Rupture of Membranes Guideline For The Management of Preterm Prelabour
Diunggah oleh
saryindrianyJudul Asli
Hak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Rupture of Membranes Guideline For The Management of Preterm Prelabour
Diunggah oleh
saryindrianyHak Cipta:
Format Tersedia
PRETERM PRELABOUR RUPTURE OF MEMBRANES (PPROM)
CLINICAL GUIDELINE FOR DIAGNOSIS AND MANAGEMENT
1. Aim/Purpose of this Guideline
1.1. This guideline gives guidance to obstetricians and midwives on the diagnosis and
management of preterm prelabour rupture of membranes (PPROM).
2. The Guidance
2.1. Preterm prelabour rupture of the membranes (PPROM) is the rupture of the
membranes prior to labour, occurring before 37+0 weeks gestation.
If fetal infection is present spontaneous delivery usually occurs within days of PPROM.
In the absence of infection the pregnancy may continue for weeks or months.1
Definitive diagnosis of intrauterine infection after preterm rupture of membranes is only
possible by culture of amniotic fluid or fetal blood because the majority of cases are
subclinical.
Normal maternal observations (temp, pulse, leucocyte count, C - reactive protein
(CRP) do not exclude intrauterine infection and vaginal swab cultures yield a high false
positive rate.
In addition, as intrauterine infection does not affect placental perfusion and fetal
oxygenation, non-invasive fetal monitoring cardiotocographs (CTG) and biophysical
profiles) may be normal in the presence of infection. 2
2.2. Diagnosis and initial inpatient management
Diagnosis is best made on history of a gush of fluid per vaginum (PV) and clinical
findings. A liquor pool in the upper vagina is the most reliable sign.
All patients should have a sterile speculum examination after 30 minutes bed
rest. The cervix must be visualised and a high vaginal swab (HVS) obtained.
Maternal coughing or straining may assist identification of liquor from the cervix.
Digital examination should be avoided.
Ultrasound may be useful where fetal presentation, size or well-being is in doubt.
Normal amniotic fluid volume on scan, whilst making the diagnosis less likely, does
not preclude PPROM. Conversely, reduced amniotic fluid on ultrasound may have
other causes.
A routine full blood count (FBC), CRP and a full set of maternal observations should
be performed and recorded on a MEOWS chart.
2.3. Prophylactic antibiotics
Administer prophylactic Erythromycin 250mg orally four times daily for 10 days
from diagnosis. This has been shown to be of potential modest benefit for the
neonate in PPROM3. Erythromycin should not be prescribed based upon a
possible diagnosis from history alone.
Co-amoxiclav should not be used because of the association with necrotising
enterocolitis.
Appropriate antibiotics should be given in suspected intrauterine infection,
either intrapartum or to cover caesarean section.
2.4. Uncertain Diagnosis
Where diagnosis is uncertain e.g. a strong history but negative speculum and delay in
confirmation of PPROM is deemed to be clinically important after consultant input,
Actiprom may be used.
2.5. Corticosteroids
Maternal corticosteroids given prophylactically to cases of preterm labour with or
without intact membranes at gestational ages 24-34+6 weeks have demonstrated a
50% reduction in neonatal death, respiratory distress and intraventricular
haemorrhage. In cases of PPROM, steroids do not increase the risk of neonatal
sepsis or chorioamnionitis but do increase the risk of endometritis.3
Two doses of Betamethasone 12mg are to be given, 24 hours apart.
Tocolysis in women with PPROM is not recommended because this treatment does
not significantly improve perinatal outcome. However, it may be used to allow inutero
transfer.4
The tocolytic of first choice is Atosiban. Prophylactic tocolysis to women with PPROM
who are not contracting should not be given.
The risk of infection is highest in the first few days after diagnosis and the length of
inpatient management should be individualised, taking into account the gestation,
other obstetric risk factors, where the woman lives and her social circumstances.
Women should be advised admission for at least 48 hours in view of the increased risk
of infection during this time.
2.6. Outpatient Management
Expectant management at home is safe after initial observation in hospital.5
The woman should be advised of the following:
Check her temperature 4 to 8 hourly
Avoid intercourse
If expectant management is appropriate, the woman should attend the Day
Assessment Unit (DAU) weekly for clinical evaluation and CTG. It is not necessary to
carry out weekly maternal FBC or C-reactive protein because the sensitivity of these
tests in the detection of intrauterine infection is low. Any additional assessments, in
the community or DAU, will be at the discretion of the obstetric team. If liquor drainage
stops, the accuracy of the diagnosis should be re-evaluated.
The woman should be instructed to contact DAU or Delivery Suite out of hours if:
Contractions establish
Preterm Prerupture PPROM
Page 2 of 10
There is vaginal bleeding
The liquor is green or offensive
She feels unwell or has a raised temperature above 37.4oC
Fetal movements are reduced
2.7. Timing of delivery
Many studies have demonstrated benefits in conservative management <34 weeks
gestation but management from 34-37 weeks is contentious.
In the absence of spontaneous preterm labour or complications such as infection that
require intervention <34 weeks, induction of labour > 34 weeks should be discussed.
RCOG Guidance suggests that delivery should be considered at 34 weeks in the
knowledge that there is little evidence that intentional delivery after 34 weeks
adversely affects neonatal outcome.
For expectant management after 34 weeks women should be counselled about the
increased risk of chorioamnionitis and its consequences versus the decreased risk of
serious respiratory problems in the neonate, admission for neonatal intensive care and
caesarean section.
Care should be individualised after careful discussion with the woman.
Counselling should bear in mind that it is self-evident that the risk of infection will be
higher with expectant management but the quoted risk in studies is small with no
longer term neonatal sequelae.
For induction of labour at 34 weeks, the issues of impaired bonding/breastfeeding,
prolonged hospitalisation and neonatal unit workload are not considered in the RCOG
guidance.
If expectant management is selected by the woman, there is no evidence to guide
practice after >37 weeks. Induction of labour will usually be offered at 37 weeks
because the maternal and neonatal morbidity associated with term induction for this
indication is low. However, a Consultant may, in discussion with the woman, opt for
on-going expectant management.
Irrespective of the gestational age, care must be made to ensure that the diagnosis of
PPROM remains accurate before starting induction of labour in order to minimise the
risk of failed induction.
2.8. Spontaneous preterm labour
If labour establishes preterm then Group B streptococcal (GBS) antibiotic prophylaxis
should be offered as per the preterm labour guideline7, 8.
2.9. PPROM and asymptomatic Group B streptococcus9
There is no good evidence base to guide management of PPROM in the presence of
GBS. Women will receive Erythromycin (section 2.3. Prophylactic antibiotics)
but there is no evidence that IV antibiotics are indicated until labour is established.
There is no evidence that the timing of delivery should be influenced by the
asymptomatic carriage of GBS.
Preterm Prerupture PPROM
Page 3 of 10
3. Monitoring compliance and effectiveness
Element to be
monitored
Counselling: active management versus expectant
management
Did the woman receive GBS antibiotic prophylaxis if required?
Lead
Maternity Risk Manager.
Tool
Compliance Monitoring Tool.
Frequency
This audit will be added to the rolling audit programme and will take
place every three years.
Reporting
arrangements
Perinatal Audit Forum
Maternity Risk Management Forum
Acting on
recommendations
and Lead(s)
Change in
practice and
lessons to be
shared
Maternity Risk Manager
Any lessons learnt will be fed back through the Maternity Risk
Management Forum and shared via the monthly Risk Management
Newsletter
4. Equality and Diversity
4.1.
This document complies with the Royal Cornwall Hospitals NHS Trust
service Equality and Diversity statement which can be found in the 'Equality,
Diversity & Human Rights Policy' or the Equality and Diversity website.
4.2.
Equality Impact Assessment
The Initial Equality Impact Assessment Screening Form is at Appendix 2.
Preterm Prerupture PPROM
Page 4 of 10
Appendix 1. Governance Information
Document Title
PRETERN PRELABOUR RUPTURE OF
MEMEBRANES (PPROM) CLINICAL
GUIDELINE FOR DIAGNOSIS AND
MANAGEMENT
Date Issued/Approved:
9th January 2014
Date Valid From:
9th January 2014
Date Valid To:
9th January 2017
Directorate / Department responsible
(author/owner):
Dr Rob Holmes
Consultant Obstetrician
Obs and Gynae Directorate
Contact details:
01872 252727
This guideline gives guidance to
obstetricians and midwives on the diagnosis
and management of preterm prelabour
rupture of membranes (PPROM).
Brief summary of contents
Rupture, membranes, PPROM, PROM,
SROM, ruptured, membranes, prolonged,
speculum, Erythromycin, steroids,
premature, Betamethasone
RCHT
PCH
CFT
KCCG
Suggested Keywords:
Target Audience
Executive Director responsible for
Policy:
Medical Director
Date revised:
9th January 2014
This document replaces (exact title of
previous version):
Guideline for the management of pre term pre
labour rupture of membranes
Approval route (names of
committees)/consultation:
Maternity Guideline Group
Obs & Gynae Directorate
Divisional Board
Divisional Manager confirming
approval processes
Head of Midwifery
Name and Post Title of additional
signatories
Not Required
Signature of Executive Director giving
approval
Publication Location (refer to Policy
on Policies Approvals and
Ratification):
Preterm Prerupture PPROM
Internet & Intranet
Page 5 of 10
Intranet Only
Document Library Folder/Sub Folder
Clinical/Midwifery and Obstetrics
Links to key external standards
None
1. Carroll SG, Ville Y, Greenough A,
Gamsu H, Patel B, Philpott-Howard J
and
Nicolaides
KH.
Preterm
Prelabour amniorrhexis: Intrauterine
infection and interval between
membrane rupture and delivery.
Arch Dis Child 1995;72:F43-46
2. Carroll SG, Papaioannou S, and
Nicolaides KH. Assessment of fetal
activity and amniotic fluid volume in
pregnancies complicated by preterm
prelabour amniorrhexis. Am J Obstet
Gynecol 1995;172:1472-1435
3. RCOG Clinical guideline No. 44
2010. Preterm prelabour rupture of
membranes
Related Documents:
4. Kenyon SL, Taylor DJ, TarnowMordi W. ORACLE Group. Broadspectrum antibiotics for preterm,
prelabour rupture of the fetal
membranes:
the
ORACLE
I
randomised
trial.
Lancet
2001;357(9261):979-88
5. RCOG Clinical guideline No. 7 2004.
Antenatal corticosteroids to prevent
respiratory distress syndrome
6. RCOG Clinical guideline No 1 (B)
2002. Tocolytic drugs for women in
preterm labour
7. Carlan SJ et al. Preterm premature
rupture of the membranes: A
randomised study of home versus
hospital
management.
Obstet
Gynecol 1991;81:61-64
8. RCHT The Management of
Threatened and Established Preterm
Labour. Nov 2010
9. RCOG Clinical Guideline No.36:
Prevention of early onset neonatal
group B streptococcal disease
Preterm Prerupture PPROM
Page 6 of 10
Training Need Identified?
No
Version Control Table
Date
Version
No
Summary of Changes
Changes Made by
(Name and Job Title)
Nov 2008 1.0
Initial issue
Rob Holmes
Obstetric Consultant
Nov 2010
1.1
Updated
Rob Holmes
Obstetric Consultant
9th
January
2014
1.2
Minor changes and updated to new best
evidence
Rob Holmes
Obstetric Consultant
All or part of this document can be released under the Freedom of Information
Act 2000
This document is to be retained for 10 years from the date of expiry.
This document is only valid on the day of printing
Controlled Document
This document has been created following the Royal Cornwall Hospitals NHS Trust
Policy on Document Production. It should not be altered in any way without the
express permission of the author or their Line Manager.
Preterm Prerupture PPROM
Page 7 of 10
Appendix 2. Initial Equality Impact Assessment Form
Name of Name of the strategy / policy /proposal / service function to be assessed (hereafter
referred to as policy) (Provide brief description): Preterm Prelabour Rupture Of Membranes
(PPROM) Clinical Guideline For Diagnosis And Management
Directorate and service area:
Is this a new or existing Policy?
Obs & Gynae Directorate
Existing
Name of individual completing
Telephone:
assessment: Elizabeth Anderson
01872 252879
1. Policy Aim*
To give guidance to obstetricians and midwives on the diagnosis and
Who is the strategy /
management of preterm, prelabour rupture of membranes (PPROM).
policy / proposal /
service function
aimed at?
2. Policy Objectives*
To ensure women receive an accurate diagnosis and appropriate
management of preterm prelabour rupture of membranes
3. Policy intended
Outcomes*
To ensure women receive a diagnosis and correct management for
preterm prelabour rupture of membranes according to best evidence.
4. *How will you
measure the
outcome?
5. Who is intended to
benefit from the
policy?
6a) Is consultation
required with the
workforce, equality
groups, local interest
groups etc. around
this policy?
Compliance Monitoring Tool.
b) If yes, have these
*groups been
consulted?
N/A
C). Please list any
groups who have
been consulted about
this procedure.
N/A
All pregnant women.
No
7. The Impact
Please complete the following table.
Are there concerns that the policy could have differential impact on:
Equality Strands:
Age
Preterm Prerupture PPROM
Yes
No
Rationale for Assessment / Existing Evidence
All pregnant women
Page 8 of 10
Sex (male, female,
trans-gender / gender
reassignment)
All pregnant women
Race / Ethnic
communities /groups
All pregnant women
Disability learning
disability, physical
disability, sensory
impairment and
mental health
problems
Religion /
other beliefs
All pregnant women
All pregnant women
Marriage and civil
partnership
All pregnant women
Pregnancy and
X
All pregnant women
maternity
Sexual Orientation,
X
All pregnant women
Bisexual, Gay,
heterosexual, Lesbian
You will need to continue to a full Equality Impact Assessment if the following have been
highlighted:
You have ticked Yes in any column above and
No consultation or evidence of there being consultation- this excludes any policies
which have been identified as not requiring consultation. or
Major service redesign or development
8. Please indicate if a full equality analysis is recommended.
Yes
No
X
9. If you are not recommending a Full Impact assessment please explain why.
N/A
Signature of policy developer / lead manager / director
Rob Holmes
Obstetric Consultant
Names and signatures of
1. Rob Holmes
members carrying out the
2. Elizabeth Anderson
Screening Assessment
Date of completion and submission
9th January 2014
Keep one copy and send a copy to the Human Rights, Equality and Inclusion Lead,
c/o Royal Cornwall Hospitals NHS Trust, Human Resources Department, Knowledge Spa,
Truro, Cornwall, TR1 3HD
A summary of the results will be published on the Trusts web site.
Signed: Elizabeth Anderson
Date : 9th January 2014
Preterm Prerupture PPROM
Page 9 of 10
Appendix 3: Recommended Management of Preterm Prelabour Rupture of
Membranes (PPROM)
No Infection
Infection
Discuss risks and
benefits of induction of
labour versus expectant
management until term
+ 10 DAYS Erythromycin
250mg qds
> 34 weeks
Labour induction
+ broad spectrum intrapartum
antibiotics
Expectant management
+ corticosteroids
+ TEN DAYS
Erythromycin 250mg
qds
+/- tocolysis
24-34 weeks
Careful assessment by an
experienced obstetrician for
consideration of expectant
management
+ antibiotics
+ corticosteroids
Expectant management
or
termination of
pregnancy (TOP)
Preterm Prerupture PPROM
< 24 weeks
Expectant management
+ antibiotics
or
TOP + antibiotics
Page 10 of 10
Anda mungkin juga menyukai
- USMLE Step 3 Lecture Notes 2021-2022: Internal Medicine, Psychiatry, EthicsDari EverandUSMLE Step 3 Lecture Notes 2021-2022: Internal Medicine, Psychiatry, EthicsPenilaian: 5 dari 5 bintang5/5 (9)
- Gravida para WorksheetDokumen1 halamanGravida para WorksheetJulie RobertsonBelum ada peringkat
- Preterm LaborDokumen17 halamanPreterm LaborInd Matthew100% (1)
- Abnormal Midwifery: by Gladys M. BSN, KRCHNDokumen352 halamanAbnormal Midwifery: by Gladys M. BSN, KRCHNMercy KeruboBelum ada peringkat
- Preterm LabourDokumen29 halamanPreterm LabourAnn Michelle Tarrobago100% (1)
- CTGDokumen38 halamanCTGfahmiBelum ada peringkat
- On MCH and Maternal Health in BangladeshDokumen46 halamanOn MCH and Maternal Health in BangladeshTanni ChowdhuryBelum ada peringkat
- 3881825Dokumen30 halaman3881825saryindrianyBelum ada peringkat
- 3 (OB Cases)Dokumen267 halaman3 (OB Cases)Sharyl Plan SarominesBelum ada peringkat
- Prolonged PregnancyDokumen40 halamanProlonged Pregnancyjan caraBelum ada peringkat
- Real Issues for COVID-19 Vaccine Immunization & Pregnancy, Breastfeeding MothersDari EverandReal Issues for COVID-19 Vaccine Immunization & Pregnancy, Breastfeeding MothersBelum ada peringkat
- RCOG Guidelines - Gestational Trophoblastic DiseaseDokumen12 halamanRCOG Guidelines - Gestational Trophoblastic Diseasemob3100% (1)
- Protocol Book For OBGYNDokumen41 halamanProtocol Book For OBGYNShabir BadakhshBelum ada peringkat
- Pregnancy Tests Explained (2Nd Edition): Current Trends of Antenatal TestsDari EverandPregnancy Tests Explained (2Nd Edition): Current Trends of Antenatal TestsBelum ada peringkat
- Case BookDokumen1 halamanCase Bookedrinsne100% (2)
- Operative Vaginal DeliveryDokumen8 halamanOperative Vaginal DeliveryGerben VillanuevaBelum ada peringkat
- Rupture of Membranes Preterm Premature Pprom 220719Dokumen5 halamanRupture of Membranes Preterm Premature Pprom 220719MuathBelum ada peringkat
- Obgyn Ob PRPM Pt1 13Dokumen6 halamanObgyn Ob PRPM Pt1 13SalmonteBelum ada peringkat
- Rcog PpromDokumen7 halamanRcog PpromDevi SyamBelum ada peringkat
- PPROM GuidelinesDokumen2 halamanPPROM GuidelinesLaiza JubyBelum ada peringkat
- Preterm Premature Rupture of Membranes (PPROM) - Assessment and Management GuidelineDokumen6 halamanPreterm Premature Rupture of Membranes (PPROM) - Assessment and Management GuidelineAlexis LambertBelum ada peringkat
- Labor Induction in The Patient With Preterm Premature Rupture of MembranesDokumen6 halamanLabor Induction in The Patient With Preterm Premature Rupture of MembranesYudhi AuliaBelum ada peringkat
- Pi Is 0020729213005055Dokumen4 halamanPi Is 0020729213005055Winna Eka PBelum ada peringkat
- Breech - Management Of: 1. PurposeDokumen15 halamanBreech - Management Of: 1. PurposeMuathBelum ada peringkat
- Preterm labour د.علية شعيبDokumen58 halamanPreterm labour د.علية شعيبMohammad BelbahaithBelum ada peringkat
- Postterm PregnancyDokumen27 halamanPostterm PregnancyChayanika KumarBelum ada peringkat
- Prolonged PregnancyDokumen41 halamanProlonged PregnancyPratiwi Anggun LestariningrumBelum ada peringkat
- 2.5 Preterm Labour: 2 Complications of PregnancyDokumen8 halaman2.5 Preterm Labour: 2 Complications of PregnancykukadiyaBelum ada peringkat
- Premature Rupture of MembranesDokumen9 halamanPremature Rupture of MembranesYessica MelianyBelum ada peringkat
- 3.1 Pprom ShangrilaDokumen31 halaman3.1 Pprom Shangrilaintan.obgBelum ada peringkat
- Premature Rupture of MembraneDokumen5 halamanPremature Rupture of MembraneEspiritu, ChriscelBelum ada peringkat
- BJOG - 2019 - Thomson - Care of Women Presenting With Suspected Preterm Prelabour Rupture of Membranes From 24 0 Weeks ofDokumen15 halamanBJOG - 2019 - Thomson - Care of Women Presenting With Suspected Preterm Prelabour Rupture of Membranes From 24 0 Weeks ofdindacBelum ada peringkat
- Group B Streptococcus: Women's & Children's Services SDMS Id No.: P2010/0528-002 Clinical Guidelines 2006Dokumen8 halamanGroup B Streptococcus: Women's & Children's Services SDMS Id No.: P2010/0528-002 Clinical Guidelines 2006Ywagar YwagarBelum ada peringkat
- 18 PromDokumen8 halaman18 PromRyubusa HayabusaBelum ada peringkat
- Summary KPDDokumen6 halamanSummary KPDOvamelia JulioBelum ada peringkat
- Postterm Pregnancy and IUFDDokumen24 halamanPostterm Pregnancy and IUFDNejib M/AminBelum ada peringkat
- Management Strategies of Neonatal Jaundice During The Coronavirus Disease 2019 OutbreakDokumen4 halamanManagement Strategies of Neonatal Jaundice During The Coronavirus Disease 2019 OutbreakPeter Alejandro Cortes PuentesBelum ada peringkat
- BRN MN 21 01 Guideline 2013 Eng Management Preterm Prelabour Rupture MembranesDokumen3 halamanBRN MN 21 01 Guideline 2013 Eng Management Preterm Prelabour Rupture Membranesd99452727Belum ada peringkat
- Labor&Delivery QuestionsDokumen3 halamanLabor&Delivery Questionsallie-jones-6489Belum ada peringkat
- PSMFM Guidelines On Common Practices Amid Covid 19Dokumen8 halamanPSMFM Guidelines On Common Practices Amid Covid 19Kismet LeeBelum ada peringkat
- Preterm Premature Rupture of Membranes: Diagnosis, Evaluation and Management StrategiesDokumen6 halamanPreterm Premature Rupture of Membranes: Diagnosis, Evaluation and Management StrategiesResi Lystianto PutraBelum ada peringkat
- Current Concepts in The Management of Premature Rupture of The MembranesDokumen21 halamanCurrent Concepts in The Management of Premature Rupture of The MembranesWike UbayBelum ada peringkat
- Management of Multiple PregnancyDokumen14 halamanManagement of Multiple PregnancyxxdrivexxBelum ada peringkat
- PROMDokumen3 halamanPROMCathlen GaranBelum ada peringkat
- PediatriDokumen7 halamanPediatriKijang 2018Belum ada peringkat
- Immunizaton During PregnancyDokumen6 halamanImmunizaton During PregnancyMohamed SulimanBelum ada peringkat
- The Clinical Content of Pre Conceptional Care Reproductive HistoryDokumen3 halamanThe Clinical Content of Pre Conceptional Care Reproductive Historyarkanthos77Belum ada peringkat
- 2013 Chakraborty Outcome of Prelabor Rupture of MembranesDokumen6 halaman2013 Chakraborty Outcome of Prelabor Rupture of MembranesRayhan AlatasBelum ada peringkat
- Premature Rupture of MembranesDokumen8 halamanPremature Rupture of Membraneshadi_abdBelum ada peringkat
- The Management of Gestational Trophoblastic DiseaseDokumen11 halamanThe Management of Gestational Trophoblastic DiseasezkoBelum ada peringkat
- Gui 233 CPG0909Dokumen5 halamanGui 233 CPG0909kyle31100% (1)
- Hiv in PregnancyDokumen8 halamanHiv in Pregnancyjh6svdhxmxBelum ada peringkat
- b2 10 1Dokumen9 halamanb2 10 1Tio Ayahnya AtharBelum ada peringkat
- Preterm Prelabor Rupture of Membranes - Management and Outcome - UpToDateDokumen35 halamanPreterm Prelabor Rupture of Membranes - Management and Outcome - UpToDatemaminyaarBelum ada peringkat
- Full Test BankDokumen1 halamanFull Test Bankjwjimmy20Belum ada peringkat
- POGS-PSMFM Interim Guidelines On Labor and Delivery For COVID EditedDokumen20 halamanPOGS-PSMFM Interim Guidelines On Labor and Delivery For COVID EditedMacky YongcoBelum ada peringkat
- Spontaneous Vaginal Delivery: Toledo, OhioDokumen6 halamanSpontaneous Vaginal Delivery: Toledo, OhioJset SixthousandBelum ada peringkat
- Antenatal Care: Sdms Id: P2010/0314-001 Wacsclinproc1.1/09 TitleDokumen14 halamanAntenatal Care: Sdms Id: P2010/0314-001 Wacsclinproc1.1/09 TitleYwagar YwagarBelum ada peringkat
- Group B Streptococcus: Women's & Children's ServicesDokumen7 halamanGroup B Streptococcus: Women's & Children's ServicesYwagar YwagarBelum ada peringkat
- Pregnancy Complication: Department of Gynaecology and ObstetricsDokumen40 halamanPregnancy Complication: Department of Gynaecology and ObstetricssanjivdasBelum ada peringkat
- Ampicillin-Rcog Guideline On PpromDokumen11 halamanAmpicillin-Rcog Guideline On PpromRida MfBelum ada peringkat
- Aggressive Intervention of Previable Preterm Premature Rupture of MembranesDokumen8 halamanAggressive Intervention of Previable Preterm Premature Rupture of MembranesVanessa Riaño GodoyBelum ada peringkat
- Postdate: When and How To Induce? F. Facchinetti, V. VaccaroDokumen5 halamanPostdate: When and How To Induce? F. Facchinetti, V. VaccaroSyahidatul Kautsar NajibBelum ada peringkat
- Anticoncepcion PostpartoDokumen14 halamanAnticoncepcion PostpartomarialecifuentesbBelum ada peringkat
- Outcome of Neonates Born To Mothers With Premature Rupture of MembranesDokumen5 halamanOutcome of Neonates Born To Mothers With Premature Rupture of MembranesDevi SilalahiBelum ada peringkat
- 29 - Fetal Growth Restriction-IUGR CPG FinalDokumen26 halaman29 - Fetal Growth Restriction-IUGR CPG FinalkukadiyaBelum ada peringkat
- Multiple Pregnancy GuidelineDokumen12 halamanMultiple Pregnancy GuidelineAlia BangeshBelum ada peringkat
- Premature Rupture of Membrane ReadingDokumen4 halamanPremature Rupture of Membrane ReadingAdrienne Nicole AlforteBelum ada peringkat
- Acute Fatty Liver of Pregnancy: Letter To EditorDokumen2 halamanAcute Fatty Liver of Pregnancy: Letter To EditorsaryindrianyBelum ada peringkat
- Pregnancy-Related Liver Disorders: Seminar Journal of Clinical and Experimental HepatologyDokumen12 halamanPregnancy-Related Liver Disorders: Seminar Journal of Clinical and Experimental HepatologysaryindrianyBelum ada peringkat
- Nelson2013 Ajog PDFDokumen7 halamanNelson2013 Ajog PDFsaryindrianyBelum ada peringkat
- Acute Fatty Liver of Pregnancy: Better Understanding of Pathogenesis and Earlier Clinical Recognition Results in Improved Maternal OutcomesDokumen8 halamanAcute Fatty Liver of Pregnancy: Better Understanding of Pathogenesis and Earlier Clinical Recognition Results in Improved Maternal OutcomessaryindrianyBelum ada peringkat
- ACG Clinical Guideline: Liver Disease and Pregnancy: Practice GuidelinesDokumen19 halamanACG Clinical Guideline: Liver Disease and Pregnancy: Practice GuidelinessaryindrianyBelum ada peringkat
- Birth After Previous Caesarean Section (C Obs 38) Re Write July 2015 1Dokumen27 halamanBirth After Previous Caesarean Section (C Obs 38) Re Write July 2015 1saryindrianyBelum ada peringkat
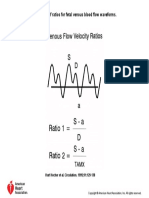
- Calculation of Ratios For Fetal Venous Blood Flow WaveformsDokumen1 halamanCalculation of Ratios For Fetal Venous Blood Flow WaveformssaryindrianyBelum ada peringkat
- 1 s2.0 S0889854515001163Dokumen18 halaman1 s2.0 S0889854515001163saryindrianyBelum ada peringkat
- Causes and Management of Surgical Wound Dehiscence: Department of General SurgeryDokumen10 halamanCauses and Management of Surgical Wound Dehiscence: Department of General SurgerysaryindrianyBelum ada peringkat
- Post Caesarean Surgical Site Infections 2Dokumen6 halamanPost Caesarean Surgical Site Infections 2saryindrianyBelum ada peringkat
- Risk Factors For Wound Dehiscence After Laparotomy - Clinical Control TrialDokumen9 halamanRisk Factors For Wound Dehiscence After Laparotomy - Clinical Control TrialsaryindrianyBelum ada peringkat
- Technical Series 2 Using PartographDokumen5 halamanTechnical Series 2 Using PartographsaryindrianyBelum ada peringkat
- Efektifitas Pijat Oketani Terhadap Bendungan Asi Pada Ibu Postpartum Di RSB - Masyita MakassarDokumen5 halamanEfektifitas Pijat Oketani Terhadap Bendungan Asi Pada Ibu Postpartum Di RSB - Masyita MakassarSyahrul IqbalBelum ada peringkat
- Dystocia SOGCDokumen16 halamanDystocia SOGCAdhitia NugrahantoBelum ada peringkat
- Quiz 2 Gestational Diabetes MellitusDokumen10 halamanQuiz 2 Gestational Diabetes MellitusShirley L. CarumbaBelum ada peringkat
- Portfolio IN Community Health Nursing: Submitted byDokumen6 halamanPortfolio IN Community Health Nursing: Submitted byJay VillasotoBelum ada peringkat
- Course Title Event Code (S) : Certified Antenatal Postnatal Exercise SpecialistDokumen4 halamanCourse Title Event Code (S) : Certified Antenatal Postnatal Exercise SpecialistAmruta BhagwatBelum ada peringkat
- Session 1Dokumen81 halamanSession 1Aida RascalBelum ada peringkat
- Shoulder DystociaDokumen22 halamanShoulder Dystociaamulan_aBelum ada peringkat
- Literature Review Low Birth WeightDokumen4 halamanLiterature Review Low Birth Weightc5qx9hq5100% (1)
- Laura Final FinalDokumen68 halamanLaura Final Finalngalame lauraBelum ada peringkat
- Perceptions and Beliefs Regarding Caesarean Section Among Pregnant Women Receiving Antenatal Care at Ishaka Adventist HospitalDokumen12 halamanPerceptions and Beliefs Regarding Caesarean Section Among Pregnant Women Receiving Antenatal Care at Ishaka Adventist HospitalKIU PUBLICATION AND EXTENSIONBelum ada peringkat
- Fetal Heart Rate Monitoring in Pregnancy and Labour 6.0Dokumen42 halamanFetal Heart Rate Monitoring in Pregnancy and Labour 6.0Wong Lee CheeBelum ada peringkat
- Placenta Abruptio BrochureDokumen2 halamanPlacenta Abruptio Brochurecompmom5Belum ada peringkat
- Dysfunctional LabourDokumen128 halamanDysfunctional LabourDebjyoti KarmakarBelum ada peringkat
- Use and Safety of Kielland S Forceps in Current.6Dokumen5 halamanUse and Safety of Kielland S Forceps in Current.6ziehonkBelum ada peringkat
- Mannual Removal of Placenta: Presented By-Bhawna Joshi MSC. (N) 2 YearDokumen23 halamanMannual Removal of Placenta: Presented By-Bhawna Joshi MSC. (N) 2 YearBhawna JoshiBelum ada peringkat
- 01 Manajemen Risiko Klinik (MRK)Dokumen32 halaman01 Manajemen Risiko Klinik (MRK)irmaBelum ada peringkat
- Latest Trend in Labor and DeliveryDokumen6 halamanLatest Trend in Labor and DeliveryVenus MaglupayBelum ada peringkat
- Management of The Rhesus Negative MotherDokumen32 halamanManagement of The Rhesus Negative MothertotalpregnancycareBelum ada peringkat
- Roisin Ryan Obstetrics Final Year RevisionDokumen78 halamanRoisin Ryan Obstetrics Final Year RevisionDanny SchBelum ada peringkat
- ATS Menjawab Soal UKN Maret 2021 HQQDokumen18 halamanATS Menjawab Soal UKN Maret 2021 HQQanton suponoBelum ada peringkat
- PartogramDokumen3 halamanPartogrammuchalaithBelum ada peringkat
- ABSTRACT AED Paola BarrigueteDokumen5 halamanABSTRACT AED Paola BarrigueteDaniBelum ada peringkat
- Obstetric & Gynecology Nursing: Topic-Physiological Changes During LabourDokumen54 halamanObstetric & Gynecology Nursing: Topic-Physiological Changes During LabourBhumi ChouhanBelum ada peringkat