Operati VLN LN
Diunggah oleh
melho.cottonJudul Asli
Hak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Operati VLN LN
Diunggah oleh
melho.cottonHak Cipta:
Format Tersedia
460
Porous Tantalum for Patellar Reconstruction
The patella increases the functional lever arm of the
quadriceps muscle by transmitting the forces across
the knee joint at a greater distance from the axis of
rotation.
The patella is anchored and stabilized over the
anterior aspect of the knee by the quadriceps and
patellar tendons in the proximal-distal axis and by
the medial and lateral retinacula in the medial-lateral
axis. Figure 3 illustrates the force vectors acting on
the patella from the extensor mechanism as well as
the lateral and medial retinacula.
The patellar blood supply is provided by the
geniculate arteries, which form an anastomotic ring
around the patella (Scapinelli, 1967). This ring lies
less than 1 cm from the peripheral border of the
patella.
Lateral retinacular release, when necessary, should
be performed 12 cm away from the lateral
patellar border.
PEARLS
We use two paint rollers secured
to the table such that the
proximal one will hold the knee
hyperexed, and the second is
placed more distally such that
the knee can be held at
approximately 90 of exion
during the procedure.
A 3-L saline bag or a roll of
surgical towels may be placed
under the operative-side buttock
to give a gentle tilt to the pelvis.
This produces slight internal
rotation of the operative leg and
makes the resting position of the
leg more natural for the
procedure.
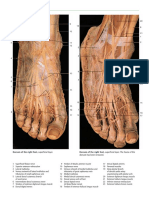
Quadriceps
Lateral retinaculum,
vastus lateralis, and
iliotibial tract
Patellar
tendon
Equipment
Leg positioning devices exist
to hold the knee in varying
degrees of exion that can be
utilized depending on surgeon
preference.
Medial retinaculum
and vastus medialis
FIGURE 3
461
PEARLS
Portals/Exposures
We leave a 2- to 5-mm rim of
retinaculum attached to the
patella as we curve our
arthrotomy incision around the
medial aspect of the patella.
This helps to give a more
anatomic closure.
We mark the quadriceps tendon
with methylene blue on both
sides of the arthrotomy to assure
an anatomic repair.
The repair should be performed
with the same degree of knee
exion as was present during the
original arthrotomy.
PITFALLS
In multiple revision situations
where there are previous incisions
over the front of the knee, the
lateral-most skin incision should
be utilized to preserve the blood
supply to the skin, which travels
from medial to lateral anteriorly.
Position the patient supine on the operating table.
Place a tourniquet on the proximal thigh of the
operative leg.
Use a leg positioner or paint roller secured to the
operating table to hold the knee in exion during
the procedure.
Instrumentation
Use two sharp towel clips, one
proximally at the superior pole
placed through the quadriceps
tendon, and one at the inferior
pole through the patellar
tendon, to stabilize the patella
during the procedure.
There are several standard approaches to the knee
for purposes of reconstruction and revision (medial
parapatellar, lateral parapatellar, subvastas,
midvastus).
The medial parapatellar approach is our preferred
approach for revision surgery.
This approach is extensile and can be modied
using a quadriceps snip, tibial tubercle osteotomy,
or quadriceps turndown to optimize exposure.
In the case of revision TKA, the previous skin incision
is most often used to prevent skin necrosis that may
be caused by a separate incision that creates a skin
bridge between the new and any previous incisions.
When there is more than one prior incision, it is
generally recommended that the most lateral
longitudinal incision that allows satisfactory
exposure be used.
The remainder of the approach is dictated by
surgeon preference.
We use a medial parapatellar incision into the knee
in primary and revision cases, as it provides a safe
and extensile approach to the knee joint.
For revision TKA, we start by making a long
midline anterior skin incision that begins
approximately 4 cm proximal to the superior pole
of the patella and is taken distally to 4 cm below
the inferior pole.
We make our deep incision in line with the
quadriceps tendon bers proximally and carry it
around the medial aspect of the patella, then
extend it distally parallel to the patellar tendon.
We leave a 2- to 5-mm cuff of tissue around the
patella for later repair.
At the time of patellar revision, the patella along with
the extensor mechanism is everted to expose the
backside of the patella.
This is most easily done with the knee in full
extension as it takes the tension off the extensor
mechanism.
Porous Tantalum for Patellar Reconstruction
Positioning
Porous Tantalum for Patellar Reconstruction
462
PEARLS
We recommend erring toward
using a larger diameter porous
tantalum shell. This may
decrease the risk of insetting the
shell and creating a stress riser
at the inferior or superior pole,
which may lead to avulsion
fractures.
We recommend deating the
tourniquet to conrm punctate
patellar bleeding prior to
implantation of the shell.
We recommend xation with #2
FiberWire sutures in conjunction
with a drill and straight Keith
needles to facilitate passage of
sutures.
PITFALLS
Excessive reaming of the patella
compromises the strength of the
remaining shell with creation of
stress risers at the superior and/
or inferior poles.
Procedure
STEP 1
Once adequate exposure of the knee is achieved and
the patellar component is exposed via eversion of
the extensor mechanism, the previous implant is
removed.
In cases of severe bone loss, the patellar button is
usually loose and is easily removed.
If this is not the case, then the button may be
sawed off at the level of the pegs using a
reciprocating saw. The remaining pegs and
cement can be ground out from the patella using
a high-speed burr.
In the case of a well-xed, cementless patellar
component with osteolysis, removal may require
sectioning of the metal baseplate with a
metal-cutting burr or a diamond wheel.
At this point, the remaining rim of patellar bone
must be reamed using an appropriately sized
spherical reamer that corresponds to the radius of
the porous tantalum shell to be implanted
(Fig. 4A and 4B).
Figures 4A, 5, and 6A from Nasser S, Poggie RA. Revision and salvage patellar arthroplasty
using a porous tantalum implant. J Arthroplasty. 2004;19:562-71.
A
FIGURE 4
463
Depending on the implant manufacturer, there may be more
than one diameter of porous tantalum shell available, as well as
different thickness options.
Selection of the shell diameter should be based on remaining
patellar bone stock (erring to the larger diameter shell).
Thickness of the component should be chosen such that
the component most closely replicates the normal thickness of
the patella (26 mm in males and 23 mm in females), unless the
thickness of the contralateral native patella is known.
PEARLS
When suturing down the shell
via the peripherally placed holes,
use a crossing star pattern to
ensure even tensioning of the
implant to the underlying soft
tissues.
Instrumentation/
Implantation
Use a small (1.6- or 2.0-mm)
drill to facilitate passage of the
sutures through the remaining
patellar bone.
Use straight Keith needles to
pass sutures through drill holes
and soft tissues.
STEP 2
Next, trial the component by tying down the shell
using several sutures to the surrounding soft tissues.
Check the tracking of the implant to ensure good
alignment within the femoral trochlea.
Once the desired positioning is achieved, place #2 or
#5 nonabsorbable braided sutures through the
peripheral holes provided on the porous tantalum
shell and into the quadriceps tendon and remaining
patellar bone.
Figure 5 shows the porous tantalum shell with the
peripheral holes numbered in a crossing star
pattern to depict the order in which the sutures
should be tied down.
FIGURE 5
Porous Tantalum for Patellar Reconstruction
Instrumentation/Implantation
Porous Tantalum for Patellar Reconstruction
464
PEARLS
B
After the bearing surface has
been cemented into the porous
tantalum shell, check the
patellar tracking.
Use either a lateral retinacular
release or medial retinacular
reeng to optimize tracking of
the patellar component.
FIGURE 6
Figure 6A shows the sutures being placed through
the peripheral holes on the porous tantalum shell
and through the patella and quadriceps tendon.
Figure 6B shows the porous tantalum shell after
suture placement.
465
STEP 3
The porous tantalum shell is manufactured to accept
the standard three-prong all-polyethylene bearing
surface.
The polyethylene bearing surface corresponding to
the femoral component of the revision hardware
should be utilized whenever possible.
Cement the polyethylene bearing surface into the
porous tantalum shell using standard cementation
and compression techniques. Figure 7 shows the
porous tantalum shell and polyethylene bearing
surface after completion of xation to the remaining
patellar bone and extensor mechanism.
STEP 4
Irrigate the knee and the nished components
thoroughly using a pulse lavage device.
Close the arthrotomy with heavy Vicryl sutures in an
interrupted fashion.
The skin and subcutaneous tissues are closed using
Vicryl and staples.
A drain may be used at the surgeons preference.
Porous Tantalum for Patellar Reconstruction
FIGURE 7
Porous Tantalum for Patellar Reconstruction
466
Postoperative Care and
Expected Outcomes
PITFALLS
Early outcome studies have
shown a potential increased risk
of patellar avulsion fractures at
the superior or inferior pole,
which may require additional
revision surgery.
Asandard physical therapy regimen as would be
instituted after primary TKA is recommended.
Include continuous passive motion machines
immediately postoperatively, range-of-motion
exercises, gait training, and conditioning exercises.
The dressings are removed on the second
postoperative day, and the staples are removed
2 weeks after surgery.
FIGURE 8A
467
There may be a role for a
protected physical therapy
regimen postoperatively, which
avoids active-resisted knee
extension exercises to
potentially decrease the
occurrence of patellar avulsion
fractures.
Follow-up radiographs are used to assess component
stability, xation, tracking, and alignment.
Anteroposterior (Fig. 8A), lateral (Fig. 8B), and
Merchants view (Fig. 8C) radiographs are
recommended postoperatively, between 4 and 12
weeks after surgery, and then based upon surgeon
preference.
We perform radiographs immediately
postoperatively, at 6 weeks, 6 months, and 1 year,
and then biennially.
Evidence
Barrack RL, Ingraham R, Matzkin E, Rorabeck CH, Engh GA. Results of revision total
knee with patellar replacement versus patellar bony shell. Clin Orthop Relat Res.
1998;356:139-43.
In this review of 113 revision total knee arthroplasties, the authors compared patient
outcomes after resection arthroplasty versus patellar replacement. (Level IV evidence
[case series])
Nelson CL, Lonner JH, Lahiji A, et al. Use of a trabecular metal patella for marked
patella bone loss during revision total knee arthroplasty. J Arthroplasty.
2003;18(Suppl 1):37-41.
This study outlines the authors technique for the use of porous tantalum for revision
surgery in which there is very poor or no patellar bone stock. The authors present
outcome data from 20 patients who underwent revision arthroplasty using this
method. (Level IV evidence [case series])
Nasser S, Poggie RA. Revision and salvage patellar arthroplasty using a porous
tantalum implant. J Arthroplasty. 2004;19:562-71.
The authors present their technique for patellar revisions using porous tantalum and
their results in a series of 11 patients. (Level IV evidence [case series])
Hanssen AD. Bone-grafting for severe patellar bone loss during revision knee
arthroplasty. J Bone Joint Surg [Am]. 2001;83:171-6.
This study looked at outcomes using the Knee Society scoring system in nine revision
total knee arthroplasties in which the patella was bone-grafted for severe bone
deciency. (Level IV evidence [case series])
Parvizi J, Seel MJ, Hanssen AD, et al. Patellar component resection arthroplasty for the
severely compromised patella. Clin Orthop Relat Res. 2002;397:356-61.
This study is a retrospective review of 35 revision total knee arthroplasties in which
the patella was treated with resection arthroplasty for decient bone stock. (Level IV
evidence [case series])
Scapinelli R. Blood supply of the human patella. J Bone Joint Surg [Br]. 1967;49:
563-70.
A laboratory study was performed in cadavers by injecting the femoral artery with
opaque contrast to demonstrate the vasculature that supplies the patella.
Porous Tantalum for Patellar Reconstruction
Controversies
PROCEDURE 33
Cancellous Patellar Bone
Grafting in Revision Total
Knee Arthroplasty
James L. Howard and Arlen D. Hanssen
Cancellous Patellar Bone Grafting
470
PITFALLS
Indications
Correct rotational positioning of
the femoral and tibial
components is a prerequisite for
a successful outcome.
Patellar bone grafting in the
setting of component malposition
will result in gradual lateral
subluxation of the patellar shell
construct.
Patellar bone grafting is indicated in severe patellar
bone deciency, which precludes adequate xation
of another patellar implant. This accounts for
approximately 10% of revision total knee arthroplasty
cases.
Cancellous patellar bone grafting provides potential
for restoration of bone stock, facilitates patellar
tracking, improves quadriceps leverage, and is
cosmetically appealing.
Examination/Imaging
Treatment Options
Structural bone grafting of the
patella
Patellar resection arthroplasty
Gull-wing osteotomy
Porous metal baseplate
Crossed Kirschner wires for
cemented xation of the
patellar component
Patellectomy should be avoided.
Examination of the extremity should include:
Skinassessment of location and shape of scars,
health of skin
Alignment
Stabilityanteroposterior and varus/valgus
Neurovascular examination
Range of motion assessment
Extensor mechanism integrity, presence of an
extensor lag
Radiographs
Anteroposterior and lateral views of the knee are
obtained.
Preoperatively, it is helpful to radiographically
assess whether the magnitude of patellar bone loss
preclude xation of another patellar implant.
Merchants views are particularly helpful in
assessing the status of the current patellar
component as well as the magnitude of patellar
bone loss.
Figure 1 shows a Merchants radiograph
demonstrating lateral subluxation of the patella
with lucency noted at the cement-bone interface
of the patellar component. The amount of
remaining patellar bone would preclude xation
of another patellar component.
Surgical Anatomy
The remaining patellar remnant consists of a shell of
anterior cortex and variable amounts of patellar rim.
In Figure 2A and 2B, the remnant consists of a shell
of anterior cortex with an intact patellar rim and
cavitary bone stock deciency.
Typically, there is a pseudomeniscus of scar tissue as
well as peripatellar brotic tissue on the undersurface
of the quadriceps tendon.
471
Cancellous Patellar Bone Grafting
FIGURE 1
Quadriceps
tendon
Patellar
tendon
Patellar
remnant
FIGURE 2
Cancellous Patellar Bone Grafting
472
Positioning
PEARLS
Portals/Exposures
Extension of the approach
proximally and distally can
make identication of the
appropriate planes easier when
elevating skin aps.
PITFALLS
Local peripatellar tissue
constitutes the basis of
cancellous patellar bone grafting,
and one should resist the
temptation to remove these
tissues during exposure.
PEARLS
If there is inadequate local soft
tissue, a free tissue ap can be
obtained from either the
suprapatellar pouch or the fascia
lata in the lateral gutter of the
knee joint.
Patients are positioned in the supine position on the
operating room table.
A tourniquet can be placed high on the patients
thigh based on surgeon preference.
The leg is prepped and draped free using an
extremity drape.
The previous midline anterior surgical incision should
be used and extended as required for the revision
arthroplasty.
If the patient has multiple anterior incisions, select
the most lateral (if feasible); otherwise, the bridge
between incisions is more likely to become
avascular.
Soft tissues should be handled carefully to minimize
trauma to the skin edges.
Minimize skin ischemia by elevating full-thickness
aps off of the musculotendinous layer.
The knee is opened with a medial parapatellar
arthrotomy.
Two marking sutures are placed at the superomedial
pole of the patella to facilitate accurate repair of the
extensor mechanism.
To mobilize the patella, adhesions in the
suprapatellar pouch, lateral gutter, and infrapatellar
area need to be released.
Retain the pseudomeniscus of scar tissue and most
of the peripatellar brotic tissue on the
undersurface of the quadriceps tendon as well as
tissue on the remaining patella.
The polyethylene insert can be removed to
decrease tension on the extensor mechanism and
simplify mobilization of the patella.
Femoral and tibial components are assessed. Careful
evaluation of femoral and tibial component rotational
position is mandatory. Revision of femoral and/or
tibial components is completed prior to patellar bone
grafting.
Procedure
STEP 1
The patellar shell is prepared by removing all brous
membrane in the crevices of the remaining patellar
bone.
The most reliable tissue for a local soft tissue ap lies
on the undersurface of the quadriceps tendon.
473
The ap is created by elevating the tissue from
proximal to distal from the undersurface of the
tendon (Fig. 3A and 3B). The base of the tissue is left
rmly attached to the superior aspect of the patella.
The tissue ap is then turned down and sewn into
the periphery of the pseudomeniscus/peripatellar
brous tissue and the remaining patellar rim.
A watertight closure is achieved using multiple
interrupted nonabsorbable size 0 sutures.
A small purse-string opening is left in one portion of
the tissue ap repair to facilitate delivery of bone
graft into the patellar defect.
Local soft
tissue flap
Quadriceps
tendon
Patellar
remnant
FIGURE 3
Cancellous Patellar Bone Grafting
Cancellous Patellar Bone Grafting
474
PEARLS
In the absence of locally
available cancellous autograft,
cancellous allograft bone can be
used.
STEP 2
Cancellous autograft is harvested from the
metaphyseal portion of the femur during femoral
preparation of the revision implant.
The bone graft is morselized into small fragments of
approximately 58 mm in height and width (Fig. 4).
This fragment size allows tight impaction of the bone
graft into the patellar shelltissue ap construct.
The bone graft is then tightly impacted through the
opening of the fascial ap into the patellar bone
defect.
Sufcient bone is added so that the nal patellar
construct has a height of between 20 and 25 mm.
STEP 3
The tissue ap is then closed completely to contain
the bone graft within the patellar shell (Fig. 5A and
5B).
The adequacy of the suture repair is examined to
ensure that the tissue ap securely contains the
impacted bone graft.
The peripatellar arthrotomy site is provisionally
repaired with several sutures or towel clips to mold
the patellar construct in the femoral trochlea as the
knee is placed through the full range of motion.
The tourniquet is released and bleeding is controlled.
The wound is irrigated.
The medial parapatellar arthrotomy is closed,
followed by closure of the subcutaneous tissue and
skin.
The limb is immobilized in a well-padded plaster
splint.
FIGURE 4
475
Cancellous Patellar Bone Grafting
Patellar bone
graft construct
B
FIGURE 5
Cancellous Patellar Bone Grafting
476
Postoperative Care and
Expected Outcomes
Surgical drains are removed on the rst postoperative
morning.
Antibiotic prophylaxis is provided for the rst 24
hours following surgery.
Deep venous thrombosis prophylaxis is individualized
based on the patient risk prole. Generally low-risk
patients receive multimodal prophylaxis consisting of
acetylsalicylic acid 325 mg orally twice daily,
antiembolism stockings (TEDS), and foot pumps.
High-risk patients receive coumadin for 6 weeks with
a target international normalized ratio of 1.72.2.
Postoperative rehabilitation is the same as the usual
protocol after revision knee arthroplasty.
Patients are mobilized on postoperative day 1 with
physiotherapy.
The knee is immobilized in a well-padded plaster
splint until the second morning after surgery. Then
the splint is removed and a light dressing applied
to the knee. Active and active-assisted knee range
of motion is then started with no restrictions.
We use a progressive weight-bearing protocol
starting with 40 pounds weight bearing for the
rst postoperative week. The patient then
progresses to 80 pounds in the second week and
120 pounds in the third week. Full weight bearing
with the use of a cane is started 4 weeks after
surgery. This is continued until the rst clinical
follow-up at 3 months.
The initial case series that described the technique
and early clinical results reported:
Improved postoperative Knee Society pain and
function scores.
Restoration of patellar bone stock with
incorporation of the bone graft and progressive
remodeling of the construct.
Figure 6A shows a postoperative Merchants
radiograph of the patellabone graft construct.
Figure 6B shows a Merchants radiograph 16
months after patellar bone grafting. There has
been molding and remodeling of the construct
against the femoral trochlea.
Complications included:
Arthrobrosis requiring manipulation
Tibiofemoral instability requiring reoperation to
increase polyethylene thickness
477
FIGURE 6
FIGURE 7
Femoral component loosening requiring revision
of the femoral component
Once patellar bone stock is restored using this
technique, it is possible to insert a new patellar
component at the time of subsequent revision
surgery.
Figure 7A shows a Merchants radiograph taken 6
years after patellar bone grafting. The patient
underwent surgery for revision total knee
arthroplasty for aseptic loosening of the femoral
component. At the time of the revision, patellar
bone stock was sufcient to allow resurfacing with
a new patellar component.
Figure 7B shows a Merchants radiograph 1 year
after revision total knee arthroplasty with a stable
patellar component in satisfactory position.
Evidence
Barrack RL, Matzkin E, Ingraham R, Engh G, Rorabeck C. Revision knee arthroplasty
with patella replacement versus bony shell. Clin Orthop Relat Res. 1998;(356):
139-43.
This study outlined the clinical results of revision total knee arthroplasties in which an
un-resurfaced bony shell was left after removing a patellar component versus those in
which a patellar component was implanted. (Level III evidence [retrospective
comparative study])
Cancellous Patellar Bone Grafting
Cancellous Patellar Bone Grafting
478
Berry DJ, Rand JA. Isolated patellar component revision of total knee arthroplasty. Clin
Orthop Relat Res. 1993;(286):110-5.
This study reported outcomes and complications in 42 knees that had isolated patellar
component revision of a total knee arthroplasty. (Level IV evidence [case series])
Buechel FF. Patellar tendon bone grafting for patellectomized patients having total
knee arthroplasty. Clin Orthop Relat Res. 1991;(271):72-8.
This study outlined the technique for restoring the moment arm to improve quadriceps
leverage after patellectomy by using a 2.5-cm diameter by 1-cm thick bone graft sewn
into the previous anatomic position of the patella, using a subsynovial pouch for
stabilization. Clinical results of seven knees were reviewed. (Level IV evidence [case
series])
Hanssen AD. Bone-grafting for severe patellar bone loss during revision knee
arthroplasty. J Bone Joint Surg Am. 2001;83:171-6.
This study reviewed the clinical results of nine patients managed with cancellous bone
grafting at the time of revision knee arthroplasty at a mean follow-up of 36.7 months.
The mean preoperative Knee Society scores for function and pain were 39 points and
40 points, respectively. At the time of nal follow-up, the Knee Society function and
pain scores showed signicant improvement to a mean pain score of 84 points and a
mean function score of 91 points. Patellar thickness improved from between 7 and
9 mm intraoperatively to 19.7 mm at nal clinical follow-up. (Level IV evidence [case
series])
Hanssen AD, Pagnano MW. Revision of failed patellar components. Instr Course Lect.
2004;53:201-6.
This lecture discussed revision of failed patellar components. The discussion included
management techniques for patellas with severe bone deciency, including patellar
resection arthroplasty, the gull-wing osteotomy, structural bone grafting of the patella,
morcellized bone grafting of the patella, and the use of a porous metal baseplate.
Nelson CL, Lonner JH, Lahiji A, Kim J, Lotke PA. Use of a trabecular metal patella for
marked patella bone loss during revision total knee arthroplasty. J Arthroplasty.
2003;18(7 Suppl 1):37-41.
This study evaluated the short-term results in 20 patients following patellar
resurfacing with a trabecular metal patella shell in the setting of severe patellar bone
loss at the time of revision total knee arthroplasty. (Level IV evidence [case series])
Pagnano MW, Scuderi GR, Insall JN. Patellar component resection in revision and
reimplantation total knee arthroplasty. Clin Orthop Relat Res. 1998;(356):134-8.
This study evaluated outcomes in 34 knees that had a revision or reimplantation total
knee arthroplasty in which the patellar component could not be reinserted because of
markedly compromised patellar bone stock. (Level IV evidence [case series])
Parvizi J, Seel MJ, Hanssen AD, Berry DJ, Morrey BF. Patellar component resection
arthroplasty for the severely compromised patella. Clin Orthop Relat Res.
2002;(397):356-61.
This study evaluated the clinical and functional results of patellar component resection
arthroplasty in 35 knees. (Level IV evidence [case series])
Rorabeck CH, Mehin R, Barrack RL. Patellar options in revision total knee arthroplasty.
Clin Orthop Relat Res. 2003;(416):84-92.
This review article outlined the various treatment options for management of the
patella in revision total knee arthroplasty.
Tabutin J. Osseous reconstruction of the patella with screwed autologous graft in the
course of repeat prosthesis of the knee. Rev Chir Orthop Reparatrice Appar Mot.
1998;84:363-7.
The study described the technique of structural bone grafting of the patella when faced
with severe patellar bone stock deciency. Two clinical cases were presented. (Level IV
evidence [case series])
PROCEDURE 34
Hinged Total Knee
Arthroplasty
Bryan D. Springer
Hinged Total Knee Arthroplasty
480
Indications
PITFALLS
Fixed hinges such as the
Waldius and Guepar were
associated with high rates of
loosening and infection (Fig. 4A).
With the advent of the modern
rotating hinge design, there is no
current indication for the use of
xed hinges (Fig. 4B).
Hinged total knee arthroplasty is utilized as a salvage
procedure for complex primary or revision total knee
arthroplasty. Indications include:
Limb salvage following periarticular tumor
resection
Severe bony deciency requiring segmental
replacement
Medial collateral ligament disruption
Extensor mechanism disruption
Signicant exion and extension gap mismatch
Treatment of periprosthetic fracture about the knee
with associated with severe bone loss in lowdemand patients (Fig. 1)
Salvage of previous nonunion/malunion of
periprosthetic fracture about the knee (Fig. 2)
Recurvatum deformity secondary to quadriceps
weakness (underlying neurologic disorder or
previous cerebrovascular accident) (Fig. 3)
FIGURE 1
FIGURE 2
481
Hinged Total Knee Arthroplasty
FIGURE 3
Controversies
Controversies exist regarding
the use of hinged total knee
arthroplasty for treatment of
periprosthetic fracture
associated with signicant bone
loss or poor-quality bone. The
general consensus is that hinged
total knee arthroplasty in
elderly, low-demand patients
allows for quicker mobilization
and recovery (Fig. 5A and 5B).
A
FIGURE 4
Hinged Total Knee Arthroplasty
482
FIGURE 5
Examination/Imaging
PREOPERATIVE EXAMINATION
Examination of skin for color, temperature changes,
and effusion that would indicate infection
Evaluation of old incisions
Vascular and neurologic status of the limb
Range of motion
Collateral ligament stability
Function of the extensor mechanism
Presence of recurvatum deformity
PREOPERATIVE PLANNING
As with any primary or revision total knee
arthroplasty, preoperative planning is essential.
Appropriate radiographs include a standing
anteroposterior view, lateral view, and Merchants
483
Hinged Total Knee Arthroplasty
FIGURE 6
view. Each of these radiographs should be evaluated
to assess bone loss and quality of remaining host
bone. In addition, a long leg hip-to-ankle view may
be utilized to assess the overall mechanical alignment
of the extremity and to assess for other hardware
that may interfere with placement of a long-stem
hinged total knee arthroplasty (e.g., total hip
arthroplasty above a total knee arthroplasty).
Templating of both the femoral (Fig. 6A) and tibial
(Fig. 6B) components is mandatory. In addition to
estimating the size of the components, templating is
utilized to estimate bone resection levels and the
need for augmentation as well as the length,
position, and size of intramedullary stems.
If performing the reconstruction for bone sarcomas,
preoperative imaging studies such as computed
tomography scans and magnetic resonance imaging
studies of the extremity should be reviewed to
determine a safe resection level about the femur or
tibia in order to gain adequate tumor-free margins.
Hinged Total Knee Arthroplasty
484
Superficial
femoral
artery
Sciatic nerve
Popliteal
artery
Tibial
nerve
Peroneal
nerve
FIGURE 7
Surgical Anatomy
PEARLS
If a large exposure is required, a
sterile tourniquet should be
utilized in order to allow
exposure to the proximal aspect
of the thigh, groin, and pelvis.
In patients with severe distal femoral or proximal
tibial bone loss or neoplastic disease, resection of the
distal femur or proximal tibia may be required. As
such, familiarity with the distal femoral and popliteal
space anatomy is important to avoid damage to the
supercial femoral artery during distal femoral
resection, the popliteal artery and sciatic nerve
during posterior dissection, and the tibial artery, tibial
nerve, and peroneal nerve during proximal tibial
dissection and resection (Fig. 7).
Positioning
The patient is placed supine on the operating table.
A nonsterile tourniquet is placed on the upper thigh.
Positioning should allow for free mobility of the knee
through the full range of exion and extension. A leg
positioner should be used to allow the knee to ex
and rest at 90 of exion to assist in femoral and
tibial preparation.
In cases in which large-scale resection of the femur
or tibia may be required, the entire extremity,
including the groin and pelvis, should be prepped
and draped.
485
Because hinged total knee
arthroplasty is often used in a
salvage situation, most patients
have had multiple previous
incisions. Large exposures and
bony resection may often
compromise the already tenuous
soft tissue envelope. Consultation
with a plastic surgeon
preoperatively to assess the need
for soft tissue coverage at the
time of the procedure may be
warranted in some cases.
Portals/Exposures
Utilize prior incisions.
When multiple incisions are present, use the most
laterally based incision. Any aps that are created
should be full thickness to avoid compromise of the
blood supply to the skin.
A standard medial parapatellar approach or extensile
exposures may be required.
Once they are exposed, removal of the failed tibial
and femoral components should proceed, preserving
as much of the remaining bone as possible. Remove
all cement and debris and dbride all bony surfaces
down to good-quality bone.
Procedure
PEARLS
Ensure the tibial reamers remain
in line with the shaft of the tibia
when reaming. Retained cement,
sclerotic bone, or tibial deformity
may inuence reamer position
and lead to cortical perforation.
STEP 1: TIBIAL PREPARATION
Prepare the tibial canal and establish a proximal tibial
supportive bony platform perpendicular to the
mechanical axis.
The tibial surface may be cut utilizing
extramedullary or intramedullary instrumentation
(Fig. 8).
PITFALLS
In patients with substantial
proximal bony deciency, a longstem cemented or cementless
tibial implant may be required
for xation. In patients with
metaphyseal or diaphyseal
deformity, an offset stem may be
required to obtain appropriate
alignment in the intramedullary
canal.
FIGURE 8
Hinged Total Knee Arthroplasty
PITFALLS
Hinged Total Knee Arthroplasty
486
FIGURE 9
Instrumentation/
Implantation
Straight reamers in 0.5-mm
increments should be available.
If deformity on the tibial
diaphysis exists, exible reamers
may be utilized.
FIGURE 10
The tibial canal is prepared by reaming to the
appropriate size and depth based on preoperative
templating or until cortical contact is made
(Fig. 9).
Determine the appropriate depth of the tibial
resection. The purpose of this cut is to obtain a
at, supportive bony platform. It may be
unnecessary to cut below all defects as these may
be lled in with bone graft or augmented.
Cut the proximal tibia using the preferred
instrumentation. Determine the need for block or
wedge augmentation and make the appropriate
bony cuts on the tibia. The tibal baseplate can
then be sized. A trial tibial component with the
appropriate-length stem and augments can then
be inserted (Fig. 10).
STEP 2: FEMORAL PREPARATION
Femoral canal preparation
Identify and progressively ream the femoral canal
to the appropriate size based on preoperative
templating or until cortical contact is made. Avoid
eccentric reaming of the femoral shaft.
If a bowed femoral stem is to be utilized, the
femoral canal should be exibly reamed.
The size of the femoral component is determined by
preoperative templating and the amount of
remaining host bone.
487
Hinged Total Knee Arthroplasty
PEARLS
If distal femoral segmental
replacement is necessary, the
distal femur should be resected
rst. When a diaphyseal
resection is required, it is
imperative to mark the rotation
of the deepest section of the
trochlear groove on the remaining
diaphyseal segment. This will
allow for correct femoral
prosthesis rotational alignment
(Fig. 12).
FIGURE 11
Femoral component rotation
The rotation of the femoral component is critical
to achieving proper exion gap symmetry and
patellofemoral mechanics. In the revision setting,
however, many of the key bony landmarks used to
determine femoral component rotation, such as
the transepicondylar axis, posterior condylar axis,
and trochlear groove, are absent or damaged
(Fig. 11).
FIGURE 12
Hinged Total Knee Arthroplasty
488
In these situations, the tibial shaft axis should be
utilized to establish femoral component rotation
and ensure a symmetric rectangular exion gap
and appropriate external rotation of the femoral
component (see Fig. 11).
Once the femoral size and rotation have been
determined, the appropriate jig system should be
used to complete the cuts on the femur. At this
juncture, note the areas of bony deciency that may
require augmentation.
STEP 3: BALANCE THE KNEE IN FLEXION
AND EXTENSION
Balancing the knee in exion
Keeping in mind that a hinged total knee
arthroplasty is often indicated to treat a signicant
exion-extension gap mismatch (>10 mm), an
attempt should be made to maximize stability in
exion.
As assessment of the exion and extension gap
asymmetry may be made by several methods,
including direct measurement and spacer blocks
(Fig. 13A and 13B).
Flexion gap stability is achieved by maximizing
femoral component anteroposterior distance and
lling this gap with appropriate posterior femoral
augmentation.
A
FIGURE 13
489
PEARLS
Particular attention should be
paid to patellofemoral tracking,
one of the most common
complications associated with
hinged total knee arthroplasty. If
patellar tracking is inappropriate,
femoral component rotation must
be evaluated and adjusted
accordingly.
Balance the knee in extension
Extension gap stability is achieved by distal
augmentation of the femur (loose extension gap)
or further resection of the distal femur (tight
extension gap).
Most hinge systems will allow a certain degree of
hyperextension. This is usually limited with an
extension stop bumper. It is important to limit any
hyperextension so as to avoid stress on the
bumper that could result in implant breakage.
STEP 4: TRIAL REDUCTION AND
RADIOGRAPHIC EVALUATION
Perform a trial reduction.
When reasonable gap balance is achieved,
assemble the trial components with the
appropriate stem length and diameter.
Distal and posterior femoral augments and tibial
augments should be utilized based on the
intraoperative assessment of gap balancing and to
accommodate for bony deciency.
With the appropriate trial components in place
(Fig. 14), the knee should be taken through a
range of motion to ensure proper stability and
patellar tracking.
The hinged components will substitute for coronal
and sagital plane imbalance.
FIGURE 14
Hinged Total Knee Arthroplasty
Hinged Total Knee Arthroplasty
490
A
FIGURE 15
PEARLS
Each rotating hinge system that
is available has a different
mechanism of linked constraint
between the femoral and tibial
component. It is important for
the surgeon to be familiar with
the system being used to ensure
proper assembly.
Intraoperative radiographs with trial components in
place are crucial to ensure appropriate alignment of
the extremity, restoration of the joint line, and
position of the stems within the intramedullary canal
of the femur (Fig. 15A and 15B).
STEP 5: ASSEMBLY AND INSERTION OF
FINAL COMPONENTS
If intraoperative trialing and radiographs conrm
appropriate alignment, stability, and patellofemoral
tracking, the nal implants should be opened
(Fig. 16).
Meticulous care and attention should be paid to
assembly of the nal components. The operating
surgeon or an experienced assistant should
assemble the nal components on the back table
(Fig. 17A17C).
Ensure the appropriate augments, stem length,
diameter, and offset match from the intraoperative
trial components. If necessary, insert the nal
components provisionally into the bone to ensure
proper t.
491
Hinged Total Knee Arthroplasty
FIGURE 16
FIGURE 17
B
A
Hinged Total Knee Arthroplasty
492
Controversies
With the additional constraint
that is achieved with the use of
a hinged component, additional
xation with intramedullary
stems is required. Both
cemented and cementless stem
xation is available for most
systems. If cementless stems are
to be used, they should be
press-t, diaphysis-engaging
stems.
The femoral and tibial canals should be copiously
lavaged and dried. The distal diaphyseal bone of the
femur and tibia should be restricted with a canal
plug if cemented stems are to be used.
The tibial and femoral components should be
cemented separately under separate mixing
conditions, allowing for the cement to fully cure
before proceeding to cementing the next
component.
Once all components have been cemented, the
linked polyethylene is assembled. Care should be
taken to ensure proper assembly of the linking
mechanism (Fig. 18A18C).
Stability and patellar tracking should again be
assessed, ensuring proper patellofemoral tracking.
FIGURE 18
493
Common complications
following hinged total knee
arthroplasty include:
Wound complications
Patellofemoral complications
Deep periprosthetic infection
Hardware failure
Postoperative Care and
Expected Outcomes
Suction drainage should be utilized and left in place
until drainage is less than 30 mL in 8 hours.
Standard postoperative antibiotics are administered
for 24 hours.
Meticulous care should be take with regard to the
soft tissue envelope. Oftentimes large exposure and
lengthy surgical time can lead to soft tissue healing
issues.
Institution of physical therapy can be started when
the soft tissue envelope allows, and progressed as
tolerated.
In general, patients are allowed to bear weight as
tolerated with an assistive device until quadriceps
strength is adequate to allow for transfer to a
cane.
Evidence
Barrack RL. Evolution of the rotating hinge for complex total knee arthroplasty. Clin
Orthop Relat Res. 2001;(392):292-9.
The author reported that clinical results, range of motion, and patient satisfaction for
revision with a rotating hinge prosthesis were compatible with those of condylar
revision total arthroplasty at short-term follow-up.
Barrack RL. Rise of the rotating hinge in revision total knee arthroplasty. Orthopedics.
2002;25:1020.
The author summarized the increasing role and expanding indications for rotating
hinged total knee arthroplasty.
Barrack RL, Lyons TR, Ingraham RQ, Johnson JC. The use of a modular rotating hinge
component in salvage revision total knee arthroplasty. J Arthroplasty. 2000;15:85866.
The authors reported on the results with a second-generation mobile-bearing hinged
total knee arthroplasty for salvage revision total knee arthroplasty. Sixteen knees were
followed for an average of 51 months. Short-term clinical and radiographic results
were encouraging in this complex group of patients.
Harrison RJ Jr, Thacker MM, Pitcher JD, Temple HT, Scully SP. Distal femur replacement
is useful in complex total knee arthroplasty revisions. Clin Orthop Rel Res.
2006;(446):113-20.
The authors reviewed the development of, indications for, technique of, and existing
literature on distal femoral replacement for complex total knee revisions.
Jones RE. Mobile bearings in revision total knee arthroplasty. Instr Course Lect.
2005;54:225-31.
This article reviews the current indications and results of mobile-bearing hinged total
knee arthroplasty.
Hinged Total Knee Arthroplasty
Complications
Hinged Total Knee Arthroplasty
494
Jones RE, Barrack RL, Skedros J. Modular, mobile-bearing hinge total knee arthroplasty.
Clin Orthop Relat Res. 2001:392:306-14.
The authors reported on the result of SROM hinged total knee arthroplasty in 30 knees
at an average follow-up of 49 months. They reported excellent midterm results with
few complications.
Springer BD, Sim FH, Hanssen AD, Lewallen DG. The kinematic rotating hinge
prosthesis for complex knee arthroplasty. Clin Orthop Relat Res. 2001;(392):181-7.
This study reviewed the Mayo Clinic experience with the kinematic rotating hinge for
complex knee arthroplasty. Sixty-nine knees were followed for an average of 75
months. Although functional scores improved, complications were numerous.
Westrich GH, Mollano AV, Sculco TP, Buly RL, Laskin RS, Windsor R. Rotating hinge
total knee arthroplasty in severly affected knees. Clin Orthop Relat Res.
2000;(379):195-208.
This retrospective article reviewed the authors experience with use of a rotating hinge
device for severely affected knees. It reported on 24 knees at an average follow-up of
33 months. Pain and function markedly improved in this severely affected group.
Anda mungkin juga menyukai
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDari EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifePenilaian: 4 dari 5 bintang4/5 (5794)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDari EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You ArePenilaian: 4 dari 5 bintang4/5 (1090)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDari EverandNever Split the Difference: Negotiating As If Your Life Depended On ItPenilaian: 4.5 dari 5 bintang4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDari EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RacePenilaian: 4 dari 5 bintang4/5 (895)
- Grit: The Power of Passion and PerseveranceDari EverandGrit: The Power of Passion and PerseverancePenilaian: 4 dari 5 bintang4/5 (588)
- Shoe Dog: A Memoir by the Creator of NikeDari EverandShoe Dog: A Memoir by the Creator of NikePenilaian: 4.5 dari 5 bintang4.5/5 (537)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDari EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersPenilaian: 4.5 dari 5 bintang4.5/5 (344)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDari EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FuturePenilaian: 4.5 dari 5 bintang4.5/5 (474)
- Her Body and Other Parties: StoriesDari EverandHer Body and Other Parties: StoriesPenilaian: 4 dari 5 bintang4/5 (821)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Dari EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Penilaian: 4.5 dari 5 bintang4.5/5 (121)
- The Emperor of All Maladies: A Biography of CancerDari EverandThe Emperor of All Maladies: A Biography of CancerPenilaian: 4.5 dari 5 bintang4.5/5 (271)
- The Little Book of Hygge: Danish Secrets to Happy LivingDari EverandThe Little Book of Hygge: Danish Secrets to Happy LivingPenilaian: 3.5 dari 5 bintang3.5/5 (400)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDari EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyPenilaian: 3.5 dari 5 bintang3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)Dari EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Penilaian: 4 dari 5 bintang4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDari EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaPenilaian: 4.5 dari 5 bintang4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDari EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryPenilaian: 3.5 dari 5 bintang3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnDari EverandTeam of Rivals: The Political Genius of Abraham LincolnPenilaian: 4.5 dari 5 bintang4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealDari EverandOn Fire: The (Burning) Case for a Green New DealPenilaian: 4 dari 5 bintang4/5 (74)
- The Unwinding: An Inner History of the New AmericaDari EverandThe Unwinding: An Inner History of the New AmericaPenilaian: 4 dari 5 bintang4/5 (45)
- URGE SURFING-DBT For Sub Use PDFDokumen5 halamanURGE SURFING-DBT For Sub Use PDFAmy Powers100% (1)
- Rise of ISIS: A Threat We Can't IgnoreDari EverandRise of ISIS: A Threat We Can't IgnorePenilaian: 3.5 dari 5 bintang3.5/5 (137)
- Handy Summary Chart Comparing The Main Medications For PsychosisDokumen3 halamanHandy Summary Chart Comparing The Main Medications For Psychosisrowanpurdy100% (2)
- Exercise HeartDokumen36 halamanExercise Heartmelho.cottonBelum ada peringkat
- Post Ira LopDokumen35 halamanPost Ira Lopmelho.cotton100% (1)
- And Wrapping 2nd EditionDokumen16 halamanAnd Wrapping 2nd Editionmelho.cottonBelum ada peringkat
- Deadman Mazin Al Khafaji Kevin BakerDokumen34 halamanDeadman Mazin Al Khafaji Kevin Bakermelho.cottonBelum ada peringkat
- Acupunctureder NomenclatureDokumen15 halamanAcupunctureder Nomenclaturemelho.cottonBelum ada peringkat
- Liechniques and Methods NodrmDokumen21 halamanLiechniques and Methods Nodrmmelho.cottonBelum ada peringkat
- Po PunctureDokumen35 halamanPo Puncturemelho.cottonBelum ada peringkat
- Anatomy UrgDokumen51 halamanAnatomy Urgmelho.cottonBelum ada peringkat
- HiolpopoDokumen16 halamanHiolpopomelho.cotton0% (2)
- AnatomertreDokumen41 halamanAnatomertremelho.cottonBelum ada peringkat
- Anatol o PioDokumen46 halamanAnatol o Piomelho.cottonBelum ada peringkat
- Hern 4 PopDokumen20 halamanHern 4 Popmelho.cottonBelum ada peringkat
- HiolpopoDokumen16 halamanHiolpopomelho.cotton0% (2)
- HioloDokumen4 halamanHiolomelho.cottonBelum ada peringkat
- Dirección: Calle Bruselas Nro. 247 - Lima 34 Web: Telf.: 0051 1 449 2190 Cel.: 995 745 900 RPM: 201 539 / #472 132Dokumen6 halamanDirección: Calle Bruselas Nro. 247 - Lima 34 Web: Telf.: 0051 1 449 2190 Cel.: 995 745 900 RPM: 201 539 / #472 132melho.cottonBelum ada peringkat
- Assignment - Define DrugDokumen10 halamanAssignment - Define DrugDaiyne C. CarbonBelum ada peringkat
- Engaging With Research: Linking Evidence With PracticeDokumen2 halamanEngaging With Research: Linking Evidence With PracticeTomáš KrajíčekBelum ada peringkat
- Psychodynamic Interpersonal Therapy For Substance Use DisordersDokumen11 halamanPsychodynamic Interpersonal Therapy For Substance Use DisordersFrancesca PalazzoloBelum ada peringkat
- Centric & Protrusive RecordDokumen51 halamanCentric & Protrusive RecordHadil AltilbaniBelum ada peringkat
- EXAM 2 ReviewDokumen14 halamanEXAM 2 ReviewAndy CordekBelum ada peringkat
- NCP 2Dokumen3 halamanNCP 2klawdin100% (1)
- AnticholinergicsDokumen33 halamanAnticholinergicspramod bhaleraoBelum ada peringkat
- First Steps in REBT - Windy DrydenDokumen44 halamanFirst Steps in REBT - Windy DrydenStefan Alexandru100% (4)
- 3 - Lectures of Capsules PracticalDokumen4 halaman3 - Lectures of Capsules PracticalsultanBelum ada peringkat
- Peroneus Longus Tendon Rupture: A Case Report: BackgroundDokumen14 halamanPeroneus Longus Tendon Rupture: A Case Report: BackgroundAlgivar DaudBelum ada peringkat
- Purifying LimeDokumen19 halamanPurifying LimeNazihCosmeticsBelum ada peringkat
- Endocrine LabDokumen15 halamanEndocrine Labapi-217439283Belum ada peringkat
- Internet AddictionDokumen6 halamanInternet AddictionstupidshitBelum ada peringkat
- QuizDokumen8 halamanQuizJohara Mae De RamaBelum ada peringkat
- Temporary Abdominal Closure: Positive ResultsDokumen8 halamanTemporary Abdominal Closure: Positive ResultsCarlos HernándezBelum ada peringkat
- Bells Palsy FPUK Web PDFDokumen11 halamanBells Palsy FPUK Web PDFRadhaKrishnanBelum ada peringkat
- I. Approach To Clinical Interviewing and DiagnosisDokumen6 halamanI. Approach To Clinical Interviewing and DiagnosisRoci ArceBelum ada peringkat
- Foundation of Guidance 1Dokumen16 halamanFoundation of Guidance 1leo sentelicesBelum ada peringkat
- Low Back Pain - Differential Diagnosis, Prognosis and TreatmentDokumen4 halamanLow Back Pain - Differential Diagnosis, Prognosis and TreatmentFifi TandionBelum ada peringkat
- Biniam 2019 CVDokumen5 halamanBiniam 2019 CVBiniam Abeelo TadeleBelum ada peringkat
- HealOzone Brochure 02 PDFDokumen9 halamanHealOzone Brochure 02 PDFAGBelum ada peringkat
- Dinis Oliveira 2010Dokumen52 halamanDinis Oliveira 2010Consuelo VegaBelum ada peringkat
- Causes and Treatment Outcome of Mechanical Bowel Obstruction in North Eastern NigeriaDokumen3 halamanCauses and Treatment Outcome of Mechanical Bowel Obstruction in North Eastern NigeriakeithBelum ada peringkat
- Manual de Interaccion Centrada en El TemaDokumen343 halamanManual de Interaccion Centrada en El Temayobelixx_2013Belum ada peringkat
- Kukuh Satriyo N - Askep InggrisDokumen15 halamanKukuh Satriyo N - Askep InggrisMesi Prasetya SBelum ada peringkat
- Acl Rupturer - TextbookDokumen26 halamanAcl Rupturer - TextbookFakhrun Nisa WitringBelum ada peringkat
- Mylan EpiPen StatementDokumen3 halamanMylan EpiPen StatementCBS This MorningBelum ada peringkat
- Smart Shoe (OPU-1719052)Dokumen1 halamanSmart Shoe (OPU-1719052)17044 AZMAIN IKTIDER AKASHBelum ada peringkat