legionellosis
Salmonellosis (including typhoid fever), listeriosis,
ehrlichiosis,
Actinomycosis, nocardiosis, Whipples disease
Fungal (candidaemia, cryptococcosis, sporotrichosis,
aspergillosis,
Malaria, babesiosis, toxoplasmosis, schistosomiasis,
fascioliasis, toxocariasis, amoebiasis, infected hydatid
cyst, trichinosis, trypanosomiasis
Cytomegalovirus, HIV, Herpes simplex, Epstein-Barr
virus, parvovirus B19
Insert pictures here
Important considerations
In patient with travel history to tropical areas: malaria,
leishmaniasis, histoplasmosis or coccidioidomycosis
IE suspected but culture negative: nutritionally variant
bacteria,
HACEK
organisms
(Haemophilusparainfluenzae,
H.
paraprophilus,
Aggregatibacterspecies,
Cardiobacteriumspecies Eikenellacorrodensand
Kingellakingae)
o
o
o
o
o
o
o
o
o
o
o
o
o
o
o
o
o
o
Neoplasm
Elderly: giant-cell arteritis, TB, colon CA
Miscellaneous: drug fever, pulmonary embolism,
factitious fever
As the duration of fever increases, the likelihood of an
infectious cause decreases
Malignancies
Lymphoma
Lymphoma
Lymphoma
Renal cell carcinoma
Hepatocellular carcinoma
Collagen Vascular Diseases
SLE, mixed connective tissue disease
Giant cell arteritis/polymyalgia rheumatica, ankylosing
spondylitis
Rheumatic fever
Polymyositis, rheumatoid arthritis
Drug Fever
No characteristic fever pattern was observed.
Maximum temperatures ranged from 38C to 43C
The mean lag time between initiation of a drug and the
onset of fever was 21 days, but lag times varied
considerably.
Alpha methyldopa and quinidine were the two drugs
most commonly implicated, but antimicrobials (as a
group) were responsible for the largest number of
episodes.
Allopurinol, carbamazepine, lamotriginephenytoin
Transcribed By: [TRANSERS]
Sulfasalazine (for IBD)furosemide
Antimicrobial
drugs
(especially
sulfonamides minocycline vancomycin -lactam
antibioticsand isoniazid)
Some cardiovascular drugs (e.g.quinidine)
Some antiretroviral drugs (e.g.nevirapine)
Interesting causes of FUO
Exercise-induced hyperthermia
Associated with moderate to strenuous exercise lasting
from half an hour up to several hours without an
increase in CRP level or ESR
(+) sweat during the temperature elevation
Factitious fever
fever artificially induced by the patient
E.g. IV injection of contaminated water)
More common among young women in health care
professions
Fraudulent fever
The patient is normothermicbut manipulates the thermometer
To check? Simultaneous measurements at different
body sites (rectumearmouth)
Another clue: Dissociation between pulse rate and
temperature
FUO in the elderly
Adult Causes
Module #, Lecture #
Usually from an atypical manifestation of a common
disease
Important DDx: Giant cell arteritis and polymyalgia
rheumatic, TB
TB -most common infectious cause of FUO
As many of these diseases are treatable, it is well
worth pursuing the cause of fever in elderly patients.
FUO in the elderly
a diagnosis is more likely in elderly patients
than in younger age groups.
Fever in
neutropenicpatients not responding to antibiotics
Insert table here
Rectal abscesses
Typhilitis
Imaging very important
HIV Associated FUO Causes
Insert picture here
o
o
o
o
Device related infection
CAUTI
VAP/HAP
SSSI
Central line associated bloodstream infections
Checked by: [TRANSHEAD]
Page 2 of 6
[SUBJECT]
[Lecture Title]
Module #, Lecture #
o Phlebitis
Pressure ulcers
Prognosis
Clinical Evaluation of FUO
o
o
o
o
o
o
o
o
o
o
History
Recent travel, exposure to pets and other animals, the
work environment, and recent contact with people
exhibiting similar symptoms.
family history for possible hereditary causes of fever
past medical history -for any previously diagnosed
conditions, such as lymphoma, rheumatic fever, or intraabdominal disorders, complications or reactivation
complete list of the patients medications
Verification of fever and fever pattern
Physical Examination
nodular or weakly pulsatile temporal artery of temporal
arteritis
telltale oral ulcers of disseminated histoplasmosis or
Behcets syndrome
choroid granuloma or epididymal nodule of
extrapulmonary tuberculosis
testicular nodule of polyarteritis nodosa
vague rectal fluctuance of a perirectal abscess
search for lymphadenopathy
Insert picture here
General Diagnostic Evaluation of FUO
Insert picture here
Diagnostic Value of Naproxen
77 patients presenting with FUO were treated with
naproxen.
Overall temperature decreased from 39.1C to 37.4C.
The sensitivity of the naproxen test for neoplastive fever
was 55% and the specificity was 62%.
Treatment
A fundamental principle in the management of classical
FUO is that therapy should be withheld, whenever
possible, until the cause of the fever has been
determined, so that treatment can be tailored to a
specific diagnosis
Empirical therapeutic trials should be reserved for those
very few patients in whom all other approaches have
failed or those so seriously ill that therapy cannot be
withheld for a further period of observation, or both
Febrile neutropenicpatients should generally receive
broad-spectrum antimicrobial therapy immediately after
samples for appropriate cultures have been obtained
FUO-related mortality rates have continuously declined
over recent decades.
The majority of fevers are caused by treatable diseases.
Risk of death related to FUO is dependent on the
underlying disease.
Other studies shows that malignancy accounts for most
FUO-related deaths.
Non-Hodgkin's lymphoma carries a disproportionately
high death toll.
In nonmalignant FUO, fatality rates are very low.
In poor regions infectious diseases are still a major
cause of FUOand outcomes may be different
The good outcome in patients without a diagnosis
confirms that potentially lethal occult diseases are very
unusual.
Epiricaltherapy with antibiotics
antituberculousagents, or glucocorticoids is
rarely required in stable patients
FUO-related mortality rates have continuously
declined over recent decades. The majority of
fevers are caused by treatable diseases, and the
risk of death related to FUO is dependent on
the underlying disease.
Nonmalignant FUO, fatality rates are very low.
The good outcome in patients without a
diagnosis confirms that potentially lethal occult
diseases are very unusual and that empirical
therapy with antibiotics, anti-tuberculous
agents, or glucocorticoids is rarely required in
stable patients. In less affluent regions,
infectious diseases are still a major cause of
FUO, and outcomes may be different
Empiric Treatment
Steroids
The ability of glucocorticoids and NSAIDs to mask fever
while permitting the spread of infection dictates that
their use be avoided unless infection has been largely
ruled out and unless inflammatory disease is both
probable and debilitating or threatening
Empirical treatment with corticosteroids may be
appropriate in patients with suspected temporal arteritis
to prevent vascular complications such as blindness or
stroke
Transcribed By: [TRANSERS]
Checked by: [TRANSHEAD]
Page 3 of 6
[SUBJECT]
[Lecture Title]
Module #, Lecture #
Differential Diagnosis
FUO differential diagnosis is extensive. Most often caused by an
atypical presentation of common diseases than by very rare
diseases. Diagnosis is more likely in elderly patients than younger
age groups. Most common infectious disease associated with FUO
in elderly patients is tuberculosis, while most frequently involved
atypical manifestation of a common disease would include: giant
cell arteritis and polymyalgia rheumatic.
Naproxen test is of low diagnostic yield.
Diagnostic approach should occur in a step-wise
fashion based on the H&P.
Patients that remain undiagnosed generally have a
good prognosis.
Treatment
Antibiotics and Anti-tuberculous Therapy
Irrevocably diminish the ability to culture fastidious bacteria or
mycobacteria. Hemodynamic instability or neutropenia is a
good indication for empirical antibiotic therapy. If the fever
does not respond after 6 weeks of empirical anti tuberculous
treatment, another diagnosis should be considered.
Most common infectious disease diagnoses:
atypical presentation of endocarditis
diverticulitis
vertebral osteomyelitis
extrapulmonary tuberculosis
Colchicine, NSAIDs, and Glucocorticoids
Rare (nonspecific):
Q fever
Whipples disease
Colchicine is highly effective in preventing attacks of familial
Mediterranean fever but is not always effective once an attack is
well under way.
Most common in tropical countries or the American Southwest:
malaria
leishmaniasis
histoplasmosis
coccidioidomycosis
If the fever persists and the source remains elusive after
completion of the later-stage investigations, supportive
treatment with nonsteroidal anti-inflammatory drugs (NSAIDs)
can be helpful.
With Urticaria, bone pain, and monoclonal gammopathy:
Schnitzlers syndrome
Early empirical trials with glucocorticoids, decrease the chances
of reaching a diagnosis for which more specific and sometimes
life-saving treatment might be more appropriate, such as
malignant lymphoma.
Most common in Neoplasms: Malignant lymphoma
More common causes of druginduced
Fever:
allopurinol
arbamazepine
amotrigine
phenytoin
sulfasalazine
furosemide
antimicrobial drugs (esp. sulfonamides,
minocycline, vancomycin, -lactam antibiotics, and
isoniazid)
some cardiovascular drugs (e.g., quinidine)
- some antiretroviral drugs (e.g., nevirapine).
The ability of NSAIDs and glucocorticoids to mask fever while
permitting the spread of infection or lymphoma dictates their
use should be avoided unless infectious diseases and malignant
lymphoma have been largely ruled out and inflammatory
disease is probable and is likely to be debilitating or threatening.
Anakinra
Anakinra, a recombinant form of the naturally occurring IL-1
receptor antagonist (IL-1Ra), blocks the activity of both IL-1
and IL-1. Anakinra is extremely effective in the treatment of
many autoinflammatory syndromes, such as familial
Mediterranean fever, cryopyrin-associated periodic syndrome,
tumor necrosis factor receptorassociated periodic syndrome,
hyper-IgD syndrome, and Schnitzlers syndrome.
Summary
FUO is often a diagnostic dilemma. The importance of
history and PE cannot be overemphasized.
In the Philippines, infections comprise ~30% of cases.
Tuberculosis (including EPTB) is a very important
differential diagnosis.
Transcribed By: [TRANSERS]
Checked by: [TRANSHEAD]
Page 4 of 6
[SUBJECT]
[Lecture Title]
Module #, Lecture #
First-Stage Diagnostic Tests
Most important step is the search for potentially diagnostic
clues (PDCs; are defined as all localizing signs, symptoms,
and abnormalities potentially pointing toward a diagnosis.
Maybe misleading but provides a concise list of probable
diagnoses.) through complete and repeated history-taking
and physical examination and the obligatory investigations.
Before further diagnostic tests are initiated, antibiotic
glucocorticoid, and anti-tuberculous treatment (mask many
diseases), should be stopped. Despite the high number of
false-positive ultrasounds and the relatively low sensitivity
of chest x-rays, the performance of these tests remains
obligatory in all patients with FUO in order to separate cases
that are caused by easily diagnosed diseases from those that
are not.
Initial step after establishing the PDC, doing the historytaking, and physical examination is to rule out factitious or
fraudulent fever, particularly in patients without signs of
inflammation in laboratory tests. Also, a limited list of the
most probable diagnoses should be made.
Absence of specific symptoms in many patients and the
relatively low cost of the test, investigation of cryoglobulins
appears to be a valuable screening test in patients with FUO.
Tests should not be used as screening procedures due to very
low diagnostic yield (absence of PDCs):
echocardiography
sinus radiography
radiologic or endoscopic evaluation of the
gastrointestinal tract
bronchoscopy
When the first-stage diagnostic tests do not lead to a
diagnosis, scintigraphy should be performed, especially
when the ESR or CRP level is elevated.
Later-Stage Diagnostic Tests
In some cases, more invasive tests are appropriate.
Abnormalities found with scintigraphic techniques often
need to be confirmed by pathology and/or culture of biopsy
specimens. If no diagnosis is reached despite scintigraphic
and PDC-driven histologic investigations or culture, secondstage screening diagnostic tests should be considered.
Scintigraphy
Noninvasive method allowing delineation of foci in all parts of the body
on the basis of functional changes in tissues which plays an important
role in the diagnosis of patients with FUO in clinical practice.
Conventional scintigraphic methods used in clinical practice are Gacitrate scintigraphy and In- or Tc-labeled leukocyte
scintigraphy. Focal infectious and inflammatory processes can also be
detected by several radiologic techniques, such as CT, MRI, and
ultrasound. Because of the lack of substantial pathologic changes in the
early phase, infectious and inflammatory foci cannot be detected at this
time.
CT and MRI routinely provide information only on part of the body,
while scintigraphy readily allows whole-body imaging. Scintigraphic
techniques do not directly provide a
definitive diagnosis, they often identify the anatomic location of a
particular ongoing metabolic process and, with the help of other
techniques such as biopsy and culture, facilitate timely diagnosis and
treatment.
In patients with unexplained fever after all of the above
procedures, the last step in the diagnostic workup (marginal
Transcribed By: [TRANSERS]
Checked by: [TRANSHEAD]
diagnostic yield, extraordinarily high cost in terms of both
expense and discomfort). Repetition of a thorough historytaking and physical examination and review of laboratory
results and imaging studies (including those from other
hospitals) are recommended.
Page 5 of 6
[SUBJECT]
[Lecture Title]
Module #, Lecture #
Fluorodeoxy Positron Emission Tomography
F-fluorodeoxyglucose (FDG) positron emission tomography (PET) has
become an established imaging procedure in FUO. FDG accumulates in
tissues with a high rate of glycolysis, which occurs not only in malignant
cells but also in activated leukocytes, and thus permits the imaging of
acute and chronic inflammatory processes. Normal uptake may obscure
pathologic foci in the brain, heart, bowel, kidneys, and bladder. In
patients with fever, bone marrow uptake is frequently increased in a
nonspecific way due to cytokine activation, which upregulates glucose
transporters in bone marrow cells.
Compared with conventional scintigraphy, FDG-PET offers the
advantages of higher resolution, greater sensitivity in chronic low-grade
infections, and a high degree of accuracy in the central skeleton. Recurrent Fever
Diagnostic
workup should consist of thorough history-taking, physical
FDG-PET/CT is a relatively expensive procedure whose availability
is
examination,
and obligatory tests. Patients
still limited compared with that of CT and conventional scintigraphy.
should
be
asked
to return during a febrile episode so that the history,
Nevertheless, FDGPET/
physical
examination,
and laboratory tests can be repeated during a
CT can be cost-effective in the FUO diagnostic workup if used at an
symptomatic
phase.
Further
diagnostic tests, such as scintigraphic
early stage, helping to establish an early diagnosis, reducing days of
imaging,
should
be
performed
only during a febrile episode because
hospitalization for diagnostic purposes, and obviating unnecessary and
abnormalities
may
be
absent
between
episodes.
unhelpful tests.
In patients with recurrent fever lasting >2 years, it is very unlikely that
the fever is caused by infection or malignancy. Further diagnostic tests
in that direction should be considered only when PDCs for infections,
vasculitis syndromes, or malignancy are present or when the patients
clinical condition is deteriorating.
Transcribed By: [TRANSERS]
Checked by: [TRANSHEAD]
Page 6 of 6
Anda mungkin juga menyukai
- g6pd CaseDokumen1 halamang6pd CaseRyan PanBelum ada peringkat
- SBCM CerebrumDokumen59 halamanSBCM CerebrumRyan PanBelum ada peringkat
- Helper For Sro GuideDokumen1 halamanHelper For Sro GuideRyan PanBelum ada peringkat
- Biochemistry Malignant Hyerthermia Guide QuestionsDokumen2 halamanBiochemistry Malignant Hyerthermia Guide QuestionsRyan PanBelum ada peringkat
- SRO Set GuideDokumen3 halamanSRO Set GuideRyan PanBelum ada peringkat
- Impact of Illness Lecture - HandoutDokumen5 halamanImpact of Illness Lecture - HandoutRyan PanBelum ada peringkat
- GSLPDokumen4 halamanGSLPRyan PanBelum ada peringkat
- CC Pituary ReviewerDokumen2 halamanCC Pituary ReviewerRyan PanBelum ada peringkat
- Symptoms: Cyanide Toxicity Is Often Associated With The Odor of Almonds On BreathDokumen2 halamanSymptoms: Cyanide Toxicity Is Often Associated With The Odor of Almonds On BreathRyan PanBelum ada peringkat
- September 2015 Exam ScheduleDokumen4 halamanSeptember 2015 Exam ScheduleRyan PanBelum ada peringkat
- Clinical Chemistry Reviewer by MTRDokumen56 halamanClinical Chemistry Reviewer by MTRRyan Pan95% (19)
- 5 X 5 WorkoutDokumen1 halaman5 X 5 WorkoutRyan PanBelum ada peringkat
- Metabolism of Unsaturated Fatty Acids and EicosanoidsDokumen45 halamanMetabolism of Unsaturated Fatty Acids and EicosanoidsRyan PanBelum ada peringkat
- Intermediate Level Strength Training ProgramDokumen2 halamanIntermediate Level Strength Training ProgramRyan PanBelum ada peringkat
- 6week Training For BenchDokumen2 halaman6week Training For BenchRyan PanBelum ada peringkat
- Gillingham Raw Bench ProgramDokumen2 halamanGillingham Raw Bench ProgramRyan PanBelum ada peringkat
- 531 Workbook PostedDokumen9 halaman531 Workbook PostedRyan Pan100% (1)
- Lascek S&CP v2.0Dokumen3 halamanLascek S&CP v2.0jr221Belum ada peringkat
- Stronglifts Madcow 5x5 Intermidiate DJDokumen9 halamanStronglifts Madcow 5x5 Intermidiate DJRyan Pan0% (1)
- Your NameDokumen1 halamanYour NameRyan PanBelum ada peringkat
- 2 Tickets To The Gun Show Workout TemplatesDokumen5 halaman2 Tickets To The Gun Show Workout TemplatesLeopoldo SFBelum ada peringkat
- The Weightrainer: Classic Powerlifting Peaking Program #1Dokumen2 halamanThe Weightrainer: Classic Powerlifting Peaking Program #1Ryan PanBelum ada peringkat
- Ed Coan 10 Week Training Cycle: Starting Squat Max Starting Bench Max Starting Deadlift MaxDokumen4 halamanEd Coan 10 Week Training Cycle: Starting Squat Max Starting Bench Max Starting Deadlift MaxStefan OlssonBelum ada peringkat
- Ws TemplateDokumen53 halamanWs TemplateRyan Pan100% (1)
- Joe Defranco - WS4SBDokumen16 halamanJoe Defranco - WS4SBsostanzapsicoattiva100% (2)
- K Ethna AbssDokumen104 halamanK Ethna AbssRyan PanBelum ada peringkat
- Articles 2013-04-22 Train Like A ThrowerDokumen24 halamanArticles 2013-04-22 Train Like A ThrowerRyan Pan0% (1)
- Dorian Yates 6 Week TrainingDokumen4 halamanDorian Yates 6 Week TrainingRyan Pan85% (13)
- 4 Week Shoulder WorkoutDokumen2 halaman4 Week Shoulder WorkoutRyan PanBelum ada peringkat
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDari EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifePenilaian: 4 dari 5 bintang4/5 (5794)
- Shoe Dog: A Memoir by the Creator of NikeDari EverandShoe Dog: A Memoir by the Creator of NikePenilaian: 4.5 dari 5 bintang4.5/5 (537)
- The Yellow House: A Memoir (2019 National Book Award Winner)Dari EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Penilaian: 4 dari 5 bintang4/5 (98)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDari EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RacePenilaian: 4 dari 5 bintang4/5 (895)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDari EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersPenilaian: 4.5 dari 5 bintang4.5/5 (344)
- The Little Book of Hygge: Danish Secrets to Happy LivingDari EverandThe Little Book of Hygge: Danish Secrets to Happy LivingPenilaian: 3.5 dari 5 bintang3.5/5 (399)
- Grit: The Power of Passion and PerseveranceDari EverandGrit: The Power of Passion and PerseverancePenilaian: 4 dari 5 bintang4/5 (588)
- The Emperor of All Maladies: A Biography of CancerDari EverandThe Emperor of All Maladies: A Biography of CancerPenilaian: 4.5 dari 5 bintang4.5/5 (271)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDari EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaPenilaian: 4.5 dari 5 bintang4.5/5 (266)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDari EverandNever Split the Difference: Negotiating As If Your Life Depended On ItPenilaian: 4.5 dari 5 bintang4.5/5 (838)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDari EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryPenilaian: 3.5 dari 5 bintang3.5/5 (231)
- On Fire: The (Burning) Case for a Green New DealDari EverandOn Fire: The (Burning) Case for a Green New DealPenilaian: 4 dari 5 bintang4/5 (73)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDari EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FuturePenilaian: 4.5 dari 5 bintang4.5/5 (474)
- Team of Rivals: The Political Genius of Abraham LincolnDari EverandTeam of Rivals: The Political Genius of Abraham LincolnPenilaian: 4.5 dari 5 bintang4.5/5 (234)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDari EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyPenilaian: 3.5 dari 5 bintang3.5/5 (2259)
- Rise of ISIS: A Threat We Can't IgnoreDari EverandRise of ISIS: A Threat We Can't IgnorePenilaian: 3.5 dari 5 bintang3.5/5 (137)
- The Unwinding: An Inner History of the New AmericaDari EverandThe Unwinding: An Inner History of the New AmericaPenilaian: 4 dari 5 bintang4/5 (45)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDari EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You ArePenilaian: 4 dari 5 bintang4/5 (1090)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Dari EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Penilaian: 4.5 dari 5 bintang4.5/5 (120)
- Her Body and Other Parties: StoriesDari EverandHer Body and Other Parties: StoriesPenilaian: 4 dari 5 bintang4/5 (821)
- Submental Abscess After Deoxycholic Acid Injection: ReferenceDokumen1 halamanSubmental Abscess After Deoxycholic Acid Injection: Referencechash75Belum ada peringkat
- Modul Normal Delivery 2016Dokumen8 halamanModul Normal Delivery 2016Alvin FarhanBelum ada peringkat
- 10 Larva MigransDokumen8 halaman10 Larva MigransDaniel JohnsonBelum ada peringkat
- Clinical Evaluation Report For Trilogy Evo Ventilator: Prepared For: Respironics, IncDokumen79 halamanClinical Evaluation Report For Trilogy Evo Ventilator: Prepared For: Respironics, Incdaphnestc0211Belum ada peringkat
- Composite Hemangioendothelioma An Unusual Presentation of A Rare Vascular TumorDokumen5 halamanComposite Hemangioendothelioma An Unusual Presentation of A Rare Vascular TumorTian Nopita SariBelum ada peringkat
- Eye & Ear IrrigationDokumen34 halamanEye & Ear IrrigationdaisyBelum ada peringkat
- Primary Carcinoid Tumor of The Urinary BladderDokumen5 halamanPrimary Carcinoid Tumor of The Urinary BladdermikalraBelum ada peringkat
- Preview of "Practice Quiz - Heart"Dokumen2 halamanPreview of "Practice Quiz - Heart"Jose Pagan100% (1)
- Hayashi Reiki ManualDokumen14 halamanHayashi Reiki Manualboomerb100% (4)
- Pre Dent Ate Period PedoDokumen16 halamanPre Dent Ate Period PedoFourthMolar.com0% (1)
- Basic and Clinical Pharmacology 12th Edition-Bertram Katzung Susan Masters Anthony Trevor-290-296 PDFDokumen7 halamanBasic and Clinical Pharmacology 12th Edition-Bertram Katzung Susan Masters Anthony Trevor-290-296 PDFalinamatei1000000Belum ada peringkat
- MethergineDokumen2 halamanMethergineJulie May33% (3)
- Price List of Hasc Hearing Aids (Rexton) W.E.F. 1/6/2012: Arena Digital FamilyDokumen6 halamanPrice List of Hasc Hearing Aids (Rexton) W.E.F. 1/6/2012: Arena Digital FamilyPaulo DantasBelum ada peringkat
- C - Syiam Amalia Rahmah - Topik 4Dokumen7 halamanC - Syiam Amalia Rahmah - Topik 4Syiam Amalia RahmahBelum ada peringkat
- Chapter 3 - Drug EducationDokumen26 halamanChapter 3 - Drug EducationHabadu HabadiBelum ada peringkat
- Alsayed Alrokh - Pharmacology Review PDFDokumen90 halamanAlsayed Alrokh - Pharmacology Review PDFAlan DafoeBelum ada peringkat
- Engorgement & Mastitis MM RH SJDokumen18 halamanEngorgement & Mastitis MM RH SJbrown_chocolate87643Belum ada peringkat
- Root Canal IrrigationDokumen3 halamanRoot Canal IrrigationIshac AbdoBelum ada peringkat
- Laws On Notifiable DiseaseDokumen43 halamanLaws On Notifiable DiseaseKenji ToleroBelum ada peringkat
- TELECARDIOLOGYDokumen11 halamanTELECARDIOLOGYNancy Prasad100% (1)
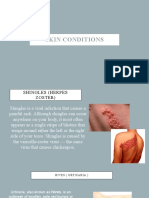
- Skin ConditionsDokumen11 halamanSkin ConditionsElza ShainidzeBelum ada peringkat
- 2009 11 Oral GalvanismDokumen2 halaman2009 11 Oral GalvanismSppatilBelum ada peringkat
- Drug StudyDokumen5 halamanDrug Studyanon_168410816Belum ada peringkat
- CH 19Dokumen5 halamanCH 19Ryan Carlo IbayanBelum ada peringkat
- ACS BookletDokumen14 halamanACS Bookletmyat25Belum ada peringkat
- TraumaAirway Management - ValDokumen36 halamanTraumaAirway Management - ValValerie Suge-MichiekaBelum ada peringkat
- 1.1.4.B ConcentrationDokumen3 halaman1.1.4.B ConcentrationAnonymous lFgKXClH0% (1)
- Stem Cell TherapyDokumen33 halamanStem Cell TherapyAnusha VergheseBelum ada peringkat
- Brochure XN-L 550 450 350 330 - MNDokumen8 halamanBrochure XN-L 550 450 350 330 - MNarkoudelosBelum ada peringkat
- Psychological DisordersDokumen21 halamanPsychological DisordersMark100% (2)