08 Placenta
Diunggah oleh
Priyanka GeorgeDeskripsi Asli:
Hak Cipta
Format Tersedia
Bagikan dokumen Ini
Apakah menurut Anda dokumen ini bermanfaat?
Apakah konten ini tidak pantas?
Laporkan Dokumen IniHak Cipta:
Format Tersedia
08 Placenta
Diunggah oleh
Priyanka GeorgeHak Cipta:
Format Tersedia
35
PLACENTA
PLACENTAL CALCIFICATION
Is a normal physiological process that occurs during pregnancy.According to some it has no
pathological /clinical significance.Others however associate various types of calcification to
significant conditions .Grading of placenta is based on calcifications.
Grade 0:smooth chorionic plate devoid of undulations and calcified areas.Normally placenta
upto 29wks is grade 0.
PL
PL
Grade 0 Placenta(PL) Grade I Placenta(PL)
Arrow-Uneven placental texture
Grade I:Scattered calcific spots with subtle undulations of chorionic plate.
Grade II: Calcific areas seen in the basal plate.Calcific septa from chorionic plate approach
basal plate.(without reaching it) dividing placenta into incomplete cotyledons.
Grade III placenta.Prominent calcifications
seen in Basal plate(arrows) &septa(arrowheads)
Grade III:Mature Placenta:Marked undulations of the chorionic plate and calcific areas
extend from chorionic plate to the basal layer dividing placenta into cotyledons.Centre of
cotyledons has sonoluscent areas.
SIGNIFICANCE OF GRADING
Two portions of placenta may have different grades and highest grade is assigned.
Institute Of Ultrasound Training,New Delhi,India.
36
According to Hopper grade I placenta before 27 wks, grade II before 32 wks and grade III
before 34 wks have high incidence of pre-ecclampsia and IUGR. BPD of 8.7 cm or less with
gradeIII placenta—chances of IUGR are increased by 8.5 times. Grade III placenta is
associated with complete lung maturity.However if a grade III placenta is found earlier in
pregnancy it is not a 100% reliable marker of fetal lung maturity.
BPD of 9.2 cm or more corelates with lung maturity because it tends to exclude early
gestational age.Placental changes may be delayed in D.mellitus and Rh sensitization.
Changes are accelerated in IUGR and hypertension.
LESIONS OF PLACENTA(Normal)
Present as hypo-echoic or anechoic lesions.Include:
1.Subchorionic fibrin deposition
2. Intervillous thrombosis
Subchorionic fibrin deposition-Multiple Maternal Lakes(arrows)P-placenta
subchorionic anechoic/hyperechoic
lesions (Arrows)
3. Perivillous fibrin deposition &maternal lakes
4.Infarcts.
On ultrasound these sonolucent spaces cannot be distinguished from one another.Only
histologically these lesions can be differentiated.These lesions are common and usually
insignificant.However the number and size of these lesions increase with the duration of
pregnancy and in some pathologic conditions such as Rh iso-immunization ,severe toxemia
and maternal hypertension.
RETROPLACENTAL AREA:shows veins which drain blood from the placenta.
Retroplacental veins(arrowheads).P-Placenta
Institute Of Ultrasound Training,New Delhi,India.
37
CONTRACTIONS OF PLACENTA:
Transient myometrial thickening results from normal uterine contractions(Braxton-Hick’s)
which are imperceptible to the mother .These contractions most commonly occur in second
trimester but can be seen earlier.Contraction causes localized thickening of placenta and /or
myometrium.A contraction may mimic Pl. previa and should be followed over
time(rescanning within 30 min. to 1 hr) to exclude that diagnosis.It should also be
distinguished from leiomyoma which will not change its shape on rescanning.
PLACENTA CRETA:
Focal or diffuse deficiency of decidua basalis.3 categories:
1.Pl.accreta vera: where villi invade the superficial part of myometrium.
2.Pl.increta: Here the myometrium is invaded even in deeper layers.
3.Pl.percreta:villi invade the myometrium completely and further cross it so as to reach the
serosa.
Increased incidence in patients with previous C.S. and uterine scars.
Ultrasound—Absence or significant decrease of usual retroplacental hypo-echoic
zone(representing decidua basalis) is seen.On U/S placenta accreta & increta cannot be
distinguished ,however placenta percreta can be diagnosed by seeing the thinning of the uterine -
bladder interface with protrusion of placental tissue into the bladder lumen.
In all the varieties of placenta creta multiple maternal lakes may be seen.
Placenta increta-There is absence of retroplacental myometrium in the lower part of placenta(curved arrow)
Retro placental myometrium is seen in the upper part (Arrowhead).Arrow shows maternal lake.F-Fetus.
• In women with placenta previa, an abnormally adherent placenta is suspected when
there is an absent decidual interface between the placenta and the myometrium.
Another sign is the presence of unusually dilated vessels at the placental site
large dilated blood vessels in the anterior
uterine wall, which is suggestive of placenta
accreta.
Institute Of Ultrasound Training,New Delhi,India.
38
Placenta percreta-Placenta invading bladder wall(between arrows) Increased blood flow seen in the same area
B
ANTEPARTUM HEMORRAGE:
Bleeding from placenta previa and abruptio placentae usually occurs at or close to term, while
retroplacental or marginal hemorrhage may occur as early as the first trimester.
Retroplacental Hemorrhage & Submembranous hemorrhage
Retroplacental hemorrhage may manifest itself in three ways: (1) external bleeding without
formation of a significant intrauterine hematoma; (2) formation of a retroplacental or
marginal hematoma with or without external bleeding and (3) formation of a submembranous
hematoma at a distance from the placenta, with or without external bleeding Sonographic
examination in cases of antepartum bleed will be negative if most of the bleeding is external.
A retroplacental or submembranous hematoma will appear as a hypoechoic or complex
collection at sonography.
In early pregnancy subchorionic hematoma may be distinguished from nonfused amnion by
evaluating the thickness of the membrane.The membrane above a subchorionic hematoma is
F
thicker than the amnion. Small hematomas of less than
Submembranous hematoma(H) d/d Old submembranous hematoma
Unfused Amnion(arrowhead)
60 c.c. are not associated with increased risk of miscarriage. Disseminated intravascular
coagulation may occur in cases of large,chronic retroplacental hematomas as a result of tissue
breakdown.
Institute Of Ultrasound Training,New Delhi,India.
39
Submembranous hematoma(H).F-fetus Retroplacental bleed(H) P-placenta;F-Fetus
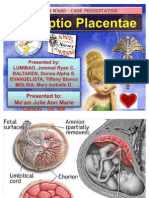
ABRUPTIO PLACENTAE:-
It is premature seperation of placenta . Clinically the pt. may have any of the following
signs: vaginal bleeding,preterm labour, abdominal pain,features of fetal distress or maternal
shock.Maternal hypertension is seen in 50% of cases. Other risk factors include previous h/o
of abruption,premature delivery,presence of fibroid, placenta previa and exposure to drugs
eg. Cocaine.
There are two types of abruptio placenta 1) Retroplacental abruption-It is a severe high
pressure bleed due to rupture of spiral arteries. 2) Marginal abruption-It is milder type of low
pressure bleed and occurs due to tears of marginal veins. Placental seperation is very little
and the bleed usually collects beneath the membranes ( sub-membranous bleed ) away from
the placenta.
ULTRASOUND- In Retroplacental bleed placenta will appear enlarged with presence of
ill-defined echogenic retroplacental collection . This echogenic area of acute bleed will
decrease in echogenicity with the passage of time and will also be more sharply demarcated
from placental tissue.
Marginal abruption shows seperation of small area of placental edge and usually hypoechoic
area of submembranous bleed adjacent to separated placenta.
Abruptio Placenta H-hematoma;P-Placenta Abruptio(late).Hematoma resolving
---
Institute Of Ultrasound Training,New Delhi,India.
40
Low lying placenta:is the one which is within 2 cm of the internal os but not covering it.
PLACENTA PREVIA
Placenta previa, in which the placenta covers part or all of the internal cervical os, is a
common cause of bleeding in the third trimester although it occurs in less than 1% of
deliveries. While diagnosing placenta previa it is important to define Internal Os.The
endocervical canal is seen on sonogram as a line of increased or decreased echogenicity.The
superior termination of endocervical canal is the Internal os.
Placenta previa-
Placenta previa is often overdiagnosed in the first two trimesters, because it is commonly
mimicked by two conditions:
1.Overfilling of the urinary bladder
2.Contractions.(suspected if myometrial wall is greater than 1.5cm).
Thus if placentaprevia is suspected it is important to re examine the patient after voiding and
/or after approximately half an hour has passed
False Pl. previa- Prevoiding. P- Placenta B-Bladder Postvoiding
----
Institute Of Ultrasound Training,New Delhi,India.
41
Uterine contraction Contraction passed
Obscured (by fetal head ) placenta previa . In such cases two techniques used to define the
lower margin of placenta :1.Elevation of presenting part by abdominal palpation 2. By raising
the foot end of the bed.
Presently the better way to document placenta previa in such cases is by:
TRANSLABIAL OR TRANSVAGINAL SCANNING
TVS is superior to both Transabdominal & Translabial scanning in diagnosing placenta
previa.
Translabial scan CompletePlacenta previa Transvaginal Scan
Succenturiate Lobe
Accessory lobe caused by failure of normal villous atrophy.
Connected to main lobe by membrane having foetal vascular supply.
Significance-1.Vessels may rupture during labour causing foetal death.
2.Retention of lobe may lead to PPH or infection.
D/D-Uterine contraction.
Lateral Placenta
Succenturiate Lobe(S)
PL-Placenta main
Institute Of Ultrasound Training,New Delhi,India.
Anda mungkin juga menyukai
- Observations on Abortion: Containing an account of the manner in which it is accomplished, the causes which produced it, and the method of preventing or treating itDari EverandObservations on Abortion: Containing an account of the manner in which it is accomplished, the causes which produced it, and the method of preventing or treating itBelum ada peringkat
- Observations on Abortion: An account of the manner in which it is accomplished, the causes, and the method of preventing itDari EverandObservations on Abortion: An account of the manner in which it is accomplished, the causes, and the method of preventing itBelum ada peringkat
- Ante Partum HemorrhageDokumen21 halamanAnte Partum HemorrhagejyothinanduriBelum ada peringkat
- Antepartum HemorrhageDokumen35 halamanAntepartum HemorrhagesubashikBelum ada peringkat
- Abnormalities of Placenta and CordDokumen47 halamanAbnormalities of Placenta and CordShrooti Shah75% (4)
- Midwifery 102 Module 2aDokumen18 halamanMidwifery 102 Module 2aWynjoy NebresBelum ada peringkat
- APHDokumen40 halamanAPHJayarani AshokBelum ada peringkat
- Ante Partum HemorrhageDokumen30 halamanAnte Partum Hemorrhagetanmai nooluBelum ada peringkat
- USG Trimester 2 & 3 PatologisDokumen48 halamanUSG Trimester 2 & 3 PatologisanggitaBelum ada peringkat
- USG Trimester 2 & 3 PatologisDokumen48 halamanUSG Trimester 2 & 3 PatologisanggitaBelum ada peringkat
- Placental AbnormalitiesDokumen42 halamanPlacental AbnormalitiesTee VillanuevaBelum ada peringkat
- Williams Obstertics, Twenty-Second Edition - Page 619 630Dokumen57 halamanWilliams Obstertics, Twenty-Second Edition - Page 619 630Bharat ThapaBelum ada peringkat
- Placental AbnormalitiesDokumen7 halamanPlacental AbnormalitiesLrak SiaBelum ada peringkat
- Abnormalities of The Placenta OutlineDokumen7 halamanAbnormalities of The Placenta OutlineSteve ShirmpBelum ada peringkat
- Antepartum Haemorrhage - FinalDokumen44 halamanAntepartum Haemorrhage - FinalMLV AbayBelum ada peringkat
- Abruptio PlacentaDokumen20 halamanAbruptio PlacentaHizkia Mangaraja Hasiholan LimBelum ada peringkat
- Placenta Previa: Case DiscussionDokumen4 halamanPlacenta Previa: Case DiscussionTin SumangaBelum ada peringkat
- Antepartum Hemorrhage (APH) : It Is A MedicalDokumen10 halamanAntepartum Hemorrhage (APH) : It Is A Medicalmed.progressBelum ada peringkat
- Introduce Myself: Chinese Name: English Name: Dong Dirong Profession: Obstetrics and Work In: Zhongnan HospitalDokumen80 halamanIntroduce Myself: Chinese Name: English Name: Dong Dirong Profession: Obstetrics and Work In: Zhongnan Hospitalapi-19641337Belum ada peringkat
- ReferatDokumen3 halamanReferatGita AmeliaBelum ada peringkat
- Cord ProlapseDokumen11 halamanCord ProlapseWilliams Emmanuel AdeyeyeBelum ada peringkat
- Abnormalities-Of-Placenta-And-Umbilical CordDokumen53 halamanAbnormalities-Of-Placenta-And-Umbilical CordPraveen YadavBelum ada peringkat
- KMTC Antepartum Hemorrhage NotesDokumen6 halamanKMTC Antepartum Hemorrhage Notesabuka.felixBelum ada peringkat
- Ectopic Pregnancy 2022 Edited 3Dokumen40 halamanEctopic Pregnancy 2022 Edited 3apule geraldhumbleBelum ada peringkat
- 10 Abnormal Umbilical CordDokumen30 halaman10 Abnormal Umbilical CordImam SuryaBelum ada peringkat
- 5f.antepartum HemorrhageDokumen31 halaman5f.antepartum HemorrhageWadhha AlsenaidiBelum ada peringkat
- APHDokumen25 halamanAPHJeffrinBelum ada peringkat
- Abruptio PlacentaDokumen45 halamanAbruptio PlacentaJosef Kevin ArcillaBelum ada peringkat
- Abruptio Placentae (Case Presentation)Dokumen46 halamanAbruptio Placentae (Case Presentation)Bansot Baltaken100% (3)
- Obstetrics V10 Common Obstetric Conditions Chapter Placenta Previa and Placenta Abruption 1665345717Dokumen17 halamanObstetrics V10 Common Obstetric Conditions Chapter Placenta Previa and Placenta Abruption 1665345717Mauricio Lopez MejiaBelum ada peringkat
- Antenatal Diagnosis of Placenta Accreta: A Review: C. H. ComstockDokumen8 halamanAntenatal Diagnosis of Placenta Accreta: A Review: C. H. Comstockpamela tyas milanaBelum ada peringkat
- Antepartum HaemorrhageDokumen74 halamanAntepartum HaemorrhageApex College of Nursing100% (1)
- Placenta AccretaDokumen84 halamanPlacenta Accretakhadzx100% (2)
- Umbilical Cord ProlapseDokumen6 halamanUmbilical Cord ProlapseJules Cantal100% (3)
- Material For CNEDokumen36 halamanMaterial For CNENidhi SharmaBelum ada peringkat
- 3rd Trimester Bleeding and Postpartum HemorrhageDokumen100 halaman3rd Trimester Bleeding and Postpartum Hemorrhagepeanutbutter ohBelum ada peringkat
- Placenta Accreta: Rose May Formoso BSN 2Dokumen4 halamanPlacenta Accreta: Rose May Formoso BSN 2MayMay AscadoFBelum ada peringkat
- Cord ProlapseDokumen4 halamanCord ProlapseCleta Escabarte Dehlin100% (1)
- Abnormal LabourDokumen21 halamanAbnormal LabourbetablockersBelum ada peringkat
- Abnormalities of PlacentaDokumen9 halamanAbnormalities of PlacentaprembarnabasBelum ada peringkat
- Sacrococcygeal Teratoma - Paediatric Surgery UnitDokumen74 halamanSacrococcygeal Teratoma - Paediatric Surgery UnitOsasumwen OsagieBelum ada peringkat
- Clin TG Abnormalities of The Placenta & CordDokumen13 halamanClin TG Abnormalities of The Placenta & CordTami Selvi100% (2)
- Trans - OB 2 (Placenta Previa & Morbidly Adherent Placenta) PDFDokumen5 halamanTrans - OB 2 (Placenta Previa & Morbidly Adherent Placenta) PDFMary Stephanie Parcon ChongBelum ada peringkat
- Week 3 Previa AbruptioDokumen28 halamanWeek 3 Previa Abruptiomico zarsadiazBelum ada peringkat
- A Case of Vasa Previa Diagnosed PrenatallyDokumen5 halamanA Case of Vasa Previa Diagnosed PrenatallydeadcorpsesBelum ada peringkat
- 2C Orev Compilation TopicDokumen56 halaman2C Orev Compilation TopicPaolo AntonioBelum ada peringkat
- Placenta: DR Nimco A Hassan Obstetrics and GynaecologyDokumen62 halamanPlacenta: DR Nimco A Hassan Obstetrics and GynaecologyMahad Maxamed AxmedBelum ada peringkat
- OB Definition of TermsDokumen9 halamanOB Definition of TermsWarrenSandovalBelum ada peringkat
- Acreta 2014Dokumen12 halamanAcreta 2014pshz92Belum ada peringkat
- MechanismDokumen14 halamanMechanismSoumabho ParuiBelum ada peringkat
- Nursing Care of A Woman and Family Experiencing A Postpartal ComplicationDokumen43 halamanNursing Care of A Woman and Family Experiencing A Postpartal ComplicationVincent Maralit MaterialBelum ada peringkat
- Placental PathologyDokumen39 halamanPlacental PathologyconstantinilieBelum ada peringkat
- Cord Prolapse: Presented ToDokumen14 halamanCord Prolapse: Presented ToNirajan MaharaBelum ada peringkat
- Placenta PreviaDokumen5 halamanPlacenta PreviaMelanie GaledoBelum ada peringkat
- Placenta Percreta and UrologistDokumen4 halamanPlacenta Percreta and Urologistcb_cristianBelum ada peringkat
- Pa and PPDokumen23 halamanPa and PPapi-19916399Belum ada peringkat
- Placental AbruptionDokumen7 halamanPlacental AbruptionNavora, Bryle TrixthaneBelum ada peringkat
- Obstructed LaborDokumen41 halamanObstructed LaborHenok Y KebedeBelum ada peringkat
- Antepartum Haemorrhage: Learning ObjectivesDokumen12 halamanAntepartum Haemorrhage: Learning Objectivesياسر كوثر هانيBelum ada peringkat
- Late Pregnancy Bleeding: Kareem Ayman Sultan 200008Dokumen67 halamanLate Pregnancy Bleeding: Kareem Ayman Sultan 200008200008Belum ada peringkat
- Data-Driven 3D Cone Chart For Powerpoint: Sample TextDokumen2 halamanData-Driven 3D Cone Chart For Powerpoint: Sample TextPriyanka GeorgeBelum ada peringkat
- Presentationgo: Lorem Ipsum Lorem Ipsum Lorem Ipsum Lorem IpsumDokumen3 halamanPresentationgo: Lorem Ipsum Lorem Ipsum Lorem Ipsum Lorem IpsumPriyanka GeorgeBelum ada peringkat
- What Is AgileDokumen4 halamanWhat Is AgilePriyanka GeorgeBelum ada peringkat
- What Is A User StoryDokumen2 halamanWhat Is A User StoryPriyanka GeorgeBelum ada peringkat
- Scrum: by Ramya PillaiDokumen48 halamanScrum: by Ramya PillaiPriyanka GeorgeBelum ada peringkat
- Unit-2 (Two) Human Resource PlanningDokumen2 halamanUnit-2 (Two) Human Resource PlanningPriyanka GeorgeBelum ada peringkat
- Aguinis pm3 Tif 07Dokumen15 halamanAguinis pm3 Tif 07Priyanka GeorgeBelum ada peringkat
- HRM KtuDokumen5 halamanHRM KtuPriyanka George100% (1)
- Evaluation of Ectopic Gestation: Clinical PresentationDokumen5 halamanEvaluation of Ectopic Gestation: Clinical PresentationPriyanka GeorgeBelum ada peringkat
- 07ovarian PathologiesDokumen5 halaman07ovarian PathologiesPriyanka GeorgeBelum ada peringkat
- 4 - FX02 PRINCE2 Sample Practitioner Paper - V1.5Dokumen58 halaman4 - FX02 PRINCE2 Sample Practitioner Paper - V1.5Priyanka GeorgeBelum ada peringkat
- Internship Report - EasternDokumen101 halamanInternship Report - EasternPriyanka George75% (4)
- MBA-3rd Sem MDU (OCD) PDFDokumen88 halamanMBA-3rd Sem MDU (OCD) PDFPriyanka George0% (1)
- (Books - Stevenson, Buffa, Aswathapa, Adams or Any OM Book) : Production & Operations ManagementDokumen20 halaman(Books - Stevenson, Buffa, Aswathapa, Adams or Any OM Book) : Production & Operations ManagementPriyanka GeorgeBelum ada peringkat
- POM Module 2 Quality NotesDokumen46 halamanPOM Module 2 Quality NotesPriyanka GeorgeBelum ada peringkat
- 1.who Is The Chief Election Commissioner of India?: Veeravalli Sundaram SampathDokumen10 halaman1.who Is The Chief Election Commissioner of India?: Veeravalli Sundaram SampathPriyanka GeorgeBelum ada peringkat
- Business QuizDokumen54 halamanBusiness QuizPriyanka GeorgeBelum ada peringkat
- TTS 16 80 400 Septic Tank DesingsDokumen16 halamanTTS 16 80 400 Septic Tank DesingsJeffrey James100% (2)
- ACCP-SCCM Critical Care Pharmacy Prep Course 2017 Vol.2 (PDF) WWW - Medicalbr.tkDokumen359 halamanACCP-SCCM Critical Care Pharmacy Prep Course 2017 Vol.2 (PDF) WWW - Medicalbr.tkRoman Lis50% (2)
- 3.3.2.4 Love AnimalDokumen8 halaman3.3.2.4 Love AnimalRina ErnawatiBelum ada peringkat
- HEALTH-TEACHING-PLAN sUGATON EVALDokumen9 halamanHEALTH-TEACHING-PLAN sUGATON EVALPrincess Faniega SugatonBelum ada peringkat
- Effect of A Physiotherapy Program in Women With Primary DysmenorrheaDokumen6 halamanEffect of A Physiotherapy Program in Women With Primary DysmenorrheaPaula RangelBelum ada peringkat
- Fun Games - 1 Min Game 01Dokumen9 halamanFun Games - 1 Min Game 01Purvi ShahBelum ada peringkat
- Body GuideDokumen46 halamanBody GuideBárbara Leite95% (22)
- PrelimDokumen10 halamanPrelimHeide Basing-aBelum ada peringkat
- Research ProposalDokumen3 halamanResearch Proposalapi-446880170Belum ada peringkat
- Approval SheetDokumen10 halamanApproval SheetSpinel Cheyne NirvanaBelum ada peringkat
- The CSI Effect - Google FormsDokumen12 halamanThe CSI Effect - Google FormsZivi DegenBelum ada peringkat
- Bicol Central Academy: Mr. Geo B. AutorDokumen4 halamanBicol Central Academy: Mr. Geo B. AutorGeo AutorBelum ada peringkat
- ErpDokumen31 halamanErpNurul Badriah Anwar AliBelum ada peringkat
- Final Project MSWDokumen57 halamanFinal Project MSWSaurabh KumarBelum ada peringkat
- HypnotherapyDokumen16 halamanHypnotherapyAnonymous lsnDTjvBelum ada peringkat
- Citations Issued Due To COVID-19Dokumen726 halamanCitations Issued Due To COVID-19Maritza NunezBelum ada peringkat
- EO Supporting The Immunization Activities - EditedDokumen2 halamanEO Supporting The Immunization Activities - EditedDem SalazarBelum ada peringkat
- Operation Management ReportDokumen12 halamanOperation Management ReportMuntaha JunaidBelum ada peringkat
- Job Shadowing PresentationDokumen12 halamanJob Shadowing Presentationapi-462381810Belum ada peringkat
- Accuracy of The Demirjian and Willems MethodsDokumen8 halamanAccuracy of The Demirjian and Willems MethodsProfessor T. A. EsanBelum ada peringkat
- Homeopathic Remedy Pictures Alexander Gothe Julia Drinnenberg.04000 1Dokumen6 halamanHomeopathic Remedy Pictures Alexander Gothe Julia Drinnenberg.04000 1BhargavaBelum ada peringkat
- Questionnaire For Stress Management in An OrganizationDokumen8 halamanQuestionnaire For Stress Management in An OrganizationTapassya Giri33% (3)
- Cebu Normal University: Submitted By: DIANA ROSE B. ZAMORASDokumen3 halamanCebu Normal University: Submitted By: DIANA ROSE B. ZAMORASDiana ZamorasBelum ada peringkat
- Ewald Hecker's Description of Cyclothymia As A Cyclical Mood Disorder - Its Relevance To The Modern Concept of Bipolar IIDokumen7 halamanEwald Hecker's Description of Cyclothymia As A Cyclical Mood Disorder - Its Relevance To The Modern Concept of Bipolar IItyboyoBelum ada peringkat
- Dental Trauma - An Overview of Its Influence On The Management of Orthodontic Treatment - Part 1.Dokumen11 halamanDental Trauma - An Overview of Its Influence On The Management of Orthodontic Treatment - Part 1.Djoka DjordjevicBelum ada peringkat
- Administration of PICU Child Health NursingDokumen37 halamanAdministration of PICU Child Health NursingJimcy100% (3)
- (Norma) Guia Fda CovidDokumen14 halaman(Norma) Guia Fda CovidJhovanaBelum ada peringkat
- CPB Online Medical Billing Syllabus - 11th - 4!17!13Dokumen2 halamanCPB Online Medical Billing Syllabus - 11th - 4!17!13Kian GonzagaBelum ada peringkat
- Rules Related Statutes All CodesDokumen150 halamanRules Related Statutes All CodesRod SatreBelum ada peringkat
- Ijtk 9 (1) 184-190 PDFDokumen7 halamanIjtk 9 (1) 184-190 PDFKumar ChaituBelum ada peringkat