15ACG Southern Regional 0008
Diunggah oleh
Raja AndrianyHak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
15ACG Southern Regional 0008
Diunggah oleh
Raja AndrianyHak Cipta:
Format Tersedia
Vivek Kaul, MD, FACG
Peri-endoscopic Management of
Antithrombotics & Anticoagulants
ACG Postgraduate Course, Nashville, TN
Dec 5, 2015
Vivek Kaul, MD, FACG
g
Segal-Watson
Professor of Medicine
Chief of Gastroenterology & Hepatology
University of Rochester Medical Center
vivek_kaul@urmc.rochester.edu
ACG 2015 Nashville Regional Postgraduate Course
Copyright 2015 American College of Gastroenterology
Vivek Kaul, MD, FACG
Objectives
Review Bleeding Risk: Endoscopic Procedures
and Interventions
Risk Stratification of Low & High risk
Thrombotic Conditions Encountered in Clinical
Practice
Review Newer AntiPlatelet Therapy Options
and
d Novel
N l Oral
O l AntiCoagulants
A tiC
l t
Discuss current concepts & best practice
principles based on available data
Balancing Risk of GI Bleeding vs Risk of
Thromboembolic Events
GI Bleeding @ Endoscopy
Thromboembolic
Event
ACG 2015 Nashville Regional Postgraduate Course
Copyright 2015 American College of Gastroenterology
Vivek Kaul, MD, FACG
Anti-Thrombotic Agents
Anticoagulants
Warfarin
Heparin
Low molecular weight heparin
Novel Oral AntiCoagulants (NOAC)
Anti-platelet agents
p
Aspirin
Non-steroidal anti-inflammatory agents
(NSAID)
Thienopyridine (clopidogrel, ticlopidine)
Glycoprotein IIb/IIIa receptor inhibitors
Focus On
Aspirin
Warfarin (vit K: II,VII, IX, X)
Clopidogrel
NOACs
Apixaban (Xa)
Rivaroxaban (Xa)
Dabigatran (Thrombin)
ACG 2015 Nashville Regional Postgraduate Course
Copyright 2015 American College of Gastroenterology
Vivek Kaul, MD, FACG
ASGE and ESGE Guidelines on Endoscopy and Antithrombotic Agents
ACG 2015 Nashville Regional Postgraduate Course
Copyright 2015 American College of Gastroenterology
Vivek Kaul, MD, FACG
So How Should We Approach This?
What do we know right now? (questions that
have been answered)
What to do with anti thrombotic agents pre
and post elective endoscopy?
What to do with anti thrombotic agents in a
patient with GI bleeding?
Review our best practices for now while we
gain more experience with newer
agents/more data becomes available
Surgical Interventions: Risk Stratification By
Bleeding Risk
Low risk
Endoscopy
biopsy
doscopy with
t b
opsy
Prostate or bladder biopsy
Electrophysiological study or
radiofrequency catheter ablation for
High risk
Complex left-sided ablation: pulmonary vein
i l ti
VT ablation
bl ti
isolation,
Spinal or epidural anesthesia; lumbar
diagnostic puncture
Thoracic surgery
Abdominal surgery
puncture)
Major orthopedic surgery
g g p y
Angiography
p y
Liver biopsy
Pacemaker or ICD implantation (unless
Transurethral prostate resection
Kidney biopsy
supraventricular tachycardia (including left
sided ablation via single transseptal
complex anatomical setting e.g. congenital
heart disease)
www.escardio.org/EHRA
ACG 2015 Nashville Regional Postgraduate Course
Copyright 2015 American College of Gastroenterology
Vivek Kaul, MD, FACG
Endoscopic Procedures:
Bleeding Risk
Risk Factors: GI Bleeding
Older age
Cigarette smoking
Sleep apnea
Male gender
CVA, DVT
Prior GI bleeding
Renal Insufficiency
ACG 2015 Nashville Regional Postgraduate Course
Copyright 2015 American College of Gastroenterology
Vivek Kaul, MD, FACG
ISTH: Definitions of Bleeding
Cardiovascular Conditions: Risk Status
ACG 2015 Nashville Regional Postgraduate Course
Copyright 2015 American College of Gastroenterology
Vivek Kaul, MD, FACG
Risk of Thromboembolic Event in
Peri-endoscopic Period
Atrial Fibrillation with h/o
/ embolic events or
valve disease
Prosthetic Valve
Coronary artery disease and stents
Deep Venous Thrombosis/Pulmonary Embolus
Stroke/Transient Ischemic Attack
Hypercoagulable states
Prosthetic Valve
High risk conditions for thromboembolic events
Bio prosthetic valve <3 months old
Mechanical valve in mitral position
Mechanical valve with previous
thromboembolic event
ACG 2015 Nashville Regional Postgraduate Course
Copyright 2015 American College of Gastroenterology
Vivek Kaul, MD, FACG
Coronary Artery Disease and Stents
High risk conditions for thromboembolic events
Recent acute coronary event <4-6
<4 6 weeks
Discontinuing dual antiplatelet therapy
in:
Drug-eluting stent < 1 year
Bare metal stent < 1 month
Stroke/Transient Ischemic Attack
High risk conditions for thromboembolic events
Cardioembolic events
Carotid artery disease
Recent carotid
endarterectomy
Hypercoagulable state
ACG 2015 Nashville Regional Postgraduate Course
Copyright 2015 American College of Gastroenterology
Vivek Kaul, MD, FACG
It is therefore strongly
recommended that the gastroenterologist /endoscopist never
be the one to instruct the patient to stop any anticoagulant or
antiplatelet therapy. This should be a recommendation pending
the patient finalizing approval by the prescriber of these
agents typically the cardiologist, neurologist, and vascular
surgeon or primary care provider.
Parth J. Parekh , MD , Jonathan Merrell , MD , Meredith Clary , MD , John E. Brush , MD, FACC , and David A. Johnson , MD, FACG, FASGE
Am J Gastroenterol 2014; 109:9 19
Antithrombotics:
Mechanisms of Action &
Current Knowledge
ACG 2015 Nashville Regional Postgraduate Course
Copyright 2015 American College of Gastroenterology
10
Vivek Kaul, MD, FACG
What do we know about Aspirin?
ASGE Guideline: Continue ASA for GI procedures
N
t di ASA ((and
d NSAID
Numerous
studies:
NSAIDs)) no
significant increase in risk of GI bleeding for
routine GI procedures like EGD/biopsy,
colonoscopy with polypectomy,
ERCP/sphincterotomy
For
High
bleeding
may elect
F Hi
h risk
i k bl
di GI procedures,
d
l t
to hold for 5-7 days if patient at low risk for
CV/CNS consequences or could continue it
Management of antithrombotic agents for endoscopic procedures.
ASGE Standards of Practice Committee. 2009
What About Adenosine Diphosphate
Antagonists (Thienopyridines)?
The thienopyridines block the ADP-dependent
ti off platelets
l t l t b
hibiti the
th P2Y
aggregation
by iinhibiting
12 receptor.
Clopidogrel, Prasugrel
Similar to Aspirin (effect upto 7-10 days), the
effect on the platelets can last for 5-7 days
after the drug has been withdrawn
No reversal agent
ACG 2015 Nashville Regional Postgraduate Course
Copyright 2015 American College of Gastroenterology
11
Vivek Kaul, MD, FACG
Adenosine diphosphate antagonists
(Thienopyridines)
Coagulation Cascade: Warfarin & NOAC
Sites of Action
ACG 2015 Nashville Regional Postgraduate Course
Copyright 2015 American College of Gastroenterology
12
Vivek Kaul, MD, FACG
Novel Oral AntiCoagulants (NOAC)
NOACs work in one of two ways:
Rivaroxaban, Edoxaban and
Apixaban: factor Xa inhibitors.
Dabigatran: directly inhibiting
thrombin DTI
NOACs
(Novel Oral Anticoagulation Agents)
Stroke prevention in AF
Prevention of DVT
Treatment of DVT
Preferred over Warfarin
Quick on/quick off
No monitoring needed
Fewer interactions
Used globally
ACG 2015 Nashville Regional Postgraduate Course
Copyright 2015 American College of Gastroenterology
13
Vivek Kaul, MD, FACG
NOAC vs Warfarin
NOAC: Proven non-inferior or superior
No monitoring needed
Faster onset of action (2-4 hrs)
Faster out of system (normal renal/hepatic function)
Decreased risk of intracranial bleeding
Apixaban 110 mg BID dose:
Decreased risk of bleeding into any site
NOACs: associated with increased GI bleeding
Antidote??
Upper GI Bleeding: NOAC Rx
ACG 2015 Nashville Regional Postgraduate Course
Copyright 2015 American College of Gastroenterology
14
Vivek Kaul, MD, FACG
Lower GI Bleeding: NOAC Rx
Management Guidelines
Elective Endoscopic Procedures
Acute GI Bleeding
ACG 2015 Nashville Regional Postgraduate Course
Copyright 2015 American College of Gastroenterology
15
Vivek Kaul, MD, FACG
General Approach to Patients on
Antithrombotics Who Need Elective Endoscopy
Delay ELECTIVE endoscopy until patient at lower risk
for thromboembolism
Discuss with patients cardiovascular or neurovascular
physician whether (or when) drugs can be stopped
Realize that only limited data exist
Guidelines from ASGE, ESGE are only suggestions Need to weigh the risks and benefits for each
individual patient
Aspirin
Stop it Rarely, if ever
ACG 2015 Nashville Regional Postgraduate Course
Copyright 2015 American College of Gastroenterology
16
Vivek Kaul, MD, FACG
How To Manage Warfarin Prior to
Endoscopic Procedures?
Avoid Vitamin K before elective procedures: delays
th
ti re-anticoagulation
ti
l ti after
ft procedure
d
therapeutic
Warfarin can usually be stopped for 4-7 days and then
be restarted the following day
1% risk of thromboembolic events after temporary
warfarin cessation
High risk patients for thromboembolic events: Bridge
with LMW heparin.
Example of Decision making in
Elective Endoscopy: Warfarin
Management of antithrombotic agents for endoscopic procedures.
ASGE Standards of Practice Committee. 2009
ACG 2015 Nashville Regional Postgraduate Course
Copyright 2015 American College of Gastroenterology
17
Vivek Kaul, MD, FACG
NOACs
No definitive guidelines yet
However, the fast onset and fast offset make
cessation and resumption easier
Usually 24 hours is enough time to hold,
unless renal insufficiency or high risk
procedure,
better.
procedure in which 48 hours may be better
Check with the prescriber
NOAC: Risk Mitigation Strategies
Ensure NOAC indicated
Refer to table
Modifiable risk factors
Etoh
Nsaids
Antiplatelet agents
H Pylori
PPI cover
Colon and EGD screen
Renal function adjustment
ACG 2015 Nashville Regional Postgraduate Course
Copyright 2015 American College of Gastroenterology
18
Vivek Kaul, MD, FACG
When to restart NOACs after a planned surgical
intervention
Procedures with immediate and complete
Resume 68 h after surgery
hemostasis:
Atraumatic spinal/epidural anesthesia
Clean lumbar puncture
Procedures associated with immobilization:
Initiate reduced venous or intermediate dose of
LMWH 68 h after surgery if hemostasis achieved.
Procedures with post-operative risk of
Restart NOACs 4872h after surgery upon
bleeding:
complete hemostasis
Thromboprophylaxis (e.g. with LMWH) can be
initiated 6-8 h after surgery
www.escardio.org/EHRA
EGD Procedures
Procedure
Risk Bleeding
Stop Aspirin?
Stop Clopidogrel or
Prasugrel?
EGD biopsy
Low
No
No
EGD with stricture
dilation
Low
No
No
EGD with APC
Low
No
Yes
EGD with stent
placement
Low
No
Yes
EGD with variceal
band ligation
High
No
Yes
EGD with PEG
placement
High
No
? (probably)
EGD with EMR/ESD
High
Yes
Boustiere, ESGE Guidelines: Endoscopy and antiplatelet agents. Endoscopy 2011
ACG 2015 Nashville Regional Postgraduate Course
Copyright 2015 American College of Gastroenterology
19
Vivek Kaul, MD, FACG
Colonoscopy Procedures
Procedure
Risk of Bleeding
Stop aspirin
Stop clopidogrel or
prasugrel?
Colonoscopy
biopsy
Low
No
No
Colonoscopy with
polypectomy <1 cm
Low
No
No
Colonoscopy with
polypectomy >1 cm
High
No
Yes
Colonoscopy with
EMR/ESD
High
Yes (?)
Yes
Boustiere // ESGE Guidelines: Endoscopy 2011
ERCP Procedures
Procedure
Risk Bleeding
Stop Aspirin?
Stop Clopidogrel or
Prasugrel?
ERCP Diagnostic
Low
No
No
ERCP with Stent
Placement
Low
No
No
ERCP with
sphincterotomy
High
No
Yes
Yes (?)
Yes
ERCP with
High
sphincterotomy and
large
balloon
l
b
ll
papillary dilation
Boustiere, ESGE Guidelines: Endoscopy and antiplatelet agents. Endoscopy 2011
ACG 2015 Nashville Regional Postgraduate Course
Copyright 2015 American College of Gastroenterology
20
Vivek Kaul, MD, FACG
EUS Procedures
Procedure
Risk Bleeding
Stop Aspirin?
Stop Clopidogrel or
Prasugrel?
EUS Diagnostic
Low
No
No
EUS with FNA Solid
Mass
Low
No
Yes (?)
EUS FNA Cysts
High
Yes
Yes
EUS FNA
Therapeutic
High
Yes
Yes
Boustiere // ESGE Guidelines: Endoscopy 2011
Management of antithrombotic agents in the ELECTIVE endoscopic setting
Management of antithrombotic agents for endoscopic procedures. ASGE Standards of Practice Committee. 2009
ACG 2015 Nashville Regional Postgraduate Course
Copyright 2015 American College of Gastroenterology
21
Vivek Kaul, MD, FACG
M
A i Thrombotic
Th
b i
Management
off Anti
Agents in the Patient with GI Bleeding
Stopping or Reversing Antithrombotic
Agents in the acutely bleeding patient
Warfarin
Consider holding warfarin
Consider vitamin K, FFP, Factor VIIa
AHA/ACC recommendations
Fresh frozen plasma (FFP) >>>>> high dose Vitamin K
Avoid high-dose Vitamin K (10 mg) in mechanical valves as may
cause hypercoag state
Low dose Vitamin K (1-2 mg) may be fine
Antiplatelet agents
Consider stopping drug
Consider platelet transfusion
ACG 2015 Nashville Regional Postgraduate Course
Copyright 2015 American College of Gastroenterology
22
Vivek Kaul, MD, FACG
Restarting Antithrombotic Agents s/p
Endoscopic Hemostasis
Resumption of aspirin + PPI has lower rate of
recurrent peptic ulcer bleeding than switching
to clopidogrel (Chan, NEJM 2005)
Continuation of low dose aspirin after
endoscopic
hemostasis
d
i h
t i results
lt iin llower allll
cause mortality (12.9% vs 1.3%) and higher
rebleed rate (10.3% vs 5.4%) (Sung JJ, Ann Int Med
2010)
Risk of Interruption of Warfarin in
GI Bleeding
Compared with holding warfarin for 30 days, restarting warfarin
after 7 days was not associated with increased risk of GIB and was
associated with decreased risk of mortality and thromboembolism
Qureshi et al, Am J Cardiol 2013.
ACG 2015 Nashville Regional Postgraduate Course
Copyright 2015 American College of Gastroenterology
23
Vivek Kaul, MD, FACG
Asia-Pacific Working Group Consensus on
Non-Variceal Bleeding (Sung JJ,Gut 2011)
Among aspirin users with high cardiothrombotic
risk & PUD bleeding, resume aspirin ASAP
Because risk of rebleeding is greatest in 1st 72 hours,
consider restart aspirin ~ 3 days after hemostasis
Uncertain about clopidogrel, but perhaps restart in 35 days
d
If dual therapy: No data; depends on type of stent and
when placed
Management of antithrombotic agents in the URGENT endoscopic setting
Based on Rebleeding Risk AND Thromboembolic Risk
Management of antithrombotic agents for endoscopic procedures.
ASGE Standards of Practice Committee. 2009
ACG 2015 Nashville Regional Postgraduate Course
Copyright 2015 American College of Gastroenterology
24
Vivek Kaul, MD, FACG
Desai GIE
2013
What About Endoscopic Therapy?
After all, we are endoscopists
We should be able to fix everything!!!
ACG 2015 Nashville Regional Postgraduate Course
Copyright 2015 American College of Gastroenterology
25
Vivek Kaul, MD, FACG
Endoloops
Endoclips
ACG 2015 Nashville Regional Postgraduate Course
Copyright 2015 American College of Gastroenterology
26
Vivek Kaul, MD, FACG
What is the Efficacy of Endoscopic
Therapy in This Setting?
Retrospective studies suggest endoscopic
therapy seems safe and effective (even with INR
>4)
Mechanical hemostasis (i.e. clips) preferred
Especially if will resume antithrombotic meds
Colonoscopy with polypectomy was safe in a
large cohort of consecutive patients on
Clopidogrel (Singh et al GIE 2009)
Endoscopic Techniques Can Decrease
Bleeding After Elective Polypectomy
Boustiere, ESGE Guidelines: Endoscopy and antiplatelet agents. Endoscopy 2011
ACG 2015 Nashville Regional Postgraduate Course
Copyright 2015 American College of Gastroenterology
27
Vivek Kaul, MD, FACG
NOACs: FIRST REVERSAL AGENT JUST
APPROVED BY FDA !!
.In
In trials,
trials a five
five-minute
minute infusion of
Idarucizumab was able to reverse
the blood thinning effects of
Dabigatran in young adults, elderly
patients and in those with mild
renal/hepatic dysfunction
Glund S, Lancet 2015
Drugs, Dec 2015
Which risk we are willing to take?
Continue
Stop
We usually can stop GI bleeding while CVA/ACS are usually
irreversible and devastating!!!
ACG 2015 Nashville Regional Postgraduate Course
Copyright 2015 American College of Gastroenterology
28
Vivek Kaul, MD, FACG
Lets simplify a bit
and review
Warfarin
Low risk endoscopy + low cardiovascular/ low
b
l risk:
i k may nott h
t
cerebrovascular
have tto stop
If High risk procedure or high CV/CNS risk:
HIGH RISK
Strongly consider heparin bridge
ACG 2015 Nashville Regional Postgraduate Course
Copyright 2015 American College of Gastroenterology
29
Vivek Kaul, MD, FACG
Thienopyridines
(Clopidogrel)
Always check with cardiologist/prescriber
TYPE of stent
AGE of stent
Stroke history
Usually
5-7
U ll if stopped
t
d iis stopped
t
d ffor 5
7 days
d
In nearly every instance, continue or
substitute aspirin
GI Bleeding Management: NOAC
Anemia/Guaiac + stools
Semi elective evaluation reasonable (~1
2wks)
Semi-elective
(~1-2wks)
Colonoscopy +/- EGD
Small bowel evaluation if needed
Typically would continue NOAC
Monitor
M it Hb/Hct
Hb/H t
Monitor for overt GI bleeding
ACG 2015 Nashville Regional Postgraduate Course
Copyright 2015 American College of Gastroenterology
30
Vivek Kaul, MD, FACG
GI Bleeding Management: NOAC
Overt/Major GI Bleeding
d as inpatient in h
Best managed
hospitall
Standard resuscitation protocols
NOAC should be held
Antiplatelet Rx: review need per case
p
y consultation
Multidisciplinary
Urgent Endoscopic evaluation
Angiographic embolization when needed
Reversal Agent for severe/life threatening
bleeding
Uncontrolled NOAC Associated GI
Bleeding
Topical thrombin & fibrin sealant
Topical hemospray powder (n/a in USA)
Systemic Tranexamic acid
Prothrombin complex concentrate
Recombinant activated factor VII
Hemodialysis & Hemoperfusion (Dabigatran)
Reversal Agent for severe/life threatening
bleeding
Surgery
ACG 2015 Nashville Regional Postgraduate Course
Copyright 2015 American College of Gastroenterology
31
Vivek Kaul, MD, FACG
Peri-endoscopic Management: NOAC
Low risk procedure: may continue NOAC
High risk procedure: interrupt NOAC
Consult with cardiologist
Knowledge of renal function
Develop
D l plan
l ffor resumption
ti
Discuss and document risks/benefits (office visit)
ANTIDOTES
Aspirin: Platelet transfusion
Warfarin: Vit K, FFP
Heparin: Protamine Sulfate
Clopidogrel: Platelet Transfusion
Dabigatran: Idarucizumab
Other NOACs: none yet
ACG 2015 Nashville Regional Postgraduate Course
Copyright 2015 American College of Gastroenterology
32
Vivek Kaul, MD, FACG
Especially Difficult Scenarios!!
Jehovahs Witness patient
The recalcitrant Cardiologist
The Cardiologist cannot be found!
LVAD patients
The patient with acute MI
Summary
Low risk for bleeding from endoscopy AND High risk for
cardiovascular/CNS event favors continuing
antithrombotic agent.
High risk for bleeding from endoscopy AND Low risk for
Cardiovascular/CNS event favors holding
antithrombotic agent.
Variables: Duration of action of agent, availability of
reversing
i agents,
t ability
bilit tto more easily
il control
t l
bleeding endoscopically, local expertise/resources all
weigh in considerably
Dont under-estimate efficacy of endoscopic therapy!
ACG 2015 Nashville Regional Postgraduate Course
Copyright 2015 American College of Gastroenterology
33
Vivek Kaul, MD, FACG
All Bleeding Eventually Stops.!!!!!!
Thank You!
ACG 2015 Nashville Regional Postgraduate Course
Copyright 2015 American College of Gastroenterology
34
Anda mungkin juga menyukai
- JOurnal - RaphDokumen57 halamanJOurnal - RaphJayakrishnu tjBelum ada peringkat
- Clinical Review: Target-Specific Oral Anticoagulants in The Emergency DepartmentDokumen12 halamanClinical Review: Target-Specific Oral Anticoagulants in The Emergency Departmentrosariris94Belum ada peringkat
- 1000 - Johnson Venous ThrombDokumen33 halaman1000 - Johnson Venous ThrombAlejandro Kanito Alvarez SBelum ada peringkat
- Tromboprofilaxia - Adherence To Apixaban For Extended Thromboprophylaxis After Major Abdominal or Pelvic Surgery For cancer-JSO2022Dokumen8 halamanTromboprofilaxia - Adherence To Apixaban For Extended Thromboprophylaxis After Major Abdominal or Pelvic Surgery For cancer-JSO2022porto_victorBelum ada peringkat
- Routine Preanaesthetic Testing: General Topics Tutorial456Dokumen6 halamanRoutine Preanaesthetic Testing: General Topics Tutorial456Ahmed SaeedBelum ada peringkat
- Venous Thromboembolism in Urologic Surgery: Prophylaxis, Diagnosis and TreatmentDokumen25 halamanVenous Thromboembolism in Urologic Surgery: Prophylaxis, Diagnosis and TreatmentapheatBelum ada peringkat
- Periprocedural Management With Antithrombotic Therapy Adult Inpatient Ambulatory Guideline 20201029Dokumen14 halamanPeriprocedural Management With Antithrombotic Therapy Adult Inpatient Ambulatory Guideline 20201029Joanne HoBelum ada peringkat
- Actualizacion Sobre El Uso de Los Nuevos Anticoagulantes OralesDokumen11 halamanActualizacion Sobre El Uso de Los Nuevos Anticoagulantes Oralesjdelta28Belum ada peringkat
- Cardiology: 27 Maret 2021Dokumen52 halamanCardiology: 27 Maret 2021Dian ParamitaBelum ada peringkat
- CCC 2014 Afvb en For WebDokumen180 halamanCCC 2014 Afvb en For WebAhmed Adel RagabBelum ada peringkat
- Periprocedural Anticoagulation v2Dokumen27 halamanPeriprocedural Anticoagulation v2Joanne HoBelum ada peringkat
- Upper GIT BleedingDokumen69 halamanUpper GIT BleedingSoleh Ramly100% (1)
- PreOp Evaluation in CKD Patients Up To DateDokumen14 halamanPreOp Evaluation in CKD Patients Up To DateMaría Fernanda RíosBelum ada peringkat
- 2020 ESC Guidelines For The Diagnosis and Management of Atrial FibrillationDokumen22 halaman2020 ESC Guidelines For The Diagnosis and Management of Atrial FibrillationFerry KrisnamurtiBelum ada peringkat
- River TrialDokumen28 halamanRiver TrialToheed AshrafBelum ada peringkat
- UGITherapyTsai Reg Training Day VersionDokumen73 halamanUGITherapyTsai Reg Training Day Versionnhanchaoxin234Belum ada peringkat
- 6.6) Diagnostic and Therapeutic Abdominal Paracentesis - UpToDateDokumen18 halaman6.6) Diagnostic and Therapeutic Abdominal Paracentesis - UpToDatefedericoBelum ada peringkat
- Gastrointestinal Bleeding On Anticoagulant Therapy Comparison of Patients Receiving Vitamin K Antagonists and Non Vitamin K Oral AntagonistsDokumen14 halamanGastrointestinal Bleeding On Anticoagulant Therapy Comparison of Patients Receiving Vitamin K Antagonists and Non Vitamin K Oral AntagonistsAthenaeum Scientific PublishersBelum ada peringkat
- In The Clinicrisk Identification &surgicalcomplicationsamaso Myear4Dokumen40 halamanIn The Clinicrisk Identification &surgicalcomplicationsamaso Myear4danielBelum ada peringkat
- Role of Endoscopy in The Management of Variceal HemorrhageDokumen7 halamanRole of Endoscopy in The Management of Variceal HemorrhageAmelia Fitria DewiBelum ada peringkat
- HAUT HMV Brazil Grand Rounds April 29 2014Dokumen74 halamanHAUT HMV Brazil Grand Rounds April 29 2014carlosrschusterBelum ada peringkat
- Ventilator Associated Pneumonia and GuidelinesDokumen28 halamanVentilator Associated Pneumonia and GuidelineshawinnurdianaBelum ada peringkat
- Antagonist Oral AnticoagulantsDokumen66 halamanAntagonist Oral Anticoagulantsbagheera316Belum ada peringkat
- Warfarin Mechanism of ActionDokumen7 halamanWarfarin Mechanism of ActionIna GrigorasBelum ada peringkat
- Critical Blood Tests During Liver TransplantDokumen33 halamanCritical Blood Tests During Liver TransplantFuad ImamBelum ada peringkat
- Apixaban Eliquis MonographDokumen14 halamanApixaban Eliquis MonographTran Minh NgocBelum ada peringkat
- Perioperative Management of Antithrombotic Therapy: An American College of Chest Physicians Clinical Practice GuidelineDokumen37 halamanPerioperative Management of Antithrombotic Therapy: An American College of Chest Physicians Clinical Practice GuidelineCG MadeleineBelum ada peringkat
- IKD6 - Contrast Associated AKIDokumen44 halamanIKD6 - Contrast Associated AKIRenal Association MauritiusBelum ada peringkat
- American College of Gastroenterology Canadian Association of GastroenterologyDokumen18 halamanAmerican College of Gastroenterology Canadian Association of GastroenterologyGW GeistBelum ada peringkat
- Outcomes of Early Versus Delayed Cholecystectomy in Patients With Mild To Moderate Acute Biliary Pancreatitis: A Randomized Prospective StudyDokumen36 halamanOutcomes of Early Versus Delayed Cholecystectomy in Patients With Mild To Moderate Acute Biliary Pancreatitis: A Randomized Prospective StudyAnonymous Uh2myPxPHBelum ada peringkat
- Pragmatic Use of NOACDokumen38 halamanPragmatic Use of NOACDr. Pradip MateBelum ada peringkat
- Jurnal KadekDokumen6 halamanJurnal KadekNikadek Ayu Dwi LestariBelum ada peringkat
- Low Molecular Weight Heparin: All Wales Medicines Strategy Group (Awmsg) Recommendations and AdviceDokumen33 halamanLow Molecular Weight Heparin: All Wales Medicines Strategy Group (Awmsg) Recommendations and AdviceAtikah Putri AtmojoBelum ada peringkat
- Arfarin: Arget UdienceDokumen4 halamanArfarin: Arget UdienceMano cempakaBelum ada peringkat
- Ectopic PregnancyDokumen46 halamanEctopic PregnancyNoegi AkasBelum ada peringkat
- GI Bleeding EmergenciesDokumen35 halamanGI Bleeding EmergenciesJabraan JBelum ada peringkat
- CCJM Warfarin PDFDokumen12 halamanCCJM Warfarin PDFmyscribeBelum ada peringkat
- Tumor Marker Test A. Prostate Specific Antigen (Psa) TestDokumen25 halamanTumor Marker Test A. Prostate Specific Antigen (Psa) TestkdfhjfhfBelum ada peringkat
- Aki GuidlineDokumen5 halamanAki GuidlineFii Fathayati PutriBelum ada peringkat
- Periprocedural Anticoagulation Guidelines - UKDokumen14 halamanPeriprocedural Anticoagulation Guidelines - UKjoshBelum ada peringkat
- Pre-Op Assessment: Dr. Ayesha Ehsan House Surgeon S-IIDokumen25 halamanPre-Op Assessment: Dr. Ayesha Ehsan House Surgeon S-IIFatima MBelum ada peringkat
- Johns Hopkins HospitalDokumen63 halamanJohns Hopkins Hospitalapi-64584013Belum ada peringkat
- Seminar On TransplantationDokumen53 halamanSeminar On Transplantationamox woldieBelum ada peringkat
- Oral Anticoagulation in Patients With Chronic Liver DiseaseDokumen23 halamanOral Anticoagulation in Patients With Chronic Liver DiseaseSophia PapathanasiouBelum ada peringkat
- GynaecologicalCancerChemoProtocols PDFDokumen7 halamanGynaecologicalCancerChemoProtocols PDFRyan IlhamBelum ada peringkat
- Antenatal CounsellingDokumen56 halamanAntenatal CounsellingDr. Prashant JainBelum ada peringkat
- Case Based Urology Learning Program: Resident's Corner: UROLOGYDokumen26 halamanCase Based Urology Learning Program: Resident's Corner: UROLOGYAbdullah BangwarBelum ada peringkat
- Perioperative Management of Patients Receiving Anticoagulants. UpToDate. 2017.Dokumen40 halamanPerioperative Management of Patients Receiving Anticoagulants. UpToDate. 2017.radiomedicBelum ada peringkat
- Penampilan Minggu 3Dokumen130 halamanPenampilan Minggu 3riski anugrahBelum ada peringkat
- Preoperative AssessmentDokumen26 halamanPreoperative Assessmentkaukab azimBelum ada peringkat
- Vte in CaDokumen50 halamanVte in CaEmmanuel Kissiedu AntiriBelum ada peringkat
- Rancangan Bentuk Sediaan Farmasi Compatibility ModeDokumen18 halamanRancangan Bentuk Sediaan Farmasi Compatibility ModeNully Andaretha SugiantoBelum ada peringkat
- Sepsis Update 2017 - 2Dokumen49 halamanSepsis Update 2017 - 2Ahmad Fathul Adzmi100% (1)
- HepatoblastomaDokumen38 halamanHepatoblastomaSaroj PandaBelum ada peringkat
- Contrast Induced NephropathyDokumen25 halamanContrast Induced NephropathyXin Yee TanBelum ada peringkat
- Common Tests For Liver Disease: Now Scheduling COVID-19 Vaccine Appointments For Ages 12+Dokumen2 halamanCommon Tests For Liver Disease: Now Scheduling COVID-19 Vaccine Appointments For Ages 12+Marie Bernadette DigoBelum ada peringkat
- Bahan CKD Jurnal ProposalDokumen6 halamanBahan CKD Jurnal ProposalArjunaPamungkasBelum ada peringkat
- Biliary AtresiaDokumen9 halamanBiliary AtresiaPrabhakar KumarBelum ada peringkat
- Kidney Biomarkers: Clinical Aspects and Laboratory DeterminationDari EverandKidney Biomarkers: Clinical Aspects and Laboratory DeterminationSeema S. AhujaBelum ada peringkat
- Dysphagia: Diagnosis and Treatment of Esophageal Motility DisordersDari EverandDysphagia: Diagnosis and Treatment of Esophageal Motility DisordersMarco G. PattiBelum ada peringkat
- 07 Antithrombotic Agents inDokumen5 halaman07 Antithrombotic Agents inRaja AndrianyBelum ada peringkat
- Disorders of Potassium Balance: Zhao Chenghai PathophysiologyDokumen24 halamanDisorders of Potassium Balance: Zhao Chenghai PathophysiologyBayu SetiaBelum ada peringkat
- 5 Potassium MetabolismDokumen32 halaman5 Potassium MetabolismRaja AndrianyBelum ada peringkat
- The Teratogenic of Imatinib Mesylate On Rat FetusesDokumen10 halamanThe Teratogenic of Imatinib Mesylate On Rat FetusesRaja AndrianyBelum ada peringkat
- FotoDokumen10 halamanFotoRaja AndrianyBelum ada peringkat
- Makroskopis UrinDokumen1 halamanMakroskopis UrinRaja AndrianyBelum ada peringkat
- Tipos de SuturasDokumen5 halamanTipos de SuturasLeandro PeraltaBelum ada peringkat
- CHN Part 2 - Vital StatisticsDokumen2 halamanCHN Part 2 - Vital StatisticsMichelle Gambol100% (1)
- NeedlestickDokumen14 halamanNeedlestickluis_chubeeBelum ada peringkat
- Copd MidtermDokumen5 halamanCopd MidtermAna Rose Dela CruzBelum ada peringkat
- Endocrine DisordersDokumen106 halamanEndocrine DisordersMansur MuhammadBelum ada peringkat
- Francisco GS Conference March 2022Dokumen69 halamanFrancisco GS Conference March 2022SamuelBelum ada peringkat
- Sesion 2 Articulo Caso Clinico 1 Urticaria PDFDokumen16 halamanSesion 2 Articulo Caso Clinico 1 Urticaria PDFQuispe Canares MariangelesBelum ada peringkat
- Thrombolytic Therapy in Acute Myocardial InfarctionDokumen7 halamanThrombolytic Therapy in Acute Myocardial InfarctionRumela Ganguly ChakrabortyBelum ada peringkat
- Absite January2014 ReviewDokumen1.226 halamanAbsite January2014 ReviewAnnTran100% (12)
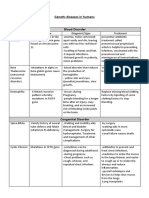
- Genetic DiseasesDokumen3 halamanGenetic DiseasesLhoshinyBelum ada peringkat
- DC Kit2 ObadiaDokumen2 halamanDC Kit2 ObadiaErnesto KangBelum ada peringkat
- Evaluation of The Painful EyeDokumen9 halamanEvaluation of The Painful EyeMuthia Farah AshmaBelum ada peringkat
- Immobilization and Death of Bacteria by Flora Seal Microbial SealantDokumen6 halamanImmobilization and Death of Bacteria by Flora Seal Microbial SealantinventionjournalsBelum ada peringkat
- Casilan, Ynalie Drug Study (Morphine)Dokumen5 halamanCasilan, Ynalie Drug Study (Morphine)Ynalie CasilanBelum ada peringkat
- Biodiversity of Micro-OrganismsDokumen32 halamanBiodiversity of Micro-Organismsapi-20234922250% (2)
- Self-Care Model Application To Improve Self-Care Agency, Self-Care Activities, and Quality of Life in People With Systemic Lupus ErythematosusDokumen8 halamanSelf-Care Model Application To Improve Self-Care Agency, Self-Care Activities, and Quality of Life in People With Systemic Lupus ErythematosusFerry EfendiBelum ada peringkat
- Cytochemistry PrimerDokumen2 halamanCytochemistry PrimerMunish Dogra100% (1)
- PolioDokumen5 halamanPolioapi-306493512Belum ada peringkat
- Emergency DrugsDokumen10 halamanEmergency DrugsnieacatleyaBelum ada peringkat
- Community-Acquired Pneumonia CaseDokumen6 halamanCommunity-Acquired Pneumonia Caseapi-648891519Belum ada peringkat
- Healing Parvo PuppiesDokumen11 halamanHealing Parvo PuppiesAshen WillowsBelum ada peringkat
- The Well-Being of The EMT: Emergency Medical Technician - BasicDokumen30 halamanThe Well-Being of The EMT: Emergency Medical Technician - Basicalsyahrin putraBelum ada peringkat
- M1 All ProgramsDokumen26 halamanM1 All ProgramsDaisy Joy MBardz100% (1)
- Case Presentation On Wilms TumorDokumen25 halamanCase Presentation On Wilms TumorDeepika100% (1)
- Dialog Percakapan Bidan Tugas Bahs Inggris DedeDokumen5 halamanDialog Percakapan Bidan Tugas Bahs Inggris DedeSardianto TurnipBelum ada peringkat
- Franco, Danica A. (Cardio)Dokumen5 halamanFranco, Danica A. (Cardio)Danica FrancoBelum ada peringkat
- NP3 Recall - Pre-IntensiveDokumen13 halamanNP3 Recall - Pre-IntensiveTristan CamilonBelum ada peringkat
- Part 1 Executive Summary PDFDokumen21 halamanPart 1 Executive Summary PDFNurul RafahBelum ada peringkat
- 701 1941 1 SMDokumen6 halaman701 1941 1 SMANNISA DAMAYANTIBelum ada peringkat
- Beyond Wedge: Clinical Physiology and The Swan-Ganz CatheterDokumen12 halamanBeyond Wedge: Clinical Physiology and The Swan-Ganz Catheterkromatin9462Belum ada peringkat