Article34015028 PDF
Diunggah oleh
Justine May GervacioJudul Asli
Hak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Article34015028 PDF
Diunggah oleh
Justine May GervacioHak Cipta:
Format Tersedia
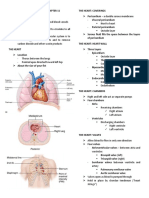
Flash Pulmonary Edema in Patients
with Chronic Kidney Disease and Continuing Nursing
Education
End Stage Renal Disease
Carol M. Headley
Barry M. Wall
lash pulmonary edema and
F acute pulmonary edema are
terms used to define the sudden
development of respiratory dis-
tress related to the rapid accumula-
tion of fluid within the lung intersti-
Flash pulmonary edema, also termed acute onset pulmonary edema, is characterized by the
sudden onset of respiratory distress related to accumulation of fluid in the lung interstitium
over a matter of minutes or hours. Chronic kidney disease is often associated with predis-
posing cardiac risk factors that make patients susceptible to development of flash pulmonary
tium secondary to elevated cardiac edema. This article highlights the connection between cardiac pathologies found in chronic
filling pressures (Little, & Braunwald, kidney disease and development of flash pulmonary edema. Nephrology nurses may be instru-
1997). For the purposes of this review, mental in reducing the risk of flash pulmonary edema by recognizing symptoms of heart fail-
flash pulmonary edema will be the ure and need for treatment of acute elevations in blood pressure.
term used. One of the first studies to
describe its occurrence linked its
development to individuals with pre-
existing coronary artery disease and Goal
hypertension (Lee, Cabin, & Francis, Recognize the risk for development of flash pulmonary edema in patients with
1988). The connection between flash chronic kidney disease and ESRD.
pulmonary edema and kidney disease
was initially described in individuals Objectives
with bilateral renal artery stenosis 1. Identify causes of flash pulmonary edema that may occur in conjunction
(Pickering et al., 1988). This associa- with chronic kidney disease and ESRD
tion has been so well characterized 2. Recognize signs and symptoms of flash pulmonary edema.
that the recommendation has been 3. Describe nursing measures that may avert development of flash pulmonary
made that anyone presenting with edema in individuals with advanced chronic kidney disease.
flash pulmonary edema be consid-
ered for evaluation for renal artery
stenosis (Missouris, Belli, &
MacGregor, 2000).
The risk for flash pulmonary tenance dialysis. The sudden onset of the past decade (Foley, Parfrey, &
edema in individuals with chronic pulmonary edema may be assumed Samak, 1998). Kidney disease is now
kidney disease (CKD), primarily end to be from excessive interdialytic known to be an independent risk fac-
stage renal disease (ESRD), has been weight gain, inaccurate dry weight tor for cardiovascular morbidity and
under emphasized in the literature. prescription, or weight scale malfunc- mortality (Levey et al., 1998; Sarnak
There are several possible explana- tions rather than from a cardiogenic et al., 2003). This article will define
tions for the lack of reports describing origin. Furthermore, treatment is flash pulmonary edema and factors
an association between flash pul- often readily available and imple- for its development, emphasizing the
monary edema and CKD, especially mented (ultrafiltration), thus the prob- relationship between cardiovascular
in patients with CKD receiving main- lem is promptly treated. disease and chronic kidney disease.
The strong association between Lastly, a case study of a patient on
cardiovascular disease and kidney hemodialysis that developed flash
Carol M. Headley, DNSc, RN, CNN, is
Nephrology Advanced Practice Nurse at The VA disease has been emphasized during pulmonary edema will be presented.
Medical Center, Memphis, TN. She is ANNAs
National Program chairperson and a member of
ANNAs Memphis Blues Chapter. This offering for 1.5 contact hours is being provided by the American Nephrology Nurses
Association (ANNA).
Barry M. Wall, MD, is Professor of Medicine at ANNA is accredited as a provider of continuing nursing education (CNE) by the American Nurses
The University of Tennessee Health Science Center, Credentialing Centers Commission on Accreditation.
Memphis, TN, and Nephrology, Associate Chief at
The VA Medical Center, Memphis, TN.
ANNA is a provider approved by the California Board of Registered Nursing, provider number CEP
00910.
Note: The authors reported no actual or potential The Nephrology Nursing Certification Commission (NNCC) requires 60 contact hours for each
conflict of interest in relation to this continuing recertification period for all nephrology nurses. Forty-five of these 60 hours must be specific to nephrology
nursing education article. nursing practice. This CNE article may be applied to the 45 required contact hours in nephrology nursing.
NEPHROLOGY NURSING JOURNAL January-February 2007 Vol. 34, No. 1 15
Flash Pulmonary Edema in Patients with Chronic Kidney Disease and End Stage Renal Disease
Figure 1 increased left atrial filling pressure
Starling Equation (Hanley & Welsh, 2004). In this type
of pulmonary edema, the rate of
Q = K[(Pmv-Ppmv)-(mv-pmv)] fluid accumulation within the lungs
is mainly dependent upon the func-
Q net transvascular flow of fluid tional capacity of the lymphatic sys-
K membrane permeability tem of the lungs to remove fluid
Pmv hydraulic pressure in the microvessels from the interstitium and alveoli
Ppmv hydrostatic pressure in the perimicrovascular interstitium
mv plasma protein osmotic pressure in the circulation
(Mason et al., 2005). As left atrial
pmv protein osmotic pressure in the perimicrovascular interstitium pressure rises, pulmonary capillary
pressures increase resulting in pro-
Note: From Staub, N.C.(1974). Pulmonary edema. Physiology Review, 54(3), page 680. tein poor fluid (edema) being forced
into the lung interstitium and alveoli.
Consequently, there is a progressive
deterioration in alveolar gas
Pathogenesis of Pulmonary and interstitial fluid oncotic pressures, exchange resulting in hypoxemia
Edema and the pressure differential across and symptoms of respiratory dis-
the capillary wall). Normally, the tress. Compensatory changes may
Edema has been described as alveolar bed within the lung serves to occur in individuals with chronically
increased volume within several protect the lung from fluid accumula- elevated left atrial pressures and per-
spaces of the body including the tion. Alveoli have very low perme- sistently elevated pulmonary capil-
blood vessels (increase in blood vol- ability for fluid and protein. Any fluid lary wedge pressures (greater than 18
ume), the lungs (pulmonary intersti- filtered into the alveoli is continuous- mmHg). In this circumstance, the
tium and alveoli), the trunk and lower ly absorbed back into the interstitium lymphatic system of the lungs
extremities (peripheral edema), as by the alveolar epithelial cells and becomes more efficient at removing
well as cavities within the abdomen drained away from the pulmonary fluid, thus reducing the likelihood for
and lungs (i.e., pleural effusions and interstitium by lymphatic vessels development of edema. It is the sud-
ascites). Peripheral edema is most evi- (Gluecker et al., 1999). den or acute elevations in left atrial
dent in the lower extremities because Non-cardiogenic pulmonary edema pressures that are more likely to
of the effect of gravity. The occur- occurs as a result of fluid accumula- result in acute pulmonary edema
rence of peripheral edema in patients tion in the alveoli resulting from a (Fraser, Mller, Colman, & Par,
with CKD may be attributed to either disruption in Starlings forces sec- 1999; Little, & Braunwald, 1997).
heavy proteinuria (over 3.5 grams ondary to increased capillary perme- It may be difficult to differentiate
termed nephrotic syndrome) or ability. The most common cause of between flash pulmonary edema and
advanced deterioration in kidney non-cardiogenic pulmonary edema is non-cardiogenic pulmonary edema
function (Bickley, Hoekelman, & acute lung injury (ALI) or acute res- since the presenting symptoms are
Bates, 1999). Pulmonary edema piratory distress syndrome (ARDS) often the same (Hanley & Welsh,
results from fluid accumulation in the associated with increased pulmonary 2004). Symptoms typically consist of
lungs at a higher rate than can be capillary permeability. Most often, dyspnea, tachypnea, and cough with
removed. The type of abnormality the concentration of protein within possible expectoration of frothy
expressed in the Starling equation the pulmonary interstitium exceeds edema fluid. The patient history and
(Figure 1) differentiates the type of 60% of the plasma protein value as determination of the factors that led
pulmonary edema.. It can predict the compared to less than 45% in cardio- to the development of the pul-
net flow of fluid across a membrane genic pulmonary edema (Hanley & monary edema becomes a priority
based upon permeability, surface Welsh, 2004). Non-cardiogenic pul- for diagnosis. Non-cardiogenic pul-
area, and hydraulic pressures (Hanley monary edema is diagnosed when monary edema is less common and
& Welsh, 2004). there is radiographic evidence of is primarily seen in individuals that
Pulmonary edema has been classi- alveolar fluid accumulation without have had recent pneumonia, sepsis,
fied into two categories dependent an elevation in the pulmonary wedge tumor, pulmonary fibrosis, trauma
upon the underlying cause: cardio- pressure greater than 18 mmHg or with multiple blood transfusions, fol-
genic and non-cardiogenic (Hanley & evidence of congestive heart failure lowing lung transplantation or resul-
Welsh, 2004). Starling forces identi- (CHF) on physical examination tant from aspiration of gastric con-
fied in the equation affect the fluid (Mason, Broaddus, Murray, & Nadel, tents.
balance between the interstitium and 2005).
the vascular bed within the lungs Cardiogenic pulmonary edema is
(capillary permeability, capillary sur- the most common type of pul-
Flash Pulmonary Edema
face area, capillary and interstitial monary edema and results from Flash pulmonary edema can origi-
fluid hydraulic pressures, capillary
16 NEPHROLOGY NURSING JOURNAL January-February 2007 Vol. 34, No. 1
nate from cardiogenic (i.e., cardiac Figure 2
dysfunction) and non-cardiogrenic Neurohormonal Responses in Heart Failure
causes (i.e., neurogenic pulmonary
edema) and occurs suddenly over a
period of minutes to hours (Lee, et al.,
1988). The syndrome of congestive Impairment
heart failure is the most common eti- in Left
Ventricular
ology for the development of flash Function
pulmonary edema. Traditionally, the
diagnosis of congestive heart failure
has been attributed to the presence of
myocardial systolic dysfunction, Reduction
defined as a disorder of myocardial in Cardiac
contractility leading to a reduced ejec- Output
tion fraction. Chronic systolic dys-
function results in a systemic process, Sympathetic
not solely confined to the heart Nervous
(Torre-Amione, 2005). Congestive System
heart failure is a multisystem disorder Increased
Oxygen
affecting the heart, skeletal muscle, Demands
kidneys, and nervous system pat- Chronic
Neurohormonal Natriuretic
terned by a complex neurohormonal Activation Peptides
process. Figure 2 depicts a simplified Increased Natriuresis &
version of the process. Neuro- RAAS Preload & Vasodilatation.
hormonal activation is key to the pro- Vasoconstriction Afterload
gressive nature of chronic heart fail- and
ure whereas flash pulmonary edema Salt & Water
occurs quickly and is primarily Retention
dependent upon a pre-existing condi-
tion (i.e., diastolic dysfunction) cou-
pled with an acute stressor (i.e., rise in Cardiac Remodeling
blood pressure). Further Heart
Chronic heart failure has been a Failure
challenge to treat because of its com- Myocyte Apoptosis,
plexity and its insidious character. Hypertrophy, Focal
Initially, neurohormonal changes pre- Myocardial Necrosis
sent in chronic heart failure are com-
pensatory and temporarily improve
cardiac output. These however, even-
tually become deleterious. Stimu-
lation of the sympathetic nervous sys-
tem is one of the earliest neurohor-
monal responses and initially pro- nervous systems becomes maladap- logic data has determined that 40% -
vides improved inotropic support to tive by contributing to cardiac 50% of patients presenting with con-
increase cardiac output. Stimulation myocyte apoptosis (programmed cell gestive heart failure have diastolic
of the renin-angiotensin-aldosterone death), hypertrophy, and focal dysfunction as the predominant etiol-
system (RAAS) causes release of myocardial necrosis ( Jackson et al., ogy. The diagnosis of diastolic heart
renin, plasma angiotensin II, and 2000). failure is made based upon the exis-
aldosterone. Angiotensin II causes Diastolic dysfunction, defined as a tence of heart failure in patients with
vasoconstriction of the efferent arteri- disorder of myocardial relaxation normal systolic function (left ventricu-
oles and the systemic circulation and resulting in impaired ventricular fill- lar ejection fraction of 50% or greater)
increased adrenal secretion of aldos- ing, may also result in the syndrome and no evidence of valvular or peri-
terone that results in sodium and of congestive heart failure. Diastolic cardial disease (Vasan, Benjamin, &
water retention by the kidneys heart failure is diagnosed when ele- Levy 1995). Some individuals will
( Jackson, Gibbs, Davies, & Lip, vated filling pressures are necessary have evidence of both systolic and
2000). However, long-term stimula- to achieve normal ventricular filling diastolic heart failure contributing to
tion of the RAAS and sympathetic (Grossman 2000). Recent epidemio- development of flash pulmonary
NEPHROLOGY NURSING JOURNAL January-February 2007 Vol. 34, No. 1 17
Flash Pulmonary Edema in Patients with Chronic Kidney Disease and End Stage Renal Disease
edema. However, diastolic heart fail- phy using color Doppler imaging dur- episodes of diastolic dysfunction and
ure occurs more frequently in patients ing the acute phase of pulmonary systolic dysfunction (Mansoor et al.,
with preserved systolic function, thus edema with a follow up exam per- 2001). Systolic dysfunction occurs
it has been attributed primarily to the formed 2-3 days later. The left ven- when there is less forward movement
disorder of diastolic dysfunction tricular ejection fraction during the of blood from the heart prompting an
(Gandhi et al., 2001). acute episode was similar to the mea- increase in diastolic volume and dias-
Although diastole involves the surement obtained 2- 3 days after pre- tolic pressure precipitating pul-
process of cardiac relaxation, active sentation (N = 30). Thus, a normal monary vascular congestion leading
energy requiring processes occur dur- left ventricular ejection fraction in a to pulmonary edema. In diastolic
ing this phase. The changes in cardiac patient with co-existing hypertension heart failure, the myocardium is less
pressure that occur during diastole and flash pulmonary edema suggests compliant, such that the left ventricle
are the result of isovolumetric relax- that the pulmonary edema is due to is unable to accept an adequate vol-
ation from the time of the aortic valve diastolic dysfunction. Transient sys- ume of blood from the venous system
closure to mitral valve opening; early tolic dysfunction and severe mitral and to fill at normal low pressures
rapid filling after mitral valve open- regurgitation were found to be infre- (Beattie, 2000). The net result is a rise
ing; and low blood flow during mid- quent causes for development of flash in diastolic pressures in order to pro-
diastole; and lastly late filling (high pulmonary edema (Gandhi et al., vide adequate ventricular filling.
blood flow) from atrial contraction. In 2001) Heart failure resulting from diastolic
diastolic heart failure, the left ventri- Other clinical conditions that have dysfunction occurs when elevated fill-
cle is stiff (reduced elastic recoil) with been identified as contributing to the ing pressures are necessary to achieve
impaired relaxation causing a reduc- development of flash pulmonary normal ventricular filling (Grossman,
tion in filling. Higher diastolic pres- edema include: a) myocardial 2000). The increased resistance to
sures are required to maintain ade- ischemia, b) acute aortic insufficiency, diastolic ventricular filling is most
quate ventricular filling (Redfield, c) acute mitral regurgitation, d) mitral commonly due to myocardial abnor-
2004). stenosis, and e) renovascular hyper- malities (myocardial hypertrophy,
The literature has shown a strong tension (Walker, Walker, & Nielsen, fibrosis, ischemia, or cardiomyopa-
association between hypertension 2001), but this paper will primarily thy), and less commonly to mechani-
and development of diastolic heart focus on diastolic heart failure as it cal abnormalities like mitral stenosis
failure, as well as a strong association relates to development of flash pul- or constrictive pericarditis (Hanley &
with development of flash pulmonary monary edema because diastolic Welsh, 2004).
edema. One study described the pres- heart failure has received less atten- Hypertension is frequently pre-
ence of systolic hypertension (systolic tion and yet is believed to be highly sent in patients presenting with flash
arterial blood pressure greater than prevalent. pulmonary edema. Chronic hyper-
160 mmHg) in 85% of patients pre- tension that is poorly controlled can
senting to hospital emergency rooms Cardiac Disease result in development of systolic and
with flash pulmonary edema diastolic dysfunction that may predis-
(Kramer, Kirkman, Kitzman, & Little, Flash pulmonary edema occurs as pose patients to the development of
2000). Studies that performed a consequence of a disruption in the flash pulmonary edema (Mansoor et
Doppler echocardiography after the normal pressure-volume relationship al., 2001). Even labile elevations in
acute episode found preserved sys- during the cardiac cycle. Ischemic blood pressures of patients with bilat-
tolic function (left ventricular ejection heart disease/coronary artery disease eral renal artery stenosis have been
fraction of 50% or greater) in the has been linked with development of shown to be associated with an
majority of patients presenting with flash pulmonary edema. Acute increased risk for development of
flash pulmonary edema. Even though myocardial ischemia has been shown flash pulmonary edema (Bloch, Trost,
systolic function was assessed as nor- to cause systolic and diastolic dys- Pickering, & Sos, 1999). As noted by
mal, the evaluation was obtained after function. Cocaine abuse has been Vasan & Levy (1996) long standing
treatment of the hypertensive episode associated with development of flash hypertension is a primary predeces-
and resolution of the pulmonary pulmonary edema for multiple rea- sor to development of left ventricular
edema, thus the presence of transient sons including its precipitation of hypertrophy (LVH). Hypertension
systolic dysfunction as a precipitating myocardial ischemia (coronary artery leads to remodeling and augmenta-
cause could not be excluded vasoconstriction), acute rise in blood tion of the left ventricular mass that
(Mansoor, Shah, & Scoble, 2001). The pressure (peripheral vasoconstric- can result in diastolic dysfunction,
primary cause for flash pulmonary tion), and development of systolic as systolic dysfunction, or both.
edema, systolic versus diastolic heart well as diastolic dysfunction (Lange & However, it is important to realize
failure, was addressed in a study that Hillis, 2001). that not everyone with LVH will
examined patients with two-dimen- The existence of coronary artery develop heart failure. Athletes some-
sional transthoracic echocardiogra- disease can cause intermittent times acquire what is called physio-
18 NEPHROLOGY NURSING JOURNAL January-February 2007 Vol. 34, No. 1
logic hypertrophy of the left ventricle Table 1
and maintain near or near-normal Prevalence of Risk Factors: Diastolic Heart Failure in CKD
exercise tolerance. Therefore, LVH
by itself does not constitute cardiac Risk Prevalence References
dysfunction (Lorell & Carabello, Hypertension 50% - 75% NKF, 2005
2000). LVH 75% - Beginning dialysis Levin, 2003
Age Average age of dialysis USRDS, 2005
Renal Artery Stenosis and Flash patient 63 years
Pulmonary Edema Ischemic heart disease 35% - CKD Levin, 2003
Renal artery stenosis (RAS) may 40% - Beginning dialysis
be identified in individuals with Heart failure 37% Foley et al., 1994
apparent normal kidney function as
well as those with a diagnosis of acute
or chronic kidney disease (Missouris,
Belli, & MacGregor, 2000). Renal malignant hypertension (Harding et has been associated with the develop-
artery stenosis (narrowing of the renal al., 1992). Renovascular hypertension ment of flash pulmonary edema
artery) is most often a result of ather- related to bilateral renal artery steno- (Ware & Matthay, 2005). This discus-
osclerosis. Fibromuscular dysplasia, is sis is strongly associated with the sion will primarily highlight the
a rare idiopathic condition in which development of flash pulmonary pathology of diastolic heart failure. A
there is an increase in the number of edema. The combination of hyper- relationship between the risk for dias-
cells in the renal artery cell wall tension and volume retention, occur- tolic heart failure in the presence of
resulting in arterial narrowing. ring as a consequence of altered kidney disease can be established by
Atherosclerotic lesions result from the intrarenal hemodynamics and aldos- examining the contributing factors
deposition of plaque within the renal terone-mediated salt and water reten- that precede there development
artery and are most often seen in indi- tion are the major contributing factos (Figure 3). Diastolic heart failure can
viduals over the age of 55, while to the development of flash pul- be caused by ischemia, left ventricu-
fibromuscular dysplasia is usually monary edema with bilateral renal lar hypertrophy (LVH), increased fill-
seen in young women. Women with artery stenosis. In contrast pulmonary ing pressures related to chronically
fibromuscular dysplasia associated edema is relatively uncommon with elevated blood pressures, infiltrative
RAS almost invariably have hyper- unilateral renal artery stenosis cardiomyopathies, ischemic heart dis-
tension. Lesions associated with fibro- (Basaria & Fred, 2002; Jaff, 2001). ease, pericarditis, the normal aging
muscular dysplasia tend to show a Unilateral renal artery stenosis leads processes, chemotherapy and genetic
much more favorable response to to renin dependent hypertension, but anomalies (Beattie, 2000; Kramer et
percutaneous transluminal angioplas- not to volume expansion, since the al., 2000; Zile & Simsic, 2000). In the
ty (PTA), stent or surgery than athero- non-affected kidney undergoes a general population, 50% of people
sclerotic lesions (Olin, 2004). pressure natriuresis/diuresis, which over the age of 70 with a diagnosis of
The most common type of RAS prevents volume expansion making congestive heart failure will have pre-
involves atherosclerotic deposition in pulmonary edema less likely to occur served systolic function and classified
the artery lumen that disrupts blood (Missouris et al., 2000). as having diastolic heart failure. For
flow to the kidney parenchyma caus- those 10 years younger (60 years of
ing ischemia. The kidney responds by Flash Pulmonary Edema and age) with congestive heart failure
secreting renin into the bloodstream, symptoms, only 15% will have dias-
leading to the production of
Kidney Disease tolic heart failure. Age also con-
angiotensin II, which is both a potent Many of the precipitating factors tributes to mortality risk. Overall,
vasoconstrictor and a major stimulus associated with development of flash prognosis is better for diastolic heart
for adrenal secretion of aldosterone pulmonary edema are frequently pre- failure (average mortality rate 5 % -
(Safian & Textor, 2001). Hypertension sent in patients with advanced stages 8%) than for systolic heart failure
resulting from activation of the RAAS of CKD (Table 1). Cardiovascular dis- (average mortality rate 10% - 15%),
is referred to as renovascular hyper- ease and CKD are strongly linked. but diastolic heart failure in patients
tension. Mild to moderate hyperten- Recent findings indicate that patients over 70 years has a 50% 5-year mor-
sion is not commonly associated with with CKD are in the highest risk tality rate (Zile & Simsic, 2000). These
RAS; however, malignant and drug group for cardiovascular disease and changes are similar to disease report-
resistant hypertension carries a high that patients with CKD are more like- ed in the elderly, but they occur 15-20
degree of suspicion for RAS, having ly to die of cardiovascular disease years earlier in kidney disease
been diagnosed in up to a third of than ESRD (Levin, 2003). (Tozawa, Iseki, Iseki, & Takishita,
patients having difficult to control or Systolic and diastolic heart failure 2002; Churchill et al., 1992). Systolic
NEPHROLOGY NURSING JOURNAL January-February 2007 Vol. 34, No. 1 19
Flash Pulmonary Edema in Patients with Chronic Kidney Disease and End Stage Renal Disease
Figure 3 and diastolic heart failure are highly
Pathogenesis of Diastolic Heart Failure in CKD prevalent in patients with advanced
CKD (Foley et al., 1994).
Increasing emphasis has been
placed on the need to control blood
Decreased pressures in all stages of CKD. Since
Glomerular hypertension is both a cause and a
complication of CKD, prevalence
Filtration Rate rates are high. Elevated blood pres-
sure is a primary contributing factor
to development of LVH and heart
failure (both systolic and diastolic).
Lucas and colleagues (2003) found
Increased that systolic hypertension and
Extracellular increased pulse pressures are com-
mon at the time of dialysis initiation.
Fluid Volume All cause mortality was significantly
higher, 14.1 deaths per 100 patient-
years for patients with uncontrolled
hypertension (BP greater than 140/90
mmHg) compared to those that were
Hypertension normotensive, 7.9 deaths per 100
patient years (RR = 1.79, P = 0.01,
95% CI = 1.152.8.). Blood pressure
control remains poor even after
beginning renal replacement therapy.
Cardiac Reports indicate that blood pressure
Remodeling: control in patients receiving dialysis is
low with 40% 90% having blood
LVH pressures higher than the National
Kidney Foundations K-DOQI rec-
ommended goal of 140/90 pre-dialy-
sis (Chalmers et al., 1999; Dhakal,
Diastolic Sloand, & Schiff, 2000; Salem, 1995).
Coronary artery disease has also
Dysfunction been recognized as a contributing fac-
tor to development of flash pul-
monary edema. Chronically elevated
blood pressure results in stiff arteries
that have diffuse arteriosclerosis.
Acute Rise in Blood Pressure Murphy (2003) reports a coronary
artery disease prevalence rate of 40%
in patients beginning dialysis, 22%
have stable angina and 8% have his-
Increased Cardiac torical documentation of a previous
myocardial infarction.
Filling Pressures The diagnosis of flash pulmonary
edema is made using a compilation of
clinical findings (Mansoor, et al.,
2001). Initial evaluation should
Flash Pulmonary include a chest x-ray and Doppler
echocardiogram. Chest radiographs
Edema characteristically demonstrate enlarge-
ment of the peribronchovascular
spaces, prominent septal lines as well
as acinar areas of increased opacity
that coalesce into frank consolidations
20 NEPHROLOGY NURSING JOURNAL January-February 2007 Vol. 34, No. 1
(Ware & Matthay, 2005). It is often
difficult to differentiate between sys- Figure 4
tolic and diastolic heart failure based Transmitral Pressures used in Diagnosis of Diastolic Dysfunction
upon patient history, physical exam,
chest radiograph, and EKG. Doppler Normal E: A Ratio and Deceleration Time
echocardiography is the most com-
monly utilized technique to assess
both systolic and diastolic ventricular A Ventricular
function. Diastolic function involves E Early passive D filling produced by
both active and passive components. ventricular filling T atrial contraction
The active phase involves energy
dependent relaxation while the pas-
sive phase predominantly reflects the
Deceleration Time
viscoelastic properties of the heart tis-
sue.
Doppler echocardiography assess- Restrictive E:A Ratio and Deceleration Time
es both of these phases by examining
pressure changes during transmitral
flow (Figure 4) in diastole. Early dias- A Ventricular
tolic flow occurs when the mitral E Early passive filling produced by
valve initially opens at the onset of ventricular filling D atrial contraction
diastole. The E wave determined by T
Doppler echocardiography serves as
an index of left ventricular relaxation, Deceleration Time
compliance, and atrial pressure. Early
passive ventricular filling is followed
by the ventricular filling produced by
atrial contraction (A wave). Deceler- Normal: 0.75 greater than E:A greater than 0.75, but less than 1.5 with DT 200
ation time (DT) is a measurement of 32 ms
the time it takes for passive filling. Mild Diastolic Dysfunction: E:A greater than or equal to 0.75 with DT greater
Deceleration time will shorten when than or equal to 230 ms
there is a decrease in left ventricular Moderate Diastolic Dysfunction ("Pseudonormal"): E:A greater than 0.75 but
less than 1.5 with DT greater than 140 ms
compliance however deceleration
Severe Diastolic Dysfunction: E:A greater than 1.5 with DT less than 160 ms
times are also affected by other
pathologies that increase the left atrial Adapted from: Haney, Sur, & Xu (2005). Diatsolic heart failure: A Review and
pressure and shorten DT. DT values Primary care perspective. Journal of the American Board of Family Practitioners,
over 240 ms indicate impaired relax- 18(3), 189-198.
ation, and under 150 ms indicate a
restrictive pattern (Gilbert, Connelly, invasive and can offer further support morphology. The radio isotope (tech-
Kelly, Pollock, & Krum, 2006). in determining the existence of dias- netium) is injected into a vein and
Interpretation of E:A ratios becomes tolic heart failure, especially when absorbed immediately by healthy tis-
more difficult when there are com- there is isolated maladaptive relax- sue. A gamma scintillation camera
bined pathologies of impaired relax- ation of the ventricles. detects the gamma rays emitted by
ation and restriction, then both left If the Doppler echocardiogram is the radio isotope. If the patients heart
atrial and ventricular pressures non-conclusive or technically inade- is normal, the technetium will be
increase leading to an increase in the quate due to a poor acoustic window, readily and evenly distributed in the
magnitude of the E wave resulting in as often occurs in patients with an cardiac images. An uneven distribu-
a normal E:A ratio (pseudonormal abnormal body habitus, then a multi- tion of technetium in the heart may
pattern) which can be unmasked by ple-gated acquisition (MUGA) scan be indicative of coronary artery dis-
maneuvers that alter cardiac preload otherwise known as a cardiac blood ease, cardiomyopathy, or blood
such as the Valsalva maneuver or pool scan may be required. This scan shunting within the heart. Use of the
administration of nitroprusside uses a radioactive isotope to evaluate gamma scintillation camera exposes
(Angeja & Grossman, 2003). Even ventricular function and detect abnor- the patient to about the same amount
though there are problems with inter- malities in the heart wall (Logeart et of radiation as a chest x-ray
pretation of E:A ratios, transmitral al., 2002). The MUGA is more accu- (Youngerman-Cole, 2005).
inflow patterns obtained with rate at calculating ejection fraction, Even though rarely done, the gold
Doppler echocardiography are non- but less efficient at identifying valve standard for the diagnosis of diastolic
NEPHROLOGY NURSING JOURNAL January-February 2007 Vol. 34, No. 1 21
Flash Pulmonary Edema in Patients with Chronic Kidney Disease and End Stage Renal Disease
heart failure continues to be cardiac tive value, greater than 90%) (Silver et sent, then associated with long-
catheterization allowing direct mea- al., 2004). Intermediate levels of BNP, standing volume expansion
surement of volumes and pressures, between 100 and 500 pg /mL had less (Mason, Broaddus, Murray, &
but at significantly higher cost and diagnostic discrimination. BNP levels Nadel, 2005).
risk (Gutierrex & Blanchard, 2004). It may be elevated in critically ill
is usually not necessary to determine patients, even in the absence of heart Flash Pulmonary Edema: A Case
the etiology for the heart failure since failure; however, BNP levels less Presentation
Doppler echocardiogram or MUGA than100 pg/ml continue to be useful
usually provide adequate diagnostic in excluding heart failure in these A 54-year-old male presented to
criteria. Pulmonary artery catheteriza- patients. BNP levels are also elevated the dialysis unit of an acute care hos-
tion can also be done and has an in patients with chronic kidney dis- pital due to inadvertent dislodgement
adverse event rate of 4.5% - 9.5%, but ease, such that a cut off level below of his tunneled venous catheter. He
it is much more precise in defining 200 pg/mL has been suggested to had been receiving chronic hemodial-
the presence of diastolic heart failure exclude heart failure when the esti- ysis for 3 years at the time of presen-
than MUGA or Doppler echocardio- mated glomerular filtration rate is tation and was oliguric. Arrange-
gram alone. If the pulmonary artery below 60 mL per minute. Chronic ele- ments were made with the interven-
occlusion pressure is greater than 18 vations in BNP may also be a hall- tional radiology department to have
mm Hg then cardiogenic pulmonary mark of patients with or at risk for this catheter removed and a new
edema exists (Harvey et al., 2005). diastolic heart failure among subjects catheter placed. He had undergone
Laboratory testing in flash pul- with preserved systolic function, inde- hemodialysis at the community dialy-
monary edema typically may include pendent of the degree of left ventricu- sis center 48 hours prior to his pre-
measurement of plasma levels of tro- lar hypertrophy (Yamaguchi et al., sentation.
ponins and brain natriuretic peptide 2004). There was no evidence of car-
(BNP). Troponin I elevation in the diopulmonary compromise on admis-
presence of kidney failure has Symptoms of Flash Pulmonary sion and he was able to ambulate to
demonstrated high prognostic value Edema the unit without difficulty. His blood
for acute coronary syndrome pressure was noticeably elevated and
(myocardial ischemia). Troponin T Complaints of severe cough and he reported holding his antihyperten-
elevation has not been recommended dyspnea are usually the primary sives that day in anticipation of
for detecting acute myocardial symptoms on presentation of flash undergoing hemodialysis. Holding
ischemia, but has been associated pulmonary edema with or without his antihypertensives on the day of
with increased mortality risk (Freda, chest discomfort. Common findings dialysis was a common practice. A
Tang, Van Lente, Peacock, & Francis, on physical examination include: chest radiograph was obtained prior
2002). In a recent study of 258 Tachypnea with use of acces- to sending the patient to intervention-
hemodialysis patients, elevations in sory muscles of breathing. al radiology to evaluate for any evi-
Troponin T (0.10 ng/mL or greater) Lung fields auscultation of dence of volume expansion since he
correlated significantly with the pres- crackles in bases and scattered would most likely miss his dialysis
ence of left ventricular hypertrophy throughout the lung fields, treatment that day (see Figure 5).
(Iliou et al., 2001). The rise and fall of rales or even decreased breath Physical examination on presenta-
Troponin I (trend) may be required to sounds. tion:
make a definitive diagnosis of acute Cardiac exam possible pres- Temperature: 97.8 F;
coronary syndrome since 1% -6% ence of an S3 indicating an Weight: 71 Kg (less than 2 kg
have been shown to have elevations increase in left ventricular end above present dry weight esti-
without symptoms (Freda et al., diastolic volume or an S4 gal- mate);
2002). lop coinciding with an increase Blood pressure: 165/116 HR
Elevations in brain natriuretic pep- in left atrial pressure, and a 89 (sitting); blood pressure
tide (BNP) have been routinely used new or changed murmur. 151/88 HR 86 (standing);
in the diagnosis of heart failure. When Jugular venous distension indi- No evidence of jugular venous
the ventricular wall stretches or there cating increased filling pres- distension;
is increased ventricular pressure, BNP sures. Cardiovascular exam: Regular
is secreted. A recent consensus panel Systolic Blood pressure may rhythm, rate 89/minute, I/VI
concluded that BNP levels below 100 be markedly elevated. Hypo- systolic murmur, - no pericar-
pg/mL indicate that heart failure is tension suggests left ventricular dial rub, no gallops;
unlikely (negative predictive value, systolic dysfunction and Lungs: Respirations were regu-
greater than 90%); while a BNP level impending cardiogenic shock. lar and unlabored, no tachyp-
greater than 500 pg/ml indicates that Peripheral edema usually nea noted, few scattered crack-
heart failure is likely (positive predic- without signs of edema, if pre- les in lung bases, otherwise
22 NEPHROLOGY NURSING JOURNAL January-February 2007 Vol. 34, No. 1
Figure 5
Standing Chest Radiograph AP Prior to Figure 6
Undergoing Catheter Replacement Portable Chest PA Radiograph 5 Hours Later
clear to auscultation; and The following findings were noted jugular vein with the tip in the
No peripheral edema present. upon his return to the dialysis unit. superior vena cava. The previ-
Past medical history was signifi- Temperature: 97.6 F; ously placed catheter had been
cant for: Blood pressure: 247/142 HR removed. There was diffuse
Coronary artery disease and 127 (sitting); bilateral pulmonary interstitial
myocardial infarction with Pulse oxygenation: 67 78% edema (see Figure 6);
coronary artery stent place- (room air); Serial Troponin I: 0.0 1.0
ment 8 months prior, Respiratory rate: 30/minute ng/mL over 24 hours (Range:
Long-standing hypertension, with use of accessory muscles; 0 0.6 no cardiac damage,
and Productive cough of frothy 0.7 1.5 non-diagnostic,
Hyperlipidemia. white sputum; greater than 1.5 Evidence of a
A 2-D Echocardiogram obtained 3 Jugular venous distention was myocardial infarction)
months earlier demonstrated: present; Other lab results included:
Diffuse hypokinesia of the left Cardiovascular exam- tachy- Platelets: 374 K/uL
ventricle, with an approximate cardia, II/VI systolic murmur, Na: 140 meq/dL
ejection fraction of 29%; loud S2, positive gallop Potassium: 4.4 meq/dL
Left ventricular diastolic dys- rhythm , no pericardial rub; HCO3: 39 meq/L
function; Lungs - decreased breath sounds BUN: 40 mg/dL
Mild eccentric left ventricular in lung bases; Creatinine: 9.8 mg/dL
hypertrophy; No peripheral edema noted; Glucose: 84 mg/dL
Trace tricuspid regurgitation; 12 Lead EKG Sinus tachy- Calcium: 10.8 mg/dL
and cardia with rate 127/minute, The treatment included:
No pericardial effusion. occasional premature ventricu- Oxygen by non-rebreather
The patient returned from the lar complexes, left atrial facemask at 60%;
interventional radiology department enlargement, left ventricular Nitroglycerin paste: 1 to
following catheter removal and place- hypertrophy and non-specific chest;
ment of a new cuffed hemodialysis ST segment changes; Labetalol: 20 mg IV over 2
catheter on a stretcher. He was noted Portable chest x-ray demon- minutes; and
to be in acute respiratory distress with strated a new dialysis catheter Acute hemodialysis with vol-
the head of the stretcher at 90. in place in the left internal ume removal.
NEPHROLOGY NURSING JOURNAL January-February 2007 Vol. 34, No. 1 23
Flash Pulmonary Edema in Patients with Chronic Kidney Disease and End Stage Renal Disease
Hemodialysis was initiated with during episodes of volume expansion. pressure and pulmonary edema
ultrafiltration of 3.5 liters over a 4- The routine practice of holding anti- through venous dilatation, but mor-
hour period. The patients blood pres- hypertensives prior to undergoing phine may also cause respiratory
sure improved, and he did not require hemodialysis in certain circumstances depression (Beattie, 2000). Lowering
endotrachial intubation. The oxygen may need to be reconsidered. The the blood pressure is a priority with
by non-rebreather facemask was practice of holding antihypertensives severely elevated blood pressures.
slowly weaned during dialysis to a is to avoid low blood pressures at the Labetalol is an effective antihyperten-
nasal cannula oxygen by the end of end of dialysis following volume sive to use in hypertensive crisis since
the dialysis treatment. He was admit- removal (Coomer, Schulman, Breyer, it can be given intravenously without
ted for observation and serial tro- & Shyr 1997). Blood pressures tend to renal adjustment (NHLBI, 2003). It
ponins to rule out myocardial infarc- normalize with the removal of can be given as a slow intravenous
tion, all of which were negative. He intravascular volume during the ultra- push starting at 20 mg over 2 min-
returned home after 24 hours with filtration process. It may be better to utes: additional 2 mg dosages can be
instructions to take his antihyperten- reduce rather than hold antihyperten- given every minute up to 300 mg
sive medications the night before dial- sives prior to dialysis to avoid such maximum dose to obtain a gradual
ysis to avoid the surge in blood pres- extremes in blood pressure (Sulkova reduction in blood pressure (NKF,
sure the morning prior to his & Valek, 1988). 2005). Lowering of the blood pres-
hemodialysis treatments. The immediate treatment of sure reduces cardiac filling pressures
patients with flash pulmonary edema and allows cardiac output to improve,
Nursing Implications is essentially the same as with any thus reducing fluid accumulation in
other type of pulmonary edema. the lungs. Additionally slowing of the
Pulmonary edema is a common Initial assessment should include heart rate will improve diastolic fill-
complication of patients with ESRD monitoring of hemodynamic parame- ing, thus improving stroke volume
(Evans, Reddan, & Szczech, 2004; ters and pulse oxymetry or arterial and cardiac output.
Shapiro, Deshetler, & Stockard, blood gases. Patients should be given Treatment of flash pulmonary
1994). Fluid and salt abuse has been oxygen. This oxygen support should edema is aimed at resolving the
reported to be the most common be provided by a non-rebreather face- immediate threat of respiratory dis-
cause of pulmonary edema in patients mask or by positive pressure ventila- tress and hypoxemia and eliminat-
receiving renal replacement therapy. tion. If the work of breathing (respira- ing/treating the underlying cause (i.e.,
How does one differentiate between tory rate greater than 30) and hypox- hypertensive crisis). Nurses assess
pulmonary edema that is associated ia is excessive (PaO2:FiO2 less than patients blood pressures pre-dialysis
with excessive fluid intake and car- 200) endotrachial intubation may be and post-dialysis, thus they are the
diogenic mediated flash (acute) pul- required (Antonelli et al., 2001). first to note changes that may place
monary edema? Pulmonary edema When hypertension is felt to be con- that patient at risk. If blood pressures
that occurs without significant interdi- tributory, obtaining immediate reduc- are assessed as above the recom-
alytic weight gain or evidence of tion in blood pressure is paramount. mended pre-dialysis reading of
peripheral edema on physical exami- Arrangement for acute dialysis with 140/90, then changes in the treatment
nation, particularly in association with ultrafiltration if the patient has regimen can be instituted. It may be
an elevation in blood pressure, already been receiving dialysis is necessary to reduce the estimated dry
strongly supports the diagnosis of most beneficial. weight to achieve a normalized pre-
flash pulmonary edema. Medications commonly used in dialysis pressure or additional antihy-
A history of ischemic heart dis- the treatment of flash pulmonary pertensives may be required. When
ease, poorly controlled hypertension, edema include a) nitroglycerin, b) hemodialysis is postponed or can-
and identification of left ventricular furosemide, and c) morphine sulfate. celed, then nurses need to remind
hypertrophy by Doppler echocardio- Nitroglycerin is a potent vasodilating patients to resume their antihyperten-
graphy may signify an increased risk drug which increases cardiac output sives in order to avoid blood pressure
for development of flash pulmonary while decreasing preload and after- extremes and risk of flash pulmonary
edema. Anemia and hypertension load. Nitroglycerin reduces pul- edema.
have been primarily associated with monary edema mainly through
the development of left ventricular venous dilatation. Patients receiving Conclusion
hypertrophy and are found in the dialysis who are oliguric or anuric
majority of patients beginning dialy- may have a mild venodilatory Patients with CKD are at risk for
sis. Poorly controlled hypertension in response to furosemide, but will not developing flash pulmonary edema.
the presence of a remodeled heart have an effective diuresis. The benefit Cardiovascular disease is highly
(i.e., LVH) may result in diastolic dys- of morphine in treatment of pul- prevalent in the kidney disease popu-
function which predisposes to the monary edema has remained contro- lation. Diastolic heart failure is often
development of pulmonary edema versial. Morphine will reduce blood unsuspected without clinical suspi-
24 NEPHROLOGY NURSING JOURNAL January-February 2007 Vol. 34, No. 1
cion since the presentation is similar York: Lippincott, Williams, and of the Chest (Volume III),
to that seen with systolic heart failure. Wilkins. Philadelphia: W. B. Saunders
The prevalence of LVH at the time Beattie, S. (2000). Heart failure with pre- Company.
patients begin dialysis increases the served LV function: Freda, A.U., Tang, B. J., Van Lente, W.H.,
Pathophysiology, clinical presenta- Peacock, W.F. & Francis, G. S. (2002).
likelihood of patients developing both
tion, treatment, and nursing implica- Cardiac troponins in renal insuffi-
systolic and diastolic dysfunction tions. The Journal of Cardiovascular ciency: Review and clinical implica-
which can lead to development of Nursing, 14(4), 24-37. tions. Journal of the American College of
flash pulmonary edema. The Bloch, M.J., Trost, D.W., Pickering, T.G., Cardiology, 40(12), 2065-2071.
National Kidney Foundation K- & Sos, T.A. (1999). Prevention of Gandhi, S.K., Powers, J.C., Nomeir, A.M.,
DOQI guidelines for cardiovascular recurrent pulmonary edema in Fowle, K., Kitzman, D., Rankin,
disease recommends that echocardio- patients with bilateral renovascular K.M. et al., (2001). The pathogenesis
grams be performed on all patients at disease through renal artery stent of acute pulmonary edema associat-
the initiation of dialysis and again placement. American Journal of ed with hypertension. New England
after achievement of prescribed dry Hyptertension, 12(1), 1-7. Journal of Medicine, 344(1), 17-21.
Chalmers, J. MacMahon, S., Mancia, G., Gilbert, R.E., Connelly, K., Kelly, D.J.,
weight and at 3 year intervals there-
Whitworth, J. Beilin, L., Hansson, L., Pollock, C.A., & Krum, H. (2006).
after (NKF, 2005). Nurses should et al., (1999). World Health Heart Failure and Nephropathy:
acknowledge and recommend treat- Organization-International Society Catastrophic and interrelated com-
ment of blood pressures that are of Hypertension Guidelines for the plications of diabetes. Clinical Journal
assessed to be elevated beyond the Management of hypertension. of the American Society of Nephrology,
current pre-dialysis blood pressure Guidelines sub-committee of the 1(2), 193-208.
recommendation of 140/90 pre-dialy- World Health Organization. Clinical Gluecker, T., Capasso, P., Schnyder, P.,
sis and 130/80 in the CKD popula- and Experimental Hypertension, 21(5-6), Gudinchet, F., Schaller, M.D.,
tion (NKF, 2005). Nurses are often 1009-1060. Revelly, J.P., et al., (1999). Clinical
the first to assess blood pressures in Churchill,D., Taylor, D., Cook, R., and Radiologic Features of Pulmonary
Laplante, P., Barre, P., Cartier, P., edema. Radiographics, 19(6), 1507-1531.
patients on dialysis and evaluate
Fay, W., Goldstein, M., Jindal, K., & Grossman, W. (2000). Defining diastolic
response to changes in therapy. Mandin, H. (1992). Canadian dysfunction. Circulation, 101(17),
Patients may institute better compli- Hemodialysis Morbidity Study. 2020-2021. Gutierrez, C. &
ance and demonstrate improvements American Journal of Kidney Disease, Blanchard, D. (2004). Diastolic heart
in blood pressure regulation with a 19(3), 214-234. failure: Challenges of diagnosis and
greater understanding of the inherent Coomer, R.W., Schulman, G., Breyer, treatment. American Family Physician,
risk. With the high preponderance of J.A., & Shyr, Y. (1997). Ambulatory 69(11), 2609-2616.
patients beginning dialysis with car- blood pressure monitoring in dialysis Haney, Sur, & Xu (2005). Diatsolic heart
diovascular disease, it is imperative patients and estimation of mean failure: A Review and Primary care
that clinicians make a more concerted interdialytic blood pressure. American perspective. Journal of the American
Journal of Kidney Disease, 29(5), 678- Board of Family Practitioners, 18(3),
effort in treating the risks for cardio-
685. 189-198.
vascular disease. Dhakal, M.P., Sloand, J.A., & Schiff, M.J. Hanley, M. & Welsh, C. (2004). Current
(2000). Prevalence of hypertension Diagnosis & Treatment in Pulmonary
References and adequacy of blood pressure con- Medicine. New York: McGraw-Hill.
Angeja, B.G. & Grossman, W. (2003). trol in hemodialysis patients. Dialysis Harding, M.B., Smith, L.R., Himmelstein,
Evaluation and management of dias- & Transplantation, 29(10), 628-637. S.I., Harrison, K., Phillips, H.R.,
tolic heart failure. Circulation, 107(5), Evans, K., Reddan, D.N., & Szczech, L.A. Schwab, S.J., et al.. (1992). Renal
657-663. (2004). Nondialytic management of Artery stenosis: Prevalence and asso-
Antonelli, M. Conti, G., Moro, M. L., hyperkalemia and pulmonary edema ciated risk factors in patients under-
Esquinas, A., Gonzalez-Diaz, G., among renal disease patients: an going routine cardiac catheterization.
Confalonieri, M. et al., (2001). evaluation of the evidence. Seminars Journal of the American Society of
Predictors of failure of noninvasive in Dialysis, 17(1), 22-29. Nephrology, 2(11), 1608-1616.
positive pressure ventilation in Foley, R., Parfrey, P., Hefferton, D., Kent, Harvey, S., Harrison, D.A., Singer, M.,
patients with acute hypoxemic respi- G., Murray, D., & Barre, P. (1994). Ashcroft, J., Jones, C.M., Elbourne,
ratory failure: A multi-center study. Advance prediction of early death in D. et al.,. (2005). Assessment of the
Intensive Care Medicine, 27(11) 1718- patients starting maintenance dialy- clinical effectiveness of pulmonary
1728. sis. American Journal of Kidney Disease, artery catheters in management of
Basaria, S., & Fred, H L. (2002). Images in 23(6), 836-845. patients in intensive care: A random-
cardiovascular medicine. Flash pul- Foley, R.N., Parfrey, P., & Samak, M.J. ized controlled trial. Lancet,
monary edema heralding renal (1998). Clinical epidemiology of car- 366(9484), 435-436.
artery stenosis. Circulation, 105(7), diovascular disease in chronic renal Iliou, M. C., Gumeron, C., Benoit, M. O.,
899. failure. American Journal of Kidney Tuppin, P. Courvoisier, C. L.,
Bickley, L.S., Hoekelman, R.A., & Bates, Disease, 32(5 suppl), S112-S119. Calonge, V. M., et al.,. (2001).
B. (1999). A guide to physical examina- Fraser, R.S., Mller, N.L., Colman, N., & Chronic hemodialysis and new car-
tion and history taking. (7th ed.). New Par, P.D. (1999). Diagnosis of Diseases diac markers evaluation (CHANCE)
NEPHROLOGY NURSING JOURNAL January-February 2007 Vol. 34, No. 1 25
Flash Pulmonary Edema in Patients with Chronic Kidney Disease and End Stage Renal Disease
study. Nephrology, Dialysis & hemodialysis patients. American Safian, R.D., & Textor, S.C. (2001). Renal-
Transplantation, 16(7), 1452-1458. Journal of Kidney Disease, 41(4), 814- artery stenosis. New England Journal of
Jackson, G., Gibbs, C. R., Davies, M. K., 821. Medicine, 344(6), 431-442.
& Lip, G. Y. (2000). ABC of heart Mansoor, S. Shah, A., & Scoble, J.E. Shapiro, R.S., Deshetler, N., & Stockard,
failure pathophysiology. British (2001). Flash pulmonary edema: A H. E.(1994). Fluid overload again: A
Medical Journal, 320(7228), 167-170. diagnosis for both the cardiologist technique to enhance fluid compli-
Jaff, M. R. (2001). Management of athero- and the nephrologist? Nephrology ance. Dialysis & Transplantation, 23(6),
sclerotic renal artery stenosis: Dialysis Transplantation, 16(7), 1311- 303-306.
Interventional versus medical thera- 1313. Silver, M. A., Maisel, A., Yancy, C.W.,
py. Current Interventional Cardiology Mason, R.J., Broaddus, V.C., Murray, J.F., McCullough, P.A., Burnett, J.C. Jr.,
Reports, 3(2), 93-99. & Nadel, J.A., (2005). Textbook of Francis, G. et al., (2004). BNP
Kramer, K. Kirkman, P. Kitzman, D., & Respiratory Medicine In W. B. Consensus Panel 2004: A clinical
Little W. C. (2000). Flash pulmonary Saunders Company (Eds.), Textbook of approach for the diagnostic, prognos-
edema: Association with hyperten- respiratory medicine, (4th ed.). New tic, screening, treatment monitoring,
sion and reoccurrence despite coro- York: W.B. Saunders Company. and therapeutic roles of natriuretic
nary revascularization. American Missouris, C. G., Belli, A. M., & peptides in cardiovascular diseases.
Heart Journal, 140(3), 451-455. MacGregor, G. A. (2000). Apparent Congestive Heart Failure, 10(5 Suppl.
Lange, R.A., & Hillis, L.D. (2001). heart failure: A syndrome caused by 3), 1-30.
Cardiovascular complications of renal artery stenosis. Heart, 83(2), Staub, N.C.(1974). Pulmonary edema.
cocaine use. New England Journal of 152-155. Physiology Review, 54(3), 678-811.
Medicine, 345(5), 351-358. Murphy, S. (2003). Management of heart Sulkova, S. & Valek, A. (1988). Role of
Lee, F.A., Cabin, H.S., & Francis, C.K. failure and coronary artery disease in antihypertensive drugs in the therapy
(1988). The syndrome of flash pul- patients with chronic kidney disease. of patients on regular dialysis treat-
monary edema: Clinical definition Seminars in Dialysis, 16(2), 165-172. ment. Kidney International, 35, S198-
and angiographic findings. Journal of National Heart, Lung, and Blood Institute. 200.
the American College of Cardiology, (2003). Seventh Report of the Joint Torre-Amione, G. (2005). Immune activa-
11(2), 151- 153. National Committee on Prevention, tion in chronic heart failure. American
Levey A.S., Beto J.A,. Coronado B.E., Detection, Evaluation, and Treatment of Journal of Cardiology, 95(11A), 3C-8C.
Eknoyan, G., Goley, R.N., Kasiske, High Blood Pressure, ( JNC VIII), Tozawa, M. Iseki, K., Iseki, C., &
B. L., et al., (1998). Controlling the Retrieved January 5, 2006 from Takishita, S. (2002). Pulse pressure
epidemic of cardiovascular disease in http://www.nhlbi.nih.gov/guide- and risk of total mortality and cardio-
chronic renal disease: what do we lines/hypertension/. vascular events in patients on chron-
know? What do we need to learn? National Kidney Foundation. (2005). ic hemodialysis. Kidney International,
Where do we go from here? National K/DOQI Clinical practice guide- 61(2), 717-726.
Kidney Foundation Task Force on lines for cardiovascular disease in United States Renal Data System.
Cardiovascular Disease. American dialysis patients. American Journal of (USRDS 2005), USRDS 2005 annu-
Journal of Kidney Diseases, 32(5), Kidney Disease, 4, 5(S1-S154), (suppl al data report Atlas of end-stage renal
853906. 3). disease in the United States.
Levin, A. (2003). Clinical epidemiology of Olin, R.W. (2004). Renal artery stenosis. Bethesda, MD: National Institute of
cardiovascular disease in chronic kid- The Mount Sinai Journal of Medicine, Diabetes and Digestive and Kidney
ney disease prior to dialysis. Seminars 71(2), 73-85. Diseases.
in Dialysis, 16(2), 101-105. Pickering, T.G., Herman, L., Devereus, Vasan, R.S., Benjamin, E J., & Levy, D.
Little, W.C. & Braunwald, E., Eds (1997). R.B., Sotelo, J E., James, G.D., Sos, (1995). Prevalence, clinical features
Assessment of cardiac function. Heart dis- T.A., et al.,. (1988). Recurrent pul- and prognosis of diastolic heart fail-
ease: A textbook of cardiovascular medi- monary edema in hypertension due ure: An epidemiologic perspective.
cine (5th ed., pp. 421-444). Phila- to Bilateral renal artery stenosis: Journal of the American College of
delphia: W.B. Saunders Company. Treatment by angioplasty or surgical Cardiology, 26(7), 1565-1574.
Logeart, D., Saudubray, C., Beyne, P., revascularization. Lancet, 2(8610). Vasan, R.S., & Levy, D. (1996). The role
Thabut, G., Ennezat, P. V., Chavelas, 551-552. of hypertension in the pathogenesis
C., et al., (2002). Comparative value Redfield, M. (2004). Understanding of heart disease: A clinical mechanis-
of Doppler echocardiography and B- Diastolic heart failure. New England tic overview. Archives of Internal
type natriuretic peptide assay in the Journal of Medicine, 350(19), 1930- Medicine, 156(16), 1789-1796.
etiologic diagnosis of acute dyspnea. 1931. Walker, F. Walker, D.A., & Nielsen, M.
Journal of the American College of Salem, M. M. (1995). Hypertension in the (2001). Flash pulmonary edema,
Cardiology, 40(10), 1794-1800. hemodialysis population: A survey of Lancet, 358(9281), 1646-1647.
Lorell, B.H. & Carabello, B.A., (2000). 649 patients. American Journal of Ware, L.B., & Matthay, M.A. (2005).
Left ventricular hypertrophy: Kidney Disease, 26(3), 461-468. Acute pulmonary edema. New
Pathogenesis, detection, and progno- Sarnak, M.J., Levey, A.S., Schoolwerth, England Journal of Medicine, 353(26),
sis. Circulation, 102(4), 470-479. A.C., Coresh, J., Culleton, B., 2788-2796.
Lucas, M.F., Quereda, C., Teruel, J.L., Hamm, L.L., et al.,.(2003). Kidney
Orte, L., Marcen, R., & Ortuno, J. disease as a risk factor for develop-
(2003). Effect of hypertension before ment of cardiovascular disease.
beginning dialysis on survival of Circulation, 108(17), 2154-2169.
26 NEPHROLOGY NURSING JOURNAL January-February 2007 Vol. 34, No. 1
Yamaguchi, H. Yoshida, J. Yamamoto, K.
Sakata, Y., Mano, T., Akehi, N., et
al.,(2004). Elevation of plasma brain
natriuretic peptide is a hallmark of
diastolic heart failure independent of
ventricular hypertrophy. Journal of the
American College of Cardiology, 43(1),
55-60.
Youngerman-Cole, S. (2005). Cardiac blood
pool scan: Test overview. Retrieved
October 13, 2006. from http://
w w w. w e b m d . c o m / h w / h e a r t _
disease/hw201275.asp.
Zile, M. R. & Simsic, J. M. (2000).
Diastolic heart failure: Diagnosis and
treatment, Clinical Cornerstone, 3(2),
13-24.
NEPHROLOGY NURSING JOURNAL January-February 2007 Vol. 34, No. 1 37
Flash Pulmonary Edema in Patients with Chronic Kidney Disease and
End Stage Renal Disease
Carol Headley, DNSc, RN, CNN and Barry M. Wall MD
Posttest 1.5 Contact Hours
Posttest Questions
(See posttest instructions on the answer form, on page 28.)
1. What statement is true about the fluid 6. Diastolic dysfunction refers to a disor- 11. Your patient has a brain natriuretic pep-
balance between the interstitium and der tide (BNP) level 700 pg/ml. What would
the vascular bed within the lungs? your next action be?
A. of myocardial relaxation resulting in
A. Alveoli have high permeability for pro- impaired ventricular filling. A. CT scan of the brain
tein and fluid. B. of myocardial stiffness that results in B. X-ray of the chest
B. Alveoli epithelial cells drain the pul- delayed ventricular emptying. C. Administer hypertensive medications
monary interstitium. C. associated with left ventricular hyper- D. Complete a physical assessment
C. The alveolar bed within the lungs serve trophy and abnormal filling.
to protect the lung from fluid accumula- D. that occurs as a result of pressure 12. Common finding(s) on physical exami-
tion. changes related to malfunctioning nation of a patient with flash pulmonary
D. The lymphatic vessels continuously valves. edema is (are)
absorb fluid from the alveoli.
7. There is a strong association between A. tachypnea only.
2. The most common cause of non-cardio- - and the development of dias- B. tachypnea and decreased breath
genic pulmonary edema is tolic dysfunction and flash pulmonary sounds only.
edema. C. tachypnea, decreased breath sounds,
A. renal artery stenosis. and new murmur only.
B. malignant hypertension. A. hypertension D. tachypnea, decreased breath sounds,
C. acute lung injury. B. left ventricular hypertrophy new murmur, and hypotension.
D. aspiration of gastric contents. C. anemia
D. volume overload 13. What common practice in dialysis units
3. What changes likely result in acute car- may contribute to flash pulmonary
diogenic pulmonary edema? 8. The increased resistance to diastolic edema?
ventricular filling in diastolic heart dis-
A. The lymphatic system becomes less ease is commonly due to A. Holding BP medications pre-dialysis
efficient in removing fluid and there is B. Inaccurate dry weight assessment
increased likelihood for development of A. myocardial hypertrophy only. C. Use of non-tunneled catheters for dial-
edema. B. myocardial hypertrophy and ischemia ysis
B. Acute elevations in left atrial pressure only. D. Eating on dialysis
result in pulmonary capillary pressure C. myocardial hypertrophy, ischemia, and
increases and fluid is forced into the mitral stenosis only. 14. Your patient arrives for dialysis with
interstitium and alveoli. D. myocardial hypertrophy, ischemia, tachypnea, hypertension, and crackles
C. Elevated pulmonary capillary wedge mitral stenosis and pericarditis. in the bases of the lungs. You feel the
pressure overwhelms the lymphatic patient has cardiogenic mediated flash
system and edema results. 9. Which statement is true about the pulmonary edema. Why?
D. Increased pulse pressure and systolic prevalence of diastolic heart failure?
hypertension leads to decrease cardiac A. Insignificant intradialytic weight gain
output and fluid leaks into the alveoli. A. 50% of persons greater than age 60 only
with CHF will have diastolic failure. B. Insignificant intradialytic weight gain
4. Congestive heart failure (CHF) is a dis- B. Prognosis for systolic heart failure is and absence of edema only
order that affects the better than diastolic heart failure. C. Insignificant intradialytic weight gain,
C. Patients over 70 years old with diastolic absence of edema, and hypertension
A. heart only. failure have a 30% 5-year mortality. only
B. heart and kidneys only. D. Kidney disease contributes to the D. Insignificant intradialytic weight gain,
C. heart, kidneys, and skeletal muscle development of diastolic heart failure at absence of edema, and hypertension
only. earlier ages. and no history of ischemic heart dis-
D. heart, kidneys, skeletal muscle and ease
nervous system. 10. What statement is true about renal
artery stenosis (RAS)?
5. What statement is true about neurohor-
monal changes in congestive heart fail- A. Chronic mild to moderate hypertension
ure (CHF)? is associated with RAS.
B. It is seen in older women with fibro-
A. Initial neurohormonal changes are muscular dysplasia.
deleterious and lead to pulmonary C. It commonly involves atherosclerotic
edema. plague deposition in the renal artery.
B. Initially stimulation of the sympathetic D. It is always associated with a decrease
nervous system decreases cardiac out- in kidney function.
put.
C. Stimulation of the RAAS causes salt
and water excretion by the kidneys.
D. Long-term stimulation leads to myocyte
apoptosis, hypertrophy, and myocardial
necrosis.
NEPHROLOGY NURSING JOURNAL January-February 2007 Vol. 34, No. 1 27
Flash Pulmonary Edema in Patients with Chronic Kidney Disease and End Stage Renal Disease
ANNJ701 ANSWER/EVALUATION FORM
Flash Pulmonary Edema in Patients with Chronic Kidney Disease and
End Stage Renal Disease
Carol M. Headley, DNSc, RN, and Barry M. Wall MD
Posttest Instructions Complete the Following:
Select the best answer and circle the Name: ____________________________________________________________
appropriate letter on the answer grid
below. Address: __________________________________________________________
Complete the evaluation.
Send only the answer form to the __________________________________________________________________
ANNA National Office; East Holly
Avenue Box 56; Pitman, NJ 08071- Telephone: ______________________ Email: _____________________________
0056; or fax this form to (856) 589- CNN: ___ Yes ___ No CDN: ___ Yes ___ No CCHT: ___ Yes ___ No
7463.
Enclose a check or money order Payment:
payable to ANNA. Fees listed in pay-
ment section. ANNA Member - $15 Non-Member - $25 Rush Processing - Additional $5
Posttests must be postmarked by
February 20, 2009. If you receive a ANNA Member: ____ Yes ____ No Member #___________________________
passing score of 70% or better, a Check Enclosed American Express Visa MasterCard
certificate for 1.5 contact hours will
be awarded by ANNA. Total Amount Submitted: _________________
Please allow 2-3 weeks for process-
Credit Card Number: _______________________________ Exp. Date: _______
ing. You may submit multiple answer
forms in one mailing, however, Name as it Appears on the Card: ______________________________________
because of various processing pro-
cedures for each answer form, you Special Note
may not receive all of your certificates Your posttest can be processed in 1 week for an additional rush charge of $5.00.
returned in one mailing. Yes, I would like this posttest rush processed. I have included an additional fee of
$5.00 for rush processing.
Note: If you wish to keep the journal intact, you may photocopy the answer sheet or access this posttest at
www.nephrologynursingjournal.net.
Online submissions through a partnership with HDCN.com are accepted on this posttest at
$20 for ANNA members and $30 for nonmembers. CE certificates will be available immediately
upon successful completion of the posttest.
Posttest Answer Grid (Please circle your answer choice):
1. a b c d 4. a b c d 7. a b c d 10. a b c d 13. a b c d
2. a b c d 5. a b c d 8. a b c d 11. a b c d 14. a b c d
3. a b c d 6. a b c d 9. a b c d 12. a b c d
Strongly Strongly Recognize the risk for development of flash
Evaluation disagree agree pulmonary edema in patients with chronic
1. The objectives were related to the goal. 1 2 3 4 5 kidney disease and ESRD
2. Objectives were met
a. Identify causes of flash pulmonary edema that may 1 2 3 4 5 I verify that I have completed this activity:
occur in conjunction with chronic kidney disease
and ESRD. _____________________________________________
b. Recognize signs and symptoms of flash pulmonary 1 2 3 4 5 (Signature)
edema.
c. Describe nursing measures that may avert devel- 1 2 3 4 5 Comments _____________________________________
opment of flash pulmonary edema in individuals with _____________________________________________
advanced chronic kidney disease.
3. The content was current and relevant. 1 2 3 4 5 _____________________________________________
4. This was an effective method to learn this content. 1 2 3 4 5
Suggested topics for future articles?_________________
5. Time required to complete reading assignment: _________ minutes.
_____________________________________________
_____________________________________________
28 NEPHROLOGY NURSING JOURNAL January-February 2007 Vol. 34, No. 1
Anda mungkin juga menyukai
- 2017 CSCPDSDokumen4 halaman2017 CSCPDSGillian Bitong AlejandroBelum ada peringkat
- DOHDeploymentProgram2018 3 PDFDokumen3 halamanDOHDeploymentProgram2018 3 PDFAirene SibleBelum ada peringkat
- ProtagorasDokumen4 halamanProtagorasJustine May GervacioBelum ada peringkat
- Research ForumDokumen34 halamanResearch ForumJustine May GervacioBelum ada peringkat
- Small Intestine Treatment-National Cancer InstituteDokumen22 halamanSmall Intestine Treatment-National Cancer InstituteJustine May GervacioBelum ada peringkat
- K PotaDokumen2 halamanK PotaJustine May GervacioBelum ada peringkat
- Career Planning Da FinalDokumen7 halamanCareer Planning Da FinalJustine May GervacioBelum ada peringkat
- Career Planning: Beginning A Job Search, Sources of Job Leads, Developing A ResumeDokumen26 halamanCareer Planning: Beginning A Job Search, Sources of Job Leads, Developing A ResumeJustine May GervacioBelum ada peringkat
- Stephen CoveyDokumen18 halamanStephen CoveyAbhijith Shetty100% (2)
- ExamsDokumen44 halamanExamsJustine May GervacioBelum ada peringkat
- GCOE Provision 4-6Dokumen29 halamanGCOE Provision 4-6Justine May GervacioBelum ada peringkat
- "Career Planning": U T R SDokumen45 halaman"Career Planning": U T R SsivapathasekaranBelum ada peringkat
- Hydrocor Tisone Body As A Whole: HypersensitivityDokumen8 halamanHydrocor Tisone Body As A Whole: HypersensitivityJustine May GervacioBelum ada peringkat
- Fatty Liver (Hepatic Stenosis) : InterventionsDokumen2 halamanFatty Liver (Hepatic Stenosis) : InterventionsJustine May GervacioBelum ada peringkat
- ReactionDokumen1 halamanReactionJustine May GervacioBelum ada peringkat
- Uloric (Febuxostat) - Side Effects, Interactions, Warning, Dosage & Uses (Dragged)Dokumen1 halamanUloric (Febuxostat) - Side Effects, Interactions, Warning, Dosage & Uses (Dragged)Justine May GervacioBelum ada peringkat
- Armed ConflictsDokumen11 halamanArmed ConflictsJustine May GervacioBelum ada peringkat
- DrugStudy EgoyDokumen10 halamanDrugStudy EgoyJustine May GervacioBelum ada peringkat
- Abletes Journal 2Dokumen4 halamanAbletes Journal 2Justine May GervacioBelum ada peringkat
- Atorvastatin Drug StudyDokumen2 halamanAtorvastatin Drug StudyJustine May Gervacio0% (1)
- Pathophysiology of End Stage Renal Failure Secondary To Hypertensive NephrosclerosisDokumen5 halamanPathophysiology of End Stage Renal Failure Secondary To Hypertensive NephrosclerosisJustine May GervacioBelum ada peringkat
- Publication CitizenCorpOverviewDokumen24 halamanPublication CitizenCorpOverviewJustine May GervacioBelum ada peringkat
- Physical Diet/Lifestyl E Chemical Immunologic Environmenta L Hereditary Hormonal BiologicDokumen1 halamanPhysical Diet/Lifestyl E Chemical Immunologic Environmenta L Hereditary Hormonal BiologicJustine May GervacioBelum ada peringkat
- Abletes JournalDokumen7 halamanAbletes JournalJustine May GervacioBelum ada peringkat
- Misagal JournalDokumen10 halamanMisagal JournalJustine May GervacioBelum ada peringkat
- Art Therapy 3 14 16Dokumen3 halamanArt Therapy 3 14 16Justine May GervacioBelum ada peringkat
- Psychosocial Theory of Erik Erikson: Group 2Dokumen22 halamanPsychosocial Theory of Erik Erikson: Group 2Justine May GervacioBelum ada peringkat
- Medical MGT DM 2Dokumen8 halamanMedical MGT DM 2Justine May GervacioBelum ada peringkat
- Medical MGT DM 2Dokumen8 halamanMedical MGT DM 2Justine May GervacioBelum ada peringkat
- Shoe Dog: A Memoir by the Creator of NikeDari EverandShoe Dog: A Memoir by the Creator of NikePenilaian: 4.5 dari 5 bintang4.5/5 (537)
- The Yellow House: A Memoir (2019 National Book Award Winner)Dari EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Penilaian: 4 dari 5 bintang4/5 (98)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDari EverandNever Split the Difference: Negotiating As If Your Life Depended On ItPenilaian: 4.5 dari 5 bintang4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDari EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RacePenilaian: 4 dari 5 bintang4/5 (890)
- Grit: The Power of Passion and PerseveranceDari EverandGrit: The Power of Passion and PerseverancePenilaian: 4 dari 5 bintang4/5 (587)
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDari EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifePenilaian: 4 dari 5 bintang4/5 (5794)
- The Little Book of Hygge: Danish Secrets to Happy LivingDari EverandThe Little Book of Hygge: Danish Secrets to Happy LivingPenilaian: 3.5 dari 5 bintang3.5/5 (399)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDari EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FuturePenilaian: 4.5 dari 5 bintang4.5/5 (474)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDari EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryPenilaian: 3.5 dari 5 bintang3.5/5 (231)
- The Emperor of All Maladies: A Biography of CancerDari EverandThe Emperor of All Maladies: A Biography of CancerPenilaian: 4.5 dari 5 bintang4.5/5 (271)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDari EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersPenilaian: 4.5 dari 5 bintang4.5/5 (344)
- On Fire: The (Burning) Case for a Green New DealDari EverandOn Fire: The (Burning) Case for a Green New DealPenilaian: 4 dari 5 bintang4/5 (73)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDari EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaPenilaian: 4.5 dari 5 bintang4.5/5 (265)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDari EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyPenilaian: 3.5 dari 5 bintang3.5/5 (2219)
- Team of Rivals: The Political Genius of Abraham LincolnDari EverandTeam of Rivals: The Political Genius of Abraham LincolnPenilaian: 4.5 dari 5 bintang4.5/5 (234)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDari EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You ArePenilaian: 4 dari 5 bintang4/5 (1090)
- Rise of ISIS: A Threat We Can't IgnoreDari EverandRise of ISIS: A Threat We Can't IgnorePenilaian: 3.5 dari 5 bintang3.5/5 (137)
- The Unwinding: An Inner History of the New AmericaDari EverandThe Unwinding: An Inner History of the New AmericaPenilaian: 4 dari 5 bintang4/5 (45)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Dari EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Penilaian: 4.5 dari 5 bintang4.5/5 (119)
- Her Body and Other Parties: StoriesDari EverandHer Body and Other Parties: StoriesPenilaian: 4 dari 5 bintang4/5 (821)
- Meddra Important Medical Event Terms List Version 241 enDokumen691 halamanMeddra Important Medical Event Terms List Version 241 enLuis Antonio Camacho CamachoBelum ada peringkat
- The-Cardiovascular-System Notes MariebDokumen7 halamanThe-Cardiovascular-System Notes MariebLol lolBelum ada peringkat
- Anatomy For Beginners 2 - CirculationDokumen18 halamanAnatomy For Beginners 2 - CirculationDefy R PradentyBelum ada peringkat
- Plant and Animal Organ Systems and Their Functions (Gas Exchange and Transport/Circulation)Dokumen24 halamanPlant and Animal Organ Systems and Their Functions (Gas Exchange and Transport/Circulation)Sherry Macalalad GarciaBelum ada peringkat
- A201 Fa Qsu3033Dokumen7 halamanA201 Fa Qsu3033Sua RezBelum ada peringkat
- High-Performance Color Doppler System Apogee 5500 Data SheetDokumen18 halamanHigh-Performance Color Doppler System Apogee 5500 Data SheetIBrahim FayedBelum ada peringkat
- Aortic StenosisDokumen8 halamanAortic Stenosisikbal rambalinoBelum ada peringkat
- Transportation in AnimalsDokumen6 halamanTransportation in AnimalskrovrainkBelum ada peringkat
- Pediatric Cardiovascular DisordersDokumen9 halamanPediatric Cardiovascular Disorderscayla mae carlos0% (1)
- Cardiac Anatomy GuideDokumen5 halamanCardiac Anatomy GuideZintan HospitalBelum ada peringkat
- Heart Anatomy GuideDokumen7 halamanHeart Anatomy GuideKaryll AguilaBelum ada peringkat
- Science 6 2ND Periodical TestDokumen9 halamanScience 6 2ND Periodical TestYvonne BautistaBelum ada peringkat
- Anatomy and Physiology of Cardiovascular SystemDokumen2 halamanAnatomy and Physiology of Cardiovascular SystemKezzel Grace MaquillaBelum ada peringkat
- 60 Pedia DisordersDokumen6 halaman60 Pedia DisordersEkoy TheRealBelum ada peringkat
- AbbreviationDokumen90 halamanAbbreviationIrwanshah MohammadBelum ada peringkat
- Transport System in Plants and AnimalsDokumen7 halamanTransport System in Plants and AnimalsBeatriz gannabanBelum ada peringkat
- Heart Sounds - PracticalDokumen7 halamanHeart Sounds - Practicalshadapaaak100% (1)
- Cambridge IGCSE: Biology 0610/22Dokumen16 halamanCambridge IGCSE: Biology 0610/22omarBelum ada peringkat
- Versana Active Spec SheetDokumen19 halamanVersana Active Spec Sheetbashir019100% (1)
- CV SystemDokumen11 halamanCV System4everiamarmyBelum ada peringkat
- Class-12 (RBSE) Biology-Ch-24 Blood Circulatory System PDFDokumen7 halamanClass-12 (RBSE) Biology-Ch-24 Blood Circulatory System PDFIshansi AgrawalBelum ada peringkat
- Circulatory System LessonDokumen13 halamanCirculatory System LessonNan Houm SianBelum ada peringkat
- Case 3: Aortic StenosisDokumen11 halamanCase 3: Aortic StenosisfmBelum ada peringkat
- Extraordinary Blood Circulation in CrocodilesDokumen5 halamanExtraordinary Blood Circulation in CrocodilesRudy Hermosillo100% (1)
- Drug Study and LaboratoryDokumen13 halamanDrug Study and LaboratoryGEOMHAI CATBAGANBelum ada peringkat
- Fisiopatologia Del Shock Cardiogenico Por Iam PDFDokumen12 halamanFisiopatologia Del Shock Cardiogenico Por Iam PDFYESSICA CARENALGABelum ada peringkat
- Myocardial Work in Nonobstructive Hypertrophic Cardiomyopathy: Implications For OutcomeDokumen8 halamanMyocardial Work in Nonobstructive Hypertrophic Cardiomyopathy: Implications For Outcomeme1921Belum ada peringkat
- Anatomi Dan Fisiologi Sistem Kardiovaskular: Hendra FirmansyahDokumen19 halamanAnatomi Dan Fisiologi Sistem Kardiovaskular: Hendra Firmansyahrandy sepasaciBelum ada peringkat
- L5 NotesDokumen9 halamanL5 Notes17 ERMINO, Nicole AngelaBelum ada peringkat
- Complications of Acute Myocardial Infarction (AMIDokumen5 halamanComplications of Acute Myocardial Infarction (AMIlourdesfercab_at_msn100% (1)