Periodontal Treatment Protocol
Diunggah oleh
venaHak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
Periodontal Treatment Protocol
Diunggah oleh
venaHak Cipta:
Format Tersedia
Periodontal Treatment Protocol (PTP) for the
General Dental Practice
Larry A. Sweeting, DDS; Karen Davis, RDH, BSDH; Charles M. Cobb, DDS, PhD
Introduction
Abstract
1
Hujoel et al estimated a 31% A sequence of interrelated steps is inherent to effective periodontal
decrease in the prevalence of periodon- treatment: early and accurate diagnosis, comprehensive treatment, and
titis between the years 1955 and 2000. continued periodontal maintenance and monitoring. A primary goal of
Further, these authors estimate an addi- periodontal therapy is to reduce the burden of pathogenic bacteria and
tional 8% decrease by the year 2020. In thereby reduce the potential for progressive inflammation and recur-
spite of the decreased use of smoking rence of disease. Emerging evidence of possible perio-systemic links
tobacco,2 better understanding of the further reinforces the need for good periodontal health. In the private
pathogenesis of periodontal diseases, practice setting, the treatment of patients with periodontal disease is best
and more refined and goal directed ther- accomplished within the structure of a uniform and consistent Peri-
apies, there remains evidence that den- odontal Treatment Protocol (PTP). Such a protocol would reinforce
tistry is not consistently achieving a accurate and timely diagnosis, treatment needs based on a specific
timely diagnosis and appropriate and diagnosis, and continual assessment and monitoring of outcomes. This
timely treatment of existing periodonti- is best achieved if everyone in the practice setting has a general under-
tis.3,4 Although the evidence is limited, standing of the etiology of periodontal diseases, the benefits of treat-
there is a strong suggestion that use of a ment, and potential consequences of nontreatment. Communication
periodontal probe for diagnosis and skills and patient education are vital components of effective therapy
recording of periodontal status in treat- since slight and even moderate stages of the disease often have few
ment records in general dental practices noticeable symptoms to the patient. Accurate documentation and report-
has yet to achieve the level of a routine ing of procedures for dental insurance reimbursement, coupled with
and consistent habit.5-9 Indeed, McFall scheduling considerations, assist general practice settings in effectively
et al8 determined that except for radi- managing the increasing volume of patients that can benefit from early
ographs, most private practice patient diagnosis and treatment of periodontal diseases. This article presents
records were so deficient in diagnostic the essential elements of a PTP including diagnosis, treatment planning,
information that periodontal status could implementation of therapy, assessment and monitoring of therapy, insur-
not be established. It should be self-evi- ance coding, introduction of the patient to periodontal therapy, and
dent that treatment requires a definitive enhanced verbal skills. In addition, considerations for implementation of
diagnosis, ie, a disease cannot be ade- adjunctive local delivery antimicrobials is presented.
quately treated unless first diagnosed.
In this regard, it is interesting to note Key Words: periodontal diseases, periodontal diagnosis, treatment
that at least one study has reported a dis- protocol, periodontal maintenance, periodontal assessment, patient
connect between dentists’ perception of education
treatment rendered and actual treatment
as recorded in patient records.10 As an
example, prophylactic procedures out-
number periodontal procedures by a
ratio of 20:111,12 and yet the prevalence of odontitis with a concomitant decrease dental office did not vary because of
chronic periodontitis (slight, moderate, in the percentage of mild-moderate dis- disease severity; and the average num-
and severe) is estimated to range from a ease cases; increase in the average num- ber of periodontal maintenance vis-
low of 7% (aged > 18 years)13 up to 35% ber of missing teeth per patient; and its/patient/year in the general dental
(aged > 30-90 years)14 of the US adult increase in the average number of teeth office was less than the standard of care
population. scheduled for extraction per patient. A according to severity of disease, eg,
Cobb et al.3 compared the pattern of similar study by Docktor et al4 based on 68% of advanced periodontitis cases
referral of periodontitis patients in 1980 patient records from 3 private peri- reported between 0 and 2 periodontal
vs 2000 using patient record data from odontal practices located within a major maintenance visits per year rather than
3 geographically-diverse private peri- metropolitan area reported the follow- the recommended every 3 months.
odontal practices. Results showed the ing: 74% of referred cases were con- Viewed in aggregate, the trends
following trends occurring over the 20- sidered advanced periodontitis, of reported by Cobb et al3 and Docktor et
year time span: decreased use of which 30% were treatment planned for al 4 support the assertion that timely
tobacco; increase in the percentage of extraction of 2 or more teeth; periodon- diagnosis and appropriate and timely
cases exhibiting advanced chronic peri- tal treatment provided by the general treatment of chronic periodontitis have
16 The Journal of Dental Hygiene Special supplement
not significantly improved over time. A
major reason for the reported scarcity of Table 1. Modified Version of the American
timely diagnosis and appropriate treat- Academy of Periodontology Suggested Guidelines
ment may be the lack of a well-estab- for a Comprehensive Periodontal Examination.18
lished office protocol for the diagnosis,
treatment, maintenance, and monitor- Assessment of medical history
ing of periodontal disease, and involve-
ment of the patient through education. Assessment of dental history
Obviously, this requires dedication of
energy, resources, effective communi- Assessment of periodontal risk factors
cation skills, and a change in practice 1. Age
philosophy. 2. Gender
3. Medications
4. Presence of plaque and calculus (quantity and distribution)
The Periodontal 5. Smoking
Treatment Protocol 6. Race/Ethnicity
(PTP) 7. Systemic disease (eg, diabetes)
8. Oral hygiene
Diagnosis 9. Socioeconomic status and level of education
Assessment of extraoral and intraoral structures and tissues
Regardless of recent advances in our
understanding of the etiology and patho- Assessment of teeth
genesis of the periodontal diseases, the 1. Mobility
assessment of traditional clinical param-
2. Caries
eters remain the foundation for peri-
odontal diagnosis.15 Generally, such clin- 3. Furcation involvement
ical parameters include probing depth 4. Position in dental arch and within alveolus
(PD), bleeding on probing (BOP), clin- 5. Occlusal relationships
ical attachment level (CAL), degree of 6. Evidence of trauma from occlusion
furcation involvement, extent of gingi-
val recession, tooth mobility, and plaque Assessment of periodontal soft tissues including peri-implant tissues
score. Clinicians typically utilize the 1. Color
results from the periodontal exam, radi- 2. Contour
ographs, and the patient’s medical and
3. Consistency (fibrotic or edematous)
dental histories to establish a diagnosis
and evolve a goal/diagnosis-directed 4. Presence of purulence (suppuration)
treatment plan. It has been clearly 5. Amount of keratinized and attached tissue gingiva
demonstrated that different interpreta- 6. Probing depths
tions of the same diagnostic information 7. Bleeding on probing
can have a dramatic impact on treatment 8. Clinical attachment levels
decisions.16 For this reason, a standard-
ized approach to periodontal assess- 9. Presence and severity of gingival recession
ments and a working protocol as to treat- Radiographic evaluation of alveolar bone loss, bone density, furcations,
ment parameters would fill a logical
root shape, and proximity, etc.
need in the average general practice set-
ting. However, due to extensive over-
laps in most classification systems, any loss. The presence, location, and extent eral dental practice, only the following
standardized approach is subject to vari- of furcation invasions should be noted, as principal diagnostic criteria can be
ations in both clinical assessments (eg, well as the location of the gingival mar- addressed: age, PD, CAL, BOP, tooth
variations in probing depth among cli- gin or CAL. Also, the patient’s age is an mobility, furcation involvement, and
nicians) as well as the interpretation important factor, especially in cases of percentage of radiographic bone loss. It
thereof. rapidly progressing disease and deter- must be emphasized that these criteria
All effective treatment protocols mining overall long-term prognosis. represent the minimal parameters for
begin with a thorough and timely diag- A modified version of the American determining a periodontal diagnosis.
nosis. Six-point probing to measure PD Academy of Periodontology (AAP) There are many other important risk and
and BOP is the standard of care. Based proposed guidelines for a comprehen- modifying factors that will impact
on the needs of the patient, current radi- sive periodontal examination is pre- development and progression of disease
ographs should be evaluated to deter- sented in Table 1. 17 However, with and all such factors must be taken into
mine the location and percentage of bone respect to a functional PTP for the gen- consideration when establishing a defin-
Special supplement The Journal of Dental Hygiene 17
itive diagnosis and a diagnosis-driven Radiographic Evidence of Bone odontal disease. It is recognized that
treatment plan.18 Loss is best determined with adequate each dental practice setting is different.
Age is of relative value in that and current radiographs,17 most typically Consequently, guidelines are intended
advanced amounts of periodontal a full-mouth periapical survey, including to be used in a manner that best meets
destruction at an earlier age tend to indi- vertical bite-wings, or a panographic the needs of the specific patient.
cate a more aggressive form of peri- radiograph supplemented with vertical Generally speaking, plaque-induced
odontitis. In contrast, chronic periodon- bite-wings and selected periapical films. periodontal diseases have historically
titis may slowly progress towards By definition, true periodontitis does not been categorized into gingivitis versus
severity over several years or decades. begin until bone loss occurs.25 Radi- periodontitis based upon whether attach-
Young age combined with moderate to ographic evaluation of the distribution ment loss has occurred. The 1999 Inter-
severe bone loss presents a tenuous and severity of bone loss, bone density, national Workshop for Classification of
long-term prognosis and requires more root anatomy, and approximation to other Periodontal Diseases21 reclassified the
aggressive therapy compared to the teeth provides specific information that plaque-induced periodontal diseases into
older patient presenting with a chronic will help in determining a proper diag- 7 different classifications. In considera-
form of periodontitis.19 nosis, treatment plan, and prognosis. tion of a working PTP that addresses
Probing depth (PD) is defined as Bleeding on Probing (BOP) is a only the common periodontal diseases,
the distance from the gingival margin simple assessment of the inflammatory this paper will address health, gingivitis,
to the base of the gingival crevice.20 The status of the gingiva.15,26 In patients with chronic periodontitis (formerly adult
periodontal pocket, represented by a deeper pockets and/or loss of clinical periodontitis), and aggressive periodon-
probing depth > 3 mm, is the principle attachment, the chances of disease pro- titis (formerly early-onset periodontitis).
habitat for gram-negative, anaerobic gression are greater as the percentage of The first 7 entries in Table 2 (see back
pathogenic bacteria.20 Deeper pockets bleeding sites increase.27 Conversely, cover) constitute a set of clinical criteria
tend to represent more extensive lack of BOP is highly correlated with (PD, BOP, percent bone loss, tooth
destruction of the underlying periodon- stability and a lack of inflammation.28 mobility, degree of furcation involve-
tium and, therefore, a potentially greater This latter statement, however, does not ment, and CAL) that will facilitate dif-
pathenogenic burden. apply to smokers as they tend to bleed ferentiation of health from gingivitis and
Clinical Attachment Level (CAL) is less when compared to nonsmokers with between the various levels of severity
defined as the distance from the CEJ to equal amounts of disease.29 of chronic periodontitis. Further, Table 2
the base of the probable crevice/pocket. In addition to the usual clinical can aid the clinician in differentiating
In cases of gingival recession, the amount parameters, the clinician is well advised between chronic and aggressive peri-
of recession is added to the PD to yield to consider other risk factors and their odontitis.
the total amount of CAL. Although more potential impact on the development and Some practice settings may prefer a
difficult to obtain, it is a better measure of progression of plaque-induced peri- system of “Periodontal Case Types” for
the total extent of damage to the under- odontal diseases.18 Risk factors that are purposes of diagnosis and record keep-
lying periodontium.20-22 sometimes overlooked in the diagnosis, ing. Table 3 presents the diagnostic clin-
Mobility is best measured by the treatment plan, and prognosis equation ical criteria as applied to Case Types for
blunt end of 2 instruments alternating include, among others: diabetes, smok- health, gingivitis, chronic periodontitis
pressure in a facial-lingual direction and ing, osteoporosis, compromised immune (slight, moderate, and severe), and
an apical direction to assess abnormal system, drug-induced gingival condi- aggressive periodontitis. These criteria
movement of the tooth. Simply tions, hormonal changes, and genetics. and Case Types are generally appropri-
assessed: Grade I mobility is slightly Patients at risk for periodontal disease ate but should be considered as guide-
more than normal; Grade II is moder- are often allowed to “slip between the lines only and not as a definitive diag-
ately more than normal; Grade III is cracks” during a routine visit because nosis. As mentioned before, there are
severe mobility facial-lingually plus api- they may be in the early stages of the numerous modifying and risk factors to
cal displacement.23 Mobility patterns are disease. Risk factors increase a patient’s consider prior to evolving a diagnosis
suggestive of possible occlusal trauma, chance of developing periodontitis. The and a diagnosis-driven treatment plan.
severe inflammation, and/or loss of sup- presence of one or more of these risk
porting alveolar bone. factors may also indicate a benefit from
Furcations represent bone loss specialty referral in some patients. Treatment Planning
between the roots of multi-rooted teeth.
A deeply invasive furcation lesion is the Development of a logical and prop-
equivalent of a poor long-term progno- Case Types and Periodontal erly sequenced treatment plan is a deriv-
sis for the involved tooth. Simply put, a Diagnosis ative of the periodontal assessment and
Grade 1 furcation involvement is incip- diagnosis. Periodontal therapy is diag-
ient bone loss only; a Grade 2 is partial As part of a PTP it is necessary to nosis-driven and, to the extent possible,
loss of bone producing a cul-de-sac; a establish diagnostic guidelines that will should address all modifying factors and
Grade 3 is total bone loss with through- provide a framework for organizing the risk factors that impact development and
and-through opening of the furcation; treatment needs of the patient. Guide- progression of plaque-induced peri-
and a Grade 4 is similar to a Grade 3, but lines are not meant to replace clinical odontal disease. An overview of a typi-
with gingival recession that visually knowledge or skills, nor do they imply a cal periodontal treatment plan is pre-
exposes the furcation opening.24 one-size-fits-all treatment plan for peri- sented in Table 4.30
18 The Journal of Dental Hygiene Special supplement
Table 3. Clinical Criteria Assigned to Periodontal Case Types of
Health, Gingivitis, Chronic Periodontitis (slight, moderate, and severe),
and Aggressive Periodontitis.
PD BOP Bone Mobility Furcations CAL Visual
Case Type (mm) (Yes/No) Loss (%) (Grade) (Grade) (mm) Inflammation
0 (Health) 0-3 No 0 None None 0 No
I (Gingivitis) 0-4 Yes 0 None None 0 Yes (localized or
generalized)*
II (Slight Chronic Periodontitis)† 4-5 Yes 10 I 1 1-2 Yes (localized or
generalized)*
III (Moderate Chronic Periodontitis)† 5-6 Yes 33 I and II 1 and 2 3-4 Yes (localized or
generalized)*
IV (Severe Chronic Periodontitis)† >6 Yes > 33 I, II, or III 1, 2, 3, or 4 >5 Yes (localized or
generalized)*
V (Aggressive Periodontitis)_† >6 Yes > 33 I, II, or III 1, 2, 3, or 4 >5 Yes (localized or
(age is significant factor) generalized)*
* Localized disease is defined as < 30% of sites are involved; and generalized disease infers >30% of sites are involved.21
†
Specialty referral may be indicated for additional treatment beyond initial therapy.
†_
Specialty referral should be considered.
Table 4. General Overview of the Major Steps in a Typical Periodontal
Treatment Plan.3
Sequence of Major Phases
1. Address acute periodontal problems and/or pain
2. Review and update medical and dental histories
3. Assessment of systemic risk factors and refer for medical consultation as needed
4. Extraoral examination
5. Oral cancer evaluation
6. Assessment of periodontal risk and modifying factors
7. Periodontal examination to include dental implants
8. Dental examination to include occlusal relationships and dental implants
9. Radiographic examination
10. Establish a definitive diagnosis
11 Generate a diagnosis-driven periodontal treatment plan and sequence of treatment
12. Determine required adjunctive restorative, prosthetic, orthodontic, and/or endodontic treatments and
sequence
13. Execute Phase I therapy (aka anti-infective or nonsurgical therapy) with consideration given to adjunc-
tive use of chemotherapeutic agents
14. Re-evaluation (assessment) of Phase I therapy
15. If end-points are not achieved, consider selective retreatment, need for surgical therapy, specialty refer-
ral, or use of adjunctive diagnostic aides, eg, microbial, genetic, medical lab tests, etc.
16. Determine interval for periodontal maintenance and continued assessment of periodontal status
Special supplement The Journal of Dental Hygiene 19
Implementation of Therapy odontitis should be managed by peri- odontal treatment and subsequent
odontal maintenance (PM), performed reporting of services for insurance reim-
There are a wide variety of treatment at an interval of 3 months for an indefi- bursement. In terms of nonsurgical peri-
options to be considered when con- nite period of time following active ther- odontal therapy, familiarity with dental
fronted with gingivitis or chronic or apy.32 The 3-month interval is critical insurance codes provides a clear method
aggressive periodontitis. However, thor- (and the standard of care for moderate to document treatment and select appro-
ough scaling and root planing (SRP) is and severe chronic periodontitis and priate procedures to maximize insurance
still considered the gold standard in peri- aggressive periodontitis) as it has been reimbursement for the patient.
odontal therapy. Beyond SRP, no one repeatedly shown to be effective in Table 5 presents a modified descrip-
treatment modality is the answer in reducing disease progression, preserv- tion of the ADA insurance codes most
every case. However, the clinician must ing teeth, and controlling the subgingi- commonly used in Phase I periodontal
have specific endpoints or goals that val bacterial burden.33-35 Nonetheless, the therapy (aka anti-infective therapy or
therapy should achieve. If such end- PM schedule should be individualized nonsurgical therapy). The descriptions
points are not achieved, then therapy and tailored to meet the needs of each are intended to reveal distinctive differ-
must be re-evaluated and a decision patient. Factors such as home care, pre- ences between procedures, and guide the
made concerning retreatment or spe- vious level of disease, tendency toward clinician in reimbursement procedures.
cialty referral for consideration of more refraction, stability indicators, etc, To simplify decisions made by
advanced therapy options. Treatment should be used in making this assess- patients, dental insurance should be
options that should be considered ment. More fragile patients may need referred to as “reimbursement,” “bene-
include:30 intervals of 2 months or less, and con- fit,” or “assistance” by the clinician and
versely, patients intercepted in early dis- other staff members rather than “cover-
• Patient education including plaque ease states who demonstrate consistent age” since the word implies complete.
control and counseling in manage- stability may need less frequent inter- Most patients with dental insurance will
ment of periodontal and systemic vals of 4-6 months. Regardless of the find it necessary to supplement what-
risk factors interval between appointments, the peri- ever insurance benefit they receive
odontal status of each patient should be toward lifetime periodontal care, as
• Scaling and root planing
re-evaluated at every maintenance many plans have contract limitations for
• Consideration of adjunctive chemo- appointment. Only through close moni- the percentage of reimbursement asso-
therapeutic agents, eg, locally or toring can disease recurrence be detected ciated with various procedures and/or
systemically administered antibi- and the maintenance interval adjusted the length of time those benefits apply.
otics and host response modifica- accordingly. Continual assessment of the For example, limitations of some insur-
tion agents. periodontium during maintenance ance plans assign benefits for PM fol-
affords the best opportunity for assur- lowing SRP but only for 24 months fol-
• Re-evaluation
ing long-term stability or providing lowing active therapy. As another
• Consideration of referral to a spe- interceptive care.34,35 example, exclusions found in other
cialist is an option that must be con- insurance plans assign benefits for SRP
sidered for both legal and ethical for generalized periodontal disease but
reasons.31 There are a variety of rea- Insurance Coding not for localized infection. Many
sons to consider referral to a peri- patients are reticent to proceed with
odontist, such as, SRP in the pres- The American Academy of Peri- treatment unless their insurance will
ence of extreme amounts of dental odontology’s Parameters of Care 200036 “pay for it.” Consequently, it is advan-
calculus or SRP with complications and the American Dental Association’s tageous for practices to have clear expla-
of systemic disease, gingival over- Current Dental Terminology37 are avail- nations about the reality of dental insur-
growth and/or inflammatory hyper- able to clinicians to guide decision-mak- ance. Figure 2 presents a sample
plasia, resective surgery, regenera- ing related to providing therapeutic peri- explanation of dental insurance that can
tive procedures for soft and hard
tissues, periodontal plastic surgery,
occlusal therapy, pre-prosthetic sur- Understanding Dental Insurance
gery, dental implants, management
of perio-systemic complications, 1. Dental insurance is a contractual agreement between the employer
phobic patients requiring conscious and insurance company. The percentage of reimbursement varies
sedation, etc. greatly dependent upon the premiums paid for a particular plan and
limitations of the agreement.
2. Maximum payable benefits around $1000 - $1500 commonly found
Periodontal Maintenance today with dental insurance plans are almost identical to the annual
Therapy and Continual maximum benefit of dental insurance plans 40 years ago.
Assessment 3. Dental insurance is a benefit designed to help defray the costs of
quality dental care, but is not all-inclusive of what an individual may
In general, data suggests that patients need or desire to obtain optimal dental health for a lifetime.
who have undergone definitive therapy
for either localized or generalized peri- Figure 2. Facts about dental insurance to share with patients.
20 The Journal of Dental Hygiene Special supplement
Table 5. Modified Description of ADA Insurance Codes
Commonly Used for Phase I Periodontal Therapy
(aka anti-infective therapy or nonsurgical therapy).
Code
Number Treatment Procedure Description
D0180 Comprehensive Indicated for new or established patients showing signs or symptoms of
Periodontal Evaluation periodontal disease and for patients with risk factors such as smoking
or diabetes. It includes evaluation of periodontal conditions, probing and
charting, evaluation and recording of the patient’s dental and medical
history and general health assessment. It may include the evaluation
and recording of dental caries, missing or unerupted teeth, restorations,
occlusal relationships and oral cancer evaluation.
D1110 Adult Prophylaxis Includes the removal of plaque, stain and calculus from tooth structures
and is intended to control local irritation to gingival tissues, thereby
preventing disease initiation.
D4355 Full Mouth Debridement Initial removal of plaque and calculus that interfere with the ability to
to Enable Comprehen- perform a comprehensive oral evaluation. This preliminary procedure is
sive Evaluation and generally followed by a comprehensive periodontal evaluation for
Diagnosis diagnosis and subsequent therapeutic periodontal procedures.
D4341 Scaling and Root Involves therapeutic treatment of 4 or more periodontally involved teeth
Planing per quadrant through definitive removal of subgingival plaque biofilm and
Generalized per root preparation in order to halt the disease from progressing, thereby
Quadrant creating an opportunity for healing. To be reported per quadrant inclusive
of updated periodontal charting and radiographs for reimbursement.
D4342 Scaling and Involves therapeutic treatment of 1 to 3 periodontally involved teeth per
Root Planing quadrant through definitive removal of subgingival plaque biofilm and
Localized per root preparation in order to halt the disease from progressing, thereby
Quadrant creating an opportunity for healing. To be reported per quadrant with
identification of specific teeth being treated inclusive of updated peri-
odontal charting and radiographs for reimbursement.
D4381 Localized Delivery of Subgingival insertion of antimicrobial medications of a therapeutic con-
Antimicrobial Agents via centration into periodontal pockets that are released over a sufficient
a Controlled Release length of time in order to suppress the pathogenic burden, and are
Vehicle into Diseased intended to enhance the clinical results of scaling and root planing alone.
Crevicular Tissue To be reported per tooth, identifying multiple treatment sites per tooth, if
indicated, inclusive of a narrative describing systemic considerations for
reimbursement such as tobacco usage, diabetes, or heart disease.
D4999 Unspecified Periodontal In the absence of a specific ADA code for complete periodontal
Procedure, by Report re-assessment following definitive periodontal therapy, this procedure
code is being utilized to determine healing response and future treat-
ment recommendations.
D4910 Periodontal Maintenance Follows the completion of active therapy to treat periodontal infection
for the lifetime of the dentition or implant replacements and includes
removal of plaque biofilm and calculus from supra and subgingival sur-
faces. It may also include site specific scaling and root planing for areas
of localized disease recurrence. It is intended to keep periodontal dis-
eases under control; therefore a patient may move from active therapy
to periodontal maintenance and back to active therapy and/or referral
during the lifetime of the dentition or implant replacements. It is not syn-
onymous with prophylaxis, and is required at varying intervals to man-
age periodontal diseases and modify risk factors. To be reported by
both general and periodontal practices on patients having undergone
active therapy irrespective of where the procedure is performed. Cur-
rent periodontal charting documenting the patient’s on-going periodon-
tal status should be submitted for reimbursement.
Special supplement The Journal of Dental Hygiene 21
be shared with patients, assisting them in during data collection and tissue assess- Enhanced Communication Skills
making independent decisions about ment, the patient should be provided a
treatment, regardless of the insurance mirror to visualize with the clinician the Each clinician will develop his/her
reimbursement schedule. evidence of periodontal disease, caries, own style of case presentation for peri-
gingival recession, tooth mobility, fur- odontal therapy and will individualize
cation involvement, etc. (Figure 1). Dur- the message to different patients. How-
Patient Education and ing periodontal probing, the patient ever, there is significant advantage if
Introduction to Periodontal should hear the pocket measurements as the entire office staff has continuity in
Therapy data is being collected and recorded. In key words that are used when dis-
a similar manner, during examination of cussing periodontal therapy with
Effective implementation of the the radiographs, the patient should be patients. Equally important is the avoid-
aforementioned concepts requires shown evidence of permanent bone loss, ance of minimizing messages such as
expertise in effective patient education and contrast that to areas without bone “just a little bit of bleeding,” or “a little
and introduction of periodontal therapy loss. Involving the patient in the dis- bone loss,” or “just a little bit of
so that patients are prepared to make covery process visually and audibly is a plaque.” It is advisable to use language
wise health decisions. Being proficient powerful tool to help patients take own- that does not trivialize conditions that
in SRP procedures has little value to the ership in their own health. are not yet severe. Terms such as “slight
patient who assumes they are visiting
the dental hygienist for a “routine clean-
ing.” This is particularly true if the
patient already has a developing or exist-
ing periodontal infection and does not
understand the need for therapeutic
intervention. Chronic periodontal dis-
eases often provide few noticeable
symptoms, especially in earlier stages
of development. Thus, the need for
effective communication, education, and
listening skills are of particular impor-
tance to today’s dental patient.
The incidence of moderate and
severe generalized chronic periodonti-
tis in the US appears to affect only 5%
to 15% of the adult population, whereas
slight disease affects approximately 35%
of the adult population.13,14,38 Thus, most
new patients and even many existing
patients will ultimately be diagnosed
with periodontal diseases. To be effec- Figure 1. Dental hygienist showing patient periodontal conditions in
tive at enrolling patients into active ther- patient’s own mouth.
apy everyone in the practice setting must
have a basic understanding of the etiol-
ogy of periodontal diseases, treatment This is also an opportune time for the bleeding,” “early bone loss,” or “slight
options, consequences of nontreatment, clinician to introduce adjunctive thera- plaque” accurately describe findings
and direct benefits of therapy. Patients pies to the patient such as the use of without overstating them. Periodontal
are more motivated to accept treatment locally delivered antimicrobials and disease is a bacterial infection leading to
recommendations when a clear diagno- other agents. For example, the clinician a host immune response that is charac-
sis has been established, they are given can communicate that locally delivered terized by inflammation and degrada-
the opportunity to see infection in their antimicrobials have been on the US mar- tion of periodontal tissues. 22 When
own mouths, their questions have been ket for many years and have been shown informing patients of periodontal dis-
answered, and they understand the value to be a safe, effective treatment option. ease, using the word “infection” is more
of treating periodontal infection in rela- Important information to convey powerful than “gum inflammation” and
tion to their overall health. includes the ease of application; the high can create a sense of urgency regarding
Many clinicians inform patients of potency of the drug at levels that will treatment. The word “hemorrhage”
their periodontal status while working kill bacteria; it does not affect the rest of indicates heavy bleeding and implies a
in their mouths with sharp instruments, the body; and there is no need for an condition outside healthy parameters.
or give a summary of findings at the end additional appointment to remove the When the patient’s gingival tissues
of the visit. Most patients are visual product since the agent biodegrades. hemorrhage easily upon provocation,
learners. Consequently, patients need to Educating the patient to all of their treat- “hemorrhage” rather than “bleeding
see the condition of their own mouth. ment options is vital to clear and evi- gum tissue” should be verbalized to the
At the beginning of every appointment, dence-based communication. patient. The words “scaling and root
22 The Journal of Dental Hygiene Special supplement
Guide for Use of Locally Delivered Antimicrobials
Where to use locally delivered antimicrobials: How to apply locally delivered antimicrobials:
➢ Pockets > 5 mm with bleeding on probing (BOP). ➢ For optimal effect from locally delivered antimicrobials
• The locally delivered antimicrobial may be used at the following must be achieved:
the time of scaling and root planing (SRP) or at the • Oral hygiene instructions and patient compliance
re-evaluation appointment 4-6 weeks following SRP. regarding the necessary oral hygiene procedures, ie,
If used first at the re-evaluation appointment, the site tooth brushing, use of interdental hygiene aids such
must have additional SRP to remove biofilm and hard as dental floss and proxabrushes, and use of antimi-
deposits that may have re-accumulated. crobial oral rinses.
➢ Residual pockets of > 5 mm with BOP or any site > 6 • Supragingival scaling and polishing.
mm following initial SRP. • Definitive subgingival SRP (generally under local
• Determined at re-evaluation appointment. anesthesia).
• If > 4 residual pockets in a given quadrant then con- • Place locally delivered antimicrobial according to
sider either retreatment (SRP) with locally delivered manufacturer’s directions. For example, in the case
antimicrobial or surgical intervention. of minocycline microspheres, place one pre-meas-
➢ Sites treatment planned for osseous grafting. ured dose per pocket. If the tooth has 2 pockets that
• Locally delivered antimicrobial placed 3 weeks prior need local delivery, 2 full doses should be adminis-
to surgical procedure. tered.
➢ Periodontal abscess • The pocket should be as biofilm and deposit free as
➢ Probing depth at the distal-facial line-angle of 2nd possible prior to insertion.
molars related to 3rd molar extractions where surgical • Insert the locally delivery product to the base of the
intervention will yield a compromised result. pocket. In the case of minocycline microspheres, the
➢ Ailing/failing dental implants (peri-implantitis) where sur- tip should be placed as far into the pocket as possi-
gical intervention is not indicated or will yield a compro- ble before activating
mised result. the syringe/handle
➢ Grade II furcation involvements (shallow or deep) when (Figures 4 and 5).
surgical intervention is not planned.
Addendum:
Who might benefit from use of locally delivered ➢ If probing depths are < 4
antimicrobials: mm, the clinician should
➢ Periodontal maintenance consider a conventional
patients with isolated adult prophylaxis coupled
probing depths of > 5 mm with oral hygiene recom-
that exhibit BOP or any mendations and/or rein- Figure 4. Initial Inser-
pocket > 6 mm (Figure 3). forcement. tion of the pre-meas-
➢ Patients wanting to avoid • If the patient exhibits ured tip for adminis-
periodontal surgery. multiple probing tration of minocycline
➢ High risk surgery patients. depths of 4 mm a peri- microspheres
• Poorly controlled (brit- odontal maintenance
tle) diabetic patients Figure 3. Pre-treatment interval of 3-4 months
• Patients with a history clinical presentation should be considered
of recent or recurrent until it can be deter-
showing PD of 6 mm
coronary or cere- mined if the patient’s
brovascular events. periodontal status is
• Patients with a compromised immune system due to stable and/or improv-
disease or medications. ing.
• Kidney dialysis patients.
• Heavy smokers (> 1/2 pack/day)
• Patients with physical disability that impacts oral Figure 5. Tip place-
hygiene efficiency ment to base of
• Mentally handicapped patients pocket for administra-
➢ Patient’s with marginal oral hygiene that is not likely to tion of minocycline
improve and thereby represent a poor surgical risk. microspheres.
➢ Please note that locally applied antimicrobials may need
to be placed more than one time to achieve the desired
result.
Special supplement The Journal of Dental Hygiene 23
planing” may sound confusing to Suggestions for • Include assessments and diagnosis
patients or imply discomfort. The words of periodontal diseases in all new
“periodontal therapy” are effective Implementation of a patient visits, routine prophylaxis
semantic choices when informing Periodontal Treatment appointments, and ongoing peri-
patients about necessary periodontal Protocol in the General odontal maintenance to insure no
treatment. “We now know” are words patient is overlooked regarding
that can introduce patients to new ideas Practice Setting diagnosis of developing periodontal
or treatment options to explain why disease or recurring disease.
information may be different than what • General dentists and dental hygien-
• Select appropriate ADA Insurance
they have heard in the past, or expected ists should schedule a meeting with
Procedure Codes for reporting peri-
to hear at their current visit. “Halting” referring periodontists and their
odontal procedures in order to max-
or “arresting disease” can be used to dental hygienists to share philoso-
imize the patient’s benefit.
describe a measurable goal for treating phies of periodontal treatment and
periodontal diseases that should be establish clarity for referrals. • Share insurance information with
obtained through intervention. “Daily patients to assist them in reducing
• Schedule a team meeting workshop
disease control” communicates to the their dependence on dental insur-
to bring all office staff up-to-date
patient that they share in the role in the ance benefits, thereby enabling
regarding periodontal assessments,
effective removal of plaque bacteria them to make independent health
diagnosis, case types, periodontal
beyond what it achieve through peri- decisions related to treatment of
risk factors, individualized treat-
odontal treatment. periodontal diseases.
ment of periodontal diseases, con-
Even though some states require
sequences of nontreatment (tooth
written consent, effective communica-
loss and possible systemic involve-
tion between the clinician and the patient
ment), and the value of periodontal Disclosure
is the important consideration of
maintenance.
informed consent,39 not the completion
of a form. Therefore, deliberate seman- • Establish continuity of the verbal Dr. Sweeting, Ms. Davis, and Dr.
tic choices should be shared by all mem- skills and terminology the office Cobb are scientific advisors for
bers of the office staff to optimize staff will utilize to communicate OraPharma, Inc.
patient understanding of their periodon- effectively to patients about peri-
tal conditions. odontal conditions.
References 10. Helminen SE, Vehkalahti M, Murtomaa H. Dentists’ per-
ception of their treatment practices versus documented
1. Hujoel PP, Bergström J, del Aguila MA, DeRouen TA. A hid- evidence. Int Dent J 2002;52:71-74.
den periodontitis epidemic during the 20th century? Com- 11. Blair, C. The economic impact of the under diagnosis of
munity Dent Oral Epidemiol 2003;31:1-6. periodontal disease in general practice. Triage 2005;1:21-25.
2. Mendez D, Warner KE. Adult cigarette smoking preva- 12. American Dental Association, Survey Center. 1999 Survey
lence: Declining as expected (not as desired). Am J Pub of Dental Services Rendered. Chicago IL: American Den-
Health 2004;94:251-252. tal Association; 1999.
3. Cobb CM, Carrara A, El-Annan E, et al. Periodontal refer- 13. Borrell LN, Burt BA, Taylor GW. Prevalence and trends in
ral patterns, 1980 versus 2000: A preliminary study. J Peri- periodontitis in the USA: The NHANES, 1988 to 2000. J
odontol 2003:74:1470-1474. Dent Res 2005;84:924-930.
4. Dockter KM, Williams KB, Bray KS, Cobb CM. Relation- 14. Albandar JM, Brunelle JA, Kingman A. Destructive peri-
ship between pre-referral periodontal care and peri- odontal disease in adults 30 years of age and older in the
odontal status at time of referral. J Periodontol United States, 1988-1994. J Periodontol 1999;70:13-29.
2006:77:1708-1716. 15. Armitage GC. Periodontal diseases: Diagnosis. Ann Peri-
5. Bader JD, Rozier G, McFall WT, Jr., Sams DH, Graves odontol 1996;1:37-215.
RC, Slome BA, Ramsey DL. Evaluating and influenc- 16. Papapanou PN, Wennstrom JL, Sellen A, Hirooka H, Gron-
ing periodontal diagnostic and treatment behaviors in dahl K, Johnsson T. Periodontal treatment needs assessed
general practice. J Am Dent Assoc 1990;121:720-724. by the use of clinical and radiographic criteria. Community
6. Cury PR, Martins MT, Bonecker M, De Araujo NS. Inci- Dent Oral Epedimiol 1990;18:113-119.
dence of periodontal diagnosis in private dental practice. 17. American Academy of Periodontology. Parameter on com-
Am J Dent 2006;19:163-165. prehensive periodontal examination. J Periodontol
7. Heins PJ, Fuller WW, Fries SE. Periodontal probe use in 2000;71(Suppl.);847-848.
general practice in Florida. J Am Dent Assoc 1989;119:147- 18. Krebs KA, Clem DS, III. American Academy of Periodon-
150. tology. Guidelines for the management of patients with
8. McFall WT, Jr., Bader JD, Rozier G, Ramsey D. Presence periodontal diseases. J Periodontol 2006;77:1607-1611.
of periodontal data in patient records of general practi- 19. Novak KF, Goodman SF, Takei HH. Determination of prog-
tioners. J Periodontol 1988;59:445-449. nosis. In: Newman MG, Takei H, Klokkevold PR, Carranza
9. Brown LJ, Johns BA, Wall TP. The economics of peri- FA, eds. Clinical Periodontology, 10th ed. Philadelphia:
odontal diseases. Periodontol 2000. 2002;29:223-234. Saunders/Elsevier; 2006; pp. 614-625.
24 The Journal of Dental Hygiene Special supplement
20. Carranza FA, Camargo PM. The periodontal pocket. In: association between plaque and gingival bleeding. Clin
Newman MG, Takei H, Klokkevold PR, Carranza FA, eds. Oral Invest 2006;10:311-316.
Clinical Periodontology, 10th ed. Philadelphia: Saun- 30. American Academy of Periodontology. Position paper.
ders/Elsevier; 2006, pp. 434-451. Guidelines for periodontal therapy. J Periodontol
21. Armitage GC. Development of a classification system for 2001;72:1624-1628.
periodontal diseases and conditions. Ann Periodontol 31. American Dental Association. Principles of ethics and code
1999;4:1-6. of professional conduct. January 2005. Available at:
22. American Academy of Periodontology. Position paper: http://www.ada.org/prof/prac/law/code/index.asp. Accessed
Diagnosis of periodontal diseases. J Periodontol August 28, 2008.
2003;74:1237-1247. 32. American Academy of Periodontology. Position paper. Peri-
23. Carranza FA, Takei HH. Clinical diagnosis. In: Newman odontal maintenance. J Periodontol 2003;74:1395-1401
MG, Takei H, Klokkevold PR, Carranza FA, eds. Clinical 33. Greenwell H, Bissada NB, Wittwer JW. Periodontics in
Periodontology, 10th ed. Philadelphia: Saunders/ general practice: Perspectives on periodontal diagnosis. J
Elsevier; 2006, pp. 540-560. Am Dent Assoc 1989:119:537-541.
24. Carranza FA, Takei HH. Bone loss and patterns of bone 34. Hirschfeld L, Wasserman B. A long-term survey of tooth
destruction. In: Newman MG, Takei H, Klokkevold PR, loss in 600 treated periodontal patients. J Periodontol
Carranza FA, eds. Clinical Periodontology, 10th ed. 1978;49:225-237.
Philadelphia: Saunders/Elsevier; 2006, pp. 452-466. 35. Tonetti MS, Muller-Campanile V, Lang NP. Changes in the
25. Armitage GC. Clinical evaluation of periodontal diseases. prevalence of residual pockets and tooth loss in treated
Periodontol 2000 1995;7:39-53 periodontal patients during a supportive maintenance care
26. Haffajee AD, Socransky SS, Lindhe J, Kent RL, Okamoto program. J Clin Periodontol 1998;25:1008-1016.
H, Yoneyama T. Clinical risk indicators for periodontal 36. American Academy of Periodontology. Parameters of care.
attachment loss. J Clinical Periodontol 1991;18:117-125. J Periodontol 2000;71: 847-880.
27. Claffey N, Egelberg J. Clinical indicators of probing attach- 37. American Dental Association. Current Dental Terminology.
ment loss following initial periodontal treatment in 2007-2008;3-27.
advanced periodontitis patients. J Clin Periodontol 38. American Academy of Periodontology. Position paper. Epi-
1995;22: 690-696. demiology of periodontal diseases. J Periodontol
28. Lang NP, Adler R, Joss A, Nyman S. Absence of bleeding 2005;76:1406-1419.
on probing – an indicator of periodontal stability. J Clin 39. American Academy of Periodontology. American Acad-
Periodontol 1990;17:714-721. emy of Pediatric Dentistry. Guideline for periodontal
29. Muller HP, Stadermann S. Multivariate multilevel models for therapy. Pediatr Dent 2005-2006;27(7 Reference Man-
repeated measures in the study of smoking effects on the ual):197-201.
Table 2. Periodontal Diagnostic Guidelines.
Case Slight Moderate Advanced
Indicator Healthy Gingivitis Periodontitis Periodontitis Periodontitis Aggressive/Refractory
a
Pocket Depth < 3 mm < 4 mm 4 - 5 mm 5 -6 mm > 6mm > 6mm
Bleeding Upon No Yesb Yesb Yesb Yesb Yesb
Probing
Six-Point Yes Yes Yes Yes Yes Yes
Probing
Bone Loss None None < 10% < 33% > 33% > 33%
Tooth None None None < Grade II < Grade III < Grade III
Mobilityc
Furcationd None None < Grade I < Grade II < Grade III/IV < Grade III/IV
Clinical None None 1 - 2 mm CAL 3 - 4 mm CAL > 5 mm CAL > 5 mm CAL
Attachment
Loss (CAL)e
Other No Only gingival Signs of inflammation Signs of inflammation Signs of inflammation Signs of inflammation
inflammation tissues affected may be present, including may be present, including may be present, including may be present, including
by the • Edema • Edema • Edema • Edema
inflammatory • Redness • Redness • Redness • Redness
process • Suppuration • Suppuration • Suppuration • Suppuration
• Alveolar bone level is • Alveolar bone level is • Alveolar bone level is • Same clinical signs as
• No alveolar 3 - 4 mm from CEJ 4 - 6 mm from CEJ • > 6 mm from CEJ advanced but includes
bone loss • Radiographic bone loss • Radiographic bone loss • Radiographic bone loss adolescents or
• Localized or present present present young adults
generalized • Localized or generalized • Localized or generalized • Localized or generalized • Localized or generalized
• Rapid cycles of disease
progression
Assessment • Prophy • Prophy • Comp. Oral Eval D0150 • Comp. Oral Eval D0150 • Comp. Oral Eval D0150 • Comp. Oral Eval D0150
• OHI • OHI • Comp. Perio Eval D0180 • Comp. Perio Eval D0180 • Comp. Perio Eval D0180 • Comp. Perio Eval D0180
• Four bitewings D0274 • Four bitewings D0274 • Four bitewings D0274 • Four bitewings D0274
• Eight bitewings D0277 • Eight bitewings D0277 • Eight bitewings D0277 • Eight bitewings D0277
• FMX D0210 • FMX D0210 • FMX D0210 • FMX D0210
• Panoramic Film D0330 • Panoramic Film D0330 • Panoramic Film D0330 • Panoramic Film D0330
• Full Mouth Debride D4355 • Full Mouth Debride D4355 • Full Mouth Debride D4355
• Occlusal Analysis D9950 • Occlusal Analysis D9950 • Occlusal Analysis D9950
• Specialty Referral • Specialty Referral
Active • Prophy • Prophy • Quadrant SRP D4341 • Quadrant SRP D4341 Quadrant SRP
• D4341
Therapy • OHI • OHI - UR, UL, LR, LL - UR, UL, LR, LL - UR, UL, LR, LL
• Localized SRP D4342 • Localized SRP D4342 • Localized SRP D4342
- UR, UL, LR, LL - UR, UL, LR, LL - UR, UL, LR, LL
• Locally Administered D4381 • Locally Administered D4381 • Locally Administered D4381 • Specialty Referral
Antimicrobials Antimicrobials Antimicrobials
• OHI D1330 • OHI D1330 • OHI D1330
• Specialty Referral • Specialty Referral • Specialty Referral
• Other Treatments • Other Treatments • Other Treatments
Ongoing 6 Months 6 Months • Perio Maintenance D4910 • Perio Maintenance D4910 Perio Maintenance
• D4910 Perio Maintenance
• D4910
Maintenance • Prophy • Prophy - 3/4/6 months - 3/4/6 months - 3/4/6 months - 3/4/6 months
• OHI • OHI • OHI D1330 • OHI D1330 • OHI D1330 • OHI D1330
• Locally Administered D4381 • Locally Administered D4381 • Locally Administered D4381 • Locally Administered D4381
Antimicrobials Antimicrobials Antimicrobials Antimicrobials
• Localized SRP D4342 • Localized SRP D4342 • Localized SRP D4342 • Localized SRP D4342
- UR, UL, LR, LL - UR, UL, LR, LL - UR, UL, LR, LL - UR, UL, LR, LL
• Other Treatments • Other Treatments • Other Treatments • Host Modulation
a ©OraPharma, Inc. 2008
Excluding gingival overgrowth and recession
b
Bleeding upon probing may not be present in individuals with periodontal disease who are smokers.
c
Tooth Mobility: Grade I: Slightly more than normal; Grade II: Moderately more than normal; Grade III: Severe mobility faciolingually and mesiodistally, combined with vertical displacement. Adapted
from Newman MG, Takei H, Klokkevold PR, Carranza FA. Carranza’s Clinical Periodontology 10th ed. Philadelphia, PA: Elsevier; 2006.
d
Furcation Grades: Grade I: Initial attachment loss with most of the bone still intact in the furcation. No radiographic changes seen; Grade II: The bone defect is definite horizontal bone loss that does
not extend all the way through. Vertical bone loss may also be present. There is an opening into the furca with a bony wall at the deepest portion. Grade III: Bone is lost across the whole width of the
furcation so no bone is attached to the furcation roof; Grade IV: Bone loss across the furcation, accompanied with gingival recession at the furcation, is clinically visible. Adapted from Newman MG,
Takei H, Klokkevold PR, Carranza FA. Carranza’s Clinical Periodontology 10th ed. Philadelphia, PA: Elsevier; 2006.
e
Adapted from Armitage GC. Development of a classification system for periodontal diseases and conditions. Ann Periodontol 1999; 4(I):1-6
Adapted from Periodontal Diagnostic Guidelines ©OraPharma, Inc. 2008
Anda mungkin juga menyukai
- The Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifeDari EverandThe Subtle Art of Not Giving a F*ck: A Counterintuitive Approach to Living a Good LifePenilaian: 4 dari 5 bintang4/5 (5795)
- The Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You AreDari EverandThe Gifts of Imperfection: Let Go of Who You Think You're Supposed to Be and Embrace Who You ArePenilaian: 4 dari 5 bintang4/5 (1091)
- Never Split the Difference: Negotiating As If Your Life Depended On ItDari EverandNever Split the Difference: Negotiating As If Your Life Depended On ItPenilaian: 4.5 dari 5 bintang4.5/5 (838)
- Hidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RaceDari EverandHidden Figures: The American Dream and the Untold Story of the Black Women Mathematicians Who Helped Win the Space RacePenilaian: 4 dari 5 bintang4/5 (895)
- Grit: The Power of Passion and PerseveranceDari EverandGrit: The Power of Passion and PerseverancePenilaian: 4 dari 5 bintang4/5 (588)
- Shoe Dog: A Memoir by the Creator of NikeDari EverandShoe Dog: A Memoir by the Creator of NikePenilaian: 4.5 dari 5 bintang4.5/5 (537)
- The Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersDari EverandThe Hard Thing About Hard Things: Building a Business When There Are No Easy AnswersPenilaian: 4.5 dari 5 bintang4.5/5 (345)
- Elon Musk: Tesla, SpaceX, and the Quest for a Fantastic FutureDari EverandElon Musk: Tesla, SpaceX, and the Quest for a Fantastic FuturePenilaian: 4.5 dari 5 bintang4.5/5 (474)
- Her Body and Other Parties: StoriesDari EverandHer Body and Other Parties: StoriesPenilaian: 4 dari 5 bintang4/5 (821)
- The Emperor of All Maladies: A Biography of CancerDari EverandThe Emperor of All Maladies: A Biography of CancerPenilaian: 4.5 dari 5 bintang4.5/5 (271)
- The Sympathizer: A Novel (Pulitzer Prize for Fiction)Dari EverandThe Sympathizer: A Novel (Pulitzer Prize for Fiction)Penilaian: 4.5 dari 5 bintang4.5/5 (121)
- The Little Book of Hygge: Danish Secrets to Happy LivingDari EverandThe Little Book of Hygge: Danish Secrets to Happy LivingPenilaian: 3.5 dari 5 bintang3.5/5 (400)
- The World Is Flat 3.0: A Brief History of the Twenty-first CenturyDari EverandThe World Is Flat 3.0: A Brief History of the Twenty-first CenturyPenilaian: 3.5 dari 5 bintang3.5/5 (2259)
- The Yellow House: A Memoir (2019 National Book Award Winner)Dari EverandThe Yellow House: A Memoir (2019 National Book Award Winner)Penilaian: 4 dari 5 bintang4/5 (98)
- Devil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaDari EverandDevil in the Grove: Thurgood Marshall, the Groveland Boys, and the Dawn of a New AmericaPenilaian: 4.5 dari 5 bintang4.5/5 (266)
- A Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryDari EverandA Heartbreaking Work Of Staggering Genius: A Memoir Based on a True StoryPenilaian: 3.5 dari 5 bintang3.5/5 (231)
- Team of Rivals: The Political Genius of Abraham LincolnDari EverandTeam of Rivals: The Political Genius of Abraham LincolnPenilaian: 4.5 dari 5 bintang4.5/5 (234)
- On Fire: The (Burning) Case for a Green New DealDari EverandOn Fire: The (Burning) Case for a Green New DealPenilaian: 4 dari 5 bintang4/5 (74)
- Case Study 25Dokumen3 halamanCase Study 25Desiree Ladner Scott86% (7)
- The Unwinding: An Inner History of the New AmericaDari EverandThe Unwinding: An Inner History of the New AmericaPenilaian: 4 dari 5 bintang4/5 (45)
- Rise of ISIS: A Threat We Can't IgnoreDari EverandRise of ISIS: A Threat We Can't IgnorePenilaian: 3.5 dari 5 bintang3.5/5 (137)
- Blood Bank Harmening Chapter 10Dokumen14 halamanBlood Bank Harmening Chapter 10ichummy19100% (3)
- ZtPyrBpzMK Naskah Publikasi PDFDokumen17 halamanZtPyrBpzMK Naskah Publikasi PDFFathiya FarhaniBelum ada peringkat
- AcetanilideDokumen4 halamanAcetanilideJinseong ChoiBelum ada peringkat
- Incision and Drainage of AbscessesDokumen25 halamanIncision and Drainage of Abscessesjaphetnwapi100% (1)
- World Service Office PO Box 9999 Van Nuys, CA 91409 USADokumen2 halamanWorld Service Office PO Box 9999 Van Nuys, CA 91409 USAmustafa hezamBelum ada peringkat
- Ch06 Blocked Fallopian TubesDokumen80 halamanCh06 Blocked Fallopian TubesAasia Najaf SoomroBelum ada peringkat
- Basics of Pharmacology: Speaker - DR - SantoshDokumen76 halamanBasics of Pharmacology: Speaker - DR - SantoshRamya ChallaBelum ada peringkat
- Critical Appraisal of Articles About Diagnostic TestsDokumen43 halamanCritical Appraisal of Articles About Diagnostic TestshardianBelum ada peringkat
- CHP 11 Moderate Nonskeletal Problems in Preadolescent ChildrenDokumen6 halamanCHP 11 Moderate Nonskeletal Problems in Preadolescent ChildrenJack Pai33% (3)
- Do You Know Me Flyer-Teacher VersionDokumen1 halamanDo You Know Me Flyer-Teacher VersionMaria Guy Del DucaBelum ada peringkat
- Daftar Obat Apotek MutiaraDokumen7 halamanDaftar Obat Apotek Mutiarafany hertinBelum ada peringkat
- LP + Askep CKD ON HDDokumen51 halamanLP + Askep CKD ON HDArista BaruBelum ada peringkat
- Quiz 5 - PSY1001 Introductory PsychologyDokumen6 halamanQuiz 5 - PSY1001 Introductory Psychologymrsdenison0% (1)
- Csa Z32 - Testing Guideline and Procedures: PO Box 20020 Red Deer, AB T4N 6X5 Phone: 403.986.2939Dokumen8 halamanCsa Z32 - Testing Guideline and Procedures: PO Box 20020 Red Deer, AB T4N 6X5 Phone: 403.986.2939tim4109Belum ada peringkat
- Innate ImmunityDokumen43 halamanInnate ImmunityhunarsandhuBelum ada peringkat
- Angelie ADokumen4 halamanAngelie AMaja TusonBelum ada peringkat
- Act 1 Urinary SystemDokumen20 halamanAct 1 Urinary Systemisabellamarie.castillo.crsBelum ada peringkat
- Healthy LivingDokumen57 halamanHealthy LivingGrover DejucosBelum ada peringkat
- Cataract SurgeryDokumen2 halamanCataract SurgeryndrabramsBelum ada peringkat
- JMM 29 119Dokumen8 halamanJMM 29 119subanant11Belum ada peringkat
- Quality Management in The Imaging Sciences 5th Edition Papp Test BankDokumen35 halamanQuality Management in The Imaging Sciences 5th Edition Papp Test Bankmisdateholinessaubzt6100% (22)
- Sample ExamDokumen13 halamanSample ExamJenny Mendoza VillagonzaBelum ada peringkat
- EYE MCQ Uploaded by Hafiz BilalDokumen2 halamanEYE MCQ Uploaded by Hafiz BilalMohammad Jamal NasirBelum ada peringkat
- ALP Crestline PDFDokumen2 halamanALP Crestline PDFJashmyn JagonapBelum ada peringkat
- MCQ Pead MockDokumen8 halamanMCQ Pead MocknoblefxBelum ada peringkat
- Unani Product List PDFDokumen109 halamanUnani Product List PDFAK50% (2)
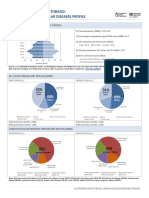
- Trinidad and Tobago: Cardiovascular Diseases ProfileDokumen2 halamanTrinidad and Tobago: Cardiovascular Diseases ProfileKay BristolBelum ada peringkat
- Intern Annual16Dokumen7 halamanIntern Annual16Akash PanwarBelum ada peringkat
- ICD X Kes HajiDokumen2 halamanICD X Kes Hajiyasin_rsdk67% (3)