Leukemia-Induced Gingival Overgrowth As An Early Manifestation in Pregnancy: A Case Report
Diunggah oleh
Liana OpriţăJudul Asli
Hak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Leukemia-Induced Gingival Overgrowth As An Early Manifestation in Pregnancy: A Case Report
Diunggah oleh
Liana OpriţăHak Cipta:
Format Tersedia
Journal of
Periodontology
&
Implant Dentistry
Case Report
Leukemia-induced Gingival Overgrowth as an Early
Manifestation in Pregnancy: A Case Report
Parichehr Behfarnia1 Parviz Deyhimi2 Abbas Haghighat3 Vahid Naemi4 Narges Naghsh5*
1
Assistant Professor, Department of Periodontology and Torabinejad Dental Research Center, School of Dentistry, Isfahan University of
Medical Sciences, Isfahan, Iran
2
Associate Professor, Department of Oral and Maxillofacial Pathology and Torabinejad Dental Research Center, School of Dentistry,
Isfahan University of Medical Sciences and, Isfahan, Iran
3
Assistant Professor, Department of Oral and Maxillofacial Surgery and Torabinejad Dental Research Center, School of Dentistry,
Isfahan University of Medical Sciences, Isfahan, Iran
4
Postgraduate Student, Department of Oral and Maxillofacial Surgery and Torabinejad Dental Research Center, School of Dentistry,
Isfahan University of Medical Sciences, Isfahan, Iran
5
Assistant Professor, Department of Periodontology and Torabinejad Dental Research Center, School of Dentistry, Isfahan University of
Medical Sciences, Isfahan, Iran
*Corresponding Author; E-mail: n_naghsh@dnt.mui.ac.ir
Received: 7 April 2014; Accepted: 7 July 2014
J Periodontol Implant Dent 2014;6(2):6063 | doi: 10.15171/jpid.2014.011
This article is available from: http://dentistry.tbzmed.ac.ir/jpid
2014 The Authors; Tabriz University of Medical Sciences
This is an Open Access article distributed under the terms of the Creative Commons Attribution License
(http://creativecommons.org/licenses/by/3.0), which permits unrestricted use, distribution, and reproduction in any medium, provided the original
work is properly cited.
Abstract
Leukemia is a neoplastic disease with early oral and periodontal manifestations such as ulceration, infection, bleeding and
gingival hyperplasia. This paper describes a 39-year-old pregnant woman with a diagnosis of acute myelomonocytic leukemia (AML), with gingival enlargement in the upper and lower jaws. A gingival biopsy was performed, followed by a
complete blood count and peripheral blood smear. From a histopathological view, infiltration of the neoplastic (myelomonocytoblastic) cells was observed and many immature lymphoid cells were revealed by the hematologic tests. The interesting clinical finding about this case was the absence of spontaneous bleeding and profuse bleeding on probing. This case
is reported to emphasize the leukemia-induced gingival enlargement in pregnancy and the early diagnosis of AML by dentists, which results in immediate treatment and management of the patient.
Key words: Gingival overgrowth, Leukemia, Oral manifestation.
Introduction
any systemic diseases produce oral changes in
different stages of their course. Leukemia is a
fatal disease of unknown etiology, which is characterized by excessive proliferation of primitive white
blood cells in the bone marrow and/or blood, and its
presence as leukemic infiltrates has been reported in
the lungs, kidneys, bowels, breasts, testes, eyes,
meninges, lymph nodes, liver, skin and the oral cavity.1 Leukemias are divided into chronic and acute
forms clinically, which in turn, are classified according to the type of the white blood cell involved, i.e.
lymphoid and myeloid.2 The association between
leukemia and pregnancy is not common.3 Most leukemias diagnosed during pregnancy are acute.4 It is
not surprising that in some patients the management
of acute leukemia will be complicated by a coexis-
Gingival Hyperplasia in a Leukemic Woman
tent pregnancy. However, the association of leukemia and pregnancy is uncommon.5 Its prevalence is
low at ~1 in 10,000 pregnancies, and as a result data
are limited to small retrospective series and case reports, rendering evidence-based recommendations
for management strategies difficult.6 Oral changes
are non-specific in patients with chronic leukemia.
Oral manifestations of acute leukemia include gingival swelling, oral ulceration, petechiae, candidiasis,
ulcerative necrotic lesions and hemorrhage.2
This paper presents a case of acute myelomonocytic leukemia (AML) with manifestations of gingival hyperplasia in the upper and lower jaws. In fact
our aim is to provide dentists with early manifestations of leukemia and gingival hyperplasia in pregnancy for immediate treatment and management of
patients.
Case Report
A 39-year-old pregnant woman (gestational age = 12
w + 6 d) with a diagnosis of gingival hyperplasia
was referred to the Department of Periodontology,
Isfahan University of Medical Sciences, complaining
of gingival enlargement that had started and developed during the last 21 days.
Medical History
Systematically she had a feeling of weakness and
fatigue and except for OCPs (oral contraceptives)
she had not used any other medications over the past
year.
General Examinations
The patient did not have other lesions on her skin or
any other abnormality.
Extraoral Examinations
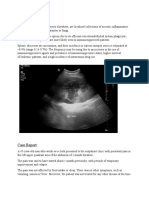
She had a submental lymphadenopathy (1 cm in diameter) that compromised both breathing and swallowing and could be palpated from skin (Figure 1).
Oral Examinations
Gingival hyperplasia was observed on the buccal,
lingual and palatal aspects of all the teeth, which re-
61
Figure 1. Submental lymphadenopathy
sulted in mouth breathing and an open bite occlusion. The gingiva was bulbous and pale. Her gingival
consistency was firm, with no spontaneous bleeding
or excessive bleeding by palpation or probing, accompanied by fetor oris with a necrotic layer around
the gingiva of the anterior teeth and an escharotic
lesion in the buccal vestibule of lower anterior teeth.
Her oral hygiene was fair (Figure 2).
Radiographic Examinations
There was no bone loss or abnormality on the panoramic radiograph. Due to the general medical status
of the patient, moderate plaque accumulation, lack of
calculus and rapid enlargement of gingivae, we
avoided any periodontal treatment and a biopsy from
anterior gingiva of the upper jaw was taken on the
same day. Because of the clinical picture and since
leukemia may appear during pregnancy, the patient
was referred to an oncology center to be under the
supervision of a hematologist. She was advised to
undergo a complete blood count test, peripheral
blood smear and bone marrow biopsy. Within a span
of two weeks we were informed that unfortunately
she had died. Therefore, it took only 5 weeks from
the appearance of the first signs of the disease for her
to die.
Figure 2. Generalized diffuse gingival hyperplasia
62
Behfarnia et al.
Histopathology
In the present histopathological study, neoplastic
proliferation of myelomonocytoblastic cells with
pleomorphism, atypism, severe hyperchromatism of
nuclei, vesicular nuclei, multiple mitotic figures, lobulated and bean-shaped nuclei and occasionally
eosinophilic cytoplasm associated with two or three
nucleated giant cells were seen diffusely in the lamina propria up to the striated squamous epithelium.
With a CD33 marker (marker of early myeloid cells
and monocytes), staining intensity was evaluated as
2+. In the blood smear study, multiple large-sized
cells with convoluted nuclei, fine chromatin and occasionally containing nucleoli, were seen, in addition
to a decrease in platelet counts. According to these
findings, a diagnosis of acute myelomonocytic leukemia (AML) was suggested. For a definitive diagnosis, further studies with bone marrow biopsy, bone
marrow aspiration and flow cytometry were suggested but unfortunately the patient died from the
disease (Figures 3-5).
diagnosis is confirmed by tissue biopsy or fine needle aspiration cytology.8
These changes are consequences of neoplastic proliferation of white blood cells, which affects the
normal production of erythrocytes, leukocytes and
Figure 3. Neoplastic proliferation of myelomonocytic
cells with pleomorphism (magnification x 100 ) H&E
Hematologic Values
The hematologic reports revealed that the patient had
a white blood cell count of 155,900/L, red blood
cells count of 2.40 million/L, platelet count of
28,000/L, hemoglobin (Hb) value of 8.6 g/dL,
MCH value of 35.8/pg and MCHC value of 36.4
g/dL. In the peripheral blood smear (PBS), severe
leukocytosis with many immature lymphoid cells,
severe thrombocytopenia, anisocytosis (+), anisochromia (few) and poikilocytosis (mild) were seen.
The results of hematologic tests confirmed the diagnosis of acute myelomonocytic leukemia (Figure 6).
Discussion
There are many systemic conditions with unvarying
manifestations in the gums and deep periodontium.
Leukemia has varying rates of development and in
most cases a reserved prognosis. Acute leukemias
are a group of neoplastic diseases with proliferation
of immature white blood cells, especially in the bone
marrow, spleen and lymph nodes. Acute myelomonocytic leukemia (AML) is an aggressive hematopoietic neoplasm, characterized by clonal proliferation of immature myeloid cells. Due to its high
rate of morbidity, early diagnosis and treatment is
essential because it can lead to death within a few
days. Some of the typical manifestations of AML are
paleness of the oral mucosa with gingival bleeding,
which can in turn develop to painless gingival hyperplasia, marrow failure, cytopenia, fever, fatigue,
mucosal pallor, petechiae and oral infection.7 The
Figure 4. Neoplastic proliferation of myelomonocytic
cells with pleomorphism (magnification x400) H&E
Figure 5. Immunohistochemistry (IHC) with marker
of CD33 shows large early myeloid cells (magnification
x400)
Gingival Hyperplasia in a Leukemic Woman
63
nimal to complete tooth coverage, creating functional and esthetic concerns.8 Leukemic gingival infiltration appears to be limited to dentate subjects,
implying a potential role for tooth-associated local
factors. In a recent research performed by
Chelghoum et al in 2005 on acute leukemia in pregnant women, it was confirmed that 84% of patients
had AML and 16% had ALL, with 76% of patients
diagnosed during the second or third trimesters.4
Gingival enlargement represents a 5% frequency as
the initial presenting complication of AML. 12
Conclusion
Figure 6. Peripheral Blood Smear (PBS) shows severe
leukocytosis with many immature lymphoeid cells.
Black arrows represent early myeloid cells and red
arrows show lymphocytes (magnification 1000).
platelets. Since oral manifestations of acute leukemia
occur early in the course of the disease, about 65%
of acute leukemia patients consult a dentist. Thus,
since acute exacerbation has been reported after such
surgical interventional procedures, dental personnel
should be alert to these findings and avoid such procedures.9 Differential diagnoses that are considered
in relation to gingival enlargement include conditional enlargement in pregnancy, drug-induced, vitamin C deficiency-induced and inflammatory and
hereditary gingival enlargement. Clinical examinations of the gingiva, including color and consistency,
rule out the source of vitamin C deficiency and pregnancy because in these situations lesions are clinically deep red or bluish red, soft and friable with a
smooth shiny surface that bleeds easily.10
Considering the medical history of the patient,
drug-induced gingival hyperplasia could not have
been the cause of enlargement. The rapid growth of
the gingivae rules out the chronic inflammatory enlargement. In hereditary gingival hyperplasia, there
is a family history of gingival enlargement that usually begins with eruption of both primary and permanent teeth.11 In the presented case, the resemblance of the lesions to fibrotic enlargement might
have led to misdiagnosis. The change in gingival
morphology and its cyanotic appearance may be a
result of reactive hyperplasia, dense leukemic infiltration of connective tissue and compression of local
vasculatures, causing ischemia.12 The susceptibility
of gingival tissues to leukemic cell infiltration is attributed to their microanatomy and expression of
endothelial adhesion molecules, increasing infiltration of leukocytes.13
The extent of gingival overgrowth ranges from mi
In our case the chief complaint of the patient was
gingival hyperplasia and respiratory problems. In
general, early diagnosis of AML by dentists results
in prompt treatment and management of the patient.
References
1.
2.
3.
4.
5.
6.
7.
8.
9.
10.
11.
12.
13.
Henderson ES, Lister TA. Leukemia, 5th ed. Philadelphia:
W.B. Saunders Company; 1990. p. 50-1.
Weckx LL, Hidal LB, Marcucci G. Oral manifestations of
leukemia. Ear Nose Throat J 1990;69:341-2.
Jurez S, Cuadrado Pastor JM, Feliu J, Gonzlez Barn M,
Ordez A, Montero JM. Association of leukemia and pregnancy: clinical and obstetric aspects. Am J Clin Oncol
1988;11:159-65. doi: 10.1097/00000421-198804000-00014
Hoxha SL, Ibishi VA, Brovina A, Hoxha M, Lulaj S. Refusal
of treatment for acute leukemia in pregnancy: a case report. J
Med Case Rep 2013 31;7:148-51. doi: 10.1186/1752-19477-148
Chelghoum Y, Vey N, Raffoux E, Huguet F, Pigneux A,
Witz B, et al. Acute leukemia during pregnancy: a report on
37 patients and a review of the literature. Cancer
2005;104:110-7. doi: 10.1002/cncr.21137
Milojkovic D, Apperley JF. How I treat leukemia during
pregnancy. Blood 2014 13;123:974-84. doi: 10.1182/blood2013-08-283580
McKenna SJ. Leukemia. Oral Surg Oral Med Oral Pathol
Oral
Radiol
Endod
2000;89:137-9.
doi:
10.1016/j.oooo.2013.03.003
Abdullah BH, Yahya HI, Kummoona RK, Hilmi FA, Mirza
KB. Gingival fine needle aspiration cytology in acute leukemia. J Oral Pathol Med 2002;31:55-8. doi:
10.1034/j.1600-0714.2002.310109.x
Stafford R, Sonis S, Lockart P, Sonis A: Oral pathoses as
diagnostic indicators in leukemia. Oral Surg Oral Med Oral
Pathol 1980;50:134-9. doi: 10.1016/0030-4220(80)90200-5
Armitage GC. Development of a classification system for
periodontal diseases and conditions. Ann Periodontol
1999;4:1-6.
Felix DE, Lukens J. Oral symptom as a chief sign of acute
monoblastic leukemia: report of case. J Am Dent Assoc
1986;113:899-900. doi: 10.14219/jada.archive.1986.0308
Cooper CL, Loewen R, Shore T. Gingival hyperplasia complicating acute myelomonocytic leukemia. J Can Dent Assoc
2000;66:789.
Williams WJ, Beutler E, Erslev AJ, Lichtman MA. Hematology, 4th ed. New York: McGraw Hill; 1990. p. 243-4.
Anda mungkin juga menyukai
- Fast Facts: Myelofibrosis: Reviewed by Professor Ruben A. MesaDari EverandFast Facts: Myelofibrosis: Reviewed by Professor Ruben A. MesaBelum ada peringkat
- Jurnalku OsccDokumen4 halamanJurnalku OsccAndiOctafiantoBelum ada peringkat
- Leukemic Gingival Enlargement: Report of A Rare Case With Review of LiteratureDokumen3 halamanLeukemic Gingival Enlargement: Report of A Rare Case With Review of LiteratureM .Hafis Habci Amran 2104113711Belum ada peringkat
- Diagnosis of Blood and Bone Marrow DisordersDari EverandDiagnosis of Blood and Bone Marrow DisordersSa A. WangBelum ada peringkat
- An Etiological Reappraisal of Pancytopenia - LargestDokumen9 halamanAn Etiological Reappraisal of Pancytopenia - LargestKaye Antonette AntioquiaBelum ada peringkat
- Chédiak Higashi SyndromeDokumen18 halamanChédiak Higashi SyndromePurwana NasirBelum ada peringkat
- Jurnal Gilut 22Dokumen7 halamanJurnal Gilut 22Yenny Dwi Anggra SudarmajiBelum ada peringkat
- EARLY RECOGNITION TO DETECT THE MALIGNANCY IN CHILDREN - Dr. ElmiDokumen8 halamanEARLY RECOGNITION TO DETECT THE MALIGNANCY IN CHILDREN - Dr. ElmiElmi AstrabelBelum ada peringkat
- A Clinicohaematological Profile of Splenomegaly: Varsha S. Dabadghao, Arundhati G.Diwan, Amol M. RaskarDokumen9 halamanA Clinicohaematological Profile of Splenomegaly: Varsha S. Dabadghao, Arundhati G.Diwan, Amol M. RaskarLianSiahaanBelum ada peringkat
- Oral Findings of Systemic Lupus Erythematosus-A Grand Round CaseDokumen5 halamanOral Findings of Systemic Lupus Erythematosus-A Grand Round CaseIntanBelum ada peringkat
- Hemangioma Oral (Gill)Dokumen4 halamanHemangioma Oral (Gill)koizorabigBelum ada peringkat
- Hemoblastosis in ChildrenDokumen40 halamanHemoblastosis in ChildrenAli Baker Algelane100% (3)
- 10 11648 J CRJ 20200802 14Dokumen3 halaman10 11648 J CRJ 20200802 14Marj MendezBelum ada peringkat
- Clinical and Pathologic Analyses of Tuberculosis in The Oral Cavity: Report of 11 CasesDokumen8 halamanClinical and Pathologic Analyses of Tuberculosis in The Oral Cavity: Report of 11 CasesMaria Lozano Figueroa 5to secBelum ada peringkat
- Leukemic Gingival Enlargement: A Report of Two Cases: Santosh Patil, Nitin Kalla, D.N.S.V Ramesh, A.R. KallaDokumen4 halamanLeukemic Gingival Enlargement: A Report of Two Cases: Santosh Patil, Nitin Kalla, D.N.S.V Ramesh, A.R. KallaYuriskaMurestininggarBelum ada peringkat
- Hansen1985 Proliferative Verrucous LeukoplakiaDokumen14 halamanHansen1985 Proliferative Verrucous LeukoplakiaJulia FerigattoBelum ada peringkat
- Chronic Myeloid Leukemia Presenting With Priapism 2329 6917 1000171Dokumen5 halamanChronic Myeloid Leukemia Presenting With Priapism 2329 6917 1000171SalwiyadiBelum ada peringkat
- Early - Stage Hodgkins Lymphoma in A Child A CaseDokumen6 halamanEarly - Stage Hodgkins Lymphoma in A Child A CaseХарш Навнітбхаі НімаватBelum ada peringkat
- Langerhans Cell Histiocytosis Literature Review and Descriptive Analysis of Oral ManifestationsDokumen4 halamanLangerhans Cell Histiocytosis Literature Review and Descriptive Analysis of Oral ManifestationsafmzamdswsfksxBelum ada peringkat
- Potentially Malignant Disorders MADE EASYDokumen11 halamanPotentially Malignant Disorders MADE EASYMohammedBelum ada peringkat
- Haematology Department Annual Report 2009-2010Dokumen14 halamanHaematology Department Annual Report 2009-2010Drashua AshuaBelum ada peringkat
- 47uppin EtalDokumen4 halaman47uppin EtaleditorijmrhsBelum ada peringkat
- Acute Lymphoblastic Leukemia RadiopediaDokumen2 halamanAcute Lymphoblastic Leukemia RadiopediaRani Henty NovitaBelum ada peringkat
- JurnalDokumen7 halamanJurnalChintya Monica AmelindaBelum ada peringkat
- Hypopituitarism in Langerhans Cell Histiocytosis Seven Cases and Literature ReviewDokumen8 halamanHypopituitarism in Langerhans Cell Histiocytosis Seven Cases and Literature ReviewafdtfngqbBelum ada peringkat
- Oral Leukoplakia and ErythroplakiaDokumen8 halamanOral Leukoplakia and ErythroplakiadeepaBelum ada peringkat
- Mesenteric Venous Thrombosis As A Complication of Appendicitis in An AdolescentDokumen5 halamanMesenteric Venous Thrombosis As A Complication of Appendicitis in An AdolescentEma DianthiBelum ada peringkat
- Understanding hematopoiesis, hemostasis disorders and shockDokumen24 halamanUnderstanding hematopoiesis, hemostasis disorders and shockRisna SariBelum ada peringkat
- Why Does My Patient Limphadenopathy or Splenomegaly?Dokumen14 halamanWhy Does My Patient Limphadenopathy or Splenomegaly?lacmftcBelum ada peringkat
- Sisay Berane 083 PancytopeniaDokumen23 halamanSisay Berane 083 PancytopeniaRas Siko SafoBelum ada peringkat
- Guizzetti - 2016Dokumen10 halamanGuizzetti - 2016Bogdan TrandafirBelum ada peringkat
- Bio Case Study 1Dokumen7 halamanBio Case Study 1Christian GallardoBelum ada peringkat
- Treatment Options For Patients With Primary Myelo BrosisDokumen11 halamanTreatment Options For Patients With Primary Myelo BrosisLink BuiBelum ada peringkat
- BMC Dermatology: Schönlein-Henoch Purpura During Pregnancy With Successful Outcome For Mother and NewbornDokumen5 halamanBMC Dermatology: Schönlein-Henoch Purpura During Pregnancy With Successful Outcome For Mother and NewbornteguhBelum ada peringkat
- Testicular Involvement of Acute Lymphoblastic Leukemia in Children and Adolescents: Diagnosis, Biology, and ManagementDokumen15 halamanTesticular Involvement of Acute Lymphoblastic Leukemia in Children and Adolescents: Diagnosis, Biology, and ManagementabdullahBelum ada peringkat
- Adenomegalias 08Dokumen10 halamanAdenomegalias 08Brenda CaraveoBelum ada peringkat
- 12 Hematological MalignanciesDokumen28 halaman12 Hematological MalignanciesalitahawarbarintBelum ada peringkat
- 2014 Kabir Et Al. - Chronic Eosinophilic Leukaemia Presenting With A CDokumen4 halaman2014 Kabir Et Al. - Chronic Eosinophilic Leukaemia Presenting With A CPratyay HasanBelum ada peringkat
- Sumber 5Dokumen4 halamanSumber 5Observasipusk lapaiBelum ada peringkat
- Guidelines for diagnosing childhood leukemiasDokumen35 halamanGuidelines for diagnosing childhood leukemiasNarendraswari Mendina KusumawardhaniBelum ada peringkat
- Hypersplenism: Review Article: November 2012Dokumen12 halamanHypersplenism: Review Article: November 2012V1QT0RBelum ada peringkat
- Oral Findings and Diagnosis of Systemic Lupus ErythematosusDokumen6 halamanOral Findings and Diagnosis of Systemic Lupus ErythematosusArditya Dwi YudistiraBelum ada peringkat
- Leukemias 2Dokumen56 halamanLeukemias 2Y. Beatrice AbigailBelum ada peringkat
- ART Mod. Grey y MariDokumen6 halamanART Mod. Grey y MarigreynerBelum ada peringkat
- 2018 AAOM Clinical Practice Statement Subject LeukoplakiaDokumen4 halaman2018 AAOM Clinical Practice Statement Subject LeukoplakiaEmiliaAndreeaBalanBelum ada peringkat
- ENT CaseDokumen16 halamanENT CaseTee MatBelum ada peringkat
- Hyperleukositosis: Bidasari Lubis-Olga Rasiyanti SiregarDokumen26 halamanHyperleukositosis: Bidasari Lubis-Olga Rasiyanti SiregarYogiPrimaZulkifliBelum ada peringkat
- 002 MedicineDokumen3 halaman002 Medicinenightfury200313Belum ada peringkat
- HES Case ReportDokumen3 halamanHES Case ReportalaaBelum ada peringkat
- The Presentation - Crohn's Disease - (3course)Dokumen17 halamanThe Presentation - Crohn's Disease - (3course)Kashif KhandaBelum ada peringkat
- Journal Reading LeukoplakiaDokumen17 halamanJournal Reading LeukoplakiaIdha FitriyaniBelum ada peringkat
- 101 FullDokumen15 halaman101 FullhelinBelum ada peringkat
- Dental Care of Children With Leukemia-An OverviewDokumen6 halamanDental Care of Children With Leukemia-An OverviewLiana OpriţăBelum ada peringkat
- All About Pleural EffusionDokumen6 halamanAll About Pleural EffusionTantin KristantoBelum ada peringkat
- Leukemia Research Paper Thesis StatementDokumen9 halamanLeukemia Research Paper Thesis Statementaparnaharrisonstamford100% (1)
- Prolonged Fever, Hepatosplenomegaly, and Pancytopenia in A 46-Year-Old WomanDokumen6 halamanProlonged Fever, Hepatosplenomegaly, and Pancytopenia in A 46-Year-Old WomanFerdy AlviandoBelum ada peringkat
- Adenoid Cystic Carcinoma of Hard Palate: A Case ReportDokumen5 halamanAdenoid Cystic Carcinoma of Hard Palate: A Case ReportHemant GuptaBelum ada peringkat
- Radiology Case Report - Splenic AbscessDokumen6 halamanRadiology Case Report - Splenic AbscessAbeebBelum ada peringkat
- WBC Disorder PPT 2Dokumen56 halamanWBC Disorder PPT 2YESHASWI PIKLEBelum ada peringkat
- Toward An Understanding of Competency Identification and Assessment in Health Care ManagementDokumen25 halamanToward An Understanding of Competency Identification and Assessment in Health Care ManagementLiana OpriţăBelum ada peringkat
- 101 Free Online Journal and Research Databases For Academics Free Resource PDFDokumen12 halaman101 Free Online Journal and Research Databases For Academics Free Resource PDFNorbert GácsérBelum ada peringkat
- Surgery of The Liver Biliary Tract: L. H. B Um ArtDokumen27 halamanSurgery of The Liver Biliary Tract: L. H. B Um ArtLiana OpriţăBelum ada peringkat
- How Does Knowledge Management Improve The Service Industry?Dokumen44 halamanHow Does Knowledge Management Improve The Service Industry?Preeti GuptaBelum ada peringkat
- ManuscriptDokumen15 halamanManuscriptLiana OpriţăBelum ada peringkat
- Ast 2017 1756Dokumen28 halamanAst 2017 1756Liana OpriţăBelum ada peringkat
- MPRA Paper 83038 PDFDokumen33 halamanMPRA Paper 83038 PDFLiana OpriţăBelum ada peringkat
- 91931-Article Text-260086-1-10-20131218Dokumen8 halaman91931-Article Text-260086-1-10-20131218Liana OpriţăBelum ada peringkat
- Systems: Organizational Learning in Health Care OrganizationsDokumen10 halamanSystems: Organizational Learning in Health Care OrganizationsLiana OpriţăBelum ada peringkat
- SOEPpapers On Multidisciplinary Panel Data Research at DIW BerlinDokumen31 halamanSOEPpapers On Multidisciplinary Panel Data Research at DIW BerlinLiana OpriţăBelum ada peringkat
- Local Ecological Knowledge in Angklung Paglak of Using Community of Banyuwangi, IndonesiaDokumen14 halamanLocal Ecological Knowledge in Angklung Paglak of Using Community of Banyuwangi, IndonesiaLiana OpriţăBelum ada peringkat
- Jpis 44 293 PDFDokumen7 halamanJpis 44 293 PDFintanchairranyBelum ada peringkat
- The Relationship Between Knowledge Management and Nursing Care PerformanceDokumen13 halamanThe Relationship Between Knowledge Management and Nursing Care PerformanceLiana OpriţăBelum ada peringkat
- 89 954 1 PBDokumen14 halaman89 954 1 PBViorelBelum ada peringkat
- Effects of Diet Restriction On Life Span and Age-Related Changes in DogsDokumen6 halamanEffects of Diet Restriction On Life Span and Age-Related Changes in DogsLiana OpriţăBelum ada peringkat
- PeridodonticsDokumen7 halamanPeridodonticsLiana OpriţăBelum ada peringkat
- Ijss Feb-10Dokumen4 halamanIjss Feb-10Liana OpriţăBelum ada peringkat
- Dental Care of Children With Leukemia-An OverviewDokumen6 halamanDental Care of Children With Leukemia-An OverviewLiana OpriţăBelum ada peringkat
- Oral Complications in Pediatric Oncology Patients: Stephen A. Fayle, Martin E.J. CurzonDokumen7 halamanOral Complications in Pediatric Oncology Patients: Stephen A. Fayle, Martin E.J. CurzonLiana OpriţăBelum ada peringkat
- Jurnal 2 PDFDokumen3 halamanJurnal 2 PDFnabila pranditaBelum ada peringkat
- L T O P: Eukemia: He Ral ErspectiveDokumen2 halamanL T O P: Eukemia: He Ral ErspectiveLiana OpriţăBelum ada peringkat
- Oral MedicineDokumen7 halamanOral MedicineAisa Nirmala SetyaniBelum ada peringkat
- Prevention of Oral Lesions in Children - 2006Dokumen5 halamanPrevention of Oral Lesions in Children - 2006Liana OpriţăBelum ada peringkat
- Oral Manifestations in Acute LeukemiaDokumen8 halamanOral Manifestations in Acute LeukemiaLiana OpriţăBelum ada peringkat
- Oral Care For Children With Leukaemia: SY Cho, AC Cheng, MCK ChengDokumen6 halamanOral Care For Children With Leukaemia: SY Cho, AC Cheng, MCK Chengvefiisphepy83312Belum ada peringkat
- Dental Care of Children With Leukemia-An OverviewDokumen6 halamanDental Care of Children With Leukemia-An OverviewLiana OpriţăBelum ada peringkat
- Oral Signs of Leukemia PDFDokumen4 halamanOral Signs of Leukemia PDFabu_ubaidah_3Belum ada peringkat
- Ajdr Inpress 29995 PDFDokumen6 halamanAjdr Inpress 29995 PDFLiana OpriţăBelum ada peringkat
- Ijss-Cr 1 (8) Ra01Dokumen4 halamanIjss-Cr 1 (8) Ra01Liana OpriţăBelum ada peringkat
- 233 241 PDFDokumen9 halaman233 241 PDFLiana OpriţăBelum ada peringkat
- Histology: Ust Faculty of Medicine and Surgery Class of 2016Dokumen14 halamanHistology: Ust Faculty of Medicine and Surgery Class of 2016Ashley Beatriz PascualBelum ada peringkat
- Cell Modification LASDokumen8 halamanCell Modification LASLiamie MedezBelum ada peringkat
- Histopathology Techniques: A Guide to Grossing, Processing, and StainingDokumen48 halamanHistopathology Techniques: A Guide to Grossing, Processing, and StainingCAMILLE MAGNO100% (3)
- Suprarenal GlandDokumen19 halamanSuprarenal GlandKay BristolBelum ada peringkat
- Transport System Question and AnswersDokumen12 halamanTransport System Question and Answerskumara guruparanBelum ada peringkat
- Living Organisms Reproduce by Two Methods: Asexual ReproductionDokumen36 halamanLiving Organisms Reproduce by Two Methods: Asexual ReproductionMary SiddBelum ada peringkat
- Chapter 17 BloodDokumen10 halamanChapter 17 BloodTony SnearlyBelum ada peringkat
- Biology Reviewer PrelimsDokumen10 halamanBiology Reviewer PrelimsShaira CogollodoBelum ada peringkat
- Bio Exp 2 Hanis HaidaDokumen10 halamanBio Exp 2 Hanis HaidaӇⱭӀƊⱭ ƘӇⱭlӀՏƳⱭ ՏƲƑƳⱭBelum ada peringkat
- Anatomy and Physiology of the BrainDokumen7 halamanAnatomy and Physiology of the BrainCUESCANO, CRISTEL G. BSMT 2-ABelum ada peringkat
- 7mm Frog Embryo - EMBLabDokumen3 halaman7mm Frog Embryo - EMBLabIvy Cruz100% (1)
- Special HistologyDokumen64 halamanSpecial HistologyElijah KamaniBelum ada peringkat
- Periodontal Ligament 1Dokumen60 halamanPeriodontal Ligament 1ashishubaBelum ada peringkat
- Bio 121 Chapter 04Dokumen78 halamanBio 121 Chapter 04tpsawyerBelum ada peringkat
- Acute and Chronic InflammationDokumen36 halamanAcute and Chronic Inflammationibnbasheer89% (18)
- Yoga Class 12Dokumen13 halamanYoga Class 12Vandan KBelum ada peringkat
- Renal Physiology Lab ReportDokumen5 halamanRenal Physiology Lab Reportpatricia ankarBelum ada peringkat
- Blood Grouping Presentation 4Dokumen13 halamanBlood Grouping Presentation 4Aisha ShahfiqueeBelum ada peringkat
- Red Blood Cell Phenotyping of Blood Donors in Islamabad, PakistanDokumen5 halamanRed Blood Cell Phenotyping of Blood Donors in Islamabad, PakistanAHNS123Belum ada peringkat
- ThyroidDokumen96 halamanThyroidNimer Abdelhadi AliBelum ada peringkat
- Wilm's Tumor Pa Tho PhysiologyDokumen1 halamanWilm's Tumor Pa Tho Physiologya_yeLBelum ada peringkat
- BIO01 CO1 PPT - An Overview of The CellDokumen60 halamanBIO01 CO1 PPT - An Overview of The CellCHRISTIAN MATTHEW DELA CRUZBelum ada peringkat
- The Physiological Effects of MassageDokumen3 halamanThe Physiological Effects of Massageanny100% (1)
- Characteristics of Blood Group Antibodies Immunoglobulin Classes and In Vitro PropertiesDokumen1 halamanCharacteristics of Blood Group Antibodies Immunoglobulin Classes and In Vitro PropertiesyepBelum ada peringkat
- Koding Diagnosa CancerDokumen6 halamanKoding Diagnosa CancerFarmasi SitostatikBelum ada peringkat
- Scrotum: DR / Kamel Male Genital System / General Surgery Page1Dokumen52 halamanScrotum: DR / Kamel Male Genital System / General Surgery Page1Mahmoud AbouelsoudBelum ada peringkat
- OogenesisDokumen10 halamanOogenesisOm Prakash SinghBelum ada peringkat
- Human Digestive System ExplainedDokumen3 halamanHuman Digestive System ExplainedSana Shakeel100% (8)
- CNS Development and OrganizationDokumen6 halamanCNS Development and OrganizationKhamron BridgewaterBelum ada peringkat
- Types, locations, symptoms and treatment of uterine fibroidsDokumen4 halamanTypes, locations, symptoms and treatment of uterine fibroidsRomeo ReyesBelum ada peringkat
- LIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionDari EverandLIT: Life Ignition Tools: Use Nature's Playbook to Energize Your Brain, Spark Ideas, and Ignite ActionPenilaian: 4 dari 5 bintang4/5 (402)
- Mindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessDari EverandMindset by Carol S. Dweck - Book Summary: The New Psychology of SuccessPenilaian: 4.5 dari 5 bintang4.5/5 (327)
- The Age of Magical Overthinking: Notes on Modern IrrationalityDari EverandThe Age of Magical Overthinking: Notes on Modern IrrationalityPenilaian: 4 dari 5 bintang4/5 (13)
- The Ultimate Guide To Memory Improvement TechniquesDari EverandThe Ultimate Guide To Memory Improvement TechniquesPenilaian: 5 dari 5 bintang5/5 (34)
- Techniques Exercises And Tricks For Memory ImprovementDari EverandTechniques Exercises And Tricks For Memory ImprovementPenilaian: 4.5 dari 5 bintang4.5/5 (40)
- The Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsDari EverandThe Ritual Effect: From Habit to Ritual, Harness the Surprising Power of Everyday ActionsPenilaian: 3.5 dari 5 bintang3.5/5 (3)
- Think This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeDari EverandThink This, Not That: 12 Mindshifts to Breakthrough Limiting Beliefs and Become Who You Were Born to BeBelum ada peringkat
- The Comfort of Crows: A Backyard YearDari EverandThe Comfort of Crows: A Backyard YearPenilaian: 4.5 dari 5 bintang4.5/5 (23)
- Summary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedDari EverandSummary: The Psychology of Money: Timeless Lessons on Wealth, Greed, and Happiness by Morgan Housel: Key Takeaways, Summary & Analysis IncludedPenilaian: 5 dari 5 bintang5/5 (78)
- Outlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisDari EverandOutlive: The Science and Art of Longevity by Peter Attia: Key Takeaways, Summary & AnalysisPenilaian: 4 dari 5 bintang4/5 (1)
- Why We Die: The New Science of Aging and the Quest for ImmortalityDari EverandWhy We Die: The New Science of Aging and the Quest for ImmortalityPenilaian: 3.5 dari 5 bintang3.5/5 (2)
- Raising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsDari EverandRaising Mentally Strong Kids: How to Combine the Power of Neuroscience with Love and Logic to Grow Confident, Kind, Responsible, and Resilient Children and Young AdultsBelum ada peringkat
- The Obesity Code: Unlocking the Secrets of Weight LossDari EverandThe Obesity Code: Unlocking the Secrets of Weight LossPenilaian: 5 dari 5 bintang5/5 (3)
- The Happiness Trap: How to Stop Struggling and Start LivingDari EverandThe Happiness Trap: How to Stop Struggling and Start LivingPenilaian: 4 dari 5 bintang4/5 (1)
- Roxane Gay & Everand Originals: My Year of Psychedelics: Lessons on Better LivingDari EverandRoxane Gay & Everand Originals: My Year of Psychedelics: Lessons on Better LivingPenilaian: 5 dari 5 bintang5/5 (4)
- Roxane Gay & Everand Originals: My Year of Psychedelics: Lessons on Better LivingDari EverandRoxane Gay & Everand Originals: My Year of Psychedelics: Lessons on Better LivingPenilaian: 3.5 dari 5 bintang3.5/5 (32)
- Raising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsDari EverandRaising Good Humans: A Mindful Guide to Breaking the Cycle of Reactive Parenting and Raising Kind, Confident KidsPenilaian: 4.5 dari 5 bintang4.5/5 (169)
- The Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaDari EverandThe Body Keeps the Score by Bessel Van der Kolk, M.D. - Book Summary: Brain, Mind, and Body in the Healing of TraumaPenilaian: 4.5 dari 5 bintang4.5/5 (266)
- The Garden Within: Where the War with Your Emotions Ends and Your Most Powerful Life BeginsDari EverandThe Garden Within: Where the War with Your Emotions Ends and Your Most Powerful Life BeginsBelum ada peringkat
- Summary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisDari EverandSummary: Outlive: The Science and Art of Longevity by Peter Attia MD, With Bill Gifford: Key Takeaways, Summary & AnalysisPenilaian: 4.5 dari 5 bintang4.5/5 (41)
- The Tennis Partner: A Doctor's Story of Friendship and LossDari EverandThe Tennis Partner: A Doctor's Story of Friendship and LossPenilaian: 4.5 dari 5 bintang4.5/5 (4)
- Summary: It Didn't Start with You: How Inherited Family Trauma Shapes Who We Are and How to End the Cycle By Mark Wolynn: Key Takeaways, Summary & AnalysisDari EverandSummary: It Didn't Start with You: How Inherited Family Trauma Shapes Who We Are and How to End the Cycle By Mark Wolynn: Key Takeaways, Summary & AnalysisPenilaian: 5 dari 5 bintang5/5 (3)
- Dark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Dari EverandDark Psychology & Manipulation: Discover How To Analyze People and Master Human Behaviour Using Emotional Influence Techniques, Body Language Secrets, Covert NLP, Speed Reading, and Hypnosis.Penilaian: 4.5 dari 5 bintang4.5/5 (110)
- Summary: Limitless: Upgrade Your Brain, Learn Anything Faster, and Unlock Your Exceptional Life By Jim Kwik: Key Takeaways, Summary and AnalysisDari EverandSummary: Limitless: Upgrade Your Brain, Learn Anything Faster, and Unlock Your Exceptional Life By Jim Kwik: Key Takeaways, Summary and AnalysisPenilaian: 5 dari 5 bintang5/5 (8)